6
Measuring Quality of Care
Morbidity and mortality from HIV disease declined dramatically in the mid-to-late 1990s due in large part to improvements in antiretroviral therapy and an increase in the proportion of individuals receiving therapy (Karon et al., 2001). The declines were unevenly distributed across HIV-infected populations, however, due to factors such as unequal access to care and variability in quality of care (Bozzette et al., 1998; Shapiro et al., 1999). A major focus of the Ryan White Comprehensive AIDS Resources Emergency (CARE) Act is not only to eliminate barriers to accessing care, but also to improve the quality of care that its clients receive.
Two major provisions of the 2000 CARE Act reauthorization emphasized aspects of quality of care. The first provision required that all Ryan White CARE Act (RWCA) grantees establish a quality-management program. Although Title III and IV grantees already had such programs in place, the new provision required Title I and II grantees to implement them.1 The purpose of the quality-management programs is to ensure that service providers adhere to established HIV clinical practices and Department of Health and Human Services (DHHS) guidelines to the extent possible; to ensure that quality-improvement strategies include support services that help people receive appropriate HIV health care
(e.g., transportation assistance, case management); and to ensure that demographic, clinical, and health care utilization information is used to monitor trends in the spectrum of HIV-related illnesses and the local epidemic (U.S. Congress, 2000a).
The second provision in the reauthorization of RWCA directed the Institute of Medicine (IOM) to study two aspects of quality assessment:
-
“The availability and utility of health outcomes measures and data for HIV primary care and support services and the extent to which those measures and data could be used to measure the quality of such funded services” (Ryan White CARE Act. 42 U.S.C. § 300ff-11 [2003]).
-
“Other factors determined to be relevant to assessing an individual’s or community’s ability to gain and sustain access to quality HIV services” (Ryan White CARE Act. 42 U.S.C. § 300ff-11 [2003]).
The focus on quality in the most recent reauthorization reflects several national trends in quality improvement and accountability. First, the health sector has seen growing interest in measuring and improving quality (IOM 2000, 2001a).2,3 In addition, numerous reports have identified a gap between care that should be provided based on available professional knowledge and technology and the care that patients actually receive (Advisory Commission on Consumer Protection and Quality in the Health Care Industry, 1988; IOM and NRC, 1999; IOM, 2000, 2001b). Significant disparities have also been identified in the quality of care for persons living with HIV disease (Cunningham et al., 1999; Shapiro et al., 1999; Stein et al., 2000). As a result, quality measurement and improvement efforts have become a central focus of the Health Resources and Services Administration HIV/AIDS Bureau (HRSA/HAB) and RWCA grantees.
Another major trend in quality improvement and accountability is the fact that federal policy and funding decisions are increasingly being based on performance indicators. The passage of the Government Performance Results Act (GPRA)4 in 1993 and other legislation5 emphasized accountability across federal government sectors and programs by requiring all federal programs to establish measurable performance goals
and to document actual results that can be linked to the budgetary process (Kates et al., 2001). As a result, HRSA/HAB and RWCA grantees must document the impact of CARE Act funds on improving access to care and treatment and in addressing unmet needs. Key GPRA performance measures for HRSA regarding RWCA include eliminating barriers to care, eliminating health disparities, assuring quality of care, and improving public health and health care access.
Progress on this broad agenda cannot be adequately measured by outcomes alone. Considering this context, the Committee interpreted this charge as a request to examine and make recommendations regarding the availability and usefulness of not only outcomes, but a broad continuum of measures for assessing and improving the quality of both primary care and support services funded through the CARE Act. Knowledge about what constitutes the best possible HIV/AIDS care is constantly changing, and the applicability of specific measures is limited by the evolving nature of the epidemic, including changes in the affected populations, the course and outcomes of infection, treatment standards, and policies and programs for financing and delivering care. Accordingly, while the Committee makes recommendations regarding measures that HRSA and grantees can use to monitor quality of care (see Recommendation 6-1), the Committee felt it could best contribute by providing a framework, criteria, and process for selecting measures that can evolve with the epidemic.
The Committee divided its work into several discrete tasks:
-
Reviewing current HRSA/HAB quality-of-care activities;
-
Developing a conceptual framework for indicators that reflects the availability and quality of the full range of services across populations and organizations;
-
Developing criteria for selecting indicators for assessing and improving HIV/AIDS services funded through RWCA;
-
Reviewing quality measures used by RWCA grantees and other major HIV providers, recommended by authoritative groups, and contained in the research literature;
-
Identifying areas that require further development;
-
Developing a process HRSA might use to select and regularly update measures; and
-
Offering recommendations based on the analysis and findings presented here.
CURRENT HRSA/HAB QUALITY-OF-CARE ACTIVITIES
HRSA/HAB and RWCA grantees have undertaken a variety of efforts to address the quality of care, treatment, and training in RWCA
programs.6 HAB has sponsored several major quality-of-care initiatives and provides a variety of technical assistance tools and training opportunities for grantees designed to help them implement quality-management programs targeting clinical, administrative, and supportive services. HAB’s quality initiatives focus on the service delivery system at various levels, including individual providers, Title I Eligible Metropolitan Areas (EMAs), and regions. Several of the initiatives have focused specifically on Title III/IV clinics and providers, although significant work is being done to implement quality-management programs through Title I and II. This section reviews the major quality initiatives of HRSA/HAB. A number of other quality efforts by HRSA/HAB, including special research projects and technical assistance guides, are presented in Table 6-1.
HIV Quality of Care Project (HIVQUAL)
Adapted from a model of quality improvement consultation developed by New York State, the HIVQUAL builds skills and capacity among Titles III and IV grantees to sustain quality improvement. The project is sponsored by HRSA/HAB and administered by the New York State Department of Health’s AIDS Institute. The project aims to improve the quality of care delivered to persons with HIV by using data to measure performance, tracking clinical indicators based on clinical practice guidelines, and providing consultations regarding Continuous Quality Improvement. The HIVQUAL project collects information on a number of quality indicators, which are discussed later in this chapter. Grantees submit collected data to the HIVQUAL Project, where they are compiled into aggregate reports and comparative tables for participants and HRSA. A software program (HIVQUAL 3) is used to facilitate the measurement of quality indicators. Participation among grantees is encouraged, but not required (HRSA, 2003c).
Institute for Health Care Improvement HIV/AIDS Collaborative
The Institute for Healthcare Improvement (IHI) HIV/AIDS Collaborative was an effort to use rapid improvement strategies to accelerate the pace of quality improvement among CARE Act grantees. IHI focused on developing a systemwide model to ensure the delivery of evidence-based clinical care and provide strong support for self-management. The long-range goal of the IHI Collaborative was to maximize the length and qual-
TABLE 6-1 Other HRSA/HAB Quality-of-Care Activities
|
HRSA/HAB Quality Initiative |
Description |
|
Outcomes Evaluation Tools |
HRSA/HAB has developed several outcome evaluation guides that provide a framework for outcomes evaluation and sample measures (HRSA, 2003f):
|
|
Special Projects of National Significance |
HRSA/HAB has sponsored a number of Special Projects of National Significance (SPNS) that have examined access, quality of care, and outcomes (HRSA, 2003d). Some projects include:
For more information on SPNS projects see: http://hab.hrsa.gov/special/evaluation2g.htm. |
|
HIV/AIDS Evaluation Monograph Series |
The monograph series of publications was created by HRSA/HAB to assist RWCA grantees in designing and implementing evaluation studies (HRSA, 2003c). Example publications include:
|
|
HRSA Center for HIV Quality Care |
The HRSA Center for Quality Care focuses on defining appropriate standards of care for clients of HRSA programs, determining the cost of that care, and conducting research on and comparing benefit packages and capitation rates in Medicaid managed care plans. The Center is also documenting community-based provider experience with managed care plans (HRSA, 2003a). |
ity of life for patients with HIV/AIDS and satisfy patient and caregiver needs while maintaining or decreasing the total cost of care. Each participating health system identified a specific population of patients (either a subset of their patients or all of them) that could be monitored for the duration of the collaborative. Grantees then changed practices and systems to improve clinical management and office efficiency. Participants identified a set of quality-of-care indicators (discussed later in this chapter), while IHI provided guidance about how to implement and test changes in the care of their pilot population. Over 80 Title III and Title IV grantee organizations participated in the first collaborative, and Title I grantees are currently participating in a new collaborative (HRSA, 2003b; IHI, 2003).
