6
Beyond the Biomedical Response
OVERVIEW
An influenza pandemic will likely spawn a plethora of legal and ethical dilemmas and political and economic consequences, and its impact will depend to a large extent on the public’s perception of and reaction to the crisis. This chapter presents a variety of social perspectives on the coming pandemic: economic, legal, and ethical implications of various response options; opportunities for collaboration between public and private sectors; and public communication strategies to address both interpandemic and pandemic influenza.
The chapter opens with a description of an economic model, based on the notion of preparation as an “insurance policy” against the next influenza pandemic, to calculate the investment necessary to prepare for a range of pandemic scenarios and responses. These calculations indicate the mutual exclusivity of two key goals of pandemic planning, minimizing overall mortality and minimizing economic impact, thus highlighting the need for a system by which to make such difficult choices and explain them to the public.
Focusing on the important role in mitigating pandemic influenza of both annual immunization (to build demand for flu vaccine, and therefore supply in the event of a crisis) and prompt vaccination against a pandemic strain, the chapter continues with a consideration of strategies to increase immunization uptake before and during a pandemic. In a pandemic—or even a severe annual flu season, as occurred in late 2003—public health officials face the difficult task of encouraging people with high priority to receive vaccine while persuading others to wait calmly and use nonmedical
measures to reduce their exposure to infection. Limited research indicates that public officials can avoid losing their credibility in such situations by sharing the dilemmas of disease control with the public in a productive and effective way.
Current understanding about the influence and causes of panic in public crises and how to remedy its effects has been advanced through recent efforts to prepare society to deal productively with terrorism. Both the September 11, 2001, terrorist attacks and subsequent anthrax assaults in the United States demonstrated that open and informative relationships among citizens, government, and public health and safety authorities are fundamental to a population’s ability to cope with unconventional health threats. In her contribution to this chapter, Monica Schoch-Spana describes a series of findings by study and research focus groups convened by the Center for Biosecurity of the University of Pittsburgh Medical Center in collaboration with Johns Hopkins University to examine governance dilemmas in bioterrorism response. These groups characterized the unique governing dilemmas posed by a major infectious outbreak and produced guidelines by which decision makers can identify opportunities to enlist public trust and cooperation in such emergencies.
Legal authority must be brought to bear on nearly every facet of pandemic preparedness, from measures designed to reduce the risk of animal-to-human transmission of disease; to surveillance and detection procedures; to medical interventions to prevent or control the spread of infection; to the imposition of voluntary or mandatory quarantine and/or isolation measures; to travel limitations, trade restrictions, and border closures. This chapter continues with an examination of the legal and ethical questions attached to major public health interventions for preventing or ameliorating pandemic influenza; it also summarizes ethical values that can inform public health practice in an emergency.
THE ECONOMIC IMPACT OF PANDEMIC INFLUENZA IN THE UNITED STATES: PRIORITIES FOR INTERVENTION
Martin I. Meltzer, Nancy J. Cox, and Keiji Fukuda1
Centers for Disease Control and Prevention, Atlanta, Georgia, USA
Reprinted from Emerging Infectious Diseases, CDC, 2003
|
1 |
Address for correspondence: Martin Meltzer, National Center for Infectious Diseases, Centers for Disease Control and Prevention, Clifton Road, Mail Stop C12, Atlanta, GA 30333; fax: 404–639–3039; e-mail: qzm4@cdc.gov. |
We estimated the possible effects of the next influenza pandemic in the United States and analyzed the economic impact of vaccine-based interventions. Using death rates, hospitalization data, and outpatient visits, we estimated 89,000 to 207,000 deaths; 314,000 to 734,000 hospitalizations; 18 to 42 million outpatient visits; and 20 to 47 million additional illnesses. Patients at high risk (15% of the population) would account for approximately 84% of all deaths. The estimated economic impact would be US$71.3 to $166.5 billion, excluding disruptions to commerce and society. At $21 per vaccinee, we project a net savings to society if persons in all age groups are vaccinated. At $62 per vaccinee and at gross attack rates of 25%, we project net losses if persons not at high risk for complications are vaccinated. Vaccinating 60% of the population would generate the highest economic returns but may not be possible within the time required for vaccine effectiveness, especially if two doses of vaccine are required.
Influenza pandemics have occurred for centuries, three times (1918, 1957, and 1968) in the 20th century alone. Another pandemic is highly likely, if not inevitable (Patriarca and Cox, 1997). In the 1918 influenza pandemic, more than 20 million people died (Simonsen et al., 1998). Improvements in medical care and technology since the last pandemic may reduce the impact of the next. When planning for the next pandemic, however, decision makers need to examine the following questions: Would it make economic sense to vaccinate the entire U.S. population if 15% were to become clinically ill? What if 25% were to become ill? To answer such questions, we conducted economic analyses of potential intervention scenarios.
Although many studies have examined or reviewed the economics of influenza vaccination (Campbell and Rumley, 1997; Carrat and Valleron, 1995; Jefferson and Demicheli, 1998; Kavet, 1977; Office of Technology Assessment, 1981; Patriarca et al., 1987; Riddiough et al., 1983; Schoenbaum, 1987), only one study (Schoenbaum et al., 1976), published in 1976, examined the economics of a vaccine-based intervention aimed at reducing the impact of an influenza epidemic in the United States. Our study examines the possible economic effects of the next influenza pandemic in the United States, analyzes these effects, and uses the results to estimate the costs, benefits, and policy implications of several possible vaccine-based interventions. These estimates can be used in developing national and state plans to respond to an influenza pandemic.2 Unlike the
|
2 |
A complete plan detailing a response to an influenza pandemic should include definition of a pandemic, points that will initiate various steps in the response plan, and details about deploying the intervention. While a U.S. federal influenza pandemic plan is being developed, a guide to aid state and territorial health officials in developing plans for their jurisdictions is available at http://www.cdc.gov/od/nvpo/pandemicflu.htm. Printed copies can be obtained from the author. |
1976 study, ours examined the effect of varying the values of a number of key input variables. Specific objectives were to provide a range of estimates regarding the number of deaths, hospitalizations, outpatient visits, and those ill persons not seeking medical care in the next influenza pandemic; provide a cost estimate of health outcomes; estimate the potential net value of possible vaccination strategies;3 evaluate the effect of using different criteria (e.g., death rates, economic returns due to vaccination) to set vaccination priorities; assess the economic impact of administering various doses of vaccine and of administering vaccine to different age groups and groups at risk; and calculate an insurance premium that could reasonably be spent each year for planning, preparedness, and practice.
Methods
The Model
Building a mathematical model of the spread of influenza is difficult largely because of differences in virus transmission and virulence, lack of understanding of the primary factors affecting the spread of influenza, and shortage of population-based data (Cliff and Haggett, 1993). Because of the difficulties in calculating realistic estimates of the numbers of cases in the next influenza pandemic, we used a Monte Carlo mathematical simulation model (Critchfield and Willard, 1986; Dittus et al., 1989; Dobilet et al., 1985), which uses predefined probability distributions of key input variables to calculate the number of illnesses and deaths that could result from an influenza pandemic. Some of the most important probability distributions we used describe the population-based rates of illness and death. These rates are based on illness and death rates reported in earlier influenza pandemics and epidemics. The model produces a range of estimated effects rather than a single point estimate. The model is not epidemiologic and thus does not describe the spread of the disease through a population.
Many details of the model are presented below and in Appendix I; a more detailed explanation and a complete list of all the variables used and the values assigned to the variables are available at Appendix II.
For interventions to contain and reduce the impact of an influenza pandemic, we used a societal perspective, which takes into account all benefits and all costs regardless of who receives and who pays.
TABLE 6-1 Estimate of Age Distribution of Cases and Percentage of Population at High Risk Used to Examine the Impact of Pandemic Influenza in the United States
|
Age Group (yrs) |
|
|
|
Percentage of All Casesa |
|
0–19 |
40.0 |
|
20–64 |
53.1 |
|
65+ |
6.8 |
|
Totalsb |
100.0 |
|
|
Percentage at High Riskc |
|
0–19 |
6.4 |
|
20–64 |
14.4 |
|
65+ |
40.0 |
|
U.S. averaged |
15.4 |
|
aThe actual number of cases will depend upon the assumed gross attack rate. The distribution of cases was based on lower and upper estimates of age-specific attack rates from the 1918, 1928–29, and 1957 epidemics and pandemics (Glezen, 1996). bTotals do not add to exactly 100% because of rounding. cPersons are categorized at high risk if they have a preexisting medical condition that makes them more susceptible to influenza-related complications. The percentages of age groups at high risk were obtained from the Working Group on Influenza Pandemic Preparedness and Emergency Response (GrIPPE, unpub. data). The Advisory Committee on Immunization Practices estimates that 27 to 31 million persons aged <65 years are at high risk for influenza-associated complications (Centers for Disease Control and Prevention, 1998). dAverage is an age-weighted average, using each age group’s proportion of the total U.S. population. |
|
Age Distribution and Persons at High-Risk
Since the age distribution of patients in the next pandemic is unknown, we assumed a distribution (Table 6-1) among the three age groups (0 to 19 years, 20 to 64 years, and 65 years and older).4 Further, each age group was divided into those at high risk (persons with a preexisting medical condition making them more susceptible to complications from influenza) and those not at high risk (Table 6-1).5 Age by itself was not considered a
|
4 |
This article presents the results for one distribution of cases by age and risk group. The background paper in Appendix II, however, contains additional results obtained by using a different distribution. |
|
5 |
The Advisory Committee on Immunization Practices estimates that 27 to 31 million people ages <65 years are at high risk for influenza-associated complications (CDC, 1998). ACIP |
risk factor; persons 65 years and older were assumed to have higher rates of illness and death than the rest of the population (Table 6-2).
Gross Attack Rates
In the model, we used gross attack rates (percentage of clinical influenza illness cases per population) of 15% to 35%, in steps of 5%. Infected persons who continued to work were not considered to have a clinical case of influenza, and were not included.
Illnesses and Deaths
The rates of adverse effects (outpatient visits, hospitalizations, deaths, and illnesses for which no medical care was sought), by age and risk group, were used to determine the number of persons in each category (Table 6-2) (Appendix II).
Net Returns of Vaccinating against an Influenza Pandemic
Vaccinating predefined segments of the population will be one of the major strategies for reducing the impact of pandemic influenza, and the net return, in dollars, from vaccination is an important economic measure of the costs and benefits associated with vaccination. We calculated the net return by using the following formula for each age and risk group:

The savings from illnesses and deaths averted and the cost of vaccinations are described in Appendix I. Some input variables are described below and in Appendix II.
|
|
also classifies all 32 million people ≥65 years as being at elevated risk for influenza-related complications (CDC, 1998). Further, the working group on influenza pandemic preparedness and emergency response has assumed that approximately 19 million household members of persons at high risk should also be vaccinated to reduce the probability of transmission to those at high risk (GrIPPE, unpub. data, 1997). |
TABLE 6-2 Variables Used to Define Distribution of Disease Outcomes of Those with Clinical Casesa of Influenza
|
Variable |
Rates per 1,000 personsb |
||
|
Lower |
Most likely |
Upper |
|
|
Outpatient visits |
|
||
|
Not at high risk |
|
||
|
0–19 yrs old |
165 |
|
230 |
|
20–64 yrs old |
40 |
|
85 |
|
65+ yrs old |
45 |
|
74 |
|
High risk |
|
||
|
0–19 yrs old |
289 |
|
403 |
|
20–64 yrs old |
70 |
|
149 |
|
65+ yrs old |
79 |
|
130 |
|
Hospitalizations |
|
||
|
Not at high risk |
|
||
|
0–19 yrs old |
0.2 |
0.5 |
2.9 |
|
20–64 yrs old |
0.18 |
|
2.75 |
|
65+ yrs old |
1.5 |
|
3.0 |
|
High risk |
|
||
|
0–19 yrs old |
2.1 |
2.9 |
9.0 |
|
20–64 yrs old |
0.83 |
|
5.14 |
|
65+ yrs old |
4.0 |
|
13 |
|
Deaths |
|
||
|
Not at high risk |
|
||
|
0–19 yrs old |
0.014 |
0.024 |
0.125 |
|
20–64 yrs old |
0.025 |
0.037 |
0.09 |
|
65+ yrs old |
0.28 |
0.42 |
0.54 |
|
High risk |
|
||
|
0–19 yrs old |
0.126 |
0.22 |
7.65 |
|
20–64 yrs old |
0.1 |
|
5.72 |
|
65+ yrs old |
2.76 |
|
5.63 |
|
aClinical cases are defined as cases in persons with illness sufficient to cause an economic impact. The number of persons who will be ill but will not seek medical care, are calculated as follows: Number illage = (Populationage × gross attack rate) − (deathsage + hospitalizationsage + outpatientsage). The number of deaths, hospitalizations, and outpatients are calculated by using the rates presented in this table. bFor Monte Carlo simulations, rates are presented as lower and upper for uniform distributions, and lower, most likely, and upper for triangular distributions (Evans et al., 1993). SOURCES: Office of Technology Assessment, 1981; Carrat and Valleron, 1995; Schoenbaum et al., 1976; Glezen, 1996; Mullooly and Barker, 1982; Barker and Mullooly, 1980; Simonsen et al., 1997; Fox et al., 1982; Glezen et al., 1987; Serfling et al., 1967; Barker and Mulooly, 1982; Glezen et al., 1982; McBean et al., 1993; Barker, 1986, and Appendix II. |
|||
Input Variables
The direct medical costs (i.e., those reimbursed by third-party payers such as health insurance companies) associated with hospitalizations, outpatient visits, and drug purchases were obtained from a proprietary database containing health insurance claims data from approximately 4 million insured persons (The MEDSTAT Group, Ann Arbor, MI) (Table 6-3). Following the methods used by McBean et al. (1993), we extracted the data for outpatient visits from the database with codes from the International Classification of Diseases, Ninth Revision (ICD-9) for pneumonia and bronchitis (ICD-9:480–487.8), acute bronchitis (ICD-9:466–466.1), and chronic respiratory disease (ICD-9:490–496). Costs for inpatient care were extracted with the same codes, when recorded as the principal diagnosis and when recorded as any of the diagnoses in a patient’s chart. Further, because influenza can cause patients with preexisting medical conditions to seek inpatient care, data were extracted for the inpatient costs of treating heart-related conditions (common preexisting conditions that place a person at high risk for influenza-related illness or death). Hospital costs attributed to pneumonia and bronchitis, acute bronchitis, chronic respiratory disease, and the identified heart conditions were then estimated as weighted averages (Appendix II).
