4
Principles of Scale-up
Much has been learned from both developed and developing nations that have accomplished large-scale antitretroviral therapy (ART), and it is now clear that effective scale-up is a realistic objective in many settings. Before this can happen, however, the stigma and discrimination that can hamper efforts to curb the global HIV/AIDS pandemic must be addressed. To initiate the scale-up process, countries will have to identify those needing treatment, as well as the various possible points of entry into treatment programs. Once persons in need have been identified, scale-up efforts should be guided by a core set of principles. The many lessons learned from previous country efforts (see Chapter 3) have allowed the World Health Organization (WHO) to formulate a set of such guidelines that countries may wish to use as a template for beginning scale-up. These guidelines include strategies for diagnosing HIV and AIDS, deciding when to initiate therapy, determining which regimen to use given the characteristics of the population needing treatment, and deciding when and how to monitor therapy.
While these strategies can serve as a useful guide, however, treatment providers must remain cognizant of the limitations associated with their particular setting. Resource-constrained settings are beset by other health problems, such as tuberculosis (TB) and malnutrition—both of which will affect the opportunities and challenges faced during scale-up. Additionally, the success of any ART program will depend upon many factors, crucial among which is adherence to therapy. The many lessons learned about adherence from past experience with ART (see Chapter 3) can be applied
during the initiation and implementation of treatment programs in resourceconstrained settings. Finally, the integration of prevention and treatment is essential, as is palliative care for AIDS patients in developing countries.
REDUCING STIGMA AND DISCRIMINATION
Stigma and discrimination, often driven by fear, can undermine efforts to treat and care for persons with HIV/AIDS. With HIV/AIDS, fear of illness, contagion, and death can affect not only patients themselves, but also those living with and caring for them, such as family members, co-workers, and health care workers. In addition to the stigma associated with the infection and the disease itself, persons with HIV/AIDS may face the stigma associated with belonging to a specific group, such as homosexuals, prostitutes, injection drug users, or persons engaging in “casual” sex. Stigma can result in silence, denial, ostracism, and violence.
Clearly, these reactions can impact interest in and ability to seek diagnosis and care for HIV/AIDS. Stigma and discrimination can discourage people from finding out about and revealing their HIV status, which in turn can affect prevention and treatment efforts. In Africa, 90 percent of HIVinfected people still do not know of their status (Harries et al., 2002); fear of stigma could be one reason for this. Stigma also can affect the quality of care received by people diagnosed with HIV/AIDS. A survey of 1,000 Nigerian physicians, nurses, and midwives, for example, assessed the prevalence of stigma and discrimination (UNAIDS, 2003a). Fully 10 percent of providers admitted to having refused care or denied admission to a hospital for a patient with HIV/AIDS. Almost 40 percent of those interviewed believed that a person’s appearance revealed his or her HIV-positive status, while 20 percent believed that people with HIV/AIDS had behaved immorally and deserved their fate. Factors contributing to these attitudes and behaviors included a lack of knowledge about the virus; a lack of protective equipment, prompting fear among health care providers of acquiring the infection from patients; and frustration at not having medications to treat HIV/AIDS patients, who therefore were “doomed” to die.
Strategies to reduce stigma may include providing information, counseling, imparting coping skills, and promoting social interaction with persons living with HIV/AIDS. It is possible that providing treatment for HIV/ AIDS may decrease stigma by restoring health, which in turn will allow those infected to live symptom-free and engage in work and community activities, and by reducing fear of contagion and death. By providing hope to people living with HIV/AIDS, the widespread availability of ART may reduce the stigma associated with seeking testing and treatment.
Unfortunately, the literature documenting effective methods for reducing the stigma associated with HIV/AIDS in resource-poor settings needs to
be strengthened considerably. Referring to health-related stigma in developing countries in general, the Fogarty International Center of the National Institutes of Health (NIH) has written: “Little is known about the pervasiveness of stigma in the developing world and how healthcare systems can tackle its negative consequences. Effective action has been slow in coming, in part because of the continuing gaps in knowledge” (NIH, 2003). In recognition of this lack of knowledge, in 2002 NIH launched a Stigma and Global Health Research Program. The first 19 awards under the program were announced in October 2003; expected 5-year funding for the program is approximately $16.5 million (NIH, 2003). The NIH grant recipients will establish a global network of researchers to “develop the field of stigma and global health research by testing hypotheses and generating data on the etiology of stigma and effective interventions for its negative effects on health” (NIH, 2003). The network will help identify best practices, opportunities, and obstacles in research on stigma related to global health. Through the studies conducted by this network and others, culture-specific interventions to reduce stigma, perhaps tailored to different demographic groups, should be tried and evaluated.
In June 2001, the United Nations General Assembly Special Session on HIV/AIDS issued a Declaration on Commitment on HIV/AIDS. This declaration included a provision for UN Member States to “develop strategies to combat stigma and social exclusion connected with the epidemic” and “enact, strengthen or enforce, as appropriate, legislation, regulations and other measures to eliminate all forms of discrimination against . . . people living with HIV/AIDS…” (UNAIDS, 2003a). According to a UNAIDS report in 2003, almost half of all African countries had adopted no legislation to prevent discrimination against people living with HIV/AIDS (UNAIDS, 2003b).
Recommendation 4-1. Governmental and community leaders at all levels of civic life should spearhead an effort to create a culture of openness and support in order to eliminate stigma and ensure the successful continuance of antiretroviral treatment and HIV prevention programs.
IDENTIFYING POINTS OF ENTRY
Identifying persons in immediate need of treatment provides one challenge for the efficient and effective scale-up of ART. As noted earlier, there are multiple possible points of entry for treatment programs, each of which may target different sectors of the population and initially identify infected persons at different stages of the disease.
Early detection and counseling to prevent subsequent transmission, with regular follow-up, are desirable even though patients initially entering
care at a later stage of infection are more likely to be immediately clinically eligible to begin ART under the WHO guidelines endorsed by the committee. The former patients also may be more likely to remain in care. At the same time, the challenges of beginning care and treatment for those in the latest stages of disease include reconstituting a highly suppressed immune system and the necessity of treating opportunistic infections, such as TB. For these and other reasons, mortality may be higher for patients entering care at later disease stages, as was the case for patients enrolled in treatment programs in Haiti (Fitzgerald, 2004) (see Chapter 3).
Existing health care facilities—already providing services for other health needs—may take on HIV/AIDS testing and treatment as scale-up unrolls. The screening of military personnel and other occupational groups can also serve as entry points for ART. Three additional points of entry may be considered during scale-up: voluntary counseling and testing centers, mother-to-child transmission prevention programs, and TB treatment and control programs.
Voluntary Counseling and Testing Programs
Only 5–7 percent of people in most developing countries know their HIV status (WHO, 2003a). Clearly then, counseling and testing must precede ART and HIV/AIDS care. At the same time, voluntary counseling and testing (VCT) centers established to provide these services offer the opportunity to address a comprehensive range of measures for HIV/AIDS prevention, treatment, and care. Though the majority of apparently healthy persons seeking to know their status can be diagnosed most effectively in VCT programs, some asymptomatic persons will be found HIV-positive through other mechanisms, such as blood bank screening. Such patients should still be referred to VCT programs to ensure that preventive counseling is provided in conjunction with entry into ART programs. Requiring that capable HIV-positive patients obtain VCT clinic counseling prior to receipt of ARVs may encourage disclosure and foster the linkage of treatment, prevention, and care.
Counseling and testing involve risk evaluation, facilitated decision making following testing, and education about preventive measures for those found to be HIV-negative or -positive. UNAIDS has identified several critical elements of counseling and testing programs: testing should be voluntary; results should be kept confidential; counseling should focus on the individual client’s needs; HIV-positive and -negative persons should be referred for ongoing support; and stigma-reducing activities should be incorporated into the services provided (CDC, 2004; UNAIDS, 2000). Centers offering VCT services can serve as an important link to medical and
support programs that provide treatment and care for those eligible to receive ART. Same-day testing sites can facilitate this linkage.
Mother-to-Child Transmission Prevention Programs
Pregnancy can provide an opportune point of entry for women who might not otherwise seek health care for themselves. In addition, antenatal clinics are used to collect data for HIV prevalence estimates (UNAIDS, 2003a).
In the history of treating and caring for those with HIV/AIDS, special attention has focused on preventing transmission of the virus from mother to child. Mother-to-child-transmission (MTCT) prevention programs have been established to provide specialized services to women during their pregnancy and then to the children they bear during the immediate postpartum period. While MTCT prevention programs can provide an opportunity for women to enter health care, in some regions of resource-poor settings only 1 percent of women have access to these services. Moreover, partner opposition can reduce the likelihood of participating in these programs.
Building on the success of these programs, the Maternal-to-Child-Transmission-Plus (MTCT-Plus) Initiative was established in 2002 (Columbia University Mailman School of Public Health, 2004). The goal of this initiative is to provide specialized care, including ART, to HIV-infected women during and following pregnancy, to their children, and to their partners. The program’s comprehensive reach provides an opportunity for family members to enter a system of care and for mothers to receive continued care following childbirth.
The MTCT-Plus Initiative is coordinated by the Mailman School of Public Health at Columbia University and is funded by private foundations and the U.S. Agency for International Development (USAID). The programs operate in 12 sites ranging from rural clinics to teaching hospitals—11 in sub-Saharan Africa and 1 in Thailand. The comprehensive HIV/AIDS care provided includes ART, therapy for the prevention and treatment of opportunistic infections, TB prevention services, nutrition support, family planning, and supportive services. Recognizing that HIV/AIDS has psychosocial as well as clinical dimensions, the programs use multidisciplinary teams of providers and supporters that include nurses, counselors, and pediatric and adult physicians.
As of November 2003, 2,000 people had been enrolled in MTCT-Plus programs. Women can enroll in the programs either during or following pregnancy; currently, 40 percent are enrolled antepartum and 60 percent postpartum. In recognition of the fact that HIV/AIDS affects families, not just individuals at risk for or with HIV/AIDS, and that family-based endeavors may improve overall treatment and care, enrollment is offered to
other members of the household as well. Of the 2,000 people enrolled as of November 2003, one-third were children, and one-fifth were partners of the (index) women.
The programs target people at the earlier stages of disease. The mean CD4 count of patients beginning treatment is 379. The index women are at a less advanced stage of disease than their partners who become enrolled. Most of the infants enrolled in the program are of indeterminate status; they are followed clinically as an effort to provide comprehensive family care.
Each MTCT-Plus site uses standardized protocols with respect to treatment eligibility criteria, treatment monitoring, toxicity management, drug regimens, and pediatric dosing. An attempt is made to harmonize these protocols with both country-specific and WHO guidelines. The antiretrovirals (ARVs) used in these programs are procured by UNICEF; approximately half are generic products.
CLINICAL PRINCIPLES
Because of the complexity of HIV and AIDS, WHO established clinical guidelines in 2003 as part of its 3-by-5 campaign (see Chapter 2) to assist programs in scale-up of ART (WHO, 2003b). These guidelines take into account experience gained in the clinical management of HIV/AIDS in the developed world and lessons learned from treating the disease in the developing world. Data from clinical trials and observational studies underlie the guidelines.
In recognition of the limitations faced by resource-constrained settings, such as cost and availability of drugs and diagnostics, the WHO guidelines offer suggestions specific to these settings. The guidelines provide a framework that can be used to standardize and simplify treatment for this complex disease and encompasses the point at which to start therapy; first- and second-line combination regimens; considerations involved in treating subgroups of patients, such as those coinfected with TB, pregnant women, and children; means of monitoring therapy; and indicators for changing regimens. As noted earlier, these recommendations are based on scientific and clinical experience and evidence, drug availability and cost, the requirement to refrigerate some ARVs, the need for and availability of laboratory monitoring, drug toxicity profiles, and the risk of drug interactions. The guidelines acknowledge limitations in areas in urgent need of research, such as the treatment of pregnant women and individuals coinfected with TB. Nonetheless, they provide a critically important starting point by outlining simple criteria and steps that can be used in even the most resource-poor settings.
The WHO guidelines can be used by providers with a range of experience in diagnosing and treating people with HIV/AIDS. The simplified,
standardized guidance they offer can be indispensable given that many ART scale-up programs in resource-limited settings need to rely on community involvement and the recruitment of unskilled workers or health care professionals with little or no experience in managing such programs. At the same time, however, HIV/AIDS experts warn that these guidelines should not be considered a substitute for local program manuals. Nor should they be used to underestimate the complex nature of ART, the need for context-specific individualized care, and the reality that early treatment decisions can profoundly alter the course of disease and limit a patient’s response to future therapy in the case of first-line failure.
