APPENDIX H
PROGRESS IN PEDIATRIC PALLIATIVE CARE IN NEW YORK STATE—A DEMONSTRATION PROJECT
James P. Donnelly, Ph.D,* Susan M. Huff, R.N., MS,† Michael L. Lindsey, Ph.D.,‡and J. Donald Schumacher, Psy.D.§
In May of 2000, the Health Care Financing Administration (HCFA) announced the initiation of a demonstration program in pediatric palliative care. The program was the result of several years of discussion, advocacy, and negotiation involving representatives of government, focus groups, and task forces, led primarily by Children’s Hospice International (CHI). The primary goal of the demonstration program is to promote the implementation and testing of the “PACC model.” “PACC,” which stands for Program of All-Inclusive Care for Children, is the pediatric palliative care model developed by CHI. The PACC model is described in detail in several CHI publications (e.g., Children’s Hospice International, 2002) and on the CHI web site (http://www.chionline.org ). The PACC model may be considered a descendant of the PACE model (Program of All-Inclusive Care for the Elderly) (Department of Health and Human Services, 1999). The PACE model was developed and tested under the auspices of HCFA in the 1980s. Both models include comprehensive, interdisciplinary support for people with life-limiting illness, but the PACC model includes critical features specific to the pediatric population.
The initial appropriation for development and testing of the Program of All-Inclusive Care for Children was $1 million for fiscal year 2000. Five states submitted proposals that were ultimately accepted for funding: Florida, Kentucky, Utah, Virginia and New York. In 2001, a second request for proposals was released, resulting in continuation of funding for the original five projects along with the addition of a project in Colorado. It is anticipated that a third year of demonstration project funding will be available in 2002. The demonstration projects have common goals of developing model programs in their states; identifying and overcoming administrative, technical, political, and other barriers to implementation; and providing evidence of cost-effectiveness. The demonstration projects may explore a range of public and private options for program financing, but development of Medicaid waiver applications that will support expanded coverage of services will be attempted by all of the projects.
New York state’s PACC demonstration project builds on a long-standing and well-regarded program in pediatric palliative care, the Essential Care program (ECP). The ECP is administered by the Center for Hospice and Palliative Care (CHPC) in Buffalo, New York, and has been providing end-of-life (EOL) care for children and families since 1988. The Essential Care program was viewed as a strong starting point for a demonstration project in the state of New York in that the strengths of the program could be documented while adding to the knowledge base both locally and in the field.
BRIEF DESCRIPTION OF THE ESSENTIAL CARE PROGRAM
The history of the Essential Care program has taken place under three administrative structures: an inpatient hospice, a children’s hospital, and currently, a more comprehensive hospice that includes a home care agency. This history reflects the complexity of sustaining an organizational base for a population that has often “fallen between the cracks.” The program has faced repeated challenges in financing but has also accumulated a wealth of clinical and administrative experience. The initial clinical experience generated some important insights about the needs of the population.
Among the key experiential lessons was the observation that parents did not want to admit their child into “hospice” and wanted to maintain hope for extended longevity. It was also evident that children and families wanted to be at home as much as possible but needed a unique network of support services to do so. Those services included counseling and other support for the well children in the family. Returning the locus of family life to the home meant that “normalization” of family life could become a realistic goal.
Physicians’ views were equally clear: They would not in most cases
certify that a child had a life expectancy of six months or less, and they were hesitant to abandon all curative treatment. They wanted to remain as active caregivers to these children and not relinquish care to a hospice physician.
It was evident that an ideal program should include all the benefits and services consistent with the hospice philosophy, without the Medicaid rules related to life expectancy and forgoing curative treatment. Thus, the need for Medicaid waivers and other approaches to creating earlier and more flexible access to palliative-type services was apparent to the Essential Care team. In the absence of substantial insurance coverage, financial support has until now included an emphasis on foundations, grants, and local fund raising. Program growth in recent years has been accompanied by parallel challenges in supporting program activities that are not reimbursed under current regulations. An upper limit on nonreimbursed costs may be imminent, threatening continued growth of the program, and might be discouraging to anyone studying the feasibility of beginning new programs in the current economic environment.
In the last three years, the average daily census has increased 85%. The current average daily census is 45, with about 30 new children admitted per year with an average length of stay of approximately 8.5 months. The average number of deaths per year is about 13, with 80% occurring at home, as most families prefer. In the 14-year history of the program, more than 350 families have been cared for. If a child’s disease goes into remission and home care services are no longer necessary, a graduation ceremony ensues. Approximately 25% of admissions eventually graduate, and half of those are readmitted and cared for until death. Thus, about one of every eight children served by the Essential Care program ultimately experiences long-term remission and cure.
While in the program, each patient receives nursing, social work, and child-life services, in addition to support from the primary physician or physician specialist. A variety of supplementary services are available, tailored to individual family situations. An overview of each care specialty is given in Addendum H.1. This set of services is quite consistent with the PACC model specifications (CHI, 2002, p. 42).
Third-party payers have played an important part in recognition of this program model. Partnerships with two local health maintenance organizations have been established since the inception of the program. In Table H.1, a breakdown of insurance coverage over the last three years is presented. Blue Cross and Blue Shield and the Independent Health Association have recognized the importance of this program model. Throughout the years they have been very generous in approving nursing visits to accommodate patient needs in the home. They recognize it is cost-effective to keep patients home and out of the acute setting. They have also been the first to approve counseling and other support services for the parents and siblings
TABLE H.1 Essential Care Pediatric Program Primary Insurance Mix in Past 36 Months (N = 124)
|
Primary Insurance |
No. of Patients |
Percentage |
|
Blue Cross/Blue Shield |
41 |
33.06 |
|
Commercial |
21 |
16.94 |
|
Independent Health Association |
39 |
31.45 |
|
Medicaid |
35 |
28.23 |
|
Total |
136a |
109.68 |
|
aThere were 12 primary insurance changes during this period, accounting for 136 primary insurance cases in the 124 families. |
||
in the home. Traditional CHHAs (certified home health agencies) do not readily approve social work visits in the home, and child life is not recognized anywhere in the country as a reimbursable discipline. Both of these health maintenance organizations recognize the importance of the expertise in pediatrics and supportive needs of parents and siblings. They are reimbursing child life under the social work code and giving our program approval for home visits. This does not account for all of the home visits that both of these disciplines make, although it is a start.
