8
Academia
The health of the public during the twenty-first century can be assured only through the cooperation and collaboration of many individuals in diverse institutional settings, each of which has important contributions to make to this important and challenging endeavor. Among the recommendations in The Future of Public Health (IOM, 1988), several focused on needed improvements in academia regarding the education of public health professionals. The report called for the following changes:
-
Creating new linkages among public health schools and programs and public health agencies at the federal, state, and local levels;
-
Developing new relationships within universities between public health schools and programs and other professional schools and departments;
-
Formulating more extensive approaches to education that encompass the full scope of public health practice;
-
Strengthening the knowledge base in the areas of international health and the health of minority groups;
-
Conducting a wide range of research that includes basic and applied research, as well as research on program evaluation and implementation; and
-
Developing new training opportunities for professionals who are already practicing in public health.
There has been progress in most of these areas. For example, collaborations and partnerships are receiving increased emphasis, practice-based
research efforts are expanding, and certificate programs and distance-learning programs aimed at providing lifelong learning to practicing public health workers have grown. Much more can be achieved, but these improvements are dependent on a critical analysis of the functions of academia, an examination of academia’s potential contributions to the public health system, and a discussion of recommendations made to enhance academia’s capacity to make these contributions.
Academia performs three important functions within the public health system. These are to (1) educate and train public health workers; (2) conduct basic and applied research in disciplines pertinent to public health; and (3) engage in community, public, and professional service. Of course, academia is not the only institution that provides education, research, and service. Federal, state, and local public health agencies, for example, provide training to public health workers. Public health agencies and the Centers for Disease Control and Prevention (CDC) conduct community-based research. Federal and state health agencies collect and disseminate valuable, credible information and statistics for the nation through vehicles such as the National Health Interview Survey, the Vital Statistics system, and the publication Morbidity and Mortality Weekly Report. The Public Health Faculty/Agency Forum, convened by CDC and the Health Resources and Services Administration (HRSA), illustrates one way in which nonacademic institutions convene and foster cooperation and coordination between academia and public health agencies in support of community health.
Although numerous federal, state, and local agencies make important contributions through education and training, information dissemination, collaborative activities, and research, these functions are central to the mission of academia. These functions are not, however, mutually exclusive. For example, service learning (defined as a method by which students learn through active participation in organized service experiences that meet actual community needs [Rhoads and Howard, 1998]) can be classified under the education and training function as well as the service function. Community-based participatory research is another example. Although it is clearly classified under the research function of academia, this approach to research is also a component of the service function because it is conducted in a collaborative fashion with the community and addresses problems identified as important by the community.
The emphasis of this chapter is on how academia fulfills its responsibilities for assuring the health of the public through education (and training), research, and service. For the purposes of this discussion, “academia” refers to all units within community and 4-year colleges and universities that contribute to assuring the health of the population.
EDUCATION AND TRAINING
The “most distinctive role of public health education lies in the preparation of public health professionals” (Fineberg et al., 1994). Because of the critical role of education in preparing public health professionals to function effectively, the Institute of Medicine (IOM) convened the Committee on Educating Public Health Professionals for the 21st Century that, concurrent with the work of the Committee on Assuring the Health of the Public in the 21st Century, has conducted an in-depth examination of the future needs of public health professional education and developed a framework and recommendations for how, over the next 5 to 10 years, education, training, and research in programs and schools of public health can be strengthened to prepare future public health professionals to improve population health.
Given the in-depth examination and analysis of public health education that was undertaken by the IOM Committee on Educating Public Health Professionals for the 21st Century, the present report will not go into detail about the future of public health education but, rather, will briefly describe the kinds of degree and professional development programs available, discusses the current workforce and its training needs, identifies problems and barriers to providing public health education, and makes recommendations for maximizing academia’s contributions to the education of the current and future public health workforce.
People who work as professionals in the public health system receive their education and training in a wide range of disciplines and in diverse academic settings, including schools of public health, medicine, nursing, dentistry, social work, allied health professions, pharmacy, law, public administration, veterinary medicine, engineering, environmental sciences, biology, microbiology, and journalism.
The master of public health (MPH) is the basic professional degree traditionally earned by public health workers, but many college graduates who work in public health are educated in other health professions. For example, nurses make up about 10.9 percent of the total public health workforce, whereas physicians comprise about 1.3 percent (HRSA, 2000a). The doctor of public health (DrPH) is offered for advanced training in public health leadership. Individuals with academic degrees (e.g., a master of science or doctorate) in the public health disciplines such as epidemiology, biostatistics, environmental health, health services and administration, nutrition, and the social and behavioral sciences also may be found in the larger state and local public health agencies and in the health care delivery system.
The 32 accredited schools of public health, along with the 45 accredited MPH programs, supply the bulk of public health graduates. The Association of Schools of Public Health (ASPH), the organization that represents accredited schools of public health, reports that in 1998–1999, the 29
accredited schools of public health graduated 5,568 students. Of all degree recipients, 89.9 percent received a master’s degree (61.5 percent received an MPH degree) and 10.1 percent received doctoral degrees (of these, 6.7 percent received a doctor of philosophy [PhD] degree and 2 percent received a DrPH degree) (ASPH, 2000). It is estimated that accredited graduate programs in community health and preventive medicine and in community health education graduate an additional 700 to 800 master’s degree students each year (Davis and Dandoy, 2001). Many of these graduate programs in public health are represented by the Association of Teachers of Preventive Medicine. Additionally, in 1997–1998 there were 9,947 master’s graduates of programs of public administration and public affairs, many of whom emphasized health policy and management and public health in their training (National Association of Schools of Public Affairs and Administration, 1998). The Association of University Programs in Health Administration reports that in 2000 there were 1,778 graduates who received master’s degrees (in health administration); some (an unknown number) of them received the MPH and master of science degrees (Association of University Programs in Health Administration, 2000). Many public health workers also receive undergraduate training from 4-year institutions that offer programs in the environmental sciences or in health education and health promotion. These programs can offer valuable continuing education to health workers by providing current scientific information in many specialized areas.
Those who graduate with training in public health are only a small part of the public health workforce. Although it is unclear exactly how many public health workers there are in the United States today, it is estimated that about 450,000 people are employed in salaried positions in public health and that an additional 2.85 million people volunteer their services (HRSA, 2000a). This is probably an undercount because, according to HRSA, states reporting the number of workers within their jurisdictions almost never include information about public health workers found in nongovernmental and community partner agencies. Additionally, limited information is obtained regarding the numbers of volunteers and salaried staff in voluntary agencies.
Kennedy and colleagues (1999), in an 18-month study of the Texas public health workforce, counted nearly 17,700 professional public health workers in that state. Only one-third of the professional public health workforce identified in that study was employed in official public health agencies, and only an estimated 7 percent had formal education in public health. Nationally, it is estimated that about 80 percent of public health workers lack basic training in public health (CDC, 2001a). Furthermore, only 22 percent of chief executives of local health departments have graduate degrees in public health (Turnock, 2001).
Public Health Education and Training
Basic public health training has changed over the years. Early public health efforts in the United States were directed toward improving sanitation and ensuring the safety of the food and water supply, controlling infectious diseases, and providing immunizations to children. Thus, in the early 1900s, the public health workforce was trained primarily in medicine, nursing, and the biological sciences (Brandt and Gardner, 2000; Garrett, 2000; Mullan, 2000). Basic public health training now requires an approach that incorporates understanding of the following:
-
Health problems must be examined in the context of defined populations;
-
Many problems of public health are deeply rooted in the behavior of individuals and in their social context;
-
Public health problems of the twenty-first century are rooted in the technologies of economic development; and
-
Public health problems continue to require the engagement of the body politic, in the form of government participation, for their solution (Fineberg et al., 1994).
Additionally, changing demographics in the United States and the importance of community engagement in problem solving contribute to the need for a more broadly trained and diverse workforce. Involvement in global health issues also argues for increased attention to workforce diversity, but achieving such diversity in the workforce is a major challenge for governmental public health agencies and other public health entities because of the inadequate number of students and faculty from ethnic minority groups. Without high school and undergraduate degree programs in public health, there is little exposure of potential minority candidates to public health as a career option. A related issue is the lack of ethnic minority faculty in programs and schools of public health. Public health agencies, schools and programs of public health, professional organizations, and other components of the public health system need to devote major efforts to identify and facilitate, through funding and other mechanisms, approaches to increase cultural diversity, as well as to enhance awareness of global health issues among public health faculty, students, and staff. For example, many schools of public health have established programs that provide students with practical experiences working abroad, offer short-term international internships as well as fellowship programs related to global health, and engage in international research collaboration on major global health issues.
Recent efforts directed toward achieving the goal of a broadly trained
workforce have focused on identifying basic competencies in public health and developing curricula that teach the information and skills necessary to meet those competencies. A number of different organizations have tackled this task. For example, the Pew Health Professions Commission (O’Neil, 1998) has developed a set of 21 competencies for successful practice that apply to physicians, nurses, and allied health professionals. The Council on Linkages Between Academia and Public Health Practice has developed a set of core competencies for public health professionals that apply to three job categories: frontline staff, senior-level staff, and supervisory management staff (Council on Linkages, 2001).
The ASPH has endorsed the core competencies developed by the Council on Linkages and plans to develop additional and complementary competencies for MPH students. Furthermore, the CDC Office of Workforce Policy and Planning (CDC, 2001b) has developed a table of competency sets (see Appendix E), differentiated into the categories of
-
Core-basic public health (addresses the essential services of public health);
-
New topical areas (emergency response, genomics, law, informatics);
-
Functional areas (leadership, management, supervisory, secretarial);
-
Discipline-specific areas (professional, technical, entry-level students); and
-
Other topical areas (e.g., maternal and child health, environmental health, health communication, sexually transmitted diseases).
The preparation of students and workers to engage in effective public health practice requires not only a definition of competencies but also an educational approach that encompasses a necessarily broad range of skills and information. Integrated approaches to education and training are crucial.
Integrated Interdisciplinary Learning
One example of an effort to promote an integrated approach to education is the Medicine/Public Health Initiative, a national consortium created in 1994 under the joint leadership of the American Medical Association and the American Public Health Association and involved in efforts to improve the working relationship and bridge the gap between medical and public health practitioners. The initiative has the following seven primary goals:
-
To engage the community and change existing thinking to focus on improving the health of the community.
