1
Introduction
There is no question that the pandemic can be defeated. No matter how terrible the scourge of AIDS, no matter how limited the capacity to respond, no matter how devastating the human toll, it is absolutely certain that the pandemic can be turned around with a joint and Herculean effort between the African countries themselves and the international community.
—Stephen Lewis
The discovery of highly active antiretroviral (ARV) therapy (ART) and its introduction in developed countries is considered by many to be one of the greatest success stories of modern medicine—this despite still-critical concerns regarding toxicity, adherence, and the widespread development of viral resistance. These concerns cannot negate the dramatic reductions in HIV-associated morbidity and mortality that have resulted from the widespread introduction of triple-combination ART in the mid-1990s. Two decades ago, it was common for HIV-infected patients to present in U.S. clinics and hospitals with only a 10-month survival as their prognosis. Today, ARV-treated patients can generally anticipate leading a good-quality life for many years.
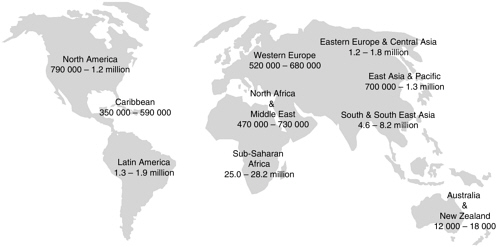
The provision of safe, effective ART to the millions of individuals in need in resource-constrained settings is likewise expected to dramatically reduce HIV/AIDS-related morbidity and mortality, improve quality of life, and increase social and political stability. The challenge is great, however, as HIV/AIDS has progressed largely unchecked in many parts of the world where the epidemic has been underestimated and shrouded in denial and stigma (see Figure 1-1).
Of the 40 million people worldwide infected with HIV, an estimated 6 million are in need of immediate, life-sustaining ART. Yet only around 400,000 people in low- and middle-income countries have access to such treatment (WHO, 2003) (see Table 1-1). Most HIV-infected individuals live in severely resource-constrained settings, where the HIV epidemic continues to grow at a rate of 5 million infections per year, compounding the
TABLE 1-1 Coverage of ART in Developing Countries, 2003 (adults by WHO region)
|
Region |
Number of People on ART |
Estimated Need |
Coverage |
|
Africa |
100,000 |
4,400,000 |
2% |
|
Americas |
210,000 |
250,000 |
84% |
|
Europe (Eastern Europe, Central Asia) |
15,000 |
80,000 |
19% |
|
Eastern Mediterranean |
5,000 |
100,000 |
5% |
|
Southeast Asia |
60,000 |
900,000 |
7% |
|
Western Pacific |
10,000 |
170,000 |
6% |
|
All WHO Regions |
400,000 |
5,900,000 |
7% |
|
SOURCE: WHO, 2003. |
|||
already enormous treatment challenge. The high AIDS mortality rate in sub-Saharan Africa, which remains the worst-affected region in the world, contrasts sharply with the decreasing HIV-related death rate in high-income countries where ARVs are widely available and affordable. Those acutely affected by the widespread lack of treatment include not only the millions of infected individuals, but also the millions of children orphaned when their parents die from HIV-related illness. Because HIV-related deaths occur disproportionately among young, economically productive adults, moreover, the epidemic is undermining the economic development and social fabric of entire countries (Bell et al., 2003; Dixon et al., 2001).
CHALLENGES AND OPPORTUNITIES: ANTIRETROVIRAL THERAPY IN RESOURCE-CONSTRAINED SETTINGS
Most of the clinical, epidemiological, behavioral, and other aspects of the HIV/AIDS pandemic have been addressed predominantly within the United States and other resource-rich settings. As a result, there are a multitude of unanswered questions regarding how best to introduce ARVs on a broad scale in resource-constrained settings, where the public health and drug delivery infrastructures are often weak or nonexistent and operational capacity is largely lacking. Although several pilot initiatives worldwide have garnered early success and proven the feasibility of implementing ART programs in resource-poor settings, we have yet to determine how these pilot initiatives can be scaled up to meet larger needs. No one program or country can provide all the answers.