The principal indirect cost was lost productivity, which was valued by using an age- and gender-weighted average wage (Table 6-3) (Haddix et al., 1996). The economic cost of a death was valued at the present net value of the average expected future lifetime earnings, weighted for gender and age (Haddix et al., 1996). All costs were standardized to 1995 US$ values.
The cost of fully vaccinating a person (i.e., administering the number of doses necessary to protect against disease) was modeled with two assumed values, approximately $21 and $62 per person fully vaccinated (Table 6-4). These costs include the cost of the vaccine, as well as its distribution and administration (health-care worker time, supplies); patient travel; time lost from work and other activities; and cost of side effects (including Guillain-Barré syndrome) (Table 6-4) (Appendix II).
Vaccine Effectiveness
The assumed levels of vaccine effectiveness used to estimate the savings gained due to a vaccine-based intervention are described in Appendix I; the equation defining savings from outcomes averted contains the rate of compliance multiplied by the assumed vaccine effectiveness. In cases requiring two doses of vaccine to satisfactorily protect against influenza-related illness and death, a person was considered compliant only after both doses.
Net Returns of Vaccination: Sensitivity Analyses
To illustrate the importance of the death rate in determining economic outcomes, we conducted further sensitivity analyses in which the death rates for persons not at high risk were one quarter or half of those used in the main analyses (Table 6-2).
Insurance Premiums
To determine how much should be spent each year to plan, prepare, and practice to ensure that mass vaccinations can take place if needed, we considered the funding of those activities as an annual insurance premium (Kaufmann et al., 1997). The premium would be used to pay for improving surveillance systems, ensuring sufficient supply of vaccine for high-priority groups (and possibly the entire U.S. population), conducting research to improve detection of new influenza subtypes, and developing emergency preparedness plans to ensure adequate medical care and maintenance of essential community services (Kaufmann et al., 1997). We calculated the premium as follows (Robinson and Barry, 1987): annual insurance premium = net returns from an intervention × the annual probability of a pandemic.
Vaccination Priorities and Distribution
During the early stages of a pandemic, the supply of influenza vaccine will likely be limited. Even if sufficient vaccine is produced to vaccinate the entire U.S. population, it will take time to administer the vaccine to all, especially if two doses are required. Because a pandemic will be caused by a new subtype of influenza, two doses of vaccine may be required. Who should receive priority for vaccination until vaccine supplies are more plentiful? To illustrate the use of the model in estimating the impact of different priorities, we created sample priority lists by using three different criteria: total deaths, risk for death, and maximizing net returns due to vaccination. In choosing the criteria for priorities, society must debate the main goal of a pandemic vaccination plan: prevent deaths, regardless of age and position in society; prevent deaths among those at greatest risk (i.e., 65 years of age); or minimize the social disruption. If the last is the goal of society, the net return due to vaccination should be used to set priorities.
The model can also be used to compare the economic consequences of plans that specify which target populations are vaccinated. To illustrate this capability, we constructed four options for prioritizing vaccine distribution. For Option A, the target population is similar to current Advisory Committee on Immunization Practices (ACIP) recommendations, with production and use of vaccine similar to current, intrapandemic recommendations (Centers for Disease Control and Prevention, 1998). We assumed 77.4
TABLE 6-3 Input Variables Used to Calculate the Economic Impact (Direct and Indirect Costs) of Health Outcomes Due to an Influenza Pandemic in the United States (in 1995 US$)
|
Outcome Category Iitem |
Age Group (yrs) |
||||
|
Type of Cost |
0–19 |
20–64 |
65+ |
Sources |
|
|
Deaths |
|
||||
|
Average age (years) |
|
9 |
35 |
74 |
Assumed |
|
PV earnings lost ($)a |
Indirect |
1,016,101 |
1,037,673 |
65,837 |
16, 30 |
|
Most likely ± min or max hospital costs ($)b |
Direct |
3,435 ± 2,632 |
7,605 ± 3,888 |
8,309 + 3,692 |
Marketscan Database; 31 |
|
Subtotal ($)c |
|
1,019,536 |
1,045,278 |
74,146 |
|
|
Hospitalizations |
|
||||
|
Most likely ± min or max hospital costs ($)b |
Direct |
2,936 ± 2,099 |
6,016 ± 2,086 |
6,856 ±3,200 |
Marketscan Database; 31 |
|
Most likely ± min or max net pay for outpatient visits ($)d |
Direct |
74 ± 40 |
94 ± 70 |
102 ± 60 |
Marketscan Database; 31 |
|
Avg. copayment for outpatients visit ($) |
Direct |
5 |
4 |
4 |
Marketscan Database |
|
Most likely ± min or max net payment for drug claims($)e |
Direct |
26 ± 9 |
42 ± 30 |
41 ± 10 |
Marketscan Database |
|
Most likely ± min or max days lostf |
Indirect |
5 ± 2.7 |
8 ± 4.8 |
10 ± 5.4 |
Marketscan Database; 31 |
|
Value 1 day lost ($)g |
Indirect |
65 |
100 or 65 |
65 |
30 |
|
Subtotal ($)c |
|
3,366 |
6,842 |
7,653 |
|
|
Outpatient visits |
|
||||
|
Avg. no. visitsh |
Direct |
1.52 |
1.52 |
1.52 |
Marketscan Database |
|
Most likely ± min or max net payment per visit($)i |
Direct |
49 ± 13 |
38 ± 12 |
50 ± 16 |
Marketscan Database |
|
Avg. copayment for outpatient visit ($) |
Direct |
5 |
4 |
4 |
Marketscan Database |
|
Most likely ± min or max net payment per prescription($)j |
Direct |
25 ± 18 |
36 ± 27 |
36 ± 22 |
Marketscan Database |
|
Avg. prescriptions per visit |
Direct |
0.9 |
1.8 |
1.4 |
Marketscan Database |
|
Avg. copayment per prescription ($) |
Direct |
3 |
3 |
3 |
Marketscan Database |
|
Days lost |
Indirect |
3 |
2 |
5 |
4,5 |
|
Value 1 day lost ($)g |
Indirect |
65 |
100 |
65 |
30 |
|
Subtotal ($)c |
|
300 |
330 |
458 |
|
|
Ill, no medical care sought |
|
||||
|
Days lost |
Indirect |
3 |
2 |
5 |
4,5 |
|
Value 1 day lost ($)g |
Indirect |
65 |
100 |
65 |
30 |
|
Over-the-counter drugs ($) |
Direct |
2 |
2 |
2 |
Assumed |
|
Subtotal ($)c |
|
197 |
202 |
327 |
|
|
aAverage present value (PV), using a 3% discount rate, of expected future lifetime earnings and housekeeping services, weighted by age and gender (Haddix et al., 1996) and adjusted to 1995 dollars (by multiplying by a factor of 1.07) (U.S. Bureau of the Census, 1997). bMost likely, with ± defining the minimum and maximum costs for a triangular distribution (Evans et al., 1993) for Monte Carlo analysis (Critchfield and Willard, 1986; Dobilet et al., 1985; Dittus et al., 1989). The values were calculated by using cost data from Marketscan Database (The MEDSTAT Group, Ann Arbor, MI) and multiplying it by a hospital cost-to-charge ratio of 0.53. The latter ratio is a weighted average of the urban and rural (urban = 0.80, rural = 0.20) cost-to-charge ratios calculated by the Health Care Finance Administration for August 1996 (The Federal Register, 1996) (31 in the table). cSubtotals are the totals for each category of outcome, using the most likely estimates. dMost likely, with minimum and maximum values of net payments for outpatient visits up to 14 days before admission date and up to 30 days after discharge date. eNet payment for drug claims associated with outpatient visits up to 14 days before admission and up to 30 days after discharge. fMost likely, with ± defining the minimum and maximum days lost due to hospitalization for a triangular distribution (Evans et al., 1993) for Monte Carlo analysis (Critchfield and Willard, 1986; Dobilet et al., 1985; Dittus et al., 1989). Calculated using length of stay in hospital data from Marketscan Database (The MEDSTAT Group, Ann Arbor, MI) and adding a total of one additional day for convalescence and pre- and posthospitalization outpatient visits for 0-19 and 20-64 years of age. For 65+ years, two additional days were added to length of stay in hospital for convalescence and pre- and posthospitalization outpatient visits. gFor 0-19 and 65+ years age groups, a day lost to influenza was valued as equivalent to an unspecified day (Haddix et al., 1996), denoting a value for time lost by care givers and family members related to taking care of a patient in these age groups. For 20-64 years of age, 60% of days lost due to hospitalizations and related convalescence and pre- and posthospitalization outpatient visits were valued as day off work ($100/day). The remaining 40% of days lost were valued as unspecified days ($65/day). For 20-64 years of age, when patients were not hospitalized at any point during their illness (i.e., outpatient status), all days lost were assumed days off work ($100/day). hThe number of visits per episode of influenza is an average across all age groups. From the database, it was found that 85% of all patients had less than three outpatient visits, with an average of 1.52 visits (Appendix II). iMost likely, with minimum and maximum values of net payments for outpatient visits without any specified association to hospita lizations. jMost likely, with ± defining the minimum and maximum cost per prescription, with the number of prescriptions per visit. |
TABLE 6-4 Cost of Vaccinationa During an Influenza Pandemic, with Specific Costs Assigned to Side Effects of Vaccination
|
Item |
Probability of Effectb |
Cost of Case of Side Effect ($)b |
Lower-Cost Scenario ($/patient) |
Upper-Cost Scenario ($/patient) |
|
Assumed cost of vaccinationa (excluding side effects) |
|
|
18 |
59 |
|
Side effects |
|
|||
|
Mildc |
0.0325 |
94 |
3.05 |
3.05 |
|
GBSd |
0.000002 |
100,800 |
0.20 |
0.20 |
|
Anaphylaxis |
0.000000157 |
2,490 |
0.01 |
0.01 |
|
Total cost per patient |
|
|
21.26 |
62.26 |
|
aThe cost of vaccination includes the cost of the vaccine, the cost of administering the vaccine, value of time spent by a person traveling to and from the place of vaccination, and patient-associated travel costs. Included in the costs of the vaccine are any costs associated with the rapid production of a larger-than-usual number of doses and the rapid delivery and correct storage of doses at vaccination sites around the country. For $18, the costs were assumed to be $10 for vaccine + administration, $4 patient time (half hour), $4 patient travel costs. For $59, the costs were assumed to be $20 for vaccine + administration (this could include the cost of two doses), $32 patient time (two trips at 2 hours per trip), and $7 patient travel costs. For comparison, a review of 10 published articles found a range of $5 to $22 per dose of vaccine, with a medium [sic] cost of $14 per dose (Jefferson and Demicheli, 1998). Additional details are provided in the background paper (see methods section). These breakdowns are illustrations only of what might be deemed reasonable estimates of time and cost. Actual costs might vary substantially and will depend on the number of doses needed to achieve a satisfactory protective response, as well as the efficiency of giving vaccinations to millions of persons. bProbabilities and average cost of treating each category of side effect were derived from Office of Technology Assessment (1981). cMild side effects include sore arms due to vaccination, headaches, and other minor side effects that may require a visit to a physician or may cause the patient to miss 1 to 2 days of work. dGBS = Guillain Barré syndrome. |
||||
million vaccinees. Option B targets the number of vaccinees as outlined in Option A plus approximately 20 million essential service providers (5 million health-care workers and 15 million providers of other service) (99.2 million vaccinees). Option C aims to achieve a 40% effective coverage of the entire U.S. population (106.1 million vaccinees), and Option D, 60% effective coverage of the entire U.S. population (159.2 million vaccinees).
The number of vaccine doses required to meet each option will depend on the number of doses per person needed to obtain an immune response. If two are needed, lack of compliance with a two-dose regimen will mean that the actual number of doses needed will be higher than double the target population for each option (i.e., >40% or >60% of the population will have to receive the first dose to ensure that 40% or 60% are fully vaccinated). If two doses are required, the cost per person vaccinated will increase (Table 6-4).
Findings
Illnesses and Deaths
The number of hospitalizations due to an influenza epidemic ranged from approximately 314,000 (5th percentile = 210,000; 95th percentile = 417,000) at a gross attack rate of 15% to approximately 734,000 (5th percentile = 441,000; 95th percentile = 973,000) at a gross attack rate of 35% (Figure 6-1). The mean numbers of persons requiring outpatient-based care ranged from approximately 18 million (gross attack rate of 15%) to 42 million (gross attack rate of 35%) (Figure 6-1). The mean numbers of those clinically ill not seeking medical care but still sustaining economic loss ranged from approximately 20 million (gross attack rate of 15%) to 47 million (gross attack rate of 35%) (Figure 6-1). The estimated number of deaths ranged from approximately 89,000 (5th percentile = 55,000; 95th percentile = 122,000) at a gross attack rate of 15%, which increased to approximately 207,000 deaths (5th percentile = 127,000; 95th percentile = 285,000) at a gross attack rate of 35% (Figure 6-1).
Groups at high risk (approximately 15% of the total U.S. population) (Table 6-1) would likely be disproportionately affected by an influenza pandemic. These groups accounted for approximately 85% of all deaths, with groups at high risk in the 20 to 64-year-old age group accounting for approximately 41% of total deaths (Table 6-5). Groups at high risk also accounted for 38% of all hospitalizations and 20% of all outpatient visits (Table 6-5).
