5
Factors Contributing to the Emergence of Resistance
OVERVIEW
Although microbial resistance results primarily as a consequence of selection pressure placed on susceptible microbes by the use of therapeutic agents, a variety of social and administrative factors also contribute to the emergence and spread of resistance. The focus of this session of the workshop was to examine these factors and to describe potential ways to minimize their role in promoting antimicrobial resistance.
In the United States and other developed countries, one leading factor is the over-prescription by physicians of antimicrobials, particularly antibiotics, even in the absence of appropriate indications. Such inappropriate physician practices are often fostered by diagnostic uncertainty, lack of opportunity for patient follow-up, lack of knowledge regarding optimal therapies, and patient demand. In many developing countries, problems typically arise because antimicrobial agents are readily available and can be purchased as a commodity without the advice or prescription of a physician or other trained health care provider.
Some common types of human behavior also play a role in promoting resistance. Of particular importance, for example, are patient self-medication and noncompliance with recommended treatments. Noncompliance occurs when individuals forget to take medication, prematurely discontinue the medication as they begin to feel better, or cannot afford a full course of therapy. Self-medication almost always involves unnecessary, inadequate, and ill-timed dosing. In some countries, problems of noncompliance and
self-medication are magnified because significant amounts of the available antimicrobials are poorly manufactured, counterfeit, or have exceeded their effective lifetimes.
Various practices common in hospitals contribute to the resistance problem as well. Indeed, hospitals are especially fertile grounds for breeding resistant microbes. They deal regularly with large numbers of patients (many with suppressed immune systems) in relatively close proximity to each other, and they frequently treat their patients with intensive and prolonged antimicrobial therapy. Large hospitals and teaching hospitals generally experience more problems with drug-resistant microbes, probably because they treat greater numbers of the sickest patients and those at highest risk of becoming infected. Transmission of drug-resistant organisms among patients may be airborne, from a point source (such as contaminated equipment), or by direct or indirect contact with a contaminated environment or the contaminated hands of staff. Failure of health care workers to practice simple control measures (e.g., hand washing and changing gloves after examining a patient) is a leading contributor to the spread of infection in hospitals.
Hospitals typically rely on two major forms of intervention to minimize resistance problems. One approach involves limiting antimicrobial use as much as possible; the other involves implementing intensive infection-control programs. Important components of these programs include surveillance; outbreak investigation and control; sterilization and disinfection of equipment; and implementation of such patient-care practices as handwashing, isolation, and barriers between infected patients.
Although much is known about how hospitals can minimize the spread of infection, research is still needed to fill some important gaps in knowledge. One need is for development of rapid, reliable diagnostic methods for identifying the presence of infection, the specific infecting organism, and the susceptibility of the microbe to various therapeutic agents. Diagnostic precision is the key to effectively modifying the current approach of widespread empiric antimicrobial use in ill patients with suspected infections. A further need is to develop materials for use in medical devices, such as catheters, that are resistant to colonization by microorganisms. In addition, continuing development of new antimicrobial agents remains a priority.
Another factor that is widely believed to contribute to resistance problems is the use of various antimicrobial agents in animals raised commercially for food, such as poultry, pigs, and cows. Participants debated just what contribution such agricultural use makes to the spread of antimicrobial resistance among human pathogens. While some participants maintained that the problem is minimal and being effectively managed by various public and private programs, others described a greater level of risk. They expressed concern that use of antimicrobials in animals, either for
therapeutic use or to promote growth, can lead to the development of drug-resistant microbes (largely bacteria, such as salmonella and campylobacter) that subsequently are transmitted to humans, usually through food products.
In response to the workshop presentation, “The Use of Antimicrobials in Food-Producing Animals,” a paper was prepared to address the public health consequences of antimicrobials in agriculture and can be found in Appendix A.
ANTIBIOTIC USE AND RESISTANCE IN DEVELOPING COUNTRIES
Iruka N. Okeke, Ph.D.
Department of Biology, Haverford College, Haverford, PA
“The ways and means for putting medicine in order must take account of the conditions of life and work among the people whom it must serve.” Walton H. Hamilton, 1932
Antimicrobial resistance adversely affects the outcome of community-and hospital-acquired infections in developing countries. For example, mortality in recent cholera and dysentery epidemics has been significantly increased by antibiotic resistance (Goma Epidemiology Group, 1995; Sengupta et al., 2000; Okeke et al., 2001). Other cases in point include tuberculosis, respiratory tract infections, infectious diarrhea, sexually transmitted diseases, and malaria. These conditions account for most of the illness in the developing world. In these countries, the infectious disease burden is typically high, whereas the options available to prescribers are few—often limited to older, cheaper, and non-patent protected drugs. Studies that have monitored resistance rates over time have documented a rising prevalence of resistance to these commonly used antimicrobials (see Figure 5-1) (Hoge et al., 1998; Okeke et al., 2000; Hsueh et al., 2002). Drugs that have been rendered ineffective or for which there are serious concerns include the broad-spectrum antibacterials tetracycline, ampicillin, trimethoprim-sulfamethoxazole chloramphenicol and streptomycin, anti-tuberculosis drugs as well as the antimalarial chloroquine. Resistance to these drugs has promoted an upsurge in the use of previously second-line, more expensive agents that are, in many cases, agents of last resort. The fluoroquinolones and sulfadoxine-pyrimethamine are two such examples, and with both, an upward trend in the proportion of resistant strains has already been identified (Okeke et al., 2000; Winstanley, 2001; Mwansa et al., 2002). Although there are other agents, currently in routine use in
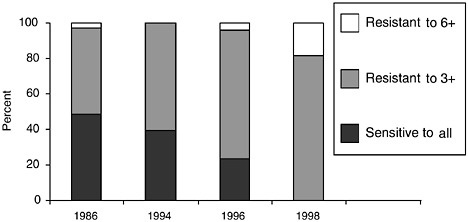
FIGURE 5-1 Trends in the proportion of Escherichia coli from healthy subjects resistant to three or more and six or more of seven antibacterial drugs. SOURCE: Okeke et al., 2000.
industrialized countries, the cost of these precludes their use by poor patients in the developing world. The extent and determinants of microbial resistance vary considerably from one geographic area to another but the current globalization trend means that the consequences transcend geographical borders (Okeke and Edelman, 2001). In some developing countries, unprescribed antibiotic use is relatively uncommon so that antibiotic use and resistance patterns may mirror what is seen in the industrialized world (O’Connor et al., 2001). In others, regulations that would encourage appropriate antibiotic use are in place but the infrastructure or the will to enforce them is not (Djimde et al., 1998; Chuc and Tomson, 1999; Okeke et al., 1999; Chatterjee, 2001; Siringi, 2001). Although there are many generalizations in this report, it must be emphasized that it is impossible to paint a picture of the current situation or draw a model for intervention that would fit every developing country. Examples are taken from different countries, but the principal focus here is on sub-Saharan Africa where the burden of infectious disease is highest and antibiotic use is commonly under-regulated (Djimde et al., 1998; Siringi, 2001).
Emergence of Resistance
Studies conducted in industrialized countries have correlated antibiotic consumption with the prevalence of antibiotic resistance. Per capita expenditure on antibiotics is lower in developing countries in spite of a greater burden of infectious disease, and microbial resistance is often highly prevalent. Some of the reasons for this are that cheaper agents are used, agricul
tural and veterinary consumption is often lower, and alternative (or no) therapy is common. However, a significant reason for high selection pressure in the face of modest antimicrobial expenditure is inappropriate antibiotic use.
Antibiotic Prescription by Health Professionals
Some of the types of antibiotic misuse in clinical practice include unjustified prescription (in such conditions as diarrhea and the common cold), under-prescription (for example, in urinary tract infections and sexually transmitted diseases), under-dosing, and short duration (Calva, 1996; Nizami et al., 1996; Paredes et al., 1996; Bartoloni et al., 1998). Antimicrobial prescription in many developing countries is almost entirely empirical and based on surveillance data obtained from locations or at a time that it is unlikely to be relevant to the ensuing situation. Broad-spectrum agents are frequently employed because susceptibility data is unavailable. In addition, the rising number of HIV-positive people increases selective pressure for resistant organisms by increasing the need for prophylactic and curative antimicrobial use.
