1
Introduction
The story of the Cuban missile crisis is well known. In the summer of 1962, in response to evidence of a significant increase in shipments from the Soviet Union to Cuba, President Kennedy ordered Air Force U-2 reconnaissance flights over Cuba. These reconnaissance missions produced evidence of ballistic missile and nuclear storage facility construction. On October 22, President Kennedy addressed the nation about the situation in Cuba and, in the end, the world breathed a long sigh of relief at the conclusion of the missile crisis, as a potentially catastrophic war was narrowly avoided.
Less well known, perhaps, is the personal story of Air Force Major Rudolph Anderson, one of the U-2 pilots who flew those reconnaissance missions. On October 27, five days after President Kennedy’s address to the nation, Major Anderson flew yet another reconnaissance mission over Cuba. He died when his U-2 jet was shot down by a Soviet-supplied surface-to-air missile, and became the sole U.S. military casualty of the Cuban missile crisis.
The following day, in a personal letter to Major Anderson’s widow, Frances, President Kennedy expressed his shock over the loss of her husband’s life. The President described the kind of sacrifice Major Anderson made by giving his life in service to his country, and referred to it as “the source of our freedom.” Kennedy went on to say, “On behalf of a grateful nation, I wish to convey to you and your children the sincere gratitude of all the people.”
Other presidents have used similar words on many occasions, dating back to the days of the Revolutionary War. However, in his letter to Mrs. Anderson, President Kennedy eloquently expressed the entire coun-
try’s feeling of indebtedness to veterans and their families who sacrifice on behalf of our nation.
It is impossible to undertake any responsible assessment of a veterans assistance program without starting here—with an understanding and acknowledgment that these programs are but one way (and, sometimes, an inadequate way) that a “grateful nation” attempts to repay its indebtedness to those who serve in the military. Any judgment about how these programs perform has to be made through this lens. That is why any comparisons between the veterans disability compensation program and similar disability assistance programs (such as Social Security Disability Insurance, workers’ compensation, or private disability retirement programs) are bound to fall short. The standard is just not the same.
Of course, this does not mean that the veterans disability compensation program is perfect or that it should not be held to high standards of performance. Careful and critical assessment of program performance is essential, but it has to be done within the context of the program’s unique circumstances.
The following is how the Department of Veterans Affairs (VA), the government agency responsible for veterans programs, expresses the unique circumstances under which a “grateful nation” provides for its veterans (VA, 2006):
For 230 years, Americans in uniform have set aside their personal aspirations and safety to procure and protect the freedoms established by the Founders of our great nation. Through their service, and, all too often, through their sacrifices, these brave men and women have earned the gratitude and respect of the entire nation.
During the Civil War, President Abraham Lincoln affirmed our nation’s commitment “… to care for him who shall have borne the battle, and for his widow and his orphan.” His eloquent words endured from his century to ours and serve today as the motto of the Department of Veterans Affairs, the federal agency responsible for honoring our debt of gratitude to America’s patriots.
PROJECT BACKGROUND
P.L. No. 108-136 (the National Defense Authorization Act of 2004) established the Veterans’ Disability Benefits Commission to “carry out a study of the benefits under the laws of the United States that are provided to compensate and assist veterans and their survivors for disabilities and deaths attributable to military service.” The law requires the commission to make recommendations to the president and to Congress about (1) the appropriateness of such benefits under the laws in effect on the date of the enactment of the act, (2) the appropriateness of the level of such benefits,
and (3) the appropriate standard or standards for determining whether a disability or death of a veteran should be compensated.
The law also requires the commission, in its report, to include an evaluation and assessment of the following:
-
the laws and regulations that determine eligibility for disability and death benefits and other assistance for veterans and their survivors;
-
the rates of such compensation, including the appropriateness of a schedule for rating disabilities based on average impairment of earning capacity; and
-
comparable disability benefits provided to individuals by the federal government, state governments, and the private sector.
In carrying out these tasks, the commission developed a comprehensive set of research questions for study in determining whether the current disability compensation design is appropriate or whether more appropriate alternatives exist. As required by its statutory mandate, the commission consulted with the Institute of Medicine (IOM) on those research questions relating to the medical aspects of contemporary disability compensation policies.
