B
Conceptual Models of Disability: Past, Present, and Future
Gale Whiteneck*
In the last quarter century, the conceptualization of disability has progressed dramatically. Two World Health Organization (WHO) international classification systems serve as bookends to this period. The WHO International Classification of Impairments, Disabilities, and Handicaps (ICIDH),1 published in 1980, suggested conceptual distinctions among three levels of performance—impairment at the organ level, disability at the person level, and handicap at the societal level. However, ICIDH sparked controversy by labeling the societal level as “handicap” and by failing to incorporate environmental factors. Twenty-one years later, WHO published its revision of ICIDH as the International Classification of Functioning, Disability and Health (ICF),2 which replaced the three dimensions with more appropriate labels (body structure and function at the organ level, activity at the person level, and participation at the societal level) and recognized the importance of environmental factors with a new categorization system.
Between these two events, several advances articulated the significant role of the environment in the lives of people with disabilities. The Americans with Disabilities Act3 established full participation in society as the goal for all people with disabilities and ensured their right to reasonable accommodation to achieve it. The National Institute on Disability and
Rehabilitation Research provided the new paradigm of disability that focused attention on the imperative of environmental modifications to improve the lives of people with disabilities.4 The Institute of Medicine’s (IOM’s) book Enabling America5 promoted the importance of environmental factors for people with disabilities. Researchers focused their attention on the development of participation and environmental measures, including the Craig Handicap Assessment and Reporting Technique,6, 7 the Community Integration Questionnaire,8 and the Craig Hospital Inventory of Environmental Factors.9, 10
Although the models theoretically incorporated the importance of environmental factors, little empirical evidence exists to support the theory. For example, spinal cord injury (SCI)-related research has linked impairment and disability to participation. Although the severity of the impairment had a strong relationship with the performance of activities of daily living, the research found no strong links between impairment or disability measures and participation.11, 12 A meta-analysis conducted by Dijkers13 concluded that participation was more strongly related to quality of life than to either impairment or disability.
MODELS OF DISABILITY
Society’s and researchers’ conceptualizations of disability have evolved over time. As noted in Enabling America5 and on the basis of public policy at the time, “In the 1950s, impairment of a given severity was viewed as sufficient to result in disability in all circumstances; in contrast, the absence of impairment of that severity was thought to be sufficient grounds to deny disability benefits” (p. 63) Although the practice of rehabilitation certainly existed before then, it was not until the 1960s and the 1970s that conceptual frameworks for modeling disability appeared. These conceptual frameworks allowed greater scientific inquiry into both disability and rehabilitation.
In 1972, WHO, recognizing a need for better methods to evaluate health care, sought to expand the medical model of illness that provided the basis for its International Classification of Disease (ICD).14 WHO recognized that ICD14 suited the study of the outcomes of acute diseases and injuries that can be prevented or cured but that the medical model did a woefully inefficient job of detecting the consequences of nonacute diseases, particularly chronic and progressive or irreversible disorders. In 1980, WHO published ICIDH1 as “a manual of classification relating to the consequences of disease.” It extended the disease-related sequence of etiology, pathology, and manifestation with the illness-related sequence of disease, impairment, disability, and handicap. Although the original ICIDH model acknowledges a role of the environment by stating that “handicaps thus reflect interaction with and adaptation to the individual’s
surroundings,” it has been criticized for its lack of an explicit recognition of the environmental role in its model.
Nagi15 also recognized the process by which a pathology (e.g., arthritis) may lead to an impairment (e.g., limited joint range of motion), which may then result in a functional limitation (e.g., an inability to type), which ultimately may result in disability (e.g., an inability to work as a secretary). Possibly because of his attention to employment rather than health care services, Nagi noted that correlations among impairments, functional limitations, and social roles, such as employment, were poor. Unlike ICIDH, Nagi’s model explicitly recognized that the environment could be studied separately from the individual and initiated research into environmental factors in the family, the community, and society that affect disability as an outcome. Fougeyrollas19 further clarified the influence of environmental factors on social participation in a manner consistent with the Nagi approach.
