2
Considerations Regarding the BR Content
The major content areas of the current Bioastronautics Roadmap (BR) include 45 risks that are assigned to one of 5 cross-cutting areas: (1) Human Health and Countermeasures, (2) Autonomous Medical Care, (3) Behavioral Health and Performance, (4) Radiation Health, and (5) Advanced Human Support Technologies (NASA, 2005). Although not emphasized in the body of the BR, the associated appendixes provide data regarding technology readiness levels and countermeasure readiness levels (NASA, 2005, Appendix A) associated with each risk; indicate some anticipated interactions among risks (NASA, 2005, Appendix B); and depict a preliminary schedule of deliverables for the 5 cross-cutting areas (NASA, 2005, Appendix C). The risks are further described by their associated research and technology questions, and all of the above are further analyzed relative to the Design Reference Missions. Together, these areas result in a multidimensional matrix that challenges both National Aeronautics and Space Administration (NASA) managers and the review committee, and the challenge is further compounded by the dynamic nature of the present and future versions of the BR.
The committee’s comments for content improvement are divided into two broad categories: overarching issues and specific issues. The overarching issues involve (1) the time dimensions of risk, (2) the interactions among risks, (3) the status of the countermeasure and technology readiness levels, and (4) linking relationships between human factors and technology in the BR. Attention to each of these overarching issues will strengthen the con-
tent of the BR and provide a framework for thinking that will benefit NASA strategists, managers, and operations personnel as they focus on risk reduction related to the ambitious objectives outlined in the President’s initiative of January 2004 (White House, 2004). Specific areas in which additional attention would be of great benefit include the following:
-
Reclassification of behavioral health risks
-
Psychological and physical impacts of space flight on performance, including use of crew selection criteria (social, demographic, and preexisting health status of astronauts, and their response to stress) to minimize adverse responses, especially in the context of longer-term missions
-
Radiation effects—establishing risk-specific radiation exposure levels
-
Assessing the sources and impact of long-duration space flight on crew health and incremental risk
-
Autonomous medical care and self-care
OVERARCHING ISSUES
Overarching issues are those factors that, in the committee’s view, deserve wide review and application throughout the current BR and in future revisions of the BR. They should be viewed as guiding principles or strategic approaches to the revision and management of the BR.
The Time Factor and Its Impact on Risk
Time is a factor that has the potential to increase risk significantly, particularly in the context of long-duration space flight such as the 30-month Mars mission outlined in the President’s initiative. Time has several dimensions that must be considered in the definition and mitigation of risk. Duration of the mission is one component. Clearly, the potential for the development of a health problem, such as new disease or injury, increases progressively from the 1-month lunar mission to the 12-month International Space Station (ISS) mission, to the 30-month Mars mission. Similarly, the consequences and countermeasures associated with disease or injury will differ depending on the time of appearance of the human health problem within the mission time frame (consider, for example, the discovery of a breast mass that appears 2 months after launch on a planned 30-
month Mars mission, versus one that occurs 2 weeks into a planned 30-day lunar mission).
Another dimension of the time factor relates to distance from Earth during the mission. Distance from Earth impacts the mitigation strategy and selection of appropriate countermeasures because increasing distance translates into increasing time delays for radio transmission to and from ground control, thus requiring greater independence of the crew when handling health-related (and other) emergencies. Further, more autonomous health care will be required on long-duration, long-distance missions, where aborting the mission or evacuating a crew member for medical care is not a feasible option.
Another dimension of time involves the emergence of a predictable health problem related to the immediate mission task(s). Neurovestibular dysfunction, such as vertigo, might be an inconvenience during some parts of a mission, whereas neurovestibular dysfunction during the docking maneuver or a lunar or Mars landing could endanger mission success and crew welfare.
Finally, to be included meaningfully in the mission planning process, biomedical countermeasures and life support technologies must be validated well in advance of the final integrated mission plan, thus adding temporal urgency to the time dimension.
The committee notes that some of these dimensions of time are partially addressed by subdividing the risk analyses into the three Design Reference Missions in the BR, but concludes that time does not achieve the attention that is required to fully address risk priorities, determine countermeasure readiness, predict the maintainability of systems and equipment, and evaluate the impact of exploration missions flight on crew health. All of these factors deserve additional visibility in the BR.
Recommendation 2.1
The committee recommends that risk assessment and mitigation (technology or countermeasure development) in the BR be enhanced by labeling risks according to their relevance to operational requirements and to temporal urgency.
Interactions Among Risks
The BR currently contains various cross-cutting categories of risk, and an additional cross-cutting area is recommended later in this chapter. How-
ever, the BR does not provide enough information on the interrelations among and between these categories, risks, and their associated mitigation strategies. Space flight necessarily involves a complex system of interdependent systems, and as a result of that interdependence, any change that affects one system may also affect other systems, sometimes in ways that are neither obvious nor anticipated.
The BR contains a list of “related risks” and “interactions” (NASA, 2005, Appendixes A and B, respectively), but without explanation of how the risks were identified and assigned to specific categories. For example, nutrition is identified as a related risk for Risk 23 (human performance failure due to poor psychosocial adaptation) but not Risk 24 (human performance failure due to neurobehavioral changes). The extensive research literature supporting the role of nutritional factors in understanding the mechanisms of depression and other mental disorders that fall within Risk 24 (e.g., Young et al., 1985; Wurtman and Wurtman, 1989) is not cited. The BR provides no explanation that nutrition is related to poor psychosocial adaptation because the quality of food—as opposed to its nutritional content—is important in maintaining group morale under conditions of prolonged isolation and confinement (Stuster, 1996; Johnson et al., 2003).
Risks and their mitigations interact in a variety of complicated and sometimes subtle ways, and a comprehensive and continuous systems approach is required to anticipate their potential interactions and the impact of risk mitigation in one area on risk in an entirely unrelated area. Ideally, this systems approach should be applied at all levels, from the most minute components to the overall system in its broadest context, in order to anticipate and identify interactions among and between risks and risk mitigations.
An example of unanticipated interactions among risks is well illustrated by the interaction between risk mitigation for water contamination aboard the NASA orbiters and consequent thyroid dysfunction in crew members. Iodine was used as the bacteriostatic agent in drinking water aboard the U.S. orbiters—a seemingly reasonable approach to water purification. However, the concentration of iodine resulted in a daily iodine intake that far exceeded the recommended daily allowance and was sufficient to cause chemical evidence of thyroid dysfunction (e.g., increases in thyroid-stimulating hormone) commonly and clinical hyper- or hypothyroidism in several astronauts (IOM, 2004). Similar chemical or clinical abnormalities did not occur among those who flew on the Russian Mir space station even for intervals up to six months, but silver nitrate was used
for water purification aboard Mir. (The problem was solved subsequently by installing an anion exchange resin filter at the water tap, but only after several years of thyroid abnormalities among flight crews.)
Other potential interactions appear in the BR. For example, many of the problems listed under Risk 25 (human performance failure due to neurobehavioral problems) are the result of problems listed under Risk 24 (human performance failure due to poor psychosocial adaptation (NRC, 1998; IOM, 2001). The poor coping skills of one crew member may result in reduced work productivity, leading to increased tension and conflict within the crew and resulting in reduced sleep and increased symptoms of depression, anxiety, and anger among all crew members (Palinkas, 1992, 2003). Whereas some of these potential interactions are identified in Appendix B of the BR, that appendix is not referenced in the body of the text and the current version of the BR does not adequately emphasize these interrelations and their implications for countermeasure development, risk management, and risk mitigation.
Recommendation 2.2
The committee recommends that greater effort be devoted to identifying and explaining the interrelations among risks and risk mitigations that are grouped within and across the cross-cutting categories in the BR.
Status of Readiness Levels
In general, the probability of an adverse event can be reduced in two ways: (1) by eliminating the risky procedure or activity or (2) through mitigation strategies and approaches that reduce the probability of adverse events to acceptable levels. Because space flight, in particular the exploration class missions, carries inherent risks, the BR emphasizes the latter approach through the development and application of countermeasures.
A variety of deliverable products result from the BR; they enable desirable outcomes or solutions to answer research and technology questions and reduce risk to support the human system in space. Progress in these areas is gauged by establishing “readiness levels” that delineate the level of maturity of countermeasures or technologies (Countermeasure Readiness Level [CRL] and Technology Readiness Level [TRL], Table 2-1). The process emulates safety improvement programs (U.S. Department of Trans-
TABLE 2-1 Countermeasure Readiness Level (CRL) and Technology Readiness Level (TRL)
|
TRL Definition |
CRL DefinitionScore |
TRL or CRL |
CRL Category |
|
Basic principles observed. |
Phenomenon observed and reported. Problem defined. |
1 |
Basic Research |
|
Technology concept and/or application formulated. |
Hypothesis formed, preliminary studies to define parameters. Demonstrate feasibility. |
2 |
Research to Prove Feasibility |
|
Analytical and experimental critical function/proof-of-concept. |
Validated hypothesis. Understanding of scientific processes underlying problem. |
3 |
|
|
Component and/or breadboard validation in lab. |
Formulation of countermeasures concept based on understanding of phenomenon. |
4 |
Countermeasure Development |
|
Component and/or breadboard in relevant environment. |
Proof of concept testing and initial demonstration of feasibility and efficacy. |
5 |
|
|
System/subsystem model or prototype demonstration in relevant environment. |
Laboratory/clinical testing of potential countermeasure in subjects to demonstrate efficacy of concept. |
6 |
|
|
Subsystem prototype in a space environment. |
Evaluation with human subjects in controlled laboratory simulating operational space flight environment. |
7 |
Countermeasure Demonstration |
|
System completed and flight qualified through demonstration. |
Validation with human subjects in actual operational space flight to demonstrate efficacy and operational feasibility. |
8 |
Countermeasure Operations |
|
System flight proven through mission operations. |
Countermeasure fully flight-tested and ready for implementation. |
9 |
|
|
SOURCE: NASA (2005, Table 5-5). |
|||
portation, 2002), beginning with a problem definition and concluding with a defined operational improvement or countermeasure.