Client Demonstration Project
The Client Demonstration Project collects client data on HIV-infected clients (tracked by unique identifiers) receiving services at CARE Act–funded providers at designated sites (EMAs or states). The client-level data permit analyses of various combinations of information on client demographics, medical status, and service utilization. The analysis of several characteristics, including CD4+ cell counts, CDC-defined disease stage, and tuberculosis status, is also possible. Though the project was originally designed to include clients who receive services from Title I and II providers, a substantial number of providers participating in the demonstration projects also receive funding from Title III and IV (HRSA, 2001, 2003a).
Primary Care Assessment Tool
The Primary Care Assessment Tool (PCAT) is a site-visit protocol developed for Title III–funded CARE Act programs. The tool, which includes a quality improvement component in the clinical section, is used to evaluate the clinical, fiscal, administrative, and support services of the grantees (HRSA, 2003e).
CARE Act Data Report
Each year all providers funded by CARE Act grantees are required to submit a CARE Act Data Report (CADR) to HRSA. Implemented in January 2002, CADR consolidated and replaced previous reporting instruments. The purpose of the CADR is to collect information on all clients who receive at least one CARE Act–eligible service during a calendar year, including information on the number and characteristics of clients
served, types of services provided, and characteristics of provider agencies. CADR also requires medical service providers to provide information on the number of clients who have been screened or treated for comorbid conditions, diagnosed with an AIDS-defining condition, and prescribed combination antiretroviral therapy. An unduplicated count of patients is not currently possible in CADR, so clients may be reported more than one time. CAREWare is a free software program that assists grantees in producing the CADR. Data from CADR are used to assess program effectiveness and quality under the GPRA (HRSA, 2002).
Other HRSA Quality Initiatives
HRSA also supports a number of other quality-of-care activities, including outcome evaluation tools, several Special Projects of National Significance, and the HIV/AIDS Evaluation Monograph Series (Table 6-1).
FOUR-DIMENSIONAL CONCEPTUAL FRAMEWORK FOR HIV QUALITY ASSESSMENT
In this section, the Committee presents a conceptual framework for assessing the quality of HIV/AIDS care. In developing its framework, the Committee relied on previous work for definitions and theory of patient-level quality, and coupled this with a public health perspective in extending previous work to include quality of care for populations.
The Committee adopted the definition of health care quality first developed by the IOM in 1990. This report defined health care quality as “the degree to which health services for individuals and populations increase the likelihood of desired health outcomes and are consistent with current professional knowledge” (IOM, 1990). This definition highlights several important aspects of quality (IOM, 2001a). First, numerous persons, providers, and organizations provide care to patients and all must be of good quality. Second, the definition acknowledges that good quality health care should produce outcomes that patients desire and that patients’ preference for treatment options may vary. Third, high-quality care does not necessarily lead to desirable outcomes. There are many factors beyond the control of providers or organizations, such as environmental or social factors, that can affect outcomes. The corollary is also true; desirable outcomes may occur despite poor quality of care. Finally, it speaks to the obligation of providers to inform themselves of most recent advances in their discipline (IOM, 2001a).
The Committee also relied heavily on the seminal work of Avedis Donabedian who conceptualized quality along three dimensions: struc-
ture (“the settings in which [health care] takes place and the instrumentalities of which it is the product”), process (“whether what is known as ‘good’ medical care has been applied”) and outcomes (“in terms of recovery, restoration of function and of survival”) (Donabedian, 1966). The Committee also based its framework on a model developed by Holzemer and Reilly (1995) that extends the work of Donabedian by focusing on the interactions and linkages between structure, process, and outcomes at the client, provider, and the care setting levels.
The Committee conceptualizes HIV quality assessment as having four key dimensions: the population of interest, the level assessed, the type of measures employed, and the spectrum of services to be evaluated (Figure 6-1).
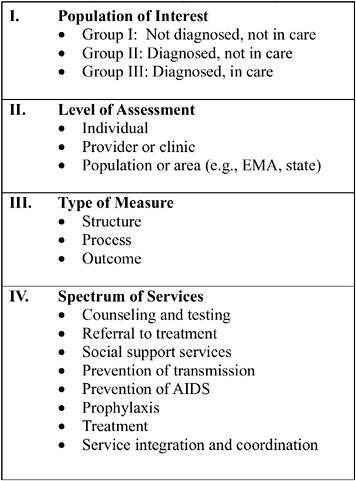
FIGURE 6-1 Dimensions of quality assessment.
Population of Interest
The HIV-infected population consists of three groups with respect to use of services: (I) those who are not yet diagnosed and thus are not in care, (II) those who are diagnosed but are not currently in care,7 and (III) those who are diagnosed and are receiving care. These categories represent a dynamic continuum. Changes in HIV prevalence and the effectiveness of screening efforts affect the flow of persons from group I to groups II and III. Shifts between groups II and III can be rapid and frequent as individuals move in and out of care owing to changes in insurance coverage or as the need for hospital or other urgent care related to an HIV-related comorbid condition arises.
When assessing care quality, the CARE Act has traditionally focused on individuals who are diagnosed and currently in care. Grantees have long sought to improve continuity of care for persons who drop out of care or receive only episodic care, and there has recently been an increased emphasis on those who are diagnosed but not yet in care. To date, few CARE Act resources have been directed to those who are not yet diagnosed. However, providers, consumers, public health officials, and Congress are focusing more attention on ensuring access to high-quality services for all who are HIV-infected (U.S. Congress, 2000b).
Among those with HIV disease, many of those not receiving care were once in care and lost access or withdrew; it is generally agreed that a high proportion of these individuals would benefit from a return to regular care. A similar argument applies to those who know of their infection but have never sought or have been unable to gain access to care, as they may well have advanced disease amenable to chemotherapy. Those with early disease will benefit from monitoring and counseling regarding their general health before their disease progresses, and indications for antiretroviral therapy could be extended to this group in the future. In addition, society benefits from efforts to prevent transmission from all currently infected individuals. Thus, knowing the relative numbers of persons in groups I, II, and III gives direct information on the overall effectiveness of the health care system in providing access to needed care. Knowing the proportions of infected persons who are undiagnosed across areas allows inference regarding access to screening and case-finding services, and about the attractance associated with the perceived high quality of care in an area. Knowing the proportions of persons who are diagnosed but not in care across areas allows inference regarding the accessibility of existing care facilities and the ability of those facilities to maintain continuity of care for treated persons.
