3
Behavioral and Social Sciences Research
The behavioral and social sciences cover a wide spectrum of health-relevant research areas. One end of the spectrum has a focus on the individual, including such areas as psychology, behavioral and cognitive neuroscience, and cognitive science. Here the focus is on the individual’s behavior, with a direct relevance for mental health and mental disorders and a strong relevance for major health problems such as obesity; drug, alcohol, and tobacco abuse; and propensity for violent behavior and crime. The other end of the spectrum has a focus on interpersonal, group, and societal behavior, including sociology, economics, education, and political science. Research in these sciences has an equally important role in identifying key factors that underlie the complex health problems besetting our society.
The behavioral and social sciences are far more complex and variable than some of the natural sciences; not only is there an almost uncountable number of factors affecting individual and social behavior, but these factors combine and interact in extremely complex and mutable ways. Partly for this reason and partly for historical and cultural reasons, research support and research training in these areas lag well behind those in other sciences. While the behavioral and social sciences have addressed fundamental health care question for decades, methods and tools developed in recent years have provided useful and effective answers to some of the nation’s most pressing health care problems.
At the same time that these sciences have been maturing, society has come to realize the absolute necessity of their research findings for the understanding, treatment, and prevention of its health problems. As a result, the behavioral and social sciences have been called on for advice to an ever-increasing degree by government agencies. This is evidenced by the number and range of government-commissioned committees, panels, and reports assigned to the Division of Behavioral and Social Sciences and Education (DBASSE) of the National Research Council. In the past 10 years, there have been over 300 publications resulting from DBASSE assignments that cover a wide range of areas directly or indirectly related to health concerns, including children and families; education, employment, and training; the environment; health and behavior; human performance; international studies; law and justice; national statistics; and population and urban studies. These studies range in scope from the level of the individual to the level of society and cover the entire range of social and behavioral sciences and extend to related fields (such as ecology and criminology).1
The social and behavioral sciences deal with many of the most complex and least predictable phenomena that affect people’s health. Mental health, for example, is an important concern at the National Institutes of Health (NIH; particularly the National Institute of Mental Health, NIMH) as well as in the government and private sector generally. Yet mental health is only one part of a much larger picture because many of the most important health problems are determined and strongly affected by behavioral, social, and economic factors. At the level of the behavior of the individual, the behavioral and social sciences produce knowledge about health issues such as drug and alcohol abuse, obesity, violent behavior, smoking, maintenance of drug treatment regimens, stress management, ability to cope with illness, and health decision making. Moreover, there are many critical health issues that emerge at a larger scale. The economics of health
care and its delivery critically determines which diseases and problems are attacked, what research is carried out, and which treatments are given. The government has recognized these factors with multimillion dollar investments in surveys, such as the Health and Retirement Survey, the National Longitudinal Survey, and the National Survey of Families and Households. The behavioral and social sciences provide critical insights and knowledge. This knowledge covers a vast array of issues concerning our ability and willingness to deal with disability and our willingness to expend income and assets for health purposes, such as:
-
promoting well-being;
-
distributing health care geographically, sociologically, and economically;
-
using and misusing health care institutions;
-
monitoring health providers’ behavior;
-
studying the psychological and social effects of morbidity and mortality;
-
tracking the social and psychological effects on treatment and recovery;
-
transferring assets and beliefs across generations;
-
documenting social support mechanisms;
-
measuring the economics of alternative health care systems;
-
verifying the effects of approaches to care and bereavement; and
-
making health decisions.
Societal, behavioral, and economic factors work together to produce such problems as drug abuse, smoking, alcohol abuse, anorexia/bulimia, and obesity. Once-treatable diseases are making a comeback in more virulent forms because reliable methods cannot be found to ensure that curative drugs are taken as prescribed. Social and sexually transmitted diseases, such as HIV/AIDS, continue to be an increasing menace. Even crime and violence are rooted in elements that require the expertise of behavioral and social sciences research. It is now accepted that many diseases, historically considered mainly a matter for biomedical research, such as heart and lung disease, drug addiction, tuberculosis, and malaria, cannot be understood and treated without the benefit of behavioral and social research. When these far-reaching health implications of behavioral, social, and economic factors are added to the more direct implications of research for mental illnesses such as depression, schizophrenia, and various neurological illnesses, it is no surprise that the research demand in the behavioral and social sciences has grown rapidly in recent years.
Support for research in the behavioral and social sciences at NIH resides primarily in the NIMH, secondarily in the National Institute on Aging (NIA) and the National Institute of Child Health and Human Development (NICHHD), and is scattered in other institutes (with the present exception of the National Institute of General Medicine. It should be noted that the primary mission of NIMH is research into the prevention and treatment of mental disorders, and the mission of NIA and NICHHD is research into the health problems of young and aging populations. Consequently, neither institute directly supports research into key factors underlying societal health problems, such as smoking, alcohol and drug abuse, obesity, and the like. A case could be made that research in the behavioral and social sciences needs to be augmented significantly by other NIH institutes and centers. Most NIH institutes would benefit from scientists knowledgeable in the techniques, methods, and findings of the behavioral and social sciences. In particular, empirical design and quantitative and statistical methodology that have been so effectively refined in the social and behavioral sciences would be useful. Thus at institutes and centers that do not presently have a direct focus on research in the behavioral and social sciences, at least some training needs to be directed toward researchers with this focus. In addition, some of the training given to researchers with other primary foci needs to be informed by appropriate training in the social and behavioral sciences, a point that is taken up directly in Chapter 8.
