4
Clinical Sciences Research
The importance of clinical research is that it brings basic biomedical discoveries to the bedside to address patient care from the physical, behavioral, and social perspectives. It is also difficult to define the scope of this research. Perhaps the best definition of clinical research is the one developed in 1998 at the Graylyn Development Consensus Conference: Clinical research is that component of medical and health research intended to produce knowledge valuable for understanding human disease, preventing and treating illness, and promoting health.1
Clinical research embraces a continuum of studies involving interactions with patients, diagnostic clinical materials or data, or populations in any of the following categories: (1) disease mechanisms (etiopathogenesis); (2) bidirectional integrative (translational) research; (3) clinical knowledge, detection, diagnosis, and natural history of disease; (4) therapeutic interventions, including clinical trials of drugs, biologics, devices, and instruments; (5) prevention (primary and secondary) and health promotion; (6) behavioral research; (7) health services research, including outcomes, and cost effectiveness; (8) epidemiology; and (9) community-based trials.2
Clinical research and its translation into preventive and clinical care, in other words, are the primary means by which the nation’s health care goals are fulfilled. It brings basic biomedical research to the bedside through the translation of increasingly remarkable basic research advances—such as the sequencing of the human genome—into human applications and into social, behavioral, and health care practice.
Nevertheless, these transformations do not happen in a vacuum. Health services research has become indispensable to understanding and informing the future of health care. Despite the promises of a newly competitive marketplace for health services, the costs of health care to all stakeholders have resumed their double-digit annual rise after a short hiatus in the late 1990s. Recent reports from the Institute of Medicine have highlighted the unacceptably poor status of the health care system as a whole3 and the consequences of the continuing problem of the lack of insurance.4 Others have described in great detail the impact of the organizational, administrative, financing, safety, access, and other deficits of the nation’s cobbled-together health care “system” on individuals, communities, businesses, and the entire nation. These persistent challenges, along with the reemergent cost growth issue, make it increasingly important that clinical research not only deal with scientific advances per se but that it encompass the assessment of health outcomes, cost effectiveness, finance, access, and other research related to the deployment and utilization of the nation’s health care services.
Despite its critical importance, the clinical research enterprise has for years been underdeveloped. Reasons include the extra time required for clinical research training; the difficulty in competing for sponsored research support; the inability to cross-subsidize clinical research from hospital and faculty practice income (as a result of major changes wrought in health care financing over the past 15 years); the debt burden that inclines many physicians in training to forgo opportunities for clinical research and focus instead on clinical care; and the unresolved status of clinical research within the culture of the academic health center, where basic science studies or clinical prowess are often valued more highly than clinical research.
This problem of clinical research underdevelopment has now been recognized as a critical issue to be addressed within funding programs—public, private, and philanthropic—and throughout the research community itself. For example, in FY 2001 the National Institutes of Health—the single largest public-sector source of funding for clinical research—awarded more than $6 billion in clinical research grants (con-
stituting 37 percent of its total extramural research dollars). Among the successful innovations supported by these funds have been a nationwide network of general clinical research centers, where an estimated 9,000 researchers pursue a broad range of clinical research projects.5 Nevertheless, the past two decades have been particularly challenging for the funding of all health professions, and especially for the support of research activities in the clinical environment that are not clearly tied to specified funding streams. Clinical research has yet to achieve the breadth and depth of currency (double entendre intended) it deserves.
Meanwhile, a key element in developing the nation’s clinical research capacity is the building of a robust cadre of clinician-scientists able to realize the promise of 21st-century medicine. This objective depends, in turn, on continuing support, incentives, and educational and professional reforms throughout the existing clinical research workforce.
DEFINING THE CLINICAL RESEARCH WORKFORCE
The clinical research workforce is as diverse as the definition of the field. It is composed of individuals with doctorates in the basic sciences, graduates of professional degree programs, graduates of health sciences and public health programs, and dual- or multiple-degree holders covering a wide range of health care research. Given the broad role these scientists play in providing the nation’s health care—their research spans the spectrum from discovery to delivery—it is difficult to categorize them. For this report efforts will be made to identify individuals who fit the Graylyn definition. However, this definition is very broad. For example, it includes behavioral and social sciences research in the context of patient care, and it is difficult to separate this from the general area of health-related behavioral research that is addressed in Chapter 3. Many of them are involved in health services research (Chapter 7) and in other efforts that are increasingly interdisciplinary (Chapter 8). However, aspects of all these activities will be incorporated into the analysis of clinical research, as appropriate.
Apart from the problem of technically distinguishing the areas in which the clinical workforce conducts its research, it is also difficult to match these areas with workforce members’ credentials—current databases focus on the specific degree and field of training for individuals and not on their research areas. This problem has hindered prior studies of the National Research Service Award (NRSA) program to the point where only partial descriptions of the workforce were given and no demographic projection of future workforce was made.
For this assessment’s purposes, the basic workforce analysis will include Ph.D.s with degrees in the health fields listed in Appendix C, the fraction of the M.D. population in medical school clinical departments that conduct NIH-supported research, and doctorates with degrees from foreign institutions who are in some way identified as clinical researchers. This formula still does not capture the complete workforce, such as M.D.s in the non–medical school part of an academic institution or in industrial laboratories. Those doing clinical trials are also difficult to identify, as departments have different ways of allocating funds for clinical trials and of supporting associated researchers (from graduate students to postdoctorates to faculty). However, each of these groups will be included in the analysis when data are available. The nursing and dental workforces, as well as the health services researchers briefly mentioned above, will also be included in clinical research, but because each of these fields has its own special workforce issues, they will be examined separately in Chapters 5, 6, and 7.
