AMO Science Improving Health
Today we have many exceptional diagnostic techniques to assist the medical profession in the diagnosis and treatment of diseases and to allow both doctors and patients to make more informed decisions about health care. Many of these techniques were developed from results obtained in AMO research. Novel, noninvasive imaging allows doctors to have far better control during surgery, resulting in less loss of healthy tissue. Magnetic imaging with polarized rare gases makes it possible to see the finest lesions in the lungs (see box “A Patient’s Story) and may even be used to image specific brain functions. Medical diagnostics are in the early stages, and new applications of the technique are still being discovered (see box “Breathable Magnets”). Lasers are also playing a major role in many areas of surgery (see box “Improving Laser Surgery”).
Since the interior of the eye is easily accessible with light, ophthalmic applications were the first widespread uses of lasers in medicine. Argon lasers are now routinely used to treat retinal detachment and bleeding of blood vessels in the retina caused by age-related macular degeneration. Today’s surgeon is not limited to the metal scalpel but now has a wide array of lasers of different wavelengths to choose from to excise tissue, depending on the disease and the type of tissue involved. The use of lasers dependent on carbon dioxide or a neodymium-doped yttrium-aluminum-garnet (YAG) rod as the lasing medium to cut tissue while simultaneously sealing blood vessels has been widely and successfully applied to many surgical problems in specialties ranging from dermatology to general surgery. Tattoos can be removed using lasers whose wavelength is selected on the basis of the
|
A PATIENT’S STORY John has received some troubling news. He has just been diagnosed with a disease that has damaged much of his lungs, rendering large portions of them useless. His lung surgeon is faced with a difficult operation, as the only way to save the patient is to remove the affected portions of the lung. But such surgical procedures have a very high failure rate, and it’s difficult to know which sections of John’s lung to remove during the surgery. Fortunately, the surgeon is aware of a new imaging technique that can let a doctor see in advance which sections of the lungs work and which are diseased. This method uses rare gas atoms prepared by a process called optical pumping to visualize the functional portions of the lung. In optical pumping, atoms are aligned, or polarized, to produce a striking result: a gaseous magnet. John need only breathe the polarized gas during an otherwise conventional magnetic resonance imaging (MRI) session. The images on page 12 superpose a conventional MRI scan of the lungs and a scan using polarized gases. |
color of the tattoo; multicolor tattoos may be removed using several lasers. Lasers are being used for the controlled removal of the surface of the skin to reduce or eliminate wrinkles (laser skin resurfacing). Other laser systems are being used to remove unwanted body hair, to treat acne (in conjunction with a topically applied cream), to remove cancerous skin, and to excise tumors in the colon. The erbium-doped YAG laser has recently been introduced for dental applications; it promises a dramatic reduction in pain and automatic decontamination,
|
BREATHABLE MAGNETS Medical imaging using magnetized rare gases was invented in 1994 to provide a way to study diseases of the lung, heart, and brain that depend on the flow of gas and blood through the vital organs. This marriage of AMO science and medical imaging grew out of the basic study of the atomic nucleus. But how did this connection between AMO physics and medical imaging come about? It started with some basic research on helium by Luis Alvarez at the University of California, Berkeley, in the 1940s. He discovered a form of helium gas, 3He, that behaves like a tiny bar magnet. 3He is abundant in the universe but exceedingly rare on Earth—the world’s supply amounts to only about 1 ton. There is more 3He in the rocks on the Moon’s surface than on our planet. In recent years, there has been a steady supply of the gas from an unusual source: Although 3He is not radioactive, it is produced from the radioactive decay of tritium, the form of heavy hydrogen present inside nuclear warheads. Because 3He is a gas, its atoms are randomly oriented at room temperature, so the total magnetism in a bottle of it is essentially zero. However, scientists studying the basic physics of atomic collisions perfected an optical pumping scheme that uses polarized laser light to align most of the 3He with their magnets pointing in the same direction. This creates a very unusual material: a gas that acts like a bar magnet. It was later recognized that this new “breathable magnet” might have marvelous properties for imaging the lung and the circulatory system. But many technical obstacles had to be overcome before this promise could be demonstrated in the 1990s, when the first magnetic images were obtained using this technique. Now, only a few years later, breathable magnets are producing dramatic images like the ones shown on the opening page of this chapter. Tiny features in the lung, brain, and circulatory system are visible for the first time. |
|
IMPROVING LASER SURGERY Following its development in the mid-1970s, researchers quickly discovered (in 1981) that the excimer laser, a product of years of AMO research, could be used to cut away skin tissue in a much better fashion than previously possible. This type of laser produces light in the ultraviolet region and, as shown in the image below of a cross section of a human aorta after it has been irradiated with an excimer laser, a laser scalpel of this type can produce a well-defined and controllable cut in biological tissue. By contrast, an image of a human aorta irradiated with longer wavelength light—pulsed green (532-nanometer) light, for example—would show an incision characterized by burning and charring. Laser surgery carried out with excimer lasers is a good example of how AMO science has led to new and improved surgical techniques. Indeed, in the ensuing years, AMO scientists collaborated further with medical doctors interested in using these effects for cutting and etching the cornea, artery walls, and skin while minimizing unwanted collateral damage.  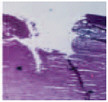 |
