Why Exploiting This Knowledge Will Be Essential to Achieving Health Improvements in the 21st Century
Raynard S. Kington
National Institutes of Health
Dr. Kington began his presentation by noting that projections from 1990 to the year 2050 show a steady decrease in the percentage of the U.S. population that is white and substantial increases in minority populations, particularly Hispanic and Asian. Hispanics, he said, will likely surpass African Americans as the country’s largest minority group well before the middle of this century.
“The reason why [such] changes in composition of the population are potentially important,” Dr. Kington said, “is because there are large differences in health outcomes across these subgroups.” He illustrated these differences. Recent data (covering 1980-1996) show much higher mortality for African Americans than for any other group (the African American mortality rate is about 50 percent higher than that of whites); there is a clustering of mortality rates among non-Hispanic whites, American Indians, and Alaska Natives; and the rates are substantially lower for Hispanics and Asians (see Figure A).
Similarly, 1995 data show that infants born of African American mothers suffer more than twice the mortality rates as those of Hispanics and non-Hispanic whites (which have virtually the same infant mortality rates), and the rates among Asian and Pacific Islanders are yet lower (see Figure B).
“But simplistic slides like that really hide a substantial amount of heterogeneity within the large groups, in particular the Hispanic groups and the Asian American groups,” Dr. Kington said. For example, infant mortal
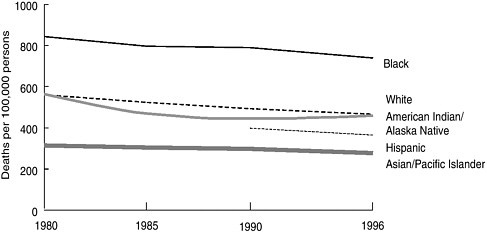
FIGURE A Mortality rates by race, 1980-1996.
ity rates for Puerto Ricans are substantially higher than those of Mexicans, Cubans, and Hispanics from Central and South America (see Figure C).
The reason for large differences in health outcomes among racial and ethnic groups in the United States, he said, “is the list of usual suspects: socioeconomic status, culture/acculturation, health risk behaviors, psycho-
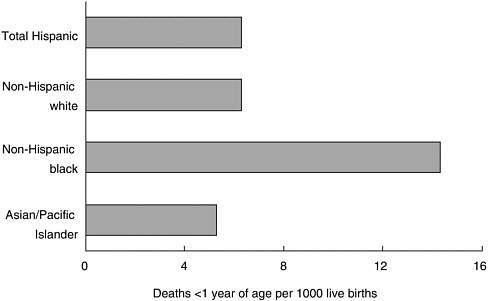
FIGURE B Infant mortality rates by race, 1995.
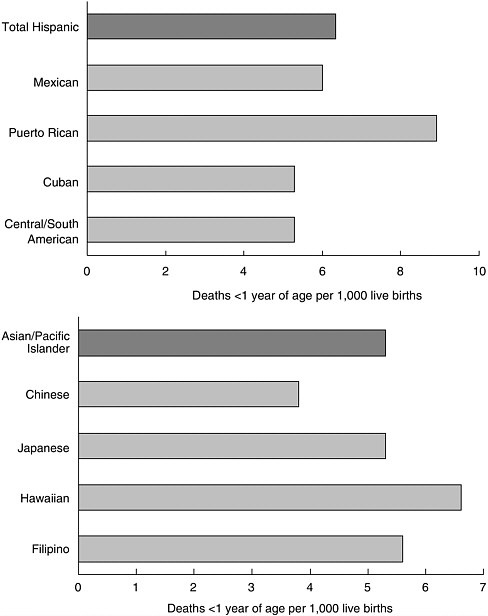
FIGURE C Infant mortality rates by Hispanic subgroup and Asian/Pacific Islander subgroup, 1995.
social factors, health care, biologic genetic factors, and environmental and occupational exposures.” His talk expanded on the first two.
Some of the differences in health outcomes can be largely accounted for by socioeconomic status, Dr. Kington said. For example, “when we just stratify by educational attainment, we see that the mortality rates for those
who have at least some college education is substantially lower than for those who have either just a high school education or have less than a high school education. [The latter group has] almost three times the mortality rate of those who have at least some college.” Similarly, with respect to income, while all groups’ wages increased substantially through the late 1960s and early 1970s, there has been a large spread since then in the changes in wages according to percentile in the population—with those at the lowest percentile having decreases—as well as a widening gap between the incomes of the highest and the lowest.
“The reason why this is relevant for the population at large and particularly relevant for minority populations,” Dr. Kington said, “is because minority populations are overrepresented along that lowest line at the bottom end of the income structure.” For example, over 50 percent of African American and Hispanic children live in households below 150 percent of the poverty line for income. “This is particularly relevant in light of the growing evidence suggesting that early life exposures and health factors set individuals on trajectories that will affect their health status for the rest of their lives.”
Another reason for large differences in health outcomes among racial and ethnic groups in the United States, Dr. Kington said, is believed to be acculturation. And “the single most important finding in this area is that an increasing number of studies have described health behaviors and health outcomes among immigrant populations as worsening with acculturation.”
For example, across a wide range of groups—including non-Hispanic whites, blacks, Asian subgroups, and Hispanic subgroups—all of the foreign-born populations have lower infant mortality rates than their U.S.-born counterparts. Dr. Kington declined to speculate on the reasons for this counterintuitive though “remarkably persistent finding.” But he noted that the “behavioral and social sciences have the potential to address some of the most pressing health problems that the country is facing—particularly those problems related to differences in health status across racial and ethnic groups and across groups as stratified by socioeconomic status.”
High-priority areas in which the behavioral and social sciences are especially well poised to make substantial contributions, he said, include:
-
reducing the infant mortality rate, especially among poor women— and poor black women in particular;
-
preventing deterioration of health status and health behaviors with acculturation of the growing immigrant population;
-
intervening in the early years of life to prevent the trajectories of health status that seem to be determined by social factors during that period;
-
developing appropriate interventions to promote healthier lifestyles among the growing Hispanic, Asian, and African American communities; and
-
informing the development of nonhealth interventions to promote improved health status.
Dr. Kington closed by citing his favorite quote from Martin Luther King’s Letter from a Birmingham Jail: “Human progress never rolls in on wheels of inevitability.”
“Clearly, in order for these changes to occur, we have to make them occur,” Dr. Kington said. “We have to think of ways to facilitate the translation of the scientific findings that we have in the behavioral and social sciences into real interventions that work in real populations and improve the health status of real people.”