Verbrugge and Jette16 proposed an expanded model of the disablement process to account for behaviors and attributes that increase the risks of or that provide buffers to functional limitations and disability, elements not specified in Nagi’s medical model. Relevant factors include both intra-individual characteristics (e.g., behavioral change and locus of control) and extraindividual characteristics (e.g., medical care, environmental barriers or adaptations, and instrumental support) that may operate at various points along the disablement trajectory.
IOM, in Disability in America,17 derived its conceptual model of disability directly from Nagi and, in fact, defined disability “by the attributes and interactions of the individual and the environment” (p. 82). In the IOM model, risk factors exist not only within the individual but also in the physical and social environments, all of which theoretically affect the disability process. In the more recent IOM report, Enabling America,5 the conceptual model was modified to emphasize that “the environment plays a critical role in determining whether each stage of disablement occurs and if transitions between the stages occur” (p. 64). The National Center for Medical Rehabilitation Research (NCMRR), in its research plan for the National Institutes of Health,18 also emphasized the environment by use of a category of function called “societal limitations,” which it defined as “restrictions attributable to social policy or barriers (structural or attitudinal) which limit fulfillment of roles or deny access to services and opportunities associated with full participation in society” (p. 25).
In addition to environmental factors, some researchers have argued that personal factors such as age, gender, and race also deserve separate consideration in disability theory. Personal factors may appear to be separate features of the individual distinct from a particular health condition or health state, yet they may influence the disability process. Such factors may also include variables such as habits, lifestyles, experiences, coping styles,
and other psychological assets that may play a confounding role in the structural modeling of disability.19
WHO’s ICF provides the most recent and, arguably, most comprehensive model of disability.2 It revises the earlier ICIDH1 by using less pejorative language (e.g., “participation” replaces “handicap” as a functional domain), explicitly incorporating environmental and personal factors as “contextual factors” that affect disability outcomes, and recognizing multiple levels and directions of potential causal relationships. Table B.1 summarizes key models of disability and illustrates the confusion attributable to the inconsistent terminology used to label conceptual domains.
ICF DOMAINS OF DISABILITY
WHO designed ICF2 to achieve a better scientific understanding of health and health outcomes. ICF provides a common language of health to enable sharing of data among countries and health care providers. ICF describes broad health-related domains that can be transformed into a meaningful and consistent coding system. The ICF Model of Disability2 is depicted in Figure B.1.
ICF has two parts: Part 1 covers functioning and disability, and Part 2 deals with contextual factors. Components of functioning and disability include body function and structure, activities, and participation. Components of contextual factors include environmental factors and personal factors. The model conceives these components as separate but related constructs with dynamic interactions between health conditions, like disease, disorders, and injuries, and contextual factors, such as personal and environmental factors.
Describing the model component body functions and structure, ICF refers to the “body” as the human organism. It includes not only physical aspects of the human body but mental functions as well. Body functions encompass the physiological and psychological functions of body systems. Body structures include the anatomical parts of the body, including the limbs and organs. ICF defines impairment as a problem in the body function or structure that results in a significant deviation or loss. Impairment does not always indicate the presence of disease and has a broader and more inclusive scope than disease. Impairments may cause other impairments; for example, impaired brain function may cause impaired cognitive function.
The ICF graphic model (Figure B.1) differentiates between the second and the third levels, activities and participation.2 Activities refer to “the execution of a task or action by an individual,” and participation refers to “involvement in a life situation.” Examples of activities include listening, walking, and eating. Participation items describe roles that people perform,
TABLE B.1 Concepts and Terminology Used by Models of Disability
|
Model, Year |
Origin |
Organ Level |
Person Level |
Societal Level |
Other Domains |
|
Nagi, 197615 |
Pathology |
Impairment |
Functional limitations |
Disability |
|
|
WHO, 19801 |
Disease |
Impairment |
Disability |
Handicap |
|
|
IOM, 199117 |
Pathology |
Impairment |
Functional limitations |
Disability |
|
|
NCMRR, 199218 |
Patho-Physiology |
Impairment |
Functional limitations |
Disability |
Societal limitations |
|
IOM, 19975 |
Pathology |
Impairment |
Functional limitations |
Disability |
Environmental factors quality of life |
|
WHO, 20012 |
Health Condition |
Body structure and function |
Activity |
Participation |
Environmental factors, personal factors |
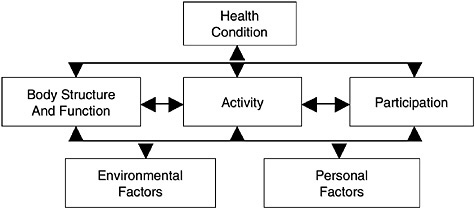
FIGURE B.1 ICF model of disability.2
such as forming relationships with others, caring for a household, or seeking and maintaining employment.
