2
Housing and Health
Housing conditions have been associated with lead poisoning, asthma, injuries, and other negative health outcomes. Children are also exposed to such toxins as environmental tobacco smoke, lead, and pesticides in their homes. Although hazards may be present in the homes of people at all income levels, children in low-income families, who have limited housing options, are at increased risk for many housing health hazards.
Children are more susceptible than adults to hazards in the home in four ways. First, they are at higher risk for exposure to toxins in the environment because, pound for pound, children breathe more air, drink more water, and eat more food than adults (National Research Council, 1993; Bearer, 1995; Landrigan et al., 1998). Second, their exposure to potential toxins is increased because of normal developmental behaviors, such as playing close to the ground and hand-to-mouth activity (Bearer, 1995). Third, because their biological systems are still developing, they sometimes are less able than adults to metabolize, detoxify, and excrete toxins. The developing neurological systems may be especially vulnerable to environmental toxins, such as lead and pesticides (Eskenazi et al., 1999; Faustman et al., 2000), with potential significant effects on the developing brain; neurobehavioral deficits caused by environmental toxins may have life-long consequences for children. Lastly, because children younger than 12 years spend about 75 percent of their time at home, they have more opportunities for exposure than adults (Wiley et al., 1991); see Figure 2-1.
The bulk of this chapter describes the major housing-related hazards for children: asthma triggers, lead, pesticides, environmental tobacco smoke,
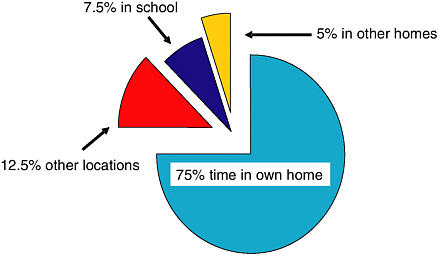
FIGURE 2-1 Time spent in the home by children younger than 12 years.
SOURCE: Data from Wiley et al. (1991).
and injuries, as well as the roles of overcrowding and special problems in rural housing. Although there are numerous possible structural deficits in low-income housing, we do not discuss these in depth except to the extent that they are related to the above health issues, which are the major areas of housing health hazards research. We then discuss the disparities in risk among children, which leads to the final section that presents our conclusion about housing and health.
HOUSING HAZARDS
The state of knowledge about housing health hazards varies widely. For example, there are decades of research on the effects of lead, including the accepted finding that lead in house paint is a leading cause of lead poisoning, while the effects of exposure to pesticides in the home is a relatively new field of study with few definitive findings. Furthermore, even for recognized hazards, strategies to mitigate them effectively continue to evolve.
Asthma Triggers
Asthma is the most prevalent and disabling environmental health problem among children, afflicting more then 4 million children in the United
States. Moreover, it appears to be increasing: between 1980 and 1996 asthma-associated school absences rose by more than 50 percent, to 14 million days per year (Mannino et al., 2002). Clearing the Air (Institute of Medicine, 2000) concluded that there is a causal relationship between exposures to allergens produced by cockroaches and dust mites and asthma exacerbations in sensitized individuals as well as between exposure to environmental tobacco smoke and exacerbations of asthma in preschool children. One study reported that exposure to environmental tobacco smoke may account for 150,000 to 300,000 excess cases of asthma in preschool children (Lanphear et al., 2001b). There also is evidence of an association between fungal exposure, which is often associated with visible mold or dampness indicators, and exacerbations of asthma in sensitized persons (Institute of Medicine, 2000). And there is suggestive evidence of an association between nonoccupational formaldehyde exposure and wheezing.
There is an association between some indoor air exposures and the development of asthma, such as exposure to house dust mite allergen and the development of asthma in susceptible children (Institute of Medicine, 2000). One study found that about 40 percent of doctor-diagnosed asthma in children and adolescents is associated with exposures to indoor pollutant and allergens in the home (Lanphear et al., 2001b). There is also an association between nitrogen dioxide and increased airway responses to inhaled allergens and chemical irritants in asthmatic persons (Institute of Medicine, 2000). These effects have been observed at concentrations that may occur in poorly ventilated kitchens with gas appliances in use. Childhood asthma is also associated with use of a gas stove or oven for heating, a practice that is most common in the southeastern United States, especially in poor and rural housing (Lanphear et al., 2001b; Centers for Disease Control and Prevention, 1997b).
