7
Everyday Health: Technology for Adaptive Aging
Eric Dishman, Judith Matthews, and Jacqueline Dunbar-Jacob
This new structure is indicated … by the minute but decisive change, whereby the question: “What is the matter with you?” with which the eighteenth-century dialogue between doctor and patient began … was replaced by that other question: “Where does it hurt?” in which we recognize the operation of the clinic and the principle of its entire discourse. Michel Foucault, The Birth of the Clinic: An archaeology of Medical Perception, 1973, p. xviii.
The archetypical question “Where does it hurt?” still governs most patient-provider encounters today and still serves as the basis for how we conceive of and operationalize healthcare within our society. As we enter the twenty-first century, it is fast becoming clear that we need a new way to think about the body, about healthcare, and especially about aging as we face the challenge of caring for the largest worldwide population of elders in human history. We need, perhaps, to ask a different question, “How can we help you live your life well?”
Strategies for addressing the everyday health concerns of our aging population increasingly rely on advances in technology to prevent, detect, and treat the complex health problems prevalent among older adults living in the community. Novel approaches range from implanted and wearable technology to distributed networks embedded in the living environment to in-home delivery of health services from remote locations. These technologies target several pressing health needs of older adults, including promoting physical function and social interaction, facilitating early diagnosis, enabling self-monitoring of health status, and assuring
adequate treatment. At the personal level, they contribute to preserving older adults′ health and well-being and support their oft-stated preference for remaining independent as long as possible. At the population level, their value lies in helping to compress morbidity, in keeping with the goal of Healthy People 2010 (U.S. Department of Health and Human Services, 2000) to increase the quality and years of healthy life.
Just as advances in science and technology converged to spawn invention of the health clinic in the 1700s,1 contemporary developments in these same arenas may herald the birth of a new era in which healthcare is increasingly based in the home and community, enabled by a range of pervasive, embedded computing and communications technologies. This evolutionary—if not revolutionary—shift from clinic-centric to community-centric healthcare will move us away from infrequent exam room encounters to everyday activities of health and wellness that put the burden of responsibility on an informed, proactive citizenry. This shift will likely coincide with revised notions of healthy aging. Traditionally associated with regular visits to the doctor to keep body parts and functions in working order, healthy aging may evolve into a more holistic process through which optimal function and life quality are achieved using an array of health-related technologies that augment human interaction and support.
But how will we get there? What kinds of problems need to be solved? How should we be conducting research to bring forth a new way of thinking about healthy aging? This chapter is about provoking questions more than providing answers—questions about how next-generation technologies should be designed and developed to support the needs of the next generation of elders. Here we express a perhaps extreme position in arguing for a shift to primary healthcare in the home—for a deep focus on aging-in-place technology research—as an antidote to the historical naturalization that put the clinic and the health professional at the center of our health and wellness universe. We ask, how can we develop evidence-based technologies for the home to enable better prevention, detection, adherence, and caregiving for the “age wave”? How can these tech-
nologies shift the burden of healthcare from tertiary to primary prevention? What kinds of solutions will expand the functional domain from a main emphasis on health status to more holistic notions of everyday health? And how do we expand the repertoire of available technologies to include devices that are more personal and embedded in our home environment as opposed to having to travel elsewhere for care? Informed by knowledge of normal aging and its attendant health conditions and guided by a conceptual model of health-related technology, the ensuing discussion points to some high-level opportunity areas for further thinking and action by a diverse set of researchers with sights set on these important sociotechnological challenges.
AGING AND ASSOCIATED HEALTH CONDITIONS
Deterioration occurs in almost all physiologic systems as people age, often accompanied by structural or anatomical changes. Some of these changes are due to lifestyle over time and some to environmental exposures, whereas others are a function of the aging organism. There is wide variation in the rate of decline among individuals and across systems. Changes in cognitive function and mobility are described in detail elsewhere in this volume, yet exhaustive discussion of aging anatomy and physiology is beyond the scope of this chapter. Nevertheless, several systemic changes that occur gradually over time, and their functional implications, are briefly presented here.2
With age, skin becomes thinner, less elastic, and more likely to tear, thus more prone to infection. Wounds heal more slowly, and the scars that form are weaker. Epidermal changes increase susceptibility to blistering and abrasion from minor trauma, decrease vitamin D synthesis, and heighten sensitivity to sun exposure. Cellular and vascular changes in the dermis reduce the skin′s capacity to respond to extremes in temperature and mute its inflammatory response to allergens, ultraviolet irradiation, chemical irritants, and microbial invasion. Loss of subcutaneous fat further decreases the skin′s capacity to insulate and protect the body (Gilchrest, 1999).
Blood vessels become thicker and more rigid with age, with blood pressure fluctuating more widely in response to catecholamines, exercise, and postural changes. Healthy older adults maintain their cardiac stroke volume and output while at rest through a cascade of adaptations that
include enlargement of the left ventricle of the heart, augmentation of systolic arterial pressure, and prolonged myocardial contraction. However, aerobic capacity to support increased activity decreases. Similarly, stiffening of the chest wall, loss of lung elastic recoil, and distortion of lung excursion due to vertebral decalcification have little effect on normal breathing in healthy older adults. Yet decreased cardiac and pulmonary reserve capacity limits stamina when older adults perform daily activities and lessens their resilience in response to physical demands posed by exercise and stress (Johnson, 2000; Lakatta, 1999).
The ratio of fat-to-lean body mass increases due to loss of muscle, bone, and organ tissue, further compromising reserve capacity, altering metabolism of essential nutrients and medications, and predisposing individuals to pain, deformity, falls, and fractures. This change in body composition also lowers energy requirements and increases the risk of micronutrient deficiency, glucose intolerance, and immune dysfunction. Although increased fat mass may protect older adults from hip fracture and hypothermia, it is an independent risk factor for many chronic disorders (e.g., heart disease, stroke, cancer, diabetes, and osteoarthritis) and functional limitations (e.g., exercise intolerance and functional dependency) prevalent among older adults (Singh and Rosenberg, 1999).
Sensory changes diminish acuity of hearing, vision, taste, and smell. Perception of pressure, vibration, and touch also decreases, raising the pain threshold (see Schaie, this volume, for a full discussion of sensory changes). These changes, along with diminished proprioception, increase the likelihood of injury (Gilchrest, 1999). In addition, joints become destabilized, stiff, and painful due to wear and tear and inflammation of component structures, limiting older adults′ mobility and further increasing their risk of falls.
Loss of bone mass beginning around age 40 is associated with impaired osteoblast (bone-forming) activity that continues over the remaining years of life, predisposing older adults—particularly older women—to fractures. Yet fractured bones typically take no longer to heal in older adults than in their younger counterparts (Khosla, Melton, and Riggs, 2000). Slower reflexes and muscular atrophy affect endurance, speed, gait, and balance, in turn affecting safe performance of motor activities such as lifting, walking, and driving (see Ketcham and Stelmach, this volume, for full discussion of changes in motor function.)
Decreased efficiency of the immune system translates to greater susceptibility to communicable diseases, reduced responsiveness to antibiotic treatment and immunizations, and longer recuperation when infections take hold. Most prominent among many factors contributing to age-related immune dysfunction are changes in the T-cell and B-cell populations. These changes include decreases in delayed-type hypersensitivity
reactions, impaired proliferation of peripheral blood mononuclear cells in response to T-cell activation, and altered cytokine production. Typically, the immune response to vaccination or infection is less robust, even when antibody production levels rival those observed in younger adults (Murasko and Bernstein, 1999).