Currently, the BR proposes 183 projected deliverables. In the context of the BR, these deliverables constitute the risk mitigation plan for the human system. A more detailed description and estimation of readiness of each deliverable is provided in Appendix C of this report. The BR emphasizes, “Roadmap activities must focus on operational issues and solutions to operational problems to support an outcome-oriented approach.” Thus, “bioastronautics research is focusing on deliverables at a readiness level of 4 or greater” (NASA, 2005, p. 17). The committee concludes that this emphasis on an applied research agenda for NASA bioastronautics is not without significant consequences and risks, especially given the relatively immature status of current countermeasure development (see Figure 2-1).
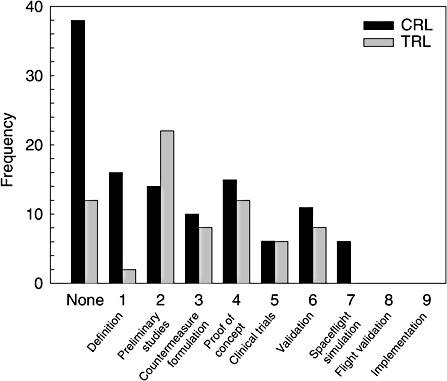
FIGURE 2-1 Countermeasure and Technology Readiness Levels.
Figure 2-1 summarizes the committee’s analysis of the BR’s proposed deliverables. An analysis of the forward work required to complete the BR risk mitigation plan reveals that 50 (27%) of the 183 proposed countermeasures and technology modifications are not yet defined. Of those that were defined, 71 (53%) are at the basic research stage of development (CRL or TRL levels 1–3), 56 (42%) are in the ground testing stage of development (CRL or TRL levels 4–6), and 6 (5%) have reached some stage of flight evaluation (CRL or TRL levels 7–9). Thus, more than half of the defined deliverables proposed in the BR rank below the stage 4 level of readiness and, thus, below the threshold for priority in bioastronautics research consideration. Included in these unranked or low-readiness areas are substantial portions of the mitigation plans on behavioral health and performance, radiation, autonomous health care, and water quality monitoring, areas that the committee finds deserving of further attention from NASA (IOM, 2005). To summarize, the state of countermeasure development significantly lags the need.
The committee finds that the majority of projected BR countermeasures, mitigations, or other deliverables are in a nascent state of readiness and are therefore unlikely to receive high-priority attention. Resources (described in Chapter 4) are unlikely to be sufficient to complete the BR mitigation plan in a time frame that enables the exploration class missions envisioned by NASA.
Establishing priorities for in-flight studies will be a significant challenge. Since NASA must address both near-term (e.g., the proposed lunar mission) and long-term (e.g., the Mars mission) objectives, the priorities for access to investigations aboard the ISS will require considerable wisdom to ensure that urgency is not confused with importance. Thus, some apparently “lower-priority” investigations may need to be manifested on the ISS earlier than others that might appear to be of higher priority. For example, studies regarding bone loss may have to take priority on the few remaining ISS flights in order to generate adequate in-flight data to support the Mars mission because countermeasures to bone loss will clearly be essential on a 30-month mission, even though that mission may be many years hence.
With the increasing likelihood that crew time, up-mass, and manning will continue to be problematic aboard the ISS, it will become increasingly important for surrogates of some sort to be used or developed to help assess the medical, nutritional, environmental, and behavioral issues that may confront astronauts who are in conditions of high stress in tight quarters for an extended period of time. The committee believes that analog environments and digital simulation will play an increasingly important role in
the evaluation and mitigation of risks to the human in space and that the BR should reflect the importance of such analog approaches.
Clearly, analog environments can be created on Earth that could duplicate many of these conditions and thus could be used both as a test of hardware and to assess the quality of instruments used to create a selection process for crews. The value of such true analogs has already been demonstrated in bringing to light the medical problems associated with iodination of drinking water and the adverse effect that high iodine levels can have on crew members’ thyroid function because this problem was demonstrated in ground-based simulations of space flight (IOM, 2004). Thus, specifically created mission analogs are useful to test not only behavioral issues but many of the medical issues that will face the crew as well. Practicality, however, would dictate that rather than “starting from scratch,” the large amount of information that already exists from analog environments such as saturation diving, polar expeditions, bed rest, centrifuge, mock Crew Exploration Vehicle (CEV) expeditions, and submarines be used appropriately.
Submarines are but one example among the many analog environments that could be used both prospectively and retrospectively to help address some of the issues that may confront astronauts. From the 1960s to the mid-1980s, medical officers were assigned to submarines, and these physicians were required to write a research thesis on a relevant research topic. This resulted in a large number of unpublished but peer-reviewed theses, which can be obtained from the Naval Undersea Medical Institute (NUMI) and the Naval Submarine Medical Research Laboratory (NSMRL). A significant percentage of these reports addressed behavioral, environmental, and medical issues that were encountered on these deterrent patrols; therefore, they may be a useful resource for retrospective information.
Continuing the example in a prospective fashion, many parallels can be drawn between the “wardroom” of a nuclear submarine and a crew of astronauts on a long mission. Typically, wardroom officers on board a nuclear submarine are college graduates with highly technical educations, including postgraduate education. They are all highly motivated and committed to their jobs, and they live in confined environments for extended intervals. Thus, in several respects they are similar to flight crews, and they might be useful surrogates to examine the efficacy of various assessment instruments (e.g., for crew interaction, cohesiveness, and leadership). There are limitations, however, to the value of analog environments, based on the
extent to which they reproduce the crew environment in the ISS or the proposed CEV. For example, the U.S. submarine service does not include women crew, nor does it usually include international crew as integral members of the wardroom team. U.S. experience might be supplemented by experience from other countries such as Norway and Denmark, whose submarines include women crew members, but this raises cultural differences as well.
Numerous other highly appropriate analog environments could be used. For example, the data from experimental saturation diving facilities could provide opportunities that mimic extravehicular activities, as well as crew quarters and environments; polar expeditions could provide information about long-term isolation; and prolonged bed rest can mimic at least several aspects of the musculoskeletal changes associated with microgravity. None by themselves is ideal, but collectively these and related approaches, supplemented by digital simulation approaches, can provide important supportive data in an era of restricted opportunities for in-flight clinical investigation.
Recommendation 2.3
The committee recommends that NASA initiate an aggressive program, including the use of animal models, analog environments, and space flight, to significantly accelerate the progress of all Countermeasure Readiness Levels and Technology Readiness Levels that are essential to support the proposed exploration agenda. Countermeasures and technologies at an undefined or low state of readiness (the majority of the current portfolio) should receive renewed attention. The committee notes further that failure to do so will jeopardize the exploration program outlined in the President’s vision for exploration of January 2004.
FUSING THE RELATIONSHIPS BETWEEN HUMAN FACTORS AND TECHNOLOGY IN THE BR
The interrelationships and interactions between technology and human health and performance are evident in all aspects of daily life, but these take on new dimensions and importance as NASA moves to more ambitious exploration agendas, especially longer-term missions. Spacecrafts have evolved considerably to accommodate these needs; consider the evolu-
tion of internal volume and crew accommodations in the sequence of spacecraft from Gemini to Apollo to Orbiter to the ISS, for example, as longer-duration missions were planned. However, the consequences of human-technology interactions become more profound as mission duration and the expectations for crew task performance increase. (New space suits that permit crew to assemble fragile, possibly gossamer-like, components of radio telescopes or other devices while working in deeper space are an example; crew quarters for a 30-month mission are another, but innumerable examples could be cited in the current and future versions of the BR.) The committee concludes that increased linkages in certain areas, specifically Human Systems Integration and Food and Nutrition, can be accomplished by modifying content in the BR. Each one of these areas is addressed in the following sections.