-
To change the educational process so that public health and medicine can enhance their understanding of each other’s practices.
-
To create joint research efforts by developing a common research agenda for public health and medicine by using the threefold approach of relaying advantages of joint research, using preventive medicine certification and training as a form of integrated learning, and supporting the funding of research that links medicine and public health.
-
To devise a shared view of health and illness so that public health and medicine can use a common conceptual framework of health and illness.
-
To work together in health care provision and integrate health promotion and prevention into clinical health care delivery systems.
-
To jointly develop health care assessment measures such as quality, effectiveness, and outcome evaluations.
-
To translate Initiative ideas into action.
The Initiative’s work led to the development of a program that funded 19 collaborative projects around the country (Phillips, 2000). The Agency for Health Care Policy and Research also funded three projects aiming to enhance cooperation between the medical and public health communities in the context of community-based health programs (AHCPR, 1997).
Preventive medicine certification and training is another example of integrated interdisciplinary learning. In preventive medicine training, the primary emphasis is on disease prevention and health promotion. There are currently 6,091 certified preventive medicine specialists in the United States, but the proportion of these specialists among all U.S. physicians is on the decline. The decline has been greatest among those training in public health, with the primary reason for the decline being inadequate funding (Lane, 2000).
In addition, it is critical for public health education to cross traditional boundaries and link more effectively with the educational programs for other health professionals. In 1998, the Josiah Macy, Jr., Foundation sponsored a conference entitled Education for More Synergistic Practice of Medicine and Public Health (Hager, 1999). The goal of the conference was to develop recommendations on how public health practitioners and physicians can be trained to collaborate with one another. During the conference, Lasker (1999) emphasized the importance of public health education for medical students, whereas Lumpkin (1999) discussed what to teach students of public health about medical practice. He pointed out that because of the changes in the issues facing public health, enrolling students no longer come primarily from the medical or nursing profession. This, in turn, means that those students do not have a working knowledge of the biomedical basis of medical treatment or of the medical treatment system.
To gain needed exposure to the academic disciplines and the actual practices of their counterparts, medical students must become acquainted
with epidemiology, biostatistics, public health policy, the elements of prevention, and other essentials of public health, whereas students of public health require familiarization with the workings of the health care delivery system, the pharmacological and therapeutic treatment of disease, and techniques of dealing with individual patients (Hagar, 1999).
Nursing education is another area for integrated interdisciplinary learning, such as linkages with education in public health. Although schools of nursing require course work in community and public health nursing at the bachelor’s level, there is a great deal of variation in the content of these programs. In 2001, there were 85 schools of nursing that offered master’s degrees in community health and/or public health nursing (Berlin, 2002). Model curricula incorporating public health content into bachelor’s nursing curricula are lacking; an insufficient number of nursing faculty are prepared in public health; and access to public health agencies for population-based clinical experience is often a problem, as is access to continuing education in population-based public health and public health nursing. For additional information about preparing nurses to enter the public health workforce, refer to Who Will Keep the Public Healthy? (IOM, 2003).
Unfortunately, efforts to integrate teaching across schools and departments face several institutional barriers. First, most schools and colleges are departmentalized, with the resources provided for teaching distributed among the departments. Departmental priorities lie with ensuring that courses for majors and service courses are taught within the department’s discipline. Faculty who teach departmental, discipline-based courses are provided with both monetary support for teaching such courses and recognition by their departmental colleagues for contributing to the department’s teaching load.
At present, either integrated interdisciplinary courses must receive funding from sources outside the various departments involved, or each department supporting the disciplines involved in integrated interdisciplinary courses must agree to contribute faculty teaching time to the teaching efforts. Even when such agreements among departments can be reached, faculty are still reluctant to participate because the development and teaching of integrated interdisciplinary courses usually require more time than that required to teach a course in one’s own discipline. This additional time is usually not recognized in either commensurate pay or teaching credit.
A second disincentive for faculty participation in integrated interdisciplinary educational approaches relates to promotion and salary review. Faculty teaching integrated interdisciplinary courses may be penalized during promotion and salary merit review because their departmental colleagues know little of their interdisciplinary teaching activities or do not value such activities as highly as they value contributions to the department’s
curriculum. Because integrated interdisciplinary teaching is important to the preparation of a well-trained workforce that is capable of addressing today’s broad array of public health issues, academic institutions must ensure that funds are available for integrated interdisciplinary teaching activities and must provide incentives in their reward structures for faculty participating in such activities.
The emerging focus of a broad education based on competencies, both basic and discipline specific, is important. However, the need for public health students to understand medical practice and for physicians to understand public health practice, including the ethical and legal foundations of public health, must be kept in mind. The committee endorses the findings of the Macy Foundation conference—that there must be greater synergy between education for medicine and education for public health—and extends that endorsement of synergy to education in other clinical health science professions.
Therefore, the committee recommends that academic institutions increase integrated interdisciplinary learning opportunities for students in public health and other related health science professions. Such efforts should include not only multidisciplinary education but also interdisciplinary education and appropriate incentives for faculty to undertake such activities. Additional discussion of the need to increase collaboration and education between public health and other health professions can be found in the report Who Will Keep the Public Healthy?, developed by the IOM Committee on Educating Public Health Professionals for the 21st Century (IOM, 2003).
Public health workers should be trained in a set of core public health competencies and should have opportunities for practical experience; and additional education and training must be tailored to and depend on the experiences, activities, and functions of particular groups. For example, current MPH students have training needs that differ from those of past graduates of such programs who have been practicing for many years in a public health agency. The training needs of public health nurses differ in critical ways from the training needs of health educators, administrators, and environmental professionals. Identification of these specific training needs requires assessment and evaluation.
Solloway and colleagues (1997) reported on a study funded by HRSA to assess state agency-based health workforce capacity and examine state training and educational needs in five states: Illinois, Maryland, Missouri, Oregon, and Rhode Island. The authors report that most state public health workers have no formal education or training in the field of public health, lack a good understanding of the goals and mission of public health, and do not have a full understanding of the activities carried out by public health
workers outside their own units or departments. They identified educational and training needs in eight areas:
-
Information systems and computer skills
-
Technical writing and presentation skills
-
Research and policy development skills
-
Management and administrative skills
-
Grantsmanship
-
Public relations
-
Transition skills
-
Leadership skills
The study also found that states need federal support to obtain technical assistance for the acquisition and use of new technologies for distance-based or remote-site learning, ongoing financial support, and symbolic support demonstrating that training and education are valued and are priorities.
Another study conducted by Reder and colleagues (1999) assessed the training needs of public health professionals in Washington State. They found that communication was the area in which public health professionals require the most training, with the four most highly rated topics being interpersonal communication, cross-cultural and cross-age communication, electronic communication, and participatory teaching and training skills.
The educational and training needs of the current public health workforce are enormous and multifaceted. Academia has an essential and unique role to play in ensuring that broad-based educational and training opportunities are available on a regional basis. All accredited MPH programs, school based or otherwise, are required to provide some continuing education; however, what is offered varies widely depending on the available resources and expertise. With the advent of new and expanding information technologies, the opportunity for schools and programs to provide education and training to a broader audience via distance learning is increasing rapidly. The means for achieving this are discussed further in the chapter on the governmental public health infrastructure (Chapter 3). Although academia can play a leadership role in the coordination of various educational and training opportunities for the public health workforce, it cannot meet all of these needs. In some cases, practitioners in the field can best provide in-service training.
Funding of Public Health Professional Education and Training
A current lack of funding is a major problem in providing training and education for both students seeking degrees and those already in the public
health workforce. According to Gebbie (1999), the primary barrier to workforce development is the “incredibly weak” budget allocated for training. This has not always been the case, however. Over the past five decades, the major sources of funds for the training of students in public health were HRSA and CDC. Table 8–1 provides a chronology of legislation authorizing funds for health professional training in public health between 1956 and 1976 (DHHS, 1980).
In 1976, Congress passed the Health Professions Educational Assistance Act (P.L. 94–484). This act provided for a number of programs in health professions education, including
-
Extensions of existing public health traineeships.
-
Grants to accredited schools of public health for student traineeships.
-
A separate program of grants to public or nonprofit private educational entities (excluding schools of public health) that offered an accredited program in health administration, hospital administration, or health policy analysis and planning.
-
Funding to public or nonprofit private educational entities (excluding schools of public health) for graduate programs in health administration.
-
Grants to assist accredited schools of public health and other public or nonprofit educational entities with accredited graduate programs in health administration, health planning, or health policy analysis and planning in meeting costs of special projects to develop new programs or expand existing ones in the same four public health disciplines mentioned above.
-
A requirement for the Secretary of Health and Human Services, in coordination with the National Center for Health Statistics, to continuously develop and disseminate statistics and other information on the supply of and need for different types of public and community health personnel.
