1
Overview of the HRSA Traumatic Brain Injury Program
A traumatic brain injury (TBI) is a brain injury caused by a sudden jolt, blow, or penetrating head trauma that disrupts the function of the brain. A 5-year-old child darts into traffic and is struck by a car. A high school quarterback collides with a running back and lies unconscious on the playing field. A young mother suffers a fractured skull and concussion when her minivan is blindsided by a drunk driver. On a summer evening, a man loses control of his bicycle when it hits a rut in the pavement; he flips over the handlebars and lands head first in the street. A soldier survives a roadside blast in Iraq, but the explosion causes his brain to move violently inside the skull.
The effects of a TBI vary from person to person, depending on the force dynamics of injury and the patient’s anatomy and physiology. When a TBI occurs, the brain may be injured in a specific location or the injury may be diffuse and located in many different parts of the brain. The effects may be temporary or permanent and include a broad range of physical, cognitive, and behavioral impairments that result from externally inflicted trauma to the brain (NIH, 1998). TBI survivors with persistent impairments may require ongoing services, such as case management, cognitive and physical rehabilitation, medical and behavioral health care, financial assistance, vocational training, housing, transportation, and other services, long after their acute injuries are treated medically. The parents, spouses, other caregivers, and especially young children in the injured person’s family may also experience intense, long-term social, psychological, and physical health effects and need services as well.
This report presents the analysis, findings, and recommendations of the Institute of Medicine’s (IOM) Committee on Traumatic Brain Injury with regard to the Federal TBI Program administered by the Health Resources and Services Administration (HRSA). The HRSA TBI Program is a congressionally mandated program intended to facilitate the development of state-level infrastructure and service delivery systems for individuals with TBI and their families, particularly with respect to family or consumer support, return to work, housing or supportive living personal assistance services, assistive technology and devices, behavioral health services, substance abuse services, and traumatic brain injury treatment and rehabilitation (Title 42 U.S. Code, Ch. 6A, 2003). The effectiveness of the HRSA TBI Program was recently called into question in a federal Office of Management and Budget (OMB) Program Assessment Rating Tool (PART) review report (OMB, 2005). In its critique, OMB found fault with the TBI Program, citing that it had neither long-term health outcomes measures nor regular independent evaluations of the program’s effects on TBI patients and their families.
To address these criticisms, HRSA contracted with the IOM in the spring of 2005 to conduct a study: (1) to assess the impact of the HRSA Program on how state systems are working or failing to work in support of individuals with a TBI; and (2) to advise HRSA on how it could improve the program to best serve individuals with TBI and their families (Box 1-1). The IOM appointed an 11-member Committee on Traumatic Brain Injury to assess the impact of the HRSA TBI Program and make recommendations to HRSA. Committee members were selected for their expertise in neurology, neuropsychology, cognitive and physical rehabilitation, clinical medicine and nursing, epidemiology, program evaluation, behavioral health, social work, and personal TBI experience.
APPROACH TO THE STUDY
The underlying premise of the HRSA TBI Program is that grants to states that meet certain requirements will facilitate the creation of infrastructure and increased capacity for serving individuals with TBI. This study is not intended as a technical evaluation of the HRSA TBI Program’s impact on either the delivery of TBI-related services or on person-level outcomes—such an analysis is not feasible given currently available data. Rather, the study’s focus is on whether the TBI Program has led to an expansion in state systems infrastructure as a precondition for better serving persons with TBI and their families.
The committee used a qualitative study method to assess the program’s impact. Qualitative methods are often used to investigate developing institutions and systems as well as to assess the impact of government programs (Caudle, 1994; Sofaer, 1999; Newcomer and Scheirer, 2001; World Bank
|
BOX 1-1 The objective of this study is to evaluate and recommend improvements to the Health Resources and Services Administration (HRSA) Federal Traumatic Brain Injury (TBI) Program. TBIs are brain injuries that result from sudden jolts, blows, or penetrating trauma to the brain. The TBI Program was created by the Traumatic Brain Injury Act of 1996 (P.L. 104-166) and later reauthorized as Title XIII of the Children’s Health Act of 2000 (P.L. 106-310). The legislation provides for state-based grant programs charged with improving service delivery, establishing policy, and securing the financial support to bring about lasting systems change in the care of persons with TBI. The focus is on a particular subset of the TBI population—those individuals with TBI (and their families) who require the services of complex public and private service systems. Since 2002, the HRSA Program has also included formula-based Protection and Advocacy (P&A) grants to states, territories, and the Native American Protection and Advocacy Project to bolster advocacy support for individuals with TBI and their families. The charge to the IOM Committee on Traumatic Brain Injury is twofold:
|
Group, 2005). Qualitative data were gathered from a variety of sources and were analyzed for key themes and recurring issues. Primary sources of data included semi-structured interviews with TBI stakeholders in seven sample states and representatives of selected national organizations (a requirement of the IOM/HRSA agreement), research literature and TBI program materials, and relevant survey data. Appendix A, Method of the Study, presents a complete description of the study methods.
