The Relationship Between Health Literacy and Medical Costs
David H. Howard, Ph.D.
INTRODUCTION
Past research has shown that individuals with low levels of health literacy are more likely to be hospitalized and have worse disease outcomes (Baker et al., 1998, 2002; Schillinger et al., 2002). The major obstacle to extending these results by examining the relationship between health literacy and spending is the lack of data containing measures of both. Some insight about the impact of health literacy on costs can be gleaned from studies that examine the impact of years of schooling on medical costs, but health literacy is a fundamentally different concept from educational attainment (Davis et al., 1994; Stedman and Kaestle, 1991). At least one study has examined the association between general literacy and costs (Weiss et al., 1994). It found no relationship, though the sample size was small (N = 402) and not representative of the overall U.S. population (over half the study subjects qualified for Medicaid because of disability). Furthermore, inpatient and outpatient costs were not analyzed separately and the analysis did not control for confounding patient characteristics. Another paper by the same author (Weiss) shows large differences in costs by grade reading level in a Medicaid population (Weiss, 1999), but descriptions of the methods and data are not available. This study examines the relationship between health literacy and costs using a unique dataset combining cost information from an administrative claims file and a health literacy measure from a beneficiary survey. Multivariate techniques are used to adjust for underlying differences in respondents’ characteristics.
Data Description
Health literacy data were collected as part of a survey of persons enrolling in a Prudential Medicare health maintenance organization between December of 1996 and August of 1997 in one of four locations: Cleveland, Ohio; Houston, Texas; South Florida (including Fort Lauderdale, Miami, and nearby areas); and Tampa, Florida. New Prudential Medicare members were contacted three months after enrollment, and those meeting the eligibility criterion were asked to complete an in-person survey. In order to be included in the study, members had to be comfortable speaking either English or Spanish, living in the community, and possess adequate visual and cognitive function. The survey included the Short Test of Functional
Health Literacy in Adults (S-TOFHLA) (Parker et al., 1995), a series of questions designed to measure health literacy. A detailed description of the survey and data has been published elsewhere (Gazmararian et al., 1999).
Prudential administrative claims databases were used to compute annual health expenditures from the date of enrollment for all eligible enrollees by site of service (inpatient, outpatient, emergency room, and pharmacy). The claims database includes costs for all medical services used by enrollees associated with insurance reimbursement. The cost for each service is the sum of Prudential’s reimbursement and the beneficiary’s out-of-pocket payment.
Table B-1 presents evidence on how closely the study sample represents the U.S. population of health-care consumers. The first column of the table presents summary statistics for the 3,260 responders, the second for the 3,245 nonresponders, and the third for participants of comparable age in the household component of the 1997 Medical Expenditure Panel Survey (MEPS) (for a description see Cohen et al., 1996–1997). Differences between samples were assessed using one-way analysis of variance (ANOVA) tests by group for three-sample comparisons of continuous variables and chi-squared tests for two-sample comparisons of binary variables. ANOVA tests for differences in the cost variables were performed on the natural
TABLE B-1 Representativeness of the Study Sample
logarithm of costs to make the variable conform to the normality assumption underlying the F-test.
Compared to nonresponders and the MEPS sample, responders incurred higher inpatient, outpatient, emergency room, and pharmacy expenditures. There were also small differences in average age (0.5 years) and the proportion with more than 12 years of schooling. Compared to MEPS respondents, Prudential respondents were less likely to need assistance with at least one activity of daily living but more likely to need assistance with at least one instrumental activity of daily living. Differences in survey administration may account for some of these inconsistencies (Wiener et al., 1990).
Spending differences between the Prudential population and the MEPS sample, which is nationally representative, may reflect the fact that study participants reside primarily in large urban areas, where reimbursement rates tend to be higher. South Florida, one of the locales from which respondents were drawn, is known to have the highest level of per beneficiary Medicare spending in the country (Center for Evaluative Clinical Sciences, 1998). The study population may also differ in health status. While Medicare managed care plans tend to enroll a healthier mix of beneficiaries compared to the traditional Medicare program (Hellinger and Wong, 2000), managed care plans that offer generous prescription drug coverage or require little in the way of cost-sharing may attract beneficiaries with chronic conditions. A final explanation for the cost differences is that MEPS fails to capture a large portion of spending for Medicare beneficiaries due to restrictive sampling criteria (Selden et al., 2001).
Raw S-TOFLHA score were converted to a discreet categorical variable for purposes of analysis (Baker et al., 1999). Persons scoring 67 and above on the S-TOFHLA were classified as having “adequate” health literacy and those scoring 66 or below were classified as having “inadequate” health literacy. Previous studies have distinguished between a “marginal” health literacy group, with scores between 56 and 66, and an “inadequate” group, with scores 55 or below (Baker et al., 2000). This study combined data from the marginal and inadequate groups to increase statistical power, as no significant cost differences were found between these two groups in preliminary analyses.
Table B-2 displays detailed summary statistics by health literacy level for the responders. Differences between groups were assessed using chisquared tests for binary variables and t-tests for continuous variables. Persons with inadequate health literacy had lower incomes and fewer years of schooling. More Caucasian subjects had adequate than inadequate health literacy, while more African Americans and Spanish-speaking Hispanics had inadequate health literacy. Physical and mental quality-of-life, as mea-
TABLE B-2 Characteristics of the Study Sample
sured by SF-12 scores (Ware et al., 1996) and chronic condition indicators, were higher in those with inadequate health literacy, indicating worse health status overall. Somewhat surprisingly, persons with inadequate health literacy are less likely to smoke or have smoked previously and less likely to consume alcohol.
Statistical Analysis
Costs by site of service were compared between the adequate and inadequate health literacy groups using a two-part regression model of medical spending. The two-part model is the standard statistical framework in empirical health economics for measuring the impact an individual characteristic on medical costs (Diehr et al., 1999). It is designed to account for the unique distribution of medical spending found in most samples; a sizeable minority of individuals do not use medical care, many use small amounts, and a few individuals incur substantial medical bills that account for a large percentage of aggregate spending. Because of the highly skewed distribution and presence of a large number of “0” values, standard statistical methods that assume the dependent variable is normally distributed yield inaccurate predictions of costs (Duan et al., 1983). The two-part model attempts to more accurately mimic the empirical distribution of medical spending by splitting the distribution into two parts and allowing the impact of independent variables, such as health literacy, on the probability of using medical care to be independent of their impact on the costs of medical care for those who use it.
The first stage of the model measures the probability of using medical care as a function of individual characteristics. Typically, logitistic or probit regression is used, where the dependent variable equals one if costs are strictly positive and zero otherwise. Probit (or probability unit) regression was used in this case. Health literacy was included as an independent variable, along with controls for age, sex, race, income, schooling, smoking, and alcohol consumption. The second stage of the model estimates the relationship between independent variables and costs among those who use medical care. Parameters are estimated via least squares regression, where the dependent variable is the logarithm of costs and the independent variables are the same as in the first stage but the sample includes only individuals who received care (i.e., those with strictly positive values for the relevant cost category).
Coefficient estimates for the two-part model are difficult to interpret in isolation, since the dependent variable of the second stage is in log, rather than constant, dollars, and it is customary to state results in terms of predicted spending levels. These are constructed by computing predicted probabilities from the first stage and then multiplying these predicted probabilities by the exponentiated second-stage predicted values and a “smearing factor” (Duan, 1983), which is needed to transform logged dollars back to constant dollars, and averaging the predicted spending levels over the entire sample. Transforming log to constant dollars via this method may produce misleading results if the variance of spending in the upper part of the distribution differs from the variance in the lower part (Manning, 1998).
To address this issue, costs were also analyzed using the modified two-part model proposed by Mullahy (1998). In this model, the first stage is the same as in the standard two-part model, but the second stage is a nonlinear equation where cost equals the exponentiated sum of dependent variables and coefficients. This modified two-part model produced estimates within 5 percent of the predicted values from the standard two-part model. Therefore, only the results from the standard two-part model are presented below.
Two values are used to summarize the effect of a binary independent variable on spending. The first is the average predicted spending level with the variable indicating inadequate health literacy set equal to zero for every respondent; the second is the average predicted spending level with the health literacy variable set equal to one. Computed predicted values in this manner nets out the impact of observable individual characteristics, such as age, on spending.
Confidence intervals for predicted values were computed via simulation; the first- and second-stage coefficients were drawn from their respective multivariate normal distributions and predicted values were computed following the steps outlined above. Repeating this routine 1,000 times produced distributions of predicted values, and the lower and upper bounds of the confidence intervals were set equal to the 2.5th percentiles and the 97.5th percentiles of the distributions, respectively.
Two models were estimated. The first (or basic) model includes controls for sex, age, income, schooling, smoking, and alcohol consumption. The second includes additional controls for physical and mental status (from the SF-12) and chronic conditions (high blood pressure, arthritis, and depression). This model does not include the 66 observations for which no physical or mental health SF-12 scores were reported, for a sample of 3,192 observations (= 3,260–66).
Results
Results from the two-part model are displayed in Table B-3. Inpatient costs are the largest component of total medical spending. Predicted inpatient spending for persons with inadequate health literacy is $993 higher than that of persons with adequate health literacy (difference in raw means: $1,859). Controlling for health status, predicted inpatient spending for persons with inadequate health literacy is about $450 higher than that of persons with adequate health literacy. The confidence intervals for inpatient spending from the basic model overlap slightly, while the confidence intervals for inpatient spending from the model that includes controls for health status display a greater degree of overlap. Examining separately the results from each stage of the two-part model helps illuminate the reasons
TABLE B-3 Predicted Health-Care Spending
for spending differences. According to the first part of the two-part model for inpatient spending (results not shown; complete regression results are available from the author upon request), persons with inadequate health literacy are more likely to use inpatient services (p < 0.05), but, among those who used inpatient care, spending did not differ by health literacy status.
In contrast to the results for inpatient spending, the predicted outpatient spending level from the basic model for persons with adequate health literacy is higher than the predicted value for persons with inadequate health literacy. Predicted spending on emergency room care is lower for persons with adequate health literacy, while the predicted values for pharmacy spending from the basic model are comparable.
These results are shown in terms of total spending by the study sample in Table B-4. The first column shows predicted total spending under the assumption that the proportion of individuals with adequate health literacy is 64 percent, the actual proportion in the study sample. The second column shows predicted total spending under the assumption that the proportion of individuals with adequate health literacy is 100 percent, representing the maximum attainable level of health literacy in the population.
TABLE B-4 In-Sample Prediction of Health Literacy and Total Costs
|
|
Percent with Adequate Literacy |
|
|
|
|
64% (actual) |
100% |
Difference |
|
Inpatient |
17,877,000 |
$16,616,000 |
$1,261,000 |
|
Outpatient |
6,079,400 |
$6,227,300 |
($147,900) |
|
Emergency room |
438,480 |
$359,910 |
$78,570 |
|
Pharmacy |
$2,263,400 |
$2,277,700 |
($14,300) |
|
NOTE: Difference column displays the mean cost in the inadequate column subtracted from the mean cost in the adequate column. Negative values are in parentheses. |
|||
Discussion
When assessing the causality of the results presented in Tables B-3 and B-4, it is important know whether health literacy, like ethnicity, is a constant, fixed characteristic of individuals or, like income, is associated with changes in health. Health literacy declines sharply with age in the study cohort (Baker et al., 2000), suggesting the latter. If so, then the relationship between health and health literacy is bidirectional; health literacy affects health and vice versa. To take an extreme example, an individual who experiences a severe stroke may lose the ability to read. It would be incorrect in such a case to attribute the costs associated with post-stroke care to illiteracy, since the stroke caused illiteracy and not the other way around. Controlling for health status, as is done in the extended model, removes the effect of health on health literacy but also removes the effect of health literacy on disease incidence, leading to estimates of the impact of health literacy on spending that are systematically lower than the true effect. Declines in health literacy by age are unrelated to the onset of chronic conditions (Baker et al., 2000), suggesting that the bias due to reverse causality is not large. Nevertheless, future studies could address this issue by taking two or more measurements of health literacy from the same respondent at different points in time.