Although ICF depicts activities and participation separately in the graphic model, it uses one coding structure for both and covers the major areas of activity that one encounters throughout a life span. The list of domains includes learning and the application of knowledge, general tasks and demands; communication; mobility; self-care; domestic life; interpersonal interactions and relationships; major life areas; and community, social, and civic life. ICF defines difficulties as activity limitations or participation restrictions and measures them by comparing the performance of an individual with a health condition (a disease, injury, or disorder) with that of an individual without the condition. The difference between what one actually sees and what one expects to see provides a measure of the limitation.
One of two contextual components of ICF, environmental factors, includes the physical, social, and attitudinal environments, or the external factors of an individual’s life. These factors can have either a negative influence (“barrier”) or a positive influence (“facilitator”) on a person’s performance in society, on an individual’s ability to carry out tasks, or on an individual’s body function and structure. ICF organizes environmental factors into two levels: individual and societal. Individual environmental factors include the immediate environment of the individual, such as home and work: the physical or material features of the environment, as well as the individual’s interaction with family, peers, acquaintances, and strangers. Societal factors include formal and informal services and systems in the community that affect a person’s life. Societal factors encompass organizations and services related to work, community activities, government agencies, communication services, and transportation services.
Finally, ICF2 identifies personal factors as “the particular background of an individual’s life and living, and comprises features of the individual that are not part of health condition or health states” (p. 17). For example, these factors include gender, minority status, age, lifestyle, habits, upbringing, coping styles, education, profession, personality characteristics, marital status, and overall behavioral patterns. All of these factors may play a role in disability at any level, and although ICF does not classify these factors because of the large social and cultural variances that exist within them, it acknowledges their potential importance.
Although much progress has been made in refining disability models, categories of function, and the role of the environment,1, 20, 21 only limited quantitative studies22, 23, 24 have attempted to validate the models.
SUMMARY AND CRITIQUE OF ICF
This author’s assessments of ICF compared with past models and the models of disability that are needed in the future can be summarized in the following title used in a recent presentation: “The ICF, one step forward, one step back, and a few steps yet to go for a complete model.”25 The one step forward was the inclusion of environmental factors; the one step back was the blurring of activities and participation; and the needed steps include the differentiation of activities and participation, the addition of quality of life to the model, elaboration of the impact of environmental factors, the development of personal factors, refinement of the graphic depiction of the model, definition of research strategies to better measure the domains of disability, and validation of the model.
Background on the Revision of ICF
ICF lists hundreds of people from scores of countries who were involved in the decade-long revision process. The author’s comments here reflect a view of that process as gleaned from attendance at dozens of North American and international meetings. Although several cosmetic changes were made to ICIDH in the revision to ICF, substantive changes were also made. The cosmetic changes that occurred in the revision to ICF were the relabeling of the domains. That was necessary from the U.S. standpoint because the term “handicap” was completely unacceptable to the disability advocacy community because of its pejorative nature. ICF made an effort to use labels that were more neutral in tone, so “impairment” became “body structure and function,” disability became “activity,” and “handicap” became “participation.” The underlying cause of all of these outcomes was relabeled “health condition,” and there was recognition that this process was not a simple linear progression but included many interactions, so
numerous arrows were added to the model. Finally, the label of the model was changed to the model of functioning and disability. That brought the model to a point where the same basic underlying concepts had simply been relabeled, but now a set of labels that would be acceptable in the United States and that were less negative toward people with disabilities was being used.