Gradual weight gain that peaks in the forties (for men) and fifties (for women) commonly reverts to weight loss after age 70 (Lipschitz, 2000). Inadequate intake, absorption, and metabolism of fluids and nutrients may predispose older adults to constipation, dehydration, electrolyte imbalance, and malnutrition. Thirst drive and appetite may be reduced at a time in life when opportunities to share meals with others become less frequent. Renal function becomes less efficient and may result in slower excretion of unwanted substances (including medications) through the kidneys, poorer urinary concentration, and acidosis (Feest, 2000).
Superimposed on these changes associated with aging are a multitude of chronic disorders that may further threaten function and well-being. The most common include arthritis, coronary artery and peripheral vascular diseases, cancer, and diabetes, as well as obstructive and restrictive pulmonary disorders and osteoporosis. The prevalence of neurologic disorders such as stroke, Parkinson′s disease, and Alzheimer′s disease, which variously cause deterioration in sensorimotor function, communication, emotional stability, and cognition, also increases with age. In addition, several geriatric syndromes, including frailty, falls, infection, incontinence, and depression, result from the complex interplay among physiologic, pharmacologic, and psychosocial factors.
Change is the operative word in geriatric healthcare in that any deviation from an older adult′s usual cognitive status, behavior, or ability to function is a red flag suggesting the need for prompt investigation and action. Older adults may not exhibit the classic signs and symptoms of a disorder that are the hallmarks of the same condition in younger adults. For example, a young adult with a urinary tract infection would likely spike a fever and experience painful urination, but an older adult might merely present with confusion or lethargy. Such nonspecific symptomatology makes diagnosis of occult conditions more difficult and treatment delays likely.
Compared with younger individuals, older adults are more likely to have multiple comorbid conditions and complicated prevention and treatment regimens. Medications may be prescribed by several different clinicians and contribute to polypharmacy, or consumption of a large number of medicines with possible additive or interactive effects. Older adults use more health resources despite access barriers that include transportation difficulties, lack of proximity to health providers and facilities, and high out-of-pocket costs for uninsured expenses. Social support may be distant
and dwindling, as older adults outlive their peers and their widely dispersed families become less available for in-home help and supervision. Due to complexity, cost, isolation, and lack of access or understanding, they may not adhere to health practices capable of improving their health and well-being. In the process, they may neglect—even endanger—themselves and, in so doing, increase their need for medical intervention and assistance with self-management.
There is wide variability in health status and function among older adults. Although most exhibit remarkable vitality, when deterioration occurs the consumption of health resources and the need for support increase considerably. Changes in lifestyle may also result, as when fear of falling undermines confidence in walking and leads to deconditioning or when embarrassment about memory loss or urinary incontinence causes withdrawal from social contact.
The debilitating effects of age-related disorders have an impact not only on affected elders, but also on family members who become their informal caregivers. Whether close at hand or far away, family members often provide extraordinary amounts of supervision and assistance to compensate for older adults′ diminishing capacities to manage independently. Caring family members may be in the position to provide tangible help with hygiene, household chores, and monitoring of health status, as well as medical appointments and medication management. Or they may be limited by time and distance to infrequent visits home to assess how the older adult is managing, patch together local resources, and then follow up with periodic, if less than ideal, phone contact. In either case, the strain on families can be substantial, with evidence that the most strained caregivers are themselves at risk for premature illness and death (Schulz and Beach, 1999).
MODEL OF HEALTH-RELATED TECHNOLOGY
Health-related technology is moving toward increasingly sophisticated ways of meeting the challenges that aging, disease, and disability pose for community-residing older adults and their families. New applications are being made of old technologies not originally developed for health purposes (e.g., using the telephone for health monitoring, information, and reminders). On the horizon are aging-in-place technologies that involve new interfaces or interaction paradigms (e.g., receiving reminders and information from unconventional—even multiple—sources, such as through the television, computer, and other household appliances). In addition, new core technologies and scientific capabilities are being developed (e.g., domestic robots, “lab on a chip” (LOC) technology, and personal electronic health records).
Technological innovation threatens to evolve inefficiently, even haphazardly, if it is not informed by a guiding framework. Thus, a model is proposed that conceptualizes health-related technology for older adults in three dimensions: level of prevention, adaptation domain, and site of operation (see Figure 7-1). Consistent with the taxonomy developed by Leavell and Clark (1965), some devices may help preserve health (primary prevention), whereas others may reduce disease risk or enable its detection and treatment as early as possible (secondary prevention). Still others may control or slow the advance of a disease (tertiary prevention). At each level of prevention, health-related technologies help older adults adapt to changes in the domains of health status, physical function, cognitive function, and social interaction. In terms of location, devices may be implanted in, worn by, or within reach of an older adult. They may be part of an embedded network of devices within the living environment, or even provide in-home access to resources based some distance from
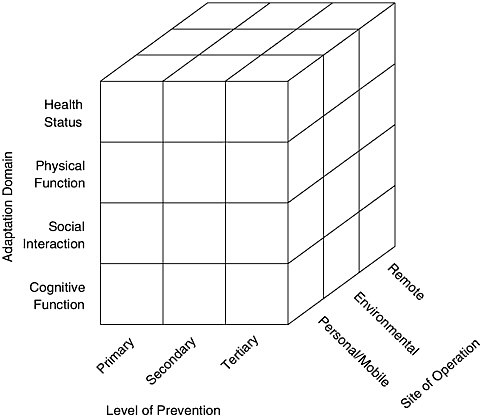
FIGURE 7-1 Three-dimensional model of health-related technology.
the home. In this model, increased emphasis is placed on primary and secondary prevention, multiple functional domains are supported, and technologies are designed more for the home and personal mobile uses.
FROM TELEMEDICINE TO EMBEDDED HEALTH TECHNOLOGIES
The most developed area of home-oriented technologies is “telemedicine” or “telehealth,” where remote connectivity and remote diagnostics have been the two primary foci. Advances in telemedicine are both exciting and promising, especially because the kinds of home portal devices marketed by companies like American TeleCare and Cybercare will begin to build consumer expectation of devices and services that work for them from the comfort of their own homes. But it is important to recognize that the understood paradigm of care here assumes that a medical professional and facility have to be in the mix. Certainly many of the potential applications for aging-in-place technologies have a medical component to them, but these technologies have the potential for greater impact when conceived as—and developed for—more broadly supporting daily health and wellness behaviors of elders in their homes. For example, the same infrastructure needed to support videoconferencing between home and clinic—a broadband Internet connection, personal computer, and video camera—can be used to connect elders with each other and their family members in elaborate, informal care networks.
Several technologies are today in their infancy but help to point the way to interesting research areas for successful aging technologies. Even after the demise of many health-related Internet start-ups, we see large informational web sites like WebMD, health-related chat and support groups, the emergence of e-mail and even instant messaging between doctors and patients, and on-line disease management planners. Instead of the push for videoconferencing as the holy grail of connecting with elders in their homes, we need research that examines all of the communication channels afforded by today′s technology to see which ones work best to support, motivate, and track healthy behaviors at home. Sometimes a low-bandwidth connection that lets a person know someone on the other end of the line is “there” may be more powerful than an immersive, high-bandwidth video link. Similarly, the adoption of multimedia technologies such as DVD, personal videorecorders, and mobile “entertainment” devices means that elders will increasingly have multiple channels through which health information, coaching, and social support can reach them. How can these devices, ostensibly adopted for entertainment purposes, provide a platform for everyday health and wellness as well?
