3
Building a 21st-Century Emergency and Trauma Care System
The committee’s vision for the emergency and trauma care system is rather simple. The committee envisions a system in which patients of all ages and in all communities receive well-planned and -coordinated emergency care services. Consideration of pediatric concerns during the planning stages will ensure that the system meets the needs of children. Dispatch, emergency medical services (EMS), emergency department (ED) providers, trauma care, public safety, and public health will be fully interconnected and united in an effort to ensure that each patient receives the most appropriate care, at the optimal location, with the minimum delay. From the standpoint of pediatric patients and their parents or guardians, delivery of emergency care services will be seamless. All service delivery will be evidence-based, and innovations will be rapidly adopted and adapted to each community’s needs. The performance of the system will be completely transparent, so that emergency medical technicians (EMTs) and parents will know which hospitals are best able to deliver care to critically ill or injured children (see Box 3-1).
The committee recognizes that improved care for children cannot be accomplished without addressing some of the failings in the larger emergency care system. The committee’s vision centers on three goals: coordination, regionalization, and accountability. While this vision may appear innovative, many of its elements have been advocated for decades. However, early progress toward achieving these elements was derailed as a result of deeply entrenched political interests and cultural attitudes, as well as funding cutbacks and practical impediments to change. These obstacles remain today, and represent the chief challenges to realizing the committee’s vision. Con-
|
BOX 3-1 A Vision of Pediatric Emergency Care in 2010 In a rural area, a car slides off the road and crashes 30 minutes from the nearest town. An automated crash notification system provides an emergency response center with detailed information about the location and characteristics of the crash. Passenger weights indicate that an adult and child, both properly restrained, are in the car. A dashboard displays information about the crash to air and ground response teams, emergency departments, and trauma facilities throughout the region. Because of the large impact of the crash, the automated triage system launches two advanced life support (ALS) response teams. An air medical response team is placed on standby. Once the EMS teams are on the scene, patients’ complete medical histories and alerts, obtained through a regional information system, are instantly available. Using an evidence-based triage protocol, one of the EMS teams determines that the child, an 8-year-old boy, is suffering from serious injuries. In accordance with regional transport protocols, the first responders call for air transport to bring the boy to the nearest trauma center. The paramedics stabilize the boy using age- and size-scaled equipment and drugs, and begin transmission of telemetry and on-board diagnostic scans to the trauma center. The other EMS team assesses the child’s father and determines that although he requires a lower level of care, he should be transported to the trauma center to accompany his son. An air transport team arrives at the scene and transports the child and father to a level I trauma center with the resources and medical experts needed to handle high-level pediatric and adult trauma cases. Care continues to be |
certed, cooperative efforts at multiple levels of government and the private sector are necessary to finally break through and achieve these goals.
This chapter is dedicated to describing the three goals of the committee’s vision for the emergency care system of the future, with a special focus on pediatric emergency care. In some areas of the country, states and regions are already developing coordinated, regionalized systems that incorporate elements of accountability; some of these efforts are described as well.
GOAL 1: COORDINATION
The current emergency care system faces a number of problems, but among the most long-standing of these is that emergency services are fragmented, resulting in poor communication and delayed services. EMS,
|
delivered en route in accordance with evidence-based treatment guidelines. The pediatric trauma specialist—alerted to the emergency when the air medical team was dispatched—performs emergency surgery when the child arrives at the hospital, and a pediatric intensivist is available for consult. The child receives the highest level of care based on the available clinical evidence. His medications, all approved for use in children, are delivered according to dosage guidelines for his age and size. The child’s pediatrician and father’s primary care provider are notified of the event. The child’s mother, who was not in the vehicle, is contacted immediately and apprised of the status of her husband and son. While understandably upset at the news, she takes some comfort in knowing that her husband and son are at a trauma center that has earned high marks for quality care delivery. When the mother arrives at the hospital, she is met by a social worker and nurse and given a clear explanation of the surgery being performed on her son. Hospital staff remain available to answer all of her questions. After surgery, the child is admitted to the hospital, where he spends a couple of days in recovery. When the child is eventually released from the hospital, the parents are given clear instructions for his continued care. A record of the event is automatically collected by the region’s emergency care information system, capturing information from the ground and flight paramedics as well as the hospital. A copy of that information is sent to both the state trauma registry and the National Trauma Data Bank. Additionally, the automatic crash notification system identifies that the crash occurred in an area where crashes are common and sends a notification to the public health department. |
hospitals, trauma centers, and public health have traditionally worked in silos, a situation that largely persists today (NHTSA, 1996). For example, public safety and EMS agencies often lack common communications frequencies and protocols for communicating with each other during disasters. Similarly, emergency care providers do not have access to patient medical histories that could be useful in decision making. Even within those silos, coordination may be limited. For example, only about half of hospitals with EDs have pediatric interfacililty transfer agreements (MCHB, 2004), which are necessary in case a hospital receives a critically ill or injured child but lacks the resources to properly manage his or her care. Jurisdictional borders also contribute to fragmentation under the current system. For example, one county in Michigan has 18 different EMS systems with different service models and protocols. Medicaid and other payer policies contribute
to geographic fragmentation when reimbursement does not follow patients seamlessly across state lines.
The problem is exacerbated in some regions by turf wars between firefighters and EMS personnel that were documented in a series of articles for USA Today (Davis, 2003). Even within EDs, there may be friction between emergency staff trying to admit patients and personnel on understaffed inpatient units who have no incentive for speeding up the admissions process. Lack of coordination between EMS and hospitals can result in delays that compromise care, and EDs may clash with on-call specialists over delays in response.
Also contributing to fragmentation is that pediatric concerns often are not included in the initial planning stages of the emergency care system. Either pediatric concerns are overlooked entirely, or planning for adult and pediatric care occurs independently. This is particularly true of disaster and trauma planning. A 2003 National Association of State EMS Directors (NASEMSD) survey found that only 14 states involved pediatric experts in state, regional, and local disaster planning. It is not surprising, then, that the majority of state disaster plans fail to address pediatric equipment and medications at hospitals (NASEMSD, 2004). Only about half of states report having designated pediatric trauma centers and trauma registries, indicating another important gap in planning (MCHB, 2004).
Importance of Linkages with Public Health
The ED has a special relationship with the community and state and local public health departments because it serves as a community barometer of both illness and injury trends (Malone, 1995). In her analysis of heavy users of ED services, Malone argued that “emergency departments remain today a ‘window’ on wider social issues critical to health care reforms” (p. 469). A commonly cited example is the use of seat belts. We now know that increased utilization of seat belts reduces the number of seriously injured car crash victims in the ED—the ED served as a proving ground for documenting the results of seat belt enforcement initiatives. Although prevention activities have been limited in the emergency care setting, that setting represents an important teaching opportunity. To take advantage of this opportunity, emergency care providers would benefit from the resources and experiences of public health agencies and experts in the implementation of injury prevention measures.
Perhaps now more than ever, with the threat of bioterrorism and outbreaks of such diseases as avian influenza and severe acute respiratory syndrome (SARS), it is essential that EMS, EDs, trauma centers, and state and local public health agencies partner to conduct surveillance for disease
prevalence and outbreaks and other health risks. Hospital EDs can recognize the diagnostic clues that may indicate an unusual infectious disease outbreak so that public health authorities can respond quickly (GAO, 2003). However, a solid partnership must first be in place—one that allows for easy communication of information between emergency providers and public health officials.
Importance of Linkages with Other Medical Care Providers
According to the American College of Emergency Physicians (ACEP), EDs “define their mission in terms of unlimited access regardless of citizenship, insurance status, ability to pay, day of week, or time of day…it is the only source of care available for certain populations” (O’Brien, 1999, p.19). Indeed, EDs fill many existing gaps within the health care network, serving as key safety net providers in many communities (Lewin and Altman, 2000). Studies have shown that a significant number of patients use the ED for nonurgent purposes because of financial barriers, lack of access to clinics after hours, transportation barriers, convenience, and lack of a usual source of care (Grumbach et al., 1993; Young et al., 1996; Peterson et al., 1998; Koziol-McLain et al., 2000; Cunningham and May, 2003). There is also evidence that clinics and physicians are increasingly using EDs as an adjunct to their practice, referring patients to the ED for a variety of reasons, such as their own convenience after regular hours, reluctance to take on a complicated case, the need for diagnostic tests they cannot perform in the office, and liability concerns (Berenson et al., 2003; Studdert et al., 2005). Unfortunately, in many communities there is little interaction between emergency care services and community safety net providers—this even though they share a common base of patients, and their actions may affect one another substantially. The absence of coordination represents missed opportunities for enhanced access; improved diagnosis, patient follow-up, and compliance; and enhanced quality of care and patient satisfaction.
Previous Calls for Improved Coordination
The value of integrating and coordinating emergency care has long been recognized. The 1966 National Academy of Sciences/National Research Council (NAS/NRC) report Accidental Death and Disability: The Neglected Disease of Modern Society called for better coordination of emergency care through Community Councils on Emergency Medical Services, which would bring together physicians, medical facilities, EMS, public health, and others “to procure equipment, construct facilities and ensure optimal emergency care on a day to day basis as well as in disaster or national
emergency” (NAS and NRC, 1966, p.7). In 1972, the NAS/NRC report Roles and Responsibilities of Federal Agencies in Support of Comprehensive Emergency Medical Services promoted an integrated, systems approach to planning at the state, regional, and local levels and called for the Department of Health, Education, and Welfare (DHEW) to take an administrative and leadership role in federal EMS activities. The Emergency Medical Services Systems Act of 1973 (P.L. 93-154) created a new grant program in the Division of EMS within DHEW to foster the development of regional EMS systems. The Robert Wood Johnson Foundation added support by funding the development of 44 regional EMS systems. Although the drive toward system development waned after the demise of the DHEW program and the block granting of EMS funds in 1981, the goal of system planning and coordination has remained paramount within the emergency care community. In 1996, the National Highway Traffic Safety Administration’s (NHTSA) Emergency Medical Services Agenda for the Future also emphasized the goal of system coordination:
EMS of the future will be community-based health management that is fully integrated with the overall health care system. It will have the ability to identify and modify illness and injury risks, provide acute illness and injury care and follow-up, and contribute to treatment of chronic conditions and community health monitoring…. [P]atients are assured that their care is considered part of a complete health care program, connected to sources for continuous and/or follow-up care, and linked to potentially beneficial health resources…. EMS maintains liaisons, including systems for communication with other community resources, such as other public safety agencies, departments of public health, social service agencies, departments of public health, social service agencies and organizations, health care provider networks, community health educators, and others…. EMS is a community resource, able to initiate important follow-up care for patients, whether or not they are transported to a health care facility. (NHTSA, 1996, pp. 7, 10)
Successes Achieved
While progress toward a highly integrated emergency care system has been slow, there have been some important successes in the coordination of emergency care services, which point the way toward solutions to the fragmentation that dominates the system today. For example, the trauma system in Maryland, described in more detail later in this chapter, provides a comprehensive and coordinated approach to the care of injured children. Children’s hospitals have also been successful at accomplishing regional coordination to ensure the transport and appropriate care of children needing specialized services. The pediatric intensive care system is a leading example
of regional coordination among hospitals, community physicians, and EMTs (Gausche-Hill and Wiebe, 2001). These are but a few examples demonstrating the possibilities for enhancing coordination of the system as a whole.
One promising public health surveillance effort is Insight, a computer-based clinical information system at the Washington Hospital Center (WHC) in Washington, D.C., designed to record and track patient data, including geographic and demographic information. The software proved useful during the 2001 anthrax attacks, when it enabled WHC to transmit complete, real-time data to the Centers for Disease Control and Prevention (CDC) while other hospitals were sending limited information with a lag time of one or more days. The success of Insight attracted considerable grant funding for the system’s expansion; WHC earmarked $7 million for Insight to link it to federal and regional agencies and to integrate it with other hospital systems (Kanter and Heskett, 2002).
Many communities have established primary care networks that integrate hospital EDs into their planning and coordination efforts. A rapidly growing number of communities, such as San Francisco and Boston, have developed regional health information organizations that coordinate the development of information systems to facilitate patient referrals and track the sharing of medical information between providers to optimize a patient’s care across settings. The San Francisco Community Clinic Consortium brings together primary and specialty care providers and EDs in a planning and communications network that closely coordinates the care of safety net patients throughout the city.
