7
Integration of Chemical and Pathogen Risk Assessment
The final element of the charge to the committee is to explore whether approaches for conducting pathogen risk assessment can be integrated with those for chemical risk assessment. This inquiry leads to a summary and synthesis of many of the previous chapters’ findings and recommendations that resulted directly or indirectly from the committee’s need to address the inherent uncertainty of the complex composition of biosolids. This uncertainty precludes the possibility of completely separating the risk-assessment and risk-management processes. Risk assessment for such mixtures is an ongoing process that requires quality control of treatment processes and some form of surveillance for adverse effects from exposure to biosolids. In this chapter, the question of whether pathogen risk assessment can be integrated with chemical risk assessment will be explored first in the agent-by-agent context of the original risk assessment used for the Part 503 rule and then in the broader and more recent context of risk assessment for complex mixtures.
AGENT-BY-AGENT RISK ASSESSMENT
The pathogen and chemical regulations of the Part 503 rule were developed differently. EPA conducted risk assessments for chemicals to establish concentration limits and loading rates but deemed microbial risk assessment to be too immature for developing risk-based limits for pathogens. Instead, EPA established treatment and site restrictions to reduce the concentrations
of pathogens in biosolids. Advances in microbial risk assessment have occurred since then, but there remains a difference in the maturity of risk-assessment procedures for chemicals and those for pathogens. The question posed is whether this difference is simply an artifact of the different stages of development of these two branches of risk assessment or whether generic differences are attributable to the nature of the agents themselves. In addressing this question, it is useful to consider the four components of the traditional risk-assessment process (hazard identification, dose-response characterization, exposure assessment, and risk characterization) and ask which, if any, of those components has inherent differences in the way pathogens and chemicals are assessed.
Hazard identification is the process of reviewing relevant biological and chemical information on an agent that might pose a health hazard. Although there are obvious differences in the types of information available on chemicals and pathogens, there appears to be little fundamental difference in the process of identifying their hazards. This is supported by a recent NRC report Classifying Drinking Water Contaminants for Regulatory Consideration (NRC 2001), in which no distinction between chemical and biological contaminants is made. In general, however, pathogens usually are grouped into generic classes with less of an agent-specific focus than is common in chemical risk assessment.
The process for characterizing dose-response relationships is not as straightforward for pathogens as it is for chemicals. The process is complicated by the possibility that exposure to a pathogen may engender an immune response that might persist and alter an individual’s subsequent susceptibility to infection or clinical disease. Acquired immunity has no relevant analog for chemical exposures in the risk-assessment context, although there are chemicals for which sustained exposure can result in tolerance for some toxic end points. Also, the converse can be true when an individual becomes sensitized to a chemical and develops serious and persistent hypersensitivity. For infectious agents, however, acquired immunity can be a major modifier of population risk. An exposed population is likely to be an unknown mixture of those with acquired immunity and those without. Moreover, the population can change over time as susceptible individuals become infected and move from one subgroup to the other. Acquired immunity might simply be addressed by developing two dose-response functions in the risk-assessment process, one for the susceptible population without immunity and a second for the population with acquired immunity. The conservative approach would be to conduct an assessment of a totally susceptible population, and although the results could be very conservative, this option would be consistent with EPA’s practice of protecting sensitive subpopulations.
Perhaps the greatest methodological difference in the risk-assessment process for chemicals and pathogens occurs in the exposure assessment process. The difference is because of the possibility of secondary transmission of infectious agents (discussed in-depth below). The challenge posed by secondary transmission is that an individual is at risk not only from direct exposure to pathogens in biosolids but also from population-level interactions that can result in exposure to and infection from individuals already infected. In addition, there are environmental pathways (e.g., contamination of surface waters used for drinking or recreation) by which an individual infected with an enteric pathogen, for example, can alter the risk for populations not primarily exposed to the pathogen in biosolids. Whatever the pathway, secondary transmission can expand the population at risk beyond those involved in the original exposure scenario. Hence, the likelihood of secondary transmission is an issue that must be addressed generally in pathogen risk assessments, as contrasted with those for chemical exposures.