NEW YORK’S DEMONSTRATION PROJECT IN YEAR ONE
New York’s approach to the demonstration project builds on the Essential Care program but also involves a network of statewide partnerships. These include the parent organization of the Essential Care program, the Center for Hospice and Palliative Care (CHPC), as well as the New York State Department of Health (DoH), and the Hospice and Palliative Care Association of New York State. The co-principal investigators of the grant are program officers in the Department of Health. The DOH has also provided consultation on many program planning and grant activities and has taken a leadership role in the study of costs and the creation of the Medicaid waiver application. The state hospice association has been very involved in coordinating advisory group activities and the statewide conference. The network of cooperation has extended to many other organizations through the New York State Advisory Group on Pediatric Hospice and Palliative Care. Establishment of the advisory group was one of the first-year goals of the project. Other objectives of the demonstration project in the first year were to
-
evaluate the cost of services and develop a methodology to calculate service costs on a statewide basis;
-
add necessary program components to complete the PACC model within Essential Care;
-
conduct a needs assessment in New York state; and
-
conduct a statewide education program in collaboration with the New York State Hospice Association on how to develop a comprehensive pediatric palliative care service, thus stimulating the generalization of the PACC model in the rest of the state.
A chronology of demonstration project activities is provided in Table H.2. The table includes basic information on events leading to the demonstration project and a detailed list of project activities in year 1 followed by a summary of goals for the second year.
TABLE H.2 Chronology of the New York State PACC Demonstration Project
|
Year |
Event |
|
|
Pre-Demonstration Project Events |
||
|
1988 |
Essential Care program established |
|
|
1997–1999 |
PACC model created by CHI Task Force |
|
|
1998 |
Essential Care program becomes part of the Center for Hospice and Palliative Care |
|
|
Demonstration Project Events |
||
|
2000 |
Demonstration Project Grant application submitted |
|
|
November |
Grant activities commence |
|
|
2001 |
January |
New York State Advisory Committee formed |
|
January |
CHI demonstration project conference |
|
|
March |
Listserv established for advisory committee |
|
|
April |
Quality-of-Life measure collaboration initiated |
|
|
March–December |
Cost assessment designed and conducted |
|
|
Year |
Event |
|
|
|
June–August |
Web-based needs assessment with professionals |
|
June–July |
Annotated bibliographies developed on communication regarding life threatening illness and QoL. |
|
|
July |
Seminar on communication held with Essential Care program staff |
|
|
July–August |
Communication study conducted |
|
|
July–August |
Videotaped case studies with families conducted |
|
|
September–November |
Conference on Development of Pediatric Palliative Care Programs held in Albany, NYa |
|
|
November |
Preliminary cost analysis suggests need for actuarial consultant |
|
|
Anticipated Project Events |
||
|
2002 |
|
Expand needs assessment sample to include children and families. |
|
Develop standardized needs assessment for community and family level assessment |
||
|
Develop 1115 Medicaid waiver application |
||
|
Continue development of methods for generalizing the Essential Care program to other areas in the state |
||
|
Continue collaboration on development of QoL measures |
||
|
aThe conference was begun as scheduled on September 11, but rescheduled and held on November 1 because the day’s events precluded completion of the conference. |
||
PROGRAM COSTS AND MEDICAID WAIVER APPLICATION DEVELOPMENT
The development of a federal 1115 Medicaid waiver is one of the expected outcomes of this demonstration project. The underlying logic for such a waiver is to remove the “six months until death” regulation and thus
get children with life-threatening diseases into palliative care at a much earlier stage of their disease. The demonstration, however, must illustrate that the costs associated with children in the program are not generally expected to be higher than the costs of those children receiving traditional program services.
Health Department staff collaborated with CHPC staff to develop a methodology for comparing Medicaid costs of children in the CHPC program with the costs of children outside the program. Because the health problems of chronically and terminally ill children are complex, our initial attempts at cost comparisons were inadequate. Building upon our experiences in year 1, we intend to devote our efforts in year 2 to developing a methodology for calculating costs in a much more sophisticated manner. To support this effort in the second year of the project, an actuarial firm has been consulted and will develop the financial analysis and models needed to support the waiver application in 2002.
The primary goals of the actuarial analyses will be to calculate the cost of care for Medicaid children with life-threatening conditions in the most accurate way possible and to compare the cost of care for Medicaid children in the Essential Care program with the costs of care of a clinically matched group of Medicaid children outside the Essential Care program. In order to achieve these goals, the actuarial organization will obtain Medicaid claims data that will include claims histories for children who died with selected diagnoses. These claims histories will include service utilization, dates of service, and diagnostic and clinical detail that will enable the analyst to develop cost estimates for these children at various stages of their disease. Using these data and comparable data from the Essential Care program, the analyst will be able to precisely compare the costs of care for children treated within the Essential Care program with those of clinically identical children outside the program at various stages of their illness.