Level of Assessment
The fundamental level for assessing quality of care is the individual patient. For example, if a clinician were assessing whether his or her patients were receiving high-quality care, it would be important to know whether patients for whom high active antiretroviral therapy (HAART) is indicated were offered such therapy. Such individual levels of quality also aggregate to the program level. For example, a measure of the quality of care provided by Title III clinics is the proportion of appropriate patients who are receiving HAART therapy. Provider organizations, including HRSA and its grantees, now commonly employ a variety of aggregated client-level measures of treatment quality in assessing clinics or practices, including monitoring, chemoprophylaxis, and antiretroviral therapy.8 However, the scientific community has given little attention to assessing the quality of care across whole communities, metropolitan areas, or states, regardless of whether patients get care at any particular facility.9
The measures and data available to assess quality vary markedly according to both the target population and the level of the assessment. For example, in assessing the quality of and access to services at the clinic level, one might assess the average wait time for an initial appointment or the use of appropriate chemoprophylaxis. While analysts have much less experience in measuring quality at the population level, they might assess access and chemoprophylaxis by measuring the average time elapsed between HIV and AIDS diagnoses. In addition, as indicated above, one might measure the overall accessibility of care by measuring the proportion of HIV-infected people who are in care, those who are diagnosed but not in care, and those who are not diagnosed.
Type of Measure
The Committee adopted the widely accepted taxonomy that classifies measures into three domains (Donabedian, 1966). Structural measures assess the characteristics and resources of an organization, such as staffing, supplies, equipment, and training. The influence of physical surroundings, availability of services, and staffing mix on the quality and costs of care is poorly understood. However, an abundance of literature has demonstrated a link between the experience of individual and institu-
tional providers (in terms of the volume and complexity of HIV services they offer) and improved clinical and economic outcomes (Kitahata et al., 1996; Turner et al., 1998; Aiken et al., 2002; Landon et al., 2002, 2003).
Process measures focus on the actions taken in the course of providing medical care, such as conducting diagnostic tests, offering appropriate therapies, promoting self-care. Process measures are important because they “cause” outcomes to the extent that medical interventions have an effect and because the acts of providing care are convenient targets for quality improvement. Although information for process measures is usually obtained from medical records, analysts can also obtain important information by asking patients about their experiences (Cleary and Edgman-Levitan, 1997; Cleary, 1999; Wilson et al., 2002). Quality assessment often aims primarily at improving processes as the key to improving outcomes because they are easier to track and modify than outcomes.
Outcome measures assess the changes in a patient’s health status. Intermediate outcome measures may assess patients’ viral load or CD4+ cell count, while longer-term outcome measures might examine morbidity, mortality, and health-related quality of life. These three major elements are interrelated and theoretically causally linked; that is, the structure of care affects the probability of good processes of care, which can in turn affect outcomes such as health status, quality of life, and patient satisfaction.
Despite compelling arguments for analyzing outcomes as ultimate indicators of quality, there are practical and theoretical impediments to doing so, at least for the individual patient and the small (in a statistical sense) aggregations of patients often used to assess providers. First, individual patient outcomes are often not closely linked to quality of care offered or provided. A broad range of factors, many of which providers do not control, determines clients’ health outcomes. Accounting for these influences is extremely difficult (Brook et al., 1996). Strong links between care and outcomes are more likely when considering a large patient group that is well defined by medical condition or demographics, when interventions target outcomes, and when well-accepted physiological, biochemical, and psychological mechanisms link medical interventions with outcomes. When assessing the quality of specific clinics or programs, it is therefore important to ensure that the outcome measures are primarily affected by the program being assessed rather than some characteristic of the subpopulation being served, and that there is evidence for the quality of the actions and programs at that clinic. For this reason, process measures are often used in lieu of outcome measures at the program or clinic level, while monitoring outcomes is a simpler and more compelling way of assessing the impact of all care provided in an area.
Spectrum of Services
Congress clearly intended to develop measures that could be used to assess the quality of both primary care and support services, and the Committee concurs that both are essential components of high-quality care (Ryan White CARE Act. 42 U.S.C. § 300ff-11). Research also shows that support services such as case management are important in reducing barriers to care (Katz et al., 2000, 2001). However, quality measurement has focused almost exclusively on clinical care.
As an individual moves along the continuum of diagnosis and care, the services that compose quality of care also change. For those not yet diagnosed, strong efforts to find, screen, and counsel them are essential; while those who are diagnosed but not in care need finding, referral, support services, and strategies for preventing transmission. Those in care, meanwhile, need not only a wide range of clinical services, including monitoring, prophylaxis, and treatment, but also social support services and efforts to prevent transmission (Figure 6-2).
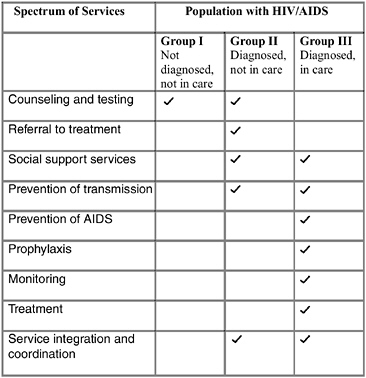
FIGURE 6-2 Spectrum of services across the HIV/AIDS population.
KEY: ![]() = service appropriate to group.
= service appropriate to group.
NOTE: This figure includes examples of services, rather than a comprehensive listing.
PRINCIPLES FOR SELECTING QUALITY-OF-CARE MEASURES
Chapter 5 discussed three overarching criteria—importance, scientific soundness, and feasibility—that could be used to evaluate measures of resource needs (Chapter 5, Box 5-2). These same criteria can be applied to evaluation of quality-of-care measures.
Importance
-
Meaningfulness: There should be consensus among clinicians, patients, or policy makers that the measure reflects an important aspect of quality of care.
-
Prevalence and seriousness of the problem: Measures should focus on common problems or care procedures that affect a sizable proportion of RWCA clients. Measures should focus on aspects of quality of care that are a general problem, or for which there is significant variation across grantees.
-
Potential for improvement: Measures should reflect aspects of care that can be improved most by RWCA grantees or through administrative changes.
-
Potential impact: Considering the prevalence and seriousness of the problem and the potential for improvement, measures should reflect the prevalence and seriousness of the problem and the potential for improvement. Measures should be selected that reflect aspects of care that can have the greatest impact on persons living with HIV infection.
Scientific Soundness
-
Reliability: Measures should be reproducible and yield consistent results when repeated in the same populations and settings. Reliability is enhanced by using standard data collection methods across clinics or populations, collecting data in a way that minimizes manipulation, and employing a common definition of the population of interest and the time period.
-
Validity: Measures should capture what they purport to measure. Measures should make sense logically or clinically (face validity), should correlate well with other measures of the same aspects of quality of care (construct validity), and should capture meaningful aspects of quality of care (content validity) (IOM, 2001a).
-
Evidence base: Measures should have a strong evidence base to support their use. For instance, structure and process measures should be clearly linked to outcomes. A number of established systems for scoring
-
the strength of evidence have been used to evaluate potential quality measures (Gross et al., 2000).
Feasibility
-
Availability of data: Data should be available at the appropriate level. For example, if the measure is to be used to assess the quality of medical clinics, each clinic should have the data; likewise, if the assessment will occur at the EMA level, each EMA should have the same data. Data should also be available in a timely manner and collected with reasonable periodicity.