EDUCATIONAL BACKGROUND
The educational background of clinical researchers is difficult to assess in the same detail as that of biomedical and behavioral and social sciences since a small fraction of M.D. graduates enter the research workforce. However, data are available on the Ph.D. portion of this workforce, and these data can be analyzed. In particular, the graduate student population in the clinical departments of doctorate-granting institutions grew at an annual rate of 5 to 10 percent in the 1990s; it then leveled off until 2002, when there was growth of about 6 percent (see Figure 4-1). This growth pattern of the number of clinical research–oriented graduate students is much different than that of the biomedical sciences, whose population was virtually constant during the 1990s. Its growth in 2002, as in the other fields, may reflect a poor economy—where continued education is an alternative to the job market. It should also be noted that the growth was primarily caused by an increase in female graduate students and that nursing graduate students were excluded from the data (as most will not receive a doctorate).
The pattern of financial support for clinical science students is also quite different from that of the other fields (see Figure 4-2). Many more are self-supported, and research and teaching assistantships make up a smaller proportion. As is the case for the other broad fields, the number of graduate students supported on research grants has grown, while levels of assistantships, traineeships, and fellowships have been constant from the 1970s until now. The growth in self-support in 2002 is consistent with the general increase in graduate student populations and the limited forms of support available from external and institutional funds.
The growth in the graduate population is reflected by the number of doctorates in the clinical sciences, which increased by a factor of 5 from the early 1970s (see Figure 4-3). This increase is largely the result of growing participation by women. The proportion of male doctorates in the
|
5 |
NIH competing and noncompeting research grants, fiscal years 1992–2002. Available at: http://grants.nih.gov/grants/award/research/rgmechtype9202.htm. |
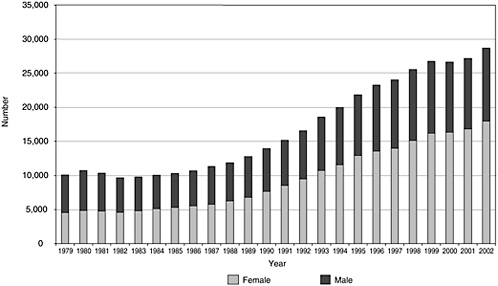
FIGURE 4-1 Graduate students in clinical departments by gender, 1979–2002 (does not include graduate students in nursing).
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
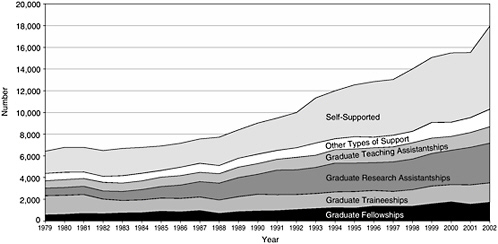
FIGURE 4-2 Type of support for graduate students in clinical sciences departments, 1979–2002 (does not include graduate students in nursing).
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
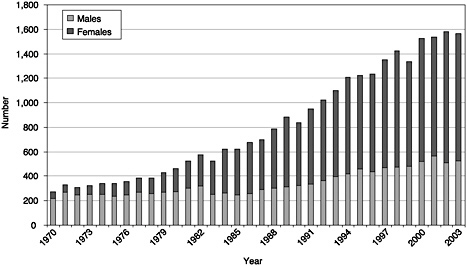
FIGURE 4-3 Doctorates in the clinical sciences by gender, 1970–2003.
SOURCE: National Science Foundation Survey of Earned Doctorates, 2001.
1990s was about 35 percent, but dropped below that level in 2002 and 2003, reflecting the decline in the male graduate student population in 2000 and 2001.
The citizenship pattern of clinical sciences doctorates, with only about 20 percent awarded to temporary residents and 5 percent to permanent residents, differs from that of the biomedical sciences. However, minority participation is similar to that of the biomedical sciences, accounting for only about 7 percent of the degrees in 2002 (see Appendix E).
In comparison to the biomedical as well as the behavioral and social sciences, clinical sciences differs significantly in time to doctoral degree and age at time of degree. Since the late 1990s, clinical sciences doctorate time to degree has been near or over 10 years, compared to about 7.5 years in the biomedical sciences and 8.5 to 9 years in the behavioral and social sciences. The age of clinical sciences doctorates at the time of receipt of their degrees averages 38 for clinical scientists, while doctorates in the other fields typically receive their degrees in their early thirties (see Appendix E). Moreover, of the three fields, clinical sciences doctorates are the least likely to have postdoctoral training. About 25 percent traditionally plan such training, in contrast to 70 percent of graduates in the biomedical sciences and 36 percent in the social and behavioral sciences.
It should be noted that these characteristics apply only to the U.S.-trained doctorates that will potentially make up the clinical research workforce. Some M.D.s and Ph.D.s with degrees from foreign institutions become part of this workforce as well, but data on this group are incomplete. Nevertheless, some indication of its contribution can be obtained from academic data. In 2002 of the 12,750 individual postdoctoral appointments in academic clinical departments, nearly 2,200 were U.S. citizens or permanent residents with M.D. degrees and 6,700 were temporary residents, a large proportion of whom were probably foreign educated with an M.D. or a Ph.D. degree. Given that the average postdoctoral appointment is 2 or 3 years and assuming that at least 50 percent of these doctorates will stay in the United States, some 2,000 researchers could be added each year to the country’s clinical workforce. The above is only a partial estimate of the supply of clinical researchers, however, because M.D.s and foreign-educated doctorates could take postdoctoral training in the nonacademic sectors or have no postdoctoral training.