The risk-characterization process for a single pathogen versus a single chemical will differ in the need to account for the implications of acquired immunity and secondary transmission. In the case of biosolids, however, that distinction is somewhat academic, because both chemicals and pathogens are part of a complex mixture, the exact composition of which can change from time to time and place to place. As noted above and in Chapters 4 and 6, methods for conducting chemical and microbial risk assessments have advanced since the promulgation of the Part 503 rule, including methods for assessing risks of chemical mixtures. These advances are clearly relevant to updating the biosolids standards. However, the additional complexity of dealing with chemical and pathogen mixtures has the potential of being counter to the recommendations of the Presidential/Congressional Commission on Risk Assessment and Risk Management (1997). In particular, the commission advised a diminished reliance on assumption-laden procedures for arriving at agent-by-agent and medium-by-medium mathematical estimates of risk. Instead, it advises assessments focused at particular exposures and health end points, clarified with stakeholder input, with the objective of achieving and sustaining practical reductions in risk. Issues about mixtures are discussed further below, and the committee outlines data needs and the nature of studies that would inform more focused assessments in Chapters 2 and 3.
SECONDARY TRANSMISSION
Most quantitative risk assessments for pathogens have focused on ingestion of waterborne pathogens (Fuhs 1975; Haas 1983; Regli et al. 1991; Ander-
son et al. 1998). In these studies, static models were used to calculate the probability of individual infection or disease as a result of a single exposure event. This approach is based on an early chemical model for risk assessment (NRC 1983). In chemical risk assessment, there is generally a straightforward relation between risk to an individual and risk to a population of similarly exposed people. For example, if a particular exposure scenario results in an estimate of an individual risk of chemically induced disease of 1×10−4, then the expected number of cases in an exposed population of 100,000 is 10. This result is valid under the assumption that any person’s probability of disease is independent of whether anyone else gets the disease. Both estimates of individual and population risk are determined by the dose-response function and the exposure assumptions, and both of those are unmodified by the disease status of others in the population. As noted above, that straightforward relation is not the case for all infectious diseases. For example, for an individual, the probability of infection from a particular pathogen in biosolids, PI, is the sum of two terms:
PI=P(directexposuretopathogen inbiosolids)+P(exposure topathogen shedby infected person)
The possibility of exposure to a pathogen shed by an infected person is peculiar to pathogens in being an important and sometimes dominant pathway of exposure. The pathway by which the shed pathogen gets from the infected to the susceptible person can be from direct contact or by circuitous routes through the environment.
The limitations of treating infectious disease transmission as a static disease process, with no interaction between those infected or diseased and those at risk, has been illustrated in studies of Giardia (Eisenberg et al. 1996), dengue (Koopman and Longini 1994), and sexually transmitted diseases (Koopman et al. 1991). However, risk-assessment approaches for environmentally mediated pathogen exposures involving secondary transmission are only now being developed (Colford et al. 2001). These approaches allow exploration of the importance of the secondary infection process. However, the need for data for execution of calculations based on these approaches is also greater than that for static risk assessments. When secondary infection is possible, risk is by definition manifested at a population level and risk calculations are dynamic in nature. (The overall risk calculation is based not only on current exposures to contaminated media but also on all subsequent secondary infections.) In addition, the existence and development of acquired immunity in the population must be accounted for in the analysis.
The dynamic systems approach was used to study the conditions under which environmentally mediated secondary transmission could be important
in the transmission of Giardia (Eisenberg et al. 1996). An exposure scenario was studied in which swimmers were exposed to Giardia from a recreational swimming impoundment filled with water reclaimed from community sewage. The important finding in this study was that the rate of infected swimmers shedding pathogens into the impoundment was a crucial factor in determining (1) the degree to which a contribution of the incidence of giardiasis came from transmission via swimming; and (2) the most effective control strategy.
Clearly, the methods of risk assessment for chemicals and pathogens have inherent differences in some elements of the risk-assessment process. Thus, the committee concludes that in conducting single-agent risk assessments, there are inherent differences between chemical and pathogenic agents that must be considered. In particular, infection of an individual from exposure to pathogens in biosolids may lead to secondary infections in others from person-to-person contact or from transmission of the pathogen to others through air, food, or water.