The Importance of Communications
Communications are a critical factor in establishing systemwide coordination. An effective communications system is the glue that can hold together effective, integrated emergency care services. It provides the key link between 9-1-1/dispatch and EMS responders and is necessary to ensure that on-line medical direction is available when needed. It enables ambulance dispatchers to tell callers what to do until help arrives and to track a patient’s progress following the arrival of EMS responders. An effective communications system also enables ambulance dispatchers to assist EMS personnel in directing patients to the most appropriate facility based on the nature of their illness or injury and the capacity of receiving facilities. It links the emergency medical system with other public safety providers—such as police and fire departments, emergency management services, and public health agencies—and facilitates coordination between the medical response system and incident command in both routine and disaster situations. It helps hospitals communicate with each other to organize interfacility trans-
fers and arrange for mutual aid. And it facilitates medical and operational oversight and quality control within the system.
GOAL 2: REGIONALIZATION
The goal of regionalization is to improve patient outcomes by directing patients to facilities with the optimal capabilities and best outcomes for any given type of illness or injury. A regionalized system ensures access to care at a level appropriate to patient needs while maintaining efficient use of available resources (Wright and Klein, 2001). Because not all hospitals within a community have the personnel and resources to support high-level pediatric emergency care delivery, critically ill and injured children should not be directed simply to the closest facility, but to the nearest facility with the pediatric expertise and resources needed to deliver high-level care.
Regionalization of emergency care is not a new concept. The Institute of Medicine (IOM) report Emergency Medical Services for Children noted that “categorization and regionalization are essential for full and effective operation of [pediatric emergency care] systems” (IOM, 1993, p. 171). Steps to regionalize certain pediatric services were supported by the American College of Critical Care Medicine and the Society of Critical Care Medicine in their 2000 Consensus Report for Regionalization of Services for Critically Ill or Injured Children (Committee on Pediatric Emergency Medicine Pediatric Section and Task Force on Regionalization of Pediatric Critical Care, 2000). Because of higher volume, regional providers gain experience in treating severely injured children, which in turn results in higher-quality care. Two recent studies found that child trauma patients have better outcomes at specialized pediatric centers (Stylianos, 2005; Densmore et al., 2006). Mortality among pediatric patients with respiratory failure or head injury is lower in hospitals that provide tertiary-level pediatric intensive care than in those that do not (Pollack et al., 1991; Tilford et al., 2005).
There is substantial evidence that regionalization of services to designated hospitals with greater experience improves outcomes and reduces costs across a range of high-risk conditions and procedures for adult patients, including cardiac arrest and stroke (Grumbach et al., 1995; Imperato et al., 1996; Nallamothu et al., 2001; Chang and Klitzner, 2002; Bardach et al., 2004). The literature also shows improved outcomes and lower costs associated with the regionalization of care for severely injured patients (Mullins and Mann, 1999; Jurkovich and Mock, 1999; Mann et al., 1999; Nathens et al., 2001; Chiara and Cimbanassi, 2003; Bravata et al., 2004), although the evidence in this regard is not uniformly positive (Glance et al., 2004). Regionalization benefits triage, medical care, outbreak investigations, security management, and emergency management. It may also be a cost-effective
strategy for developing and training teams of response personnel (Bravata et al., 2004).
An example of a pediatric regionalization effort is the regionalization of neonatal care. The use of neonatal intensive care services in the 1960s and 1970s proved to decrease neonatal mortality (Williams and Chen, 1982), but not all hospitals could purchase and support the sophisticated equipment and specialized staff needed to care for the small number of infants requiring such care (Holloway, 2001). In the interest of using resources efficiently and ensuring access to neonatal care, in 1976 a Committee on Perinatal Health organized by the March of Dimes recommended the development of a regionalized system of neonatal intensive care (Cifuentes et al., 2002). Under the system, premature or very ill newborns were to be transferred to the nearest designated center to receive the level of care they required (Jones, 2004). While it is difficult to draw a definitive conclusion, studies suggest that regionalization has contributed to lower neonatal mortality rates (Bode et al., 2001; Holloway, 2001; Cifuentes et al., 2002).
Another example is organized trauma systems, which have been shown to improve outcomes of trauma care and to reduce mortality from traumatic injury through regionalization (Mullins et al., 1994; Jurkovich and Mock, 1999; MacKenzie, 1999; Mullins and Mann, 1999; Nathens et al., 2000; MacKenzie et al., 2006). While the literature has long reported benefits of such systems for adult patients, there is less evidence for children (Wright and Klein, 2001); however, the limited available research indicates benefits from regionalized pediatric trauma care. The initiation of a regionalized trauma system in Oregon resulted in a reduction in the risk of death from serious pediatric injuries (Hulka et al., 1997; Hulka, 1999). In New York, the triage of moderately to severely injured children to centers within regionalized systems reduced the risk of death compared with nonregionalized systems operating in other parts of the state (Cooper et al., 1993; Hulka, 1999).
Many states and/or communities have taken steps toward regionalizing pediatric emergency care by designating hospitals that meet certain requirements as “stand-by emergency departments approved for pediatrics” (SEDPs), “emergency departments approved for or accepting pediatrics” (EDAPs), and/or “emergency pediatric centers” (EPCs) (Gausche-Hill and Wiebe, 2001). In some areas, only EDAP or EPC hospitals are allowed to accept pediatric patients who have been transported by advanced life support (ALS) EMS providers. However, a state-by-state analysis shows that many states have still not formally regionalized pediatric intensive care or trauma (Adomako and Melese-d’Hospital, 2004). Most pediatric trauma patients are not brought to pediatric trauma centers, and they receive less-than-optimal care as a result (Densmore et al., 2006).
Simply designating hospitals as SEDPs, EDAPs, or EPCs and formalizing pediatric EMS transport protocols to reflect those designations is not sufficient, however. As noted in Chapter 2, the vast majority of children do not access EMS before arriving at an ED (McCaig and Burt, 2005), and in part for this reason, most children are seen in general EDs (Gausche-Hill et al., 2004). In all likelihood, many of these EDs are not designated as SEDPs, EDAPs, or EPCs; this is certainly so if the state lacks a designation process. It is natural for many parents simply to bring their children to the closest ED. Therefore, all hospitals, especially those not recognized as having the ability to care for critically ill or injured pediatric patients, must be linked to a broader regional system. There must be clear protocols for transferring such patients from an ED without specialized pediatric capabilities to a better-equipped facility. Regionalization of emergency care helps ensure that pediatric patients receive definitive care as soon as possible, even in rural or remote areas.
Concerns About Regionalization
One concern about the regionalization of pediatric emergency and trauma care is that moving too many children to regional centers would further dilute the pediatric experience of community hospitals. But all hospitals must have some baseline of pediatric readiness. As noted above, they must have the capability to stabilize pediatric patients and must have formal transfer agreements in place with regional pediatric centers.
Another concern is that regionalizing services could adversely impact the overall availability of other services in a community. For example, loss of certain type of patients could result in the closure of a hospital unit or an entire hospital, particularly a small, rural hospital. The survival of small, rural facilities may require identification and treatment of those illnesses and injuries that do not require the capacities and capabilities of larger facilities, as well as repatriation to the local facility after stabilization at the tertiary center for long-term care and follow-up. A systems approach to regionalization considers the full effects of regionalizing services on a community. Determining the appropriate metrics for this type of analysis and defining the process for applying them within each region are significant research and practical issues. Nonetheless, in the absence of rigorous evidence to guide the process, planning authorities should take these factors into account in developing regionalized systems of emergency care.
Configuration of Services
The design of the emergency care system envisioned by the committee bears similarities to the inclusive trauma system concept that was espoused
by the American College of Surgeons (ACS) and has been widely adopted throughout the United States. Under the ACS approach, every hospital in the community can play a role in the trauma system by undergoing verification and designation as a level I to level IV/V trauma center, based on its capabilities. Trauma care is optimized in the region through protocols and transfer agreements that are designed to direct trauma patients to the most appropriate level of care available given the type of injury and the relative travel times to each center. As discussed earlier, the advantages of such a system are evident from studies demonstrating improved outcomes when patients receive care at designated facilities with specialized resources. These benefits accrue to pediatric patients as well as adults (Stylianos, 2005; Densmore et al., 2006).
The committee’s vision expands this concept beyond trauma to encompass all illnesses and injuries, and beyond hospitals to encompass the entire continuum of emergency care—including 9-1-1 and dispatch and prehospital EMS, as well as clinics and urgent care providers that may play a role in emergency care. In this model, every provider organization can play a role in providing emergency care in the community according to its capabilities. All hospitals are categorized in a manner similar to the way some states and communities have designated SEDPs, EDAPs, and EPCs. Initially, this categorization may simply be based on the existence of a dedicated pediatric ED; recommended pediatric equipment; and specialized pediatric services, such as pediatric neurosurgery. Over time, the categorization process may evolve to include detailed information, such as the times specific emergency procedures are available; arrangements for on-call pediatric specialty care; service-specific outcomes; or general emergency service indicators, such as time to treatment, frequency of diversion, and ED boarding. Prehospital EMS services may be similarly categorized according to pediatric capabilities. The result is a complete inventory of emergency care assets and capabilities within a community.
A standard national approach to the categorization of emergency care providers that reflects both adult and pediatric capabilities is needed. Categories should reflect meaningful differences in the types of emergency care available, yet be simple enough to be understood easily by the provider community and the public. The use of national definitions will ensure that the categories are understood by providers and by the public across states or regions of the country, and will also promote benchmarking of performance.
The committee concludes that a standard national approach to the categorization of emergency care is essential for the optimal allocation of resources and provision of critical information to an informed public. Therefore, the committee recommends that the Department of Health and Human Services and the National Highway Traffic Safety Administration, in part-
nership with professional organizations, convene a panel of individuals with multidisciplinary expertise to develop evidence-based categorization systems for emergency medical services, emergency departments, and trauma centers based on adult and pediatric service capabilities (3.1). The categorization systems should be developed within 18 months of the release of this report. The two federal agencies should fund the process and convene the panel of emergency care experts and medical professionals to review the literature and develop the categorization systems. The multidisciplinary nature of the process should help ensure that the categories reflect the viewpoints of the various stakeholders and facilitate familiarity with the categories, as well as their adoption. The results of this process should be a complete inventory of emergency care assets for each community, which should be updated regularly to reflect the rapid changes in delivery systems nationwide.
Treatment, Triage, and Transport
The information generated by the implementation of recommendation 3.1 could be used to develop protocols that would guide EMTs in the transport of patients. But more research and discussion are needed to develop transport protocols. For example, it is unclear whether pediatric dispatch cards, which vary across jurisdictions, are appropriate. More research and discussion are needed to determine under what circumstances patients should be brought to the closest hospital for stabilization and transfer as opposed to being transported directly to the highest level of care, even if that facility is farther away. A debate remains over whether EMS providers should perform ALS procedures in the field or whether rapid transport to definitive care is best (Wright and Klein, 2001). The answer to this question likely depends, at least in part, on the type of emergency condition. It is evident, for example, that whether a patient will survive out-of-hospital cardiac arrest depends almost entirely on actions taken at the scene, including rapid defibrillation, provision of cardiopulmonary resuscitation (CPR), and perhaps other ALS interventions. Delaying these actions until the unit reaches a hospital results in dismal rates of survival and poor neurological outcomes. Conversely, there is little that prehospital personnel can do to stop internal bleeding from major trauma. In this instance, rapid transport to definitive care in an operating room offers the victim the best odds of survival. For example, a recent study showed that bypassing a level II trauma center in favor of a more distant level I trauma center may be optimal for head trauma patients (McConnell et al., 2005).
EMS responders who provide stabilization before the patient arrives at a critical care unit are sometimes subject to criticism because of a strongly held bias among some physicians that out-of-hospital stabilization only delays definitive treatment without adding value; however there is little evidence
that the prevailing “scoop and run” paradigm of EMS is always optimal (Orr et al., 2006). Decisions regarding the appropriate steps to take should be resolved using the best available evidence. The committee concludes that there should be a national approach to the development of prehospital protocols. Therefore, the committee recommends that the National Highway Traffic Safety Administration, in partnership with professional organizations, convene a panel of individuals with multidisciplinary expertise to develop evidence-based model prehospital care protocols for the treatment, triage, and transport of patients, including children (3.2). These protocols should be developed within 18 months of the release of this report. NHTSA should fund the process and convene the panel of emergency care experts and medical professionals to review the literature and develop the protocols. In addition, the process of updating these protocols will be important because it will determine how rapidly patients receive the current standard of care. This effort need not start from scratch. The Model Pediatric Protocols developed by the National Association of EMS Physicians and supported by the Emergency Medical Services for Children (ESM-C) program, which cover the treatment of pediatric patients in the prehospital environment, can serve as a starting point for the initiative as it relates to pediatric patients.