Creating the Cross-Cutting Category “Human Systems Integration”
The BR lists six risks that correspond to human factors and behavior and performance. Four of these risks (23, 24, 25, and 26) fall within the cross-cutting category “Behavioral Health and Performance,” and two of the risks (44 and 45) fall within the cross-cutting category “Advanced Life Support.” These classifications reflect two separate perspectives, one based in the social, behavioral, and clinical sciences and one based on engineering and technology. However, both perspectives are critical to understanding human behavior and performance in space. These perspectives are also united by their treatment of the human both as a system of systems (e.g., bone, muscle, cardiovascular, respiratory, and neuropsychological) and as a component of a larger system of systems (e.g., advanced life support). Keeping these six risks in two separate cross-cutting areas may create certain limitations to understanding the linkages among these risks and, thus, may impair understanding of the interactions among risks and risk mitigation strategies.
As evidence of the linkage among risks that currently fall within two separate cross-cutting categories, both Risk 24 (human performance failure due to poor psychosocial adaptation) and Risk 45 (poorly integrated ground, crew, and automation functions) address ground–crew interactions. In Risk 24, the risks are framed in psychological terms such as displacement of hostility (Kanas et al., 2000), whereas in Risk 45 they are framed in technological terms (Caldwell, 2000, 2005). Although the two risks emphasize different causes of dysfunctional ground–crew relations, the causes
are in fact interconnected to a greater extent than is reflected in the current separate classifications, and mitigation of these risks will likely require a combination of both engineering and psychological solutions. For example, poor engineering of information transmission routines within mission control, and between the crew and mission control, may impede ground–crew communication and decision making, resulting in increased ground–crew tension, increased hostility, and reduced cooperation in task completion (Kanas et al., 2000, 2001a,b). The committee noted that dysfunctional ground–crew communications have impacted previous missions, including quite publicly the ground–crew tension that was evident during Skylab 3 (Zimmerman, 2003, pp. 73–80).
The link between humans and engineering is essential for enhancing mission success and crew performance. For example, Callaghan et al. (1992) observed that the development of methods was as important as the development of standards. Similarly, Whitmore et al. (1999) indicated that the first research priority for the ISS should be in-flight research tools to understand habitability. The second priority was to identify human factors critical to habitability and determine how these could be tested in microgravity and analog environments. Adams (1999) also emphasized the need for habitability studies. Other researchers have highlighted the importance of human systems integration. Peacock et al. (2001), for example, identified the following technology issues for manned space missions: (1) limitations to astronaut mobility and force output while wearing extravehicular activity (EVA) clothing, (2) need for physical restraints and mobility aids in microgravity, and (3) maintaining spatial orientation. The need for enhanced human–robot interactions was identified by Gross et al. (2002), and Hartman (2003) identified the human systems interaction considerations associated with the martian weather, which includes temperature extremes (−87°C to −25°C) and windstorms that will cause dust to lodge in seams and crevices and reduce visibility to less than 1 meter at times, all in an atmosphere that is almost pure CO2, with a barometric pressure that is 1 percent that of Earth’s surface (about equivalent to the pressure at 110,000 feet above Earth).
The committee concluded that human factors are a high priority in space engineering design, especially in an era of planetary exploration. Linking human factors with engineering perspectives in the BR is essential for the development of countermeasures. For example, the extent of musculoskeletal weakness upon arrival in a gravitational environment after long-duration space flight will depend considerably on the engineering and tech-
nology (e.g., artificial gravity, exercise equipment) that are incorporated in the CEV. Similar arguments apply to the control of radiation exposure and the identification of coping skills and other preventive measures to address the human factors associated with prolonged space flight.
Recommendation 2.4
The committee recommends that NASA create a cross-cutting category that spans the two existing categories of “Behavioral Health and Performance” and “Space Human Factors Engineering” risks listed currently in the area of the “Advanced Human Support Technologies.” This new category should be labeled “Human Systems Integration,” consistent with the terminology currently in use by the U.S. Department of Defense (2004) and the Human Systems Integration section in NASA Headquarters. Further, the committee implies by this recommendation that NASA consider placing other risks in this category over time, to facilitate collaborative effort by clinical and engineering scientists in defining, measuring, and mitigating each of the Human Systems Integration risks.
Creating the Cross-Cutting Area “Food and Nutrition”
Maintaining the crew’s overall health will be essential for the success of exploration missions, and food safety, food quality, and nutrition will play a major role in achieving overall health. Extensive reviews of the impact of nutrition on space travelers have been conducted (Stein, 2001; Lane and Feeback, 2002). The composition, safety, quality, and quantity of food and water may all impact the physical and mental health of the crew during space missions, particularly when such missions are long term.
Establishing the optimal nutrient requirements for the crew in space is critical not only for the maintenance of the crew’s health during flight—the most immediate concern of the BR—but also for the health of astronauts after they return to Earth. However, there are very few data on the nutrient requirements of human subjects in extraterrestrial environments, and the problems posed by this scarcity of data are compounded by the small sample size from which existing data on the role of nutrition in maintaining human health in space are drawn. Thus, weight management and plasma levels of lipids, vitamins and minerals, salts, protein, and carbohydrate may be impacted by nutritional intake, in conjunction with the amount of physi-
cal activity undertaken by the crew and by space flight itself. Smith and Heer (2002) pointed to the need to ensure adequate dietary intake (and synthesis, when applicable) of various nutrients involved in bone and calcium homeostasis, including calcium, vitamins D and K, protein, sodium, and phosphorus. Similarly, homeostasis of red and white blood cells, as well as vascular integrity, bone mass, and osmolality, may be altered by the quality of nutrition (Smith et al., 2005), whereas crew morale can be affected by the appearance and quality of food (Kerwin and Seddon, 2002). In addition, adequate quantity and quality of water must be ensured.
Despite the efforts by NASA’s nutrition and food scientists, there is evidence that astronauts have had energy intakes 30 percent to 40 percent lower than their needs during space missions (Smith and Lane, 1999), not because of faulty planning in terms of nutrient intake or unbalanced menus, but because of such factors as time constraints (e.g., time for meal preparation and consumption), work overload, and lack of appetite. Moreover, it is well established that astronauts’ energy expenditures in space are unchanged or even increased from those on Earth (Lane et al., 1997; Stein et al., 1999).
According to Smith et al. (2005), several changes in nutritional status after space flight have been observed. In addition to insufficient energy intake, vitamin D levels were altered after long-duration missions (4 to 6 months), even when the vitamin was taken as a supplement during flight. Further, there was evidence that the metabolism of this vitamin may have been affected by the long-term stay of cosmonauts in the Mir station. Altered vitamin D status, in turn, was associated with increased bone resorption after landing. The same authors reported severe decreases of up to 45 percent for magnesium and phosphorus concentrations. The former may be of concern in long-term missions because of the role of magnesium in preventing formation of renal stones (Su et al., 1991).
Other vitamin levels are also affected by prolonged human exposure to the space environment. The level of vitamin K, an important element in maintaining bone health, was reported to decrease during space flight, and levels of vitamin E and folate may have decreased also (Smith et al., 2005). According to Smith et al., it is not known whether the observed decrease in folate—attributed to inadequate food intake, not to food processing techniques—would be accentuated during prolonged space missions. A review by Lucock (2000) suggests that the role of this B vitamin in maintaining good health may extend beyond prenatal conditioning and a positive influence on cardiovascular disease, to encompass several types of cancer, dementia, and affective disorders.
Decreased red blood cell (RBC) mass after short- and long-term space missions—at a rate of more than 1 percent per day, eventually reaching as high as 10 percent to 15 percent after 2 weeks of flight—is another concern reported and discussed by Smith (2002). He indicated that data from the Spacelab Life Sciences Shuttle missions showed that the release of new RBCs is decreased by weightlessness and that newly released RBCs, larger than the more mature circulating cells, are then selectively removed from the circulation. Such decreases in RBC mass were accompanied by decreases in body fluid volume, and both effects were attributed to the body’s apparent sense of decreased blood volume requirement. As a result, anemia has been observed during many space missions. Destroyed RBCs, in turn, release iron, which is then stored, as evidenced by increased levels of sodium ferritin (Alfrey et al., 2000). Although indices of iron metabolism and erythropoiesis returned to normal within days of landing, increased levels of stored iron and its availability in tissue would suggest a need to reduce iron intake during long-duration missions, given that the long-term effects of this condition are unknown (Smith, 2002).
Muscle loss early in flight has been reported to occur as a result of reduced protein synthesis by inactive muscle (Ferrando et al., 1996) and to continue at a slower rate throughout space missions. As a result, astronauts returning from missions as short as 1 or 2 weeks have exhibited lack of coordination, weakness, and fatigue (Edgerton and Roy, 1994; Riley et al., 1995). These conditions, described by Adams et al. (2003) and reviewed by Baldwin et al. (2003), may adversely influence performance on extended missions.
In addition to nutritional intake, the space environment itself may have marked effects on the nutritional status of astronauts; the above-mentioned hematological changes during space flight are but one example. Another is the adverse effect of increased radiation in space, which may accelerate the degradation or oxidation of food components and alter the potential mitigation of these effects through the protective action of antioxidants (including various vitamins). Antioxidants could be added to food to protect both the foods and their intended consumers (Lane and Schoeller, 1999). As stated in a short, on-line version of these authors’ work, “As long as space travelers can take food from earth with them, it may be possible to design diets that are capable of reducing these problems and other problems. However, as voyages become longer and longer, and the crews become more dependent on food that they will grow and process during their flight, this becomes more of a problem. It is already apparent that as the
diet of astronauts becomes more vegetarian, plant sources rich in calcium and high in antioxidants with a high energy content will be most desirable” (Lane and Schoeller, 2005).