The importance of secondary transmission depends in part on the level of acquired immunity to the pathogen in the community. In assessing the likelihood of secondary transmission, it is clear that the use of the dynamic modeling approach to fully assess the risks of the pathogen component of biosolids for all pathogens and all exposure scenarios would be a complex undertaking. Generally, site-specific data (e.g., population size) are required, and the models are themselves analytically complex. The use of default parameter values and appropriately structured analysis may be able to provide a practical procedure for using the modeling approach to explore the importance of immunity and secondary transmission in preliminary analyses. At present, however, it may be more practical to use less comprehensive methods as a form of preliminary analysis to address the importance of these effects. The objective of such a preliminary analysis would be to determine whether a particular pathogen possesses characteristics that result in secondary transmission and, if so, determine the possible pathways through which this transmission can occur.
For pathogens that can be transmitted via infected individuals, the preliminary analysis can proceed following the standard format of chemical risk assessment with the focus on the susceptible individual. A new feature of this process is the need to determine the existence of exposure pathways connecting a susceptible individual to others in the community assumed to be infected already. If plausible pathways do not exist, then no further analysis is needed. Alternatively, if such pathways are identified, it will be necessary to explore their importance. If their importance is low with respect to direct exposure, no further action is needed, whereas a significant risk with respect to background incidence of disease suggests the need for a comprehensive assessment.
From another perspective, the issue here is to gain some insight into what is termed the “force of infection” by infectious disease epidemiologists (Anderson and May 1991). The force of infection represents the probability that a given susceptible host becomes infected per unit time only because of the presence of other infected individuals in the population. A complicating feature of the concept is that the force of infection is generally assumed to be linearly proportional to the number of infected individuals in the population. This proportion in turn depends on the level of population immunity. Those factors again underscore that if pathways of secondary infection exist, it is only possible in an approximate way to carry out the preliminary analyses on an individual basis rather than at the population level. A feasible approach might be to conduct a two-tiered evaluation, the first dealing with the potential for secondary transmission of a set of candidate pathogens and the second analyzing the exposure pathways for those pathogens with a secondary transmission potential.
COMPLEX MIXTURES
It is a challenge to integrate the outcomes of each agent-specific risk assessment into a comprehensive whole, even for simple mixtures. One reason for the difficulty is the lack of information usually available on the biological interactions between components of the mixture. The second reason is the challenge to characterize in a useful way the range of risks that might occur. For biosolids, the possible adverse outcomes of exposure will include acute and chronic effects from chemical exposures and principally acute effects from exposures to pathogens. Further, these effects will range from short-term non-life-threatening outcomes like irritation and diarrhea to chronic life-threatening outcomes like cancer. Although the exposure-assessment component of the risk-assessment process will characterize the extent of various chronic versus acute hazards for specific population groups, an integrated assessment will sometimes be needed to balance the risk of outcomes of modest severity with those of great severity.
This same challenge exists for mixtures of chemical agents alone, as discussed in EPA’s “Supplementary Guidance for Conducting Health Risk Assessment of Chemical Mixtures” (EPA 2000). This document offers valuable guidance on the assessment of risks arising from the chemical mixtures found in biosolids. The strategic guidance from that document that can be extrapolated to biosolids is that it is preferable to base risk assessments on studies of exposure to the whole mixture, for example, epidemiological studies of biosolids workers. However, as noted in Chapter 3, that type of data is not available for biosolids in either sufficient amount or quality, consequently
making it necessary to use a component-based approach to assess risks from pathogens and chemicals in biosolids.
Although the chemical mixtures document discusses in some detail the various options available for risk characterization, including guidance on the formulation of hazard indexes, there is no equivalent guidance, either from EPA or in the scientific literature, for mixtures of pathogens, let alone the chemical-pathogen mixture that biosolids comprise. Introducing risks from pathogens to the process of integrating diverse outcomes in the risk characterization step would seem to present no new challenges beyond the implications of acquired immunity and secondary infection discussed previously. However, despite progress in integrating risks for mixed chemical exposures, the possibility of pathogen-pathogen or chemical-pathogen interactions between the components in either inhibiting or enhancing the adverse effects expected from individual exposures presents an array of unexplored issues in the context of risk assessment. That pathogen-pathogen and chemical-pathogen interactions occur is illustrated by examples, including the increased likelihood of tuberculosis infection among workers exposed to silica dusts (Hnizdo and Murray 1998; Ding et al. 2002). Of greater relevance to biosolids is the experimental demonstration that short-term inhalation exposures to nitrogen dioxide increase the susceptibility of rodents to pneumonia (Coffin et al. 1977; Gardner et al. 1977). The committee concludes that the knowledge base for generating summary indexes of risk for finite mixtures of chemicals and pathogens is incomplete. However, research is clearly needed to synthesize existing information on potential interaction of chemicals and pathogens that might be associated with biosolids exposures and lead to an increased susceptibility to infection, particularly by inhalation.