Treatments may require modification to reflect local resources, capabilities, and transport times; however, the basic pathophysiology of human illness is the same in all areas of the country. Once in place, the national protocols could be tailored to local assets and needs. Regional protocols should reflect the state of readiness of given facilities within a region at a given point in time. Real-time, concurrent information on the availability of hospital resources and specialties should be made available to EMS providers to inform transport decisions. Figure 3-1 shows an example of the service configuration in a regionalized system.
In addition to the use of the EMS system to direct patients to the optimum location for emergency care, hospital emergency care designations should be posted prominently. Particularly for pediatric patients, who are generally transported to the ED by their parents or caregivers rather than by EMS, public information about an ED’s pediatric capabilities is essential.
Again, the concept of categorization of hospitals based on capabilities is not new. It was recommended not only in the 1993 IOM Report Emergency Medical Services for Children, but also in the 1966 NAS/NRC report Accidental Death and Disability (NAS and NRC, 1966). According to that report:
Hospital emergency departments should be surveyed…to determine the numbers and types of emergency facilities necessary to provide optimal emergency treatment for the occupants of each region…. Once the required numbers and types of treatment facilities have been determined, it may be necessary to lessen the requirements at some institutions, increase them in others, and even
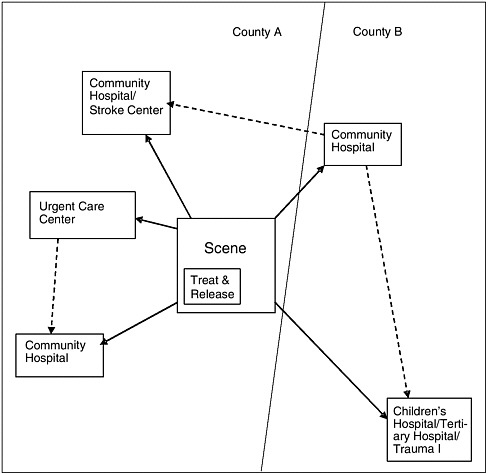
FIGURE 3-1 Service configuration in a regionalized system. The figure illustrates some potential transport options within a regionalized system. The basic structure of current EMS systems is not altered, but protocols are refined to ensure that patients go to the optimal facility given their type of illness or injury, the travel time involved, and facility status (e.g., ED and intensive care unit bed availability). For example, instead of taking a pediatric trauma victim to the closest general community hospital within the county, EMTs could cross county lines and transport the patient to a nearby pediatric center. Over time, based on evidence on the effectiveness of alternative delivery models, some pediatric patients may be transported to a nearby urgent care center for stabilization or treated and released at the scene. Whichever pathway the patient follows, communications are enhanced, data collected, and the performance of the system evaluated and reported so that future improvements can be made.
redistribute resources to support space, equipment, and personnel in the major emergency facilities. Until patient, ambulance driver, and hospital staff are in accord as to what the patient might reasonably expect and what the staff of an emergency facility can logically be expected to administer, and until effective transportation and adequate communication are provided to deliver casualties to proper facilities, our present levels of knowledge cannot be applied to optimal care and little reduction in mortality and/or lasting disability can be expected. (p. 20)
GOAL 3: ACCOUNTABILITY
Accountability is perhaps the most important of the three goals envisioned by the committee because it is necessary to achieving the other two. Lack of accountability has contributed to the failure of the emergency care system to adopt these changes in the past. Without accountability, participants in the system need not accept responsibility for failures and can avoid making changes necessary to improve the delivery of care.
Accountability is difficult to establish in emergency care because responsibility is dispersed across many different components of the system; thus it is difficult even for policy makers to determine where system breakdowns occur and how they can subsequently be addressed. When hospitals lack transfer agreements, when providers receive no continuing pediatric education, and when pediatric specialists and on-call specialists are not available, no one party is to blame—it is a system failure. Ambulance diversion is another good example. When a city recognizes it has an unacceptably high frequency of diversion, whom should it hold accountable? EMS can blame the hospitals for crowding and excessively long off-loading times; hospitals can blame the on-call specialists or the discharge sites that are unwilling to take additional referrals; and both can blame the state public health department for inadequate funding of community-based alternatives or community physicians for excessive referrals of their patients to the ED.
The unpredictable and infrequent nature of emergency care contributes to the lack of accountability. Most people have limited exposure to the emergency care system—an ambulance call or a visit to the ED is a rare event. Therefore, the performance of the system is generally not in the forefront of public awareness. Further, public awareness is hindered by the lack of nationally defined indicators of system performance. Few localities can answer basic questions about their emergency care services, such as how well 9-1-1, dispatch, prehospital EMS, hospital emergency and trauma care, and other components of the system perform and how their performance compares with that in other regions and the rest of the nation. Consequently, few understand the present crisis facing the system. By and large, the public assumes that the system functions better than it actually does (Harris Interactive, 2004).
Building Accountability
The committee believes three steps are required to bring accountability into the emergency care system: development of national performance indicators, measurement of performance within communities, and public dissemination of information on system performance.
Development of National Performance Indicators
There is currently no shortage of standards-setting efforts. ED performance measures have been developed by Qualis Health and Lindsay (Lindsay et al., 2002). The Data Elements for Emergency Department Systems (DEEDS) project and Health Level Seven (HL7) are working to develop uniform specifications for ED performance data (Pollock et al., 1998; National Center for Injury Prevention and Control, 2004; Health Level 7, 2005; Personal communication, R.W. Sattin, November 30, 2005). And the ACS and several partners have developed surgical process and outcome measures under the National Surgical Care Improvement Project.
The EMS Performance Measures Project is coordinated by the National Association of State EMS Officials in partnership with the National Association of EMS Physicians, and is supported by NHTSA and the Health Resources and Services Administration (HRSA). The project is working to develop consensus measures of EMS system performance that will assist in demonstrating the system’s value and defining an adequate level of EMS service and preparedness for a given community (EMS Performance Measures Project, 2005). The consensus process of the project has sought to unify disparate efforts to measure performance previously undertaken nationwide that have lacked consistency in definitions, indicators, and data sources. Work undertaken under the project in 2004 resulted in the development of 138 indicators of EMS performance. This list was pared down to 25 indicators in 2005. The list included system measures such as “What are the time intervals in a call?” and “What percentage of transports is conducted with red lights and sirens?” and clinical measures such as “How well was my pain relieved?” The questions were defined using data elements from the National EMS Information System (NEMSIS) dataset so that results could be compared across EMS systems.
In addition, statewide trauma and EMS systems are evaluated by the ACS, HRSA’s Division of Trauma and EMS, and NHTSA’s Office of EMS. There are also various components of the system with independent accrediting bodies. Hospitals, for example, are accredited by the Joint Commission on Accreditation of Healthcare Organizations, ambulance services are accredited by the Commission on Accreditation of Ambulance Services, and air medical services are voluntarily accredited by the Commission on
Accreditation of Medical Transport Systems. Each of these organizations collects performance information.
However, many performance measurement efforts have two major shortcomings. First, many such efforts do not specifically address pediatric performance measures. As discussed in Chapter 5, it is critical that information systems incorporate specific attributes of pediatric illness and injury. Second, the measures developed cannot be used to assess the performance of the full emergency care system within each community and benchmark that performance against statewide and national performance metrics. A credible entity to develop such measures would not be strongly tied to any one component of the emergency care continuum. One approach would be to form a collaborative entity that would include representation from all of the system components—hospitals, trauma centers, EMS agencies, physicians, nurses, and others. Certainly individuals with pediatric expertise must be involved as well.
Another approach would be to work with an existing organization, such as the National Quality Forum (NQF), to develop a set of emergency care–specific measures. NQF grew out of the President’s Advisory Commission on Consumer Protection and Quality in the Health Care Industry in 1998. It operates as a not-for-profit membership organization made up of national, state, regional, and local groups representing consumers, public and private purchasers, employers, health care professionals, provider organizations, health plans, accrediting bodies, labor unions, supporting industries, and organizations involved in health care research or quality improvement. NQF has reviewed and endorsed measure sets applicable to several health care settings and clinical areas and services, including hospital care, home health care, nursing-sensitive care, nursing home care, cardiac surgery, and diabetes care (NQF, 2002, 2003, 2004a,b, 2005).
The committee concludes that a standard national approach to the development of performance indicators is essential and recommends that the Department of Health and Human Services convene a panel of individuals with emergency and trauma care expertise to develop evidence-based indicators of emergency and trauma care system performance, including the performance of pediatric emergency care (3.3). The federal government must play a lead role in this effort because of the need for an independent, national process involving the broad participation of every component of emergency care. The Department of Health and Human Services (DHHS) should fund the process and convene the panel of individuals with emergency and trauma care expertise to review the research and develop performance indicators. The committee intends this to be a discrete project to be conducted within a brief timeframe. The set of performance indicators should be selected within 18 months of the release of this report.
The measures developed should include structure and process measures,
but evolve toward outcome measures over time. They should be nationally standardized so that statewide and national comparisons can be made. Measures should evaluate the performance of individual provider organizations within the system, as well as that of the system as a whole. Measures should also be sensitive to the interdependence among the components of the system; for example, EMS response times may be related to EDs going on diversion. Naturally, measures should also be appropriate for assessing the performance of pediatric emergency care. To this end, it may be necessary to include additional, pediatric-specific measures in data collection efforts.
Furthermore, because an episode of emergency care can span multiple settings, each of which can have a significant impact on the final outcome, it is important that patient-level data from each setting be captured and combined. Currently it is difficult to piece together an episode of emergency care. To address this need, states should develop guidelines for the sharing of patient-level data from dispatch through post–hospital release. The federal government should support such efforts by sponsoring the development of model procedures that can be adopted by states to minimize their administrative costs and liability exposure as a result of sharing these data.
Measurement of Performance
Using measures developed through a national consensus process, performance data should be collected on a regular basis from all of the emergency care providers in a community. The data should be tabulated in ways that can be used to measure, report on, and benchmark system performance. For example, emergency care systems across the country might be tasked with providing data on time-critical pediatric conditions, such as respiratory arrest. Data from the various system components would allow researchers to measure how well the system ensures the appropriate performance of each link in the chain of survival for the care of children (9-1-1, first response, EMS, ED, trauma), and would be useful for ongoing feedback and process improvement. Using their regulatory authority over health care services, states should play a lead role in collecting and analyzing these performance data. Careful attention by the states will be required to ensure that the reporting of performance measures by provider organizations results in real improvements in care processes and outcomes, as opposed to being simply cosmetic paper exercises that demonstrate compliance.
While a full-blown data collection and reporting system for performance measurement is the desired ultimate outcome, the committee believes a handful of key indicators of regional system performance should be collected and promulgated as soon as possible. These could include, for example, indicators of diversion, boarding, and EMS times to arrival. It is essential that pediatric indicators be included in initial data collection and
performance assessment efforts. Examples include time to administration of antibiotics for treatment of meningitis or time to first nebulization for treatment of asthma. Indicators should also aim to be outcome-based. For example, systems could collect data on pediatric respiratory arrest or respiratory failure—time-sensitive sentinel conditions that are amenable to an outcome assessment.
Public Dissemination of Information on System Performance
Public dissemination of performance data is crucial to drive the needed changes in the delivery of emergency care services. Dissemination can take various forms, including public report cards, annual reports, and state public health reports. Public dissemination of health care information is still in a state of development despite the proliferation of such initiatives over the past two decades. Problems include the costs associated with data collection, the sensitivity of individual provider information, concerns about the interpretation of data by the public, and a lack of public interest. There are many examples from which to learn: the Health Plan Employer Data and Information Set (HEDIS), which reports on managed care plans to purchasers and consumers; the Centers for Medicare and Medicaid Services’ (CMS) reports on home health and nursing home care—the Home Health Compare and Nursing Home Compare websites, respectively (CMS, 2005e); and Hospital Compare from the Hospital Quality Alliance, which reports comparative quality data on hospitals (CMS, 2005d). A number of states and regional business coalitions have also developed report cards on managed care plans and hospitals (State of California Office of the Patient Advocate, 2005). Because of the unique status of the emergency care system as an essential public service and the public’s limited awareness of the significant problems facing the system, the public is likely to take an active interest in this information. The committee believes dissemination of these data will have an important impact on public awareness and the development of integrated regional systems.
Public reporting can be at a detailed or aggregate level. Because of the potential sensitivity of performance data, they should initially be reported in the aggregate, at the national, state, and regional levels, rather than at the level of the individual provider. Prematurely reporting provider performance data may inhibit participation and divert providers’ resources to public relations rather than corrective efforts. At the same time, however, movement toward public reporting should begin as swiftly as possible. Moreover, individual providers should have full access to their own data so they can understand and improve their individual performance, as well as their contribution to the overall system. Over time, information on individual provider organizations should become an important part of the
public information on the system. Eventually, the data may be used to drive performance-based payment for emergency care.