BEHAVIORAL AND SOCIAL SCIENCES RESEARCH WORKFORCE
The behavioral and social sciences workforce is as difficult to identify as the biomedical workforce but for different reasons. In particular, it is difficult to identify scientists who are doing basic health-related research, as opposed to those who are involved in clinical practice. Past studies of research training needs in the behavioral sciences generally defined the target workforce as Ph.D.s trained in anthropology, sociology, speech and hearing sciences, and psychology, with the exception of clinical, family, and school psychology. However, since professional organizations in psychology indicate that nonresearch-oriented doctorates are now receiving doctor of psychology (Psy.D.) degrees, the category of clinical psychology is included but not the other practice-oriented fields. Appendix C lists the fields included in the behavioral and social sciences. This inclusion is also supported by an experiment in which NIH was asked to identify whether the research topics for the theses of a sample of the Ph.D. population in the above-listed fields, including clinical psychology, would be considered for NIH funding. The results of this analysis showed that about 90 percent of the thesis topics could be funded and therefore a large portion of the clinical psychology Ph.D.s could pursue research careers. This may be an overestimate of the workforce, but it might provide a more accurate assessment. Whenever possible, the identification of those who do not participate in research will be addressed in the following analysis of the workforce. In particular, attempts were made to identify institutions with professional programs in clinical psychology and to exclude their doctorates from the analysis.
The critical role played by the behavioral and social sciences workforce is increasingly recognized as a key element in both the maintenance of good health and the treatment of disease. The research workforce that addresses the types of diseases and health problems described earlier in this chapter is much broader than the behavioral and social sciences as defined for this study. For example, even in the treatment of what are often considered biologically based diseases, behavior is a factor in getting patients to take their medicine or to participate in physical activities that would help or prevent their condition. These research areas have an interdisciplinary component with the life sciences, behavioral and social sciences, and even the physical sciences. Interdisciplinarity further complicates analysis of the workforce because people trained outside the medical field are doing research important to the medical community (e.g., an economist studying the public health system). However, it would be impossible to factor these researchers into the current workforce assessment.
Another complication is how students identify their research area when they receive their doctorates. The increasing tendency for some research areas in the biomedical and behavioral sciences to converge (neuroscience is the most notable example) may lead to the classification of some doctorates in the behavioral sciences as biomedical. This factor may lead to an undercount of doctorates in the behavioral sciences and an overcount in the biomedical sciences. These difficulties notwithstanding, an attempt has been made to identify doctoral fields for analysis and potential problems in the analyses. The behavioral and social sciences workforce will consist of Ph.D. graduates from universities in the United States in the fields listed in Appendix C and of foreign graduates seeking careers in science and engineering in this country. This definition of the behavioral and social sciences workforce will provide a general estimate of the number of investigators and an indication of the major trends affecting this workforce, such as changes in size, age, and composition.
EDUCATIONAL TRENDS
The pool of college graduates in the behavioral and social sciences from which graduate programs would normally draw increased from about 74,000 in 1987 to almost 132,000 in 2001. In 1987 about 11 percent or 7,894 of these graduates matriculated to graduate programs in doctoral-granting institutions and in 2001 to about 6 percent or 8,305. The number of first-year graduate students was fairly constant during the late 1990s at about 8,500 and increased to 8,996 in 2002. This first-year enrollment resulted in a total full-time graduate enrollment of about 31,500 in 1987 and almost 40,000 in 2002. A portrait of the gender makeup of the graduate students (see Figure 3-1) shows a significant change from the late 1970s, when there were only a few more males than females, to 2002 when females outnumbered males by 2.5 to 1.
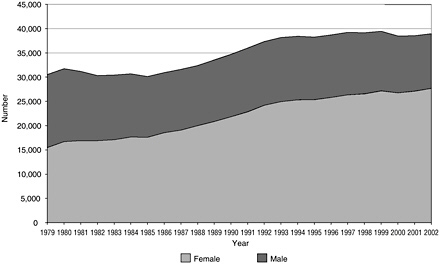
FIGURE 3-1 Graduate students in the behavioral and social sciences by gender, 1979–2002.
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
The picture of support for graduate education at doctoral-granting institutions in the behavioral and social sciences is very different from that in the biomedical sciences (see Figure 3-2). Traditionally, about half of the graduate students are supported by their own funds or other sources, because external funding from traineeships is small and declining and teaching assistantships are the major source of support.
The fairly constant size of the graduate student population seen in Figure 3-1 is reflected in the number of doctoral degrees through 2000 (see Figure 3-3). However, over the period from 2000 to 2003, the number of doctorates declined by 368 or about 8.2 percent. From just a few hundred in 1970 the number of doctoral degrees granted to women grew to 2,908 in 2000 but declined slightly to 2,724 in 2003. The
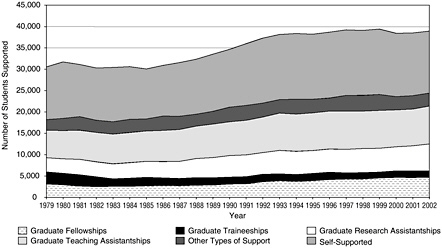
FIGURE 3-2 Graduate support in the behavioral and social sciences, 1979–2002.
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
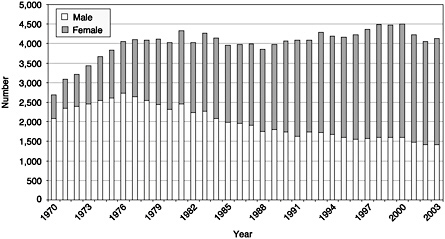
FIGURE 3-3 Doctorates granted in the behavioral and social sciences, 1970–2003.
