1
Introduction
Imagine opening your morning paper and seeing the headline “Interventions Succeed in Preventing 100,000 Cancer Cases and 60,000 Cancer Deaths Each Year.” Reading further, you learn not only that lives had been saved from cancer but also that remarkable gains had been made in reducing heart disease, diabetes, and other major health threats. Such a promising headline is within reach because prevention interventions are available today that can sharply reduce the future burden of cancer and, at the same time, reduce the risk for other chronic diseases. This report of the National Cancer Policy Board reviews the evidence that such a dramatic impact is possible and calls for a national strategy to ensure that the promise of cancer prevention and early detection is realized.
The National Cancer Policy Board was established in March 1997, at the Institute of Medicine (IOM) and National Research Council to address issues that arise in the prevention, control, diagnosis, treatment, and palliation of cancer. The 21-member Board includes consumers, health care providers, and investigators in several disciplines. In this report, the Board addresses four questions:
-
What lifestyle and health care behaviors contribute to the burden of cancer?
-
What share of new cases of cancer and cancer deaths could be prevented with changes in lifestyle and health care behaviors?
-
What interventions work to bring about health-enhancing behavioral change?
-
What steps can be taken to overcome barriers to using effective interventions and to improve what is known about cancer prevention and early detection?
In the preparation of this report, the Board listened to presentations made by representatives of federal agencies at its quarterly meetings and commissioned six background papers on cancer prevention and early detection.1 Several of the report’s chapters were based on these commissioned papers. The six papers and their authors are as follows:
-
Quantifying the Contribution of Risk Factors to Cancer Incidence and the Estimated Reduction in Cancer Burden Through Selected Risk Factor Modifications, Graham A. Colditz, Catherine Tomeo Ryan, Charles H. Dart III, Geetanjali Datta, Laurie Fisher, and Beverly Rockhill
-
Interventions to Promote Key Behaviors in Cancer Prevention and Early Detection, Edwin B. Fisher, Ross C. Brownson, Amy A. Eyler, Debra L. Haire-Joshu, and Mario Schootman
-
Interventions to Reduce Obesity and Maintain a Healthy Weight, Suzanne Phelan and Rena R. Wing
-
The Effectiveness of Screening for Cancer and Its Unfulfilled Potential in the United States: A Review of the Evidence, Steven H. Woolf
-
Fulfilling the Potential of Lung Cancer Prevention and Early Detection. What Are the Implications of Adopting New Technologies in the Face of Uncertain Science? Parthiv J. Mahadevia, Farin Kamangar, and Jonathan M. Samet
-
Provider, System, and Policy Strategies to Enhance the Delivery of Cancer Prevention and Control Activities in Primary Care, Judith Ockene, Jane Zapka, Lori Pbert, Suzanne Brodney, and Stephenie Lemon
The Board has also drawn on its previous work on tobacco control (IOM, 1998, 2000a) and has benefited from other recent IOM reports relating to behavior and health (IOM, 2001a,b, 2000b,c, 1999a,b) and by prevention-related reports of the President’s Cancer Panel (President’s Cancer Panel, 1998, 1994).
FRAMEWORK OF THE REPORT
The Board chose to focus its attention on opportunities to fulfill the potential of cancer prevention and early detection in light of current epidemiological knowledge and evidence regarding the effectiveness of interven-
|
1 |
Copies of the commissioned papers are available at the National Cancer Policy Board website, www.IOM.edu/ncpb. |
tions to reduce cancer risk. The Board recognized that a number of personal behaviors are known to contribute to the burden of cancer but limited its review of primary prevention to tobacco use, physical activity, obesity, diet, and alcohol use. Examples of behaviors known to contribute to cancer risk but not considered in this review include exposure to sun, and exposure to cancer-causing viruses through sexual activity (e.g., human papillomavirus) and blood contacts such as intravenous drug use (e.g., hepatitis B virus). The Board elected to focus on factors that are risks for common cancers and that also have a large impact on the incidence of other major diseases, including cardiovascular disease, stroke, diabetes, and osteoporosis. Other important areas of prevention, for example, chemoprevention, were excluded from this report, but will likely be the subject of future Board work. Cancer screening modalities are reviewed in some detail and a case study on lung cancer screening is presented to illustrate issues related to adoption of new, yet unproven, technology. As described in detail below, the report’s chapters provide reviews of the evidence regarding the associations between the selected health behaviors and cancer, interventions to bring about improvements in health behaviors, and opportunities to improve the delivery of preventive services and improve population health.
