2
Indoor Environments and Occupants’ Health: What Do We Know?
Mark J. Mendell
Why are indoor environments important to people’s health? People in the United States spend about 85 percent of their time indoors. Also, indoor exposures to pollutants are different from outdoor exposures, often at higher concentrations. Furthermore, a given amount of pollutant released indoors is a thousand times more effective at causing human exposure than when released outdoors. A growing body of scientific evidence now suggests that indoor environments are associated with a variety of adverse health effects and related economic impacts.
A number of factors affect indoor environmental quality (IEQ), including a building’s design, construction, operation (including ventilation and thermal control), and maintenance (including the ventilation system and the building structure, housekeeping, and preventing leaks), the furnishings and contents, and its use—whether it is an office building, hospital, laboratory, etc. Occupants’ activities are also important. Pollutants can come from outdoor air or soil and substantially influence what is happening indoors.
WHAT DO WE KNOW ABOUT THE RELATIONSHIP OF IEQ TO THE HEALTH OF BUILDING OCCUPANTS? HOW CERTAIN ARE WE OF THESE RELATIONSHIPS, THAT IS, WHAT IS THE SOURCE OF THIS KNOWLEDGE?
In scientific research the highest degree of certainty is provided through documented causal relationships. For example, with an infectious disease, you can document the cause-and-effect relationship between the organism, the environment, and the people exposed and infected.
Documentation of causal relationships requires a large body of scientific research, significant findings replicated in different settings and populations, findings that are consistent across studies, and studies that are biologically plausible and free of substantial error from bias and confounding. It is also helpful to demonstrate that, when the suspected causal exposure is greater, the risk of the disease is greater as well. It is often difficult to convincingly document many relationships that we believe may be causal. We have different levels of certainty about whether many of the specific aspects of IEQ cause health problems for occupants.
In terms of IEQ and occupants’ health, causal relationships have been documented as shown in Table 2.1.
Research has clearly documented that the bacterium Legionella pneumophila can grow in water systems in buildings and cause a number of diseases in occupants, including Legionnaire’s disease, which has a high rate of fatality, and Pontiac fever, which causes a mild fever in most people who are exposed.
TABLE 2.1 Documented Causal Relationships Between IEQ and Occupants’ Health
|
Causal Agent |
Resulting Health Effect |
|
Legionella pneumophila (bacterium) |
Legionnaire’s disease Pontiac fever |
|
Microorganisms (unidentified) |
Hypersensitivity pneumonitis/humidifier fever |
|
Carbon monoxide |
Carbon monoxide poisoning |
|
Lead |
Lead poisoning, neurological damage |
|
Environmental tobacco smoke/radon/asbestos |
Lung cancer |
Two distinct diseases—hypersensitivity pneumonitis and humidifier fever—are caused by microorganisms growing in contaminated ventilation systems, contaminated humidification systems, and buildings with water damage from leaks. Causation of these serious diseases from exposures in buildings has been repeatedly documented, although in many cases the specific microorganisms causing the diseases have not been identified.
Carbon monoxide causes serious health effects, including death. In commercial buildings it generally results from entry of vehicle exhaust into indoor air by way of connected parking garages. In homes, carbon monoxide exposures often result from poorly vented combustion appliances.
Lead is present in old paint in older buildings such as homes and schools. Lead poisoning, which can result in serious neurological effects, sometimes occurs when infants and children eat the dust and particles from peeling paint. Lead poisoning is not known to be a significant problem in commercial buildings.
Substantial evidence exists that radon and asbestos occurring at high levels in occupational settings cause lung cancer. There is also clear evidence from studies, mostly of people living with active smokers, that environmental tobacco smoke causes lung cancer. An individual is not likely to observe the relationships between tobacco smoke, radon, asbestos, and lung cancer because it may take 20 to 30 years for the disease to manifest.
Although the causal relationships are not fully documented, there is persuasive scientific evidence linking a number of other indoor environmental factors to occupant health (see Table 2.2). A body of research with replicated significant findings exists, but the evidence is not sufficient to convince everyone that a causal relationship exists between a certain exposure and specific health effects.