Clearly, HRSA should develop a more complete evaluation strategy to assess whether individuals with TBI have benefited from the HRSA Program. Many federal agencies require significant improvements in their evaluation information and capacity, according to OMB and the U.S. General Accountability Office (GAO) (GAO, 2003; OMB, 2004). The committee suggests that HRSA follow GAO’s approach to building evaluation capacity in government agencies. GAO recommends four essential elements for a government-based evaluation infrastructure: (1) a culture of evaluation made evident through routine evaluations of how well programs are working to achieve agency goals; (2) quality data that are credible, reliable, and
consistent; (3) analytic expertise in both technical methods and the relevant program field; and (4) collaborative partnerships with program partners or sister agencies to leverage resources and expertise.
ORGANIZATION OF THE REPORT
This report presents the Committee on Traumatic Brain Injury’s assessment of the impact of the HRSA TBI Program. The report is organized as follows:
-
This chapter, Chapter 1, Overview of the HRSA Traumatic Brain Injury Program, introduces the report and establishes the context for the committee’s assessment of the HRSA TBI Program’s impact by describing the program’s legislative history, program administration, and grants design.
-
Chapter 2, Epidemiology and Consequences of Traumatic Brain Injury—An Invisible Disability, provides further background by describing the epidemiology and consequences of TBI, focusing on the subset of the TBI population (and their families) who require post-acute TBI services because of persistent impairments.
-
Chapter 3, Service Needs and Sources of Funding and Supports for People with TBI-Related Disabilities, provides additional background by describing the post-acute service needs and available sources of funding and support for TBI survivors with TBI-related disabilities.
-
Chapter 4, Assessment of the HRSA TBI Program, presents the committee’s findings regarding the impact of the HRSA TBI Program, along with the committee’s recommendations.
Additional research and background materials prepared as part of the committee’s evaluation are presented in the report’s appendixes:
-
Appendix A, Methods of the Study, describes the committee’s approach to the evaluation, including a public workshop, site visits, and stakeholder interviews in seven states.
-
Appendix B, Interview Guide Developed by the IOM Committee on Traumatic Brain Injury, is a discussion guide that was developed and used for semi-structured interviews with TBI stakeholders in seven states.
-
Appendix C, State TBI Programs and Protection and Advocacy Systems: Characteristics and Accomplishments, by State, includes three detailed tables summarizing for each state: (1) the characteristics of the state’s TBI program, (2) the reported accomplishments of the state TBI program, and (3) the reported goals and accomplishments of protection and advo-
-
cacy (P&A) systems for people with disabilities with respect to P&A for people with TBI.
-
Appendix D, Profiles of TBI Initiatives in Seven States, describes the TBI programs in Alabama, California, Colorado, Georgia, New Jersey, Ohio, and Washington. The profiles summarize each state’s HRSA TBI Program grant history; resources; services for people with TBI and their families; interorganizational collaboration and coordination; TBI-related data, monitoring, and evaluation; and successes and challenges of the HRSA grant experience.
-
Appendix E, Stakeholders Assess the HRSA TBI Program: A Report on National Interviews and Interviews in Seven States, is a specially commissioned report on a series of semi-structured interviews with stakeholders in the seven states (referenced above).
-
Finally, Appendix F presents the glossary, abbreviations, and acronyms.
The remaining pages of this chapter give an overview of the HRSA TBI Program, including the program’s legislative mandate, administration by HRSA, and the two major components of the grant program.