CURRENT APPROACHES
A number of current efforts to establish emergency care systems achieve some or all of the committee’s goals of coordination, regionalization, and accountability. Some are purely voluntary, while others have the force of state regulation. Some are local and regional in scope, while others are statewide or national. This section highlights several such efforts that provide insights for future initiatives.
The Maryland EMS and Trauma System
Maryland has a unique statewide system that coordinates all EMS and trauma activity throughout the state. The Maryland Institute for EMS Systems (MIEMSS) is an independent state agency governed by an 11-member board that is appointed by the governor. The system provides training and certification, has established statewide EMS protocols, coordinates care through a central communications center, and operates the air medical system in coordination with the Maryland State Police. The system is funded in part through a surcharge on state driver’s license fees.
Coordination
MIEMSS has an EMS for children program that oversees grants from the federal EMS-C program and provides a focal point for statewide resources and networking on emergency care for children and their families. The Maryland EMS for children program develops state guidelines and resources for care, reviews pediatric emergency care and facility regulations, and coordinates pediatric education programs. Additionally, the program works with organizations, including the Safe Kids Coalition, the National Study Center for Trauma and Emergency Medical Systems, the Maryland Highway Safety Office, and the American Trauma Society, to foster and support education and injury prevention programs.
A statewide communications center coordinates all communications between EMS and other components of the system. The system links ambulances, helicopters, and hospitals and enables direct communications between components at any time. For example, a paramedic in western Maryland can talk directly with a local ED physician or obtain on-line consultation with a specialty hospital in Baltimore. While the local 9-1-1 centers initiate dispatch, they are usually too busy to follow patients through the
continuum of care. The statewide communications center provides support by maintaining communications links, providing medical direction, and maintaining continuity of care. The center has direct links to incident command to facilitate management of EMS resources as an event unfolds.
The state also is developing a new wireless digital capability that will connect EMS with other public safety entities (police, fire, emergency management, public health) throughout the state. In addition, the state has developed a County Hospital Alert Tracking System (CHATS) to monitor the status of hospitals and EMS assets so ambulances can be directed to less crowded facilities. This capability can also be applied to individual services—for example, patients with acute coronary syndrome can be directed to facilities based on the current availability of reperfusion suites. The Facility Resource Emergency Database system was designed to gather detailed information electronically from hospitals on bed availability, staffing, medications, and other critical capacity issues during disasters, but is also used to monitor and report on system capacity issues on a regular basis.
The state ensures coordination and compliance with protocols through its statewide training, provider designation, and licensure functions. In addition to providing EMS training and certification, the system offers statewide disaster preparedness training for members of the National Disaster Medical System.
Regionalization
While EMS and 9-1-1 are operated locally, they utilize statewide protocols that promote regionalization of pediatric services to two designated centers. Regionalization is also used to direct adult patients to trauma, stroke, burn, eye, perinatal, and hand referral centers. The control of air medical services by the state facilitates the regionalization of care through the active operation of dispatch.
Accountability
The state monitors performance at the provider and system levels through a provider review panel that regularly evaluates the operation of the system. As a state agency, the system reports on its performance goals and improvements. Also, CHATS enables participating hospitals and the public to view the status of hospitals at all times through its website, including data on availability of cardiac monitor beds, ED beds, and trauma beds. Paper ambulance run sheets are being replaced with an electronic system so that data can be collected and analyzed quickly to facilitate real-time performance improvement.
While Maryland is relatively advanced in achieving the goals of coor-
dination, regionalization, and accountability, it is not clear how easily its system could be replicated in other states. The system has benefited from strong and stable leadership in the state office, adequate funding, a high concentration of resources, and limited geography—features that many states do not currently enjoy.
Austin/Travis County, Texas
Austin/Travis County and four surrounding counties agreed to form a single EMS and trauma system to provide seamless care to emergency and trauma patients throughout the region. The initiative, 10 years in the making, started with a fragmented delivery system consisting of the Austin EMS system, 13 separate fire departments, and a 9-1-1 service run through the sheriff’s office that lacked unified protocols. These different entities agreed to come together to form a unified system that would coordinate all emergency care within the region. The system operates through a Combined Clinical Council that includes representatives of the different agencies and providers within the geographic area, including fire departments, 9-1-1, EMS, air medical services, and corporate employers. This is a “third service” system—it is separate from fire and other public safety entities.
Coordination
Coordination of care is achieved through several means. A unified set of clinical guidelines was developed and is maintained by the system in accordance with current clinical evidence. These guidelines provide a common framework for the care and transport of patients throughout the system. Any changes to the guidelines must be evaluated and approved by the Combined Clinical Council.
All providers in the region have a common set of credentials and are given badges that identify them as certified providers within the system, substantially reducing the multijurisdictional fragmentation that is common across metropolitan areas. In addition, there is no distinction within the system between volunteer and career providers. The integrated structure facilitates both incident command and disaster planning.
Regionalization
The unified system supports the regional emergency and trauma care system through clinical operating guidelines that determine the care and transport of all emergency and trauma patients. But the system is focused more on coordination and medical direction of EMS than on regionalization of care.
Accountability
A Healthcare Quality Committee is charged with reviewing the performance of the system and recommending specific actions to improve quality.
San Diego County, California
San Diego County has a regionalized trauma system that is characterized by a strong public–private partnership between the county and its five adult and one children’s trauma centers. Public health, assessment, policy development, and quality assurance are core components of the system, which operates under the auspices of the state EMS Authority.
Coordination
A countywide electronic system (QA Net) provides the real-time status of every trauma center and ED in the county, including the reason for diversion status, intensive care unit (ICU) bed availability, and trauma resuscitation capacity. The system has been in place for over 10 years and is a critical part of the coordination of emergency and trauma care in the county.
A regional communications system serves as the backbone of the emergency and trauma care system for both day-to-day operations and disasters. It includes an enhanced 9-1-1 system and a countywide network that allows all ambulance providers and hospitals to communicate. The network is used to coordinate decisions on EMS destinations and bypass information, and allows each hospital and EMS provider to know the status of every other hospital and provider on a real-time basis. Because the system’s authority comes from the state to the local level, all prehospital and emergency hospital services are coordinated through one lead agency. This arrangement provides continuity of services, standardized triage, treatment and transport protocols, and an opportunity to improve the system as issues are identified.
Regionalization
The county is divided into five service areas, each of which has at least a level II trauma center. Adult trauma patients are triaged and transported to the appropriate trauma center, while the children’s hospital provides trauma care to all seriously injured children below the age of 14. Serious burn cases are taken to the University of California-San Diego Burn Center. The county is considering regionalization for other conditions, such as stroke and heart attack, based on the trauma model. The system includes the designation of
regional trauma centers, designation of base hospitals to provide medical direction to EMS personnel, establishment of regional medical policies and procedures, and licensure of EMS services.
Accountability
Accountability is driven by a quality improvement program in which a medical audit committee meets monthly to review systemwide patient deaths and complications. The committee includes trauma directors; trauma nurse managers; the county medical examiner; the chief of EMS; and representatives of key specialty organizations, including orthopedic surgeons and neurosurgeons, as well as a representative for nondesignated facilities. A separate prehospital audit committee that includes ED physicians and prehospital providers also meets monthly and discusses any relevant prehospital issues.
Palm Beach County, Florida
An initiative currently under way in Palm Beach County, Florida, is more limited in scope than the systems highlighted above and is in the initial stages of development. The goal of the initiative is to find regional solutions to the limited availability of physician specialists who provide on-call emergency care services. In spring 2004, physician leaders, hospital executives, and public health officials formed the Emergency Department Management Group to address this problem. One approach being explored is to attack the rising cost of malpractice insurance for emergency care providers, which discourages specialists from serving on on-call panels. The organization is developing a group captive insurance company to offer liability coverage for physicians providing care in county EDs.
Coordination
The Emergency Department Management Group is developing a web-based, electronic ED call schedule so the EMS system can track which specialists are available at all hospitals throughout the county. This will enable the system to direct transport to the most appropriate facility based on a patient’s type of injury or illness.
Regionalization
The Emergency Department Management Group is exploring the regionalization of certain high-demand specialties, such as hand surgery and neurosurgery, so that the costs of maintaining full on-call coverage can be
concentrated in those few hospitals where the volume of cases makes it feasible to maintain such coverage. Hospitals throughout the county would pay a “subscription fee” to support the cost of on-call coverage at designated hospitals. The fee would be set at a level below what it would cost to have hospitals manage their on-call coverage individually.
Accountability
The initiative includes the development of a countywide quality assurance program under which all hospitals would submit certain data elements for assessment. It is unclear at this time how far this system would go toward public disclosure of system performance.
NEED FOR A DEMONSTRATION PROGRAM
States and regions face a variety of situations, and no one approach to building emergency care systems will achieve the goals discussed in this chapter. There is, for example, substantial variation across states and regions in the level of development of trauma systems; the effectiveness of state EMS offices and regional EMS councils; and the degree of coordination and integration among fire departments, EMS, hospitals, trauma centers, and emergency management. The baseline conditions and needs also vary. For example, rural areas face very different problems from those of urban areas, and an approach that works for one may be counterproductive for the other.
In addition to these varying needs and conditions, the problems involved are too complex for the committee to prescribe an a priori solution. A number of different avenues should be explored and evaluated to determine what does and does not work. Over time and over a number of controlled initiatives, such a process should yield important insights about what works and under what conditions. These insights can provide best-practice models that can be widely adopted to advance the nation toward the committee’s vision.
The process described here is one that can be supported effectively through federal demonstration projects. Such an approach can provide funding critical to project success; guidance for design and implementation; waivers from federal laws that might otherwise impede the process; and standardized, independent evaluations of projects and overall national assessment of the program. At the same time, the demonstration approach allows for significant variations according to state and regional needs and conditions within a set of clearly defined parameters. The IOM report Fostering Rapid Advances in Health Care: Learning from System Demonstrations articulated the benefits of the demonstration approach: “There is
no accepted blueprint for redesigning the health care sector, although there is widespread recognition that fundamental changes are needed…. For many important issues, we have little experience with alternatives to the status quo…. [T]he committee sees the launching of a carefully crafted set of demonstrations as a way to initiate a ‘building block’ approach” (IOM, 2002).
The committee therefore recommends that Congress establish a demonstration program, administered by the Health Resources and Services Administration, to promote coordinated, regionalized, and accountable emergency care systems throughout the country, and appropriate $88 million over 5 years to this program (3.4). The demonstration projects should aim to optimize emergency services for both adults and children. The essential features of the proposed program are described below.
Recipients
Grants would be targeted at states, which could develop projects at the state, regional, or local level; cross-state collaborative proposals would be encouraged. Grantees would be selected through a competitive process based on the quality of proposals and assessment of the likelihood of success in achieving the stated goal(s). Grantees could propose approaches addressing one, two, or all three of the goals of coordination, regionalization, and accountability. Proposals would not have to address more than one goal, but should address the implications of the proposed project for both pediatric and adult patients.
Purpose of the Grants
Each proposal would be required to describe the proposed approach in detail, explain how it would achieve the stated goal(s), identify who would carry out the responsibilities associated with the initiative, identify the costs associated with its implementation, and describe how success would be measured. Proposals should describe the state’s current stage of development and sophistication with regard to the stated goal(s) and explain how the grant would be used to enhance system performance in that regard.
Grants could be used in a number of different ways. Grant funds could be used to enhance communications so as to improve coordination of services; of particular interest would be the development of centralized communications centers at the regional or state level. Grants could be used to establish convening and planning functions, such as the creation of a regional or state advisory group of stakeholders for the purposes of building collaboration and designing and executing plans to improve coordination. Grant funds could be used to hire consultants and staff to manage the planning and
coordination functions, as well as to pay for data collection, analysis, and public reporting. In very limited circumstances, they could also be used to implement information systems for the purpose of improving coordination of services. Grant funds should not, however, be used for routine functions that would be performed in the absence of the demonstration project, such as the hiring or training of pediatric specialists or the purchase of pediatric equipment. Funds could also be used to enhance linkages between rural and urban emergency services within broadly defined regions so as to improve rural emergency care through communications, telemedicine, training, and coordination activities.
Funding Levels
The committee proposes a two-phase program. In phase I, the program would fund up to 10 projects at up to $6 million over 3 years. The committee recommends support for 10 projects for two reasons. First, the committee hopes that the publication of its recommendations in this report will stimulate a desire among states and communities to undertake efforts to achieve the committee’s vision. Resources should be available to encourage and support these efforts. Second, there is likely to be considerable variation in the types of projects proposed. A good number of projects will be needed to generate appropriate lessons learned.