Finally, issues of palatability, variety, cultural preferences and expectations, and the social interactions and connotations of mealtime must be considered. Although food science and nutrition are two separate disciplines, their interrelation is so important that many universities across the nation and elsewhere—recognizing the need to more closely integrate these disciplines—have merged their food science and nutrition departments in recent years.
In view of the many facets of potential physiological and psychological impacts of nutrition on the crew during prolonged space missions, and the resulting effects on crew performance and physical and mental health during and after space missions, particularly long-term missions, the committee concurs that nutrition is a cross-cutting theme and should continue to be reflected as such in the BR. However, the committee emphasizes that nutrition alone does not encompass all of the concerns related to diet and believes that the title should be expanded to encompass the technology aspects of food safety and quality (Risk 38) and the clinical aspects of human nutrition (Risk 16) to further link the technology with the human factors, as recognized in universities around the world.
Recommendation 2.5
The committee recommends that the cross-cutting area “Nutrition” be renamed and expanded to “Food and Nutrition” to more fully encompass the concepts of dietary needs for space flight and emphasize the relationships between nutrition and food technology. Further, the committee recommends that the impact of inadequate food and nutrition on processes related to mental and physical health risks and maintenance of the space environment and life support systems be defined from the standpoints of food safety, quality, and quantity, and interventions proposed if problems occur.
SPECIFIC ISSUES
Specific issues are those areas that deserve focused attention and refinement in the BR in order to more effectively accomplish its goals as a man-
agement tool. They should be viewed as tactics for the BR, whereas the overall issues should be viewed as strategies.
Reclassification of Behavioral Health Risks
The existing cross-cutting category “Behavioral Health and Performance” in the BR includes four categories of risk: human performance failure due to poor psychosocial adaptation (Risk 24), human performance failure due to neurobehavioral problems (Risk 25), mismatch between crew cognitive capabilities and task demands (Risk 26), and human performance failure due to sleep loss and circadian rhythm problems (Risk 27). Unfortunately, there is considerable overlap in these categories. Both Risks 25 and 26 make reference to cognitive problems. Risks 24 and 25 both include mood disorders. Further, human performance failure due to poor psychosocial adaptation (Risk 24) belies the fact that there are three separate determinants or moderators of poor psychosocial adaptation under conditions of prolonged isolation and confinement (Palinkas, 2001). These include intrapersonal factors such as personality styles and strategies for coping with stress; interpersonal factors such as group cooperation and conflict; and organizational factors such as the cultural systems of the participating national space agencies and contractors, the values they embody, and their influence on health and behavior.
The countermeasures to address these problems are not well defined in the BR. Thus, reference is made to the use of screening and selection as a potential countermeasure to each of the four risks identified in behavioral health and performance. However, the BR does not acknowledge that there are at least two potential strategies for screening and selection. Screening and selection of astronaut personnel in the U.S. space program has traditionally been based on a “select-out” philosophy that excludes those with any diagnosable psychiatric disorder or high likelihood of developing such a disorder (Santy, 1994). Although this approach has generally been successful in minimizing decrements in behavior and performance during short-duration missions (1 to 14 days), the advent of longer-duration missions, ranging from earlier 3-month assignments aboard the Mir Space Station to the proposed 3-year mission to Mars, has generated greater interest in an approach that is based on a “select-in” philosophy. Such an approach would seek to identify candidates whose personality traits enhance their ability to function at high levels (both physically and mentally) while expe-
riencing chronic stress and to interact productively as a member of a crew (Santy, 1994).
Another option would be to expand the range of mental disorders that are considered as part of the select-out criteria. People with personality disorders often make their own interpersonal problems worse because they are rigid, inflexible, and unable to adapt to the social challenges they face (Chen et al., 2004; Pagano et al., 2004), and they create problems for those around them as well. Some personality disorders, including narcissism (Morf and Rhodewalt, 2001), would be expected to disrupt group cohesion and interfere with interpersonal relations involving other members of the space crew as well as Earth-based support personnel.
The committee concludes that empirical evaluation of current (and proposed) select-in and select-out procedures must be conducted among members of the astronaut corps during all phases of training and mission preparation. At present, the BR offers no guidelines for improving select-out procedures to reduce the likelihood of human performance failure due to poor psychosocial adaptation, neurobehavioral changes, cognitive overload, or disruption of sleep and circadian rhythms. Additional screening criteria that might benefit from further research include history of family disorders, childhood experiences of abuse or trauma, and stress reactivity.
Two other approaches for screening should also be given further consideration in crew selection. One involves the method of selection of specific crew members from among the pool of eligible astronauts. At present, these decisions appear to be made with little consideration of an external professional evaluation of crew compatibility.
Recommendation 2.6
The committee recommends that the Astronaut Office and representative flight surgeons be consulted regarding the crew selection process in order to place greater emphasis on the roles of crew compatibility and team performance in overall mission success.
The second approach involves the use of analog environments and behavioral challenges to evaluate individual and team performance. After selection of a specific set of crew members and during their training for a mission, the crew should be assessed while it responds to carefully designed stressful experiences that would mimic events that could occur during a flight. These experiences might provide an opportunity to observe ways in
which crew members respond, and these patterns might actually predict future performance more accurately than other kinds of assessment procedures. The committee recognizes that some of these concepts may be included in some of the research and technology questions in the BR, but they are not prominent and thus are pointed out here to emphasize that they should be part of the behavioral health planning process.
Similarly, the BR provides only modest guidance regarding incorporation of evidence-based interventions or countermeasures for mental disorders that might be experienced in space. There is evidence to support cognitive–behavioral treatments for depression or anxiety disorders in other populations (DeRubeis et al., 1999; Roy-Byrne et al., 2005), but their effectiveness in space flight or flight simulation is unknown. For example, brief forms of cognitive and interpersonal therapy have been demonstrated to be effective in the treatment of depression (Hollon et al., 2002; DeRubeis et al., 2005; Otto et al., 2005), but it is not clear that these interventions would be effective in a mode that did not allow for face-to-face discussions, or in which significant communication delays would impose extended pause times in the conversation. Careful evaluation of these procedures should be conducted using analog environments.
The committee concluded that the BR does not provide clear guidance for the research necessary to develop effective countermeasures for behavioral health risks of extended flight. In part, this is the result of a process that has “lumped” together certain distinct risks into the same category and, in part, due to “splitting” the same phenomena (e.g., mood disorders and cognitive performance) into more than one risk category without explication of their interrelationships. This has tended to both trivialize the risks and complicate efforts to develop effective countermeasures.
Recommendation 2.7
The committee recommends that behavioral health risks within the proposed new cross-cutting category of Human Systems Integration be grouped into categories based on clinical outcomes such as interpersonal conflict, affect regulation, decrements in cognitive performance, mood disorders, and sleep disorders, rather than categories such as psychosocial, neurobehavioral, cognitive, and circadian rhythms, and that the interrelations between these categories be delineated clearly.
The committee suggests convening a workshop of investigators, flight operations medical personnel, and expert clinicians who have experience in behavioral interventions for the management of mental disorders that develop during times of prolonged stress. The purpose would be to estimate the likelihood of such disorders developing during a 30-month extended mission, to identify the personality characteristics associated with a low risk for the development of such disorders, and to recommend evidence-based behavioral interventions to minimize the severity of the disorders if they do develop.
Finally, the committee notes that the BR contains no references to human sexuality, and this oversight should be corrected. Whereas the committee recognizes the task-oriented nature of both the crew and the mission, it concludes that ignoring the potential consequences of human sexuality is not appropriate when considering extended-duration missions. Areas of concern for the 30-month Mars mission include the potential psychological and physiological consequences of sexual activity, consequences that could endanger life, crew cohesion, performance, and mission success. Some risks can be eliminated but others cannot. For instance, the risk of pregnancy might be mitigated by crew selection. However, the long lead time to answer questions about the efficacy, safety, and side effects of contraceptive medications may require that studies to answer these questions be completed prior to crew selection or that other measures be used to mitigate the risk of pregnancy.
Recommendation 2.8
The committee recommends that issues of human sexuality be addressed in the BR in relation to long-duration missions such as the proposed Mars Design Reference Mission.
Psychological and Physical Impacts of Space Flight on Performance
To more fully address human behavior and performance issues during long-duration space flight, NASA must address a number of significant psychological and biological factors that will influence the ability of astronauts and crews to perform effectively. Effective performance includes the maintenance of individual high-level cognitive, communication, and physical skills and the maintenance of overall crew skills and teamwork. The latter require effective interactions with Earth-based support and recovery systems, as well as harmonious, flexible, and effective group relations among
crew members over long periods of time and in an environment that may be associated with a variety of stresses.