Another caveat to this study is that though the analysis included fairly extensive controls for individual characteristics, including income, education, smoking, and alcohol consumption, there still may be unobserved individual characteristics correlated with both health literacy and spending that confound the results. For example, if individuals with low health literacy are also distrustful of the medical care system and are reluctant to seek medical attention, then the results will understate the impact of health literacy on costs.
Some insight on the validity of these results may be gained by examining differences in spending by site of service. Studies have shown that patients with low levels of health literacy receive fewer preventive services (Lindau et al., 2002; Scott et al., 2002), frequently fail to follow medication instructions (Andrus and Roth, 2002), and have worse health outcomes (Schillinger et al., 2002). The results of this study are consistent with these findings; individuals with inadequate health literacy make greater use of services designed to treat complications and advanced cases of disease, as indicated by higher spending for inpatient and emergency room care. Simultaneously, they use fewer services designed to manage disease, as evidenced by lower spending for outpatient care.
In conclusion, these results lend support to the hypothesis that individuals with low levels of health literacy incur higher medical costs, but, because of the limitations discussed above, no definitive conclusions can be drawn from the analysis. Results were sensitive to the inclusion of controls for health status, and the confidence intervals around predicted inpatient spending from the basic model overlapped by a small amount. Although it is impossible to prove causality, future studies should take advantage of statistical methods, such as propensity score estimators (Coyte et al., 2000; Rubin, 1997), designed to estimate treatment effects efficiently and the diagnostic information contained on claims to determine if expenditures are higher for persons with the conditions thought to be most responsive to patient knowledge. Data with repeated measurements of health literacy over time would also be helpful, especially for assessing the responsiveness of health literacy to health. For the time being, researchers should be cautious in terms of justifying interventions to improve health literacy based on potential cost savings.
REFERENCES
Andrus MR, Roth MT. 2002. Health literacy: A review. Pharmacotherapy. 22(3): 282–302.
Baker DW, Parker RM, Williams MV, Clark WS. 1998. Health literacy and the risk of hospital admission. Journal of General Internal Medicine. 13(12): 791–798.
Baker DW, Williams MV, Parker RM, Gazmararian JA, Nurss J. 1999. Development of a brief test to measure functional health literacy. Patient Education and Counseling. 38: 33–42.
Baker DW, Gazmararian JA, Sudano J, Patterson M. 2000. The association between age and health literacy among elderly persons. Journals of Gerontology Series B—Psychological Sciences & Social Sciences. 55B(6): S368–S374.
Baker DW, Gazmararian JA, Williams MV, Scott T, Parker RM, Green D, Ren J, Peel J. 2002. Functional health literacy and the risk of hospital admission among Medicare managed care enrollees. American Journal of Public Health. 92(8): 1278–1283.
Center for Evaluative Clinical Sciences. 1998. The Dartmouth Atlas of Health Care. Chicago, IL: American Hospital Publishing.
Cohen JW, Monheit AC, Beauregard KM, Cohen SB, Lefkowitz DC, Potter DE, Sommers JP, Taylor AK, Arnett RH 3rd. 1996–1997. The Medical Expenditure Panel Survey: A national health information resource. Inquiry. 33(4): 373–389.
Coyte PC, Young W, Croxford R. 2000. Costs and outcomes associated with alternative discharge strategies following joint replacement surgery: Analysis of an observational study using a propensity score. Journal of Health Economics. 19(6): 907–929.
Davis TC, Mayeaux EJ, Fredrickson D, Bocchini JA Jr, Jackson RH, Murphy PW. 1994. Reading ability of parents compared with reading level of pediatric patient education materials. Pediatrics. 93(3): 460–468.
Diehr P, Yanez D, Ash A, Hornbrook M, Lin DY. 1999. Methods for analyzing health care utilization and costs. Annual Review of Public Health. 20: 125–144.
Duan N. 1983. Smearing estimate: A nonparametric retransformation method. Journal of the American Statistical Association. 78: 605–610.
Duan N, Manning WG Jr, Morris CN, Newhouse JP. 1983. A comparison of alternative models for the demand for medical care. Journal of Business and Economic Statistics. 1: 115–126.
Gazmararian JA, Baker DW, Williams MV, Parker RM, Scott TL, Green DC, Fehrenbach SN, Ren J, Koplan JP. 1999. Health literacy among Medicare enrollees in a managed care organization. Journal of the American Medical Association. 281(6): 545–551.
Hellinger FJ, Wong HS. 2000. Selection bias in HMOs: A review of the evidence. Medical Care Research and Review. 57(4): 405–439.
Lindau ST, Tomori C, Lyons T, Langseth L, Bennett CL, Garcia P. 2002. The association of health literacy with cervical cancer prevention knowledge and health behaviors in a multiethnic cohort of women. American Journal of Obstetrics & Gynecology. 186(5): 938–943.
Manning WG. 1998. Much ado about two: Reconsidering retransformation and the two-part model in health economics. Journal of Health Economics. 48: 375–391.
Mullahy J. 1998. Much ado about two: Reconsidering retransformation and the two-part model in health econometrics. Journal of Health Economics. 17(3): 247–281.
Parker RM, Baker DW, Williams MV, Nurss JR. 1995. The Test of Functional Health Literacy in Adults: A new instrument for measuring patients’ literacy skills. Journal of General Internal Medicine. 10(10): 537–541.
Rubin DB. 1997. Estimating causal effects from large data sets using propensity scores. Annals of Internal Medicine. 127(8 Pt 2): 757–763.
Schillinger D, Grumbach K, Piette J, Wang F, Osmond D, Daher C, Palacios J, Sullivan GAD, Bindman AB. 2002. Association of health literacy with diabetes outcomes. Journal of the American Medical Association. 288(4): 475–482.
Scott TL, Gazmararian JA, Williams MV, Baker DW. 2002. Health literacy and preventive health care use among Medicare enrollees in a managed care organization. Medical Care. 40(5): 395–404.
Selden TM, Levit KR, Cohen JW, Zuvekas SH, Moeller JF, McKusick D, Arnett RH 3rd. 2001. Reconciling medical expenditure estimates from the MEPS and the NHA, 1996. Health Care Financing Review. 23(1): 161–178.
Stedman L, Kaestle C. 1991. Literacy and Reading Performance in the United States from 1880 to Present. New Haven, CT: Yale University Press. Pp. 75–128.
Ware J Jr, Kosinski M, Keller SD. 1996. A 12-Item Short-Form Health Survey: Construction of scales and preliminary tests of reliability and validity. Medical Care. 34(3): 220–233.
Weiss BD. 1999. How common is low literacy? In: 20 Common Problems in Primary Care. Weiss BD, Editor. New York: McGraw-Hill. Pp. 468–481.
Weiss BD, Blanchard JS, McGee DL, Hart G, Warren B, Burgoon M, Smith KJ. 1994. Illiteracy among Medicaid recipients and its relationship to health care costs. Journal of Health Care for the Poor & Underserved. 5(2): 99–111.
Wiener JM, Hanley RJ, Clark R, Van Nostrand JF. 1990. Measuring the activities of daily living: Comparisons across national surveys. Journal of Gerontology. 45(6): S229–S237.
Improving Chronic Disease Care for Populations with Limited Health Literacy
Dean Schillinger, M.D.
The problem with communication is the assumption that it has occurred.
—George Bernard Shaw
Introduction
Chronic disease management is one of the major challenges facing health-care systems and patients in industrialized nations. Nearly three-quarters of all health-care resources are devoted to the treatment of chronic diseases, and nearly one-half of the U.S. population has one or more chronic condition (Institute for Health and Aging, 1996). The collaboration between the system of care, providers, patients, and the community to provide the best health outcomes adds a layer of complexity to the delivery of health care to individuals with chronic disease. Effective disease management is based on systematic, interactive communication between patients and the providers and health system with whom they interact (Norris et al., 2002a, b; Von Korff et al., 1997), all occurring in the context of a community whose resources meet patients’ needs (Wagner, 1995).
This paper uses the definition of disease management provided by the Task Force on Community Preventive Services, a nonfederal Task Force convened in 1996 by the Department of Health and Human Services (HHS) to provide leadership in the evaluation of community, population, and health-care system strategies to address a variety of public health and health promotion topics, and appointed by the Director of the Centers for Disease Control and Prevention (Norris et al., 2002a, b). Disease management is an organized, proactive, multicomponent approach to health-care delivery that involves all members of a population with a specific disease, is focused on the spectrum of the disease and its complications (including the prevention of co-morbid conditions), and is integrated across the relevant aspects of the delivery system.
The last few decades have seen tremendous advances in the care of chronic conditions, including an array of new therapeutic options, risk-factor modification for secondary prevention of co-morbid conditions, the availability of home monitoring tools, and the growth of disease manage-
The research reported herein was supported, in part, through grants from the National Center for Research Resources (K-23 RR16539), the Soros Open Society Institute, and The Commonwealth Fund.
ment programs (Bodenheimer, 1999; Diabetes Control and Complications Trial Research Group, 1993, 1996; McCulloch et al., 2000; United Kingdom Prospective Diabetes Study Group, 1998). Despite these advances, health quality and clinical outcomes of patients with chronic diseases vary across sociodemographic lines (American Diabetes Association, 1998; CDC, 2000; Fiscella et al., 2000; Piette, 1999; Vinicor et al., 2000). Much of the burden of chronic disease falls on the elderly and those of low socioeconomic status, populations that have also been shown to have disproportionately high rates of health literacy problems (Gazmararian et al., 1999a; Williams et al., 1995b). It is increasingly apparent that the health-care system has not evolved to serve those with limited health literacy. The prevalence of limited health literacy, compounded by a health-care system in which scientific advances and market forces place greater technical and self-management demands on patients and their families, may help to create unequal outcomes despite what some consider equal access (IOM, 2001, 2003).
There currently is a lack of precision and uniformity regarding the meaning of the term “health literacy” (American Medical Association, 1999; Davis et al., 1991; HHS, 2000; Nutbeam, 2000) and little consensus as to the extent to which literacy equates with health literacy (see Chapter 2 in this report). There is general agreement, however, that (1) literacy and numeracy skills are deeply embedded in the construct of health literacy and (2) the problems associated with having limited health literacy are most intense for those individuals with limited literacy skills. The ensuing discussion in this chapter is based on these two assumptions.
The purpose of this article is to (1) briefly review the elements of the most well-accepted model to restructure chronic disease care delivery, the Chronic Care Model of Wagner and others (1995), (2) describe the ways in which limited health literacy may lead to worse chronic disease outcomes, (3) use the Chronic Care Model to consider opportunities to reduce health literacy-related disparities, and (4) reflect on strategies to develop quality-of-care indicators to promote improvement in chronic disease care for patients with limited health literacy.
