2
Understanding Population Health and Its Determinants
For most people, thinking about health and health care is a very personal issue. Assuring the health of the public, however, goes beyond focusing on the health status of individuals; it requires a population health approach. As noted in Chapter 1, America’s health status does not match the nation’s substantial health investments. The work of assuring the nation’s health also faces dramatic change, systemic problems, and challenging societal norms and influences. Given these issues, the committee believes that it is necessary to transform national health policy, which traditionally has been grounded in a concern for personal health services and biomedical research that benefits the individual. Such repositioning will affirm and expand existing commitments to reflect a broader perspective. Approaching health from a population perspective commits the nation to understanding and acting on the full array of factors that affect health.
To best address the social, economic, and cultural environments at national, state, and local levels, the nation’s efforts must involve more than just the traditional sectors—the governmental public health agencies and the health care delivery system. As has been outlined in the preceding pages, what is needed is the creation of an effective intersectoral public health system. Furthermore, the efforts of the public health system must be supported by political will—which comes from elected officials who commit resources and influence based on evidence—and by “healthy” public policy—which comes from governmental agencies that consider health effects in developing agriculture, education, commerce, labor, transportation, and foreign policy.
This chapter describes the rationale behind a transformed approach to
addressing population health problems. This approach identifies key determinants of the nation’s health and presents evidence for their consideration in developing effective national strategies to assure population health and support the development of a public health system that blends the strengths and resources of diverse sectors and partners (IOM, 1997).
A POPULATION PERSPECTIVE
For nations to improve the health of their populations, some have cogently argued, they need to move beyond clinical interventions with high-risk groups. This concept was best articulated by Rose (1992), who noted that “medical thinking has been largely concerned with the needs of sick individuals.” Although this reflects an important mission for medicine and health care, it is a limited one that does little to prevent people from becoming sick in the first place, and it typically has disregarded issues related to disparities in access to and quality of preventive and treatment services. Personal health care is only one, and perhaps the least powerful, of several types of determinants of health, among which are also included genetic, behavioral, social, and environmental factors (IOM, 2000; McGinnis et al., 2002). To modify these, the nation and the intersectoral public health system must identify and exploit the full potential of new options and strategies for health policy and action.
Three realities are central to the development of effective population-based prevention strategies. First, disease risk is currently conceived of as a continuum rather than a dichotomy. There is no clear division between risk for disease and no risk for disease with regard to levels of blood pressure, cholesterol, alcohol consumption, tobacco consumption, physical activity, diet and weight, lead exposure, and other risk factors. In fact, recommended cutoff points for management or treatment of many of these risk factors have changed dramatically and in a downward direction over time (e.g., guidelines for control of “hypertension” and cholesterol), in acknowledgment of the increased risk associated with common moderately elevated levels of a given risk factor. This continuum of risk is also apparent for many social and environmental conditions as well (e.g., socioeconomic status, social isolation, work stress, and environmental exposures). Any population model of prevention should be built on the recognition that there are degrees of risk rather than just two extremes of exposure (i.e., risk and no risk).
The second reality is that most often only a small percentage of any population is at the extremes of high or low risk. The majority of people fall in the middle of the distribution of risk. Rose (1981, 1992) observed that exposure of a large number of people to a small risk can yield a more absolute number of cases of a condition than exposure of a small number of people to a high risk. This relationship argues for the development of
strategies that focus on the modification of risk for the entire population rather than for specific high-risk individuals. Rose (1981) termed the preventive approach the “prevention paradox” because it brings large benefits to the community but offers little to each participating individual. In other words, such strategies would move the entire distribution of risk to lower levels to achieve maximal population gains.
The third reality, provided by Rose’s (1992) population perspective, is that an individual’s risk of illness cannot be considered in isolation from the disease risk for the population to which he or she belongs. Thus, someone in the United States is more likely to die prematurely from a heart attack than someone living in Japan, because the population distribution of high cholesterol in the United States as a whole is higher than the distribution in Japan (i.e., on a graph of the distribution of cholesterol levels in a population, the U.S. mean is shifted to the right of the Japanese mean). Applying the population perspective to a health measure means asking why a population has the existing distribution of a particular risk, in addition to asking why a particular individual got sick (Rose, 1992). This is critical, because the greatest improvements in a population’s health are likely to derive from interventions based on the first question. Because the majority of cases of illness arise within the bulk of the population outside the extremes of risk, prevention strategies must be applicable to a broad base of the population. American society experienced this approach to disease prevention and health promotion in the early twentieth century, when measures were taken to promote sanitation and food and water safety (CDC, 1999b), and in more recent policies on seat belt use, unleaded gasoline, vaccination, and water fluoridation, some of which are discussed later in this chapter.
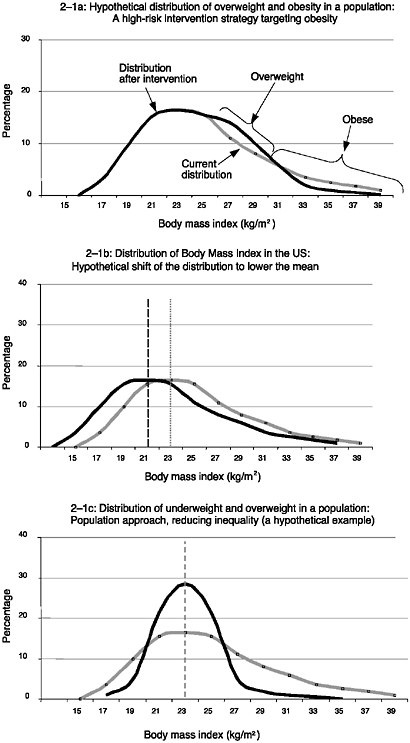
The committee recognizes that achieving the goal of improving population health requires balancing of the strategies aimed at shifting the distribution of risk with other approaches. The committee does, however, endorse a much wider examination, and ultimately the development, of new population-based strategies. Three graphs illustrate different models for risk reduction (see Figure 2–1).
These hypothetical models assume etiological links exist among all exposures and disease outcomes. Figure 2–1a shows the effects of an intervention aimed at reducing the risk of those in the highest-risk category. In this example, people with the highest body mass index (BMI)1 are at in
creased risk for cardiovascular heart disease and a plethora of chronic illnesses. Intervening medically, for example, to decrease risk (by lowering levels of obesity, as measured by BMI) ultimately decreases the proportion of the population with the highest BMIs. Such measures among very high-risk individuals may even be endorsed in cases where the “intervention” itself carries a substantial risk of poor outcome or side effects. However, use of such an intervention would be acceptable only in those whose medical risk was very high. Moreover, interventions in high-risk groups may have a limited effect on population outcomes because the greater proportion of those with moderate risk levels may ultimately translate into more chronic disease or other poor health outcomes.
Figure 2–1b illustrates Rose’s classic model whereby the greatest benefit is achieved by shifting the entire distribution of risk to a lower level of risk. Because most people are in categories of moderately elevated risk as opposed to very high risk, this strategy offers the greatest benefit in terms of population-attributable risk, assuming that the intervention itself carries little or no risk. The hypothetical example shows what might occur if social policies or other population-wide measures were adopted to promote small decreases in weight in the general population. The committee embraces this kind of model of disease prevention in the case of policies such as seat belt regulation and the reduction of lead levels in gasoline.
The final hypothetical model (Figure 2–1c), although not discussed by Rose explicitly, illustrates a reduction in the distributions of those at highest and lowest risk with no change in the distribution of those with a mean level of risk. This model is appropriate for illustrating phenomena relating to inequality, where redistribution of some good (e.g., income, education, housing, or health care) reduces inequality without necessarily changing the mean of the distribution of that good. One hypothetical example is the association between low income and poor health. In many cases, there is a curvilinear association between these goods and health outcomes, with decreased health gains experienced by those at the upper bounds of the distribution. For example, data on income suggest that there are large differences in the health gains achieved per dollar earned for those at the lower end of the income distribution and fewer differences in the health gains achieved per dollar earned for those at the upper end. Thus, the curvilinear association, if it were a causal one, would suggest that substantial gains in population-level health outcomes may be achieved by a redistribution of some resources without actual changes in the means.
These graphs help to illustrate three different strategies for improving the health of the population. The nation has often endorsed the first strategy without a critical examination of the other two, especially the second one. The American public has grown accustomed to seeing differences in exposures to risk, both environmental and behavioral, and disparities in
health outcomes. Acknowledging these gradients fully will help develop true population-based intervention strategies and help the partners who collaborate to assure the public’s health move to take effective actions and make effective policies.
Understanding and ultimately improving a population’s health rest not only on understanding this population perspective but also on understanding the ecology of health and the interconnectedness of the biological, behavioral, physical, and socioenvironmental domains. In some ways, conventional public health models (e.g., the agent–host–environment triad) have long emphasized an ecological understanding of disease prevention. Enormous gains in the control and eradication of infectious diseases rested upon a deep understanding of the ecology of specific agents and the power of environmental interventions rather than individual or behavioral interventions to control disease. For example, in areas where sanitation and water purification are poor, individual behaviors, such as hand washing and boiling of water, are emphasized to reduce the spread of disease. However, when environmental controls become feasible, it is easy to move to a more “upstream”2 intervention (like municipal water purification) to improve health. The last several decades of research have resulted in a deeper understanding not only of the physical dimensions of the environment that are toxic but also of a broad range of related conditions in the social environment that are factors in creating poor health. These social determinants challenge the discipline of public health to more fully incorporate them.
Over the past decade, several models have been developed to illustrate the determinants of health and the ecological nature of health (e.g., see Dahlgren and Whitehead [1991], Evans and Stoddart [1990], and Appendix A). Many of these models have been developed in the United Kingdom, Canada, and Scandinavia, where population approaches have started to shape governmental and public health policies. The committee has built on the Dahlgren-Whitehead model—which also guided the Independent Inquiry into Inequalities in Health in the United Kingdom—modifying it to reflect special issues of relevance in the United States (see Figure 2–2). This figure serves as a useful heuristic to help us think about the multiple determinants of population health. It may, for instance, help to illustrate how the health sector, which includes governmental public health agencies and the health care delivery system, must work with other sectors of government such as education, labor, economic development, and agriculture to
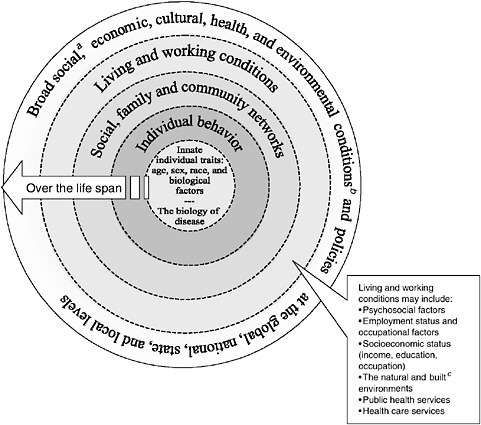
FIGURE 2–2 A guide to thinking about the determinants of population health.
NOTES: Adapted from Dahlgren and Whitehead, 1991. The dotted lines between levels of the model denote interaction effects between and among the various levels of health determinants (Worthman, 1999).
aSocial conditions include, but are not limited to: economic inequality, urbanization, mobility, cultural values, attitudes and policies related to discrimination and intolerance on the basis of race, gender, and other differences.
bOther conditions at the national level might include major sociopolitical shifts, such as recession, war, and governmental collapse.
cThe built environment includes transportation, water and sanitation, housing, and other dimensions of urban planning.
create “healthy” public policy. Furthermore, the governmental sector needs to work in partnership with nongovernmental sectors such as academia, the media, business, community-based organizations and communities themselves to create the intersectoral model of the public health system first alluded to in the 1988 Institute of Medicine (IOM) report and established in this report as critical to effective health action.
Most models of health determinants identify macro-level conditions
and policies (social, economic, cultural, and environmental) as potent forces in shaping midlevel (working conditions, housing) and proximate (behavioral, biological) determinants of health. Macro-level or upstream determinants (such as policies and societal norms) and micro-level determinants (such as sex or the virulence of a disease agent) interact along complex and dynamic pathways to produce health at a population level. As mentioned above, exposures at the environmental level may have a greater influence on population health than individual vulnerabilities, although at an individual level, personal characteristics including genetic predispositions interact with the environment to produce disease. For instance, smoking is a complex biobehavioral activity with both significant genetic heritability and nongenetic, environmental influences, and many studies have shown an interaction between smoking and specific genes in determining the risk of developing cardiovascular disease and cancers. It is also important to note that developmental and historical conditions change over time at both a societal level (e.g., demographic changes) and an individual level (e.g., life course issues) and that disease itself evolves as agents change in virulence.
In the pages that follow, the committee provides a concise discussion of the key determinants that constitute the ecology of health, including environmental and social determinants, and elaborates in more detail on the social influences on health. This decision was made in recognition of a longer history in studying the ways in which environment shapes population health.
THE PHYSICAL ENVIRONMENT AS A DETERMINANT OF HEALTH
At least since the time of Hippocrates’ essay “Air, Water and Places,” written in 400 B.C.E., humans have been aware of the many connections between health and the environment. Improved water, food, and milk sanitation, reduced physical crowding, improved nutrition, and central heating with cleaner fuels were the developments most responsible for the great advances in public health achieved during the twentieth century. These advantages of a developed nation are taken for granted, but in fact, they could deteriorate without adequate support of the governmental public health infrastructure.
Environmental health problems, historically local in their effects and short in duration, have changed dramatically within the last 25 years. Today’s problems are also persistent and global. Together, global warming, population growth, habitat destruction, loss of green space, and resource depletion have produced a widely acknowledged environmental crisis (NRC, 1999). These long-term environmental problems are not amenable to quick technical fixes, and their resolution will require community and
societal engagement. At the local and community levels, environmental issues are equally complex and are also related to a range of socioeconomic factors. A brief look at some of the evidence on environmental determinants of health may help shed some light on why health is not equally shared.
The importance of “place” to health status became increasingly clear in the last decades of the twentieth century. The places in which people work and live have an enormous impact on their health. The characteristics of place include the social and economic environments, as well as the natural environment (e.g., air, water) and the built environment, which may include transportation, buildings, green spaces, roads, and other infrastructure (IOM, 2001b). Environmental hazards in workplaces and communities may range from tobacco smoke to pesticides to toxic housing. Rural areas may present increased health risks from pesticides and other environmental exposures, whereas some environmental threats to health can occur because of urban living conditions.
