7
Integration of CAM and Conventional Medicine
A distinct trend toward the integration of complementary and alternative medicine (CAM) therapies with the practice of conventional medicine is occuring. Hospitals are offering CAM therapies, health maintenance organizations (HMOs) are covering such therapies, a growing number of physicians use CAM therapies in their practices, insurance coverage for CAM therapies is increasing, and integrative medicine centers and clinics are being established, many with close ties to medical schools and teaching hospitals. How does a new therapy move from the idea stage to the practice stage? What is the extent of integration of CAM and conventional medicine? Why is such integration occurring? What approaches are being used to offer integrated services? This chapter explores these and other questions related to the integration of CAM and conventional medicine.
FROM IDEA TO PRACTICE
Ideally, conventional medical tests and treatments go through a series of scientific challenges that, if met, allow the test or the treatment to become part of conventional medical practice. However, there are and there always will be exceptions. As noted in Chapter 4, some new practices offer dramatic and evident benefits that may justifiably hasten their acceptance. Sometimes, enthusiasm for the intervention, founded on the plausibility of the benefits and the absence of satisfactory alternatives, speeds acceptance, despite a dearth of evidence (e.g., screening for and treatment of prostate cancer).
Because the emphasis on evidence-based decision making is relatively
new, many current conventional medical practices did not follow what is now considered to be the normative pathway of translation because they became accepted practice before this pathway was fully established. Many practices that are widely accepted, however, continue to undergo scrutiny, and their indications often change as research identifies those patients who benefit the most from them. An example is coronary bypass surgery which became accepted treatment before undergoing controlled clinical trials. The evident effectiveness of coronary bypass surgery in reducing symptoms of stable angina fostered great enthusiasm for the procedure, with many clinicians assuming that its effectiveness would be similar in reducing the risks of heart attack and death because of coronary disease. When bypass surgery was already well established, a number of RCTs showed that it improved the life expectancies of patients with severe coronary artery disease but had little effect on patients with mild disease. In addition, it had no effect on heart attack rates. Similarly, patients with acute coronary syndromes that threatened to evolve into myocardial infarction received percutaneous coronary interventions long before RCTs showed that this strategy was superior (by a small margin) to thrombolysis with drugs.
In this idea pathway, the acceptance of new interventions in clinical practice depends on a cycle (Figure 7-1) that begins with a creative idea derived from either an advance in science or a clinical observation. That creative insight is the basis for hypotheses about treatment effectiveness. Hypotheses are tested through a series of evaluation steps before they are accepted, first by early adopters and then more widely. As acceptance grows, a number of forces shape the level of integration of the intervention into clinical practice. These forces may include difficulty in acquiring technical skills, the supply of practitioners or the capacity to deliver the intervention, and coverage decisions made by health plans and other payers. Patient demand for services also affects acceptance and integration. Patient demand is influenced by evidence of effectiveness, but it is also influenced
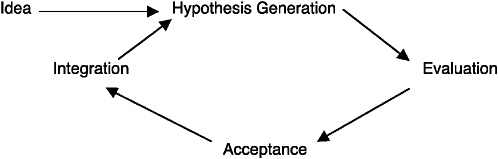
FIGURE 7-1 Translation: from idea to practice.
by individual experience with the treatment and the presence or absence of satisfactory alternatives. After its acceptance, ongoing questioning of the value of an intervention relative to those of other new and established interventions is necessary to refine clinical practice and generate new creative ideas that lead to further clinical advances.
The number of steps or challenges has increased over the past several decades. The process will evolve further, and as the nation looks forward to a health care system in which conventional practice and CAM coexist in close harmony, these processes will apply to new tests and treatments from both the traditions of practice. Several factors are noteworthy, however. First, the series of steps represents a logical progression; however, the process is not uniformly followed in conventional medicine. Second, most existing CAM therapies already exist in practice; that is, patients are using these therapies. This means that the cycle must begin at the integration step so that studies can be carried out to evaluate the therapies already in use. Third, new measures and methods must be developed to adequately reflect patients’ experiences with CAM as well as the outcomes most relevant to current users. For therapies that are not well supported by empirical evidence, studies addressing general questions of treatment effectiveness may be most appropriate. For therapies that are well supported, studies that address the underlying mechanisms of action, that identify subgroups of patients in whom the treatment works more or less well, or that test modifications to a general approach to treatment may be appropriate. These steps are not linear; a therapy may be involved in activities at several steps simultaneously, and adoption into practice does not terminate the process. Indeed, the evaluation process continues as new information about a therapy is generated. Given these caveats, a more in-depth exploration of the conceptual model for translation from idea to practice is provided below.
Hypothesis Generation
As noted in Figure 7-1, the first step in the translation process is the generation of an idea. All accepted clinical practices were once just a good idea. The creative insight may have come from a practitioner, a researcher, or even a patient. It may have been derived from an advance in science or from recognition of an unmet clinical need. In any case, once a good idea has become a new treatment, it must be tested.
Evaluation
Once ideas have been generated, they must pass through several stages of evaluation. First, it is necessary to decide which interventions should have priority for evaluation and which types of research designs are best
for those evaluations. In effect, research committees at drug companies and National Institutes of Health study sections perform this function by deciding which proposals shall receive funding. The committee suggests that the following criteria (also discussed in Chapter 4) be used when CAM interventions are considered for testing. Clearly, no intervention will meet all criteria, and a therapy should not be excluded from consideration because it does not meet any one particular criterion, for example, biological plausibility.
-
A biologically plausible mechanism exists for the intervention, with recognition that the science base on which plausibility is judged is a work in progress.
-
Research could plausibly lead to the discovery of biological mechanisms of disease or treatment effect.
-
The condition is highly prevalent (e.g., diabetes mellitus).
-
The condition causes a heavy burden of suffering.
-
The potential benefit is great.
-
Some evidence already exists that the intervention is effective.
-
Some evidence that there are safety concerns exists.
-
The research design is feasible and likely to yield an unambiguous result.
-
The target condition or the intervention is important enough to have been detected by existing population surveillance mechanisms.
Next in the evaluation part of the cycle is the conduct of preliminary studies to establish feasibility. One example of this process is the Phase I and Phase II trials required by the Food and Drug Administration for new drugs. These studies evaluate whether the intervention does what it claims to and characterizes adverse effects.
If the intervention meets the challenges imposed by the Phase I and II trials, it becomes a candidate for adoption as a medical practice and moves to the next challenge: clinical trials to test its effects with larger numbers of patients.
Acceptance
Several things happen during the acceptance phase of the translation cycle. Once research results are available, dissemination begins. Researchers publish their findings in peer-reviewed journals and make presentations at scientific meetings. This step requires a careful peer-review process and competent researchers to evaluate the evidence and recommend the findings for publication or presentation. The articles may be published in CAM-related journals (e.g., Journal of Complementary and Alternative Medicine)
and journals that focus on conventional medicine (e.g., Annals of Internal Medicine and New England Journal of Medicine). Various professional organizations hold scientific sessions at which the investigators present the research results.
After much clinical testing, the accumulating body of evidence provides a basis for strong conclusions about efficacy and effectiveness. At this point, experts on evidence evaluation perform systematic reviews and meta-analyses to estimate the size of the effect of the intervention. These research syntheses form the basis of the next steps. Many syntheses of research on CAM appear, for example, in the Cochrane Collaboration reviews, discussed in Chapter 5.
During the acceptance portion of the cycle, professional organizations and clinical practices also create guidelines to best practices. The American College of Physicians and Kaiser-Permanente are among the organizations that develop guidelines that describe a professional consensus, and these are nearly always based on syntheses of the evidence about best practices.
Payers then decide on coverage policy. Coverage policy is important to the adoption of new tests and treatments, although many patients pay out of pocket for CAM services that payers do not cover. Evaluations may be conducted by an internal group or through a contract with an outside agency. Although the coverage decision is science based (which means that it draws on the findings presented in published studies), it may also be negotiated by providers and major purchasers.