Between 1980 and 1987, spending by the Bureau of Health Professions (which is part of HRSA in the Department of Health and Human Services [DHHS]) for education in all health professions declined yearly, from a high of $411,469,000 in 1980 to $189,353,000 in 1987. General-purpose traineeship grants to schools of public health went from $6,842,000 in 1980 to $2,958,000 in 1987. Curriculum development grants, funded at $7,456,000 in 1980, were not funded at all in 1981 and 1982; but the funding recovered slowly in 1983, with funding at $1,740,000, and increased in 1984 to $2,856,000 and reached $9,787,000 in 1987. Grants for graduate programs in health administration were
TABLE 8–1 Funding Legislation for Health Professional Training
|
Legislation |
Description |
|
P.L. 84–911. Health Amendments Act of 1956 |
Authorized a 3-year program of grants to public or other nonprofit institutions or to individuals for traineeship awards for graduate or specialized training in public health. |
|
P.L. 85–544. Public Health— Training and Services—Grants-in-Aid |
Authorized awards of not more than $1 million in grants-in-aid for provision in public or nonprofit accredited schools of public health of comprehensive professional training, specialized consultative services, and technical assistance in the fields of public health and the administration of state and local public health programs. |
|
P.L. 86–106. An Act to Extend Certain Traineeship Provisions of the Health Amendments Act of 1956 |
Extended for 5 years (through fiscal year [FY] 1964) the authority for traineeship awards for graduate or specialized training in public health. |
|
P.L. 86–720. An Act to Amend Title III of the Public Health Service Act to Authorize Project Grants for Graduate Training in Public Health |
Authorized the award of project grants to schools of public health and to schools of nursing and engineering that provide graduate or specialized training in public health for nurses or engineers, for the purpose of strengthening or expanding graduate public health training in such schools. Appropriation authorizations for the grants were $2 million a year for FY 1961 through 1965. |
|
P.L. 87–395. Community Health Services and Facilities Act of 1961 |
Extended for FY 1962 through 1966 the authority for grants-in-aid to schools of public health and increased the authorization from $1 million to $2.5 million. |
|
P.L. 88–497. Graduate Public Health Training Amendments of 1964 |
Extended for 5 years (through FY 1969) the authority for traineeship awards for professional public health personnel. Dollar limitations were $4.5 million for FY 1965, $7 million for FY 1966, $8 million for FY 1967, and $10 million each for FYs 1968 and 1969. Also increased authorization for project grants for graduate or specialized training in public health to $2.5 million for FY 1965 and extended the program for 4 additional years. |
|
P.L. 89–109. Community Health Services Extension Amendments of 1965 |
Extended through FY 1967 the grants-in-aid for schools of public health. |
|
Legislation |
Description |
|
P.L. 89–749. Comprehensive Health Planning and Public Health Services Amendments of 1966 |
Transferred authority for grants-in-aid to schools of public health and extended authority to FY 1968, with a $5 million appropriation authorized. |
|
P.L. 90–174. Partnership for Health Amendments of 1967 |
Extended for 2 years (through FY 1970) the authority for grants-in-aid to schools of public health, with up to $7 million authorized for 1970. |
|
P.L. 90–490. Health Manpower Act of 1968 |
Extended for 2 years (through FY 1971) authority for traineeship awards for professional public health personnel, with up to $14 million authorized for FY 1971, and extended through FY 1971 authority for project grants for graduate or specialized training in public health, with up to $12 million authorized for 1971. |
|
P.L. 91–208. Public Health Service Act Amendments |
Extended through FY 1973 authority for traineeship awards, with up to $18 million authorized for 1973. Also extended through FY 1973 authority for project grants for graduate or specialized training in public health, with up to $14 million authorized for FY 1971. Also extended through FY 1973 the authority for grants-in-aid, with up to $15 million authorized for FY 1973. |
|
P.L. 93–45. Health Programs Extension Act |
Extended through FY 1974 authority for traineeship awards, for project grants for graduate or specialized training in public health, and for grants-in-aid to schools of public health. For FYs 1975 and 1976, Congress passed continuing appropriations acts providing continuing authority and funding for public health training programs that would otherwise have expired on June 30, 1974. |
|
SOURCE: DHHS (1980). |
|
funded at $2,967,000 in 1980, dropped to $726,000 in 1981, and rose to $1,416,000 in 1982, where they remained fairly steady, with funding in 1987 being $1,482,000 (DHHS, 1988).
The 1990s saw funding levels remain approximately constant, so that increases in tuition and other costs have actually resulted in a reduction in the amount of public health professional education provided.
The Bureau of Health Professions has begun to create a nationwide network of Public Health Training Centers (HRSA, 2000b). The purpose of the program is to improve the nation’s public health system by strengthening the technical, scientific, managerial, and leadership competence of the current and future public health workforce. Each of the Public Health Training Centers for each respective state or region will work to
-
Assess the educational needs of and training materials and facilities available to local and state public health agencies;
-
Use distance-learning technology and other new educational approaches to provide both basic and specialized public health education;
-
Improve public health providers’ ability to interpret and make informed decisions based on relevant data and information;
-
Establish on-site educational programs in underserved areas;
-
Develop field-based educational opportunities for students from traditional on-campus graduate public health programs;
-
Develop new curricula for public health practitioners on emerging public health issues such as bioterrorism, behavioral and mental health, domestic and societal violence, and environmental health issues; and
-
Train lay workers from local boards of health and community health offices.
The centers are designed to offer training and continuing education programs to about 100,000 public health students and professionals each year. To date, 14 centers have been funded. These centers involve 35 academic institutions and more than 42 states. Funding levels range from about $250,000 to $500,000 per year per center, although the recommended levels were $1 million. Although this is a needed program, funds are insufficient to compensate for the reduction in training funds experienced over the past two decades. Adequate funding, especially in states with small and medium populations, would create the opportunity to release staff to prepare and provide training programs and to increase the number of sessions provided. Additionally, adequate funding would allow the training center to hire distance-learning specialists to aid in the preparation of courses.
CDC has also been a major supporter of education for public health professionals. The CDC Graduate Certificate Program (GCP) was a federally sponsored initiative directed primarily toward CDC field officers, state health department personnel, and selected others with at least 3 to 5 years of experience in public health practice. The programs were designed for midcareer professionals in public health practice who desired to further their professional standing. The program provided the means by which Public Health Advisors working in state and local health departments across the country could earn a graduate certificate in public health from one of four
accredited schools of public health: Tulane University School of Public Health and Tropical Medicine, Emory University Rollins School of Public Health, Johns Hopkins University Bloomberg School of Public Health, and University of Washington School of Public Health and Community Medicine.
Although originally designed for CDC staff, the GCP was later opened to all interested public health professionals. Core courses in epidemiology, health policy, health management, biostatistics, behavioral sciences, and health education were typically delivered in the first half of the program. In the later phase, students focused on one of the following specialty tracks: epidemiology and surveillance, health policy and management, or community health. The Graduate Certificate Program in Public Health began in 1996 and ended in January 2001, leaving programs with no resources to continue the training program.
In recent years, schools of public health have made praiseworthy efforts to form critical links with practice and community sectors. Most schools of public health now require practicums of their students; the development of collaborations and partnerships has received increasing emphasis (discussed below in the section Service); practice-based research efforts have been expanded (discussed in the section Research); and certificate programs and distance-learning programs aimed at providing lifelong learning to practicing public health workers have grown.
Development of certificate programs that emphasize core public health concepts is one response to the 1988 recommendation for programs aimed at educating the current workforce. This type of certificate is an abbreviated version of the MPH. The content of the program tends to emphasize the concepts from the five core content areas of knowledge basic to public health taught in MPH programs. Some schools also offer certificate programs that follow courses of study in the specific content areas of public health. Admissions standards and completion requirements vary with each certificate program. Courses within certificate programs generally must be taken for academic credit. The certificate is issued by the sponsor upon satisfactory completion of course work.
Academic institutions also offer summer institutes and courses aimed at the current workforce. A variety of subjects are covered in this manner, from basic biostatistics, epidemiology, and geographic information system applications to management and administration for middle to upper managers. Such programs can range in length from a 1-day course to weeklong offerings. At present, the majority of students pursuing degrees in professional public health programs are educated via classroom-based instruction. Such face-to-face contact in teaching is important for a number of reasons, not the least of which is that these close and continuing relationships help break down racial, cultural, and class barriers and promote trust and a sense of community (Citrin, 2001). Additionally, most planning and
collaborative work is best done at meetings and work sessions that physically bring people together.
Many academic institutions, along with state health agencies and CDC, offer short courses, seminars, or workshops addressing specific public health training needs. One approach taken to meet the demand for distance-based training is the Public Health Training Network. This network has provided training to nearly 1 million people on a wide range of subjects in a variety of formats: print-based self-instruction, interactive multimedia, videotapes, two-way audio conferences, and interactive satellite videoconferences (CDC, 2001c).
As distance-learning technology improves and new electronic delivery modalities become more widespread, online in-service training opportunities will be more accessible. These new approaches under development will assist in providing training opportunities for public health workers who are not able to participate in classroom-based educational programs. The use of web-based tools for education is referred to as distance learning (Riegelman and Persily, 2001). Distance-learning programs and new information technologies are perceived to be a boon to meeting the educational needs of the public health workforce in the United States (Cannon et al., 2001). Although this development builds on more than two decades of computer networking activities (e.g., e-mail and bulletin board systems), increased access to the Internet has produced phenomenal growth in the extent and scope of online education. Teaching and learning on the World Wide Web demand new and special skills from teachers and learners alike.
Another educational approach attracting attention is service learning, defined as the “method under which students learn and develop through active participation in thoughtfully organized service experiences that meet actual community needs, that are integrated into the student’s academic curriculum or provide structured time for reflection, and that enhance what is taught in school by extending student learning beyond the classroom and into the community” (Rhoads and Howard, 1998). According to Porter and Monard (2001) “understanding and fostering reciprocity is a central aim of service-learning programs,” meaning that service-learning programs differ from other practical educational approaches in that their intent is to benefit both the provider and the recipient of the service and to emphasize equally the provision of service and the learning experience (Cauley et al., 2001).
According to Howard (2001), three criteria must be met for a course to be considered service learning:
-
Service that is both relevant and meaningful to all stakeholder parties must be provided in the community.
-
The service must not only serve the community but also enhance student academic learning.
-
The service must also directly and intentionally prepare students for active civic participation in a diverse democratic society.
Service-learning programs benefit the community, the student, and academia. Academia depends on this type of learning to teach students about real-world public health. Students are able to translate their academic learning into practice activities. The community, particularly in rural and inner-city areas that may be experiencing a shortage of health professionals, is able to reap the benefit of services provided by students in these learning situations.
On the basis of the findings detailed in the preceding pages, the committee identifies the need for increased funding of public health training and education. Funding is needed to support existing and emerging mechanisms for training and education of public health students, public health workers, and others. The committee recommends that Congress increase funding for HRSA programs that provide financial support for students enrolled in public health degree programs through mechanisms such as training grants, loan repayments, and service obligation grants. Funding should also be provided to strengthen the Public Health Training Center program to effectively meet the educational needs of the existing public health workforce and to facilitate public health worker access to the centers. Support for leadership training of state and local health department directors and local community leaders should continue through funding of the National and Regional Public Health Leadership Institutes and distance-learning materials developed by HRSA and CDC.
The following section discusses the second important contribution of academia, research.