The urgent demand to provide free or affordable ARVs to the millions of people in need must be tempered by awareness of the crucial importance
of acting rationally and making decisions based on the best scientific evidence so that the long-term durability of individual patient regimens and the sustainability of ART programs will not be jeopardized. A lack of careful planning could create conditions conducive to treatment failure and the development of drug-resistant virus, leading ultimately to disillusionment and demoralization. While avoiding delays in delivering treatment, the international and national communities of donors, planners, and providers must remain vigilant in seeking continued improvements and necessary course corrections to maximize treatment benefits and extend as many lives as possible. Failed programs using first-line regimens, regardless of the reasons for failure, necessitate much more costly and less-sustainable second-line regimens or result in the termination of ART for affected patients; they also limit treatment opportunities for others afflicted today and for the tens of millions of additional HIV-infected persons anticipated over the next decade or so.
Ultimately, the best lessons may be learned from ART scale-up itself. Critical to the long-term success of these programs will be their ability to recognize where both desired outcomes and failures are encountered. These programs, their leaders, and their funders will require sufficient flexibility and commitment to quality to ensure that changes, when necessary, are made.
For now, ART programs already in various stages of implementation throughout the developing world provide advice worth heeding (see Figure 1-2). Some of these programs have met with success, others with high rates
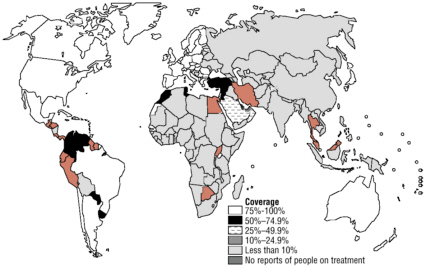
FIGURE 1-2 Estimated worldwide coverage with antiretroviral treatment at the end of 2003.
SOURCE: WHO, 2004.
of drug resistance. Suboptimal introduction of ART in both Cote d’Ivoire (Adje et al., 2001) and Gabon (Vergne et al., 2002), for example, has led to high levels of drug resistance in treated patients, as well as treatment failure due to unsustainable drug supplies (and consequent inadequate dosing) and health care infrastructures without the capacity to detect resistance. ART programs in Uganda (Weidle et al., 2002), Senegal (Laurent et al., 2002), and Haiti (Mukherjee et al., 2003; Farmer et al., 2001), on the other hand, have shown preliminary success, with clinical, biological, and therapeutic results similar to those seen in developed-country cohorts—this despite variable HIV-1 subtypes and advanced stages of disease at treatment outset.
Questions remain about the impact—positive or negative—that major investments in ART will have overall on health care systems in developing countries (Benatar, 2004; Walton et al., 2004). Evidence-based assessments are still needed to determine the effects of large-scale ART programs on HIV/AIDS prevention efforts and other health care initiatives. It will be important to determine in different settings the extent to which integration of ART programs into the general health care system will be most appropriately balanced with other needs. This is of particular concern because of the already strained and often inadequate overall health care infrastructure and workforce in many developing countries for the delivery of effective medical care and treatment (Narasimhan et al., 2004; USAID, 2003).
Despite these challenges and unresolved issues, recent ARV price cuts due to international competition among generic and proprietary drug manufacturers have led to a conviction that it is possible to provide universal, comprehensive HIV/AIDS treatment and care. In fact, general consensus exists today that minimization of resistance can be achieved by accelerating the introduction of ARVs worldwide in a rational manner.
This conviction, coupled with growing political, ethical, and humanitarian concerns, has elevated HIV/AIDS to the top of the political and financial agendas of many national governments and international organizations. Increased domestic and external funding for HIV/AIDS programs and continuing drug price negotiations are enabling a growing number of low- and middle-income countries to provide or promise affordable ARVs and other HIV-related medications to at least some of their citizens (Pogge, 2002).
BEYOND THE BIOMEDICAL MODEL
HIV/AIDS, like many other emerging infectious diseases, is symptomatic of major changes in the ways people live in today’s world. The pandemic has arisen in the wake of complex social and economic forces that have widened disparities in health and wealth, disrupted living conditions, and created new ecological niches for the emergence or reemergence of
disease (Garrett, 1995). While the biomedical approach to responding to the global HIV/AIDS crisis is a necessary first step and has already demonstrated its strength by prolonging the lives of tens of thousands of people, a sustainable response will require addressing the upstream social, economic, and environmental events and factors that have led to the emergence of this pandemic and will likely influence the emergence of future pandemics as well (Benatar, 2002). As with tuberculosis, for example, HIV/AIDS has largely become a disease of the poor, so understanding and addressing threats that perpetuate and aggravate poverty and marginalize the millions of HIV-infected people worldwide is especially important (Houweling et al., 2001; Katz, 2002; Murray and Lopez, 1999; The Return of the White Plague, 2003; Wood et al., 2002).