The Step Forward
The addition of environmental factors was the major step forward in this process, and among the U.S. delegation this was the highest priority. In fact, without that addition, the model would have remained unacceptable to disability advocacy groups and therefore would not have been used. The addition of environmental factors was the major part of adding broader contextual factors that included both environmental and personal factors. It took a few years for environmental factors to be incorporated into the draft model, and they seemed to slip out and periodically needed championing to keep them in. Eventually, they were maintained, and in the author’s view, that was probably the major step forward in the conceptualization of disability outcomes.
The Step Backward
The loss of a clear distinction between activity and participation was the step backward. In the development of the category schemes and in the listing of the elements of the domains of activity and participation, there were disagreements. One school of thought was that everything is an activity and the issue is just one of the complexity of the activity. Therefore, for that group, the desire was to have a very long list of activities. From the U.S. perspective and the perspective of the delegations from other English-speaking countries, there was a desire to maintain the concept of participation in terms of performance as a member of society—working, going to school, parenting, and socializing—as a separate and distinct dimension. This was controversial. In the preliminary draft that was tested, a distinction between activity and participation was made; and a list of activities, as well as a list of participation, was made. Although there were disagreements about whether something was an activity or participation, a consensus on how to resolve these controversies was starting to develop among the delegations from the English-speaking countries. At the last minute, however, WHO decided to say that activity and participation both have the same elements. That resulted in one list of elements for the combined activity and participation domain—a decision that blurs the distinction between activity and participation.
The problem was further complicated by the last-minute introduction of two qualifiers to these dimensions—capacity and performance—with the implications that capacity was related to activity and that performance was related to participation. Furthermore, the suggestion that capacity should be measured in a uniform standard environment whereas participation should be measured in the real world also added confusion to the conceptual model.
SEVEN STEPS TO IMPROVE THE MODEL
It is the view of the author that seven steps are warranted to improve the present ICF Model of Disability. These steps represent conceptual clarifications and enhancements as well as research strategies that can be used to implement and validate the model. Both conceptual and empirical advances are needed to move the disability field forward. These advances are envisioned as iterative processes, in which the conceptual model guides research and empirical evidence informs theory, which culminate in a revised and validated Model of Disability (ICF-2). Continuing empirical work must proceed, without waiting for a perfect model, to inform theoretical perspectives. On the other hand, improved conceptualizations will guide the disability field. In the author’s view, the primary role of ICF and its revisions are to guide and evaluate research, policy, and practice rather than to serve as a classification scheme. Although implementation of the proposed revisions will be a challenge, they will be worth the effort and will lead to a better theoretical understanding of disability, which, in turn, can improve the lives of people with disabilities.
Step 1: Distinguishing Activity and Participation in the Next Model Revision
The blurring of activity and participation was a step backward that must be repaired. In the next revision of ICF, distinctions between activity and participation need to be clarified as the first step in improving the present model.
Several themes differentiate these two important concepts. First, and most importantly, activity is at the individual person level, whereas participation is at the societal level. Activities are more likely to be performed alone, whereas participation elements would more likely be performed with others. In some sense, activity is a simpler concept, whereas participation is a more complex process. Activity is related more closely to the extent of impairment, whereas participation is related more closely to perceived quality of life. Meta-analysis13 demonstrates that the severity of the impairment is highly correlated with activities of daily living but is not strongly related
to quality of life, whereas participation is more closely related to quality of life. Activity may be thought of as less environmentally dependent, whereas participation is more environmentally dependent. Although, conceptually, environmental factors play a role in both levels, it does seem clear that participation is the area that is the most influenced by the environment. Activity is embraced by the medical model of disability, whereas participation emerges from a social model of disability. The measurement of activity is a focus of rehabilitation, whereas the measurement of participation reflects the outcomes most important to individuals with disabilities, their family members, and society. Activity is more typically assessed in a rehabilitation setting, whereas participation should be assessed in the community setting. Activity is more often assessed by a clinician or professional, whereas participation is more often a self-report of the individual with a disability. Finally, in the current state of the science, all activity limitations cannot yet be eliminated, but theoretically, most participation restrictions can be eliminated. Although all disabilities cannot be cured, society is in a position, at least theoretically, to return people to active, productive lives that are well integrated into family and community life. Society is better prepared to maximize participation than to maximize activity.
