B
Metabolic Monitoring at NASA: A Concept for the Military
Kira Bacal, M.D., Ph.D., M.P.H., Wyle Laboratories and Life Sciences, and Johnson Space Flight Center, NASA, Houston, Texas
NASA’s (National Aeronautics and Space Administration) Johnson Space Center (JSC) Office of Space Medicine, in collaboration with NASA’s Ames Research Center and the Stanford University Medical Center, has been interested in the field of metabolic monitoring for some time. In the aerospace environment crew time is a very precious commodity due to limited resources and limited personnel; metabolic monitoring can be used to optimize crew function and minimize the risk of fatigue and illness through the observation and interpretation of physiological data. By using a variety of sensors to monitor both the individual’s biomarkers and the ambient environment, data can be captured and then correlated and analyzed using software models. These tools anticipate metabolic irregularities, provide feedback to the operator, and advise appropriate interventions to prevent unwanted consequences. The same systems also monitor the user for compliance with the recommendations and evaluate the efficacy of the recommendations.
Given its operational milieu, NASA is particularly interested in remote metabolic monitoring. The majority of aerospace operations take place at sites far distant from clinical care providers and decision makers, thus any system that enhances the situational awareness of the control team is helpful. The astronaut and warfighter share many similar traits: both are highly trained individuals who are engaged in prolonged and exhausting efforts in a hostile environment. Whether the individual is searching for enemy patrols in the desert or repairing a satellite during a spacewalk, there is a similar level of both effort expended and physiological demands. In addition, both individuals are engaged in time-critical tasks and are far from medical support. For these reasons prevention of illness or injury, rather than its care, is desirable.
In the space environment, as in the military, operations can be divided into two categories: nominal and contingency. The latter category contains unsched-
uled events, such as illness or injury, and the medical resources brought to bear should be those that best conform to an adapted terrestrial standard of care. In contingency conditions, therefore, only approved medical devices and accepted treatment guidelines are employed, while unproven equipment or monitoring of novel parameters is eschewed as the information thus provided lacks an appropriate clinical context. Given the numerous confounding factors and unknowns about pathology and pathophysiology in the microgravity environment, it is imperative that, to the greatest extent possible, medical care on orbit proceeds from accepted practices.
Conversely, nominal operations, which can include activities such as spacewalks, exercise, or research studies to define “space-normal” physiology, can and often do use new tools and monitor novel parameters. Often associated with research activities, nominal operations utilize both proven and innovative technologies to gather data, develop predictive models, and validate these predictions.
Under nominal operations the goal of metabolic monitoring is to intervene before a medical event occurs. Some of the on-orbit conditions that could be prevented in this way include dehydration, fatigue, heat stress, hyperventilation, and hypothermia. In addition, monitoring can also assist in the evaluation of specific performance metrics, such as cognition, workload, situational awareness, memory, and concentration, to ensure that critical or complex tasks are performed by competent operators. Fatigue is a constant concern in space operations because circadian cues are disrupted and sleep shifting is common, and it is thus considered ideally suited to monitoring. Fatigue was implicated as a factor in the collision of a Progress resupply rocket with the Mir space station, and crewmembers aboard the International Space Station (ISS) have also cited occasions where they performed complex and dangerous tasks (e.g., moving a Soyuz from one docking port to another) when extremely fatigued. The applicability of these concerns to military operations is readily apparent.
Also similar to military operations, space missions have very limited personnel. Space shuttle missions generally have seven-person crews, while the ISS crew complement is only three. (In the wake of the Columbia tragedy, there are currently only two crewmembers aboard the ISS. When the Shuttle fleet returns to flight status, it is anticipated that the program will return to a three-person crew.) Because of these tight personnel constraints, any tasks that can be transferred from human to artificial intelligence will free crewmembers for other mission-critical tasks. In addition, by transferring skill sets from personnel to equipment, medical decision-making, targeted assessment, and clinical judgment can be standardized and moved farther forward (onto the battlefield or on orbit) than otherwise possible. During nominal operations this “smart” technology can utilize predictive algorithms in order to analyze captured data and avoid preventable medical events.