SOURCE: National Science Foundation Survey of Earned Doctorates, 2001.
number of degrees granted to males dropped from a high of about 2,700 in the mid-1970s to a low of 1,411 in 2003. The decline in doctorates is a reflection of the graduate enrollment declines of the late 1990s, or the problem cited earlier with the classification of doctorates into closely related biomedical fields. On the one hand, the small increase in doctorates in 2003 may reflect the enrollment increases in the early 2000s and may predict a return to the degree production of the late 1990s in a few years. On the other hand, any increase may be temporary, since it may be a result of the national economic situation and will not continue into the future. Time to degree has increased by 3 years in total time and 2 years in registered time (see Appendix E). These increases have been greater than in the biomedical sciences by about a half a year. Similarly, the median age at time of degree has increased to almost 33 and is one of the highest in science and engineering.
Historically, behavioral and social sciences doctorates did not tend to go on to postdoctoral training, but this trend is changing. This fact by itself would tend to suggest that such doctorates could begin research careers earlier than biomedical doctorates, but such a trend is largely offset by the longer graduate training period. Recently, however, the fraction of doctorates planning on a postdoctoral appointment increased from about one-tenth in 1970 to more than one-third in 2003. Females are more likely to have additional research training since in recent years 15 percent of the females and 9.3 percent of the male doctorates have planned to pursue postdoctoral training. Another interesting aspect of the behavioral and social sciences doctoral population is the increased participation in postdoctoral training by individuals with degrees in clinical psychology (see Figure 3-4). This characteristic of clinical psychology doctorates also supports their inclusion in this assessment of personnel needs. For many years postdoctoral training was not considered essential, as was the case for other behavioral and social sciences fields, but in the early 1990s this changed and in recent years almost half of the behavioral and social sciences doctorates have planned to pursue postdoctoral training.
The large and increasing number of female doctorates seeking postdoctoral training suggests a special concern in the behavioral and social sciences. The traditional responsibilities of women to bear children and care for their families may lead to times when highly skilled researchers need to work in a less traditional format or even be absent from the workforce. Given the rapid pace of science, NIH might consider addressing this situation not only with retraining programs but also special postdoctoral research grants to keep
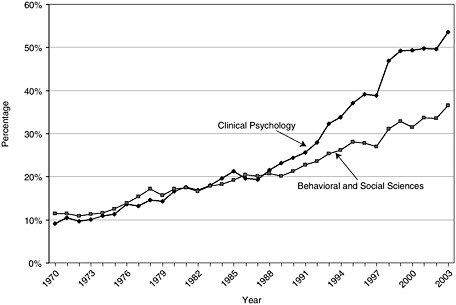
FIGURE 3-4 Doctorates planning postdoctoral training, 1970–2003.
SOURCE: National Science Foundation Survey of Earned Doctorates, 2001.
trained researchers in the workforce during periods in which personal priorities make it impossible to carry a full workload.
The proportion of doctorates facing potential immigration and visa difficulties is presently under 10 percent. An increasing proportion of doctorates in the biomedical sciences with temporary resident status and the problems that might occur if their residency status is jeopardized are not strongly seen in the behavioral and social sciences. Another positive development is the increase in minorities with doctorates. In the 1970s only 1 or 2 percent of the behavioral and social sciences doctorates went to minorities, but that has changed. In recent years, almost 15 percent of the doctorates have gone to minorities.
EMPLOYMENT TRENDS
The behavioral and social sciences workforce grew steadily from 27,356 in 1973 to 99,145 in 2001. Most of the growth can be attributed to the increasing number of female doctorates (see Figure 3-5); while they are not a majority of the workforce, their numbers have increased at an average annual rate of 11 percent since the late 1980s. In this same time period, the growth in the number of male workers was only 2 percent. If the postdoctoral population is included in the workforce, the rates of growth have not changed since they comprise only a small part of the workforce. Figure 3-6 shows the number of postdoctoral appointments by employment sector and the rapid growth in appointments in recent years. However, the number of appointments declined from its high of 2,583 in 1997 to 2,093. This decline is similar to that in the biomedical sciences and may be due to higher stipends imposed by NIH because interest on the part of new doctorates in postdoctoral training remains high, as seen by the data in Appendix E.
While the academic sector accounts for three-quarters of the appointments, as was the case for the biomedical sciences, there is stronger participation in the industrial sector. The other notable difference in postdoctoral training is the citizen/permanent resident and temporary resident ratio in academic institutions. In the biomedical sciences it is 1.4 to 1 with more temporary residents, compared to the behavioral and social sciences with a ratio of 3.6 to 1 with more citizens and permanent residents. It is possible that this difference reflects a divergence in technical training at virtually all levels of education between the U.S. and foreign systems. For example, the need for researchers with technical training (including laboratory training, instrumentation abilities, computational expertise, and mathematical and modeling skills) may have led to a large infusion of foreign researchers in the biomedical fields. If so, the increasing need for such types of training in the social and behavioral sciences may produce a tendency for a movement of the pattern seen in the social and behavioral sciences to that seen in the biomedical sciences.
The distribution of the nonpostdoctoral workforce in the behavioral and social sciences is very different from that in the biomedical sciences (see Figure 3-7). While academic employment is still the largest sector, industrial employment is growing at a rapid rate and almost equals that in educational institutions. The nonprofit sector is comparatively larger than in the biomedical sciences. By comparison, the
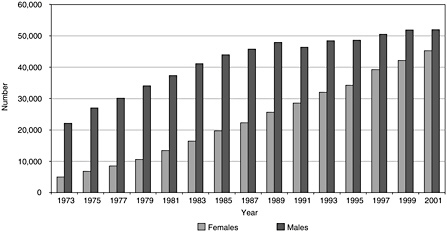
FIGURE 3-5 Behavioral and social sciences workforce (excluding postdoctorates) by gender, 1973–2001.