Chapter 2 examines estimates of the reductions of cancer incidence and mortality rates that are achievable through major favorable shifts in the distribution of modifiable risk factors in the U.S. population such as smoking, physical activity, and dietary practices and through increased rates of adherence to cancer screening recommendations.
Chapter 3 summarizes evidence regarding the links between the following five lifestyle behaviors and cancer: tobacco use, physical inactivity, overweight and obesity, poor diet, and alcohol use.
Chapter 4 examines how individual behaviors can be changed through direct services or via community-based approaches such as worksite- or school-based programs or public education campaigns. The chapter also reviews current evidence on the effectiveness of behavioral and educational interventions to promote four key behaviors in cancer prevention: nonsmoking, healthy diet, physical activity, and healthy weight.
Chapter 5 reviews the principles of assessing the effectiveness of screening for cancer and summarizes evidence of the effectiveness of screening for colorectal cancer, breast cancer, prostate cancer, and cervical cancer.
Chapter 6 identifies challenges inherent in systems of care and interventions to improve the rates of participation in cancer screening programs.
Chapter 7 presents a case study on screening for lung cancer to illustrate the dilemma of decision making in the face of uncertain science.
Chapter 8 reviews the status of professional education and training in cancer prevention and early detection with a focus on primary care providers.
Chapter 9 describes selected federal programs that support cancer prevention and early detection through the development of national objectives
and guidelines, information dissemination, surveillance, facilitation of statewide program planning and evaluation, and provision and payment for services.
Chapter 10 surveys ongoing health services research that addresses cancer prevention and early detection and that is sponsored by selected federal agencies and private organizations.
Chapter 11 summarizes the key findings and presents the Board’s recommendations for action by the U.S. Congress, the states, health care providers and systems of care, and the public at large.
This chapter provides background information on the burden of cancer and defines the terms cancer prevention and early detection as used in this report.
THE BURDEN OF CANCER
Cancer ranks second only to heart disease as the leading cause of death in the United States (Table 1.1) (Anderson, 2001). The rates of death from cancer began to fall in the U.S. about 10 years ago (Figures 1.1 and 1.2), but
TABLE 1.1 Deaths and Percent of Total Deaths for Leading Causes of Death by Sex: United States, 1999
|
|
Males |
Females |
||||
|
Cause of death |
Ranka |
Deaths |
% of total deaths |
Ranka |
Deaths |
% of total deaths |
|
All causes |
— |
1,175,460 |
100.0 |
— |
1,215,939 |
100.0 |
|
Diseases of heart |
1 |
351,617 |
29.9 |
1 |
373,575 |
30.7 |
|
Malignant neoplasms |
2 |
285,832 |
24.3 |
2 |
264,006 |
21.7 |
|
Cerebrovascular diseases |
3 |
64,485 |
5.5 |
3 |
102,881 |
8.5 |
|
Accidents (unintentional injuries) |
4 |
63,535 |
5.4 |
7 |
34,325 |
2.8 |
|
Chronic lower respiratory diseases |
5 |
62,415 |
5.3 |
4 |
61,766 |
5.1 |
|
Diabetes mellitus |
6 |
31,150 |
2.7 |
5 |
37,249 |
3.1 |
|
Influenza and pneumonia |
7 |
27,718 |
2.4 |
6 |
36,012 |
3.0 |
|
Intentional self-harm (suicide) |
8 |
23,458 |
2.0 |
— |
5,741 |
0.5 |
|
Chronic liver disease and cirrhosis |
9 |
17,115 |
1.5 |
— |
9,144 |
0.8 |
|
Nephritis, nephrotic syndrome and nephrosis |
10 |
17,016 |
1.4 |
9 |
18,509 |
1.5 |
|
Alzheimer’s disease |
— |
13,391 |
1.1 |
8 |
31,145 |
2.6 |
|
Septicemia |
— |
13,395 |
1.1 |
10 |
17,285 |
1.4 |
|
aRank based on number of deaths. — Category not applicable. SOURCE: Anderson (2001). |
||||||
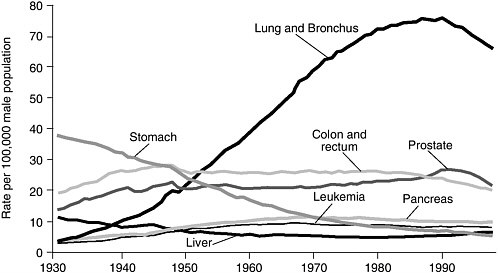
FIGURE 1.1 Age-adjusted cancer death rates,* for males by site, U.S. 1930– 1997.