More than three-quarters of Americans live in urban areas (Bureau of the Census, 1993). Although rural Americans experience certain health-related disadvantages (e.g., health care access issues due to transportation and availability) (Slifkin et al., 2000; NCHS, 2001), some of the health effects of the inner city (i.e., decay and crime) are often dramatic and may be related to broader social issues. The “urban health penalty”—the “greater prevalence of a large number of health problems and risk factors in cities than in suburbs and rural areas” (Leviton et al., 2000:863)—has been frequently discussed and studied (Lawrence, 1999; Freudenberg, 2000; Geronimus, 2000). A variety of political, socioeconomic, and environmental factors shape the health status of cities and their residents by influencing “health behaviors such as exercise, diet, sexual behavior, alcohol and substance use” (Freudenberg, 2000:837). The negative environmental aspects of urban living—toxic buildings, proximity to industrial parks, and a lack of parks or green spaces, among others—likely affect those who are already at an economic and social disadvantage because of the concentration of such negative aspects in specific pockets of poverty and deprivation (Lawrence, 1999; Maantay, 2001; Williams and Collins, 2001). Urban dwellers may experience higher levels of air pollution, which is associated with higher levels of cardiovascular and respiratory disease (Hoek et al., 2001; Ibald-Mulli et al., 2001; Peters et al., 2001). People who live in aging buildings and in crowded and unsanitary conditions may also experience increased levels of lead in their blood, as well as asthma and allergies (Pertowski, 1994; Pew Environmental Health Commission, 2000; CDC, 2001a). These examples illustrate some of the profound effects of the physical environment on health. The places where people live may expose them to harmful factors.
Methylmercury: A Case Study
The case of methylmercury as an environmental pollutant illustrates the potentially dramatic effects of the physical environment on health. Environmental toxins are a specific form of environmental hazard, caused in most cases by industrial enterprises, and the adverse effects of such toxins on the nervous system have been well documented. High levels of exposure to certain environmental pollutants are known to cause acute effects including convulsions, paralysis, coma, and death. The effects of lead on health and development have been documented for decades, and policy action regarding leaded gasoline and lead-based paints has been taken, with positive effects on child health. However, there is growing concern about emerging evidence that other ubiquitous pollutants such as polychlorinated biphenyls (PCBs) and mercury may cause behavioral problems and affect mood and social adjustment. The adverse impacts of exposure to these pollutants may be most profound during fetal development and early childhood. Amidst growing national concern about developmental disabilities, exposure to mercury in the environment represents an emerging and preventable environmental health threat.
The National Research Council (NRC) report Toxicological Effects of Methylmercury (NRC, 2000) examined the evidence of adverse health impacts resulting from exposure to mercury, focusing on consumption of seafood contaminated by releases to the environment. Fossil fuel combustion represents the major source of mercury released to the environment. The deposition of mercury on the land and in surface waters results in conversion to forms that accumulate in the food chain. This bioaccumulation can result in very high concentrations of mercury in some fish, which are the main source of exposure for the population. The developing brain is particularly sensitive to the adverse effects of mercury exposure. Prenatal exposures may interfere with the growth and development of neurons and cause irreversible damage to the nervous system. Infants whose mothers were exposed to high levels in poisoning episodes in Minamata, Japan, and in Iraq were born with severe disabilities, including mental retardation, cerebral palsy, blindness, and deafness (EPA, 1997; NRC, 2000). More recently, epidemiological studies of lower-level exposure from maternal fish consumption have raised concerns about subtle neurodevelopmental deficits.
The NRC report concluded that the evidence of developmental neurotoxic effects from mercury exposure is strong and called for revision of the Environmental Protection Agency (EPA) reference dose that provides public health guidance on acceptable population exposure levels. This conclusion was based on epidemiological studies of low-level chronic exposure from seafood consumption. The population at risk consists of women of childbearing age and their children. Frequent consumers, par-
ticularly of fish that tend to accumulate high levels of mercury, may be exposing their unborn children to levels of mercury in the range that has been shown to be associated with developmental deficits. Based upon the available data on fish consumption, the NRC committee estimated that as many as 60,000 newborns may be at risk for adverse neurodevelopmental effects from in utero exposure to mercury. Recently, the Centers for Disease Control and Prevention (CDC) released the first National Exposure Report, which provided dramatic confirmation of the emerging threat of mercury. Ten percent of a national sample of women of childbearing age had mercury levels in their blood within 1/10 of potentially hazardous levels, indicating a narrow margin of safety for many women (CDC, 2001c).
Currently, 40 states have issued fish consumption advisories to reduce exposure to mercury. EPA and the Food and Drug Administration (FDA) have also recently revised their guidance concerning consumption of fish species that have been shown to have high levels of mercury. Ultimately, the threat of mercury can be most effectively reduced through control of the sources of pollution. However, control of sources from the burning of fossil fuels may be decades away. In the meantime, prevention of adverse public health impacts from mercury will require a partnership among health care providers, public health agencies, and others.
The example of methylmercury clearly illustrates the serious impact of just one environmental risk factor. The influences of many other environmental risk factors on health have not been fully documented, and evidence of the influence of environmental factors for some health conditions like asthma is rapidly accumulating (Trust for America’s Health, 2001). The association between certain chronic diseases and environmental causes is devastatingly clear, yet knowledge about the scope of environmental health risks and their impact on the public’s health is limited. Most states do not track environmental risk factors like pesticides and other hazards or most chronic diseases (such as asthma) and birth defects (Pew Environmental Health Commission, 2001). Certainly, a significant amount of work remains to be done to address the physical environment’s powerful influence on health status. A great deal about health determinants in the built and natural environments has been learned in recent decades, but much more is yet to be examined.
THE SOCIAL DETERMINANTS OF HEALTH
Most recently, social epidemiologists and other researchers have focused on identifying the social equivalents of leaded gasoline and environmental tobacco smoke. Among the greatest advances in understanding the factors that shape population health over the last two decades, and clearly
since the last Institute of Medicine (IOM, 1988) report on the health of the public, has been the identification of social and behavioral conditions that influence morbidity, mortality, and functioning.
The evidence amassed strongly and consistently points to the importance of these conditions as significant determinants of population health. Because they also feature prominently in the committee’s determinants-of-health model, the evidence related to four conditions whose importance is robustly supported is reviewed here: (1) socioeconomic position, (2) race and ethnicity, (3) social networks and social support, and (4) work conditions. Additionally, we discuss the evidence related to a fifth condition that has been and that still is the subject of great interest as well as controversy: ecological-level influences, namely, economic inequality and social capital.3 The present analysis reviews key evidence related to these five conditions that has been presented more extensively in Health and Behavior (IOM, 2001).
Socioeconomic Status and Health
A strong and consistent finding of epidemiological research is that there are health differences among socioeconomic groups. Lower mortality, morbidity, and disability rates among socioeconomically advantaged people have been observed for hundreds of years; and in recent decades, these observations have been replicated using various indicators of socioeconomic status (SES) and multiple disease outcomes (Syme and Berkman, 1976; Kaplan and Keil, 1993). SES is defined in terms of education, income, and occupation. Furthermore, educational differentials in mortality have increased in the United States over the past three decades, leading to a growing inequality, even though mortality rates have dropped for all groups (Feldman et al., 1989; Pappas et al., 1993; Tyroler et al., 1993).
Although it may be measured as level of education or income, SES is a complex phenomenon often based on indicators of relationships to work (occupational position or ranking), social class or status, and access to power. From a policy perspective as well as an etiological perspective, it is important to understand which of the components is critical—for instance, if education is found to be important, the policies that may be implemented would differ from the policies needed if income was found to be the most influential factor. In fact, most research has not tested such competing hypotheses directly, so in the examples that follow, these have not been disaggregated, although the indicators used in each study are explicitly identified.
Several major studies have ascertained that education, income, and occupation, as indicators of SES, are associated with mortality and with mortality due to certain causes. The National Longitudinal Mortality Study found that mortality was strongly associated with all three measures of SES (Rogot et al., 1992; Sorlie et al., 1992, 1995) (see Box 2–1).
The Multiple Risk Factor Intervention Trial followed 320,909 white and African-American men for 16 years (Davey Smith et al., 1996a, 1996b) and found that the median family income in one’s zip code of residence was predictive of death from a variety of causes. Heart disease, the leading cause of death in the United States, provides a strong example of the association between SES and mortality. Research has documented the relationship between SES and cardiovascular disease (NCHS, 1992; Kaplan and Keil, 1993), and the British Whitehall longitudinal study of civil servants found that those in the lowest grades of employment were at the highest risk for heart disease (Marmot et al., 1991).
A striking finding that emerges from analyses of occupation- and area-based income measures is the graded and continuous nature of the association between socioeconomic position and mortality, with differences persisting well into the middle socioeconomic ranges (Davey Smith et al., 1990; Blane et al., 1997; Macintyre et al., 1998). For example, in the Whitehall studies (Davey Smith et al., 1990; Marmot et al., 1991), the
|
BOX 2–1 Linking SES to Health: Findings from the National Longitudinal Mortality Study
SOURCES: Rogot et al. (1992) and Sorlie et al. (1992, 1995). |
individuals in each employment grade had worse health and a higher rate of mortality than those in the grade above.
Although many of the studies that focused on occupation-, education-, or area-level SES showed a gradient that is virtually linear, studies that focus on income often show somewhat different results. For example, in work by Backlund and colleagues (1996), the association between (increasing) income and (decreasing) mortality is clearly curvilinear, with the decline in the mortality rate with increasing income greatest among those in groups earning less than $25,000 per year but with the decline with increasing income being much less among those earning between $25,000 and $60,000 per year. This curvilinear relationship suggests diminishing returns of income as one approaches the highest income categories, although some association may persist. This curvilinear association between income and health is what lays the framework for findings that more egalitarian societies (i.e., those with a less steep differential between the richest and the poorest) have better average health, because a dollar at the bottom “buys” more health than a dollar at the top. Whether SES has a linear or curvilinear relationship with health has enormous implications for understanding both the etiologic associations and the policy implications of this research. In either case, however, it is important to note that a “threshold” model focused exclusively on the very poorest segments and ignoring others near the bottom and the working poor will not address the relatively poor population health outcomes for the U.S. population as a whole. The major reason for this is because there are groups in the moderate-risk categories of working poor and working class who contribute disproportionately large numbers to death rates and poor health outcomes.
SES is linked to health status through multiple pathways (such as distribution of health care, psychosocial condition, toxic physical environments, and health-related behaviors), but these relationships have not yet been fully elucidated. It is also likely that some degree of reverse causation influences the strength of these associations. Studies in which education rather than income or occupation is used as an indicator of SES are stronger in this regard since most people are not influenced by serious chronic diseases related to cardiovascular disease, stroke, or cancer in ways that inhibit their level of educational attainment in their adolescence and early twenties. Furthermore, although many studies have included a broad range of covariates in their multivariable analyses, it is of course possible that unobserved attributes account for some observed disparities. There is ample evidence that SES is strongly related to access to and the quality of preventive care, ambulatory care, and high-technology procedures (Kaplan and Keil, 1993); but health care appears to account for a small percentage of the variation in health status among different SES groups. It has been argued that differential access to health care programs and services is not entirely
responsible for socioeconomic differentials in health (Wilkinson, 1996), because causes of death that apparently are not amenable to medical care show socioeconomic gradients similar to those for potentially treatable causes (Mackenbach et al., 1989; Davey Smith et al., 1996a). Furthermore, similar gradients persist in countries with universal coverage, such as the United Kingdom.
Despite the past century’s great advances in sanitation, which have contributed to the sharp increase in life expectancy observed among all socioeconomic groups, the socioeconomic gradient in health status persists. It has been proposed, and to some extent documented, that the gap in health status by SES may still be attributable to the effects of crowded and unsanitary housing, air and water pollution, environmental toxins, an inadequate food supply, poor working conditions, and other such deficits that have historically affected and that still disproportionately affect those in the lower socioeconomic strata (USPHS, 1979; Williams, 1990; Adler et al., 1994; Sargent et al., 1995; McLoyd, 1998). Studies that incorporate assessments of material deprivation and aspects of the physical environment will be important to explicate these important potential pathways.
Considerable evidence links low SES to adverse psychosocial conditions. People in lower socioeconomic positions are not only more materially disadvantaged, but also have higher levels of job and financial insecurity; experience more unemployment, work injuries, lack of control, and other social and environmental stressors; report fewer social supports; and more frequently, have a cynically hostile or fatalistic outlook (Berkman and Syme, 1979; Karasek and Theorell, 1990; Adler et al., 1994; Heaney et al., 1994; Bosma et al., 1997).
There is most often, especially in the United States, a striking and consistent association between SES and risk-related health behaviors such as cigarette smoking, physical inactivity, a less nutritious diet, and heavy alcohol consumption. This patterned behavioral response has led Link and Phelan (1995) to speak of situations that place people “at risk of risks.” Understanding why “poor people behave poorly” (Lynch et al., 1997) requires recognition that specific behaviors formerly attributed exclusively to individual choice have been found to be influenced by the social context. The social environment influences behavior by shaping norms: enforcing patterns of social control (which can be health promoting or health damaging); providing or denying opportunities to engage in particular behaviors; and reducing or producing stress, for which engaging in specific behaviors (such as smoking) might be an effective short-term coping strategy (Berkman and Kawachi, 2000). Both physical and social environments place constraints on individual choice. Over time, those with more economic and social resources have tended to adopt health-promoting behaviors and reduce risky behaviors at a faster rate than those with fewer economic resources.
Socioeconomic disparities in health in the United States are large, are persistent, and appear to be increasing over recent decades, despite the general improvements in many health outcomes. The most advantaged American men and women experience levels of longevity that are the highest in the world. However, less advantaged groups experience levels of health comparable to those of average men and women in developing nations of Africa and Asia or to Americans about half a century ago (Berkman and Lochner, 2002). Furthermore, these wide disparities coupled with the large numbers of people in these least-advantaged groups contribute to the low overall health ranking of the United States among developed, industrialized nations. A major opportunity for us to improve the health of the U.S. population rests on our capacity to either reduce the numbers of the most disadvantaged men, women, and children in the highest risk categories or to reduce their risks for poor health.