Recommendation 4-2. Before countries develop their own directives, the World Health Organization’s 2003 guidelines for the treatment of adults, children, and pregnant women should serve as an initial template for the design of antiretroviral therapy programs with respect to when to start therapy, which regimens to use, how to monitor the progress of therapy, and when to switch drugs or terminate therapy. As new evidence becomes available, through the efforts of international, national, and local research, the WHO guidelines, particularly with regard to pregnant women and those coinfected with tuberculosis, may require refinement or modification.
One clinical principle that deserves mention is that because therapy for HIV/AIDS is an ongoing process, an adequate longitudinal medical record is an essential tool in patient management. In many developing countries, medical records systems will need significant improvement, especially where those records are currently held by the patient or where documentation is organized around discrete visits rather than continuity of care. Relevant training in longitudinal medical record keeping and changes in patient flow through the clinic should be considered, where needed, to facilitate this process.
The remainder of this section reviews in turn considerations involved in using the laboratory to diagnose, initiate, and monitor ART; selecting a treatment regimen; treating dual epidemics of HIV and TB; treating women; treating pregnant women; treating children; and addressing the role of nutrition in HIV/AIDS and its treatment.
Using the Laboratory to Diagnose, Initiate, and Monitor ART
In the developed world, laboratory and clinical criteria weigh heavily in the initiation and monitoring of ART. Cost and infrastructure needs may limit the ability of resource-constrained settings to use such a laboratory-intensive approach for treating patients with HIV/AIDS.
In the developed world, standard tests administered prior to beginning therapy include a test to detect HIV, followed by a confirmatory test; a test to determine CD4 T cell count—a marker of immune function and disease stage; and a test to determine the amount of virus present in the blood (viral RNA or viral load)—a marker of disease burden. The WHO guidelines do recommend baseline HIV testing and, when possible, CD4 T cell count (or the surrogate marker, total lymphocyte count [TLC]) prior to initiation of therapy (see Appendix B, Table A). While a confirmatory test to diagnose HIV is preferable, if a second test (e.g., rapid antibody test, Western Blot) is not available, therapy should proceed based on clinical criteria defining AIDS stage (see Appendixes B and E).
In the developed world, CD4 T cell count and viral RNA load are assessed throughout therapy to monitor progress and determine the success of the therapeutic regimen. When laboratory tests such as CD4 T cell count and viral load are not available, the WHO guidelines recommend the use of clinical criteria for symptomatic appraisals to ensure that therapy can be monitored in settings without sophisticated laboratory capacity or personnel.
Finally, because of potential side effects and toxicities of ARVs—and the progression of HIV infection—additional baseline laboratory tests obtained in less resource-constrained countries include determinations of red blood cell count, renal function, liver enzymes and function, and lipid status (U.S. Department of Health and Human Services, 2003). WHO recommends additional tests such as these when infrastructure allows (see Appendix B, Table E).
Laboratory testing can be costly and require sophisticated laboratory infrastructure and trained technicians. A CD4 T cell count is typically determined using a flow cytometer for measurement and is costly. Of note, there are no data indicating what degree of CD4 or viral load testing translates into cost-effective clinical or public health benefits. For example, in the United States, no trial has been conducted to compare clinical end-points between patients who received viral load testing and those who did not.
Less-expensive technologies and surrogate laboratory markers are available and have been used in the developing world to monitor therapy. While a flow cytometer is commonly used to quantify CD4 T cell count and assess disease stage and progression, some countries have used alternative technologies to garner this information. A West African study, for example, demonstrated the utility of Dynabeads, a low-cost alternative to the flow cytometer based on epifluorescent microscopy (Diagbouga et al., 2003). The cost of an epifluorescent microscope is approximately half that of the least-expensive flow cytometry equipment, and the reagent cost per assay is only 12 percent of the cost of the assay for a CD4 T cell count (Diagbouga
et al., 2003). Another technology, the Cytosphere bead assay, is reportedly easier to use but more expensive (US$8/test, compared with $3–5/ Dynabead test, as of December 2002). Even these alternative technologies, however, are limited by the need for trained technicians, an element of subjective interpretation, the need for refrigeration and a reliable power source, and fatigue associated with the manual nature of the technology. Because of these concerns and limited formal evaluation, WHO has recommended that both methods be evaluated in a multicenter study before being officially recommended to laboratories in the developing world.
As noted, TLC has been suggested as a surrogate for CD4 T cell count; indeed, it is recommended by WHO. Since the CD4 T cell is one type of lymphocyte, CD4 T cell count correlates with TLC. A number of reports have shown TLC to be a useful predictor of significant immunosuppression, as measured by a CD4 cell count of less than 200/µL in HIV-infected persons. If TLC were used to determine who was eligible to start therapy, a lower level would increase specificity (by increasing the likelihood that people with high CD4 counts would not be incorrectly targeted for therapy) but decrease sensitivity (by increasing the likelihood that people with low CD4 counts would not be identified).
The cost of laboratory tests is only one of many costs associated with laboratory monitoring of HIV/AIDS patients. The procurement and proper use of assays and reagents depend on an enormous amount of infrastructure, which may include data management programs; laboratory equipment and supplies (e.g., refrigerators, freezers, centrifuges, thermocyclers, and pipettes); proficiency testing programs; laboratory accrediting agencies, and skilled technicians. At an even more basic level, effective laboratory monitoring relies on a range of nonlaboratory resources that are taken for granted in resource-rich countries, such as reagent-grade water, electrical power, and theft prevention measures. Securing infrastructure and resources can be very costly and is particularly important given that theft is a large problem in many resource-constrained settings. It may be particularly challenging to obtain and maintain these resources in rural areas of resource-constrained settings, where infrastructure may be even weaker.
Recognizing the infrastructure costs and limitations in resource-constrained settings, WHO has set forth guidelines for conducting laboratory testing prior to initiating therapy, for monitoring therapy, and for defining treatment failure (see Box 4-1). The WHO recommendations are tiered for primary health centers, district hospitals, and regional referral hospitals.
Recommendation 4-3. Donors and program managers should plan and budget for laboratory activities that will foster more accurate and effective HIV diagnosis and management, using the World Health Organization’s 2003 guidelines as the initial template. Incorporating
|
BOX 4-1
SOURCE: WHO, 2003b. |
emerging evidence and resources into their decision-making process, countries should consider developing population-specific guidelines reflective of the best possible practices in their particular circumstances. In those localities where it is possible to go beyond the WHO guidelines, treatment failure should be defined through viral RNA determination; otherwise, it should be defined by means of clinical or other laboratory markers consistent with the guidelines.
Recommendation 4-4. Under the leadership of their ministries of health and national reference laboratory experts, all countries should develop hierarchical laboratory networks that integrate the local, district, and referral hospital levels through tiered quality assurance programs and provide referral support for increasingly complex laboratory assays. Full development of these networks is not required before the initiation of scaled-up antiretroviral therapy programs, however. National reference laboratories should promulgate tier-specific quality assurance protocols, and donors supporting ART programs should provide the means
to properly ensure acceptable technical performance by these laboratory networks. Dedicated funds, training, and other resources to ensure the maintenance of laboratory equipment employed in these networks should be provided. To better facilitate the diagnosis and treatment of HIV infection in infants less than 18 months of age, the laboratory networks should put in place a capacity for the direct detection of HIV, such as HIV DNA, HIV RNA, or HIV p24 antigen.
Clinical criteria for monitoring treatment progress have been used in developing countries. While there are many reasons during both health and disease for weight gain or loss, patient weight has been one clinical marker used in developing countries to judge the success of ART. In the event that clinical criteria are used for treatment monitoring, however, it must be recognized that such criteria do not always provide an accurate assessment of viral suppression, and even patients who appear to be doing well may fail in their regimen if viral suppression is not above a certain threshold. Initial treatment regimens should be selected based on this awareness. The degree to which laboratory services for toxicity monitoring are used also requires special consideration in resource-constrained settings with limited infrastructure. The necessity for laboratory monitoring may be tailored to the use of certain ARVs. For example, when nevirapine is used in combination with other drugs, hepatoxicity testing may be important, whereas when zidovudine is used, a hemoglobin determination for anemia might be considered.
Selecting a Treatment Regimen
In the developed world, regimen selection is quite intricate because of the availability of numerous drugs and the infrastructure needed to deliver and monitor therapy, the affordability of drugs (through third-party payers in some cases), and the ability to tailor regimens to virus susceptibility. Because resource-constrained settings may not have these advantages, WHO has recommended four first-line regimens for HIV/AIDS treatment. These regimens, summarized in Table 4-1, take into account toxicities, appropriateness for use in TB-coinfected patients and in pregnant women, availability as a fixed-dose combination (FDC) (see Box 4-2), cost, and laboratory monitoring requirements. Regimen design also must take into account the population being treated with respect to age, gender, pregnancy status, and comorbid infections.
According to the WHO guidelines, ARV regimens that have been shown scientifically to be ineffective or less effective than other available regimens should not be used. Specifically, mono- or dual-therapy regimens and nucleoside-only regimens should be avoided. According to a recent
TABLE 4-1 WHO-Recommended Antiretroviral Therapy Regimens for Persons in Resource-Constrained Settings
|
Regimen |
Major Potential |
Toxicities Used forWomen ofChildbearing Age During Pregnancy |
Used for Those with TB Coinfection |
Fixed-Dose Combination Available |
Laboratory Monitoring Requirements |
|
d4T/3TC/NVP |
d4T-related neuropathy, pancreatitis, and lipoatrophy; NVPrelated hepatotoxicity and severe rash |
Yes |
Yes, in rifampicinf ree continuation phase of TB treatment; used with caution in rifampicin-based regimens |
Yes |
No |
|
ZDV/3TC/NVP |
ZDV-related gastrointestinal intolerance, anemia, and neutropenia; NVP-related hepatotoxicity and severe rash |
Yes |
Yes, in rifampicin-free continuation phase of TB treatment; used with caution in rifampicin-based regimens |
Yes |
Yes, because of ZDV-associated bone marrow suppression |
|
d4T/3TC/EFV |
d4T-related neuropathy, pancreatitis, and lipoatrophy; EFV-related central nervous system toxicity and potential for teratogenicity |
No |
Yes, but EFV should not be given to pregnant women or women with childbearing potential unless effective contraception can be ensured |
No (d4T/3TC available in FDC) |
No |
|
ZDV/3TC/EFV |
ZDV-related gastrointestinal intolerance, anemia, and neutropenia; EFV-related central nervous system toxicity and potential for teratogenicity |
No |
Yes, but EFV should not be given to pregnant women or women with childbearing potential unless effective contraceptioncan be ensured |
No(ZDV/3TC available in FDC) |
Yes, because of ZDV-associated bone marrow suppression |
|
NOTE: 3TC = lamivudine; d4T = stavydubel; EFV = efavurebzl; FDC = fixed-dose combination; NVP = nevirapine; TB = tuberculosis; ZDV = zidovudine. SOURCE: Adapted from WHO, 2003:Table B. |
|||||
|
BOX 4-2 Fixed-dose combinations (FDCs) are pills that contain more than one drug per tablet. FDCs are available for a variety of disease conditions, including HIV and AIDS. The World Health Organization has recommended using FDCs, when available, for the treatment of HIV/AIDS, provided their quality and bioequivalence to individual drug therapy have been proven, and they would be advantageous to individual programs delivering ART. FDCs have a number of potential advantages:
At the same time, FDCs pose several challenges:
SOURCES: MSF Briefing Note, 2004; WHO, 2003b. |
Cochrane review of randomized controlled trials comparing the effects of three- or four-drug ARV regimens versus two-drug regimens, the latter were associated with higher levels of failure of viral suppression and resistance (Rutherford et al., 2004) (see also Chapter 3). Although it may be desirable in some cases to reduce the number of drugs for adherence or toxicity reasons, ART with at least three drugs should be the standard.
Recommendation 4-5. Antiretroviral therapy programs should be designed to optimize the balance between individual efficacy and population effectiveness while minimizing toxicity and resistance. ART regimens or programs shown to be significantly less effective or ineffective—such as mono- or dual-therapy and nucleoside-only regimens—must be avoided. Because resources and population and patient needs will vary considerably among different countries and regions, countries should develop population-specific guidelines.
An initial template guiding regimen selection may prove especially useful to programs that have not yet developed their own treatment guidelines.
The need for such a template is illustrated by the case of Harare, Zimbabwe, where national guidelines were not available to the practitioners and pharmacists who prescribed and stocked ARVs. The treatment and management of HIV/AIDS patients in that setting have been described as “therapeutic anarchy,” with at least 17 percent of 92 patients receiving AZT monotherapy, a regimen not recommended by HIV/AIDS experts (Nyazema et al., 2000; U.S. DHHS, 2003).