Based on successful results that appeared to be replicable and sustainable in other states, the program would launch phase II, in which smaller, 2-year demonstration grants—up to $2 million each—would be made available to up to 10 additional states. This phase of the program would also include a technical assistance program designed to disseminate results and practical guidance to all states. Program administration would encompass evaluation of the program throughout its 5 years, including reports and public comments at 2.5 and 5 years after program initiation. The committee estimates funding for the program as follows:
-
Phase I grants: $60 million (over 3 years)
-
Phase II grants: $20 million (over 2 years)
-
Phase II technical assistance: $4 million (over 2 years)
-
Overall program administration: $4 million (over 5 years)
-
Total program funding: $88 million (over 5 years)
Granting Agency
No single agency has responsibility for the multiple components of the nation’s emergency care system. This responsibility is currently shared among multiple agencies—principally NHTSA, HRSA, CDC, and the De-
partment of Homeland Security (DHS). If, as recommended below, a lead agency is established to consolidate funding and provide leadership for these multiple activities, it would be the appropriate agency to lead this proposed effort. Until that consolidation occurs, however, the committee believes this demonstration program should be placed within HRSA. HRSA currently directs the EMS-C program and sponsored the Trauma-EMS Systems Program, both of which share many of the broad goals of the proposed demonstration program. HRSA has already shown a willingness and ability to collaborate effectively with other relevant federal agencies and should be encouraged to consider them as partners in this enterprise. The agency or agencies that oversee the program should be sure that grantees address pediatric concerns within their demonstration projects.
REDUCING BARRIERS TO IMPLEMENTATION
If the process of redesigning the emergency care system to achieve the goals outlined by the committee is to be successful, it must be supported. As stated in Fostering Rapid Advances in Health Care, “…we must both plant the seeds of innovation and create an environment that will allow success to proliferate. Steps must be taken to remove barriers to innovation and to put in place incentives that will encourage redesign and sustain improvements” (IOM, 2002). The process used to redesign the system must include payment policies that reward successful strategies. It must recognize the interdependencies within emergency care and address systemic problems. It must balance the interests of many different stakeholders. And it must involve leadership at many levels taking responsibility for creating change. A number of institutional barriers to the adoption of coordinated, regionalized, accountable emergency care systems currently exist. These include payment systems, the legal framework that defines much of the structure of emergency care delivery, and the level of coordination of emergency care at the federal level.
Aligning Payment with Incentives
No major change in health care can take place without strong financial incentives. The way emergency care services are reimbursed reinforces certain modes of delivery that are inefficient and are a barrier to achieving the committee’s vision of emergency care. Under Medicare and Medicaid, for example, prehospital providers are not paid unless they transport a patient to the hospital. This makes it difficult for regional systems to introduce innovations such as “treat and release” or other nontransport approaches that could result in better care for patients and more efficient system design. CMS and all other payers should eliminate this requirement and develop
a payment system for prehospital care that reflects the costs of providing those services.
Similarly, many hospitals do not have a strong economic motivation to address the problems of ED crowding, boarding, and ambulance diversion; indeed, they may even benefit from these practices. Several payment approaches could eliminate this perverse incentive. One is to eliminate or compensate for the differential in payment between scheduled and ED admissions that relates to differences in both payer mix and severity of illness. Another approach is to provide hospitals with direct financial rewards or penalties based on their management of patient throughput. CMS, through its purchaser and regulatory power, has the ability to drive hospitals to address and manage patient flow and ensure timely access to quality care for its clients. All payers, including Medicare, Medicaid, and private insurers, could also develop contracts that would penalize hospitals for chronic delays in treatment, crowding, and diversion. CMS should lead the way in the development of innovative payment approaches that would accomplish these objectives. All payers should be encouraged to do the same.
Adapting the Legal and Regulatory Framework
The way hospitals and EMS agencies deliver emergency care is shaped largely by federal laws, including the Emergency Medical Treatment and Active Labor Act (EMTALA) and the Health Insurance Portability and Accountability Act (HIPAA). The application of these laws to the actual provision of care is guided by regulatory rules and advisories, enforcement decisions, and court decisions, as well as by providers’ understanding of these.
EMTALA was passed in 1986 to prevent hospitals from refusing to serve uninsured patients and “dumping” them on other hospitals. The act established a mandate for hospitals and physicians who provide emergency and trauma care to provide a medical screening exam to all patients and properly stabilize patients or transfer them to an appropriate facility if an emergency medical condition exists (GAO, 2001). This requirement applies regardless of patients’ ability to pay.
EMTALA also has implications for the regional coordination of care. The act was written to provide individual patient protections—it focuses on the obligations of an individual hospital to an individual patient (Rosenbaum and Kamoie, 2003). The statute is not clearly adaptable to a highly integrated regional emergency care system in which the optimal care of patients may diverge from conventional patterns of emergency treatment and transport.
Until recently, EMTALA appeared to hinder the regional coordination of services in several ways—for example, requiring a hospital-owned ambulance to transport a patient to the parent hospital even if it was not the
optimal destination for that patient, requiring a hospital to interrupt the transfer to administer a medical screening exam for a patient being transferred from ground transport to helicopter if the hospital’s helipad was used, and limiting the ability of hospitals to direct nonemergent patients who entered the ED to an appropriate and readily available ambulatory care setting. Interim guidance published by CMS in 2003 appeared to mitigate these problems (CMS, 2003). It established, for example, that a patient visiting an off-campus hospital site that does not normally provide emergency care does not create an EMTALA obligation, that a hospital-owned ambulance need not return the patient to the parent hospital if it is operating under the authority of a communitywide EMS protocol, and that hospitals are not obligated to provide treatment for clearly nonemergency situations as determined by qualified medical personnel. Further, hospitals involved in disasters need not adhere strictly to EMTALA if operating under a community disaster plan. Despite these changes, however, uncertainty surrounding the interpretation and enforcement of EMTALA remains a damper on the development of coordinated, integrated emergency care systems.
In 2005, CMS convened a technical advisory group to study EMTALA and address additional needed changes (CMS 2005a,b,c). To date, the advisory group has focused on incremental modifications to the act. While the recent CMS guidance and deliberations of the EMTALA advisory group are positive steps, the committee envisions a more fundamental rethinking of EMTALA that would support and facilitate the development of regionalized emergency systems, rather than simply addressing each obstacle on a piecemeal basis. The new EMTALA would continue to protect patients from discrimination in treatment while enabling and encouraging communities to test innovations in the design of emergency care systems, such as direct transport of patients to non–acute care facilities—dialysis centers and ambulatory care clinics, for example—when appropriate.
HIPAA was enacted to facilitate electronic transmission of data between providers and payers while protecting the privacy of patient health information. In protecting patient confidentiality, HIPAA can present certain challenges for providers, such as making it more complicated for a physician to send information about a patient to another physician for a consultation. Regional coordination is based on the seamless delivery of care across multiple provider settings. Patient-level information must flow freely between these settings—from dispatch to emergency response to hospital care—to ensure that appropriate information will be available for clinical decision making and coordination of services. Current interpretations of HIPAA would make it difficult to achieve the required degree of information fluidity. Additionally, HIPAA can be a barrier to family-centered care by limiting access to information to parents or legally identified caregivers of children.
Both EMTALA and HIPAA protect patients from potential abuses and
serve invaluable purposes. As they are written and interpreted, however, compliance with these statutes can be difficult and costly for providers. More important, the acts are likely to impede the development of regional systems. The committee believes appropriate modifications could be made to both acts that would preserve their original purpose while reducing their adverse impact on the development of regional systems. The committee recommends that the Department of Health and Human Services adopt rule changes to the Emergency Medical Treatment and Active Labor Act and the Health Insurance Portability and Accountability Act so that the original goals of the laws are preserved, but integrated systems may further develop (3.5).
Coordinating Federal Leadership in Emergency Care
The committee’s vision of a coordinated, regionalized, and accountable emergency and trauma care system for adults and children is impeded by the structure of federal programs that currently support emergency and trauma care. To function effectively, the components of the emergency and trauma care system must be highly integrated. Operationally, this means that all of the key players in a given region—hospital emergency and trauma departments, EMS dispatchers, state public health officials, trauma surgeons, EMS agencies, ED nurses, hospital administrators, firefighters, police, community safety net providers, and others—must work together to make decisions, deploy resources, and monitor and adjust system operations based on performance feedback.
As documented in this report, however, fragmentation, silos, and entrenched interests prevail throughout emergency and trauma care. The organization of federal government programs that support and regulate emergency and trauma care services largely reflects the fragmentation of emergency and trauma care services at the local level. Responsibility for emergency and trauma care is widely dispersed among multiple federal agencies within DHHS, the U.S. Department of Transportation (DOT), and DHS. This situation reflects the history and inherent nature of emergency and trauma care—essential public services that operate at the intersection of medical care, public health, and public safety (police, fire departments, and emergency management agencies).
In the 1960s, the mounting toll of highway deaths led NHTSA to become the first government home for EMS, where it has remained. Thus although EMS is primarily a medical discipline, federal responsibility for EMS rests with DOT. This responsibility was recently reinforced by the elevation of NHTSA’s EMS program to the status of the Office of EMS within the agency. Today, NHTSA sponsors a number of workforce and research initiatives and the development of the National EMS Information System,
and it recently received funding for a major nationwide initiative to promote the development of next-generation 9-1-1 service.
DHHS has played an important supporting role in the development of EMS and has taken the lead role with respect to hospital-based emergency and trauma care. It housed the Division of Emergency Medical Services and the Division of Trauma and EMS for many years, and most recently the Trauma-EMS Systems Program. All of these programs have been eliminated; the latter was recently zeroed out of the federal budget for fiscal year 2006. DHHS continues to support CDC’s National Center for Injury Prevention and Control, the EMS-C program, and the National Bioterrorism Hospital Preparedness program. These programs have made important contributions to emergency and trauma care despite inconsistent funding and the frequent threat of elimination. The Agency for Healthcare Research and Quality (AHRQ), another DHHS agency, has historically been the principal federal agency funding research in emergency care delivery, including much of the early research on management of out-of-hospital cardiac arrest. Recently, AHRQ has funded important studies of ED crowding, operations management, and patient safety issues. It is active as well in funding research on preparedness, bioterrorism planning, and response.
DHS also plays an important role in emergency and trauma care. The Federal Emergency Management Agency (FEMA), once an independent cabinet-level agency now housed in DHS, provides limited amounts of grant funding to local EMS agencies through the U.S. Fire Administration. DHS also houses the Metropolitan Medical Response System (MMRS), a grant program designed to enhance emergency and trauma preparedness in major population centers. This program was migrated from DHHS to DHS in 2003. In addition, DHS houses the Disaster Medical Assistance Team (DMAT) program, through which health professionals volunteer and train as locally organized units so they can be deployed rapidly, under federal direction, in response to disasters nationwide. However, this program will migrate to DHHS in January 2007.
Efforts have been made to improve interagency collaboration at the federal level, especially in recent years. Over the last decade, federal agencies have worked collaboratively to provide leadership in the emergency and trauma care field, to minimize gaps and overlaps across programs, and to pool resources to jointly fund promising research and demonstration programs. For example, NHTSA and HRSA jointly supported the development of the Emergency Medical Services Agenda for the Future, which was published in 1996. This degree of collaboration has not been universal, however, and has been evident in some agencies more than others. Furthermore, collaborative efforts are limited by the constraints of agency authorization and funding. At some point, agencies must pursue their own programmatic goals at the expense of joint initiatives. Furthermore, to the
degree that successful collaboration has occurred, it has generally depended on the good will of key individuals in positions of leadership, limiting the sustainability of these efforts when personnel changes occur.
In an effort to enhance the sustainability of collaborative initiatives, a number of agencies have participated in informal planning groups. For example, the Interagency Committee on Emergency Medical Services for Children Research (ICER), which is sponsored by HRSA, brings together representatives from a number of federal programs for the purposes of sharing information and improving research in emergency and trauma care for children.
A broader initiative is the Federal Interagency Committee on EMS (FICEMS), a planning group designed to coordinate the efforts of the various federal agencies involved in emergency and trauma care. FICEMS was established in the late 1970s. After a subsequent period of dormancy, it was reconstituted in the mid-1980s. The organization had no statutory authority until 2005, when it was given formal status by the Safe, Accountable, Flexible, Efficient Transportation Equity Act: A Legacy for Users (SAFETEA-LU), DOT’s reauthorization legislation. While the focus of FICEMS is EMS, the group has in practice reached beyond the strict boundaries of prehospital care to facilitate coordination and collaboration with agencies involved in other aspects of hospital-based emergency and trauma care (see Box 3-2). NHTSA is charged with providing administrative support for FICEMS, which must submit a report to Congress annually. The central aims of the group are as follows:
-
To ensure coordination among the federal agencies involved with state, local, or regional EMS and 9-1-1 systems.