The burden of asthma falls disproportionately on certain groups. Asthma is disproportionately high in urban areas characterized by high levels of poverty and minority populations (Institute of Medicine, 2000), particularly among African Americans and Puerto Rican children living on the East Coast. However, very high rates of asthma have also been reported in less urban areas with low levels of poverty.
Specific exposures associated with asthma are also more common in certain population groups. Cockroach sensitization is more common among inner-city poor children (Institute of Medicine, 2000). In contrast, formaldehyde pollution is more common in newly constructed or renovated buildings or in those containing new furniture or carpets with materials that contain formaldehyde resins (Institute of Medicine, 2000). Tightly constructed buildings, such as mobile homes, often contain high formaldehyde concentrations.
The level of asthma triggers can be increased by building defects, such
as inadequate ventilation and moisture accumulation. High moisture levels promote mold growth and attract rodents and cockroaches. Children in low-income families are more likely than other children to be exposed to structural hazards in the home (Cummins and Jackson, 2001). Some experts have concluded that disparities in asthma mortality may be at least partly attributable to disproportionate exposure to “indoor environmental asthma triggers associated with living in substandard housing” (Krieger and Higgins, 2002, p. 760).
Research has shown that some strategies to limit exposures are effective at improving symptoms or lung function in asthmatics. A combination of physical measures has been found to reduce the levels of dust mite allergens and clinical symptoms. There is also suggestive evidence that cockroach extermination plus cleaning of beds, carpets, and clothing can reduce cockroach allergen levels (Institute of Medicine, 2000; Morgan et al., 2004). However, either cleaning or extermination alone appears ineffective. Thus, interventions to remove sources of allergens that are known to cause exacerbations in sensitive individuals may prove, when rigorously studied, to be ineffective. This possibility suggests that, unless measures intended to ameliorate hazards are carefully studied, families may be subjected to expensive but ineffective interventions. Moreover, interventions that reduce the level of exposure may not result in clinical benefits. To date, integrated interventions to reduce cockroach allergen levels have not been able to reduce them below levels that are clinically significant. And there is insufficient evidence on whether reduction in cockroach allergen levels reduces asthma severity. Clearing the Air (Institute of Medicine, 2000) called for more research to “address the feasibility and generalizability of intervention programs on target populations “ (p. 17) and concluded that “often it is not known what degree of mitigation would be necessary to reduce the risk of attacks in known asthmatic individuals” (p. 406). See Box 2-1 for an example of a recent research project designed to better understand the connection between housing conditions and asthma.
Lead
In the 1950s and 1960s hospitalizations of children for acute lead encephalopathy led government actions to prohibit lead in interior paint, gasoline, and tin cans. Although the average blood lead concentrations of U.S. children fell by more than 80 percent during the ensuing 30 years, levels of childhood lead exposure classified as toxic by Centers for Disease Control and Prevention (currently defined as a blood lead concentration of 10 micrograms per deciliter (µg/dl) or higher) still affect 4.4 percent of children younger than 6 years of age (Pirkle et al., 1998). Infancy is a peak period of vulnerability due to the confluence of mouthing behavior and
|
BOX 2-1 The Interventions Study on Reducing Asthma Triggers in the Home is an activity of the Healthy Public Housing Initiative (HPHI), a community-centered project designed to engage public housing residents in a collaborative process aimed to improve both the health and quality of life of residents and building conditions. The HPHI is a collaborative including the Harvard School of Public Health, the Boston University School of Public Health, the Tufts University School of Medicine, and a wide variety of actively involved partners that include public housing residents, the Boston Housing Authority, two tenant task forces, the Boston Public Health Commission, the Committee for Boston Public Housing, a pediatric asthma specialist, and specialists in energy efficiency and housing policy and finance. Three pilot surveys conducted revealed that many environmental health problems reported by residents are associated with the physical conditions of housing, such as water leaks, moisture and mold growth, insufficient ventilation, and pest infestation. With the connection between indoor environmental conditions and resident health established, the HPHI hypothesized that these problems could be addressed through a combination of building improvements, change in maintenance policy, and community health education programs. With input from focus groups with public housing residents, the HPHI designed a study to test the hypothesis that housing-based interventions will reduce asthma triggers. The study tested the effectiveness of interventions designed to reduce known environmental asthma triggers. The interventions included air filters, new mattresses, deep cleaning, integrated pest management, and resident education; they were conducted in 44 households that had 57 asthmatic children. HPHI measured the change in the health status and quality of life of children with asthma after the completion of the interventions. The study also looked at the health benefits, through pre- and postsurvey results, that might have resulted from the building |
increasing mobility (Lanphear et al., 2002). Blood lead levels are higher among African American children than among non-Hispanic white children at all ages; see Figure 2-2: 22 percent of urban, African American children under 6 years were estimated to have blood lead levels above 10 µg/dl (Pirkle et al., 1998). An estimated 1.2 million U.S. children in low-income families younger than 6 years old live in housing that contains one or more lead hazards (Jacobs et al., 2002). Lead poisoning has become concentrated in poor, black children living in substandard housing in innercity neighborhoods (Cummins and Jackson, 2001).