Legislative Mandate for the HRSA TBI Program
The HRSA TBI Program was initially authorized by the Traumatic Brain Injury Act of 1996 (P.L. 104-166, 1996). That act marked the beginning of a multipronged federal endeavor to address the needs of persons with TBI. It authorized three federal agencies within the U.S. Department of Health and Human Services—HRSA, the Centers for Disease Control and Prevention, and the National Institutes of Health—to implement several first-time, federal TBI initiatives and to coordinate their activities as appropriate (Box 1-2).
Congress clearly intended the HRSA TBI Program to be a federal-state partnership.1 The focus of the HRSA TBI Program is on meeting the needs of a particular subset of the TBI population—namely, individuals with TBI (and their families) with post-acute impairments who require the services of complex public and private service systems. HRSA’s role was envisioned as spurring state action to bring about improvements and lasting change in state-level service systems for TBI survivors and their families. Under the HRSA TBI Program, HRSA competitively awards federal grants to states, territories, and the District of Columbia to improve their infrastructure and
|
BOX 1-2 The Traumatic Brain Injury Act of 1996 (P.L. 104-166) directed three agencies of the U.S. Department of Health and Human Services—the Health Resources and Services Administration, the Centers for Disease Control and Prevention, and the National Institutes of Health—to implement several first-time programs related to TBI and to coordinate their activities as appropriate. Health Resources and Services Administration (HRSA). HRSA was mandated to implement a program of grants to states and territories to help them improve their TBI infrastructure and service systems for meeting the post-acute needs of individuals with TBI and their families. Centers for Disease Control and Prevention (CDC). CDC was directed to address prevention of TBI by (1) tracking its incidence and prevalence; (2) conducting research to identify effective prevention strategies; and (3) implementing public information and education programs to increase public awareness of the consequences of brain injury. National Institutes of Health (NIH). NIH was given the responsibility for (1) conducting a consensus conference; (2) developing programs that expand participation of academic centers of excellence in TBI treatment and rehabilitation research and training; and (3) conducting basic and applied research on more effective diagnosis and prognosis, therapies that retard, prevent, or reverse brain damage after TBI, and the continuum of care from acute care through rehabilitation. SOURCE: P.L. 104-166. |
services to better meet the post-acute needs of individuals with TBI and their families.
When it reauthorized the HRSA TBI Program in the Children’s Health Act of 2000 (P.L. 106-310, 2000), Congress expanded HRSA’s mandate. Specifically, it authorized HRSA to provide federal grants to federally mandated P&A systems for the disabled—commonly referred to as P&A systems—in the states, territories, and District of Columbia to help ensure their provision of P&A services for individuals with TBI and their families (Box 1-3).
Apart from the HRSA TBI Program and other TBI-related programs identified in Box 1-2, several federal programs provide cash support, health coverage, or other supports to eligible persons with TBI (discussed in Chapter 3). In addition, the National Institute on Disability and Rehabilitation Research (NIDRR) within the U.S. Department of Education funds the TBI Model Systems of Care program—the locus of federal research on the
|
BOX 1-3 In 1975, Congress enacted the Developmental Disabilities Assistance and Bill of Rights Act (P.L. 103-230). That act established the federal Protection and Advocacy for Developmental Disabilities Program and laid the groundwork for a comprehensive nationwide network of protection and advocacy (P&A) organizations for people with developmental disabilities. The Protection and Advocacy for Persons with Developmental Disabilities (PADD) Program, administered by the Administration for Children, Youth, and Families within the U.S. Department of Health and Human Services, is mandated to do the following for people with developmental disabilities:
The 1975 act conditioned a state or territory’s receipt of federal funds under the PADD program on the existence of “a system to protect and advocate the rights of individuals with developmental disabilities” and led to the establishment of federally funded, state-administered P&A systems in all 50 states, U.S. territories, and the District of Columbia. P&A systems are required by law to be independent of public and private service providers. Since 1975, Congress has expanded the responsibilities of P&A systems in the states and territories to include P&A for individuals with mental illness and other severe disabilities, including individuals with TBI. SOURCE: Administration on Developmental Disabilities, 2005. |
course of brain injury recovery and outcomes following the delivery of a coordinated system of emergency care, acute neurotrauma management, comprehensive inpatient rehabilitation, and long-term interdisciplinary follow-up services. There are 16 TBI Model Systems of Care sites throughout the country.2 These sites provide comprehensive systems of brain injury
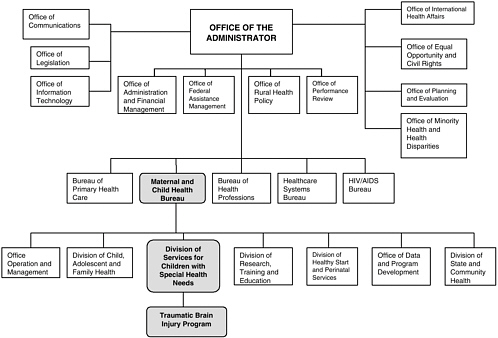
FIGURE 1-1 The HRSA TBI Program’s place in the HRSA bureaucracy, 2005.