As in industrialized countries, prescribers are subjected to pressure from patients (Paredes et al., 1996). In addition, health professionals rarely have the opportunity to review cases and are often dealing with life-threatening disease. Hence, antibiotics are often prescribed when unnecessary. Advocates of appropriate antibiotic use advise the prescriber to weigh the benefits to the individual against the risk to public health. This presents a dilemma even to those health professionals that are aware of the long-term consequences of antibiotic abuse. This is because many of the benefits to the individual actually impact public health. For example, the untreated, or improperly treated, but surviving, patient serves as a reservoir of resistant pathogens. Secondly, treatment failures in health centers will lead to lowered confidence by patients and consequent upsurge of visits to unorthodox practitioners, encouraging unsanctioned antibiotic distribution. Since health professionals frequently have only one opportunity to administer therapy, there is the inclination to use broad-spectrum therapy to increase the chances of successful treatment. These factors serve to dissuade health professionals who are aware of the consequences of inappropriate antimicrobial use from putting their knowledge into practice (Larsson et al., 2000). The dilemmas faced by prescribers are further complicated by the practices of patients in developing countries, who are more likely to fail to complete a prescribed course of antibiotics or to admit to reserving part of it for future use (Calva, 1996; Pechere, 2001).
Multiplicity of Sources
Patients in many developing countries will often seek care for the same ailment from multiple sources, a practice that prevents follow-up and confuses case history (Needham et al., 2001). This is a function of the wide variety of sources for antimicrobial drugs and the fact that many of these sources will dispense antibiotics without prescription (Chuc and Tomson, 1999; Wachter et al., 1999). Djimde et al. classified the sources of antimalarials in Malian villages as including sanctioned (physicians, pharmacists, nurses, pharmacy sellers, and midwives) and unsanctioned (stall keepers, itinerant vendors, and tradesmen dealing in clothing, confectionary, cosmetics, and motorcycle parts) (Djimde et al., 1998). The situation is similar in many other developing countries, and pharmacy premises, although sanctioned, often serve as an outlet for unprescribed antibiotics because of the competitive pressure from unsanctioned providers (Chuc and Tomson, 1999; Okeke et al., 1999). Unsanctioned providers tend to have shabbier premises and a smaller range of medicines but they flourish because they are often cheaper due to lower overheads. They are more accessible to the majority of the population than doctors and nurses and will accept a non-physiologic cause of disease. Unfortunately, they may supply poor quality medicines (but these are often dispensed by sanctioned providers) and could serve as an outlet for illicitly sourced drugs. As they often lack basic training on drug handling, they are often unaware or incapable of storing their wares appropriately. They have been known to ignore or are unaware of expiry dates and to mix batches, brands, and even different drugs. They also have limited (if any) clinical training and therefore offer diagnosis and prescription that may be incorrect (Wachter et al., 1999). Antibiotic choice is based on experience, folklore, or customer preference usually in complete disregard of the long-term consequences of antibiotic misuse. These providers supply antimicrobials to a varied but significant proportion of the populaces they serve. They are therefore a crucial target group for optimizing antibiotic use. Antibiotic policies directed at medical services alone will only affect a minority of treatments when unsanctioned persons are major providers. It is however difficult to integrate unsanctioned providers into official policies because they are often technically illegal.
Another category of health providers that must be taken into account is the traditional medicine practitioners. In a Malian study 23 percent of rural antimalarial consumers preferred herbs or traditional medicines (Djimde et al., 1998). Indeed, many herbal remedies have demonstrated some antimicrobial activity in vitro, and traditional medicine represents a potential alternative to antibiotic therapy, which could reduce selective pressure to orthodox antibiotics. To date, very few of these natural products have been
subjected to scientific or clinical evaluation. The majority remain unevaluated and recipes are often held as family secrets akin to a trade secret (Sofowora, 1982). Traditional practitioners receive years or decades of apprenticeship in traditional medicine and herbs but have no training in Western clinical methods. Importantly, one traditional practitioner recently admitted adulterating his concoctions with antibiotics, and the extent to which this practice occurs is not known (Okeke et al., 1999). If traditional practitioners are using Western medicines, there is a need to ensure that they receive appropriate training in diagnosis, treatment, and undesirable effects, including antibiotic resistance.
In some developing countries, patients prefer to seek care from sanctioned providers, even though it is available from other sources (O’Connor et al., 2001). In many other countries, unsanctioned and traditional providers are more commonly frequented by the unwell. We have sought to identify reasons why patients seek care from unorthodox sources. In a study designed to determine the health-seeking practices of educated Nigerians, a cohort of university undergraduates was followed for one year. The students were all entitled to free medical care provided by physicians at the University Health Center and drug supply from an attached pharmacy. Within the year, of 43 students who had diarrhea, only 16 percent sought treatment at the health center. Twelve percent did not seek treatment at all but 72 percent resorted to self-medication, at their own expense, even though they could obtain medical care at no cost. Furthermore, 80 percent of the self-medicators took at least one antibacterial medicine and 45 percent took more than one antimicrobial (see Table 5-1). Clearly, factors other than cost and health care availability influence antibiotic misuse. Another relatively affluent population we studied were West Africans resident in Nigeria that had traveled by air to another country. Most of the travelers had visited Europe or North America. Of the 424 travelers to
TABLE 5-1 Use of Unprescribed Antibiotics by Students with Diarrhea
|
Antibiotic or combination |
No. (%) of self-medicated cases |
|
Tetracycline alone |
7 (22.6) |
|
Metronidazole alone |
7 (22.6) |
|
Pthalyl sulphathiazole alone |
3 (9.7) |
|
Tetracycline + Metronidazole |
10 (32.3) |
|
Tetracycline + Pthalyl sulphathiazole |
3 (9.7) |
|
Tetracycline + Metronidazole + Pthalyl sulphathiazole |
1 (3.2) |
|
Total taking at least one unprescribed antibiotic |
25 (80.6) |
|
Loperamide |
1 (3.2) |
|
Herbals |
3 (9.7) |
whom a questionnaire was administered, 52.4 percent traveled with at least one antimalarial and 30.4 percent with at least one antibacterial drug. Only 19.8 percent said that they would visit a doctor or clinic if they fell ill during their travels. The rest preferred to take medicines they had brought with them or obtain medicines from friends (Okeke et al., in press). These findings appear to suggest that the reasons why antibiotics are abused in sub-Saharan Africa are not entirely economic. Working in Zambia, Needham et al. (2001) have identified barriers to tuberculosis diagnosis, which give some insight of factors that lead patients to self-medicate or obtain treatment from unorthodox sources. Significant factors they identified included female sex (p < 0.02) and education (p < 0.04), but not economic or health factors. There was considerable delay in diagnosis if a patient made prior health seeking encounters, particularly to unsanctioned and traditional providers (p < 0.001).
Sub-Standard Medicines
Even when antibiotic prescription and use is optimal, sub-therapeutic dosing and consequent resistant selection can arise from poor quality antibiotic preparations. A recent survey of tablets claiming to contain the antimalarial Artesunate from Cambodia, Laos, Myanmar, Thailand, and Vietnam found that as many as 38 percent of the samples did not contain the drug (Newton et al., 2001). Multiple reports have described the dispensing of medicines in Nigeria that contain as little as half of their label content (Okeke and Lamikanra, 1995, 2001; Taylor et al., 2001). Some of the medicines are counterfeit—they were intentionally formulated with less than the stated content (Chatterjee, 2001; Newton et al., 2001), but significant proportions contain degraded drugs (Okeke and Lamikanra, 1995, 2001). Degradation of heat- and moisture-labile antibiotics occurs very readily in tropical developing countries where ambient temperatures may approach 40°C and humidity is high enough to distort capsule shells and soften tablets. The packaging of many pharmaceuticals may be insufficient to protect them in tropical developing countries, and in some cases it may be desirable to reformulate them for this environment or modify shelf life recommendations. One rationale for employing uniform shelf lives in temperate and tropical countries is that labels indicate that medicines are to be stored under controlled conditions. Indeed, local regulations usually stipulate that pharmacy premises in the tropics must be air-conditioned. In reality, frequent power cuts may mean that the air is only intermittently conditioned, warehouses and unsanctioned premises are almost never air-conditioned, and imported drugs may languish for many months at ports.
Dissemination
The warm moist climate and close proximity of non-human vectors in tropical countries increase the likelihood that pathogenic and commensal bacteria will survive in the environment and be transmitted to humans (Rosas et al., 1997). In many developing countries, these factors combine with poor sanitation and shortfalls in infection control to create havens for the amplification and dissemination of resistant strains in the community (Graczyk et al., 2001). Overcrowding, a direct consequence of urban migration, increases the chance that this dissemination will occur. The world’s fastest-growing cities are in developing countries, many of which cannot provide potable water or safe sanitation for a majority of their residents (McMichael, 2000). Antibiotic misuse also tends to be more common in crowded areas and may be a feature of urban social change (Bojalil and Calva, 1994; Chuc and Tomson, 1999). Separate studies have suggested that cities serve as havens for the exchange of pathogenic and antibiotic-resistant organisms. In contrast to a Dutch study, which found that there was very little difference in the carriage of E. coli resistant to antibiotics in a rural and an urban area (Bonten et al., 1992), studies in Nigeria and Nepal have demonstrated that urban residents are more likely to harbor resistant bacteria than people residing in rural or provincial areas (Lamikanra and Okeke, 1997; Walson et al., 2001).