ART scale-up in resource-constrained settings will depend on the generous support of wealthy nations, at least in the near future (see Table 1-2). Yet sustaining improved health care and population health in the distant future will ultimately require new, ambitious ways of thinking about how to enhance the capabilities of people and nations so they can become self-sufficient and independent of philanthropy. For example, debt roll-back or a shift toward fairer trade rules could be implemented concurrently with the introduction of ART to boost the capacity of local governments in poor countries to provide the education and health care needed to promote greater self-sufficiency (Benatar, 2003). The importance of sustainability and the need to address upstream economic, social, and ecological factors that to date have received inadequate consideration are now beginning to receive the scholarly attention they deserve (Ferraro and Rosser, 1994; Pettifor, 2003a,b; Labonte et al., 2004; Sreenivasan, 2002).
Long-term sustainability aside, even a successful short-term response requires addressing social and behavioral aspects of HIV/AIDS that lie outside the traditional realm of epidemiological and biomedical modeling of infectious disease transmission. Improving patient adherence to therapy, for example, involves more than patient education. It also requires addressing social problems that contribute to program dropout, such as AIDS-related stigma and familial dysfunction (e.g., the disruption that ensues when more than one family member is infected with HIV). Likewise, minimizing increased risky behavior once ARVs become widely available will involve more than patient or public education: it will require addressing the underlying, pervasive social conditions that generate such behavior.
Global disparities in health, disease, and behavior and, most particularly, the forces that generate these disparities pose great threats to the implementation of medical interventions that offer hope for the future. Understanding and acknowledging these forces that imperil global health and having the will to address them are essential complements to the introduction of modern treatments.
TABLE 1-2 Income and Health Resources of Selected Countries
|
Country |
Gross National Income per Capita ($) 2002a |
Health Expenditures per Capita ($) 1997–2000 |
Physicians per 1,000 People 1995–2000 |
|
United States |
35,060 |
4,499 |
2.8 |
|
Brazil |
2,850 |
267 |
1.3 |
|
PEPFAR Countriesb |
|||
|
Botswana |
2,980 |
191 |
NAc |
|
Cote d’Ivoire |
610 |
16 |
0.1 |
|
Ethiopia |
100 |
5 |
NAc |
|
Guyana |
NAc |
NAc |
NAc |
|
Haiti |
440 |
21 |
0.2 |
|
Kenya |
360 |
28 |
0.1 |
|
Mozambique |
210 |
9 |
NAc |
|
Namibia |
1,780 |
136 |
0.3 |
|
Nigeria |
290 |
8 |
NAc |
|
Rwanda |
230 |
12 |
NAc |
|
South Africa |
2,600 |
255 |
0.6 |
|
Tanzania |
280 |
12 |
0.0 |
|
Uganda |
250 |
10 |
NAc |
|
Vietnam |
430 |
21 |
0.5 |
|
Zambia |
330 |
18 |
0.1 |
|
aFollowing current statistical practice, the World Bank recently adopted new terminology in line with the 1993 System of National Accounts (SNA). Therefore, gross national product per capita is now called gross national income per capita. (See http://www.worldbank.org/data/changinterm.html for more information.) bPEPFAR = The President’s Emergency Plan for AIDS Relief. cNA = not available. SOURCE: World Bank, 2004. |
|||
GOALS OF THE STUDY
In consideration of the issues outlined above, the Institute of Medicine was asked to provide a rapid, independent review and assessment of ART scale-up programs under way and in development. This fast-track study was initiated in late November 2003 to provide guidance and establish a framework of principles for decision making in anticipation of the growing number of investments in ART scale-up programs. The Committee on Examining the Probable Consequences of Alternative Patterns of Widespread Antiretroviral Drug Use in Resource-Constrained Settings was charged to provide (1) an examination and evaluation of current ART implementation programs, efficacy studies, infrastructure costing models, existing guide-
lines for program implementation, and models that demonstrate successful scale-up of ART programs; (2) a study of the role of ongoing well-developed operations research in the field and in parallel with treatment implementation to establish sustainability outcome measures; (3) a determination of the components necessary for a systematic, structured framework to achieve a balance between resistance development and transmission and the need to provide treatment in resource-constrained settings; and (4) an assessment of current research on ARV resistance and toxicity, including the likely effects on the malnourished individuals with high disease burden found in resource-poor settings.