-
Cost or burden of measurement: Data should be collected at reasonable cost and should not impose an excessive burden on grantees. Measures based on data that are already being collected for other purposes, or that are publicly available, are more feasible than measures that require new data collection. Similarly, the use of a small set of indicators rather than lengthy questionnaires would reduce the burden on patients and providers. Feasible measures should also be robust to different documentation practices.
There is an implied hierarchy in applying these criteria. Measures should first be considered for their importance, then scientific soundness and feasibility. Measures that are scientifically sound and feasible but do not reflect an area of importance should not be included. HRSA and grantees should select measures that are the most important in terms of the potential impact on the clients served by RWCA. Measures that are important and scientifically sound but not feasible should not be automatically discarded but considered for the future.
The feasibility criterion is particularly important in assessing quality of care under RWCA. The Committee is well aware of the data-collecting and -reporting burden experienced by grantees. RWCA grantees often receive funds from numerous other public and private sources, each of which has their own data-reporting requirements, format, and timeframes (Ryan White CARE Act 2002 Grantee Conference, August 22–23, 2003, Washington, DC: Meeting with Title I EMAs). Even within the RWCA, collecting and reporting required data is a substantial burden. For example, the CADR, which all grantees are required to complete annually, asks literally hundreds of questions, many of which are difficult to answer. HRSA could both reduce the burden of data collection on RWCA grantees and obtain more useful information on quality of care by focusing on a limited set of measures.
EXISTING QUALITY-OF-CARE MEASURES FOR HIV/AIDS
The Committee reviewed the quality measures commonly used by key organizations and often-cited studies. The Committee summarizes measures used by following nine sources: HIVQUAL, Institute for Healthcare Improvement Collaborative on HIV/AIDS (Title III), Evaluation of Quality Improvement for HIV Care (EQHIV), HIV Cost and Services Utilization Study (HCSUS), Infectious Disease Society of America (IDSA), FACCT, California Health Care Foundation Quality Assessment tool (developed by RAND), HIV Quality Enhancement Research Initiative (HIV-QUERI), and University Health System Consortium (UHC) (Table 6-2).
While there is some consistency in the measures used across these sources, there is also a great deal of variation in how the measures are defined and implemented. This review also indicates that many sources use numerous process measures and, to a lesser extent, outcomes measures. Process measures, almost all of which were closely related to well-accepted clinical guidelines,10 were over 10 times more frequent than outcome measures. Comparable attention has not been devoted to measures of structure, such as the availability of clinicians with the appropriate expertise and experience, despite studies linking increased provider expertise, capacity, and number of HIV-specific services to longer patient survival and prevention of opportunistic conditions (Kitahata et al., 1996; Bennett et al., 1989; Ball and Turner, 1991; Turner et al., 1998). The Committee identified relatively few measures of support services, and no systematic efforts to assess patient experiences with care. Finally, the Committee found that all measures focused on the provider level. No population-level process or outcome measures of quality were in routine use, although they serve as important indicators of the overall impact of the epidemic and prevention/treatment/support programs in an area.11 A brief summary of the provider-level quality-of-care measures used by different sources is included below. A detailed review of measures used by these sources is included in Appendix E.
Summary of Provider-Level Quality-of-Care Measures
Measures are organized according Donnabedian’s structure, process, and outcome framework.
|
10 |
See DHHS guidelines (http://www.aidsinfo.nih.gov/guidelines/) and International AIDS Society-USA guidelines (Yeni et al., 2002; http://www.iasusa.org/). |
|
11 |
HRSA/HAB is working with the Institute for Healthcare Improvement and grantees to develop population-based measures for Title I EMAs. |
Structural Measures
The Committee found no structural measures of quality recommended or used by these sources, although certain process measures, such as visits with HIV specialists, imply the availability of appropriate healthcare services.
Process Measures
Aggregations of patient-level process-of-care measures dominated this group. The measures of process quality used by the programs divide into five categories: prevention, screening and monitoring, antiretroviral treatment, prophylactic treatment for opportunistic infections, and social and support services.
Prevention
Three sources had quality measures focused on prevention activities. One monitored counseling and testing of pregnant women, one measured counseling regarding high-risk behaviors, and another measured tobacco use assessment.
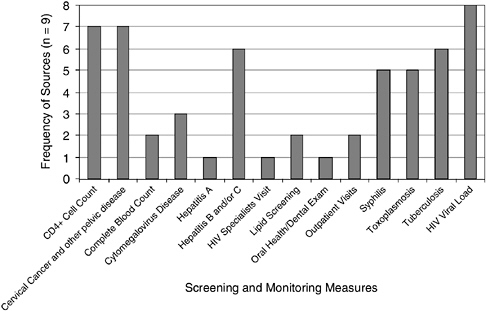
Screening and Monitoring
Eight sources measured viral load monitoring. Seven sources measured cervical cancer screening and CD4+ cell counts; six monitored tuberculosis screening; six monitored hepatitis B and/or C screening; five monitored toxoplasmosis and syphilis screening; three tracked screening for cytomegalovirus disease; two sources each monitored complete blood count, whether individuals were in care (outpatient visits), and lipid screening. One source tracked each of the following: hepatitis A, oral health/dental exam, and visits with an HIV specialist (Figure 6-3).
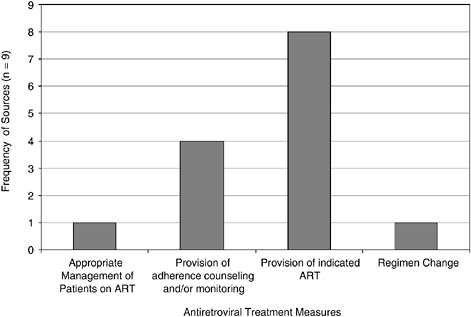
Antiretroviral Treatment
All nine sources had measures of antiretroviral therapy. Eight sources had measures of provision of indicated antiretroviral therapy (ART). Four sources had measures of adherence counseling and/or monitoring. One source measured appropriate management of patients on ART, and another monitored changes in treatment regimens (Figure 6-4).