The Chronic Care Model
Health-care delivery is poorly organized to meet the needs of patients with chronic diseases. Rushed practitioners find it difficult to follow established practice guidelines, limited coordination hampers multidisciplinary care, inadequate training leaves many patients ill-equipped to manage their illnesses, and lack of active follow-up leads to preventable deterioration in function. Some managed care organizations and integrated delivery systems have attempted to correct deficiencies in management of chronic diseases.
To guide the reorganization of chronic disease care, Dr. Ed Wagner and others developed the Chronic Care Model (see Figure B-1), which summarizes the basic elements for improving care in health systems at multiple levels (Wagner, 1998, 2003). These include the health system, health-care delivery system design, decision support, clinical information systems, the community, and self-management support. For example, a community that has the infrastructure and resources to facilitate patients’ self-care activities (transportation to appointments, safe recreational spaces for exercise, adequate produce for healthy food choices, opportunities for educational or communal engagement); a health system that trains patients to be active participants through self-management educational activities (such as group medical visits or other organized, skill-building activities); a clinic that restructures its care delivery through multidisciplinary teams, planned visits, or home visits; or a practice that uses disease registries to track patients’ progress, stratify intensity of care, promote outreach, and maintain continuity—all would represent efforts consistent with the Chronic Care Model. Focusing on these components could foster interactions between patients
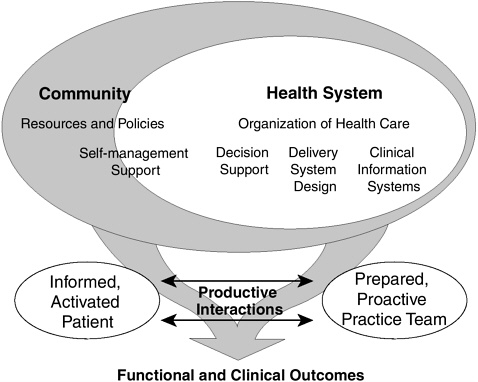
FIGURE B-1 Model for improvement of chronic illness care.
SOURCE: Wagner (1998). Reprinted with permission of the American College of Physicians.
who take an active part in their care and providers who are backed up by resources and expertise. The Chronic Care Model integrates the published evidence in chronic disease management, including the importance of executive leadership and incentives to promote quality, systems to track and monitor patients’ progress and support timely provider decision-making (Piette, 2000), patient self-management training (Lorig et al., 1999; Von Korff et al., 1997), and community-oriented care. Patients and providers prepared in these ways are likely more able to engage in productive interactions that promote system efficiency and patient well-being (Norris et al., 2002a).
A growing body of research demonstrates that self-management practices and clinical outcomes in chronic disease care vary by patients’ level of health literacy (Kalichman and Rompa, 2000; Schillinger et al., 2002; Williams et al., 1998b). The Chronic Care Model and similar comprehensive, population-based disease management approaches may offer insights into the ways in which limited health literacy affects chronic disease care and identify potential points of intervention. Preliminary evidence from a small randomized trial suggests that disease management strategies can reduce health literacy-related disparities in diabetes care (Rothman et al., 2003) and that tailoring communication to those with limited health literacy might affect outcomes in chronic anticoagulation and diabetes care (Schillinger et al., 2002, 2003b). However, we were unable to locate published results of any comprehensive disease management systems specifically designed to improve chronic disease care for individuals with limited health literacy. Developing such a system would likely benefit not only those with limited health literacy, but all chronic disease patients, as many of the barriers faced by those with limited health literacy are also experienced, albeit it a somewhat lesser extent, by those with adequate health literacy.
How Limited Health Literacy Affects Chronic Disease Outcomes
Limited health literacy has been shown to be associated with worse health status (Weiss et al., 1992), higher utilization of services (Baker et al., 1997, 1998) and worse clinical outcomes (Kalichman and Rompa, 2000; Schillinger et al., 2002). Whether limited health literacy is a marker for other determinants of health, such as socioeconomic status, or is in the causal pathway to poor health is currently a matter of some debate. For chronic disease care, which relies on self-management, self-advocacy, ongoing monitoring, and interactive communication, it is reasonable to hypothesize that health literacy may be one determinant of health outcomes.
Limited health literacy may affect many aspects of chronic disease care. It may influence the interaction between provider and patient, impact the ability of the health system to communicate successfully with the patient,
and affect the availability of community resources for chronic disease patients and their families (Figure B-2). By reviewing this framework, we can begin to generate a set of priorities for targeted study and intervention that reflects a blending of what we have learned from the Chronic Care Model and what is known about empowering low-literacy adults from the field of adult education (Roter et al., 1998, 2001).
Office-Based Clinician–Patient Communication
Much of chronic disease care takes place in the context of a medical office visit. Communication about chronic diseases during outpatient visits may be hampered by several factors. These include the relative infrequency and brevity of visits, language barriers and limited literacy, differences between providers’ and patients’ agendas and communication styles, lack
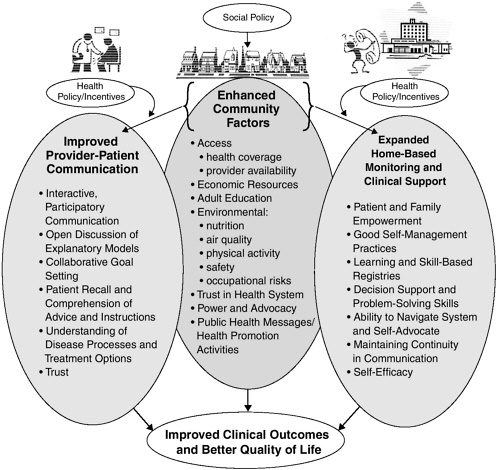
FIGURE B-2 Improving chronic disease care: a framework based on health literacy and related research.
of trust between the patient and provider, overriding or competing clinical problems, lack of timeliness of the visit in relation to disease-specific problems, and the complexity and variability of patients’ reporting of symptoms and progress of their disease.
Patients with chronic diseases and limited health literacy have been shown to have less knowledge of their condition and of its management (Williams et al., 1998a, b) often despite having received standard self-management education. Patients with limited health literacy have greater difficulties accurately reporting their medication regimens and describing the reasons for which their medications were prescribed (Schillinger et al., 2003b; Williams et al., 1995a; Win and Schillinger, 2003) and more frequently have explanatory models that may interfere with adherence (Kalichman et al., 1999). While patients with limited health literacy clearly have problems with literacy and numeracy skills in the health-care setting, patients also experience difficulties with oral communication. A recent study among patients with diabetes demonstrated that those patients with limited health literacy (as measured by the Short Test of Functional Health Literacy in Adults [S-TOFHLA] [Nurss et al., 1995]) appear to have particular problems with both the decision-making and the explanatory, technical components of dialogue (Schillinger et al., 2004). Patients with limited health literacy may also be less likely to challenge, ask questions of the provider (Baker et al., 1996; Street, 1991), or disclose poor understanding (Baker et al., 1996), and may cope by being passive or appearing uninterested (Cooper and Roter, 2003; Roter, 2000; Roter and Hall, 1992; Roter et al., 1997). Clinicians tend to underestimate the information needs of patients (Cegala, 1997) and underuse interactive teaching strategies that may be especially useful for patients with limited health literacy (Schillinger et al., 2003b). Clinicians’ frequent use of jargon in clinical encounters may be particularly problematic for patients with limited health literacy. This jargon can range from technical jargon (words that have meaning only in the clinical context, e.g., “glucometer”), quantitative jargon (words for which clinical judgment is required to accurately interpret, e.g., “excessive wheezing”), to lay jargon (words for which two meanings exist, one with clinical meaning and the other with lay meaning, e.g., “your weight is stable”). Clinicians are often unaware of the mismatch between their process of giving information and patients’ process of recalling, understanding, and acting on the information (Davis et al., 2002b; Doak et al., 1998; Williams et al., 2002).
Home-Based Monitoring and Clinical Support
Chronic care involves an ongoing process of patient assessments, adjustments to treatment plans, and reassessments to measure change in pa-
tient health status. Without timely and reliable information about patients’ health status, symptoms, and self-care, the necessary health education, treatments, or behavioral adjustments may come late or not at all. This can compromise patients’ health and increase the likelihood of poor outcomes.
To best manage chronic disease, patients must remember any self-care instructions they have received from their provider, be able to correctly interpret symptoms or results of self-monitoring, and appropriately solve problems regarding adjustments to the treatment regimen, as well as when and how to contact the provider should the need arise. A number of studies demonstrate that patients remember and understand as little as half of what they are told by their physicians (Bertakis, 1977; Cole and Bird, 2000; Crane, 1997; Rost and Roter, 1987; Roter, 2000) and the more information provided, the less the patient is able to recall (Chow, 2003). Patients with limited health literacy are likely to understand and remember at even lower rates (Schillinger et al., 2004). In addition, they may be less equipped to overcome gaps when they are at home due to knowledge deficits (Williams et al., 1998a, b) and difficulties reading or interpreting instructions (Crane, 1997; Williams et al., 1998b). Cross-sectional studies involving patients with diabetes suggest that traditional self-management education may not eliminate health literacy-related disparities in chronic disease outcomes (Schillinger et al., 2002; Williams et al., 1998b).
Only a minority of clinical practices provide any form of care management that involves outreach and support in the patient’s home (Casalino et al., 2003). In addition, home-based disease-specific education, monitoring, and clinical support increasingly rely on patients and providers interacting via web-based or “e-health” interfaces (Robert Wood Johnson Foundation and the National Cancer Institute, 2002). While these interfaces have been suggested as a potential method of increasing interaction between patients and providers (Robert Wood Johnson Foundation and the National Cancer Institute, 2002), they may present overwhelming barriers to patients with limited health literacy. Individuals with limited health literacy may have trouble accessing the web (Fox and Fallows, 2003), difficulties reading from web sites (Berland et al., 2001), and problems with navigation once they get online (Robert Wood Johnson Foundation, 2002; Zarcadoolas et al., 2002). Accreditation of health-related web sites (such as the Health on the Net Foundation Code of Conduct) does little to improve readability of diabetes web sites (Kusec et al., 2003).
Simply transforming text versions of disease-specific education to more visually oriented media (i.e., CD-ROM), while associated with improvements in satisfaction, does not appear to increase knowledge among patients with limited health literacy (Kim et al., 2001). Focus groups of patients with limited health literacy have identified health system navigation (finding resources within the health system, such as knowing whom, for
what, and when to call for assistance with a problem) as a particularly daunting aspect of chronic disease management (Baker et al., 1996).