As shown in Figure B-1, the concept of operations for this technology calls for the acquisition of data from a variety of sensors. This information is then integrated and delivered to an analytic program that can provide immediate
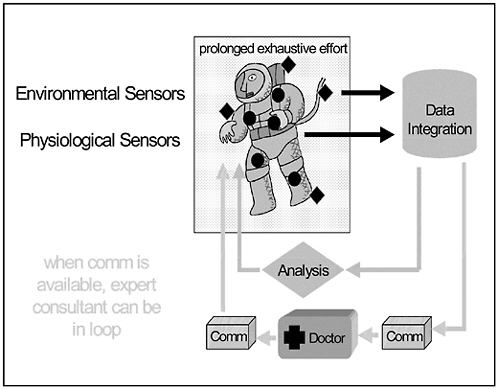
FIGURE B-1 Concept of operations.
feedback to the operator. In addition, when skilled personnel are available at a remote site, the data can be packaged and sent down a communications relay for human-based interpretation, and guidance based on the information can be provided.
There are numerous parameters that can be monitored. The selection will vary depending on the mission, the personnel, and the areas of interest. In addition, the level and type of parameter must be specified, such as individual data, group information, environmental details, and/or interactive information. For example, monitoring of an individual could report basic vital signs (e.g., body temperature, pulse oximetry, heart rate, respiratory rate, blood pressure, heart rate variability, electrocardiogram tracing) or less conventional measures (e.g., lactate levels, tissue pH, muscle creatine kinase). Individual monitoring might also focus on trends, describing specific changes within a single person over a period of time, such as a spacewalk, exercise period, or forced march. Data could also be grouped to provide critical information about the status of the crew or squad as a whole; this knowledge might be of more utility if gaining mission objectives is a higher priority than preserving individual health. Similarly, the
selection of environmental parameters will likewise vary depending on the mission, but the parameters might include items such as ambient temperature, barometric pressure, or individual activity level. Self-reported criteria (e.g., perceived exertion or interpretation of mission or task success) can also be handled in a similar fashion, with the information thus obtained being integrated with data from other sensors to provide a more global picture of the condition of the individual or team.
In order to maximize efficacy, a “smart system” is needed to obtain and present information in the most efficient way to both the end user (astronaut or warfighter) and the remote consultants (e.g., a ground-based flight surgeon or a commanding officer). In addition, analysis techniques for rapid diagnosis and intervention are required—data without a relevant context will be unusable to most operators. The components of such a system include:
-
Sensors. Many of these, particularly those for standard physiological parameters, are readily available, commercial off-the-shelf items.
-
Data integration. Information derived from multiple sensors will usually be packaged in different ways; currently there are few standards for medical data management. As a result, the monitoring system must have a way to standardize the data, integrate it, and then extract relevant parameters. In addition, trends for individual subjects need to be identified and the standardized data needs to be exported to both the algorithm library and a data store.
-
Data storage. At each stage the data must be stored for future (or real-time) downloads and review.
-
Algorithm library. In the absence of a clinician to process the information, this software provides the initial guidance to interpret the data and act upon it. In this component, the data is sent to a store of executable algorithms and decision trees, including both diagnostic and therapeutic protocols, which “crunch” the data and pass it to the next step.
-
Feedback/recommendation generation. Analysis by the algorithms or decision trees will in turn generate recommendations to prevent, mitigate, diagnose, or treat a medical event since the simple relay of data from the sensors to the average crewmember will not be of value. Prioritized alarms must also be provided, as the operator will not have the medical training to know which of several abnormal readings are most pressing. In a military example, if a casualty sustains a penetrating injury to the chest, the caregiver’s top priority may initially be to address hemorrhage and a falling blood pressure. However, if respiratory arrest then occurs, a new alarm must intervene and guide the caregiver to direct attention to that problem, otherwise his or her lack of medical training may lead to prioritizing tasks inappropriately.