Integration
Once an intervention becomes available for general clinical use, it becomes subject to a process that encourages the adoption of knowledge-based therapies. Factors influencing the adoption of the intervention include use by influential practitioners in the community, ease of use, drug company and device manufacturer sales representatives, advertisements in medical journals, advertisements on television and in other media, presentations and booths at professional meetings, and continuing education events. A more ill-defined process leads to the discarding of technologies that had become established before testing but that fell short of their initial promise when they were subjected to careful clinical testing.
Clinical organizations, often at the behest of payers, develop processes to encourage practitioners to follow best practices. Payers and other organizations create incentives for clinical practitioners to follow best practices and hold them accountable. Once a therapy has been accepted into practice, the cycle does not terminate. As new information is accumulated through practice and additional research, the therapy may be reevaluated.
This conceptual model of how new ideas for interventions move into
practice also applies to the integration of CAM and conventional medical therapies, in which many CAM therapies that are new to conventional medicine are being accepted by conventional medical practicioners or integrated into conventional practices. Osteopathic medicine is an example of a discipline that developed separately from conventional medicine, moved through the stages of translation from idea to practice, and is fully accepted as an effective treatment modality. Whorton (2002) describes how Andrew Taylor Still, a frontier physician, founded osteopathy. Still’s point of departure for his new system was his view of the body as a machine which should function well if it were mechanically sound. His system was designed to improve health by treating the patient as a whole through improving the circulation and correcting abnormal mechanics. He condemned the prevalent use of drugs by medical practitioners.
In 1892 the first osteopathic school was opened (the American School of Osteopathy), offering training in manipulation as well as classroom instruction in anatomy. Despite resistance by conventional medicine, in 1896 Vermont became the first state to license osteopaths. By the 1920s forty states licensed osteopaths to practice, although it was not until 1973 that osteopathy was licensed in all states.
Some in the osteopathic community argue that osteopathy grew out of a separate tradition, that it has maintained its distinctiveness, and that it should not be considered congruent with conventional medicine. Those who maintain that osteopathy remains a distinct system cite two main reasons: a holistic approach with a focus on preventive care and the “use of osteopathic manipulation as part of the overall therapeutic approach” (Howell, 1999). Others believe that the similarities of osteopathic medicine with conventional medicine greatly outweigh any differences. “Overall, osteopathic medical schools have come to resemble allopathic medical schools in most respects; some students even share classes” (Howell, 1999).
Whether or not osteopathy remains a unique approach to medicine, it has come to be recognized as an effective approach to treatment.
The next section explores trends in the integration of CAM and conventional medicine.
GROWING INTEGRATION OF CAM
In 1998, the American Hospital Association began collecting in its annual survey information about hospitals that offer CAM services and found that only 6 percent of hospitals reported that they offered such CAM services. By 2001, the number of hospitals offering CAM therapies had more than doubled to 15 percent “indicating a steadily growing interest by hospitals to enter into this arena” (Ananth, 2002). HMOs are also increasingly interested in offering CAM therapies. In 1997, Landmark Healthcare,
Inc., commissioned a survey of HMO use of CAM therapies. One hundred fourteen HMOs were surveyed between November 1998 and January 1999, which was 25 percent of all HMOs in existence at the time of the survey. The results showed that two-thirds of HMOs (67 percent) offered at least one form of alternative care, the most common being chiropractic (65 percent) and acupuncture (31 percent) (Landmark Healthcare, Inc., 1999).
Cancer treatment centers also frequently use CAM therapies. Three such programs are briefly described here. The Memorial Sloan-Kettering Cancer Center has developed an Integrative Medicine Service that offers inpatients music therapy, massage therapies and reflexology, and mind-body therapies. Outpatient services include “massage, acupuncture, reflexology, meditation, self-hypnosis and other mind-body therapies, music and sound therapies, and counseling in nutrition and herb-drug issues, as well as classes in yoga, tai chi, chair aerobics, the Alexander technique, Pilates mat, etc.” (Cassileth, 2002).
The University of Texas M.D. Anderson Cancer Center supports an integrative medicine program that incorporates research, education, and a clinical program. That facility, called “Place … of wellness,” opened in 1998. “Place … of wellness offers more than 75 complementary therapy program opportunities, free of charge, to help with the non-medical issues of living with cancer. It is a bridge between standard medical care and spiritual healing that we call complementary and integrative medicine” (M.D. Anderson Cancer Center, 2004). Therapies include mind-body approaches such as guided imagery and progressive relaxation; physical therapies such as yoga, tai chi, massage, and acupuncture; and nutritional support.
The Dana-Farber Cancer Institute has established the Zakim Center for Integrated Therapies. The center defines integrated therapies as “individual treatments that are used in addition to (or as a complement to) traditional cancer treatment such as chemotherapy and radiation” (Dana-Farber Cancer Institute, 2004). Therapies include massage therapy, acupuncture, and nutritional guidance. The center’s website states, “When patients integrate these therapies into their medical and surgical care, they are creating a more comprehensive treatment plan and helping their own bodies to regain health and vitality” (Dana-Farber Cancer Institute, 2004).
In addition, a nonprofit organization of health professionals, the Society for Integrative Oncology (SIO), was created in 2003 to provide “a convenient forum for presentation, discussion, and peer review of evidence-based research and treatment modalities in the discipline known as integrative medicine” in cancer care. (SIO, 2004).
Use of CAM by Conventional Practitioners
Several efforts have been made to examine the extent to which CAM services are being incorporated into physicians’ practices. Berman and colleagues (1995) surveyed physicians’ attitudes toward CAM and found a high interest in such services. Furthermore, they found that some therapies were already being used by the responding physicians. Of the 180 respondents, more than 90 percent considered legitimate medical practices to include diet and exercise, behavioral medicine, biofeedback, and counseling or psychotherapy. In addition 50 percent believed that acupuncture, massage therapy, and hypnotherapy were legitimate medical practices. Blumberg et al. (1995) surveyed primary care internists and board-certified family physicians and found that of the 572 respondents, more than half would “encourage patients who raise the possibility” of using CAM. Furthermore, 57 percent indicated they would refer their patients for treatment.
Gordon and colleagues (1998) surveyed adult primary-care physicians and obstetrics-gynecology physicians and nurse practitioners from a large northern California HMO. During the 12 months before the survey, “90 percent of adult primary care physicians and obstetrics-gynecology clinicians recommended at least one alternative therapy.” Table 7-1 provides the percentages by type of therapy.
Another survey by Berman and colleagues (1998) found that almost 20 percent of the physicians had used in their practice 9 of the therapies listed in Table 7-2 and that one-third or more were open to using 17 of them. Table 7-2 displays the percentage of physicians who have incorporated various CAM modalities or who would do so.
A review of the literature by Astin et al. (1998) found that “large numbers of physicians are either referring to or practicing some of the more prominent and well-known forms of CAM and that many physicians believe that these therapies are useful or efficacious.” Analysis across surveys revealed that the rates of physician referral were 43 percent for acupuncture, 40 percent for chiropractic, and 21 percent for massage, with about half of the physicians indicating belief in the efficacies of these therapies. For homeopathy and herbal approaches, 26 and 23 percent of physicians, respectively, believed in the efficaces of these therapies.
