Page 1
Mammography and Beyond
A SUMMARY OF A STUDY BY THE INSTITUTE OF MEDICINE
X-ray mammography screening is the current mainstay for early breast cancer detection. It has been proven to detect breast cancer at an earlier stage and to reduce the number of women dying from the disease. However, it has a number of limitations.
These current limitations in early breast cancer detection technology are driving a surge of new technological developments, from modifications of x-ray mammography such as computer programs that can indicate suspicious areas, to newer methods of detection such as magnetic resonance imaging (MRI) or biochemical tests on breast fluids. To explore the merits and drawbacks of these new breast cancer detection techniques, the Institute of Medicine of the National Academy of Sciences convened a committee of experts. During its year of operation, the committee examined the peer-reviewed literature, consulted with other experts in the field, and held two public workshops.
In addition to identifying promising new technologies for early detection, the committee explored potential barriers that might prevent the development of new detection methods and their common usage. Such barriers could include lack of funding from agencies that support research and lack of investment in the commercial sector; complicated, inconsistent, or unpredictable federal regulations; inadequate insurance reimbursement; and limited access to or unacceptability of breast cancer detection technology for women and their doctors. Based on the findings of their study, the committee prepared a report entitled Mammography and Beyond: Developing Technology for Early Detection of Breast Cancer, which was published in the spring of 2001. This is a non-technical summary of that report.
The committee concluded that a great deal of work remains to be done, particularly in the field of cancer markers (the study of biological characteristics, or markers, associated with cancer). This area holds promise, however, for improving the accuracy of breast cancer screening, diagnosis, and prognosis. The committee noted that improved imaging technologies that allow doctors to detect
Page 2
breast abnormalities at an earlier, pre-invasive stage may lead to more overtreatment of women unless the imaging procedures are coupled with molecular marker technology that can determine which abnormalities are likely to spread aggressively and become life-threatening.
The committee provided several suggestions for improving the process of developing new technologies, including government support for the discovery and development of markers associated with breast cancer or breast cancer precursors, more consistent FDA regulations regarding approval of cancer detection devices, and a coordinated approval and coverage assessment scheme for screening tests.
The committee also made several recommendations intended to optimize the use and benefit of the proven technologies that are currently available. Those recommendations include expanding the breast cancer screening program of the Centers for Disease Control and Prevention (CDC) for women without health insurance, studying reimbursement rates for x-ray mammography to determine whether they adequately cover the total costs of providing the procedure, and determining whether there is a current or impending shortage of radiologists trained in breast imaging.
The rationale for these recommendations is summarized in this report.
INTRODUCTION
Breast cancer takes a tremendous toll on women in the United States. Next to skin cancer, breast cancer is the most common cancer in women, and the second leading cause of cancer death in women in the United States (lung cancer is the leading cause of cancer death). Each year invasive breast cancer is diagnosed in 180,000 women, and more than 40,000 women die from this disease. Until research uncovers a way to prevent breast cancer, or to cure all women with the disease regardless of when their tumors are found, the best hope for reducing its toll is early detection when tumors are small and local. Treatment in the early stages is more likely to be effective. Researchers hope that early detection of breast cancer by screening could eventually be as effective in saving lives as the Papanicolau (Pap) smear used for cervical cancer screening ( Figure 1).