THE CLINICAL RESEARCH WORKFORCE
Because clinical research is conducted by individuals with different degrees and no single data source comprehensively captures their activities, it is best to look at the clinical research workforce from the perspective of the different degrees that lead to becoming a clinical researcher. The basic workforce is the 17,180 doctorates with a Ph.D. in the clinical fields listed in Appendix C and as characterized in Appendix E, Table E-6. In addition, in 2001 the Association of American Medical Colleges (AAMC) roster of medical school faculty identified another 3,090 M.D.s with U.S. doc-
torates and R01 support as well as 750 individuals with Ph.D.s from foreign institutions and R01 support, for a total of about 21,000. A slightly different result is obtained from 2001 NIH data, which counted 4,563 M.D. principal investigators with R01 support, bringing the total for M.D.s and Ph.D.s to just under 22,500. However, neither of these counts captures the clinical researchers in the M.D. population who are not principal investigators on R01 grants; this could increase the M.D. research population by a factor of 2 or 3.
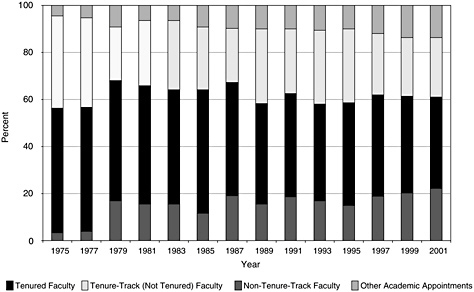
As was the case with the educational characteristics of clinical doctorates, data on their career progression and employment characteristics are only well known for Ph.D.s from U.S. institutions (Appendix E). This workforce has grown significantly over the past three decades, rising from about 2,500 in the early 1970s to about 17,000 in 2001 (see Figure 4-4). Much of this growth was in the academic sector, but the industrial sector also showed a significant increase. The growth in the academic sector in recent years has mainly resulted from the employment of non-tenure-track faculty and other academics (usually research associates; see Figure 4-5).
Tenured and tenure-track faculty still form the majority in academia, but their percentage fell from around 80 percent in the mid-1980s to 64 percent in 2001. This decline was not unexpected, given the tendency of many fields in recent years toward temporary or soft-money positions.
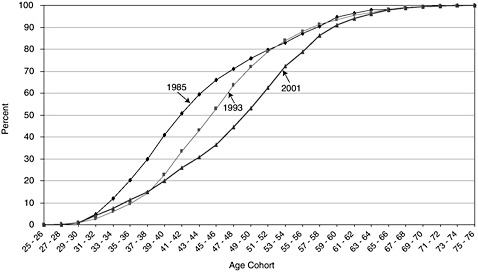
A major concern for the clinical research enterprise is the increase in the average age at which individuals receive their doctorates; this and other factors have contributed to the aging of the workforce. Between 1985 and 2001, the median age of the workforce increased from the 41- to 43-year cohort to the 49- to 50-year cohort (see Figure 4-6).
The Ph.D. workforce age distribution is greater by a few years on average than the age distribution for M.D. clinical researchers in medical schools. For example, the median age of Ph.D. clinicians is 50, while that of research clinical faculty in medical schools is a little under 47 (see Figure 4-7).
The declining interest of new doctorates in postdoctoral training is shown in Appendix E, Table E-5. Only a few hundred (about 2 percent) U.S.-trained clinical sciences doctorates held postdoctoral positions in recent years, and almost all of these positions were in academic institutions. However, the picture is somewhat different if the academic postdoctoral pool is examined on the basis of institutions’ clinical departments. In 2002 there were almost 4,000 U.S. citizen or permanent resident Ph.D.s in these positions (see Figure 4-8). The number of temporary residents was about the same, but their percentage, like that of the biomedical sciences, was increasing. The difference between the data reported in Table E-6 and the data in Figure 4-8 is probably due to Ph.D.s with biomedical doctorates moving into clinical departments for training purposes.
Table E-6 shows that minorities represented 8.7 percent of the clinical research population in 2001, even though their numbers had grown from about 100 in 1973 to a little over 1,000 in 2001. This percentage is greater than in the bio-
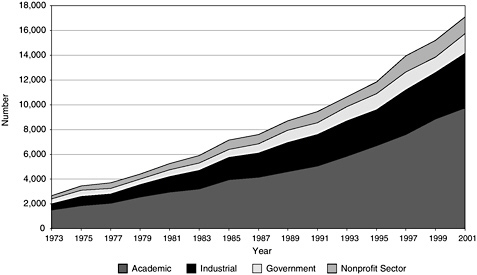
FIGURE 4-4 Employment sectors in the clinical sciences, 1973–2001.
SOURCE: National Science Foundation Survey of Doctorate Recipients.
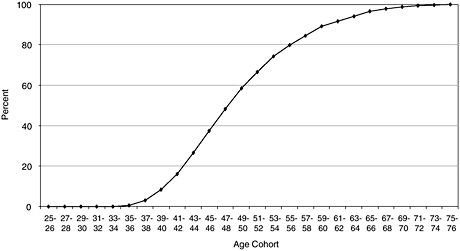
FIGURE 4-7 Age distribution of research clinical faculty in medical schools, 2002.