STUDY APPROACH
The committee formed to conduct this study encompassed broad international expertise in the clinical and basic research aspects of HIV/AIDS, epidemiology, virology, pathology, ethics, behavioral science, community medicine, health care financing and policy, and public health. The members of the committee were also chosen for their first-hand experience with HIV/ AIDS in a wide range of middle- and low-income countries. The committee members are listed at the beginning of the report and are briefly profiled in Appendix G.
The data needed for this study were identified by the committee members and other experts representing disciplines relevant to the committee’s charge. Although a large proportion of the findings on HIV/AIDS in developing countries has been published in international and national journals and reports, many important findings have appeared in local journals, the proceedings of meetings, and unpublished reports prepared for the World Health Organization (WHO) and other international organizations. To tap this knowledge base, the committee enlisted a broad range of experts with recent research or service experience in developing countries. Data and supportive evidence were provided by these experts through workshop presentations, commissioned papers, and technical consultation on chapters of this report (for additional information, see Appendix A). The framework for the committee’s deliberations included an overview of the available epidemiological parameters; a review of the existing knowledge base on interventions; and projections of the feasibility, cost, and impact of proposed interventions.
The combined weight of such evidence, the committee believes, has produced an accurate account of the state of knowledge concerning the introduction of ARVs in resource-constrained settings and the capacity of local health care systems to provide such treatment. Evaluation of the available evidence enabled the committee to identify gaps in knowledge and to propose strategies for a research agenda that would fill these gaps. The
findings, strategies, and recommendations presented in this report were developed from this broad base of evidence.
ORGANIZATION OF THE REPORT
This report reviews the issues surrounding the large-scale introduction of ART into resource-constrained settings; conditions necessary for the long-term sustainability of quality ART programs; and steps that must be taken to achieve an appropriate and adequate balance among the priorities, benefits, and risks of introducing ART into these settings. The report is organized into six chapters.
Following this introduction, Chapter 2 describes some of the most recent initiatives and investments by international donors and national governments that will provide the foundational elements of large-scale ART programs in the developing world. In highlighting these efforts, the committee describes issues that will require further resolution as ART programs evolve, such as the need for global and national coordination of financial, technical, and human resource investments; ethical considerations at the international, national, and local levels; and, the importance of ensuring the long-term fiscal sustainability of these programs to avert the dire medical consequences of treatment interruption or termination. (Additional ethical issues for consideration are presented in Appendix D.)
Chapter 3 responds to the committee’s charge to examine and evaluate current ART programs and to assess what these programs and additional research reveal about the potential implications of the emergence of drug-resistant strains of HIV. To this end, it describes the phenomenon of the evolution of drug-resistant viruses, tools for anticipating the magnitude of drug resistance among populations, and the current and potential implications of such developments for ART scale-up in resource-constrained settings. The chapter also includes a collection of lessons learned from ART programs in developing countries with varying degrees of resource constraints, disease burden, and overall health care infrastructure. (Additional background information on ARV-resistant viruses is contained in Appendix B.)
In setting forth the principles to be applied in scaling up ART programs, Chapter 4 outlines a set of framework components that the committee believes to be essential for establishing effective, quality care that can respond to the overwhelming burden of HIV/AIDS in many resource-constrained environments. In responding to its charge in this area, the committee built its findings and recommendations upon extant knowledge from the field and the outcomes of operations research related to ART programs in developed and developing countries. Informed by these lessons learned, Chapter 4 identifies the obstacles and opportunities involved in developing
ART programs that encompass the reduction of stigma and discrimination, as well as the identification of points of entry for treatment, such as programs for voluntary counseling and testing and tuberculosis treatment and control. A guiding set of clinical principles is described that is grounded in an assessment of existing program implementation guidelines. Strategies are included for selecting treatment regimens; for using laboratories to diagnose, initiate, and monitor therapies; and for meeting the treatment needs of special populations, such as pregnant women, children, and those suffering also from opportunistic infections, especially tuberculosis. Emphasis is placed on the benefits of treatment programs that are synergized with prevention efforts, and on the critical importance of adherence to treatment to ensure the life-sustaining effects of the therapy and prevent the emergence of drug-resistant virus that not only would result in individual treatment failure, but also might jeopardize the long-term durability of select drug regimens at the population level.