Several of the risks associated with space flight involve human responses to stress. Stress-related performance decrements in extended space flight have been documented. Sauer et al. (1997) reviewed the evidence and postulated that sustained stress will result in a decrease in motivation and increased risk of errors. They stated that Soviet scientists reported decreased information processing speed within the first nine days of a space flight, especially for first-time crew members. Isolation studies conducted in the former Soviet Union using spacecraft simulators indicated that performance decrements included increased decision time, increased errors of commission, and decreased attention span. Cognitive effects associated with fatigue were also noted in hyperbaric chamber isolation studies. In actual extended space flights, fatigue increased over time, with associated increases in errors.
The physiological response to stress includes increased concentration of stress hormones (e.g., catecholamines, cortisol), and these alterations may affect a number of the risks identified in the BR (including Risks 5, 6, 8, 9, 10, 24, 25, 26, 27, and 28). Examples of altered human health associated with stress responses include cardiac dysrhythmias (Mackstaller and Alpert, 1997), enhanced bacterial growth (Klaus, 2002; Lyte, 2004), altered immune function with increased risk of infection (Rabin, 1999; Miller et al., 2004), exacerbation of allergies (Wright et al., 2005), and emergence or exacerbation of autoimmune disease (Ackerman et al., 2002). Further, stress hormone increases are associated with altered central nervous system function (Zarkovic et al., 2003; Brown et al., 2004), sleep disturbances, and altered circadian rhythms (Maschke and Hecht, 2004). Therefore, infectious disease, autoimmune disease, atherosclerotic heart disease, hypertension, and the mental conditions of depression and possibly accelerated loss of cognition may be influenced by the hormonal response to stress presented by an extended-duration space mission (McEwen et al., 1999). Although not all of these relationships have specifically been demonstrated during space flight, the prudent approach would be to assume that these relationships persist in space, at least until such time as this assumption is disproved (an unlikely possibility, given the limited opportunity mentioned earlier to collect significant data during flight).
Whereas many of these concerns are suggested in the BR, their specific links to stress hormones—and the implications thereof—are not emphasized, and neither are the implications for crew selection. The likelihood of
maintaining mental and physical health during periods of prolonged space flight may be enhanced if crew members (1) have low responses to stress (low stressor-induced elevation of cortisol and catecholamines) and (2) are trained in coping skills that minimize the stressor-induced increase of these hormones. This would involve selecting astronauts who are low stress responders and who have good stress coping skills.
Another source of concern in long-duration space flights is the possibility that crew members might experience major mood swings related to either depression or mania at various times during the flight. For example, the etiology of clinical depression is undergoing reevaluation based on new studies indicating that increased levels of glucocorticoids can damage neurons that are important to the genesis of depression (Sapolsky, 2004).
Based on this and related evidence in the stress–response literature, the committee concluded that stress–response analyses should be included among selection criteria. Selection criteria that might be considered by NASA include low stress responsiveness determined by Stroop test measurements of blood pressure and heart rate (Probst et al., 1997; Seibt et al., 1998; McCaffery et al., 2003) and performance on psychological tests and personality questionnaires that have been demonstrated to be related to the ability to interact, communicate, and work effectively with others in a closed environment for extended intervals.
Radiation Effects: Establishing Risk-Specific Radiation Exposure Levels
Exposure to ionizing radiation from the solar wind, solar particle events (SPEs), galactic cosmic rays (GCRs) and other sources is a major concern for space flight beyond low Earth orbit (LEO). Complex deoxyribonucleic acid (DNA) damage from radiation may result in cell death, causing acute symptoms if enough cells in a tissue are affected. Also, DNA damage repair mechanisms (e.g., nonhomologous end joining) for complex damage are not error free, and repair errors can result in cellular mutations that contribute to eventual carcinogenesis. Whole-body radiation at doses high enough to cause serious acute effects has been associated with substantial—and probably unacceptable—increases in lifetime cancer risk in terrestrial populations (Hall, 2000). Therefore, radiation protection measures aimed at minimizing radiation-related cancer risk are also likely to protect against severe acute effects. A possible exception to this general observation is that central nervous system (CNS) tissue may be more vulnerable than other
tissues, and CNS impairment may occur following exposure to high-mass, high-Z, high-energy (HZE) radiation from GCRs at low doses and low dose rates.
It is now well established that the radiation dose (mainly due to gamma rays) from the atomic bombings of Hiroshima and Nagasaki is also associated with increased risk for nonmalignant disease, particularly heart disease, stroke, respiratory disease, and digestive disease, and that the impact in terms of mortality may be roughly comparable to that seen for solid cancers (Preston et al., 2003). Radiation-induced cataracts are another established late health effect. Thus, any assessment of radiation-related health effects should include both malignant and nonmalignant disease.
The International Commission on Radiological Protection (ICRP) system of differential weighting of doses by radiation quality and by tissue—depending on susceptibility to radiation-related disease and the severity of such disease in terms of mortality and morbidity—may be a useful model for construction of a common metric for radiological risk (ICRP, 1991). (See also the successor document to ICRP 60, now in preparation; supporting documents and the report will be made available for public review on www.icrp.org prior to finalization.) However, the radiation environment of space travel beyond LEO is more complex, and less well understood, than the mostly low-dose radiation encountered by radiation workers and the general public that is the main concern of the broader radiation protection community. Also, individual tolerance for late health effect risks may be greater among the astronaut community than among the general population, although possibly not greater than that of some radiation workers. The NASA adaptation of the ICRP weighting scheme should be tailored to its unique exposure scenarios and should take more account of uncertainties in radiation dose and associated risks (i.e., it should address in a probabilistic way the question, How high could such risks plausibly be?).
Continuing experimental studies of biological effects from exposure to the radiation from GCRs—including experimental carcinogenesis—should refine our understanding of the relative biological effectiveness of such radiation compared to gamma and X-rays, so that the extensive dose– response information for these sparsely ionizing types of radiation can be adapted for application to risks associated with GCR exposure. As demonstrated by Cucinotta et al. (2001), it is possible to make meaningful inferences about cancer risk associated with exposure to GCRs based on expert judgment, with quantified subjective uncertainty estimates about the relative biological effectiveness of HZE radiation. Such inferences can and
should be refined in the light of new research findings after these findings have been reviewed and evaluated by the wider radiation research community.
The amount of radiation exposure will have potential impact on the crew’s health through increased risk of malignancy; altered hematopoieses due to bone marrow suppression; increased susceptibility to infection mediated by immune system suppression and possible mutation of microorganisms allowing them to escape from regulation by the innate host defense system; and unknown effects in tissue, such as CNS effects due to tissue damage and subsequent inflammatory response. Radiation therapy for patients with malignancy often has fatigue as a side effect (Jacobsen and Thors, 2003). Whether radiation exposure may pose a similar problem on long-term missions should be evaluated. Radiation risks differ considerably between a 12-month mission in LEO aboard the ISS and a 30-month mission to Mars because the latter will be exposed to significantly greater galactic cosmic radiation, for example.
Although the major technology issue is protecting astronauts from health risks associated with exposure to radiation, there are potential performance decrements associated with radiation exposure at lower levels than those that affect health. Astronauts traveling beyond LEO—particularly on lengthy missions—will have a high probability of exposure to GCRs, which are more numerous and energetic near the solar minimum, and to SPEs, which occur more frequently near the solar maximum. The effects of such exposures, especially those to GCRs, are not known, but some of these effects can be estimated with substantial (and quantifiable) uncertainty on the basis of present knowledge. As new experimental and theoretical information is accumulated, this uncertainty should decrease. According to Wilson et al. (2002), some protection against these effects may be afforded by either lunar or martian surfaces.
Adverse radiation effects on pharmacological preparations and food nutrients may also occur during missions. Some drugs are stable in a high-radiation environment, whereas others will not tolerate even moderate exposure to sunlight on Earth. Those currently deemed radiation-stable have not been studied in the unique HZE radiation environment characteristic of long-duration missions beyond LEO.
The committee concludes that radiation effects are given ample weight in the BR, and its suggestions are intended to draw NASA’s attention to ways in which the BR might be refined, and perhaps simplified, when considering ra-
diation risks and risk mitigation. Further, the committee concurs with NASA’s assessment that the duration of the mission and the distance from Earth will determine the amount and type of radiation exposure and the required shielding for both the vehicle itself and the protective wear for EVA, with the associated weight and design implications. However, the conventional rule of thumb for terrestrial radiation protection (i.e., that protection against late radiation effects such as increased cancer risk will also protect against acute radiation effects) may not hold for HZE from GCRs, particularly with regard to CNS impairment. Therefore, the committee also concludes that NASA must conduct further research to clarify the extent to which protracted or low-dose HZE radiation exposure might contribute to mission-damaging CNS effects.
Recommendation 2.9
The committee recommends that a safe radiation exposure level be established by NASA for each relevant risk, based on projected flight duration and distance from Earth, and that the technology to keep the level of exposure below that limit be ensured. Inherent in this recommendation, and consistent with Recommendation 2.3, the committee concludes that NASA must conduct further research to clarify the extent to which protracted or low-dose HZE radiation exposure might contribute to mission-damaging CNS effects.