SOURCE: National Science Foundation Survey of Doctorate Recipients.
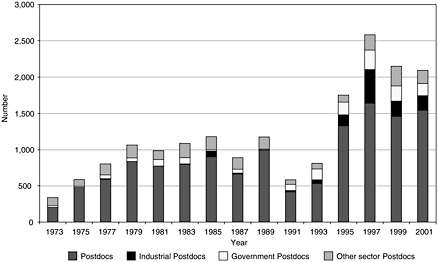
FIGURE 3-6 Trends in postdoctoral appointments by sector, 1973–2001.
SOURCE: National Science Foundation Survey of Doctorate Recipients.
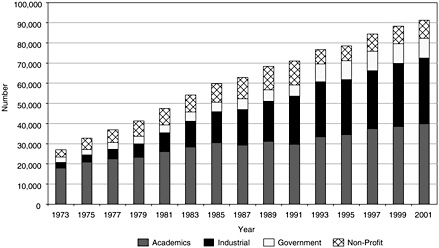
FIGURE 3-7 Behavioral and social sciences workforce by sector of employment, 1973–2001.
SOURCE: National Science Foundation Survey of Doctorate Recipients.
workforce in the behavioral and social sciences is almost as large as the biomedical sciences, with growth at about the same rate, 6.2 percent for the biomedical sciences and 5.4 percent for the behavioral and social sciences. The age distribution for the workforce, excluding postdoctoral appointees, for 1985 is similar for both the behavioral and the biomedical sciences but differs in that the median age in 2001 was 2.5 years older for the behavioral and social sciences workforce (see Table 3-1).
Another way to look at the aging of the behavioral and social sciences workforce is to compare the age distribution over time; note that there will be significant retirement in the next 10 years from the 55 to 65 age group (see Figure 3-8).
Academic employment in the behavioral and social sci-
TABLE 3-1 Median Age Cohort for the Biomedical Sciences and the Behavioral and Social Sciences
|
|
Median Age 1985 |
Median Age 2001 |
|
Biomedical sciences |
40.7 Years |
46.2 Years |
|
Behavioral and social sciences |
40.6 Years |
48.8 Years |
|
SOURCE: National Science Foundation Survey of Doctorate Recipients. |
||
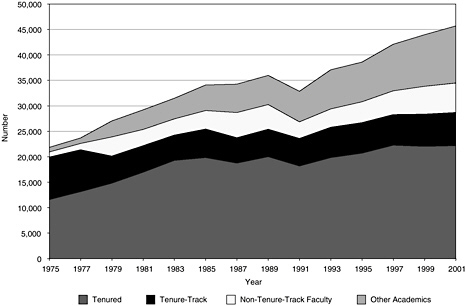
ences more than doubled from 1975 to 2001. Much of that growth was in nontenured positions and other academic categories, which together represent about one-third of the total academic staff in 2001. The size of the tenured and tenure-track staff has been almost constant since the late 1990s and grew by only 11 percent from 1989 to 1999 (see Figure 3-9).
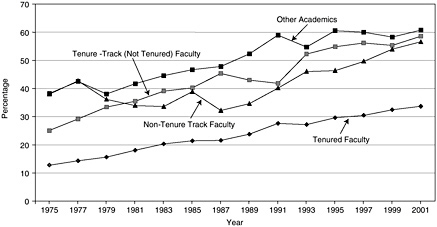
Over the past 10 years two-thirds of the doctorates have been awarded to women. This is reflected in academic appointments, with about 60 percent of nontenured positions held by women (Figure 3-10). Those in tenured positions are far below their 47 percent representation in the workforce, but over time this should change as more women in tenure-track positions receive tenure.
The number of minorities in the behavioral and social sciences workforce increased dramatically from 520 in 1975 to 8,534 in 2001 (see Appendix E). While the number has grown in recent years by about 15 percent per year and is greater than the 5 percent growth of the total workforce, they still remain a small percentage of the overall workforce. In 2001, underrepresented minorities comprised 8.6 percent of behavioral and social scientists, compared to 1.9 percent in 1973. There are, however, twice as many in the behavioral and social sciences workforce compared to the biomedical sciences workforce, which is about the same size overall.
RESEARCH TRAINING AND THE NATIONAL RESEARCH SERVICE AWARD PROGRAM
In general, the National Research Service Award (NRSA) program plays a smaller role in research training in the behavioral and social sciences than in the basic biomedical fields. Comparing the number of awards in Table 3-2 with a similar table in Chapter 2, the awards in the behavioral sciences are about one-tenth of those in the biomedical sciences. In terms of the percentage of students supported, less than 1 percent of the 40,000 graduate students in the behavioral and social sciences in 2002 had NRSA support. By comparison, about 9.3 percent of the biomedical sciences graduate students had NRSA support. It has been argued that much of the research in the behavioral and social sciences is not health related and that therefore, training in these research areas is not supportable under the NRSA program. The sample dissertation review, referred to at the beginning of this chapter, contradicts that reasoning because 90 percent of the reviewed dissertation abstracts were considered to be in areas fundable by NIH personnel.
NIH’s basic mission is to support health-related research, and NIH has historically tended to consider such research to lie primarily in the physical structure of the body and hence
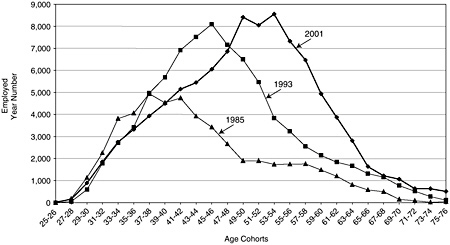
FIGURE 3-8 Age distribution of the behavioral and social sciences workforce, 1985, 1993, and 2001.