Subclinical lead toxicity is associated with deleterious and persistent effects of lead exposure on brain function (Bellinger et al., 2003). In one study, there was an estimated 7.4 point drop in IQ scores associated with an initial 10 µg/dl increase in blood lead level (Canfield et al., 2003a). There is some evidence that even blood lead concentrations below 10 µg/dl are associ-
|
systems upgrades and unit modifications that are part of the housing authority’s energy modernization program. The project also evaluated resident response to the interventions, their cost effectiveness, and the ease of implementation. Lastly, the project examined any benefits from the residents’ active involvement. The residents were involved in every stage of the project by working with university partners to assess initial conditions, determining the best mix of interventions to test, evaluating results, and developing action plans. Residents who worked with the project team received training in indoor environmental health, surveying and testing techniques, and identification of appropriate health outreach programs. The housing authority provided support to enhance continued employment opportunities after the completion of the project. More than 50 percent of asthmatic children in the study are allergic to the cockroach antigen. A large number of samples taken prior to the intervention showed levels of cockroach antigen in bedrooms and kitchens above the threshold for sensitization and exacerbation by this antigen. Determinants of pest-related allergen levels are lack of housing renovation, holes in walls, housekeeping practices, and season. The integrated pest management intervention (deep cleaning, application of gels, sanitation improvements, repair of cracks, crevices and holes) resulted in the reduction of pest allergen levels, which were sustained over 3-4 months and then began to rise, showing the need to implement the intervention on a regular basis to maintain results. In addition, asthma-related quality of life (measured based on symptoms, activity limitations, and emotional function) in enrolled children improved significantly during the health education phase and again over the course of the intervention. Based on these results, the Boston Housing Authority intends to develop a comprehensive integrated pest management program that includes resident educators. SOURCES: Brugge et al. (2003a); Hynes et al. (2004); Levy et al. (2004); and H. Patricia Hynes (personal communication, 2005). |
ated with deficits in cognitive and motor skills (Lanphear et al., 2000; Canfield et al., 2003a; Bellinger et al., 2003; Chiodo et al., 2004). A child’s ability to write, draw and construct can be adversely affected by deficits in visual-motor, visual-spatial, and fine-motor coordination (Dietrich et al., 1993a). Poor postural stability can result in clumsiness that can prevent full engagement in sport and recreational activities (Bhattacharya et al., 1988). Deficiencies in impulse control or “executive functions,” such as planning, organization, and anticipation of consequences, can occur and may be associated with academic underachievement and behavioral problems (Bellinger et al., 1994; Canfield et al., 2003a; Byers and Lord, 1943; Gittelman and Eskenazi, 1983). Thus, blood lead levels that were previously thought to be safe may be hazardous to children.
Housing built before 1978, when lead was banned in house paint, is the primary source of lead exposure for children today (Lanphear et al., 1998a;
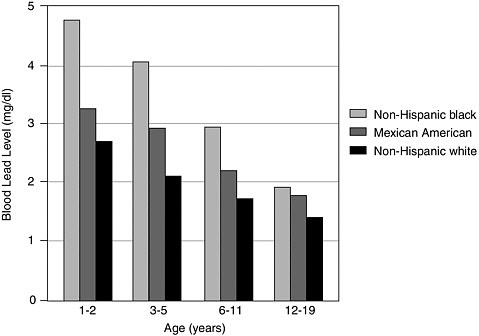
FIGURE 2-2 Racial and ethnic differences in mean blood lead levels among U.S. children, 1988-1994.
SOURCE: Adapted from Pirkle et al. (1998).