Treating Dual Epidemics of HIV and TB
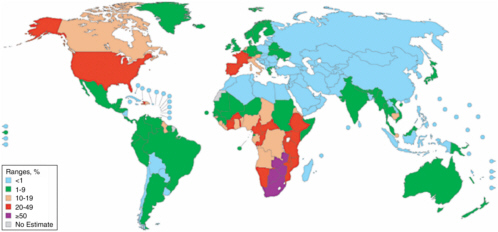
The TB and HIV/AIDS epidemics exist in parallel in many resourceconstrained settings (see Box 4-3). Of the 42 million people worldwide infected with HIV, an estimated 11 million are coinfected with TB (WHO, 2003c) (see Figure 4-1). While ART programs may be new for many countries, these same countries may have experience with TB control and treat-
|
BOX 4-3 Tuberculosis (TB) is one of the leading causes of AIDS-related death; together, TB and HIV/AIDS represent the two greatest infectious disease killers in the world. Worldwide, 42 million people are infected with HIV, and 2 billion are infected with TB. Of the 42 million people with HIV, nearly one-third are coinfected with TB. In sub-Saharan Africa, TB is the leading cause of death in coinfected persons (Ridzon and Mayanja-Kizza, 2002). Primary TB infection occurs when a person inhales a threshold amount of Mycobacterium tuberculosis bacilli. In most persons, no signs or symptoms are present, and the infection is contained. This then becomes “latent” TB infection. If the immune system is sufficiently compromised—which occurs in a variety of noninfectious diseases—latent TB can progress to active TB, which can be pulmonary, or extrapulmonary or disseminated. Most active TB results in pulmonary disease. With advanced immune compromise, such as when a person has AIDS (CD4 cell count < 200 /mm3), extrapulmonary or disseminated disease is more likely. Examples of extrapulmonary TB infection include brain abscesses, meningitis, pericarditis, gastric TB, scrotal TB, and bone marrow infection. While the risk of developing active disease from latent TB infection is 10 percent during the lifetime of an immunocompetent person, the risk in a person with HIV/AIDS is 4–10 percent yearly (Corbett et al., 2003; Fennelly and Ellner, 2004). Additionally, having TB accelerates the progression of HIV/AIDS (Ridzon and Mayanja-Kizza, 2002). TB is the most common opportunistic infection in HIVinfected patients. Additionally, TB is the only opportunistic infection that can be transmitted to persons without HIV. Of note, though, is that HIV-infected persons |
ment programs. As the rate of coinfection is high, the latter programs may, as noted earlier, be a useful point of entry for HIV/AIDS diagnosis and care. Indeed, it is estimated that 500,000 people with HIV/AIDS could be reached through existing TB programs (Kim, 2004). WHO recognizes this opportunity to detect HIV/AIDS cases and recommends that in countries with an HIV prevalence exceeding 5 percent, HIV testing and counseling be offered to everyone with TB (WHO, 2003a).
In 1998, the World Health Initiative began its ProTEST initiative to provide collaborative services for both HIV and TB (London School of Hygiene and Tropical Medicine, 2002; Elzinga and Nunn, 2002; Gorkom, 2003). The project was begun in South Africa, Malawi, and Zambia and later expanded to additional African countries. VCT is used as the entry point for prevention and care services. Clients are screened for sexually transmitted infections, including HIV, and HIV-infected persons are
|
with TB are no more infectious than HIV-negative persons with TB (Ridzon and Mayanja-Kizza, 2002). Latent TB is noninfectious. TB can be difficult to diagnose in immunocompromised people; if diagnosed, however, it is easily treatable. Treatment reduces morbidity and mortality in TB– HIV coinfected persons. Even treatment of latent TB infection can be successful. Using isoniazid for latent TB infection and highly active antiretroviral therapy (HAART) for HIV can reduce the risk of conversion from latent to active TB infection. With one exception, treatment for active TB is the same for HIV-infected and HIV-negative persons and requires the administration of multiple drugs in combination. The one exception is the rifamycin component of therapy, which requires a particular type of administration for HIV-infected persons who simultaneously are on HAART. With respect to the treatment of HIV and of TB, because of drug–drug interactions, pill burden, and potentially additive toxicities of regimens, the decision to start therapy for each condition and when to do so requires careful consideration and additional research. The 2003 WHO guidelines for the treatment of HIV-infected persons in resource-limited settings provide some initial guidance for beginning treatment for HIV in the coinfected (WHO, 2003b). (For further information, refer to Appendix B, Table A. and Section VIII C.) Directly observed therapy for TB has been shown to be effective in both the developed and developing worlds and may be considered, when feasible, for improving adherence and treatment outcomes. Finally, the emergence of multidrug-resistant tuberculosis (MDR-TB) in the setting of HIV treatment should be noted. TB in HIV clinics in general, and MDR-TB specifically, constitutes an important nosocomial threat that should be addressed proactively through appropriate infection control initiatives. SOURCES: Fennelly and Ellner, 2004; WHO, 2003c,d. |
screened for TB. Those diagnosed with infections are then referred for further support and treatment.
The immune deficiency created by HIV infection increases the risk of developing active TB, while TB increases the mortality of those with HIV (Havlir and Barnes, 1999). Indeed, TB is the leading cause of death in HIV-positive patients in the developing world (Corbett et al., 2003; Harries et al., 2002). Specifically, individuals latently infected with TB who are HIV-negative have a 10 percent lifetime risk of developing active TB after infection, while those who are HIV-positive may have nearly a 10 percent annual risk of developing active disease (Corbett et al., 2003). The coexistence of the two diseases in populations thus has implications for disease progression and prevention, as well as treatment priorities.
Recommendation 4-6. Program managers, international donors, and national policy makers should ensure that strong tuberculosis control programs continue in parallel with antiretroviral treatment scale-up programs, given that nearly one-third of HIV-infected persons in the world are coinfected with tuberculosis. Because dual infection with HIV and tuberculosis poses a life-threatening diagnostic and therapeutic dilemma, strong HIV care programs must include capabilities for diagnosis, treatment, and prophylaxis of tuberculosis. Tuberculosis treatment programs should be supported as an important point of entry for HIV testing and consideration for ART. It is critical to overall treatment success that these coexisting epidemics be addressed in parallel.
Case finding and treatment for each of these epidemics in parallel can have profound effects on morbidity and mortality. The experience in Brazil highlights some of these successes. As in the United States, when ART was made more widely accessible in Brazil, the number of cases of pulmonary TB declined (Schechter, 2004); the incidence of TB fell by 80 percent when highly active antiretroviral therapy (HAART) was introduced. Furthermore, when TB prophylaxis was prescribed for HIV-infected patients, TB mortality decreased by 80 percent in just 4 years (Levi and Vitória, 2002). In South Africa, similar success was seen. In an observational study, patients receiving HAART had a significantly lower incidence of TB than those not receiving HAART, with an overall risk reduction of 81 percent.
Isoniazid has proven effective in reducing the incidence of active TB in HIV-positive patients and has been used effectively in some resource-constrained settings, such as those in Africa (Harries et al., 2002). In a review of randomized controlled trials comparing TB preventive therapy with placebo for HIV-positive individuals, it was found that preventive therapy reduced the rate of active TB by 50 percent over an average follow-up
period of 15 to 33 months. This review included trials conducted in resource-poor settings, such as Haiti and sub-Saharan Africa (Wilkinson et al., 1998).
The WHO-sponsored ProTEST projects, previously discussed as a point of entry for case finding, combine comprehensive services for the HIV/AIDS and TB epidemics. The goal is to reduce disease burden more efficiently than would be possible if care and treatment programs for each were run separately (Elzinga and Nunn, 2002).
Treating each disease in a coinfected person is complicated by treatment costs, drug interactions, pill burden, and patient acceptance of both diagnoses. WHO has suggested initial guidelines but recognizes that data are limited on which to base specific treatment recommendations for this special population. In cases in which HIV disease stage cannot be determined by CD4 T cell count, WHO recommends ART for all HIV-positive patients with TB. Additionally, WHO recommends that the treatment for TB remain a central priority and not be compromised by ART. The timing of treatment for both infections poses a challenge. WHO recommends beginning ART 2 weeks to 2 months after the patient has been stabilized on TB treatment. While ART may be lifesaving for those with TB and advanced HIV, consideration of pill burden, drug interactions, and toxicity must help guide decisions to treat both infections.
The ART regimen selected for coinfection reflects the risk of rifampicin drug interactions with nonnucleoside reverse transcriptase inhibitors (NNRTIs) and protease inhibitors (PIs); the first-line regimen for patients with coinfection is (zidovudine or stavudine) + lamivudine + efavirenz. Using abacavir instead of efavirenz offers, among other advantages, lower pill burden and no interaction with rifampicins. Of note, however, abacavir is associated with hypersensitivity syndrome and decreased viral potency; for these reasons, it was removed from the first-line regimen options for persons with HIV. Using nevirapine instead of efavirenz also is possible but must be done with caution while using rifampicin because of effects on immunological response and toxicity.
As the two epidemics have similar characteristics, including the need for long-term treatment, the possibility of drug resistance, and multidrug therapy with strict adherence requirements, TB control programs could provide a model for delivery of ART for HIV (Gupta et al., 2004; Harries et al., 2002). In particular, directly observed therapy programs for TB have been used as models for the treatment of HIV/AIDS (see Chapter 3).
Beyond the threat of TB in general as an opportunistic infection, there is the additional concern of the emergence of multidrug-resistant tuberculosis (MDR-TB) in HIV patients and its nosocomial spread. In Lima, Peru, Campos and colleagues (2003) found that the prevalence of MDR-TB was 43 percent in HIV-infected persons with TB versus 2–3 percent in non–
HIV-infected persons with TB. This finding may be attributable to concentration of HIV care in hospital-based clinics where MDR-TB patients also were obtaining care. During the scale-up of clinics for ART, it will be essential that rigorous attention be paid to environmental, personal protective, and administrative measures to ensure effective infection control. As these measures can be costly and necessitate infrastructural work, proactive planning and budgeting are important. Overcrowded, poorly ventilated clinics that bring together large numbers of HIV-infected persons, some with active TB, will be a recipe for disaster.
As important as TB is among the opportunistic infections in HIV/AIDS patients, it is only one of several for which an intervention may be beneficial. Table 4-2 summarizes recommendations for prophylaxis and immuni-
TABLE 4-2 U.S. Recommendations for Opportunistic Infection Prophylaxis and for Vaccinations in Persons with HIV/AIDS
|
CD4 Count Risk Factor |
Infectious Agent |
Prophylaxis Recommended |
First Line Prophylaxis |
|
< 200 |
Pneumocystis carinii |
Yes |
trimethoprim-sulfamethoxazole |
|
< 100 |
Toxoplasma gondii |
Yes |
trimethoprim-sulfamethoxazole |
|
|
fungal infections |
No |
|
|
< 50 |
Mycobacterium avium complex |
Yes |
azithromycin (or clarithromycin) |
|
|
cytomegalovirus |
No |
|
|
Any |
Mycobacterium tuberculosis |
Yes if PPDa > 5 mm |
isoniazid, pyridoxine, rifampin, pyrazinamideb |
|
Any |
Pneumococcus |
Yes |
pneumococcal vaccine |
|
Any |
influenza |
Yes |
influenza vaccine |
|
Any |
hepatitis B |
Yes |
hepatitis vaccine |
|
Any |
hepatitis A |
Yes if history of hepatitis B or C and seronegative for hepatitis A |
hepatitis vaccine |
|
aPositive tuberculin skin test. bA combination of these drugs is required, and regimen selection should be based upon MTB resistance epidemiology. |
|||
zation for opportunistic infections in the United States. While all of these recommendations may not be indicated in highly resource-constrained countries, prophylaxis with cotrimoxazole does provide significant benefit (Grimwade and Swingler, 2004) in settings with susceptible organisms. Specifically, a Cochrane Review meta-analysis of three African trials indicated that cotrimoxazole was associated with a reduction in death (relative risk 0.69 [95 percent confidence interval 0.55 to 0.87]), morbid events (0.76 [0.64 to 0.9]), and hospitalization (0.66 [0.48 to 0.92]).