SOURCE: National Science Foundation Survey of Doctorate Recipients.
TABLE 3-2 National Research Service Award Predoctoral Trainee and Fellowship Support in the Behavioral and Social Sciences
|
|
1975 |
1980 |
1985 |
1990 |
1995 |
2000 |
2001 |
2002a |
|
Traineeships (T32)b |
204 |
479 |
495 |
577 |
410 |
434 |
321 |
240 |
|
Fellowships (F30, F31)b |
122 |
43 |
47 |
46 |
73 |
169 |
225 |
194 |
|
aFor 2002 and possibly 2001, the data are incomplete for traineeships since educational institutions report on the number of students trained in certain fields and the information was last processed in February 2003 bSee Appendix B for complete explanation of awards. SOURCE: NIH IMPACII Database. |
||||||||
in biochemistry, genetics, and similar fields. Behavioral and social sciences research has traditionally been considered less relevant to the NIH mission. This may also be seen in the fact that NIH does not house an institute devoted to basic and applied research in the behavioral and social sciences. What research training there is in this area has tended to reside in NIMH, but NIMH has a mission to focus on mental disorders. Consequently, training in research-relevant areas for many other health problems with a social and behavioral component (such as smoking, obesity, drug abuse, violence, alcoholism) has lagged far behind society’s needs. There may be added concerns for research training in the behavioral and social sciences by NIMH due to a recent decision by this institute to shift research funding to areas deemed to have more relevance to public health issues, such as neurological diseases and major mental disorders.2
Thus, research training in the behavioral and social sciences is not supported through a dedicated NIH institute or center but instead through the coordination of training and research by the Office of Behavioral and Social Science Research (OBSSR) in the Office of the Director. In recent years NIMH has supported a majority of the predoctoral trainees and fellows, followed by NICHHD, the NIA, the National Institute on Drug Abuse, the National Institute on Alcohol Abuse and Alcoholism, and the National Cancer Institute (NCI). A review of the 1,972 T323 training grants in 2002 showed that 98 were primarily in the behavioral and social sciences and about 150 others had some behavioral aspects to the training. Table 3-3 shows the distribution of the 98 awards across the NIH institutes and centers. Only 8 of the 21 institutes that could support T32 training made awards. NIMH far outnumbers the other institutes and centers for making these awards. If the institutes and centers with awards that contain behavioral aspects were included, this number would increase to 11 with the addition of the National Institute of Allergy and Infectious Diseases, the National Institute on Deafness and Other Communication Disorders, and the National Institute of Neurological Disorders and Stroke.
The institutes and centers listed in Table 3-3 are the principal supporters of behavioral and social sciences research and training, with combined expenditures of $1.7 billion in 2001. Another 14 institutes and centers also provided $295 million in support in 2001. While NCI is a major supporter of behavioral and social sciences research, it provides little NRSA program training support in this area. NCI has used the R25T training mechanism to support training programs focusing on behavioral, prevention, control, and population sciences. In 2004, NCI made six awards under this mechanism to support behavioral science training.
A particularly notable omission from the list of institutes that support training in the behavioral and social sciences is the National Institute of General Medical Sciences (NIGMS). A few behavioral and social sciences doctoral students receive NIGMS training support, but only under institutional NRSA training grants that are focused on biomedical or clinical training. At one time NIGMS did support behavioral training but now claims that such training falls outside its mission. NIGMS has resisted calls from Congress to
TABLE 3-3 T32 Training Grants in the Behavioral and Social Sciences, 2002
|
NIH Institutes |
Number |
|
National Institute on Alcohol Abuse and Alcoholism (NIAAA) |
4 |
|
National Institute on Aging (NIA) |
6 |
|
National Institute on Drug Abuse (NIDA) |
6 |
|
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDKD) |
2 |
|
National Institute of Child Health and Human Development (NICHD) |
13 |
|
National Institute of Mental Health (NIMH) |
46 |
|
National Institute of Nursing Research (NINR) |
7 |
|
National Heart, Lung, and Blood Institute (NHLBI) |
10 |
|
SOURCE: Tabulation from NIH IMPACII Database. |
|
|
2 |
Agres, T. 2002. |
|
3 |
See Appendix B for a complete explanation of awards. |
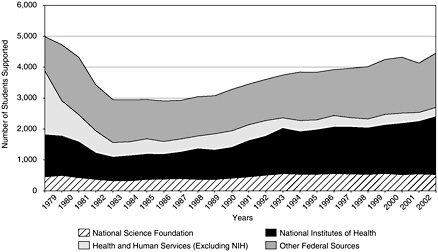
FIGURE 3-11 Funding sources for graduate education in the behavioral and social sciences, 1979–2002.
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
develop collaborations with other institutes and centers at NIH to support behavioral research.4
Institutes and centers tend to support training in the behavioral and social sciences that is directed at particular subfields and often do not require interdisciplinary or multidisciplinary aspects generally found in training grants in the biomedical or clinical sciences. In order to encourage interdisciplinarity, it should not be forgotten that training support in the behavioral and social sciences promotes outreach and collaboration with other sciences.