SOURCE: American Association of Medical Colleges Faculty Roster Database.
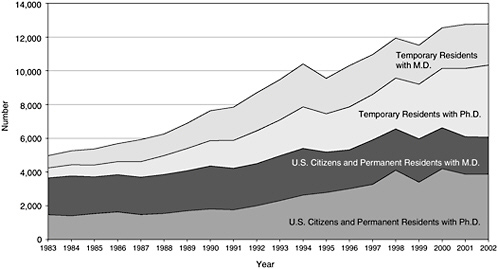
FIGURE 4-8 Postdoctoral appointments in clinical departments by citizenship and degree.
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
medical sciences and about the same as that of the behavioral and social sciences. The data show, as in the other fields, a small number of temporary residents in the research population, but these are only individuals who were trained in U.S. institutions. There may actually be a larger percentage of temporary residents in the workforce when those with foreign doctorates are included.
The discussion until now has dealt only with part of the clinical sciences workforce (Ph.D.s), but medical doctors also participate in research. As seen in Figure 4-8, a number of M.D.s hold postdoctoral positions in clinical departments. In 2002 the number of postdoctoral positions occupied by U.S. citizens, permanent residents, and temporary residents was almost equally shared by M.D.s and Ph.D.s. However, the number of citizens/permanent residents, which was fairly constant in the late 1990s, is now declining, while the number of temporary residents in these positions is growing. This may also be a sign of the decreased postdoctoral participation noted in other fields by U.S. doctorates.
The number of domestic- and foreign-trained M.D. researchers on medical school faculties is estimated at 3,700. An additional 1,585 M.D./Ph.D.s received NIH support. About 40 percent of the M.D. grants were in clinical research areas, and 20 percent of the grants to M.D./Ph.D.s would be for clinical research. Therefore about 1,800 M.D. or M.D./ Ph.D. researchers should be added to the 17,000 Ph.D.s educated in U.S. institutions in clinical fields. Although this brings the total to at least 18,800 clinical researchers, it is probably an underestimate, since a significant number of M.D.s work in industry to conduct or support clinical trials in the pharmaceutical and biotechnology companies, and the government employs M.D.s as researchers in its hospitals and laboratories. Also, about 15 percent of medical school faculties consist of researchers with foreign-earned doctorates; if this is typical, the above estimate should be increased again by 10 to 15 percent to at least 21,000.
While the exact number of M.D. clinical researchers is not known, it appears that individuals with Ph.D.s have dominated the field in recent years. There does not appear to be a change in the number of M.D.s in clinical research since the 1970s. While only 2,600 Ph.D.s made up the workforce and only a few hundred degrees were awarded each year in the 1970s, the Ph.D. workforce has since grown by a factor of 7. There may be several reasons for this change, but a logical one is the increased education debt incurred by medical school graduates. Most physicians and dentists today begin their professional careers with sizable education debts (though graduates of dual-degree—M.D.-Ph.D. or D.D.S.-Ph.D.—programs are the exception). From 1991 to 2001 the average medical school debt of M.D. graduates increased more than 50 percent, from almost $43,000 (in 2001 dollars) to just over $70,000. The level of educational debt for dental students is even higher—in 2001 it was over $75,000. This is primarily because dental students must purchase their dental instruments during their clinical training.
Although health care professionals are permitted to postpone payments on their student loans during NRSA or other authorized research training programs, this option may not be widely used. Even if it were, the fact is that additional training places its own financial and other burdens on young physicians. They must find time for research—an increasingly difficult challenge—particularly for those working in today’s highly competitive health care market. Another obstacle for physician-investigators has been the limitation on salaries for NIH-funded investigators. It is now set at $175,000. While that is not an insignificant sum, it is below what many practicing clinicians or medical faculty can earn.
The M.D./Ph.D. programs were created as a way to bring more M.D.s into clinical research, but as noted earlier only about 20 percent of M.D./Ph.D.s pursue clinical research careers. Education debt does not appear to be the reason, as their debt averaged only about $15,000 in 2001. It is more likely that the research work they were exposed to during their Ph.D. program attracted them to a research career in the biomedical sciences instead.
Aside from the formal dual-degree programs, other mechanisms are being tried to encourage M.D.s to enter clinical research. Examples include master-level programs in special areas, such as Duke University’s academic training in quantitative and methodological principles of medical genomics. Such programs appear to be very popular and may help redirect more physicians into clinical research.
CLINICAL WORKFORCE ISSUES
For more than a decade now, concern has been expressed about the vitality of the clinical research enterprise. In 1997, Ahrens published a treatise that described the problems facing patient-oriented research and the economic and social factors that were driving the system.6 He called for special training programs and greater cooperation between clinically trained M.D.s and technically trained Ph.D.s. Many other similar commentaries have been written, expressing the fear that because clinical investigators are not renewing themselves, many of the modern-day advances in biomedical research are not being translated into patient care.7,8 For example, between 1983 and 1998 the number of physician-scientists decreased by 22 percent, from 18,535 to 14,479.9 Another indication of the gap between basic research and the application of that research is the decline from 1995 to 2001 in the number of M.D.s applying for and receiving F32 postdoctoral fellowships.