Jacobs et al., 2002), and homes built before 1940 have the greatest burdens of lead-based-paint hazards (Jacobs et al., 2002). An extensive body of research links exposure to lead in the home with elevated blood lead levels in children (Charney et al., 1983; Clark et al., 1985; Rhoads et al., 1999; Lanphear et al., 2002). A recent survey estimated that 38 million homes still have lead-based paint, and another 24 million homes have significant lead-based-paint hazards (Jacobs et al., 2002). Moreover, 16 percent of homes had one or more lead dust hazards on floors or windowsills.
Research has clarified the sources and pathways for children’s exposure to lead in urban homes. Lead from deteriorating exterior paint or building renovations or demolitions contaminates soil and street dust, which are tracked into the home from foot traffic (Aschengrau et al., 1994; Mielke and Reagan, 1998; Wolz et al., 2003; Farfel et al., 2003). Lead from deteriorating interior paint contaminates house dust (Lanphear and Roghmann, 1997). Household floor dust contaminated with lead gets on the hands of young children, who then put their hands in their mouths (Charney et al., 1980; Lanphear et al., 1998c). This is one way that lead enters the gastrointestinal tract of a child, is absorbed into the blood, and ultimately
affects the child’s developing central nervous system (Sayre et al., 1974). Another, more direct pathway is lead in drinking water, most commonly from lead pipes (Levin et al., 1989; Lanphear et al., 2002).
Because the ingestion of flaking and chipping paint is associated with elevations in children’s blood lead levels, it was clear that removal of lead paint from homes would be desirable. However, research showed the importance of how lead paint abatement was carried out. Lead paint abatements, if improperly conducted or if not followed with meticulous post-abatement cleanups, actually dispersed lead in dust in homes, resulting in increased blood lead levels in children (Chisholm, 1986; Farfel and Chisholm, 1990; Amitai et al., 1991; Rey-Alvarez and Menke-Hargrave, 1987; Swindell et al., 1994; Aschengaru et al., 1997; Centers for Disease Control and Prevention, 1997a).
This research demonstrated the importance of evaluating interventions that are intended to reduce hazards to discover if there are any unanticipated adverse effects. Without such research, children might have been made worse off with the lead abatement strategies. The research findings about lead abatement interventions led to public policies to protect children. The Department of Housing and Urban Development (HUD) and the Environmental Protection Agency now have policies that require certification of personnel who conduct lead-based abatements; restrict the methods used to conduct abatements; require post-abatement cleanups; preclude families from residing in homes during abatements and until post-abatement cleanups are completed; and require post-abatement reassessment of the levels of lead in children’s homes (U.S. Department of Housing and Urban Development, 1995; U.S. Environmental Protection Agency, 2001). Many state and local governments have implemented similar requirements.
Pesticides
Two of the most common classes of insecticides in the United States, organophosphates and carbamates, are considered toxic to the human central nervous system and can cause acute poisoning (Eskenazi et al., 1999). The effects of nontoxic levels of exposure in children, which do not produce overt symptoms, has not been extensively studied on humans, although there is substantial evidence from research with laboratory animals (Eskenazi et al., 1999). The limited research in humans exposed to low levels of certain pesticides, such as organochlorines (Rogan et al., 1986) and organophosphates (Young et al., 2005), raise concerns about possible neurodevelopmental effects on children. Research has been recently undertaken to better understand the pathways and effects of exposure to agricultural pesticides and other widely used pesticides on children; see Box 2-2 for an example of this research.