RESEARCH
Relevant, high-quality research is essential to health assessment, policy development, and assurance. Such research provides fresh insights and creative solutions to health problems and supplies the evidence base necessary for policy development and assurance activities. Public health practice is grounded in science, both the traditional medical and natural sciences (e.g., biology, microorganisms, vectors, and risks in the physical environment) and, increasingly, the social and behavioral sciences (e.g., anthropology, sociology, and psychology) that “affect our understanding of human culture and behaviors influencing health and illness” (Turnock, 2001). It is in academia that most such research is conducted. In addition to basic biomedical research and epidemiological studies that contribute to an understanding
of what makes people healthy, research on the multiple determinants of health has begun to enrich the understanding of the numbers and complexities of factors that determine the health of the population (see Chapter 2 for a more comprehensive discussion of the determinants of health).
Increased understanding of the determinants of health has demonstrated the importance of social and behavioral factors to health. McGinnis and Foege (1993) reported that about half of all causes of mortality in the United States are linked to social and behavioral factors and accidents. Several studies have shown the relationship between unintentional injuries and certain risk factors: for example, accessibility to firearms, use of alcohol and tobacco, and use of seat belts (Turnock, 2001). Other research has shown the influence of psychological risk factors on disease; for example, the management of diabetes is influenced by coping skills and family stresses; other research demonstrates that acute stress may trigger myocardial ischemia (IOM, 2001).
Another important area for increased research is public health systems research. Bialek (2000) makes the point that there is little scientific evidence about what constitutes effective public health departments. He defines public health systems research as “a field of inquiry using quantitative or qualitative methodology to examine the impact of the organization, financing, staffing, and management of systems on the access to, delivery, cost, outcomes, and quality of population-based services.” Turnock (2001) states that improving public health practice requires research that explicates the links and relationships of key processes, programs, and services or outputs. The limited amount of public health systems research conducted to date has produced some important findings, such as the findings that the effectiveness of local health departments does not appear to be influenced by jurisdiction size and full-time leadership appears to positively influence effectiveness (Bialek, 2000). The committee believes that public health systems research is an important area for increased attention.
Despite the many achievements of research, much remains to be accomplished. The vast majority of the nation’s health research resources have been directed toward biomedical research endeavors that cannot, by themselves, address the most significant challenges to improving the public’s health (IOM, 2000). Past and current research funding priorities focus especially on risk factor identification through either large- or small-scale epidemiological studies. Comparatively few resources have been devoted to supporting prevention research, community-based research, or the translation of research findings into practice. For example, in the area of obesity, a great deal of research is needed about causes and about appropriate and effective interventions. Despite a significant reduction since 1990 in the amount of dietary fat consumed by the population, the rate of obesity has increased significantly. Clearly, achieving a reduction in obesity is not as
simple as changing one risk factor, but will require interventions on multiple determinants at various levels.
Only 1 to 2 percent of the U.S. health care budget is spent on prevention, and a like imbalance exists between funding for basic biomedical research and for population-based prevention research (Scrimshaw et al., 2001). As a consequence, although the scientific literature includes an enormous amount of information about physical and biological risk factors for disease and disability, as well as more limited information about social and behavioral determinants of health, little of this knowledge has been translated into forms that are accessible or useful to local public health practitioners or to the community.
Although many scholars agree on the importance of prevention research, exact definitions of the term vary. According to Scrimshaw and colleagues (2001), this “lack of a consistent definition for prevention research decreases the conceptual clarity of the term and impedes the development of a clear understanding of prevention research.” Brownson and Simoes (1999) assert that prevention research focuses on determining the underlying causes of death, injury, and disability; research discoveries are then applied at the community level. CDC defines prevention research as research directly applicable to public health practice (Doll et al., 2001). Sattin (2001) states that prevention research is a multidisciplinary approach to discovering new ways to prolong the health, well-being, and self-sufficiency of all Americans; it focuses on preventing disease, injury, and disability. Scrimshaw and colleagues (2001) describe how prevention is frequently defined in terms of the self-interest of the person giving the definition.
Prevention is frequently categorized into three levels: primary, secondary, and tertiary. Primary prevention in public health is aimed at preventing an illness or disability from occurring. Secondary prevention efforts include interventions in illness to prevent continued illness or disability, whereas tertiary prevention activities attempt to limit further progression of illness or disability or to postpone death. Clinical preventive services are generally considered secondary or tertiary preventions. To increase the clarity of its discussion, the committee has chosen to define population-based prevention research using a modified version of the definition developed by the Association of Schools of Public Health (Spencer, 2000) for population-based prevention research, which
-
Addresses health problems that affect large numbers of people;
-
Involves a definable population and operates at the level of the whole person;
-
Evaluates the application and impacts of new discoveries on the actual health of the population; and
-
Focuses on behavioral or environmental (social, economic, cultural, physical) factors associated with primary and secondary prevention of disease in populations; the behavioral, biological, or clinical variations among populations; or the integration of behavioral, biological, and environmental factors.
As discussed previously, prevention research (including clinical preventive services research) has been underfunded and undervalued, yet it is crucial to understanding how to improve health. The following section of this chapter discusses the specific research approaches that the committee believes will, if properly funded, contribute greatly to the understanding of the determinants of health and to evaluation of the effectiveness of public health interventions.
Population-Based Research
The term population-based research means that the research focuses on groups or populations rather than individuals (Scrimshaw et al., 2001). Population-based research draws on populations or random samples of populations at a national, state, or local level. In general, it builds on an understanding of the determinants of health that includes multiple levels of influence, from environmental (both social and physical) to behavioral to individual (biological, genetic). Although all research does not incorporate all potential levels, increased understanding of etiology and prevention will come about by working at multiple levels. Examples of well-known population-based research include the Framingham Heart Study, which continues to yield new insights, and the Woman’s Health Initiative (see Box 8–1).
Although population-based studies are often used to generate hypotheses about the potential risk factors for disease, population studies can also test hypotheses developed in earlier studies. Most of the earlier population-based data collection focused on the biological and environmental risk factors for disease. There is, however, an increasingly rich amount of data about the social determinants of health (see Chapter 2), and investigators are poised on the brink of being able to link these social risk factors with biomedical factors, thereby developing a more complex model of disease and health through population-based studies.
Community-Based Research
Community-based research is an overarching concept of collaborative research that encompasses many different types of studies (e.g., applied, descriptive, and evaluative). Community-based participatory research is defined as research that involves all stakeholders in each aspect of a study
|
BOX 8–1 Research Definitions for Academia The term population based means that the research focuses on groups or populations rather than individuals (Scrimshaw et al., 2001). The following definitions are used in this report:
|
designed to evaluate the application and impact of new discoveries aimed at improving the health of a defined population, frequently involving the evaluation of interventions designed to promote health in community settings.
Community-based research is often divided into three distinct phases: formative, process, and summative (Valente, 2002). The length and nature of each of these stages vary depending on the type of project and type of study, but some general parameters can be described. Community-based research requires active partnerships between the community and researchers who may or may not be members of that community (Green et al., 2001). Partnerships and coalitions are necessary because no one agency has the resources, access, and trust relationships to address the wide range of community determinants of public health problems (Green et al., 2001). Clark (1999) states that research needs a three-way partnership of academia, public health practice groups, and community-based organizations. A key factor in establishing successful partnerships is trust (Nelson et al., 1999). Lack of trust and perceived lack of respect are frequently perceived to hinder effective community-based research (Israel et al., 1998).
The Formative Phase
In the first or formative phase, researchers and the community engage in activities that lay the groundwork for a successful partnership (Valente, 2002). Such activities include defining and agreeing on the mission, goals, and outcomes of the research; identifying strengths and assets within the community and the research institution; determining responsibilities; and establishing the decision-making process. Although some relations may already exist among potential partners, further developmental activities must be undertaken for each new project. For example, an existing network or coalition on tobacco prevention may be expanded to include nutrition activities. This network would then have to conduct a formal needs assessment that involves both the researchers and the community to identify health needs and set goals and objectives. The formative phase, whether it entails expanding an existing partnership or developing new relations among researchers and the community, is time-consuming and cannot be carried out without sufficient funds to support the activities described.
The Process Phase
During the process phase, potential intervention strategies and research instruments are designed and pilot tested among small community samples (Valente, 2002). Agreement must be reached on the health promotion strategies, specific media and messages, and research instruments after repeated iterations. Once agreement is reached, baseline data are collected and the intervention is implemented. Depending on the nature of the intervention, this phase could be short (e.g., 3 months) or quite long (years).
The Summative Phase
The summative phase of research begins after the intervention is completed or at a point when some assessment is needed (Valente, 2002). The summative phase includes collection of follow-up data and interviews with key stakeholders (such as project administrators or program recipients). This phase includes data analysis to determine the impact, specify the lessons learned, and develop recommendations for future activities (e.g., whether to expand the program and whether or how to modify the program). The summative phase is iterative because results need to be shared with key stakeholders. If the program is expanded and disseminated to other communities or settings, effectiveness evaluation is needed to determine whether the program can be generalized to these other settings and what lessons are learned as the program is implemented elsewhere.
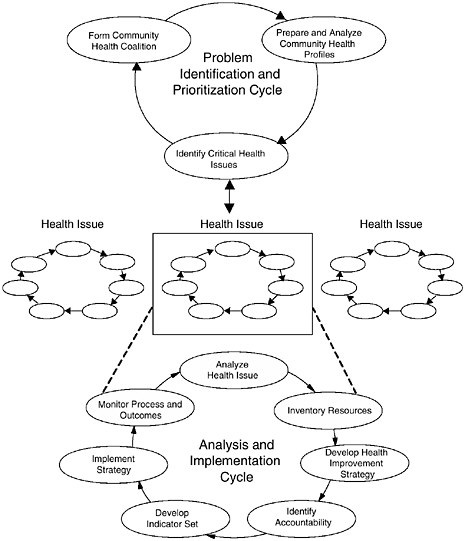
FIGURE 8–1 The Community Health Improvement Process (CHIP).
SOURCE: IOM (1997b).
Time Estimates for Research
Time estimates for each of these phases are imprecise, but experience has shown that, at a minimum, each phase will take at least 2 years in a modest-size program. A specific example of community-based research in which academia has the potential to contribute in many ways is the Community Health Improvement Process discussed in Chapter 4 (see Figure 8–1).