Treating Women
Globally, women make up 50 percent of those afflicted by the AIDS pandemic. In sub-Saharan Africa, more woman than men are infected with HIV. In this region, teenage girls are infected at rates up to four to seven times those of their teenage male counterparts (Fleischman, 2004; UNAIDS/ WHO, 2003). There are biological, economic, and sociocultural reasons for this disparity (Fleischman, 2003). Biologically, women are more susceptible to HIV for several reasons, including the efficiency with which male-to-female sexual transmission occurs through the large mucosal surfaces of the female genital tract. Moreover, economic dependence upon men may create an inequitable power relationship that can have far-reaching consequences for women’s health. From a sociocultural perspective, women may have limited power to negotiate when and with whom they have sex, as well as whether to use safer sex practices, and they also may have limited access to information about HIV prevention.
Women may be less likely to get tested or to seek and receive treatment because of gender-based inequalities. In a Kampala hospital, only 10 percent of women had disclosed their HIV status to their partners, with fear of abandonment and discriminination being the most common reasons cited (Phillips, 2004). Fear of violence also affects women’s decision to seek testing and care. Globally, from 10 to 50 percent of women report being physically abused by intimate male partners at some point during their lifetime, and this abuse can be accompanied by sexual violence (Heise et al., 1999; UNAIDS, 2004). At a VCT center in Tanzania, 37 percent of women reported a history of one or more physically abusive partners, and HIV-positive women were more than twice as likely as HIV-negative women to report that their current partner was physically or sexually abusive (Maman et al., 2002). A recent study in South Africa also found that women in controlling or violent relationships were at higher risk of contracting HIV infection (Dunkle et al., 2004). Other factors that could influence access to and use of ART by women include household and childrearing responsibilities affecting the priority accorded to obtaining health care; lack of control over finances in the household; and a focus on treatment of other members
of the family, including the unborn children of women when pregnant (e.g., in programs for prevention of MTCT).
Treating Pregnant Women
Much research has been conducted on the treatment of pregnant women with HIV/AIDS in both the developed and developing worlds, and reduction of MTCT of HIV in developed countries is considered one of the greatest success stories of the HIV/AIDS pandemic. Despite what has been learned, however, success has not been widespread. In sub-Saharan Africa, where it is common for more than 10 percent of pregnant women to be infected with HIV, only 1 percent of pregnant women in some countries have access to services aimed at preventing MTCT (WHO, 2003a).
In the early 1990s in the United States, prior to the availability of ARV prophylaxis for MTCT, approximately 1,600 HIV-infected babies were born to about 6,000 HIV-infected mothers—a transmission rate of about 25 percent (Mofenson, 2003a). Following a seminal study of zidovudine prophylaxis given to mothers ante- and intrapartum and to newborns postpartum, this rate of transmission dropped to 8 percent (Mofenson, 2003b). This study, the Pediatric AIDS Clinical Trial Group (PACTG) protocol 076, used a complex three-part zidovudine regimen administered to HIV-infected women beginning at 14 to 34 weeks gestation, then intravenously during labor, and finally to the newborn for 6 weeks (Mofenson, 2003b).
The rate of transmission in the developed world has now decreased to less than 2 percent with the use of HAART, cesarean delivery, and avoidance of breastfeeding (Mofenson, 2003a,b). As a result of these interventions, the number of infants born with HIV each year has been reduced to 400 (Mofenson, 2003a). European countries have reported similar successes (European Collaborative Study, 2001; The Italian Register for Human Immunodeficiency Virus Infection in Children, 2002). The mechanisms by which the three-part zidovudine regimen afforded such protection in PACTG 076 were (1) a modest decrease in the mother’s viral load, thereby exposing the baby to less virus transplacentally; (2) preexposure prophylaxis of the baby through transplacental passage of the drug; and (3) postexposure prophylaxis of the baby after the baby had passed through the birth canal.
Despite its potency, a three-part zidovudine regimen is too complex and expensive for use in severely resource-constrained settings. Accordingly over the past 10 years, other effective and less-expensive ARV interventions for prevention of MTCT have been identified. Single-dose nevirapine is one such intervention. Not only does nevirapine prophylaxis work, but nevirapine-based programs are feasible and cost-effective for resource-limited settings. In a recent 12-month study conducted in Lusaka, Zambia,
1,654 mothers and 1,157 infants were administered nevirapine. It is estimated, based on expected transmission rates in the absence of the intervention, that at least 190 infants participating in this study were spared HIV infection (Stringer et al., 2003). Start-up costs aside, estimated expenditures were US$9.34 per patient counseled (17,263 pregnant women were voluntarily counseled), $12.96 per patient tested (12,438 women were tested), $55.12 per seropositive woman identified (2,924 women), and $848.26 per infection averted.
Single-dose nevirapine has been compared with other regimens. Results from the South African Intrapartum Nevirapine Trial demonstrated the similar efficacy and safety of two intrapartum/postpartum prevention regimens in breastfeeding women: multiple-dose zidovudine/lamivudine and single-dose nevirapine (Moodley et al., 2003). Both regimens can be implemented in settings where women may have only limited antenatal care or where a woman’s first visit to a clinic or hospital is during labor.
Because of the described advantages of cost, availability, simplicity, and efficacy, nevirapine has been used as the cornerstone of MTCT prevention in resource-constrained settings. In these settings, its use has decreased MTCT from about 30 percent to 15 percent (Stephenson, 2004).
Unfortunately, as discussed more fully in Chapter 3, recent data have raised concerns about the emergence of nevirapine resistance and its implications both for programs to prevent MTCT and for future use of the drug in an ART regimen for mothers after childbirth. A recent study from Thailand found that women with a history of limited nevirapine exposure for a single pregnancy had reduced rates of successful treatment response with a nevirapine-containing treatment regimen (Jourdain et al., 2004).
Recognizing what was known about the advantages and disadvantages of nevirapine for prevention of MTCT, WHO found that the established benefit of single-dose nevirapine in preventing MTCT outweighed the then-perceived potential risks. WHO currently recommends nevirapine alone or in more-potent combinations with another medication(s) (e.g., zidovudine), depending on local circumstances (WHO, 2004a). However, the ongoing accumulation of data on the emergence of nevirapine resistance after single-dose therapy and possible “archiving” of resistant strains suggests that current policies regarding single-dose use should be reassessed and less-problematic alternatives vigorously explored. Reflecting these concerns about nevirapine resistance and its implications for future therapeutic options for both mother and child, WHO’s 3-by-5 guidelines suggest that determining whether single-dose nevirapine prophylaxis compromises subsequent NNRTI-based HAART is “the most pressing operational research question facing the field.” Women who have received previous single-dose nevirapine for prevention of MTCT should be considered eligible for future NNRTI-based regimens, but with the awareness that their treatment re-
sponses may be compromised. Recognizing that heavily planned, protocol-driven treatment systems often change slowly, efforts addressing reassessment of treatment guidelines should encompass not only identifying the mechanisms necessary to ensure that the guidelines are timely, but also for rapidly implementing any new guidelines generated.
Even with ART prophylaxis, a major obstacle to preventing MTCT is preventing transmission that occurs through breastfeeding. In resource-limited settings, where the majority of HIV-infected mothers breastfeed, the risk of MTCT with no intervention is about 30–45 percent at 24 months after delivery (DeCock et al., 2000). Evidence suggests that most of the transmission that results from breastfeeding occurs early on. One study, conducted in Nairobi, Kenya, showed that 75 percent of transmission through breastmilk had occurred by the time the infant was 6 months old (Nduati et al., 2000). In this study, the only randomized controlled trial of formula feeding versus breastfeeding, 42 percent of HIV transmission to the infant was attributable to breastfeeding.
Another study, from Malawi, followed 672 infants (HIV-negative at birth) born to HIV-infected women. Forty-seven children became HIVinfected while breastfeeding but none after weaning. Incidence per month was 0.7 percent during ages 1 to 5 months, 0.6 percent during ages 6 to 11 months, and 0.3 percent during ages 12 to 17 months (p = 0.01 for trend) (Miotti et al., 1999).
In the South African Intrapartum Nevirapine Trial, which included both formula-fed and breastfed infants, all of whom received effective prophylaxis against intrapartum HIV transmission, breastfeeding was identified as the most significant risk factor for MTCT. During the first 4 weeks of life, breastfed infants were 2.2 times more likely to be HIV-infected, and breastfed infants between the ages of 4 and 8 weeks were 7.9 times more likely to be infected than their non-breastfed counterparts. In the absence of HAART, breastfeeding may also impair the health of the HIV-infected mother: the mortality rate of women randomized to breastfeed their infants was three times that of women randomized to formula-feed their infants (Mbori-Ngacha, 2001).
Nonetheless, the health benefits of breastfeeding for the infant create a significant dilemma for programs designed to prevent MTCT for women in resource-constrained settings. In such settings, clean water and affordable commercial infant formula often are not widely available, and poor hygiene and sanitation conditions increase the risk and transmission of the types of diarrheal and respiratory infections for which breastfeeding provides protection. In those resource-poor settings where there is a lack of safe, affordable, and sustainable alternatives to breastfeeding, WHO recommends that HIV-infected women exclusively breastfeed their infants during the first 6 months of life. It is this early period of breastfeeding that is believed to
provide the maximum health benefits to the infant in terms of nutrition and protection against diarrheal and respiratory infections (WHO Collaborative Study Team on the Role of Breastfeeding on the Prevention of Infant Mortality, 2000).
A number of ongoing and planned clinical trials are addressing whether short-course ART, including HAART, given to the mother and/or infant during the lactation period can reduce transmission through breastfeeding (Gaillard et al., 2004). Recent data show that women with advanced HIV disease (i.e., with higher viral loads in their breastmilk) are more likely to transmit the virus through breastmilk, suggesting that treatment with HAART may reduce the risk of MTCT (Rousseau et al., 2003). In a study conducted among pregnant women in the United States, Europe, Brazil, and the Bahamas, single-dose nevirapine did not further reduce MTCT transmission in women who were receiving standard HAART (Dorenbaum et al., 2002). As mentioned in the 2003 WHO treatment guidelines, several countries are considering using short-course triple-combination therapy for prevention of MTCT even in women who would not yet need HAART for their own HIV infection. While HAART may not only reduce perinatal HIV transmission to the infant but also minimize the emergence of nevirapine or 3TC resistance, which is a critical problem, the potential toxicity of such intense drug exposure in both mother and fetus may preclude this approach. Further study of these issues is needed before a recommendation can be made.
As part of a recently published Institute of Medicine report entitled Improving Birth Outcomes: Meeting the Challenge in the Developing World, a variety of nonretroviral strategies for reducing MTCT, including cesarean section, are discussed (IOM, 2003). The report notes that while in North American and European studies, elective cesarean section reduced the risk of perinatal HIV transmission by more than 50 percent, independent of treatment with zidovudine, its use can be associated with higher complication rates in HIV-infected women. Especially problematic is use of caesarean section in developing countries, where poor medical facilities and inappropriate staffing may further foster an increased rate of maternal complications.
While research has progressed, and rates of MTCT in the developed world are declining, UNAIDS notes that prevention of MTCT is virtually nonexistent in some of the hardest-hit countries of sub-Saharan Africa, where more than 70 percent of countries report having no such programs (UNAIDS, 2003a). Even with recent drug price cuts, most resource-constrained settings cannot support the mother–child health care infrastructure required for the implementation of MTCT prophylaxis. The problem is compounded by the social stigma of HIV infection discussed earlier and by societal or individual perceptions that treatment is not available or too
complicated—all factors that may discourage women from using available health care or counseling services.
Treating Children
The vast majority of the 3.2 million children living with HIV acquired the infection through MTCT, and 90 percent of these perinatal infections occurred in resource-limited settings (Mofenson, 2003a). As discussed above, the MTCT routes of transmission are transplacentally during pregnancy, during labor and delivery when the infant’s skin and mucus membranes are exposed to HIV in the mother’s genital tract, and postnatally through breastfeeding.
Children account for 14 percent of all new HIV infections and 16 percent of all AIDS-related deaths (UNAIDS, 2003a). Yet children are one of the most neglected populations living with HIV/AIDS for numerous reasons, including limited or challenging pediatric ART formulations (e.g., tablets too big to swallow), a belief that therapy in children may not be effective, and a lack of pediatricians and social workers specializing in the care and treatment of this population. Despite these potential limitations, pediatric ART programs in Romania and Botswana have demonstrated success in treating HIV/AIDS (Baylor International Pediatric AIDS Initiative, 2004). Moreover, it has been learned that addressing the needs of children can serve as an important point of entry to HIV/AIDS care for the entire family.