|
BOX 2-2 The Center for the Health Assessment of Mothers and Children of Salina Study (CHAMACOS) is designed to try to understand and reduce the environmental health risks of pesticide and other environmental exposures among socioeconomically disadvantaged children living in a rural agricultural community in Salinas Valley in Monterey County, California. The keystone project is a longitudinal birth cohort study that began with 600 pregnant women; the study is currently following their children, who are now 5 years old. The study has four components: (1) the levels and routes of children’s exposure to pesticides and other environmental agents; (2) the potential health effects associated with these exposures; (3) the mechanisms for these potential health effects; and (4) interventions to reduce children’s exposure to pesticides. The first component characterizes the magnitude and pathways of pesticide exposure in children by measuring prenatal and postnatal pesticide exposure, characterizing population-level exposure correlates, and identifying exposure-prone behavior. The second component focuses on the relationship of pesticide exposure and allergens and neurodevelopment, somatic growth, and asthma and other respiratory illness. The third component examines mechanisms of neurotoxicity and the relationship of multiple exposures found in agricultural environments, including pesticides and allergens on immunomarkers. The interventions focus on reducing the amount of children’s pesticide exposure due to residues brought home by their farm-working parents. There were two different interventions over two growing seasons, in 2003 and 2004. During the first growing season, the technical intervention provided farm workers with coveralls and gloves and installed warm-water facilities for hand washing in the fields. During the second growing season, the intervention was an in-depth pesticide education program with farm worker households specifically aimed at prevention exposure to children. Results to date include the demonstration of higher levels of urinary pesticide metabolites in the pregnant women in comparison with national reference data, an association of maternal pesticide metabolite levels and shorter gestational duration, and abnormal reflexes in the neonates. Analyses of the mechanism and intervention studies are now under way, with results expected in 2006. SOURCES: Eskenazi et al. (2004); Young et al. (2005); Bradman et al. (2005); and Brenda Eskenazi (personal communication, 2005). |
An estimated 80 to 90 percent of American households use pesticides (Whitemore et al., 1994; Adgate et al., 2001). Exposure can be frequent and at high levels to control cockroach and rodent problems (Whyatt et al., 2002; Gurunathan et al., 1998; Davis and Ahmed, 1998; Bradman et al., 2005). Poor housing conditions are associated with both the presence of
rodents and cockroaches and the use of pesticides (Bradman et al., 2005). A recent report documented widespread residential pesticide exposure in New York City among pregnant women (Whyatt et al., 2002). The study also noted an association between housing disrepair and the proportion of pregnant women who use pesticides. Pesticide exposure in rural agricultural environments may be compounded by spray drift or take-home exposure when farm workers track agricultural pesticides into their homes on their shoes or clothing (Bradman et al., 2005; Fenske, 1997).
Environmental Tobacco Smoke
Tobacco smoke contains more than 4,000 chemicals, including 43 carcinogens. Between 1988 and 1994, an estimated 38 percent of U.S. children younger than 6 years were exposed to environmental tobacco smoke—also referred to as second-hand smoke and passive smoking (Pirkle et al., 1996). Although exposure to environmental tobacco smoke is not unique to homes, it is included here since homes are a significant source of exposure for children, particularly young children, and research on environmental tobacco smoke is often conducted in homes.
Cotinine, a biomarker of exposure to environmental tobacco smoke, is used as an indicator of childhood exposure (Benowitz, 1996). Children have significantly higher serum cotinine than nonsmoking adults (Groner et al., 2004), and younger children have higher levels of cotinine than older children (Centers for Disease Control and Prevention, 2003; Willers et al., 1995). The higher levels of biomarkers in younger children could be due to a number of factors, including greater time inside the home; differences in proximity to a smoker; metabolism; increased respiratory rates; or ingestion of nicotine-contaminated house dust (Matt et al., 2000).
The World Health Organization concluded that environmental tobacco smoke exposure “causes a variety of adverse health effects in children, including lower respiratory tract infections such as pneumonia and bronchitis, coughing and wheezing, worsening of asthma, and middle ear disease” (World Health Organization, 1999, p. 3). Several reviews have concluded that parental smoking has adverse effects on pulmonary function in children (Environmental Protection Agency, 1992; U.S. Department of Health and Human Services, 1986; National Cancer Institute, 1999). For young children, the major source of exposure is smoking by parents and other household members, particularly their mothers. As children grow older, the relative contribution of other exposure sources, including sources outside the home, increases (World Health Organization, 1999).
The association between parental smoking and asthma has remained when studies have controlled for a long list of potential confounders, including gender, age, urbanization, education, crowding, dampness, mold,
cooking fuel, parental respiratory symptoms, parental asthma, and the child’s smoking (Weitzman et al., 1990; Martinez et al., 1992; Agabiti et al., 1999). Pneumonia is more common during the first year of life in smoking households, even when controlling for parental symptoms, birth weight, and family size (Strachen and Cook, 1998b). Children in smoking households are at greater risk for hospitalization for respiratory illness (Chen et al., 1986; Anderson et al., 1988). Environmental tobacco smoke has been associated with an approximate doubling of the risk of lower respiratory tract infection in children, with the risk declining after the age of 2 (Li et al., 1999). In four of five studies, the incidence of tonsillectomy is twice as high for children who live in households with smokers in comparison with children living in homes without smokers (Willatt, 1996; Said et al., 1978; Hinton et al., 1993; Stahlberg et al., 1986; Strachen and Cook, 1998a).