Economic Impact of an Influenza Pandemic
Without large-scale immunization, the estimates of the total economic impact in the United States of an influenza pandemic ranged from $71.3 billion (5th percentile = $35.4 billion; 95th percentile = $107.0 billion) (gross attack rate of 15%) to $166.5 billion (5th percentile = $82.6 billion; 95th percentile = $249.6 billion) (gross attack rate of 35%) (Table 6-6). At any given attack rate, loss of life accounted for approximately 83% of all
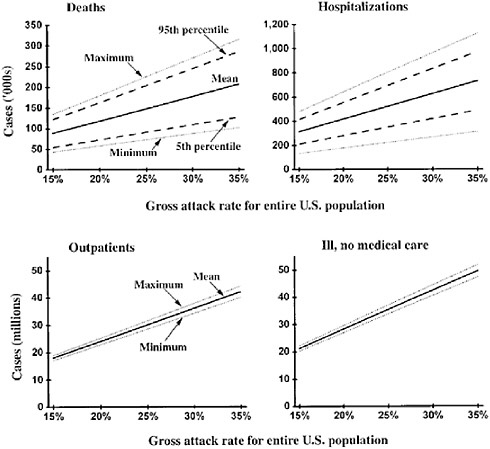
FIGURE 6-1 Impact of influenza pandemic in the United States: mean, minimum, maximum, and 5th and 95th percentiles of total death, hospitalizations, outpatients, and those ill (but not seeking medical care) for different gross attack rates. Note that for each gross attack rate, data are totals for all age groups and risk categories.
economic losses. Outpatients, persons ill but not seeking medical care, and inpatients accounted for approximately 8%, 6%, and 3%, respectively, of all economic losses (Table 6-6) (Appendix II).
Net Value of Vaccination
If it cost $21 to vaccinate a person and the effective coverage were 40%, net savings to society would result from vaccinating all age and risk groups (Figure 6-2). However, vaccinating certain age and risk groups rather than others would produce higher net returns. For example, vaccinating patients ages 20 to 64 years of age not at high risk would produce
TABLE 6-5 Impact, by Age Group, Death, Hospitalizations, and Outpatients Accounted for by Groups at High Risk During an Influenza Pandemica
|
Category |
Age Group (yrs) |
Total Cases at High Risk (%) |
||
|
Mean |
5th |
95th |
||
|
Death |
0–19 |
9.0 |
1.4 |
20.2 |
|
20–64 |
40.9 |
11.1 |
60.9 |
|
|
65 + |
34.4 |
22.7 |
52.1 |
|
|
Total |
84.3 |
|
|
|
|
Hospitalizations |
0–19 |
4.6 |
2.1 |
7.9 |
|
20–64 |
14.7 |
7.4 |
23.4 |
|
|
65 + |
18.3 |
11.0 |
27.6 |
|
|
Total |
37.6 |
|
|
|
|
Outpatients |
0–19 |
5.0 |
4.7 |
5.4 |
|
20–64 |
10.4 |
9.8 |
11.0 |
|
|
65 + |
4.0 |
3.9 |
4.2 |
|
|
Total |
19.5 |
|
|
|
|
aSee Table 6-1 for distribution of groups at high and not at high risk within the U.S. population. |
||||
higher net returns than vaccinating patients ages 65 years of age and older who are at high risk (Figure 6-2). At a cost of $62 per vaccinee and gross attack rates of less than 25%, vaccinating populations at high risk would still generate positive returns (Figure 6-2). However, vaccinating populations not at high risk would result in a net loss (Figure 6-2).
Sensitivity Analyses
At a vaccination cost of $21.26 per vaccinee, reducing the death rates to half and one quarter of the initial values (Table 6-2) left positive mean net returns for all age groups not at high risk. However, at a vaccination cost of $62.26 per vaccinee, reducing death rates to half and one quarter of the initial values resulted in negative mean net returns for all age groups not at high risk. The results are much less sensitive to increases in gross attack rate than to increases in death rate. For example, assuming a cost of $62.26 per vaccinee and death rates that are half the initial rates, increasing the gross attack rate from 15% to 25% still resulted in negative net returns for all age groups, regardless of assumed level of vaccine effectiveness.
TABLE 6-6 Costs (Direct and Indirect) of Influenza Pandemic per Gross Attack Rate:a Deaths, Hospitalizations, Outpatients, Illnesses, and Total Costs (in 1995 US$)
|
|
Cost per Gross Attack Rate ($ millions) |
||||
|
|
15% |
20% |
25% |
30% |
35% |
|
Deaths |
|||||
|
Mean |
59,288 |
79,051 |
98,814 |
118,577 |
138,340 |
|
5th percentile |
23,800 |
31,733 |
39,666 |
47,599 |
55,532 |
|
95th percentile |
94,907 |
126,543 |
158,179 |
189,815 |
221,451 |
|
Hospitalizations |
|||||
|
Mean |
1,928 |
2,571 |
3,214 |
3,856 |
4,499 |
|
5th percentile |
1,250 |
1,667 |
2,084 |
2,501 |
2,917 |
|
95th percentile |
2,683 |
3,579 |
4,472 |
5,367 |
6,261 |
|
Outpatients |
|||||
|
Mean |
5,708 |
7,611 |
9,513 |
11,416 |
13,318 |
|
5th percentile |
4,871 |
6,495 |
8,119 |
9,742 |
11,366 |
|
95th percentile |
6,557 |
8,742 |
10,928 |
13,113 |
15,299 |
|
Ill, no medical care soughtb |
|||||
|
Mean |
4,422 |
5,896 |
7,370 |
8,844 |
10,317 |
|
5th percentile |
3,270 |
4,360 |
5,450 |
6,540 |
7,629 |
|
95th percentile |
5,557 |
7,409 |
9,262 |
11,114 |
12,967 |
|
Grand totals |
|||||
|
Mean |
71,346 |
95,128 |
118,910 |
142,692 |
166,474 |
|
5th percentile |
35,405 |
47,206 |
59,008 |
70,810 |
82,611 |
|
95th percentile |
106,988 |
142,650 |
178,313 |
213,975 |
249,638 |
|
aGross attack rate = percentage of clinical influenza illness per population. bPersons who become clinically ill due to influenza but do not seek medical care; illness has an economic impact (e.g., half day off work). |
|||||
Implications for Policy
The amount of the insurance premium to spend on planning, preparedness, and practice for responding to the next influenza pandemic ranged from $48 million to $2,184 million per year (Table 6-7). The amount was sensitive to the probability of the pandemic, the cost of vaccinating a person, and the gross attack rate. Because higher costs of vaccination reduce net returns from an intervention, increased vaccination costs reduced the premiums. Conversely, increases in gross attack rates (all other inputs held constant) increased the potential returns from an intervention and thus the amount of premiums.
When risk for death is used as the criterion for who will be vaccinated first, persons ages 65 years and older receive top priority (Table 6-8); however, when mean net returns due to vaccination are used as the crite-
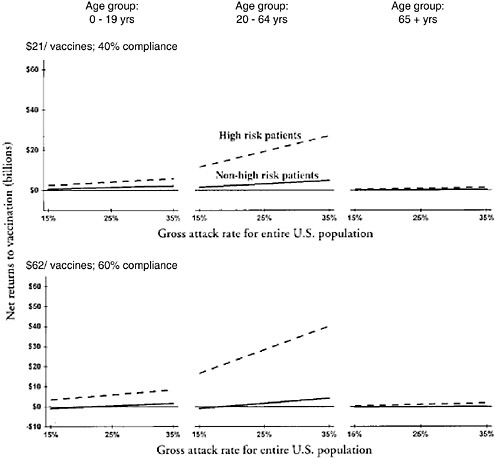
FIGURE 6-2 Mean net returns due to vaccination, by age group, for different gross attack rates and percentages of compliance. Case-age distributions are given in Table 6-1. Assumed vaccine effectiveness is the same as the high vaccine effectiveness defined in Appendix I.
rion, that group receives the lowest priority (Table 6-8). Regardless of criteria used, persons at high risk ages 0 to 19 and 20 to 64 years would always receive priority over persons not at high risk from the same age groups (Table 6-8).
While Option A would ensure positive mean net returns, Option B would result in greater mean net returns (Figure 6-3). Changing the strategy from vaccinating specific groups (Option B) to vaccinating 40% of the population decreased mean net returns (Figure 6-3). Only Option D resulted in higher mean net returns than Option B. Note, however, that the 5th and 95th percentiles for each option overlapped with those of other options. Thus, the differences in mean values between the options may not occur in practice.
TABLE 6-7 The Mean Annual Insurance Premiuma for Planning, Preparing, and Practicing to Respond to the Next Influenza Pandemic
|
|
Mean (s.d.) Insurance Premium ($ Millions) |
||||||
|
Low Vaccine Effectivenessb × 40% Compliance Probability of Pandemic |
High Vaccine Effectivenessb × 60% Compliance Probability of Pandemic |
||||||
|
Gross Attack Rate |
Cost of Vaccination per Vaccinee ($) |
1 in 30 years |
1 in 60 years |
1 in 100 years |
1 in 30 years |
1 in 60 years |
1 in 100 years |
|
15% |
21 |
306(122) |
153(61) |
92(37) |
872 (341) |
435 (170) |
262(103) |
|
|
62 |
162(122) |
81 (61) |
48 (37) |
654(341) |
326(170) |
196(103) |
|
25% |
21 |
561 (204) |
280 (102) |
168 (61) |
1,528 (569) |
762(284) |
459 (171) |
|
|
62 |
416 (204) |
207 (102) |
125 (61) |
1,311 (569) |
653(284) |
394 (171) |
|
35% |
21 |
815 (286) |
406 (142) |
245 (86) |
2,184 (796) |
1,089 (397) |
656 (239) |
|
|
62 |
670 (286) |
334 (142) |
201 (86) |
1,967 (796) |
980(397) |
591 (239) |
|
aDefined here as the amount of money to be spent each year to plan, prepare, and practice to ensure that such mass vaccinations can take place if needed. See text for description of calculating premiums. The mathematically optimal allocation of such funds for each activity requires a separate set of calculations. bLow and high levels of vaccine effectiveness are defined in Appendix I. |
|||||||
TABLE 6-8 Setting Vaccination Priorities: Which Age Group or Group at Risk Should be Vaccinated First?
|
Priority |
Criteria for Prioritization |
||
|
Risk for Deatha |
Total Deathsb |
Returns Due to Vaccination |
|
|
1 (top) |
High risk 65+ yrs |
High risk 20–64 yrs |
High risk 20–64 yrs |
|
2 |
Not at high risk 65+ yrs |
High risk 65+ yrs |
High risk 0–19 yrs |
|
3 |
High risk 0–19 yrs |
High risk 0–19 yrs |
Not at high risk 20–64 yrs |
|
4 |
High risk 20–64 yrs |
Not at high risk |
Not at high risk 65+ yrs 0–19 yrs |
|
5 |
Not at high risk |
Not at high risk |
High risk 65+ yrs 20–64 yrs 20–64 yrs |
|
6 (bottom) |
Not at high risk 0–19 yrs |
Not at high risk 0–19 yrs |
Not at high risk 65+ yrs |
|
aPriorities set by risk for death are set according to lower-limit estimates of deaths per 1,000 population for each age and risk group. bThe priority list using the total deaths criteria was set by examining the percentage of total deaths that each age and risk group contributed to the total deaths estimated due to a pandemic. The group with the highest percentage (i.e., contributes the largest number of deaths) is listed as having the highest priority. |
|||
Conclusions
Impact of an Influenza Pandemic
Although the next influenza pandemic in the United States may cause considerable illness and death (Figure 6-1), great uncertainty is associated with any estimate of the pandemic’s potential impact. While the results can describe potential impact at gross attack rates from 15% to 35%, no existing data can predict the probability of any of those attack rates actually occurring. In addition, the groups at high risk are likely to incur a disproportionate number of deaths (Table 6-5); 50% or more of the deaths will likely occur among persons age 65 years and older (Appendix II), a distribution also found in the influenza pandemics of 1918, 1957, and 1968 (Simonsen et al., 1998).
Our results illustrate that the greatest economic cost is due to death (Table 6-6). Therefore, all other things being equal, the largest economic returns will come from the intervention(s) that prevents the largest number
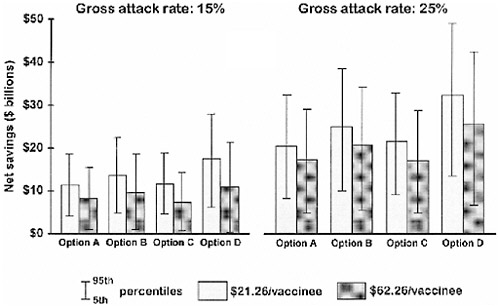
FIGURE 6-3 Four options for responding to an influenza pandemic: mean net economic returns. Notes: a) Bars show mean net returns for each option and assumed cost of vaccination. b) Option A: Similar to current Advisory Committee on Immunization Practices recommendations, with production and use similar to current, intrapandemic recommendations (CDC, 1998). Assumed approximately 77 million vaccinees. Option B: Number of vaccines as outlined in Scenario A plus 20 million essential service providers (5 million health-care workers + 15 million other service providers). Option C: Aim to achieve a 40% coverage of total U.S. population. Option D: Aim to achieve 60% coverage of total U.S. population (Appendix II).
of deaths. A limitation of the model is that, beyond the value of a lost day of work (Table 6-3), the model does not include any valuation for disruptions in commerce and society. For example, if many long-distance truck drivers were unavailable to drive for 1 or 2 weeks, there might be disruptions in the distribution of perishable items, especially food. These multiplier effects are not accounted for in this model, mainly because an estimate of an appropriate multiplier will depend on who becomes ill, how many become ill, when they become ill, and for how long they are ill.
All other factors being held constant, the net returns due to vaccination are sensitive to the combination of price and gross attack rate, with some scenarios generating negative mean returns (Figure 6-2). Further, some scenarios with a positive mean net return had a negative 5th percentile (Appendix II). The fact that negative results can be generated should serve as a warning that many interventions may not guarantee a net positive economic return.
Implications for Policy
The premium that could be spent each year for influenza pandemic response (planning, preparedness, and practice) depends most on the assumed probability of the pandemic (Table 6-7). The wide range in premiums presents a cautionary tale of the difference between possibility and probability of an influenza pandemic. What cannot be stated with any certainty are the probability of a pandemic and the number of persons who will become ill and die. Deciding the difference between possibility and probability was a key decision point in the swine flu incident of 1976–1977 (Neustadt and Fineberg, 1978).
