Below is the uncorrected machine-read text of this chapter, intended to provide our own search engines and external engines with highly rich, chapter-representative searchable text of each book. Because it is UNCORRECTED material, please consider the following text as a useful but insufficient proxy for the authoritative book pages.
6 Cancer Cancer is the second-leading cause of death in the United States. Among men 50â64 years old, the group that includes most Vietnam veterans (see Table 6-1), the risk of dying from cancer nearly equals the risk of dying from heart disease, the main cause of death in the United States (US Census, 1999). About 564,830 Americans of all ages were expected to die from cancer in 2006âmore than 1,500 per day. In the United States, one-fourth of all deaths are from cancer (Jemal et al., 2006). This chapter summarizes and presents conclusions about the strength of the evidence from epidemiologic studies regarding associations between exposure to the compounds of interestâ2,4-dichlorophenoxyacetic acid (2,4-D), 2,4,5- trichlorophenoxyacetic acid (2,4,5-T) and its contaminant 2,3,7,8-tetrachloro- dibenzo-p-dioxin (TCDD), picloram, and cacodylic acidâand various types of cancer. If a new study reports on only a single type of cancer and does not revisit a previously studied population, its design information is summarized here with its results; design information on all other new studies can be found in Chapter 4; Appendix C contains cumulative tables that summarize studies that looked at multiple endpoints or involved repeatedly investigated populations that have contributed evidence to this series of reports. In an evaluation of a possible connection between herbicide exposure and risk of cancer, how exposures of study subjects were assessed is of critical importance in determining the overall relevance and usefulness of ï¬ndings. As noted in Chapter 5, there is a great variety in detail and accuracy of exposure as- sessment among studies. A few studies used biologic markers of exposure, such as the presence of a compound in serum or tissues; some developed an index of exposure from employment or activity records; and others used surrogate mea- 261
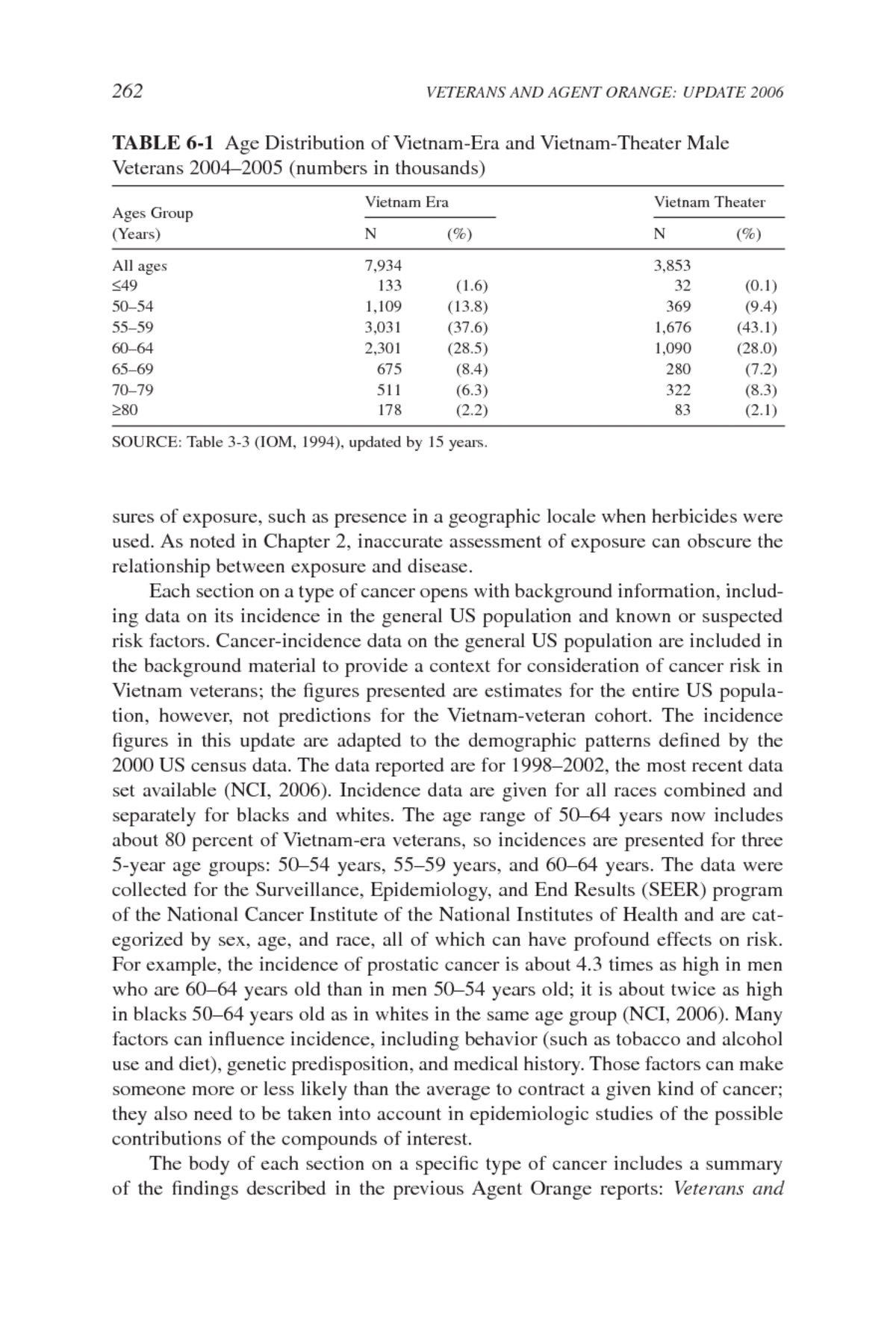
262 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-1 Age Distribution of Vietnam-Era and Vietnam-Theater Male Veterans 2004â2005 (numbers in thousands) Vietnam Era Vietnam Theater Ages Group (Years) N (%) N (%) All ages 7,934 3,853 49 133 (1.6) 32 (0.1) 50â54 1,109 (13.8) 369 (9.4) 55â59 3,031 (37.6) 1,676 (43.1) 60â64 2,301 (28.5) 1,090 (28.0) 65â69 675 (8.4) 280 (7.2) 70â79 511 (6.3) 322 (8.3) 80 178 (2.2) 83 (2.1) SOURCE: Table 3-3 (IOM, 1994), updated by 15 years. sures of exposure, such as presence in a geographic locale when herbicides were used. As noted in Chapter 2, inaccurate assessment of exposure can obscure the relationship between exposure and disease. Each section on a type of cancer opens with background information, includ- ing data on its incidence in the general US population and known or suspected risk factors. Cancer-incidence data on the general US population are included in the background material to provide a context for consideration of cancer risk in Vietnam veterans; the ï¬gures presented are estimates for the entire US popula- tion, however, not predictions for the Vietnam-veteran cohort. The incidence ï¬gures in this update are adapted to the demographic patterns deï¬ned by the 2000 US census data. The data reported are for 1998â2002, the most recent data set available (NCI, 2006). Incidence data are given for all races combined and separately for blacks and whites. The age range of 50â64 years now includes about 80 percent of Vietnam-era veterans, so incidences are presented for three 5-year age groups: 