TABLE 6-2 Selected Sources of Commonly Used Quality Measures
|
Source |
Sponsor |
|
HIV Quality of Care Program (HIVQUAL) |
HRSA/HAB and the New York State Department of Health AIDS Institute |
|
Institute for Health Care Improvement (IHI) Collaborative for Improving Care for People with HIV/AIDS |
HRSA/HAB |
|
Evaluation of Quality Improvement for HIV Care (EQHIV)a |
AHRQ |
|
HIV Cost and Services Utilization Study (HCSUS) |
A consortium of private and government sponsors; work conducted by The RAND Corporation |
|
Description |
|
Adapted from a model of quality-improvement consultation first developed by New York State, HIVQUAL (sponsored by HAB and administered by the New York State Department of Health AIDS Institute) builds capacity and capability among Title III and IV grantees to sustain quality improvement. The project aims to improve the quality of care delivered to persons with HIV through the use of aggregate data to measure performance, the measurement of clinical indicators that are based on clinical practice guidelines, and provision of continuous quality-improvement consultations and coaching. The HIVQUAL project measures a number of quality indicators (discussed later in this chapter). The data collected by grantees are submitted to the HIVQUAL Project, where they are compiled into aggregate reports and comparative tables for participants and HRSA. A software program (HIVQUAL 3) developed through this project helps facilitate the measurement of quality indicators. Participation among grantees is encouraged but not required (HRSA, 2003c) |
|
The IHI HIV/AIDS Collaborative was a collaborative effort to accelerate the pace of quality improvement among CARE Act grantees. IHI focused on developing a systemwide model of care to ensure the delivery of evidence-based clinical care, and strong support for self-management. Through the Collaborative, participating grantee organizations identified a set of quality-of-care indicators. IHI provided guidance about how to implement and test changes in the care of pilot populations. More than 80 Title III and Title IV grantee organizations participated in the first Collaborative, and Title I grantees are currently participating in a new Collaborative (HRSA, 2003b; IHI, 2003). |
|
Starting in 1999, HRSA required Title III grantees to undergo continuous quality improvement (CQI) training using the IHI breakthrough series approach. The goal of this project is to assess the quality of care provided by participating clinics, changes in such care subsequent to quality training, and the organizational characteristics and policies related to such changes. EQHIV is a controlled observational study examining the outcomes of the CQI training. The study will compare three groups of Title III clinics: (1) clinical HIV programs receiving new Title III funds as of July 1999 that receive CQI training; (2) clinical HIV programs already receiving Title III funding that will receive CQI training; and (3) clinical HIV programs already receiving Title III funding that will not receive CQI training. |
|
HCSUS was the first major research effort to collect information on a nationally representative sample of people in care for HIV infection. The study provides information on the health care services persons with HIV disease are receiving, and on the costs of those services, to inform policy making and resource allocation. The study was conducted May 1994 through October 2000. HCSUS consisted of a core study and seven supplemental studies. The core study used data on over 3,700 HIV-positive persons in care in hospitals, clinics, and private practices in 28 urban areas and 24 clusters of rural counties in the United States. The core study examined cost, use, andquality of care; access to care; unmet needs for care; quality of life; social support; knowledge of HIV; clinical outcomes mental health; and the relationship of |
|
Description |
|
these variables to provider type and patient characteristics. Seven supplemental studies used data from the core study to examine HIV in rural areas, early disease stages, mental health, older persons with HIV, drug use, oral health, and antiretroviral therapy (HRSA, 2003c). |
|
These measures are extracted from the 1999 U.S. Public Health Service/IDSA guidelines on the prevention of opportunistic infections in persons infected with HIV. In an accompanying article, Gross et al. (2000) identify performance measures to assess compliance with the guidelines on preventing opportunistic infections and to assist in their implementation. |
|
Wu and colleagues produced a discussion paper in 1998 for the FACCT that examines issues related to quality-of-care assessment for people with HIV/AIDS. Specifically, Wu et al. discuss potential indicators “that could be used to examine the performance of providers and organizations in managed care organizations, to compare organizations, and to inform quality improvement activities” (Wu et al., 1998). The paper includes a discussion of practical issues in collecting indicator data, sampling issues, and a review of a number of potential indicators. Wu and colleagues published an article adapted from the report in 2000 (Wu et al., 2000). |
|
The RAND Corporation produced the report Quality of Care for Oncological Conditions and HIV: A Review of the Literature and Quality Indicators, for the California Health Care Foundation in 2000 (Asch et al., 2000). RAND developed quality indicators for HIV disease using six practice guidelines, five reviews, and an extensive MEDLINE search of medical literature from 1993 to 1996. |
|
HIV-QUERI seeks to develop a “comprehensive and continuously improving HIV disease management system that integrates administrators, physicians, nurses, pharmacists and patients in a coordinated fashion” within the Veterans Health Administration (VHA). Building on guidelines for standards of HIV care from entities such as the International AIDS Society and the IDSA, as well as the DHHS, CDC, VHA, FACCT, and the NCQA, HIV-QUERI has collected and adapted these guidelines to the VHA to generate indicators of best practice. (VA, 2003). |
|
This study was conducted to help participants improve clinical processes based on comparative information from actual practice in the era of combination antiretroviral therapy (as opposed to pre-CART, to which most of the published studies on adherence to recommended guidelines in HIV patient care refer). Institutional enrollment in the project was voluntary and self-selected. Selected members of the National Association of Public Hospitals and Health Systems are also eligible to participate in UHC benchmarking studies. Forty organizations participated. Project participation included the selection of a minimum of 40 patients and submission of a patient log, completion of a cross-sectional survey on clinic organizational structure and processes, and a retrospective patient-level medical record abstraction tool. |
Prophylactic Treatment for Opportunistic Infections
Prophylaxis for opportunistic infections, such as Pneumocystis carinii pneumonia (PCP) (n = 8) and Mycobacterium avium vomplex (MAC) (n = 6), are the next most commonly used indicators, generally for patients who have a low or very low CD4+ cell count, respectively. Five sources collected data on patients’ receipt of influenza and pneumococcal (“pneumonia”) vaccines. Two sources measured patients’ receipt of the hepatitis B vaccination series and prophylaxis for tuberculosis and toxoplasmosis (Figure 6-5).
Social and Support Services
Only three sources reviewed by the Committee monitored indicators of social and support services. IHI had optional indicators for self-management/goal setting and support services. HIVQUAL had indicators for mental health assessment and substance abuse treatment. The HCSUS study asked patients to assess their access to critical support services by indicating whether, in the previous six months, they had needed any of five types of services: income assistance, housing assistance, home health
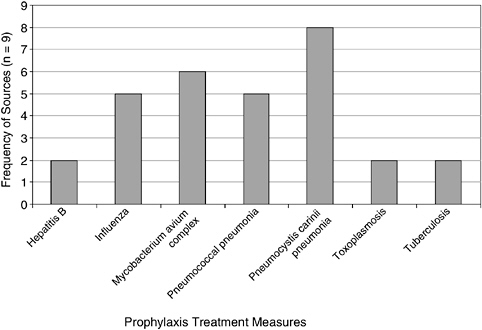
FIGURE 6-5 Frequency of prophylactic treatment quality measures among select sources.
care, mental health care, and substance abuse treatment. Any subject who answered yes to any of these questions was asked if those needs were met.
Health Outcomes
Outcome measures used are classified into three major groups: CD4+ cell counts, viral load counts, and emergency room visits and hospitalizations. Two sources measured CD4+ cell counts and viral load levels, and one source each measured patients’ emergency room visits and hospitalizations.
Population-Level Quality-of-Care Measures
Most quality assessment is designed to improve service quality and patient care, and thus focuses on the provider level, which by definition covers only people receiving treatment at a defined set of facilities or enrolled in a specific HMO. However, population-based measures are important in assessing the overall impact of RWCA in a region. Although several potential measures have been developed, research in this area has been limited.
One recent study utilized a Pneumocystis carinii pneumonia (PCP) index, defined by zip code as the number of PCP-related hospitalizations for residents divided by the number of residents living with AIDS), to identify geographic areas within New York City where residents were at increased risk for PCP (Arno et al., 2002). The PCP index is an example of a population-based measure that can be used to identify areas in need of public health interventions and improvements in HIV service delivery. This measure has the added advantage of being easy to generate and requiring only a few data sources (surveillance and service utilization data).