|
LASER REFRACTIVE SURGERY— A FAREWELL TO SPECTACLES? The success of laser refractive surgery is a story of sophisticated lasers that were developed for basic research and then found new applications in clinical medicine. This transition has occurred through partnerships between basic research scientists, technologists in start-up companies, and the medical community. One of the early laser surgical procedures—utilized first in Russia—uses radial incisions directly in the cornea (radial keratotomy, or RK) to alter the curvature of the surface. This method produced vision improvement, but it was difficult to control the extent of the correction accurately. In the early 1980s it was discovered that the outer layer of the eye’s cornea is extremely sensitive to excimer laser light. The 193-nanometer light emitted by the argon fluoride excimer laser can be used to etch away corneal tissue with high precision. Medical researchers postulated that this ability to destroy tissue might be used to resculpt the curvature of the eye’s optical surface with great precision and control. This idea led to the transition from RK to laser-assisted in situ keratomilieusis (LASIK), which has faster recovery times and more immediate results than RK. LASIK involves ablating tissue under the outer surface of the cornea. The corneal surface tissue is surgically opened to form a thin, transparent flap. Then, following programmed laser ablation of the underlying tissues, the flap is replaced. This is where great skill, surgical experience, and the right keratome (corneal cutting device) are critical. The results can be dramatic, especially for the severely myopic. New technologies now being developed promise to improve this procedure further. In many cases, these technologies come directly from basic research labs, where there are similar exacting requirements for laser performance. One very recent development is the use of ultrafast femtosecond lasers to replace the mechanical blade that cuts the corneal flap. The laser uses femtosecond light pulses—a femtosecond is a billionth of a millionth of a second—to photoablate tissue at the rate of thousands of laser pulses per second. This produces smoother surface cuts than blades and virtually eliminates the risk of infection. The same technology might soon obviate the creation of a corneal flap. This is because ultrafast lasers can damage material beneath a transparent surface without harming the surface itself, through a process called nonlinear multiphoton absorption. |

FIGURE 5
both welcome contributions to the treatment of dental disease. The days of tolerating the vibration and noise associated with drilling to prepare dental cavities for filling may be numbered. Today, millions of people suffer from near- or far-sightedness and require either contact lenses or glasses to see clearly. Glasses, however, can be broken or forgotten, and contacts require careful cleaning. A new procedure, laser-assisted in situ keratomilieusis (LASIK), is enjoying widespread use because it is an outpatient surgical procedure that produces very good vision correction for many individuals. In LASIK (Figure 5), the surgeon uses an excimer laser to “sculpt” the structure of the eye with the goal of achieving vision correction without lenses or contacts (see box “Laser Refractive Surgery—A Farewell to Spectacles?”).
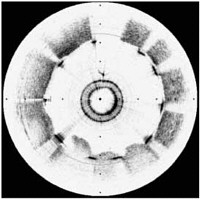
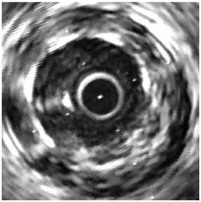
FIGURE 6 Two images of the same artery using the OCT method (left) and ultrasound (right).
Nearly 7 million Americans suffer from coronary heart disease (CHD), and nearly 500,000 die of the disease each year. CHD is caused by a thickening of the inside walls of the coronary arteries. This thickening, called arteriosclerosis, narrows the space through which blood can flow, decreasing and sometimes completely cutting off the supply of oxygen and nutrients to portions of the heart. A new optical imaging technique, called optical coherence tomography (OCT), is now being developed that promises to dramatically improve the diagnosis and treatment of this disease.
OCT uses a bright optical source introduced into an artery by a fiber catheter (the central ring in the left portion of Figure 6). A broad range of infrared colors from this bright source reflects from the various layers in the lining of the artery at different times. A detector compares these times with a reference clock to form a high-resolution map of the artery wall. As can be seen from Figure 6, the resolution is much higher than with the older ultrasound techniques. An OCT image of a cross section of an artery (left) is compared with a lower-resolution intravascular ultrasound image (right).
The images were acquired following the deployment of a stent, a wire frame tube inserted to prevent collapse of the artery and ensure the unclogged flow of blood. The individual struts of the
stent are opaque to both infrared light and ultrasound, resulting in shadowing of the vessel lumen underlying them. In the ultrasound image this shadowing is less apparent than in the OCT image because of its coarser resolution. Determining that the stent struts are in close proximity to the vessel lumen is clinically very important to the stent deployment. Stents are commonly used to prevent initial or secondary heart attacks. The new OCT imaging technique will clearly improve health care for many of us.