The explosion of mobile devices today, especially with the expanding
and diversifying repertoire of diagnostics that can be plugged into them, is an important trend toward personal, home-based care for older adults. The market for diabetics seems to be the most developed at this point, with a vast number of glucometers and nutrition analysis programs that work in personal digital assistants (PDAs) and personal computers (PCs). Tools like pulse oximeters are moving from large, stand-alone devices in hospitals to PC cards for laptops or even small, compact flash plug-ins for PDAs. Most of these devices are being targeted for use by medical professionals, but as they become cheaper and more available, and as even simple household devices like bathroom scales, thermometers, and blood pressure cuffs are being connected to the Internet, consumers will begin to purchase and use this kind of equipment, whether or not their physicians are prepared to deal with that fact. More and more, devices are becoming embedded into “everyday technologies” like cell phones that can monitor heart rate, PDAs that know how many steps we have taken, or clothing such as the VivoMetrics Lifeshirt™ system that tracks “Every Breath, Every Heartbeat.”3
As much as we need to move beyond clinic-centric thinking, it is clear from the kinds of technologies mentioned above that we also need to escape our past conceptions of computing and communications technologies. Not that many years ago the prospect of a PC per household was unimaginable, so we have to ask ourselves: Where are computing and communications technologies going? What technology paradigms are just over the horizon of our current imaginations? And what are we shifting to?
There are many visions of the future of computing and communications technologies, but the recurring themes include embedded, pervasive technologies that surround us: intelligent, assistive, and even proactive technologies that work on our behalf and personalized, adaptive, customized technologies that fit our individual needs and preferences. Marc Weiser, considered the father of “ubiquitous computing,” defined the paradigm this way:
Ubiquitous computing names the third wave in computing, just now beginning. First there were mainframes, each shared by lots of people. Now we are in the personal computing era, person and machine staring uneasily at each other across the desktop. Next comes ubiquitous computing, or the age of calm technology, when technology recedes into the background of our lives.4
|
3 |
|
|
4 |
This is a widely used quote from Weiser, found in articles and on the Internet, including http://www.ubiq.com/hypertext/weiser/UbiHome.html. |
Perhaps the best way to capture this post-PC paradigm shift is in the word “embedded,” which carries an important double meaning in this chapter. First, it suggests technologies that are embedded more naturally and easily into our everyday lives and environments. Second, it suggests our movement toward a community-centric agenda of embedding health and wellness activities into everyday routines. The National Research Council (2001, p. 6) describes this new technology paradigm as “embedded networks,” or “EmNets” for short, indicating that
Computing and communications technologies will be embedded into everyday objects of all kinds to allow objects to sense and react to their changing environments. Networks comprising thousands of millions of sensors could monitor the environment, the battlefield, or the factory floor; smart spaces containing hundreds of smart surfaces and intelligent appliances could provide access to computational resources.
Research Topics and Technology Capabilities for Aging in Place
Few of the embedded network technologies needed for the age of aging in place have to be created explicitly for the purposes of everyday health and wellness. It is doubtful that economic or business models would support such a path of innovation anyway. These technologies will already be embedded into people′s everyday lives, just as cell phones and Internet access have become reliable “norms” for people of a certain socioeconomic class in many parts of the world. We need research that explores what new capabilities for home health are afforded by these increasingly commonplace technologies. The “connected home”—meaning not just the literal house but also the car, the workplace, and the public places people regularly frequent with their personal mobile technologies—is an infrastructure being built and motivated in most cases by digital entertainment and high-definition TV, by cellular networks for anytime communication with others, and by the need for more robust home security systems.
Given the wide range of tools that will be available to impact health status, physical and cognitive function, and social interaction, what should we be doing with them? What outcomes are really needed to drive independent living and a good quality of life for tomorrow′s elders? And given those outcomes, which of these technologies can be brought to bear to achieve these outcomes? A quick review of much of today′s health intervention and outcomes research seems to suggest that things are backwards. So many studies begin with a “new” technology like a web site or a PDA and ask, “What is this technology good for? Can it do this, or that, and how well?” But first we need to know the behaviors and activities to
|
BOX 7-1 It has been more than 10 years since Sarah′s husband died of lung cancer. For the first 5 years she stayed in the four-bedroom rural home on the outskirts of St. Louis that they had lived in for almost three decades. But the house became too much to manage as her heart disease progressed, so 5 years ago she moved into the ground-floor apartment of a complex that is closer to town. Except for holidays or the rare event when she pays for a cab to take her to the theatre, Sarah, age 84, lives a rather lonely existence with her two cats. Her daughter Judy lives about 6 hours away, works full time, takes care of two young children, but still tries to check in with Sarah several times a week. Sarah wishes it were several times a day. She is prone to weeks-long bouts of depression, especially in the winter, when she cannot go outside to enjoy her small patio garden. During those down times, she tends to hibernate in bed or at the television, eating very little and getting little more exercise than going to the bathroom or answering the door for her meals-on-wheels delivery. |
support, and then we can design—or more often repackage—technologies that are most likely to achieve the desired goal.
Perhaps the greatest challenge for aging-in-place research is matching up the diversity of human needs with the palette of technological capabilities that are emerging in our time. Looking through the lens of two case studies (or vignettes) about elder households helps to address both the human and the technological components. One is about 84-year-old “Sarah” who has chronic heart disease and lives alone in an apartment (see Box 7-1). The other is about “Jim” and “Jennie” who still live together in their home in spite of Jim′s multiple health problems: high blood pressure, diabetes, and increasing cognitive decline due to Alzheimer′s (see Box 7-2).
These examples, based on two households observed by social scientists in Intel′s recent “Proactive Health” study,5 provide the context for describing numerous capabilities—and related research issues—that are ripe for elaboration by real prototype development and outcomes studies. These should not be taken as “prescriptions” for real products in any way, but as foils for discussing key technology research areas that are critical to an aging-in-place agenda.
The Sarah scenario is a sad but too-frequent story of the severe social isolation, depression, and decline in health status that accompanies retirement for many millions of elders, especially once they leave their own
|
5 |
See http://www.intel.com/research/prohealth for a general description of the kinds of research Intel is conducting to understand aging-in-place needs and technology opportunities. |
|
BOX 7-2 Jim, age 78, and Jennie, age 81, live in their suburban home of 50 years in Charlotte, North Carolina. Their one adult child lives in California, so they rarely see him, but he calls every Sunday evening. They have been quite active in their retirement years with travel to the nearby coast and mountains with friends. That is, until Jim began forgetting names and repeating things almost 2 years ago. A few weeks ago, Jennie finally drove him to the doctor—she only drives during daylight hours—only to discover that he has Alzheimer′s. It makes sense to her, given how much Jim has declined over the past 2 months—so much so that she has to leave him sticky notes everywhere and to remind him of just about everything, especially to take his medications for high blood pressure and diabetes. The only upside is that he does not seem to get bored with the healthy meals she fixes him because he forgets they had the same thing the day before. Jennie still feels pretty healthy and energetic—she walks daily because it helps with her mild arthritis. But she grows tired more easily, especially having to monitor Jim′s every move. Fortunately, Martha, a neighbor, stops to check in on them daily, and Peter, a home health nurse, comes to the house to give Jennie a few hours twice a week to go shopping. |
homes for an apartment, assisted living facility, or nursing home. It allows us to explore the possibilities of technologies not only to help Sarah manage her heart disease, but also to increase her opportunities for social engagement and intellectual stimulus. The Jim and Jennie scenario, perhaps not as bleak as Sarah′s situation, provides fodder for examining the complex changes that take place as couples grow old together, especially when someone like Jim, with multiple ailments, begins to decline much more rapidly than Jennie. In their story, a nearby neighbor and a home-care nurse serve as foils to illustrate the issues of multiple-household connectivity and care. In the discussion that follows, we weave the stories of Sarah and Jim and Jennie into the fabric of a conversation about core technologies and capabilities that are emerging in an embedded networks paradigm. The list of nine research areas below (see Table 7-1) is hardly exhaustive, and many of the categories overlap.