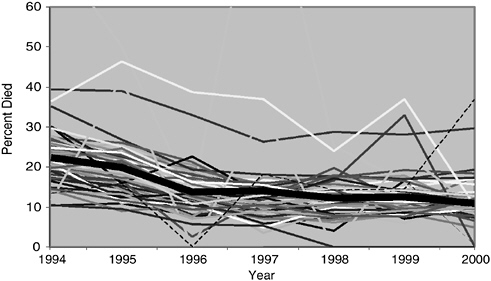
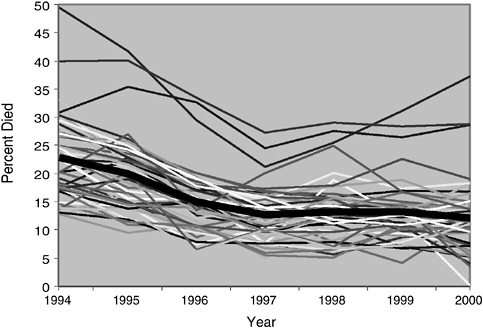
In a separate analysis, the Committee examined another potential population-level measure—the 12-month case fatality rate—which measures the proportion of people who die within 12 months after they are diagnosed with HIV infection. Figures 6-6 and 6-7 show a general decline in the 12-month case fatality rate after the introduction of HAART in the mid-1990s before the measure levels off. One notable aspect of these graphs is that they show two- and threefold variations in fatality rates among EMAs, and several EMAs show rising rates.
Another potential population-based quality measure is the proportion of patients in an area who have an AIDS diagnosis within 12 months of their HIV diagnosis. This measure can be calculated using data from the HIV and AIDS reporting system. Currently, these data are only avail-
able for states with name-based HIV reporting in place as CDC does not accept code-based data.
A recent report by the CDC highlights other potential measures that could be applied at the population level (CDC, 2003a). Using data from four supplemental surveillance studies12 conducted in selected geographic areas, CDC reports on a number of measures including: HIV-infected persons ever prescribed ART; HIV-infected persons currently prescribed ART; HIV-infected persons ever diagnosed with PCP; HIV-infected persons currently prescribed prophylaxis for PCP; and HIV-infected persons receiving a tuberculin skin test. Such measures would be difficult to obtain routinely from all relevant jurisdictions because they require estimates of the number of persons in a defined area who are infected and in care. However, a combination of intensive, targeted surveys, the current population surveys, the Area Resource File, and regional and local data could be used to estimate these populations.
While population measures are critical in monitoring the overall health of the population in a region, population-based outcomes and other measures may be influenced by a number of factors. Kates and colleagues (2001) refer to this as the “problem of attribution,” that is the difficulty of ascribing client-level or local-level outcomes to a state or federal program. They note several challenges to the effective measurement of health programs: “Variation in health systems infrastructure, market dynamics, epidemiology, and demographics makes it difficult to connect federal level activities to effects at the local level. In addition, because clients of federal programs may receive services at multiple locations, each with multiple funding sources, it is difficult to align a federal program activity (or grant dollar) with a client level outcome such as reduction in morbidity and mortality. Indeed, individual client characteristics and varying levels of disease severity may require sophisticated case mix adjustment to make comparisons meaningful” (Kates et al., 2001, p. 147).
FINDINGS
HRSA and RWCA-funded clinics and programs are doing an admirable job of defining, assessing, and attempting to improve the quality of care received by HIV-infected individuals. RWCA-funded clinics have established quality management and improvement programs, and states and EMAs either have or are establishing such programs. HRSA has sponsored numerous research and demonstration projects and a national quality-improvement collaborative to enable RWCA clients to receive the best-possible care. In many ways, RWCA-funded programs have a more advanced approach to measuring and improving quality of care than most general medical facilities. Yet, HRSA, RWCA grantees, and providers could still do much more to measure and improve quality of care. Current efforts are not guided by a common conceptual framework and measures are often not standardized. This is understandable given the recent development of quality-management programs, particularly under Titles I and II. From a programmatic point of view, the primary limitation is that the measures are not defined and measured in a comparable manner across jurisdictions. Thus, it would be very hard for HRSA to assess the relative quality of care across clinics, EMAs, or states, using the data currently available. A more organized and coherent approach would be beneficial.
Based on its review of selected quality-of-care measure sets in the previous section, the Committee recommends a standardized set of structure, process, and outcome quality measures for assessing and facilitating quality improvement at the clinic level and at the EMA/state levels (see Recommendation 6-1). For the well-developed process measures of clinical care, measures were selected if at least four of the nine groups included them. Other measures were identified using the expert judgment of the Committee.
A critical step in improving the current situation of uncoordinated data collection would be reaching a consensus on how different indicators should be defined and implemented and then putting into place a mechanism for ensuring the quality of the ensuing data. Although there are many ways of doing this, the NCQA and the National Quality Forum have developed procedures and policies that could be emulated or modified. For example, NCQA has technical advisory groups that provide advice on the importance, scientific soundness, and feasibility of possible measures, and it maintains a standing Committee on Performance Measurement that evaluates recommendations from technical experts and staff. The Committee on Performance Measurement includes representatives from the Office of Personnel Management, a state Medical Association, corporate health care purchasers, health care systems, business coa-
litions, professional organizations, the American Association of Health Plans, patient advocacy groups, insurance companies, a state department of human services, researchers, Centers for Medicare & Medicaid Services (CMS), CDC, the Veterans Administration, and the AHRQ. A comparable set of procedures could be established by HRSA.
Finding 6-1 The RWCA legislation’s emphasis on development of outcome measures is appropriate because tracking outcomes is a crucial element for accountability, and helpful in quality improvement. However, outcome measures alone are not sufficient because outcomes may be influenced by many factors not under the control of grantees, and because structure and process measures can uniquely identify areas for specific improvement.
Finding 6-2 Quality measures for HIV/AIDS that are in wide use are based on broadly accepted clinical guidelines and are appropriate. However, these measures are not standardized, which has hindered efficient evaluation of RWCA programs. Moreover, these measures are generally restricted to evaluating providers via examination of aggregated patient-level clinical data. Measures examining a more complete spectrum of services including, for example, those assessing support services, are important but are not yet in wide enough use to allow for consensus to emerge about specific measures for HIV care. Examples of potential measures of supportive services include the provision of case management, benefits advocacy, or substance abuse and mental health services.
Finding 6-3 Measures of access to needed medical and nonmedical services are also lacking. Such measures have been developed for other diseases (e.g., cancer and heart disease) and could be adapted to HIV/AIDS. Examples of potential access measures include those that focus on continuity of care (e.g., identification of primary care provider), access to needed specialty care, and access to needed nonmedical care.
Finding 6-4 Population-based measures are essential in monitoring HIV care in an EMA, region, or state and identifying areas for improvement. Current efforts to assess overall quality of care in EMAs and states are rudimentary and no population-based measures are in wide use. These measures should not be interpreted as direct measures of the quality of care being provided by specific clinics, but rather as reflecting the cumulative effects of many influences on case quality and outcomes. Additional work is needed to further develop these measures.
RECOMMENDATIONS
The Committee’s recommendations are an effort to support and extend the excellent work of HRSA and RWCA grantees in quality assessment and improvement.