Vaccination priorities depend on the objectives. If preventing the greatest number of deaths is the most important goal, society should ensure that those in the groups at high risk become vaccinated first, followed by those age 65 years or older who have no preexisting medical conditions making them more susceptible to complications from influenza (Table 6-8). However, if maximizing economic returns is the highest priority, persons 0 to 64 years of age, regardless of risk, should be vaccinated first (Table 6-8). Results also illustrate the need to be precise in defining the criterion used for setting priorities. For example, stating that preventing death will be the criteria used is not sufficiently precise because different priority lists can be drawn up using death rates versus total deaths (Table 6-8).
The criteria used to generate the results in Table 6-8 do not define the entire set of possible methods of setting priorities. Society may decide to use another criterion or set of criteria. Priorities for vaccination may also depend on the epidemiology of the pandemic. For example, if the strain causing the pandemic were particularly virulent among those ages 20 to 40 years, that age group may receive highest priority. Since the epidemiology of the next pandemic is unknown, any plan must allow flexibility in determining criteria for setting priorities. Table 6-8 provides a starting point for debate regarding who should be vaccinated first.
The net returns for the four scenarios modeled (Figure 6-3) further illustrate the need to clearly set criteria, goals, and objectives for a vaccine-based intervention for the next influenza pandemic. Some may state that Options C and D represent a more egalitarian means of distributing vaccine. However, egalitarianism would cost society more since the mean net returns from Options C are lower than those from Option B (Figure 6-3). Option D produces higher returns than Option B (Figure 6-3), but vaccinating 60% of the U.S. population in a short time would be difficult, especially if two doses of vaccine are required. If two doses were required, Option D would mean producing, delivering, and administering approximately 320 million doses of vaccine in a 2- to 3-month period, which has never been accomplished in the United States.
Acknowledgments
We thank Nancy Arden, Rob Breiman, Bill Jordan, Marty Meyers, Alicia Postema, Steve Schoenbaum, Larry Schonberger, Larry Sparks, and Ray Strikas for their help and encouragement.
Dr. Meltzer is senior health economist, Office of the Director, National Center for Infectious Diseases, Centers for Disease Control and Prevention. His research interests focus on assessing the economics of public health interventions such as oral raccoon rabies vaccine, Lyme disease vaccine, and hepatitis A vaccine, as well as estimating the economic burden of bioterrorism, dengue, pandemic influenza, and other infectious diseases. His research uses various methods, including Monte Carlo modeling, willingness-to-pay surveys (contingent valuation), and the use of non-monetary units of valuation, such as Disability Adjusted Life Years.
APPENDIX I
For the equation in the main text defining net returns due to vaccinations, savings from outcomes averted and the costs of vaccination are calculated as follows:

TABLE High and Low Levels of Assumed Vaccine Effectiveness
|
Disease Outcomes |
||||||
|
Highc |
Lowc |
|||||
|
0–19 yrs |
20–64 yrs |
65+ yrs |
0–19 yrs |
20–64 yrs |
65+ yrs |
|
|
Death |
0.70 |
0.70 |
0.60 |
0.40 |
0.40 |
0.30 |
|
Hospitalization |
0.55 |
0.55 |
0.50 |
0.55 |
0.55 |
0.50 |
|
Outpatient visits |
0.40 |
0.40 |
0.40 |
0.40 |
0.40 |
0.40 |
|
Ill, no medical care sought |
0.40 |
0.40 |
0.40 |
0.40 |
0.40 |
0.40 |
|
aVaccine effectiveness is defined as the reduction in the number of cases in each of the age and disease categories. bWithin a defined age group, it was assumed that there was no difference in vaccine effectiveness between subgroups at high risk and not at high risk. cThe terms high and low level of effectiveness are subjective and reflect only a judgment of the levels of effectiveness in the two scenarios relative to each other. |
||||||
APPENDIX II
A background paper, containing additional methodological details and results, is available electronically at the following URL: http.www.cdc.gov/ncidod/EID/vol5no5/meltzerback.htm.
INCREASING AWARENESS AND UPTAKE OF INFLUENZA IMMUNIZATION
Glen Nowak, PhD
Office of Health Communications
National Immunization Program
Centers for Disease Control and Prevention
Although much of this section focuses on the communication challenges presented by the need to increase public awareness of and uptake of seasonal influenza immunization, pandemic influenza will require similar efforts to enlist public support and cooperation. In both cases—as in most such circumstances—it is important to recognize that good communication is necessary, but not entirely sufficient, to achieving desired behavioral outcomes. Policies and incentives are also usually necessary to motivate many people to get annual flu shots (e.g., those people who believe influenza vaccination is helpful, but who are not willing to experience much inconvenience to get vaccinated).
It is crucial to note that good communication requires more than simply releasing facts, figures, and statistics to the public (Working Group on Governance Dilemmas in Bioterrorism Response, 2004). Many times, campaigns or efforts designed to achieve adoption of health promotion behaviors or recommendations rely primarily on the provision of numbers and statistics. The assumption is that people will conclude that the disease or adverse health outcome is more likely than they may have assumed. A 2004 campaign designed to increase attention and concern about deep vein thrombosis (DVT), for example, featured print ads pointing out that “DVT strikes 2 million Americans each year and that complications from this disorder cause up to 200,000 deaths per year—more than breast cancer, car crashes and AIDS combined.” Although the campaign likely caused a modest increase in awareness of DVT and ways to prevent it, many (and perhaps most) people who may be affected by DVT probably remain unaware or unconvinced of this health threat. Providing numbers and statistics is helpful, but motivating people to take health-protective action requires doing more than simply listing morbidity and mortality statistics. The challenge of changing and influencing human behavior is difficult, and often far more difficult than it seems.
The 2003–2004 Flu Season: A Recipe for Increasing Immunization Uptake
A variety of factors occurred during the 2003–2004 flu season that illustrate some of the elements and events that can significantly affect interest in, and demand for, influenza vaccine. These events occurred in a chronological fashion analogous to a “recipe” for increasing vaccine uptake. However, as the events of 2003–2004 also illustrate, many of the important ingredients in this recipe are outside the control of health officials and practitioners. For example, one factor that helped to facilitate initial media and public interest in influenza vaccination was the fact that influenza’s arrival coincided with the immunization season. The convergence of influenza and the influenza vaccination season works in at least two ways to facilitate vaccination. First, it provides reporters and the media with a reason and an angle for influenza vaccination stories. Second, the presence or imminent presence of influenza not only raises the awareness, interest, and motivation levels of people, but the availability of vaccine means people can act on their concern. During that season, when people began to hear about flu, they could immediately take protective action.
A second element that helps to foster high motivation or demand for vaccine is the association of the dominant strain or initial cases of the disease with severe illness and/or outcomes. In the 2003–2004 influenza season, many of these initial cases (at least those that received significant and visible media attention) occurred among people for whom the public generally does not perceive influenza to cause serious complications. When influenza causes grave illness and death among children, healthy adults, or healthy seniors, the media are more likely to deem influenza as “news” (i.e., different and unusual enough to warrant attention). In 2003–2004, several of the initial serious influenza cases also occurred in cities and communities with large daily newspapers and major television stations, further increasing the visibility of the harm being caused by the disease. Many stories focused on individual patients or people who were deemed especially newsworthy because they did not fit the stereotypical profile of a flu casualty, such as a frail elderly person.
A third boost to immunization was provided in the 2003–2004 season when medical experts and public health authorities publicly (i.e., via press releases and the media) expressed alarm about the severity of the initial influenza cases. Many of the experts quoted in news stories predicted dire outcomes (e.g., more people than expected becoming sick with influenza) and urged influenza vaccination. Such statements, in turn, often received considerable attention and use by other media (e.g., stories on television and radio stations often cited experts who had been quoted in newspapers). It is important to note that in the 2003–2004 influenza season, the media
and public health officials appeared to be working in concert. The media needed spokespeople on these issues, and public health officials needed outlets to inform the public that many people needed to receive influenza vaccination because they were susceptible to serious complications from influenza.
The 2003–2004 influenza season also illustrated the importance of “real-people” and “real-life” cases in fostering media and public interest in a vaccine-preventable disease. In November, one of the families who had a child who died from influenza held a press conference to urge other parents to get their children vaccinated. This event not only helped to boost the visibility of influenza immunization recommendations, but it also caused reporters in many parts of the country to investigate whether children in their areas were being harmed by influenza.
Although severe cases of influenza among children have occurred every year, it is relatively rare for reporters to recognize that fact or write about it. In 2003–2004, however, not only did they recognize that it could be happening in their communities, but they looked, and then wrote, about the impact influenza was having on children. The end result was increased media attention and visibility—which, in turn, fostered parent awareness and motivation. Visible, tangible, and meaningful examples of the seriousness of a vaccine-preventable disease, such as pictures of affected children and accounts of their families’ grief and concern, is often highly motivating.
As a result of the confluence of all these events (i.e., flu arriving during the flu vaccination season, the initial cases causing severe illness among people not generally perceived to experience severe complications, and experts predicting a “bad” flu season), the 2003–2004 flu season was presented in the media in terms that facilitated continued media interest and that motivated public behavior. Early on, people learned or were told that it was going to be a severe flu season, a message that is more motivating than being told the flu season would be “typical” or “not so bad.” This is important because while many people for whom an influenza vaccination is recommended routinely seek one, many others wait to hear or see how bad the flu season is before they take action. Heading into late November 2003, some medical and public health officials began talking about “pandemic influenza,” further heightening media and public interest in both flu and flu vaccination.
For those interested in increasing the number of people who receive an annual influenza vaccination, one of the important lessons from the 2003–2004 influenza season is that several of the factors that help generate media attention to, and public demand for, flu shots are ones that cannot be affected or controlled by public health officials or medical professionals. A large amount of the media interest and consumer demand for flu vaccination is related to four factors: when influenza arrives; who is impacted in
terms of illness; the severity, duration, and extent of the illness caused by the circulating strains; and people’s perceptions regarding their individual (and/or family’s) susceptibility to experiencing a severe case of influenza.
As risk communication principles illustrate (Sandman, 1993), it is often the case that increasing the adoption of a medical recommendation (e.g., greater adoption of influenza immunization by people in at-risk groups) involves the creation of concern, anxiety, and worry. This is particularly true among people who do not routinely take the recommended action (e.g., receive an annual vaccination). There has to be some motivating level of fear before people take action, and that may play out in any number of ways. It could be a perception that many (or more) people are falling ill, a sense that the illness is especially severe, or a belief that one is vulnerable to contracting and experiencing serious illness.
Public Communication Challenges
The efforts and experiences of the past few years in trying to increase annual influenza vaccine uptake in the United States illustrates that a variety of factors must be considered as part of pandemic influenza communication planning. These factors all stem from the situation that (1) recommendations and perceptions regarding influenza vaccination are not universal, and (2) the development of effective communication plans and messages requires segmenting the audience/population based on relevant differentiating characteristics (Sandman and Lanard, 2004). People—including medical experts—have a variety of beliefs regarding the importance and value of influenza vaccination (Davis et al., 2002). This is a concern, particularly because (as will be discussed further) the so-called mass media, upon which many pandemic plans depend to disseminate information, no longer effectively reach the mass audiences (i.e., 30 percent or more of U.S. households at one time) they once did. Instead, when it comes to influenza and influenza vaccination, there are a number of distinct societal segments, each of which has different perspectives and needs that matter when it comes to developing communication messages (Sandman and Lanard, 2004). Furthermore, each segment also likely utilizes and favors different media outlets for news and information.
A key communication challenge in a pandemic will be to reduce the confusion created by mixed messages and to avoid, where possible, intentionally sending messages that provide confusing and potentially contradictory advice. Completely eliminating mixed messages from the pandemic influenza environment is likely an impossible objective. A better and more realistic objective is to utilize extensive communication and policy collaboration and partnerships to achieve highly visible, consistent recommendations and actions.
When it comes to reducing the impact and number of mixed or conflicting messages, a number of things need to be kept in mind. First, situations that involve multiple experts and organizations, differing expertise, a wide range of stakeholders (e.g., from scientists to policy makers), and a plethora of media typically lend themselves to “mixed” messages, conflicting advice, and seemingly contradictory recommendations. In many cases, a lack of scientific data or consensus help foster the presence of conflicting messages. Thus, it is important to recognize that “mixed” and “conflicting” messages are, strictly speaking, unavoidable. However, as recent examples involving avian influenza, influenza vaccine supply shortages, and Severe Acute Respiratory Syndrome (SARS) illustrate, extensive collaboration on policies and communications greatly enhances the visibility of “consensus” messages and recommendations.
Second, it’s important to realize that “policies” and “behaviors” communicate—in many cases, more powerfully and effectively than words. As a result, many “mixed” or “conflicting” messages arise because patients or members of the public see or perceive a contradiction between what is being recommended and the actions of those making the recommendation. In the case of influenza vaccination, for example, one of the mixed messages that exists in the minds of many people for whom annual flu vaccination is recommended is the relatively low uptake among health care professionals (Brunell, 2004). As a result, many people assume that the vaccine must be unnecessary or ineffective, or their doctor or nurse would surely receive it.
It is also possible for messages that are designed to increase influenza immunization among people at high risk for severe illness to have unintended consequences. In the case of medical recommendations, this can happen through the use of the images and pictures used in education or public information materials. Often, posters, brochures, and television public service announcements contain pictures of people who are in, or believed to be in, the targeted population. Through focus group research, a few years ago, we learned of an “unintended” consequence related to influenza immunization education materials that targeted people 65 years old and older. In having focus group participants discuss some of the posters commonly used in the 1990s, we learned that many people in that age group did not deem these materials as relevant to them. One reason was the use of models and pictures that focused on elderly people and people in generally poor health. Healthy and active people who were 65 and older who did not seek an annual flu vaccination frequently said, “I don’t need a flu shot. A flu shot is for elderly or frail people. I’m healthy and active.” In their mind, most influenza vaccination materials fostered the perception that immunization was recommended for elderly people, particularly those in poor health or in nursing homes. If they didn’t consider themselves to be “elderly,” or if they considered themselves to be healthy and active, they tended
not to believe they should get vaccinated. A more effective communication approach is to use images of healthy and active seniors and to call attention to the fact that “an annual influenza vaccination helps you stay healthy and active.”