COMMUNICATION
Communication in the context of palliative and hospice care for children is at once extremely important and extremely challenging. In the absence of a program of all-inclusive care such as Essential Care, discussions within families and between families and care providers about issues related to a child’s condition are typically rare and conducted under the most stressful of circumstances around a medical crisis. A hallmark of the Essential Care program is regular discussion of issues related to the child’s and family’s well-being with trusted professionals throughout the course of care. The extensive experience of the Essential Care program staff results in communication that balances complex issues and dynamics related to family and individual functioning, disease status, and prognosis. The approach
might be characterized as similar to Bluebond-Langner’s (1996) recommended strategy of “shuttle diplomacy,” in which care is taken to assess the readiness of family members for discussion of topics. The goal of this strategy is to find a balance between respecting the individual’s and family’s desire to carry on normal life by focusing on topics other than illness and the potential benefits of open discussion of critical issues.
Since the demonstration project in New York is based on an existing program, goals were developed to document communication within the program and to compare Essential Care communication practices with models available in the literature. Our literature review on the topic of communication of threatening information in both medical and nonmedical circumstances was followed with a presentation to the Essential Care team. An annotated bibliography was then made available for members of the team. Based on this review, as well as a review of evaluation research methods, it was concluded that case studies would be productive both in advancing understanding about communication within the Essential Care program, and in documenting the nature of communication as an outcome of the demonstration project.
Two levels of case study have been conducted in the first year, and described in the following:
-
Chart Reviews. A coding form to analyze the frequency of communication about ten key issues was developed. The coding form was based on the analysis of literature on communication as well as the clinical expertise of the Program Director and grant researcher. The fifty most recently closed cases were chosen for study. Two trained doctoral students in psychology who had been hired to assist with the project over the summer of 2001 reviewed each chart. The range of EoL conversations in this sample was zero to 51, with a mean of 15.5. The three most frequent topics were prognosis, fear of future, and death/dying/grief. The frequency of discussion of the ten topics is shown in Figure H.1. Additional results of the review were presented at the educational conference and will be included in a separate manuscript.
-
Video Case Studies. The first aspect of Tobin’s (1999) model is recognition of “the individuality of the disease and choice.” Video documentaries may be one of the most effective means of capturing the individuality of the child and family. Videotaped interviews with patients, family members and staff members involved in one ongoing case and one closed case were conducted. The tapes were transcribed and studied by a committee that included the program director, the grant researcher, the director of public relations at the CHPC, a CHPC graphic artist, and an experienced television producer. The goal of the video case studies was to capture the individual story of the patient, family, and program interaction. The tapes
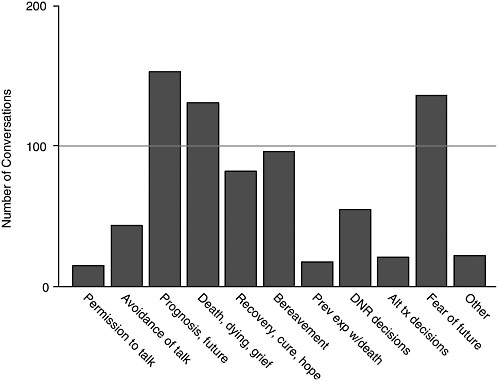
FIGURE H.1 Relative frequency of various topics documented in Essential Care charts.
-
will be used in professional education and in local program marketing efforts.
Another application of the video case studies is to code segments by the items in the needs assessment and then create interactive concept maps in which the needs statements are illustrated by video clips. For example, the following comment could be used to illustrate the importance of home-based care. This comment was made by the mother of a 2-year-old boy who died at home with the support of the Essential Care program. She was commenting on her perception of how the program helped her and her family:
The biggest difference I would have to say is the week that we had him home. They made it possible. That week was the most precious week we had with him. They made it possible for him to have time at home after a couple weeks in the hospital with all of the hustle and bustle there—to come home, have a quiet home, special family time. They made it possible to have these pumps available here—to have that family together again one more time. Because Bryce knew we weren’t going to have it anymore.
And it was so important to get out of that hospital setting . . . to have him home, and they made it possible.
Two case studies were completed in the first project year; additional studies may be completed depending on funding. One case involves a family whose young child died after battling an aggressive form of cancer (cited above). The second involves a family with two children diagnosed with incurable neurologic disease that follows a relatively slower course. The interviews include patients, parents, and staff members, and include specific focus on communication in the context of care.
The case studies may be continued in a variety of ways. One way in which the chart study might be continued would be to identify how economic costs might be affected by communication as well as direct quality-of-life (QoL) benefits. The video case studies could be extended to other cases illustrating other issues in pediatric palliative care. We hope to create a set of 10 cases or so that would provide excellent material for research as well as training of palliative care professionals.
PATIENT AND FAMILY NEEDS ASSESSMENT
As of this writing there are no comprehensive, quantitative reports of needs assessments of children or families of children with life-limiting illness in the available literature. Contributing factors may include the complexity of the issues, the traditional focus in health care on adult problems, and perhaps the fact that this is an area that has generated more emotional than behavioral (action) responses in our country. The New York state demonstration project included provisions for a needs assessment to be conducted in conjunction with the cooperating stakeholder groups: the Essential Care program; the New York State Advisory Committee on Pediatric Palliative Care and its parent organization, The Hospice and Palliative Care Association of New York State; the New York State Department of Health; other experts invited by the advisory committee; and families who are currently caring or have previously cared for a child with a life threatening illness.
The specific goals and methodology of the needs assessment were developed in a series of meetings and Listserv discussions with representatives of all stakeholder groups. The discussion that follows outlines the methods and preliminary results of the needs assessments along with discussion of the limits of the analysis and follow-up plans.