Nagi made a strong conceptual basis for differentiating activities and participation in Appendix A of Disability in America,2 in which he attempted to clarify the distinction between performance at the level of the person (which he called “functional limitations”) and performance at the societal level (which he called “disability”). For Nagi, role performance was the defining concept at the societal level. He, like Parsons,26 viewed “role performance” as an organized system of participation by an individual in a social system, whereas tasks are more specialized than roles and can be viewed as subsystems of roles. Nagi argued that activities of daily living are task behaviors that are parts of (but different from) role expectations inherent in a person’s family, vocational, and social lives. Furthermore, Nagi suggested that tasks or activities were attributes or properties of individuals in isolation, whereas roles and participation were relational concepts requiring consideration of environmental factors in which the roles were performed. This early conceptual focus on roles as the defining characteristic of performance at the societal level may offer an effective way to differentiate activities and participation in ICF-2.
Step 2: Quality of Life, a Key Missing Component of ICF
ICF offers a comprehensive model of objective disability outcomes and provides rehabilitationists and researchers with a system for categorizing disability. However, it does not address the subjective perceptions and preferences of people with disabilities. It is for this reason that disability
researchers have criticized ICF for lacking a subjective dimension and recommended augmentation of ICF with an additional dimension—quality of life25—as the second step in the revision of ICF.
Although WHO does not include the concept of quality of life in the ICF Model of Disability, it has recognized both the importance of the quality-of-life concept and its relationship to disability outcomes. WHO defined quality of life as “the perception of individuals of their position in life, in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards, and concerns.”27 According to WHO, the determinants of quality of life include the consequences of disability, particularly handicap or participation.1 On the basis of WHO documents, Barbotte and colleagues described quality of life as a wide-ranging concept “affected by people’s social relationships, physical health, psychological state and level of independence, and by their relationship to salient features of their environment”28 (p. 1048).
Quality of life, defined as a self-appraisal of subjective well-being or life satisfaction made by the person with a disability, might be acknowledged by the ICF WHO Model of Disability in one of three ways: (1) it could be added as a separate domain to the right of participation, indicating that the extent of quality of life is the ultimate outcome of the disability process; (2) it could be added as a qualifier to each of the present domains of ICF, indicating that satisfaction with participation, activities, and even body structures and functions is an important aspect of disability; or (3) it could be excluded from the model itself but acknowledged as a key life outcome influenced by the disability process. This author favors the first approach. The exclusion of quality of life from the model but acknowledgment of its importance fails to require that the subjective assessment of the individual with a disability be included in any comprehensive assessment of disability. The incorporation of a subjective satisfaction qualifier as part of each current domain adds conceptual confusion to each of the domains and fails to focus attention on a unique outcome of critical importance. Only the actual addition of a new quality-of-life domain acknowledges the validity of the subjective perceptions of people with disabilities and that those perceptions are distinct outcomes of the disability process.
Quality of life could be measured simply by using a standardized assessment of global life satisfaction29 or an instrument that assesses satisfaction with domains of life;30 but it should not be a composite measure of Health-Related Quality of Life (HRQOL), including impairment, activity limitation, participation restriction, and quality-of-life indicators, as is often the case with HRQOL measures.31 The author suggests that the inclusion of a new quality-of-life domain is more important than the addition of a quality-of-life taxonomy with a coding system. Furthermore, the potential difficulty of adding a new domain and the complexity that it brings will be
outweighed by the conceptual importance of the subjective assessment by the person with a disability. Quality of life was first recognized as an important domain by Enabling America, 5 and its addition to ICF is a critical revision.