-
To identify state, local, or regional needs in EMS and 9-1-1 services.
-
To recommend new or expanded programs, including grant programs, for improving state, local, or regional EMS and implementing improved EMS communications technologies, including wireless 9-1-1.
-
To identify ways of streamlining the process through which federal agencies support state, local, or regional EMS.
-
To assist state, local, or regional EMS in setting priorities based on identified needs.
-
To advise, consult, and make recommendations on matters relating to the implementation of coordinated state EMS programs.
Problems with the Current Structure
Despite recent efforts at improved federal collaboration, there is widespread agreement that the various components of emergency care (EMS for
|
BOX 3-2 FICEMS Membership The 2005 Safe, Accountable, Flexible, Efficient Transportation Equity Act: A Legacy for Users designated the following agencies as members of FICEMS. Each year, members elect a representative from one of these member organizations as the FICEMS chairperson.
|
adults and children, trauma care, hospital-based care) individually have not received sufficient attention, stature, and funding within the federal government. The scattered nature of federal responsibility for emergency care limits the visibility necessary to secure and maintain federal funding. The result has been marked fluctuations in budgetary support and the constant risk that key programs will be dramatically downsized or eliminated. The lack of a clear point of contact for the public and for stakeholders makes it difficult to build a unified constituent base that can advocate effectively for funding and provide feedback to the government on system performance. The lack of a unified budget has created overlaps, gaps, and idiosyncratic funding of various programs (for example, separate hospital surge capacity initiatives are currently taking place in AHRQ, CDC, HRSA, and DHS).
Finally, the lack of unified accountability disperses responsibility for system failures and perpetuates divisions between public safety and medical-based emergency and trauma care professionals. The degree to which the scattered responsibility for emergency and trauma care at the federal level has contributed to this disappointing performance is unclear. Regardless, the committee believes a new approach is warranted.
Alternative Approaches
Strong federal leadership for emergency and trauma care is at the heart of the committee’s vision for the future, and continued fragmentation of responsibility at the federal level is unacceptable. The committee considered two options for remedying the situation: (1) maintain the status quo, giving the FICEMS approach time to strengthen and mature, or (2) designate or create a new lead agency within the federal government for emergency and trauma care. Some of the key differences between these two approaches are summarized in Table 3-1.
Option 1: Maintain the status quo and allow FICEMS to strengthen The committee considered the ramifications of maintaining the status quo. The problems associated with fragmented federal leadership of emergency care, documented above, include variable funding, periodic program cuts, programmatic duplication, and critical program gaps. With the recent enactment of a statutory framework for FICEMS, however, the committee considered the possibility that the need for a lead federal agency has diminished. The committee carefully examined the rationale for delaying the move toward a lead federal agency and allowing FICEMS time to gain strength. The central argument in support of this strategy is that there have been a number of recent improvements in collaboration at the federal level, and these efforts should be given a chance to work before an unproven and politically risky approach is pursued. Several recent developments support this view: the enactment of a statutory framework for FICEMS; the increasing level of collaboration among some federal agencies; the substantial new NHTSA funding for a next-generation 9-1-1 initiative; and the elevation of the NHTSA EMS program to the Office of EMS, which has the potential to improve visibility and funding for EMS, and perhaps other aspects of emergency and trauma care, within the federal government.
While the committee applauds these positive developments, setbacks have occurred as well. As noted above, DHHS’s Division of Emergency Medical Services, its Division of Trauma and EMS, and most recently its Trauma-EMS Systems Program were recently zeroed out of the federal budget. Federal funding for AHRQ, nonbioterrorism programs at CDC, and other federal programs related to emergency and trauma care at the
TABLE 3-1 Comparison of the Current FICEMS Approach and the Committee’s Lead Agency Proposal
|
|
Maintain the Status Quo, Allowing FICEMS to Gain Strength |
Designate or Create a New Lead Agency |
|
Description |
|
|
|
Authority |
|
|
|
Funding |
|
|
|
Collaboration |
|
|
|
Public Identity |
|
|
|
Professional Identity |
|
|
|
|
Maintain the Status Quo, Allowing FICEMS to Gain Strength |
Designate or Create a New Lead Agency |
|
Efficiency |
|
|
|
Transition |
|
|
federal level have been cut. These developments suggest that a fragmented organizational structure at the federal level would significantly hinder the creation of a coordinated, regionalized, accountable emergency and trauma care system. FICEMS can be a valuable body, but it is a poor substitute for formal agency consolidation. FICEMS is expressly focused on EMS, and ultimately has limited power over even this sphere. It is not a federal agency and therefore cannot regulate, spend, or withhold funding. It cannot even hold its own member agencies accountable for their actions—or lack of action.
Option 2: Designate or create a new federal lead agency The possibility of a lead agency for emergency and trauma care has been discussed for years and was highlighted in the 1996 report Emergency Medical Services Agenda for the Future. While the concept of a lead agency promoted in that report was focused on prehospital EMS, the committee believes a lead agency should encompass all components involved in the provision of emergency and trauma care. This federal lead agency would unify federal policy development related to emergency and trauma care, provide a central point of contact for the various constituencies in the field, serve as a federal advocate
for emergency and trauma care within the government, and coordinate grants so that federal dollars would be allocated efficiently and effectively.
A lead federal agency could better move the emergency and trauma care system toward improved integration; unify funding and other decisions; and represent all emergency and trauma care patients, providers, and settings, including prehospital EMS (both ground and air), hospital-based emergency and trauma care, pediatric emergency and trauma care, rural emergency and trauma care, and medical disaster preparedness. Specifically, a federal lead agency could:
-
Provide federal leadership on important policy issues that cut cross agency boundaries.
-
Create unified accountability for the performance of the emergency and trauma care system.
-
Rationalize funding across the various aspects of emergency and trauma care to optimize the allocation of resources in achieving system outcomes.
-
Coordinate programs to eliminate overlaps and gaps in current and future funding.
-
Create a large combined federal presence, increasing the visibility of emergency and trauma care within the government and among the public.
-
Provide a recognizable entity that would serve as a single point of contact for stakeholders and the public, resulting in consolidated and efficient data collection and dissemination and coordinated program information.
-
Enhance the professional identity and stature of emergency and trauma care practitioners.
-
Bring together multiple professional groups and cultures, creating cross-cultural and interdisciplinary interaction and collaboration that would model and reinforce the integration of services envisioned by the committee.
Although creating a lead agency could yield many benefits, such a move would also involve significant challenges. Numerous questions must be addressed regarding the location of such an agency in the federal government, its structure and functions, and the possible risk of weakening or losing current programs. HRSA’s rural EMS and EMS-Trauma System programs have already been defunded, and the EMS-C program is under the constant threat of elimination. There is real concern that proposing an expensive and uncertain agency consolidation could jeopardize programs already at risk, such as EMS-C, as well as cripple new programs just getting started, such as NHTSA’s enhanced 9-1-1 program. This is particularly likely if there is resistance to the consolidation from within the current agency homes for these programs.
A related concern is that the priority currently given to certain programs could shift, resulting in less support for existing programs. EMS advocates have expressed concern that hospital-based emergency and trauma care issues would dominate the agenda of a new unified agency. The pediatric community is worried about getting lost in a new agency, and has fought hard to establish and maintain strong categorical programs supported by historically steady funding streams. There is concern that under the proposed structure, the current focus of the EMS-C program could get lost or diminished or simply lose visibility in the multitude of programs addressed by the new agency.
There is also the potential for administrative and funding disruptions. Combining similar agencies, particularly those that reside within the same department, may be straightforward. But combining agencies with different missions across departments with different cultures may prove highly difficult. The problems experienced during the consolidation of programs in DHS increase anxiety about this proposal.
Another concern is that removing medical-related functions from DHS and DOT could exacerbate rather than reduce fragmentation. Operationally, nearly half of EMS services are fire department–based. Thus, there is concern that separating EMS and fire responsibilities at the federal level could splinter rather than strengthen relationships.
The Committee’s Recommendation
Despite the concerns outlined above, the committee believes the potential benefits of consolidation outweigh the potential risks. A lead federal agency is required to fully realize the committee’s vision of a coordinated, regionalized, and accountable emergency and trauma care system. The committee recognizes that a number of challenges are associated with the establishment of a new lead agency, though it believes these concerns can be mitigated through appropriate planning. The committee therefore recommends that Congress establish a lead agency for emergency and trauma care within 2 years of the release of this report. The lead agency should be housed in the Department of Health and Human Services, and should have primary programmatic responsibility for the full continuum of emergency medical services and emergency and trauma care for adults and children, including medical 9-1-1 and emergency medical dispatch, prehospital emergency medical services (both ground and air), hospital-based emergency and trauma care, and medical-related disaster preparedness. Congress should establish a working group to make recommendations regarding the structure, funding, and responsibilities of the new agency, and develop and monitor the transition. The working group should have representation from federal and state agencies and professional disciplines involved in emergency care (3.6).
Objectives of the lead agency The lead agency’s mission would be to enhance the performance of the emergency and trauma care system as a whole, as well as to improve the performance of the various components of the system, such as prehospital EMS, hospital-based emergency care, trauma systems, pediatric emergency and trauma care, prevention, rural emergency and trauma care, and disaster preparedness. The lead agency would set the overall direction for emergency and trauma care planning and funding; would be the primary collector and repository of data in the field; and would be the key source of information about emergency and trauma care for the public, the federal government, and practitioners themselves. It would be responsible for allocating federal resources across all of emergency and trauma care to achieve systemwide goals, and should be held accountable for the performance of the system and its components.
Location of the lead agency The lead agency would be housed within DHHS. The committee considered many factors in selecting DHHS over DOT and DHS. The factor that drove this decision above all others was the need to unify emergency and trauma care within a medical care/public health framework. Emergency and trauma care is by its very nature involved in multiple arenas—medical care, public safety, public health, and emergency management. The multiple identities that result from this multifaceted involvement reinforce the fragmentation that is endemic to the emergency and trauma care system. For too long, the gulf between EMS and hospital care has hindered efforts at communication, continuity of care, patient safety and quality of care, data collection and sharing, collaborative research, performance measurement, and accountability. It will be difficult for emergency and trauma care to achieve seamless and high-quality performance across the system until the entire system is organized within a medical care/public health framework while also retaining its operational linkages with public safety and emergency management.
Only DHHS, as the department responsible for medical care and public health in the United States, can encompass all of these functions effectively. Although DOT has played an important role in both EMS and acute trauma care and has collaborated effectively with other agencies, its EMS and highway safety focus is too narrow to represent all of emergency and trauma care. DHS houses the Fire Service, which is closely allied with EMS, particularly at the field operations level. But the focus of DHS on disaster preparedness and bioterrorism is also too narrow to encompass the broad scope of emergency and trauma care.
Because emergency and trauma care functions would be consolidated in a department oriented toward medical care and public health, there is a risk that public safety and emergency management components could re-
ceive less attention, stature, or funding. Therefore, it is imperative that the mission of the new agency be understood and clearly established by statute so that the public safety and emergency management aspects of emergency and trauma care will not be neglected.
Programs included in the lead agency The committee envisions that the lead agency would have primary programmatic responsibility for the full continuum of EMS; emergency and trauma care for adults and children, including medical 9-1-1 and emergency medical dispatch; prehospital EMS (both ground and air); hospital-based emergency and trauma care; and medical-related disaster preparedness. The agency’s focus would be on program development and strategic funding to improve the delivery of emergency and trauma care nationwide. It would not be primarily a research funding agency, with the exception of a few of the existing grant programs mentioned above. Funding for basic, clinical, and health services research in emergency and trauma care would remain the primary responsibility of existing research agencies, including the National Institutes of Health (NIH), AHRQ, and CDC. Because of the limited research focus of the lead agency, it would be imperative for existing research agencies, NIH in particular, to work closely with the new agency and strengthen their commitment to emergency and trauma care research. On the other hand, it may be appropriate to keep certain clinical and health services research initiatives with the programs in which they are housed, and therefore bring them into the new agency. For example, responsibility for funding the infrastructure for the Pediatric Emergency Care Applied Research Network (PECARN) would be moved into the new agency along with the rest of the EMS-C program.