Wireless Broadband
Aside from her two cats, Sarah′s biggest companion is the television—it is, in fact, the center of gravity in her small apartment, especially since “downsizing” forced her to give up her computer-craft room from her previous home. What would it mean for Sarah to have computing anywhere in the home? Or for her television, connected to the Internet, to become her resource for learning how to manage her heart disease? How
TABLE 7-1 Selected Core Technologies and Their Capabilities
|
Technology |
Values to Aging in Place |
|
Wireless broadband |
Anywhere in the home, any device connectivity Rich and multiple streams of health information delivery |
|
Biosensors and bodily diagnostics |
Real-time, routine chemical analysis Targeted drug delivery and effects analysis |
|
Activity sensors and behavioral diagnostics |
Location, object, and person tracking around the home Regular activity and activities of daily living measurement and assessment |
|
Information fusion and inference engines |
Personal baselines and alerts to meaningful deviations Reliable data even from temperamental technologies |
|
Personal health informatics |
Central repository for personal and professional health information Tools for easy visualization of long-term trends |
|
Ambient displays and actuator networks |
Lightweight ways to notice “okayness” of loved ones Smart home controls of all devices and appliances |
|
Agents, assistants, coaches, companions |
Reminding and coaching of activities of daily living that are declining Companionship for intellectual stimulus and support |
|
Adaptive, distributed interfaces |
Any device interactivity—do not have to use a personal computer to compute Interface experience personalized for familiarity and function |
|
Remote community and collaboration |
Multiple modes and media for communicating across distance Ways of representing and feeling “presence” at lonely times |
might Sarah, like so many elders, better manage her long list of medications if reminders could track her down on whatever device she is closest to and most familiar with? What are the opportunities for her to watch her favorite childhood shows again, perhaps at the same time and with a shared audio connection with a long lost friend who lives two time zones away? How would such a network get installed, who would care for it, and what would happen in the event of its failure if it were to become Sarah′s lifeline to the rest of the world?
Wireless broadband for the home is one of the foundational technologies for EmNets, as it provides a building block for many of the capabilities described above. With the emergence of WiFi (wireless fidelity) net-
works in the United States and the explosion of cell phone technology throughout much of the world, we are moving soon to a technoscape filled with high-speed wireless “anywhere” connectivity that will change the ways health systems can diagnose, track, convince, engage, and assist us. High-speed data transfer will allow for richer content (Sarah′s favorite shows from the past “downloaded” to her network) as well as multiple data streams to multiple devices simultaneously (a pill reminder propagating from the alarm clock to the TV to the PDA). The always-on aspect of the network will afford constant real-time monitoring of activities of daily living, and the anywhere-in-the-home connectivity will mean every device and location can become a locus for gathering or delivering health-related information without running wires everywhere.
With the Health Insurance Portability and Accountability Act (HIPAA) and future legislative mandates protecting private data, security technologies must be built into these wireless networks to protect everything from low-bandwidth raw data (a sensor tracking how often someone uses the restroom or how restless he or she is at night) to high-bandwidth information (a multimedia coach providing instruction about physical therapy exercises through a PDA or personal medical record information being delivered on a television). Again, this kind of functionality will not necessarily be installed because of aging care needs. But once installed, what does it have to offer to new ways of caring for ourselves and our loved ones? We need research programs that move beyond testing outcomes of web-site- and CD-ROM-based interventions to ones that prototype and experiment with an entire “connected home” infrastructure.
Biosensors and Bodily Diagnostics
Given her heart problems, would Sarah′s eating habits change if she had access to an ongoing analysis of her cholesterol? If there were an easy, noninvasive way for Jim to track hormones and other chemicals in his body, would he allow his wife and doctor to track the progression of his Alzheimer′s? What would be the trade-offs to knowing “What′s next?” in his likely decline versus just letting things unfold? We already see the advent of new home diagnostic equipment to support telemedical applications. Over the next decade, we will see an explosion of smaller and cheaper biosensor technologies that can detect and track various aspects of bodily function. These will help give older adults, their family caregivers, and health professionals an awareness of health status and disease progression that was never before possible. From “on-the-body” diagnostic equipment—wearables like watches, patches, clothing, and shoes—to “in-the-body” technologies—consumables, injectables, implantables—there will be a wide selection of biosensors available for in-home diagnosis.
Two important areas of research in this domain are in micro-electromechanical systems and LOC technologies. Microelectro-mechanical systems will include microscopic motors that can flow through the bloodstream to a particular location and monitor some key organ or chemical activity. LOC technologies are chips that can externally (through blood, urine, sweat, saliva, and other fluid samples) and internally do chemical analyses to help understand what is going on. Numerous social questions emerge in such a world of biosensors. In what cases will people like Sarah or Jim view the diagnostic data themselves? Under what circumstances should the data be sent out to a family caregiver or health professional, and who decides? What types of people will change their behaviors as a result of having access to such detailed, ongoing biological data? What can researchers learn about the aging process itself by having access to a widespread database of longitudinal biological data?
Activity Sensors and Behavioral Diagnostics
Although biosensors have become a headline- and venture capital-grabbing topic, a smaller but equally important technology research area is activity sensors that enable a kind of everyday behavioral diagnostics that may redefine how we engage in prevention and early detection and monitor adherence to treatment. Jennie knows that Jim is becoming more dependent on her as his memory fails, so much so that she finally takes him to the doctor for an official diagnosis of Alzheimer′s, but can a system help determine more reliably which functions are failing? Jennie feels she has to be there at every moment to help Jim with even the simplest of activities of daily living—putting on clothes in the morning, helping him microwave soup for lunch, or reminding him to do a few laps around the basement to stay fit, given his diabetes and obesity. What are the possibilities of a system tracking and assisting Jim′s activities over a long period of time—perhaps even developing behavioral baselines and “signatures” that reveal potential decline long before Jennie or Jim recognize or admit to it? What would be the value or detriment of such forecasting for Jim, his family, and his physician?
Many homes today already have alarm systems that include simple activity sensor networks. They may consist of equipment as simple as today′s motion (light) or badge sensors (usually infrared or radio frequency) that, when networked together and focused more on the internal activities of the household (as opposed to just keeping criminals out), have the potential for us to create monitoring systems that give us a new lens on our own behaviors. Would Judy come by to see her mother more often if a location system alerted her that Sarah has not left the house for
days and, in fact, has not even gotten up from the sofa except for occasional bathroom and kitchen trips? More complex sensor systems, such as high-resolution cameras used for three-dimensional tracking, may provide a diagnostic capability that could eventually change how we treat physically disabling diseases in the home. For example, Jennie may well be willing to put up with a system monitoring her gait and movements around the house if it might offer her an early warning that her arthritis has gotten worse or that she needs to see a doctor because her stride length has radically decreased over the past month. Clearly the privacy and control issues of such systems are a key component for researchers to tackle—and we need to realize that different generations, cultures, and individuals may have extraordinarily different reactions to a sensor network that is recording, analyzing, and perhaps even “publishing” their every move.