-
Displays. In order to provide feedback to the operator, a local display of some kind is necessary. In addition, display of the information at a remote location enables clinicians at this site to supervise and intercede as appropriate.
Perhaps the most innovative hardware required by such a system is the data integration piece. This device must accept input from diverse data streams and packets (e.g., RS-232, RS-485, USB, 1394, Ethernet) that originate from a wide variety of sensors and medical equipment, repackage these inputs into a homogeneous format, and send the concatenated information on for integration into the algorithm library. For the ISS environment, a concept of operations has been developed that makes use of a common interface established through network appliances rather than via computers (which require human intervention). In this way, the crew needs to attach the patient, power, and communication interfaces, but does not need to establish, maintain, or troubleshoot the connections. Instead, the connections are automatically established and maintained by dedicated embedded microprocessors that are programmed to work with the specific hardware. The main goal of the device is to ensure that medical data is quickly, reliably, and accurately transmitted with a minimum amount of effort by the crew.
Toward this end, the Medical Informatics Branch of Space Medicine at NASA-JSC, in conjunction with the NASA-Ames Research Center and Stanford University, has commenced development of a Medical Communications Interface Adapter (MCIA), which is envisioned as a “smart hub,” or universal adapter for processing and downloading data from all medical devices, for accepting inputs from multiple sensors, and for providing output as multiplexed telemetry data. Three primary subsystems have been identified: an external data interface that receives information from the various devices, a data-handling subsystem that processes the information into a homogeneous format, and a ground communications subsystem that transmits the information to an algorithm library, to a data storage device, to a local display, and to remote sites (e.g., the Flight Surgeon console in the Mission Control Center). Among the medical devices currently on board or proposed for the ISS with which the MCIA would interface are a physiological monitor/defibrillator, a blood analyzer, an intravenous pump, and a ventilator. Medical teams in the military (e.g., the USAF Critical Care Air Transport Team) often use similar equipment, so this configuration may be of interest to the military as well.
Once the sensors have gathered the data and the MCIA (or equivalent) has processed it into a standard, integrated form, the data needs to be put into a clinical context. Raw data, or even consolidated information, is of little utility to a nonexpert. Telling nonclinicians that “serum lactate values have increased 20 percent within 5 minutes” does not provide them with information they can use. However, that same data, in conjunction with an algorithm library and a recommendation store, can generate useful instructions, such as “Rest in the shade for 3 minutes” or “A 5-minute break in upper arm activities is advised.” Information in this form can be utilized by any nonclinician as it requires no specialized knowledge to interpret or implement.
The value of analysis is thus twofold. On a local level, analysis can provide specific advice to an individual. This tactical advice (e.g., eat, rest, hydrate) al-
lows the warfighter or astronaut to maximize his or her work capacity. When an analysis is performed remotely on groups, it can permit strategic planning by providing flight control teams, squad leaders, or other decision makers the means by which to assess group strength and condition. In developing the best way to analyze the data, numerous factors must be considered. Generally speaking, terrestrial, validated medical algorithms and guidelines should be used whenever possible for diagnostic and therapeutic purposes. There are numerous medical algorithms (broadly defined as “any computation, formula, survey, or look-up table useful in health care”) and treatment guidelines available in the medical literature. In addition, there are commercially available, validated, off-the-shelf diagnostic tools and medical information couplers. To the greatest extent possible, these existing tools should be used rather than attempting to develop new tools as the validation process can be prohibitive in terms of both cost and time. Naturally, all of these tools are intended for terrestrial, often hospital-based, use, and they will require adaptation to an austere environment, be it military or aerospace.
Desirable features of a real-time analysis tool include smart agent-based software, multiple parameters (including environmental and physiological data), prescribed trend analysis, model-based predictions, voice-based interaction (a dialogue system), operator-initiated inquiries, and unsolicited audible suggestions or advice.