More recently the Centers for Disease Control and Prevention (CDC) recommended annual influenza vaccination for those ages 50 to 64 years and 6 to 23 months (Harper et al., 2004). In developing education materials for these groups, recent focus group research indicated that many parents and people in the newly recommended age category expect those materials to describe tangible and explicit benefits for adopting that recommendation. Their reactions could be summarized as, “There must be some reason(s) that it’s now recommended that I receive an annual influenza vaccination—I’d like to know what that reason is” or “something must have changed so that I’m now in a group that is recommended for annual vaccination, what’s changed?” Many parents of 6- to 23-month-olds wondered, “Why now, why the change? I didn’t have an influenza vaccination when I was a child. Five years ago with my first child it wasn’t necessary. What has changed that makes this necessary today?” Many of these parents believed they had no evidence from their daily experience that such a change was warranted.
Another significant pandemic (and general) influenza immunization challenge pertains to “nuanced” communications and advice. It is common, especially in circumstances that are relatively new or where broad/deep scientific and medical consensus is lacking, to develop policies, recommendations, and messages that contain caveats, clauses, and fine distinctions. In the case of policies and recommendations, this can be necessary and unavoidable. Unfortunately, when it comes to public, patient, media, and even health care practitioners, much of this “nuance” is lost and/or unrecognized. The media frequently simplify recommendations and messages, and thus fail to transmit all the nuances, while people in media and target audiences usually fail to recognize, understand, or appreciate clauses and distinctions. Furthermore, the media, health care practitioners, and the public generally prefer, and better understand, direct, simple, and clear messages. They also often fail to use or define words with the same degree of nuance as those making and putting forward the overall policies. For example, in the case of influenza vaccination, an attempt was made for a couple of years to “encourage” annual vaccination of 6- to 23- month-old children—versus “recommend” annual vaccination. Focus group research and calls from physicians and parents consistently indicated that for these groups, “encourage” and “recommend” were synonymous. Many health care professionals even asked why different words were used. More recently, focus group discussions with parents of 6- to 23-month-old children indicated that some found the reference to 23 months confusing. They
asked, “Does that mean that my 2-year-old doesn’t need the flu vaccination?” Clearly, we need to pay more attention to these sorts of inadvertent consequences of our well-intended and carefully crafted messages.
Three Population Segments
Our experience indicates that Americans broadly fall into three population segments with regard to influenza vaccination. One segment consists of people who routinely receive the annual influenza vaccine, including many of those whom we recommend do so. Considerable data indicate that most people 65 and older—perhaps 65 to 70 percent of those in this age group—regularly receive an annual influenza vaccination, typically relatively early in September and October.
An even larger group consists of Americans who sometimes receive an annual influenza vaccination; these also include people for whom vaccination is recommended. People in this group often monitor the flu season and make a decision each year whether there is sufficient reason to take the time and make the effort to be immunized. They appear to be swayed by factors such as information about the severity of the strain, the likelihood that they or someone they know will contract influenza, and their perceived likelihood of transmitting severe disease. Many people in this “wait and see” group ultimately will decide to get immunized, and likely do so in November or December.
Finally, there is a group of people who do not get or intend to get an influenza vaccination, and they, too, include some people for whom immunization is recommended. However, recent data suggest that most people in this group are 18 to 49 years old, so on average they have relatively low risk of flu complications. However, older people in this group often have reached their decision against immunization based on a firmly held belief or conviction—and have held their position for years (and in some cases, decades). To change their minds will require far more than telling them that 36,000 people a year die from influenza (CDC, 2004a). They probably know that influenza causes serious harm (and often have experienced influenza), but they are not convinced that the vaccine is either safe or effective; rather, many believe the vaccine will cause them to get the flu either directly or by somehow rendering their immune system more susceptible to the virus.
Targeting Pandemic Communications
In the event of a pandemic, public officials would need to tailor messages to reach the three groups (as well as other segments; see Sandman and Lanard, 2004) described above in order to respond to their individual perceptions regarding influenza immunization—and these messages would
need to be conveyed through an increasingly fractured mass media. Most American households receive at least 10 television channels, and as many as 50 to 100 if they have cable or satellite service. In addition, hundreds of websites offer medical and health information. Daily newspaper readership, once a unifier of the American population, is declining, particularly among 18- to 49-year-olds. Additional factors to be considered in reaching the American public with information about pandemic influenza include:
-
The increasing cultural and ethnic diversity of American society (e.g., materials and messages need to be provided in multiple languages and involve the use of multiple spokespeople).
-
Variable health literacy, with crucial deficits among some populations.
-
“Information overload” that divides public attention to the extent that people need to be exposed to a message 10 to 12 times (a number that has doubled over the past decade) before it receives attention, and presumably many more before people actually gain knowledge and change their behavior.
In addition, communication challenges or issues can arise when the desire/need to motivate large numbers of people to take action meets the logistical issues and challenges that arise in implementing large-scale programs (e.g., vaccinating large numbers of people). Thus, it can be relatively easy to put out messages that seemingly tell people they need to act quickly, but “not too quickly” because of an inability to accommodate demand. It is difficult to tell people that everyone needs to act, but that “we don’t want everyone to act at once.” Thus the message to “be afraid, but not too afraid” represents the crux of many health communication challenges. In the case of pandemic influenza, the goal is to have people understand that there are some individuals who ought to act immediately to protect their health and lives through immunization, and others who can and will need to wait until a later point (and that there are actions or steps that those who are being asked to wait can take to help reduce their risk).
To effectively develop and communicate the various messages and recommendations that will need to be used in a pandemic, a comprehensive and highly coordinated approach to communication is necessary. This will require a strong investment in research and collaborations to help determine which messages resonate, particularly among people who are not usually inclined to get an influenza vaccination. The use of less nuanced messages and advice should be investigated, coupled with the development and use of portfolios of messages and materials that recognize the cultural and racial diversity that exists in this country.
We also need to go beyond the news media in terms of developing communication plans that allow our messages greater visibility, scope, and frequency of delivery to the public (Glass and Schoch-Spana, 2002). To do so will be costly because broad coverage means getting the message across in the vast numbers of existing mass media outlets.
Finally, ensuring the effectiveness of public communication during an influenza pandemic will require a greater understanding and use of risk communication principles (Sandman, 1993). Health officials will need to learn how to share the dilemmas they face with the public in a productive and effective fashion. We are going to have to acknowledge uncertainty and gaps in scientific knowledge. When faced with the necessity of setting priorities for who will receive limited amounts of vaccine, we must be ready to provide effective coping strategies and advice to those who must wait their turn.
STRATEGIES TO REMEDY PANIC IN A PANDEMIC: LESSONS FROM BIODEFENSE
Monica Schoch-Spana, PhD
Center for Biosecurity
University of Pittsburgh Medical Center
“How will the public react to a biological attack?” is a fundamental question underpinning U.S. policy and practice in the realm of terrorism preparedness and response. Over the past 6 years, widely divergent approaches to the issue of mass responses to bioterrorism have emerged.6 When catastrophic terrorism was a serious but postulated danger, officials frequently conceived public reactions to a biological event as part and parcel of the crisis to be contained: for example, the “worried well” who would pour into hospitals, hindering health care workers’ ability to treat “real” victims. The complex realities of September 11, 2001, and the anthrax letter attacks have helped refine many authorities’ understanding of the public not simply as a problem to be managed, but a constituency to be served—anxious people who need good information about the danger and what to do about it. This essay advances a third approach, encouraging authorities to place current commitments to improving public communication within a broader understanding of the governance dilemmas that bioterrorism and other health emergencies pose.
From Crowd Management to Credible Communication
Attitudes and operational approaches among U.S. decision makers and professional responders toward the public have shifted from an emphasis on containing disorder to communicating information in the bioterrorist context. Playing one-dimensional roles in hypothetical scenarios, members of the public usually surfaced as mass casualties or hysteria-driven mobs who self-evacuate affected areas or who resort to violence to gain access to scarce, potentially life-saving antibiotics and vaccines (Schoch-Spana, 2003). Prior to 2001, official response systems were often built around the notion of the public as a problem to be managed during a crisis; this bias, which remains to a certain extent today, precludes careful consideration of, and planning for, ways to solicit the cooperation of affected populations. Emphasis instead is on crowd control, not enhancing the people’s ability to cope with a public health emergency.
Communication failures, however, during the serial tragedies of 2001 spurred recognition of the essential role of public outreach in managing the effects of a bioattack. Following the anthrax crisis, federal health authorities identified risk communication and health information dissemination as one of seven priority areas required to upgrade the ability of state and local health departments to respond to bioterrorism. Critical reflection on responses to the 2001 terrorist attacks also spurred the release of many helpful analyses and guidebooks for officials regarding successful communication with the media and the larger public (U.S. Department of Health and Human Services, 2002; Ethiel, 2002; CDC, 2002; Fischhoff, 2002). Practitioner and policy-maker interest in public communication remains high: Typically, two of the top five articles that are downloaded each month from the journal, Biosecurity and Bioterrorism, have a focus on communication (Personal communication, Jackie Fox, Biosecurity and Bioterrorism). U.S. and World Health Organization pandemic influenza planning similarly recognizes risk communication as a critical public health intervention (Gellin, 2004; Stöhr, 2004).
Managing Infectious Disease Threats in the Information Age
The anthrax letter scare in 2001 revealed the many communication challenges that can arise in an uncertain, evolving, large-scale health crisis that involves infectious disease.7 Briefly reviewed here are select findings from a national, qualitative study of public communication experiences during that event (see Table 6-9) (U.S. Department of Health and Human
TABLE 6-9 Research Design: Public Communication During 2001 Anthrax Scare
|
Method |
23 small, moderated, taped, and transcribed discussions held June 2002 to June 2003 |
||
|
Sites |
Based on proximity or distance to 2001 events; varying size and density as well as regional diversity: |
||
|
|
Baltimore, MD |
New York, NY |
Seattle, WA |
|
|
Kansas City, MO |
San Antonio, TX |
Washington, DC |
|
Subjects |
Professional responders – Local political leaders, health and safety officials, doctors, nurses, journalists, and Red Cross (n = 66) |
General public – Workers at risk of anthrax exposure: e.g., mail handlers, congressional and media outlet staff (n = 66) – Grassroots leaders from diverse groups and neighborhoods (n = 82) |
|
Services, 2002). The findings and implications drawn out in Figure 6-4 underscore that the Information Age presents both opportunities and obstacles in managing infectious disease threats. In general, communication deficits during the anthrax crisis point to the need for proactive remedies in the precrisis period.
Parallels between the anthrax scare and an influenza pandemic make the former case relevant to the larger issue of prevention and response. Like influenza, anthrax infection during fall 2001 was seen as something of an “everyman’s” disease by virtue of the postal system’s involvement (most people receive mail) and the inexplicable deaths of Kathy Nguyen and Ottilie Lundgren, apparent bystanders who were not members of the then-defined “at-risk” populations.8 The September 11 attacks, too, had fostered a widespread sense of vulnerability. However, limits to generalizing from this case study exist; for example, an influenza pandemic threatens the possibility of widespread, high morbidity and mortality, a significant contrast with the U.S. anthrax experience.
Contemporary Outbreaks Can Have Broad Impact Due to Their Increasing “Spectacle” Quality
In today’s information-saturated environment, outbreaks affect diffuse publics without immediate epidemiological and physical involvement. Simi-
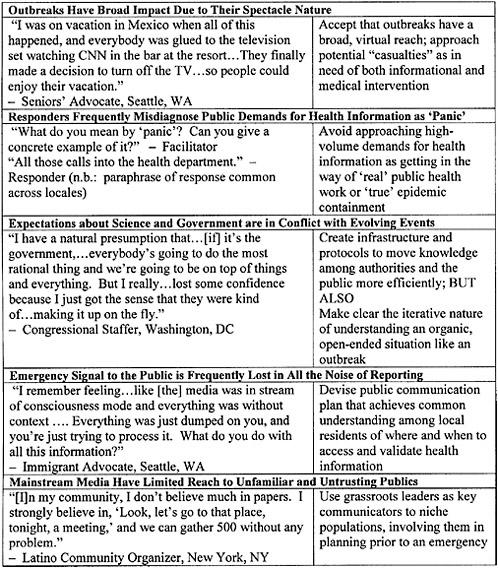
FIGURE 6-4 Communication dilemmas in the Information Age: Lessons learned during 2001 anthrax scare.
larly, at the peak of the global SARS outbreak, the New York City Department of Health discovered that some residents were transposing what they were reading and seeing about Hong Kong and other hard-hit areas to conditions in New York, where the impact had been minimal (Roberts, 2003). The crisis elsewhere, that is, became the baseline for what was perceived to be happening locally. Word of, and worry about, epidemics can move readily throughout diverse populations, leading to demands on
public health and safety officials and medical practitioners outside of disease epicenters.
Authorities Frequently Misdiagnose Public Demands for Health Information as “Panic”
Powder scares, anthrax exposure tests, and health information demands—by a majority of people at no or minimal risk of infection—produced excess demands on physicians, hospitals, law enforcement, and public health and safety personnel. Overburdened and confronting a lethal event, many authorities understandably interpreted such demands as “panic,” that is, a problem of public irrationality or overreaction. From the vantage point of persons consciously looking for expert guidance on health matters in a novel threat situation, however, such demands are reasonable. Characterizing high-volume information requests in a crisis as panic obscures more systemic deficits within U.S. health care and public health systems, such as limited ability to ramp up activity to meet unforeseen, large-scale demand and a lower professional and institutional priority placed on health risk and crisis communication.
The Emergency “Signal” to the Public Is Frequently Lost in the “Noise” of Reporting
Officials’ need and desire to convey clear and consistent messages must contend with diverse media, instantaneous reporting, and a potentially overwhelming amount of information available to the members of the public, who lack clear criteria for sorting “noise” from critical information. Research subjects reported alternating between a feast and famine of information: At certain times, they felt starved for official guidance that came out at a trickle; at other times, they felt inundated by the disparate, evolving bits of information streaming from news sources. A truly “public” broadcast system (noncommercial and noncompetitive) that provided a reliable flow of information, with regularly scheduled updates, was judged absent during the anthrax attacks and was frequently offered as the possible technological and institutional solution for the twin problems of information scarcity and overload.