The capacity of laboratories in developing countries to conduct susceptibility testing and to diagnose infections needs to be strengthened. Not only is resistance surveillance insufficient or lacking, the ability to diagnose many infections and thereby prescribe appropriate and timely treatment is hampered by inadequate laboratory support. In many localities, the extent of the antibiotic resistance problem is not known and empirical antibiotic prescription is akin to guesswork. Similarly, evidence about resistance is of necessity commonly anecdotal. Even if interceptive strategies to control resistance are implemented, there are no local means of measuring the success or otherwise of such policies.
Conclusion
This report attempts to highlight a number of factors that predispose the emergence and spread of antibiotic resistant organisms in developing countries. Implementation of the World Health Organization’s (WHO) Global Strategy for Containment of Antimicrobial Resistance will potentially address all of these issues (WHO, 2001). Priority should be given to education, directed at distributors and consumers as well as prescribers of antibiotics, infection control to prevent the dissemination of resistant strains, quality assurance of antibiotics and other medicines, and the insti
tution of functional and sustainable laboratories for antibiotic resistance surveillance. The real challenge however will be implementing this strategy on a country- and sub-country-specific basis, taking the special features of each developing country into account to ensure sustainability. For example, in some countries, targeting educational intervention at physicians may reduce inappropriate use (O’Connor et al., 2001). In particular, it would be desirable to present incentives for prudent antibiotic use in order to address the gaps between knowledge and practice seen in health professionals and lay-people. In other areas, the approach must be different because of the extensive prescription of antibiotics by unsanctioned providers and patients themselves; antibiotic policies that target orthodox clinical practitioners and premises will have only limited impact. In these cases, policies and interventions that reach unconventional distributors and the patients themselves are more likely to have a broad and sustained effect. Most importantly, interventions will have to be tailored to specific countries and communities since the factors that determine their success will be to a large extent cultural.
HEALTHCARE-ACQUIRED INFECTIONS: HOSPITALS AS A BREEDING GROUND FOR ANTIMICROBIAL RESISTANCE
Lindsay E. Nicolle, M.D., F.R.C.P.C.
Department of Internal Medicine and Medical Microbiology University of Manitoba, Winnipeg, Manitoba, Canada
Hospitalized populations are more likely to be colonized or infected with resistant microorganisms compared with community populations (Datta, 1969; McGowan et al., 1974). This association of acute care hospitalization with antimicrobial resistance was recognized soon after the introduction of antimicrobial therapy (McGowan et al., 1975). Widespread outbreaks of penicillin-resistant Staphylococcus aureus in the late 1950s reinforced this observation (LaForce, 1993). Repeatedly, review articles from 20–30 years ago identified the problem and the association of resistance with widespread empiric antimicrobial use (Jackson, 1979; Weinstein and Kabins, 1981; McGowan, 1983).
While antimicrobial resistance is more frequent in acute care hospitals, the prevalence of resistance across hospitals is highly variable. Some of this variability mirrors geographic variation in prevalence of resistant organisms. Large hospitals providing tertiary care and teaching hospitals have a higher prevalence of resistance than smaller community hospitals and have repeatedly been the site where new resistance is first described. This is the experience of methicillin-resistant Staphylococcus aureus (MRSA) emer
gence in U.S. hospitals (Haley et al., 1982), and was repeated in the 1990s with the emergence of vancomycin resistant enterococci (VRE) (Fridkin et al., 2001).
Determinants of Resistance
The high prevalence of antimicrobial resistance in acute care facilities, and repeated emergence of new resistance, is attributable to both patient and facility characteristics (see Table 5-2). Persons at highest risk of acquiring infection are found in hospitals. These include patients at extremes of age with biologically impaired immune systems, such as premature neonates and the very old. Other patients have acquired immunodeficiency, which is often therapeutically induced. These include the increasing numbers of solid organ and bone marrow transplant patients and profoundly neutropenic patients, as well as patients with severe trauma or extensive burns. These highest risk patients are primarily cared for in large, tertiary care, teaching hospitals. Hospitalized patients experience repeated interventions for monitoring or therapy which further impair normal host defenses and increase the risk of infection. Indwelling urethral catheters, central vascular lines, endotracheal tubes, and surgical wounds permit access of microorganisms to normally sterile body sites. Recent evolution in health care delivery with shortened hospital stay and increased patient acuity means patients now hospitalized are at even greater risk for infection.
TABLE 5-2 Variables Which Promote the Emergence and High Prevalence of Resistant Organisms in Acute Care Facilities
|
Patient variables |
Inherent immunocompromised status e.g., neonate, very old Acquired immunocompromised status e.g., transplant patients, profound neutropenia, extensive burns Therapeutic interventions which compromise normal defenses e.g., indwelling urethral catheters, central lines, endotracheal tubes, surgical procedures |
|
Intense antimicrobial use |
Systemic: 30–50% of patients • Therapeutic • Prophylactic Topical use |
|
Institutionalization |
Increased opportunities for transmission • Shared equipment • Shared staff • Airborne |
Intense antimicrobial use in acute care facilities ensures that infections, when they occur, are likely to be with an organism of increased resistance. From 30 to 50 percent or more of patients admitted to an acute care facility receive prophylactic or therapeutic systemic antimicrobials. In very high risk populations, such as intensive care unit patients or bone marrow or solid organ transplant units, virtually all patients receive antimicrobial therapy which is usually broad-spectrum and often more than one agent. There is also substantial topical antimicrobial use for burns and other skin lesions, although use of topical agents is not well described. The intensity of antimicrobial use has been repeatedly correlated with the emergence and prevalence of antimicrobial resistant organisms in the individual patient, and within the hospital unit or facility as a whole (McGowan, 1983; Fridkin et al., 2001).
Institutionalization increases the frequency of transmission of organisms among patients through a shared environment, equipment, and staff. Transmission may be airborne, as in the case of multiply drug resistant tuberculosis, from a point source such as contaminated equipment, or by direct or indirect contact through a contaminated environment or on the hands of staff. The likelihood of a patient acquiring a resistant organism correlates with the prevalence of resistant organisms in other patients in the unit or facility (Bonten et al., 1998). The frequency of antimicrobial resistance is highest in special care units such as intensive care units, burn units, or transplant units where severely ill patients, multiple invasive devices, intense antimicrobial use, and close spatial clustering combine.
Acquisition of Antimicrobial Resistance
An antimicrobial resistant organism may be acquired by emergence of resistance in endogenous flora, or by acquisition from other patients and the environment. Emergence from endogenous flora has been frequently reported among gram-negative organisms with inducible beta-lactamases and in Pseudomonas aeruginosa. A recent important example is the emergence of glycopeptide intermediate MRSA (GISA). These strains have usually developed in patients with persistent or relapsing MRSA infection associated with foreign bodies such as hemodialysis catheters which have not been removed, and after prolonged vancomycin therapy.
An organism may be transmitted from another patient in an outbreak setting where an increased number of cases is observed, or as endemic transmission where a continuing, stable, number of cases occur. A patient may also acquire a resistant organism, such as an aminoglycoside resistant S. marcescens, and the genetic resistance elements may be transferred to other colonizing flora resulting in resistance in other species such as K. pneumoniae or E. coli (McGowan, 1983; Alford and Hall, 1987).
There is overlap between these two types of acquisition. Once a patient develops endogenous resistance, the strain may be transmissible to other patients, leading to an outbreak or endemic colonization or infection with the resistant organism. Organisms which may initially cause outbreaks, such as MRSA and VRE, may subsequently become endemic in the facility.
Impact of Antimicrobial Resistance
Studies repeatedly report that acquisition of an antimicrobial resistant infection is associated with negative outcomes for the patient and the facility (Holmberg et al., 1987). These include increased mortality, increased morbidity, increased length of stay, and increased costs due, at least partly, to the need for more costly alternative antimicrobial therapy and infection control interventions.
While the conclusion that antimicrobial resistance in acute care facilities has negative impacts is valid, there are some methodologic concerns with studies measuring outcomes. Antimicrobial resistant organisms are not usually of greater virulence, so increased morbidity or mortality will result only if initial antimicrobial therapy not effective for the infecting organism is given. Where empiric therapy is effective for the resistant organism, excess morbidity or mortality would not occur. This concern certainly drives increasing use of broader spectrum empiric antimicrobial therapy, which is costly, but this practice also means that morbidity and mortality due to resistant organisms in acute care facilities in developed countries remains limited.