Racial and Ethnic Disparities in Health
A substantial body of research documents the relationship between racial and ethnic disparities and differences in health status. Numerous studies have shown that minority populations may experience burdens of disease and health risk at disproportionate rates because of complex and poorly understood interactions among socioeconomic, psychosocial, behavioral, and health care-related factors (NCHS, 1998; DHHS, 2000; IOM, 2002). Although Americans in general experienced substantial improvements in life expectancy at all ages throughout the twentieth century, substantial gaps in life expectancy, morbidity, and functional status remain between white and minority populations. Life expectancy at birth for African Americans in 1990 was the same as that for whites in 1950. Even after controlling for income, African-American men and women have lower life expectancies than white men and women at every income level (for example, see Geronimus et al. [1996] and Anderson et al. [1997]). When indicators of SES are considered, these differences, which are often substantial across a diversity of health outcomes, are commonly reduced but remain significant. Few studies have adequately controlled for SES in terms of the inclusion of economic indicators of wealth, homeownership, or other sources of income. Although these indicators should be included, they are unlikely to reduce disparities between African Americans and whites because data suggest that there are even greater disparities in wealth (all assets) than in household income between these two groups (Ostrove et al., 1999). This phenomenon has led researchers to investigate the health effects of discrimination itself. Aspects of discrimination might influence health through any number of mechanisms, including SES. However, conceptualizing discrimination (whether it applies to racial or ethnic minori
ties, women, homosexuals, or groups of different ages) as a stressful experience that can influence disease processes through a number of potential pathways is a major advance in scientific thinking over the past decade (Krieger and Sidney, 1996). Additionally, although many disparities are measured across broad racial and ethnic classifications, there is significant health status differentiation or “hidden heterogeneity” within, for instance, Asian-American and Pacific Islander populations (NCHS, 1998). The acknowledgment of disparities itself may generalize or aggregate groups that are highly heterogeneous because of variations ranging from the date of immigration and level of acculturation to genetic, social, and cultural differences (Williams and Collins, 1995; Korenbrot and Moss, 2000).
African Americans and other minority populations experience worse health from infancy to old age. Although the national infant mortality rate has decreased over the years to about 7 per 1,000, the rate among African-American infants is nearly twice as high, 14 per 1,000, and that among American Indians is 9.3 per 1,000, whereas it is 5.8 per 1,000 among whites (NCHS, 2002).
Rates of illness such as asthma are much higher among African Americans than among whites, as are levels of obesity, diabetes, and other cardiovascular risk factors that are often established in adolescence and young adulthood. For example, the prevalence of obesity among African Americans is 29.3 percent and that among Hispanics is 21.5 percent, whereas it is 18.5 percent among whites (CDC, 2002). In 2000, the rate of diabetes-related mortality in non-Hispanic African Americans was 49.4 (per 100,000), whereas it was 32.4 in Hispanics and 20.8 in non-Hispanic whites (CDC, 2001b). Rates of death due to HIV/AIDS are 31.9 among African Americans and 3.7 among whites (CDC, 2000).
Some of the racial and ethnic differences in health status may be associated with the fact that minority populations often encounter the health care system in very different ways in terms of both access and quality of care (Fiscella et al., 2000). For a variety of reasons—both structural (having to do with the health care system itself) and financial or cultural—racial and ethnic minorities encounter barriers to health care that often result in less than optimal care and worse outcomes (Carlisle et al., 1997; Epstein and Ayanian, 2001; IOM, 2002). For example, many studies have concluded that African-American patients are significantly less likely than white patients to receive certain revascularization procedures to treat coronary artery disease (Epstein and Ayanian, 2001). Barriers to care may include linguistic differences, a lack of insurance or difficulties with payment, immigration status, social issues such as trust and some pervasive but subtle forms of racism and discrimination, and even logistical problems related to distance and transportation (Thomas, 2001; IOM, 2002). African-American and Hispanic children are more likely to
be uninsured than white children and are less likely to have a usual source of health care (Weinick and Krauss, 2000). Recent research indicates that disparities in access persist even after controlling for socioeconomic circumstances and health insurance coverage status (Roetzheim et al., 1999; Weinick and Krauss, 2000). Among other disparities in health care, African Americans have been shown to be less likely to receive certain diagnostic testing; adequate pain medication; early-stage diagnoses of cancer; dialysis as initial treatment for end-stage renal disease, placement on a kidney transplant waiting list, or a kidney transplant; and preventive rather than acute asthma control measures (IOM, 2002). Hispanics are also likely to experience similarly unequal access to health care services (IOM, 2002). With regard to treatment for HIV infection, once tested, HIV-infected African Americans are less likely to receive antiretroviral and related therapies (IOM, 2002). This is in the context of the fact that HIV infection is spreading more rapidly among African Americans and Hispanics than among whites.
Although many studies indicate that certain racial differences in health persist among people of similar SES, it is also true that many minority groups are likely to be poorer and more disadvantaged than whites. This overlap along both racial and economic lines creates a kind of “double jeopardy,” which is associated with substantially increasing risks for poor health. In terms of the association between poverty and minority status, in 1998, for instance, 10 percent of non-Hispanic white children lived in poverty, whereas 36.4 percent of African-American children and 33.6 percent of Hispanic children lived in poverty (CDC, 2000). When health outcomes are examined by level of education of the mother, family income, and ethnicity and race, enormous differences emerge between the least-advantaged African-American children and the most advantaged white children. For instance, among African-American children living below the poverty line, 22 percent have elevated blood lead levels, whereas 6 percent of African-American children in high-income families and slightly more than 2 percent of white children in high-income families have elevated blood lead levels. These patterns are persistent and are seen for other outcomes such as low birth weight and hospitalizations for asthma (NCHS, 1998). Such pronounced disparities have led to a presidential initiative targeted at ethnic and racial health disparities in six specific areas (White House, 1998; Office of Minority Health, 2000). Also, the elimination of health disparities is a goal of Healthy People 2010 (DHHS, 2000).
Social Connectedness and Health
The association between social connectedness and health has received much attention in recent years. Concepts of social connectedness relate to
social integration at the broadest level, social networks, social support, and loneliness. Social connectedness may be conceptualized as a societal characteristic related to civic trust and social capital. This area-level experience is discussed in a later section. This section reviews the evidence that the structure of social ties is related to health outcomes and discusses pathways that may link such social experiences to health. People form ties to others the moment they are born. The survival of newborns depends upon their attachment to and nurturance by others over an extended period of time (Baumeister and Leary, 1995). The need to belong does not stop in infancy, but rather, affiliation and nurturing social relationships are essential for physical and psychological well-being throughout life.
Over the past 20 years, 13 large prospective cohort studies in the United States, Scandinavia, and Japan have shown that people who are isolated or disconnected from others are at increased risk of dying prematurely from various causes, including heart disease, cerebrovascular disease, cancer, and respiratory and gastrointestinal conditions (Berkman and Syme, 1979; Blazer, 1982; House et al., 1982, 1988; Welin et al., 1985; Schoenbach et al., 1986; Orth-Gomer and Johnson, 1987; Cohen, 1988; Kaplan et al., 1988; Seeman et al., 1988, 1993; Sugisawa et al., 1994; Seeman, 1996; Pennix et al., 1997). Studies of large cohorts of people enrolled in health maintenance organizations or occupational cohorts also report that social integration is critical to survival, although it may not be as critical an influence on the onset of disease (Vogt et al., 1992; Kawachi et al., 1996).
Powerful epidemiological evidence supports the notion that social support, especially intimate ties and the emotional support provided by them, is associated with increased survival and a better prognosis among people with serious cardiovascular disease (Orth-Gomer et al., 1988; Berkman et al., 1992; Case et al., 1992; Williams et al., 1992) and strokes (Friedland and McColl, 1987; Colantonio et al., 1992, 1993; Glass et al., 1993; Morris et al., 1993). The lack of social support, expressed in terms of conflict or loss of intimate ties, is also associated with health outcomes and risk factors such as neuroendocrine changes in women (Kiecolt-Glaser et al., 1997), high blood pressure (Ewart et al., 1991), elevated plasma catecholamine concentrations (Malarkey et al., 1994), and autonomic activation (Levenson et al., 1993). Caregivers of relatives with progressive dementia are characterized by impaired wound healing (Kiecolt-Glaser et al., 1995, 1998). Social conflicts have been shown to increase susceptibility to infection (Cohen et al., 1998).
Several studies have recently shown that older men and women with high levels of social engagement and networks have slower rates of cognitive decline (Bassuk et al., 1999; Fratiglioni et al., 2000) and better survival independent of physical activity (Glass et al., 2000). The pathways by which social networks might influence health are multiple and include
pathways related to health behaviors, health care, access to material resources such as jobs, and direct physiological responses leading to disease development and prognosis. For instance, evidence suggests that, in general, social network size or connectedness is inversely related to risk-related behaviors. People who are socially isolated are more likely to engage in such behaviors as tobacco and alcohol consumption, to be physically inactive, and to be overweight (Berkman and Glass, 2000). Behavioral pathways such as these do not appear to account for a large part of the association between social isolation and poor health, but they are important to consider. It is important to note that networks themselves have generally been shown to exert powerful influences on the behavior of both adolescents and adults, so that networks can either promote health or increase risk depending on the norms of the networks themselves.
Experimental work with animals and humans indicates that social isolation can have a direct effect on physiologic function and subsequent diseases. Animals that are isolated in adulthood, that experience maternal separation, or that are not nurtured in infancy develop more atherosclerosis; have poor, inefficient, or exaggerated neuroendocrine responses; and may have higher levels of immunosuppression (Nerem, 1980; Shively et al., 1989; Suomi, 1991; Meaney et al., 1996). Among humans and primates, those who lack affiliation and strong social networks have been shown to be more likely to develop colds, have stronger stress responses in terms of neuroendocrine reactions and higher levels of cardiovascular reactivity, and have altered immune responses (Glaser et al., 1992, 1999; Kirschbaum et al., 1995; Cohen et al., 1997; Sapolsky et al., 1997; Roy et al., 1998; Cacioppo et al., 2000). There is limited research on whether access to material goods and resources is a mechanism through which social networks might influence health, and this is an important area for investigation. We do know, however, that networks have the capacity to provide informational and instrumental support effectively. Although much of the research in this area examines the effects of close relationships and social support, there is also evidence that weak social ties may also have indirect positive effects on health and well-being. For instance, a classic investigation of how people find jobs suggests that weak ties to others may be more helpful in enabling people to find jobs, providing access to one of the most critical life opportunities. Whereas one’s close friends and relatives (who are likely to belong to the same social circles) may often provide redundant information, weak social ties (e.g., a friend of a friend) may allow individuals to tap into new sets of information (Granovetter, 1995). Instrumental and informational support, two critical components of the support paradigm, relate to help with practical matters such as grocery shopping; rides to the doctor; and information about health care, behavior, and risk. Finally, many of the observational data linking social connectedness to health
outcomes do not permit us to rule out issues of reverse causation or the possibility that some unobserved condition explains these associations. More experimental work is needed to answer these questions completely. Much of the experimental work cited here supports the concept that social isolation increases the risk for poor health. However, a recent clinical trial, Enhancing Recovery in Coronary Heart Disease, aimed at improving social support to reduce mortality and reinfarction among subjects after myocardial infarction, found no effect (NIH, 2001). Developing both clinical and population-based experimental studies is the next step in this work.
A large body of evidence accumulated over the last two decades consistently points to the importance of social connectedness, and incorporation of this evidence would involve the inclusion of nurturing community and social networks. As we think of broad social determinants of health that could be influenced to improve health, social connections may be one example that has the support of a number of sectors. Because social relationships influence health through such a myriad of pathways, broad health improvements may be facilitated by considering and enacting policies that support social connections.
Work-Related Conditions and Health
Two decades of research show that the workplace not only generates adverse health effects due to economic circumstances such as downsizing and unemployment or to work conditions such as job demands, control, latitude, and threatened job loss (Karasek and Theorell, 1990), but also generates protective health effects such as social ties that may help counteract the physical and mental adverse effects of work stressors (Buunk and Verhoeven, 1991). The “demand–control” model was developed to describe the psychosocial work environment (Karasek and Theorell, 1990), and other empirical studies have tested the predictive validity of the model with respect to physical health, for instance, by examining the effects of reward relative to effort (Sigerist, 1996).
It has been hypothesized that job strain (the combination of a psychologically demanding workplace and a low level of job control) leads to adverse health outcomes, and findings show that job control is an important component of health-promoting work environments (Johnson et al., 1996; North et al., 1996; Bosma et al., 1997, 1998; Theorell et al., 1998). Schnall and colleagues (1994) found that lower levels of job control (the opportunity to use and develop skills and to exert authority over workplace decisions) were predictive of adverse cardiovascular disease outcomes in 17 of 25 studies, whereas high psychological demands of work had similarly negative effects in only 8 of 23 studies.
The links between unemployment and health have been investigated by
European researchers and, to a somewhat more limited extent, U.S. researchers. Although longitudinal studies of European populations have demonstrated a significant relationship between unemployment and higher standardized mortality ratios (SMRs), even after adjusting for age and social status (Moser et al., 1984, 1986, 1987; Costa and Segnan, 1987; Iversen et al., 1987; Martikainen, 1990; Kasl and Jones, 2000; Stefansson, 1991), U.S. data based on the U.S. National Longitudinal Mortality Study (Sorlie and Rogot, 1990) have shown no significant association between age, education, and income-adjusted SMRs and unemployment for either men or women. However, other U.S. epidemiological findings associate unemployment or risk of job loss with health conditions such as depression and engagement in negative health behaviors such as substance abuse, poor diet, and inactivity (Dooley et al., 1996). Analysis of panel data from the U.S. Epidemiologic Catchment Area study suggested that the 1-year incidence of clinically significant alcohol abuse was greater among those who had been laid off than among those who had not (Catalano et al., 1993). Examination of cases of job loss due to factory closures is important because worker characteristics in such cases have no effect on the loss of jobs. Morris and Cook (1991) reviewed longitudinal studies of factory closures and found that the job loss experience exerts a negative effect on physical health.
The impact of threatened job loss has received increased attention recently. European studies found negative effects on health because of threatened job loss or organizational change, although there were no significant differential trends in weight, blood pressure, or blood glucose over time.
The Whitehall II cohort of British civil servants (Ferrie et al., 1995, 1998) found that white-collar workers under threat of major organizational change (elimination or transfer to the private sector) may experience adverse changes in self-rated health, long-standing illness, sleep patterns, and number of physical symptoms and may experience minor psychiatric morbidity. Longitudinal data on male Swedish shipyard workers threatened with job loss and on stably employed controls (Mattiasson et al., 1990) showed that serum cholesterol concentrations increased significantly among the former group. In a study of Finnish government workers (Vahtera et al., 1997), downsizing was associated with increased medically certified sick leave. Among American automobile workers (Heaney et al., 1994), extended periods of job insecurity were associated with increased physical symptoms. However, workers who remain in an organization after a downsizing do not experience a decline in well-being, despite an increase in work demands (Parker et al., 1997). Contrary to work conditions related to involuntary job loss, retirement does not appear to have negative health consequences (Moen, 1996; Kasl and Jones, 2000).