Mainstream Media Have Limited Reach Among Unfamiliar and Untrusting Publics
Mass media reach the largest number of people the most quickly, and many research subjects reported that despite the overwhelming amount of information available via news reports, they still found much of what they
were seeking. At the same time, grassroots civic leaders and smaller media outlets serving ethnic and immigrant communities were seen to provide a better route for reaching populations that either do not routinely use or do not trust mainstream media, or who are suspicious of official government pronouncements. In an era where information technology promises to connect everyone, “lower tech” options such as person-to-person communication networks may be the more appropriate outreach mechanism for disenfranchised populations.
Expectations About Science and Government Are in Conflict with Uncertain, Evolving Events
“Some government expert somewhere must know what to do in this kind of crisis” was an operating assumption for many research subjects when they recalled their anthrax experience. In an era where satellites can read license plate numbers, people understandably have high expectations about the ability of government officials and technical experts to “know” something. People not directly affected by the attacks posited that authorities did not provide adequate updates of emergency information either because they were acting in a deliberate, paternalistic manner and with-holding information, or they were unable to convey the information efficiently out of incompetence. A third explanation—that absolute understanding of the danger and its medical aspects was lacking—was relatively absent. People directly affected by events recounted having their belief in an omniscient government undermined by firsthand experience of the tentative nature of authorities’ approach to the crisis.
Communication as a Means to an End, Not an End in Itself
As 2001 demonstrated, open and informative relationships among citizens, government, and public health and safety authorities are fundamental to a population’s ability to cope with unconventional health threats. Abundant communication technologies prove both benefit and burden for authorities having to contain an infectious disease threat. U.S. leaders and professional responders should be lauded for embracing effective crisis and risk communication as remedies for a potentially anxious, skeptical, and/or resistant public. Powerful cultural and technological forces—for example, computerization, media proliferation, the Internet, e-mail—make it easy, however, to think of social life merely in terms of information exchange. Authorities should be careful not to approach improved communication as the “quick social fix” for the more complex, underlying tensions that precede or emerge during bioattacks or other health crises (Sorenson, 2004).
Public communication and risk communication have become code words with which to skirt the more complex realities associated with com-
munity responses to bioterrorist and other infectious disease threats. When authorities say they want better communication with the public, what they tend to mean is public “buy-in,” public compliance, and understanding—possibly even absolution—when tough choices arise for officials, such as how to distribute scarce resources in an emergency. When members of the public indicate that they want better communication from officials, what they are asking for is inclusion, consideration, and mutual respect as peer decision makers; expert guidance on which they can act; and proof that their needs have justly been considered by people in authority. As the United States gravitates toward communication as a key to bioterrorism readiness, everyone should reflect on what that communication is meant to accomplish.
Governance Dilemmas as Critical Contexts for Public Communication
The larger social and political context for public communication practice was the analytic focus of the Working Group on Governance Dilemmas in Bioterrorism Response (2004). Whether “natural” or “deliberate” in origin, a large outbreak poses unique governing dilemmas. Leaders must tend to immediate life-and-death matters such as caring for the sick, ward off socially corrosive effects like ostracism of the afflicted, and stem dramatic economic effects for victims and affected locales alike. Conflicts of interest, priority, and purpose can emerge in pursuit of these goals. The Working Group prepared a set of analytic templates for decision makers faced with these difficult situations to better prepare them to safeguard the public’s trust and cooperation during a response to an infectious disease threat. The framework was intended to stave off the temptation of leaders to focus on the managerial and scientific aspects of response to the neglect of civic, social, ethical-moral, and economic dimensions that also matter to communities.
What Defines “Leadership” During an Epidemic or Biological Attack?
Five strategic goals help distinguish successful leadership during an epidemic or bioattack in twenty-first-century America. An informed and involved public, along with guidance and material support from respected leaders, can help achieve these aims:
-
Limit death and suffering through proper preventive, curative, and supportive care; tend to the greater vulnerability of children, the frail elderly, and the physically compromised.
-
Defend civil liberties by using the least restrictive interventions to contain an infectious agent that causes communicable disease.
-
Preserve economic stability, managing the financial blow to victims as well as the near- and long-term losses of hard-hit industries, cities, and neighborhoods.
-
Discourage scapegoating, hate crimes, and the stigmatization of specific people or places as “contaminated” or unhealthy.
-
Bolster the ability of individuals and the larger community to rebound from unpredictable and traumatic events; provide mental health support to those who need it.
What Leadership Dilemmas May Arise in an Epidemic, and How Might They Be Averted?
Large-scale outbreaks are complex events that provoke fear and contradictory impulses. Because an epidemic’s impact—illness, death, lost livelihood, disrupted commerce—is troubling to consider, leaders and the larger public may deny that a problem exists, or intervene too quickly without regard to the negative effects of their actions. Once acknowledged, an epidemic exerts immense political and social pressure for swift, decisive, visible response (Rosenberg, 1989), more so in the case of a deliberate epidemic. Apparent and sometimes genuine conflicts among strategic goals can arise. The most common dilemmas facing past leaders have been balancing disease control imperatives with those of individual liberty, economic stability, and stigma prevention (Box 6-1).
What Situations Splinter the Social Trust Necessary to Cope with Health Crises, and How Might They Be Defused?
Mutual confidence and obligation among decision makers, citizens and their leaders, and community members are the basis for achieving any and all strategic goals. Breaches of social trust, however, are a common predicament for leaders during outbreaks and are likely to arise during a bioattack (Box 6-2). Conditions that confound social trust involve preconceptions about “the government,” “the public,” or “the media”; the social and economic fault lines that are exacerbated by disease and dread of it; and questions about the morally defensible use of communal resources in times of crisis.
Governing successfully during large, fast-moving, lethal epidemics requires a dynamic collaboration among members of a community and the community’s leaders. Officials who have realistic expectations about the societal challenges posed by large outbreaks will be better prepared to protect and actively support cooperation and trust between a community and its leaders. In the absence of an engaged public, resolution of the
|
BOX 6-1 Stop disease that spreads from person to person while upholding individual freedoms
Protect the economy while using disease controls that disrupt commerce
Restore social bonds when people feel at the mercy of a mysterious disease
|
|
BOX 6-2 Prevent unproductive fear, denial, or skepticism on the part of the public when delivering crisis updates
Earn confidence in the use of scarce resources despite existing social and economic gaps
Maintain credibility when decisions must be made before all the facts are in
|
immediate health crisis is rendered far more difficult, and the resilience of affected communities is diminished.
Increasing emphasis on enhanced public communication is a positive development within biodefense, and public health preparedness and response more broadly. Nonetheless, this development must be supplemented with robust discussion among leaders, and between authorities and the larger population, as to what an optimal response looks like, and from whose point of view.
Acknowledgments
The Working Group on Governance Dilemmas in Bioterrorism Response and the research focus groups—the findings of which are presented here—were convened by the Center for Biosecurity of the University of Pittsburgh Medical Center in collaboration with the Johns Hopkins University and supported under award MIPT-2003J-A-019 from the Oklahoma City Memorial Institute for the Prevention of Terrorism (MIPT) and the Office for Domestic Preparedness, Department of Homeland Security, and award 2000-10-7 from The Alfred P. Sloan Foundation. Points of view expressed in this document do not necessarily represent the official position of MIPT, the U.S. Department of Homeland Security, or the Sloan Foundation.
PUBLIC HEALTH PREPAREDNESS AND ETHICAL VALUES IN PANDEMIC INFLUENZA
Lawrence O. Gostin9
Georgetown University
Severe Acute Respiratory Syndrome (SARS) garnered a great deal of public attention because it was novel and its potential for spread was unknown. However, the SARS coronavirus is significantly less virulent than pandemic influenza viral infections. Influenza pandemics have occurred roughly two to three times per century, causing untold morbidity and mortality (Kolata, 1997). The Spanish influenza pandemic of 1918 caused more
than 20 million deaths in a world less than one-third the size of the current global population (Stevens et al., 2004). Modern epidemiologists now estimate that more than 50 million people died. These deaths did not occur primarily among infants and old people as suggested by conventional wisdom. Approximately half the deaths were among people in the prime of their lives. As John Barry explains in his recent book, “One cannot know with certainty, but if the upper estimate of the death toll is true as many as 8 to 10 percent of all young adults then living may have been killed by the virus. And they died with extraordinary ferocity and speed” (Barry, 2004).
The Institute of Medicine (IOM) has noted three essential prerequisites for an influenza pandemic: (1) the identification of a novel viral subtype in animal populations such as swine or poultry, (2) viral replication causing disease in humans, and (3) efficient human-to-human transmission (Institute of Medicine, 2004). The species “jump” from animals to humans could occur through a process known as “reassortment.” If a person is exposed to both animal and human viral infections, the “genetic mixing” could lead to a strain that is transmissible from human to human, sometimes in ways that are highly resistant to vaccination or antiviral treatment.
Since 1997, the first two prerequisites—a novel viral strain in animals and transmission from animals to humans—have been met on four occasions. The most recent episode occurred in 2004 with H5N1 influenza found in Vietnam and Thailand (CDC, 2004b). The avian influenza outbreak resulted in the culling of large chicken populations, including farms in the United States, with severe economic and trade impacts (Dao, 2004). There is now intense interest in influenza preparedness (Webby and Webster, 2003), with major planning initiatives being undertaken by the World Health Organization (WHO, 2004a) and the IOM (2004).
The potential for pandemic spread of a “fit” influenza strain leads to intriguing ethical and legal questions about public health interventions that could severely disrupt trade, economics, travel, and personal liberty. National and global public health agencies have mooted a wide range of interventions, asking penetrating questions such as: Should intrusive powers be exercised? At what stage in the outbreak should interventions commence and with what safeguards? Planning for the next pandemic includes not simply influenza but other novel infections, both naturally occurring and intentionally disseminated (Weinstein, 2004).
This section examines the principal therapeutic and nontherapeutic public health interventions for preventing or ameliorating pandemic influenza. In each case, the hard legal and ethical questions likely to arise are explored. Thereafter, the section provides several ethical values that can help evaluate public health interventions.
Public Health Interventions to Prevent or Ameliorate Pandemic Influenza
Animal/Human Interchange
A critical early preventive strategy is to control animal populations and prevent the species jump from animals to humans (see Table 6-10). Humans are highly vulnerable to animal infections due to the close proximity of animal and human populations in farming and distribution of poultry and meat (Emanuel, 2003). Strategies to diminish the risk include separation of animal and human populations; occupational health and safety in animal work (e.g., infection control and disinfection); and control of diseased or exposed animal populations (e.g., culling).
The international community faces daunting problems in implementing these strategies. International food safety law does not emphasize animal/ human interchange. The Codex Alimentarius Commission, administered by WHO and the Food and Agricultural Organization (FAO), regulates food hygiene and labeling. Codex’s main concern is with the safety of the food supply and fair standards for international trade in food.10 Occupational health and safety rules are primarily found at the national level, and country safeguards are highly variable. Countries may have a self-interest in continuing intensive farming and food distribution. These methods are cost-effective from an economic perspective, but do not necessarily result in safe practices to prevent animal-to-human transmission of disease.
Even if strong international health standards did exist, public health authorities would continue to face the problem of when to implement aggressive strategies such as culling. Premature interventions have profound economic implications affecting livelihoods and trade. However, weak or tardy interventions risk devastation to animal and human populations.
Global Surveillance
Surveillance of novel infections in humans offers early warning, providing an opportunity for a timely response (see Table 6-10). Experts recommend various surveillance activities, many of which were used in the 2003
TABLE 6-10 Public Health Interventions: Purposes and Values
|
Public Health Intervention |
Purposes and Objectives |
Strategies to Achieve Public Health Purpose |
Ethical Issues and Recommendations |
|
Animal/Human Interchange |
Prevent “species jump” by reducing proximity of animals and humans |
Separation of animals and humans; occupational health and safety; control of diseased animals |
Safeguard economic interests in farming while protecting the public’s health |
|
Global Surveillance |
Timely and systematic monitoring of health threats |
Cover all threats of global importance; prompt country reporting; use “small-world networks” |
Ensure privacy safeguards for individuals and protection of groups |
|
Case Contact Investigations |
Prevent spread of infection to contacts of infected or exposed persons |
Offer counseling, vaccination, and/or treatment to infected or exposed persons |
Conduct investigations with sensitivity and respect for individuals and their contacts |
|
Vaccination and Medical Treatment |
Prophylaxis, amelioration of symptoms, and/or reduced infectiousness |
Offer or require vaccination or antiviral therapy to at-risk or infected persons |
Balance bodily integrity with the common good; ensure fair allocation of scarce resources; make therapeutics available to developing countries |
SARS outbreaks: testing and screening; health questionnaires, notices, and declarations; fever monitoring (self-monitoring, thermal scanning); and reporting and monitoring trends (Gostin et al., 2003).
Despite its importance, many countries do not conduct effective and timely surveillance. Prompt notification of an infectious disease threat can affect a country’s tourism, trade, and prestige. Consequently, some governments do not respond promptly to WHO requests for information. Many countries, moreover, lack the infrastructure and resources to conduct surveillance. As a result, national surveillance activities are highly variable.
The current International Health Regulations (IHR) are weak, applying only to three diseases: cholera, plague, and yellow fever. However, WHO’s draft revised IHR, if adopted, would significantly strengthen international rules for surveillance. They would apply to all health threats of interna-
|
Public Health Intervention |
Purposes and Objectives |
Strategies to Achieve Public Health Purpose |
Ethical Issues and Recommendations |
|
Community Hygiene |
Promote safer behaviors among the population |
Health education on hand washing, disinfection, masks, ventilation, and avoidance of contacts |
Balance health benefits with costs and cultural sensitivities; ensure equitable access |
|
Travel and Border Controls |
Prevent cross-border spread of infectious disease |
Travel advisories; border restrictions; regulation of conveyances; stop-lists |
Health is salient; avoid unnecessary restriction of trade; safeguard against discrimination |
|
Decreased Social Mixing/ Increased Social Distance |
Increase social distance to avoid rapid spread of infection in public settings |
Close civic activities, meeting places, and transportation systems |
Avoid heavy costs and diminished freedoms; deliver services to the vulnerable |
|
Civil Confinement |
Separate the infected or exposed from the healthy |
Isolation; quarantine; cordon sanitaire |
Provide due process; ensure safe and humane setting; consider compensation; gain public’s trust |
tional importance; mandate country notifications; gather reports from unofficial sources; and provide for real-time event management (WHO Secretariat, 2004). Global surveillance could further benefit from “small-world networks” consisting of health professionals, scientists, and nongovernmental organizations continuously monitoring disease threats (Gostin, 2004). It should be possible to supplement the surveillance provided by official sources with multiple public/private sources through the Internet and other modern communication vehicles.