In response to these concerns, NIH established in 1995 a Director’s Panel on Clinical Research. A report issued in 1997, generally called the Nathan report (after its chairman,
David G. Nathan), made recommendations concerning the need for more data on clinical research, the training of investigators, the expansion of clinical research centers, and the creation of partnerships. Shortly thereafter, in 2000, Congress passed the Clinical Research Enhancement Act, which called on NIH to implement many of the Nathan report’s recommendations; and a 2003 Report Card later found that NIH had indeed implemented many of them.10 In the area of training and career progression, three new K awards were established for clinicians. These included the K23, to support the career development of young investigators in patient-oriented research; the K24, to provide release time for midcareer clinicians to focus on research or mentor young researchers in patient-oriented research; and the K30, to allow for the development of clinical research training programs. Table 4-1 shows the growth in these awards since their establishment in 1998.
These programs appear to be fulfilling their mission, since 80 to 90 percent of the applicants are M.D.s, and they enjoy a higher acceptance rate than the Ph.D. applicants. The programs have also led the way for other organizations, such as the Doris Duke Charitable Foundation and the Howard Hughes Medical Institute, to establish similar programs.
In terms of training, NIH responded to the panel’s report by encouraging internships at NIH for medical students and the establishment of a loan relief program that allows M.D.s to pay back their medical loans by making a 50 percent commitment to research for a period of 2 years. This program has been very successful in attracting physicians to research careers.
Other programs that appear to be successful at training clinical researchers come in the form of course work directed at physicians or Ph.D. students. For example, Duke University offers a master’s level program for clinical fellows to develop quantitative and methodological principles of clinical research. The program offers formal courses in research design, research management, and statistical analysis. Another example is the joint Harvard/MIT Medical Engineering Medical Physics Ph.D. program that is aimed at training Ph.D. scientists in both their physical science or engineering specialty and the fundamentals of clinical medicine. Other forms of these programs range from a single course to a formal degree program, and there is some evidence to show that the graduates participating in these programs follow a clinical research path and join clinical departments in medical centers.11,12
THE MEDICAL SCIENTIST TRAINING PROGRAM
Another effort aimed at addressing the shortage of individuals in translational research has been the establishment
TABLE 4-1 NIH Clinical Career Awards 1999–2002
|
Year |
K23 |
K24 |
K30 |
|
1999 |
142 |
81 |
35 |
|
2000 |
327 |
158 |
57 |
|
2001 |
496 |
215 |
57 |
|
2002 |
664 |
261 |
59 |
|
SOURCE: NIH IMPACII Database. |
|||
of dual-degree programs, such as the Medical Scientist Training Program (MSTP) at the National Institute of General Medical Sciences (NIGMS). This program, which dates back to the 1960s, has produced several thousand M.D./ Ph.D.s who are highly qualified researchers. While the intent of the MSTP program is to develop translational research, it has not brought large numbers of individuals into patient-oriented research. Part of the problem might be the lure of bench science research, but there is also a long training period for these physician-scientists, which includes a postdoctoral appointment, internship, and residency. In the process, physicians may lose some of their medical skills in that they are not practicing medicine full time. The combination of the time commitment, loss of skills, and administrative challenges of research on human subjects may make basic research more attractive than patient-oriented research.13,14
Another career path for physician-scientists regards “late bloomers” who have an M.D. and for some reason decide to forgo private practice and pursue a research career. This path is generally longer than that of the M.D./Ph.D.s, as it includes medical school, a residency program, subspecialty fellowship training, and then a period of 3 to 6 years of research training. Prior to the medical scientist training programs, nearly all physician-scientists followed this path. Now the M.D./Ph.D.s make up about 30 percent of physician-scientists, according to NIH grant statistics, and at present only 2.5 percent of medical school graduates decide later to become researchers. While M.D./Ph.D. researchers leave medical school with relatively low debt, the debt of late bloomers stands at about $100,000 upon graduation and continues to grow through residency and fellowship training. If an individual elects a research career, it is almost impossible to begin bringing down this debt while on a $40,000 research training salary.
While increases in the number of individuals supported through the MSTP program would help alleviate the shortage of clinical researchers, ways to attract the late bloomers into research are also needed. For now the loan repayment program introduced a few years ago as part of the Public
Health Improvement Act has helped reduce the debt problem and possibly direct physicians into research careers. However, the program is small, with only about 250 trainees per year in authorized patient-oriented research programs receiving up to $35,000 each year for 2 years for repayment of their medical school debts and an additional 39 percent of the repayments to cover federal taxes, and possible reimbursement of state taxes that result from these payments. Also, there is a debate about whether the program should be expanded to allow repayment for M.D.s entering basic research training programs. While the addition of M.D.s to the bench science workforce may strengthen this research area, the added dollars for the program may be more effectively spent in attacking the shortage of clinical researchers.
ROLE OF THE NATIONAL RESEARCH SERVICE AWARD PROGRAM
Earlier in this chapter, Figure 4-2 showed that clinical sciences graduate students’ level of support from traineeships and fellowships was relatively constant—at about 3,500 students—and it also showed a decrease in the importance of these external support since the 1980s, as the number of research assistantships grew steadily to over 3,600 in 2002. This change in overall support is similar to the support from NIH, with an increase in clinical sciences research assistantships to the point where their number is a little greater than the level of trainee and fellowship support in 2002, though not to the level seen in the biological sciences (see Figure 4-9). It should also be noted that the National Science Foundation provides very little support for graduates, with about 100 awards equally divided between fellowships and research assistantships. However, another major source of support is the non-NIH part of the U.S. Department of Health and Human Services (DHHS), which in 2002 supported about 400 students on traineeships or fellowships.