Ecological-Level Influences: The Importance of Place in Population Health
Social characteristics of individuals are closely related to health. Among the most important findings to emerge from public health research over recent years is the extent to which characteristics of areas exert independent effects on health. This ecological4 approach has been rediscovered and is now embedded in a multilevel framework. The major idea is that characteristics of places—neighborhoods, schools, work sites, and even nations— carry with them health risks for the individuals who live in those environments. The health risk conferred by these places is above and beyond the risk that individuals carry with them. Thus, we might view characteristics of physical environments (e.g., parks and buildings) as well as social environments (e.g., levels of inequality and civic trust) as truly properties of places, not individuals. In this section, the committee reviews evidence related to two aspects of places—economic inequality and social capital— that are assessed at an ecological level to examine their effects on health. These findings are relatively new and undoubtedly will be refined with further research. Economic inequality may exert an effect on health in addition to the effect of individual income on health. Such an effect may be particularly robust for people in the United States who are at the lower ends of the distribution.
The United States is among the richest countries in the world, yet it is also one of the most (and increasingly) unequal in terms of the distribution of its wealth as measured by a wide and growing gap between the best-off and the worst-off quintiles (Weinberg, 1996; Jencks, 2002) (see Box 2–2). At a national level, the hypothesis linking income inequalities and health would predict that two countries with the same average income but different income distributions would experience different patterns of mortality, with the country with the more even distribution having a longer life expectancy overall. Cross-national studies initially supported an association between income equality and population longevity, but more recent research, which includes newer and more accurate data for more countries, suggests that the area-level effects of inequality across nations may not hold over time (Lynch et al., 2001; Gravelle et al., 2002; Rodgers, 2002). Recent studies have shown the cross-national correlation between economic inequality and mortality to be very weak or virtually nonexistent (Kunst et al., 1998). Furthermore, in several countries (Canada, for example), inequalities at the level of provinces or neighborhoods within cities often have been found to be not significant in terms of health status. In the United
|
BOX 2–2 Income Inequality in the United States
|
States, however, data are more consistent in supporting the area-level effect of inequality net of individual effect. For example, Kaplan and colleagues (1996) and Kennedy and colleagues (1996) independently found that the degree of household income inequality in the 50 states was associated with the state-level variation in total mortality, as well as with the state-level variations in infant mortality and rates of death from coronary heart disease, cancer, and homicide. The findings persisted after controlling for urban–rural proportion and for health behavior variables such as cigarette smoking rates.
Lynch and colleagues (1998) observed a relationship between income inequality and mortality at the level of U.S. metropolitan areas. Although income inequality is strongly correlated with poverty (R = 0.73), the adverse effect of income inequality on health outcomes does not appear to be explained entirely by the fact that places that exhibit income inequality have greater concentrations of poor people, who in turn have a higher risk of mortality (compositional effects). There is also evidence of a contextual effect of income inequality directly on individual health (Wilkinson, 1992; Kennedy et al., 1998; Soobader and LeClere, 1999). Kennedy and colleagues (1998) reported that people residing in states with the greatest income inequality were 1.25 times more likely to report being in fair or poor health than were those living in the most egalitarian states. The effect of income inequality was statistically significant and independent of absolute income levels.
These findings pose the challenge of explaining why the effects of inequality are more significant and conclusive in the United States than in other developed nations. Some (Kawachi and Kennedy, 1997) have argued that inequality is associated with a lack of investment in education, devel-
opment, and social services and is also related to weak civic and social bonds—or a lack of trust—between people (Wilkinson, 1996; Kawachi et al., 1997; Kawachi and Berkman, 2000). Some countries buffer the effects of inequality with stronger social service programs. Investigators have argued that U.S. analyses have not adequately considered other state-level or country-level social and demographic factors (e.g., racial composition) that may not be “downstream” in the causal chain linking inequality to health (Deaton and Lubotsky, 2001). These questions remain challenges to a new field. However, it is important to note that these studies are all examining the contextual or area-level effects of inequality, net of individual or “compositional” effects. No one has disputed the strong and consistent effects of SES on individual health. New research on area-level efforts related to neighborhoods, work sites, and states and even across countries poses considerable methodological challenges (Deaton, 2002). Nonetheless, such research holds great potential to help us understand the ways in which both the social and the physical (built and natural) environments may affect health and behavior.
Social participation and integration can also be conceived of as both individual and societal characteristics (Kawachi and Kennedy, 1997). Some investigators have started to conceptualize these dimensions at an ecological or group level. At the group level, a socially cohesive society, or one in which most citizens are socially integrated, is one that is endowed with stocks of “social capital,” which consists partly of moral resources such as trust between citizens and norms of reciprocity. This has led investigators to examine the area-level effects of these domains. Particular interest has been focused on the relationship between social capital and health. At a group level, more socially integrated societies seem to have lower rates of crime, suicide, and mortality from all causes and a better overall quality of life (Wilkinson, 1996; Kawachi and Kennedy, 1997; Kawachi and Berkman, 2000).
Kawachi and colleagues (1997) analyzed social capital indicators across the United States in relation to state-level death rates. The per capita density of membership in voluntary groups was inversely correlated with age-adjusted mortality from all causes. Density of civic association, group membership, and levels of interpersonal trust (i.e., percentage of citizens endorsing the expectation that altruistic behaviors will be returned in kind at some future time) were also associated with lower mortality. Kawachi and colleagues (1999) also carried out a multilevel study of the relationship between the above indicators of state-level social capital and individual self-rated health. A strength of this study was the availability of information on individual medical and behavioral confounding variables, including health insurance coverage, cigarette smoking, and being overweight, and on sociodemographic characteristics, such as household in
come, education, and whether one lived alone. Even after adjustment for these variables, people residing in states with low levels of social capital were more likely to report fair or poor health. The odds ratio for fair or poor health in association with living in areas with the lowest levels of interpersonal trust as opposed to the highest levels of interpersonal trust was 1.41.
There are several plausible mechanisms by which social cohesion might influence health through contextual effects. At the neighborhood level, social capital might influence health behaviors by promoting the more rapid diffusion of health information. Sampson and colleagues (1997) provide evidence that ”collective efficacy,” or the extent to which neighbors are willing to exert social control over deviant behavior, plays an important role in preventing crime and delinquency. Neighborhood social capital also could affect health by increasing access to local services and amenities (Sampson et al., 1997). Finally, neighborhood social capital could influence health through direct psychosocial pathways by providing social support and acting as the source of self-esteem and mutual respect.
Although there has been a great deal of interest in these area-level studies of social capital, there has also been a fair amount of skepticism regarding their validity. Several social scientists (Portes and Landolt, 1996; Sandefur and Laumann, 1998; Durlauf, 1999) have voiced concerns about the ambiguity of the concept, the potential for social capital to lead to undesirable outcomes related to the exclusion of certain groups, and insufficient attention to the determinants of social capital itself or the causal patterning between it and other social conditions. Future studies will be strengthened with the addition of items tapping the conceptual richness of the domain of social capital and the capacity to distinguish it from other closely related constructs of social networks and SES.
POPULATION-LEVEL PREVENTIVE INTERVENTIONS
The evidence presented and discussed in this chapter aims to demonstrate that taking into account the environmental and social determinants of health is essential to creating effective population-level interventions for health improvement. Health risk is related to a complex of social, economic, and political factors that both surpass and powerfully interact with “downstream” elements such as individual behaviors, biological traits, and access to health care services. There have been few empirical tests of population-based approaches to health promotion that focused on risk-related social conditions, but in an effort to understand how such approaches might work, several examples are presented to illustrate the effectiveness and efficiency (e.g., cost) of population-based interventions to prevent disease and promote health.
Preventive interventions at the population level may be classified as universal, selective, and indicated, borrowing the classification developed by Gordon (IOM, 1994b). A universal measure is one that would be desirable for everyone in an eligible population. It would focus on shifting the entire population distribution rather than on targeting only relatively high-risk individuals, as illustrated earlier in this chapter. It would likely involve an agreed-on public policy requiring broad-based public understanding and political support. A selective preventive measure is one that is desirable only when an individual is a member of a subgroup of the population whose risk of becoming ill is above average. These are the more traditional population-oriented public health education interventions targeted toward the high-risk segments of the population. Finally, an indicated preventive measure is one that is applicable to persons who, on examination, manifest a risk factor, condition, or abnormality that identifies them individually as being at high risk for the future development of a disease. This type of intervention, usually provided in the context of clinical practice, deals only with individuals diagnosed with a disease, not with the nameless statistical subset of a population as in selective preventive measures. For example, a universal preventive measure for heart disease could include the provision of general advice to consume a diet low in fat accompanied by a regulatory policy requiring food labeling. A selective intervention could include a program focusing on diet and behavioral changes for overweight individuals who do not exercise regularly, and an indicated preventive measure might include antihypertensive medication for those diagnosed as hypertensive.
Although many studies have looked at the effectiveness of preventive measures, few have studied universal, population-level strategies. In some cases, however, such as tobacco use prevention and automobile-related injury prevention population-based strategies (e.g., laws) have been used successfully, largely because of recognition of the broad determinants of health. Results of these interventions indicate that, at least in some cases, a population-level strategy or, to use Gordon’s classification, a universal measure may be more optimal and cost-effective than interventions targeted further downstream (i.e., at the individual level). Acting on the most upstream level of determinants of health typically means the level of national policy. This may help shift national norms and values that lead to the passage, adoption, and ultimately, success of the respective legislation, as in the case of seat belt legislation, which has steadily and gradually normalized this behavior across America, or tobacco policy, which has curbed the use of tobacco (e.g., through changes in the social landscape of outdoor advertising and sanctions on smoking in the workplace and public places such as restaurants). Alternately, upstream policy interventions may also refer to modifying the broader, social determinants of health such as income (e.g., through the provision of earned income tax credits and minimum wage increases), education, and social connectedness.
Policy making at the national, state, and local levels has the potential to positively shape population health by addressing specific elements of the determinants of health, such as inadequate housing, unavailability of family-friendly social and work policies, lack of public transportation, lack of safe public spaces, and so forth. The health consequences of contaminated water and leaded gasoline have been well elaborated. It is now time to determine their social equivalents—elements of the social environment that influence health status—and take action to shape them in support of population health. Such action may focus not only on education, decent housing, and a living wage but also on the political choices that move the broad (social and other) determinants of health in a positive direction. For example, certain health care disparities (e.g., disparities in access and quality) are created in part by political choices and by allowing public and private insurance programs to limit coverage for preventive health care and for conditions related to mental health, substance abuse, and oral health.
Seat Belt Laws
Federal legislation has been an important strategy in reducing motor vehicle injuries (IOM, 1998). Between 1966 and 1970, highway safety acts authorized the federal government to set safety standards for new vehicles and equipment (e.g., standard safety belts for all automobile occupants) and to develop a coordinated national highway safety program, established in 1970 as the National Highway and Traffic Safety Administration.
A number of early studies found seat belts to be cost-effective (Warner, 1982). A more recent report outlines the benefits of safety belts based on medical and financial information from the Crash Outcome Data Evaluation System. A 1996 report to Congress revealed that safety belts are highly effective in reducing morbidity and mortality and in decreasing the severity of injuries (e.g., the inpatient charge for unbelted accident victims was 55 percent greater than the charge for those who wore seat belts) (NHTSA, 1996). Other evidence suggests smaller, although still significant, differences between injuries experienced by belted and unbelted accident victims. National averages indicate that for each occupant involved in a crash, medical costs average $2,930 for restrained riders and $5,630 for unrestrained riders (in 1995 dollars) (Miller et al., 1998).
Although there are ethnic differences in seat belt use, rates of seat belt use are higher in states that implement and enforce restraint laws (Davis et al., 2001; Schiff and Becker, 2002). Seat belt laws have had a significant impact on modifying behavior and thus decreasing risk and improving health outcomes across the population. Such strong effects for any single piece of legislation illustrate that this orientation can be effective. A meta-analysis of research regarding the effectiveness of interventions to
increase the use of seat belts found that both primary seat belt laws (a motorist can be stopped for not wearing a seat belt) and secondary seat belt laws (a motorist stopped for other reasons can also be cited for not wearing a seat belt), as well as enhanced enforcement policies (e.g., more officers and checkpoints for seat belts), are effective (Dinh-Zarr, 2001). An economic analysis found that the benefit–cost ratio for passage of a seat belt law was $260 per new user. The benefit–cost ratio per quality-adjusted life year showed that all three interventions offered net cost savings (Miller, 2001). The case of seat belt legislation demonstrates that such upstream or population-level measures aiming to prevent disease and disability may be effective in transforming social norms and ultimately changing behavior.
The Case of Tobacco
Tobacco prevention and cessation efforts have offered many lessons about the links between behavior and disease and how to intervene effectively to improve population health. CDC described the “antismoking campaign” dating from the first Surgeon General’s report as one of the major public health successes of the second half of the twentieth century (Warner, 2000). Effective antismoking campaigns are generally comprehensive, multidimensional interventions involving several aspects of prevention and control. One of the most important lessons learned from the tobacco experience is that the social context or social environment serves as a potent force in shaping smoking behavior. Therefore, measures such as creating educational and information-filled environments (from counteradvertising to truthful labeling and Surgeon General’s warnings) and enacting regulations to restrict smoking in buildings or public spaces and to control tobacco marketing and sales (to minors) have been effective in changing smoking behavior.
School-based antismoking interventions constitute an effective prevention strategy, although one that is resource intensive (and thus not sufficiently accessible), given the state-of-the-art programs needed to assure success (DHHS, 1994; Warner, 2000). The Growing Up Tobacco Free report (IOM, 1994a) has detailed three categories of tobacco prevention strategies: information dissemination approaches, effective education approaches, and social influence approaches. According to that report, the former two strategies fail to address the relationship between the acquisition of knowledge and behavior and the addictive nature of tobacco, nor do they address the social context in which smoking occurs, which often involves peer pressure and norms about use. The third strategy (the social influence approach) was developed to address the deficiencies of earlier strategies, and in a meta-analysis of 143 adolescent drug use prevention
programs, it was found that peer programs based on this strategy had the greatest effects on all outcome measures for the average school-based population (Tobler, 1986). Multiple levels of influence and multiple determinants affect the uptake of smoking, from individual characteristics and behaviors to population-level advertising and availability. Also, as noted earlier in the context of generic population health improvement, upstream approaches, including action at the community or population level, may be more cost-effective than downstream approaches directed at specific individuals (Corbett, 2001). Such measures, it seems, make use of the characteristics of social networks and relationships that may be used as elements to further protect health. Although recognizing the importance of approaches that go beyond individuals and their behavior, use of a social influences strategy may not work well if it is used alone, as in the case of the Hutchinson Smoking Prevention Project, a long-term randomized trial that used a school-based social influences approach and concluded that it lacked long-term effectiveness to deter smoking (Peterson et al., 2000). According to Warner (2000), success is more likely when a broad array of multisectoral, multilevel, upstream interventions is used.