In recognition of the growing use of CAM therapies by individual conventional medical practitioners, the Federation of State Medical Boards of the United States developed Model Guidelines for the Use of Complementary and Alternative Therapies in Medical Practice. The guidelines focus on “encouraging the medical community to adopt consistent standards, ensuring the public health and safety by facilitating the proper and effective use of both conventional and CAM treatments, while educating physicians
TABLE 7-1 Alternative Therapies Being Used or Recommended by Adult Primary-Care and Obstetrics-Gynecology Clinicians for Patient Care
|
Alternative Therapy |
Percentage of Adult Primary-Care Clinicians (n = 624) |
Percentage of Obstetrics-Gynecology Clinicians (n = 157) |
|
Manipulation therapies |
72.9 |
68.1 |
|
Chiropractic |
33.6 |
37.6 |
|
Osteopathy |
5.1 |
5.7 |
|
Acupuncture |
57.2 |
42.7 |
|
Acupressure |
30.9 |
30.6 |
|
Massage therapy |
42.5 |
44.6 |
|
Body work |
7.5 |
12.1 |
|
Ingested therapiesa |
29.5 |
54.1 |
|
Herbal or botanical medicine |
8.8 |
29.3 |
|
Homeopathic medicine |
2.7 |
9.5 |
|
Special diet |
18.3 |
28.0 |
|
Megadoses of vitamins, etc. |
8.3 |
21.7 |
|
Mind-body therapies |
74.8 |
70.7 |
|
Meditation, mindfulness |
48.9 |
45.8 |
|
Relaxation techniques |
67.6 |
63.7 |
|
Guided imagery, visualization |
16.7 |
22.9 |
|
Biofeedback |
31.9 |
22.9 |
|
Hypnosis, self-hypnosis |
11.5 |
14.0 |
|
Movement therapies |
27.7 |
26.1 |
|
Yoga |
19.5 |
22.9 |
|
Tai chi, chi gong |
17.9 |
10.2 |
|
Supportive therapies |
84.9 |
80.2 |
|
Religious healing or prayer |
13.6 |
12.7 |
|
12-step program, support group |
58.0 |
48.4 |
|
Psychological counseling |
78.7 |
77.1 |
|
aMany of the clinicians who indicated that they used or recommended a special diet described the type only as “low fat” or “low sodium.” Thus, the prevalence reported for this modality is likely inflated by providers who recommended more conventional diets for patients with heart disease, diabetes mellitus, or hypertension. Excluding special diet, the proportions of clinicians who reported that they recommended ingested therapies are 16.3 percent for adult primary-care physicians and 42.0 percent for obstetrics-gynecology clinicians. SOURCE: Gordon et al. (1998). |
||
on the adequate safeguards needed to assure these services are provided within the bounds of acceptable professional practice” (FSMB, 2002).
Nurses also use CAM therapies in their practices. Sparber (2001) presented the results of an investigation of State Boards of Nursing (BONs) positions on nurses’ practice of CAM therapies and found that 47 percent
TABLE 7-2 Percentage of Physicians Who Have Used or Who Would Use CAM Practices, by Specialty (n = 783)
|
Practice |
Total Sample |
Total |
Pediatrics |
Internal Medicine |
Family and General Practice |
|
|
Have Used |
Would Use |
|||||
|
Diet, exercise |
92.3 |
6.5 |
98.8 |
98.9 |
99.1 |
98.4 |
|
Counseling, psychotherapy |
71.2 |
24.5 |
95.7 |
96.1 |
94.8 |
96.1 |
|
Behavioral medicine |
47.3 |
43.8 |
91.1 |
92.6 |
91.5 |
92.5 |
|
Biofeedback, relaxation |
44.1 |
47.6 |
92.7 |
92.1 |
91.5 |
92.5 |
|
Massage, therapeutic touch |
33.7 |
30.9 |
64.6 |
51.7 |
62.5 |
72.5 |
|
Prayer, spiritual direction |
29.2 |
32.4 |
61.6 |
57.6 |
59.9 |
65.1 |
|
Vegetarianism |
24.0 |
39.0 |
63.0 |
55.1 |
63.8 |
66.9 |
|
Meditation |
24.0 |
42.8 |
66.8 |
57.6 |
65.1 |
73.2 |
|
Hypnotherapy |
19.9 |
48.0 |
67.9 |
62.9 |
65.7 |
71.2 |
|
Chiropractic |
19.2 |
29.0 |
48.2 |
32.9 |
50.6 |
54.5 |
|
Megavitamin |
16.2 |
21.3 |
37.5 |
18.9 |
38.7 |
45.9 |
|
Acupuncture |
11.7 |
48.7 |
60.4 |
47.7 |
68.9 |
60.7 |
|
Acupressure |
10.1 |
36.5 |
46.6 |
30.1 |
44.6 |
56.6 |
|
Herbal medicine |
8.2 |
34.3 |
42.5 |
34.2 |
43.6 |
46.1 |
|
Homeopathic medicine |
5.9 |
27.9 |
33.8 |
26.3 |
29.4 |
41.2 |
|
Art therapy |
5.0 |
39.5 |
44.5 |
44.6 |
42.8 |
44.5 |
|
Electromagnetic applications |
3.8 |
20.6 |
24.4 |
18.2 |
21.9 |
27.2 |
|
Native American medicine |
2.8 |
29.8 |
32.6 |
26.4 |
33.9 |
34.9 |
|
Traditional Oriental medicine |
2.4 |
33.5 |
35.9 |
29.4 |
38.1 |
37.6 |
|
SOURCE: Adapted from Berman et al. (1998). |
||||||
of the BONs permitted nurses to practice a range of CAM therapies and an additional 13 percent were in the process of discussing whether to allow nurses to perform such therapies. The Minnesota Board of Nursing has developed a statement of accountability with several specific points on the use of CAM in nursing. The document states, “[N]urses who employ integrative therapies in their nursing practice to meeting nursing and patient goals developed through the nursing process are held to the same accountability for reasonable skill and safety as they are with the implementation of conventional treatment modalities”(Minnesota Board of Nursing, 2003). The Gillette Nursing Summit, held in May 2002, was convened to “identify common concerns and a set of core recommendations that would enable nurses to provide leadership in this emerging field” of integrated health and healing (Kreitzer and Disch, 2003) and resulted in the development of recommendations related to integrated health care in the areas of research, education, clinical care, and policy. Tracy et al. (2003) evaluated nurses’ attitudes toward CAM use in critical care and found that nurses are open to the use of CAM therapies, with many already incorporating CAM therapies into their own practices. Kreitzer et al. (2002) questioned medicine, nursing, and pharmacy faculty and students at the University of Minnesota and found that “more than half of the medical and nursing faculty either would personally provide or refer a CAM practitioner for acupuncture, biofeedback, chiropractic, hypnosis or guided imagery, massage, and meditation…. Pharmacy faculty were less likely to provide CAM therapies or refer [a patient] to a CAM practitioner, though more than 50 percent would do so for herbal medicine and nutritional supplements and more than 40 percent for acupuncture, chiropractic, massage, or prayer or spiritual healing.”
Reimbursement for CAM Services
Coverage of CAM services is an important issue for the integration of conventional medicine and CAM. In 1999 a study examining insurance coverage of CAM services was conducted in New York, New Jersey, and Connecticut. “Virtually all of the insurance carriers in the survey cover chiropractic services in some form,” almost 40 percent (17 of 43) cover acupuncture, and 37 percent (16 of 43) cover massage therapy (Cleary-Guida et al., 2001). Weeks (1999) found that although the extent of CAM integration into benefit designs in early 1999 was “extremely limited,” most national plans either had a CAM product or a CAM strategy team. The different coverage options identified by Weeks appear in Table 7-3.