In addition to existing functions, the lead agency would become the home for future programs related to emergency and trauma care, including new programs that would be dedicated to the development of inclusive systems of emergency and trauma care.
Working group While the committee envisions consolidation of most of the emergency care–related functions currently residing in other agencies and departments, it recognizes that many complex issues are involved in determining which programs should be combined and which left in their current agency homes. A deliberate process should be established to determine the exact composition of the new agency and to coordinate an effective transition. For these reasons, the committee is recommending the establishment of an independent working group to make recommendations regarding the structure, funding, and responsibilities of the new agency, and to coordinate and monitor the transition process. The working group should include representatives from federal and state agencies and profes-
sional disciplines involved in emergency care. The committee considered whether FICEMS would be an appropriate entity to assume this advisory and oversight role and concluded that, as currently constituted, it lacks the scope and independence to carry out this role effectively.
Role of FICEMS FICEMS is a highly promising entity that is complementary to the proposed new lead agency. FICEMS would play a vital role during the proposed interim 2-year period by continuing to enhance coordination and collaboration among agencies and providing a forum for public input. In addition, it could play an important advisory role to the independent working group. Once the lead agency had been established, FICEMS would continue to coordinate work between the lead agency and other agencies, such as NIH, CMS, and DoD, that would remain closely involved in various emergency and trauma care issues.
Structure of the lead agency While the principle of integration across the multiple components of emergency and trauma care should drive the structure, operation, and funding of the new lead agency, the committee envisions distinct program offices to provide focused attention and programmatic funding for key areas, such as the following:
-
Prehospital EMS, including 9-1-1, dispatch, and both ground and air medical services
-
Hospital-based emergency and trauma care
-
Trauma systems
-
Pediatric emergency and trauma care
-
Rural emergency and trauma care
-
Disaster preparedness
To ensure that current programs would not lose visibility and stature within the new agency, it would be critical for each program office to have equal status and reporting relationships within the agency’s organizational structure. The committee lacks the expertise to specify the organizational structure in further detail. Rather, it envisions a national dialogue over the coming year—coordinated by the proposed independent working group, aided by input from FICEMS, and with the involvement of the Office of Management and Budget and congressional committees with jurisdiction—to implement the committee’s recommendation.
Funding for the lead agency Existing programs transferring to the new agency would bring with them their full current and projected funding. Congress should also establish additional funding to cover the costs associ-
ated with the transition to and the new administrative overhead associated with the lead agency. In addition, Congress should add new funding for the offices of hospital-based emergency and trauma care, rural emergency and trauma care, and trauma systems. In light of the pressing challenges confronting emergency care providers and the American public, this would be money well spent. While the committee is not qualified to estimate the costs associated with establishing a unified lead agency, it recognizes that these costs would be substantial. At the same time, however, the committee believes that substantial cost savings would result from reduced duplication and lower overhead. New funding that flowed into the agency would result in new programming, rather than an increase in existing overhead.
Mitigation of concerns regarding the establishment of a lead federal agency The committee recognizes that transitioning to a single lead agency would be a difficult challenge under any circumstances, but would be especially difficult for an emergency and trauma care system that is already under duress from funding cutbacks, elimination of programs, growing public demand on the system, and pressure to enhance disaster preparedness. During this critical period, it is imperative that support for emergency and trauma care programs already in place in the various federal agencies be sustained. In particular, the Office of EMS within NHTSA has ongoing programs that are critical to the EMS system. Similarly, existing emergency care–related federal programs, such as those in HRSA’s EMS-C program and Office of Rural Health Policy and at CDC, should be supported during the transition period. If the committee’s proposal is to be successful, the constituencies associated with established programs must not perceive that they are being politically weakened during the transition.
The committee believes the proposed consolidation of agencies would enhance support for emergency and trauma care across the board, benefiting all current programs. But it also believes avoiding disruptions that could adversely affect established programs is critically important. Therefore, the committee considers it imperative for legislation creating the new agency to protect current levels of funding and visibility for existing programs. The new agency should balance its funding priorities by adding to current funding levels, not by diverting funds away from existing programs.
The committee acknowledges the concern that removing medical-related emergency and trauma functions from DHS and DOT would create additional fragmentation. The committee believes the public safety aspects of emergency and trauma care must continue to be addressed as a core element of the emergency and trauma care system. But the primary focus of the system must be medical care and public health if the recognition, stature, and outcomes that are critical to the system’s success are to be achieved.
THE EMERGENCY MEDICAL SERVICES FOR CHILDREN PROGRAM
It is the committee’s hope and expectation that in the future, existing deficiencies in pediatric emergency care will be eliminated, and providers will be equally prepared for the care of both children and adults. However, the work of the EMS-C program today remains relevant and vital.
In the chapters that follow, the committee outlines a number of recommendations for improving pediatric emergency care. Implementing these recommendations will require the leadership of a well-recognized, well-respected entity not just within pediatrics, but within the broader emergency care system. The EMS-C program, with its long history of working with federal partners, state policy makers, researchers, providers, and professional organizations across the spectrum of emergency care, is in the best position to assume this leadership role. The committee recommends that Congress appropriate $37.5 million per year for the next 5 years to the Emergency Medical Services for Children program (3.7).
The committee is not suggesting that the EMS-C program should assume full responsibility for funding the implementation of the recommendations presented in this report; rather, the program should serve as a facilitator to initiate the implementation process. For example, the EMS-C program could convene national conferences involving individuals with multidisciplinary expertise to address how the committee’s various recommendations should be implemented. However, additional funding will be needed to ensure that the program has the capacity to initiate these efforts. An additional $500,000 should be allocated to the program’s budget to sponsor four to five national conferences per year.
The program’s budget should also be expanded to accommodate an increase in the award size for the State Partnership Grants. In fiscal year 2005, EMS agencies (or a designated alternative) in 54 U.S. states and territories received grant support from the program to institutionalize pediatric EMS improvements. In many states, however, the award from the EMS-C program ($100,000 to $115,000) represents the state’s largest or only investment in pediatric emergency care. After covering salary and overhead for a staff person, the current size of the grant leaves little to be spent on programmatic initiatives. An additional $8 million per year is needed to increase the annual award amount to $250,000 per state/territory. This additional funding would better enable a state representative to initiate improvements, which could include organizing pediatric disaster drills, increasing the level of available pediatric emergency care training, participating in and organizing statewide pediatric emergency care planning, and meeting with provider organizations to encourage and facilitate improvements in pediatric preparedness.
The EMS-C program also provides financial support for the infrastructure of PECARN through its network demonstration cooperative agreements. The importance of PECARN cannot be overstated. While it remains small in size, it is perhaps the best resource for conducting multicenter randomized trials in pediatric emergency care. As the network is currently organized, however, its linkages to prehospital providers are limited, thereby constraining the ability of researchers to conduct analyses across the continuum of care. Additional funding is needed to build a sustainable link between the four research nodes of PECARN and the prehospital providers in those nodes. EMS-C program funding should be increased to provide each research node $1 million per year to establish data linkages with local prehospital providers, for a total cost of $4 million per year. Looking to the future of PECARN, its administrators should also explore the possibility of integrating more general hospitals into the network and expanding research nodes in the south and southeast to improve the network’s geographic reach.
Finally, the program is in need of additional funding that could be directed toward special initiatives or one-time projects addressing important needs. For example, the program is currently funding two projects for the development of clinical practice guidelines ($250,000 per year for 3 years for each project). Justification for expanding this initiative is provided in Chapter 4, where the committee calls for the development, evaluation, and updating of pediatric clinical practice guidelines. An additional $5 million per year would allow the EMS-C program to support approximately 18 similar large projects. Examples of other types of special projects that could be supported with this funding are the development of pediatric dosing guidelines for certain medications and the development of labeling techniques to reduce medication errors.
The 5-year timeframe is suggested so that the program will have the capacity to address the deficiencies in the pediatric emergency care system quickly. The program should focus on creating sustainable activities and strive to integrate pediatrics into emergency care planning at the federal, state, and local levels. The proposed 5-year period is not intended as a limit on federal funding dedicated to improving pediatric emergency care; indeed, there will always be a need to monitor and study emergency care for children. However, the committee’s expectation is that the various elements of emergency care leadership at the federal level will be better integrated and consolidated in the future (as discussed above). Support for pediatric emergency care will always remain a vital aspect of that federal leadership, but it may not be in the form of a separate program. After 5 years, it will be necessary to reexamine how best to identify and fund pediatric emergency care objectives at the federal level, as well as to reevaluate future funding levels for the EMS-C program.
SUMMARY OF RECOMMENDATIONS
3.1 The Department of Health and Human Services and the National Highway Traffic Safety Administration, in partnership with professional organizations, should convene a panel of individuals with multidisciplinary expertise to develop evidence-based categorization systems for emergency medical services, emergency departments, and trauma centers based on adult and pediatric service capabilities.
3.2 The National Highway Traffic Safety Administration, in partnership with professional organizations, should convene a panel of individuals with multidisciplinary expertise to develop evidence-based model prehospital care protocols for the treatment, triage, and transport of patients, including children.
3.3 The Department of Health and Human Services should convene a panel of individuals with emergency and trauma care expertise to develop evidence-based indicators of emergency and trauma care system performance, including the performance of pediatric emergency care.
3.4 Congress should establish a demonstration program, administered by the Health Resources and Services Administration, to promote coordinated, regionalized, and accountable emergency care systems throughout the country, and appropriate $88 million over 5 years to this program.
3.5 The Department of Health and Human Services should adopt rule changes to the Emergency Medical Treatment and Active Labor Act and the Health Insurance Portability and Accountability Act so that the original goals of the laws are preserved, but integrated systems may further develop.
3.6 Congress should establish a lead agency for emergency and trauma care within 2 years of the release of this report. The lead agency should be housed in the Department of Health and Human Services, and should have primary programmatic responsibility for the full continuum of emergency medical services and emergency and trauma care for adults and children, including medical 9-1-1 and emergency medical dispatch, prehospital emergency medical services (both ground and air), hospital-based emergency and trauma care, and medical-related disaster preparedness. Congress should establish a working group to make recommendations re-
garding the structure, funding, and responsibilities of the new agency, and develop and monitor the transition. The working group should have representation from federal and state agencies and professional disciplines involved in emergency and trauma care.
3.7 Congress should appropriate $37.5 million per year for the next 5 years to the Emergency Medical Services for Children program.
REFERENCES
Adomako SA, Melese-d’Hospital I. 2004. State-by-State Profiles: The Integration of Pediatric Care Components into the EMS System. Rockville, MD: MCHB, NHTSA, HRSA.
Bardach NS, Olson SJ, Elkins JS, Smith WS, Lawton MT, Johnston SC. 2004. Regionalization of treatment for subarachnoid hemorrhage: A cost-utility analysis. Circulation 109(18):2207–2212.
Berenson RA, Kuo S, May JH. 2003. Medical malpractice liability crisis meets markets: Stress in unexpected places. Issue Brief (Center for Studying Health System Change) 68:1–7.
Bode MM, O’Shea TM, Metzguer KR, Stiles AD. 2001. Perinatal regionalization and neonatal mortality in North Carolina, 1968–1994. American Journal of Obstetrics and Gynecology 184(6):1302–1307.
Bravata D, McKonald K, Owens D, Wilhelm ER, Brandeau ML, Zaric GS, Holty JC, Sundaram V. 2004. Regionalization of Bioterrorism Preparedness and Response. Rockville, MD: AHRQ.
Chang RK, Klitzner TS. 2002. Can regionalization decrease the number of deaths for children who undergo cardiac surgery? A theoretical analysis. Pediatrics 109(2):173–181.
Chiara O, Cimbanassi S. 2003. Organized trauma care: Does volume matter and do trauma centers save lives? Current Opinion in Critical Care 9(6):510–514.
Cifuentes J, Bronstein J, Phibbs CS, Phibbs RH, Schmitt SK, Carlo WA. 2002. Mortality in low birth weight infants according to level of neonatal care at hospital of birth. Pediatrics 109(5):745–751.
CMS (Centers for Medicare and Medicaid Services). 2003. Emergency Medical Treatment and Active Labor Act (EMTALA) Interim Guidance. Letter to State Survey Agency Directors. Ref: S&C-04-10.
CMS. 2005a. Report Number One to the Secretary, U.S. Department of Health and Human Services, from the Inaugural Meeting of the Emergency Medical Treatment and Labor Act Technical Advisory Group. Washington, DC: CMS.
CMS. 2005b. Report Number Two to the Secretary, U.S. Department of Health and Human Services, from the Emergency Medical Treatment and Labor Act Technical Advisory Group. Washington, DC: CMS.
