4
Potential Psychological Risks
When a woman chooses to donate her eggs for use in the in vitro fertilization (IVF) process or scientific research, it is a very personal decision, one with a variety of psychological implications and consequences. Or as Susan Klock, professor in the departments of obstetrics and gynecology and of psychiatry at Northwestern University, described it, “There is a whole psychology about why a woman does this and what she thinks and feels about being an oocyte donor.” And so, in addition to the potential physical risks, the donation process potentially carries with it a number of psychological risks as well.
Those potential risks can be classified into three broad categories (see Box 4-1), Klock said: the psychological aspects of the donor screening process, the psychological aspects of the procedure itself, and a post-donation psychological adjustment to the donation. There have been relatively few studies of the psychology of oocyte donation, she said, and the studies that have been done have generally been small ones with relatively few subjects. Still, it is possible to describe some basic findings about the psychological effects on women who donate their eggs.
POTENTIAL PSYCHOLOGICAL RISKS IN THE SCREENING PROCESS
The egg donor recruitment process is straightforward, Dr. Klock said. An IVF program that is looking for donors or an independent recruiter will place advertisements in university newspapers, on the Internet, and in other places where they can reach large numbers of women in
|
BOX 4-1 Summary of Potential Psychological Risks
|
the 21- to 34-year-old age range, which is best for donors. Potential donors then contact the program and are sent forms to fill out providing background information about their medical condition and details about who they are and why they are interested in being an egg donor. Later the recruiter will review that information and bring the potential donor in to talk with her about what it’s like to be a donor and to put her through a medical and a psychological screening.
Statistics show that only about 12 percent of women who inquire about being a donor actually complete the screening process and complete a donation cycle, Dr. Klock said (see Figure 4-1).
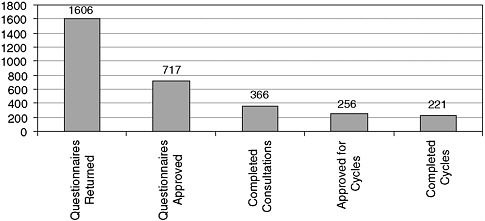
FIGURE 4-1 Impact of donor screening on eventual donation.
SOURCE: Center for Reproductive Medicine and Infertility (unpublished data).
The psychological screening interview typically takes about 60 to 90 minutes, and it is done as a face-to-face discussion. “We put as our purpose for these screenings to give the donor an opportunity to talk about the very complex issues that go along with the decision to be a donor,” Dr. Klock said. The American Society of Reproductive Medicine provides guidelines for how to do the screening interviews. The screening is best done, she said, by a licensed mental health professional who has expertise working in assisted reproductive technologies. This expertise is important because a familiarity with the field provides a context that helps the interviewer know which questions to ask.
“When you begin a screening interview,” Dr. Klock said, “the first thing that becomes apparent from the donor is the question of motivation. You listen for this in the interview: Why do you want to be an egg donor? And without fail, two ideas come up. The first is, ‘I want to help somebody. I know somebody who’s gone through infertility. I know somebody who can’t have a child. I want to help somebody.’” And the second motivation is usually the compensation. Egg donors in Chicago typically get $7,500 for a single cycle, Dr. Klock said. The compensation is somewhat more in some places, somewhat less in others, but it is substantial enough that it can, when combined with the chance to help someone, make the donation process an appealing opportunity for some women.
Other motivations that potential donors mention include an interest in science, wanting to find out about one's own fertility, and making up for a previous reproductive loss.
In addition to the applicant’s motivations for donating, an interviewer will typically cover a number of other standard topics, Dr. Klock said. “We talk about psychosocial issues, the women’s reproductive history, her family history, her educational background. And then we also talk about the use and disposition of the oocytes.” The interview will also typically include a psychological test, most often the Minnesota Multiphasic Personality Inventory, the MMPI-II. “It’s the most widely used psychological test in the United States. It’s also the test that’s used to screen for professionals in high-risk jobs: airline pilots, firefighters, police officers.”
During the interview, the screener is looking for various factors that would exclude the applicant from being allowed to donate eggs. “We’re looking for substance abuse or addiction issues, impaired cognitive functioning, or the inability to provide informed consent,” Dr. Klock said. In particular, if a woman doesn’t really understand the procedure that she’s
about to undergo, she is not fully able to give informed consent, and she will be excluded from being a donor on that basis. Furthermore, a women who has suffered from mental illness or who has a family history of mental illness will also generally be excluded. In this case, the reason is not so much a medical or ethical one but rather that very few women undergoing IVF with donated eggs will select a donor with such a history.