The levels of graduate student support and Ph.D. production in the 1990s shown in Figure 4-2 are also reflected in the rapid growth in NRSA support of predoctoral trainees and fellows (see Table 4-2). Like the other two broad fields in this study, support was rather constant in the 1990s but declined in 2001, possibly because of higher stipend levels and the fixed NRSA budgets for the training programs. The differences between the numbers shown in Table 4-2 and
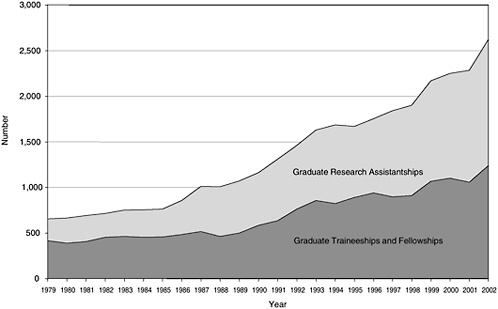
FIGURE 4-9 NIH predoctoral support in the clinical sciences, 1979–2002.
SOURCE: National Science Foundation Survey of Graduate Students and Postdoctorates in Science and Engineering.
TABLE 4-2 National Research Service Award Predoctoral Trainee and Fellowship Support in the Clinical Sciences
|
|
1975 |
1980 |
1985 |
1990 |
1995 |
2000 |
2001 |
2002a |
|
Traineeships (T32)b |
83 |
609 |
559 |
641 |
1,334 |
1,395 |
1,577 |
875 |
|
Fellowships (F30, F31)b |
4 |
129 |
44 |
151 |
108 |
126 |
143 |
151 |
|
aFor 2002 and possibly 2001, the data are incomplete for traineeships since educational institutions report on the number of students trained in certain fields and the information was last processed in February 2003. bSee Appendix B for a complete explanation of awards. SOURCE: NIH IMPACII Database. |
||||||||
Figure 4-9 are due to NRSA support through other DHHS agencies, such as the Agency for Healthcare Research and Quality.
Data on postdoctoral-level training support broken down by individual federal agency source are not collected, but information on the type of training—at least in academic institutions—is available (see Figure 4-10). The traineeships and fellowships portion of this support has been increasing at a slow rate, while the number of individuals on research grants has increased fivefold since the late 1970s.
The NRSA contribution to postdoctoral training support mirrors the general trend for fellows and trainees but at a lower level, given that support is available from sources other than NIH (see Table 4-3).
In addition to predoctoral and postdoctoral program support in the clinical sciences from the NRSA mechanism, dual-degree programs are another attractive option for health care professionals seeking clinical research training. Currently, NIH has three dual-degree training programs: (1) the MSTP, (2) the individual M.D./Ph.D. fellowships, and (3)
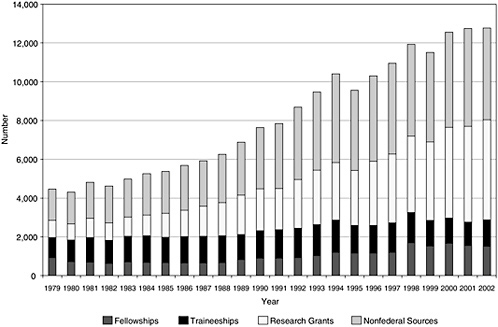
FIGURE 4-10 Academic postdoctoral support in the clinical sciences, 1979–2002.
SOURCE: National Science Foundation Survey of Doctorate Recipients.
TABLE 4-3 NRSA Postdoctoral Trainee and Fellowship Support in the Clinical Sciences
|
|
1975 |
1980 |
1985 |
1990 |
1995 |
2000 |
2001 |
2002a |
|
Traineeships (T32)b |
332 |
1,465 |
1,660 |
1,649 |
1,889 |
1,854 |
1,830 |
941 |
|
Fellowships (F32)b |
177 |
205 |
185 |
94 |
68 |
88 |
81 |
65 |
|
aFor 2002 and possibly 2001, the data are incomplete for traineeships since educational institutions report on the number of students trained in certain fields and the information was last processed in February 2003. bSee Appendix B for a complete explanation of awards. SOURCE: NIH IMPACII Database. |
||||||||
the Dental Scientist Training Program (DSTP). The MSTP is the largest and oldest program, dating back to 1964, and today is used to train about 1,000 students annually at 35 medical schools and universities. Fellowships for M.D./ Ph.D. training, a more recent development, were instituted in 1989 by the National Institute of Mental Health, the National Institute on Alcohol Abuse and Alcoholism, and the National Institute on Drug Abuse to encourage dual-degree training in the areas of mental health, behavior, and neuroscience. This much smaller fellowship program supports about 40 students a year. The most recent dual-degree training program is the DSTP, which was created following recommendations from the 1994 study of the NRSA program. However, the DSTP is small and supports only a few students at three dental schools.
These dual-degree programs are very attractive to M.D. or D.D.S. students because they provide several career options and result in lower levels of education debt. However, relatively few participants receive much-needed training in clinical research methods. In 1996 an analysis of the fields of study chosen by MSTP participants found that nearly 60 percent of graduates from the late 1980s and early 1990s received their Ph.D.s in five basic science fields: biochemistry, neuroscience, molecular biology, cell biology, and pharmacology. Further, in their subsequent research careers, MSTP graduates focused almost entirely on laboratory-oriented research, and they sought NIH funding for such research projects at the same rate as did Ph.D.s.