CMS. 2005c. Report Number Three to the Secretary, U.S. Department of Health and Human Services, from the Emergency Medical Treatment and Labor Act Technical Advisory Group. Washington, DC: CMS.
CMS. 2005d. Hospital Compare. [Online]. Available: http://www.hospitalcompare.hhs.gov/hospital/home2.asp [accessed November 23, 2005].
CMS. 2005e. Medicare Spotlights. [Online]. Available: http://www.medicare.gov [accessed November 22, 2005].
Committee on Pediatric Emergency Medicine Pediatric Section and Task Force on Regionalization of Pediatric Critical Care. 2000. Consensus report for regionalization of services for critically ill or injured children. Pediatrics 105(1):152–155.
Cooper A, Barlow B, DiScala C, String D, Ray K, Mottley L. 1993. Efficacy of pediatric trauma care: Results of a population-based study. Journal of Pediatric Surgery 28(3):299–303; discussion 304–305.
Cunningham P, May J. 2003. Insured Americans drive surge in emergency department visits. Issue Brief (Center for Studying Health System Change) 70:1–6.
Davis R. 2003, July. The method: Measure how many victims leave the hospital alive. USA Today. P. A1.
Densmore JC, Lim HJ, Oldham KT, Guice KS. 2006. Outcomes and delivery of care in pediatric injury. Journal of Pediatric Surgery 41(1):92–98; discussion 92–98.
EMS Performance Measures Project. 2005. Performance Measures in EMS. [Online]. Available: http://www.measureems.org/performancemeasures2.htm [accessed January 5, 2006].
GAO (General Accounting Office). 2001. Emergency Care. EMTALA Implementation and Enforcement Issues. Washington, DC: GAO.
GAO. 2003. Infectious Diseases: Gaps Remain in Surveillance Capabilities of State and Local Agencies. Washington, DC: GAO.
Gausche-Hill M, Wiebe R. 2001. Guidelines for preparedness of emergency departments that care for children: A call to action. Pediatrics 107(4):773–774.
Gausche-Hill M, Lewis R, Schmitz C. 2004. Survey of US Emergency Departments for Pediatric Preparedness: Implementation and Evaluation of Care of Children in the Emergency Department: Guidelines for Preparedness. Unpublished results.
Glance LG, Osler TM, Dick A, Mukamel D. 2004. The relation between trauma center outcome and volume in the national trauma databank. Journal of Trauma-Injury Infection & Critical Care 56(3):682–690.
Grumbach K, Keane D, Bindman A. 1993. Primary care and public emergency department overcrowding. American Journal of Public Health 83(3):372–378.
Grumbach K, Anderson GM, Luft HS, Roos LL, Brook R. 1995. Regionalization of cardiac surgery in the United States and Canada. Geographic access, choice, and outcomes. Journal of the American Medical Association 274(16):1282–1288.
Harris Interactive. 2004. Trauma Care: Public’s Knowledge and Perception of Importance. Rochester, NY: The Coalition for American Trauma Care.
Health Level 7. 2005. Emergency Care Special Interest Group. [Online]. Available: http://www.hl7.org/Special/committees/emergencycare/index.cfm [accessed November 30, 2005].
Holloway MY. 2001. The Regionalized Perinatal Care Program. Princeton, NJ: The Robert Wood Johnson Foundation.
Hulka F. 1999. Pediatric trauma systems: Critical distinctions. The Journal of Trauma 47(Suppl. 3):S85–S89.
Hulka F, Mullins RJ, Mann NC, Hedges JR, Rowland D, Worrall WH, Sandoval RD, Zechnich A, Trunkey DD. 1997. Influence of a statewide trauma system on pediatric hospitalization and outcome. The Journal of Trauma 42(3):514–519.
Imperato PJ, Nenner RP, Starr HA, Will TO, Rosenberg CR, Dearie MB. 1996. The effects of regionalization on clinical outcomes for a high risk surgical procedure: A study of the whipple procedure in New York state. American Journal of Medical Quality 11(4):193–197.
IOM (Institute of Medicine). 1993. Emergency Medical Services for Children. Washington, DC: National Academy Press.
IOM. 2002. Fostering Rapid Advances in Health Care: Learning from System Demonstrations. Washington, DC: National Academy Press.
Jones J. 2004. Neonatal nursing: The first six weeks. Critical Care Nursing (Suppl.):6–8.
Jurkovich GJ, Mock C. 1999. Systematic review of trauma system effectiveness based on registry comparisons. Journal of Trauma-Injury Infection & Critical Care 47(Suppl. 3): S46–S55.
Kanter RM, Heskett M. 2002. Washington Hospital Center (B): The Power of Insight. Watertown, MA: Harvard Business School Publishing.
Koziol-McLain J, Price DW, Weiss B, Quinn AA, Honigman B. 2000. Seeking care for nonurgent medical conditions in the emergency department: Through the eyes of the patient. Journal of Emergency Nursing 26(6):554–563.
Lewin ME, Altman S. 2000. America’s Health Care Safety Net. Washington DC: National Academy Press.
Lindsay P, Schull M, Bronskill S, Anderson G. 2002. The development of indicators to measure the quality of clinical care in emergency departments following a modified-delphi approach. Academic Emergency Medicine 9(11):1131–1139.
MacKenzie EJ. 1999. Review of evidence regarding trauma system effectiveness resulting from panel studies. Journal of Trauma-Injury Infection & Critical Care 47(Suppl. 3): S34–S41.
MacKenzie EJ, Rivara FP, Jurkovich GJ, Nathens AB, Frey KP, Egleston BL, Salkever DS, Scharfstein DO. 2006. A national evaluation of the effect of trauma-center care on mortality. New England Journal of Medicine 354(4):366–378.
Malone RE. 1995. Heavy users of emergency services: Social construction of a policy problem. Social Science Medicine 40(4):469–477.
Mann NC, Mullins RJ, MacKenzie EJ, Jurkovich GJ, Mock CN. 1999. Systematic review of published evidence regarding trauma system effectiveness. Journal of Trauma-Injury Infection & Critical Care 47(Suppl. 3):S25–S33.
McCaig LF, Burt CW. 2005. National Hospital Ambulatory Medical Care Survey: 2003 Emergency Department Summary. Hyattsville, MD: National Center for Health Statistics.
McConnell KJ, Newgard CD, Mullins RJ, Arthur M, Hedges JR. 2005. Mortality benefit of transfer to level I versus level II trauma centers for head-injured patients. Health Services Research 40(2):435–457.
MCHB (Maternal and Child Health Bureau). 2004. Emergency Medical Services for Children. Five Year Plan 2001–2005: Midcourse Review. Washington, DC: EMS-C National Resource Center.
Mullins RJ, Mann NC. 1999. Population-based research assessing the effectiveness of trauma systems. Journal of Trauma-Injury Infection & Critical Care 47(Suppl. 3):S59–S66.
Mullins RJ, Veum-Stone J, Helfand M, Zimmer-Gembeck M, Hedges JR, Southard PA, Trunkey DD. 1994. Outcome of hospitalized injured patients after institution of a trauma system in an urban area. Journal of the American Medical Association 271(24):1919–1924.
Nallamothu BK, Saint S, Kolias TJ, Eagle KA. 2001. Clinical problem-solving of nicks and time. New England Journal of Medicine 345(5):359–363.
NAS, NRC (National Academy of Sciences, National Research Council). 1966. Accidental Death and Disability: The Neglected Disease of Modern Society. Washington, DC: National Academy of Sciences.
NASEMSD (National Association of State EMS Directors). 2004. Pediatric Disaster and Terrorism Preparedness. Falls Church, VA: NASEMSD.
Nathens AB, Jurkovich GJ, Rivara FP, Maier RV. 2000. Effectiveness of state trauma systems in reducing injury-related mortality: A national evaluation. The Journal of Trauma 48(1):25–30; discussion 30–31.
Nathens AB, Jurkovich GJ, Maier RV, Grossman DC, MacKenzie EJ, Moore M, Rivara FP. 2001. Relationship between trauma center volume and outcomes. Journal of the American Medical Association 285(9):1164–1171.
National Center for Injury Prevention and Control. 2004. DEEDS—Data Elements for Emergency Department Systems. [Online]. Available: http://www.cdc.gov/ncipc/pub–res/deedspage.htm [accessed November 25, 2005].
NHTSA (National Highway Traffic Safety Administration). 1996. Emergency Medical Services Agenda for the Future. Washington, DC: U.S. DOT.
NQF (National Quality Forum). 2002. National Voluntary Consensus Standards for Adult Diabetes Care. [Online]. Available: http://www.qualityforum.org/txdiabetes–public.pdf [accessed November 23, 2005].
NQF. 2003. National Voluntary Consensus Standards for Hospital Care: An Initial Performance Measure Set. [Online]. Available: http://www.qualityforum.org/txhospmeasBEACHpublicnew.pdf [accessed November 23, 2005].
NQF. 2004a. National Voluntary Consensus Standards for Nursing Home Care. [Online]. Available: http://www.qualityforum.org/txNursingHomesReportFINALPUBLIC.pdf [accessed November 23, 2005].
NQF. 2004b. National Voluntary Consensus Standards for Nursing-Sensitive Care: An Initial Performance Measure Set. [Online]. Available: http://www.qualityforum.org/txNCFINALpublic.pdf [accessed November 23, 2005].
NQF. 2005. National Voluntary Consensus Standards for Home Health Care. [Online]. Available: http://www.qualityforum.org/webHHpublic09-23-05.pdf_ [accessed November 23, 2005].
O’Brien PM. 1999. The emergency department as a public safety net. In: Fields W, ed. Defending America’s Safety Net. Dallas, TX: American College of Emergency Physicians.
Orr RA, Han YY, Roth K. 2006. Pediatric transport: Shifting the paradigm to improve patient outcome. In: Fuhrman B, Zimmerman J, eds. Pediatric Critical Care (3rd edition). Mosby, Elsevier Science Health. Pp. 141–150.
Peterson LA, Burstin HR, O’Neil AC. 1998. Non-urgent emergency department visits: The effect of having a regular doctor. Medical Care 36:1249–1255.
Pollack MM, Alexander SR, Clarke N, Ruttimann UE, Tesselaar HM, Bachulis AC. 1991. Improved outcomes from tertiary center pediatric intensive care: A statewide comparison of tertiary and nontertiary care facilities. Critical Care Medicine 19(2):150–159.
Pollock DA, Adams DL, Bernardo LM, Bradley V, Brandt MD, Davis TE, Garrison HG, Iseke RM, Johnson S, Kaufmann CR, Kidd P, Leon-Chisen N, MacLean S, Manton A, McClain PW, Michelson EA, Pickett D, Rosen RA, Schwartz RJ, Smith M, Snyder JA, Wright JL. 1998. Data elements for emergency department systems, release 1.0 (deeds): A summary report. Deeds Writing Committee. Journal of Emergency Nursing 24(1):35–44.
Rosenbaum S, Kamoie B. 2003. Finding a way through the hospital door: The role of EMTALA in public health emergencies. Journal of Law, Medicine & Ethics 31(4):590–601.
State of California Office of the Patient Advocate. 2005. 2005 HMO Report Card. [Online]. Available: http://www.opa.ca.gov/report_card/ [accessed January 12, 2006].
Studdert DM, Mello MM, Sage WM, DesRoches CM, Peugh J, Zapert K, Brennan TA. 2005. Defensive medicine among high-risk specialist physicians in a volatile malpractice environment. Journal of the American Medical Association 293(21):2609–2617.
Stylianos S. 2005. Outcomes from pediatric solid organ injury: Role of standardized care guidelines. Current Opinion in Pediatrics 17(3):402–406.
Tilford JM, Aitken ME, Anand KJS, Green JW, Goodman AC, Parker JG, Killingsworth JB, Fiser DH, Adelson PD. 2005. Hospitalizations for critically ill children with traumatic brain injuries: A longitudinal analysis. Critical Care Medicine 33(9):2140–2141.
Williams RL, Chen PM. 1982. Identifying the sources of the recent decline in perinatal mortality rates in California. New England Journal of Medicine 306(4):207–214.
Wright JL, Klein BL. 2001. Regionalized pediatric trauma systems. Clinical Pediatric Emergency Medicine 2:3–12.
Young GP, Wagner MB, Kellermann AL, Ellis J, Bouley D. 1996. Ambulatory visits to hospital emergency departments. Patterns and reasons for use. 24 hours in the ED Study Group. Journal of the American Medical Association 276(6):460–465.


















