Such upstream measures include taxation of cigarettes, which appears to affect tobacco consumption among youth and adults and both the initiation and the cessation of tobacco-smoking (Chaloupka et al., 2002). It also appears to have a more powerful impact among lower-income groups than higher-income groups, an important concept because most of the educational interventions are believed to be more effective among more highly educated groups (Evans and Farelly, 1998; Warner, 2000). Overall, on average it appears that an approximately 10 percent increase in the price of cigarettes will produce a 4 percent reduction in demand. Policies based on taxation have the potential to have a significant impact on smoking rates nationwide (Warner, 2000), although the effectiveness of taxation on teenagers becomes somewhat attenuated in adulthood, underscoring the need for interventions on several fronts (Glied, 2002). An added benefit of tax increases is the production of revenue while the level of consumption declines. Cigarette taxation is an excellent example of a cost-effective preventive strategy aimed at the entire population. It is serving to broaden the face of policy interventions in public health, leading to consideration of taxation in relation to alcohol consumption, unhealthy diets, and even gun control. It is feasible that such economic disincentives could affect a broad range of other social and behavioral conditions as well.
In a recent effort to develop a model for evaluating the outcomes of youth-targeted tobacco prevention and control programs, the Social Science Research Center at Mississippi State University developed a Social Climate Survey. Baseline data were obtained in 1999, and national data were added to the model in 2000 for comparison purposes. The Social
Climate Survey measures beliefs, norms, and practices related to tobacco use, sale, taxation, and regulation in seven social institutional areas: family and friendship groups, education, government and political order, work, health and medical care, recreation/leisure/sports, and mass communication or culture. Data from the surveys have indicated that implementation of a comprehensive, multidimensional approach to tobacco prevention and cessation will affect the social climate in which decisions regarding tobacco use are made (McMillen et al., 2001).
Some of the most striking examples of the environmental embeddedness and social implications of health risk come from the study of alcohol and tobacco product advertising. For example, a study of billboards in Chicago was compared to census data and demonstrated that the density of advertising for alcohol was five times higher in poor and minority urban wards than in other geographic areas and that the density of advertising for tobacco products was three times higher (Hackbarth et al., 1995). An observational study of tobacco billboard advertising in St. Louis used geographic information systems and found that advertisements were concentrated in low-income and minority neighborhoods, as well as in close proximity to public school property (Luke et al., 2000). Such data support recent efforts to control tobacco advertising, adding this to the arsenal of taxation and limits on smoking in public places.
THE PUBLIC HEALTH SYSTEM IN ACTION: A SCENARIO
In this section, the committee uses the specific scenario of a risk to population health—namely, obesity—to present and discuss the contributions that communities, the health care delivery system, employers and business, the media, academia, and the governmental public health infrastructure can make to improve health. Food and eating are integral to the life of individuals and communities. Families, friends, and neighbors gather around meals; and both the process of eating and the food itself are heavily imbued with cultural, social, and even emotional meaning. This helps explain why eating and nutrition perfectly exemplify the influence of multiple determinants on health. The development of obesity itself is influenced by multiple determinants of health, from the genetic to the social and environmental, and the public health partners must consider these many dimensions in formulating their responses.
Obesity: Magnitude and Future Trends
The problems of overweight and obesity in America have reached epidemic proportions and threaten the health and quality of life of millions of adults and children. According to CDC’s 1999 National Health and Nutri-
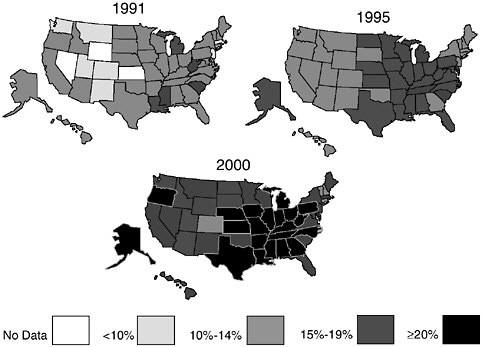
FIGURE 2–3 Obesity trends among U.S. adults: Behavioral Risk Factor Surveillance System (BRFSS), 1991, 1995, 2000.
NOTE: Obesity is BMI ≥ 30, or –30 lbs overweight for 5′4″ woman.
SOURCE: CDC (www.cdc.gov/nccdphp/dnpa/obesity/trend/maps/slide/003.htm), citing Mokdad et al. (1999).
tion Examination Survey, more than 61 percent of adults are either overweight or obese and at least 13 percent of children ages 6 to 11 and 14 percent of adolescents ages 12 to 19 are overweight. The prevalence of obesity among adults has grown by nearly 20 percent over the past 30 years, and the number of children who are overweight has tripled in the same period (see Figure 2–3) (CDC, 2001a).
Obesity is a growing concern because it poses a higher risk and results in a higher incidence of health conditions such as diabetes, cardiovascular disease, stroke hypertension, osteoarthritis, and certain cancers than other risk factors (NIH, 1998; Allison et al., 1999; Must et al., 1999; Williamson, 1999; Tataranni and Bogardus, 2001; Tuomilehto et al., 2001).
The human and economic costs are impossible to ignore. Every year an estimated 300,000 U.S. adults die of causes that may be attributed to obesity; in addition, others suffer from chronic disease and an impaired quality of life (Allison et al., 1999; Mokdad et al., 2000). According to another estimate, as many as 309,000 to 582,000 deaths in 1990 were
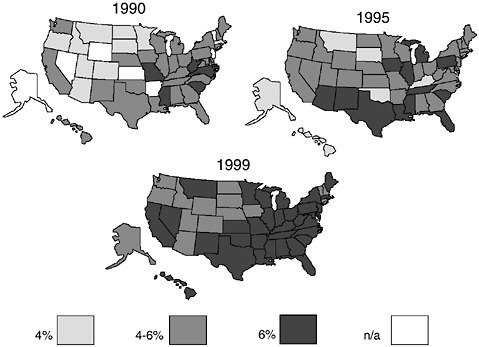
FIGURE 2–4 Diabetes and Gestational Diabetes trends among adults in the United States: BRFSS 1990, 1995, and 1999.
SOURCES: CDC (www.cdc.gov/diabetes/pubs/glance.htm) and Mokdad et al. (2000).
associated with poor diet and inadequate physical activity (McGinnis and Foege, 1993). Should the number of overweight and obese Americans continue to grow at its current rate, obesity will surpass tobacco as the most preventable cause of death and illness in the United States. Additionally, the estimated direct and indirect costs associated with obesity are $100 billion annually (Wolf and Colditz, 1998), and this figure does not take into consideration the cost of treating the uninsured or the personal impact of obesity on quality of life.
The fact that the prevalence and incidence of type II diabetes mellitus (see Figure 2–4) have increased exemplifies the association between weight and health. The rise in the rate of obesity during the past decade has been paralleled by a 25 percent increase in the rate of type II diabetes (Harris et al., 1998). The rapid and large rate of increase in obesity among children is especially alarming, given that childhood obesity is clearly associated with obesity in adulthood and subsequent health problems. For instance, until recently, type I diabetes was the most prevalent type of diabetes among children. However, new studies have shown that the rate of type II diabetes is increasing dramatically and that 85 percent of children with type II
diabetes are either overweight or obese (ADA, 2000). Approximately 63 percent of the total direct costs associated with obesity are related to type II diabetes (Wolf and Colditz, 1998).
Although the prevalence and growth of obesity affect all segments of the population, there are notable trends among certain segments. Men are more likely to be overweight, whereas women are more likely to be obese. Obesity also increases with age until the mid-60s; this may be partly because Americans over the age of 65 are more likely to be malnourished. The prevalence of obesity among African Americans and Hispanics, especially women, is significantly higher than that among other populations. People with lower education and income levels also have increased rates of obesity, as do people living in the southeastern region of the United States (CDC, 2000).
The causes of obesity are both complex and multifaceted. Although genetic factors do play a role in determining whether a person has a propensity for obesity, nutritional, behavioral, and environmental factors are more significant (Hill and Peters, 1998). Americans are consuming more calories, eating higher-calorie foods, and exercising less than ever before. Work is more likely to be sedentary than in the past; and more time is spent watching television, playing video games, or using computers. High-calorie food choices are widely available and easily affordable as more Americans turn to fast food and prepared meals on a daily basis. Furthermore, food portions have become “supersized,” surpassing the Department of Agriculture and Department of Health and Human Services (DHHS) recommended dietary guidelines for how much food Americans should consume each day. At the same time, the number of physical education programs in schools is declining, and people in some communities lack access to affordable and nutritional food options and safe areas in which to exercise (Hill and Peters, 1998; CDC, 1999a; Crespo et al., 2001; Dietz, 2001; French et al., 2001).
The association between obesity and socioeconomic factors illustrates the value of a population perspective and the need to consider the multiple determinants of health in addressing population health improvement.
Engaging Partners
Changing patterns in infectious diseases typically attract attention and significant mobilization of funding and action. Chronic disease has often been less of a priority for public health and health care organizations, but the evidence of escalating obesity in the United States is alarming and should motivate widespread action to contain and reverse the effects of this silent epidemic. Such concerted action cannot be undertaken successfully by governmental public health agencies alone; it requires the resources and efforts of other partners within the public health system. Taking action to
address the problem of obesity also requires that all entities in the public health system engage in partnerships; demonstrate accountability to their patients, communities, clients, employers, and each other; make program and policy decisions based on the evidence (e.g., community assessments and effectiveness data); and communicate effectively with other partners and the public. For example, communities and community-based organizations can assess the extent of overweight and obesity in the community and engage in a range of activities, from traditional, modestly successful methods that involve the provision of education and information to more innovative and powerful efforts to change the community conditions that make sedentary living and unhealthy eating “the path of least resistance.” They can encourage the adoption of active lifestyles by working with community development and planning agencies to make parks and playing fields safe and accessible. As discussed in Chapter 4, communities can also make changes in their physical surroundings, by engaging in a variety of activities to improve neighborhood safety and livability, and by increasing the amount of green space and the recreational options available to children. Schools can become sites for community recreation centers that are affordable and easy to access. Communities could also facilitate the formation of community walk groups that meet on a regular basis to exercise together and share knowledge and success stories. The recently launched Hearts N’Parks program sponsored by the National Heart, Lung, and Blood Institute and the National Recreation and Park Association is getting communities interested and mobilized to become physically active by planning a variety of community and educational activities (NIH, 2002).
In the area of nutrition, school cafeterias can also modify their offerings to support better food choices by students. Through partnerships with schools, communities can work to change children’s eating and physical activity habits by providing support and information to help teachers and school staff modify curricula and change cafeteria menus, and by not permitting vending machines with sugar- and fat-laden products in the school setting. For example, the Los Angeles Unified School District discontinued soda vending on all school premises in the district, thus removing an element that has been linked to childhood obesity (Wood, 2002). Communities could also develop relationships with farmers to make fresh fruits and vegetables more readily available and affordable through weekly markets. Neighborhood restaurants and grocery stores could offer and advertise healthier foods. In partnership with local media, health officials, large and small businesses, and others, community groups can spearhead public awareness campaigns and emphasize the importance of physical activity and the opportunities available, as well as the need to make healthy food choices, within a context of enhanced access, affordability, and cultural appropriateness.
The health care delivery system can provide training and resources to all health care providers and professionals to recognize and monitor individuals who are overweight or obese and to inform and educate patients about the risks and the changes that they can make and the benefits that they will receive. Health care plans should base administrative policy decisions on the evidence (e.g., the association between eating, exercise, and chronic disease and the three times greater likelihood that patients who are counseled about weight loss by their health care providers will actually try to lose weight). The health care sector should also work to adopt the National Institutes of Health’s (NIH’s) 1998 Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults and partner with researchers to establish treatment protocols (e.g., pharmacotherapy and surgery) that are safe, effective, and tailored to individual needs and circumstances. Health care systems and providers should also communicate and work collaboratively with health departments and community-based and national associations and advocacy groups focused on educating the public about the link between obesity and chronic disease.
Businesses and employers can play a major role in carrying out some essential public health services. The contributions of employers may range from providing health insurance plans that offer comprehensive preventive services to supporting research about and implementation of workplace promotion of weight management (e.g., by providing healthy cafeteria and vending machine alternatives and the space, equipment, and time for physical activity). Food industry businesses may also provide point-of-sale nutritional information and healthier menu options.
The news and entertainment media can play a unique part in addressing the problem of obesity. The media can serve primarily as a source of information about the associations between physical activity and nutrition, weight, and chronic disease. Through reporting and entertainment, the media creates a forum for discussing Americans’ increasing girth, its implications for overall health, the social and cultural correlates, and related issues that may increase awareness. Local media may collaborate with local health officials to communicate locally relevant information and to highlight opportunities for community-based physical activity. By taking part in tackling this major population health concern, the media can better fulfill its accountability to the public to provide accurate and timely information.
The academic setting can make many contributions to addressing obesity and its impact on overall population health, especially to the evidence base. For example, research has demonstrated that educational approaches aimed at improving individual knowledge and action about food choices and exercise have been largely ineffective at preventing weight gain (Nestle and Jacobson, 2000; Jeffery, 2001). Academic research is necessary to enhance current monitoring and surveillance tools to more accurately track
obesity, eating habits, and physical activity among all adults, children, specific populations, and states. Also needed is the development of more precise and consistent assessment tools for measuring obesity and overweight among children. It is also important for academia to continue to support, evaluate, and implement projects related to environmental conditions and policies for their impact on decreasing obesity and increasing healthy eating habits and physical activity. Academia can also disseminate data more broadly to interested parties on initiatives, programs, and policies that are effective and document and analyze how obesity affects mental health, development, and socialization; continue to research the relationship between obesity and various medical conditions; and develop prevention and treatment protocols to address them. Academic researchers can continue to evaluate treatment strategies made available by advances in technology, pharmacokinetics, and genetic research.
The role of the governmental public health infrastructure in responding to the obesity epidemic is multifaceted. Such efforts may include supporting the activities of other partners, funding NIH and academic research on obesity, helping to develop the Dietary Guide for Americans (a collaboration between DHHS and the Department of Agriculture), and spearheading a variety of initiatives such as food labeling. The role of the federal government in addressing obesity is essential, as it sets the pace for the nation and underscores this as a critical issue in assuring population health. In June 2002, in the wake of the 2001 Surgeon General’s report on obesity, President George W. Bush launched a new initiative, HealthierUS, that encourages Americans to pursue physical activity, healthy eating, and other healthy choices and to get preventive screenings (White House, 2002). In July 2002, CDC launched a multicultural Youth Media Campaign (entitled “VERB: It’s what you do.”) targeting youth across the nation (DHHS, 2002). The campaign encourages children between ages 9 and 13 to choose a “verb” (e.g., swim, run, or bowl) that fits their personality and interests and to start applying that verb in their daily lives. The campaign aims to engage children in a type of physical activity that they enjoy and, ultimately, to help them reap the related benefits of enhanced self-esteem, social connectedness, confidence, and discipline. At the local level of governmental public health agencies, health departments may administer or collaborate with the Department of Agriculture’s Women, Infants and Children (WIC) food supplementation program that provides nutritious foods and education to mothers and children up to age 5. They may also collaborate with local school programs and engage in many other community-based efforts that target overweight and obesity through a wide range of activities.