The lack of support notwithstanding, efforts are being made by OBSSR to foster interdisciplinarity by highlighting research that joins the behavioral and social sciences with other health sciences. In July 2002, OBSSR held a workshop on interdisciplinary training in the behavioral, social, and biomedical sciences. It addressed a variety of issues, including the type and level of training, barriers that prevent investigators from doing interdisciplinary research, relevant fields for interdisciplinary training, and what fraction of the NIH training portfolio should support interdisciplinary training. More recently a working group for the NIH Advisory Council to the Director in a draft report recommended that OBSSR coordinate transinstitute basic research initiatives, and designate a home at NIH to foster basic behavioral and social sciences research that is not linked to the mission of the categorical institutes and centers.5
The M.D./Ph.D. programs, particularly the Medical Scientist Training Program (MSTP) at NIGMS, foster interdisciplinarity. The MSTP was recently expanded to include Ph.D. study in the computer sciences, social and behavioral sciences, economics, epidemiology, public health, bioengineering, biostatistics, and bioethics. However, only a few institutions have students pursuing dual degrees with a Ph.D. in the behavioral and social sciences. The areas of computer science, biostatistics, and bioinformatics seem to be more attractive. Some institutions with well-established programs have expressed difficulty in developing a unified M.D./Ph.D. program with their behavioral and social sciences departments. Generally, the MSTP programs are housed in a biomedical sciences department or a medical school, and as such students are more likely to pursue biomedical research paths.
As shown in Figure 3-2, less than one-quarter of the graduate student population in doctoral-granting institutions in the behavioral and social sciences is supported by fellowships, traineeships, and research grants. While one of the missions of the National Science Foundation (NSF) is the support of the behavioral and social sciences, NSF support is only about one-tenth the total federal support and less than one-third of the support provided by NIH (see Figure 3-11).
It should be noted that total graduate support has declined since the 1970s and early 1980s, mainly due to reductions by
|
4 |
Statement from the NIGMS justifying its 2003 budget request: “The Institute’s research training programs mirror the areas of science that fall within the mission of the National Institute of General Medical Sciences. Except for a few fields of inquiry, behavioral studies largely fall outside of the Institute’s research mission, and are instead deemed to be within the missions of other institutes at the National Institutes of Health.” Also see http://www.psychologicalscience.org/advocacy/issues/nigms_observer.cfm. |
|
5 |
Draft Report of the Working Group of the NIH Advisory Committee to the Director on Research Opportunities in the Basic Behavioral and Social Sciences, http://obssr.od.nih.gov/Activities/Basic%20Beh%20Report_complete.pdf, December 2, 2004. |

FIGURE 3-12 Graduate student support by NIH, 1979–2002.
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
the non-NIH part of the U.S. Department of Health and Human Services. The current number of graduate students supported by NIH is about the same as in the 1970s. However, the proportion with NIH support has declined due to an increase in the total number of graduate students. In proportion to the total number of graduate students, NIH support has declined since the 1970s. The form of support has also changed over time. In the 1970s and early 1980s, NIH supported mainly graduate fellowships and traineeships, but by the 1990s its support shifted to research grants. Consequently, by 2001 over two-thirds of the support provided by NIH was in the form of research grants, and in 2002 it grew again by about 15 percent (see Figure 3-12).
As is the case at the predoctoral level, NRSA program support of postdoctoral training in the behavioral and social sciences is a fraction, between 10 and 15 percent, of that in the biomedical sciences (see Table 3-4). The decline in the number of postdoctoral positions supported by the NRSA program is similar to that in the biomedical sciences. This may be due to similar reasons: the higher stipend levels and the eligibility of individuals for NRSA support. There are no data on general postdoctoral support from NIH, but the picture for postdoctoral training support from all federal sources also shows growth in research grant support and the decline in trainee and fellowship support (see Figure 3-13). NIH’s efforts to shift research training in the behavioral and social
TABLE 3-4 National Research Service Award Postdoctoral Trainee and Fellowship Support in the Behavioral and Social Sciences
|
|
1975 |
1980 |
1985 |
1990 |
1995 |
2000 |
2001 |
2002a |
|
Traineeships (T32)b |
29 |
173 |
334 |
254 |
281 |
240 |
207 |
108 |
|
Fellowships (F32)b |
131 |
99 |
83 |
76 |
94 |
102 |
109 |
111 |
|
aFor 2002 and possibly 2001, the data are incomplete for traineeships since educational institutions report on the number of students trained in certain fields and the information was last processed in February 2003. bSee Appendix B for a complete explanation of awards. SOURCE: NIH IMPACII Database. |
||||||||
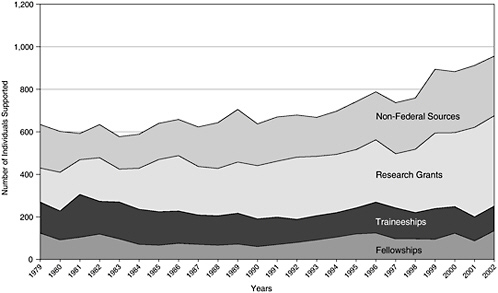
FIGURE 3-13 Academic postdoctoral support in the behavioral and social sciences, 1979–2002.
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
sciences from the predoctoral to the postdoctoral level in the late 1970s and 1980s can be seen by comparing predoctoral support level in Figure 3-12 and postdoctoral support in Figure 3-13.
The discussion in Chapter 2 of an outcomes analysis for NRSA- and non-NRSA-supported researchers at the predoctoral and postdoctoral levels presented a case for reversing the trend toward more training on research grants. For the behavioral and social sciences, the same conclusions cannot be drawn. The most recent assessment of the career outcomes of NRSA predoctoral trainees and fellows in the behavioral and social sciences did not yield results that were clear-cut evidence. NRSA trainees and fellows, particularly those who received support at the start of graduate school, completed their Ph.D.s faster than other students, but there was no clear difference with regard to employment or research productivity. These findings should be interpreted with caution though since the number of trainees supported under the NRSA program is smaller in the behavioral and social sciences, and the sample used to assess the outcomes is also smaller and more prone to error.