Step 3: Elaborating the Complexity of Environmental Factors
The third step needed in the revision of ICF is elaboration of environmental factors. It was a tremendous step forward to acknowledge the role of environmental factors. The environmental factors research that has been done has given some insight into the relationship between environmental factors and participation. Conceptually, models have always suggested that the more barriers that people encounter, the lower their participation is and that barriers actually prevent people from participating in society. On the other hand, the theories suggest that the more facilitating the environment is, the more likely it is that people with disabilities will fully participate in society. In initial environmental research, most correlations between environmental barriers and participation were negative, as expected. However, it was a surprise to find a few positive correlations between some environmental factors and participation, indicating a more complex relationship. The data seemed to suggest that when people encounter barriers, their participation is less; but they also suggest that for those people who persevered and got out and involved in the community and fully participated, they also witnessed and perceived more environmental barriers. It is not a simple one-way relationship.
Only two disability studies have systematically examined environmental barriers and their relationship to other ICF concepts and quality of life: one in traumatic brain injury (TBI)32 and one in SCI.24 The TBI study surveyed 73 participants from one TBI model system program at their first anniversary of injury, with respondents reporting a greater impact from environmental barriers also reporting lower levels of participation and life satisfaction.32
The SCI study surveyed 2,726 participants from the 16 federally designated SCI model systems as they crossed their 1st, 5th, 10th, 15th, 20th, or 25th anniversary of injury. Environmental barriers accounted for only 4 percent of the variation in participation, but they accounted for 10 percent of the variation in quality of life. The SCI study supported the inclusion of environmental factors in models of disability, like ICF, but concluded that environmental factors had a stronger relationship to quality of life than they did to societal participation.24 This last finding of the SCI study raises the pivotal question: do environmental factors directly influence participation, which in turn influences quality of life, or do environmental factors more directly influence quality of life? Environmental barriers may reduce
participation, or the struggle to overcome barriers and fully participate may reduce quality of life. There is much to learn about the actual role of environmental factors in the disability process, and researchers need to develop some theory underlying the concept that helps explain under what conditions barriers actually mean that participation does not occur and under what conditions people move beyond those barriers and participate. Considerable theory building will be required to accomplish this third step in revising ICF.
Step 4: An Understanding and Taxonomy of Personal Factors
The fourth step needed to improve ICF is the development of personal factors. However, this step is controversial. The current conceptual model acknowledges that contextual factors, including both environmental and personal factors, play a major role in disability outcomes. Environmental factors are considered everything external to the individual—physical, attitudinal, and policy factors. Personal factors should be thought of as all of the factors that are internal to the individual but unrelated to the disability itself, including the preexisting conditions, demographic factors, and personal characteristics that existed before an impairment occurred or that are not directly related to the disabling process. Looking for demographic differences in disability outcomes is an area in which investigators are comfortable, but efforts to venture into the arena of personal factors beyond demographics have not been made. Psychological factors and personality factors are seldom examined, possibly for reasons of political correctness. The concern of advocacy groups is that if it begins to be suggested that motivation or compliance with treatment is an important factor in producing disability outcomes, then the field is precariously on the verge of once again suggesting that the problem lies with the individual instead of the environment. Advocacy groups would then once again challenge the medical model because it failed to consider environmental factors. Therefore, it is critical that people with disabilities and advocacy groups be fully involved in any development of a personal factors taxonomy. Furthermore, careful consideration will be needed when something that might seem to be a personal factor might better be viewed as psychological structure or function. However, eventually, to have a complete model that is able to predict a major portion of the variances in outcomes, personal factors will likely need to be included. Therefore, the development of a personal factors taxonomy with a better theoretical understanding of the significance of personal factors needs to be one of the steps in the ICF revision process.
Step 5: Refining a Graphic Representation of the Model
Neither the complex diagram of multiheaded arrows and boxes of ICF nor the “man on the mat” diagrams in Enabling America provide a clear depiction of the interaction of health conditions with contextual factors that produce disability outcomes. If a more compelling graphic depiction that clarified the nature of conceptual relationships in an intuitive manner could be developed, the more widespread adoption of the revised model would be more likely. Refining the graphic is therefore listed as the fifth step in revising the ICF.