SOURCE: Adapted from U.S. Department of Health and Human Services, 2005: http://www.hrsa.gov/orgchart.htm and http://www.hrsa.gov/org/mchb.html.
care to individuals, from acute care through community reentry. The NIDRR TBI Model Systems of Care program includes a national, longitudinal dataset that is designed to provide information about best practices and the short- and long-term consequences of TBI.
The HRSA TBI Program’s Place in the HRSA Bureaucracy
The HRSA TBI Program is dwarfed within its parent agency (Figure 1-1). HRSA, an agency with a budget of nearly $7.4 billion in FY 2005, has broad national responsibilities for helping improve the health of uninsured, underserved, and special needs populations; preparing for public health emergencies; and strengthening the health care workforce (DHHS, 2005).
HRSA operates five bureaus (the Maternal and Child Health Bureau, Bureau of Primary Health Care, Bureau of Health Professions, Healthcare Systems Bureau, and HIV/AIDS Bureau). It also operates 11 special offices charged with either programmatic duties such as rural health policy and minority health disparities or administrative tasks such as financial management and information technology. The organizational home of the HRSA TBI Program, which is intended to help persons of all ages, is the Maternal and Child Health Bureau of HRSA; originally, in the Division of Child, Family, and Adolescent Health and, more recently, in the Division of Services for Children with Special Health Care Needs.
Budget for the HRSA TBI Program
The history of federal appropriations for the HRSA TBI Program from FY 1997 to FY 2005 is shown in Table 1-1. Federal appropriations for the HRSA TBI Program are essentially “seed monies” that states can leverage to develop more substantial sources of support for TBI services. In FY 1997 and FY 1998, Congress appropriated from $2.9 million to $3.0 million for the HRSA TBI Program. This amount covered spending on personnel and other administrative costs, TBI-related technical assistance, and TBI Program Grants to the 50 states, 5 territories,3 and the District of Columbia (Martin-Heppel, 2005). By FY 2001, the appropriation for the program had risen to $5.0 million.
In FY 2002, when the HRSA TBI Program was expanded to include separate state grants to state P&A systems, the appropriation was increased
|
3 |
U.S. territories are Puerto Rico, U.S. Virgin Islands, Guam, American Samoa, and the Northern Mariana Islands. These territories are not included in the IOM committee’s evaluation of the Federal TBI Program in Chapter 4. |
TABLE 1-1 HRSA TBI Program Appropriations and Spending, FY 1997 to FY 2005 ($ in millions)
|
|
2005 |
2004 |
2003 |
2002 |
2001 |
2000 |
1999 |
1998 |
1997 |
|
Appropriationa |
$9.30 |
$9.50 |
$9.50 |
$7.50 |
$5.00 |
$5.00 |
$5.00 |
$3.00 |
$2.90 |
|
Spending |
|
||||||||
|
TBI Program Grants |
2.03 |
4.78 |
4.19 |
4.16 |
4.80 |
4.33 |
3.89 |
2.75 |
2.20 |
|
PATBI Grants to P&A Systems |
3.00 |
3.00 |
3.00 |
1.50 |
— |
— |
— |
— |
— |
|
TBI Technical Assistance Centerb |
3.47 |
0.77 |
1.45 |
0.97 |
0.15 |
0.59 |
0.93 |
NA |
0.58 |
|
NDRN |
0.05 |
0.05 |
0.07 |
— |
— |
— |
— |
— |
— |
|
Other |
0.42 |
0.49 |
0.48 |
0.71 |
0.01 |
0.04 |
0.14 |
NA |
.05 |
|
Total Spending |
$8.97 |
$9.09 |
$9.19 |
$7.34 |
$4.96 |
$4.96 |
$4.96 |
NA |
$2.83 |
|
NOTE: Dollars are rounded to the nearest thousand. PATBI = Protection and Advocacy for TBI; P&A = protection and advocacy; NDRN = National Disability Rights Network (formerly known as the National Association of Protection and Advocacy); NA = not available. aTotal appropriations are not available to the TBI Program; each year HRSA “taps” the appropriation to help cover the agency’s overall administrative, evaluation, and other costs. bFunds distributed to the TBI Technical Assistance Center (TBI TAC) in FY 2005 are intended to cover expenses for FY 2005 through early FY 2007. SOURCE: Martin-Heppel, 2005. |
|||||||||
to $7.5 million. Since FY 2003, the federal appropriation for the HRSA TBI Program has been in the range of $9.3 to $9.5 million.