50â54 years, 55â59 years, and 60â64 years. The data were collected for the Surveillance, Epidemiology, and End Results (SEER) program of the National Cancer Institute of the National Institutes of Health and are cat- egorized by sex, age, and race, all of which can have profound effects on risk. For example, the incidence of prostatic cancer is about 4.3 times as high in men who are 60â64 years old than in men 50â54 years old; it is about twice as high in blacks 50â64 years old as in whites in the same age group (NCI, 2006). Many factors can inï¬uence incidence, including behavior (such as tobacco and alcohol use and diet), genetic predisposition, and medical history. Those factors can make someone more or less likely than the average to contract a given kind of cancer; they also need to be taken into account in epidemiologic studies of the possible contributions of the compounds of interest. The body of each section on a speciï¬c type of cancer includes a summary of the ï¬ndings described in the previous Agent Orange reports: Veterans and
CANCER 263 Agent Orange: Health Effects of Herbicides Used in Vietnam, hereafter referred to as VAO (IOM, 1994); Veterans and Agent Orange: Update 1996, referred to as Update 1996 (IOM, 1996); Update 1998 (IOM, 1999); Update 2000 (IOM, 2001); Update 2002 (IOM, 2003); and Update 2004 (IOM, 2005). That is fol- lowed by a discussion of the most recent scientiï¬c literature, a discussion of biologic plausibility, and a synthesis of the material reviewed. Where appropri- ate, the literature is discussed by exposure type (occupational, environmental, or service in Vietnam). Each section ends with the committeeâs conclusion regard- ing the strength of the evidence from epidemiologic studies. The categories of association and the committeeâs approach to categorizing the health outcomes are discussed in Chapters 1 and 2. As explained in the following paragraphs, this committee has slightly modiï¬ed the format in which it has satisï¬ed the other two aspects of its charge. Biologic plausibility corresponds to the third element of the committeeâs congressionally mandated statement of task. In previous updates, it had been discussed in the conclusion section for each health outcome after a statement of the committeeâs judgment about the adequacy of the epidemiologic evidence of an association between exposure to the compounds of interest and the outcome. In fact, the degree of biologic plausibility itself inï¬uences whether the commit- tee perceives positive ï¬ndings to be indicative of a pattern of association or the product of statistical ï¬uctuations. To provide the reader with a more logical se- quence, in this update sections on biologic plausibility have been placed between the presentation of epidemiologic evidence and the synthesis of the evidence, which leads to the committeeâs conclusion about the adequacy of the evidence to support an association. Information on biologic mechanisms that could contribute to the generic (rather than tissue- or organ-speciï¬c) carcinogenic potential of the compounds of interest is summarized in the section on biologic plausibility that precedes the synopsis of conclusions for the entire chapter. It distills toxicologic information concerning the mechanisms by which the compounds of interest affect carcino- genesis, as presented in more detail in Chapter 3; such information, of course, applies to all the cancer sites discussed individually in this chapter. When biologic plausibility is discussed in the chapterâs sections on particular cancer types, the generic information is implicit, and only toxicologic information peculiar to carcinogenesis at the site in question has been presented. Considerable uncertainty remains about the magnitude of potential risk posed by exposure to the compounds of interest. Many of the occupational, environ- mental, and veterans studies reviewed by the committee did not control fully for important confounders. There is not enough information about individual Viet- nam veterans to compare with exposures presented in scientiï¬c research studies. The committee therefore cannot accurately estimate the risk to Vietnam veterans that is attributable to exposure to the compounds of interest. Previous reports in the VAO series have had a rather formulaic statement to that effect as the third