Unfortunately, academic institutions have undervalued community-based participatory research. It is sometimes perceived as lacking in rigorous methodology because it cannot use the randomized, single-intervention
evaluation approach. However, practice research demonstrates increased relevance to social goals with the translation of research findings into community action, thereby demonstrating the value to the nation of the use of public resources devoted to academic research; communities benefit from a program based on knowledge of evidence-based practice and community-relevant issues. Therefore, the committee recommends that federal funders of research and academic institutions recognize and reward faculty scholarship related to public health practice research.
Funding of Prevention Research
The Centers for Disease Control and Prevention
CDC, in collaboration with local, state, and other federal health and education agencies, plays a major role in prevention activities in the United States. In terms of research, CDC defines prevention research as research that is directly applicable to public health practice and views it as an important part of the CDC mission (Doll et al., 2001).
CDC has both intramural and extramural research programs. Intramural research (or CDC-directed research) is carried out within its laboratories or in the field in collaboration with state and local health departments. Extramural research, in which decision making regarding the study approach rests with the grantee, was, until the early 1970s, a relatively small grants program. During the next two decades it became decentralized, with programs developed and administered independently through CDC’s Centers, Institutes, and Offices (CIOs). More recently, CDC has begun to expand further as a supporter of extramural research (Doll et al., 2001).
CDC has three categories of extramural research programs: (1) program- or CIO-generated research; (2) investigator-initiated research; and (3) research centers of excellence. The following descriptions and examples of these types of research are taken from Doll et al. (2001).
Program- or CIO-Generated Research In program- or CIO-generated research, the topic (and perhaps the research approach as well) is determined by the CIO, which then publishes a request for application (RFA). Proposals are submitted to the CIO and then reviewed. Research topics in program-generated research have included the influence of folic acid on neural tube defects in China and the effectiveness of an intervention to reduce dating violence.
Another approach to program-generated research is to enter into cooperative agreements with health-related professional organizations with which CDC has agreements (e.g., the Association of the Schools of Public Health, the Minority Health Foundation, and the Association of American
Medical Colleges). Funding announcements are mailed to members of these organizations. Funds for the projects are provided by the CIOs and are administered by CDC’s Public Health Practice Program Office (PHPPO).
Investigator-Initiated Research at CDC In the investigator-initiated approach to research, applicants propose research in topic areas of their choosing or under broad topic areas provided by the CIOs. The Extramural Prevention Research Program (also known as the Prevention Research Initiative [PRI]) is one of the largest investigator-initiated research efforts at CDC and is administered by PHPPO. In 1999, with a budget of $12.5 million, CDC began the PRI and funded 50 research service endeavors at academic health centers, research centers, and university-affiliated programs. The average grant was approximately $250,000, and most service endeavors were funded for 3 years. Awards covered a range of subjects and included prevention of specific diseases (e.g., asthma and sexually transmitted diseases) and injury prevention (Sattin, 2001).
All grants and cooperative agreements in this program are externally peer reviewed and are administered by the scientifically appropriate CIOs. Plans for 2002 called for emphasizing investigator-initiated research grants in topic areas that cross-cut diseases, injuries, and conditions and that address gaps in individual CIO agendas. Awards are to be for larger amounts to allow evaluation of service endeavors targeting large populations or the subgroups at highest risk (Doll et al., 2001). A major problem, however, is the lack of a central, organized focus for investigator-initiated research. There is no defined unit to which applications are submitted, and there is no single source of information on the availability of grants.
All applications submitted to CDC requesting research funding are subject to review. CDC uses two approaches to review applications: (1) objective review and (2) external peer review. Objective review is a process that includes an independent assessment of the technical or scientific merit of research by panels composed of federal reviewers only, predominantly from CDC. The peer review process includes an independent assessment of the technical or scientific merit of research by predominantly nonfederal reviewers, scientists with knowledge and expertise equal to that of the researchers whose work they review (Sattin, 2001).
Although CDC has been active and is a leader in prevention research, there are several barriers to maximizing its investigator-initiated prevention research. First, although CDC has recently funded increased numbers of investigator-initiated research projects, this remains a relatively small endeavor that is too dependent on CIO-specific programs. Another barrier relates to the fact that CDC staff frequently play a more directive role than is acceptable for academic research. Additionally, project funding is often for too short a time, and indirect cost allowances (which are based on the
assumption that funding is for a health department that already receives substantial CDC funds) are too low to attract researchers from academic institutions with higher indirect rates.
Although CDC has strengthened its peer review process for investigator-initiated proposals, problems still exist. For example, administrative staff with no scientific training or scientists with no extramural program training frequently manage the peer review process and monitor funded projects (Doll et al., 2001). Finally, because CDC has no centralized office for the planning and coordinating of extramural peer review research programs, it is frequently difficult to know where to submit investigator-initiated proposals.
Prevention Research Centers The Prevention Research Center (PRC) program was authorized by Congress (P.L. 98–551) and established by CDC. This program, the largest research center program at CDC, is administered by the National Center for Chronic Disease Prevention and Health Promotion (Doll et al., 2001). To be funded as a PRC, a university must have a school of public health or a school of medicine or osteopathy with an accredited preventive medicine residency program, and the center must collaborate with individuals and organizations in the communities to determine research priorities (Doll et al., 2001). Each PRC focuses on projects related to a specific public health theme. The 24 currently funded PRCs and their research themes are listed in Table 8–2.
According to Scrimshaw and colleagues (2001), PRCs are the locus of leadership in community-based prevention efforts. They are intended to serve as bridges between science and practice and from academia to state and local health departments, health care providers and provider organizations, and community organizations, as well as CDC. Evaluation research is embedded in many of the PRC interventions; the centers also train public health professionals in applied prevention research (IOM, 1997a). Scrimshaw and colleagues (2001) attribute the successes of the PRCs to the fact that their research is collaborative, community based, interdisciplinary and multidisciplinary, problem solving and solution oriented, and “disseminative” and translatable.
Unfortunately, according to the IOM report (1997a) Linking Research and Public Health Practice, PRCs have not achieved the vision for which they were created, in large part because of insufficient funding. None were funded at their initially recommended level of $1 million per year. Most PRCs received only half of this amount, even though annual inflation increases would suggest the need for funding at levels higher than the original $1 million per year. Thus, the PRCs have not been able to build the infrastructure necessary to sustain the prevention research initiatives for which they were intended.
TABLE 8–2 Prevention Research Centers, 2001
|
Institution |
Year First Funded |
Research Theme |
|
University of Alabama, Birmingham |
1993 |
Bridging the gap between public health science and practice in underserved communities |
|
University of Arizona, Tucson |
1998 |
Promoting the health of multiethnic communities of the Southwest |
|
University of California, Berkeley |
1993 |
Chronic disease prevention: partnerships for action with families, neighborhoods, and communities |
|
University of California, Los Angeles |
1998 |
Starting adolescent health promotion and risk reduction at home |
|
University of Colorado, Denver |
1998 |
Promoting healthy lifestyles in rural communities |
|
Columbia University, New York City |
1990 |
Putting health promotion into action through community collaboration |
|
Harvard University, Boston |
1998 |
Nutrition and physical activity in children and youth |
|
University of Illinois, Chicago |
1990 |
A life-span approach to chronic disease prevention |
|
The Johns Hopkins University, Baltimore |
1993 |
Promoting adolescent health through families and communities |
|
University of Kentucky, Lexington |
2000 |
Controlling cancer in central Appalachia |
|
University of Michigan, Ann Arbor |
1998 |
Closing gaps and improving health through families and communities |
|
University of Minnesota, Minneapolis |
1996 |
Teen pregnancy prevention and youth development |
|
Morehouse School of Medicine, Atlanta |
1998 |
Risk reduction and early detection in African-American and other minority communities |
|
University of New Mexico, Albuquerque |
1995 |
Partnerships with Native American communities to improve health and well-being |
|
University of North Carolina, Chapel Hill |
1986 |
Improving community health through workplace health promotion |
|
Institution |
Year First Funded |
Research Theme |
|
University of Oklahoma, Oklahoma City |
1994 |
Promoting healthy behavior in Native American populations |
|
St. Louis University, St. Louis |
1994 |
Chronic disease prevention in high-risk communities |
|
University of South Carolina, Columbia |
1993 |
Promoting health through physical activity |
|
University of South Florida, Tampa |
1998 |
Community-based marketing for disease prevention and health promotion |
|
University of Texas, Houston Health Science Center |
1986 |
From healthy children to healthy adults |
|
Tulane Medical Center, New Orleans |
1998 |
Environmental agents and the health of communities |
|
University of Washington, Seattle |
1986 |
Keeping older adults healthy and independent by using community partnerships |
|
West Virginia University, Morgantown |
1994 |
Health promotion and disease prevention in rural Appalachia |
|
Yale University, New Haven |
1998 |
Public health initiatives across the prevention spectrum |
|
SOURCE: Doll et al. (2001). |
||
The committee recommends that the U.S. Congress provide funds for CDC to enhance its investigator-initiated program for prevention research while maintaining a strong CIO-generated research program. CDC should take steps that include
-
Expanding the external peer review mechanism for review of investigator-initiated research;
-
Allowing research to be conducted over the more generous time lines often required by prevention research; and
-
Establishing a central mechanism for coordination of investigator-initiated proposal submissions.
Furthermore, CDC should authorize an analysis of the funding levels necessary for effective Prevention Research Center functioning, taking into account the levels authorized by P.L. 98–551 as well as the amount of prevention research occurring in other institutions and organizations.
National Institutes of Health
The National Institutes of Health (NIH) is the single largest source of health research funding, with a fiscal year 2000 research budget of nearly $20 billion (compared to CDC’s total research budget of $570 million) (IOM, 2002). Although NIH emphasizes biomedical research, it is increasingly funding what it terms prevention research. It has invested in large-scale community trials (Green et al., 2001), conducts research on risk factors for disease, and evaluates drugs for secondary prevention of disease.
The National Institute of Environmental Health Sciences (NIEHS) developed a program in collaboration with the Environmental Protection Agency and CDC to “promote translation of basic research findings into applied intervention and prevention methods.” NIEHS conducts multidisciplinary basic, applied research, and “community-based prevention research,” including studies on the causes and mechanisms of children’s disorders having an environmental etiology; studies to identify relevant environmental exposures; intervention studies to reduce hazardous exposures and their adverse effects; and studies to decrease the prevalence, morbidity, and mortality of environmentally related childhood diseases (NIH, 2002a).
