1
Introduction
According to projections of the U.S. Census Bureau, the demographics of the United States population will change dramatically over the next five decades. By 2050 whites will comprise 53 percent of the general population, Hispanics 25 percent, Asians nearly 9 percent, and blacks 15 percent (see Figure 1-1). Females will outnumber males by over 6 million, and the average age of the population will become older, with one in five persons over the age of 65. For the biomedical community these demographic changes present considerable challenges for both research and healthcare delivery.
The increased diversity in the population has not been reflected in the composition of the healthcare and biomedical research workforces, which is an issue of considerable concern to the biomedical and healthcare community. Indeed, the need for diversity in the healthcare workforce was recently examined by the Institute of Medicine (2004a).
If the need for diversity in healthcare delivery is acute, the need in the clinical research workforce is even more so. Before healthcare practices can be developed and introduced into primary care, much research must be conducted, both basic and clinical. Because of the historically lower rates of participation in research by women and ethnically diverse groups, both among the workforce and as participants in clinical trials, the challenge of meeting the complex healthcare needs of an ever more diverse population is particularly difficult.
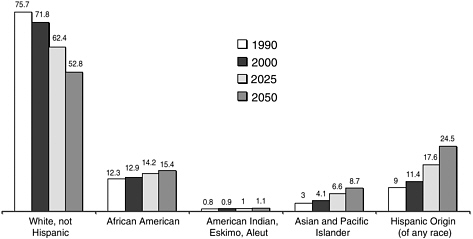
FIGURE 1-1 Percent of the population by race or ethnicity: 1990, 2000, 2025, and 2050.
SOURCE: U.S. Census Bureau, decennial census and population projections.
The need for greater diversity in the clinical research workforce is compelling. Racial and ethnic minority healthcare professionals are more likely to serve minority populations (Cantor et al., 1996; Komaromy et al., 1996). Minority patients are more likely to select healthcare professionals with their own ethnic background (Saha et al., 1999). Consequently, healthcare professionals from racial and ethnic minority groups may be more successful in recruiting minority patients to participate in clinical research. Such efforts are critical to linking scientific advancements with quality service and delivery in underserved minority communities.
In some ways minority researchers may be better positioned to formulate the right research questions as well as to devise ways to answer them. When compared with the majority population, minority populations in the United States experience higher rates of disease and mortality (e.g., cancer, cardiovascular disease, diabetes, HIV/AIDS, infant mortality), and they are less likely to receive regular, high-quality medical and preventive healthcare services (NIH, 1994; Corbie-Smith et al., 1999; Giuliano et al., 2000; Killien et al., 2000; Gifford et al., 2002). Specifically, black men are more likely to be diagnosed with prostate cancer. Asian Americans are more likely to get stomach and liver cancer. The American Indian population has the lowest cancer survival rates of all (Haynes, 1999). Some of these disparities can be attributed to socioeconomic differences and poorer access to
health insurance. However, access to quality health care for these populations may also be affected by the diversity of the healthcare and clinical research workforce (NIH, 1994; Corbie-Smith et al., 1999; Giuliano et al., 2000; Killien et al., 2000; Gifford et al., 2002).
Gender adds yet another dimension to an already complex problem. Since the establishment of the Office of Research on Women’s Health at the National Institutes of Health, a tremendous amount of information has been gained. In biomedical research, gender is clearly a critical factor in understanding human health (IOM, 2001a). Minority women and white women experience different rates of disease. Among Hispanic and Vietnamese American women, cervical cancer rates are higher. African American women are also less likely to survive breast cancer, although they are less likely than others to develop it (Haynes, 1999).
Women are critical to clinical research not only as participants in clinical trials but also as researchers. A driving factor in the need to recruit women into the clinical research workforce is that they are likely to be the majority of M.D. recipients in the future and therefore the pool from which researchers must be drawn. In the past few decades the number of M.D.s awarded to women has steadily increased; in 2003 females accounted for almost 50 percent of medical school enrollment (AAMC, 2003). In the basic sciences women currently receive half of the bachelor’s degrees issued in the biological sciences and over 40 percent of the Ph.D.s (NSF, 2004), and the trend is toward continued increases in their proportions of these degrees.
Clearly then, women and underrepresented minorities are crucial to replenishing the clinical research workforce. A diverse workforce in the sciences leads to many benefits—among others, a wide diversity of perspectives leading to better opportunities for scientific advancement, and a potentially intensified focus on understanding and eradicating health disparities among different ethnic and racial groups (Crowley et al., 2004). Research indicates that cultural differences are often at the core of miscommunication and dissatisfaction in the physician–patient relationship; culture also can significantly influence patient health outcomes (Anderson, 1995; Airhihenbuwa et al., 1996; Berger, 1998; Hunt et al., 1998). Moreover, diverse teams can outperform homogeneous ones (Lippman, 2000; Sessa and Taylor, 2000). Managers who are exposed to professionally and culturally diverse colleagues cultivate new ideas by drawing on a larger pool of information and experiences.
LESSONS FROM THE BUSINESS SECTOR
Researchers in the business sector have learned that a diversified staff facilitates marketing to a more diversified customer base, which increases market share (Allen and Montgomery, 2001). They have also learned that companies with reputations for good diversity management are more successful in attracting and retaining top-quality employees (Ferraro and Martin, 2000). Likewise, companies with high ratings on equal employment opportunities outperform those with poor ratings on hiring and advancing women and minorities (Adler, 2001). Fortune 500 companies with the highest percentages of women executives deliver earnings far in excess of the median compared with large firms with the fewest women. Among initial public offerings, companies with women in senior management received higher valuations and had better long-term performance (Church, 2001).