Patient colonization or infection with a resistant organism is not random. Patients from whom resistant organisms are isolated are characterized by a greater risk of infection due to underlying disease and immunosuppression, have received more antimicrobial therapy, and have longer hospital stays because of their illness or complications of therapy. These same characteristics identify patients with a greater likelihood of mortality, morbidity, prolonged length of stay, and cost of hospitalization irrespective of the presence of an antimicrobial resistant organism. Thus, there are substantial potential biases in any study of outcomes attributable to antimicrobial resistance. This partially explains the wide variation in impacts of resistant organisms reported in different studies. For case-control studies, differences in outcomes between patients with and without infections with antimicrobial resistant organisms become less marked as matching of case and control patients becomes more rigorous (Howard et al., 2001).
The major negative impact of antimicrobial resistance is, in fact, only a potential risk. With increasing acquisition of resistance, an organism not susceptible to any available antimicrobial therapy will evolve. This is of greatest concern for common, virulent, organisms such as S. aureus and E.
coli, which are important bacterial pathogens in both hospitals and the community. The likelihood, time course, and costs of such a development cannot currently be estimated.
Containment of Antimicrobial Resistance
Concerns about antimicrobial resistance have been repeatedly raised over many decades, and recommendations to limit progression have been made (McGowan, 1983; Goldman et al., 1996; Schlaes et al., 1997). The two major interventions are infection control to prevent transmission, and limitation of antimicrobial use. A recent consensus statement notes that all previous efforts have failed, and views this as a failure of leadership by both administration and medical staff who have not taken ownership of the problem (Goldman et al., 1996).
Infection Control
Infection control programs are effective in preventing hospital infections (Scheckler et al., 1998). These programs are essential for safe patient care and risk management in acute care facilities, regardless of the presence of antimicrobial resistance. Important activities include surveillance, outbreak investigation and control, patient care practices such as isolation, handwashing and barriers, and sterilization and disinfection of equipment. Hospital infection control activity should also decrease antimicrobial resistant infections and colonization.
Perhaps the evidence most strongly supporting efficacy of infection control in controlling antimicrobial resistance is found in reports of control of outbreaks of antimicrobial resistant strains. Over 200 such outbreaks have been reported since 1970 (Nicolle, 2001). The organisms most frequently described are MRSA, aminoglycoside resistant or extended spectrum beta-lactamase (ESBL) producing enterobacteriaceae, VRE, and Acinetobacter spp. Outbreak investigation and control was reported to eradicate or control infections and colonization with the outbreak strain in 80 to 90 percent of episodes. A common theme, however, is that initial infection control interventions of education, intensified handwashing, and barrier precautions did not achieve control. Further measures such as cohorting, closing units to new admissions, antiseptic handwashing, and either antimicrobial restriction or specific intensified antimicrobial use were required to achieve control.
While this experience is compelling evidence for the effectiveness of infection control, there are limitations to acknowledge. A substantial publication bias is likely, as reports describing a successful outcome will more often be submitted for publication. The majority of reports originate from
academic tertiary care centers, where there may be increased resources and expertise for infection control. The durability of a successful outcome is usually not known. Many facilities may have initial success with eradicating MRSA and VRE, but subsequently have re-emergence with endemic transmission established. Studies are also noncomparative, and describe multiple interventions. Thus, the effectiveness of a specific intervention cannot be evaluated. A final observation is that the antimicrobial resistant phenotype is a unique marker for organism identification which facilitates early outbreak recognition. Seen from this perspective, antimicrobial resistance may make infection control interventions more effective.
The efficacy of infection control interventions in limiting endemic antimicrobial resistance is less clear. The most convincing reports supporting efficacy are from Europe, where some facilities have only recently changed practice from a hygienic model of infection control to one based on infection surveillance. When multifaceted control programs including screening, staff education, intensified barrier precautions, and intensified handwashing have been newly implemented in intensive care units with a high prevalence of resistance, decreased prevalence and incidence of infection and colonization with MRSA and ESBL producing organisms has been reported (Cosseron-Zerbib et al., 1998; Harbath et al., 2000; Souwein et al., 2000). These approaches, however, have been standard practice for most North American facilities. An increasing prevalence of MRSA and VRE has been observed despite appropriate continuing infection control practice (Goetz and Muder, 1992; Brooks et al., 1998). Infection control interventions may have delayed and limited resistance expansion, but cannot prevent establishment or progression altogether.
Another element of infection control practice is antimicrobial use to prevent infection. There is a trade-off, however, between prevention of infection, and the induction of even more antimicrobial resistance, especially among colonizing organisms (Flynn et al., 1987; Terpstra et al., 1999). This trade off is usually considered acceptable where valid clinical trials have documented improved patient outcomes. This is the case for appropriate prophylactic antimicrobial use for selected clean and clean-contaminated surgical procedures. More problematic is the widespread use of topical mupirocin for eradication of MRSA colonization. Widespread mupirocin use for preventing MRSA colonization has repeatedly been followed by emergence of mupirocin-resistant MRSA strains (Miller et al., 1996). Use of prophylactic antimicrobials, even when appropriate, contributes to the larger problem of antimicrobial resistant organisms within acute care facilities.
Finally, despite development of multifaceted national guidelines for control of selected high profile resistant organisms, the prevalence of these antimicrobial resistant organisms has continued to increase. The ongoing
MRSA outbreak in Britain (Austin and Anderson, 1999) and the continuing spread of VRE in the United States (CDC, 1999) are examples. While incomplete application of national recommendations at the institutional level may explain this failure, it must be appreciated that there are limitations in what infection control interventions, by themselves, may achieve in limiting emergence and dissemination of important resistant organisms in acute care facilities.
Antimicrobial Use Strategies
Throughout the United States in the 1970s and early 1980s tertiary care institutions repeatedly reported large, continuing outbreaks with aminoglycoside resistant gram-negative organisms (McGowan, 1983; Alford and Hall, 1987). Enterobacteriaceae and Pseudomonas aeruginosa were the most common organisms, and burn units were often identified as the source. Intensification of infection control measures had partial success in controlling this resistance in some facilities, but other institutions reported no improvement despite repeated and varied interventions (Alford and Hall, 1987). From the mid-1980s, however, these organisms were no longer identified as a significant problem in acute care facilities. This apparent spontaneous disappearance of widespread, important resistance likely resulted from changes in antimicrobial use with introduction of alternate gram-negative agents, and burn wound management with more rapid covering of the burn wound surface. Most important, however, was likely discontinuing the widespread use of topical aminoglycosides for burn wound prophylaxis. This is an example of how modifications in antimicrobial use may be a powerful determinant in limiting even widespread resistance.
Several activities to optimize antimicrobial use have been suggested (see Table 5-3) (Marr et al., 1988; Goldman et al., 1996; Schlaes et al., 1997). Despite the prominence of the concerns with antimicrobial resistance and continuing attention to this issue, there is limited systematic comparative evaluation of the efficacy of the proposed interventions. Educational strategies have, in fact, repeatedly been shown to have little long-term impact. Even optimal antimicrobial use in an acute care facility may not limit antimicrobial resistance given the large numbers of patients, especially in high risk units, who require antimicrobial therapy for legitimate clinical indications. The continuing approach to management of antimicrobial resistant organisms within acute care facilities is, in fact, ever-intensified use of broad-spectrum antimicrobials to “cover” ever-expanding antimicrobial resistance.
One study relevant to antimicrobial use and restriction described an outbreak of Klebsiella aerogenes in a neurosurgical unit in Britain from
TABLE 5-3 Recommendations Suggested for Optimizing Antimicrobial Use in Acute Care Facilities
|
• restrictive formulary • automatic stop orders • automatic substitution • guidelines for antimicrobial use • optimal surgical prophylaxis • education • academic detailing • required consultation/approval • antimicrobial resistance reports |
1966 to 1968 (Price and Sleigh, 1970). Patients on this unit routinely received prophylactic cloxacillin for a continuing outbreak of penicillin-resistant S. aureus, and prophylactic ampicillin to prevent meningitis with cerebrospinal fluid leaks. Widespread colonization and infection with K. aerogenes emerged, including uniformly fatal cases of meningitis. The initial response to controlling this outbreak was intensification of infection control interventions including cohorting or placing patients in private rooms, and high dose colistin therapy to prevent and eradicate colonization. These strategies had minimal impact, and deaths from K. aerogenes meningitis continued. The draconian intervention of removal of all antimicrobial agents for either prophylaxis or therapy was then undertaken. There was a prompt and sustained disappearance of the outbreak strain, and during the subsequent four months while no antimicrobials were used there were no further cases of meningitis. Complete withdrawal of antimicrobial therapy is, of course, an intervention of the last resort and not an option which could currently be entertained for most acute care units. However, this study is intriguing in suggesting aggressive antimicrobial control may have profound and unpredicted impacts.