Eight Centers for Children’s Environmental Health and Disease Prevention Research were funded to conduct the first set of studies that will focus on respiratory disease and growth and development. The National Institute of Child Health and Human Development web page (NIH, 2002b) describes several prevention research projects, which include studies designed to conduct the following activities:
-
Test the efficacy of a multicomponent program of school-based interventions for the primary prevention of problem behavior in a sample of middle school students;
-
Identify determinants of the lack of age-appropriate immunizations;
-
Examine the efficacy of an integrated system of office-based primary pediatric care interventions for the prevention of medically attended injuries;
-
Assess determinants of parent-to-child transfer of responsibility for asthma self-management;
-
Determine whether parent and teen expectations predict teens’ driving behaviors during their first year of driving; and
-
Determine relevant factors and effective interventions for family management of type 1 diabetes.
Despite the many NIH-funded research activities labeled as prevention research, these efforts tend to focus on individual health and on secondary prevention and risk factor analysis rather than on the health of populations
(Scrimshaw et al., 2001). This committee has defined community-based prevention research as a collaborative approach that involves all stakeholders in each aspect of a study designed to evaluate the application and impact of new discoveries aimed at improving the health of a defined population. The findings detailed in this section demonstrate that assuring adequate funding for prevention research is a population health priority and is particularly relevant to the work of the nation’s federal agencies engaged in public health research. Therefore, the committee recommends that NIH increase the portion of its budget allocated to population- and community-based prevention research that
-
Addresses population-level health problems;
-
Involves a definable population and operates at the level of the whole person;
-
Evaluates the application and impacts of new discoveries on the actual health of the population; and
-
Focuses on the behavioral and environmental (social, economic, cultural, physical) factors associated with primary and secondary prevention of disease and disability in populations.
Furthermore, the committee recommends that the Director of NIH report annually to the Secretary of DHHS on the scope of the population-and community-based prevention research activities undertaken by the NIH centers and institutes.
SERVICE
Although service has traditionally been viewed as a responsibility of academic faculty, it has been seen as less important than the functions of teaching and research. However, in public health there is growing discussion about the importance of service as a scholarly activity that contributes not only to the knowledge base but also to improving the health of the public. This section examines the role of academia in providing service to the community through collaborative efforts (participation in training centers and institutes, service learning, and other mechanisms). Next, barriers to active participation in service are discussed, and a recommendation for overcoming the impediments to faculty participation in scholarly service activities is made.
A Pew Health Professions Commission report (O’Neil, 1998) stated, “The nation and its health professionals will be best served when public service is a significant part of the typical path to professional practice.” The academic community provides three kinds of service:
-
Community service, that is, service to state and local health departments, community organizations, and individuals;
-
Policy guidance, that is, helping to inform the public debate; and
-
Service to the profession, for example, providing peer review for professional journals, serving as officers of professional associations, and serving on committees both within academia and for professional organizations.
As the center of expertise in research and teaching, academia is uniquely positioned to provide technical assistance and service, based on credible evidence from its research and the expertise of its faculty and students, for the development and implementation of programs and policies designed to assure and improve the health of the public. For example, state public health departments might use academically developed information about computer technology and health informatics to implement a statewide surveillance and information system. Community workers might use the results of research on nutrition and behavior modification to organize a campaign designed to address the current obesity epidemic. Health care delivery systems use information and expertise developed in academia to design and implement smoking cessation programs and to coordinate efforts aimed at preventing and managing diabetes. Businesses and employers rely on academia for consultation on the design, implementation, and analysis of therapeutic intervention studies. Policy makers might respond to information emerging from academia that points to the need for new legislative or regulatory programs, for example, the presence of toxic residues in children resulting from exposure to residential pesticide use. Finally, the media use evidence developed in academia to inform the public regarding the impact of global infections on health.
Collaboration
As communities try to address their health issues in a comprehensive manner, all of the stakeholders will need to sort out their roles and responsibilities, which will vary from community to community. These interdependent sectors must address issues of shared responsibility for various aspects of community health and individual accountability for their actions. They also must participate in the process of communitywide social change that is necessary for health improvement efforts and related performance monitoring to succeed (IOM, 1997b).
Fundamental to effective service is effective collaboration. Emerging emphasis is being placed on academia’s participation in collaborations, partnerships, and coalitions as mechanisms for improving the health of the public. Nelson and colleagues (1999) define collaboration as “a purposive
relationship between partners committed to pursuing both an individual and a collective benefit.” According to Berkowitz (2000), collaboration is “a method used by members of communities when developing coalitions, by organizations when doing strategic planning, and by researchers who desire the partnership of those being studied.” Feighery and Rogers (1990) define a coalition as “an organization of individuals representing diverse organizations, factions or constituencies who agree to work together in order to achieve a common goal.”
Collaborations are attractive for a number of reasons. They emphasize communitywide behavioral change through the use of a “multicomponent, multisector” approach to changing the environments that establish and maintain behaviors (Roussos and Fawcett, 2000). Success in affecting today’s public health problems and their determinants requires the resources and trust relationships of a broad-based coalition of partners (Green et al., 2001). Bringing together people with different perspectives increases the potential to identify new and better ways of thinking about health issues (Lasker, 2000). Additionally, governmental financial and programmatic constraints require health partnerships, coalitions, and shared resources to achieve public health objectives (Baker et al., 1994).
What makes for a successful collaboration? The results of a study conducted by Kegler and colleagues (1998) to identify factors that contribute to coalition effectiveness suggest that coalitions with higher-quality action plans are better able to mobilize resources and implement activities, and that good communication, devotion of sufficient staff time to the coalition, a sense of cohesion, and a defined structure with multiple task forces appear to be related to the ability to implement activities. Such findings support the idea that developmental or formative activities are important for project success. Butterfoss and colleagues (1993) suggest that coalitions develop in stages (formation, implementation, maintenance, and outcomes) and that different sets of factors may be important to coalition functioning at each stage. For example, articulation of a clear mission, a spirit of cooperation, and positive expectations of outcomes are important during the formation stage, whereas formalization or definition of operational procedures, a strong central leadership, pooling of member assets (e.g., staff support, fundraising capability, meeting space, and access to relevant policy makers), the degree of membership participation, the continued perception of the partners that the benefits outweigh the costs of participation, and skills training are important during the implementation and maintenance stages.
Active involvement by many different parts of the community is believed to increase the likelihood of success for collaborative efforts (Feighery and Rogers, 1990; Israel et al., 1998; Lantz et al., 2001; Seifer and Krauer, 2001). Coalitions take time to coalesce; and the issues to be addressed
immediately include agreement on a mission statement with goals and objectives, clarification of roles and relationships, definition of a decision-making process, development of an organizational structure, the frequency and length of meetings, and the benefits for each member of the coalition (Feighery and Rogers, 1990).
The benefits of successful collaborative efforts and partnerships are many. Collaborations can reduce disparity in access to information, resources, and skills; increase public health’s understanding of community needs and assets; and lead to the development of a process for continual improvement in public policy and health systems (Berkowitz, 2000). Additional benefits include the freedom to become involved in new issues without bearing sole responsibility for managing or developing those issues; developing widespread public support for issues, actions, or unmet needs; developing a critical mass for action; minimizing duplication of effort and services; mobilizing a broad array of talents, resources, and approaches to problem solving; providing a mechanism for recruiting participants with diverse backgrounds and beliefs; and having flexibility in providing an opportunity to exploit new resources in changing situations (Butterfoss et al., 1993; Green et al., 2001).
Centers and Institutes
Academia engages in service to the community in many ways. One approach to service is through various centers and institutes. For example, in 2002 the University of Washington’s Center for Ecogenetics and Environmental Health conducted a town meeting to engage in discussions with the community on racial disparity, poverty, and pollution. Activities brought together researchers, legislators, and community members to discuss the health risks of pesticides to agricultural workers and their families, contamination of seafood by marine toxins and chemical pollutants, hazardous waste sites, culturally appropriate research strategies, and links between indoor and outdoor air pollution and asthma. These discussions led to a number of projects designed to address community-identified concerns and needs.
The three newly funded CDC Centers for Genomics and Public Health, located at the University of Michigan, University of North Carolina, and University of Washington, are another mechanism through which service to the community can be provided. Each center will develop a regional hub of expertise for the use of genetic information to improve health and prevent disease. In addition to contributing to the knowledge base on genomics and public health and providing training for the public health workforce, the centers are to provide technical assistance to regional, state, and local public health organizations. “With this collaborative approach, CDC hopes to
. . . demonstrate—through real examples—the translation of gene discoveries into disease prevention and improved health” (CDC, 2001d).
Of primary importance in providing service to the working public health community is the Public Health Leadership Institute. The institute was developed as a collaborative effort of CDC and the Western Consortium for Public Health to provide leadership training for senior public health officers in state and local health departments. The University of North Carolina now coordinates its efforts. Each year a cohort of senior public health officials is selected to participate in a 12-month program that includes self-study, teleconferences, electronic seminars, action-learning projects, and an intensive on-campus week. The curriculum is centered around four modules concerning the challenges to public health: the study of the future, leadership and vision, communication and information, and political and social change (Scutchfield et al., 1995). The institute has spawned the development and growth of regional leadership training efforts aimed at increasing the leadership skills of public health practitioners at various levels of the system. Other approaches to service include the summer institutes and courses discussed above in the section Education and Training. These institutes and courses provide education and training to state and local health departments and other members of the community.
Academia’s contributions to service also can be seen in the work of the Centers for Public Health Preparedness funded by CDC. There are academic centers, specialty centers, and local exemplar centers (see Table 8–3).
Academic centers aim to increase individual preparedness at the front line by linking schools of public health, state and local public health agencies, and other academic and community health partners. Specialty centers focus on a topic, professional discipline, core public health competency, practice setting, or application of learning technology. Local exemplar centers develop advanced applications at the community level in three areas: integrated communications and information systems, advanced operational readiness assessment, and comprehensive training and evaluation. Table 8– 3 lists the centers in existence as of the writing of this report.
The centers work in collaboration with partners across their regions to assure a well-trained and prepared public health workforce, informed health care providers, and an alert citizenry to protect against terrorism. In September 2000, CDC, the Association of Schools of Public Health, state and local public health agencies, and other academic communities entered into a partnership to begin development of a national system of Centers for Public Health Preparedness (DHHS, 2002).