The current mainstays for breast cancer detection are regular physical exams by women themselves and their doctors, and annual or biannual x-ray mammogram screening. Monthly breast self-exams by women and regular physical exams of the breast by their doctors are aimed at finding any unusual lumps. Such physical exams, when performed carefully, can detect tumors at a smaller size than they would otherwise be found. But research showing that mammography can reduce the number of women dying from breast cancer is
Page 3
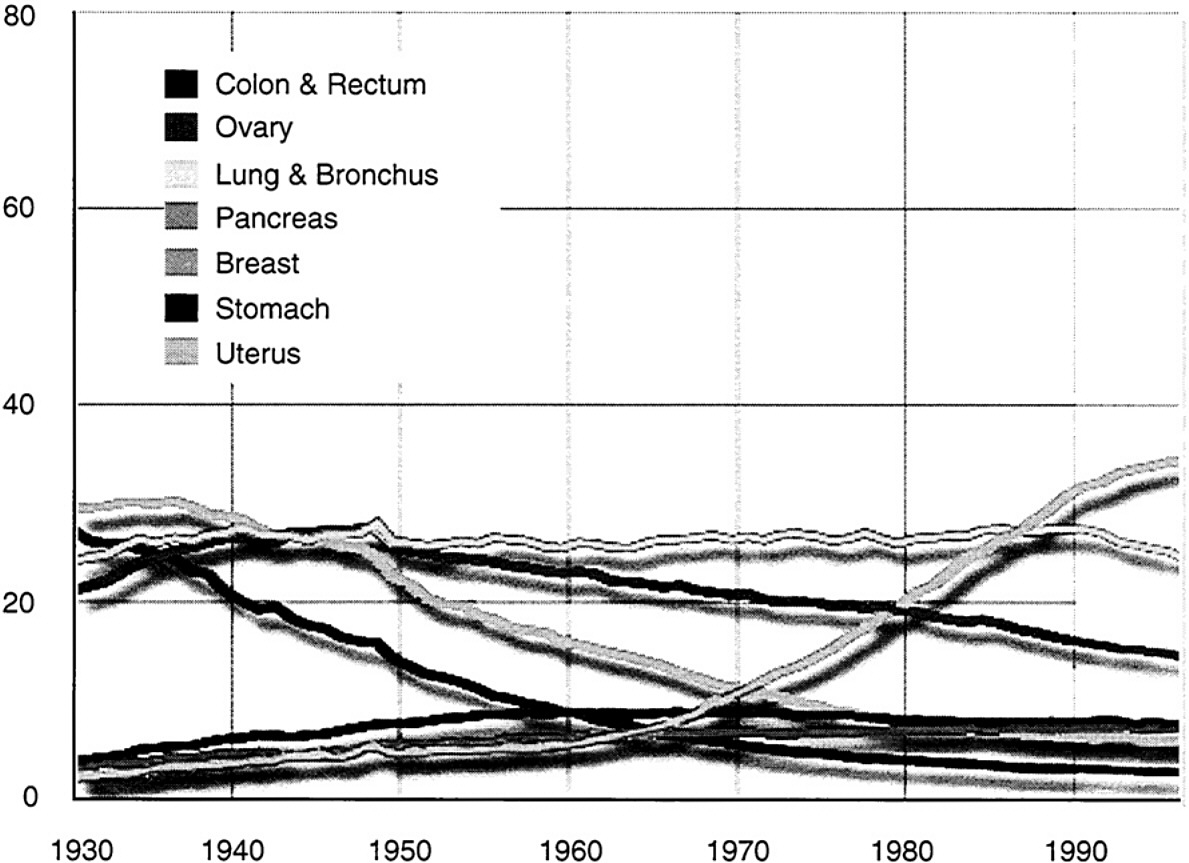
~ enlarge ~
FIGURE 1 Age adjusted cancer death rates, females by site, 1930-1996. Per 100,000, age-adjusted to the 1970 US standard population. Uterus cancer death rates are for uterine cervix and uterine corpus combined. Note: Due to changes in ICD coding, numerator information has changed over time. Rates for cancers of the uterus, ovary, lung & bronchus, and colon & rectum are affected by these coding changes. SOURCE: US Mortality Public Use Data Tapes 1960-1996, US Mortality Volumes 1930-1959, National Center for Health Statistics, Centers for Disease Control and Prevention, 1999; American Cancer Society, Surveillance Research.
much stronger than research for physical breast exams.
With x-ray mammography screening, radiologists examine two x-rays taken of each breast from different angles (mammograms) for abnormalities associated with malignant tumors ( Figure 2). Research reveals that regular mammography screening, when coupled with appropriate treatment, can detect cancer at an earlier stage and reduce the number of women dying from breast cancer.