Methodology
The grant team reviewed numerous possible approaches to needs assessment. The following issues were identified as critical in the planning of
the assessment: (1) scope of needs assessment, (2) sample and participants, and (3) fit of method to scope and sampling.
The scope was defined as the needs of children with life-limiting illness and the families of children with life-limiting illness in New York state. The sampling strategy of the study was defined at three levels:
-
the New York State Children’s Palliative Care Advisory Group,
-
the professional networks of experts in children’s palliative care needs beginning with the advisory group and extending to colleagues throughout the state, and
-
the children and families who have experienced treatment for a life-limiting illness. (This third level of the assessment is to be undertaken in 2002.)
The statewide scope and sampling considerations lead to consideration of Web-based assessment methods with the ultimate choice of a method known as Concept Mapping (Trochim, 1989).
Briefly, Concept Mapping (CM) is a systematic approach to tapping the shared expertise of a group and constructing statistically based graphic models of the areas examined by the group. There are typically six steps in the process, and they are described in detail by Trochim (1989). Compared with focus group methods, CM provides a more rigorous statistical basis for modeling needs, including multidimensional scaling and cluster analysis. The statistical procedures guide the analyst in producing the most valid and reliable representation of the data. Human judgment is not removed from the process, however, and is critical in the cluster analysis and the interpretation of the resulting maps. The CM analysis may typically include a variety of follow-up studies, several of which are being planned presently in New York. The present discussion of the needs assessment is intended to stimulate and support the efforts of new groups as they consider the issues involved in conceptualizing and measuring the complex needs of children and their families.
Procedures
Phase 1: Brainstorming on Child and Family Needs
The first phase of the study was accomplished by the use of two Web pages, one devoted to brainstorming the needs of children with life-limiting illness, and the second focused on the needs of the families of children with life-limiting illness. Initially, the members of the New York State Advisory Committee were invited to participate in the brainstorming. This was fol-
lowed by invitations to colleagues of advisory committee members. The same procedure was followed for the family needs assessment.
Phase 2: Structuring the Needs Statements
The statements generated in the brainstorming phase were edited for the occurrence of duplicates and for clarity. The statements were then added to a database on the Concept Systems server, and new Web pages were constructed. The members of the advisory committee were assigned user names and passwords in order to participate in the sorting and rating of the statements. Committee members were instructed to log on to the site and first complete a free sort of the items. The sorting allowed each person to establish piles of similar items and to name the piles.
Following the sorting, committee members were asked to rate each item as to relative importance and feasibility. The importance was rated on a 1 to 5 scale of which 1 represented “relatively unimportant” and 5 represented “extremely important.” The feasibility ratings also ranged from 1 to 5, with 1 representing “not feasible” and 5 representing “already being done.”
They were also asked to complete demographic items identifying their professional specialty, years of work with the population, work setting, county of residence, and whether or not they had ever had a child member of their immediate family diagnosed with a life-threatening condition. Twelve members of the committee contributed usable data by completing all of the tasks. The needs rating phase was then extended to colleagues, just as the brainstorming in Phase 1 had been.
Results1
The brainstorming on children’s needs resulted in 74 unique needs statements contributed by 50 experts in pediatric palliative care. The complete list of children’s needs is presented in Addendum H.2. The brain-storming on family needs produced 63 unique statements from 40 individual experts in pediatric palliative care throughout New York state. The list of family needs statements is given in Addendum H.3.
The statistical analysis proceeded in two major steps. The first step was to submit the sorting data to a two-dimensional nonmetric multidimensional scaling (MDS) analysis. (All analyses were completed using The Concept System, Version 1.751.) The MDS analysis combined all of the
separate sorts, resulting in a two-dimensional representation of all of the statements. An X–Y value for each statement defines its position on the map, with items closer to one another representing more similar constructs and those further apart reflecting less similar ideas. The MDS results were then examined in a hierarchical cluster analysis. The cluster analysis involved an iterative process in which each possible solution from 20 to 3 clusters was examined for interpretability and statistical indicators of adequacy of the solution. In the following section, the results of the concept mapping of children’s needs are presented.
Children’s Needs
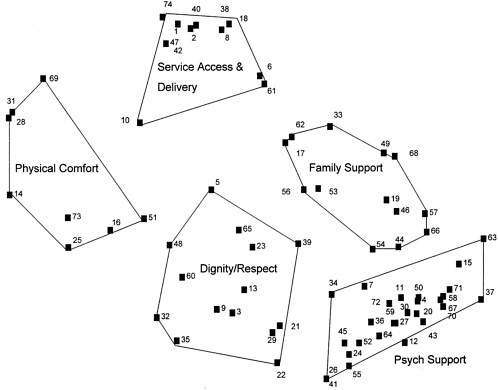
Of the 17 possible solutions examined, several provided interesting arrangements of the children’s needs, but the five-cluster solution appeared best in terms of interpretability and parsimony. The five-cluster map includes the following needs: (1) dignity–respect; (2) physical comfort; (3) psychological support; (4) family support; and (5) system access and delivery. The five-cluster map, with the individual items labeled by statement number is presented in Addendum H.4.
-
Dignity–respect. The central cluster in the concept map of children’s needs includes such items as, “honesty,” “maintaining a sense of self,” “to be valued as an individual by having preferences solicited and acted upon to the extent reasonable,” “privacy,” “confidentiality,” and “culturally sensitive care.” These items reflect core aspects of human dignity, which are often included in humanistic accounts of end-of-life processes such as Tobin’s, Peaceful Dying (Tobin, 1999) but are rarely if ever included in QoL measurement models. The relatively central location of the cluster is also significant because it indicates that this cluster is the one that is most closely related to all other clusters. Thus, the dignity–respect cluster is informative not only in suggesting core needs of children, but also in a theoretical sense. This map suggests that dignity and respect deserve attention from program planners and evaluators as central aspects of a child’s life that should receive explicit attention in program planning and evaluation.