Private sector companies have thus begun to recognize that diversity is associated with enhanced productivity and lower turnover costs among highly trained employees. The economic advantages of a diverse workforce are even greater for businesses that serve a diverse clientele (McCracken, 2000). In 1991 the accounting firm Deloitte and Touche was experiencing a high rate of attrition among women professionals, which company leaders initially attributed to societal reasons. The realization among those leaders that a sizable share of the company’s primary product—its talent—was leaving each year led to cultural changes at Deloitte and Touche that have been widely regarded as successful. During the nine years after the implementation of an initiative for retention and advancement of women, the proportion of women full partners and directors increased from 5 percent to 14 percent, and attrition rates for men and women equalized. In addition, overall retention rates improved substantially, which saved an estimated $250 million in hiring and training costs and has supported increased productivity among the retained staff (Mueller, 1998).
IMPLICATIONS FOR ACADEMIC HEALTH CENTERS
What are the implications of these “lessons” for academic health centers? A recent study concluded that academic health centers (AHCs) that benefit from women’s intellectual capital receive both short- and long-term payoffs (Morahan and Bickel, 2002). Female patients are seeking female surgeons and subspecialists. Likewise, students are seeking female role models in these fields (Bickel, 2001; Morahan and Bickel, 2002). As
the proportion of women students continues to increase, only those institutions able to recruit and retain women in all departments will have the best house staff, faculty, and administrators (Cox, 1993). The absence of women in key positions can be a negative signal to female candidates.
A growing number of studies indicate that positive academic and social outcomes for students can be attributed to diversity in higher education that benefits the training of health professionals (IOM, 2001b). Bowen and Bok (1998) studied the educational and career outcomes of two cohorts of majority and minority students attending selective colleges and universities. They found that the minority graduates of these institutions attained levels of academic achievement that were on a par with those of their nonminority peers. More specifically, these minority graduates obtained professional degrees in fields such as law, medicine, and business at rates far higher than the national averages for all students (Bowen and Bok, 1998). Similar findings were obtained in a study of the academic outcomes of college students attending racially and ethnically diverse colleges and of those attending less diverse institutions. Gurin (1999) concluded that students can best develop the capacity to understand the ideas and feelings of others in an environment characterized by a diverse student body, equality among peers, and discussion of the rules of civic discourse.
Although it should not be assumed that women and other underrepresented individuals would choose research topics directly related to their populations, their enhanced representation and involvement may improve perspective and understanding in hypothesis generation for all research in which they are involved. Furthermore, those who belong to a group of interest are more likely to have personal experience that will aid in the selection of testable hypotheses and methods appropriate to the population. The participation of minority groups in clinical trials is enhanced by the participation of minority clinical research investigators (NIH, 2002b).
THE FOCUS OF THIS STUDY
To examine this issue the National Research Council’s Committee on Opportunities to Address Clinical Research Workforce Diversity Needs for 2010, supported in part by the Office of Research on Women’s Health at the National Institutes of Health, conducted a study of opportunities to enhance participation and promote diversity in the clinical research workforce. The committee developed the study charge, which was to highlight new paradigms in clinical research and research training (inter-
disciplinary research and team science) and to issue recommendations for improvements in the training of nurse and physician clinical research investigators. In its work the committee focused on the following questions:
-
What is the benefit of increasing the representation of women and underrepresented ethnic groups in the clinical research workforce? Will increased diversity improve delivery of the results of clinical research to minority communities?
-
What are the needs of the private and public sectors? Are the current approaches to training clinical investigators meeting the needs of academia, industry, and public health? Where is demand exceeding supply?
-
What training programs and career tracks appear to foster the development and retention of women and minorities in the clinical research workforce?
-
What research related to the evaluation of existing training efforts needs to be funded? What are the important measures of outcome?
To address these questions the committee gathered information from numerous sources and held a workshop of stakeholders—clinical researchers, academic health center deans, and funders of clinical research in 2003. The information gathering was directed toward assessing current progress on increasing the participation of women and underrepresented minorities in clinical research and identifying workforce sectors that require attention (see Appendix A for biographies of the workshop speakers, Appendix B for a list of workshop participants, and Appendix C for the workshop agenda).
The workforce and training needs for all biomedical research, including clinical research, have been monitored by the National Institutes of Health since 1975. As mandated by Congress, the National Research Council has conducted an ongoing assessment of the nation’s overall need for biomedical and behavioral research personnel, the subject areas in which researchers are needed and the numbers of personnel required in those areas, and the type of training needed by researchers. The original study committee interpreted the charge to include clinical research, and it monitored clinical research scientists and training. The monitoring of clinical research has continued throughout the series of reports issued in conjunction with the study.
Each study report in the series has cited the challenges encountered in trying to estimate the workforce and training needs for the clinical research
community. The primary obstacle cited is the dearth of data on the clinical research workforce.
The committee for the study described in this volume agreed with the biomedical research workforce study reports that the lack of a clear, agreed-upon definition for clinical research is a significant obstacle to the collection of data. Based on this and other information, the current study committee concentrated its effort on the recruitment of M.D.s, M.D./Ph.D.s and Ph.D. nurses into clinical research.
The study committee found that clinical research presented a set of challenges different from those posed by basic science for students considering research careers. Chapter 2 provides a framework for understanding the systemic challenges facing those who educate, fund, and employ clinical researchers. Chapter 3 outlines the current status of women and underrepresented minorities in clinical research, as well as the programs that have been devised to aid their advancement. The specific needs of nursing professionals are addressed in Chapter 4. Chapter 5 presents the study’s conclusions and recommendations.