Although surveillance is an essential public health strategy, even routine activities such as reporting affect privacy because government collects sensitive health information. Acute outbreaks can trigger more extreme measures such as continuous monitoring of certain populations (i.e., health care workers, immigrants, and travelers). An outbreak of a novel influenza
strain will inevitably raise questions about the appropriate scope of government surveillance and its effects on privacy. Surveillance needs to take place, therefore, with privacy safeguards firmly in place.
Case Contact Investigations
Case contact investigation is a classical form of surveillance. It involves identifying infected or exposed persons and following their recent contacts. This provides an opportunity to interrupt the spread of infection (see Table 6-10). Persons exposed or infected can be offered antiviral therapy as a prophylaxis or treatment. Those who are infectious or potentially infectious can be separated from the healthy population.
Case contact investigation is ostensibly voluntary because the “index case” is under no formal obligation to reveal his or her contacts. Nevertheless, its use in sexually transmitted infections and HIV/AIDS has proved highly controversial (Bayer and Toomey, 1992). The index case may feel coerced into giving information, investigations inherently pose privacy risks, and individuals may experience stigma and discrimination. These investigations, therefore, need to be conducted with sensitivity and respect for individuals and their family, friends, or associates.
Vaccination and Medical Treatment
The dominant strategy for seasonal influenza is to use vaccinations and antiviral therapy (see Table 6-10). Recommended vaccination of high-risk populations (e.g., children and the elderly) has become standard in developed countries, and mass vaccination could be recommended in the event of a more severe outbreak. Antiviral therapy, although not as effective as vaccination, can be used for prophylaxis, alleviation of symptoms, and reduction of infectiousness (Longini et al., 2004).
Therapeutic interventions raise distinct ethical and legal concerns. Although mandating competent adults to be vaccinated or treated for their own protection is a difficult notion to espouse, the law permits a reasonable interference with bodily integrity to prevent harm to the community (Jacobson v. Massachusetts, 197 U.S. 11 [1905]).
Although officials have the legal authority to compel vaccination or treatment to protect the public, the political and ethical dimensions of doing so are complex. There is a long history of opposition to vaccinations among certain sections of the population (Spier, 2001). Anti-vaccination sentiments are not always irrational because immunizations can pose risks, as well as confer benefits. Mass vaccination to avert an influenza epidemic can go horribly wrong, as occurred with swine flu in 1976: The CDC campaign to immunize the American population cost $134 million and
caused Guillain-Barré syndrome in some vaccine recipients (Neustadt and Fineberg, 1983).
When used appropriately, vaccination or treatment can confer considerable benefit to the individual and ultimately to a population. Pandemic influenza would likely result in a paucity of vaccines and antiviral medications, raising the hard problem of fair allocation of scarce resources. What ethical values should guide rationing decisions: private need (treatment of the sick); public need (prevention among vulnerable populations); maintenance of essential services (health care workers and “first responders”); or political influence (priority for those with political connections)? Justice may require that therapeutic interventions be used to benefit the most people possible, irrespective of their power or influence. This would militate toward the use of “public need” as the principal ethical value. Therapeutics, therefore, would be used primarily for prevention and targeted to those who pose the greatest risk of transmission. The ethical value of “public need” might also require use of therapeutics for emergency workers to ensure maintenance of essential services and ongoing assistance to the public. This would place private need and political influence lower on the priority scale.
The global reality is that rich countries will have much less scarcity than poor countries. The ethical question then arises as to whether developed countries would be expected to forego some of their precious stockpile of vaccines and antiviral medications for the sake of poorer countries experiencing a higher burden of morbidity and mortality from influenza. One might argue that it is in the richer country’s self-interest to do so because infectious disease can and does travel across the globe. Ethical analysis would prove difficult—do developed countries have an obligation to reduce the burden of disease in developing countries? If all human life has the same worth, then it may be ethically desirable to devote therapeutic resources to poor regions experiencing higher burdens of disease. This allocation of resources is likely to have the maximum beneficial effect on morbidity and premature mortality.
Community Hygiene
One of the most valuable means of infection control is also the least intrusive. Health education to promote safer behaviors such as hand washing, disinfection, masks, ventilation, and avoidance of contacts can be highly effective (see Table 6-10). Community hygiene, although largely uncontroversial, can impose costs (e.g., purchasing and distributing equipment) and cause social unrest (e.g., exaggerated concerns about health risks). Hygiene measures are also culturally sensitive—notice the difference in mask-wearing habits in Asia as compared to North America and Europe.
Under what circumstances should public health authorities issue a national recommendation for aggressive hygiene measures given the costs and cultural expectations? Probably the most important concern would be the cost effectiveness of the hygiene measure. If a hygiene measure is clearly cost effective, then the public has the right to know how to adopt that measure in a safe way. Vulnerable members of the community may also need economic and technical assistance to ensure equitable access to essential hygiene measures. If a measure is not cost effective, then public health authorities have an obligation to inform the public about the lack of effectiveness and the risks. In some cases, such as the use of masks, the evidence for, or against, effectiveness may be unclear. In such instances, the principle of transparency may suggest that public health officials should state honestly the lack of conclusive evidence, leaving the judgment to the individual.
Travel and Border Controls
One of the first instincts in the face of infectious disease threats is to protect national borders (see Table 6-10). Consequently, international or national health agencies may issue travel advisories, establish border restrictions, or regulate conveyances such as airplanes, ships, and trains. They might similarly use “stop-lists” to prevent specified individuals or groups from traveling. The IHR afford WHO considerable authority to regulate international travel and control borders.
Travelers legitimately claim the right to know health risks, but restrictions significantly affect tourism and trade. Consequently, travel advisories can be politically charged, as were WHO advisories concerning SARS in Ontario, Canada (Krauss, 2003). A delicate balance exists between trade and health. Indeed, the draft revised IHR directs WHO to “provide security against the international spread of disease while avoiding unnecessary interference with international traffic” (WHO, 2004b).
When faced with a hard tradeoff between maximization of health or of trade, which should prevail and why? Arguably, health should take precedence over trade because of the fundamental value of human functioning and life itself. Despite the effects on tourism and trade, the public has a legitimate interest in knowing if there are health hazards in regions where they intend to travel. National and international public health agencies have an obligation to take steps that are necessary to prevent the spread of infection across borders. Thus, it would be legitimate to prevent travel of a person who poses a significant risk of transmission. What public health authorities may not do is use infectious disease control as a pretext for discrimination by targeting individuals based on their nationality, race, religion, or other status.
Decreased Social Mixing/Increased Social Distance
Most Americans take for granted the freedom to associate with others in a variety of social settings. Yet public health authorities could restrict social mixing and increase social distance to avert a serious infectious disease threat (see Table 6-10). This might involve closures of civic activities (e.g., schools, workplaces), meeting places or large gatherings (e.g., sports events, theatres, business meetings), and transportation systems (e.g., mass transit, airlines). The purpose behind restrictions on mixing is to prevent rapid spread of infection in settings where multiple people congregate.
The U.S. Constitution affords individuals the freedom to associate, but courts would likely defer to reasonable regulation of congregate settings to prevent transmission of infection (New York v. New St. Mark’s Baths, 497 N.Y.S.2d 979 [1986]). As with other interventions, closures entail heavy costs in lost revenue as well as in diminished freedoms. When an infectious disease outbreak deeply affects a society’s everyday activities, public health authorities will have to cogently explain the justifications for the chosen intervention and gain the public’s confidence prior to implementation. Critical legal and logistical questions loom: Which authority has the power to close a venue; what criteria should be used to trigger a closure and when should the restriction be lifted; and how will services be delivered to vulnerable populations who may be at risk in an isolated residence or shelter?
Civil Confinement
The potential for a mass outbreak raises the specter of civil confinement to separate the infected or exposed from healthy individuals (see Table 6-10). This might entail isolation of infected persons, quarantine of exposed persons, or quarantine of a geographic area (cordon sanitaire). Civil confinements may take place in hospitals or other institutions or in a person’s home. New conceptions to separate the healthy from the infectious include “sheltering in place,” which public health authorities analogize to a “snow day.”
Many states modernized their public health statutes in the aftermath of the terrorist attacks on September 11, 2001 (Gostin et al., 2002). Public health law reform is necessary to ensure that states and localities have the legal authority for isolation and quarantine (Gostin, 2002). In order to meet constitutional standards, state law must have clear criteria for the use of civil confinement and offer procedural due process (Greene v. Edwards, 263 S.E.2d 661 [W.Va. 1980]).
Civil confinement, of course, raises powerful civil liberties concerns. Not only is isolation or quarantine a deprivation of liberty, but enforcement can sometimes be intrusive. For example, during the SARS outbreaks, some countries used electronic bracelets, web cameras, and police. It will
also be important to ensure that judicial hearings are available, particularly in a mass outbreak. Isolation or quarantine will have to take place in a humane and habitable environment. Vulnerable persons will need to be protected against reexposure to infection, offered care and treatment, and ensured the necessities of life such as safe food and water (Barbera et al., 2001). There may also be the need to consider compensation for lost work. Individuals are confined for the good of the community and have to forego their livelihood and other essential activities. Above all, public health authorities need to maintain the public’s trust. To what extent would orders for civil confinement dissipate trust and reduce cooperation?
Acting Under Conditions of Uncertainty: The Key Scientific and Social Questions
Influenza pandemic preparedness requires careful consideration of the public health strategy as well as the legal and ethical implications. Several key scientific questions loom: Are specific interventions proven cost effective? What combination of measures is most cost effective? During what phase of the pandemic should interventions be implemented? When should public health measures be discontinued?
Although the foregoing interventions have been widely used, many still lack adequate evidence of cost effectiveness. Even if individual interventions are known to be cost effective, public health authorities will have to form a judgment as to the combination of measures that will be maximally effective. They will need to decide when to initiate and when to end an intervention.
The decision to intervene is a difficult one because public health authorities may be acting under conditions of scientific uncertainty. It may be unclear whether serologic tests are reliable, vaccines or treatments are safe and effective, and coercive interventions are acceptable to the population. To be effective, agencies may have to intervene at the earliest stages, before the threat level is clear. If interventions are well targeted and timed, then public health officials may prevent untold economic and human harm. However, if the interventions overreach, officials will be accused of disregarding essential economic interests and fundamental human rights.
These scientific questions are important because public health interventions do not take place in a vacuum. They raise fundamental economic, political, and legal questions that need to be considered.
Economics
As mentioned earlier, public health interventions can have dire effects on the economy. They impede individual economic freedoms to travel and
pursue a business or livelihood. They also affect local, national, and regional economies through the impacts on trade, travel, tourism, and agriculture. Countries may have built-in disincentives to conduct surveillance and response in an energetic and public way.
Political
Infectious disease outbreaks can have intense sociopolitical ramifications. Diseases affect a country’s prestige as well as its economy, and the electorate may hold politicians accountable. As a result, political leaders may try to deemphasize the threat or delay taking definitive action, which has occurred in numerous epidemics ranging from HIV/AIDS to SARS.
Legal and Constitutional
Infectious disease outbreaks take place in countries with vastly different legal and constitutional traditions. Public health planning may be undertaken within liberal democracies guaranteeing full protection of human rights or they may take place in less democratic, perhaps more authoritarian, societies. During the SARS outbreaks, for example, countries behaved very differently in their response to and protection of civil liberties (Sapsin et al., 2003). Infectious diseases tend to bring out the best and worst in societies. History demonstrates the potential for overreaction, stigma, and discrimination in the face of a severe epidemic (Gilman, 1999). Consequently, the legal and constitutional dimensions will be important in confronting a severe epidemic (Gostin, 2000).
Ethical Values Underpinning Public Health Preparedness: The Cross-Cutting Issues
Public health authorities have a mandate to protect the population’s health. It is crucial, however, that they act ethically. Ethical values are usually too broad to determine precisely whether a particular activity is morally appropriate. Nevertheless, it should be possible to articulate several ethical values that can inform public health practice, particularly in an emergency.
Transparency
The ethical value of transparency requires officials to make decisions in an open and fully accountable manner. Government officials must be willing to make clear the basis for public health measures. They should honestly and openly inform the public about what is known and not known;
openly acknowledge when new evidence warrants reconsideration of policies; and educate the public about the goals of intervention and the steps taken to safeguard individual rights.
Protection of Vulnerable Populations
Diseases that may differentially affect segments of the population have usually imposed the additional burden of social opprobrium. Public health officials may inadvertently amplify the process as they conduct their surveillance activities. Although they may not be able to prevent stigmatization completely, officials have an obligation to take steps to mitigate the suffering that may attend their efforts by underscoring the irrationality and inequity of ethnic stereotyping. Consultation with representatives of the communities most at risk will be important for both instrumental reasons and as an expression of social solidarity. Individuals should feel a sense of participation in crucial decisions affecting their lives and communities. People place their trust in political leaders and, in return, deserve due consideration of and respect for their health and human rights.
Fair Treatment and Social Justice
Justice requires that the benefits and burdens of public health action be fairly distributed, thus precluding the unjustified encumbering of already socially vulnerable populations. Equitable public health action is based on science and assures reasoned, population-based policies. Procedural justice requires a fair and independent hearing for individuals who are subjected to burdensome public health action. Due process requirements are inherently important because fair hearings affirm the dignity of the person; due process is also instrumentally important because it ensures accurate decision making.
The Least Restrictive Alternative
International human rights law is guided by the principle of proportionality: interventions should be necessary and proportional to the risk posed (Siracusa principles, 1985). Interventions should be the least restrictive alternative necessary to prevent or ameliorate the health threat. Requiring the least restrictive/intrusive alternative represents a means to impose limits on state interventions consistent with the traditions of privacy, freedom of association, and individual liberty. The standard does not require officials to utilize less-than-optimal interventions, but rather to select the least intrusive alternative that can best achieve the identified health objective.