Information Fusion and Inference Engines
Although Sarah, Jim, and Jennie are unlikely to know or care about the underlying “artificial intelligence” technologies used in their sensor networks, it is important to mention the need for computer science research to transform raw sensor data, both biological and behavioral, into useful, meaningful information. Neither Sarah′s daughter nor her primary care physician is likely to want every bit of raw data in the weight and motion sensors that could be placed in her bed to monitor how well she is sleeping. But both of them may well want to know that over the past month Sarah has become more agitated while sleeping (multiple weight sensors in the bed), has tripled the number of times she gets up to go to the bathroom at night (location tracking), has lost about six pounds (weight sensors), and has initiated a lot fewer phone calls or e-mails than normal (everyday device tracking). The important capability here is for systems to establish baselines using multiple data sources and then to alert the appropriate people of deviations from those baselines. And they should do so even in light of the network and sensor failures that are bound to happen in Sarah′s home: the infamous ice storms of St. Louis wiping out electricity for a few hours, her cats jostling various sensors and sleeping on her bed at times, or Sarah herself, feeling irritated that “Big Brother” is watching, unplugging the weight sensors from the network.
The computing technologies to create reliable trending, often from unreliable and “noisy” sensor data, will have to be quite advanced to deal with the complex rhythms of home life, which are often much less controlled and routine than in nursing homes or hospitals. Multiple approaches to classic artificial intelligence problems are likely to be needed
for different purposes in the system: dynamic Bayesian networks and other statistical approaches, hierarchical approaches, and learning-based systems that may be comparing a current activity or behavior to a decade′s worth of prior data. Experts in information fusion and sensor networks will have to work hand in hand with medical experts of all kinds—gerontologists, biochemists, psychologists, etc.—to identify classes of activities that need to be tracked and the sensor approaches that can even begin to provide the raw data to such an inference system.
Personal Health Informatics
In an age when Sarah is still trying to get her complete medical record from her old doctor, now that she has found a new physician closer to her new apartment, and Jennie finds it difficult to know all of the medicines that Jim is supposed to be taking for his diabetes, high blood pressure, and Alzheimer′s, it is almost impossible to imagine the kind of lifelong database needed—and created—by embedded networks in the home. Given that most hospitals and clinics have failed to adopt data standards to enable ubiquitous electronic medical records, what are the strategies and issues for doing this for electronic personal medical records that Sarah or Jim might accumulate over a lifetime? How can Jennie keep an accurate record of all of Jim′s activities as his doctor has requested, but more importantly, how can she be empowered to decide whether or not she wants to share all of that personal information about her husband with her health plan? As XML and other metadata standards are developed, and as HIPAA-compliant data transfer systems are honed, we are finally likely to see the beginnings of powerful systems to support personal health informatics. This will likely explode as genetic testing and genomics advance and consumers pay much more attention—and want access—to their extended families′ medical histories.
Even if we had all of the data in one place today, there are a host of research questions about people′s abilities to use those data. What are the most effective, useful, understandable, meaningful ways to display personal health and wellness data to different consumers? Certainly the commonplace problem of visual decline suggests the need for larger and higher-contrast screens for many elders, but how might information display be designed with their needs in mind? What are the most appropriate ways to display large data sets—such as activity sensor logs for the entire household, long-term trend analyses of someone′s sleep habits, or changes in an individual′s exercise regimen over decades—to people who often are not experts at reading traditional charts and graphs? Most people already feel overloaded by information. So research into personal health informatics has many challenges, including simplifying, personalizing,
and contextualizing data into information that consumers can themselves act on.
Ambient Displays and Actuator Networks
Much of the above discussion of biobehavioral sensor networks has been about how data are input into the system automatically and routinely, how the data are translated into information and inferences about behavior or health status, and how the data might be stored and used in some sort of personal health informatics database. But what is the output of such systems? If a wireless broadband sensor network allows for distributed input, it also affords distributed, highly customizable output. Research is needed to show us the possibilities for “ambient displays”—that is, for more passive displays of information embedded into everyday objects and devices.
Medication reminders on the television or instructions for Jim to dress himself presented through his radio alarm clock are certainly plausible interactions in the near future, but what about more abstract, even sometimes playful, displays? Given Sarah′s heart condition and sedentary, solitary lifestyle of late, and as Jim grapples with obesity from his diabetes, both of them may benefit from an at-a-glance means of noticing “how are my eating habits this week?” This nutritional prompting and trend analysis could certainly be displayed directly on a computer monitor or TV, but it is not far-fetched to consider the whimsical, more haptic example of the refrigerator door becoming harder to open to privately signal to Jim or Sarah that they have been there too often lately. Different people are likely to respond to different kinds of prompts or reminders, and many may well prefer something more abstract, private, even playful. The refrigerator is an excellent example of how the home network can not only afford sensor input, but also serve as an actuator network—as a means of controlling and animating the environment far beyond today′s home control networks used for lighting, heating, and music.
The research of Mynatt and colleagues (2001) on ambient photograph frames provides a provocative example of using a simple digital photograph frame of a grandparent with iconic butterflies surrounding the image to represent the general well-being of a distant relative.6 How might a distant caregiver respond to such an abstracted, at-a-glance display? Does it provide enough information and reassurance? Or would more detailed data be needed? We can apply the concept to Sarah and her daughter Judy who lives about 6 hours away. What new social interac-
tions would emerge if Judy had a photograph frame—or equivalent display on one of her television channels for that matter—that displayed Sarah′s general “okayness”: that she has eaten properly today, taken her meds, gotten a little bit of exercise, but had very little social contact?
Sometimes even simpler displays bring people closer together or allow them to check in on a faraway loved one. For example, Ambient Devices sells Ambient Orb™—a small plastic orb-shaped light that can be made to represent whatever data set the user wants.7 Increasingly pressed to care for Jim′s every need as his Alzheimer′s progresses, Jennie may well get a sense of moral support just by having her lamp glow whenever her neighbor Martha is at home. This can be instrumented today with a simple motion sensor in Martha′s house to cue the orb in Jennie′s living room, or even with regular lamps through smart home networking technologies like X-10 that can be found at almost any Radio Shack.
Agents, Assistants, Coaches, and Companions
Most of today′s personal computing experiences might be thought of as reactive or interactive computing in that the user has to go to the computer and enter all of the data to be able to get something useful back from the system. Proactive computing, a term coined by Tennenhouse (2000), calls for a paradigm in which embedded networks of multiple kinds of computing devices allow systems to act more proactively on our behalf when we want them to. This transition is more necessity than nicety because there will be hundreds if not thousands of computing elements in our homes, and no human will be able to pay attention to each and every component.
But how will tomorrow′s elders and their caregivers interact with the kind of “intelligence” needed to support proactive systems? A continuum of increasingly intelligent systems will prove crucial to the future of aging-in-place technologies: from existing “agents” or software “bots” that do our bidding on information searches on the web to more capable online “assistants” that we rely on for certain kinds of expertise, to more media-rich and responsive “coaches” that may help watch and guide our actions, to eventual “companions” that may provide meaningful social interaction at times. An extended example using Jennie′s predicament as an elder caregiver for her husband with Alzheimer′s helps to elucidate this continuum. Her husband Jim has a commonly complex healthcare
situation with his high blood pressure, obesity, diabetes, and now Alzheimer′s. In supporting his everyday health needs, Jennie may well activate an on-line agent to search for highly customized information that takes into account all of Jim′s conditions and potential drug interactions. Eventually, the information may become so difficult for her to track and translate from medical jargon that she may consult a virtual personal medical assistant, much like the one being developed at the University of Rochester Center for Future Health,8 regarding which medication she should administer to Jim for his headache.