Recommendation 6-1 Quality measures: HRSA should adopt quality measures that are comprehensive with respect to populations (diagnosed in care; diagnosed but not in care; not diagnosed, not in care), level of assessment (provider and population levels), types of measures (structure, process, and outcome), and spectrum of services (clinical and supportive services). At a minimum, HRSA and grantees should strongly consider inclusion of the following standard set of measures to assess the quality of care provided by RWCA-funded providers and EMA and state-level programs. Standard definitions and detailed criteria for these measures need to be developed by HRSA in collaboration with grantees, affected communities, and other stakeholders after a rigorous examination of the importance, scientific soundness, and feasibility of potential measures.
|
I. CLINIC LEVEL MEASURES |
||
|
A. Structure |
1. Proportion of providers with appropriate expertise and experience in treating patients with HIV* |
|
|
|
2. Availability of case management services |
|
|
B. Process |
Screening for: |
|
|
3. Cervical cancer* |
||
|
4. Hepatitis B |
||
|
|
a. And administration of hepatitis B vaccine if negative |
|
|
5. Hepatitis C* |
||
|
6. Syphilis* |
||
|
7. Toxoplasmosis |
||
|
8. Tuberculosis* |
||
|
Performance of the following clinical monitoring tests: |
||
|
9. CD4+ cell count and HIV viral load (process)* |
||
|
Antiretroviral Treatment: |
||
|
10. Provision of indicated antiretroviral treatment* |
||
|
11. Provision of adherence counseling and monitoring |
||
|
Vaccinations and Prophylaxis for Opportunistic Infections: |
||
|
12. Influenza vaccination |
||
|
13. Pneumoccocal pneumonia vaccination |
||
|
14. Hepatitis B vaccination if patient not immune |
||
|
15. If indicated, Mycobacterium avium complex (MAC) |
||
|
16. If indicated, Pneumocystis carinii pneumonia* (PCP) |
||
|
C. Outcomes |
17. Monitoring of CD4+ cell count and viral load values* |
|
|
18. Proportion of patients with a history of an AIDS-defining opportunistic condition* |
||
|
19. Proportion of patients who have >2 missed scheduled clinic appointments per year |
||
|
20. Hospitalizations and emergency room visits without hospital admission* |
||
|
21. Proportion of patients with unmet need for support services (e.g., assistance with obtaining housing).^ |
||
|
II. AREA (E.G., EMA OR STATE) LEVEL MEASURES |
||
|
|
Outcome measures related to access and care: |
|
|
22. Proportion of HIV-infected persons in an area who are not diagnosed^ |
||
|
23. Proportion of diagnosed persons in area who are receiving regular care^ |
||
|
24. Proportion of people with HIV who died within 12 months of an HIV diagnosis* |
||
|
25. Proportion of people with HIV who progressed to AIDS within 12 months of initial HIV diagnosis* |
||
|
Key: * indicates high priority; ^ indicates high priority, but may require further development. Other measures are important, but of lower priority. |
||
Recommendation 6-2 Infrastructure development: The Secretary of Health and Human Services (HHS) should provide additional resources to HRSA and CDC to develop infrastructure for monitoring quality at the patient, clinic, and population levels. This infrastructure development strategy has three major components:
-
HRSA should enhance support for information technology and personnel to enable clinics to collect, aggregate, and report a focused set of clinical and patient-reported data.
-
HRSA should collaborate with CDC and other agencies to develop innovative population-based measures that can be captured using existing data sources or other community-based information-gathering activities, such as surveys of unmet needs.
-
Congress should enhance flexibility in the administrative caps at the grantee level to promote infrastructure development.
Recommendation 6-3 Collaborative quality activities: The Secretary of HHS should convene a working group, not restricted to, but including the NCQA, state insurance commissioners, state Medicaid officials, and representatives from HRSA, CDC, the CMS, providers of community, outpatient, and inpatient care, and members of the
relevant research communities, to consider strategies for promoting greater collaboration between public health departments and public-and private-sector providers in order establish tools and methods to assess systems of care and quality, building on the successful collaborative models developed by the CDC for immunization (e.g., Clinic Assessment Software Application and Assessment Feedback Incentives Exchange).
REFERENCES
Advisory Commission on Consumer Protection and Quality in the Health Care Industry. 1998. Quality First: Better Health Care for All Americans. Washington, DC: U.S. Government Printing Office.
Aiken L, Clarke S, Sloane D, Sochalski J, Silber J. 2002. Hospital nurse staffing and patient mortality, burse burnout, and job dissatisfaction. Journal of the American Medical Association 288(16):1987–93.
Arno PS, Gourevitch MN, Drucker E, Fang J, Goldberg C, Memmott M, Bonuck K, Deb N, Schoenbaum E. 2002. Analysis of a population-based Pneumocystis carinii pneumonia index as an outcome measure of access and quality of care for the treatment of HIV disease. American Journal of Public Health 92(3):395–8.
Asch SM, Kerr EA, Hamilton EG, Reifel JL, McGlynn EA, Eds. 2000. Quality of Care for Oncologic Conditions and HIV: A Review of the Literature and Quality Indicators. Santa Monica, CA: Rand Health.
Ball JK, Turner BJ. 1991. AIDS in U.S. Hospitals in 1986-1987: A National Perspective. Rockville, MD: Agency for Health Care Policy and Research.
Bennett CL, Garfinkle JB, Greenfield S, Draper D, Rogers W, Mathews C, Kanouse DE. 1989. The relation between hospital experience and in-hospital mortality for patients with AIDS-related PCP. Journal of the American Medical Association 261:2975–9.
Bozzette SA, Berry SH, Duan N, Frankel MR, Leibowitz AA, Lefkowitz D, Emmons CA, Senterfitt JW, Berk ML, Morton SC, Shapiro MF. 1998. The care of HIV-infected adults in the United States. HIV Cost and Services Utilization Study Consortium. New England Journal of Medicine 339(26):1897–904.
Bozzette SA, Phillips B, Asch S, Gifford AL, Lenert L, Menke T, Ortiz E, Owens D, Deyton L. 2000. Quality Enhancement Research Initiative for Human Immunodeficiency Virus/Acquired Immunodeficiency Syndrome: Framework and Plan. Medical Care 38(6 Suppl 1):160–9.
Brook RH, McGlynn EA, Cleary PD. 1996. Quality of health care. Part 2: Measuring quality of care. New England Journal of Medicine 335(13):966–70.
CDC (Centers for Disease Control and Prevention). 2003a. Selected measures of access to and utilization of treatment and prophylaxis for HIV-infected persons. HIV/AIDS Surveillance Supplemental Report. 9(3).
CDC. 2003b. IOM Request: Data on Early Progression and Early Deaths. (Email commuication P. Sweeney, CDC, March 20, 2003).
CDC. 2003c. Morbidity Monitoring System. (Email communication, Patricia Sweeney, October 16, 2003).
Cleary PD. 1999. The increasing importance of patient surveys. British Medical Journal 319:720–1.
Cleary PD, Edgman-Levitan S. 1997. Health care quality: Incorporating consumer perspectives. Journal of the American Medical Association 278(19):1608–12.
Cunningham W, Andersen R, Katz M, Stein M, Turner B, Crystal S, Zierler S, Kuromiya K, Morton S, St Clair P, Bozzette S, Shapiro M. 1999. The impact of competing subsistence needs and barriers on access to medical care for persons with human immunodeficiency virus receiving care in the United States. Medical Care 37(12):1270–81.
Donabedian A. 1966. Evaluating the quality of medical care. The Milbank Memorial Fund Quarterly 44(3 Supp):166–206.
Gross PA, Asch S, Kitahata M, Freedberg KA, Barr D, Melnick DA, Bozzette S. 2000. Performance measures for guidelines on preventing opportunistic infections in patients infected with human immunodeficiency virus. Clinical Infectious Diseases 30(Suppl 1):S85–S93.
Holzemer W, Reilly CA. 1995. Variables, variability, and variations research: Implications for medical informatics. Journal of the American Medical Informatics Association 2(3):183–9.