MSTP students are generally directed toward doctoral study in the basic biomedical sciences simply because their institutions are oriented toward laboratory research in these fields. Recognizing a need, NIGMS has issued new MSTP guidelines that urge medical schools with training grants to extend their programs across disciplines to give M.D./Ph.D. students “a breadth of doctoral research training opportunities” in fields that include computer science, the social and behavioral sciences, economics, epidemiology, public health, bioengineering, biostatistics, and bioethics.
However, most M.D./Ph.D. programs have been slow to respond, as evidenced by little change in the descriptions of the programs. Finding mechanisms that will encourage students in these dual-degree programs to conduct clinical research remains a challenge.
RESEARCH LABOR FORCE PROJECTIONS
The lack of data for characterizing the clinical sciences workforce makes it extremely difficult to make accurate predictions of this workforce. Using the limited data from the Survey of Doctorate Recipients, the AAMC Faculty Roster, and 1990 U.S. Census data on immigrants, the 2001 potential clinical research population was estimated at 25,283. This included a combination of 19,105 U.S.-trained Ph.D.s and M.D.s, together with 6,178 individuals with doctorates from foreign institutions. This included individuals in postdoctoral positions but did not count the 563 doctorates with degrees in clinical fields who are unemployed or the 1,700 who are in positions that would not be considered scientific or related to clinical research. The employed workforce in the clinical sciences is 23,020. Table 4-4 shows the change in this workforce over the past decade for U.S.-educated Ph.D.s. However, this is only part of the total potential workforce in that there are foreign-trained doctorates who are employed and a few U.S. doctorates who leave the country and return at a later time. Estimating this foreign component is difficult, however, as no database describes the demographics of this group. The AAMC and 1990 U.S. Census data were used to provide the total workforce estimates given above, but no time series or characteristics were available.
It is also difficult to estimate how the science and engineering workforce in the clinical sciences will change over the next 10 years. Its size is influenced by the number of doctorates graduating each year, unemployment levels in the field, the number of foreign-trained doctorates, and retirement rates. It is possible to estimate some of these factors for U.S.-trained Ph.D.s, but only crude estimates have been made for the M.D. and foreign-earned degree holders.
The following is a short summary of the findings from the life table for clinical researchers. An analysis and the full details can be found in Appendix D. Graduates from U.S. Ph.D. programs are the largest and most relevant source of new researchers. The size of this group grew significantly in
TABLE 4-4 Potential Workforce in the Clinical Sciences by Employment Status, 1991–2001
|
|
1991 |
1993 |
1995 |
1997 |
1999 |
2001 |
||
|
Employed in S&E |
9,111 |
10,424 |
11,506 |
13,716 |
14,779 |
16,765 |
||
|
Percentage |
89.9 |
87.1 |
83.7 |
88.1 |
86.6 |
87.8 |
||
|
Employed Out of S&E |
654 |
815 |
1,315 |
785 |
1,328 |
1,394 |
||
|
Percentage |
6.5 |
6.8 |
9.6 |
5.0 |
7.8 |
7.3 |
||
|
Unemployed, Seeking Work |
149 |
163 |
171 |
170 |
203 |
127 |
||
|
Percentage |
1.5 |
1.4 |
1.2 |
1.1 |
1.2 |
0.7 |
||
|
Unemployed, Not Seeking, Not Retired |
79 |
327 |
266 |
388 |
333 |
404 |
||
|
Percentage |
0.8 |
2.7 |
1.9 |
2.5 |
2.0 |
2.1 |
||
|
Postdoctorates |
140 |
234 |
485 |
514 |
431 |
415 |
||
|
Percentage |
1.4 |
2.0 |
3.5 |
3.3 |
2.5 |
2.2 |
||
|
Total |
10,133 |
11,963 |
13,743 |
15,573 |
17,074 |
19,105 |
||
|
SOURCE: National Science Foundation Survey of Doctorate Recipients. |
||||||||
the 1990s, and unlike the pattern in the biomedical sciences, this growth continued into 2001. Since there appears to be continuing growth in the workforce, only median estimates are presented here for the inputs to the life-table model. A constant-supply scenario is unrealistic, and continued strong growth might not be sustained. The annual number of U.S. Ph.D.s grows from 1,551 in 2001 to 1,807 in 2011, and the inflow of foreign-degree holders increases from 504 in 2001 to 708 in 2011. This estimate of growth in the foreign population is problematic, however, because it is based on estimates of the growth rate in the 1990s and the resulting population in 2001. Current immigration restrictions will have an impact on the number of foreign scientists who will be able to emigrate. Table 4-5 shows the results of the multistate life-table analysis for the period from 2001 to 2011, under the median scenarios. The 4 or 5 percent growth rate is much greater than in the biomedical sciences and in the 10-year period is projected to almost double.