But mammography is not perfect. Studies have shown that routine mammography screening can reduce the number of deaths from breast cancer by about 25–30% among women between the ages of 50 and 70. A lesser benefit was seen among women aged 40–49. Screening mammography cannot eliminate all deaths from breast cancer because it does not detect all cancers, including some that are detected by physical exam. As many as 15% percent of breast cancers may be missed by mammography screening. Some tumors may also develop too quickly to be identified at the most treatable stage using the standard screening intervals.
In addition, it is technically difficult to consistently produce mammograms
Page 4
of high quality, and interpretation is subjective and can be variable among radiologists. Mammograms are particularly difficult to interpret in women with dense breast tissue, which is especially common in young women. The dense tissue interferes with identification of abnormalities associated with tumors, leading to a higher rate of false test results (both positive and negative) in these women. These difficulties associated with dense tissue are especially problematic for women who wish to begin screening at a younger age because their family history or genetic test results suggest they are at high risk of developing breast cancer.
Mammogram screening also frequently gives inconclusive results, often requiring additional invasive, expensive, and discomforting follow-up procedures, such as surgical biopsies, in which a suspicious area of the breast is removed and examined by a pathologist. As many as three-quarters of such biopsies are negative, that is, they do not reveal the presence of a malignant tumor.
Another limitation of mammography is that the methods for classifying the abnormalities it detects are based on the appearance of the tissue structure ( Figure 3). The ability to determine the lethal potential of breast abnormalities by using this method is crude at best. Because the basic understanding of the biology of breast cancer is not yet complete, some of the breast abnormalities mammography can detect may not be aggressive malignancies requiring intensive treatment, but rather pre-malignant or non-invasive conditions that will not progress to life-threatening disease. Because of this uncertainty, doctors tend to be cautious, treating all such questionable abnormalities as cancers. As a result, some women may be unnecessarily treated for cancer and affected by the psychological distress associated with cancer diagnosis.
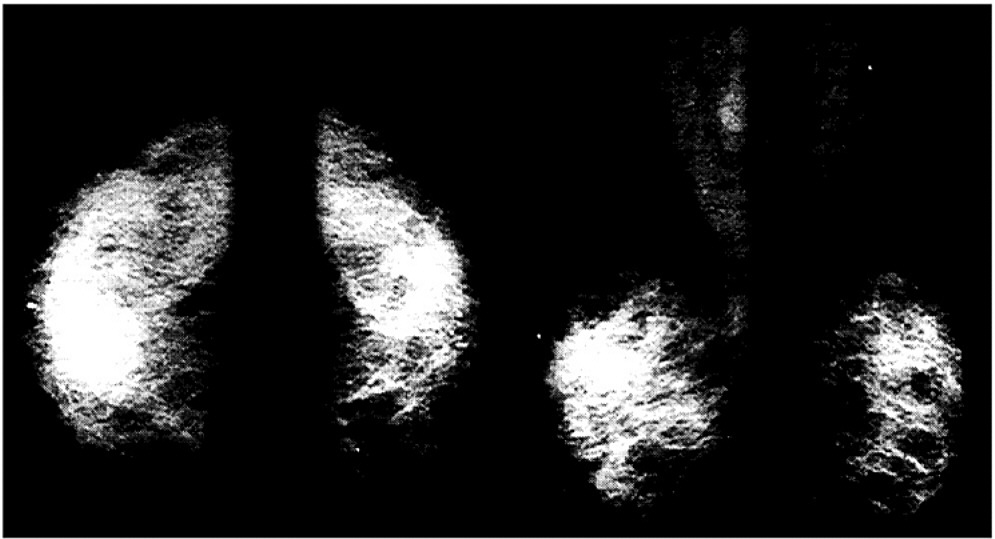
~ enlarge ~
FIGURE 2 An example of conventional x-ray film mammography. SOURCE: Miraluma Educational CD-ROM, Dupont Radiopharmaceutical Division, The DuPont Merck Pharmaceutical Company.