*Per 100,000, age-adjusted to the 1970 standard population.
NOTE: Due to changes in ICD coding, numerator information has changed over time. Rates for cancers of the liver, lung and bronchus, and colon and rectum are affected by these coding changes. Data obtained from U.S. Mortality Public Use Data Tapes 1960–1968, U.S. Mortality Volumes 1930–1959, National Center for Health Statistics, Centers for Disease Control and Prevention, 2000.
SOURCE: ACS, 2002a.
cancers still account for 23 percent of all deaths in this country (Anderson, 2001). In 2002 cancers claimed the lives of an estimated 555,500 Americans (ACS, 2002a) (Table 1.2). For every 100,000 persons in the United States, cancer claims an estimated 1,747 years of life before age 75 (National Center for Health Statistics, 2001). Estimates are that, on average, each individual who dies of cancer loses 15 years of expected life (Ries et al., 2002).
As demonstrated in Table 1.2, in 2002 lung, breast, prostate, and colon cancer accounted for roughly half of all new cancer cases and half of all deaths due to cancer (ACS, 2002a). Accordingly, the burden due to these four cancers must be reduced if total cancer incidence and mortality rates are to be affected.
The lifetime probability2 of developing cancer is 43 percent for males
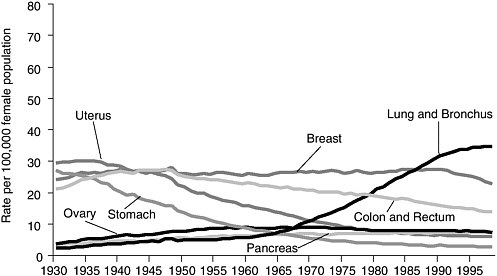
FIGURE 1.2 Age-adjusted cancer death rates,* for females by site, U.S. 1930–1997.
*Per 100,000, age-adjusted to the 1970 standard population.
NOTE: Due to changes in ICD coding, numerator information has changed over time. Rates for cancers of the liver, lung and bronchus, and colon and rectum are affected by these coding changes. Data obtained from U.S. Mortality Public Use Data Tapes 1960–1968, U.S. Mortality Volumes 1930–1959, National Center for Health Statistics, Centers for Disease Control and Prevention, 2000.
SOURCE: ACS, 2002a.
and 38 percent for females (ACS, 2002a). The stresses that cancer imposes on society and the health care system are formidable. The American Cancer Society estimates that 1.3 million new cases of invasive cancer were diagnosed in 2002 (Table 1.2) (ACS, 2002a). Each year, the United States spends an estimated $56.4 billion in direct medical costs caring for patients with this disease. In addition, there is an estimated $100.3 billion cost associated with lost productivity due to illness or premature death (ACS, 2002a).
The estimated 8.9 million Americans alive today with cancer (Ries et al., 2000b) suffer considerable morbidity as well as risk for premature mortality. Both the disease itself and its treatment can diminish quality of life. Patients may be burdened with pain and other physical symptoms, anxiety and depression, decreased functional status, disrupted life routines, impaired well-being, disability, overwhelming medical bills, and the many ordeals of obtaining treatment. Family members, friends, and other caregivers who aid in the coping process may also suffer from the disease. Cancer is thus an affliction that touches the lives of most Americans.