The commission asked IOM to convene two committees of experts to address the following six tasks (with one committee addressing tasks 1 through 5 and the other addressing task 6):
-
Conduct a comprehensive review of VA’s “Schedule for Rating Disabilities” (the “Rating Schedule”). Assess whether the schedule is an appropriate, valid, and reliable instrument for evaluating medical impairment and determining degree of disability.
-
Examine adequacy and appropriateness of medical criteria used to qualify veterans for special purpose and ancillary benefits including individual unemployability (IU).
-
Determine if the methods for determining and coding impairments and the methods for determining their severity are medically sound for single and multiple conditions.
-
Assess the medical criteria currently used to qualify veterans for secondary and aggravated service-connected conditions and how to measure and control for the effect of natural disease progression.
-
Assess how medical expertise is used to evaluate veterans throughout the claims process. Comment on the appropriateness of medical credentials and training requirements needed to support the disability evaluation and rating process.
-
Review the current scientific methodology used to support pre-
-
sumptive compensation decisions. Suggest alternate models that better leverage scientific knowledge for these decisions.
In response to the request, IOM formed the Committee on Evaluation of the Presumptive Disability Decision-Making Process for Veterans to address task 6. That committee’s report will be issued separately.
IOM also formed the Committee on Medical Evaluation of Veterans for Disability Compensation (hereafter referred to simply as “the committee”) to respond to tasks 1 through 5. The remainder of this report provides the findings, conclusions, and recommendations of that committee.
The committee consists of 16 experts representing disciplines of particular relevance to these tasks, as specified by the commission, including experts in clinical medicine, mental health, disability medicine, legal medicine (disability), physical rehabilitation, private-sector disability programs, veteran health compensation policy, and the veterans health system. In addressing these five tasks, the committee considered specific questions posed for it by the commission. (The original five tasks evolved into six specific study questions, with the exception of task 2, which produced two separate study questions):
-
How well do the medical criteria in the Rating Schedule and VA rating regulations enable the assessment and adjudication of the proper levels of disability to compensate both for the impact on quality of life and impairment in earnings capacity? Provide an analysis of the descriptions associated with each condition’s rating level that considers progression of severity of condition as it relates to quality-of-life impairment and impairment in average earnings capacity.
-
Certain criteria and/or levels of disability are required for entitlement to ancillary and special-purpose benefits. To what extent, if any, do the required thresholds need to change? Determine from a medical perspective at what disability rating level a veteran’s medical or vocational impairment caused by disability could be improved by various special benefits (such as adapted housing, automobile grants, clothing allowance, and vocational rehabilitation). Consideration should be given to existing and additional benefits.
-
Analyze the current application of the IU benefit to determine whether the Rating Schedule descriptions need to more accurately reflect a veteran’s ability to participate in the economic marketplace. For the population of veterans with disabilities, analyze the cohort that has been rated as being unemployable. Examine the base rating level to identify patterns. Determine if the Rating Schedule description of the condition provides a barrier to assigning the base disability rating level commensurate with the veteran’s true vocational condition.
-
What are the advantages and disadvantages of adopting universal medical diagnostic codes rather than using a unique system? Compare and contrast the advantages and disadvantages of the Rating Schedule and the American Medical Association Guides to the Evaluation of Permanent Impairment (AMA Guides).
-
From a medical perspective, analyze the current VA practice of assigning service connection on “secondary” and “aggravation” bases. In secondary claims, determine what medical principles and practices should be applied in determining whether a causal relationship exists between two conditions. In aggravation claims, determine what medical principles and practices should be applied in determining whether a preexisting disease was increased because of military service or was increased because of the natural process of the disease.
-
Compare and contrast the role of medical clinicians in the claims and appeals processes in VA and the Department of Defense (DoD), in Social Security, and in the various federal employee disability benefits programs.
The committee met five times between May 25, 2006, and January 8, 2007. Three of these meetings included sessions open to the public, and the committee heard from a wide range of individuals and organizations with interest or expertise in veterans health and disability, as well as experts in measurement of disability and quality of life.