It is important to note that, even if a summary index of the risk of an adverse response to mixtures was available, it would not necessarily reflect the total hazard of exposure to biosolids because of the inability to identify all of its hazardous constituents and their potential for interaction in vivo. Moreover, the composition of biosolids is susceptible to unanticipated changes from time to time and place to place. Thus, it is not possible to conduct a risk assessment for biosolids at this time (or perhaps ever) that will lead to risk-management strategies that will provide adequate health protection without some form of ongoing monitoring and surveillance. There is a degree of uncertainty that, when exceeded in the risk-assessment process, requires some form of active health and environmental tracking in the risk-management strategy to ensure against unanticipated outcomes. This situation led the committee to conclude that although the Part 503 agent-specific risk-assessment process can be improved with new risk assessment methodology, the remaining uncertainty for complex mixtures of chemicals and biological agents
is sufficient to preclude the development of risk-management procedures based on these agent-specific analyses that can reliably result in acceptable levels of risk. Some form of process quality assurance and ongoing surveillance must be done to ensure that effects not anticipated by the chemical- and pathogen-specific risk assessments do not occur. Strategies for the management of risks arising from biosolids exposure should include audits of process performance and management practices, periodic hazard surveillance, and studies of health outcomes, including epidemiological studies and studies in response to episodic events.
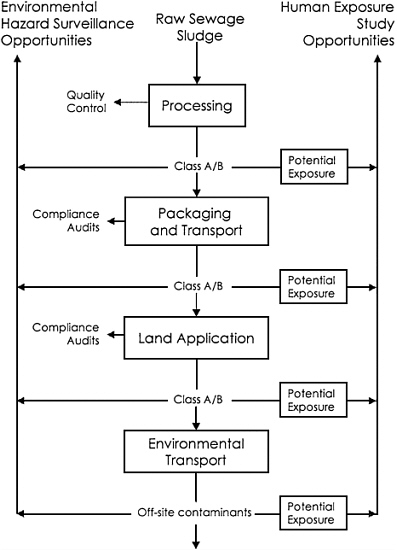
As recounted in this report, the various steps in the treatment, transport, application, and use of biosolids present multiple opportunities for both human exposure and monitoring and surveillance of the process to ensure minimization of risks. Figure 7–1, adapted for biosolids (Halperin 1996), attempts to summarize the process, the opportunities for hazard surveillance, and the opportunities for study of exposed human populations. Also shown are the points in the process amenable to quality control and compliance audits to ensure that the management practices assumed in the risk assessment process or required by the Part 503 rule are, in fact, carried out appropriately.
In Figure 7–1, each of the center boxes is a process to which biosolids are subjected, beginning with the original treatment process (top) that converts the raw sewage sludge into Classes A or B biosolids, which are then packaged or otherwise prepared for transport and delivery to the application site. Biosolids are then applied to land where they are subject to weathering, and some of the constituents may be transported off-site. The right side of the figure shows a second set of boxes that represent human exposures to biosolids at any point between initial processing and final decay or inactivation of off-site contaminants. Exposed populations can be monitored or studied at particular times and locations to assess the relation between any abnormal health conditions and the biosolids exposure experienced. Any information gained from studying health outcomes is collected and fed back into the risk assessment to support or improve the risk-management process, as indicated by the vertical line on the far right of the figure.
The left side of the figure shows the stages in the process amenable to quality-assurance activities or hazard surveillance. At any point in the process, it is possible to obtain bulk samples of biosolids (or biosolids-soil mixtures) to determine whether its hazardous constituents are present in expected or unexpected concentrations. It is also possible to monitor the media of exposure to chemicals or pathogens originating in biosolids (e.g., personal air monitoring of workers engaged in land application).
With respect to quality assurance, as indicated in Chapter 2, a need exists to verify the efficacy of treatment technologies used for pathogen control.
Because the regulations for pathogen control are technologically based rather than risk based, it is important to verify that the technology is achieving the intended results. Such verification includes a review of the management practices required for Class B land application, because they are predicated on the assumption that further pathogen reduction is achieved through the implementation of such practices.