States that receive TBI State Program Grants must provide matching funds of $1 for each $2 of federal grant funds they receive. In the early years of the HRSA TBI Program, FY 1997 to FY 2000, the match was required to be in cash. Since FY 2001, states have been permitted to use in-kind contributions including plant, equipment, or services.
In January 2005 and January 2006, the Administration has recommended zeroing out the TBI Program budget in the subsequent fiscal years (DHHS, 2005; DHHS, 2006). As of 2005, Congress was planning to continue funding at or near current levels, around $9 million (NASHIA, 2005).
Staffing for the HRSA TBI Program
The HRSA TBI Program has been operating with minimal staff—one full-time program director. The program director’s position has turned over four times since 1997. The current program director, a commissioned officer of the Public Health Service, has been running the HRSA TBI Program since October 2004.
A TBI Technical Assistance Center (TBI TAC), operated under contract to HRSA by the National Association of State Head Injury Administrators (NASHIA),4,5 supplements the skeletal staff for the HRSA TBI Program. TBI TAC is responsible for encouraging information and resource exchange, supporting the development of promising practices, and providing individualized assistance to state TBI programs and state-based protection and advocacy systems. It employs staff specialists who develop and disseminate special materials, plan annual grantee meetings, maintain a grantee listserv, and conduct site visits to state agencies.
Two TBI TAC activities are particularly notable. First, TBI TAC operates a web-based collaborative space (www.tbitac.nashia.org/tbics/), called TBICS. TBICS is available to all HRSA TBI Program grantees; other interested organizations and individuals may access TBICS, with permission. Second, TBI TAC has developed a set of performance benchmarks that state grantees may use to assess their progress in establishing an infrastructure (HRSA, 2005). HRSA’s payments to TBI TAC have fluctuated over the
years along with fluctuations in the availability of funds (Currier and Zeltinger, 2005). In recent years, TBI TAC’s operating budget has averaged around $1million.
GRANTS PROVIDED UNDER THE HRSA TBI PROGRAM
As noted earlier, the HRSA TBI Program encompasses two major programs: (1) the TBI State Grants Program, which awards grants to states, U.S. territories, and the District of Columbia to help them improve their infrastructure and capacity to provide post-acute services for persons with TBI and their families; and (2) the Protection and Advocacy for TBI (PATBI) Program, which awards grants to federally mandated P&A systems in states, U.S. territories, and the District of Columbia to help ensure their provision of P&A services for individuals with TBI and their families. Additional information about both is provided below.
TBI State Grants Program
HRSA has awarded grants to states and other entities to help them improve their TBI infrastructure and capacity on a competitive basis since the first grant cycle in FY 1997. Grants awarded under the TBI State Grants Program fall into three categories: Planning Grants, Implementation Grants, and Post-Demonstration Grants (Box 1-4).