Challenges to pediatric HIV/AIDS treatment remain, however. They include the following:
-
Biological and behavioral constraints imposed by the size and age of the patient
-
Problems associated with infant diagnosis
-
Differences in drug disposition in children
-
Changes in drug disposition during development from infant to toddler to child to adolescent
-
Developmental changes that affect the way a child is counseled regarding adherence
-
Limited pediatric formulations and the need to break adult tablets into halves or quarters for use in children
-
Poor palatability of many pediatric formulations
-
The generally low priority assigned to pediatric HIV/AIDS care (children can rarely advocate for themselves)
-
Lack of experience among health professionals in the treatment and monitoring of pediatric HIV/AIDS
Among the pediatric issues that should receive priority is the need for liquid formulations and appropriate FDCs to supplement the ongoing use of single drugs where a more customized regimen is needed. The need to refrigerate some pediatric formulations is a complicating factor.
The question has been raised as to whether pediatric HIV/AIDS cases should be treated separately during ART scale-up or integrated into an adult–pediatric care system. Although integrating the two might maximize the utilization of minimal resources, there is concern that children will become lost in the effort, especially since, as noted, most children do not or cannot advocate for themselves. Thus there may be advantages to establishing a dedicated team within each ART program to focus on the specific needs of children. Ideally, as the Baylor International Pediatric AIDS Initiative has shown, this would be done within the context of treating the whole family. Relevant here is the importance of recognizing, for example, the vulnerability of children to the spread of TB from contagious family members. Hence, as part of family-centered care, household contacts should be evaluated for active TB. The fact that it is often very difficult to separate children from family members with whom they live makes a “one-stop” treatment program attractive. This strategy has been so successful for the Baylor initiative that its challenge now is accepting the overwhelming number of families that wish to enroll (Kline, 2004).
The 2003 WHO guidelines for scale-up of ART provide further specific guidance on initiating treatment in both infants and children (WHO, 2003b). A particular issue awaiting better resolution is the case of the HIV-positive infant less than 18 months of age in a circumstance in which neither a CD4 percent nor a virological assay can be obtained. Current WHO guidelines indicate that asymptomatic infants less than 18 months of age (WHO Stage I) should not be placed on therapy unless a CD4 count is obtained and found to be <20 percent.
Addressing the Role of Nutrition in HIV/AIDS and Its Treatment
Malnutrition affects one in every three people worldwide. Fully 20 percent of people in the developing world are affected, and the HIV/AIDS epidemic is occurring largely in these populations. Many of the complications of HIV infection and the associated opportunistic infections can result in micro- and macronutrient deficiencies and weight loss (Nerad et al., 2003; Kotler, 2000). (Micronutrients comprise vitamins and minerals; they have a role in immune function. Macronutrients are carbohydrates, proteins, fat, and fiber; they have a role in energy balance and in preventing wasting.) The infection-related complications that lead to malnutrition include anorexia; oral and esophageal symptoms, such as pain, that limit food intake; malabsorption; and diarrhea. The resulting malnourished state
in persons with HIV/AIDS further impairs immune function and can accelerate disease progression (Kiure et al., 2002).
ART can lead to improved nutritional status. However, the use of ART requires an understanding of the interactions between diet and drugs and the adverse effects than can compromise nutritional status, as well as recognition of the metabolic complications of drugs (Castleman et al., 2003). ARVs may require certain foods for absorption and efficacy, and their absorption can be influenced by the presence of food in the gastrointestinal tract. For example, a high-fat meal enhances the absorption of tenofovir (a nucleoside reverse transcriptase inhibitor [NRTI]) and inhibits the absorption of indinavir (a PI). Excess or inadequate absorption of drugs can result in clinical toxicity or the development of resistance, respectively. Of note, the five drugs recommended by WHO for first-line therapy combinations in resource-limited settings have no food requirements (U.S. DHHS, 2003). However, efavirenz, one of these five drugs, will have increased blood levels if taken with high-fat/high-calorie meals; thus it is recommended that this drug be taken on an empty stomach (U.S. DHHS, 2003).
Side effects of ART may affect nutritional status by leading to a loss of micro- and macronutrients or to decreased food consumption. For example, zidovudine (an NRTI) may cause anorexia, nausea, or vomiting. Didanosine (an NNRTI) may cause diarrhea. These adverse effects clearly could result in direct loss of nutrients in the body (e.g., from vomiting or diarrhea) or inhibition of nutrient intake (e.g., from anorexia or nausea).
Finally, the metabolic complications of therapy can affect short- and long-term morbidity and mortality. For example, the PI class of ARVs can cause changes in the metabolism of lipids and result in hypercholester-olemia and hypertriglyceridemia. This class of drugs can also result in insulin resistance, which can lead to diabetes mellitus.
As many of the clinical trials and prospective studies of ARVs and their effects have occurred in the developed world, the extent to which the relationships among disease, drugs, and nutrition are a factor of the developed world’s diet and nutritional status is unclear. At this time, it is also unclear what effect malnutrition will have on the success of ART scale-up on a large scale. It is clear that many people living with HIV/AIDS in the developing world lack access to sufficient quantity and quality of nutritious foods. In a May 2003 report entitled Nutrient Requirements for People Living with HIV/AIDS, WHO recognizes the limited research done in this area—specifically in resource-constrained settings—and poses research questions viewed as crucial for gaining a better understanding in this area (WHO, 2003d; see also Chapter 6). It is known, however, that micro- and macronutrients affect the progression of HIV disease and the bioavailability and efficacy of particular drugs. Indeed, a recent study has suggested that supplementation with vitamin B complex, vitamin C, and vitamin E can signifi-
cantly delay the progression of AIDS and associated disease complications among HIV-infected women (Fawzi et al., 2004). Clearly, then, food and nutrition assistance programs should be a resource available to those using ART.
THE IMPORTANCE OF ADHERENCE
As noted, ART for HIV/AIDS involves taking a complex regimen of drugs with, at times, unforgiving requirements, such as dosage timing and coadministration with food. Following this regimen scrupulously is central to durable and effective HIV therapeutic responses. A first step in successful adherence, however, is agreement on all the dimensions that this term should encompass. Numerous possible interpretations of adherence fall short of the recognition that to be adherent, patients must access properly stored ARVs and then take all prescribed drugs at the prescribed frequency and intervals and when called for with alimentation. Wider-than-recommended intervals can lead to intermittently suboptimal drug concentrations and a heightened risk of resistance emergence (see Chapter 3). The complexity of the task of assessing adherence defies the use of a single simple measurement. Indicative of the challenge is that investigators have pursued multiple approaches to ascertain different aspects of compliance, including the following:
-
Percentage of doses taken—total doses taken/number of prescribed doses
-
Proportion of days correct doses taken—number of days correct doses were taken/number of days of follow-up
-
Mean doses per day—number of doses taken/number of days cap was opened
-
Mean interdose interval—sum of all intervals between doses/number of doses taken
-
Drug holidays—count of intervals that were more than 3 days
-
Proportion of days with no doses taken—number of days with no recorded dose/number of days of follow-up
-
Dose difference—mean difference between the time each dose was taken and the “correct time” as projected from the first dose
-
Proportion of doses in dosing periods—two periods defined around the prescribed interval (either 4-hour or ±25 percent interval length)
The problem of poor adherence, however measured, to prescribed, self-administered medications generally is well documented, particularly for chronic and asymptomatic conditions (WHO, 2003e). As noted, however, one concern associated with poor adherence that is specific to ART is the
risk of emergence of drug-resistant virus. It has been shown that even short-term poor adherence (e.g., for as little as a week) can result in rapid rebound of plasma viremia and treatment failure, progression to AIDS, the development of multidrug resistance, and death. At the population level, poor adherence leading to the emergence of resistance could compromise the long-term sustainability of ART scale-up initiatives. Resistant infections are more expensive and challenging to treat. Considering the limitations of poor countries, these challenges may effectively eliminate practical options for the second-line therapies that are used in better-resourced settings. Thus there is an urgent need to standardize the definition of adherence and the measures required to document it, to assess reasons for poor adherence, and to address the problem through culturally appropriate strategies. This need is addressed in Chapter 6 as a topic for operations research.
Recommendation 4-7. Antiretroviral therapy program managers, international donors, and national planners should take the necessary measures and provide resources to ensure the strict adherence to therapy that is fundamental to program success. Such measures should include timely and adequate provision of drugs and health care, knowledgeable and available providers, and appropriate patient education. ART programs should encourage community involvement in the development of adherence interventions. This involvement should include people living with HIV/AIDS, family members, and community and religious leaders. Additionally, in special populations—such as migrant workers, trucking and transportation workers, and the military—multisite and transnational program links may need to be established.
Poor adherence is common. Several U.S. studies have assessed adherence rates and their implications for HIV/AIDS. In a U.S. study of rural patients receiving ART, only 50 percent of the patients reported consistent adherence within the previous week (Heckman et al., 2004). In another U.S. study, nearly 33 percent of patients reported having missed a medication dose in the past 5 days, and 18 percent had missed doses weekly over the past 3 months; the frequency of missed doses correlated with detectable viral loads (Catz et al., 2000). In another U.S. study involving 185 patients at the Johns Hopkins Outpatient Center, cumulative adherence was only 70 to 89 percent; the missing of a single scheduled clinic visit in the previous month was associated with increased viral rebound and clinically significant resistance (Sethi et al., 2003). In yet another prospective cohort study of 140 HIV-infected individuals at a county hospital HIV clinic, subjects took 71 percent of prescribed doses over a 48-week period, with more than 95 percent of patients achieving suboptimal adherence (i.e., less than 95 percent) (Golin et al., 2002).
Many factors contribute to poor adherence (see Box 4-4). In a recent
WHO report on adherence to long-term therapies, the simplicity of the dosage regimen (e.g., using FDCs) and drug side effects were identified as the two most important therapy-related factors influencing adherence (WHO, 2003e).
About 25–33 percent of patients experience either short- or long-term side effects while using ART. These side effects include diarrhea, nausea, stomach pains, fatigue, lipodystrophy, and neuropathies. Results of a number of studies indicate that the existence of side effects per se is not as important in affecting adherence as the patient’s capacity to tolerate them. Patients may be able to tolerate very uncomfortable side effects if they have sufficient support and motivation.
Financial constraints can affect adherence as well. In a study of HIV/ AIDS patients in Botswana, the cost of therapy was found to be the most significant barrier to adherence; 44 percent of patients self-reported that the cost of the treatment directly interfered with their ability to comply with the regimen (Weiser et al., 2003).
Another factor affecting adherence is the patient’s readiness to begin and maintain treatment (Tuldra and Wu, 2002). Since daily ART is a reminder of HIV/AIDS and potential death, many patients do not want to be on therapy at all. “Battle fatigue” can arise from the continuous need to struggle to be adherent and behave according to instruction. These observations emphasize the need to enlist patients as partners in their care and to ask them whether they feel ready to begin therapy for HIV/AIDS.
Patient education and continued support during therapy can also affect adherence. Education and support can be provided by a number of people on a health care team. One study showed that pharmacist-led interventions, which included educational counseling and telephone support, significantly improved adherence. Reminders offered by health care providers or technological devices can improve adherence. The use of alarmed medical vials and handheld devices to remind patients to take their medication have improved adherence in resource-rich settings (Simoni et al., 2003).
Direct supervision of medication intake can improve adherence. In Haiti, community health workers visit patients with HIV/AIDS in their homes daily to assist them with ART and provide support and referral when questions or complications arise (see Chapter 3 for a discussion of this program) (WHO, 2003f). The program has been found to reduce mortality, to lessen AIDS-related stigma, and to be effective in terms of clinical and virological criteria (Farmer et al., 2001). It is possible, however, that these successful outcomes are not attributable solely to the program, but may be due in part to intensive community support for these people living with HIV/AIDS (Liechty and Bangsberg, 2003). Another factor to consider before embarking on such a program is patient confidentiality. Given the
|
BOX 4-4 Patient variables
Treatment regimen
Disease characteristics
Patient–provider relationship
Clinical setting
SOURCES: Ickovics and Meade, 2002; Laniece et al., 2003; Orrell et al., 2003; Weiser et al., 2003. |
stigma and discrimination that have been associated with HIV/AIDS, as discussed earlier in this chapter, patients may not want their status disclosed to a community health worker observing them (Liechty and Bangsberg, 2003).
Studies have shown that good adherence is feasible in resource-constrained settings under certain circumstances. Adherence in some such settings exceeds that often observed in the United States. In a 48-week South African study of adherence among 289 indigent HIV-infected patients, mean adherence was 93.5 percent; there was no association between level of adherence and socioeconomic status, sex, or HIV stage (Orrell et al., 2003). And in a 2-year Senegalese study of adherence in 158 patients, patients had taken 91 percent of each monthly dose, on average, and all patients reported having taken the full monthly dose during two-thirds of the months studied (Laniece et al., 2003).