Weeks (2001) concluded in another article that “The dominant trend during 1998 to 2000 … was a conservative move to offer CAM through discounted, value-added affinity programs. When plans actually cover CAM
TABLE 7-3 CAM Coverage Offered by Some Insurance Policies
|
Insurance plans offer different levels or types of coverage for CAM services: Offer CAM, but only subsequent to a state mandate, and therefore without any internal, proactive process Include direct access to numerous CAM services, but only for workers’ compensation claims Have CAM services, but in only one or two of perhaps two dozen distinct insurance or HMO “products” that it offers to purchasers Promote a CAM program, but only to its group purchasers and not to individuals Administer an insurance policy for a self-insured company that has some CAM coverage, but the plan does not offer the coverage Allow conventional medical providers to offer certain CAM therapies but not cover those services when they are provided by members of distinct CAM professions Have an offering for which the purchaser must pay more (rider) and that is outsourced to a CAM network but has little to no internal expertise in CAM Create a program that allows members to access CAM services on a discounted basis but not as a covered benefit Cover a certain provider category, such as chiropractor, for only very limited conditions, such as low back pain |
|
SOURCE: Weeks (1999). |
services, most do so as an added benefit contracted by employers or groups through insurance riders with services provided at an added cost and through credentialed networks of practitioners.” In this context, it is noteworthy that Wolsko et al. (2002) found that the extent of insurance coverage for CAM providers and the use of CAM therapies for wellness are strong correlates of the frequent use of CAM providers. Furthermore, about 8.9 percent of the U.S. population was responsible for more than 75 percent of the visits to CAM providers.
It should be noted that not all CAM practitioners are convinced that insurance coverage is positive for the future practice of complementary and alternative medicine. Cleary-Guida et al. (2001) cautioned that “the consequences of including CAM services in health insurance plans are unknown and require careful consideration.” One concern is whether the quality of and levels of reimbursement for CAM services will deteriorate once they are covered by health insurance and subjected to the limitations imposed by carriers or the restrictions of managed care organizations. Other practitioners believe that CAM “will never fulfill its promise if it cannot be delivered via direct pay insurance” (Clohesy Consulting, 2003). Between these extremes are those who believe that it is possible to maintain the desire of integrative medicine for a system of relationship-based care yet also for CAM services to qualify for insurance reimbursement.
The data presented above indicate that hospitals, managed care organizations, and conventional practitioners have incorporated some CAM therapies into the provision of health care services. The next section discusses what is known about the reasons for integration of CAM and conventional medicine.
WHY IS INTEGRATION OCCURRING?
The reasons why individuals choose to use CAM therapies were explored in Chapter 2. Although few studies have focused on why health care institutions and practioners are incorporating CAM therapies, this section examines the available evidence about why institutions and practitioners (both conventional medicine and CAM) are moving toward integrated care.
The American Hospital Association survey of hospitals found that 49 percent of respondents indicated that patient demand was the primary motivation for offering CAM services, whereas another 24 percent stated that offering these services reflected their organizational mission. Survey respondents stated other motivators for offering CAM: clinical effectiveness (45 percent), attracting new patients (41 percent), and differentiation from competitors (36 percent). Major obstacles to implementing successful CAM programs included physician resistance (63 percent), budgetary constraints (52 percent), lack of internal expertise (39 percent), and credentialing of providers (33 percent). The survey also found that the principal form of payment for hospital-based CAM services is patient selfpay (76 percent) (Ananth, 2002).
In the Landmark Healthcare, Inc. (1999) survey of HMOs, the respondents indicated that their reasons for offering alternative care were market, employer, or consumer demand (71 percent); the effectiveness of the therapies (29 percent); or state mandates or legal requirements (29 percent). The most important factors that HMOs take into account when they evaluate CAM providers are quality of care, the credentials and qualifications of the providers, and price competitiveness (Landmark Healthcare, Inc., 1999).
As part of a literature review and survey designed to determine which insurers had special policies for CAM coverage and which hospitals were offering CAM, Pelletier et al. (1997) determined that “consumer demand for CAM is motivating more insurers and hospitals to assess the benefits of incorporating CAM.” Follow-up studies in 1998 and 1999 produced similar results. Weeks (1999) examined the forces shaping CAM coverage, the extent of coverage offered by insurers and health care plans, and models for inclusion or coverage and found that key motivators for CAM inclusion are “mission, marketplace, mandates, and medicine.”
Few studies have specifically focused on why physicians are increasingly interested in and positive about CAM. Some evidence, indicates, how-
ever, that physicians want to know more about CAM to better “keep up with their patients’ growing interest in and use of CAM” (Ruggie, 2004). Corbin Winslow and Shapiro (2002) found that 84 percent of physicians thought that they needed to learn more about CAM. The strongest reason for this was so that they could better communicate with their patients about the use of CAM. In addition, physician recommendation of CAM (48 percent) was most strongly associated with physician CAM self-use, with physicians who used one or more CAM therapies being seven times more likely to recommend CAM to their patients.
Sikand and Laken (1998) found that sex, ethnicity, practice type, and location of medical training have a significant effect on pediatricians’ attitudes toward CAM therapies. Female physicians were found to have more favorable attitudes toward CAM than male physicians, and white physicians where found to have more favorable attitudes than physicians of color. Graduates of U.S. medical schools also had more favorable attitudes toward CAM than their foreign-born or -trained physicians. Blumberg et al. (1995) found that physician involvement in CAM was likely to be higher among younger or female physicians, physicians practicing in the western United States, and family practitioners than among the internists surveyed.
Some hypothesize that conventional medical practitioners are incorporating CAM because of frustrations with the constraints of practice, such as a lack of time necessary for a meaningful patient-practitioner interaction or a loss of autonomy in practice (Snyderman and Weil, 2002). Others suggest that some practitioners, frustrated with a lack of interventions to reduce the effects of chronic conditions (reported to be the leading cause of illness, disability, and death [IOM, 2001]), may be turning to CAM therapies that emphasize prevention and wellness.
Few would argue against the notion that health care practitioners desire to provide the best care for their patients. Some restrict the definition of “best care” to those therapies found in conventional medicine; however, the growing body of evidence demonstrating that some CAM therapies are safe and effective is likely to be a factor contributing to the increased use of CAM by both health care practitioners and health care institutions. Such incorporation is often referred to as integrative medicine. The next section explores the emerging approach to health care frequently called integrative medicine.
INTEGRATIVE MEDICINE
Integrative medicine is described as more than just the sum of conventional medicine plus CAM. Maizes et al. (2002) defines integrative medicine as “healing-oriented medicine that reemphasizes the relationship between patient and physician, and integrates the best of complementary and
alternative medicine with the best of conventional medicine.” Berndtson (1998) defines the term somewhat similarly, placing emphasis on use of evidence. He writes “integrative medicine refers to a clinical approach that combines the strengths of conventional and alternative medicine with a bias toward options that are considered safe, and which, upon review of the available evidence, offer a reasonable expectation of benefit to the patient.”
According to Snyderman and Weil (2002), integrative medicine is a movement, driven by consumers, which is attracting the attention of academic health centers. They write that the focus of integrative medicine is on health and healing and agree with Maizes that the patient-physician relationship is key. They further state, “integrative medicine focuses on preventive maintenance of health by paying attention to all relative components of lifestyle, including diet, exercise, stress management, and emotional well-being. It insists on patients being active participants in their health care as well as on physicians viewing patients as whole persons—minds, community members, and spiritual beings, as well as physical bodies. Finally, it asks physicians to serve as guides, role models, and mentors, as well as dispensers of therapeutic aids.”
Hess (2002) views integration as a process that involves a spectrum of options. In his view, at one end of the spectrum (strong integration), patients, under the care of a qualified health professional, are allowed to replace conventional therapies with other options. “At the ‘weak’ end of the integration spectrum, choices are mostly adjuvant to conventional therapeutic packages…. The difference corresponds roughly to the tradeoff in medical ethics between autonomy and paternalism.”
Integrative medicine may also be a response to the growing recognition of health professionals that many factors contribute to the health of individuals and the public. Why some people are healthy and others are not has to do “not only with disease and illness, but also with who we are, where we live and work, and the social and economic policies of our government” (IOM, 2003b). This statement reflects the evolution in thinking about health and its determinants that has occurred over the past 50 years. Until about the middle of the twentieth century, health was measured using negative indicators, e.g., mortality and disease rates. Populations with higher mortality rates were considered less healthy than those with lower rates. Such rates continue to be broad indicators of the health of a society.