Research Needs
Antimicrobial resistance in acute care facilities is a large and complex issue. Despite identification of this problem immediately after antimicrobial use became widespread, and continuous attention, the problem is greater today than ever. This is, in part, the price for the remarkable advances in antimicrobial agents, which have allowed prevention and treatment of infections in highly compromised patients, leading to even more vulnerable populations. To address the problem now, interventions known to be effec
tive must be rigorously applied, and continuing, targeted, systematic evaluation of potential effective interventions must be pursued. Some issues for further research and evaluation have been identified in the previous discussion of infection control and antimicrobial use. There are several other approaches that require intensive study.
Knowledge of the basic science of nosocomial transmission and pathogens is incomplete. Some strains of MRSA disseminate widely and rapidly, whereas other strains in the same environment are not transmitted among patients. Organism characteristics determining transmission in a facility are not known. The “big four” nosocomial infections of urinary tract, surgical site, ventilator-associated pneumonia, and central line are all primarily associated with foreign materials. A more complete understanding of interactions between the organism, the device, and the host will be essential to understand these infections, and associated resistance development.
Another need is development of rapid, reliable diagnosis to identify the presence of infection, the specific infecting organism, and antimicrobial susceptibilities. Diagnostic precision is the key to effectively modifying the current approach of widespread empiric antimicrobial use in ill patients with suspected infections. Without this improved diagnostic capability, it is not realistic to expect to modify current antimicrobial practices. A further need is development of materials resistant to colonization by organisms to limit infection and colonization with antimicrobial resistant organisms on medical devices. Given the prominent role of these devices in nosocomial infection, technological development of medical devices resistant to colonization by microorganisms is a priority.
Comprehensive strategies addressing the problem of antimicrobial resistance consistently identify a need for continuing development of antimicrobials as a priority. New antimicrobials will certainly be needed for patients in acute care facilities, where new resistance is always most likely to emerge. Development of additional antimicrobials, however, is unlikely to alter the paradigm of antimicrobial resistance in acute care facilities. This will remain a spiral of ever increasing resistance and empiric antimicrobial use until alternative effective approaches to prevention and management of nosocomial infections are developed.
THE USE OF ANTIMICROBIALS IN FOOD-PRODUCING ANIMALS
Thomas R. Shryock, Ph.D.
Elanco Animal Health, Greenfield, IN
The ultimate goal of food animal production is to deliver a safe, affordable, nutritious high-quality food product to the consumer. In the United
States in 2000, the food animal population totals were 8.4 billion chickens, 97 million cattle, and 98 million pigs. In order to raise this quantity of animals in today’s commercial livestock and poultry operations, efficiencies of scale include grouping hundreds to tens of thousands of animals together on a single farm. This necessitates the application of herd health measures, applied on a population basis, to maintain a high level of herd (or flock) health status, since an epidemic disease outbreak would decimate the population. Measures such as vaccination, limited commingling, adequate ventilation and temperature controls for minimizing environmental extremes, biosecurity, appropriate nutrition and housing, and producer quality assurance programs and practices are currently used in modern agriculture. However, these measures are not always sufficient to prevent or control disease. The use of antimicrobial agents as a strategic tool to maintain animal health remains an essential component of today’s food animal production system.
Antimicrobial agents are used in food animal production to prevent disease in high-risk animals and to control or treat disease; or to improve the ability of the animal to convert feed to muscle. Unlike the situation in human medicine where individual patients can be treated, food animal medicine is often practiced on a population basis for reasons of animal welfare, logistics, and efficiency since it is impractical to individually treat each animal in a group that consists of hundreds to tens of thousands. Herd health medicine also relies heavily on preventive medicine strategies to control or prevent disease in high risk populations. Addition of antimicrobial agents to feedstuffs, or by water, or parenteral administration to groups of animals by injection to prevent or control disease progression is done strategically when certain criteria are met. These criteria include prior experience of a disease outbreak associated with animal movement or weather extremes, or a noticeable increase in clinical signs of disease in a few animals in the group. This early therapeutic administration to the entire group is warranted, since many animals will have been exposed to the index cases and are now “incubating” the pathogens. Left untreated, as time elapses, more animals will “break” with clinical signs. Strategic application of an antimicrobial agent at the right time can minimize the pathogen load within a sufficient number of animals in the group (by allowing the host immune defenses to control the infection) and ultimately restore the group to an acceptable health status. Thus, preventive medicine, as a part of a herd health program, is in some cases the best way to maintain healthy animals. It is not appropriate to allow the majority of animals to suffer or die unnecessarily before beginning treatment (which is likely to fail at that late stage of the disease course). Many critics of this well-established practice incorrectly refer to the administration of “subtherapeutic” doses of antimicrobial agents in this instance, when in fact, the doses were developed to be
therapeutic for those animals exhibiting signs of disease and are sufficient to benefit those animals that are incubating the pathogen and would soon break with disease. Routine administration of antimicrobials to healthy animals, with the intention of doing so as “insurance” or to “cover” poor management or hygiene is not a practice used by the leading production companies because it would be expensive, unsuccessful, and an unsustainable method of animal production. The administration of antimicrobials to enhance performance or growth of the animals may reflect the intention of the producer, but frequently the antimicrobial agents are in reality controlling an unrecognized subclinical disease exposure in the animals.
With respect to specific animal species, the use of antimicrobial agents is quite diverse (GAO, 1999; NRC, 1999; Prescott et al., 2000; Muirhead, 2001). Most poultry production requires the use of ionophores to prevent coccidia (intestinal parasites) infections, which otherwise would devastate a flock. Some antibiotics are administered at hatching, to reduce the prevalence and/or severity of infections that occur in day-old chicks due to vaccination stress on the immature immune system. In poultry house situations, rapid onset of respiratory or enteric diseases requires that antimicrobial agents be administered at the earliest opportunity to prevent significant morbidity and mortality in the flock. For the most part, poultry are medicated via feed or water because it would be impractical to individually treat thousands or tens of thousands of birds. Swine production can be divided into several stages from gestation, to farrowing, to nursery, to grower and finisher. Each stage has its own unique needs for antimicrobial usage, but in particular respiratory disease and enteric disease can frequently spread rapidly throughout a herd and require antimicrobial intervention. Thus strategically timed oral medications in groups of high risk pigs to prevent disease at times of movement, high stress, or waning maternal antibody may be needed. Injectable products are used when needed for therapy to individual sick sentinel pigs of the herd, that is, those showing the most and earliest clinical signs. Beef cattle that are affected by respiratory disease are usually treated with injectable antibiotics. Liver abscesses, coccidiosis and metabolic diseases are also common in feedlot cattle and are prevented or controlled by administration of antimicrobial agents in feed (Nagaraja et al., 1996; McGuffey et al., 2001; Muirhead, 2001). Infections in dairy cattle are usually cases of mastitis which are treated in acute cases or at “dry off” by intramammary infusion of antimicrobial agents. The use of antimicrobial agents in aquaculture is minimal (only tetracycline and a sulfa are approved), with applications done only in certain situations via medicated feed.
The antimicrobial agents that are used in food animal production are similar to those used in human medicine, but with several key exceptions (GAO, 1999). The Food and Drug Administration (FDA) or their equiva
lent in other countries has approved all of these products for use after a thorough review of the drug manufacturers’ data that demonstrate efficacy, safety, and quality of the medicinal product. The common classes of antibiotics used in both humans and animals are: beta-lactams (including cephalosporins), tetracyclines, macrolides, aminoglycosides, lincosamides, sulfonamides, streptogramins, and fluoroquinolones. Examples of compounds not used (or minimally used) in humans, but important in food animals include: ionophores, avilamycin, bacitracin, carbadox, flavomycin, and pleuormutilins. It should be noted that some antimicrobial agents such as chloramphenicol and vancomycin are banned from use in food animals in the United States and other countries (Payne et al., 1999). Some of the antimicrobial agents used in food animals are approved for delivery by both a parenteral and an oral route, but in many cases only a feed administration route is approved and/or feasible for a variety of reasons. A detailed compendium of the technical aspects of feed additives is available (Muirhead, 2001). The actual amount of antimicrobials distributed by manufacturers in the U.S. animal sector has been reported (but doesn’t include the amount of generic products distributed) (Muirhead, 2002). Of the total amount of 10,936 tons of active antimicrobials reported sold in 2001, 35 percent was classified as ionophore/arsenical, 33 percent was tetracycline, and 18 tons (<1 percent) was fluoroquinolone. Overall, 83 percent of the total was used for disease and 17 percent used for performance improvement. A separate estimation of U.S. usage, based on many assumptions, was calculated to be 12,300 tons just for a non-traditionally defined designation of “non-therapeutic” uses (Mellon et al., 2001).