-
Physical comfort. Meeting the physical comfort needs of children with life-limiting illnesses is widely acknowledged as a primary goal of palliative care. In fact, the definition of the term “palliation” or “palliative care” suggests this set of needs more than any other. In the New York state assessment, the two items with the highest importance ratings were “effective pain management” and “consistent pain assessment” (the average rating for both items was 5.0 on a scale in which 5 indicated “most impor-
-
tant”). Other items in this cluster reflected needs for information related to such care and to active patient participation.
-
Psychological support. In our statewide study, more than one-third of the needs statement generated by the experts reflect psychological functioning. The items included a number of important needs that all children have, such as “love,” “access to peers,” and “fun.” The majority of statements were specific to children with life-limiting illness such as “to be reassured that he or she is important and will be remembered” and “pleasant distractions from the situation.” The items in this cluster also included those needs related to spirituality, such as “prayers” and “spirituality in their care.” In practice, program planners may want to consider these as a separate dimension in the assessment of individual child and family needs.
-
Family support needs. The fourth cluster included needs related to maintenance of family functioning, including home-based child-life services and sibling support. There were also a number of items that reflected the need for the child’s access to family when hospitalized and for as much care as possible to be delivered in the home. This set of needs will vary with the individual family circumstances (e.g., geographic proximity to treatment, number of siblings). One item called for “family-focused care,” which might also serve as a general theme for this cluster of needs.
-
Service system access and delivery. One of the prime motivations of all of the demonstration projects is to contribute to the expansion of service system access and delivery. It was not surprising to find that one of the clusters of the needs assessment involves these same issues. Among the items included in the assessment were those related to access policies (“access to palliative care benefit from the time of diagnosis without a time constraint” and “reduction of barriers imposed by the six-month limit of the hospice benefit”) and more programmatic issues such as “ability for nurse practitioners or doctors to make home visits,” “ability to transition in and out of the hospital as needed,” and “competent pediatric-trained professional caregivers.” Thus, new programs must consider system factors in terms of who will have access under what circumstances and what services shall be delivered in which settings.
Children’s Needs Importance Ratings
The next step in the analysis involved examination of the statement and cluster ratings. Ratings were completed by 40 professionals in pediatrics, including members of the state advisory group and colleagues invited personally by members of the advisory group. Of the 10 highest-rated individual needs statements, four were in the comfort needs cluster, two were in the dignity–respect cluster, two were in the psychosocial cluster, and two were in the service system access and delivery cluster. The analysis of the
importance ratings revealed a limited response range, with most of the needs statements being rated at the high end of the scale. This finding suggests that all needs are at least somewhat important, and the task of discriminating relative importance in this area is a difficult one at the population level. Individual differences may still occur in the assessment of children and family needs on a case basis, however.
In addition to the relative importance of each need statement, experts were asked to rate the feasibility of meeting each need given current policies and resources. As with the importance ratings, the highest rated items in terms of feasibility reflected dignity–respect and comfort needs (Addendum H.4). This may be seen as good news, in that dignity–respect and comfort needs are highly rated in terms of importance. However, at the other end of the feasibility scale are many of the system delivery and access needs. This is not surprising, since it is difficult to change systems, and indeed the justification for the demonstration projects has much to do with generating data to support system changes.
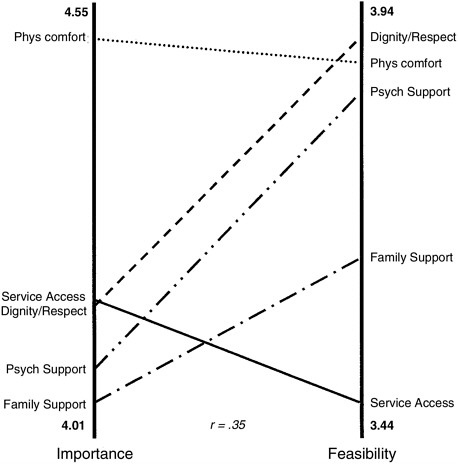
Pattern matching is an analysis that allows comparison of two rating scales. In order to identify the degree to which importance and feasibility are congruent, a pattern match graph was generated (Addendum H.5). The graph shows that comfort needs are both highly important and highly feasible in terms of service delivery. Other clusters in the ladder graph show less congruence, resulting in an overall correlation of 0.35. Future applications of pattern matching include analysis of the degree to which needs are perceived as having been met by palliative programs.
In the second year of the demonstration project, the needs assessment will be extended to include responses from children and families. The sampling of children and families is intended to first assist with validation of the needs model and items. Secondly, we will test interview and self-report versions of the needs assessment. When the assessment has been piloted with families, it will be made available throughout the state and to other demonstration projects.
Longer-term uses of the needs assessment data include integrating the results into a descriptive program model and a testable program theory. The descriptive model will be used to illustrate the relationship of needs, services, and outcomes within the Essential Care program. The program theory will include testable propositions about the effectiveness of specific program activities in meeting the needs of the population. The needs model may also be adapted for use in studies designed to estimate the number of children and families, as well as the greatest areas of need, to be included in expanded Medicaid coverage. This could be accomplished by creation of a survey that could be conducted in local communities or statewide with the support of an organization such as the Hospice and Palliative Care Association of New York State. In addition, the needs assessment could be part of
a program evaluation design. Finally, the assessment can be translated into clinical practice via development of a standardized assessment instrument used in treatment planning.