Certain members of the population face a disproportionate burden
TABLE 1.2 Estimated Number of New Cancer Cases and Cancer Deaths in the United States, 2002
from cancer. The incidence of most cancers increases with age, making elderly individuals the group most burdened by cancer. The majority (58 percent) of new cases of cancer occur among those age 65 and older (Ries et al., 2002). For women the risk of dying from cancer is increasing, mainly because of the increasing incidence of lung cancer among women.
Cancer is the leading cause of death among women ages 35 to 64 (National Center for Health Statistics, 2001). Like age and sex, family history is another risk factor that cannot be modified but that is an important indicator of increased susceptibility.
Cancer incidence is correlated with adverse socioeconomic conditions, which affect the lives of many Americans. In the United States, people are more likely to die from cancer if they are poor, have limited education, or both. For example, the probability that a 65-year-old man will die from lung cancer is 547.9/100,000 if his annual family income is less than $10,000, but the risk decreases to 273.6/100,000 if his annual family income exceeds $25,000 (National Center for Health Statistics, 1998). Certain racial and ethnic groups in the United States, African Americans in particular, are at substantially higher risk for cancer (Table 1.3).
There are many differences in host susceptibility, lifestyle, the environment, and health modifiers that are independently associated with each of these demographic factors, and the complex interrelationships among these factors have not been fully described to account for the racial and ethnic disparities in cancer risk (Berkman and Kawachi, 2000).
African Americans are more likely than the rest of the population to suffer morbidity and die from cancer (Table 1.3). The rate of mortality from cancer among African Americans is 33 percent greater than that among whites (218.2/100,000 and 164.5/100,000, respectively) (ACS, 2002a). The fact that health outcomes are worse in certain populations also has multifaceted explanations, some of which include documented disparities in access to and the quality of health care (Berkman and Kawachi, 2000; Smith, 1998). For certain populations cancers are more advanced at diagnosis, partly because the individuals in those populations have less exposure to screening services, as documented later in this report. African Americans are less likely than whites to be diagnosed with cancer at a localized stage and, for each stage of diagnosis for almost every cancer, African Americans have lower 5-year survival rates than whites (Table 1.4) (Greenlee et al., 2001; Ries et al., 2000a). The failings of the health care system are only part of the explanation for these disparities. Personal health behaviors, biological factors, adherence to treatment, and a complex sociological and environmental milieu are interwoven factors contributing to morbidity and death from cancer.
Cancer is characterized by abnormal cell growth; but it is really more than 100 different diseases, each with a unique profile in terms of the
TABLE 1.3 Incidence and Mortality Ratesa by Site, Race, and Ethnicity, United States, 1992–1998
|
Incidence |
White |
Black |
Asian/Pacific Islander |
American Indian |
Hispanicb |
|
All Sites |
|||||
|
Males |
470.4 |
596.8 |
327.7 |
227.7 |
319.7 |
|
Females |
354.4 |
337.6 |
252.1 |
186.3 |
237.7 |
|
Total |
401.4 |
445.3 |
283.4 |
202.7 |
270.0 |
|
Breast (female) |
115.5 |
101.5 |
78.1 |
50.5 |
68.5 |
|
Colon & rectum |
|||||
|
Males |
51.4 |
57.7 |
47.3 |
33.5 |
35.2 |
|
Females |
36.3 |
44.7 |
31.0 |
24.6 |
23.2 |
|
Total |
42.9 |
50.1 |
38.2 |
28.6 |
28.4 |
|
Lung & Bronchus |
|||||
|
Males |
69.6 |
107/2 |
51.9 |
44.3 |
36.0 |
|
Females |
43.6 |
45.7 |
22.7 |
20.6 |
18.7 |
|
Total |
54.7 |
71.6 |
35.5 |
31.0 |
26.0 |
|
Prostate |
144.6 |
234.0 |
82.8 |
47.8 |
103.4 |
|
Mortality |
White |
Black |
Asian/Pacific Islander |
American Indian |
Hispanicb |
|
All Sites |
|||||
|
Males |
203.2 |
297.7 |
125.6 |
125.3 |
128.8 |
|
Females |
138.0 |
166.6 |
82.4 |
90.8 |
84.3 |