Antimicrobial use in food animals has been a subject of discussion for over 30 years. A large number of reports, conferences, meetings, research studies and other communications have been produced. It is outside the scope of this short paper to review all of the key literature on this subject; however, a number of recent reviews and reports are provided for further information (IOM, 1998; Bezoen et al., 1999; Commonwealth of Australia Government, 1999; GAO, 1999; Barton, 2000). The primary concern has been that the use of antimicrobial agents in food animals will select for resistance to those agents in intestinal bacteria, and via foodborne transmission, an infection in humans will develop that is untreatable. A newer variation on this theme has been that foodborne commensal bacteria might transfer their resistance genes to existing susceptible normal human flora, and thereby set the stage for a non-treatable infection at a later time in the person’s life. The bacteria at issue are limited to salmonella, campylobacter and enterococci, and vary with the animal species. Additional areas of concern include environmental contamination with excreted antimicrobials or their metabolites; residue concentrations of antimicrobials in edible tissues; and direct zoonotic transmission.
Some antimicrobial classes and routes of administration generate more concern than others. For example fluoroquinolone water medication use in poultry has resulted in a Notice of Opportunity for Hearing for the sponsor from the FDA, but the use of an injectable fluoroquinolone in cattle has not. In Europe, use of fluoroquinolones in animals is not considered to put human health at undue risk, but should be monitored (WHO, 1998; CVMP, 2001). Feed additive uses for efficiency claims and disease prevention have also come under scrutiny by some government officials, physicians, microbiologists, and others. The antimicrobial agents involved primarily include tetracyclines, beta-lactams, sulfonamides, macrolides, lincosamides, streptogramins, and bacitracin. The European Union Commission has legislatively removed the efficiency claim authorizations of several antimicrobial agents, and plans to remove the authorizations for the remaining agents in a few years. In the United States, the Center for Veterinary Medicine (CVM) is conducting a risk assessment on E. faecium and virginiamycin use.
Since foodborne bacterial transmission is an essential component of the issue, it represents a critical control point for ensuring food safety from all pathogens, not just those with antibiotic resistance genes. If one looked at a short list of the chain of events that are needed to “go wrong” in order for an antibiotic-resistant foodborne disease to result in an adverse outcome for a typical patient, it would include the following:
-
Antibiotic-resistant bacteria are present in a particular group of animals.
-
Selection of pre-existing strain with resistance gene(s) or a resistance mutation in the presence of an antibiotic.
-
Strain maintains itself in the presence of other gut flora until slaughter (with or without continued antibiotic selection pressure).
-
Fecal contamination of the carcass occurs during processing leaving bacteria on the meat.
-
Carcass decontamination measures are ineffective or incomplete.
-
Food product processing, shipment, or storage may result in the growth of the contaminating bacteria.
-
Cooking at an inadequate temperature and duration fails to kill the bacteria or the food is recontaminated after cooking by improper handling.
-
Human consumption of food results in resistant bacterial colonization or infection.
-
Infection severity requires physician care or hospitalization; antibiotic prescribed that is of the same class as was used on the farm.
-
Clinical resolution of infection may not be as rapid or complete as with a susceptible strain; culture and susceptibility testing in lab compel change in antibiotic.
-
Outcome is that the treatment period is prolonged or the patient may possibly die.
It should be obvious that not all foodborne bacteria are antibiotic-resistant. Each stage of the chain of events represents a decrease in the total number of “chances” for something to “go wrong” in the subsequent stage. For example, at step 7 only improperly cooked or recontaminated food is likely to result in cases of foodborne disease. Of the fraction of people exposed in step 7, not all will get sick in step 8. In essence, this is the type of rationale that comprises a risk assessment. One could use this approach to identify key steps to direct interventions to minimize bacterial transfer or impact from all foodborne pathogens, not just those with antibiotic resistance genes.
Thus the central issue is not whether antibiotic use in food animals can select for resistance in particular types of bacteria which can then cause foodborne disease in people that is more difficult to treat. The real issue is what is the frequency at which this occurs and to what extent should resources be used to intervene? In other words, should 50 percent of the available resources be directed to the use of antibiotics in food animals if the “resistance contribution” is 5 percent?
Many intervention recommendations have already been made (and are currently in the implementation phase) to minimize the contribution of food animal antibiotic use to the overall concern in human medicine. Additional reports with such guidance are cited here for reference (WHO, 2000; OIE, 2001; Torrence, 2001; U.S. Government, 2001; FDA, 2002a; FDA, 2002b). In general, the following themes can be found across these reports:
Risk assessment. This approach seeks to objectively evaluate the likelihood of an adverse effect through hazard identification, hazard characterization, exposure assessment, and risk characterization; and could potentially be used predictively to evaluate the effect of proposed intervention strategies as a part of the risk management phase.
Reduction in antibiotic usage. This approach seeks to reduce the need to use antibiotics by emphasizing improved hygiene, vaccination, housing, etc., in an effort to avoid disease outbreaks in the first place. In some recommendations, elimination of certain antibiotics or uses is advocated.
Rational or responsible antibiotic use. The development and implementation of a series of guidelines to veterinarians and other animal care specialists on the proper use of antibiotics is strongly advocated. Indeed, many veterinary organizations have already done so and producers are now incorporating them into their quality assurance programs.
Regulatory reform to address resistance. Regulatory reform is ongoing in the United States, the European Union, Australia, and many other coun
tries with respect to the requirements that antibiotic manufacturers will have to meet in order to maintain their products or have new ones approved.
Resistance and usage monitoring. Monitoring of foodborne pathogens, principally campylobacter, salmonella and E. coli, and the “indicator” E. faecium for changes in antibiotic susceptibility patterns is ongoing in many countries, although test methods, isolate collection schemes, etc., are not optimal or consistent. Monitoring of the quantities of drug usage to assess reduction in antibiotice use is done in several small countries, and is being done on a self-reporting basis by the veterinary pharmaceutical industry in the United States and the European Union.
In conclusion, the use of antibiotics in food animals is essential to maintain a consistent supply of healthy animals entering the food chain. Although some antibiotic-resistant foodborne bacteria do make their way through the food chain to cause disease in consumers, the magnitude and clinical impact of that event remains unclear. In the larger context of human antibiotic resistance, antibiotic-resistant foodborne bacteria are a minor component compared to hospital- and community-acquired infections and antibiotic use. Nevertheless, the food animal production sector is doing its part to minimize antibiotic resistance by participating in the five activities above while continuing to deliver a safe, abundant food supply to the nation.
In response to this paper, “The Use of Antimicrobials in Food-Producing Animals,” a paper was prepared to address the public health consequences of antimicrobials in agriculture and can be found in Appendix A.
REFERENCES
Alford RH and Hall A.1987. Epidemiology of infections caused by gentamicin-resistant Enterobacteriaeceae and Pseudomonas aeruginosa over 15 years at the Nashville Veteran’s Administration Medical Center. Reviews of Infectious Diseases9:1079–1086.
Austin DJ and Anderson RM. 1999. Transmission dynamics of epidemic methicillin-resistant Staphylococcus aureus and vancomycin resistant Enterococcus in England and Wales. Journal of Infectious Diseases179:883–891.
Bartoloni A, Cutts F, Leoni S, Austin CC, Mantella A, Guglielmetti P, Roselli M, Salazar E, Paradisi F. 1998. Patterns of antimicrobial use and antimicrobial resistance among healthy children in Bolivia. Tropical Medicine and International Health3:116–123.
Barton MD. 2000. Antibiotic use in animal feed and its impact on human health. Nutrition Research Reviews13:279–299.
Bezoen A, van Haren W, Hanekamp JC. 1999. Emergence of a Debate: AGPs and Public Health Human Health and Antibiotic Growth Promoters (AGPs): Reassessing the Ris k. [Online]. Available: http://www.euronet.nl/~ssf/hanagp1.html.
Bojalil R and Calva JJ. 1994. Antibiotic misuse in diarrhea. A household survey in a Mexican community. Journal of Clinical Epidemiology47:147–156.
Bonten MJM, Slaughter S, Ambergen AW, van Voorhis J, Nathan C, Weinstein RA. 1998. The role of “colonization pressure” in the spread of vancomycin-resistant enterococci. Archives of Internal Medicine158:1127–1132.