Under contingency operations the main focus of data analysis should be directed toward diagnostic and therapeutic algorithms. For example, in the context of an episode of abdominal pain, the system can send sensor data to diagnostic tools in order to obtain first a presumptive diagnosis of, for example, appendicitis, and then use this diagnosis to select appropriate treatment guidelines and algorithms that will in turn generate recommendations regarding stabilizing care and the need for immediate surgery. The system can then monitor the casualty’s response to these measures and update or modify the diagnosis and treatment recommendations accordingly.
Algorithms and guidelines for contingency operations are in varying stages of development. For treatment guidelines, there is a great deal of published material—perhaps almost too much—that can be adapted. However, because these guidelines and algorithms are derived from and developed by different medical specialties, different approaches, and even different nations, additional work is required to integrate them into a single consensus position on the best treatment modality. Diagnostic algorithms are less widely available and tend to be least helpful for illnesses with vague or general symptoms and signs. For example, as any clinician would attest, determining the cause of “abdominal pain” or “dizziness” can be very difficult. By contrast, diagnostic tools can be more easily applied to conditions with a clear mechanism or pathognomonic findings, such as “mechanical airway obstruction” or “tension pneumothorax.”
There is likely to be only minor use of predictive algorithms in contingency operations for space compared with the use of diagnostic and treatment guide-
lines. Once an event has occurred, more attention will be focused on addressing it than on predicting its course. One exception might be in the case of a serious traumatic injury. In the absence of care from a surgical intensive care unit, a trauma scoring system might be employed to predict the patient’s condition so that this information could assist in a decision about the timing of a crew evacuation.
For nominal operations, however, predictive and preventive algorithms will be more widely used. For example, these algorithms could determine whether a continuing trend in body temperature presages imminent heat exhaustion, which interventions in the short term could prevent this from occurring, and which intervention would be most appropriate. Unfortunately, these algorithms are generally in the very early stages of development, and it will be necessary to develop and test research models before these tools become operational.
To perform research into the early tracking of signs and symptoms and their predictive value in describing the condition’s ultimate outcome or natural history, data gathering must occur at the outpatient- or family practice-based level, rather than at the inpatient- or subspecialty-based level. Research that is primarily located in the hospital will focus on the later stages of pathology and thus be less useful to our needs. Our interest lies in the earliest (perhaps asymptomatic) stages of a potentially disabling condition, and thus data must be gathered from primary caregivers or even from the lay public (as in, “What makes you go to the doctor for some headaches but not for others?”).
Like predictive algorithms, preventive algorithms and guidelines are also in very rudimentary form. They are often anecdotal or qualitative (e.g., “Stay out of the sun!”) rather than quantitative (e.g., “Rest in shade for 5 minutes.”), and a relatively small number have been rigorously validated. Given that the system sensors gather information about physiological parameters in a highly quantified manner, it may be that the data they obtain can be fed back into predictive algorithm models so that the algorithms will also (eventually) be able to anticipate the onset of symptoms quite precisely.
Algorithm development by the Office of Space Medicine is at an early stage. Rules must be established for both format and content. For authoring activities, a standard, user-friendly format is needed for all algorithm developers. In addition, the format must be able to integrate into the current informatics system so as to avoid lengthy data-entry steps. In terms of the content contained in the algorithms, it is necessary to ensure a standardized approach across authors with clear logic flow, shared assumptions, appropriate evidence, and explicit decision points. A process must be established for thorough review by all stake-holders, and an evidence-based rationale for each point must be included. Ideally, the format should lend itself to easy incorporation of content references. Lastly, the algorithm must be displayed in such a way as to permit easy use by the operators.