HRSA (Health Resources and Services Administration). 2001. The Ryan White CARE Act. [Online]. Available: http://hab.hrsa.gov/data2/cdemosum.htm [accessed July 31, 2003].
HRSA. 2002. Instruction for completing the Ryan White CARE Act data report (CARE Act Data Report): Cross—Title Data Report. January, 2002. [Online]. Available: http://www.careactdatasupport.hrsa.gov/CADRforms/instruct.pdf [accessed July 31, 2003].
HRSA. 2003a. Report and Studies: Client Demonstration Projects. [Online]. Available: http://hab.hrsa.gov/data2/cdemosum.htm [accessed July 31, 2003].
HRSA. 2003b. Special Initiatives: HIV/AIDS Breakthrough Series Collaborative. [Online]. Available: http://hab.hrsa.gov/special/breakthrough.htm [accessed June 30, 2003].
HRSA. 2003c. Special Initiatives: HIV/QUAL Continuous Quality Program. [Online]. Available: http://hab.hrsa/gov/special/hivqual.htm [accessed June 30, 2003].
HRSA. 2003d. Special Initiatives: Initiatives/Collaboratives (by topic). [Online]. Available: http://www.hab.hrsa.gov/special/evaluation2g.htm [accessed July 31, 2003].
HRSA. 2003e. Tools for Grantees: Primary Care Assessment Tool (PCAT). [Online]. Available: http://hab.hrsa.gov/tools/pcat.htm [accessed July 31, 2003].
HRSA. 2003f. Outcomes Evaluation Technical Assistance Guide: Primary Medical Care Outcomes, Titles I and II of the Ryan White CARE Act. [Online]. Available: ftp://ftp.hrsa.gov/hab/guide.pdf [accessed July 31, 2003].
IHI (Institute for Healthcare Improvement). 2003. Improving Care for People Infected with HIV. [Online]. Available: http://www.ihi.org/collaboratives/breakthroughseries/HIV/charter.asp [accessed July 31, 2003].
IOM (Institute of Medicine). 1990. Medicare: A Strategy for Quality Assurance. Vol. 2. Lohr K, Ed. Washington, DC: National Academy Press.
IOM. 2000. To Err Is Human: Building a Safer Health System. Washington, DC: National Academy Press.
IOM. 2001a. Envisioning the National Health Care Quality Report. Hurtado MP, Swift EK, Corrigan JM, Eds. Washington, DC: National Academy Press.
IOM. 2001b. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press.
IOM and NRC (Institute of Medicine and National Research Council). 1999. Ensuring Quality Cancer Care. Hewitt M, Simone JV, Eds. Washington, DC: National Academy Press.
Karon JM, Fleming PL, Steketee RW, De Cock KM. 2001. HIV in the United States at the turn of the century: An epidemic in transition. American Journal of Public Health 91(7):1060–8.
Kates K, Marconi K, Mannie TE. 2001. Developing a performance management system for a federal public health program: The Ryan White CARE ACT Titles 1 and 2. Evaluation and Programs Planning 24:145–55.
Katz M, Cunningham W, Mor V, Andersen R, Kellogg T, Zierler S, Crystal S, Stein M, Cylar K, Bozzette S, Shapiro M. 2000. Prevalence and predictors of unmet need for supportive services among HIV-infected persons: impact of case management. Medical Care 38(1):58–69.
Katz M, Cunningham W, Fleishman J, Andersen R, Kellogg T, Bozzette S, Shapiro M. 2001. Effect of case management on unmet needs and utilization of medical care and medications among HIV-infected persons. Annals of Internal Medicine 135(8 Pt 1):557–65.
Kitahata MM, Koepsell TD, Deyo RA, Maxwell CL, Dodge WT, Wagner EH. 1996. Physicians’ experience with the acquired immunodeficiency syndrome as a factor in patients’ survival. New England Journal of Medicine 334(11):701–6.
Landon BE, Wilson IB, Wenger NS, Cohn SE, Fichtenbaum CJ, Bozzette SA, Shapiro MF, Cleary PD. 2002. Specialty training and specialization among physicians who treat HIV/AIDS in the United States. Journal of General Internal Medicine 17(1):12–22.
Landon BE, Wilson IB, Cohn SE, Fichtenbaum CJ, Wong MD, Wenger NS, Bozzette SA, Shapiro MF, Cleary PD. 2003. Physician specialization and antiretroviral therapy for HIV: Adoption and use in a national probability sample of persons infected with HIV. Journal of General Internal Medicine 18(4):233–241.
McKinney M, Marconi K. 2002. Delivering HIV services to vulnerable populations: A review of CARE act-funded services. Public Health Reports 117:99–113.
Shapiro MF, Morton SC, McCaffrey DF, Senterfitt JW, Fleishman JA, Perlman JF, Athey LA, Keesey JW, Goldman DP, Berry SH, Bozzette SA. 1999. Variations in the care of HIV-infected adults in the United States: Results from the HIV Cost and Services Utilization Study. Journal of the American Medical Association 281(24):2305–15.
Stein MD, Crystal S, Cunningham WE, Ananthanarayanan A, Andersen RM, Turner BJ, Zierler S, Morton S, Katz MH, Bozzette SA, Shapiro MF, Schuster MA. 2000. Delays in seeking HIV care due to competing caregiver responsibilities. American Journal of Public Health 90(7):1138–40.
Turner B, Markson L, Cocroft J, Cosler L, Hauck WW. 1998. Clinic HIV-focused features and prevention of Pneumocystis carinii pneumonia. Journal of General Internal Medicine 13(1):16–23.
UHC (University Health System Consortium). 2002. HIV Ambulatory Care Clinical Benchmarking Executive Summary. 12.
U.S. Congress. 2000a. Congressional Record 146(123):S10032.
U.S. Congress, House of Representatives. Committee on Commerce. 2000b. Report on Ryan White CARE Act Amendments of 2000 (106-788). 106th Cong., 2d Sess. July 25, 2000.
VA (Veterans Health Administration). 2003. HIV Quality Enhancement Research Initiative (HIV-QUERI). [Online]. Available: http://www.va.gov/chrr/active_trials/queri_factsheetHIV.pdf [accessed July 31, 2003].
Wilson IB, Ding L, Hays RD, Shapiro MF, Bozzette SA, Cleary PD. 2002. HIV patients’ experiences with inpatient and outpatient care: Results of a national survey. Medical Care 40(12):1149–60.
Wu A, Gifford A. 1998. Quality of Care Indicators for HIV/AIDS: A Discussion Paper for the Foundation for Accountability. [Online]. Available: http://www.facct.org/facct/doclibFiles/documentFile_302.pdf [accessed July 31, 2003].
Wu AW, Gifford A, Asch S, Cohn SE, Bozzette SA, Yurk R. 2000. Quality-of-care indicators for HIV/AIDS. Disease Management and Health Outcomes 7(6):315–30.
Yeni P, Hammer SM, Carpenter CC, Cooper DA, Fischl MA, Gatell JM, Gazzard BG, Hirsch MS, Jacobsen DM, Katzenstein DA, Montaner JS, Richman DD, Saag MS, Schechter M, Schooley RT, Thompson MA, Vella S, Volberding PA. 2002. Antiretroviral treatment for adult HIV infection in 2002: Updated recommendations of the International AIDS Society-USA Panel. Journal of the American Medical Association 288(2):222–35.