Step 6: Developing Improved Measures of the Domains of Disability
The final two steps advocated for advancing the conceptual understanding of disability have more to do with the application of the model than its revision. Both current and future models of disability require extensive testing. The reliability and practicality of the taxonomy must be evaluated, but more importantly, the implied relationships among the concepts must be assessed. A prerequisite of that task is the availability of psycho-metrically sound measures of the ICF concepts. Although many measures of impairment and activities of daily living have been developed, the measurement of participation is a relatively new field and the measurement of environmental factors is in its infancy. Considerable psychometric evaluation of existing and newly developed instruments is needed to reach a consensus on standardized methods of quantifying each of the domains of the disability. Major surveys need to incorporate reliable and valid measures specifically designed to assess the conceptual domains of ICF rather than simply trying to retrofit existing survey questions to the ICF taxonomy by developing “crosswalks” to ICF codes.
Step 7: Validate the Model
Once valid and reliable tools are developed, they can be applied in multivariate analyses to determine the strength of relationships among ICF concepts. Replication of such work with multiple populations with different impairments will be needed. The development of a research strategy to tackle this problem would be a significant step and contribution to the field, but full validation of the model also requires the use of the model to guide interventions to improve the lives of people with disabilities. Therefore, the final step includes the design, implementation, and rigorous evaluation of interventions based on the conceptual model. The ultimate test of a model is whether it facilitates effective interventions. The revised conceptual model,
in combination with the empirical tests of the model, should provide the information necessary to direct effective interventions.
CONCLUSIONS
As IOM begins the process of reconsidering its seminal works Disability in America and Enabling America, published nearly 15 and 10 years ago, respectively, clear advances have occurred in the conceptualization of disability, but more work is needed in clarifying concepts. WHO’s ICF has incorporated a major concept advocated by Enabling America—environmental factors—and ICF, as the currently accepted international model, should be the starting point for advocating future conceptual revisions. Seven steps have been outlined to improve the ICF conceptualization, including the differentiation of activities and participation, the addition of quality of life to the model, elaboration of the impact of environmental factors, the development of personal factors, refinement of the graphic depiction of the model, definition of research strategies to better measure the domains of the model, and validation of the model by testing the interrelationships among its concepts and deriving interventions to improve the lives of people with disabilities.
REFERENCES
1. World Health Organization. International Classification of Impairments, Disabilities and Handicaps: a Manual of Classification Relating to the Consequences of Disease. Geneva, Switzerland: World Health Organization; 1980.
2. World Health Organization. International Classification of Functioning, Disability, and Health. Geneva, Switzerland: World Health Organization; 2001.
3. The Americans with Disabilities Act. P.L. 101-336. 1990.
4. National Institute on Disability and Rehabilitation Research. National Institute on Disability and Rehabilitation Research (NIDRR) Long Range Plan for Fiscal Years 1999-2003. Web Page. Available at http://www.ncddr.org/new/announcements/nidrr_lrp/index.html. Last accessed October 18, 2005.
5. Institute of Medicine. Enabling America: Assessing the Role of Rehabilitation Science and Engineering. Washington, DC: National Academy Press; 1997.
6. Whiteneck GG, Charlifue SW, Gerhart KA, Overholser JD, Richardson GN. Quantifying handicap: a new measure of long-term rehabilitation outcomes. Archives of Physical Medicine and Rehabilitation 1992; 73:519–526.
7. Whiteneck G, Brooks C, Charlifue S, et al. Guide for Use of CHART: Craig Hospital Assessment and Reporting Technique. Englewood, CO: Craig Hospital; 1992.
8. Willer B, Rosenthal M, Kreutzer J, Gordan W, Rempel R. Assessment of community integration following rehabilitation for traumatic brain injury. Journal of Head Trauma and Rehabilitation 1993; 8:75–87.
9. Craig Hospital Research Department; Craig Hospital Inventory of Environmental Factors (CHIEF) Manual, Version 3.0. Englewood, CO: Craig Hospital; 2001.
10. Whiteneck G, Harrison-Felix C, Mellick D, Brooks C, Charlifue S, Gerhart K. Quantifying environmental factors: a measure of physical, attitudinal, service, productivity and policy barriers. Archives of Physical Medicine and Rehabilitation 2004; 85:1324–1335.