Advances in laser technology are also enabling a new treatment of the main cause of vision loss in people over 50: age-related macular degeneration (AMD). In a patient with AMD, the central portion of the retina (the back surface of the eye responsible for vision) becomes progressively damaged by leakage of blood and fluid from blood vessels. Lasers are already used to treat this condition by making controlled scars within the eye on the retina. While this treatment controls the disease, it does so at the cost of creating some irreversible vision loss. The new treatment, recently approved by the Food and Drug Administration (FDA), uses a combination of laser light and a new drug to treat the abnormal blood vessels in the eye, which are the cause of the problem. This new drug is injected into the patient, and light from a laser is used to convert the molecules of the drug to a reactive form. This reactive form of the drug locally creates a small, highly controlled scar that is confined to the abnormal vessels. While not a cure, the treatment allows some forms of the disease to be controlled without loss of vision. In contrast to earlier laser treatments, which used large and expensive lasers, the new approach uses a relatively inexpensive diode laser, similar to those in CD players, to activate the drug. Referred to as photodynamic therapy, the technique has also been approved by the FDA for relief of the symptoms of cancer of the esophagus; it allows the patient to continue to swallow when otherwise she or he might be unable to do so. Other cancer applications are also being developed.
Future advances in medicine that will be used to treat cancers and other terminal conditions will be linked to our knowledge of the four-letter genetic code for life stored in DNA. This code is based on four molecules, called G, C, A, and T. Three billion of these molecules form the DNA present in every cellular nucleus in our bodies. Much research has been devoted to sequencing the human genome, a truly massive international effort. Knowledge of the genetic sequence for many organisms will be one of the great achievements of this new century and will lead to unimaginable new therapies for disease. At the heart of each commercial genesequencing machine is a device called a fluorescence spectrometer, which is an optical instrument that measures the colors of light being emitted by fluorescent molecules. To sequence a piece of DNA, each of the molecules G, C, A, and T is labeled or tagged with a different colored fluorescent dye through a chemical reaction. By reading the colors of the dyes, the sequence can be obtained. The contribution of AMO science to this work rests on pushing the state of the art with advanced light sources and detectors to achieve new levels of sensitivity and selectivity. For example, if a laser beam can be used to detect labeled bases inside of or exiting from a tiny capillary, the enhanced sensitivity allows the detection of smaller amounts of the material of interest.
Ultrasensitive optical detection has been the target of research and development in AMO science for many years, with the original goals being military applications and the quest for scientific insight that results from pushing the limits of detection all the way down to single photons from a single molecule (see box “Medpen”).
|
MEDPEN A miniature development that may help save lives on the battlefield is a handheld laser called the laser medical pen, or Medpen, developed by the Air Force. It can cut like a scalpel and also stop bleeding. The purpose of the Medpen is life support in combat situations, enabling the physician or paramedic to coagulate blood and close wounds under battlefield conditions. The same device could also be used for domestic emergencies, such as stabilizing accident victims at a crash site. Less than 12 inches long and less than 1 inch in diameter, the Medpen delivers 5 watts of continuous power at a wavelength of 980 nm (invisible infrared light). Its 3-volt battery can power it for 20 minutes, long enough for most emergency situations. Medpen is made possible by tremendous advances in diode laser technology, most notably in efficiency, reliability, and miniaturization.  |
Concurrently, basic AMO research has sought to understand how chemical reactions can produce light at the molecular level. Today, these disparate research efforts are being combined to generate a fascinating new array of medical applications.
One such application is the imaging of the effects of drug treatments on live subjects (Figure 7). Its goal is to understand by noninvasive means the mechanisms of disease and the complex genetic program that controls the development of mammals. This approach uses the fact that light can pass through tissues in much the same way as light from a flashlight passes through one’s hand
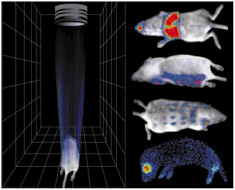
FIGURE 7 New imaging techniques capable of detecting light produced inside a living subject allow observation of the effects of antitumor drugs, antibiotics, or antiviral treatments. The images on the right are scans of living mice that would allow researchers to investigate the effects of various drugs on different parts of the body without having to resort to harmful invasive techniques.
in a dark room. The source of light in the images of live mice is internal; that is, researchers use the genes from fireflies and other glow-in-the-dark (bioluminescent) organisms to place molecular indicator lights inside mammalian cells. These labeled cells are then used in combination with pathogens and drug treatments in animal models of human disease. The light that comes through the skin from the marked chemiluminescent cells is extremely weak, but it can be detected one photon at a time with an ultrasensitive imaging detector to reveal growth rate and movement of the cells within the living animal. This level of sensitivity is comparable to that of the human eye after full adaptation to the dark.
Using this novel approach, it is now possible to observe the effects in the body of antitumor drugs and antibiotic or antiviral treatments. Indeed an ultimate goal is to make the body essentially transparent for medical diagnostics, and to use advanced optical tools to understand how pathogens cause disease and how the host organism responds to pathogens and treatments, without having to resort to invasive surgical techniques.