During the first 2 years of the HRSA TBI Program’s existence, states and territories were able to compete for 1-year demonstration project awards (NASHIA, 2005). Under the TBI State Grants Program, the grants for which states were eligible depended on their status with respect to their progress in developing the four core components of a state’s TBI infrastructure. The four core components of a state’s TBI infrastructure are the following:
-
Statewide TBI advisory board. An advisory board charged with advising and making recommendations on ways to improve coordination of TBI services must be established. The board is obligated to hold public hearings and other community outreach efforts to encourage citizen participation in the TBI Program. Members of the advisory board must include representatives of the involved state agencies, public and nonprofit private health-related organizations, state disability advisory or planning groups, members of a state or local organization representing persons with TBI, local injury control programs (if such programs exist), and individuals who are TBI survivors or the family members of such individuals.
-
Lead state agency for TBI. A state agency and a staff position responsible for coordination of state TBI activities must be designated.
|
BOX 1-4 Planning Grants Planning Grants to states are intended to help states build the necessary infrastructure for a coordinated TBI service system. States must use the Planning Grants to establish four mandatory components of a TBI system infrastructure—namely, a statewide TBI advisory board, a lead state agency for TBI, a statewide TBI needs/resources assessment, and a statewide TBI action plan. Planning Grants of $75,000 per year were available for up to 2 years. Implementation Grants Implementation Grants to states are designed to encourage states to execute various program implementation activities, including carrying out the state’s TBI action plan, programs to address identified needs, and initiatives to improve access. Implementation Grants of $200,000 per year were available for up to 3 years. Post-Demonstration Grants Post-Demonstration Grants to states of $100,000 for 1 year were intended to further state efforts to build TBI service capacity and are available to states after their satisfactory completion of an Implementation Grant. These grants were first established when the HRSA TBI Program was reauthorized in the Children’s Health Act of 2000. SOURCE: HRSA, 1997. |
-
Statewide TBI needs/resources assessment. A statewide assessment of TBI needs and resources, with an emphasis on resources, must be completed or updated within the last 5 years and include the full spectrum of care and services from initial acute treatment through community reintegration for individuals of all ages having TBI.
-
Statewide TBI action plan. A statewide “action plan” to provide a culturally competent, comprehensive community-based system of care that encompasses physical, psychological, educational, vocational, and social aspects of TBI services and addresses the needs of individuals with TBI, as well as family members, must be developed.
Under the TBI State Grants Program, states that had an established plan for developing the four core components of a TBI infrastructure were
eligible to compete for a Planning Grant. States that had evidence that the four components were already in place were eligible to compete for an Implementation Grant. Post-Demonstration Grants intended to further efforts to build state-level TBI service capacity were established following the reauthorization of the HRSA TBI Program in the Children’s Health Act of 2000. In order to compete for these grants, states must have satisfactorily completed an Implementation Grant.
Federal statute circumscribes the services that states can fund with TBI State Program Grants (Box 1-5). Eligible services include interventions with the assumed potential to empower patients and families, to improve coordination of care, and to expedite access for underserved persons. HRSA prohibits grantees from using TBI State Program Grants to support primary injury prevention, research, or the provision of direct services (although the authorizing legislation is silent on this point) (HRSA, 2003; Martin-Heppel, 2005).
Protection and Advocacy for TBI (PATBI) Program
P&A systems for people with disabilities in the states, territories, and the District of Columbia, initially required as a condition of receiving federal P&A funds under the Developmental Disabilities Assistance and Bill of Rights Act of 1975 (P.L. 103-230, 1975), currently exist in all 50 states and U.S. territories. Federal law requires that the P&A agency in a state or territory be independent of public and private service providers.
HRSA has distributed PATBI Grants to P&A systems in states, territories, the District of Columbia, and the Native American Protection and Advocacy Project to bolster advocacy support for individuals with TBI and their families since FY 2002. As noted earlier, the PATBI Grants Program was authorized as a component of the HRSA TBI Program in the Children’s Health Act of 2000.
To be eligible for a PATBI Grant, the P&A system in a state or territory must have local authority to pursue legal, administrative, and other appropriate means to, for example, help persons with TBI establish their eligibility for treatment, community-based services, or change in living arrangements (HRSA, 2003). A P&A system may use the PATBI Grant to provide information, referrals, and advice; individual and family advocacy; legal representation; and specific assistance in self-advocacy for persons with TBI and their families.