In addition, members of the committee and staff visited several VA regional offices and a VA medical center to observe compensation claims processing. They spoke with a variety of individuals, including regional office directors and assistant directors, clinicians, veterans service representatives, rating veterans service representatives, and decision review officers.
Agencies, organizations, and other groups who provided data, other information, and statements to the committee included the following (in alphabetical order):
-
African American PTSD Association
-
American Legion
-
American Medical Association
-
American Psychiatric Association
-
Board of Veterans Appeals
-
Department of Veterans Affairs
-
Disabled American Veterans
-
Missouri Veterans Commission
-
Navy Physical Evaluation Board
-
Office of the Secretary of Defense
-
Veterans’ Disability Benefits Commission
-
Veterans of Foreign Wars, National Veterans Service
-
Vietnam Veterans of America
BRIEF OVERVIEW OF THE VETERANS DISABILITY COMPENSATION PROGRAM
VA administers federal veterans assistance programs. Generally, a veteran must have been discharged from active military service under other than dishonorable conditions to qualify for assistance. Veterans benefits include, but are not limited to
-
health care;
-
compensation for service-connected disabilities;
-
assistive devices and special benefits for service-connected disabilities;
-
disability pension;
-
education and training;
-
vocational rehabilitation;
-
home loan guaranty;
-
life insurance; and
-
burial and memorial benefits.
A variety of stakeholders are involved in these veterans benefit programs, with separate, but interrelated, roles and interests. These include the following:
-
Veterans and their dependents and survivors—These are the recipients of veterans benefits, as well as other veterans, dependents, and survivors who wish to receive benefits, but who do not qualify.
-
Members of the general public—The public, which funds these programs through the taxes they pay, have a keen interest in ensuring that these programs are efficient, effective, fair, and accurate.
-
The legislative branch of the U.S. government—Congress makes the laws that authorize payment of veterans benefits and prescribe the overall program structure.
-
The executive branch of the U.S. government—Under the direction of the president, VA administers these programs.
-
The judicial branch of the U.S. government—The Court of Appeals for Veterans Claims has jurisdiction over appeals of VA decisions.
-
Providers of health-care services to veterans and their families within the VA hospitals and clinics
-
Evaluators of impairment and disability (physicians and others)
-
VA raters (interpreters of the regulations governing disability)
-
Those within VA who resolve the disputes that may arise concerning presence or absence of disability and its extent
-
Veterans service organizations and other advocacy groups—Veterans service organizations include groups chartered by Congress or recognized by VA for purposes of representing veterans in claims (such as the American Legion, Vietnam Veterans of America, Veterans of Foreign Wars, Paralyzed Veterans of America, and Disabled American Veterans) and other non-chartered groups. These also include state and local veterans service organizations.
The VA disability compensation program (which is described in much greater detail later in this report) provides a monthly, tax-exempt, cash payment to veterans who are disabled due to an illness or injury that is “service-connected.” A disability is “service-connected” if the particular illness or injury that results in disability was incurred while the individual was on active duty in the armed forces of the United States, or if a preexisting illness or injury was made worse (aggravated) during active duty service. A disability is also service connected if, although it was not incurred during active duty service, it was nevertheless either caused or made worse by another service-connected disability (i.e., it is a “secondary” disability).
Determining whether a disability was incurred while an individual was on active duty (i.e., a direct service connection) is relatively straightforward. If a veteran’s illness or injury causes disability and it was coincident with (i.e., it occurred or began during) active duty, then direct service connection is established. The concept of “incurred while/during” active duty should not be confused with the medical concept of “caused by.” The subtle difference is intentional and undoubtedly represents a manifestation of the nation’s gratitude explained earlier. “Incurred while” is an assumption of national responsibility for the risks accepted during service.
Establishing service connection based on aggravation of a preexisting condition or based on a secondary disability is more complex. In the case of a secondary disability, there must be a causal relationship between the veteran’s current (secondary) disability and another (primary) service-connected disability. In the case of aggravation of a preexisting condition, service connection is established when there is an increase in disability (i.e., a worsening of the preexisting condition) during the service that is not caused by natural progression of the condition. However, VA applies a presumption of aggravation “unless there is a specific finding that the increase in disability is due to the natural progress of the disease.”1 Such determinations require complex medical judgments, which gave rise to task 4 of the commission’s request to IOM, which is concerned with the
medical principles and practices that should apply when evaluating secondary or aggravation cases. These issues are discussed in detail in Chapter 9 of this report.