CONCLUDING OBSERVATIONS
In the previous sections, the committee has outlined what population health means in terms of understanding not only the risks of various exposures to individuals but also the importance of incorporating concepts related to the distribution of risk in populations. This chapter has outlined a way to understand how social, environmental, and biological conditions shape population health. Population-based interventions, such as tobacco control policies, show that it is possible to implement cost-effective strategies that benefit society as a whole and improve the health of many segments of the population. Population health improvements will have to focus attention on both overall improvement in the nation’s health and reduction of the disparities in health, as recommended by Healthy People 2010. To achieve this goal, the nation will have to develop innovative strategies for interventions for a broad set of health determinants. Many of the determinants of health are part of the broad economic and social context and, thus, beyond the direct control of administrators in public- and private-sector health care organizations. Action on these strategies at the national level will require an alignment of public policy in the agriculture, commerce, education, and treasury sectors of government, among others, to promote health. This includes providing resources to support the population-based research necessary to further our understanding of the social etiology of disease and disability. Efforts to curb tobacco use have a 50-year history from the appearance of the first surgeon general’s report. There is now a high level of consensus and political will to act. Effective public health systems must be vehicles to accelerate such efforts to save thousands of lives that will otherwise be lost. The special role of the governmental public health infrastructure is to advocate for and educate others about the evidence to support such policy actions and to assure that the public health system—the diverse array of individuals and organizations that must act together for health at the community level—is both committed to and equipped for implementation of a coordinated set of strategies to attain the highest levels of health for the nation. The next chapters of this report explore the potential role of each component of the public health system in achieving this goal.
Assurance is one of the three core public health functions put forth by the 1988 IOM report The Future of Public Health. The special role of the governmental public health infrastructure in this mission will be that of steward, facilitator, and supporter rather than actor in every situation, because assuring a healthy nation cannot be accomplished through a single plan of action or through the efforts of a single governmental agency or sector of the economy. Instead, it will require a coordinated set of strategies that must be implemented by all Americans—as individuals, families and community mem-
bers, businesses and workers, and citizens. With each sector of society assuming a portion of the responsibility for improving the health of the nation, it becomes increasingly possible to achieve the nation’s true potential for a population with excellent health and the fewest possible disparities.
The chapters that follow discuss several partners within a redefined public health system that has as its backbone the governmental public health infrastructure but that includes the resources, perspectives, and actions of other stakeholders who are partners in the public health system. Each of these partners can increase the relevance of its contributions to population health by considering the multiple determinants of health, especially those that contribute to unequal opportunities for good health.
REFERENCES
Adler NE, Boyce T, Chesney MA, Cohen S, Folkman S, Kahn RL, Syme SL. 1994. Socioeconomic status and health: the challenge of the gradient. American Psychologist 49(1):15–24.
Allison DB, Fontaine KR, Manson JE, Stevens J, VanItallie TB. 1999. Annual deaths attributable to obesity in the United States. Journal of the American Medical Association 282(16):1530–1538.
American Diabetes Association (ADA). 2000. Type 2 diabetes in children and adolescents. Pediatrics 105(3, Pt. 1):671–680.
Anderson RT, Sorlie P, Backlund E, Johnson N, Kaplan GA. 1997. Mortality effects of community socioeconomic status. Epidemiology 8:42–47.
Atkinson AB, Rainwater L, Smeeding TM. 1995. Income Distribution in OECD Countries: Evidence from the Luxembourg Income Study. Paris: Organization for Economic Cooperation and Development.
Backlund E, Sorlie PD, Johnson NJ. 1996. The shape of the relationship between income and mortality in the United States: evidence from the National Longitudinal Mortality Study. Annals of Epidemiology 6(1):12–20.
Bassuk SS, TA Glass, LF Berkman. 1999. Social disengagement and incident cognitive decline in community-dwelling elderly persons. Annals of Internal Medicine 131(3):165–173.
Baumeister RF, Leary MR. 1995. The need to belong: desire for interpersonal attachments as a fundamental human motivation. Psychological Bulletin 117:497–529.
Berkman L, Syme S. 1979. Social networks host resistance and mortality: a nine-year follow-up of Alameda County residents. American Journal of Epidemiology 109:186–204.
Berkman L, Glass T. 2000. Social integration social networks social support and health. In Berkman L, Kawachi I (Eds.). Social Epidemiology. New York: Oxford University Press.
Berkman L, Kawachi I (Eds.). 2000. Social Epidemiology. New York: Oxford University Press.
Berkman LF, Lochner KA. 2002. Social determinants of health: meeting at the crossroads. Health Affairs 21(2):291–293.
Berkman LF, Leo-Summers L, and Horwitz RI. 1992. Emotional support and survival after myocardial infarction: a prospective population-based study of the elderly. Annals of Internal Medicine 117:1003–1009.
Blane D, Bartley M, Davey Smith G. 1997. Disease aetiology and materialistic explanations of socioeconomic mortality differentials. European Journal of Public Health 7:385–391.
Blazer D. 1982. Social support and mortality in an elderly community population. American Journal of Epidemiology 115:684–694.
Bosma H, Marmot MG, Hemingway H, Nicholson AC, Brunner E, Stansfeld SA. 1997. Low job control and risk of coronary heart disease in Whitehall II (prospective cohort) study. British Medical Journal 314:558–565.
Bosma H, Peter R, Siegrist J, Marmot M. 1998. Two alternative job stress models and the risk of coronary heart disease. American Journal of Public Health 88:68–74.
Brown LR, Renner M, Flavin C. 1997. Vital Signs 1997. New York: W. W. Norton and Company.
Bureau of the Census. 1993. United States 1790–1990. Table 4. Available online at www.census.gov/population/censusdata/table-4.pdf. Accessed October 10, 2002.
Buunk BP, Verhoeven K. 1991. Companionship and support at work: a microanalysis of the stress-reducing features of social interactions. Basic and Applied Social Psychology 12:243–258.
Cacioppo JT, Ernst JM, Burleson MH, McClintock MK, Malarkey WB, Hawkley LC, Kowalewski RB, Paulsen A, Hobson JA, Hugdahl K, Spiegel D, Bernston GG. 2000. Lonely traits and concomitant physiological processes: the MacArthur social neuroscience studies. International Journal of Psychophysiology 35:143–154.
Carlisle DM, Leake BD, Shapiro MF. 1997. Racial and ethnic disparities in the use of cardiovascular procedures: associations with type of health insurance. American Journal of Public Health 87(2):263–267.
Case RB, Moss AJ, Case N, McDermott M, Eberly S. 1992. Living alone after myocardial infarction. Journal of the American Medical Association 267:515–519.
Catalano R, Dooley D, Wilson G, Hough R. 1993. Job loss and alcohol abuse: a test using data from the Epidemiologic Catchment Area Project. Journal of Health and Social Behavior 34:215–225.
CDC (Centers for Disease Control and Prevention). 1999a. Neighborhood safety and the prevalence of physical inactivity—selected states, 1996. Morbidity and Mortality Weekly Report 48:143–146.
CDC. 1999b. Ten great public health achievements—United States, 1900–1999. Morbidity and Mortality Weekly Report 48(12):241–243.
CDC. 2000. The Fact Book 2000/2001. Available online at http://www.cdc.gov/maso/factbook/main.htm. Accessed August 12, 2002.
CDC. 2001a. CDC FactBook 2000/2001: Profile of the Nation’s Health. Atlanta, GA: CDC.
CDC. 2001b. State trends in health and mortality. Prepared by the National Center for Health Statistics, CDC. Available online at http://www.cdc.gov/nchs/datawh/statab/morttables.htm. Accessed October 14, 2002.
CDC. 2001c. Blood and hair mercury levels in young children and women of childbearing age—United States, 1999. Morbidity and Mortality Weekly Report 50(8):140–143.
CDC. 2002. Prevalence of obesity among U.S. adults, by characteristics. Data from the Behavioral Risk Factor Surveillance System (1991–2000). Available online at http://www.cdc.gov/nccdphp/dnpa/obesity/trend/prev_char.htm. Accessed October 13, 2002.
Chaloupka FJ, Cummings KM, Morley CP, Horan JK. 2002. Tax, price and cigarette smoking: evidence from the tobacco documents and implications for tobacco company marketing strategies. Tobacco Control 11(Suppl. 1):I62–I72.
Cohen S. 1988. Psychosocial models of the role of social support in the etiology of physical disease. Health Psychology 7:269–297.
Cohen S, Doyle WJ, Skoner DP, Rabin BS, Gwaltney JM Jr. 1997. Social ties and susceptibility to the common cold. Journal of the American Medical Association 277:1940–1944.
Cohen S, Frank E, Doyle WJ, Skoner DP, Rabin BS, Gwaltney JM. 1998. Types of stressors that increase susceptibility to the common cold in healthy adults. Health Psychology 17:214–223.
Colantonio A, Kasl S, Ostfeld A. 1992. Depressive symptoms and other psychosocial factors as predictors of stroke in the elderly. American Journal of Epidemiology 136:884–894.
Colantonio A, Kasl SV, Ostfeld AM, and Berkman LF. 1993. Psychosocial predictors of stroke outcomes in an elderly population. Journal of Gerontology 48:S261–S268.
Corbett KC. 2001. Susceptibility of youth to tobacco: a social ecological framework for prevention. Respiration Physiology 128:103–118.
Costa G, Segnan N. 1987. Unemployment and mortality. British Medical Journal (Clinical Research Edition) 294:1550–1551.
Crespo CJ, Smit E, Troiano RP, Bartlett SJ, Macera CA, Andersen RE. 2001. Television watching, energy intake, and obesity in US children: results from the third National Health and Nutrition Examination Survey, 1988–1994. Archives of Pediatrics and Adolescent Medicine 155(3):360–365.
Dahlgren G, Whitehead M. 1991. Policies and Strategies to Promote Social Equity in Health. Stockholm: Institute for the Futures Studies.
Davey Smith G, Shipley MJ, Rose G. 1990. Magnitude and causes of socioeconomic differentials in mortality: further evidence from the Whitehall Study. Journal of Epidemiology and Community Health 44:265–270.
Davey Smith G, Neaton JD, Wentworth D, Stamler R, Stamler J. 1996a. Socioeconomic differentials in mortality risk among men screened for the Multiple Risk Factor Intervention Trial II. Black men. American Journal of Public Health 86:497–504.
Davey Smith G, Wentworth D, Neaton JD, Stamler R, Stamler J. 1996b. Socioeconomic differentials in mortality risk among men screened for the Multiple Risk Factor Intervention Trial. I. White men. American Journal of Public Health 86:486–496.
Davis JW, Bennink L, Kaups KL, Parks SN. 2002. Motor vehicle restraints: primary versus secondary enforcement and ethnicity. Journal of Trauma 52(2):225–228.
Deaton A. 2002. Policy implications of the gradient of health and wealth. Health Affairs 21(2):13–30.
Deaton A, Lubotsky D. 2001. Mortality, inequality and race in American cities and states. Working Paper No. 8370. Cambridge, MA: National Bureau of Economic Research, Inc.
DHHS (Department of Health and Human Services). 2000. Healthy People 2010, Vol. I. A Systematic Approach to Health Improvement. Available online at www.health.gov/healthypeople/Document/html/uih/uih_2.htm. Accessed November 16, 2001.
DHHS. 2002. HHS launches new campaign to encourage physical activity and healthy behaviors for kids: “VERB: It’s what you do.” aims to spark “activity movement” among kids. DHHS press release. Available online at www.hhs.gov/news/press/2002press/20020717b.html. Accessed August 9, 2002.
Dietz WH. 2001. The obesity epidemic in young children. Reduce television viewing and promote playing. British Medical Journal 322(7282):313–314.
Dinh-Zarr TB, Sleet DA, Shults RA, Zaza S, Elder RW, Nichols JL, Thompson RS, Sosin DM. 2001. Reviews of evidence regarding interventions to increase the use of safety belts. American Journal of Preventive Medicine 21(4 Suppl.):48–65.
Dooley D, Fielding J, Lennart L. 1996. Health and unemployment. Annual Review of Public Health 17:449–465.
Durlauf S. 1999. The case “against” social capital. Research Paper No. 9929. Social Systems Research Institute, University of Wisconsin, Madison. Available online at http://www.ssc.wisc.edu/econ/Durlauf/research.html. Accessed October 14, 2002.
EPA (Environmental Protection Agency). 1997. Mercury study report to Congress. Volume I, Executive Summary. Washington, DC: EPA.
Epstein AM, Ayanian JZ. 2001. Racial disparities in medical care. New England Journal of Medicine 344(19):1471–1473.
Evans RG, Stoddart GL. 1990. Producing health, consuming healthcare. Social Science and Medicine 31(12):1347–1363.
Ewart CK, Taylor CB, Kraemer HC, Agras WS. 1991. High blood pressure and marital discord: not being nasty matters more than being nice. Health Psychology 10:155–163.
Feldman J, Makuc D, Kleinman J, Cornoni-Huntley J. 1989. National trends in educational differentials in mortality. American Journal of Epidemiology 129:919–933.
Ferrie J, Shipley M, Marmot M, Stansfeld S, Davey Smith G. 1995. Health effects of anticipation of job change and non-employment: longitudinal data from the Whitehall II study. British Medical Journal 311:1264–1269.
Ferrie J, Shipley M, Marmot M, Stansfeld S, Davey Smith G. 1998. The health effects of major organisational change and job insecurity. Social Science and Medicine 46:243–254.
Fiscella K, Franks P, Gold MR, Clancy CM. 2000. Inequality in quality: addressing socioeconomic, racial, and ethnic disparities in health care. Journal of the American Medical Association 283(19):2579–2584.
Fratiglioni L, Wang HX, Ericsson K, Maytan M, Winblad B. 2000. Influence of social network on occurrence of dementia: a community-based longitudinal study. Lancet 355:1315–1319.
French SA, Story M, Jeffery RW. 2001. Environmental influences on eating and physical activity. Annual Review of Public Health 22:309–335.
Freudenberg N. 2000. Time for a national agenda to improve the health of urban populations. American Journal of Public Health 90(6):837–840.
Friedland J, McColl M. 1987. Social support and psychosocial dysfunction after stroke: buffering effects in a community sample. Archives of Physical Medicine and Rehabilitation 68(8):475–480.