264 VETERANS AND AGENT ORANGE: UPDATE 2006 entry in the conclusion section for each cancer type, corresponding to the second element in the committeeâs statement of task as dictated by the congressional mandate. The (at least currently) insurmountable problems of deriving meaning- ful estimates of the risks of various health outcomes to Vietnam veterans are explained in Chapter 1 and the summary of this report, but the point is no longer reiterated for every health outcome addressed. AN EXHAUSTIVE AND UNAMBIGUOUS SYSTEM FOR ADDRESSING CANCER TYPES The Department of Veterans Affairs (VA) requested that the present commit- tee ensure that evaluations of the possibility of associations between exposures to the compounds of interest and various types of cancer be framed in such a fashion that a corresponding conclusion would be available for any type of cancer that might be diagnosed in a veteran and that it would be clear which conclusion would be applicable when a veteran ï¬led a claim. VA also expressed concern that the episodic nature of the VAO series may have interfered with recognition and evaluation of cumulatively usable amounts of epidemiologic information on some uncommon cancers; in particular, VA asked for a focused examination of available information on cancer of the tonsil and acute myelogenous leukemia (AML). The committee therefore screened the studies that contributed results on the cancer types discussed in prior updates for results on tonsil cancer, AML, and other uncommon sites while gaining an over- view of how cancer sites are typically grouped to report ï¬ndings. VA had indicated that a grouping system for reporting the committeeâs con- clusions based on the International Classiï¬cation of Diseases (ICD) codes would be appropriate to match the diagnostic information presented in veteransâ claims. ICD is used to code and classify mortality data from death certiï¬cates. ICD CM (clinical modiï¬cation) is used to code and classify morbidity data from medical records, hospital records, and surveillance surveys. The 10th edition (ICD-10) came into use in 1999 and constitutes a marked change from the previous four versions that evolved into the ninth edition (ICD-9). ICD-9 was in effect from 1979 to 1998; because ICD-9 is the version most prominent in the research re- viewed in this series, it has been used when codes are given for a speciï¬c health outcome. The ï¬rst modiï¬cation made in this update toward addressing VAâs request was to change the order in which cancer types are discussed, which had evolved from the original VAO report. The more systematic order of major and minor categories of cause of death for cancer sites established by the National Institute for Occupational Safety and Health (NIOSH) is now followed with minor ex- ceptions. The NIOSH groups map the full range of ICD-9 codes for malignant neoplasms (140â208), and this somewhat coarser gradient has been adopted as an exhaustive organizing principle for the present chapter. Appendix B discusses