Maternal smoking during pregnancy has been identified as a major cause of sudden infant death syndrome (SIDS), the leading cause of death of infants from 1 month to 1 year of age in the United States, as well as reduced birth weight and decreased lung function (Etzel et al., 1997; World Health Organization, 1999; DiFranza et al., 2004). Both the National Cancer Institute and the Surgeon General have concluded that there is sufficient data to infer a causal relationship between maternal smoking in general and SIDS (National Cancer Institute, 1999; U.S. Department of Health and Human Services, 2004; Kharrazi et al., 2004).
Childhood exposure has also been identified with impaired neurobehavioral development and as a possible contributor to cardiovascular disease in adulthood (World Health Organization, 1999; Eskenazi and Castorina, 1999; Fried et al., 1998). Epidemiologic studies suggest that prenatal and early passive exposure to tobacco smoke may contribute to negative behavioral and neurocognitive effects (Eskenzai and Trupin, 1995; Fried et al., 1992, 1998; Yolton et al., 2005), although the evidence to date is considered inconclusive given the confounding of a range of other characteristics common among women who smoke. There is also emerging evidence that environmental tobacco smoke may be associated with increased rates of dental caries (Aligne et al., 2003) and the metabolic syndrome in overweight youth (Weitzman et al., in press).
There is some evidence that suggests that there may be biological differences in susceptibility to housing health hazards. For example, for a given exposure to environmental tobacco smoke, African American children have significantly higher blood lead levels, cotinine levels, and DNA adducts (an altered form of DNA that occurs as the result of exposure to a carcinogen) (Pirkle et al., 1998; Wilson et al., 2005; Richie et al., 1997).
Legislative strategies that restrict where and when people can smoke in public settings are of little use in reducing exposure in homes. Strategies to
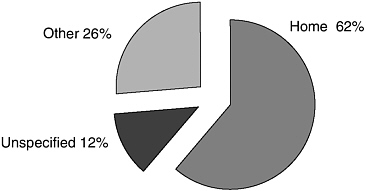
FIGURE 2-3 Fatal injuries by place of occurrence in U.S. children, 1985-1997.
SOURCE: Data from Nagaraja et al. (2005).
reduce exposure in homes will have to focus on household decision makers, possibly by educating them about the risks to children from environmental tobacco smoke and ways to eliminate exposures. Smoking during pregnancy has reduced by 33 percent over the past decade (Mathews, 2001); this may be attributable to increased recognition of the harmful effects on the fetus of smoking while pregnant.
Injuries
In the United States in 1998, injuries accounted for 5,189 deaths in children aged 1 to 15 years—40 percent of all childhood mortality (Murphy, 2000). Nonfatal injuries and subsequent disability also account for a major proportion of health service utilization in children (Danseco et al., 2000). Excluding motor vehicle injuries, the majority of fatal injuries in children occur in the home (Scheidt et al., 1995; Powell and Tanz, 2002; Nagaraja et al., 2005; see Figure 2-3). The youngest children are especially vulnerable; 90 percent of fatal injuries among children younger than 5 years occurred in the home (Nagaraja et al., 2005).
Residential injuries can be caused by poor design or disrepair of the home, such as poor lighting, damaged stairs, flooring and railings, or broken windows. Indeed, “housing factors are important determinants (of household injuries) amenable to intervention” (Matte and Jacobs, 2000, p. 10). Injuries can also be caused by poor maintenance of home design elements (National Center for Healthy Housing, 2002). For example, there is some evidence that smoke alarms may be less common in low-income households (Sharp and Carter, 1992). Injuries can also be due to consumer
products in the home such as toys, appliances, electrical equipment, or chemicals (National Center for Healthy Housing, 2002).
There are few data available on any disparities that may exist in injury risks by racial and ethnic status. The rates of nonfatal injuries that occur in the residential environment are lower among minority children (Phelan et al., 2005), although this reported difference may be due to more limited access to health care by minority children and resultant lower rates of reporting. In contrast, the rate of fatal injuries that occur in the home environment is substantially higher for African American children than for white children (Nagaraja et al., 2005). O’Campo and colleagues (2000) reported a relationship between the frequency of housing code violations at the neighborhood level and the risk of injury-producing events among children.