One other exclusionary factor is what Dr. Klock referred to as excessive current life stress. “This is kind of a global term,” she explained. “If a woman is in the midst of a divorce, or if a woman has just been a victim of a violent crime, this is not a great time for her to be an egg donor.”
Studies show that between 2 and 27 percent of potential donors are excluded for psychological reasons, and it is this exclusion that offers the major psychological risk in the screening process. If an applicant is excluded for a psychological reason, the interviewer must explain to her what psychological issues have been discovered and then provide appropriate referrals if there is a problem that needs to be dealt with.
“So the potential risk here,” Dr. Klock explained, “is uncovering a previously undetected or undiagnosed psychological problem. That is a very jarring thing for a woman to experience. Sitting in the office with her, talking with her about that, she can tend to feel rejected, inferior. It can be a huge blow to her self-esteem. ‘Why? You don’t even want my eggs. Oh, I feel terrible.’ And that’s a very real concern for women from a psychological perspective.”
Another potential risk is the possibility of uncovering something in the medical screening that the applicant didn’t know about, particularly something that could affect her future fertility. That can also affect a woman psychologically.
POTENTIAL PSYCHOLOGICAL RISKS OF THE DONATION PROCEDURE
The donation procedure itself carries certain potential psychological risks as well, but these tend to be less threatening. They are also temporary, not lasting much past the procedure itself.
One issue is the effect of the hormone injections that the donors give themselves to prepare their ovaries to produce as many eggs as possible. Dr. Klock described a study performed by a pair of doctors who surveyed a group of donors after they had completed a donation cycle. The study found that fully half the donors reported mood swings and irritabil-
ity during the hormone treatment. “This is very similar to what we see among our own IVF patients,” she said. “They talk about feeling irritable, rejection-sensitive, lots of crying, lots of low mood, and it does seem to be linked to the use of those medications.”
Another issue is concern associated with the egg retrieval surgery. One study of donors conducted by investigators at Dartmouth Medical School found that 83 percent reported high anxiety on the day of retrieval. Besides this anxiety, donors also listed the daily injections, the frequent travel to the clinic, and pain as the most difficult aspects of the donation process itself.
The good news about these potential psychological risks, Dr. Klock said, is that they do not appear to carry over past the donation. Once the surgery is done and the medication is out of a woman’s system, the psychological symptoms vanish.
It seems likely, Dr. Klock noted, that the potential psychological risks both here and in the screening process will be the same for research donors as they are for women donating their eggs for reproductive purposes.
POTENTIAL PSYCHOLOGICAL RISKS OF POST-DONATION ADJUSTMENT
There have been at least seven published studies looking at the post-donation psychological adjustment of women who donated their eggs for other women’s pregnancies. The studies were generally done as mail-out surveys anywhere from two weeks to seven years after the retrieval surgery, although one survey was done using post-donation exit interviews.
The surveys found that the typical donor is a single, white, high school graduate with some college education who has never had children. “This does not tend to be a very diverse group demographically,” Dr. Klock commented.
The psychological risks identified by these studies tend to center on such issues as future fertility and whether a child or children had resulted from the donation. One 1995 study, for example, surveyed 32 donors 18 months after their donations. The donors reported that the most difficult aspects of the donation process itself were refraining from intercourse and the mood swings that they experienced while on the medication. Half of them reported having second thoughts about having donated, and the reasons they gave were concerns about compromising their own fertility
and never knowing if a child resulted from their donation. Or, as Dr. Klock put it, “The thing that is sticking in their minds is, ‘In 18 years am I going to be answering the door to one of my offspring?’ This is something that tends to stay with them and is a source of concern and sometimes regret.” This particular concern will not be an issue for research donors, of course, because their eggs will not figure in a subsequent pregnancy.
In another survey of 24 women done 2 years after donation, 87 percent wanted to know if a pregnancy had resulted, over half were worried about the medical risks, and 17 percent regretted donating. By the same token, a majority were satisfied with their donation, and 42 percent said they would donate again.
And, indeed, although the surveys uncover a minority of women with various concerns, a majority of women seem to be satisfied with their donation experience. In a study done of 24 donors at the Cleveland Clinic contacted 6 and 12 months post-donation, 78 percent reported being very satisfied with the donation process, and 74 percent stated they would be willing to donate again. Donors said that the best aspects of the donation were helping another woman, being a medical pioneer, and the financial compensation. And this is a good lesson for recruiting donors for research purposes, Dr. Klock said. Egg donors often like to think of themselves as being in the medical world, as being a medical pioneer, and it is common for them to be involved in other medical programs—giving blood, for instance, or taking part in medical studies.