Community and Environmental Factors
Data from the National Adult Literacy Survey (Kirsch, 1993) demonstrate regional variation in literacy rates that parallels neighborhood patterns of socioeconomic status, immigrant status, age, and race and ethnicity. Studies in health-care settings (Gazmararian et al., 1999b; Williams et al., 1995b) indicate that patients with limited health literacy comprise a large sector of patients in public hospitals and community clinics that predominantly serve socioeconomically disadvantaged populations, and in private health systems that serve the elderly or those with low incomes, such as Medicare and Medicaid managed care organizations. Little work has been done exploring the relationship between limited health literacy and neighborhood characteristics, particularly those of direct relevance to chronic disease management. Recent work from social epidemiology (Berkman and Kawachi, 2000) and literacy theory (Wallerstein and Bernstein, 1988) can inform how community factors can either assist or hamper disease management efforts for patients with limited health literacy. Communities that have high rates of limited health literacy may be less able to assert political power and advocate for the health and health-care needs of their community (Nutbeam, 2000). Residents of medically underserved areas experience greater difficulties accessing a regular source of health care, a problem that has been shown to be associated with preventable hospitalizations for chronic conditions (Bindman et al., 1995). Other environmental attributes of communities, such as the availability of goods and services that promote health, the quality of the air and recreational physical space, and occupational risks associated with neighborhood employment may each interact with limited health literacy to lead to worse health. In addition, recent studies examining disparities in quality of care demonstrate racial and ethnic differences in level of trust in the health-care system that may influence how these communities interact with the health-care system (IOM, 2003). Finally, the focus of health promotion messages and activities that take place at the community level may not be aligned with the needs of patients with limited health literacy (Nutbeam, 2000).
Shaping the Chronic Care Model for Patients with Limited Health Literacy
One of the underlying assumptions of the Chronic Care Model is that the reorganization of health care will lead to more productive interactions between informed, involved patients, and prepared, proactive practice
teams, which will, in turn, lead to better outcomes (Figure B-1). In order for this assumption to hold for populations with limited health literacy, we need to think more critically about the ways in which we communicate across the levels described above to ensure that interactions indeed are productive. If we apply the Chronic Care Model without also attending to the unique challenges to chronic disease management posed by limited health literacy, we may improve care for many but run the risk of perpetuating disparities in outcomes for those with limited health literacy.
In order to engage in more productive interactions with patients who have limited health literacy, solutions must primarily affect the nature, quality, and extent of communication. Previous research indicates patients want practical, concise information focused on the identification of the problem, what specifically the patient needs to do, why it is in their best interest, and what outcomes they can expect (Davis et al., 2001, 2002a, b). Communication strategies commonly employed by health professionals are often only marginally effective for those with limited health literacy. At present, clinicians do not have the means to uncover how patients learn best, nor the tools to more effectively engage patients who do not appear to be maximally benefiting from clinical interactions. In order to support patients’ acquisition of self-management skills and increase confidence to carry out self-management tasks, efforts should be made to develop tools to assess how patients learn in the clinical setting, and to expand the repertoire of options to match patients’ learning style or preferences. Some principles derived from the field of adult education may be relevant to chronic disease communication (Brookfield, 1986; Roter et al., 2001; Wallerstein, 1992). Learners (patients) should be involved in developing health education messages, materials, and programs (Davis et al., 1998a, b; Rudd and Comings, 1994). Learning should be participatory; patients should be actively involved in setting the agenda or curriculum and, at times, even leading it so as to ensure relevance (relating and reflecting on experience), encourage ongoing involvement, promote the development of behavior change through critical thinking (thoughtful action), and support other learners to succeed. This involvement will help ensure the education is relevant, understandable, culturally sensitive, and empowering. Interactions should involve exploration and problem-based learning (Cooper et al., 2003). Patient education activities should be designed so as to engage patients in ways relevant to their lives and their conditions and that enhance problem-solving skills (Center for Literacy Studies, 2003). Such activities educational focus may lead to patient-generated goal-setting, an important intermediate objective in successful chronic disease care (Anderson, 1995; Anderson et al., 1995). Group medical visits, an innovation in which groups of patients who share a common condition regularly meet with a health provider, have the potential to operate via these principles. Results of a small trial with diabetes
patients suggests that, when designed with the collaboration of an expert in adult education, such visits can dramatically improve outcomes (Trento et al., 2001, 2002).
As chronic disease education, monitoring, and clinical support move beyond the office walls to include e-health and other forms of telemedicine, it is critical that patients with limited health literacy are not left behind (Robert Wood Johnson Foundation and the National Cancer Institute, 2002). Individuals with limited health literacy must be involved in all stages of intervention design and testing. This participatory development method allows for input during the generative phase of an intervention, provides opportunities for feedback during multiple points of pilot testing, and can engender trust and participation during the evaluation phase (Houts et al., 1998; Jacobson et al., 1999). As an example, our recent work at San Francisco General Hospital involves the development of an automated telephone diabetes management system for patients with limited health literacy. The idea for a telephone-based intervention was generated, in part, from patients. The program was developed with the active involvement of adult learners and patients with limited health literacy, which significantly altered numerous aspects of the program. Patients wanted to hear that we are actively listening and care about their well-being. They preferred narrative instead of instruction-based health education. Patients recommended we reduce the speed with which messages are delivered and limit the amount of technical language in order to make the messages more understandable. We are currently evaluating the effect of this system on diabetes-related outcomes.
If all patients with chronic diseases are to benefit from emerging technologies, particularly interventions that involve the Internet, research must explore how to best design such programs for patients with limited health literacy (Robert Wood Johnson Foundation and the National Cancer Institute, 2002). Such research will also require professional collaboration between disciplines such as computer science, health communication, education, economics, marketing, sociology, and library and information science.
If we are to redesign the health-care delivery system and better support patients in their self-management, it is important to recognize the needs that patients with limited health literacy have expressed with regards to system navigation. We must better understand the elements of successful system navigation and apply this understanding to support patients’ navigation and self-advocacy skills, and better equip patients to get what they need from a complex system. We need to partner with patients with limited health literacy to identify those aspects of the system that represent bottle-necks and to design solutions that lower such barriers.
A crucial component to reducing the burden of limited health literacy lies with the providers of health care. In order to boost provider prepared-
ness, we need to prime the workforce to more effectively care for patients who have chronic diseases and limited health literacy. Training of all health professionals that focuses on communication strategies to enhance clinician self-awareness (Frankel and Stein, 2001), mutual learning, partnership-building, collaborative goal-setting, and behavior change for chronic disease patients is essential (Wagner, 2003; Youmans and Schillinger, 2003). Such training should be expanded to include all members of the multidisciplinary health team, including lay health educators, both as learners and teachers. These efforts must be informed by new health communication research that involves patients with limited health literacy, a segment often under-represented in clinical research.
Community efforts should focus on developing relationships that foster trust, providing resources to measure and meet community needs, and ultimately preparing members of a community to effectively advocate for the needs of their community (Figueroa et al., 2002). Public health messages should take into account the health literacy skills of the population to whom the message is being targeted, involve the population from the beginning, and make use of appropriate channels to convey these messages (Bird et al., 1998).
Measuring Progress
In order to promote progress in chronic care delivery for patients with limited health literacy, quality-of-care measures must be designed to capture health literacy-related performance. If incentives are aligned to improve quality, such measures of health-care quality can, in turn, lead to the creation of standards of care and improve practice. There are several possible approaches to measuring the extent to which health systems are meeting the needs of patients with limited health literacy. An indirect approach, advocated by those involved in initiatives to reduce racial and ethnic disparities in quality of care (IOM, 2003; Sehgal, 2003) is to use existing measures of quality, such as Medicaid Health Plan Employer Data and Information Set indicators (that currently do not include any health literacy-specific indicators), and stratify a system’s performance by race or ethnicity, or, in this case, health literacy level. Such an approach would enable a comparison of performance in process or outcome measures among those with inadequate health literacy in comparison to those with adequate health literacy. A health system can be considered improving if overall performance is improving and if the extent of health literacy-related variation in performance is narrowing over time. The main challenge to this strategy is the complexity involved in measuring health literacy. Current instruments take between 3 and 7 minutes and require inperson administration (Baker et al., 1999). Education level is not a useful
proxy for health literacy, as there is only a modest correlation between education and health literacy. There also are interactions between education and other demographic characteristics (e.g., ethnicity, age, primary language) on health literacy (Beers et al., 2003; Guerra and Shea, 2003). A recent study suggests that a single questionnaire item may have reasonable sensitivity and specificity in detecting inadequate health literacy and appears to perform well if the prevalence of inadequate health literacy in the population is high enough (Chew and Bradley, 2003). In order for a strategy of reducing health literacy-related disparities by measuring health literacy-related quality is to succeed, research to develop a rapid and reliable measure of health literacy is needed.
A second approach is to develop novel measures of quality that may be less disease-specific, yet have particular relevance to patients with limited health literacy across chronic conditions. To our knowledge, relatively little work has been done in this regard. For example, the National Center for Quality Assurance (NCQA) for managed care organizations has created standards regarding the readability of the patient appeal of denial of services form (NCQA, 2003). While arguably of importance, the approach of assessing quality by measuring document readability is obviously narrow in scope, and does not capture a more comprehensive view of the patient experience. Other possibilities include measuring patients’ reports of their experiences of communication (Schillinger et al., 2004), rates of discordance between patients’ and providers’ reports of medication regimens (Schillinger et al., 2003a), the extent to which home monitoring and support for chronic disease is available (Norris et al., 2002b), the range of learning options and media available to patients, the ease with which one can navigate a health system, or capturing the degree to which a health system has a family and community orientation (Starfield, 1998). In order for significant progress to be made, it is essential that research is done to develop appropriate quality indicators for health literacy-related performance.
CONCLUSIONS
Despite wide variation in literacy levels, our society places high literacy demands on its members. It is apparent that attempts to reduce health literacy-related disparities must revolve around either directly addressing the problem of basic literacy and/or creating a health-care system in which the gap between the literacy demands of the system and the literacy skills of the patients it serves is significantly narrowed. Modern chronic disease care requires that patients play an active role in their care, and that clinicians and the health systems in which they work take on the challenge of partnering with patients to promote successful outcomes. Meeting these goals is
often most challenging for those patients who have the greatest need. When considered as a barrier to successful health communication as well as a marker for problems with navigation and self-advocacy, it becomes clear that the concerns related to limited health literacy are inescapably linked to the challenges of chronic disease management. In order to ensure that the Chronic Care Model and increasingly sophisticated chronic disease management programs can benefit patients with limited health literacy, attention must be paid to tailor design and implementation with the involvement of patients with limited health literacy, and to expand the reach of such programs. By promoting meaningful, collaborative communication between patients and the providers and systems that serve them, such a reorganization is likely to benefit all patients with chronic diseases.
REFERENCES
American Diabetes Association. 1998. Economic consequences of diabetes mellitus in the U.S. in 1997. Diabetes Care. 21(2): 296–309.
American Medical Association. 1999. Health literacy: Report of the Council on Scientific Affairs. Ad Hoc Committee on Health Literacy for the Council on Scientific Affairs, American Medical Association. Journal of the American Medical Association. 281(6): 552–557.
Anderson RM. 1995. Patient empowerment and the traditional medical model. A case of irreconcilable differences. Diabetes Care. 18(3): 412–415.
Anderson RM, Funnell MM, Butler PM, Arnold MS, Fitzgerald JT, Feste CC. 1995. Patient empowerment. Results of a randomized controlled trial. Diabetes Care. 18(7): 943–949.
Baker DW, Parker RM, Williams MV, Pitkin K, Parikh NS, Coates W, Imara M. 1996. The health care experience of patients with low literacy. Archives of Family Medicine. 5(6): 329–334.
Baker DW, Parker RM, Williams MV, Clark WS, Nurss J. 1997. The relationship of patient reading ability to self-reported health and use of health services. American Journal of Public Health. 87(6): 1027–1030.
Baker DW, Parker RM, Williams MV, Clark WS. 1998. Health literacy and the risk of hospital admission. Journal of General Internal Medicine. 13(12): 791–798.