Many studies have shown that low ventilation rates in buildings are associated with an increase in building-related symptoms among occupants. The term “building-related symptoms,” what others might call “sick building syndrome,” is defined as a set of nonspecific symptoms reported subjectively by occupants of a building that often improve when they leave the building. Symptoms include eye, nose, and throat irritations; headaches; fatigue; difficulty breathing; itching; and dry, irritated skin. It is difficult to study these symptoms because they do not indicate a specific identifiable disease. There are probably a number of exposures and biological response processes occurring simultaneously in the causation of these symptoms. In addition, these symptoms are known to be
TABLE 2.2 Persuasive Scientific Evidence Linking IEQ and Occupants’ Health
|
Agent/Factor |
Observed Health Effects |
|
Low ventilation rate (no threshold?) |
Building-related symptoms |
|
Visible moisture and mold |
Asthma and respiratory symptoms |
|
Air-conditioning or humidification systems (presence of) |
Building-related symptoms |
|
High temperatures (even within comfort envelope) |
Building-related symptoms Reduced performance Poorer perceived air quality |
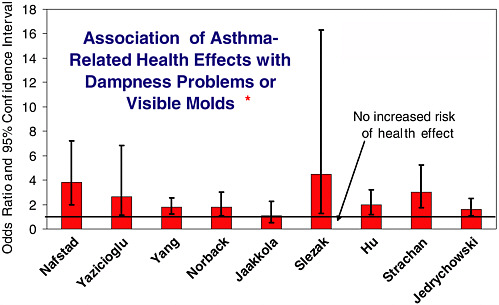
FIGURE 2.1 Association of asthma-related health effects with dampness problems or visible molds.
SOURCE: Institute of Medicine. 2000. Clearing the Air: Asthma and Indoor Air Exposures. Washington, D.C.: National Academy Press.
influenced by psychological factors. The challenge to identifying specific causal indoor exposures is to disentangle the biological processes that together present this confusing set of symptoms.
Clear evidence exists that visible moisture and mold in buildings are related to an increase in asthma and respiratory symptoms among occupants, although it is still not known what it is about the moisture that actually causes the adverse health effects. Current measurements of molds have not yet implicated specific molds as the key problem resulting from moist conditions.
The Institute of Medicine has reviewed the available science on building moisture’s effects on occupants’ health. Figure 2.1 identifies nine studies that consistently found some increase in risk associated with dampness. For almost all of them the confidence interval exceeds one, meaning that it is a statistically significant increase. But it is not known, in a way that can be measured and regulated, what the dampness represents in terms of specific exposures causing the illness.
Air-conditioning and humidification systems have been shown to be associated with an increase in building-related symptoms compared to buildings without such systems. Again, the causal exposures for this health effect are not known. The presence of these ventilation systems may pose a risk that, if the systems are poorly designed and maintained, they may become contaminated, thereby increasing the occurrence of building-related symptoms among occupants.
Also, high temperatures—particularly above the currently accepted comfort envelope (approximately 23 to 26 degrees Celsius, or 73 to 79 degrees Fahrenheit, in summer) and even at the higher end within the comfort envelope are associated with an increase in building-related symptoms, a reduction in occupants’ performance, and a perception of poor air quality.
There are a number of other items for which only suggestive scientific evidence for a cause-effect relationship is available. For these there are relatively few studies, studies with conflicting findings, or studies with some
TABLE 2.3 Suggestive Scientific Evidence Linking IEQ and Occupants’ Health
|
Agent/Factor |
Observed Effects |
|
Low ventilation rate |
Increased transmission of respiratory disease (flu, colds) Decreased performance |
|
HVAC moisture/contamination |
Lower respiratory tract symptoms |
|
Bacterial endotoxin |
Building-related symptoms |
|
Airborne fungi |
Building-related symptoms |
|
Formaldehyde at low concentrations |
Development of allergies |
|
Volatile organic chemicals |
Irritation symptoms |
|
Carpet and fleecy materials |
Building-related symptoms |
|
Very low humidity |
Dryness symptoms |
|
Soft plastic materials |
Development of allergies/asthma |
|
Recent renovation |
Development of allergies |
|
Poor space cleaning |
Building-related symptoms |
|
Increased view (or daylighting) |
Increased performance |
errors. It is important to remember that just because a number of studies show that two things are correlated statistically, it does not necessarily mean that one causes the other (see Table 2.3).