Bonten M, Stobberingh E, Philips J, Houben A. 1992. Antibiotic resistance of Escherichia coli in fecal samples of healthy people in two different areas in an industrialized country. Infection20:258–262.
Brooks S, Khan A, Stoica D, Griffith J, Friedman L, Mukherji R, Hameed R, Schupf N. 1998. Reduction in vancomycin-resistant Enterococcus and Clostridium difficile infections following change to tympanic thermometers. Infection Control and Hospital Epidemiology 19:333–336.
Calva J. 1996. Antibiotic use in a periurban community in Mexico: a household and drug-store survey. Social Science and Medicine42:1121–1128.
CDC (Centers for Disease Control and Prevention). 1999. National Nosocomial Infections Surveillance (NNIS) System report, data summary from January 1990–May 1999, issued June 1999. American Journal of Infection Control27:520–532.
Chatterjee P. 2001. India’s trade in fake drugs—bringing the counterfeiters to book. The Lancet357:1776.
Chuc NT and Tomson G. 1999. “Doi moi” and private pharmacies: a case study on dispensing and financial issues in Hanoi, Vietnam. European Journal of Clinical Pharmacology 55:325–332.
Commonwealth of Australia Government. 1999. The Use of Antibiotics in Food-Producing Animals: Antibiotic-Resistant Bacteria in Animals and Humans: Report of the Joint Expert Technical Advisory Committee on Antibiotic Resistance (JETACAR). [Online]. Available: http://www.health.gov.au/pubs/jetacar.pdf.
Cosseron-Zerbib M, Roque Afonso AM, Naas T, Durand P, Meyer L, Costa Y, El Helali N, Huault G, Nordmann P. 1998. A control programme for MRSA containment in a paediatric intensive care unit: evaluation and impact on infections caused by other microorganisms. Journal of Hospital Infection40:225–235.
CVMP (Committee for Veterinary Medicinal Products). 2001. Position Statement: Reflection by the CVMP within a European context on the intention of the FDA to withdraw the use of the fluoroquinolone enrofloxacin in poultry. [Online]. Available: http://www.emea.eu.int/pdfs/vet/press/pos/001401en.pdf.
Datta N. 1969. Drug resistance and R factors in the bowel bacteria of London patients before and after admission to hospital. British Medical Journal2:407–411.
Djimde A, Plowe CV, Diop S, Dicko A, Wellems TE, Doumbo O. 1998. Use of antimalarial drugs in Mali: policy versus reality. American Journal of Tropical Medicine and Hygiene 59:376–379.
FDA (Food and Drug Administration). 2002a. Center for Veterinary Medicine and Judicious Use of Antimicrobials. [Online]. Available: http://www.fda.gov/cvm/fsi/JudUse.htm.
FDA. 2002b. CVM Antimicrobial Activities: Surveillance, Research, Education, and Interna tional Coordination. [Online]. Available: http://www.fda.gov/cvm/antimicrobial/AR2002Rpt.pdf.
Flynn DM, Weinstein RA, Nathan C, Gaston MA, Kabins SA. 1987. Patients’ endogenous flora as the source of “nosocomial” Enterobacter in cardiac surgery. Journal of Infec tious Diseases156:363–368.
Fridkin SK, Edwards JR, Courval JM, Hill H, Tenover FC, Lawton R, Gaynes RP, McGowen JE Jr. 2001. The effect of vancomycin and third-generation cephalosporins on prevalence of vancomycin-resistant enterococci in 126 US adult intensive care units. Annals of Internal Medicine135:175–183.
GAO (General Accounting Office). 1999. Food Safety: The Agricultural Use of Antibiotics and Its Implications for Human Health. GAO/RCED-99-74. Washington, DC: GAO.
Goetz AM and Muder RR. 1992. The problem of methicillin-resistant Staphylococcus aureus: A critical appraisal of the efficacy of infection control procedures with a suggested approach for infection control programs. American Journal of Infection Control20:80– 84.
Goldman DA, Weinstein RA, Wenzel RP, Tablan OC, Duma RJ, Gaynes RP, Schlosser J, Martone WJ. 1996. Strategies to prevent and control the emergence and spread of antimicrobial-resistant micro-organisms in hospitals: A challenge to hospital leadership. Journal of the American Medical Association275:234–240.
Goma Epidemiology Group. 1995. Public health impact of Rwandan refugee crisis: what happened in Goma, Zaire, in July, 1994. The Lancet345:339–344.
Graczyk TK, Knight R, Gilman RH, Cranfield MR. 2001. The role of non-biting flies in the epidemiology of human infectious diseases. Microbes and Infection3:231–235.
Haley RW, Hightown AW, Khabbaz RF, Thornsberry C, Martone WJ, Allen JR, Hughes JM. 1982. The emergence of methicillin-resistant Staphylococcus aureus infections in United States hospitals: Possible role of the house staff-patient transfer circuit. Annals of Inter nal Medicine97:297–308.
Harbarth S, Martin Y, Robner P, Henry N, Auckenthaler R, Pittet D. 2000. Effect of delayed infection control measures on a hospital outbreak of methicillin-resistant Staphylococ cus aureus. Journal of Hospital Infection46:43–49.
Hoge CW, Gambel JM, Srijan A, Pitarangsi C, Echeverria, P. 1998. Trends in antibiotic resistance among diarrheal pathogens isolated in Thailand over 15 years. Clinical Infec tious Diseases26:341–345.
Holmberg SD, Solomon SL, Blake PA. 1987. Health and economic impacts of antimicrobial resistance. Reviews of Infectious Diseases9:1065–1078.
Howard D, Cordell R, McGowan JE Jr, Packard RM, Scott RD II, Solomon SL. 2001. Measuring the economic costs of antimicrobial resistance in hospital settings: Summary of the Centers for Disease Control and Prevention—Emory Workshop. Clinical Infec tious Diseases33:1573–1578.
Hsueh PR, Chen ML, Sun CC, Chen WH, Pan HJ, Yang LS, Chang SC, Ho SW, Lee CY, Hsieh WC, Luh KT. 2002. Antimicrobial drug resistance in pathogens causing nosocomial infections at a university hospital in Taiwan, 1981–1999. Emerging Infectious Diseases8:63–68.
IOM (Institute of Medicine). 1998. Antimicrobial Resistance: Issues and Options.Washington, DC: National Academy Press.
Jackson GG. 1979. Antibiotic policies, practices and pressures. Journal of Antimicrobial Chemotherapy5:1–4.
LaForce FM. 1993. The control of infections in hospitals: 1750 to 1950. In: Wenzel RP, ed. Prevention and Control of Nosocomial Infections.2nd ed. Baltimore, MD: Williams and Wilkins. Pp. 1–12.
Lamikanra A and Okeke IN. 1997. A study of the effect of the urban/rural divide on the incidence of antibiotic resistance in Escherichia coli. Biomedical Letters.55:91–97.
Larsson M, Kronvall G, Chuc NT, Karlsson I, Lager F, Hanh HD, Tomson G, Falkenberg T. 2000. Antibiotic medication and bacterial resistance to antibiotics: a survey of children in a Vietnamese community. Tropical Medicine and International Health5:711–721.
Marr JJ, Moffet HL, Kunin CM. 1988. Guidelines for improving the use of antimicrobial agents in hospitals: a statement by the Infectious Diseases Society of America. Journal of Infectious Diseases157:869–876.
McGowan JE Jr. 1983. Antimicrobial resistance in hospital organisms and its relation to antibiotic use. Reviews of Infectious Diseases5:1033–1048.
McGowan JE Jr, Barnes MW, Finland M. 1975. Bacteremia at Boston City Hospital, occurrence and mortality during 12 selected years (1935–1972) with special reference to hospital-acquired cases. Journal of Infectious Diseases132:316–335.
McGowan JE Jr, Garner C, Wilcox C, Finland M. 1974. Antibiotic susceptibilities of gram-negative bacilli isolated from blood cultures: Results of tests with 35 agents and strains from 169 patients at Boston City Hospital during 1972. American Journal of Medicine 57:225–238.
McGuffey RK, Richardson LF, Wilkinson JID. 2001. Ionophores for dairy cattle: Current status and future outlook. Journal of Dairy Science84(Suppl.):E194–E203.
McMichael AJ. 2000. The urban environment and health in a world of increasing globalization: issues for developing countries. Bulletin of the World Health Organization 78:1117–1126.
Mellon M, Benbrook C, Benbrook KL. 2001. Hogging It: Estimates of Antimicrobial Abuse in Livestock. [Online]. Available: http://www.ucsusa.org/index.html.