Efforts to redefine health in the 1950s, however, were spurred by the World Health Organization view of health as “a state of complete physical, mental, and social well being, and not merely the absence of disease or infirmity” (WHO, 1948). This broadened view of what constitutes health led to a rethinking about the determinants of health and how to measure those determinants. According to Bausell and Berman, Engel argued that the context in which the patient operates must be taken into account, that
is, a biological, sociological, and psychological model of health should be used (Bausell and Berman, 2002). Lalonde (1974) described a framework of determinants that included environment, lifestyle, human biology, medical care, and health care organization. Evans and Stoddart (1994) developed a more complex model that distinguished among disease, health, functioning, and well-being, arguing that both behavioral and biological responses to the social and physical environments should be included in the understanding of what contributes to health or the lack thereof. A 1999 Institute of Medicine (IOM) report described a model of determinants that showed how individual characteristics and environmental characteristics influence health-related quality of life.
Two recent IOM reports (2003a,b) encourage the use of an ecological model of health, that is, a model of health that emphasizes the linkages and relationships among multiple factors (or determinants) affecting health (Figure 7-2). “An ecological model assumes that health and well being are affected by interaction among multiple determinants including biology, behavior, and the environment” (IOM, 2003b). The report also states that “an ecological approach to health is one in which multiple strategies are developed to impact determinants of health relevant to the desired health outcomes.” This ecological approach has some similarities to what CAM practitioners refer to as a holistic approach to care.
According to Tauber (2002, p.185), holism was first defined in 1926 by Jan Smuts in a publication called Evolution and Holism. As applied to medicine, holism “refers not only to the relational character of medical description and therapy but to the scope of the medical gaze.” Ruggie (2004) reports that in the 1970s the word holistic referred to health care practices based on the interconnectedness of mind and body. Bausell and Berman (2002), reporting on a study by Barrett et al. (2000), describe holism as representing “a belief in the importance of basing treatment upon people as whole individuals, of taking a multidimensional view of illness, and of trying to get to the heart of the problem rather than simply treating symptoms.”
The key point in all these definitions is similar to the idea of the ecological approach, that is, multiple factors influence the health of an individual, and health care practitioners should consider each of these factors in attempting to understand and improve health.
As discussed earlier in this chapter, the level of integration of conventional and CAM therapies is growing. That growth generates the need for tools or frameworks to make decisions about which therapies should be provided or recommended, about which CAM providers to whom conventional medical providers might refer patients, and the organizational structure to be used for the delivery of integrated care. The committee believes that the overarching rubric that should be used to guide the development of
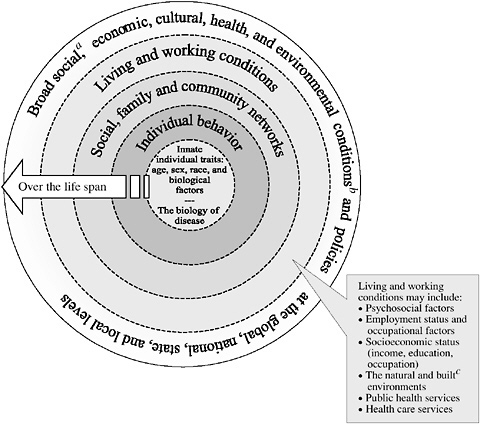
FIGURE 7-2 A guide to thinking about the determinants of population health.
NOTE: The dotted lines between the different levels of the model denote interaction effects between and among the various levels of health determinants (Worthman, 1999). aSocial conditions include, but are not limited to, economic inequality, urbanization, mobility, cultural values, attitudes, and policies related to discrimination and intolerance on the basis or race, gender, and other differences. bOther conditions at the national level might include major sociopolitical shifts, such as recession, war, and governmental collapse. cThe built environment includes transportation, water and sanitation, housing, and other dimensions of urban planning.
SOURCE: The Future of the Public’s Health (IOM, 2003a).
these tools should be the goal of providing comprehensive care that is safe and effective, that is collaborative and interdisciplinary, and that respects and joins effective interventions from all sources. Chapters 3, 4, and 5 addressed issues of efficacy and effectiveness and provided a framework for decision making that states that the same principles of evidence and stan-d dards of treatment effectiveness should apply to all treatments, whether
they are currently labeled as conventional medicine or CAM. The next section presents a conceptual model for deciding when to translate new therapies (CAM or conventional medicine) into practice.
ADVISING PATIENTS
The committee believes that any framework for decision making should encourage patients and practitioners to engage in shared decision making about treatment. One of the 10 rules outlined in the IOM report Crossing the Quality Chasm (2001) is that the patient should be viewed as the source of control. The report states, “Patients should be given the necessary information and the opportunity to exercise the degree of control they choose over health care decisions that affect them. The health system should be able to accommodate differences in patient preferences and encourage shared decision making.” Such statements can be applied to the desire for shared decision making about CAM therapies as well as those of conventional medicine.
Eisenberg (1997) recommends a nine-step strategy for advising patients:
-
Ask the patient to identify the principal symptom.
-
Suggest that the patient keep a symptom diary.
-
Discuss the patient’s preferences and expectations.
-
Review issues of safety and efficacy.
-
Identify a suitable licensed provider.
-
Provide the patient with key questions to ask the provider during the initial consultation.
-
Schedule a follow-up visit (or telephone call) to review the treatment plan.
-
Follow up to review the response to treatment.
-
Provide documentation.
The fourth step of the process proposed by Eisenberg is a review of the safety and efficacy of the treatment under discussion. At this step Cohen and Eisenberg (2002) propose that practitioners may wish to guide their recommendations for treatment for both conventional and CAM therapies by evaluating whether the medical evidence:
-
supports both safety and efficacy (option A);
-
supports safety, but evidence regarding efficacy is inconclusive (option B);
-
supports efficacy, but evidence regarding safety is inconclusive (option C); or
-
indicates either serious risk or inefficacy (option D).
Thus, within the framework suggested in Chapter 6 of this report, if the medical evidence supports both safety and efficacy (option A), liability is unlikely and clinicians should recommend the therapy; if the medical evidence indicates either serious risk or inefficacy (option D), liability is probable and clinicians should avoid and actively discourage the patient from using the therapy. If the medical evidence supports safety, but evidence regarding efficacy is inconclusive (option B), or if the medical evidence supports efficacy but evidence regarding safety is inconclusive (option C), then clinicians should caution the patient. If the patient chooses to try the therapy despite the cautionary advice the practitioner should continue to monitor both the efficacy and the safety of the therapy. Figure 7-3 portrays the options graphically.
If patients demand and expect to use therapies for which sufficient evidence to justify the practitioner’s recommendation is lacking, then, depending on the medical evidence, the practitioner should caution the patient and monitor efficacy (option B), caution the patient and monitor safety (option C), or encourage the patient to avoid the therapy (option D). In general, if patients choose to make their own decisions, against their conventional practitioner’s advice, the practitioner should document this in the patient’s medical record. From a liability perspective, the more acute and severe the condition is or the more curable the condition is by conventional medical therapies, the more important it is to monitor and, as neces-
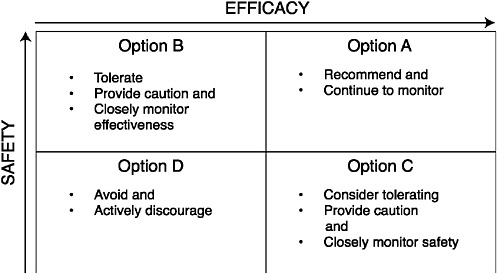
FIGURE 7-3 Clinical risk and the therapeutic posture.
SOURCE: Adapted from Cohen and Eisenberg (2002).
sary, treat the patient by conventional medical practices (Adams et al., 2002; Cohen and Eisenberg, 2002).
The information presented above provides a framework for clinicians. The guidelines developed by the Federation of State Medical Boards also offer information for clinicians to consider (see Appendix E). Conventional medical practitioners should also take into account ethical considerations, as discussed in Chapter 6 when they are advising patients whether to pursue CAM therapies.