RESEARCH LABOR FORCE PROJECTIONS
As mentioned earlier in this chapter, individuals with doctorates in clinical psychology are considered part of the research workforce and as such may tend to overestimate the size of the actual workforce. Another uncertain component of the workforce are foreign-trained researchers now in the United States. Characterizing this component has proven problematic for the other two broad fields but is less so in the behavioral and social sciences since they appear to make up a small fraction of the population. The 1990 U.S. Census data estimate this group at about 3 percent of the workforce, and data from the U.S. Department of Education Survey of Postsecondary Faculty place the faculty percentage a little lower, at about 2 percent. In either case the numbers are small and will not have a significant effect on the projections. Table 3-5 shows the change in this workforce for U.S.-educated Ph.D.s over the past decade. A comparison of this workforce with that in the other broad fields shows a similar unemployment rate for those seeking employment and a rate for those not seeking employment similar to the biomedical sciences. As expected, the proportion of postdoctoral positions is lower than in the biomedical sciences and similar to that in the clinical sciences.
A life-table estimate of the science and engineering workforce in the behavioral and social sciences for the next 10 years is less problematic, since the variability introduced by the foreign doctorates is much less. The following is a short summary of the findings from the life-table analysis; full details can be found in the Appendix D.
TABLE 3-5 Potential Workforce in the Behavioral and Social Sciences by Employment Status, 1991–2001
|
|
1991 |
1993 |
1995 |
1997 |
1999 |
2001 |
|
Employed in S&E |
74,814 |
80,327 |
82,674 |
89,570 |
93,796 |
97,010 |
|
Percentage |
86.3 |
86.3 |
84.4 |
86.6 |
86.0 |
85.1 |
|
Employed out of S&E |
8,424 |
8,576 |
10,513 |
7,807 |
8,914 |
10,644 |
|
Percentage |
9.7 |
9.2 |
10.7 |
7.5 |
8.2 |
9.3 |
|
Unemployed, seeking work |
1,396 |
1,098 |
573 |
672 |
972 |
789 |
|
Percentage |
1.6 |
1.2 |
0.6 |
0.6 |
0.9 |
0.7 |
|
Unemployed, not seeking, not retired |
1,439 |
2,296 |
2,342 |
2,784 |
3,204 |
3,418 |
|
Percentage |
1.7 |
2.5 |
2.4 |
2.7 |
2.9 |
3.0 |
|
Postdoctorates |
606 |
813 |
1,868 |
2,631 |
2,164 |
2,136 |
|
Percentage |
0.7 |
0.9 |
1.9 |
2.5 |
2.0 |
1.9 |
|
Total |
86,679 |
93,110 |
97,970 |
103,464 |
109,050 |
113,997 |
|
SOURCE: National Science Foundation Survey of Doctorate Recipients. |
||||||
Graduates from U.S. Ph.D. programs will be the major contributor to the future workforce in the behavioral and social sciences, but since that population has shown little or no growth in the past, the projected growth and that of the workforce will be small. Table 3-6 shows the results of the multistate life-table analysis for the period from 2001 to 2011 under the median scenarios.
The projected median growth scenario for Ph.D. graduates increases from 4,221 in 2001 to only 4,619 in 2011, or about 0.5 percent per year. The inflow of foreign-trained Ph.D.s is only about 100 per year. Given this and the slow growth in the number of doctorates for U.S. institutions, the employed workforce is projected to grow from 102,193 in 2001 to 119,840 in 2011. This translates into about a 17 percent growth in the workforce and an annual growth rate of about 1.5 percent. This is the lowest growth rate of the three broad fields. The other segments of the workforce, except for postdoctoral appointments, are projected to decline over
TABLE 3-6 Projected Workforce by Status for the Median Scenario, 2001–2011
|
|
2001 |
2002 |
2003 |
2004 |
2005 |
2006 |
2007 |
2008 |
2009 |
2010 |
2011 |
|
U.S. Doctorates |
|||||||||||
|
Workforce |
113,997 |
116,267 |
118,368 |
120,408 |
122,375 |
124,247 |
125,960 |
127,497 |
128,868 |
130,101 |
131,154 |
|
Employed in S&E |
99,146 |
101,902 |
104,256 |
106,418 |
108,416 |
110,281 |
111,957 |
113,432 |
114,729 |
115,887 |
116,874 |
|
Out of science |
10,644 |
10,615 |
10,566 |
10,534 |
10,533 |
10,530 |
10,521 |
10,519 |
10,526 |
10,534 |
10,532 |
|
Unemployed |
789 |
565 |
496 |
468 |
453 |
449 |
451 |
457 |
462 |
466 |
468 |
|
Unemployed, not seeking |
3,418 |
3,185 |
3,050 |
2,989 |
2,974 |
2,988 |
3,031 |
3,089 |
3,151 |
3,215 |
3,281 |
|
Postdoctorates |
2,391 |
2,527 |
2,651 |
2,746 |
2,842 |
2,905 |
2,968 |
3,021 |
3,072 |
3,109 |
3,144 |
|
Foreign Doctorates |
|||||||||||
|
Workforce |
3,469 |
3,470 |
3,465 |
3,454 |
3,438 |
3,423 |
3,411 |
3,395 |
3,376 |
3,349 |
3,312 |
|
Employed in S&E |
3,047 |
3,049 |
3,046 |
3,046 |
3,041 |
3,038 |
3,036 |
3,030 |
3,018 |
2,997 |
2,966 |
|
Out of science |
313 |
300 |
294 |
282 |
269 |
258 |
247 |
239 |
233 |
227 |
223 |
|
Unemployed |
5 |
12 |
13 |
13 |
13 |
12 |
13 |
12 |
11 |
11 |
10 |
|
Unemployed, not seeking |
104 |
108 |
111 |
112 |
113 |
113 |
114 |
113 |
114 |
113 |
112 |
|
Postdoctorates |
69 |
69 |
69 |
70 |
71 |
73 |
73 |
74 |
75 |
74 |
74 |
|
Total |
|||||||||||
|
Workforce |
117,466 |
119,737 |
121,833 |
123,862 |
125,813 |
127,670 |
129,371 |
130,892 |
132,244 |
133,450 |
134,466 |
|
Employed in S&E |
102,193 |
104,951 |
107,302 |
109,464 |
111,457 |
113,319 |
114,993 |
116,462 |
117,747 |
118,884 |
119,840 |
|
Out of science |
10,957 |
10,915 |
10,860 |
10,816 |
10,802 |
10,788 |
10,768 |
10,758 |
10,759 |
10,761 |
10,755 |
|
Unemployed |
794 |
577 |
509 |
481 |
466 |
461 |
464 |
469 |
473 |
477 |
478 |
|
Unemployed, not seeking |
3,522 |