Service learning (also discussed above in the section Education and Training) is another way in which academic institutions engage in community service. Academic service-learning organizations and activities are growing and include the following: (1) service-learning centers on college
TABLE 8–3 Centers for Public Health Preparedness
|
Type |
Location |
|
Academic centers |
University of Illinois at Chicago School of Public Health University of North Carolina, Chapel Hill, School of Public Health University of Washington School of Public Health and Community Medicine Columbia University Mailman School of Public Health University of Iowa College of Public Health University of South Florida College of Public Health St. Louis University School of Public Health |
|
Specialty centers |
Dartmouth College Medical School Interactive Media Laboratory Saint Louis University School of Public Health The Johns Hopkins University Bloomberg School of Public Health and the Georgetown University Law Center University of Findlay (Ohio) National Center of Excellence for Environmental Management |
|
Local exemplar centers |
DeKalb County Health Department Denver Public Health Monroe County Health Department |
campuses across the United States that support and facilitate student and faculty work in communities; (2) the National Service-Learning Exchange, which provides training and technical assistance to service-learning programs; (3) campus compact (a national organization of more than 750 college and university presidents), which offers workshops, tool kits, and publications aimed at encouraging student and faculty involvement in community and public service; (4) research opportunities and studies; and (5) a planned National Center for Service-Learning Research (Howard, 2001).
Barriers and Solutions
There are barriers to establishing successful collaborations and partnerships. Clark (1999) outlined four barriers or gaps:
-
Communication—a lack of a shared language and emphases;
-
Access—little access to skilled public health faculty by some practitioners and communities;
-
Credibility—practitioner skepticism of academic understanding and vice versa; and
-
Expectations—the failure of what it takes to operate in the real world to meet academic standards of scientific rigor.
Other investigators include as barriers perceived threats to a sense of autonomy, disagreement about community needs, conflicts over funding decisions, a lack of consensus about membership criteria or coalition structure, failure to include relevant constituencies, and a lack of leadership (Feighery and Rogers, 1990; Kreuter et al., 2000).
A continuing barrier to scholarly service and one of great concern relates to faculty rewards, promotion, and tenure. Public health practice activities are not generally valued or rewarded by most academic institutions. Israel and colleagues (2001) write that multiple means are needed to provide evidence and recognition of the scholarship of public health practice. They list a number of matters that must be addressed to overcome this barrier. For example, peer-reviewed journals must recognize difficult methodological issues associated with conducting community-based participatory research and should be willing to publish such articles. Universities need to expand their evaluation of reputable journals. Because faculty members may assist communities in preparing grant proposals, these activities should be recognized and valued by academic institutions. Similarly, training activities for and technical assistance to community partners should be given credit toward tenure and promotion.
Practice Scholarship
Efforts are in progress to overcome the institutional lack of recognition of public health practice and service as scholarly endeavors. Maurana and colleagues (2000) report on two evidence-based models for documenting and assessing community scholarship activities. The first model, the Points of Distinction Project, is part of the Outreach Committee of Michigan State University. This model identified quantitative and qualitative indicators of success for four dimensions of quality outreach. The service must have significance, in that the issues addressed are of importance and value to project goals. The context of the service is crucial, in that it should have a close fit with the environment, use appropriate expertise and methods, have a substantial degree of collaboration, and use resources sufficiently and creatively. The scholarship of the service should demonstrate appropriate application, generation, and use of knowledge. Lastly, the service should be able to demonstrate that it has influence on issues, institutions, and individuals.
The second model is the Competency-Based Model of Alverno College in Milwaukee, Wisconsin. This model divides scholarly activity into four competencies, each of which specifies skills, activities, and requirements
that faculty must master for promotion. These skills include being able to teach effectively, work responsibly in the college community, develop and pursue a research agenda, and serve the wider community.
The model proposed by Maurana and colleagues (2000) defines community scholarship as “the products that result from active, systematic engagement of academics with communities for such purposes as addressing a community-identified need, studying community problems and issues, and engaging in the development of programs that improve health.” They offer standards and criteria for assessment of this scholarship. Criteria evaluate goals, preparation, methods, results presentation, and reflective critique. The model also describes four types of community scholarship products:
-
Resources, such as how-to manuals, technical assistance, and tools and strategies to assess community strengths and assets or concerns;
-
Program outcomes, such as improved community health outcomes, increased community leadership and funding for health, and integration of students and residents into community-based efforts or creative education;
-
Dissemination, such as presentations, journal articles, and leadership at the national, state, and community levels; and
-
Other products, such as new or strengthened partnerships and coalitions and program development grants.
In Demonstrating Excellence, ASPH (1999:9) discusses the issue of service as scholarship:
Service is relevant as scholarship if it requires the use of professional knowledge, or general knowledge that results from one’s role as a faculty member. This knowledge is applied as consultant, professional expert, or technical advisor to the university community, the public health practice community, or professional practice organizations. The dimension of scholarship distinguishes practice-based service from a form of service known traditionally as the general responsibilities of citizenship.
To meet the requirements of scholarship as defined by ASPH, academic service must be provided through community-based participatory research, service learning or the work of the Prevention Research Centers, Centers for Genomics and Public Health, and Centers for Public Health Preparedness. Such activities to improve the health of the community not only fulfills academia’s obligation of service but also expands the knowledge base and contributes to improvements in the health of the public. The value of these contributions is great and should be acknowledged by academic institutions in their promotion and tenure policies.
For these reasons, the committee recommends that academic institu
tions develop criteria for recognizing and rewarding faculty scholarship related to service activities that strengthen public health practice.
CONCLUDING OBSERVATIONS
Academia, as one component of the public health system, provides important contributions to the health of the public in three ways: educating and training public health workers; conducting research in disciplines pertinent to public health; and engaging in community, public, and professional service. Numerous activities have been undertaken to educate and train the current and future public health workforce through methods such as classroom-based instruction, distance-learning programs, and training and leadership institutes. Stagnant and shrinking resources allocated to public health training are, however, impeding the ability of academic institutions to address today’s new and emerging health problems. If it is true that the public health workforce is at the heart of the nation’s ability to respond to new challenges such as emerging infections and preparedness against terrorist attacks, then that public health workforce must be adequately educated and trained to successfully face those challenges. This cannot be accomplished without making the training and education of public health workers the number one priority as demonstrated through adequate funding.
Academia has made major contributions to prolonging life and increasing the quality of life through research. Basic research has provided the knowledge necessary to develop precious vaccines that protect against debilitating and deadly diseases, whereas research on the determinants of health has demonstrated the importance of social and behavioral factors to health. However, comparatively few resources have been devoted to supporting prevention research, community-based research, or the translation of research findings into practice. Such resources must be found and allocated if academia is to continue to have a major impact on the health of communities. With the collaboration and partnership of academia, scholarly service has the potential to make great strides in engaging the community in improving its own health. However, without a restructuring of the reward system within universities and colleges, this most promising approach to change encounters barriers that are difficult to surmount.
Improvement of the public’s health faces great challenges. Academia is committed to working in partnership with other components of the public health system to meet these challenges. Yet, to be successful, the role of academia must be valued, and funding must be available to develop the programs and approaches needed for education and training, research, and service to improve the public’s health.
REFERENCES
AHCPR (Agency for Health Care Policy and Research). 1997. AHCPR funds project to foster collaboration between medicine and public health. In Research Activities Newsletter, No. 202. AHCPR Publication 97–0024. Rockville, MD: AHCPR.
ASPH (Association of Schools of Public Health). 1999. Demonstrating Excellence. Washington, DC: ASPH. Available online at http://www.asph.org/uploads/demon.pdf. Accessed March 17, 2002.
ASPH. 2000. 1999 Annual Data Report: Applications, New Enrollments & Students, and Fall 1999 Graduates, 1998–99 with Trends, 1989–1999. Washington, DC: ASPH.
Association of University Programs in Health Administration. 2000. Health Services Administration Education Director of Programs 2001–2002. Washington, DC: Association of University Programs in Health Administration.
Baker EL, Melton RJ, Stange PV, Fields ML, Koplan JP, Guerra FA, Satcher D. 1994. Health reform and the health of the public: forging community health partnerships. Journal of the American Medical Association 272(160):1276–1282.
Berkowitz B. 2000. Collaboration for health improvement: models for state, community, and academic partnerships. Journal of Public Health Management and Practice 6(1):67–72.
Berlin L. 2002. Special tabulation from the American Association of Colleges of Nursing 2001–2002 database. Washington, DC: American Association of Colleges of Nursing.
Bialek, R. 2000. Building the science base for public health practice. Journal of Public Health Management and Practice 6(5):51–58.
Brandt AM, Gardner M. 2000. Antagonism and accommodation: interpreting the relationship between public health and medicine in the United States during the 20th century. American Journal of Public Health 90(5):707–715.
Brownson RC, Simoes EJ. 1999. Measuring the impact of prevention research on public health practice. American Journal of Preventive Medicine 16(3 Suppl.):72–79.
Butterfoss FD, Goodman RM, Wandersman A. 1993. Community coalitions for prevention and health promotion. Health Education Research: Theory & Practice 8(3):315–330.
Cannon MM, Umble KE, Steckler A, Shay S. 2001. “We’re living what we’re learning”: student perspectives in distance learning degree and certificate programs in public health. Journal of Public Health Management and Practice 7(1):49–59.
Cauley K, Canfield A, Clasen C, Dobbins J, Hemphill S, Jaballas E, Walbroehl G. 2001. Service learning: integrating student learning and community service. Education for Health 14(2):173–181.
CDC (Centers for Disease Control and Prevention). 2000. Proceedings from the Public Health Workforce Development Expert Panel Workshop, November 1–2, 2000, Calloway Gardens, GA. Atlanta, GA: CDC.
CDC. 2001a. A Global Life-Long Learning System: Building a Stronger Frontline Against Health Threats. A Global and National Implementation Plan for Public Health Workforce Development. Revision date: January 5, 2001. Atlanta, GA: CDC.
CDC. 2001b. A collection of competency sets of public health-related occupations and professions. Available online at www.phppo.cdc.gov/workforce. Accessed August 30, 2001.
CDC. 2001c. What is PHTN? The history. Available online at http://www.phppo.cdc.gov/phtn/history.asp. Accessed October 31, 2002.