QUALITY OF LIFE
Assessment of health-related quality of life has been one of the fastest growing areas in heath psychology and medicine. Yet most of the activity in this field has focused on adult populations. In the pediatric area, there are as yet no well-accepted measures of quality of life for children and families in pediatric palliative or hospice care. Measurement of patient and family satisfaction is already standard practice in the Essential Care program; thus, the focus of the research activity has been patient and family quality-of-life.
We conducted a literature review and found that there are no currently available measures of QoL for the population. We also identified the leading research teams in the world in pediatric QoL assessment. One of the most active and productive research teams is the group led by Jim Varni, Ph.D., at the Center for Child Health Outcomes in San Diego (Varni et al., 1999a,b; 1998). The team has produced a well-developed measurement system known as the PedsQL. Dr. Varni’s research team is currently developing a module for assessment of quality of life for children in palliative care, to be known as the PedsQL Palliative Care Module. We have agreed to collaborate in the development and testing of the measure. At this writing our San Diego colleagues are in the process of obtaining institutional review board approval to collect data with the pilot module. We will then coordinate pilot testing of the measure with colleagues throughout the state via the advisory committee.
REFERENCES
Bluebond-Langner M (1996). In the shadow of illness. Princeton, NJ: Princeton University Press.
Children’s Hospice International (2002). PACC Implementation Manual. Alexandria, VA: Children’s Hospice International.
Department of Health and Human Services (1999). Medicare and Medicaid Programs of All-Inclusive Care for the Elderly (PACE). Retrieved April 8, 2002, from http://www.hcfa.gov/medicaid/pace/pacereg.pdf.
Health Care Finance Administration (2000). Solicitation announcing a children’s hospice grant opportunity. Retrieved January 22, 2002, from http://www.hcfa.gov/medicaid/chi6800.htm.
Tobin DR (1999). Peaceful dying. Cambridge, MA: Perseus.
Trochim W (1989). An introduction to concept mapping for planning and evaluation. In: Trochim W, ed. Evaluation and Program Planning, 12:1–16.
Varni JW, Katz ER, Seid M, Quiggins DJL, Friedman-Bender A (1998). The Pediatric Cancer Quality of Life Inventory-32 (PCQL-32): I. Reliability and validity. Cancer82:1184– 1196.
Varni JW, Seid M, Kurtin PS (1999a). Pediatric health-related quality of life measurement technology: A guide for health care decision makers. Journal of Clinical Outcomes Management6:33–40.
Varni JW, Seid M, Rode CA (1999b). The PedsQL: Measurement model for the Pediatric Quality of Life Inventory. Medical Care37:126–139.
ADDENDUM H.1
DESCRIPTION OF SERVICES PROVIDED BY ESSENTIAL CARE PROGRAM BY DISCIPLINE
Nursing
-
Oversees coordination of disciplines and patient care in the home
-
Provides skilled nursing visits, case management in the home, coordination of home visit schedules
-
Shares on-call responsibilities
Social Work
-
Works directly with the parents or the child’s primary caregiver
-
Addresses concrete social issues, financial issues related to the disease; offers community resource referrals
-
Serves as a patient and family advocate
-
Provides counseling related to parenting and spousal communication
-
Facilitates empowerment in parents and family, advocates for choices in caregiving
-
Addresses anticipatory loss and grief issues, assists with funeral planning, and transition to bereavement program
-
Facilitates spiritual care resources (pastoral care or coordinating with the family’s community spiritual support)
Child Life
-
Assesses responses and needs of children to health care experiences
-
Attempts to minimize stress and anxiety for the sick child and siblings in home
-
Prepares children for health care experiences such as medical events or invasive procedures
-
Provides experiences to foster growth, development, self-esteem and independence
-
Facilitates developmentally appropriate play and interaction at home and in the acute care setting
Physicians
-
Physicians are available for consultation on an outpatient basis and will conduct home visits when necessary
-
The Essential Care medical director provides consultation services, including
-
Attendance at weekly team meetings
-
Program admission consultation
-
Consultation and liaison to child’s primary physicians
-
Availability for home visits when necessary
Pastoral Care
-
Pastoral care is offered in the hospital and is available at home.
Art and Music Therapy
-
This is available on a per diem basis at home for children.
Psychology
-
Consultations are available on an outpatient basis.
Allied Therapy
-
Physical therapy, occupational therapy, speech, and nutrition consultation are available at home and in the acute setting.
Home Health Aides
-
Utilized as needed to supplement home care services
Volunteers
-
Utilized to support the family and program staff through a variety of activities including baby-sit siblings, cook and clean for families, run errands, provide transportation for clinic visits or for families to visit the child while he or she is hospitalized
Ancillary Services
-
Services include outpatient lab blood work done in the home setting and pharmacy services at home
-
Durable medical equipment and supplies are available as needed
-
Physical therapy, occupational therapy, speech, nutritional counseling are available at home
Supplementary Services
-
Day care. Essential Care does not provide day care, however, volunteers do provide families with babysitting and short-term respite at home, and community resources are accessed for longer term arrangements
-
Support groups are available for children and their families who are facing the impending loss of a loved one and for those children who have suffered the death of a sibling, parent or grandparent
-
Long distance needs. Ronald McDonald House and/or Kevin Guest House (Buffalo, New York) are available and utilized when necessary for family traveling into Buffalo from out of town
-
Respite. Comprehensive respite services may be developed as part of the demonstration project in future years.