Many Alzheimer′s family caregivers experience severe burnout, depression, and exhaustion because of the around-the-clock care demanded by their charges. Jennie has to be concerned about her own increasing arthritis pain, especially now that she has to help Jim get in and out of bed every day, but she hates taking the pain pills prescribed to her because they make her drowsy. An exercise coach on her computer, using a network of cameras and wearable sensors, may guide Jennie in doing proper physical therapy exercises to help her alleviate her pain without drug therapies. Although this sounds like science fiction, researchers at a number of universities are already working on sensor networks and software to allow for this very kind of interaction.9 Finally, if Jennie′s own physical disability increases as she ages, it is conceivable that a robotic companion, equipped with a sophisticated surveillance and reminder system, may be of help by carrying items from one place to another, keeping track of Jim′s whereabouts when he is elsewhere in the house, and serving as a walker capable of autonomous navigation if she (or Jim) needs it. The collaborative Nursebot Project10 at the University of Pittsburgh, Carnegie Mellon University, and the University of Michigan is a perfect example of research going on today to make this kind of robotic companionship a reality.
In addition to the host of technical research needed to build out this agents-to-companions continuum, numerous usability, social, and psychological research topics warrant investigation. We know very little about how people in general will prefer to interact with “intelligent” systems, if at all. How will the baby boomer cohort take to the idea of
|
8 |
|
|
9 |
Researchers at the Massachusetts Institute of Technology Media Laboratory and the Center for Future Health have been working on video-monitored systems to help people conduct proper Tai Chi exercises. See press articles at http://www.rochester.edu/prReview/V62N2/featur2a.html and at http://www.rochester.edu/pr/releases/med/future.htm. |
|
10 |
See http://www-2.cs.cmu.edu/~nursebot/ for details about the Nursebot research project. |
having more explicitly proactive software tools working on their behalf? What are effective strategies for representing that intelligence in the home? Will some elders prefer a centralized source for intelligence—some sort of computing companion that cuts across all of their applications from entertainment to healthcare? And will others want each device or each application domain to have its own intelligence and representation? How important are anthropomorphism and conversational interaction with these systems? Much of this is uncharted territory because very few research platforms exist to answer these kinds of questions. But even with today′s “artificial intelligence” in video game characters and with early consumer robots like the playful AIBO® from Sony or the vacuuming Roomba™ from iRobot,11 we can begin to craft research programs that will help us understand the potential of agents, assistants, coaches, and companions to the future of health-related technologies for aging in place.
Adaptive, Distributed Interfaces
The issues surrounding how people will interact with robots and online coaches suggest a larger question: What are the trade-offs to having adaptive, distributed interfaces in an embedded, networked world? Embedded networks will afford mass customization so that each device can adjust its interaction paradigm according to the needs and preferences of the user. At the simplest level, Sarah′s “connected home” can know which room she is in, which device she is closest to, and which device or interface she prefers based on a trend analysis of her past usages. If her computing time is concentrated all in one place—such as the living room where her television is located—rather than distributed across multiple everyday devices, will she spend even more “screen time” parked on her sofa instead of getting exercise to help with her heart condition? The benefits and detriments of distributed interfaces have yet to be determined to any significant degree, but many of the component technologies are here today and could be integrated into test-bed environments to begin to research these important issues.
Someone like Jim needs more than a distributed system. Adaptability is imperative. As his Alzheimer′s progresses, he is likely to first lose his abilities to use newer devices (like a PC or PDA), but is it possible for him to use familiar, overlearned devices like his telephone and TV for new capabilities? For example, if his activities of daily living monitoring system were also to remind him to take his numerous medications on time,
|
11 |
See http://www.aibo.com/ for Sony′s AIBO® robot and http://www.roombavac.com/ for iRobot′s Roomba™. |
would he respond to prompts inserted between commercials on his TV or delivered to him as a verbal reminder over the phone? The answer is probably “yes” for some persons with Alzheimer′s and “no” for others, with the factors leading to lucidity one day and confusion the next not well understood.
That very variability suggests that a system to help Jim has to adapt not only its locus (the device on which the prompt appears) but also its modality (the type of prompt—text, verbal, video, or all of the above) and its level of support (simple reminding versus step-by-step instructions for locating and taking his pills). Even more important, how can such a system wait to deliver its prompt until the last possible moment in hopes of Jim remembering on his own accord so that he does not become prematurely dependent on his cognitive computing aid? Of course, while Jennie is alive and well, she is likely to be Jim′s pill reminding “system,” but many people with cognitive decline are not lucky enough to have a full-time caregiver with them at every moment. For those who do not, how might they interact with support systems—through what devices and modalities—and what kinds of interface paradigms will lead to the best possible outcomes? How can those systems adapt and “grow old” with a person to meet increasing needs for medical, physical, cognitive, and social support?
Remote Community and Collaboration
This last but certainly not least important research area for aging in place concerns the social interaction domain. Social support and intellectual engagement, so often overlooked in the clinic-centric view, are two of the most pressing needs for many people in their retirement years. The depression described in the Sarah scenario is all too common. The move to her apartment took her away from longtime neighbors and nearby friends. Her daughter Judy loves her very much, but she lives 6 hours away and is dealing with a full-time job and a family of her own. So as not to be a burden, Sarah often tells Judy, “Everything is fine, dear” on the phone, hiding the sedentary, solitary nature of her existence. How might EmNets and proactive computing technologies give Judy a clearer view of her mother′s plight? How might they afford new virtual and co-present social interactions for Sarah so that her sofa is not a cave for hibernation but Grand Central Station for connecting her with people all over the world?
In a world where “connected television” is commonplace, Sarah should be able to find people her own age or with her own interests in theatre and crafts who can “watch” TV together over an open audio link, or just chat while doing a craft or eating a meal. Text-based instant mes-
saging today begins to show us the ways in which these open, always-on channels with other people start to provide new comfort and new ways to “be together.” But how will people interact with or through other modalities like audio, video, audio plus occasional stills, even abstracted animations? How can Sarah safely show her availability and interests to a select group of potential companions? Perhaps a “connected telephone” is all that is needed in the short term for Sarah and Judy′s situation. If Judy gets an e-mail from the system telling her that her mother has had no phone or e-mail contact with anyone this week, would she be more likely to call or perhaps even ask a friend who lives nearby to visit? There are clearly technological, social, privacy, and interface issues in such scenarios, but tools already exist to begin testing outcomes of such capabilities, which go well beyond the web-site and e-mail studies commonly done today.
For someone like Jennie, these same technologies may simply offer comfort in knowing that someone else is there for her, even if she never actually asks them for assistance. Might she find solace and strength, for example, in seeing her small “social network” ticker tape at the bottom of her TV screen, showing that Peter, the home-care nurse, and her neighbor Martha are available at that exact moment if she should need them? How might Peter be able to optimize his “quality time” during home visits to Jim by looking in advance at the behavioral and medical data accumulated since his last home visit? Is Jennie willing to let Martha have access to some kind of real-time warning system that shows the overall well-being or stress of Jim and Jennie′s household so that Martha may stop by when Jennie is having a bad day?