As with the other components of the BR, it will be essential to follow the developments in both biological research and shielding technology to ensure crew health and safety for longer-duration, higher-radiation-exposure exploratory missions.
Assessing the Sources and Impact of Long-Duration Space Flight on Crew Health and Incremental Risk
Crew performance can be compromised by (1) intrinsic health alterations that occur spontaneously due to natural processes in the space environment, (2) aspects of the space environment that impair health, and (3) inadequate or malfunctioning life support systems. Differences among the Design Reference Missions (ISS, Moon, and Mars), in terms of factors such as duration, amount of gravity, and type and extent of radiation exposure, are examples of how the mission itself will influence the interactions be-
tween risks associated with natural processes, the space environment, and life support systems. Thus, the risk priority and potential for interactions among these sources will vary based on the Design Reference Mission, and these factors will impact the severity, implications, and countermeasure development that would be appropriate for each situation. Whereas the BR relates the human health risks to the Design Reference Missions, it does not specifically categorize the etiology of the risk, and operational decisions may depend significantly on the source of these risks.
Recommendation 2.10
The committee recommends that, wherever possible, NASA use actuarial data (such as those in the Longitudinal Study of Astronaut Health and the related comparison group of Johnson Space Center employees, as well as additional sources such a genomic data, where available) to estimate and/or model the likelihood of intrinsic health alterations for crew who will be part of the Mars mission. Utilization of this information as part of the selection criteria for astronauts should be considered. After intrinsic health risks are estimated, NASA should then estimate and/or model the contribution of the space environment and life support system malfunction to increased risk.
The committee notes that such approaches are used currently for the assessment of radiation risks and believes that the expansion of this concept will benefit NASA operations and decision making, as well as the astronauts, as they assess the risks of long-duration exploration missions. Because of the complexity of risk determination in the context of limited available research information, it may be useful also to look beyond traditional actuarial tables and utilize advanced computer simulations of human physiology to target mechanisms of risk and assist in the development of countermeasures. Such broad-based models of human physiology are readily available and have been used successfully to focus research design and delineate mechanisms. They can also be used in a predictive fashion when it is impossible to test the conditions through experimentation. A quantitative and integrative approach could be used to guide the BR process when objective data are unavailable or when sample sizes are unusually limited.
Autonomous Medical Care and Self-Care
The committee recognized that health care will, of necessity, be limited during space flight, and it will not be feasible to manage all medical conditions optimally during the three reference missions. The current status of CRLs clearly illustrates the magnitude of the problem for bioastronautics in general and for autonomous health care specifically. To prepare for risk mitigation and autonomous medical care to the extent possible, it may be helpful to consider the research issues in three categories, based on the type of problem and the nature of the research required to address the problem. These categories are the following:
-
Biological issues: biological and pharmacological questions requiring basic research with cell cultures, animals, drugs, and so forth, in the space environment (most likely during the ISS and lunar missions).
-
Operational issues: adaptations needed to make equipment and procedures operate effectively in microgravity or the environment of the ISS or exploration vehicle. Some of these studies can be conducted during parabolic flight with brief microgravity or simulated on Earth, whereas others will require validation in flight.
-
Health care delivery issues: conditions that could be treated during a mission and the equipment and supplies required to implement that treatment. Some of these issues can be studied in analog environments; others may be explored by “thought experiments” with expert clinicians, on the basis of current and expected future development of novel diagnostic and therapeutic capabilities. Both approaches should be supplemented with digital simulations of acute responses and chronic adaptation that use models of contemporary research findings.
The BR addresses fundamental issues of wound and fracture healing and acknowledges that further studies must be done in the space environment. Anecdotal evidence suggests that lacerations and abrasions heal slowly in the space environment (Kirkpatrick et al., 1997). The complex interaction between the immune system, inflammation, and wound healing implies that alteration in any part of the system might affect the functioning of the system as a whole (Yang and Glaser, 2002). If a specific issue related to wound healing is identified, basic research to determine the nature of the deficit might yield an insight into the specific therapy. For example, high-dose corticosteroids impair wound healing, and this deficit is at least par-
tially ameliorated by administration of vitamin A (Talas et al., 2002, 2003). Similar studies into fracture healing and the immune system in a prolonged space environment are outlined in the BR. Because of the likelihood that injuries will occur and the paucity of mitigation strategies at present, these and related studies must be given high priority. Similarly, the issue of drug stability in high-radiation environments mentioned earlier (see discussion of radiation) has to be addressed.
In the operational category, studies during parabolic flight have provided some guidance into issues such as airway management, cardiopulmonary resuscitation (CPR), control of body fluids (e.g., blood) in microgravity, and suction. A simple example of the operational challenges is apparent in the application of CPR: both victim and rescuer must be mechanically stabilized in order to deliver effective chest compression in microgravity, and there are few data that evaluate the effectiveness of CPR in providing organ perfusion under these conditions. Neither adequate suction—a basic requirement for airway management—nor the capability to vary inhaled oxygen concentration is currently available on the ISS (Bacal et al., 2004).
Both the biological and the operational research issues are aimed not at fundamental science, but at support of the specific health care delivery issues that are focused on crew health and mission success. What to treat? What not to treat? What to take in the vehicle’s medical supply manifest? Precedents from the body of literature on health care rationing may be applicable to guide some of these health care delivery questions. An extensive review of the literature on health care in nonterrestrial environments, including a compilation of translated relevant Russian scientific literature, indicated that “the majority of resuscitative and surgical interventions required to stabilize a severely injured astronaut are feasible in a microgravity environment” (Kirkpatrick et al., 1997). However, the applicability of other health care techniques in such environments and the limitations imposed by upload volume and mass may preclude the availability of many techniques and impose a limited selection of options based on risk assessment and logistics. Cost–utility analysis should incorporate probabilistic modeling of the likelihood of encountering a specific adverse event and the benefit—both to the mission and to the individual—of taking action during the mission to mitigate the health problem (Sculpher et al., 2004; Seifan and Shemer, 2005).
As an example, what is the probability that a crew member will develop a malignancy during the mission? Breast cancer might serve as an
example of these concerns. It is generally thought that breast cancer is diagnosed years after the first cells become cancerous and begin to multiply. Annual mammography, ultrasound, and physical examination still miss tumors that become apparent only in retrospect, and some women develop and present rapidly growing breast cancer between annual screening exams. The most sensitive diagnostic modality available currently is a magnetic resonance (MR) scan. However, even if crew were screened pre-flight with all of the available diagnostic modalities, it is conceivable that during the approximately 30-month duration of a projected Mars mission, a subclinical tumor might become clinically manifest. If the only treatment options were radical extirpative surgery, cytotoxic chemotherapy, focused radiation therapy, or some other complex and highly specialized modality, it appears unlikely that treatment would be implemented during the mission. This is an example of the time factor cited earlier. The longer the mission, the more likely is a clinically acute problem to surface. As previously mentioned (see the section on page 26 titled “The Time Factor and Its Impact on Risk”), mission duration will affect access to definitive medical care.
However, new diagnostic and therapeutic approaches may well alter current conclusions. The combination of more precise screening technologies and less invasive or debilitating therapies suggests that both diagnosis and treatment of early malignancies may be feasible in the future. Focused ultrasound is currently being used to seal bleeding vessels (Nields, 2005). Handheld diagnostic ultrasound units are a reality at present. Transcutaneous radio-frequency ablation is being used currently to eradicate small breast tumors (Wood et al., 2002). Thus it is conceivable that developments in ultrasound, MR, or some combination of focused energy diagnostic and therapeutic modalities may allow precise transcutaneous ablation of small tumors by the time a Mars mission is flown. Such a handheld unit would find other applications for other conditions such as treatment of trauma (Noble et al., 2002; Cornejo et al., 2004) and hence be a highly desirable addition to the medical supplies aboard the CEV. Under these circumstances, breast cancer—and perhaps some other malignancies—could move from the category of “cannot treat during mission” to the category of “pursue periodic screening and initiate treatment during mission.” This example illustrates the benefits of focusing the mitigation strategies on the three areas described above and of using an iterative process to evaluate the current status of risks and mitigation strategies, as well as the importance again of linking technology, insight derived from models and simulation, and expert opinion when addressing risk mitigation in the BR.
A factor to be considered in deciding what to treat is that in the worst case, when Earth and Mars are most distant, communications can take up to 20 minutes one-way. Thus, any treatment regimen that necessitates real-time help from Earth would not be feasible, and the determination of what can and cannot be treated with a given crew and equipment mix must take into consideration that delays in communication may be as much as 40 minutes.
Crew selection will have a significant impact on health care delivery. For example, health care delivery approaches can be more sophisticated if a physician is selected as a crew member, and the reverse is true as well—a physician may be required if sophisticated care is deemed appropriate a priori. The committee noted that selection of an international crew could make the health delivery issues more complex because both expectations of and approaches to care differ among countries. Analog environment studies, quantitative risk–utility analyses, and multinational conferences may assist in resolving these questions, which must be addressed prospectively.