|
Total |
164.5 |
218.2 |
101.2 |
105.4 |
102.6 |
|
Breast (female) |
24.3 |
31.0 |
11.0 |
12.4 |
14.8 |
|
Colon & rectum |
|||||
|
Males |
20.6 |
27.3 |
12.9 |
11.9 |
13.0 |
|
Females |
13.9 |
19.6 |
8.9 |
8.9 |
8.0 |
|
Total |
16.8 |
22.8 |
10.7 |
10.3 |
10.2 |
|
Lung & Bronchus |
|||||
|
Males |
67.8 |
96.2 |
33.8 |
41.8 |
30.5 |
|
Females |
34.6 |
33.6 |
15.1 |
20.9 |
10.9 |
|
Total |
48.8 |
59.1 |
23.3 |
30.1 |
19.3 |
|
Prostate |
22.4 |
53.1 |
9.8 |
14.0 |
15.9 |
|
aPer 100,000, age-adjusted to the 1970 U.S. standard population. bHispanic is not mutually exclusive from white, black, Asian/Pacific Islanders, and American Indian. NOTE: Incidence data are from NCIS 11 SEER areas; mortality data are from the National Cancer Center for Health Statistics and include all states, except data for Hispanics. Data for Hispanics include deaths that occurred in all states except Connecticut, Louisiana, New Hampshire, and Oklahoma. SOURCE: ACS, 2002a. |
|||||
population at risk, symptoms, and prognosis. As cancers of the lung, breast, prostate, and colon together make up more than half of all new cancer cases, they are important targets for prevention. Invasive cervical cancer is a less common cancer among women, in large part because of the application of effective screening programs (NIH, 1996).
TABLE 1.4 Five-Year Relative Survival Rates, by Racial or Ethnic Group and Stage at Diagnosis, United States, 1989–1996
Lung Cancer
After deaths due to heart disease and stroke, cancer of the lung and bronchus is the third leading cause of death in the United States and is the leading cause of cancer deaths (National Center for Health Statistics, 1998), estimated to claim 154,900 lives in 2002 (ACS, 2002a). With 169,400 new cases expected in 2002, cancer of the lung and bronchus is also the third most common cancer, following prostate cancer in men and breast cancer in women. Lung cancer has one of the poorest prognoses of all cancers, with a 5-year survival rate of only 14 percent (Ries et al., 2000a). The lifetime probability of developing lung cancer is 1 in 12 for males and 1 in 17 for females. Lung cancer trends have followed tobacco use trends by 10 to 20 years. The incidence of lung cancer in males began to decline in the 1980s, but the rate has been increasing in females, only recently beginning to stabilize, a trend attributed to past increased rates of tobacco use by women. These tragic consequences of tobacco use among women were first manifest in 1987, when lung cancer replaced breast cancer as the leading cause of cancer deaths in women, now accounting for an estimated 25 percent of cancer deaths in females (ACS, 2002a). Most lung cancer deaths (87 percent) can be attributed to tobacco use (ACS, 2002b).
As noted earlier, the rate of mortality from lung cancer is higher in low-income persons (National Center for Health Statistics, 1998). The incidence of cancer of the lung and bronchus is considerably higher in African Americans (71.6/100,000) than in whites (54.7/100,000), as are mortality rates from cancer of the lung and bronchus (59.1/100,000 versus 48.8/ 100,000, respectively). Hispanics, Asians and Pacific Islanders, and American Indians have lower incidences of lung cancer and lower rates of mortality from lung cancer than African Americans and whites (Table 1.3) (ACS, 2002a).
Breast Cancer
Breast cancer is the most commonly diagnosed cancer in women, accounting for an estimated 203,500 new cases in 2002, or about 31 percent of all new cancers in women. The lifetime probability of developing breast cancer is 1 in 8. An estimated 39,600 women died of breast cancer in 2002 (ACS, 2002a).
The risk of breast cancer increases with age and a family history of breast cancer. Up to 20 percent of women in the general population have a family history of breast cancer, but less than 5 percent of women are at high risk for hereditary breast cancer syndromes (Warner et al., 1999). A variety of susceptibility genes, the most well known being BRCA1 and BRCA2, substantially increase the risk of developing breast cancer, but such mutations occur in a relatively small proportion of the general population.