In particular, Dr. Klock said, reproductive donors are very interested in the outcome of their donation. They want to hear whether their donated eggs allowed a woman to give birth to a child. Dr. Klock said she believes that something similar will be true for women donating for research purposes. “If women are going to this kind of effort, they want to know that the reason that they were motivated to do this was met, whether that was a research goal or a reproductive goal.”
Finally, the surveys showed that the donors who were motivated more by altruism and wanting to help others were more likely to be satisfied with their experience later on than were donors who were motivated mostly by the financial compensation. However, the role of financial compensation should not be dismissed. According to Dr. Klock, altruism and compensation often go hand in hand. Furthermore, in one study conducted 3 to 18 months post-donation, only 11 percent of participants reported that they would donate again if no compensation was provided.
Another study, three years post-donation, found that approximately half of the donors were motivated by financial reasons.
These surveys offer a number of lessons, Dr. Klock said. Overall, from 44 to 79 percent of the donors were satisfied with the experience. And a third of the donors were satisfied enough to complete more than one donation cycle.
Such repeat donors are very important to recruiters and IVF programs. Because the screening process is so labor-intensive, it saves a great deal of time and effort to have women who donate again and again, and this will be just as true for research donors as for reproductive donors. It is difficult, however, to know how the factors that lead women to donate multiple times for reproductive purposes will play when the donations are for research instead. When the purpose is reproduction, for example, some women may feel their need to help another woman is met after donating once; in the case of research programs, this same sort of thinking may not come into play. Another factor that may keep women from donating multiple times to a reproductive program is the fear of multiple offspring. If she donates eggs to multiple women, the possibility exists of having two or more biological offspring who were not aware that they are siblings, opening the door to the possibility of inadvertent incest. This would obviously not be a concern for research donors.
In contrast to the majority of women who are satisfied with the donation process, a minority of donors report having had a negative emotional reaction or regretting their decision to donate. “I see this as a failure in the screening process,” Dr. Klock said. “We are not doing a good enough job in screening out donors who are ambivalent.” In response, she said, she and colleagues are working on a project to modify a kidney donor ambivalence scale to see if it can be used to uncover some of the ambivalence that egg donors may feel. Another way to filter out more of these ambivalent donors, she said, would be to have a greater time lag between the time a donor is accepted into a program and the time that she undergoes the donation cycle. “I think just a little bit of time can allow a woman to fully think about the implications of what she may opt to do.”
One other fact came to light from the surveys that is of particular interest to those looking to recruit women as research donors: 25 percent of the reproductive donors questioned said they would not want their eggs used to create research embryos. So it seems clear that not all of the women who donate their eggs for reproductive purposes would be willing to donate them for research. By the same token, there may well be
women who would not donate their eggs for reproduction but who would donate for research.
In conclusion, Dr. Klock said, the main negative psychological effects on egg donors after their donation were the regret and worry that were present for a minority of donors. The regrets can best be dealt with through a better selection process, which keeps out those who are ambivalent about the donation and thus likely to feel regrets later on, while the worries are best dealt with by communication and further research. Research is also necessary to counter the limitations of the studies discussed today, which include small sample sizes, single center, and cross-sectional design. Multicenter, longitudinal studies are needed in this area. “It is incumbent on us,” she said, “to have meetings like this to review what the potential risks are and then communicate them to the women to the extent that we know them at the time. We need to continue to study and follow up on women who have gone through donation cycles to know what the potential risks are and how to counsel them appropriately.”
SUMMARY: WHAT WE KNOW ABOUT THE PSYCHOLOGICAL RISKS OF OOCYTE DONATION
There are three main categories of psychological risk associated with donating eggs: issues associated with the screening process, problems surrounding the donation procedure itself, and the post-donation adjustment to the donation.
The main risk in the first category is that the screening process may reveal some previously unknown psychological or medical condition that disqualifies the woman from donating and that is uncomfortable or psychologically threatening to the applicant.
During the donation process, women report mood swings and irritability caused by the fertility drugs, pain caused by their injection, and anxiety in anticipation of the surgical procedure. The issues disappear after the procedure is complete.
After the eggs have been donated, the main psychological issues that donors experience are related to worries about future fertility and concerns about children conceived from their eggs. The latter will clearly not