These monthly cash payments are intended to compensate veterans for the loss of earning capacity that results from the disability. However, the amount of compensation is not based on the specific veteran’s actual loss of earnings. Rather, it is based on the “average” impairment in earning capacity caused by the disability. Further, although not explicit in the law, the legislative history of the VA disability compensation program is believed to include an implicit congressional intent to compensate veterans for non-economic losses, such as loss or loss of use of a limb or organ that may not affect ability to work but reduces the quality of life of the veteran (VA, 2004).
The amount of compensation is set by law, based on a percentage disability rating (from 0 to 100 percent, in increments of 10 percent). The percentage rating is determined according to the Rating Schedule, which is intended to reflect the relative severity of the disability, meaning impairment of earning capacity. However, there are persistent questions about the extent to which the Rating Schedule compensates for impairment of average earning capacity. As one obvious example, although the disability ratings increase in 10 percent increments, the associated dollar payments do not. There are additional questions. According to the Government Accountability Office, the last comprehensive review of the validity of the Rating Schedule as a measure of loss of earning capacity was performed in the early 1970s (VA, 1971). It measured the difference between the earning capacity of veterans with disabilities and the earnings of veterans without disabilities, controlling for age, education, and region of residence. Of the approximately 700 diagnostic codes studied, almost half (330) overestimated loss of earning capacity and more than 10 percent (75) underestimated loss of earning capacity (GAO, 1997). Given the additional 35 years of medical, social, technological, occupational, and economic changes that have transpired since that study was conducted, one would expect the correlation between the Rating Schedule and actual economic loss to be even more tenuous today. In addition, there has never been a study of the extent to which the Rating Schedule compensates for reduction in quality of life. These issues, which correspond to the commission’s task 1, are discussed in detail in Chapter 4 of this report.
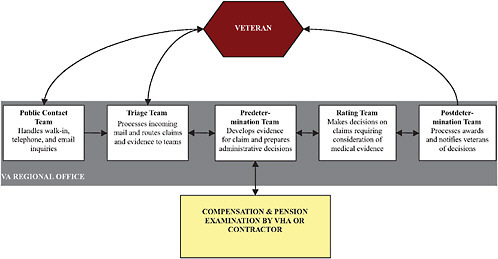
When a veteran files a claim for disability compensation (see Figure 1-1 for an overview of the claims application and development process), the disability rating is made by a rating veterans service representative (RVSR) working on a rating team. RVSRs are nonmedical personnel who review veterans’ medical records and apply the Rating Schedule based on those records. Generally, an applicant’s claim file will include a compensation and pension examination, conducted either by medical personnel at a VA medi-
cal facility or by a contract examination provider using VA’s examination protocols. However, physicians or other health-care professionals are not directly involved in making the rating decisions. Health-care professionals’ involvement is generally limited to the examination component of the claim process and, on occasion, to providing opinions on such issues as whether an impairment occurred or was aggravated during service or is a secondary consequence of a service-connected condition. Health-care professionals are not asked for their judgment on the degree of disability resulting from an impairment, and they are not available to advise raters on the meaning of medical evidence while they are deciding a case.
In 2006, Veterans Benefits Administration (VBA) regional offices received over 654,000 claims for disability compensation.2 Just over 81 percent of these were reopened claims (claims that were initially denied or where the veteran was not satisfied with the disability rating) and the rest were original claims. VBA made decisions on 628,000 claims.3 It took an average of 177 days to process claims requiring compensation and pension examinations.4
A veteran who is dissatisfied with his or her rating decision may file an appeal (see Figure 1-2 for an overview of the appeal process) with the local
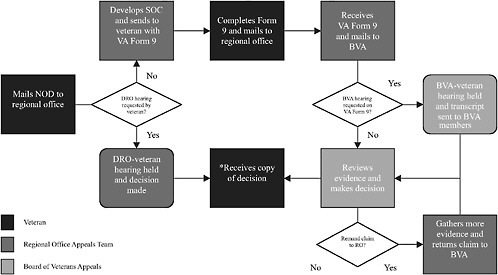
FIGURE 1-2 VA appeal process. (on facing page)
*NOTE: If a veteran is not satisfied with the decision, he or she can (1) reopen the claim with the regional office, (2) file a motion with the Board of Veterans Appeals (BVA) for reconsideration, (3) file a motion with BVA because there was clear and unmistakable error in BVA’s initial decision, or (4) file an appeal with the U.S. Court of Appeals for Veterans Claims.