Additional essential components of ART scale-up are described in Chapter 5. Inextricably linked to the success of drug interventions will be logistics systems that ensure the safe and timely procurement and delivery of the drugs and include effective information and data collection systems. This chapter emphasizes the paramount importance of a properly trained workforce that comprises not only those who will administer ART, but also those who will effectively manage, monitor, and continuously optimize the scale-up of ART programs and ensure the adequate training and allocation of human and technical resources. (Further analysis of these issues is presented in Appendix E.) Barriers to be overcome in developing these multidimensional resources include the lack of adequate training programs and access to education in most resource-constrained countries, the effects of “brain drain” that usurps talented yet limited in-country resources, and the inability to sustain and secure a robust supply chain of drugs because of unreliable funding sources.
In all of its findings and recommendations throughout Chapters 2 through 5 regarding the components of a system for scaling up ART, the committee emphasizes the critical need for a learn-by-doing approach and the current paucity of data to support such efforts. The unprecedented nature of the scale-up of ART programs to treat many millions of people in resource-constrained settings leaves decision makers and practitioners without a well-evaluated, evidence-based strategy at the outset of program implementation. Thus, Chapter 5 concludes by detailing how discretely and adequately funded monitoring and evaluation of new and expanding ART programs can provide multiple benefits, including the ongoing realignment and optimization of ART programs and systems with regard to their effectiveness, quality, and allocation of human, technical, and financial resources; the development of an evidence base and scientific knowledge that
can inform the design and implementation of new programs in the future (identifying earlier programs or elements that worked and should be expanded and those that should be abandoned); and the provision of data and evaluation results that establish accountability and allow for the measurement of intended outcomes essential to securing continued funding by international donors and national and local governments.
In the report’s final chapter, the committee continues to highlight the need to know more and to develop better strategies and more effective tools so as to improve the effectiveness of treatment programs for HIV/AIDS. The chapter sets forth priorities for an operations, clinical, and behavioral research agenda that will enable both iterative and breakthrough improvements for ART. The report concludes with a sobering call to the many decision makers, researchers, and practitioners who will take up arms against this deadly plague to heed the crucial lesson learned from ongoing investigations: that within the imperative to act now, it will also be important to act well.
|
Defining a Country’s Wealth Low income = a country having an annual gross national income (GNI) per capita equivalent to $735 or less in 2002. Middle income = a country having an annual GNI per capita between $736 and $9,075 in 2002. High income = a country having an annual GNI per capita equivalent to $9,076 or greater in 2002. Note: Gross national income is equivalent to gross national product according to the new World Bank terminology. SOURCE: World Bank, 2004. |
REFERENCES
Adje C, Cheingsong R, Roels TH, Maurice C, Djomand G, Verbiest W, Hertogs K, Larder B, Monga B, Peeters M, Eholie S, Bissagene E, Coulibaly M. 2001. High prevalence of genotypic and phenotypic HIV-1 drug-resistant strains among patients receiving antiretroviral therapy in Abidjan, Cote d’Ivoire. Journal of Acquired Immune Deficiency Syndromes 26:501–506.
Bell C, Devarajan S, Gersbach H. 2003. The Long-Run Economic Costs of AIDS: Theory and an Application to South Africa. Washington, DC: World Bank.
Benatar SR. 2002. The HIV/AIDS pandemic: A sign of instability in a complex global system. Journal of Medicine and Philosophy 27:163–177.
Benatar SR. 2003. Ethics and tropical disease: Some global considerations. In: Manson P, ed. Tropical Diseases. 21st Edition. London, UK: Saunders. Pp. 85–93.
Benatar SR. 2004. Health care reform and the crisis of HIV and AIDS in South Africa. New England Journal of Medicine 351(1):81–92.
Dixon S, McDonald S, Roberts J. 2001. The impact of HIV and AIDS on Africa’s economic development. British Medical Journal 324(7331):232–234.
Farmer P, Leandre F, Mukherjee JS, Claude M, Nevil P, Smith-Fawzi MC, Koenig SP, Castro A, Becerra MC, Attaran A, Kim JY. 2001. Community based approaches to HIV treatment in resource-poor settings. Lancet 358:404–409.
Ferraro V, Rosser M. 1994. Global debt and third world development. In: World Security: Challenges for a New Century. Klare M, Thomas D, eds. New York: St. Martin’s Press. Pp. 332–355.