Women who carry mutations in these genes face a 48 to 74 percent probability of developing breast cancer by age 80 (Anglian Breast Cancer Study Group, 2000). Other risk factors include a personal history of breast cancer, biopsy-confirmed atypical hyperplasia, a long menstrual history (menstrual periods that started early and ended late in life), nulliparity or having a first child after age 30, postmenopausal obesity, and higher socioeconomic status. Use of oral contraceptives, prolonged use of hormone replacement therapy, and increased alcohol intake have also been suggested as risk factors for breast cancer. Although breast cancer is more common in white women (115.5/100,000) than in African-American women (101.5/ 100,000), the mortality rate is lower for white women (24.3/100,000) than for African-American women (31.0/100,000) (Table 1.3) (ACS, 2002a).
Prostate Cancer
Prostate cancer is the most common cancer among men in the United States (excluding basal and squamous cell skin cancer), accounting for 189,000 new cases in 2002, or approximately 30 percent of all newly diagnosed cancers in men. The lifetime probability of developing prostate cancer is 1 in 6. The incidence of prostate cancer increased sharply from 1988 to 1992, a phenomenon attributed to increased rates of screening (Potosky et al., 1995), but the incidence has declined in subsequent years (ACS, 2002a). An estimated 30,200 men are expected to die of prostate cancer in 2002, making it the second most common cause of death from cancer in men (ACS, 2002a).
The risk of prostate cancer increases with age. More than 70 percent of diagnoses occur after age 65. A family history of prostate cancer modestly increases risk (ACS, 2002a). Prostate cancer is considerably more common in African-American men (234.2/100,000) than in white men (144.6/100,000), and is less common in Hispanics (103.4/100,000), Asians and Pacific Islanders (82.8/100,000), and Native Americans (47.8/ 100,000) (Table 1.3). African Americans have the highest prostate cancer incidence rates and death rates in the world (Parkin et al., 1997). Similar disparities exist with regard to the rate of mortality from prostate cancer (Table 1.3) (ACS, 2002a).
Colorectal Cancer
Colorectal cancer is the third most common cancer in the United States, accounting for an estimated 148,300 new cases in 2002. The lifetime probability of developing colorectal cancer is 1 in 17 for men and 1 in 18 for women. The disease is more common in African Americans than whites. Between 1992 and 1998, the incidence rate of colon cancer was approxi-
mately 42.9/100,000 in whites and 50.1/100,000 in African Americans (ACS, 2002a).
The American Cancer Society estimates that 56,600 Americans died of colorectal cancer in 2002, making it the second most common cause of death from cancer. Rates of mortality from colorectal cancer are higher for African Americans (22.8/100,000) and whites (16.8/100,00) than for Hispanics, Asians and Pacific Islanders, and Native Americans (10.2 to 10.7/ 100,000) (Table 1.3) (Greenlee et al., 2001).
A personal history of colorectal polyps, or chronic inflammatory bowel disease, or a family history of hereditary colorectal cancer syndrome place individuals at higher risk for colorectal cancer (ACS, 2002a). Approximately 90 percent of all colorectal cancer cases and deaths are thought to be preventable, through dietary or other lifestyle changes in conjunction with screening (ACS, 2002a).
Cervical Cancer
Decades ago, cervical cancer was a common cause of death from cancer, but the mortality rate has fallen significantly: 40 percent since 1973 (Agency for Health Care Policy and Research, 1999), a trend largely attributed to routine screening for cervical cancer by cytological examination (Pap smear). Nonetheless, an estimate of 13,000 new cases of invasive cervical cancer occurred in 2002 (ACS, 2002a). The lifetime probability of developing cervical cancer is 1 in 117. Largely through successes in early detection and treatment, cervical cancer currently accounts for only 2 percent of cancer deaths in women, with 4,100 deaths from cervical cancer estimated to occur in 2002 (ACS, 2002a). Cervical cancer is now considered a sexually transmitted disease, mediated by exposure to human papillomavirus. Infection with this virus is the most important risk factor for the disease. Other risk factors include onset of sexual intercourse at an early age, multiple sexual partners (or sex with individuals who have had multiple sexual partners), and cigarette smoking.