CANCER 265 the issue in more detail and delineates the correspondence between the NIOSH cause-of-death groupings and ICD-9 codes (Table B-1); the groupings for mortal- ity are largely congruent with those of the SEER program for cancer incidence (see Table B-2, which presents equivalences between the ICD-9 and ICD-10 systems). The groups provide a comprehensive framework for software routinely used by epidemiologists to generate expected values based on the demographics of the cohort being studied and have well-documented correspondence with the more detailed ICD coding system in its successive iterations (Robinson et al., 2006). When conditions reported on in epidemiologic research are speciï¬ed in ICD ranges, the speciï¬city may not be as reï¬ned as might be desired for some purposes, and errors of misclassiï¬cation in the research process cannot be ex- cluded, but the grouping intended is unambiguous. This rearrangement following a largely anatomic sequence should make locating a particular cancer easier for readers and facilitated the committeeâs iden- tiï¬cation of ICD codes for malignancies that had not been explicitly addressed in previous updates (as noted in italics in Table B-1). VAO reportsâ default cat- egory for any health outcome for which no epidemiologic research ï¬ndings have been recovered has always been âinadequate evidenceâ of association, which in principle is applicable to speciï¬c cancers. In this update, it still is the case that failure to review a speciï¬c cancer or other condition separately reï¬ects the paucity of information, so there is indeed inadequate or insufï¬cient information to categorize such a disease outcome. However, in response to VAâs request and in light of our review of how ârare cancersâ are grouped or presented when they do have reported results, we state here how each of these previously overlooked ICD codes will be treated in this and future updates: ⢠ICD-9 149, other buccal cavity and pharynxâroutinely included in full buccal cavity and pharynx range, 140â149. ⢠ICD-9 152, small intestineârarely reported individually; to be encom- passed in conclusions for colorectal cancers. ⢠ICD-9 156, gallbladder and extrahepatic bile ductsâto be tracked under hepatobiliary cancers. ⢠ICD-9 158â159, retroperitoneum and other and unspeciï¬ed digestive cancersârarely reported individually; to be encompassed in conclusions for colorectal cancers. ⢠ICD-9 162.0, tracheaâintended grouping with lung and bronchus has not always been explicitly stated. ⢠ICD-9 163, pleuraârarely reported individually and not as yet seen for the chemicals of interest; would be considered with mediastinum and other and unspeciï¬ed respiratory cancers. ⢠ICD-9 164.0, thymusâto be considered with thyroid and other endocrine cancers. ⢠ICD-9 164.2â164.9, mediastinumârarely reported individually and not
266 VETERANS AND AGENT ORANGE: UPDATE 2006 as yet seen for the chemicals of interest; would be considered with pleura and other and unspeciï¬ed respiratory cancers. ⢠ICD-9 165, other and unspeciï¬ed respiratory cancersârarely reported individually and not as yet seen for the chemicals of interest; would be considered with pleura and mediastinum as other respiratory cancers. ⢠ICD-9 179, unspeciï¬ed parts of uterusâto be considered with female reproductive system. ⢠ICD-9 181, placentaâto be considered with female reproductive system. ⢠ICD-9 183.2â183.9, fallopian tube and other uterine adnexaâto be con- sidered with female reproductive system. ⢠ICD-9 184, other female genital organsâto be considered with female reproductive system. ⢠ICD-9 187, penis and other male genital organsâto be considered with testis as other male reproductive organs (excluding prostate). ⢠ICD-9 189.3â189.9, urethra, paraurethral glands, and other and unspeci- ï¬ed urinaryârarely reported individually and not as yet seen for the chemicals of interest; would be considered with bladder cancer. ⢠ICD-9 190, eyeâto be considered with brain and other parts of nervous system. ⢠ICD-9 193, thyroidâto be considered with thymus and other