Garrett L. 1995. The Coming Plague: Newly Emerging Diseases in a World Out of Balance. New York: Penguin Books.
Houweling TA, Kunst AE, Malkenbach JP. 2001. World Health Report 2000: Inequality index and socioeconomic inequalities in mortality. Lancet 357:1671–1672.
Katz A. 2002. AIDS, individual behavior and unexplained remaining variation. African Journal of AIDS Research 1:125–142.
Labonte R, Schrecker T, Sanders D, Mecus W. 2004. Fatal Indifference: The G8, Africa, and Global Health. Ottawa, Canada: University of Cape Town Press.
Laurent C, Diakhate N, Gueye NF, Toure MA, Sow PS, Faye MA, Gueye M, Laniece I, Toure Kane C, Liegeois F, Vergne L, Mboup S, Badiane S, Ndoye I, Delaporte E. 2002. The Senegalese government’s highly active antiretroviral therapy initiative: An 18-month follow-up study. AIDS 16:1363–1370.
Mukherjee J, Colas M, Farmer P, Leandre F, Lambert W, Raymonville M, Koenig S, Walton D, Nevil P, Louissant N, Orelus S. 2003. Access to Antiretroviral Treatment and Care: The Experience of the HIV Equity Initiative. Cange, Haiti: WHO.
Murray CJ, Lopez AD. 1999. Mortality by cause for eight regions of the world: Global burden of disease study. Lancet 349:1269–1276.
Narasimhan V, Brown H, Pablos-Mendez A, Adams O, Dussault G, Elzinga G, Nordstrom A, Habte D, Jacobs M, Solimano G, Sewankambo N, Wilbulpolprasert S, Evans T, Chen L. 2004. Responding to the global human resources crisis. Lancet 363(9419):1469–1472.
Pettifor A. 2003a. The Legacy of Globalization: Debt and Deflation. Pettifor A, ed. New York: Palgrave Press.
Pettifor A. 2003b. Resolving international debt crises fairly. Ethics and International Affairs 17(2)2–9.
Pogge T. 2002. World Poverty and Human Rights: Cosmopolitan Responsibilities and Reforms. Cambridge, UK: Polity Press.
Sreenivasan G. 2002. International justice and health. Ethics and International Affairs 16(2)81–90.
The Return of the White Plague. 2003. Gandy M, Zumla Z, eds. New York: Oxford Univer-sity Press.
UNAIDS. 2003. AIDS Epidemic Update. Geneva: UNAIDS.
USAID (U.S. Agency for International Development). 2003. The Health Sector Human Resource Crisis in Africa: An Issues Paper. [Online]. Available: http://www.aed.org/ToolsandPublications/upload/healthsector.pdf [accessed August 23, 2004].
Vergne L, Malonga-Mouellet G, Mistoul I, Mavoungou R, Peeters M, Monsaray H, Delaporte E. 2002. Resistance to antiretroviral treatment in Gabon: Need for implementation of guidelines on antiretroviral therapy use and HIV-1 drug resistance monitoring in developing countries. Journal of Acquired Immune Deficiency Syndromes 29:154–158.
Walton DA, Farmer PE, Lambert W, Leandre F, Koenig SP, Mukherjee JS. 2004. Integrated HIV prevention and care strengthens primary health care: Lessons from rural Haiti. Journal of Public Health Policy 25(2):137–158.
Weidle P, Malamba S, Mwebaze R, Sozi C, Rukundo G, Downing R, Hanson D, Ochola D, Mugyenyi P, Mermin J, Samb B, Lackritz E. 2002. Assessment of a pilot antiretroviral drug therapy programme in Uganda: Patients’ response, survival, and drug resistance. Lancet 360:34–40.
WHO (World Health Organization). 2003. Treating 3 Million by 2005. Making it Happen. The WHO Strategy. Geneva: WHO. [Online]. Available: http://www.who.int/3by5/en/ [accessed July 26, 2004].
WHO. 2004. The World Health Report 2004: Changing History. Geneva: WHO.
Wood E, Montaner JS, Chan K, Tyndall MW, Schechter MT, Bangsberg D, O’Shaughnessy MV, Hogg RS. 2002. Socioeconomic status, access to triple therapy, and survival from HIV-disease since 1996. AIDS 16:2065–2072.
World Bank. 2004. World Development Report 2004: Making Services Work for Poor People. Washington, DC: World Bank.