Page 5
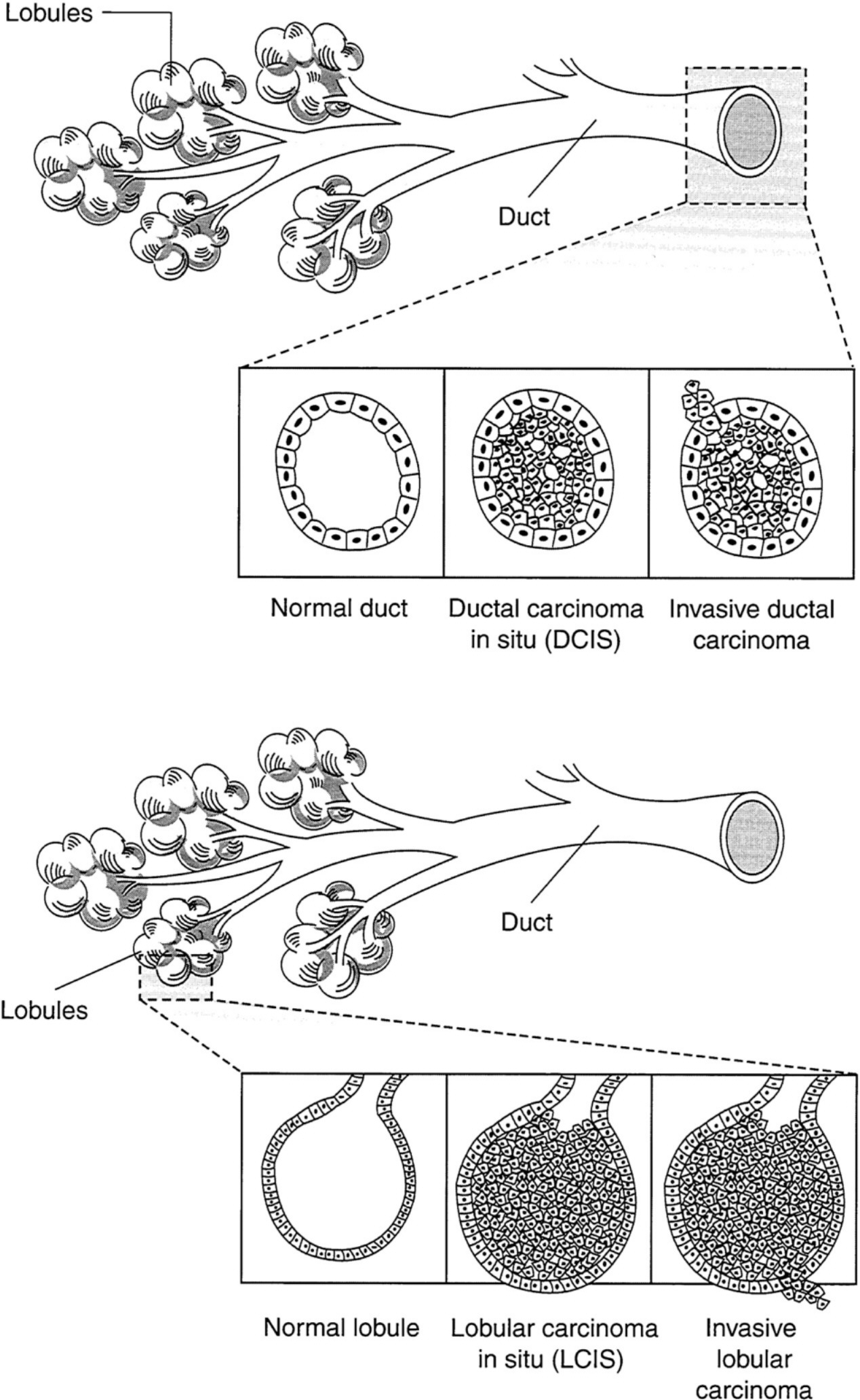
~ enlarge ~
FIGURE 3 Schematic representation of ductal (a) and lobular (b) carcinoma of the Breast (adapted from Love, 1995, p. 220).