Because research regarding both conventional and CAM therapies is ongoing and the medical evidence can change rapidly, the clinician should communicate regularly with the patient regarding any new developments. If, for example, it turns out that high-dose antioxidants negatively interact with chemotherapy, then this information may change the decision to continue the use of high-dose antioxidants during chemotherapy or may change reliance on them as part of a CAM regimen for a period instead of chemotherapy (Cohen and Rosenthal, in press).
If a decision is made to include a therapy provided by another practitioner, the focus of decision making then shifts to identifying practitioners with acceptable expertise. When a patient is referred to a CAM provider, it is important for the conventional medical practitioners to inquire about the provider’s training, practice experience, scope of practice, and history of malpractice litigation or professional discipline. Health care institutions are also faced with challenges as they move to consider providing both CAM and conventional medical care. The next section explores issues related to the provision of CAM therapies in health care institutions.
HEALTH CARE INSTITUTIONS
Health care institutions face a number of potential operational barriers to the provision of integrative medicine, including issues of financial sustainability and the development of appropriate clinical models for the provision of medical care by teams comprising various conventional medical and CAM providers. Kreitzer (2001) explored a process for strategic planning and decision making about the inclusion of CAM in existing health care settings. Steps in the planning process include
-
defining who is responsible for gathering information, generating recommendations, and making decisions;
-
identifying and clarifying mandates, both formal (e.g., charters, articles of incorporation and legislation) and informal (tradition or expectations);
-
clarifying the mission and values of the health care system;
-
assessing the external environment for opportunities and challenges (i.e., political climate, economic and social trends, and potential client population); and
-
assessing the internal environment (e.g., people resources and their skills, provider perceptions, and level of interest).
The outcomes from these five steps provide the information necessary for the development of a strategic plan that addresses such issues as whether CAM will be implemented in a systemwide effort or incrementally and whether CAM services will be organized around a core or a center within the system or dispersed throughout the system. Once strategies are developed, all actions and decisions necessary to implement the strategies can be identified (Kreitzer, 2001).
In developing approaches that include both CAM and conventional medical therapies, health care institutions may take advantage of existing health care institution policies and guidelines to address liability concerns, implement risk management practices, and otherwise find ways to appropriately include CAM therapies and providers in existing systems of care. For example, a major area of focus involves credentialing of CAM providers. Such credentialing has parallels to existing hospital mechanisms for credentialing and offering clinical privileges to conventional medical providers; yet credentialing of CAM providers must also incorporate information regarding the standards of education and training, competence, and scopes of practice required by licensing laws in a given state and established by various CAM professional organizations (Eisenberg et al., 2002). Ina (2001) provides guidance for the institutional credentialing process, recommending that source documents should include
-
a comprehensive provider application and contract;
-
professional license or certification requirements;
-
records indicating satisfactory completion of specialty training;
-
required professional insurance standards;
-
required years of experience;
-
peer review of the practitioner’s application and all related documents;
-
practitioner capabilities for data reporting and profiling; and
-
a thorough on-site review of provider offices, records, and operations.
The process of credentialing can be undertaken by the institution itself or through contract with an outside consultant or vendor. According to Ina (2001), 50 percent of organizations surveyed in the report of Landmark
Healthcare, Inc. (1999) contracted with an outside vendor to credential CAM practitioners.
The development of appropriate clinical models to implement care that includes both CAM and conventional medical therapies is an additional challenge for this emerging field of integrative medicine. The next section explores various approaches.
APPROACHES TO INTEGRATION
There are several approaches to the integration of CAM and conventional medicine. As Rolfe and Hohenstein (2001) state, “In arrangements with less integration, practitioners are in business for themselves, and merely lease space in an integrative medical center” but have little interaction with one another. In another model, hospitals might hire alternative practitioners as staff to deliver specific services for which the hospital collects dollar-for-dollar revenue on the basis of services delivered (Sol and Faass, 2001). Models with high levels of integration include those that use a multidisciplinary team approach to care. Some models have physician oversight of all practitioners, whereas others use a more collaborative approach or team structure that may have a physician as the director for the center.
Donald Novey, in his presentation to the IOM committee at its meeting in September 2003, discussed four existing program models: the consultant model, the primary-care model, the fitness center model, and the virtual center model. The consultant model, which is also known as the specialty model, is one in which patients are referred to CAM providers for particular therapies. This model is noncompetitive; physicians feel confident referring patients to the CAM consultants because patients will return to the physician for their primary care. However, revenue is dependent on the provision of CAM services, and therefore, a high volume of CAM services must be maintained.
The primary-care model is a blend of conventional primary medical care (usually internal medicine or family practice) with nontraditional (CAM) medical care housed in the same setting. The advantage of this model is that revenues are generated from both the CAM practice and the primary-care medical practice. However, because it is not clear whether the practice is mainstream or alternative, difficulties may arise with referrals. There is also competition with other primary-care practices. The fitness center model is one in which integrative medicine services are located within a fitness center. Such a system has high visibility and attracts a population that focuses on wellness. It is also a system that can be used to promote the merchandising of particular items, if desired. The virtual model offers services in various sectors of a facility or health care system that are coordinated by a director of CAM services.
In 1998, The Integrator’s Clinic Benchmarks Study surveyed 29 clinics offering integrative medical care. That study identified four distinct categories of clinic models for integrative medicine. In the complementary health services model, services are usually limited to education, massage, body work, and some energy therapies, such as therapeutic touch. The CAM-centric services model provides the services of licensed CAM providers, such as acupuncturists and chiropractors, and has a limited involvement of medical doctors. In the integrative, CAM-centric service delivery model the leader is usually a medical doctor or a doctor of osteopathy (DO) who not only acts as the team leader for those providing services but also provides reassurance to the physicians who practice more conventional medicine. Most services are provided by nonmedical, non-DO practitioners. The model in which most care is provided by integrative medical physicians who have skills in one or more CAM modalities is the integrative medical doctor/DO-centric service delivery model. The following are general findings that held true across all models:
-
To break even, large clinics (those with more than 6,000 square feet of clinic space) need a core of integrative medical doctor and DO providers.
-
Chiropractors are a significant patient draw.
-
Thorough integration requires the involvement of a medical doctor or DO champion.
-
Ongoing subsidies are needed if only CAM services are offered.
A report prepared for the Philanthropic Collaborative for Integrative Medicine (Clohesy Consulting, 2003) found that the most important catalysts for establishing a program integrating CAM and conventional care were
-
a leadership-level champion,
-
faculty members or practitioners who are committed to the program and who have had positive personal experiences with CAM,
-
a visionary philanthropist or other source of capital, and
-
consumer demand.
The Clohesy Consulting (2003) report described five models for integrative medicine clinics. In the first model multiple practitioners are integrated into a staff team. Services are provided under one roof, and the team collaborates in the planning and provision of care. A major challenge is paying for staff time spent in collaborative meetings and conferences. Furthermore, patient costs are high because of the high cost of the practitioner-patient interface, the expense of integrated medical records needed, and technology may be too high for start-up efforts.
A second model, which is similar to conventional medicine, includes a patient care team, as discussed above for the first model described by Clohesy Consulting, but it also adds a network of providers from the community to collaborate on patient care. Quality control may be more difficult because not all patient care services are provided by the patient care team. It is sometimes difficult to maintain the outside network of credentialed practitioners; turf issues may affect overall care; and the need for shared technology and record keeping may be problematic.
The third model discussed in the report by Clohesy Consulting is one in which the patient is the integrator of care, which is provided through a center or a community network. Although this model reduces the collaborative costs among practitioners, there is a loss of continuity of care. Furthermore, the patient may not be well enough informed to make appropriate decisions about his or her care and may become frustrated with attempting to coordinate his or her health care services.
In the concierge or advocate model, the fourth model, one designated person integrates care for both the patient and practitioners. This is less costly than team coordination but the patient may feel limited by using the network of the selected advocate, and there are currently no standards for how the role of the advocate should be performed.