Miller MA, Dascal A, Portnoy J, Mendelson J. 1996. Development of mupirocin resistance among methicillin-resistant Staphylococcus aureus after widespread use of nasal mupirocin ointment. Infection Control and Hospital Epidemiology17:811–813.
Muirhead S, ed. 2001. 2002 Feed Additive Compendium. Minnetonka, MN: Miller Publishing.
Muirhead S. 2002. Survey shows drop in antibiotic use. Feedstuffs74:1, 3.
Mwansa J, Mutela K, Zulu I, Amadi B, Kelly P. 2002. Antimicrobial sensitivity in enterobacteria from AIDS patients, Zambia. Emerging Infectious Diseases8:92–93.
Nagaraja TG, Laudert SB, Parrott JC. 1996. Liver abscesses in feedlot cattle. Part II. Incidence, economic importance, and prevention. The CompendiumS264–S273.
Needham DM, Foster SD, Tomlinson G, Godfrey-Faussett P. 2001. Socio-economic, gender and health services factors affecting diagnostic delay for tuberculosis patients in urban Zambia. Tropical Medicine and International Health6:256–259.
Newton P, Proux S, Green M, Smithuis F, Rozendaal J, Prakongpan S, Chotivanich K, Mayxay M, Looareesuwan S, Farrar J, Nosten F, White, NJ. 2001. Fake artesunate in southeast Asia. The Lancet357:1948–1950.
Nicolle LE. 2001. Infection Control Programmes to Control Antimicrobial Resistance. Geneva: WHO.
Nizami SQ, Khan IA, Bhutta ZA. 1996. Drug prescribing practices of general practitioners and paediatricians for childhood diarrhoea in Karachi, Pakistan. Social Science and Medicine42:1133–1139.
NRC (National Research Council). 1999. The Use of Drugs in Food Animals: Benefits and Risks.Washington, DC: National Academy Press.
O’Connor S, Rifkin D, Yang YH, Wang JF, Levine OS, Dowell SF. 2001. Physician control of pediatric antimicrobial use in Beijing, China, and its rural environs. Pediatric Infectious Disease Journal20:679–684.
OIE (Office International des Epizooties). 2001 (October 2–4). OIE Guidelines. Paper resulting from the 2nd OIE International Conference on Antimicrobial Resistance: Use of Antimicrobials and Protection of Public Health, Paris, France. [Online]. Available: http://www.anmv.afssa.fr/oiecc/conference/guidelines.htm.
Okeke IN and Edelman R. 2001. Dissemination of antibiotic-resistant bacteria across geographic borders. Clinical Infectious Diseases33:364–369.
Okeke IN and Lamikanra A. 1995. Quality and bioavailability of tetracycline capsules in a Nigerian semi-urban community. International Journal of Antimicrobial Agents5:245– 250.
Okeke IN and Lamikanra A. 2001. Quality and bioavailability of ampicillin capsules in a Nigerian semi-urban community. African Journal of Medicine and Medical Sciences 30:47–51.
Okeke IN and Lamikanra A. In press. Export of antimicrobial drugs by West African travelers. Journal of Travel Medicine.
Okeke IN, Abudu AB, Lamikanra A. 2001. Microbiological investigation of an outbreak of acute gastroenteritis in Niger State, Nigeria. Clinical Microbiology and Infection7:514– 516.
Okeke IN, Fayinka ST, Lamikanra A. 2000. Antibiotic resistance trends in Escherichia coli from apparently healthy Nigerian students (1986–1998). Emerging Infectious Diseases 6:393–396.
Okeke IN, Lamikanra A, Edelman R. 1999. Socioeconomic and behavioral factors leading to acquired bacterial resistance to antibiotics in developing countries. Emerging Infectious Diseases5:18–27.
Paredes P, de la Pena M, Flores-Guerra E, Diaz J, Trostle J. 1996. Factors influencing physicians’ prescribing behaviour in the treatment of childhood diarrhoea: knowledge may not be the clue. Social Science and Medicine42:1141–1153.
Payne MA, Baynes RE, Sundlof SE, Craigmill A, Webb AI, Riviere JE. 1999. Drugs prohibited from extralabel use in food animals. Journal of the American Veterinary Medical Association215:28–32.
Pechere JC. 2001. Patients’ interviews and misuse of antibiotics. Clinical Infectious Diseases 33:S170–173.
Prescott JF, Baggot JD, Walker RD, eds. 2000. Antimicrobial Therapy in Veterinary Medi cine. 3rd ed. Ames, IA: Iowa State University Press.
Price DJ and Sleigh JD. 1970. Control of infection due to Klebsiella aerogenes in a neurosurgical unit by withdrawal of all antibiotics. Lancet2:1213–1215.
Rosas I, Salinas E, Yela A, Calva E, Eslava C, Cravioto A. 1997. Escherichia coli in settled-dust and air samples collected in residential environments in Mexico City. Applied and Environmental Microbiology63:4093–4095.
Scheckler WE, Brimhall D, Buck AS, Farr BM, Friedman C, Garibaldi RA, Gross PA, Harris JA, Hierholzer WJ, Martone WJ, McDonald LL, Solomon SL. 1998. Requirements for infrastructure and essential activities of infection control and epidemiology in hospitals: A consensus panel report. Infection Control and Hospital Epidemiology19:114–124.
Schlaes DM, Gerding DN, John JF Jr, Craig WA, Bornstein DL, Duncan RA, Eckman MR, Farrer WE, Greene WH, Lorian V, Levy S, McGowan JE Jr, Paul SM, Riskin J, Tenover FC, Watanakunakorn C. 1997. Society for Healthcare Epidemiology of America and Infectious Diseases Society of America Joint Committee on the Prevention of Antimicrobial Resistance: Guidelines for the prevention of antimicrobial resistance in hospitals. Infection Control and Hospital Epidemiology18:275–291.
Sengupta PG, Niyogi SK, Bhattacharya SK. 2000. An outbreak of Eltor cholera in Aizwal town of Mizoram, India. Journal of Communicable Diseases32:207–211.
Siringi S. 2001. Over-the-counter sale of antimalarial drugs stalls Kenyan disease strategy. The Lancet357:1862.
Sofowora A. 1982. Medicinal Plants and Traditional Medicine in Africa.Chinchester: John Wiley and Sons.
Souwein B, Traore O, Aublet-Cuvelier B, Bret L, Sirot L, Laveran H, Deteix P. 2000. Role of infection control measures in limiting morbidity associated with multi-resistant organisms in critically ill patients. Journal of Hospital Infection45:107–116.
Taylor RB, Shakoor O, Behrens RH, Everard M, Low AS, Wangboonskul J, Reid RG, Kolawole JA. 2001. Pharmacopoeial quality of drugs supplied by Nigerian pharmacies. The Lancet357:1933–1936.
Terpstra S, Noordhoek GT, Voerten HGJ, Hendriks B, Degener JE. 1999. Rapid emergence of resistant coagulase negative staphylococci on the skin after antibiotic prophylaxis. Journal of Hospital Infection43:195–202.
Torrence, ME. 2001. Activities to address antimicrobial resistance in the United States. Pre ventive Veterinary Medicine51:37–49.
U.S. Government. 2001. A Public Health Action Plan to Combat Antimicrobial Resistance. [Online]. Available: http://www.cdc.gov/drugresistance/actionplan.
Wachter DA, Joshi MP, Rimal B. 1999. Antibiotic dispensing by drug retailers in Kathmandu, Nepal. Tropical Medicine and International Health4:782–788.
Walson JL, Marshall B, Pokhrel BM, Kafle KK, Levy SB. 2001. Carriage of antibiotic-resistant fecal bacteria in Nepal reflects proximity to Kathmandu. Journal of Infectious Diseases184:1163–1169.
Weinstein RA and Kabins SA. 1981. Strategies for prevention and control of multiple drug-resistant nosocomial infection. American Journal of Medicine70:449–454.
WHO (World Health Organization). 1998. Use of Quinolones in Food Animals and Potential Impact on Human Health. [Online]. Available: http://www.who.int/emc-documents/zoonoses/whoemczdi9810c.html.
WHO. 2000. WHO Global Principles for the Containment of Antimicrobial Resistance in Animals Intended for Food. Report of a WHO Consultation with the Participation of the Food and Agriculture Organization of the United Nations and the Office Interna tional des Epizooties. Geneva, Switzerland 5–9 June 2000. [Online]. Available: http://www.who.int/emc/diseases/zoo/who_global_principles.html.
WHO. 2001. WHO Global Strategy for Containment of Antibiotic Resistance.Geneva: WHO.
Winstanley P. 2001. Modern chemotherapeutic options for malaria. The Lancet Infectious Diseases1:242–250.





