Geronimus AT. 2000. To mitigate, resist or undo: addressing structural influences on the health of urban populations. American Journal of Public Health 90(6):867–872.
Geronimus AT, Bound J, Waidmann TA, Hillemeier MM, Burns PB. 1996. Excess mortality among blacks and whites in the United States. New England Journal of Medicine 335:1552–1558.
Glaser R, Kiecolt-Glaser JK, Bonneau RH, Malarkey W, Kennedy S, Hughes J. 1992. Stress-induced modulation of the immune response to recombinant hepatitis B vaccine. Psychosomatic Medicine 54:22–29.
Glaser R, Rabin B, Chesney M, Cohen S, Natelson B. 1999. Stress-induced immunomodulation: implications for infectious diseases? Journal of the American Medical Association 281:2268–2270.
Glass TA, Matchar DB, Belyea M, Feussner JR. 1993. Impact of social support on outcome in first stroke. Stroke 24(1):64–70.
Glass TA, Dym B, Greenberg S, Rintell D, Roesch C, Berkman LF. 2000. Psychosocial intervention in stroke: Families in Recovery from Stroke Trial (FIRST). American Journal of Orthopsychiatry 70(2):169–181.
Glied S. 2002. Youth tobacco control: reconciling theory and empirical evidence. Journal of Health Economics 21(1):117–135.
Granovetter M. 1995. Getting a Job: A Study of Contacts and Careers. Cambridge, MA: Harvard University Press.
Gravelle H, Wildman J, Sutton M. 2002. Income, income inequality and health: what can we learn from aggregate data? Social Science and Medicine 54(4):577–589.
Hackbarth DP, Silvestri B, Cosper W. 1995. Tobacco and alcohol billboards in 50 Chicago neighborhoods: market segmentation to sell dangerous products to the poor. Journal of Public Health Policy 16(2):213–230.
Hacker A. 1997. Money: Who Has How Much and Why. New York: Scribner.
Harris MI. 1998. Diabetes in America: epidemiology and scope of the problem. Diabetes Care 21(Suppl. 3):C11–C14.
Heaney C, Israel B, House J. 1994. Chronic job insecurity among automobile workers: effects on job satisfaction and health. Social Science and Medicine 38:1431–1437.
Hill JO, Peters JC. 1998. Environmental contributions to the obesity epidemic. Science 280(5368):1371–1374.
Hoek G, Brunekreef B, Fischer P, van Wijnen J. 2001. The association between air pollution and heart failure, arrhythmia, embolism, thrombosis, and other cardiovascular causes of death in a time series study. Epidemiology 12(3):355–357.
House J, Robbins C, Metzner H. 1982. The association of social relationships and activities with mortality: prospective evidence from the Tecumseh Community Health Study American. Journal of Epidemiology 116:123–140.
House JS, Landis KR, Umberson D. 1988. Social relationships and health. Science 241(4865):540–545.
Ibald-Mulli A, Stieber J, Wichmann HE, Koenig W, Peters A. 2001. Effects of air pollution on blood pressure: a population-based approach. American Journal of Public Health 91(4):571–577.
IOM (Institute of Medicine). 1988. The Future of Public Health. Washington, DC: National Academy Press.
IOM. 1994a. Growing up Tobacco Free: Preventing Nicotine Addition in Children and Youths. Washington, DC: National Academy Press.
IOM. 1994b. Reducing Risks for Mental Disorders: Frontiers for Preventive Intervention Research. Washington, DC: National Academy Press.
IOM. 1997. Improving Health in the Community. Washington, DC: National Academy Press.
IOM. 1998. Reducing the Burden of Injury: Advancing Prevention and Treatment. Washington, DC: National Academy Press.
IOM. 2000. Promoting Health: Intervention Strategies from Social and Behavioral Research. Washington, DC: National Academy Press.
IOM. 2001. Health and Behavior. Washington, DC: National Academy Press.
IOM. 2002. Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Washington, DC: The National Academies Press.
Iversen L, Andersen O, Andersen P, Christoffersen K, Keiding N. 1987. Unemployment and mortality in Denmark 1970–80. British Medical Journal 295:879–884.
Jeffery RW. 2001. Public health strategies for obesity treatment and prevention. American Journal of Health Behavior 25:252–259.
Jencks C. 2002. Does inequality matter? Daedalus Summer:49–65. Available online at www.daedalus.amacad.org/issues/winter2002/Jencks.pdf. Accessed October 2, 2002.
Johnson JV, Stewart W, Hall EM, Fredlund P, Theorell T. 1996. Long-term psychosocial work environmental and cardiovascular mortality among Swedish men. American Journal of Public Health 86:324–331.
Kaplan G, Salonen J, Cohen R, Brand R, Syme S, Puska P. 1988. Social connections and mortality from all causes and cardiovascular disease: prospective evidence from eastern Finland. American Journal of Epidemiology 128:370–380.
Kaplan GA, Keil JE. 1993. Socioeconomic factors and cardiovascular disease: a review of the literature. Circulation 88:1973–1998.
Kaplan GA, Pamuk E, Lynch JW, Cohen RD, Balfour JL. 1996. Inequality in income and mortality in the United States: analysis of mortality and potential pathways. British Medical Journal 312:999–1003.
Karasek R, Theorell T. 1990. Healthy Work. New York: Basic Books.
Kasl S, Jones B. 2000. The impact of job loss and retirement on health. In Berkman L, Kawachi I (Eds.). Social Epidemiology. New York: Oxford University Press.
Kawachi I, Berkman L. 2000. Social cohesion, social capital and health. In Berkman L, Kawachi I (Eds.). Social Epidemiology. New York: Oxford University Press.
Kawachi I, Kennedy BP. 1997. Socioeconomic determinants of health: health and social cohesion: why care about income inequality? British Medical Journal 314:1037–1040.
Kawachi I, Colditz GA, Ascherio A, Rimm EB, Giovannucci E, Stampfer MJ, Willett WC. 1996. A prospective study of social networks in relation to total mortality and cardiovascular disease in men in the USA. Journal of Epidemiology and Community Health 50:245–251.
Kawachi I, Kennedy B, Lochner K, Prothrow-Stith D. 1997. Social capital, income inequality and mortality. American Journal of Public Health 87:1491–1498.
Kawachi I, Kennedy BP, Glass R. 1999. Social capital and self-rated health: a contextual analysis. American Journal of Public Health 89:1187–1193.
Kawachi I, Subramanian SV, Almeida-Filho N. 2002. A glossary for health inequalities. Journal of Epidemiology and Community Health 56:647–652.
Kennedy BP, Kawachi I, Prothrow-Stith D. 1996. Income distribution and mortality: cross-sectional ecologic study of the Robin Hood Index in the United States. British Medical Journal 312:1004–1007.
Kennedy BP, Kawachi I, Glass R, Prothrow-Stith D. 1998. Income distribution, socioeconomic status and self rated health in the United States: multilevel analysis. British Medical Journal 317:917–921.
Kiecolt-Glaser JK, Marucha PT, Malarkey WB, Mercado AM, Glaser R. 1995. Slowing of wound healing by psychological stress. Lancet 346:1194–1196.
Kiecolt-Glaser JK, Glaser R, Cacioppo JT. 1997. Marital conflict in older adults: endocrinological and immunological correlates. Psychosomatic Medicine 59:339–349.
Kiecolt-Glaser JK, Page GG, Marucha PT, MacCallum RC, Glaser R. 1998. Psychological influences on surgical recovery: perspectives from psychoneuroimmunology. American Psychologist 53:1209–1218.
Kirschbaum C, Klauer T, Filipp SH, Hellhammer DH. 1995. Sex-specific effects of social support on cortisol and subjective responses to acute psychological stress. Psychosomatic Medicine 57(1):23–31.
Korenbrot CC, Moss NE. 2000. Preconception, prenatal, perinatal and postnatal influences on health, pp. 125–169. In Promoting Health: Intervention Strategies from Social and Behavioral Research. Washington, DC: National Academy Press.
Krieger N, Sidney S. 1996. Racial discrimination and blood pressure: the CARDIA study of young black and white adults. American Journal of Public Health 86(10):1370–1378.
Kunst AE, Groenhof F, Mackenbach J, European Union Working Group on Socioeconomic Inequalities in Health. 1998. Occupational class and cause specific mortality in middle aged men in 11 European countries: comparison of population based studies. British Medical Journal 316:1636–1642.
Lawrence J. 1999. Urban health: an ecological perspective. Review of Environmental Health 14(1):1–10.
Levenson RW, Carstensensen LL, Gottman JM. 1993. Long-term marriage: age gender and satisfaction. Psychology and Aging 8:301–313.
Leviton LC, Snell E, McGinnis M. 2000. Urban issues in health promotion strategies. American Journal of Public Health 90(6):863–866.
Link B, Phelan J. 1995. Social conditions as fundamental causes of disease. Journal of Health and Social Behavior (Special Issue):80–94.
Luke D, Esmundo E, Bloom Y. 2000. Smoke signs: patterns of tobacco billboard advertising in a metropolitan region. Tobacco Control 9:16–23.
Lynch J, Kaplan GA, Pamuk ER, Cohen RD, Heck KE, Balfour JL, Yen IH. 1998. Income inequality and mortality in metropolitan areas of the United States. American Journal of Public Health 88:1074–1080.
Lynch J, Davey Smith G, Hillemeiera M, Shawe M, Raghunathanb T, Kaplan G. 2001. Income inequality, the psychosocial environment, and health: comparisons of wealthy nations. Lancet 358(9277):194–200.
Lynch JW, Kaplan GA, Salonen JT. 1997. Why do poor people behave poorly? Variation in adult health behaviors and psychological characteristics by stages of the socioeconomic life course. Social Science and Medicine 44:809–819.
Maantay J. 2001. Zoning, equity, and public health. American Journal of Public Health 91(7):1033–1041.
Macintyre S, Ellaway A, Der G, Ford G, Hunt K. 1998. Do housing tenure and car access predict health because they are simply markers of income or self-esteem? A Scottish study. Journal of Epidemiology and Community Health 52:657–664.
Mackenbach JP, Stronks K, Kunst AE. 1989. The contribution of medical care to inequalities in health: differences between socioeconomic groups in decline of mortality from conditions amenable to medical intervention. Social Science and Medicine 29:369–376.
Malarkey WB, Kiecolt-Glaser JK, Pearl D, Glaser R. 1994. Hostile behavior during marital conflict alters pituitary and adrenal hormones. Psychosomatic Medicine 56:41–51.
Marmot MG, Davey Smith G, Stansfield S, Patel C, North F, Head J, White I, Brunner E, Feeney A. 1991. Health inequalities among British civil servants: the Whitehall II Study. Lancet 337:1387–1393.
Martikainen P. 1990. Unemployment and mortality among Finnish men 1981–5. British Medical Journal 301:407–411.
Mattiasson I, Lindegarde F, Nilsson J, Theorell T. 1990. Threat of unemployment and cardiovascular risk factors: longitudinal study of quality of sleep and serum cholesterol concentrations in men threatened with redundancy. British Medical Journal 301:461–465.
McGinnis JM, Foege WH. 1993. Actual causes of death in the United States. Journal of the American Medical Association 270(18):2207–2212.
McGinnis JM, Williams-Russo P, Knickman JR. 2002. The case for more active policy attention to health promotion. To succeed, we need leadership that informs and motivates, economic incentives that encourage change, and science that moves the frontiers. Health Affairs 21(2):78–93.
McLoyd VC. 1998. Socioeconomic disadvantage and child development. American Psychologist 53(2):185–204.
McMillen RC, Frese W, Cosby AG. 2001. The National Social Climate of Tobacco Control, 2000–2001. Starkville, MS: Social Science Research Center, Mississippi State University.
Meaney MJ, Diorio J, Francis D, Widdowson J, LaPlante P, Caldji C, Sharma S, Seckl JR, Plotsky PM. 1996. Early environmental regulation of forebrain glucocorticoid receptor gene expression: implications for adrenocortical responses to stress. Developmental Neuroscience 18(1–2):49–72.
Miller T, Lestina D, Spicer R. 1998. Highway crash costs in the United States by driver age, blood alcohol level, victim age, and restraint use. Accident Analysis and Prevention 30(2):137–150.
Miller TR. 2001. The effectiveness review trials of Hercules and some economic estimates for the stables. American Journal of Preventive Medicine 21(4 Suppl.):9–12.
Moen P. 1996. A life course perspective on retirement gender and well being. Journal of Occupational Health Psychology 1:131–144.
Mokdad AH, Serdula MK, Dietz WH, Bowman BA, Marks JS, Koplan JP. 1999. The spread of the obesity epidemic in the United States, 1991–1998. Journal of the American Medical Association 282(16):1519–1522.
Mokdad AH, Ford ES, Bowman BA, Nelson DE, Engelgau MM, Vinicor F, Marks JS. 2000. Diabetes trends in the U.S.: 1990–1998. Diabetes Care 23(9):1278–1283.
Morris J, Cook D. 1991. A critical review of the effect of factory closures on health. British Journal of Industrial Medicine 48:1–8.
Morris PL, Robinson RG, Andrzejewski P, Samuels J, Price TR. 1993. Association of depression with 10-year poststroke mortality. American Journal of Psychiatry 150(1):124–129.
Moser K, Fox A, Jones D. 1984. Unemployment and mortality in the OCPS Longitudinal Study. Lancet 2(8415):1324–1329.
Moser K, Fox A, Jones D, Goldblatt P. 1986. Unemployment and mortality: further evidence from the OCPS Longitudinal Study 1971–1981. Lancet 1(8477):365–367.
Moser K, Goldblatt P, Fox A, Jones D. 1987. Unemployment and mortality: comparison of the 1971 and 1981 longitudinal study census samples. British Medical Journal 294:86– 90.
Must A, Spadano J, Coakley EH, Field AE, Colditz G, Dietz WH. 1999. The disease burden associated with overweight and obesity. Journal of the American Medical Association 282(16):1523–1529.
NCHS (National Center for Health Statistics). 1992. Vital Statistics of the United States 1992. Washington DC: Government Printing Office.
NCHS. 1998. Health, United States, 1998. With Socioeconomic Status and Health Chartbook. Atlanta, GA: National Center for Health Statistics, Centers for Disease Control and Prevention, Department of Health and Human Services.
NCHS. 2001. Health, United States, 2001. With Urban and Rural Health Chartbook. Atlanta, GA: National Center for Health Statistics, Centers for Disease Control and Prevention, Department of Health and Human Services.
NCHS. 2002. Health, United States, 2002. With Chartbook on Trends in the Health of Americans. DHHS Publication No. 1232. Atlanta, GA: National Center for Health Statistics, Centers for Disease Control and Prevention, Department of Health and Human Services.