Improved adherence with FDCs was found in a retrospective study from Spain (Ibarra et al., 2003). In this study of 76 patients, mean adherence improved from 93.7 to 96.1 percent (p < 0.01). Similarly, a 16-week study comparing a combination tablet of lamivudine and zidovudine administered with a PI and a regimen with all three of these drugs administered separately found that patients in the former group were less likely to miss doses at week 8 (p = 0.007) and week 16 (p = 0.046) (Eron et al., 2000). The two regimens studied had similar clinical outcome with respect to treatment failure.
FDCs can improve adherence for two reasons. First, they reduce pill burden. This has the clinical benefit of preventing a patient from using only mono or dual therapy, which, as noted previously, has been shown to cause treatment failure and drug resistance. In a meta-analysis of 23 clinical trials involving 31 independent treatment groups, higher pill burden was associated with fewer patients with plasma HIV RNA levels 50 copies/ml at 48 weeks (p < 0.01) (Bartlett et al., 2001). This result suggests that, while different drug combinations may provide comparable activity in terms of pharmacokinetics, differences in daily pill burden can significantly affect treatment outcomes. Second, FDCs eliminate the need to purchase more than one drug, which may reduce costs and, in turn, improve adherence to a prescribed regimen. Additionally, FDCs can simplify supply management since fewer pills need to be accounted for, ordered, and distributed.
Recognizing the benefit of FDCs, WHO recommends their use in ART scale-up programs when the formulations are available and of assured quality with proven bioequivalence. Of note, not all of the FDCs listed by WHO in its recommendations for scale-up have been prequalified as of this writing. More studies are needed to compare FDCs, blister packaging of the single formulations, and “loose” single formulations.
INTEGRATION OF PREVENTION AND TREATMENT
With 40 million people currently infected with HIV, 6 million in need of immediate treatment, and funding and resources to meet only a fraction of this need, it will be important for extensive prevention activities to be conducted while ART scale-up proceeds. Indeed, prevention and treatment need not be regarded as mutually exclusive efforts (Blower and Farmer, 2003); they can and should work in parallel and even synergistically. Though details regarding prevention are largely beyond the scope of this report, prevention activities should include general HIV health communication and education; counseling and testing; efforts to delay sexual activity for youth; encouragement of correct and consistent condom use with casual partners and in other circumstances associated with risk; and targeted prevention initiatives for high-risk transmitters, such as female sex workers, long-distance truckers, and military populations. Prevention messages must be sensitive to local cultural interpretations. For example, in some settings, “faithfulness” or “fidelity” may not be understood as monogamy. Some believe one can be “faithful” to a small number of regular partners. The existence of regular sexual networks can challenge the interpretation of the word “casual.” Conceptualizations such as “zero grazing” may be better understood.
The introduction of ART on the scale proposed by WHO, UNAIDS, and the President’s Emergency Plan for AIDS Relief (PEPFAR) could have a direct secondary beneficial effect on HIV prevention, but the major impact could be indirect through the increased public attention paid to HIV, widespread testing and counseling, and stigma reduction that could accompany such programs. HIV/AIDS treatment will have the primary impact of decreasing morbidity and mortality; if accompanied by prevention counseling, it should also reduce transmission from persons under treatment by altering behavior and theoretically by reducing viral load and infectivity (Blower and Farmer, 2003; Blower et al., 2000, 2003a). Additionally, as noted earlier, the availability of ART may increase the use of VTC, which serves as a cornerstone of prevention activities by providing hope to those currently discouraged from being tested and treated.
Recommendation 4-8. National and international program planners should coordinate and integrate stronger and more effective HIV/AIDS prevention initiatives concurrently with the scale-up of antiretroviral therapy programs. Prevention initiatives should focus on those at risk for acquiring or transmitting HIV infection, in addition to those receiving treatment. To be optimally successful, voluntary counseling and testing programs and programs to prevent mother-to-child transmission should encompass both preventive and therapeutic dimensions.
National and community leaders should be strong advocates for effective HIV prevention efforts and engage government agencies and community groups in sectors beyond health, including education and public relations, as well as legislative leaders (to prevent discrimination).
In 2003, the U.S. Centers for Disease Control and Prevention and other U.S. health, research, and policy-making organizations developed recommendations for incorporating HIV prevention initiatives into HIV treatment plans in the United States (CDC, 2003). The three main components recommended were (1) screening for HIV transmission risk behaviors, for sexually transmitted diseases (whose presence is often an indication of potential risk for acquiring HIV), and for pregnancy; (2) providing brief behavioral risk-reduction interventions in an office setting (e.g., offering simple, straightforward messages about the use of condoms and clarifying misconceptions about infectiousness while on ART) and referring selected patients for additional interventions; and (3) facilitating notification and counseling of sexual and needle-sharing partners of infected persons. It is as yet unclear how to apply some of these recommendations most effectively in the cultural milieu of different resource-constrained settings. Operations research can help identify the best alternatives. One potential concern in particular resource-constrained settings relates to the third of these recommendations: in cultures where HIV/AIDS is clouded by stigma and discrimination, partner notification under a “forced” disclosure policy could result in abuse and violence. This concern, however, should not be an excuse for inaction or timidity in addressing an important need, but rather a stimulous for exploring new approaches to involving male partners.
The 1996 National Research Council report Preventing and Mitigating AIDS in Sub-Saharan Africa: Research and Data Priorities for the Social and Behavioral Sciences reviews 26 AIDS prevention programs in Africa. These include a variety of community-, population-, and institution-based intervention programs. The report documents changes resulting from these programs, including more condom usage, reductions in teenage sexual activity and in numbers of sexual partners, improvements in fidelity and treatment and control of sexually transmitted diseases, and reductions in HIV seroconversion (National Research Council, 1996). More-recent African studies involving community and family approaches likewise document the potential of preventive interventions (Roth et al., 2001). It is worth noting, however, that some of this work has also highlighted underreporting of unprotected sex by study participants (Allen et al., 2003).
As noted above, placing infected persons on ART can impact the prevention of some new cases through prevention counseling and decreases in viral load. Quinn and colleagues (2000) report from a community-based study of more than 15,000 persons in Uganda that the mean serum HIV-1
RNA viral load level was significantly higher among HIV-1–positive subjects whose partners had seroconverted than among those whose partners had not seroconverted (90,254 copies per milliliter vs. 38,029 copies per milliliter, p = 0.01). Reflecting the population benefits of suppressed viral replication, no instances of transmission were noted from the 51 HIVinfected partners with less than 1,500 copies per milliliter. Overall in this community, however, transmission was substantial, with 90 of 415 initially seronegative partners seroconverting (11.8 per 100 person-years) (Quinn et al., 2000). Modeling studies also suggest that suppression of viral load in a high proportion of infected people can significantly reduce transmission in a population (Blower et al., 2000, 2003a, 2004).
While treatment for HIV/AIDS could positively impact the prevention of new cases by decreasing viral load and reducing the infectiousness of those already afflicted with the disease, past experience with the introduction of treatment in the developed world has highlighted the potential for an increase in behaviors linked to HIV/AIDS transmission (Blower and Farmer, 2003; Blower et al., 2000, 2001). Substantial decreases in HIV mortality in the United States and other developed countries have been accompanied by a resurgence of HIV infection rates among some communities of gay men in these countries (Katz et al., 2002; Miller et al., 2000).
An observational study of adults—mainly homosexual men—with AIDS in the era of HAART found an increase in sexually transmitted infections over a 4-year period in the late 1990s. A survey of 54 homosexual men found that 26 percent felt “less concerned about becoming HIV-positive” with the availability of ART. This increase in risky behavior following receipt of ART in the developed world has not been documented for other risk groups (e.g., intravenous drug abusers, heterosexuals). Factors that could contribute to this increase in risk behaviors, also called “disinhibition,” include a greater sense of security from knowing that therapy is available and improved health, leading to more or resumption of higher-risk sexual activities. Another concern is that the increase in life expectancy that can be brought about by ART affords a greater opportunity for HIV-positive persons to infect others (although as noted, treated patients should have decreased HIV viral load burdens and thus be less infectious).
Modeling has been used to predict the interactions between use of ART and risk behaviors and the subsequent effect on HIV prevalence. Given otherwise optimal ART scale-up conditions (i.e., use of potent regimens that completely suppress viral replication, near-perfect adherence, and widespread use), but absent efforts to prevent increased risk behaviors, the potential benefits of increased ARV usage could be masked by increased transmission resulting from such behaviors, as was seen in the gay community in the United States (Blower and Farmer, 2003; Blower et al., 2000, 2003a,b, 2004; Velasco-Hernandez et al., 2002). Evidence from both em-
pirical and modeling studies, then, demonstrates that HIV prevention activities must be strengthened and integrated into ART scale-up programs if success in combating the pandemic is to be achieved.
PALLIATIVE CARE FOR AIDS PATIENTS IN DEVELOPING COUNTRIES
Despite advances in the treatment of AIDS patients and the potential for adding even decades of additional quality life to what might have been the case without ARVs, many of these persons will eventually face death due to the infection. Thus a humane approach to this disease includes steadfast care not only while the patient is responsive to ARVs, but also when all that can be offered is palliative care. Comprehensive national programs to care for patients with HIV/AIDS should address the needs of those who are in the terminal stage of AIDS.
WHO defines palliative care as care that:
-
Provides relief from pain and other distressing symptoms.
-
Affirms life and regards dying as a normal process.
-
Intends neither to hasten nor to postpone death.
-
Integrates the psychological and spiritual aspects of patient care.
-
Offers a support system to help patients live as actively as possible until death.
-
Offers a support system to help the family cope during the patient’s illness and in its own bereavement.
-
Uses a team approach to address the needs of patients and its families, including bereavement counseling, if indicated.
-
Enhances quality of life and may also positively influence the course of illness.
-
Is applicable early in the course of illness in conjunction with other therapies intended to prolong life, such as chemotherapy or radiation therapy, and includes those investigations needed to better understand and manage distressing clinical complications.
There are particular challenges to palliative care in developing countries. Palliative care of terminal AIDS patients often centers on pain management. A Ugandan study found that more than half of terminally ill patients cited pain as their chief problem (Kikule, 2003). Morphine and other analgesic opioids are inexpensive, though tight regulations hinder their availability in developing countries (Carlisle, 2003). Table 4-3, based on 2001 figures for per capita morphine consumption in African countries heavily affected by HIV/AIDS, highlights this problem. According to David Joranson of the Pain and Policy Studies Group, University of Wisconsin/
TABLE 4-3 Per Capita Consumption of Morphine, 2001
|
Country |
Per Capita Consumption (mg) |
|
Global mean |
5.9 |
|
Africa regional mean |
0.5 |
|
South Africa |
3.7 |
|
Namibia |
2.5 |
|
Botswana |
1.7 |
|
Uganda |
0.1 |
|
Tanzania |
0.09 |
|
Zambia |
0.03 |
|
Rwanda |
0.01 |
|
Mozambique |
0.01 |
|
Kenya |
0.003 |
|
Cote d’Ivoire |
0.002 |
|
Ethiopia |
0.0002 |
|
Nigeria, Haiti, and Guyana |
NAa |
|
Global mean |
5.9 |
|
aNA = not available. These countries did not report for 2001. NOTE: 2001 consumption is estimated with 2000 United Nations Population Data. SOURCE: David Joranson, Pain and Policy Studies Group, University of Wisconsin/WHO Collaborating Center, using 2003 International Narcotics Control Board and United Nations Demographic Yearbook, 2000. |
|
WHO Collaborating Center, the 14 countries originally selected for PEPFAR accounted for only 0.8 percent of the world’s morphine consumption in 2001 (personal communication to Hellen Gelband). Joranson further notes:
All of the 14 governments are parties to the United Nation’s Single Convention on Narcotic Drugs, 1961, but it is clear from the consumption statistics that there has been little effort aimed at ensuring the availability of opioids which is a treaty obligation. This may be due to many reasons, or barriers, involving pain relief being a low healthcare priority in cancer and AIDS, lack of infrastructure to deliver medical care and pain relief, lack of medical demand (prescriptions) for opioids, inadequate education of physicians, general misunderstanding and fear of morphine, and lack of governmental action.
It has been reported that patients in India have significant difficulty receiving morphine because of government fears of its diversion for nonmedical use (Ghooi and Ghooi, 2003). Culture-specific palliative guidelines are rare, though some research has been done. A recent study to determine the palliative needs of Ugandans concluded that a “good death” occurs
when patients are at home, free from pain, and without stigma, and do not feel dependent on others for their basic needs (Kikule, 2003).