Jim, at least on his most coherent days, may well avail himself of these kinds of communication technologies to help maintain his sense of purpose in life. Even though it is unsafe for him to continue using his basement saws to do woodworking, he can use the same infrastructure installed for today′s “telemedicine” to conduct his own “telementoring” sessions with high school students who may be taking shop. Or he can collaboratively browse old photos or genealogy web sites with his son who lives in California. The competing TV commercials in the Internet battle between software titans AOL and MSN show that many of these social networking technologies are already here. The seeds of these more advanced collaborative capabilities are planted in today′s data-sharing, peer-to-peer software programs such as Napster, Groove, and the numerous collaboration tools for businesses and professionals. Granted, today′s elders may not have access or abilities to use solutions like these, but we need to begin research today to build evidence for or against the utility of embedded network capabilities applied to aging-in-place challenges. These technologies can be reworked to start to test some of these new social support and caregiving paradigms—and to build a body of knowl-
edge around radically new computing experiences that can begin to address the epidemic of social isolation expected to spread widely over the coming decades.
CHALLENGES FOR HEALTH-RELATED TECHNOLOGIES RESEARCH
Technology development in isolation is unlikely to get us very far in constructing evidence-based systems that can transform the way we care for our aging population. We suggest six strategies, each of which should occur concurrently and collaboratively, for approaching research that involves engineering, computer science, and the health and behavioral sciences.
Imagination: Moving Beyond Today′s Clinical and Computing Models
The largest challenge facing anyone trying to transform the future of everyday health in aging is not technology but imagination. Hence, celebrating the “birth of a new era” is meant to challenge us to begin to go beyond our clinic-centric notion of disease care to a community-centric notion of healthy aging, in step with the birth of new technological approaches incorporating embedded networks and proactive computing. The three-dimensional model of health-related technology presented in this chapter further suggests that some research resources be taken “out of the box” of tertiary prevention in clinics and hospitals and dedicated to finding creative solutions for promoting health and preventing disease in community-residing older adults.
Identification: Finding and Prioritizing Problems to Pursue
Recognizing that research resources are limited, we must ask: What are the most important, high-impact problems that embedded network technologies and proactive computing should try to address? Within each of the support domains, what kinds of behavioral changes and interventions are most needed to improve health status, physical and cognitive function, and social interaction? How can social engagement, intellectual stimulus, and personal motivation be supported through embedded technologies? How will the needs, daily activities, and everyday technologies for today′s elders compare with those of the baby boomers moving into retirement? How will cultural, political, socioeconomic, and gender differences affect development and diffusion of such technologies?
These kinds of questions call for a range of qualitative and quantitative techniques (focus groups, surveys, anthropological fieldwork, demographic analysis, segmentation analysis, cross-cultural comparison) to be used to understand the daily lives and often unarticulated needs of older adults. One of the biggest challenges is to examine the entire household—situated within a particular community—as the unit of analysis.
Iteration: Concept Testing and Refinement
Iterative design is crucial to development of home-based systems that will help with aging in place. Long before major investments are made to develop and deploy embedded health technologies, we need research conducted on conceptual and experiential prototypes12 that are quicker and cheaper to build. Small-scale outcomes studies of experiential prototypes are needed prior to engaging in larger studies that incorporate more thoroughly developed systems.
These can be done by human factors experts, interaction designers, and social scientists working with engineering teams and health professionals to create an array of artifacts for “testing” with elders, their informal care networks, and their professional caregivers. A rigorous, iterative process from simple sketches or storyboards to “vision videos” to on-screen animations to “informances”13 to concept prototypes (often called “wizard-of-oz” prototypes) to usable prototypes should yield useful results all along the way and help to ensure that the final products are technological interventions that deliver positive outcomes. Many technology components are available today to begin testing models and interfaces, even if the economies of scale have not made them cheap enough for mass distribution or the applications have not made them compelling enough for mass consumption.
Infrastructure: Deep Dives on Enabling Technologies
Much of the engineering research needed to develop these technologies will—and should—occur independent of aging-in-place applications.
But a portion of this enterprise should examine the unique needs of this domain, such as potential legislative mandates for home-based data security (next-generation HIPAA?) that must be built into the core architecture. What capabilities have we missed or mischaracterized that will likely impact the home health “platform” over the coming decade? Also, what core technologies and capabilities will be developed for other applications like digital entertainment and home security that can be exploited for home health and aging-in-place purposes? Finally, it is crucial to understand how aging-in-place technologies will be developed and diffused differently in different parts of the world, where key underlying technologies (e.g., cable networks versus cellular networks) may differ radically as a result of historical, social, and economic conditions.
Interfaces: Exploration of Human-Machine Interaction
Well before usability research is conducted on a fully implemented application or device, we need plausibility and livability research that examines the likely uptake of these new technologies by their intended audiences, as well as the “fit” of the technologies into their daily lives. An overarching principle of importance here is “mass customization,” not only of the graphical user interface, but of the whole interaction paradigm. The devices or form factors (size and type of display such as on a laptop versus a desktop computer), input and output paradigms, adaptive interfaces, multiple modalities, and interface personalization and dispersion will create a level of interface customization—and potential confusion—that we have never seen before. Interfaces for the aging population will need to move beyond today′s limited “access” approach to interface strategies that support people with different and changing cognitive and physical function.
Integration: Testing Whole Systems in Situ
True systems integration research will be essential to the development of successful aging-in-place technologies. Treating the entire home as a “system” means doing technology research into interoperability and adaptive architecture like we have never seen before. Because EmNets involve input (from intentional user input to automatic sensor input) and output throughout and across multiple devices, form factors, and interfaces, testing of single devices in isolation will be insufficient, if not impossible. It will be necessary to test the synergy of many connected, intelligent devices as part of a larger system. This will present enormous installation challenges, both for researchers and for end users, especially in the many years required to retrofit older homes and earlier networks.
Furthermore, outcome studies that require large numbers of households for randomized clinical trials will likely be infeasible. Instead, researchers will need to rely on quantitative strategies, single case studies, and small-sample intervention designs to evaluate consumer satisfaction and utility.
Collaboration in conducting true systems integration research will require teamwork not only across multiple disciplines, including healthcare, gerontology and other social sciences, and technology, but also across multiple organizations—industry, government, and academe. Funding for such ambitious endeavors will require more jointly sponsored initiatives by the National Institutes of Health, the National Science Foundation, and the National Institute of Standards and Technology. Greater utilization of cooperative agreements and contracts will be needed to bring together the various players who can develop and evaluate these complex technologies. Several questions arise: How can “open-source” research platforms for the home be constructed across competing universities and businesses to help accelerate home health research and development efforts? Given the diversity and scale of players who must cooperate to do good, successful aging technology research, it is also clear that we will need to negotiate new models of intellectual property and new incentive structures to help organizations maintain a competitive spirit while also collaborating with their competitors.
Diffusion of these technologies will alter the structure and function of our healthcare system and have implications for educational preparation of older adults, their families, and our work force. The shift toward remote sites handling older adults′ primary care needs and simple conditions, with clinics and hospitals focusing almost exclusively on diagnosis and treatment of complex acute and chronic conditions, will necessitate training a new cadre of individuals with expertise in home installation and systems maintenance. Training will also be needed to ensure that healthcare professionals and paraprofessionals know how to employ these tools appropriately in the home and from remote sites, particularly in light of their poor adoption of existing technologies (e.g., Internet and email, CD-ROMs, PDAs) for use with older adults and their families. Although the upcoming baby boomer cohort may be more tech-savvy than their elders, they will not necessarily be more sophisticated in understanding complex technologies. It will be incumbent on technology developers to work toward maximally intuitive interfaces. Likewise, we will need to do a better job educating older adults and their families about the capabilities and limitations of health-related technologies and about how to use them—as utilization is now largely limited to the most aggressive consumers—thus promoting realistic expectations of performance and not overselling the prospect of promising results.