Baker DW, Williams MV, Parker RM, Gazmararian JA, Nurss J. 1999. Development of a brief test to measure functional health literacy. Patient Education and Counseling. 38: 33–42.
Beers BB, McDonald VJ, Quistberg DA, Ravenell KL, Asch DA, Shea JA. 2003. Disparities in health literacy between African American and non-African American primary care patients. Journal of General Internal Medicine. 18(S1): 169.
Berkman LF, Kawachi, IO. 2000. Social Epidemiology. Oxford: Oxford University Press.
Berland GK, Elliott MN, Morales LS, Algazy JI, Kravitz RL, Broder MS, Kanouse DE, Munoz JA, Puyol JA, Lara M, Watkins KE, Yang H, McGlynn EA. 2001. Health information on the Internet: Accessibility, quality, and readability in English and Spanish. Journal of the American Medical Association. 285(20): 2612–2621.
Bertakis KD. 1977. The communication of information from physician to patient: A method for increasing patient retention and satisfaction. Journal of Family Practice 5(2): 217–222.
Bindman AB, Grumbach K, Osmond D, Komaromy M, Vranizan K, Lurie N, Billings J, Stewart A. 1995. Preventable hospitalizations and access to health care. Journal of the American Medical Association. 274(4): 305–311.
Bird JA, McPhee SJ, Ha NT, Le B, Davis T, Jenkins CN. 1998. Opening pathways to cancer screening for Vietnamese-American women: Lay health workers hold a key. Preventive Medicine. 27(6): 821–829.
Bodenheimer T. 1999. Disease management—Promises and pitfalls. New England Journal of Medicine. 340(15): 1202–1205.
Brookfield, S. 1986. Understanding and Facilitating Adult Learning. 1st edition. San Francisco, CA: Jossey-Bass.
Casalino L, Gillies RR, Shortell SM, Schmittdiel JA, Bodenheimer T, Robinson JC, Rundall T, Oswald N, Schauffler H, Wang MC. 2003. External incentives, information technology, and organized processes to improve health care quality for patients with chronic diseases. Journal of the American Medical Association. 289(4): 434–441.
CDC (Centers for Disease Control and Prevention). 2000. National Diabetes Fact Sheet. Atlanta, GA: Centers for Disease Control and Prevention.
Cegala DJ. 1997. A study of doctors’ and patients’ communication during a primary care consultation: Implications for communication training. Journal of Health Communication. 2(3): 169–194.
Center for Literacy Studies. 2003. Equipped for the Future: EFF Center for Training and Technical Assistance. University of Tennessee [Online]. Available: http:www.nifl.gov/lincs/collections/eff/eff.html [accessed: September, 2003].
Chew LD, Bradley KA. 2003. Brief questions to detect inadequate health literacy among VA patients. Abstract. Journal of General Internal Medicine. 18(Supplement 1): 170.
Chow KM. 2003. Information recall by patients. Journal of the Royal Society of Medicine. 96(7): 370.
Cole, SA, Bird J. 2000. The Medical Interview: The Three-Function Approach. 2nd edition. St. Louis: Mosby.
Cooper LA, Roter DL. 2003. Patient-provider communication: The effect of race and ethnicity on process and outcomes in health care. In: Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Smedley BD, Stith AY, Nelson AR, Editors. Washington, DC: The National Academies Press. Pp. 336–354.
Cooper HC, Booth K, Gill G. 2003. Patients’ perspectives on diabetes health care education. Health Education Research. 18(2): 191–206.
Crane JA. 1997. Patient comprehension of doctor-patient communication on discharge from the emergency department. Journal of Emergency Medicine. 15(1): 1–7.
Davis TC, Crouch MA, Long SW, Jackson RH, Bates P, George RB, Bairnsfather LE. 1991. Rapid assessment of literacy levels of adult primary care patients. Family Medicine. 23(6): 433–435.
Davis TC, Berkel HJ, Arnold CL, Nandy I, Jackson RH, Murphy PW. 1998a. Intervention to increase mammography utilization in a public hospital. Journal of General Internal Medicine 13(4): 230–233.
Davis TC, Fredrickson DD, Arnold C, Murphy PW, Herbst M, Bocchini JA. 1998b. A polio immunization pamphlet with increased appeal and simplified language does not improve comprehension to an acceptable level. Patient Education and Counseling. 33(1): 25–37.
Davis TC, Fredrickson DD, Arnold CL, Cross JT, Humiston SG, Green KW, Bocchini JA Jr. 2001. Childhood vaccine risk/benefit communication in private practice office settings: A national survey. Pediatrics. 107(2): E17.
Davis TC, Fredrickson DD, Bocchini C, Arnold CL, Green KW, Humiston SG, Wilder E, Bocchini JA Jr. 2002a. Improving vaccine risk/benefit communication with an immunization education package: A pilot study. Ambulatory Pediatrics. 2(3): 193–200.
Davis TC, Williams MV, Marin E, Parker RM, Glass J. 2002b. Health literacy and cancer communication. Ca: A Cancer Journal for Clinicians. 52(3): 134–149.
Diabetes Control and Complications Trial Research Group. 1993. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. New England Journal of Medicine. 329(14): 977–986.
Diabetes Control and Complications Trial Research Group. 1996. Lifetime benefits and costs of intensive therapy as practiced in the diabetes control and complications trial. Journal of the American Medical Association. 276(17): 1409–1415.
Doak CC, Doak LG, Friedell GH, Meade CD. 1998. Improving comprehension for cancer patients with low literacy skills: Strategies for clinicians. [Review] [50 refs]. Ca: A Cancer Journal for Clinicians. 48(3): 151–162.
Figueroa ME, Kincaid DL, Rani M, Lewis G. 2002. Communication for Social Change Working Paper Series. Communication for Social Change: An Integrated Model for Measuring the Process and Its Outcomes. New York: The Rockefeller Foundation and Johns Hopkins University Center for Communication Programs.
Fiscella K, Franks P, Gold MR, Clancy CM. 2000. Inequality in quality: Addressing socioeconomic, racial, and ethnic disparities in health care. Journal of the American Medical Association. 283(19): 2579–2584.
Fox S, Fallows D. 2003 (July 16). Internet Health Resources: health searches and email have become more commonplace, but there is room for improvement in searches and overall Internet access. Washington, DC: Pew Internet & American Life Project.
Frankel RM, Stein T. 2001. Getting the most out of the clinical encounter: The four habits model . Journal of Medical Practice Management. 16(4): 184–191.
Gazmararian JA, Baker DW, Williams MV, Parker RM, Scott TL, Green DC, Fehrenbach SN, Ren J, Koplan JP. 1999a. Health literacy among Medicare enrollees in a managed care organization. Journal of the American Medical Association. 281(6): 545–551.
Gazmararian JA, Baker DW, Williams MV, Parker RM, Scott T, Greemn DCFSN, Ren J, Koplan JP. 1999b. Health literacy among Medicare enrollees in a managed care organization. Journal of the American Medical Association. 281(6): 545–551.
Guerra CE, Shea JA. 2003. Functional health literacy, comorbidity and health status. Journal of General Internal Medicine. 18(Supplement 1): 174.
HHS (U.S. Department of Health and Human Services). 2000. Healthy People 2010: Understanding and Improving Health. Washington, DC: U.S. Department of Health and Human Services.
Houts PS, Bachrach R, Witmer JT, Tringali CA, Bucher JA, Localio RA. 1998. Using pictographs to enhance recall of spoken medical instructions. Patient Education and Counseling. 35(2): 83–88.
Institute for Health and Aging. 1996. Chronic Care in America: A 21st Century Challenge. Princeton, NJ: The Robert Wood Johnson Foundation.
IOM (Institute of Medicine). 2001. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press.
IOM. 2003. Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Washington, DC: The National Academies Press.
Jacobson TA, Thomas DM, Morton FJ, Offutt G, Shevlin J, Ray S. 1999. Use of a low-literacy patient education tool to enhance pneumococcal vaccination rates: A randomized controlled trial. Journal of the American Medical Association. 282(7): 646–650.
Kalichman SC, Rompa D. 2000. Functional health literacy is associated with health status and health-related knowledge in people living with HIV-AIDS. Journal of Acquired Immune Deficiency Syndromes & Human Retrovirology. 25(4): 337–344.
Kalichman SCP, Ramachandran BB, Catz SP. 1999. Adherence to combination antiretroviral therapies in HIV patients of low health literacy. Journal of General Internal Medicine. 14(5): 267–273.
Kim SP, Knight SJ, Tomori C, Colella KM, Schoor RA, Shih L, Kuzel TM, Nadler RB, Bennett CL. 2001. Health literacy and shared decision making for prostate cancer patients with low socioeconomic status. Cancer Investigation. 19(7): 684–691.
Kirsch IS (Educational Testing Service (ETS)). 1993. Adult Literacy in America: A First Look at the Results of the National Adult Literacy Survey. Washington, DC: U.S. Government Printing Office.
Kusec S, Brborovic O, Schillinger D. 2003. Diabetes websites accredited by the Health on the Net Foundation Code of Conduct: Readable or not? Studies in health technology and informatics. Vol. 95. In: The New Navigators: From Professionals to Patients. Baud R, Fieschi M, Le Beux P, Ruch P, Editors. Amsterdam, NE: IOS Press.
Lorig KR, Sobel DS, Stewart AL, Brown BW Jr, Bandura A, Ritter P, Gonzalez VM, Laurent DD, Holman HR. 1999. Evidence suggesting that a chronic disease self-management program can improve health status while reducing hospitalization: A randomized trial. Medical Care. 37(1): 5–14.
McCulloch DK, Price MJD, Hindmarsh M, Wagner EH. 2000. Improvement in diabetes care using an integrated population-based approach in a primary care setting. Disease Management. 3(2): 75–82.
NCQA (National Committee for Quality Assurance). 2003. Measuring the Quality of America’s Health Care. [Online]. Available: http://www.ncqa.org [accessed: July, 2003].
Norris SL, Nichols PJ, Caspersen CJ, Glasgow RE, Engelgau MM, Jack L, Isham G, Snyder SR, Carande-Kulis VG, Garfield S, Briss P, McCulloch D. 2002a. The effectiveness of disease and case management for people with diabetes. A systematic review. American Journal of Preventive Medicine. 22(4 Supplement): 15–38.
Norris SL, Nichols PJ, Caspersen CJ, Glasgow RE, Engelgau MM, Jack L, Snyder SR, Carande-Kulis VG, Isham G, Garfield S, Briss P, McCulloch D. 2002b. Increasing diabetes self-management education in community settings. A systematic review. American Journal of Preventive Medicine . 22(4 Supplement): 39–66.
Nurss JR, Parker RM, Williams MV, Baker DW. 1995. TOFHLA: Test of Functional Health Literacy in Adults. Snow Camp, NC: Peppercorn Books & Press.
Nutbeam D. 2000. Health literacy as a public health goal: A challenge for contemporary health education and communication strategies into the 21st century. Health Promotion International. 15(3): 259–267.
Piette JD. 1999. Satisfaction with care among patients with diabetes in two public health care systems. Medical Care. 37(6): 538–546.
Piette JD. 2000. Interactive voice response systems in the diagnosis and management of chronic disease. American Journal of Managed Care. 6(7): 817–827.
Robert Wood Johnson Foundation. 2002. Annual Report 2001. Princeton, NJ: The Robert Wood Johnson Foundation.