Research on injuries has led to changes in housing laws to better protect children. During the 1970s, health officials in New York City recognized that there were significant numbers of children who were injured or killed by falls from windows and that the incidence was significantly higher during the summer months. Many of these injuries and deaths occurred in low-income areas and lived in housing stock of poor quality or in tenement-type buildings. A pilot project studied the effects of education and provision of free window guards in preventing such falls. Subsequently, it was expanded to all 5 boroughs, leading to a 35 percent reduction in the number of children who died from falls in the city between 1973 and 1975 (Speigel and Lindaman, 1977). The city then passed a law in 1976 that required owners of multiple dwellings to install window guards in housing with residents younger than 10 years old. Follow-up through 1993 showed a consistent decrease in the number of childhood fall-related deaths. In this case, a simple epidemiological observation led to an intervention whose efficacy was demonstrated by research, which in turn led to effective policy changes.
Scald burns from household tap water provide another example of how research can lead to policy changes. Scald burns account for 50-60 percent of all burns in children (Purdue et al., 2002). In 1978, scald burns from tap water were estimated to account for 7-17 percent of all childhood scald burns that required hospitalization (Feldman et al., 1978). Studies of parent education encouraging them to lower the maximum household water temperature were shown to be ineffective. In contrast, studies of passive regulation of household water temperature by limiting the settings on hot water heaters proved effective in reducing scald burns (Webne et al., 1989). These findings led to legislation and changes in building codes to ensure that hot water heaters are set at safe temperatures, leading to a significant decline in childhood scald burns (Feldman et al., 1978).
Safe hot water heater temperatures also protect children from steam radiator burns (Quinlan, 1996). The Consumer Product Safety Commis-
sion and the plumbing industry have published a voluntary standard under which the maximum allowable temperature at the water outlet to the bathing area should be 120°F. There are also national standards by the major plumbing code-making bodies that specify a maximum temperature of 120°F for delivered hot water.
Overcrowding
Overcrowding1 can contribute to the transmission of infectious diseases such as tuberculosis and respiratory diseases (Krieger and Higgins, 2002) and can cause or exacerbate mental stress (Jones, 2003). Overcrowding is an increasing problem for foreign-born households, especially families with children (Capps, 2001; Center for Housing Policy, 2003). In 2000, 43 percent of foreign-born Hispanic households were crowded, compared with 30 percent in 1980. (The comparable numbers for native-born Hispanics were 15 and 14 percent, respectively; Joint Center for Housing Studies, 2004, Table A-8). Farm workers experience similarly disproportionate high rates of overcrowding. A 2001 study found that almost 52 percent of all housing units for farm workers were crowded, and 74 percent of the units included children (Housing Assistance Council, 2000). In comparison, only 2 percent of all U.S. households and 3 percent of nonmetropolitan households are crowded (U.S. Census Bureau, 1997).
Rural Housing
Approximately 22 million (22 percent) of all occupied housing units in the United States are in nonmetropolitan areas (Housing Assistance Council, 2000). However, housing-based health risks in agricultural and rural households have received relatively little research attention (Bradman et al., in press), although rural housing conditions clearly present many risks to children.
More than 7.7 million rural housing units include children, and 35 percent of these have problems with cost, crowding, or adequacy. Of all rural units with children, 2.8 million were built before 1960, and of these, only 8 percent have been tested for lead (Housing Assistance Council, 2000). Hispanic-headed households in rural areas occupy substandard hous-
ing at twice the rate for all rural households (Housing Assistance Council, 2000).
A recent study of approximately 650 homes of pregnant Latina women living in poverty in an agricultural community documented many housing hazards (Bradman et al., in press). Pest infestations were common, with 60 percent of the homes containing cockroaches and 31 percent containing rodents. Housing disrepair was widespread: 58 percent had peeling paint, 43 percent had mold, 25 percent had water damage, 16 percent had leaks under sinks, and 11 percent had rotting wood. Of all the homes, 76 percent of the homes were overcrowded. Fewer than 3 percent of them had no adverse conditions (Bradman et al., in press).
RISK DISPARITIES
As discussed above, the scientific literature documents that certain housing health hazards are more common in poor-quality housing, which is more prevalent among the homes of children in low-income families and that outcomes such as asthma, fatal injuries, and lead poisoning are also more prevalent among these children. These disparities may result directly from greater exposures to hazards in older, dilapidated, or poorly maintained housing. In comparison with the general population, low-income and African American people are 2.2 and 1.7 times more likely, respectively, to live in homes with severe physical problems (Krieger and Higgins, 2002, citing American Housing Survey data).