In a number of studies, low ventilation rates have been associated with increased transmission of a variety of infectious respiratory diseases such as flu and colds and decreased occupant performance. The presence of moisture or contamination in heating, ventilation, and air-conditioning (HVAC) systems has been associated with an increase in respiratory symptoms. This can be seen in data collected by the National Institute for Occupational Safety and Health (NIOSH) from a large number of buildings that were investigated for health complaints (see Figure 2.2).
The NIOSH study found that when a building has poor drainage in the pans underneath the air-conditioning cooling coils, there is a 160 percent increase in the risk of multiple work-related respiratory symptoms. These symptoms include wheezing, shortness of breath, tight chest, and cough. If there is debris in the air intake of the building, there is a 100 percent increase in risk for these multiple building-related respiratory symptoms. Although these are simply symptoms, they may indicate serious respiratory disease or sensitization, such as asthma.
Bacterial endotoxin, a substance often found in the environment, comes from bacteria that like moist locations. Several studies have found bacterial endotoxin to be related to an increase in building-related symptoms among occupants. Airborne fungi also have been measured and in some recent studies found to be related to an increase in symptoms, although in many studies they have not been related to symptoms.
Formaldehyde at surprisingly low concentrations has been found to be related to risk of development of asthma and allergies. Volatile organic chemicals are another exposure producing inconsistent findings in many studies. A growing number of recent studies have revealed that overall volatile organic chemicals and specific organic chemicals in indoor air have been related to irritation symptoms.
The presence of carpet and fleecy materials such as cloth-covered partitions or walls has been found to be related to an increase in building-related symptoms. Extremely low humidity has been associated with dry, irritated skin. But it is important to note that this does not mean that buildings should be humidified, because the risks associated with humidifiers, and potentially with high humidity, are much greater than those for low humidity.
Soft plastic materials (such as vinyl wallpaper) or objects with plasticizers (the chemical additives that keep plastics soft and pliable) that emit the plasticizers into the air are associated with the development of allergies and asthma in children. This is a new area of research and is potentially very important.
In addition, recent renovation of a building has been shown to be related to the development of allergies in infants because the new paint, flooring, and other materials emit volatile organic chemicals into the indoor air.
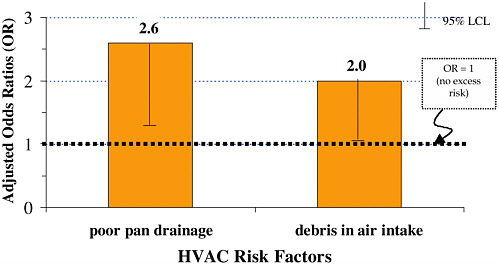
FIGURE 2.2 Risk factors for multiple work-related respiratory symptoms.
SOURCE: 1993 NIOSH Office Investigations**
** Mendell et al., American Journal of Industrial Medicine 2003
Poor space cleaning in office buildings has also been shown in some studies, but not all, to be related to increases in occupants’ symptoms. In terms of positive influences, a few studies have shown that increased views out windows or possibly day lighting are related to increased occupant performance, but it is not yet clear how to interpret these results.
Overall, there are no specific limits for exposures to measured volatile organic chemicals or microorganisms that have been shown to serve as a breakpoint between acceptable and unacceptable indoor conditions. Therefore, identified risk factors, like dampness or the presence of certain exposure sources, are often used to indicate unmeasured causal exposures in indoor air. Because we lack certain specific exposures known to be important to measure, it is difficult to characterize indoor environmental quality in buildings in terms of whether exposures are acceptable. That, unfortunately, is the state of the science with respect to many aspects of IEQ and occupants’ health.