The work being conducted by the Medical Informatics and Health Care Systems branch (led by Dr. James Logan) is called the Global Onboard Detailed
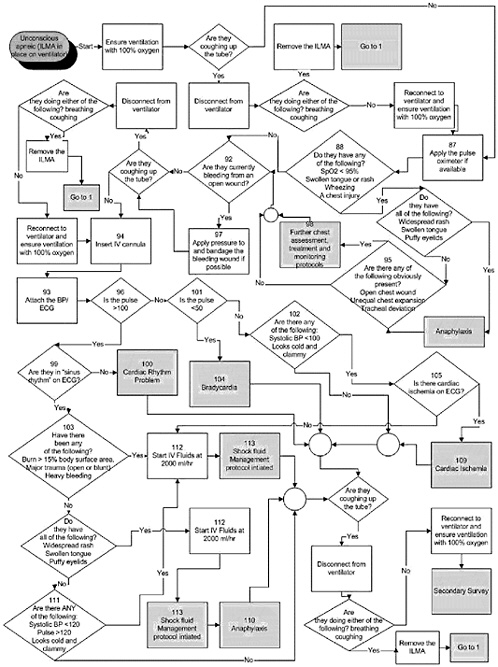
Diagnostic and Evaluation Systemic Survey (GODDESS). It is divided into two subtasks: one to provide an initial evaluation and stabilization of the patient, the other to initiate more detailed diagnostic and therapeutic activities. In the ISS Systemic Initial Survey (ISIS), the goal is to identify and address any immediate, life-threatening conditions and then to direct the caregiver to the appropriate diagnostic and treatment pathway. The content (see Figure B-2) and format for ISIS have been developed and are currently in the validation process. The Astronaut Total Health Network Algorithms section (ATHeNA) will contain both diagnostic and treatment pathways. A format for ATHeNA is in development, and several treatment guidelines are currently in draft form. Once the guidelines have been written and validated, the section will be integrated with ISIS and the entire system validated in an end-to-end fashion.
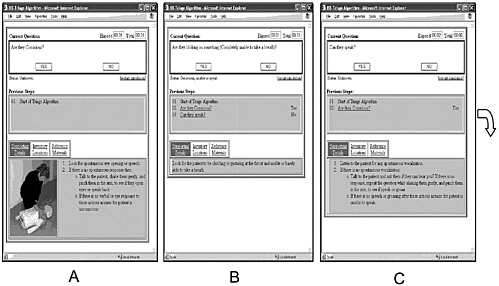
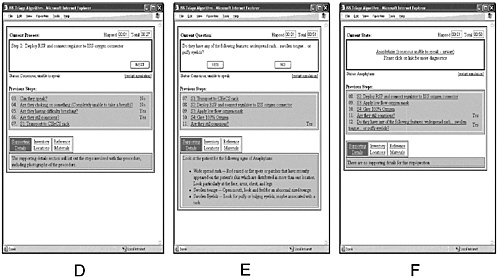
As shown in Figure B-3, the ISIS interface is to be immediately activated upon recognition of a medical event. The standardized questions begin with “Are they conscious?” (A). For example, in a case of anaphylaxis, the caregiver would answer “Yes.” ISIS would then ask the caregiver, “Can they speak?” (B). Subsequent questions are designed to rule out an obstructed airway (C) and to initiate care (D). Within a few moments, additional questions discriminate among various conditions (E) until anaphylaxis is identified as the presumptive diagnosis (F). At this point, ISIS has completed its role and ATHeNA takes over, although this transition is transparent to the user.
Using the same interface, ATHeNA guides the caregiver through the proper treatment guidelines, providing inventory locations, supplemental information, and additional guidance as required. If the chief complaint had been of lower acuity than anaphylaxis (e.g., abdominal pain, headache, or nausea), ISIS would simply have ruled out the life-threatening conditions and ATHeNA would have initiated a secondary survey in which the caregiver (or patient himself, depending on his condition) would have answered a series of diagnostic questions designed to lead to a presumptive diagnosis. The patient’s individual medical history would have been automatically fed into the software so that if, for example, a person with abdominal pain had an appendectomy in the past, appendicitis would have automatically been removed from the differential, but pain due to adhesions would have been added.