WHO’s Program on Cancer Control and Departments of Care for HIV-AIDS are currently enganged in an intitiative to enhance palliative care in southern Africa. The principal objectives are as follows (WHO, 2004b):
-
To develop/reinforce palliative care programs with a public health approach in response to the needs and gaps identified, considering:
-
A holistic approach to palliative care, giving special emphasis to pain relief.
-
A systemic approach to program implementation that considers policy development, provision of care, drug availability, training, and education in the context of HIV/AIDS and cancer health problems.
-
Integration with the existing health system at all levels of care, with special emphasis on home-based care.
-
A team approach at the organizational and care levels.
-
The elements of good quality performance, including improving access, acceptability, efficiency, and effectiveness.
-
-
To advocate for drug availability and policy development among the governments of the participating countries.
-
To develop a network among the participating countries that will:
-
Promote the exchange of information and collaboration.
-
Advocate for the integration of such programs into national strategic plans for health and social services.
-
|
WHO Staging System for HIV Infection and Disease in Adults and Adolescents1 Stage I
Stage II
|
|
Stage III
Stage IV
And/or performance scale 4: bedridden > 50% of the day during the last month
|
REFERENCES
Allen S, Meinzen-Derr J, Kautzman M, Zulu I, Trask S, Fideli U, Musonda R, Kasolo F, Gau F, Haworth A. 2003. Sexual behavior of HIV discordant couples after HIV counseling and testing. AIDS 17(5):733–740.
Bartlett JA, DeMasi R, Quinn J, Moxham C, Rouseau F. 2001. Overview of the effectiveness of triple combination therapy in antiretroviral-naive HIV-1 infected adults. AIDS 15:1369–1377.
Baylor International Pediatric AIDS Initiative. 2004. Baylor International Pediatric AIDS Initiative Homepage. [Online]. Available: http://bayloraids.org/ [accessed February 19, 2004].
Blower SM, Farmer P. 2003. Predicting the public health impact of antiretrovirals: Preventing HIV in developing countries. AIDScience 3(11).
Blower SM, Gershengorn HB, Grant RM. 2000. A tale of two futures: HIV and antiretroviral therapy in San Francisco. Science 287:650–654.
Blower SM, Aschenbach AN, Gershengorn HB, Kahn JO. 2001. Predicting the unpredictable: Transmission of drug-resistant HIV. Nature Medicine 7(9):1016–1020.
Blower SM, Ma L, Farmer P, Koenig S. 2003a. Predicting the impact of antiretrovirals in resource poor settings: Preventing HIV infections whilst controlling drug resistance. Current Drug Targets-Infectious Disorders 3:345–353.
Blower SM, Schwartz EJ, Mills J. 2003b. Forcasting the future of HIV epidemics: The impact of antiretroviral therapies and imperfect vaccines. AIDS Reviews 5(2):113–125.
Blower SM, Bodine EJ, Kahn J, McFarland W. 2004. The impact of the antiretroviral rollout on drug resistant HIV in Africa: Insights from empirical data & theoretical models. AIDS [in press].
Campos PE, Suarez PG, Swanchez J, Zavala D, Arevalo J, Ticona E, Nolan CM, Hooton TM, Holmes KK. 2003. Multidrug resistant Mycobacterium tuberculosis in HIV-infected persons in Peru: Prevalence and risk factors. Emerging Infectious Diseases 9:1571–1578.
Carlisle D. 2003. Africans are dying of AIDS without pain relief. British Medical Journal 327:1069.
Castleman T, Suemo-Fosso E, Cogill B. 2003. Food and Nutrition Implications of Antiretroviral Therapy in Resource Limited Settings. Food and Nutrition Technical Assistance Project. Academy for Educational Development. [Online]. Available: http://www.fantaproject.org/downloads/pdfs/tn7_ARVs.pdf [accessed July 29, 2004].
Catz SL, Kelly JA, Bogart LM, Benotsch EG, McAuliffe TL. 2000. Patterns, correlates, and barriers to medication adherence among persons prescribed new treatment for HIV disease. Health Psychology 19:124–133.
CDC (Centers for Disease Control and Prevention). 2003. Incorporating HIV Prevention into the Medical Care of Persons Living with HIV: Recommendations of CDC, the Health Resources and Services Administration, the National Institutes of Health, and the HIV Medicine Association of the Infectious Diseases Society of America. [Online]. Available: www.cdc.gov/mmwr/PDF/rr/rr5212.pdf [accessed February 21, 2004].
CDC. 2004. Global Aids Program: Strategies. 2.1 Voluntary Counseling and Testing (VCT). [Online]. Available: http://www.cdc.gov/nchstp/od/gap/Strategies/2_1_vct.htm [accessed July 29, 2004].
Columbia University Mailman School of Public Health. 2004. MTCT-Plus: Saving Mothers, Saving Families. [Online]. Available: http://www.mtctplus.org/index.html [accessed July 29, 2004].
Corbett E, Watt C, Walker N, Maher D, Williams B, Raviglione M, Dye C. 2003. The growing burden of tuberculosis. Archives of Internal Medicine 163(9):1009–1021.
DeCock KM, Fowler MG, Mercier E, de Vincenzi I, Saba J, Hoff E, Alnwick DJ, Rogers M, Shaffer N. 2000. Prevention of mother-to-child HIV transmission in resource-poor countries: Translating research into policy and practice. Journal of the American Medical Association 283:1175–1182.
Diagbouga S, Chazallon C, Kazatchkine MD, van dePerre P, Inwoley A, M’boup S, David MP , Tenin AT, Soudre R, Aboulker JP, Weiss L. 2003. Successful implementation of a low-cost method for enumerating CD4+ T lymphocytes in resource-limited settings: The ANRS 12-26 study. AIDS 17:2201–2208.
Dorenbaum A, Cunnungham CK, Gelber RD, Culnane M, Mofenson L, Britto P, Rekacewicz C, Newell ML, Delfraissy JF, Cunningham-Schrader B, Mirochnick M, Sullivan JL, International PACT G 316 Team. 2002. Two-dose intrapartum/newborn nevirapine and standard antiretroviral therapy to reduce perinatal HIV-1 transmission: A randomized trial. Journal of the American Medical Association 288:189–198.
Dunkle K, Jewkes R, Brown H, Gray G, McIntryre J, Harlow S. 2004. Gender-based violence, relationship power, and risk of HIV infection in women attending antenatal clinics in South Africa. Lancet 363(9419):1415–1421.
Elzinga G, Nunn P. 2002. TB and HIV: Joint problems, joint solutions? Bulletin of the World Health Organization 80(6):469–470.
Eron JJ, Yetzer ES, Ruane PJ, Becker S, Sawyer GA, Fisher RL, Tolson JM, Schaefer MS. 2000. Efficacy, safety, and adherence with a twice-daily combination lamivudine/ zidovudine tablet formulation, plus a protease inhibitor, in HIV infection. AIDS 14:671–681.
European Collaborative Study. 2001. HIV-infected pregnant women and vertical transmission in Europe since 1986. AIDS 15(6):761–770.
Farmer P, Leandre F, Mukherjee J, Gupta R, Tarter L, Kim JY. 2001. Community-based treatment of advanced HIV disease: Introducing DOT-HAART (directly observed therapy with highly active antiretroviral therapy). Bulletin of the World Health Organization 79(12):1145–1151.
Fawzi W, Msamanga G, Spiegelman D, Wei R, Kapiga S, Villamor E, Mwakagile D, Mugusi F, Hertzmakr E, Essex M, Hunter D. 2004. A randomized trial of multivitamin supplements and HIV disease progression and mortality. New England Journal of Medicine 351(1):23–32.
Fennelly K, Ellner J. 2004. Tuberculosis. In: Gorbach, Bartlett, Blacklow, eds. Infectious Diseases, 3rd Edition. Philadelphia, PA: Lippincott, Williams & Wilkins.
Fitzgerald, D. 2004 (January 27). Lessons Learned from the Use of ARVs in Very LowResource Settings: The Haiti Experience. Paper presented at the Institute of Medicine Workshop on Antiretroviral Scale-up in Resource Constrained Settings. Washington, DC. Institute of Medicine Committee on Antiretroviral Drugs in Resource-Constrained Settings.
Fleischman J. 2003. Fatal Vulnerabilities: Reducing the Acute Risk of HIV/AIDS among Women and Girls. Center for Strategic and International Studies Task Force on HIV/ AIDS. [Online]. Available: http://www.csis.org/africa/0302_fatalvulnerabilities.pdf [accessed July 29, 2004].
Fleischman J. 2004. Breaking the Cycle: Ensuring Equitable Access to HIV Treatment for Women and Girls. Center for Strategic and International Studies Task Force on HIV/ AIDS. [Online]. Available: http://www.csis.org/africa/0402_breakingcycle.pdf [accessed July 29, 2004].
Gaillard P, Fowler MG, Dabis F, Coovadia H, Van der Horst C, Van Rompay K, Ruff A, Taha T, Thomas T, DeVincenzi I, Newell ML, Ghent IAS Working Group on HIV in Women and Children. 2004. Use of antiretroviral drugs to prevent HIV-1 transmission through breastfeeding: From animal studies to randomized clinical trials. Journal of Acquired Immune Deficiency Syndrome 35:178–187.
Ghooi RB, Ghooi SR. 2003. Freedom from pain: A mirage or a possibility? Experience in attempts to change laws and practices in India . Journal of Pain & Palliative Care Pharmacotherapy 17:3–4.
Golin CE Liu H, Hays RD, Miller LG, Beck CK, Ickovics J, Kaplan AH, Wenger NS. 2002. A prospective study of predictors of adherence to combination antiretroviral medication. Journal of General Internal Medicine 17:756–765.
Gorkom J. 2003 (February 3–6). TB/HIV Lessons Learned: ProTEST Meeting. Paper presented at the ProTEST Lessons Learned Workshop, Durban, South Africa.
Grimwade K, Swingler G. 2004. Cotrimoxazole prophylaxis for opportunistic infections in adults with HIV (Cochrane Review). In: The Cochrane Library, Issue 2. Chichester, UK: John Wiley & Sons.
Gupta R, Irwin A, Raviglione M, Kim J. 2004. Scaling up treatment for HIV/AIDS: Lessons learned from multi-drug resistant tuberculosis. Lancet 363:320–324.
Harries A, Hargreaves N, Chimzizi R, Salaniponi. 2002. Highly active antiretroviral therapy and tuberculosis control in Africa: Synergies and potential. Bulletin of the World Health Organization 80(6):464–469.
Havlir D, Barnes P. 1999. Tuberculosis in patients with human immunodeficiency virus infection. New England Journal of Medicine 340(5):367–373.
Heckman BD, Anderson ES, Sikkema KJ, Kochman A, Kalichman SC, Anderson T. 2004. Adherence to antiretroviral therapy in rural persons living with HIV disease in the United States. AIDS Care 16:219–230.
Heise L, Ellsberg M, Gottemoeller M. 1999. Ending violence against women. Population Reports, Series L, no. 11. Baltimore, MD: Johns Hopkins University School of Public Health, Population Information Program. [Online]. Available: http://www.infoforhealth.org/pr/l11/violence.pdf [accessed July 29, 2004].
Ibarra I, Martin-Bengoechea MJ, Peral J, Santos A, Illaro A, Lertxundi U. 2003. Assessing adherence in a treatment simplification. 2nd IAS Conference on HIV Pathogenesis and Treatment, Paris.
Ickovics JR, Meade CS. 2002. Adherence to antiretroviral therapy among patients with HIV: A critical link between behavioral and biomedical sciences. Journal of Acquired Immune Deficiency Syndrome 31:98–102.
IOM (Institute of Medicine). 2003. Improving Birth Outcomes: Meeting the Challenge in the Developing World. Washington, DC: The National Academies Press.
Jourdain G, Ngo-Giang-Huong N, Tungyai P, Kummee A, Bowonwatanwong C, Kantipong P, Lechanachai P, Hammer S, Lallemant M; Perinatal HIV Prevention Trial Group. 2004 (February 8–11). Exposure to Intrapartum Single-Dose Nevirapine and Subsequent Maternal 6-Month Response to NNRTI-Based Regimens. Paper presented at the 11th Conference on Retroviruses and Opportunistic Infections, San Francisco, CA.
Katz MH, Schwarz SK, Kellogg TA, Klausner JD, Dilley JW, Gibson S, McFarland W. 2002. Impact of highly active antiretroviral treatment on HIV seroincidence among men who have sex with men: San Francisco. American Journal of Public Health 92:388–394.
Kikule E. 2003. A good death in Uganda: Survey of needs for palliative care for terminally ill people in urban areas. British Medical Journal 327:192–194.