endocrine cancers. ⢠ICD-9 194, other endocrine cancersâto be considered with thyroid and thymus as endocrine cancers. ⢠ICD-9 195, other and ill-deï¬ned sitesârarely reported individually and not as yet seen for the chemicals of interest; would be considered with other and unspeciï¬ed cancers. ⢠ICD-9, 196â198, stated or presumed to be secondary of speciï¬ed sitesâ rarely reported individually and not as yet seen for the chemicals of inter- est; would be considered with other and unspeciï¬ed cancers. ⢠ICD-9, 199, site unspeciï¬edârarely reported individually and not as yet seen for the chemicals of interest; would be considered with other and unspeciï¬ed cancers. This committeeâs search of previously reviewed studies for results on ton- sil cancer and AML also identiï¬ed sets of previously considered papers with reported ï¬ndings speciï¬cally on lip cancer (ICD-9 140) and on tongue cancer (ICD-9 141), which both fall within the range for cancers of the oral (buccal) cavity. The current update includes separate sections discussing the site-speciï¬c results. In future updates, however, ï¬ndings for these sites will be tracked on the results tables for the broader grouping that contains them: buccal cavity, nose, and pharynx (ICD-9 140â149, 160) for tonsil, tongue, and lip, and leukemias (ICD- 9 204â208) for AML. For the digestive cancers, in future updates esophageal,
CANCER 267 stomach, colorectal, hepatobiliary, and pancreatic cancers will be broken out into sections with individual conclusions. Care will be taken to specify as precisely as possible in results tables when ï¬ndings are being reported for a subsite of a particular grouping. ORAL, NASAL, AND PHARYNGEAL CANCER Oral, nasal, and pharyngeal cancers (ICD-9 140â149, 160) are found in many anatomic subsites, including the structures of the mouth (inside lining of the lips, cheeks, gums, tongue, and hard and soft palate) (ICD-9 140â145), oropharynx (ICD-9 146), nasopharynx (ICD-9 147), hypopharynx (ICD-9 148), other buccal cavity and pharynx (ICD-9 149), and nasal cavity and paranasal sinuses (ICD-9 160). Although those sites are anatomically diverse, cancers that occur in the nasal cavity, oral cavity, and pharynx are for the most part similar in descriptive epidemiology and risk factors. The exception is cancer of the nasopharynx, which has a different epidemiologic proï¬le. The American Cancer Society (ACS) estimated that about 30,990 men and women would receive a diagnosis of oral or pharyngeal cancer in the United States in 2006 and 7,430 men and women would die from these diseases (Jemal et al., 2006). Less than 10 percent as many cancers originate in the nasal cavity. Most oral, nasal, and pharyngeal cancers are squamous-cell carcinomas. Naso- pharyngeal carcinoma (NPC) is the most common malignant tumor of the naso- pharynx; it is relatively rare in the United States, where it accounts for about 0.25 percent of all cancers. There are three types of NPC: keratinizing squamous- cell carcinoma, nonkeratinizing carcinoma, and undifferentiated carcinoma. The average annual incidences reported in Table 6-2 show that men are at greater risk than women for those cancers and that the incidences increase with age, although there are few cases, and care should be exercised in interpreting the numbers. Tobacco and alcohol use are established risk factors for oral and pharyngeal cancers. Reported risk factors for nasal cancer include occupational exposure to nickel and chromium compounds (Hayes, 1997), wood dust (Demers et al., 1995), and formaldehyde (Blair and Kazerouni, 1997). Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and oral, nasal, and pharyngeal cancers. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Studies evaluated previously and in this report are summarized in Table 6-3.