DEFINITIONS OF CANCER PREVENTION AND EARLY DETECTION
Primary Prevention
The most desirable strategy for the amelioration of suffering from cancer is primary prevention, a public health approach which keeps people from acquiring cancer in the first place. Unfortunately, the fundamental etiologies of cancer are not fully understood, making a definitive strategy for primary prevention elusive. Epidemiological data shed insights on potentially modifiable risk factors associated with certain cancers (e.g., expo-
sure to tobacco, obesity, a diet low in fruits and vegetables, excessive alcohol intake, workplace carcinogens), but the quality and consistency of the evidence regarding the precise causal roles of these factors in carcinogenesis are mixed (see Chapter 3). Nonetheless, healthier lifestyles and reduced levels of exposure to carcinogens offer great promise as effective means of reducing the incidence of cancer.
Chief among these is avoiding the use of tobacco, which accounts for an estimated 30 percent of cancer deaths in the United States (ACS, 2002b). Helping the 23.5 percent of adults who smoke cigarettes (ACS, 2002b) discontinue their habit and preventing youth from adopting the habit of tobacco use will save more lives than the sum of all the incremental benefits of improving cancer screening rates or cancer treatments. Other primary preventive strategies also offer promise. One-third of cancer deaths are thought to be related to nutrition and other lifestyle factors including body weight, physical activity, and food choices (Byers et al., 2002).
Secondary Prevention
Until the ability to prevent the occurrence of cancer (primary prevention) becomes a reality, a complementary strategy is secondary prevention, the early detection of cancer through screening. The fundamental tenet of screening for cancer is that detection of the disease before symptoms develop enables detection at a less advanced stage and that the institution of treatment before symptoms develop will produce improved health outcomes. Although this syllogism seems intuitive and is widely assumed to be true by both health professionals and the lay public, the value of early detection is not proven for many cancers (see Chapter 5).
Tertiary Prevention
While not the topic of this report, tertiary prevention involves limiting disability and providing rehabilitation when disease has already occurred and left residual damage (Mausner and Kramer, 1985). The National Cancer Policy Board has a study in progress, Cancer Survivorship: Improving Care and Quality of Life After Treatment, that will address issues related to tertiary prevention. The Board addressed issues related to symptom control and end-of-life care in its report, Improving Palliative Care for Cancer (Institute of Medicine, 2001d).
Health Promotion
Major stages in the evolution of public health have been described as addressing first, communicable diseases, and second, chronic, noncommu-
nicable diseases. Some suggest that society has entered a third “public health revolution” with a focus on advancing health, with health defined following the World Health Organization’s formulation, as “physical, mental and social well-being, not merely the absence of disease and infirmity” (Breslow, 1999, p. 1031). The term health promotion is often coupled with that of disease prevention and has been defined as “the process of enabling people to increase control over, and to improve their health” (Breslow, 1999, p. 1030). The concept of health promotion has emerged, in part, because of increases in longevity and time spent without significant disability. Health promotion then “seeks the development of community and individual measures which can help people to develop lifestyles that can maintain and enhance the state of well-being” (Breslow, 1999, p. 1030). The concept of health promotion underlies many of the approaches to reducing the risk of cancer among individuals and populations.
SUMMARY AND CONCLUSIONS
In 2002 an estimated 1.3 million new cases of cancer were diagnosed and over half a million deaths were due to cancer. Cancer is a diverse set of conditions, but just four cancers contribute disproportionately to cancer’s toll, accounting for half of all newly diagnosed cases and deaths: cancers of the lung and bronchus, breast, prostate, and colon and rectum. Especially burdened by cancer are individuals who are elderly and socially and economically disadvantaged. Members of certain minority groups including African Americans are also more likely than others to suffer morbidity and die from cancer. Primary prevention through elimination of risk factors such as smoking and poor nutrition is the most effective way to reduce the burden of cancer. Secondary prevention, the early detection of cancer at its most treatable stage, can also be effective for selected cancers. The remainder of this report reviews recent progress and current opportunities for primary and secondary prevention of cancer in the United States.