Robert Wood Johnson Foundation and the National Cancer Institute. 2002. A Research Dialogue: Online Behavior Change and Disease Management Research. [Online]. Available: http://www.rwjf.org/publications/publicationsPdfs/onlineBehaviorChange.pdf [accessed: November 10, 2003].
Rost K, Roter D. 1987. Predictors of recall of medication regimens and recommendations for lifestyle change in elderly patients. Gerontologist. 27(4): 510–515.
Roter DL. 2000. The outpatient medical encounter and elderly patients. Clinics in Geriatric Medicine. 16(1): 95–107.
Roter DL, Hall JA. 1992. Doctors Talking with Patients/Patients Talking with Doctors: Improving Communication in Medical Visits. Westport, CT: Auburn House.
Roter DL, Stewart M, Putnam SM, Lipkin M Jr, Stiles W, Inui TS. 1997. Communication patterns of primary care physicians. Journal of the American Medical Association. 277(4): 350–356.
Roter DL, Rudd RE, Comings J. 1998. Patient literacy. A barrier to quality of care. Journal of General Internal Medicine. 13(12): 850–851.
Roter DL, Stashefsky-Margalit R, Rudd R. 2001. Current perspectives on patient education in the US. Patient Education and Counseling. 44(1): 79–86.
Rothman R, Pignone M, Malone R, Bryant B, Crigler B. 2003. A primary care-based, pharmacist led, disease management program improves outcomes for patients with diabetes: A randomized controlled trial Journal of General Internal Medicine. 18(Supplement 1): 155.
Rudd RE, Comings JP. 1994. Learner developed materials: An empowering product. Health Education Quarterly. 21(3): 313–327.
Schillinger D, Grumbach K, Piette J, Wang F, Osmond D, Daher C, Palacios J, Sullivan GaD, Bindman AB. 2002. Association of health literacy with diabetes outcomes. Journal of the American Medical Association. 288(4): 475–482.
Schillinger D, Machtinger E, Win K, Wang F, Chan L-L, Rodriguez ME. 2003a. Are pictures worth a thousand words? Communication regarding medications in a public hospital anticoagulation clinic Journal of General Internal Medicine 18(Supplement 1): 187.
Schillinger D, Piette J, Grumbach K, Wang F, Wilson C, Daher C, Leong-Grotz K, Castro C, Bindman AB. 2003b. Closing the loop: Physician communication with diabetic patients who have low health literacy. Archives of Internal Medicine. 163(1): 83–90.
Schillinger D, Bindman A, Stewart A, Wang F, Piette J. 2004. Functional health literacy and the quality of physician-patient communication among diabetes patients. Patient Education and Counseling. 52(3): 315–323.
Sehgal AR. 2003. Impact of quality improvement efforts on race and sex disparities in hemodialysis. Journal of the American Medical Association. 289(8): 996–1000.
Starfield B. 1998. Primary Care: Balancing Health Needs, Services, and Technology. New York: Oxford University Press.
Street RL Jr. 1991. Information-giving in medical consultations: The influence of patients’ communicative styles and personal characteristics. Social Science and Medicine. 32(5): 541–548.
Trento M, Passera P, Tomalino M, Bajardi M, Pomero F, Allione A, Vaccari P, Molinatti GM, Porta M. 2001. Group visits improve metabolic control in type 2 diabetes: A 2-year follow-up. Diabetes Care. 24(6): 995–1000.
Trento M, Passera P, Bajardi M, Tomalino M, Grassi G, Borgo E, Donnola C, Cavallo F, Bondonio P, Porta M. 2002. Lifestyle intervention by group care prevents deterioration of Type II diabetes: A 4-year randomized controlled clinical trial. Diabetologia. 45(9): 1231–1239.
United Kingdom Prospective Diabetes Study Group. 1998. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 352(9131): 837–853.
Vinicor F, Burton B, Foster B, Eastman R. 2000. Healthy people 2010: Diabetes. Diabetes Care. 23(6): 853–855.
Von Korff M, Gruman J, Schaefer J, Curry SJ, Wagner EH. 1997. Collaborative management of chronic illness. Annals of Internal Medicine. 127(12): 1097–1102.
Wagner EH. 1995. Population-based management of diabetes care. Patient Education and Counseling. 26(1–3): 225–230.
Wagner EH. 1998. Chronic disease management: What will it take to improve care for chronic illness? Effective Clinical Practice. 1(1): 2–4.
Wagner, EH. 2003. The Chronic Care Model: Improving Chronic Illness Care. [Online]. Available: http://www.improvingchroniccare.org/change/model/components.html [accessed: March, 2003].
Wallerstein N. 1992. Powerlessness, empowerment, and health: Implications for health promotion programs. American Journal of Health Promotion. 6(3): 197–205.
Wallerstein N, Bernstein E. 1988. Empowerment education: Freire’s ideas adapted to health education. Health Education Quarterly. 15(4): 379–394.
Weiss BD, Hart G, McGee DL, D’Estelle S. 1992. Health status of illiterate adults: Relation between literacy and health status among persons with low literacy skills. Journal of the American Board of Family Practice. 5(3): 257–264.
Williams MV, Parker RM, Baker DW, Coates W, Nurss J. 1995a. The impact of inadequate functional health literacy on patients’ understanding of diagnosis, prescribed medications, and compliance. Academic Emergency Medicine. 2: 386.
Williams MV, Parker RM, Baker DW, Parikh NS, Pitkin K, Coates WC, Nurss JR. 1995b. Inadequate functional health literacy among patients at two public hospitals. Journal of the American Medical Association. 274(21): 1677–1682.
Williams MV, Baker DW, Honig EG, Lee TM, Nowlan A. 1998a. Inadequate literacy is a barrier to asthma knowledge and self-care. Chest. 114(4): 1008–1015.
Williams MV, Baker DW, Parker RM, Nurss JR. 1998b. Relationship of functional health literacy to patients’ knowledge of their chronic disease. A study of patients with hypertension and diabetes. Archives of Internal Medicine. 158(2): 166–172.
Williams MV, Davis T, Parker RM, Weiss BD. 2002. The role of health literacy in patient-physician communication. Family Medicine. 34(5): 383–389.
Win K, Schillinger D. 2003. Understanding of warfarin therapy and stroke among ethnically diverse anticoagulation patients at a public hospital. Journal of General Internal Medicine. 18(Supplement 1): 278.
Youmans S, Schillinger D. 2003. Functional health literacy and medication management: The role of the pharmacist. Annals of Pharmacotherapy. 37(11): 1726–1729.
Zarcadoolas C, Blanco M, Boyer JF, Pleasant A. 2002. Unweaving the Web: An exploratory study of low-literate adults’ navigation skills on the World Wide Web. Journal of Health Communication. 7(4): 309–324.
Outside the Clinician–Patient Relationship: A Call to Action for Health Literacy
Barry D. Weiss, M.D.
Many governmental, corporate, and nonprofit businesses, organizations, and agencies have, or should have, an interest in the health literacy problem—because limited health literacy is prevalent in the groups for which these entities are responsible. These entities can be broadly categorized as insurers, employers, and advocacy groups.
Insurers should have an interest in the health literacy problem because they pay for the medical care provided to individuals with limited literacy skills, and these individuals have higher illness rates and higher health-care costs than the population in general. Employers should care about literacy because they pay for the health insurance of their workers who have limited literacy skills, and they also lose worker productivity as a result of their employee’s limited literacy. Advocacy groups should care about the literacy problem because limited literacy skills often prevent their constituents from achieving full potential in society. Methods by which these and other organizations and systems might help improve America’s health literacy issue are shown in Table B-5, below.
Insurers
Several entities provide medical insurance coverage groups in which low literacy is most prevalent. They include the publicly funded Medicare and Medicaid programs and the military’s Tricare program.
Medicare
The Medicare program is a federally funded program that provides health insurance benefits to most elderly U.S. citizens. Medicare’s costs are heavily influenced by limited health literacy because of the high rate of limited literacy skills among elderly individuals. According to the Centers for Medicare and Medicaid Services, around 35 million persons over 65 years old currently receive Medicare benefits, and the number of beneficiaries increases annually (Figure B-3).
Federal expenditures for the Medicare program now exceed $240 billion per year for medical benefits, administrative costs, and program integrity costs, representing some 20 percent of all health-care spending in the country. These costs will all increase as the number of beneficiaries continues to grow (Figure B-4) (CMS, 2002).
TABLE B-5 How Organizations and Systems Might Act to Improve America’s Health Literacy
|
Insurers |
|
|
|
Employers |
|
|
|
Advocacy Organizations |
|
|
|
Governmental and Social Service Agencies |
|
|
|
|
|
Others |
|
|
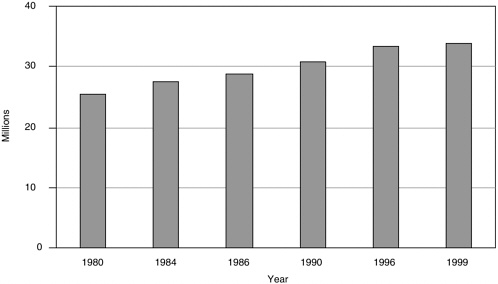
FIGURE B-3 Number of Medicare enrollees.
SOURCE: Number of Medicare Enrollees, by Age of Enrollee: Selected Calendar Years July 1, 1980–1999. Center for Medicare & Medicaid Services, Office of Information Services (http://hcms.hhs.gov/review/supp/table7b.pdf).
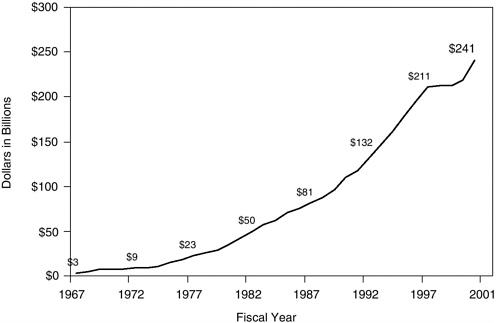
FIGURE B-4 Federal spending for Medicare. Note that overall spending includes benefit dollars, administrative costs, and program integrity costs (federal spending only).
SOURCE: Medicare Program Spending. Centers for Medicare and Medicaid Services, Office of the Actuary, June 2002 (http://www.cms.hhs.gov/charts/default.asp).
By combining Medicare expenditure figures with results from the National Adult Literacy Survey (NALS), which indicate that 80 percent of persons over 65 have limited literacy skills, one can estimate that about 80 percent of Medicare beneficiaries—32 million individuals—have limited literacy skills. Thus, most of the $240 billion annual Medicare expenditures are related to providing benefits for persons with limited literacy. Addressing the health literacy of Medicaid enrollees (Table B-5) can potentially result in substantial cost savings for the Medicare program.
Medicaid
The Medicaid program, funded by state and federal tax dollars, provides medical insurance benefits for about 45 million persons, most of whom are poor (CMS, 2000). Total expenditures by the Medicaid system were $175 billion per year in 1998, accounting for about 15 percent of all health-care spending in the United States (Health Care Financing Administration, 2000). The cost of the Medicaid program is expected to grow to $444 billion by 2010 (Figure B-5).