Unemployment remains at 1 percent or less, and the portion of the workforce remaining in science is about 90 per-
TABLE 4-5 Projected Workforce by Status for the Median Scenario, 2001–2011
|
|
2001 |
2002 |
2003 |
2004 |
2005 |
2006 |
2007 |
2008 |
2009 |
2010 |
2011 |
|
U.S. Doctorates |
|||||||||||
|
Workforce |
19104 |
20177 |
21273 |
22368 |
23454 |
24536 |
25621 |
26694 |
27744 |
28785 |
29818 |
|
Employed in S&E |
17180 |
18281 |
19344 |
20405 |
21459 |
22504 |
23546 |
24563 |
25541 |
26498 |
27444 |
|
Out of science |
1394 |
1389 |
1441 |
1482 |
1504 |
1529 |
1559 |
1597 |
1646 |
1703 |
1764 |
|
Unemployed |
127 |
128 |
132 |
134 |
137 |
141 |
147 |
153 |
160 |
165 |
170 |
|
Unemployed, Not Seeking |
404 |
380 |
356 |
347 |
354 |
361 |
369 |
381 |
396 |
410 |
426 |
|
Postdoctorates |
507 |
546 |
585 |
620 |
659 |
705 |
750 |
785 |
813 |
834 |
859 |
|
Foreign Doctorates |
|||||||||||
|
Workforce |
6178 |
6661 |
7166 |
7691 |
8232 |
8796 |
9381 |
9985 |
10608 |
11246 |
11898 |
|
Employed in S&E |
5840 |
6299 |
6781 |
7281 |
7791 |
8314 |
8853 |
9415 |
10001 |
10604 |
11218 |
|
Out of science |
306 |
329 |
353 |
380 |
412 |
456 |
505 |
551 |
595 |
636 |
677 |
|
Unemployed |
10 |
11 |
12 |
11 |
11 |
12 |
12 |
12 |
12 |
14 |
15 |
|
Unemployed, Not Seeking |
22 |
22 |
19 |
19 |
17 |
15 |
12 |
5 |
1 |
0 |
0 |
|
Postdoctorates |
320 |
343 |
366 |
390 |
414 |
440 |
464 |
486 |
508 |
531 |
552 |
|
Total |
|||||||||||
|
Workforce |
25282 |
26838 |
28439 |
30059 |
31686 |
33332 |
35002 |
36679 |
38352 |
40031 |
41716 |
|
Employed in S&E |
23020 |
24580 |
26125 |
27686 |
29250 |
30818 |
32399 |
33978 |
35542 |
37102 |
38662 |
|
Out of science |
1700 |
1718 |
1794 |
1862 |
1916 |
1985 |
2064 |
2148 |
2241 |
2339 |
2441 |
|
Unemployed |
137 |
139 |
144 |
145 |
148 |
153 |
159 |
165 |
172 |
179 |
185 |
|
Unemployed, Not Seeking |
426 |
402 |
375 |
366 |
371 |
376 |
381 |
386 |
397 |
410 |
426 |
|
Postdoctorates |
827 |
889 |
951 |
1010 |
1073 |
1145 |
1214 |
1271 |
1321 |
1365 |
1411 |
|
SOURCE: NRC analysis. See Appendix Tables D-9, D-11, and D-12. |
|||||||||||
cent. The one thing this model does not account for is the possible growth in the physician-scientist workforce as the result of expansions in the M.D./Ph.D. programs—that is, the movement of more medically trained doctors into research careers.
CONCLUSION
The importance of clinical research cannot be underestimated in today’s health care system. Recent efforts to offset the growing shortage of clinical researchers, especially those initiatives aimed at attracting physician-scientists into patient-oriented research, have not been fully evaluated. One program that has been in existence for many years is the MSTP, but it has not brought researchers into patient-oriented research. The MSTP has produced a highly qualified workforce in the basic health sciences, but the potential remains for these scientists to become more involved in translational or patient-oriented research. The forces that constrain the clinical sciences workforce are beyond the control of training programs, as they involve national policies on health care and its delivery systems. Additionally, because many areas of clinical research require medical training, predoctoral support is not possible under a program like NRSA. Intervention must occur at a point beyond the doctorate, with postdoctoral and career development programs.
RECOMMENDATIONS
Recommendation 4-1: This committee recommends that the total number of NRSA positions awarded in the clinical sciences should remain at least at the 2003 level. Furthermore, the committee recommends that training levels after 2003 be commensurate with the rise in the total extramural research funding in the biomedical, clinical, and behavioral and social sciences.
Data on the number of predoctoral and postdoctoral traineeships in 2001 appear to be consistent with earlier years. In 2001 there were over 1,577 predoctoral NRSA training slots in the clinical sciences and 1,830 at the postdoctoral level. Projecting these numbers into 2003, on the basis of a 4.4 percent increase in total predoctoral training and a 5.6 percent increase in postdoctoral training, yields estimates of 1,665 and 1,910, respectively. The 2002 data on fellowships are probably more current at 151 predoctoral and 96 postdoctoral positions, and since there was little change in the level of fellowship support from 2002 to 2003, these levels could be applied to 2003. For both the traineeships and fellowships at the predoctoral and postdoctoral levels, NRSA support is only a small fraction of the total training support (see Figures 4-2 and 4-10). Much more comes from research grants and the retraining of physicians through the K23 and K24 programs or self-support at the predoctoral level.
The relatively low unemployment among Ph.D.s in the clinical sciences and the fact that the pool of postdoctorates appears to be stabilizing suggest that the NRSA training level should be maintained at least at the 2003 level and increase with extramural research funding.
The discussion following Recommendation 2-1 with regard to the quality of NRSA programs and relative balance of biomedical training to the workforce also applies to the behavioral and social sciences.
Recommendation 4-2: This committee recommends that training grants be established for physicians to acquire the skills necessary for clinical investigation.
Clinical research, such as clinical trials and outcome assessment, can be carried out by individuals in a variety of fields, but a shortage of well-trained people appears to exist. Attracting physicians into these areas is highly desirable. Training should include clinical trial design, statistics, and epidemiology. Training programs should be structured so that physicians can maintain other professional activities while pursuing this training and receiving degrees at the master’s level.