• NOD (notice of disagreement): A written notice to the regional office that the veteran disagrees with the initial rating decision.
• SOC (statement of case): A detailed explanation of the evidence, laws, and regulations used by the regional office in deciding a claim.
• Form 9 (VA’s Substantive Appeal form): A form on which the veteran indicates the benefit he or she wants, any mistakes found on the SOC, and a request for a personal hearing.
• DRO (decision review officer): A regional office staff member responsible for holding post-decisional hearings and processing appeals.
regional office. Members of an appeals team working at the regional office handle these cases. When a veteran requests an appeal, he or she has the option of having an informal hearing with a regional office staff member, called a Decision Review Officer (DRO), for reconsideration of the case. If the DRO decides that the reconsideration upholds the RO’s initial decision, the appeal is moved forward for review by an administrative law judge on the Board of Veterans Appeals (BVA). Alternatively, a veteran may choose to skip the regional office hearing step and instead have a hearing with a BVA member, or have no hearing and let the claim go directly to BVA.
In 2006, VA received 101,240 appeals notices (notices of disagreement) and almost 12,000 BVA hearings were held. BVA made a total of 39,000 decisions on appeals. Of these, 19.3 percent were grants, 32 percent were remands, 46.3 percent were denials, and 2.4 percent were other dispositions. The appeals resolution time averaged 657 days.5
BVA may request a new medical examination or an independent medical opinion, but health professionals are not involved in making the appeal decision. The absence of direct involvement in the rating process by health-care professionals has raised concerns about the quality and accuracy of the assessments, particularly in cases that involve complex medical judgments (e.g., secondary and aggravation cases and multiple conditions, as discussed above). Such concerns are at the heart of the commission’s task 5. Health-care professionals involved in the claims and appeals processes are discussed throughout the remainder of this report, particularly in Chapter 5 and Appendix D.
When a veteran is found to have a ratable disability, a diagnostic code is used to show the basis for the rating and for statistical analysis. These codes do not correspond to any widely used diagnostic coding system, such as the World Health Organization’s International Classification of Diseases (ICD) or the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders (DSM). Adopting such a standardized coding system might help VA organize and analyze data for research, management, and policy development, and match and compare data across program agencies. However, changing to a new coding system could be difficult and costly.
Beyond the issue of impairment coding, there are also widely used and regularly updated disability rating systems, such as the AMA Guides to the Evaluation of Permanent Impairment, that could be used instead of the Rating Schedule and might provide for a more valid and reliable assessment process. However, changing over to such a system would be a significant departure from the current process and would require a major overhaul of the VA compensation claim system. These issues give rise to the commission’s task 3, and they are addressed in detail in Chapter 8 of this report.
In addition to regular monthly compensation payments, veterans can also qualify for additional special-purpose and ancillary benefits, including vocational rehabilitation, specially adapted homes, automobile assistance, and clothing allowance. Eligibility for these benefits is based on meeting specific qualification criteria and/or disability rating levels. For example, to qualify for vocational rehabilitation and employment services, a veteran must have a service-connected disability rated at (or likely to be rated at) 20 percent or more, as well as an “employment handicap.”6 To qualify for automobile assistance, a veteran must be rated totally and permanently disabled or have one of a specified list of service-connected impairments: loss or loss of use of one or both hands or feet; permanent impairment of vision of both eyes to a certain degree; or ankylosis of one or both knees, or one or both hips. The commission, as a part of task 2, asked IOM to evaluate whether the qualification criteria for ancillary benefits are appropriate or need to change. These issues are discussed in detail in Chapter 6 of this report.