In FY 2002, HRSA distributed $1.5 million in PATBI Grants on a competitive basis (Table 1-1 above) (NAPAS, 2005). P&A systems in the states were eligible for $50,000 grants; P&A systems in U.S. territories and the American Indian Consortium were eligible for $20,000 grants. Appro-
|
BOX 1-5 States may use their TBI State Program Grants to do the following:
States may also use their TBI State Program Grant funds to build state-level capacity for the following:
SOURCE: P.L. 106-310, 2000. |
priations for the PATBI Program were doubled to $3.0 million in FY 2003. Since then, PATBI Grants to P&A systems have been formula-based, so all states and territories have received the grants, with annual allotments ranging from a minimum of $50,000 up to $117,000 (California).
REFERENCES
Administration on Developmental Disabilities. April 2005. State Protection and Advocacy Agencies. [Online] Available: http://www.acf.hhs.gov/programs/add/states/pas.html [accessed 12/04/2005].
Caudle SL. 1994. Using qualitative approaches. In: Handbook of Practical Program Evaluation, Wholey, Hatry, and Newcomer (Eds.), San Francisco, CA: Jossey-Bass.
Currier K, Zeltinger R. 2005. Traumatic Brain Injury Technical Assistance Center. Presentation at the meeting of the Institute of Medicine Workshop on Traumatic Brain Injury. Washington, DC: The National Academies.
DHHS (Department of Health and Human Services). March 2005. Overview of the HRSA Budget Numeric Table. [Online] Available: http://www.hhs.gov/budget/05budget/healthres.html [accessed 11/28/2005].
——. February 2, 2006. Budget in Brief Fiscal Year 2006. [Online] Available: http://www.hhs.gov/budget/06budget/FY2006BudgetinBrief.pdf [accessed 2/6/2006].
GAO (Government Accountability Office). 2003. Program Evaluation: An Evaluation Culture and Collaborative Partnerships Help Build Agency Capacity. GAO-03-454. Washington, DC: GAO.
HRSA (Health Resources and Services Administration). 1997. Application Buidance for TBI Demonstration Grants Program.
——. 2003. Application Guidance for Competition for Competing TBI P&A Projects. Rockville, MD: DHHS.
——. 2005. Program Guidance FY 2005. Rockville, MD.
Martin-Heppel J (JMartin-Heppel@hrsa.gov). Budget data. E-mail to Jill Eden (jeden@nas.edu). November 30, 2005.
NAPAS (National Association of Protection & Advocacy Systems). 2005. The Protection and Advocacy for Individuals with TBI Program: Report of Activities for 2004. Washington, DC: NAPAS.
NASHIA (National Association of State Head Injury Administrators). November 2005. Capitol News. [Online] Available: http://www.nashia.org [accessed 11/27/2005].
Newcomer K, Scheirer M. 2001. Using Evaluation to Support Performance Management: A Guide for Federal Executives. Arlington, VA: PricewaterhouseCoopers Endowment for the Business of Government.
NIH (National Institutes of Health). 1998. NIH Consensus Statement: Rehabilitation of Persons With TBI. Bethesda, MD: NIH.
OMB (Office of Management and Budget). 2004. What Constitutes Strong Evidence of a Program’s Effectiveness? [Online] Available: http://www.whitehouse.gov/omb/part/2004_program_eval.pdf [accessed 12/5/2005].
——. 2005. Traumatic Brain Injury. In Department of Health & Human Services PART Assessments. [Online] Available: http://www.whitehouse.gov/omb/expectmore/summary.10002172.2005.html [accessed 12/05/2005].
P.L. 103-230. Developmental Disabilities Assistance and Bill of Rights Act of 1975. 1975.
P.L. 104-166. Traumatic Brain Injury Act of 1996.
P.L. 106-310. Children’s Health Act of 2000.
Sofaer S. 1999. Qualitative methods: What are they and why use them? Health Services Research. 34(5): 1101–1116.
State grants for projects regarding brain injury. 2003. Title 42 U.S. Code, Ch. 6A. GPO (Government Printing Office) Access. [Online] Available: http://www.access.gpo.gov/uscode/title42/chapter6a_subchapterx_parte_.html [accessed2/9/2006].
World Bank Group. 2005. Understanding Impact Evaluation. [Online] Available: http://www.worldbank.org/poverty/impact/index.htm [accessed 12/15/2005].
