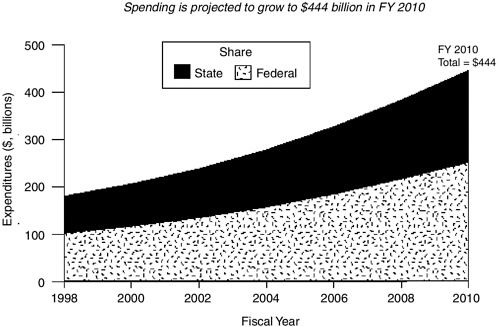
FIGURE B-5 Predicted Medicaid expenditures.
SOURCE: Health Care Financing Administration. A Profile of Medicaid: Chartbook 2000, Section III. Medicaid Expenditures. Pp. 27–51 (http://www.cms.hhs.gov/charts/medicaid/2Tchartbk.pdf).
The rate of limited literacy is high among Medicaid enrollees. A study of a random sample of Medicaid enrollees in Arizona (Weiss et al., 1994) found that the mean literacy skills of the enrollees were at just over grade-level 5. More than a quarter of subjects had reading skills at or below the fourth-grade level, in contrast to the eighth-grade average reading level of U.S. adults. Subjects in the study who indicated that their preferred language for reading was Spanish had their literacy skills assessed in Spanish, and their average reading level was at grade level 3.1.
The limited literacy skills of Medicaid enrollees are associated with high health-care costs. Indeed, in the Arizona study Medicaid recipients with the highest reading levels had average annual health-care costs of $2,969, similar to the $2,400 average cost of health care for all U.S. citizens at the time of the study. In contrast, those with reading levels at or below grade-level 3 had annual health-care costs averaging $10,688 (Weiss and Palmer, 2004). These results are remarkable, given that the subjects had relatively homogenous sociodemographic characteristics (all poor and unemployed or employed at very low-paying jobs), and the statistical relation-
ship between literacy and costs remained strong even after a multivariable analysis that accounted for education, gender, ethnic group, and preferred language. Thus, to the extent that interventions to improve health literacy (Table B-5) can reduce health-care costs, such interventions can potentially result in substantial cost savings for Medicaid programs.
Tricare
The Tricare program provides health insurance benefits for the nation’s military personnel (active- and non-active-duty) and their dependents. The program covers direct medical care, prescriptions, dental care, and a variety of other health-related benefits.
Tricare is an expensive program. Spending by the federal government for direct medical and administrative costs totaled $8.3 billion in 1998 for some 4 million Tricare enrollees (Stoloff et al., 2000).
As noted earlier, many military recruits have limited literacy skills. Given the association between limited literacy and higher health-care costs, and given the cost of the Tricare system, significant cost savings might accrue to the U.S. military if the health literacy skills of the military recruits were improved. Thus, the military is an entity with large potential gain from improvement in its members’ health literacy.
As mentioned, the military currently engages in literacy-skill enhancement for its recruits to enable them to function adequately in the roles as soldiers. Incorporating health knowledge within literacy training (Table B-5) might provide further benefit by reducing excess costs related to limited health literacy.
Employers
Business leaders have long recognized the need for literacy enhancement in the workforce, as workers’ limited literacy skills often interfere with productivity and safety (Rockefeller Foundation Conference Proceedings, 1989). This concern is of particular importance for businesses that employ large numbers of routine service providers and production workers, because these groups have an over-representation of undereducated individuals (Reich, 1992). Some large employers already offer literacy training to their employees to address concerns about workplace literacy (Academy of Human Resource Development, 2000; Askov and Van Horn, 1993; National Institute for Literacy, 1994).
Businesses should also have an interest in health literacy because of its relationship to health-care costs. Government agencies have reported that nearly two-thirds of Americans under age 65 obtain health insurance through their workplace (Monheit and Vistnes, 1997), with more than 150
million workers and dependents in the United States, and an additional 5 million retirees, receiving job-based health insurance benefits (Gabel et al., 2000). On average, health benefits currently cost employers about $1.29 per hour per employee (U.S. Department of Labor, 2002).
The result of these costs, based on recent data from the Agency for Healthcare Research and Quality (AHRQ), is that each year private employers in the United States pay in the range of $350 billion to cover the cost of hospitalizations and physicians’ services for their employees and families (Table B-6) (AHRQ, 2000). Public employers, including federal, state, and local governments, pay approximately $60 billion dollars per year. These costs rise annually—an 8 percent increase in 2000 and an 11 percent increase in 2001—with similar increases anticipated in the future (Mercer, 2003). Health insurance premiums paid by employers increase at a faster rate than wages or overall inflation (Gabel et al., 2001). Indeed, the Health Care Financing Administration has estimated that by 2008, healthcare spending in the United States will reach $2.2 trillion (CMS, 2003).
To the extent that improving literacy skills will reduce health-care costs, employers would benefit substantially from initiatives that improve worker literacy. This is especially true for employers with a workforce that includes large numbers of routine service and production workers, as these groups have high rates of limited literacy. Partners in such initiatives could
TABLE B-6 National Totals for Enrollees and Cost of Hospitalization and Physician Service Health Plans for the Private Sector, United States, 2000
|
Enrollee Category |
Total (in thousands of persons) |
|
Total Enrollees |
71,253 |
|
Active enrollees |
64,284 |
|
Enrollees through COBRA |
2,766 |
|
Retired enrollees |
4,203 |
|
Costs |
Total (in millions of dollars) |
|
Total Costs |
349,612 |
|
Employer contribution single coverage |
69,066 |
|
Employer contribution family coverage |
191,916 |
|
Employee contribution single coverage |
18,251 |
|
Employee contribution family coverage |
70,379 |
|
SOURCE: Agency for Healthcare Research and Quality, Center for Cost and Financing Studies. 2000 Medical Expenditure Panel Survey—Insurance Component (http://meps.ahrq.gov/MEPSDATA/ic/2000/Tables_IV/TableIVA1.htm). |
|
include not only employers, but also community-based literacy programs and local governments seeking to attract employers that would be drawn to communities with a more literate workforce.
An additional approach to improving workforce literacy, including health literacy, could focus on science education in secondary schools and universities, where most students currently are taught basic science facts, rather than applied health sciences—and many students study little or no science at all. Indeed, data from the National Center for Education Statistics indicate that only 75 percent of U.S. high school students take more than one science course. While biology is the most popular science course offered in high school (i.e., most students select biology as their one science course), only about 1 in 6 takes an advanced course in biology (National Center for Education Statistics, 2001). The result is that many, if not most, students, even some destined for a career in the health sciences, graduate from high schools without a substantive understanding of the anatomy, physiology, and etiology of common diseases like atherosclerosis, diabetes, and cancer. Incorporating an applied “health literacy approach” into science education in schools and universities could have a major benefit for improving the health literacy of the nation’s workforce and for reducing health-care expenditures for employers (Table B-5).
Advocacy Organizations
There are many national-level organizations with missions dedicated to improving opportunities and quality of life for their constituents. Of note, some of these organizations advocate on behalf of the groups with the highest rates of limited literacy—the elderly, Hispanics, and African Americans—and these organizations could implement programs to improve their constituents’ health literacy (Table B-5). Although not discussed here, there are also advocacy groups on both local and national levels that represent the other high-risk groups, such as other ethnic minority groups, immigrants, the homeless, the poor, and prisoners.
Advocates for the Elderly
The most well known, and perhaps the most important, senior citizens’ advocacy group is the American Association of Retired Persons (now known only by the acronym AARP)—which represents over 35 million older Americans (AARP, 2002). In addition to general advocacy on behalf of the nation’s elderly, AARP places particular emphasis on health and the cost of health care for senior citizens.
Given the very high rate of limited literacy among older individuals, and relationship of those limited literacy skills to health status, health-care
costs, employment opportunities, and quality of life, a focus on literacy—including health literacy—would advance AARP’s mission and improve quality of life for its constituents. Other senior citizens’ advocacy groups share similar goals.
Advocates for Hispanics
There are many advocacy organizations for Hispanics, but two stand out as particularly respected and influential: the National Council of La Raza and the Mexican American Legal Defense and Educational Fund. In addition, the National Hispanic Medical Association has particular interest in health-related issues, which could include health literacy.
National Council of La Raza
The National Council of La Raza is a private, nonprofit organization established in 1968. It has 270 formal affiliates in 40 states, and a much broader network of 20,000 groups and individuals nationwide. Its mission is to “improve life opportunities for Hispanic Americans” (National Council of La Raza, 2003). Life opportunities are diminished when individuals have limited literacy skills, and the literacy skills of Hispanics are currently the lowest of any major ethnic group in the United States (Table B-7). Enhancing literacy skills, including health literacy skills, as an area of emphasis for the National Council of La Raza and similar organizations has the potential to improve economic opportunities and health care for Hispanic Americans.
Mexican American Legal Defense and Educational Fund
The Mexican American Legal Defense and Educational Fund is a national nonprofit organization whose mission includes assuring that “there are no obstacles preventing [the Latino] community from realizing its dreams…” (Mexican American Legal Defense and Educational Fund, 2003). Limited literacy is one such obstacle, and the Mexican American Legal Defense and Educational Fund could participate in efforts to enhance literacy and health literacy skills of Hispanics.
National Hispanic Medical Association
The National Hispanic Medical Association is an organization that represents Hispanic medical providers. The organization expresses a commitment to providing policy makers and health-care providers with expert medical information, and to supporting and strengthening delivery of health
TABLE B-7 Percentage of Adult Population Groups with Literacy Skills at NALS Levels 1 or 2
|
|
Percent |
|
|
Group |
Level 1 |
Level 2 |
|
All NALS Respondents |
22 |
28 |
|
Age |
||
|
16–54 years |
15 |
28 |
|
55–64 years |
28 |
33 |
|
65 years and older |
49 |
32 |
|
Highest Education Level Completed |
||
|
0–8 years |
77 |
19 |
|
9–12 years (no high school graduation) |
44 |
37 |
|
High school diploma/GED (no college study) |
18 |
37 |
|
Racial/Ethnic Group |
||
|
White |
15 |
26 |
|
American Indian/Alaska Native |
26 |
38 |
|
Asian Pacific Islander |
35 |
25 |
|
Black |
41 |
36 |
|
Hispanic (all groups) |
52 |
26 |
|
Immigrants to U.S. (various countries of origin) |
||
|
0–8 years of education prior to arrival in U.S. |
60 |
31 |
|
9 + years of education prior to arrival in U.S. |
44 |
27 |
|
SOURCE: Unadjusted averages of prose and document literacy scores on the NALS as reported on Tables 1.1A, 1.1B, 1.2A, and 1.2B in Kirsch I, Jungeblut A, Jenkins L, Kolstad A. Adult Literacy in America: A First Look at the Results of the National Adult Literacy Survey. Washington, DC: National Center for Education Statistics, U.S. Department of Education; September, 1993, and on Table B3.13 in U.S. Department of Education. National Center for Education Statistics. English Literacy and Language Minorities in the United States, NCES 2001–464, by Greenberg E, Macías RF, Rhodes D, Chan T. Washington, DC: 2001. |
||
services to Hispanic communities across the nation (National Hispanic Medical Association, 1997). Aiding in the improvement of health literacy for Hispanics would go hand in hand with these goals, and it would seem logical for the National Hispanic Medical Association to participate in health literacy efforts.
Advocates for African-Americans
African-Americans are also represented by a number of advocacy organizations. Two of the most respected organizations are the National Association for the Advancement of Colored People (NAACP) and the National Urban League. The National Medical Association, the organization that
represents African-American physicians, also has a specific interest in the health status of African-American citizens.