The final model is the patient oriented delivery system (PODS) model. In this model, patients meet together with one practitioner in a group setting. Although patients learn from one another by this approach and the cost of educational or consultative care is reduced, the model works best for those problems that benefit from a group process rather than problems that require one-on-one treatment.
Most integrative medical centers are structured for self-pay and all face sustainability challenges (Clohesy Consulting, 2003). For example, because most are small, they do not generate sufficient revenue to hire more practitioners. However, to attract more patients and, therefore, have higher incomes, they first need to hire more practitioners. Another problem relates to reimbursement for services. For centers that do accept direct insurance payment, because insurers do not reimburse for the full costs of integrative medicine consultations and therapies, the more patients these centers see, the more money they lose.
Centers that bring in research grants are able to use the overhead from these grants to balance income and expenditures. For many centers in academic settings, however, the overhead income must be given to the university, which returns a smaller portion of the collected dollars to the center, thereby making it more difficult for the center to make up budget deficits. Potential solutions to the financial difficulties of integrative medical centers have been identified:
-
philanthropy,
-
devising products or services to earn income1 (e.g., charging for community education, and creating a retail operation to sell related products such as an herbal pharmacy), and
-
cost-containment strategies (e.g., minimizing full-time staff and using consultants, hiring CAM practitioners with an existing clientele, so that their work is profitable as quickly as possible, and conceptualizing the center as a “mall,” with each practitioner renting space as an individual businessperson).
CONCLUSIONS AND RECOMMENDATIONS
Health care that integrates CAM therapies with conventional medicine has been termed “integrative medicine” by many (Berndtson, 1998; Hess, 2002; Maizes et al., 2002; Snyderman and Weil, 2002). The committee believes that whatever term is used, the goal should be the provision of comprehensive care that is safe and effective, care that is collaborative and interdisciplinary, and care that respects and joins effective interventions from all sources. Furthermore, the committee believes that this comprehensive approach should be based on the 10 rules outlined in the IOM report Crossing the Quality Chasm (2001):
-
Care based on continuous healing relationships
-
Customization based on patient needs and values
-
Patient as the source of control
-
Shared knowledge and the free flow of information
-
Evidence-based decision making
-
Safety as a system property
-
Need for transparency
-
Anticipation of needs
-
Continuous decrease in waste
-
Cooperation among clinicians
A comprehensive system uses the best scientific evidence available regarding benefits and harm, recognizes the importance of compassion and caring, encourages patients to share in decision making about therapeutic options, and promotes choices in care that can include CAM therapies where appropriate. Such comprehensive care is evidence based and requires that decisions be made on the basis of the results of scientific inquiry (see Chapter 3 for a discussion of the use of evidence in decision making).
Scientific inquiry into little understood or unproven ideas, no matter what the source of the ideas, can lead to new information that in turn can lead to improvements in health care for the public. The committee believes that a therapy should be chosen on the basis of what is known about its safety and effectiveness, not on whether it is a conventional therapy or CAM. There is more to be gained by abandoning decision making on the basis of the source of ideas and instead, embracing the idea of knowledge-based therapies.
When the effectiveness of CAM and conventional medical treatments is studied, it is unlikely that the results will show that all treatments in one modality are effective and that all treatments in the other are ineffective. It is more likely that the treatments offered by both major modalities will be shown to be effective. Studies currently show that patients frequently use more than one modality of medical care (as opposed to choosing one over the other), and that pattern will probably continue and may even expand as evidence of treatment effectiveness accumulates. Therefore, it will be important to understand how CAM and conventional medical treatments (and providers) interact with each other and to study models of how CAM and conventional medical treatments can be provided in integrated and coordinated ways.
Unfortunately, little information is available about the outcomes and the effectiveness of various models of integration. What are patient outcomes? How do these outcomes compare with those for patients with similar conditions treated in conventional medical care facilities? What are the costs of such treatments, and how do the costs compare with those of conventional approaches to the provision of medical care? These and many other questions must be answered to provide practitioners (of both conventional medicine and CAM) and policy makers with the information necessary to make decisions about the future of integrative medical practice. There is an urgent need for health systems research efforts that focus on identifying the elements of various models of integrative medicine, the outcomes of care delivered through these models, and whether these models are cost-effective compared with the cost of care obtained in conventional medical practice settings.
Therefore, the committee recommends that the National Institutes of Health and other public and private agencies sponsor research to compare
-
the outcomes and costs of combinations of CAM and conventional medical treatments and models that deliver such care
-
models of care delivery involving CAM practitioners alone, both CAM and conventional medical practitioners, and conventional medical practitioners alone. Outcome measures should include reproducibility, safety, cost-effectiveness, and research capacity.
The committee believes that research aimed at answering questions about outcomes of care are crucial to ensuring that health care professionals are providing evidence-based comprehensive care that encourages a focus on healing, recognizes the importance of compassion and caring, emphasizes the centrality of relationship-based care, encourages patients to share in decision making about therapeutic options, and promotes choices in care that can include CAM therapies where appropriate.
To address health problems in both the population and the individual in the United States, the committee believes that it is important that private and public purchasers, other governmental entities, health care organizations, clinicians, and patients work together to implement a comprehensive framework for care. This framework should include both conventional medical and CAM approaches to health promotion, disease prevention, and the treatment of illness that have been shown to be safe and effective. To the extent that evidence indicates that models of health care that integrate CAM and conventional therapies (e.g., integrative medicine clinics) offer patients benefits, more research on these benefits would be useful. Therefore, the committee recommends that the Secretary of the U.S. Department of Health and Human Services and the Secretary of the U.S. Department of Veterans Affairs support research on integrated medical care delivery, as well as the development of a research infrastructure within such organizations and clinical training programs to expand the number of providers able to work in integrated care.
The committee does not expect that the level of scientific certainty about the effectiveness of delivery models that will be achieved will be the same as that achieved for treatments. This is because, as those involved in health systems research are well aware, many local variations and circumstances affect the effectiveness of the delivery models.
The next chapter discusses educational programs and the educational needs of both conventional medicine and CAM practitioners.
REFERENCES
Adams KE, Cohen MH, Eisenberg D, Jonsen AR. 2002. Ethical considerations of complementary and alternative medical therapies in conventional medical settings. Ann Intern Med 137(8):660–664.
Ananth S. 2002. Health Forum/AHA 2000-2001 Complementary and Alternative Medicine Survey. Chicago, IL: Health Forum LLC.
Astin JA, Marie A, Pelletier KR, Hansen E, Haskell WL. 1998. A review of the incorporation of complementary and alternative medicine by mainstream physicians. Arch Intern Med 158:2303–2310.
Barrett B, Marchand L, Scheder J, Appelbaum D, Chapman M, Jacobs C, Westergaard R, St Clair N. 2000. Bridging the gap between conventional and alternative medicine. J Fam Pract 49(3):234–239.
Bausell RB, Berman BM. 2002. Commentary: Alternative medicine: Is it a reflection of the continued emergence of the biopsychosocial paradigm? Am J Med Qual 17(1):28–32.
Berman BM, Singh BK, Lao L, Singh BB, Ferentz KS, Hartnoll SM. 1995. Physicians’ attitudes toward complementary or alternative medicine: A regional survey. J Am Board Fam Pract 8(5):361–366.
Berman BM, Singh BB, Hartnoll SM, Singh BK, Reilly D. 1998. Primary care physicians and complementary-alternative medicine: Training, attitudes, and practice patterns. J Am Board Fam Pract 11(4):272–281.
Berndtson K. 1998. Complementary and alternative medicine. Integrative medicine: Business risks and opportunities. Physician Exec 24(6):22–25.
Blumberg DL, Grant WD, Hendricks SR, Kamps CA, Dewan MJ. 1995. The physician and unconventional medicine. Altern Ther Health Med 1(3):31–35.