Kim J. 2004 (January 27). The Challenge of HIV in 2004 and the UNAIDS/WHO “3 by 5” Program. Paper presented at the Institute of Medicine Workshop on Antiretroviral Drug Use in Resource Constrained Settings, Washington, DC. Institute of Medicine Board on Global Health.
Kiure A, Msamanga G, Fawzi W. 2002. Nutrition and HIV infection. In: Essex M, Mboup S, Kanki P, Marlink R, Tlou S, eds. AIDS in Africa. 2nd Edition. Boston, MA: Plenum Publishers.
Kline M. 2004 (January 27). Pediatric Considerations for ARV Programs in ResourceConstrained Settings. Paper presented at the Institute of Medicine Workshop on Antiretroviral Scale-up in Resource Constrained Settings, Washington, DC. Institute of Medicine Committee on Antiretroviral Drug Use in Resource-Constrained Settings.
Kotler D. 2000. Nutritional Alterations Associated with HIV Infection. Journal of AIDS Research 25(Supplement 1):s81–s87.
Laniece I, Ciss M, Desclaux A, Diop K, Mbodj F, Ndiaye B, Sylla O, Delaporte E, Ndoye I. 2003. Adherence to HAART and its principle determinants in a cohort of Senegalese adults. AIDS 17:S103–S108.
Levi GC, Vitória MA. 2002. Fighting against AIDS: The Brazilian experience. AIDS 16:2373–2383.
Liechty C, Bangsberg D. 2003. Doubts about DOT: Antiretroviral therapy in resource-poor countries. AIDS 17:1383–1387.
London School of Hygiene and Tropical Medicine. 2002. Issue No. 000004: The Cost Effectiveness of the Zambian ProTEST Project. [Online]. Available: http://www.lshtm.ac.uk/dfid/tb/Briefing%20Note%205.htm [accessed March 31, 2004].
Maman S, Mbwambo J, Hogan N, Kilonzo G, Campbell J, Weiss E, Sweat M. 2002. HIVpositive women report more lifetime partner violence: Findings from a voluntary counseling and testing clinic in Dar es Salaam, Tanzania. American Journal of Public Health 92(8):1331–1337.
Mbori-Ngacha D. 2001. Morbidity and mortality in breastfed and formula-fed infants of HIV-1-infected women: A randomized clinical trial. Journal of the American Medical Association 286(19):2413–2420.
Miller M, Meyer L, Boufassa F, Persoz A, Sarr A, Robain M, Spira A. 2000. Sexual behavior changes and protease inhibitor therapy. AIDS 14:F33–F39.
Miotti PG, Taha TE, Kumwenda NI, Broadhead R, Mtimavalye LA, Van der Hoeven L, Chiphangwi JD, Liomba G, Biggar RJ. 1999. HIV transmission through breastfeeding: A study in Malawi. Journal of the American Medical Association 282(8):744–749
Mofenson L. 2003a. Tale of two epidemics: The continuing challenge of preventing mother-to-child transmission of human immunodeficiency virus. The Journal of Infectious Diseases 187:721–724.
Mofenson L. 2003b. Advances in the prevention of HIV vertical transmission. Seminars in Pediatric Infectious Diseases 14(4):295–308.
Moodley D, Moodley J, Coovadia H, Gray G, McIntyre J, Hofmyer J, Nikodem C, Hall D, Gigliotti M, Robinson P, Boshoff L, Sullivan JL, South African Intrapartum Nevirapine Trial (SAINT) Investigators. 2003. A multicenter randomized controlled trial of nevirapine versus a combination of zidovudine and lamivudine to reduce intrapartum and early postpartum mother-to-child transmission of HIV-1. Journal of Infectious Diseases 187:725–735.
MSF Briefing Note. 2004 (February). Two Pills a Day Saving Lives: Fixed-Dose Combinations (FDCs) of Antiretroviral Drugs. Geneva: Medécins sans Frontières.
National Research Council. 1996. Preventing and Mitigating AIDS in sub-Saharan Africa: Research and Data Priorities for the Social and Behavioral Sciences . Washington, DC: National Academy Press.
Nduati R, Mbori-Ngacha D, Richardson B, Overbaugh J, Mwatha A, Ndinya-Achola J, Bwayo J, Onyango FE, Hughes J, Kreiss J. 2000. Effect of breastfeeding and formula feeding on transmission of HIV-1: A randomized clinical trial. Journal of the American Medical Association 283:1167–1174.
Nerad J, Romeyn M, Silverman E, Allen-Reid J, Dieterich D, Merchant J, A Pelletier V, Tinnerello D, Fenton M. 2003. General nutrition management in patients infected with human immunodeficiency virus. Clinical Infectious Diseases 36(Supplement 2).
NIH (National Institutes of Health). 2003. Fogarty International Center Announces First Awards for Research Program in Stigma and Global Health. [Online]. Available: http://www.nih.gov/news/pr/oct2003/fic-27.htm [accessed August 24, 2004].
Nyazema NZ, Khoza S, Landman I, Sibanda E, Gael K. 2000. Antiretroviral (ARV) drug utilisation in Harare. Central African Journal of Medicine 46(4):89–93.
Orrell C, Bangsberg DR, Badri M, Wood R. 2003. Adherence is not a barrier to successful antiretroviral therapy in South Africa. AIDS 17:1369–1375.
Phillips D. 2004. Making Women Central to Family Care: Global Health Council. [Online]. Available: http://www.globalhealth.org/reports/report.php3?id=139 [accessed July 29, 2004].
Quinn TC, Wawer MJ, Sewankambo N, Serwadda D, Li C, Wabwire-Mangen F, Meehan MO, Lutalo T, Gray RH. 2000. Viral load and heterosexual transmission of human immunodeficiency virus type 1. New England Journal of Medicine 342(13):921–929.
Ridzon R, Mayanja-Kizza H. 2002. Tuberculosis. In: Essex, M, Mboup S, Kanki P, Marlink R, Tlou S, eds. AIDS in Africa. 2nd Edition. Boston, MA: Plenum Publishers.
Roth DL, Stewart KE, Clay OJ, van der Straten A, Karita E, Allen S. 2001. Sexual practices of HIV discordant and concordant couples in Rwanda: Effects of a testing and counseling programme for men. International Journal of Sexually Transmitted Diseases and AIDS 12(3):181–188.
Rousseau CM, Nduati RW, Richardson BA, Steele MS, John-Stewart GC, Mbori-Ngacha DA, Kreiss JK, Overbaugh J. 2003. Longitudinal analysis of human immunodeficiency virus type 1 RNA in breast milk and of its relationship to infant infection and maternal disease. Journal of Infectious Diseases 187:741–747.
Rutherford GW, Sangani PR, Kennedy GE. 2004. Three- or four- versus two-drug antiretroviral maintenance regimens for HIV infection (Cochrane Review). In: The Cochrane Library, Issue 1. Chichester, UK: John Wiley & Sons.
Schechter, M. 2004 (January 27). Lessons Learned from the Scale-up of Antiretroviral Treatment in Brazil. Paper presented at the Institute of Medicine Workshop on Antiretroviral Drug Use in Resource-Constrained Settings, Washington, DC. Institute of Medicine Board on Global Health.
Sethi AK, Celentano DD, Gange SJ, Moore RD, Gallant JE. 2003. Association between adherence to antiretroviral therapy and human immunodeficiency virus drug resistance. Clinical Infectious Diseases 37:1112–1118.
Simoni JM, Frick PA, Pantalone DW, Turner BJ. 2003. Antiretroviral adherence interventions: A review of current literature and ongoing studies. Topics in HIV Medicine 11:185–198.
Stephenson J. 2004. Researchers report findings on HIV drug resistance, new infections. Journal of the American Medical Association 291(12):1431–1433.
Stringer EM, Sinkala M, Stringer JS, Mzyece E, Makula I, Goldenberg RL, Kwape P, Chilufya M, Vermund SH. 2003. Prevention of mother-to-child transmission of HIV in Africa: Successes and challenges in scaling-up a nevirapine-based program in Lusaka, Africa. AIDS 17:1377–1382.
The Italian Register for Human Immunodeficiency Virus Infection in Children. 2002. Determinants of mother-to-infant human immunodeficiency virus 1 transmission before and after the introduction of zidovudine prophylaxis. Archives of Pediatric and Adolescent Medicine 156(9):915–921.
Tuldra A, Wu AW. 2002. Interventions to improve adherence to antiretroviral therapy. Journal of Acquired Immune Deficiency Syndrome 31:S154–S157.
UNAIDS (Joint United Nations Programme on HIV/AIDS). 2000. Voluntary Counseling and Testing (VCT): UNAIDS Technical Update 2000. [Online]. Available: http://www. unaids.org [accessed August 24, 2004].
UNAIDS. 2003a. AIDS Epidemic Update. [Online]. Available: http://www.unaids.org [accessed August 24, 2004].
UNAIDS. 2003b. Combating Stigma and Discrimination Is Vital to Improving Access to AIDS Care. [Online]. Available: http://www.unaids.org [accessed May 28, 2004].
UNAIDS. 2004. Violence against Women and AIDS. [Online]. Available: http://www.unaids.org/html/pub/una-docs/gcwa_violence_02feb04_en_pdf.pdf [accessed July 29, 2004].
UNAIDS/WHO (Joint United Nations Programme on HIV/AIDS and World Health Organization). 2003. AIDS Epidemic Update: December 2003. [Online]. Available: http://www.unaids.org/html/pub/publications/irc-pub06/jc943-epiupdate2003_en_pdf.pdf [accessed July 29, 2004].
U.S. DHHS (United States Department of Health and Human Services). 2003. Guidelines for the Use of Antiretroviral Agents in HIV-1-Infected Adults and Adolescents. [Online]. Available: http://AIDSinfo.nih.gov [accessed August 24, 2004].
Velasco-Hernandez JX, Gershengorn HG, Blower SM. 2002. Could widespread use of combination antiretroviral theapy eradicate HIV epidemics? The Lancet Infectious Diseases 2:487–493.
Weiser S, Wolfe W, Bangsberg D, Thior I, Gilbert P, Makhema J, Kebabetswe P, Dickenson D, Mompati K, Essex M, Marlink R. 2003. Barriers to antiretroviral adherence for patients living with HIV infection and AIDS in Botswana. Journal of the Acquired Immune Deficiency Syndrome 34(3):281–288.
WHO (World Health Organization). 2003a. Emergency Scale-up of Antiretroviral Therapy in Resource-Limited Settings: Technical and Operational Recommendations to Achieve 3 by 5. [Online]. Available: http://www.who.int/3by5/publications/documents/zambia/en/ [accessed June 30, 2004].
WHO. 2003b. Scaling up Antiretroviral Therapy in Resource-Limited Settings: Treatment Guidelines for a Public Health Approach. 2003 Revision. [Online]. Available: http://www.who.int/3by5/publications/documents/arv_guidelines/en/ [accessed June 30, 2004].
WHO. 2003c. Guidelines for Implementing Collaborative TB and HIV Programme Activities. [Online]. Available: http://www.who.int/gtb/publications/tb_hiv/2003_319/tbhiv_guidelines.pdf [accessed June 30, 2004].
WHO. 2003d. Nutrient Requirements for People Living with HIV/AIDS: Report of a Technical Consultation. Geneva: WHO.
WHO. 2003e. Adherence to Long-term therapies: Evidence for Action. Geneva: WHO.
WHO. 2003f. Access to Antiretroviral Treatment and Care: The Experience of the HIV Equity Initiative in Cange, Haiti. [Online]. Available: http://www.who.int/hiv/pub/prev_care/en/Haiti_E.pdf [accessed June 30, 2004].
WHO. 2004a. Draft Guidelines. [Online]. Available: http://www.who.int/3by5/publications/documents/en/pmtct_2004.pdf [accessed May 28, 2004].
WHO. 2004b. A Community Health Approach to Palliative Care for HIV and Cancer Patients in Africa. [Online]. Available: http://www.who.int/cancer/palliative/projectproposal/en [accessed June 30, 2004].
WHO. 2004c. Stop TB Working Group on TB/HIV. Available: www.stoptb.org/Working_Groups/TBHIV/ [accessed August 24, 2004].
WHO Collaborative Study Team on the Role of Breastfeeding on the Prevention of Infant Mortality. 2000. Effect of breastfeeding on infant and child mortality due to infectious diseases in less developed countries: a pooled analysis. Lancet 355:451–455.
Wilkinson D, Squire SB, Garner P. 1998. Effect of preventive treatment for tuberculosis in adults infected with HIV: Systematic review of randomized placebo controlled trials. British Medical Journal 317:625–629.