NAACP
NAACP is the nation’s oldest and largest civil rights organization. NAACP has a specific health division, with goals that include “developing national health advocacy and education initiatives that promote equity in health status,” “sponsoring collaborative initiatives with other national and local health groups,” and “expanding outreach on health advocacy and awareness in communications” (NAACP, 2003). Assuring adequate health literacy as a component of initiatives meets all of those goals, and NAACP may thus be an effective advocate for enhancing health literacy among African Americans.
National Urban League
The National Urban League has affiliates in more than 100 cities in 24 states. While the organization’s goal is broadly aimed at enabling “African Americans to secure economic self-reliance, parity and power and civil rights,” its mission also includes a specific goal of “ensuring that our children are well educated” (National Urban League, 2002). Efforts to improve literacy in general, and health literacy in particular, would fall within the mission of the National Urban League.
National Medical Association
The National Medical Association represents the interests of more than 25,000 African-American physician and their patients. One of the organization’s key missions is “to improve the status of health and quality and availability of health care to African-American and underserved populations” (National Medical Association, 2003). This mission would be enhanced by efforts to improve health literacy.
Other Organizations and Systems
There are many other organizations and systems that provide services to groups with high rates of limited literacy. Among these are prison systems and social service agencies that work with undereducated individuals. Professional organizations that represent health-care providers (in addition to the National Medical Association and National Hispanic Medical Association) also have a role to play in improving health literacy (Table B-5).
Prison Systems
Inmates in most prisons already have access to literacy improvement programs. Given the large and growing size of the U.S. prison population, however, and the costs associated with providing health care to prisoners, incorporating health literacy content might enhance current literacy improvement programs.
Social Service Agencies
Social service agencies in virtually all U.S. communities interact with low-literate individuals every day, because clientele of these agencies include large numbers of unemployed persons with limited education. Some of these agencies, particularly adult education programs, focus on literacy enhancement as a core mission through adult basic education, GED programs, and “English as a Second Language” programs.
The majority of individuals with limited literacy, however, do not enter such education programs. Rather their interaction with social service agencies is often through county and state public assistance programs, unemployment agencies, childcare programs, and others. These social service agencies spend large sums of money providing services to their clientele, and those sums might be reduced if clientele had better literacy skills that permitted easier entry into the workforce. To the extent that clientele of these agencies have chronic health problems—and many do—costs might further be reduced if clientele had better health literacy.
Public assistance, unemployment, and childcare agencies could link with local adult education programs, or with national literacy programs such as ProLiteracy America (Proliteracy Worldwide, 2002), to facilitate easy referral into literacy training programs. In fact, literacy training programs could be located on site with, or in close geographic proximity to, a variety of social service agencies, including medical clinics whose clients might benefit from literacy enhancement. Such partnerships, some emphasizing health literacy, are currently in place in a number of communities (Community Health Partners, 2003; El Paso Community College/ Community Education Program, 2001). More such partnerships should be encouraged.
Professional Associations
Finally, professional associations representing health-care providers have an interest in assuring and improving health and health care for individual patients. With evidence showing that limited literacy skills are associated with poorer health status, all professional associations representing
health-care providers should have a de facto interest in improving health literacy.
Some professional associations, such as the American Medical Association, have already produced educational materials to enhance health providers’ understanding of the health literacy problem and give them suggestions for how to more effectively communicate with patients (Weiss, 2003). The materials include educational monographs and videotapes, train-the-trainer programs, and outreach efforts to local medical societies. Other professional organizations, such as the American Academy of Neurology, the Virginia Medical Society, the Iowa Medical Society, and the Georgia Academy of Family Physicians have also developed programs, or are planning to do so.
Additional efforts from professional associations could include lobbying efforts aimed at securing support for health literacy content in adult basic education programs. Finally, professional organizations could improve the public’s health literacy by working with school systems to develop and implement health education curricula for use in elementary and secondary schools.
CONCLUSION
The unique vocabulary and concepts of medicine make it difficult for many individuals to fully understand health information provided to them by clinicians. This lack of understanding translates into poor health literacy—i.e., a limited ability to read, understand, and use health information to make effective health-care decisions and follow recommendations for treatment. While limited health literacy occurs in all segments of society, it is a particular problem for individuals with limited reading skills (i.e., limited general literacy).
Limited literacy is more prevalent in certain groups. These groups include the elderly, racial and ethnic minorities, persons with limited education, immigrants, prisoners, the poor and homeless, and military recruits. In some of these groups, such as the elderly, certain ethnic minorities, and persons who did not complete school, the prevalence of limited literacy exceeds 80–90 percent.
Persons with limited general and health literacy, on average, have poorer health knowledge, poorer health status, and higher health-care costs than do persons with higher-level literacy skills. The relationship between limited literacy and poorer health and higher costs is strong and independent of other socioeconomic factors.
Based on results of the NALS, about half of U.S. adults have literacy skills that are inadequate to meet the demands of today’s health system. Health-care systems could address this problem through processes and poli-
cies that enhance employee awareness of patients’ health literacy skills, and by delivering information in ways that patients can understand.
A variety of public and private entities have a stake in the health literacy problem. These include health insurers, employers, and advocacy groups. Insurers have a stake in the problem because of the high cost of health care for persons with limited literacy. For example, because limited literacy skills are so common among the elderly, most of Medicare’s $240 billion annual budget goes to providing care for persons with limited literacy.
Employers, especially those that employ large numbers of undereducated service and production workers, also have a stake in health literacy. Employers pay the high cost of their employee’s health insurance benefits, and their businesses lose productivity due to higher rates of illness among employees with limited literacy.
REFERENCES
AARP. 2002. AARP Facts. [Online]. Available: http://www.aarp.org/what_is.html [accessed: August, 2003].
Academy of Human Resource Development. 2000. Workforce Development. Symposium 37 [concurrent Symposium Session at AHRD Annual Conference, March 8–12, 2000]. Raleigh-Durham, NC: Academy of Human Resource Development.
AHRQ (Agency for Healthcare Research and Quality, Center for Cost and Financing Studies). 2000. Medical Expenditure Panel Survey—Insurance Component. [Online]. Available: http://meps.ahrq.gov/MEPSDATA/ic/2000/Tables_IV/TableIVA1.htm [accessed August, 2003].
Askov EN, Van Horn B. 1993. Adult educators and workplace literacy: Designing customized basic skills instruction. Adult Basic Education. 3(2): 115–125.
CMS (Centers for Medicare and Medicaid Services). 2000. Medicaid Eligables—Fiscal Year 2000 by Maintenance Assistance Status and Basis of Eligability. [Online]. Available: http://www.cms.hhs.gov/medicaid/msis/00total.pdf [accessed: August, 2003].
CMS. 2002. Medicare Program Spending. [Online]. Available: http://www.cms.hhs.gov/charts/series/sec3-a.ppt [accessed: August, 2003].
CMS. 2003. Health Accounts: Estimates. [Online]. Available: http://hcfa.gov/stats/NHE-proj/[accessed: August, 2003].
Community Health Partners. 2003. A Partnership for Health. [Online]. Available: http://chphealth.org/ [accessed: August, 2003].
El Paso Community College/Community Education Program. 2001. The El Paso Collaborative Health Literacy Curriculum. [Online]. Available: http://www.worlded.org/us/health/docs/elpaso/index.htm [accessed: August, 2003].
Gabel J, Levitt L, Pickreign J, Whitmore H, Holve E, Hawkins S, Miller N. 2000. Job-based health insurance in 2000: Premiums rise sharply while coverage grows. Health Affairs. 19(5): 144–151.
Gabel J, Levitt L, Pickreign J, Whitmore H, Holve E, Rowland D, Dhont K, Hawkins S. 2001. Job-based health insurance in 2001: Inflation hits double digits, managed care retreats. Health Affairs. 20(5): 180–186.
Health Care Financing Administration. 2000. A Profile of Medicaid: Chartbook 2000. [Online]. Available: http://www.cms.hhs.gov/charts/medicaid/2Tchartbk.pdf [accessed: August, 2003].
Mercer, WM. 2000. 15th Annual Mercer/Foster Higgins National Survey of Employer-Sponsored Health Plans. [Online]. Available: http://imercer.com/us/imercercommentary/BBfinal.pdf [accessed: August, 2003].
Mexican American Legal Defense and Education Fund. 2003. Mission Statement. [Online]. Available: http://www.maldef.org/about/mission.htm [accessed: August, 2003].
Monheit AC, Vistnes JP 1997. MEPS Research Findings No. 2. Health Insurance Status of Workers and Their Families. Rockville, MD: Agency for Health Care Policy and Research.
NAACP (National Association for the Advancement of Colored People). 2003. NAACP Health Division Fact Sheet . [Online]. Available: http://www.naacp.org/programs/health/FactSheet.shtml [accessed: August, 2003].
National Center for Education Statistics. 2001. The 1998 High School Transcript Study Tabulations: Comparative Data on Credits Earned and Demographics for 1998, 1994, 1990, 1987, 1982 High School Graduates. Washington, DC: U.S. Department of Education, Office of Educational Research and Improvement.
National Council of La Raza. 2003. Mission Statement. [Online]. Available: http://www.nclr.org/about/index.html [accessed: August, 2003].
National Hispanic Medical Association. 1997. Home Page. [Online]. Available: http://www.nhmamd.org [accessed: August, 2003].
National Institute for Literacy. 1994. What Kind of Adult Literacy Policy Do We Need If We Are Serious About Enabling Every Adult to Become a High Skills/High Wage Worker in the Global Economy? Washington, DC: National Institute for Literacy.
National Medical Association. 2003. National Medical Association Overview. [Online]. Available: http://www.nmanet.org [accessed: August, 2003].
National Urban League. 2002. Mission Statement. [Online]. Available: http://www.nul.org/about/mission.htm [accessed: August, 2003].
Proliteracy Worldwide. 2002. Proliteracy America. [Online]. Available: http://www.proliteracy.org/proliteracy_america/index.asp [accessed: August, 2003].
Reich RB. 1992. The Work of Nations: Preparing Ourselves for 21st Century Capitalism. New York: Vintage Press.
Rockefeller Foundation Conference Proceedings. 1989. Literacy and the Marketplace. New York: The Rockefeller Foundation.
Stoloff, PH, Lurie, PM, Goldmerg, L, Almendarez, M 2000. Evaluation of the TRICARE Program: FY 2000 Report to Congress. [Online]. Available: http://www.defenselink.mil/pubs/tricare02202001.pdf [accessed: August, 2003].
U.S. Department of Labor. Bureau of Labor Statistics. 20002. Cost of Health Benefits in Private Industry, March 2002. [Online]. Available: http://www.bls.gov/opub/ted/2002/jul/wk3/art01.htm [accessed: August, 2003].
Weiss BD. 2003. Health Literacy: A Manual for Clinicians. Chicago, IL: American Medical Association Foundation.
Weiss BD, Palmer R. 2004. Relationship between health care costs and very low literacy skills in a medically needy and indigent Medicaid population. Journal of the American Board of Family Practice. 17(1): 44–47.
Weiss BD, Blanchard JS, McGee DL, Hart G, Warren B, Burgoon M, Smith KJ. 1994. Illiteracy among Medicaid recipients and its relationship to health care costs. Journal of Health Care for the Poor & Underserved. 5(2): 99–111.














