The right side of the figure shows the points in the process where human exposures can occur and, by implication, the different populations and circumstances that might be involved. Although routine human health surveillance is unnecessary and impractical because of the wide variety of possible outcomes, the committee believes that specific circumstances might afford opportunities for health effects studies, such as epidemiological studies of occupational groups or investigations arising from reports of disease outbreaks plausibly connected to biosolids exposure.
FINDINGS AND RECOMMENDATIONS
Ideally, risk assessment of biosolids should be based on complex-mixture data to include risks from chemicals and pathogens. However, that type of data is not available in either sufficient quantity or quality (see Chapter 3), and methods have not been developed for integrating and characterizing the range of risks that might occur from exposure to mixtures of chemicals and pathogens. Thus, it remains necessary to use a component-based approach to assess risks from pathogens and chemicals in biosolids. The committee found that although the chemical-specific risk assessments conducted to establish the Part 503 regulations can be improved by using new risk-assessment methodology, the remaining uncertainty for complex mixtures of chemical and biological agents is sufficient to preclude the development of risk-management procedures that can reliably result in acceptable levels of risk. Some form of treatment-process quality assurance and ongoing surveillance must be done to ensure that effects not anticipated by the agent-specific risk assessments do not occur.
Recommendations:
-
Figure 7–1 should be used by EPA as a framework for managing the risks from exposure to biosolids. The framework includes audits of treatment-process performance and management practices, periodic hazard surveillance, and studies of health outcomes, including preplanned studies and studies in response to episodic events. For example, as recommended in Chapters 2 and 6, surveys should be conducted to verify that Class A and Class B treatment processes perform as assumed by engineering principles, and determinations of
-
pathogen density and destruction across the treatment process and in the soil over time should be completed. Recommendations contained in Chapter 5 also address the need for process-performance measures that can be monitored and used in site-specific surveys of performance. In Chapter 3, the nature and objectives of hazard surveillance studies and studies of health outcomes of exposed populations are described more fully. All the recommendations reflect the committee’s concern that the complex risk-assessment task posed by biosolids cannot serve as a useful and reliable guide without an ongoing effort to ensure that the assumptions underlying the assessment are valid and that the risk-management procedures put in place in response to the assessment are being routinely implemented. Broad-scale and site-specific feedback, graphically depicted in Figure 7–1, is needed.
-
Research should be conducted to synthesize existing information on potential interaction of chemicals and pathogens that might be associated with biosolids exposures and lead to an increased susceptibility to infection, particularly by inhalation.
Methods for conducting chemical and microbial risk assessment have advanced since the promulgation of the Part 503 rule in 1993. In reviewing these methods, the committee found that there are inherent differences between chemical and pathogenic agents that must be considered in single-agent risk assessments. In particular, infection of an individual from exposure to pathogens in biosolids might result in secondary infections in others. The secondary infections might be caused by person-to-person contact or transmission of the pathogen to others through air, food, or water. The importance of secondary transmission depends in part on the level of acquired immunity to the pathogen in the community. Another development of importance is the recommendation of the Presidential/Congressional Commission on Risk Assessment and Risk Management to diminish reliance on assumption-laden procedures for arriving at agent-by-agent and medium-by-medium mathematical estimates of risk in favor of stronger interaction with stakeholders in achieving and sustaining practical reductions in risk.
Recommendation: As outlined in Chapters 5 and 6, future risk assessments of biosolids components should be conducted using the most current methods and data. For pathogens, it is important that risk assessments include an evaluation of the potential for secondary transmission of disease. Representatives from all stakeholders should be included in future risk assessments. Stakeholders can provide information and insights into the use of biosolids in practice and the potential health problems, which are particularly important in the development of exposure assessment. Involving stakeholders throughout the risk-assessment process provides opportunities to bridge gaps in understanding language, values, and perspectives.
The committee is aware that this report poses a challenge to EPA in that much of the discussion in this chapter, as well as in Chapters 3 and 4, recom-
mends very different emphases in updating the Part 503 rule than are reflected in the charge to the committee. In many ways, the contents of Chapters 2, 5, and 6 are a more direct response to the charge, which is grounded in the original approach and methodology, while acknowledging that this review would be carried out in the context of new developments. However, the committee believes that the differences in point of view and approach underlying its response to the various elements of the charge accurately reflect the counter-vailing currents in the broader risk-assessment community and the differences in perspective among those directly involved in the management of biosolids risks. The overall objective of the process, which this report is a part of, is to better assess and manage the risks associated with the land application of biosolids in the United States.