Still, we can look to some of the risk factors that are known to be important and determine what we need to do to improve indoor environments for the people living and working in them. The research indicates that we should:
-
Eliminate indoor environmental tobacco smoke,
-
Prevent indoor dampness and mold,
-
Provide adequate outdoor air ventilation,
-
Control Legionella in building water systems (guidelines available from American Society of Heating, Refrigerating, and Air-Conditioning Engineers and others),
-
Keep HVAC systems clean and dry—first by the initial design and then by operations and maintenance,
-
Use natural ventilation where feasible,
-
Improve temperature control and avoid higher temperatures, and
-
Limit/control indoor sources of volatile organic chemicals.
So how much of a problem do we have? Some of the best data available on the state of commercial buildings in the United States are from the Environmental Protection Agency’s (EPA) Building Assessment and Survey
Evaluation Study, which included 100 representative office buildings during the 1990s and collected information on various factors and exposures.
Scientific research has shown, as mentioned above, that occupants in buildings with water damage or poorly maintained drain pans are clearly at risk for developing respiratory illnesses. EPA’s statistics show that:
-
40 percent of the buildings had no scheduled cleaning of the drain pans,
-
30 percent had very dirty drain pans,
-
34 percent had current water damage in occupied spaces,
-
71 percent had past water damage in occupied spaces,
-
15 percent had current water damage from leaking roofs, and
-
50 percent had past water damage from the roofs.
Overall, 43 percent of the buildings had some current water damage and 85 percent had past water damage. These are sobering numbers for estimating the potential magnitude of existing problems related to IEQ and human health.
The National Occupational Research Agenda Indoor Environment Team made some estimates based on available data of the potential magnitude of benefits that might result from improved indoor work environments, such as offices. The estimates excluded costs of deaths and focused only on the costs of health care and lost productivity at work. It estimated that 6 million to 8 million respiratory infections could be prevented each year, at an annual savings of $3 billion to $5 billion. One million to 4 million episodes of asthma and allergies could be prevented, at a savings of $200 million to $600 million a year. And building-related symptoms could be prevented in 8 million to 30 million people, resulting in a productivity benefit of $4 billion to $70 billion annually.
Furthermore, as many as 3,000 cases of Legionnaire’s disease (associated with more than 70 deaths) could be prevented annually, for a savings of at least $30 million. If we could eliminate environmental tobacco smoke from workplaces, 2,000 to 11,000 deaths could be prevented each year from heart disease and lung cancer, for a savings of $30 million to $140 million. This figure does not include the possible additional benefits to students in schools, patients in hospitals, or visitors to public buildings.
There are multiple forces likely to change building design, operation, and maintenance practices that will, in turn, improve IEQ in buildings, including an increasing recognition of the health and productivity benefits of good indoor environmental quality; increasing costs of health care; increasing demand for excellent health and healthy environments; and, across multiple sectors, greater recognition of accountability for providing healthy indoor environments. Hopefully, as the demand for improved IEQ builds, we will have increased ability and knowledge to take appropriate actions.
In summary, there is a clear need to better implement what is known about good indoor environmental quality to improve the health and performance of building occupants. Improved IEQ starts with appropriate design and construction of buildings and continues with good operations and maintenance practices throughout the life of each building.
ABOUT THE PRESENTER
Mark J. Mendell, Ph.D., is an environmental epidemiologist, with the Lawrence Berkeley National Laboratory’s Indoor Environment Division. Dr. Mendell has conducted research on health effects of indoor environments for many years and has been published extensively. He was formerly at the National Institute for Occupational Safety and Health, where for six years he led the National Occupational Research Agenda Indoor Environment Team. His research interests include the effects of indoor chemical and microbiologic pollutants in offices, schools, and homes on asthma, infectious disease, and building-related symptoms, with specific interests in risks related to ventilation systems, indoor chemical emissions, and indoor moisture.