11. Whiteneck G. Outcome analysis in spinal cord injury rehabilitation. In: Rehabilitation Outcomes: Analysis and Measurement. Fuhrer MJ, ed. Baltimore, MD: Paul H. Brookes Publishing Co.; 1987:221–231.
12. Whiteneck G. Outcome evaluation and spinal cord injury. NeuroRehabilitation 1992; 2:31–41.
13. Dijkers M. Quality of life after spinal cord injury: a meta analysis of the effects of disablement components. Spinal Cord 1997; 35:829–840.
14. World Health Organization. International Classification of Disease, 9th Revision. Clinical Modifications. Ann Arbor, MI: Commission of Professional and Hospital Activities; 1986.
15. Nagi SZ. An epidemiology of disability among adults in the United States. The Milbank Memorial Fund Quarterly 1976; 54:439–467.
16. Verbrugge LM, Jette AM. The disablement process. Social Science & Medicine 1994; 38:1–14.
17. Pope A, Tarlov A. Disability in America: Toward a National Agenda for Prevention. Washington, DC: National Academy Press; 1991.
18. National Institutes of Health. Research Plan for the National Center for Medical Rehabilitation Research. NIH Publication 93-3509. Washington, DC: U.S. Department of Health and Human Services; 1993.
19. Fougeyrollas P. Documenting environmental factors for preventing the handicap creation process: Quebec contributions relating to ICIDH and social participation of people with functional differences. Disability and Rehabilitation 1995; 17:145–153.
20. Fougeyrollas P. Explanatory models of the consequences of disease and trauma: the handicap creation process . ICIDH, International Network 1993:6.
21. Whiteneck G, Fougeyrolles P, Gerhart G. Elaborating the model disablement. In: Assessing Medical Rehabilitation Practices: the Promise of Outcomes Research. Fuher M ed. Baltimore, MD: Paul H. Brookes Publishing Co.; 1997:91–102.
22. Heinemann A, Whiteneck G. Relationships among impairment, disability, and life satisfaction in persons with traumatic brain injury. Journal of Head Trauma Rehabilitation 1995; 10:54–63.
23. Hall MK, Hamilton BB, Gordon WA, Zasler N.D. Characteristics and comparisons of functional assessment indices: Disability Rating Scale, Functional Independence Measure, and Functional Assessment Measure. Journal of Head Trauma Rehabilitation 1993; 8:60–74.
24. Whiteneck G, Mead M, Dijkers M, Tate D, Bushnik T, Forchheimer M. Environmental factors and their role in participation and life satisfaction after spinal cord injury. Archives of Physical Medicine and Rehabilitation 2004; 85(11):1793–1803.
25. Whiteneck G. The ICF: one step forward, one step back, and a few steps to go to a complete model. Presentation to conference on State of the Science: Outcome Research in Post-Acute Care . April 24-25, 2003, Washington, DC. Organized by Boston University. Web Page. Available at http://www.bu.edu/cre/webcast/testwhiteneck.doc. Last accessed October 18, 2005.
26. Parsons, T. Definitions of health and illness in the light of American values and social structure. In: Patients, Physicians and Illness. Jaco EG, ed. Glencoe, IL: Free Press; 1958.
27. World Health Organization. Study protocol for the World Health Organization project to develop a quality of life assessment instrument: WHOQOL. Quality of Life Research 1993; 2:153–159.
28. Barbotte E, Guillemin F, Chau N. Prevalence of impairments, disabilities, handicaps, and quality of life in general population: a review of recent literature. Bulletin of the World Health Organization 2001; 79(11):1047–1055.
29. Diener E, Emmons R, Larsen J, Griffin S. The Satisfaction with Life Scale. Journal of Personality Assessment 1985; 49(1):71–75.
30. Flanagan J. A research approach to improving our quality of life. American Psychologist 1978; 33:138–147.
31. Ware J, Sherbourne C. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Medical Care 1992; 30:473–483.
32. Whiteneck G, Gerhart K, Cusick C. Identifying environmental factors that influence the outcomes of people with traumatic brain injury. Journal of Head Trauma Rehabilitation 2004; 19(3):191–204.

