3,293 |
3,161 |
3,101 |
3,087 |
3,101 |
3,145 |
3,202 |
3,265 |
3,328 |
3,393 |
|
Postdoctorates |
2,460 |
2,596 |
2,720 |
2,816 |
2,913 |
2,978 |
3,041 |
3,095 |
3,147 |
3,183 |
3,218 |
|
SOURCE: NRC Analysis, See Appendix Tables D-9, D-11, and D-12. |
|||||||||||
the same 10-year period. Postdoctoral appointments in the behavioral and social sciences have increased over the past decade, and this is projected to continue, with about one-third more doctorates in postdoctoral positions in 2011 than in 2001. Unemployment is projected to remain low and even decline to about 0.4 percent of the potential workforce in 2011.
CONCLUSION
In assessing the overall picture for the behavioral and social sciences, the situation is similar to that for the biomedical sciences—namely, unemployment is low and the number of Ph.D.s entering the job market in the future is consonant with reasonable expectations about job availability. Appendix D discusses the uncertainties in the workforce model used to generate this conclusion. Based on this limited model, the status quo appears appropriate. However, all of these conclusions need to be placed in a broader context, which will be discussed in Chapter 10.
Finally, the NRSA program plays a special role in setting standards and attracting people to specific fields. This is vital for the health of the training system. A marked difference in training in the behavioral and social sciences relative to the biomedical sciences is in the concentration of support in a single institute, the NIMH. Because of the interdisciplinary nature of the subject matter and its general importance to the health of the nation, this does not seem desirable. A better distribution of training support across all NIH institutes and centers (including NIGMS) would be preferable. A specific recommendation in this regard is made in Chapter 5, but this issue also merits mention here.
RECOMMENDATIONS
Recommendation 3-1: This committee recommends that the total number of NRSA program positions in the behavioral and social sciences should remain at least at the 2003 level. Furthermore, the committee recommends that training levels after 2003 be commensurate with the rise in the total extramural research funding in the biomedical, clinical, and behavioral and social sciences.
Data on the number of predoctoral and postdoctoral traineeships in the behavioral and social sciences are incomplete after 2000.6 In 2000 there were 434 predoctoral trainees and 240 postdoctoral trainees. There was an 8.5 percent increase in the total number of predoctoral NRSA positions from 2000 to 2003 and an 8.4 percent increase in postdoctoral NRSA training positions. Assuming these increases also held for the behavioral and social sciences, approximately 471 predoctoral and 260 postdoctoral NRSA training slots would have been filled in the behavioral and social sciences in 2003. Fellowship data are probably more current, since these awards are made to individuals in specific training areas, and the predoctoral and postdoctoral awards in 2002 were 194 and 111, respectively. This level of predoctoral support was probably also true for 2003, since there was little change in the total number of NRSA fellowships from 2002 to 2003. Therefore, the total number of individuals in the behavioral and social sciences supported by the NRSA mechanism in 2003 is about 665 at the predoctoral level. This is only a small fraction of the total support for graduate students. Much more comes from institutional support through teaching assistantships and self-support. Similarly, postdoctoral support is more likely to come from research grants and other forms of institutional support (see Figure 3-13).
The recommendation links the training level in the behavioral and social sciences to extramural research support across NIH, since all of the three broad fields for which NRSA training is available are becoming more interdisciplinary and training is needed to meet this trend. While NIH currently classifies research grants into a single area of research, it is also quick to recognize that the research may involve many fields and that expertise is needed in these fields to carry out the research.
The relatively low unemployment among Ph.D.s in the behavioral and social sciences suggests that having 2003 serve as a baseline for NRSA program support and having increases based on increases in extramural research support are both justified.
The discussion following Recommendation 2-1 with regard to the quality of the NRSA program and the relative balance of biomedical training to the workforce also applies to the behavioral and social sciences.
Recommendation 3-2: This committee recommends that each NIH institute and center incorporate the behavioral and social sciences into its training portfolio, including institutes and centers that have not emphasized these disciplines in the past.
The behavioral and social sciences are critical for the understanding, prevention, and treatment of most major health problems. For historical rather than rational reasons, most training has been centered in just a few NIH institutes and centers. In the case of NIGMS, Congress specifically instructed that the behavioral and social sciences be included, but this has not been done as of 2004. The result is that health decisions that arise in many institutes and centers are made without sufficient input from scientists and decision makers who have knowledge of and training in the techniques of the behavioral and social sciences.