The committee concluded that it will be valuable to categorize health care risks into those with minimal and easily managed outcomes through those of increasing severity and decreasing capability for management due to complexity, distance, or duration of the mission in order to prioritize the biological, operational, and care delivery strategies related to the risks defined in the BR.
Recommendation 2.11
The committee recommends that a system be developed for quantitatively evaluating the mental and physical health risks that could affect mission success and crew health and that priorities for countermeasure development (i.e., definitive treatment vs. palliation) be established for the most likely conditions to be encountered during each reference mission. A panel of outstanding medical clinicians should be used to assist NASA medical operations staff in characterizing the likelihood, importance, and “treatability” of each condition.
REFERENCES
Ackerman KD, Heyman R, Rabin BS, Frank E, Anderson BP, Baum A. 2002. Stressful life events precede exacerbations of multiple sclerosis. Psychosom. Med. 64: 916–920.
Adams CM. 1999. The role of habitability studies in space facility and vehicle design. Houston, TX: Lockheed Martin Space Operations Company.
Adams GR, Caiozzo VJ, Baldwin KM. 2003. Skeletal muscle unweighting: spaceflight and ground based models. J. Appl. Physiol. 95: 2185–2201.
Alfrey CP, Rice L, Smith SM. 1999. Iron Metabolism and the changes in red blood cell metabolism. In Lane HW, Schoeller DA (eds.) Nutrition in Spaceflight and Weightlessness Models. Boca Raton, FL: CRC Press.
Bacal K, Beck G, McSwain NE Jr. 2004. A concept of operations for contingency medical care on the International Space Station. Mil. Med. 169(8): 631–641.
Baldwin KM, Edgerton VR, Roy RR. 2003. Muscle loss in space: physiological consequences. In Mark H, Salkin M, Yousef A (eds.) Encyclopedia of Space Sciences and Technology. Hoboken, NJ: Wiley & Sons, Inc.
Brown ES, Varghese FP, McEwen BS. 2004. Association of depression with medical illness: does cortisol play a role? Biol. Psychiatry 55: 1–9.
Caldwell BS. 2000. Information and communication technology needs for distributed communication and coordination during expedition-class spaceflight. Aviat. Space Environ. Med. 71(9 Suppl): A6–A10.
Caldwell BS. 2005. Analysis and modeling of information flow and distributed expertise in space-related operations. Acta Astronaut. 56: 996–1004.
Callaghan TF, Gosbee JW, Adam SC. 1992. Operational space human factors: methodology for a DSO (Paper 921156). Warrendale, PA: SAE International.
Chen H, Cohen P, Johnson JG, Kasen S, Sneed JR, Crawford TN. 2004. Adolescent personality disorders and conflict with romantic partners during the transition to adulthood. J. Personal. Disord. 18(6): 505–525.
Cornejo CJ, Vaezy S, Jurkovich GJ, Paun M, Sharar SR, Martin RW. 2004. High-intensity ultrasound treatment of blunt abdominal solid organ injury: an animal model. J. Trauma 57(1): 152–156.
Cucinotta FA, Schimmerling W, Wilson JW, Peterson LE, Badhwar G, Saganti P, Dicello JF. 2001. Space radiation cancer risks and uncertainties for Mars missions. Rad. Res. 156 (5): 682–688.
DeRubeis RJ, Gelfand LA, Tang TZ, Simons AD. 1999. Medications versus cognitive behavior therapy for severely depressed outpatients: mega-analysis of four randomized comparisons. Am. J. Psychiatry 156(7): 1007–1013.
DeRubeis RJ, Hollon SD, Amsterdam JD, Shelton RC, Young PR, Salomon RM, O’Reardon JP, Lovett ML, Gladis MM, Brown LL, Gallop R. 2005. Cognitive therapy vs. medications in the treatment of moderate to severe depression. Arch. Gen. Psychiatry 62(4):409–416.
Edgerton VR, Roy RR. 1994. Neuromuscular adaptation to actual and simulated weightlessness. Adv. Space Biol. Med. 4: 33–67.
Ferrando AA, Lane HW, Stuart CA, Davis-Street J, Wolfe RR. 1996. Prolonged bed rest decreases skeletal muscle and whole body protein synthesis. Am. J. Physiol. 270: E627– E633.
Gross AR, Briggs GA, Glass BJ, Pedersen L, Kortenkamp DM, Wettergreen DS, Nourbakhsh I, Clancy DJ. 2002. Advances in robotic, human, and autonomous systems for missions of space exploration. Proc. 53rd International Astronautical Congress, Houston, TX.
Hall EJ. 2000. Radiobiology for the Radiologist, 5th Ed. Philadelphia: Lippincott Williams & Wilkins.
Hartman WK. 2003. A Traveler’s Guide to Mars. The Mysterious Landscapes of the Red Planet. New York: Workman Publishing.
Hollon SD, Thase ME, Markowitz JC. (2002). Treatment and prevention of depression. Psychological Science in the Public Interest 3: 39–77.
ICRP (International Commission on Radiological Protection). 1991. ICRP Publication: 1990. Recommendations of the International Commission on Radiological Protection, 60. Annex A. Annals of the ICRP. 21(1–3).
IOM (Institute of Medicine). 2001. Safe Passage: Astronaut Care for Exploration Missions. Washington, DC: National Academy Press.
IOM. 2004. Review of NASA’s Longitudinal Study of Astronaut Health. Washington, DC: The National Academies Press.
IOM. 2005. Preliminary Considerations Regarding NASA’s Bioastronautics Critical Path Roadmap. Washington, DC: The National Academies Press.
Jacobsen PB, Thors CL. 2003. Fatigue in the radiation therapy patient: current management and investigations. Semin. Radiat. Oncol. 13: 372–380.
Johnson JC, Boster JS, Palinkas LA. 2003. Social roles and the evolution of networks in extreme and isolated environments. J. Math. Sociol. 27: 89–121.
Kanas N, Salnitskiy V, Grund EM, Gushin V, Weiss DS, Kozerenko O, Sled A, Marmar CR. 2000. Interpersonal and cultural issues involving crews and ground personnel during Shuttle/Mir space missions. Aviat. Space Environ. Med. 71(9 Suppl.): A11–A16.
Kanas N, Salnitskiy V, Grund EM, Weiss DS, Gushin V, Kozerenko O, Sled A, Marmar CR. 2001a. Human interactions during Shuttle/Mir space missions. Acta Astronaut. 48(5): 777–784.
Kanas N, Salnitskiy V, Grund EM, Weiss DS, Gushin V, Kozerenko O, Sled A, Marmar CR. 2001b. Human interactions in space: results from Shuttle/Mir. Acta Astronaut. 49(3–10): 243–260.
Kerwin J, Seddon R. 2002. Eating in space—from an astronaut perspective. Nutrition 18: 921–925.
Kirkpatrick AW, Campbell MR, Novinkov OL, Goncharov IB, Kovachevich IV. 1997. Blunt trauma and operative care in microgravity: a review of microgravity physiology and surgical investigations with implications for critical care and operative treatment in space. J. Am. Coll. Surg. 184(5): 441–453.
Klaus DM. 2002. Space microbiology: microgravity and microorganisms. In Britton G (ed.) The Encyclopedia of Environmental Microbiology. New York: John Wiley & Sons, pp. 2996–3004.
Lane HW, Gratebeck RJ, Schoeller DA, Davis-Street J, Socki RA, Gibson EK. 1997. Comparison of ground-based and space flight energy expenditure and water turnover in middle-age healthy male US astronauts. Am. J. Clin. Nutr. 65: 4–12.
Lane HW, Feeback DL. 2002. History of nutrition in space flight: overview. Nutrition 18(10): 797–804.
Lane HW, Schoeller DA (eds.). 1999. Nutrition in Spaceflight and Weightlessness Models. Boca Raton, FL: CRC Press.
Lane HW, Schoeller DA. 2005. Cited: Nutrition challenges during space travel—solutions can benefit us all. Medicinal Food News. On-line [available: http://www.medicinalfoodnews.com/vol06/issue3/space.htm]. Accessed 5/05/05.
Lucock M. 2000. Folic acid: nutritional biochemistry, molecular biology, and role in disease processes. Mol. Genet. Metab. 71(1–2): 121–138.
Lyte M. 2004. Microbial endocrinology and infectious disease in the 21st century. Trends Microbiol. 12: 14–20.
Mackstaller L, Alpert J. 1997. Atrial fibrillation: a review of mechanism, etiology, and therapy. Clin. Cardiol. 20: 640–650.
Maschke C, Hecht K. 2004. Stress hormones and sleep disturbances—electrophysiological and hormonal aspects. Noise Health 6: 49–54.
McCaffery JM, Bleil M, Pogue-Geile MF, Ferrell RE, Manuck SB. 2003. Allelic variation in the serotonin transporter gene-linked polymorphic region (5-HTTLPR) and cardiovascular reactivity in young adult male and female twins of European–American descent. Psychosom. Med. 65: 721–728.