Ethical issues related to the use of these technologies will need to be considered, but they should not be any more complex than those encountered in our current system of healthcare. Just as individuals are now responsible for their own lifestyles, treatment regimens, and follow-up at specified intervals, so too will they retain control over whether to heed recommendations for changing their behavior and adhering to prescribed regimens. As is true for health-related technology in the home today, understanding who is capable of using what technology will be important, and ongoing reassessment of its appropriateness and adequacy in relation to a person′s functional and motivational status will continue to be imperative.
Ensuring privacy will pose a difficult, although arguably surmount-able, challenge. Safeguarding personal data, including designating who can have legitimate access to those data, will likely entail broadening the current HIPAA mandate. Protection will be needed for the raw data gathered from a variety of nontraditional sources (e.g., opening of the refrigerator door, periods of ambulation, pressure applied to a chair or bed) from which inferences are made about an individual′s health status, physical function, cognitive function, and social interaction. The economic benefit of these health-related technologies remains an open question. In a best-case scenario, preventing or slowing physical and cognitive decline and reducing complications from chronic disorders could result in significant cost savings. Lower costs would conceivably result from fewer office visits, lower hospitalization rates, and lower rates of institutionalization, more than offsetting the cost of the technologies themselves. Medication noncompliance is now estimated to account for 6 percent of all emergency room visits (Toh, Low, and Goh, 1998) and 11 percent of hospital admissions (Col, Fanale, and Kronholm, 1990). The economic impact of reducing this problem alone could be enormous. Although such improvements would provide welcome budgetary relief, the downside is that healthcare workers may consider their jobs threatened and healthcare organizations may fear for their continued viability. These concerns would likely be resolved through job reorganization and modification of facilities to accommodate the new roles and services necessitated by the shift from clinic-centric to community-centric healthcare.
Although our focus in this chapter has been largely on the United States, it is important to recognize that the challenge of dealing with the “age wave” is not unique to the United States. Given that other countries are already facing—and dealing with—the aging crisis, we need to consider that technologies and expertise may come into our culture from abroad and that cultural differences in the treatment of elders may mean that many technologies and contexts of care do not necessarily translate well across geopolitical boundaries. In the transition from the archetypical
medical question “Where does it hurt?” to “How can we help you live your life well?” perhaps we will discover that the promise of everyday health through embedded technologies is not only about improving the health and well-being of our older population, but is about enabling all of us to live the well-lived life.
REFERENCES
Berger, J. (1991). Ways of seeing (3rd ed.). New York: Penguin Books.
Col, N., Fanale, J.E., and Kronholm, P. (1990). The role of medication noncompliance and adverse drug reactions in hospitalizations of the elderly. Archives of Internal Medicine, 150(4), 841-845.
Dishman, E. (2003). Designing for the new old: Asking, observing, and performing future elders. In B. Laurel (Ed.), Design research: Methods and perspectives (pp. 41-48). Cambridge, MA: MIT Press.
Feest, T. (2000). Renal disease. In J.G. Evans, T.F. Willliams, B.L. Beattie, J.P. Michel, and G.K. Wilcock (Eds.), Oxford textbook of geriatric medicine (pp. 654-663). Oxford, England: Oxford University Press.
Foucault, M. (1973). The birth of the clinic: An archeology of medical perception. New York: Random House.
Gilchrest, B.A. (1999). Aging of the skin. In W.R. Hazzard, J.P. Blass, W.H. Ettinger, J.B. Halter, and J.G. Ouslander (Eds.), Principles of geriatric medicine and gerontology (pp. 573-590). New York: McGraw-Hill.
Hazzard, W.R., Blass, J.P., Ettinger, W.H., Halter, J.B., and Ouslander, J.G. (1998). Principles of geriatric medicine and gerontology. New York: McGraw-Hill.
Johnson, B.D. (2000). Age-associated changes in pulmonary reserve. In J.G. Evans, T.F. Williams, B.L. Beattie, J.P. Michel, and G.K. Wilcock (Eds.), Oxford textbook of geriatric medicine (pp. 483-497). Oxford, England: Oxford University Press.
Ketcham, C.J., and Stelmach, G.E. (2004). Movement control in the older adult. In National Research Council , Technology for adaptive aging (pp. 64-92). Steering Committee for the Workshop on Technology for Adaptive Aging. R.W. Pew and S.B. Van Hemel (Eds.). Board on Behavioral, Cognitive, and Sensory Sciences. Division of Behavioral and Social Sciences and Education. Washington, DC: The National Academies Press.
Khosla, S., Melton, L.J., and Riggs, B.L. (2000). Involutional osteoporosis. In J.G. Evans, T.F. Williams, B.L. Beattie, J.P. Michel, and G.K. Wilcock (Eds.), Oxford textbook of geriatric medicine (pp. 617-625). Oxford, England: Oxford University Press.
Lakatta, E.G. (1999). Circulatory function in younger and older humans in health. In W.R. Hazzard, J.P. Blass, W.H. Ettinger, J.B. Halter, and J.G. Ouslander (Eds.), Principles of geriatric medicine and gerontology (pp. 645-660). New York: McGraw-Hill.
Leavell, H.R., and Clark, E.G. (1965). Preventive medicine for the doctor in his community (3rd ed.). New York: McGraw-Hill.
Lipschitz, D.A. (2000). Nutrition and ageing. In J.G. Evans, T.F. Williams, B.L. Beattie, J.P. Michel, and G.K. Wilcock (Eds.), Oxford textbook of geriatric medicine (pp. 139-150). Oxford, England: Oxford University Press.
Murasko, D.M., and Bernstein, E.D. (1999). Immunology of aging. In W.R. Hazzard, J.P. Blass, W.H. Ettinger, J.B. Halter, and J.G. Ouslander (Eds.), Principles of geriatric medicine and gerontology (pp. 573-590). New York: McGraw-Hill.
Mynatt, E.D., Rowan, J., Craighill, S., and Jacobs, A. (2001). Digital family portraits: Providing peace of mind for extended family members. In Proceedings of the 2001 ACM conference on human factors in computing systems (CHI 2001). Seattle, WA: ACM.
National Research Council. (2001). Embedded, everywhere: A research agenda for networked systems of embedded computers. Washington, DC: National Academy Press.
Schaie, K.W. (2004). Cognitive aging. In National Research Council, Technology for adaptive aging (pp. 43-63). Steering Committee for the Workshop on Technology for Adaptive Aging. R.W. Pew and S.B. Van Hemel (Eds.). Board on Behavioral, Cognitive, and Sensory Sciences. Division of Behavioral and Social Sciences and Education. Washington, DC: The National Academies Press.
Schulz, R., and Beach, S.R. (1999). Caregiving as a risk factor for mortality: The Caregiver Health Effects Study. Journal of the American Medical Association, 282(23), 2215-2219.
Singh, M.A., and Rosenberg, I.H. (1999). Nutrition and aging. In W.R. Hazzard, J.P. Blass, W.H. Ettinger, J.B. Halter, and J.G. Ouslander (Eds.), Principles of geriatric medicine and gerontology (pp. 81-96). New York: McGraw-Hill.
Tennenhouse, D. (2000). Proactive computing. Communications of the ACM, 43(5), 43-50.
Toh, S.L., Low, C.L., and Goh, S.H. (1998). Drug related visits of geriatrics to the emergency room. Abstract of presentation at American Society of Health-System Pharmacists Annual Meeting 55 INTL-3.
U.S. Department of Health and Human Services. (2000). Healthy People 2010. (Conference Edition in Two Volumes). Washington, DC: U.S. Department of Health and Human Services.






