The Public Health Paradox
There is no way to avoid the dilemmas posed by acting without full scientific knowledge. Failure to move aggressively in the early stages of pandemic influenza can have catastrophic consequences. Actions that prove to have been unnecessary will be viewed as draconian and based on hysteria. The only safeguard is the adoption of ethical values in formulating and implementing public health decisions. Public health policy will reflect in a profound way the manner in which humane societies both implicitly and explicitly balance the common good with respect for personal rights.
REFERENCES
Barbera J, Macintyre A, Gostin L, Inglesby T, O'Toole T, DeAtley C, Tonat K, Layton M. 2001. Large-scale quarantine following biological terrorism in the United States: Scientific examination, logistic and legal limits, and possible consequences. JAMA 286(21):2711–2717.
Barker WH. 1986. Excess pneumonia and influenza associated hospitalization during influenza epidemics in the United States, 1970–78. Am J Public Health 76:761–765.
Barker WH, Mullooly JP. 1980. Impact of epidemic type A influenza in a defined adult population. Am J Epidemiol 112:798–813.
Barker WH, Mullooly JP. 1982. Pneumonia and influenza deaths during epidemics: Implications for prevention. Arch Intern Med 142:85–89.
Barry JM. 2004. The Great Influenza: The Epic Story of the Deadliest Plague in History. 1st ed. New York: Viking.
Bayer R, Toomey KE. 1992. HIV prevention and the two faces of partner notification. Am J Public Health 82:1158–1164.
Blendon RJ, Benson JM, DesRoches, CM, Herrmann MJ. 2001. Harvard School of Public Health/Robert Wood Johnson Foundation Survey Project on Americans’ Response to Biological Terrorism, Study 2: National and Three Metropolitan Areas Affected by Anthrax, November 29–December 3, 2001. [Online]. Available: http://www.hsph.harvard.edu/press/releases/blendon/report2.pdf [accessed January 7, 2002].
Brunell PA, ed. 2004. Importance of vaccinating healthcare workers against influenza. CME monograph from Infectious Diseases in Children. Selected article: Piedra PA. Time has come to make vaccination mandatory. [Online]. Available: http://idinchildren.com/monograph/0402/article6.asp [accessed February 10, 2005].
Campbell DS, Rumley MA. 1997. Cost-effectiveness of the influenza vaccine in a healthy, working-age population. J Occup Environ Med 39:408–414.
Carrat F, Valleron A-J. 1995. Influenza mortality among the elderly in France, 1980–90: How many deaths may have been avoided through vaccination? J Epidemiol Community Health 49:419–425.
CDC (Centers for Disease Control and Prevention). 1998. Prevention and control of influenza: Recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR 47(RR-6):1–26.
CDC. 2002. Crisis and Emergency Risk Communication. Atlanta, GA: CDC.
CDC. 2004a. Questions and Answers: The Disease. [Online]. Available: http://www.cdc.gov/flu/about/qa/disease.htm.
CDC. 2004b. Outbreaks of avian influenza A (H5N1) in Asia and interim recommendations for evaluation and reporting of suspected cases—United States, 2004. MMWR 53(5):97–100.
Cliff AD, Haggett P. 1993. Statistical modelling of measles and influenza outbreaks. Stat Methods Med Res 2:43–73.
Critchfield GC, Willard KE. 1986. Probabilistic analysis of decision trees using Monte Carlo simulation. Med Decis Making 6:85–92.
Dao J. 2004 (February 16). Bird flu outbreak has farmers jittery. New York Times. Sect. A P. 12.
Davis MM, McMahon SR, Santoli JM, Schwartz B, Clark SJ. 2002. A national survey of physician practices regarding influenza vaccine. J Gen Intern Med 17(9):670–676.
Dittus RS, Roberts SD, Wilson JR. 1989. Quantifying uncertainty in medical decisions. J Am Coll Cardiol 14:23A–28A.
Dobilet P, Begg CB, Weinstein MC, Braun P, McNeil BJ. 1985. Probabilistic sensitivity analysis using Monte Carlo simulation: A practical approach. Med Decis Making 5:157–177.
Emanuel EJ. 2003 (May 12). Preventing the next SARS. New York Times. Sect. A. P. 25. Ethiel N, ed. 2002. Terrorism: Informing the Public. Chicago, IL: McCormick Tribune Foundation.
Evans M, Hastings N, Peacock B. 1993. Statistical Distributions. 2nd ed. New York: John Wiley.
Fischhoff B. 2002. Assessing and communicating the risks of terrorism. In: Teich AH, Nelson SD, Lita SJ, eds. Science and Technology in a Vulnerable World. Washington, DC: American Association for the Advancement of Science. Pp. 51–64.
Fox JP, Hall CE, Cooney MK, Foy HM. 1982. Influenza virus infections in Seattle families, 1975–1979. Study design, methods and the occurrence of infections by time and age. Am J Epidemiol 116:212–227.
Gellin B. 2004 (June 16). U.S. Pandemic Influenza Preparedness and Response. Prepared for Institute of Medicine Workshop on Pandemic Influenza: Assessing Capabilities for Prevention and Response, Washington, DC: Institute of Medicine Forum on Microbial Threats.
Gilman SL. 1999. Disease and stigma. Lancet 354(Suppl):SIV15.
Glass TA, Schoch-Spana M. 2002. Bioterrorism and the people: How to vaccinate a city against panic. Clin Infect Dis 34(2):217–223.
Glezen WP. 1996. Emerging infections: Pandemic influenza. Epidemiol Rev 18:64–76.
Glezen WP, Payne AA, Snyder DN, Downs TD. 1982. Mortality and influenza. J Infect Dis 146:313–321.
Glezen WP, Decker M, Joseph SW, Mercready RG. 1987. Acute respiratory disease associated with influenza epidemics in Houston, 1981–1983. J Infect Dis 155:1119–1126.
Gostin LO. 2000. Public Health Law: Power, Duty, Restraint. Berkeley, CA, and New York, NY: University of California Press and Milbank Memorial Fund.
Gostin LO. 2002. Public health law in an age of terrorism: Rethinking individual rights and common goods. Health Affairs 21(6):79–93.
Gostin LO. 2004. International infectious disease law: Revision of the World Health Organization’s International Health Regulations. JAMA 291(21):2623–2627.
Gostin LO, Sapsin JW, Teret SP, Burris S, Mair JS, Hodge JG Jr, Vernick JS. 2002. The Model State Emergency Health Powers Act: Planning and response to bioterrorism and naturally occurring infectious diseases. JAMA 288:622–628.
Gostin LO, Bayer R, Fairchild AL. 2003. Ethical and legal challenges posed by Severe Acute Respiratory Syndrome: Implications for the control of severe infectious disease threats. JAMA 290(24):3229–3237.
Gursky E, Inglesby TV, O’Toole T. 2003. Anthrax 2001: Observations on the medical and public health response. Biosecurity and Bioterrorism 1(2):97–110.
Haddix AC, Teutsch SM, Shaffer PA, Dunet DO. 1996. Prevention Effectiveness. New York: Oxford University Press.
Harper SA, Fukuda K, Uyeki TM, Cox NJ, Bridges CB; CDC Advisory Committee on Immunization Practices (ACIP). 2004 (May 28). Prevention and control of influenza: Recommendations of the Advisory Committee on Immunization Practices. MMWR Recommendations and Reports 53(RR-6):1–40.
IOM (Institute of Medicine). 2004. Learning from SARS: Preparing for the Next Disease Outbreak. 1st ed. Washington, DC: The National Academies Press.
Jefferson T, Demicheli V. 1998. Socioeconomics of influenza. In: Nicholson KG, Webster RG, Hay AJ, eds. Textbook of Influenza. London, England: Blackwell Science. Pp. 541–547.
Kaufmann AF, Meltzer MI, Schmid GP. 1997. The economic impact of a bioterrorist attack: Are prevention and postattack intervention programs justifiable? Emerg Infect Dis 3:83–94.
Kavet J. 1977. A perspective on the significance of pandemic influenza. Am J Public Health 67:1063–1070.
Kolata G. 1997 (March 21). Genetic material of virus from 1918 flu is found. New York Times. Sect. A. P. 2.
Krauss C. 2003 (April 26). The SARS epidemic: Toronto; Canada increases pressure on World Health Organization to lift travel advisory. New York Times. Sect. A. P. 8.
Longini IM Jr, Halloran ME, Nizam A, Yang Y. 2004. Containing pandemic influenza with antiviral agents. Am J Epidemiol 159(7):623–633.
McBean AM, Babish JD, Warren JL. 1993. The impact and cost of influenza in the elderly. Arch Intern Med 153:2105–2111.
Mullooly JP, Barker WH. 1982. Impact of type A influenza on children: A retrospective study. Am J Public Health 72:1008–1016.
Neustadt RE, Fineberg HV. 1978. The swine flu affair: Decision making on a slippery disease. Washington, DC: U.S. Department of Health, Education, and Welfare.
Neustadt R, Fineberg HV. 1983. The Epidemic That Never Was: Policy Making in the Swine Flu Scare. 1st ed. New York: Vintage Books.
Office of Technology Assessment, U.S. Congress. 1981. Cost Effectiveness of Influenza Vaccination. Washington, DC: Government Printing Office.
Patriarca PA, Cox NJ. 1997. Influenza pandemic preparedness plan for the United States. J Infect Dis 176(Suppl 1):S4–S7.
Patriarca PA, Arden NH, Koplan JP, Goodman RA. 1987. Prevention and control of type A influenza infections in nursing homes: Benefits and costs of four approaches using vaccination and amantadine. Ann Intern Med 107:732–740.
Riddiough MA, Sisk JE, Bell JC. 1983. Influenza vaccination: Cost-effectiveness and public policy. JAMA 249:3189–3195.
Roberts S. 2003. Communicating with the public about public health preparedness. In: DIMACS Working Group on Modeling Social Responses to Bioterrorism Involving Infectious Agents. New Brunswick, NJ: Rutgers University.
Robinson LJ, Barry PJ. 1987. The Competitive Firm’s Response to Risk. New York: Macmillan.
Rosenberg CE. 1989. What is an epidemic?: AIDS in historical perspective. Daedalus 118(2):1–17.
Sandman PM. 1993. Responding to Community Outrage: Strategies for Effective Risk Communication. Fairfax, VA: American Industrial Hygiene Association.
Sandman PM, Lanard J. 2004 (October 22). Flu Vaccine Shortages: Segmenting the Audience. [Online]. Available: http://psandman.com/col/flu-1.htm.
Sapsin JW, Thompson TM, Stone L, DeLand KE. 2003. International trade, law, and public health advocacy. J Law Med Ethics 31(4):546–556.
Schoch-Spana M. 2003. Educating, informing, and mobilizing the public. In: Levy BS, Sidel VW, eds. Terrorism and Public Health. New York: Oxford University Press. Pp. 118–135.
Schoenbaum SC. 1987. Economic impact of influenza: The individual’s perspective. Am J Med 82(Suppl 6A):26–30.
Schoenbaum SC, McNeil BJ, Kavet J. 1976. The swine-influenza decision. N Eng J Med 295:759–765.
Serfling RE, Sherman IL, Houseworth WJ. 1967. Excess pneumonia-influenza mortality by age and sex in three major influenza A2 epidemics, United States, 1957–58, 1960 and 1963. Am J Epidemiol 86:433–441.
Simonsen L, Clarke MJ, Williamson GD, Stroup DF, Arden NH, Schonberger LB. 1997. The impact of influenza epidemics on mortality: Introducing a severity index. Am J Public Health 87:1944–1950.
Simonsen L, Clarke MJ, Schonberger LB, Arden NH, Cox NJ, Fukuda K. 1998. Pandemic versus epidemic influenza mortality: A pattern of changing age distribution. J Infect Dis 178:53–60.
Siracusa principles on the limitation and derogation provisions in the International Covenant on Civil and Political Rights. 1985. Hum Rights Q 7(1):3.
Sorenson J. 2004. Commentary: Risk communication and terrorism. Biosecurity and Bioterrorism 2(3):229–231.
Spier RE. 2001. Perception of risk of vaccine adverse events: A historical perspective. Vaccine 20(Suppl 1):S78–S84.
Stevens J, Corper AL, Basler CF, Taubenberger JK, Palese P, Wilson IA. 2004. Structure of the uncleaved human H1 hemagglutinin from the extinct 1918 influenza virus. Science 303(5665):1866–1870.
Stöhr K. 2004 (June 16). WHO: Priority Public Health Interventions Before and During Influenza Pandemics. Prepared for Institute of Medicine Workshop on Pandemic Influenza: Assessing Capabilities for Prevention and Response, Washington, DC: Institute of Medicine Forum on Microbial Threats.
The Federal Register. 1996. 61(170):46301–46302.
Thomas P. 2003. The Anthrax Attacks. Washington, DC: The Century Foundation. [Online]. Available: http://www.homelandsec.org/WGneed/CaseStudies/full.pdf [accessed August 6, 2003].
U.S. Bureau of the Census. 1997. Statistical Abstract of the United States: 1997. 117th ed. Washington, DC: U.S. Bureau of the Census.
U.S. Department of Health and Human Services. 2002. Communicating in a Crisis: Risk Communication Guidelines for Public Officials. Washington, DC: U.S. Department of Health and Human Services.
Webby RJ, Webster RG. 2003. Are we ready for pandemic influenza? Science 302(5650): 1519–1522.
Weinstein RA. 2004. Planning for epidemics: The lessons of SARS. N Engl J Med 350(23): 2332–2334.
WHO (World Health Organization). 2004a. WHO Consultation on Priority Public Health Interventions Before and During an Influenza Pandemic. Geneva, Switzerland: WHO.
WHO. 2004b. Intergovernmental Working Group on the Revision of the International Health Regulations. Working paper for regional consultations. IGWG/IHR/working paper 12.2003. Geneva, Switzerland: WHO.
WHO Secretariat. 2004. Revision of the International Health Regulations. Publication EB113/ 3 Rev.1. Geneva, Switzerland: WHO.
Working Group on Governance Dilemmas in Bioterrorism Response. 2004. Leading during bioattacks and epidemics with the public’s trust and help. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 2(1):25–40.


























