McEwen BS, de Leon MJ, Lupien SJ, Meaney MJ. 1999. Corticosteroids, the aging brain and cognition. Trends Endocrinol. Metab. 110: 92–96.
Miller GE, Cohen S, Pressman S, Barkin A, Rabin BS, Treanor JJ. 2004. Psychological stress and antibody response to influenza vaccination: when is the critical period for stress, and how does it get inside the body? Psychosom. Med. 66: 215–223.
Morf CC, Rhodewalt F. 2001. Unraveling the paradoxes of narcissism: a dynamic self-regulatory processing model. Psychological Inquiry 12: 177–196.
NASA (National Aeronautics and Space Administration). 2005. Bioastronautics Roadmap—a risk reduction strategy for human space exploration. On-line [available: http://ston.jsc.nasa.gov/collections/TRS/-techrep/Sp-2005-6113.pdf]. Accessed 1/6/2006.
Nields MW. 2005. Industry perspective: maximizing the benefit of improved detection with guided and monitored thermal ablation of small tumors. Technol. Cancer Res. Treat. 4(2): 123–130.
Noble ML, Vaezy S, Keshavarzi A, Paun M, Prokop AF, Chi EY, Cornejo C, Sharar SR, Jurkovich GJ, Martin RW, Crum LA. 2002. Spleen hemostasis using high-intensity ultrasound: survival and healing. J. Trauma 53(6): 1115–1120.
NRC (National Research Council). 1998. A Strategy for Research in Space Biology and Medicine into the Next Century. Washington, DC: National Academy Press.
Otto JW, Smits JAJ, Reese HE. 2005. Combined psychotherapy and pharmacotherapy for mood and anxiety disorders in adults: review and analysis. Clinical Psychology: Science and Practice 12: 72–86.
Pagano ME, Skodol AE, Stout RL, Shea MT, Yen S, Grilo CM, Sanislow CA, Bender DS, McGlashan TH, Zanarini MC, Gunderson JG. 2004. Stressful life events as predictors of functioning: findings from the collaborative longitudinal personality disorders study. Acta Psychiatr. Scand. 110(6): 421–429.
Palinkas LA. 1992. Going to extremes: the cultural context of stress, illness and coping in Antarctica. Soc. Sci. Med. 35(5): 651–664.
Palinkas LA. 2001. Psychosocial issues in long-term space flight: overview. Gravitat. Space Biol. Bull. 14(2): 25–34.
Palinkas LA. 2003. The psychology of isolated and confined environments: understanding human behavior in Antarctica. Am. Psychologist 58(5): 353–363.
Peacock B, Rajulu S, Novak J, Rathjen T, Whitmore M, Maida J, Woolford B. 2001. Human factors and the international space station. Proc. Human Factors and Ergonomics Soc. 45th Annual Meeting: 125–129.
Preston DL, Shimizu Y, Pierce DA, Suyama A, Mabuchi K. 2003. Studies of mortality of atomic bomb survivors: Report 13: Solid cancer and non-cancer diseases mortality: 1950–1997. Radiat. Res. 160: 381–407.
Probst M, Bulbulian R, Knapp C. 1997. Hemodynamic responses to the Stroop and cold pressor tests after submaximal cycling exercise in normotensive males. Physiol. Behav. 62: 1283–1290.
Rabin BS. 1999. Stress, Immune Function, and Health: The Connection. New York: John Wiley & Sons.
Riley DA, Thompson JL, Prippendorf B, Slocum GR. 1995. Review of spaceflight and hindlimb suspension unloading induced sarcomere damage and repair. Basic Appl. Myology 5: 139–145.
Roy-Byrne P, Berlliner L, Russo J, Zatzick D, Pitman R. 2005. Treatment preferences and determinants in victims of sexual and physical assault. J. Nervous and Mental Disease 191(3): 161–165.
Santy PA. 1994. Choosing the Right Stuff: The Psychological Selection of Astronauts and Cosmonauts. Westport, CT: Praeger Scientific.
Sapolsky RM. 2004. Is impaired neurogenesis relevant to the affective symptoms of depression? Biol. Psychiatry 56: 137–139.
Sauer J, Wastrell DG, Hockey GRJ. 1997. Skill maintenance in extended spaceflight: a human factors analysis of space and analogue work environments. Acta Astronautica 39(8): 579–587.
Sculpher MJ, Pang FS, Manca A, Drummond MF, Golder S, Urdahl H, Davies LM, Eastwood A. 2004. Generalisability in economic evaluation studies in healthcare: a review and case studies. Health Technol. Assess. 8(49): iii–iv, 1–192.
Seibt R, Boucsein W, Scheuch K. 1998. Effects of different stress settings on cardiovascular parameters and their relationship to daily life blood pressure in normotensives, borderline hypertensives and hypertensives. Ergonomics 41: 634–648.
Seifan A, Shemer J. 2005. Economic evaluation of medical technologies. Isr. Med. Assoc. J. 7(2): 67–70.
Smith SM. 2002. Red blood cell and iron metabolism during space flight. Nutrition 18: 864–866.
Smith SM, Heer MH. 2002. Calcium and bone metabolism during space flight. Nutrition 18: 849–852.
Smith SM, Lane HW. 1999. Gravity and space flight: effects on nutritional status. Curr. Opin. Clin. Nutr. Metab. Care 2: 335–338.
Smith SM, Zwart SR, Block G, Rice BL, Davis-Street JE. 2005. The nutritional status of astronauts is altered after long-term space flight aboard the International Space Station. J. Nutrition 135: 437–443.
Stein TP. 2001. Nutrition in the space station era. Nutr. Res. Rev. 14: 87–117.
Stein TP, Leskiw MJ, Schluter MD, Hoyt RW, Lane HW, Gratebeck RJ, LeBlanc AD. 1999. Energy expenditure and balance during spaceflight on the space shuttle. Am. J. Physiol. 276: R1739–R1748.
Stuster J. 1996. Bold Endeavors: Lessons from Polar and Space Exploration. Annapolis, MD: Naval Institute Press.
Su CJ, Shevock PN, Khan SR, Hackett RL. 1991. Effect of magnesium on calcium oxalate urolithiasis. J. Urol. 145: 1092–1095.
Talas DU, Nayci A, Atis S, Comelekoglu U, Polat A, Bagdatoglu C, Renda N. 2003. The effects of corticosteroids and vitamin A on the healing of tracheal anastomoses. Int. J. Pediatr. Otorhinolaryngol. 67(2): 109–116.
Talas DU, Nayci A, Atis S, Polat A, Comelekoglu U, Bagdatoglu C, Renda N. 2002. The effects of corticosteroids on the healing of tracheal anastomoses in a rat model. Pharmacol. Res. 45(4): 299–304.
U.S. DOD (U.S. Department of Defense). 2004. Defense Acquisition Guidebook. DoDD 5000.1 On-line [available: http://akss.dau.mil/dag].
U.S. DOT (U.S. Department of Transportation). 2002. National Review of the Highway Safety Improvement Program. Washington, DC: Federal Highway Administration. On-line [available: http//www.tfhrc.gov/pubrds/02mar/04.htm].
White House. 2004. President Bush announces new vision for space exploration program. Remarks by the President on U.S. space policy. On-line [available: http://www.whitehouse.gov/news/releases/2004/01/20040114-3.html]. Accessed 5/26/05.
Whitmore M, Adolf JA, Woolford BJ. 1999. Research priorities for the International Space Station. Houston, TX: NASA Johnson Space Center.
Wilson JW, Clowdsley MS, Cucinotta FA, Tripathi RK, Nealy JE, De Angelis G. 2002. Deep space design environments for human exploration. On-line. [available: http://techreports.larc.nasa.gov/ltrs/PDF/2002/mtg/NASA-2002-wsc-jww2.pdf]. Accessed 4/19/05.
Wood BJ, Ramkaransingh JR, Fojo T, Walther MM, Libutti SK. 2002. Percutaneous tumor ablation with radiofrequency. Cancer 94(2): 443–451.
Wright RJ, Cohen RT, Cohen S. 2005. The impact of stress on the development and expression of atopy. Curr. Opin. Allergy Clin. Immunol. 5: 23–29.
Wurtman RJ, Wurtman JJ. 1989. Carbohydrates and depression. Sci. Am. 260: 68–75.
Yang EV, Glaser R. 2002. Stress-induced immunomodulation and the implications for health. Int. Immunopharmacol. 2: 315–324.
Young SN, Smith SE, Pihl RO, Ervin FR. 1985. Tryptophan depletion causes a rapid lowering of mood in normal males. Psychopharmacology 87: 173–177.
Zarkovic M, Stefanova E, Ciric J, Penezic Z, Kostic V, Sumarac-Dumanovic M, Macut D, Ivovic MS, Gligorovic PV. 2003. Prolonged psychological stress suppresses cortisol secretion. Clin. Endocrinol. 59: 811–816.
Zimmerman R. 2003. Leaving Earth: Space Stations, Rival Superpowers, and the Quest for Interplanetary Travel. Washington, DC: Joseph Henry Press.



