REFERENCES
Anderson, R.M., and R.M.May. 1991. Infectious Diseases of Humans: Dynamics and Control. New York, NY: Oxford University Press.
Anderson, M.A., M.H.Stewart, M.V.Yates, and C.P.Gerba. 1998. Modeling the impact of body contact recreation on pathogen concentrations in a source drinking water reservoir. Water Res. 32(11):3292–3306.
Coffin, D.L., D.E.Gardner, G.I.Sidorenko, and M.A.Pinigin. 1977. Role of time as a factor in the toxicity of chemical compounds in intermittent and continuous exposures. Part 2. Effects of intermittent exposure. J. Toxicol. Environ. Health 3(5–6):821–828.
Colford, J., J.Eisenberg, B.Lewis, J.Scott, D.Eisenberg, and J.Soller. 2001. A Dynamic Model to Assess Microbial Health Risks Associated with Beneficial Use of Biosolids. Status Report 5. WERF Project #98-REM-1. Prepared by EOA, Inc., Oakland, CA, and School of Public Health, University of California, Berkeley, CA, for Water Environment Research Foundation, Alexandria, VA. March 2001.
Ding, M., F.Chen, X.Shi, B.Yucesoy, B.Mossman, and V.Vallyathan. 2002. Diseases caused by silica: Mechanisms of injury and disease development. Int. Immunopharmacol. 2(2–3):173–182.
Eisenberg, J.N., E.Y.Seto, A.W.Olivieri, and R.C.Spear. 1996. Quantifying water pathogen risk in an epidemiological framework . Risk Anal. 16(4):549–563.
EPA (U.S. Environmental Protection Agency). 2000. Supplementary Guidance for Conducting Health Risk Assessment of Chemical Mixtures. EPA/630/R-00/002. August 2000. National Center for Environmental Assessment, Office of Research and Development, U.S. Environmental Protection Agency, Washington, DC. [Online]. Available: http://www.epa.gov/nceawww1/raf/chem_mix.htm [December 26, 2001].
Fuhs, O.W. 1975. A probabilistic model of bathing beach safety. Sci. Total Environ. 4(2):165–175.
Gardner, D.E., D.L.Coffin, M.A.Pinigin, and G.I.Sidorenko. 1977. Role of time as a factor in the toxicity of chemical compounds in intermittent and continuous exposures. Part 1. Effects of continuous exposure. J. Toxicol. Environ. Health 3(5–6):811–820.
Haas, C.N. 1983. Estimation of risks due to low doses of microorganisms: A comparison of alternative methodologies. Am. J. Epidemiol. 118(4):573–582.
Halperin, W.E. 1996. The role of surveillance in the hierarchy of prevention. Am. J. Ind. Med. 29(4):321–323.
Hnizdo, E., and J.Murray. 1998. Risk of pulmonary tuberculosis relative to silicosis and exposure to silica dust in South African gold miners. Occup. Environ. Med. 55(7):496–502.
Koopman, J.S., and I.M.Longini Jr. 1994. The ecological effects of individual exposures and nonlinear disease dynamics in populations. Am. J. Public Health 84(5):715–716.
Koopman, J.S., I.M.Longini Jr., J.A.Jacquez, C.P.Simon, D.G.Ostrow, W.R.Martin, and D.M.Woodcock. 1991. Assessing risk factors for transmission of infection. Am. J. Epidemiol. 133(12):1199–1209.
NRC (National Research Council). 1983. Risk Assessment in the Federal Government: Managing the Process. Washington, DC: National Academy Press.
NRC (National Research Council). 2001. Classifying Drinking Water Contaminants for Regulatory Consideration. Washington, DC: National Academy Press.
Presidential/Congressional Commission of Risk Assessment and Risk Management. 1997. Risk Assessment and Risk Management in Regulatory Decision-Making. Final Report. Washington, DC: The Commission.
Regli, S., J.B.Rose, C.N.Haas, and C.P.Gerba. 1991. Modeling risk from giardia and viruses in drinking water. Am. Water Works Assoc. J. 83(11):76–84.