Poor families also lack the resources to move to better quality housing; and there is a severe shortage of affordable low-income housing (see U.S. Department of Housing and Urban Development, 2001). Nowhere in the United States can a minimum wage job generate sufficient income to rent a two-bedroom home at the local HUD fair-market rent (National Low Income Housing Coalition, 2004). In 2004, the average hourly wage needed to pay the national average rent for a two-bedroom unit without spending more than 30 percent of household income for housing was $15.37, which is almost triple the federal minimum wage of $5.15 (National Low Income Housing Coalition, 2004). Consequently, many low-income families have no choice but to live in older dwellings that present health risks such as deteriorating lead paint. For example, of the 29 census tracts in Rhode Island with the highest concentrations of old housing, 25 are in low-income neighborhoods (Rhode Island Kids Count, 2003).2
Many children in the United States live in poverty. According to the
U.S. Census Bureau, the poverty rate among children was 17.6 percent in 2003, its highest level in 10 years (U.S. Census Bureau, 2004). The number of children living in extreme poverty, defined as an after-tax income below half the poverty level, was 5 million in 2001 (National Center for Children in Poverty, 2003); this number represents 7 percent of all children in the United States. Children of color are more likely to be poor. In 2001, nearly 1 million black children lived in extreme poverty, which was the highest level in the 23 years for which there are data (Children’s Defense Fund, 2003).
Research shows that severely limited purchasing power forces low-income families to choose among the basic necessities of housing, food, health care, and clothing with the result that for many people, unhealthy, poor-quality housing is a necessary reality (Rothenberg, 1971). A recent study showed that, among households in the bottom income quintile, those that devote less than 20 percent of their budgets to housing are able to spend $80 more a month on food and $49 more on health care, on average, than households that spend at least 50 percent of their budgets for housing (Joint Center for Housing Studies, 2004). In 1999, 42 percent of very-low-income families with children in private rental housing lived in severely inadequate housing or spent more than half of their income for housing, what HUD refers to as “worst case housing needs” (U.S. Department of Housing and Urban Development, 2001).
It is difficult to separate the effects of race or ethnicity on health disparities from the effects of socioeconomic disadvantages. Poverty, poor education, and poor access to health care are more prevalent in minority groups and are also associated with adverse health outcomes (Institute of Medicine, 2003). In addition to these effects, there may also be effects due to housing discrimination (see Turner et al., 2002).
Children who are at increased risk for housing health hazards are often the focus of research. Ultimately, the knowledge gained from that is more likely to benefit children at high risk, but as noted through this report, research targeted at high-risk groups also raises ethical concerns because of their many vulnerabilities. In addition, as noted in Chapter 1 and discussed further in Chapter 4, there are few market incentives to translate housing research into improved housing or reduction of hazards. Public resources to ameliorate housing hazards are limited at the same time that operating costs are higher for older properties and low-income housing, the very properties most likely to contain health hazards and to be occupied by low income families; see Box 2-3. Low-income families cannot usually afford to move to better housing.
|
BOX 2-3 Many factors affect the economics, and ultimately the availability, of low-cost, private-market housing. Empirical studies generally confirm that low-income housing may be relatively more expensive because of greater operating costs, depreciation costs, higher rates of tenant turnover, higher rental collection costs, or delinquencies in payment (Muth, 1969). Recent increases in utility costs, property taxes, and insurance premiums have also put even greater upward pressures on rental operating costs (Goodman, 2004). Other maintenance costs, such as mold eradication, which threatens to become a pervasive economic as well as health problem, can also cause an increase in operating costs (Goodman, 2004). Older housing, especially in low-income neighborhoods, also tends to have higher operating costs relative to newer housing. For example, one research survey estimated that utility costs are 55 percent less for properties built in the 1990s than for properties of the same quality, size, and location built in the 1970s (Goodman, 2004). In general, properties built since 1980 cost at least 10 percent less to operate than properties built before 1970 (Goodman, 2004). |
CONCLUSIONS
Hazards present in the home environment pose numerous and substantial health risks to children in both urban and rural environments, with children in low-income families at greater risk. Housing that is both affordable and hazard free is an increasingly scarce commodity for low-income families. An increase in affordable housing and broader requirements for abatement of hazards would offer prospects of genuinely healthy housing for all children. This has largely been accomplished in some public housing, particularly for lead. However, the private low-income housing market provides limited incentives for landlords to do so. The economics of low-income housing suggests that even if it were technically feasible to eliminate all housing health hazards to children, doing so might exacerbate existing private-market shortages or push up housing costs. Thus, under current housing policies, there is a need for research to identify interventions that are not only effective at ameliorating housing health hazards but also cost effective.

