ADDENDUM H.2
CHILDREN’S NEEDS STATEMENTS WITH IMPORTANCE RATINGS
|
28) |
Effective pain management |
5.00 |
|
31) |
Consistent pain assessment |
5.00 |
|
10) |
Comforting atmosphere with pain control |
4.91 |
|
32) |
Quality of life |
4.91 |
|
26) |
Prayers |
4.73 |
|
43) |
Love |
4.73 |
|
69) |
Accurate assessment and effective treatment of pain and non-pain symptoms |
4.73 |
|
74) |
Reduction of barriers imposed by the six-month limit of the hospice benefit |
4.73 |
|
1) |
Access to palliative care benefit from the time of diagnosis without a time constraint (such as the hospice regulation) |
4.55 |
|
3) |
Honesty |
4.55 |
|
14) |
Clear, developmentally appropriate explanations of care options, benefits and burdens |
4.55 |
|
29) |
To maintain a sense of self |
4.55 |
|
51) |
The right to say no |
4.55 |
|
60) |
Comfort |
4.55 |
|
73) |
To have a say in the treatment plan |
4.55 |
|
19) |
Unlimited access to family, as desired by the child |
4.45 |
|
20) |
Fun |
4.45 |
|
24) |
To be reassured that he or she is important and will be remembered |
4.45 |
|
53) |
Family-focused care |
4.45 |
|
9) |
To be clearly valued as an individual by having preferences solicited and acted upon, to the extent reasonable |
4.36 |
|
15) |
Opportunities to be cared for by loving family |
4.36 |
|
21) |
Sense of control over life or some aspects of it |
4.36 |
|
47) |
Competent pediatric-trained professional caregivers |
4.36 |
|
49) |
As much time at home as possible (and as little time in the hospital) |
4.36 |
|
63) |
Parents who are mentally healthy and functional under stress |
4.36 |
|
2) |
Coordinated health care provided in a timely, convenient, and pleasant environment |
4.27 |
|
6) |
Consistency in professional caregivers throughout the illness, including the end stage |
4.27 |
|
11) |
Talk about their feelings and fears |
4.27 |
|
33) |
Flexibility to receive care wherever it is safe |
4.27 |
|
48) |
Assessment of personal goals of care |
4.27 |
|
52) |
Knowing he or she won’t be forgotten and will still be loved, talked to, and visited even after death |
4.27 |
|
68) |
Being able to remain in familiar surroundings with familiar people |
4.27 |
|
71) |
Continuity of “normal life” within their family, school, faith or social community, and circle of friends |
4.27 |
|
7) |
To address fears with a competent professional |
4.18 |
|
8) |
Not spending hours and hours in clinics and waiting rooms |
4.18 |
|
17) |
Translators if the child’s first language is not English |
4.18 |
|
34) |
Access to peers |
4.18 |
|
37) |
Parents who are receiving sufficient support so that they can focus on the child and siblings as much as possible |
4.18 |
|
39) |
Privacy |
4.18 |
|
46) |
Child-life intervention in the home |
4.18 |
|
65) |
Confidentiality |
4.18 |
|
5) |
Developmentally appropriate activities and information |
4.09 |
|
25) |
Understandable information about supportive and palliative and hospice care to reduce anxiety and unknowns |
4.09 |
|
27) |
Pleasant distractions from the situation |
4.00 |
|
30) |
Stimulation (via school activity, play, family activities, etc.) |
4.00 |
|
36) |
To acknowledge the sadness of the child and those who love him or her about the illness and possibility of death |
4.00 |
|
41) |
Spirituality in their care |
4.00 |
|
45) |
Focus on the child’s hopes and dreams, including assistance when their hopes and dreams will likely not be met |
4.00 |
|
62) |
Care for the health care provider so that they can care for the children in a more caring and nurturing way |
4.00 |
|
66) |
To have the critical nature of the illness and possibility of death acknowledged |
4.00 |
|
67) |
Regular contact with peers |
4.00 |
|
16) |
Assessment of perceptions of burdens and benefits of care |
3.91 |
|
40) |
The ability to transition in or out of the hospital as needed |
3.91 |
|
35) |
To be physically touched and soothed (e.g., massage) |
3.82 |
|
42) |
More nurses/home health aides who are pediatric trained |
3.82 |
|
58) |
To not feel that the child has caused many other losses for the family (e.g., financial struggles) |
3.82 |
|
59) |
People, things, activities that make the child smile and laugh |
3.82 |
|
12) |
Nonjudgmental love, touch, long talks, looking out a window, feeling the sun |
3.73 |
|
18) |
Being able to give home blood transfusions, especially platelets so the child does not bleed out at home |
3.73 |
|
56) |
Alternative therapies such as art and music |
3.73 |
|
61) |
Nutritional support in the home |
3.73 |
|
64) |
To create a personal legacy |
3.73 |
|
4) |
Laughter for release (e.g., visiting clown programs) |
3.64 |
|
23) |
Culturally sensitive care |
3.64 |
|
54) |
Play therapy that focuses on illness-related topics |
3.64 |
|
70) |
Ability to share with children having same illness in a safe, encouraging environment |
3.64 |
|
72) |
Help with the visual part of the illness so that the child feels as good as possible about his or her body and appearance |
3.64 |
|
13) |
Assessment of preferences and goals for social interaction and facilitation of those preferences and goals |
3.55 |
|
44) |
Peer support groups |
3.55 |
|
50) |
Networking with other children experiencing a similar illness, treatment, etc. |
3.55 |
|
55) |
Assessment of concerns around meaning, loss, and spiritual issues and effective means of addressing these |
3.55 |
|
38) |
Ability for nurse practitioners and doctors to make home visits |
3.45 |
|
22) |
Self-relaxation skills |
3.09 |
|
57) |
Access to a child-friendly Web site for information, chats, etc. |
3.00 |