Cassileth BR. 2002. The integrative medicine service at Memorial Sloan-Kettering Cancer Center. Semin Oncol 29(6):585–588.
Cleary-Guida MB, Okvat HA, Oz MC, Ting W. 2001. A regional survey of health insurance coverage for complementary and alternative medicine: Current status and future ramifications. J Altern Complement Med 7(3):269–273.
Clohesy Consulting. 2003. Mapping the Emergence of Integrative Medicine. Cedar Falls, IA: Clohesy Consulting.
Cohen MH, Eisenberg DM. 2002. Potential physician malpractice liability associated with complementary and integrative medical therapies. Ann Intern Med 136(8):596–603.
Cohen MH, Rosenthal D. In press. Legal issues in integrative oncology. Integrat Oncol.
Corbin Winslow L, Shapiro H. 2002. Physicians want education about complementary and alternative medicine to enhance communication with their patients. Arch Intern Med 162(10):1176–1181.
Dahlgren G, Whitehead M. 1991. Policies and Strategies to Promote Social Equity in Health. Stockholm, Sweden: Institute for Future Studies.
Dana-Farber Cancer Institute. 2004. Zakim Center for Integrated Therapies. [Online]. Available: http://www.dana-farber.org/pat/support/zakim_default.asp [accessed June 17, 2004].
Eisenberg D. 1997. Advising patients who seek alternative medical therapies. Ann Intern Med 127(1):61–69.
Eisenberg DM, Cohen MH, Hrbek A, Grayzel J, Van Rompay MI, Cooper RA. 2002. Credentialing complementary and alternative medical providers. Ann Intern Med 137(12):965–973.
Evans RG, Stoddart GL. 1994. Producing Health, Consuming Healthcare. In: Evans RG, Barer ML, Marmor TR, eds. Why Are Some People Healthy and Others Not? The Determinants of Health of Populations. New York: Aldine de Gruyter. Pp. 27–64.
FSMB (Federation of State Medical Boards). 2002. Model Guidelines for the Use of Complementary and Alternative Therapies in Medical Practice. Dallas, TX: Federation of State Medical Boards.
Gordon NP, Sobel DS, Tarazona EZ. 1998. Use of and interest in alternative therapies among adult primary care clinicians and adult members in a large health maintenance organization. West J Med 169(3):153–161.
Hess DJ. 2002. Complementary or alternative? Stronger vs weaker integration policies. Am J Public Health 92(10):1579–1581.
Howell D. 1999. The paradox of osteopathy. N Engl J Med 341(19):1465–1468.
Ina VS. 2001. Credentialling Complementary Practitioners. In: Faass N, ed. Integrating Complementary Medicine into Health Systems. Gaithersburg, MD: Aspen Publishers Inc. Pp. 188–206.
IOM (Institute of Medicine). 1999. Gulf War Veterans: Measuring Health. Washington, DC: National Academy Press.
IOM. 2001. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press.
IOM. 2003a. The Future of the Public’s Health. Washington, DC: The National Academies Press.
IOM. 2003b. Who Will Keep the Public Healthy? Washington, DC: The National Academies Press .
Kreitzer MJ. 2001. Visioning and Planning. In: Faass N, ed. Integrating Complementary Medicine into Health Systems. Gaithersburg, MD: Aspen Publishers Inc. Pp. 49–55.
Kreitzer MJ, Disch J. 2003. Leading the way: The Gillette Nursing Summit on integrated health and healing. Altern Ther Health Med 9(1):3A–10A.
Kreitzer MJ, Mitten D, Harris I, Shandeling J. 2002. Attitudes toward CAM among medical, nursing, and pharmacy faculty and students: A comparative analysis. Altern Ther Health Med 8(6):44–47, 50–53.
Lalonde M. 1974. A New Perspective on the Health of Canadians. Ottawa, Ontario, Canada: Ministry of Supply and Services.
Landmark Healthcare, Inc. 1999. The Landmark Report II on HMOs and Alternative Care. Sacramento, CA: Landmark Healthcare, Inc.
Maizes V, Schneider C, Bell I, Weil A. 2002. Integrative medical education: Development and implementation of a comprehensive curriculum at the University of Arizona. Acad Med 77(9):851–860.
M.D. Anderson Cancer Center. 2004. Place … of wellness. [Online]. Available: http://www.mdanderson.org/departments/wellness/ [accessed June 17, 2004].
Minnesota Board of Nursing. 2003. Minnesota Board of Nursing Home Page. [Online]. Available: www.nursingboard.state.mn.us [accessed January 13, 2005].
Pelletier KR, Marie A, Krasner M, Haskell WL. 1997. Current trends in the integration and reimbursement of complementary and alternative medicine by managed care, insurance carriers, and hospital providers. Am J Health Promot 12(2):112–122.
Rolfe LK, Hohenstein LK. 2001. Strategic Planning in the Integration of Complementary Medicine. In: Faass N, ed. Integrating Complementary Medicine into Health Systems. Gaithersburg, MD: Aspen Publishers Inc. Pp. 76–89.
Ruggie M. 2004. Marginal to Mainstream: Alternative Medicine in America. Cambridge, United Kingdom: Cambridge University Press.
Sikand A, Laken M. 1998. Pediatricians’ experience with and attitudes toward complementary/alternative medicine. Arch Pediatr Adolesc Med 152(11):1059–1064.
SIO (Society for Integrative Oncology). 2004. Society for Integrative Oncology Home Page. [Online]. Available: http://www.integrativeonc.org/index.php [accessed June 17, 2004].
Snyderman R, Weil AT. 2002. Integrative medicine: Bringing medicine back to its roots. Arch Intern Med 162(4):395–397.
Sol N, Faass N. 2001. Integrative Programs in Hospital Environments. In Faass N, ed. Integrating Complementary Medicine into Health Systems. Gaithersburg, MD: Aspen Publishers Inc. Pp. 90–94.
Sparber A. 2001. State boards of nursing and scope of practice of registered nurses performing complementary therapies. Online J Issues Nurs 6(3):10.
Tauber AI. 2002. The Quest for Holism in Medicine. In: Callahan D, ed. The Role of Complementary and Alternative Medicine: Accomodating Pluralism. Washington, DC: Georgetown University Press. Pp. 172–189.
Tracy MF, Lindquist R, Watanuki S, Sendelbach S, Kreitzer MJ, Berman B, Savik K. 2003. Nurse attitudes towards the use of complementary and alternative therapies in critical care. Heart Lung 32(3):197–209.
Weeks J. 1999. Insurance Coverage for Alternative Therapies. In: Micozzi MS, ed. Current Review of Complementary Medicine. Philadelphia, PA: Current Medicine, Inc. Pp. 107–119.
Weeks J. 2001. Major Trends in the Integration of Complementary and Alternative Medicine. Pp. 4–11 in Nancy Faass (ed.) Integrating Complementary Medicine into Health Systems. Gaithersburg, MD: Aspen Publishers, Inc.
WHO (World Health Organization). 1948. Constitution of World Health Organization Basic Documents. Geneva, Switzerland: World Health Organization.
Whorton JC. 2002. Nature Cures: The History of Alternative Medicine in America. New York: Oxford University Press.
Wolsko PM, Eisenberg DM, Davis RB, Ettner SL, Phillips RS. 2002. Insurance coverage, medical conditions, and visits to alternative medicine providers: Results of a national survey. Archives of Internal Medicine 162(3):281–287.
Wootton JC, Sparber A. 2001. Surveys of complementary and alternative medicine: Part I. General trends and demographic groups. J Altern Complement Med 7(2):195–208.
Worthman CM. 1999. Epidemiology of Human Development. In: Panter-Brick C, Worthman CM, eds. Hormones, Health, and Behavior: A Socio-Ecological and Lifespan Perspective. New York: Cambridge University Press. Pp. 47–104.






