A veteran with a rating of at least 60 percent for a single disability or 70 percent for a combination of disabilities (provided that one of the disabilities is rated at least 40 percent) can qualify for a 100 percent disability rating and compensation if he or she is unable to secure or retain employment because of the service-connected disabilities. This is known as “individual unemployability” (IU), which is considered to be one of the most controversial of the additional benefits because (1) an IU rating decision is based on an individualized assessment of the applicant’s vocational capacity rather than on the standard Rating Schedule concept of average impairment of earning capacity, and (2) the number of veterans granted IU has more than doubled between 2000 and 2006.
Generally (as noted above), the percentage disability rating is based on average impairment of earning capacity—not on any specific veteran’s actual loss of earning capacity. Consequently, some veterans who have a particular medical condition or conditions that warrant less than a 100 percent rating nevertheless may be totally precluded from engaging in employment because of the actual effects of the condition or conditions. IU allows such an individual to be compensated at 100 percent if he or she is “unable to secure or follow a substantially gainful occupation as a result of service-connected disabilities.”7 Concerns have been raised about a dramatic increase in the number of veterans receiving IU, including a high percentage of individuals receiving the benefit who are beyond the normal age of retirement. There are also concerns about the extent to which the
benefit encourages veterans to return to productive employment through vocational rehabilitation. The IU benefit is also a subject of the commission’s task 2, and is addressed in detail in Chapter 7 of this report.
To carry out its work, the committee reviewed known historical and current evidence, including detailed information on the Rating Schedule updates that have been carried out since 1945, and heard from numerous experts in the relevant subject areas. Many committee members visited regional offices in different parts of the country to try to better understand firsthand the operations of the current system, particularly the handling of claims as related to the medical questions they had been asked to address. After carefully considering this body of information, committee members put a great deal of thought into possible scenarios that might more optimally employ the structure of or improve the current system. They discussed possible alternatives to the current system as part of their effort to bring this system into the 21st century, and recommended ways both to enhance the system and to approach future research with an eye on making improvements.
The committee’s report characterizes veterans with disabilities in the 21st century (Chapter 2); defines veterans disability (Chapter 3); describes the Rating Schedule’s history and current structure (Chapter 4) and the evaluation process (Chapter 5); discusses medical criteria for ancillary benefits (Chapter 6), individual unemployability (Chapter 7), the potential role of other diagnostic classifications (e.g., the ICD and the DSM) and rating schedules (e.g., the AMA Guides) (Chapter 8), and service connection on aggravation and secondary bases (Chapter 9); and offers suggestions for building a 21st century disability evaluation system (Chapter 10). Appendix C contains the paper “The Relationship between Impairments and Earnings Losses in Multicondition Studies,” which is strategic to part of Chapter 4’s discussions. Appendix D compares the role of medical personnel in various disability benefits programs. Acronyms are provided at the front of the report, and the committee charge is found in Appendix B to assist the reader in following the text more easily and in understanding the committee’s responses to the tasks assigned by the commission. Appendix A provides biographical sketches of committee members, consultants, and staff.
REFERENCES
GAO (Government Accountability Office). 1997. VA disability compensation: Disability ratings may not reflect veterans’ economic losses. GAO/HEHS-97-9. http://www.gao.gov/archive/1997/he97009.pdf (accessed February 20, 2007).
VA (Department of Veterans Affairs). 1971. Economic validation of the Rating Schedule. In Veterans Administration proposed revision of Schedule for Rating Disabilities. Submitted to the Committee on Veterans’ Affairs, U.S. Senate, 93rd Cong., 1st Sess., February 12. Senate Committee Print No. 3. Washington, DC: U.S. Government Printing Office.
VA. 2004. VA disability compensation program legislative history. http://www.1888932-2946.ws/vetscommission/e-documentmanager/gallery/Documents/Reference_Materials/LegislativeHistory_12-2004.pdf (accessed February 10, 2007).
VA. 2006. Federal benefits for veterans and dependents. http://www.va.gov/opa/vadocs/fedben_pt1.pdf (accessed February 10, 2007).