ADDENDUM H.3
CHILDREN’S NEEDS STATEMENTS WITH FEASIBILITY RATINGS
|
26) |
Prayers |
4.78 |
|
43) |
Love |
4.78 |
|
35) |
To be physically touched and soothed (e.g., massage) |
4.33 |
|
5) |
Developmentally appropriate activities and information |
4.22 |
|
15) |
Opportunities to be cared for by loving family |
4.22 |
|
24) |
To be reassured that he or she is important and will be remembered |
4.22 |
|
28) |
Effective pain management |
4.22 |
|
60) |
Comfort |
4.22 |
|
61) |
Nutritional support in the home |
4.22 |
|
31) |
Consistent pain assessment |
4.11 |
|
36) |
To acknowledge the sadness of the child and those who love him or her about the illness and possibility of death |
4.11 |
|
65) |
Confidentiality |
4.11 |
|
3) |
Honesty |
4.00 |
|
12) |
Nonjudgmental love, touch, long talks, looking out a window, feeling the sun |
4.00 |
|
13) |
Assessment of preferences and goals for social interaction and facilitation of those preferences and goals |
4.00 |
|
20) |
Fun |
4.00 |
|
27) |
Pleasant distractions from the situation |
4.00 |
|
29) |
To maintain a sense of self |
4.00 |
|
30) |
Stimulation (via school activity, play, family activities, etc.) |
4.00 |
|
39) |
Privacy |
4.00 |
|
41) |
Spirituality in their care |
4.00 |
|
53) |
Family-focused care |
4.00 |
|
73) |
To have a say in the treatment plan |
4.00 |
|
7) |
To address fears with a competent professional |
3.89 |
|
11) |
Talk about their feelings and fears |
3.89 |
|
25) |
Understandable information about supportive and palliative and hospice care to reduce anxiety and unknowns |
3.89 |
|
40) |
The ability to transition in or out of the hospital as needed |
3.89 |
|
48) |
Assessment of personal goals of care |
3.89 |
|
51) |
The right to say no |
3.89 |
|
52) |
Knowing he or she won’t be forgotten and will still be loved, talked to, and visited even after death |
3.89 |
|
54) |
Play therapy that focuses on illness-related topics |
3.89 |
|
59) |
People, things, activities that make the child smile and laugh |
3.89 |
|
69) |
Accurate assessment and effective treatment of pain and non-pain symptoms |
3.89 |
|
4) |
Laughter for release (e.g., visiting clown programs) |
3.78 |
|
14) |
Clear, developmentally appropriate explanations of care options, benefits, and burdens |
3.78 |
|
21) |
Sense of control over life or some aspects of it |
3.78 |
|
32) |
Quality of life |
3.78 |
|
34) |
Access to peers |
3.78 |
|
37) |
Parents who are receiving sufficient support so that they can focus on the child and siblings as much as possible |
3.78 |
|
58) |
To not feel that the child has caused many other losses for the family (e.g., financial struggles) |
3.78 |
|
9) |
To be clearly valued as an individual by having preferences solicited and acted upon, to the extent reasonable |
3.67 |
|
10) |
Comforting atmosphere with pain control |
3.67 |
|
19) |
Unlimited access to family, as desired by the child |
3.67 |
|
22) |
Self-relaxation skills |
3.67 |
|
33) |
Flexibility to receive care wherever it is safe |
3.67 |
|
45) |
Focus on the child’s hopes and dreams, including assistance when their hopes and dreams will likely not be met |
3.67 |
|
47) |
Competent pediatric-trained professional caregivers |
3.67 |
|
49) |
As much time at home as possible (and as little time in the hospital) |
3.67 |
|
55) |
Assessment of concerns around meaning, loss, and spiritual issues and effective means of addressing these |
3.67 |
|
56) |
Alternative therapies such as art and music |
3.67 |
|
68) |
Being able to remain in familiar surroundings with familiar people |
3.67 |
|
2) |
Coordinated health care provided in a timely, convenient, and pleasant environment |
3.56 |
|
17) |
Translators if the child’s first language is not English |
3.56 |
|
46) |
Child life intervention in the home |
3.56 |
|
66) |
To have the critical nature of the illness and possibility of death acknowledged |
3.56 |
|
67) |
Regular contact with peers |
3.56 |
|
70) |
Ability to share with children having same illness in a safe, encouraging environment |
3.56 |
|
72) |
Help with the visual part of the illness so that the child feels as good as possible about his or her body and appearance |
3.56 |
|
1) |
Access to palliative care benefit from the time of diagnosis without a time constraint (such as the hospice regulation) |
3.44 |
|
16) |
Assessment of perceptions of burdens and benefits of care |
3.44 |
|
23) |
Culturally sensitive care |
3.44 |
|
44) |
Peer support groups |
3.44 |
|
50) |
Networking with other children experiencing a similar illness, treatment, etc. |
3.44 |
|
57) |
Access to a child-friendly Web site for information, chats, etc. |
3.44 |
|
62) |
Care for the health care provider so that they can care for the children in a more caring and nurturing way |
3.44 |
|
64) |
To create a personal legacy |
3.44 |
|
63) |
Parents who are mentally healthy and functional under stress |
3.33 |
|
8) |
Not spending hours and hours in clinics and waiting rooms |
3.22 |
|
18) |
Being able to give home blood transfusions, especially platelets so the child does not bleed out at home |
3.22 |
|
38) |
Ability for nurse practitioners and doctors to make home visits |
3.22 |
|
71) |
Continuity of “normal life” within their family, school, faith or social community, and circle of friends |
3.22 |
|
6) |
Consistency in professional caregivers throughout the illness, including the end stage |
3.11 |
|
42) |
More nurses/home health aides who are pediatric trained |
3.00 |
|
74) |
Reduction of barriers imposed by the six-month limit of the hospice benefit |
3.00 |