CDC. 2001d. Centers for Disease Control and Prevention (CDC) Awards Funds for Genetics Programs. CDC National Center for Environmental Health (NCEH) news release, October 18, 2001. Available online at www.cdc.gov/genomics/activities/fund2001.htm. Accessed October 31, 2002.
CDC and Agency for Toxic Substance and Disease Registry (ATSDR). 1999. Strategic Plan for Public Health Workforce Development: Toward a Life-Long Learning System for Public Health Practitioners. Atlanta, GA: CDC.
Citrin T. 2001. Enhancing public health research and learning through community-academic partnerships: the Michigan experience. Public Health Reports 116:74–78.
Clark, NM. 1999. Community/practice/academic partnerships in public health. American Journal of Preventive Medicine 16(3 Suppl.):18–19
Council on Linkages. 2001. Core Competencies for Public Health Professionals. Washington, DC: Public Health Foundation.
Davis MV, Dandoy S. 2001. Survey of Graduate Programs in Public Health and Preventive Medicine and Community Health Education. Washington, DC: Association of Teachers of Preventive Medicine and the Council on Education for Public Health.
DHHS (Department of Health and Human Services). 1980. Chronology of Health Professions Legislation: 1956–1979. Washington, DC: Office of Program Development, Bureau of Health Professions, Health Resources Administration.
DHHS. 1988. Bureau of Health Professions: Selected Summary Data on Fiscal Years 1980–87 Awards. ODAM Report 3–88. Washington, DC: Office of Data Analysis and Management, Bureau of Health Professions, Health Resources and Services Administration.
DHHS. 2002. HHS announces new funding for academic centers. Press release, February 6. Available online at www.hhs.gov/news. Accessed March 2, 2002.
Doll L, Berkelman R, Rosenfield A, Baker E. 2001. Extramural prevention research at the Centers for Disease Control and Prevention. Public Health Reports 116(Suppl. 1):10– 19.
Feighery E, Rogers T. 1990. Building and Maintaining Effective Coalitions, 2nd ed. Palo Alto, CA: Stanford Health Promotion Resource Center.
Fineberg HV, Green GM, Ware JH, Anderson BL. 1994. Changing public health training needs: professional education and the paradigm of public health. Annual Review of Public Health 15:237–257.
Garrett L. 2000. Betrayal of Trust: The Collapse of Global Public Health. New York: Hyperion.
Gebbie KM. 1999. The public health workforce: key to public health infrastructure. American Journal of Public Health 89(5):660–661.
Green LW, Mercer SL. 2001. Can public health researchers and agencies reconcile the push from funding bodies and the pull from communities? American Journal of Public Health 91(12):1926–1929.
Green L, Daniel M, Novick L. 2001. Partnerships and coalitions for community based research. Public Health Reports 116(Suppl. 1):20–30.
Hager, M. 1999. Education for More Synergistic Practice of Medicine and Public Health. New York: Josiah Macy, Jr., Foundation.
Howard J (Ed.). 2001. Service-Learning Course Design Workbook. Ann Arbor, MI: OCSL Press.
HRSA (Health Resources and Services Administration). 2000a. The public health workforce: enumeration 2000. Prepared for HRSA by Kristine Gebbie, Center for Health Policy, Columbia University School of Nursing, December. Washington, DC: HRSA.
HRSA. 2000b. Public health training centers. Available online at http://bhpr.hrsa.gov/publichealth/phtc.htm. Accessed October 31, 2002.
IOM (Institute of Medicine). 1988. The Future of Public Health. Washington, DC: National Academy Press.
IOM. 1997a. Linking Research and Public Health Practice: A Review of CDC’s Program of Centers for Research and Demonstration of Health Promotion and Disease. Washington, DC: National Academy Press.
IOM. 1997b. Improving Health in the Community: A Role for Performance Monitoring. Washington, DC: National Academy Press.
IOM. 2000. Promoting Health: Intervention Strategies from Social and Behavioral Research. Washington, DC: National Academy Press.
IOM. 2001. Health and Behavior: The Interplay of Biological, Behavioral, and Societal Influences. Washington, DC: National Academy Press.
IOM. 2002. The National Clinical Research Enterprise: Draft Discussion Paper of the Clinical Research Roundtable. Washington, DC: National Academy Press.
IOM. 2003. Who Will Keep the Public Healthy? Educating Public Health Professionals. Washington, DC: National Academy Press.
Israel BA, Schulz AJ, Parker EA, Becker AB. 1998. Review of community-based research: assessing partnership approaches to improve public health. Annual Review of Public Health 19:173–202.
Israel BA, Schulz AJ, Parker EA, Becker AB. 2001. Community-based participatory research: policy recommendations for promoting a partnership approach in health research. Education for Health 14(2):182–197.
Kegler MC, Steckler A, McLeroy K, Malek SH. 1998. Factors that contribute to effective community health promotion coalitions: a study of 10 project ASSIST coalitions in North Carolina. Health Education & Behavior 25(3):338–353.
Kennedy VC, Spears WD, Loe HD, Jr., Moore FI. 1999. Public health workforce information: a state-level study. Journal of Public Health Management Practice 5(3):10–19.
Kreuter MW, Lezin NA, Young LA. 2000. Evaluating community-based collaborative mechanisms: implications for practitioners. Health Promotion Practice 1(1):49–63.
Lane DS. 2000. A threat to the public health workforce: evidence from trends in preventive medicine certification and training. American Journal of Preventive Medicine 18(1):87– 96.
Lantz PM, Viruell-Fuentes E., Israel BA, Softley D, Guzman R. 2001. Can communities and academia work together on public health research? Evaluation results from a community-based participatory research partnership in Detroit. Journal of Urban Health: Bulletin of the New York Academy of Medicine 78(3): 495-507.
Lasker RD. 1999. What to teach medical students about public health for synergistic practice, pp. 148–158. In Hager M (Ed.). Education for More Synergistic Practice of Medicine and Public Health. New York: Josiah Macy, Jr., Foundation.
Lasker RD. 2000. Promoting Collaborations that Improve Health. Prepared for Discussion at Community-Campus Partnerships for Health’s 4th Annual Conference. New York: The New York Academy of Medicine Division of Public Health
Lumpkin J. 1999. What to teach students of public health about medical practice. In Hager M (Ed.). Education for More Synergistic Practice of Medicine and Public Health. New York: Josiah Macy, Jr., Foundation.
Maurana C, Wolff M, Beck BJ, Simpson DE. 2000. Working with Communities: Moving from Service to Scholarship in the Health Professions. Prepared for Discussion at Community-Campus Partnerships for Health’s 4th Annual Conference. San Francisco, CA: Community-Campus Partnerships for Health.
McGinnis JM, Foege WH. 1993. Actual causes of death in the United States. Journal of the American Medical Association 170(18):2207–2211.
Mullan F. 2000. Public health then and now. American Journal of Public Health 90(5):702– 706.
National Association of Schools of Public Affairs and Administration. 1998. Survey of Enrollment and Degrees—Academic Year 1997–1998. Washington, DC: National Association of Schools of Public Affairs and Administration.
Nelson JC, Rashid H, Galvin VG, Essien JDK, Levine LM. 1999. Public/private partners: key factors in creating a strategic alliance for community health. American Journal of Preventive Medicine 16(3 Suppl.):94–102.
NIH (National Institutes of Health). 2002a. Centers for Children’s Environmental Health and Disease Prevention Research. Division of Extramural Research and Training (DERT) website. Available online at www.niehs.nih.gov/dert/. Accessed October 31, 2002.
NIH. 2002b. Current research. Prevention Research Branch, National Institute for Child Health and Human Development (NICFD), NIH. Available online at www.nichd.nih.gov/about/despr/prbrsh.htm. Accessed October 31, 2002.
O’Neil EH, Pew Health Professions Commission. 1998. Recreating Health Professional Practice for a New Century. San Francisco, CA: Pew Health Professions Commission.
Phillips DF. 2000. Medicine–public health collaboration tested. Journal of the American Medical Association 283(4):465–467.
Porter M, Monard K. 2001. Ayni in the global village: building relationships of reciprocity through international service-learning. Michigan Journal of Community Service Learning Fall5–17.
Reder S, Gale JL, Taylor J. 1999. Using a dual method needs assessment to evaluate the training needs of public health professionals. Journal of Public Health Management and Practice 5(6):62–69.
Rhoads R, Howard J (Eds.). 1998. Academic Service Learning: A Pedagogy of Action and Reflection. San Francisco, CA: Josey-Bass Publishers.
Riegelman R, Persily NA. 2001. Health information systems and health communications: narrowband and broadband technologies as core public health competencies. American Journal of Public Health 91(8):1179–1195.
Roussos ST, Fawcett SB. 2000. A review of collaborative partnerships as a strategy for improving community health. Annual Review of Public Health 21:369–402.
Sattin RW. 2001. The Prevention Research Initiative and the peer review process at CDC. Public Health Reports 116(Suppl. 1):254–256.
Scrimshaw SC, White L, Koplan J. 2001. The meaning and value of prevention research. Public Health Reports 116(Suppl. 1):4–9.
Scutchfield FD, Spain C, Pointer DD, Hafey JM. 1995. The Public Health Leadership Institute: leadership training for state and local health officers. Journal of Public Health Policy 16(3):304–323.
Seifer S, Krauer P. 2001. Toward a policy agenda for community-campus partnerships. Education for Health 14(2):156–162.
Solloway M, Haack M, Evans L. 1997. Assessing the Training and Education Needs of the Public Health Workforce in Five States. Washington, DC: Center for Health Policy Research, Workforce Study Group, The George Washington University Medical Center.
Spencer HC. 2000. Testimony before the IOM Committee on Assuring the Health of the Public in the 21st Century. Washington, DC: Institute of Medicine.
Sullivan TJ. 2001. Methods of Social Research. Fort Worth, TX: Harcourt Brace and Co.
Turnock BJ. 2001. Public Health: What It Is and How It Works. Gaithersburg, MD: Aspen Publishers, Inc.
Valente TW. 2002. Evaluating Health Promotion Programs. New York: Oxford University Press.











