Once a presumptive diagnosis is reached through ISIS or ATHeNA, appropriate treatment begins and the patient’s response is monitored. In addition to the data obtained through the medical devices (such as blood pressure, heart rate, or temperature), the system also prompts the caregiver to reassess the patient at regular intervals and information regarding response to analgesics, appetite, nausea, and other subjective parameters is entered, so constant review and revision of the diagnosis and treatment occurs. For a ventilated patient, ATHeNA makes use of closed-loop algorithms to adjust the ventilator settings so as to ensure maximum efficacy. Eventually, perhaps tasks such as medication administration (e.g., sedatives, antibiotics, analgesics) will be automatically
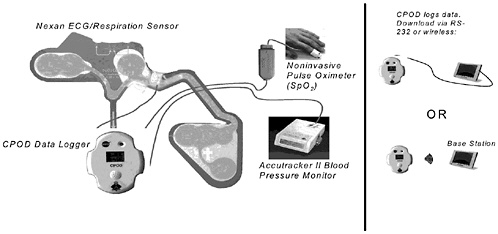
FIGURE B-4 A schematic of the LifeGuard Monitoring System.
performed by ATHeNA, though in the short term it is likely that this will continue to require human intervention, presumably with guidance from ATHeNA.
The GODDESS project is obviously intended for use in contingency operations. An example of a project intended for use under nominal conditions is Stanford and NASA-Ames’ LifeGuard Monitoring System, which is in its final stages of testing. LifeGuard is an example of a novel system designed to obtain, aggregate, and analyze physiological data, display it locally, transmit it, and recommend interventions. The current model can interface with a variety of commercially available sensors (e.g., the Nexan ECG/respiration sensor, the Accutracker II blood pressure monitor, and a noninvasive pulse oximeter) that all connect to a CPOD Data Logger. The CPOD then logs the data and-downloads it via an RS-232 or a wireless (see Figure B-4). Table B-1 contains an example of the functional and performance requirements levied against the device.
In summary, remote metabolic monitoring systems are of utility in multiple operational environments, including aerospace and military activities. To create such tools, it is first necessary to identify the parameters of interest (e.g., physiological, environmental), then to capture, process, and transmit the data. Following analysis, in which potential or actual medical conditions are diagnosed and appropriate interventions are developed, these data (with recommended actions) can be displayed both locally and remotely. The system then continues to monitor the intervention and its outcome and provides updated advice. In this way,
TABLE B-1 Sample Requirements for the LifeGuard Monitoring System
|
Measured Parameters |
Device Functionality |
Derived Parameters |
Base Station Functions |
Data Transfer Requirements |
|
Electrocardiogram (2 channels) |
Acquisition/signal conditioning of all sensor data |
Respiration rate (from respiration waveform) |
Download data from wearable device |
Wired (RS-232) and short-range (10m) wireless |
|
Respiration (raw waveform) |
Analog to digital conversion |
Heart rate (from electrocardiogram) |
Store downloaded data on storage media |
Data is downloaded to base station one user at a time |
|
Body temperature |
Data logging (internal memory in wearable device) |
|
Display downloaded data |
Single base station |
|
Activity (2-axis acceleration) |
Data transmission to base station on demand |
|
Derive parameters (respiration and heart rates) |
Minimum operational lifetime of wearable device: 8 hr |
|
Pulse oximetry |
Status display |
|
|
Wearable device, pager-size |
|
Blood pressure (noninvasive) |
|
|
|
|
technology can move specialized knowledge farther forward operationally, providing artificial substitutes for the skilled professionals who are so often in short supply. Work of this nature must be interdisciplinary in approach, utilizing engineers, information specialists, and clinicians in order to build a functional, validated, and user-friendly system.
Acknowledgments: NASA-Johnson Space Center/National Space Biomedical Research Institute: Jim Logan, Rick Pettys, Subhajit Sarkar, M.G. Sriram, Christopher Stokes; NASA-Ames Research Center/Stanford University: Sekou Crawford, John Hines, Kevin Montgomery.