Nerem RM, Levesque MJ, Cornhill JF. 1980. Social environment as a factor in diet-induced atherosclerosis. Science 208(4451):1475–1476.
Nestle M, Jacobson MF. 2000. Halting the obesity epidemic: a public health policy approach. Public Health Reports 115(1):12–24.
NHTSA (National Highway Traffic Safety Administration). 1996. Report to Congress on benefits of safety belts and motorcycle helmets, based on data from the Crash Outcome Data Evaluation System (CODES). DOT HS 808–347. Washington, DC: Department of Transportation.
NIH (National Institutes of Health). 1998. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults. The Evidence Report. Rockville, MD: National Heart, Lung, and Blood Institute, National Institutes of Health.
NIH. 2001. Study finds no reduction in deaths or heart attacks in heart disease patients treated for depression and low social support. News Release, November 12, 2001, National Heart, Lung and Blood Institute, National Institutes of Health, Rockville, MD.
NIH. 2002. About Hearts N’ Parks. Available online at http://www.nhlbi.nih.gov/health/prof/heart/obesity/hrt_n_pk/. Accessed October 14, 2002.
North FM, Syme SL, Feeney A, Shipley M, Marmot M. 1996. Psychosocial work environment and sickness absence among British civil servants: the Whitehall II study. American Journal of Public Health 86:332–340.
NRC (National Research Council). 1999. Our Common Journey: A Transition Toward Sustainability. Washington, DC: National Academy Press.
NRC. 2000. Toxicological Effects of Methylmercury. Washington, DC: National Academy Press.
Office of Minority Health. 2000. Assessment of State Minority Health Infrastructure and Capacity to Address Issues of Health Disparity. Developed by COSMOS Corporation for the Office of Minority Health, Office of Public Health and Science, Department of Health and Human Services. Available online at http://www.omhrc.gov/omh/sidebar/cossmo/cover.htm. Accessed October 14, 2002.
Orth-Gomer K, Johnson J. 1987. Social network interaction and mortality: a six-year follow-up study of a random sample of the Swedish population. Journal of Chronic Diseases 40:949– 957.
Orth-Gomer K, Unden AL, Edwards ME. 1988. Social isolation and mortality in ischemic heart disease. A 10-year follow-up study of 150 middle-aged men. Acta Medica Scandinavica 224(3):205–215.
Ostrove JM, Feldman P, Adler NE. 1999. Relations among socioeconomic status indicators and health for African-Americans and whites. Journal of Health Psychology 4(4):451–463.
Pappas G, Queen S, Hadden W, Fisher G. 1993. The increasing disparity in mortality between socioeconomic groups in the US, 1960–1986. New England Journal of Medicine 329:103– 109.
Parker S, Chmiel N, Wall T. 1997. Work characteristics and employee well-being within a context of strategic downsizing. Journal of Occupational Health Psychology 2:289–303.
Pennix BW, van Tilburg T, Kriegsman DM, Deeg DJBoeke AJ, van Eijk JT. 1997. Effects of social support and personal coping resources on mortality in older age: the Longitudinal Aging Study, Amsterdam. American Journal of Epidemiology 146:510–519.
Pertowski C. 1994. Lead poisoning, pp. 311–320. In From Data to Action: CDC’s Public Health Surveillance for Women, Infants, and Children. Centers for Disease Control and Prevention Maternal & Child Health Monograph. Available online at http://www.cdc.gov/nccdphp/drh/datoact/. Accessed October 14, 2002.
Peters A, Dockery DW, Muller JE, Mittleman MA. 2001. Increased particulate air pollution and the triggering of myocardial infarction. Circulation 103(23):2810–2815.
Peterson AV, Kealey KA, Mann SL, Marek PM, Sarason IG. 2000. Hutchinson Smoking Prevention Project: long-term randomized trial in school-based tobacco use prevention— results on smoking. Journal of the National Cancer Institute 92(24):1979–1991.
Pew Environmental Health Commission. 2000. America’s environmental health gap: why the country needs a nationwide health tracking network. Pew Environmental Health Commission, Johns Hopkins University School of Public Health. Available online at http://healthyamericans.org/resources/files/healthgap.pdf. Accessed October 2, 2002.
Pew Environmental Health Commission. 2001. Transition report to the new administration: strengthening our public health defense against environmental threats. Pew Environmental Health Commission, Johns Hopkins University School of Public Health. Available online at http://healthyamericans.org/resources/files/transition.pdf. Accessed October 2, 2002.
Portes A, Landolt P. 1996. The downside of social capital. The American Prospect 26:18–21.
Proctor BD, Dalakar J. 2002. Poverty in the United States: 2001. Current Population Reports, P60–219. Washington, DC: Bureau of the Census, Department of Commerce.
Rodgers GB. 2002. Income and inequality as determinants of mortality: an international cross-section analysis. International Journal of Epidemiology 31(3):533–538.
Roetzheim RG, Pal N, Tennant C, Voti L, Ayanian JZ, Schwabe A, Krischer JP. 1999. Effects of health insurance and race on early detection of cancer. Journal of the National Cancer Institute 91(16):1409–1415.
Rogot E, Sorlie P, Johnson N. 1992. Life expectancy by employment status income and education in the National Longitudinal Mortality Study. Public Health Reports 107:457–461.
Rose G. 1981. Strategy of prevention: lessons from cardiovascular disease. British Medical Journal 282:1847–1851.
Rose G. 1992. The Strategy of Preventive Medicine. Oxford: Oxford University Press.
Roy MP, Steptoe A, Kirschbaum C. 1998. Life events and social support as moderators of individual differences in cardiovascular and cortisol reactivity. Journal of Personality and Social Psychology 75(5):1273–1281.
Sampson RJ, Raudenbush SW, Earls F. 1997. Neighborhoods and violent crime: a multilevel study of collective efficacy. Science 277:918–924.
Sandefur RF, Laumann OE. 1998. A paradigm for social capital. Rationality and Society 10(4):481–501.
Sapolsky RM, Alberts SC, Altmann J, 1997. Hypercortisolism associated with social subordinance or social isolation among wild baboons. Archives of General Psychiatry 54(12):1137–1143.
Sargent JD, Brown MJ, Freeman JL, Bailey A, Goodman D, Freeman D. 1995. Childhood lead poisoning in Massachusetts communities: its association with sociodemographic and housing characteristics. American Journal of Public Health 85(4):528–534.
Schiff M, Becker T. 1996. Trends in motor vehicle traffic fatalities among Hispanics, non-Hispanic whites and American Indians in New Mexico, 1958–1990. Ethnicity & Health 1(3):283–291.
Schnall P, Landsbergis P, Baker D. 1994. Job strain and cardiovascular disease. Annual Review of Public Health 15:381–411.
Schoenbach V, Kaplan B, Freedman L, Kleinbaum D. 1986. Social ties and mortality in Evans County Georgia. American Journal of Epidemiology 123:577–591.
Schwartz LM, Woloshin S. 1999. Changing disease definitions: implications for disease prevalence. Analysis of the Third National Health and Nutrition Examination Survey, 1988– 1994. Effective Clinical Practice 2(2):76–85.
Seeman T. 1996. Social ties and health: the benefits of social integration. Annals of Epidemiology 6:442–451.
Seeman T, Kaplan G, Knudsen L, Cohen R, Guralnik J. 1988. Social network ties and mortality among the elderly in the Alameda County Study. American Journal of Epidemiology 126:714–723.
Seeman T, Berkman L, Kohout F, LaCroix A, Glynn R, Blazer D. 1993. Intercommunity variation in the association between social ties and mortality in the elderly: a comparative analysis of three communities. Annals of Epidemiology 3:325–335.
Shively CA, Clarkson TB, Kaplan JR. 1989. Social deprivation and coronary artery atherosclerosis in female cynomolgus monkeys. Atherosclerosis 77(1):69–76.
Sigerist J. 1996. Adverse health effects of high-effort/low-reward conditions. Journal of Occupational Health Psychology 1:27–41.
Slifkin R, Goldsmith L, Ricketts T. 2000. Race and place: urban-rural differences in health for racial and ethnic minorities. North Carolina Rural Health Research Program, University of North Carolina at Chapel Hill, Cecil G. Sheps Center for Health Services Research, Working Paper No. 66. Available online at www.shepscenter.unc.edu/research_programs/Rural_Program/wp.html. Accessed October 10, 2002.
Soobader MJ, LeClere FB. 1999. Aggregation and the measurement of income inequality: effects on morbidity. Social Science and Medicine 48:733–744.
Sorlie P, Rogot E. 1990. Mortality by employment status in the National Longitudinal Mortality Study. American Journal of Epidemiology 132:983–992.
Sorlie P, Rogot E, Anderson R, Johnson N, Backlund E. 1992. Black-white mortality differences by family income. Lancet 340:346–350.
Sorlie P, Backlund E, Keller JB. 1995. US mortality by economic, demographic, and social characteristics: the National Longitudinal Mortality Study. American Journal of Public Health 585:949–956.
Stefansson C. 1991. Long-term unemployment and mortality in Sweden 1980–1986. Social Science and Medicine 32:419–423.
Sugisawa H, Liang J, Liu X. 1994. Social networks social support and mortality among older people in Japan. Journal of Gerontology 49:S313.
Suomi SJ. 1991. Early stress and adult emotional reactivity in rhesus monkeys. Ciba Foundation Symposium 156:171–183.
Syme S, Berkman L. 1976. Social class susceptibility and sickness. American Journal of Epidemiology 104:1–8.
Tataranni PA, Bogardus C. 2001. Changing habits to delay diabetes. New England Journal of Medicine 344(18):1390–1392.
Theorell T, Tsutsumi A, Hallquist J, Reuterwall C, Hogstedt C, Fredlund P, Emlund N, Johnson JV. 1998. Decision latitude job strain and myocardial infarction: a study of working men in Stockholm. The SHEEP Study Group Stockholm Heart Epidemiology Program. American Journal of Public Health 88:382–388.
Thomas SB. 2001. The color line: race matters in the elimination of health disparities. American Journal of Public Health 91(7):1046–1048.
Tobler NS. 1986. Meta-analysis of 143 adolescent drug prevention programs: quantitative outcome results of program participants compared to a control or comparison group. Journal of Drug Issues 16(4):537–567.
Trust for America’s Health. 2001. Short of breath: our lack of response to the growing asthma epidemic and the need for nationwide tracking. Available online at http://healthyamericans.org/resources/files/shortofbreath.pdf. Accessed October 10, 2002.
Tuomilehto J, Lindstrom J, Eriksson JG, Valle TT, Hamalainen H, Ilanne-Parikka P, Keinanen-Kiukaanniemi S, Laakso M, Louheranta A, Rastas M, Salminen V, Uusitupa M. 2001. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. New England Journal of Medicine 344(18):1343–1350.
Tyroler HA, Wing S, Knowles MG. 1993. Increasing inequality in coronary heart disease mortality in relation to educational achievement profiles of places of residence United States 1962 to 1987. Annals of Epidemiology 3:S51–S54.
USPHS (U.S. Public Health Service). 1979. Healthy People: the Surgeon General’s report on health promotion and disease prevention. DHEW (PHS) Publication No. 79–55071. Washington, DC: U.S. Public Health Service.
Vahtera J, Kivimaki M, Pentti J. 1997. Effect of organizational downsizing on health of employees. Lancet 350:1124–1128.
Vogt TM, Mullooly JP, Ernst D, Pope CR, Hollis JF. 1992. Social networks as predictors of ischemic heart disease, cancer, stroke, and hypertension: incidence survival and mortality. Journal of Clinical Epidemiology 45:659–666.
Warner KE. 1982. Mandatory passive restraint systems in automobiles: issues and evidence. Technology and handicapped people. Background Paper No. 1. Office of Technology Assessment, U.S. Congress. Washington, DC: Government Printing Office
Warner KE. 2000. The need for, and value of, a multi-level approach to disease prevention: the case of tobacco control, pp. 417–449. In Promoting Health: Intervention Strategies from Social and Behavioral Research. Institute of Medicine. Washington, DC: National Academy Press.
Weinberg DH. 1996. A Brief Look at Postwar US Income Inequality. Census Bureau Current Population Reports, P60–191. Washington, DC: U.S. Bureau of the Census, Department of Commerce.
Weinick RM, Krauss NA. 2000. Racial/ethnic differences in children’s access to care. American Journal of Public Health 90(11):1771–1774.
Welin L, Tibblin G, Svardsudd K, Tibblin B, Ander-Peciva S, Larsson B, Wilhelmsen L. 1985. Prospective study of social influences on mortality. The study of men born in 1913 and 1923. Lancet 1(8434):915–918.
The White House. 1998. President Clinton announces new racial and ethnic health disparities initiative. White House fact sheet, February 21, 1998. Available online at http://raceandhealth.hhs.gov/sidebars/sbwhats.htm. Accessed August 19, 2002.
The White House. 2002. President Bush launches HealthierUS initiative. Press release. Available online at www.whitehouse.gov/news/releases/2002/06/20020620-6.html. Accessed August 9, 2002.
Wilkinson RG. 1992. Income distribution and life expectancy. British Medical Journal 304:165–168.
Wilkinson RG. 1996. Unhealthy Societies: The Afflictions of Inequality. London: Routledge.
Williams DR. 1990. Socioeconomic differentials in health: a review and redirection. Social Psychology Quarterly 53:81–99.
Williams DR, Collins C. 1995. U.S. socioeconomic and social differences in health: patterns and explanations. Annual Review of Sociology 21:349–386.
Williams DR, Collins C. 2001. Racial residential segregation: a fundamental cause of racial disparities in health. Public Health Reports 116(5):404–416.
Williams RB, Barefoot JC, Califf RM, Haney TL, Saunders WB, Pryor DB, Hlatky MA, Siegler IC, Mark DB. 1992. Prognostic importance of social and economic resources among medically treated patients with angiographically documented coronary artery disease. Journal of the American Medical Association 267(4):520–524.
Williamson DF. 1999. The prevention of obesity. New England Journal of Medicine 341(15):1140–1141.
Wolf AM, Colditz GA. 1998. Current estimates of the economic cost of obesity in the United States. Obesity Research 6(2):97–106.
Wolff E. 2000. Reconciling Alternative Estimates of Wealth Inequality from the Survey of Consumer Finances. American Enterprise Institute Seminar on Economic Inequality, February 9, 2000.
Wood D. 2002. A farewell to fizz from LA lunchrooms. The Christian Science Monitor, August 30, 2002, p. 1.
Worthman CM. 1999. Epidemiology of human development, pp. 47–104. In Panter-Brick C, Worthman CM (Eds.). Hormones, Health, and Behavior: A Socio-Ecological and Lifespan Perspective. Cambridge: Cambridge University Press.