268 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-2 Average Annual Incidence (per 100,000) of Nasal, Nasopharyngeal, Oral Cavity and Pharynx, and Oropharynx Cancers in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Nose, Nasal Cavity, and Middle Ear: Men 1.2 1.1 1.2 1.6 1.5 1.8 2.0 2.0 3.0 Women 0.6 0.6 0.4 1.0 1.1 0.3 1.1 1.1 1.6 Nasopharynx: Men 1.8 1.0 1.7 2.3 1.5 1.8 3.1 1.6 4.5 Women 0.7 0.3 0.8 0.6 0.3 0.3 1.2 0.6 0.4 Oral Cavity and Pharynx: Men 28.4 27.6 42.0 37.2 36.4 53.1 47.9 47.3 66.1 Women 9.2 8.7 11.6 12.6 12.7 15.5 17.3 17.5 19.0 Oropharynx: Men 1.0 0.8 3.1 1.1 1.0 3.2 2.2 2.0 6.5 Women 0.1 0.1 0.2 0.6 0.5 1.8 0.2 0.2 0.0 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational International Agency for Research on Cancer (IARC) cohort of 60,468 pulp and paper industry workers. A jobâexposure matrix (JEM) was applied to 58,162 individual work histories to estimate exposure to nonvolatile organochlorine compounds (which would include TCDD). Deaths from cancers of the oral cavity and pharynx were signiï¬- cantly fewer among those who had been exposed to nonvolatile organochlorine compounds (n 15; standardized mortality ratio [SMR] 0.51, 95% conï¬dence interval [CI] 0.29â0.85) but not among those who had never been exposed (n 33; SMR 0.92, 95% CI 0.63â1.29). Alavanja et al. (2005) reported that among the private pesticide applicators in the Agricultural Health Study (AHS), there were 66 cases of buccal-cavity can- cer, which represented a signiï¬cant deï¬cit compared with the general population (standardized incidence ratio [SIR], 0.66, 95% CI 0.51â0.83). The correspond- ing results for commercial pesticide applicators were based on much smaller numbers of cases, so the conï¬dence interval on the SIR was wide. Among the spouses of private applicators, the SIR for buccal cavity cancer was 0.73 (95% CI 0.40â1.22) on the basis of 14 cases. Nasal and pharyngeal cancers were not
CANCER 269 TABLE 6-3 Selected Epidemiologic StudiesâOral, Nasal, and Pharyngeal Cancer Estimated Exposed Relative Risk Reference Study Population a,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean IARC cohort of pulp and paper workers et al., 2006 Exposure to nonvolatile organochlorine compounds (oral cavity and pharynx) Never 33 0.9 (0.6â1.3) Ever 15 0.5 (0.3â0.9) Alavanja US Agriculture Health Studyâincidence (buccal cavity) et al., 2005 Private applicators (men and women) 66 0.7 (0.5â0.8) Lip 25 1.4 (0.9â2.1) Spouses of private applicators ( 99% women) 14 0.7 (0.4â1.2) Lip 2 1.4 (0.2â5.1) Commercial applicators (men and women) 5 0.9 (0.3â2.2) Lip 3 2.7 (0.6â8.0) Blair et al., US Agriculture Health Study (buccal cavity and pharynx) 2005a Private applicators (men and women) 5 0.3 (0.1â0.7) Spouses of private applicators ( 99% women) 0 0.0 (0â25.4) ât Mannetje Phenoxy herbicide producers (men and women) (ICD-9 et al., 2005 140â149) 2 2.8 (0.3â9.9) Lip (ICD-9 140) 0 * Mouth (ICD-9 141â145) 2 5.4 (0.7â20) Oropharynx (ICD-9 146) 0 * Nasopharynx (ICD-9 147) 0 0.0 (0.0â42) Hypopharynx and other (ICD-9 148â149) 0 * Phenoxy herbicide sprayers ( 99% men) (ICD-9 140â149) 1 1.0 (0.0â5.7) Lip (ICD-9 140) 0 * Mouth (ICD-9 141â145) 0 0.0 (0.0â7.5) Oropharynx (ICD-9 146) 0 * Nasopharynx (ICD-9 147) 1 8.3 (0.2â46) Hypopharynx and other (ICD-9 148â149) 0 * Torchio Italian licensed pesticide users et al., 1994 Buccal cavity and pharynx 18 0.3 (0.2â0.5) Reif et al., New Zealand forestry workersâincidence 1989 Buccal cavity 3 0.7 (0.2â2.2) Nasopharyngeal 2 5.6 (1.6â19.5) Studies Reviewed in Update 2004 Nordby Norwegian farmers born 1925â1971âincidence, lip et al., 2004 Reported pesticide use * 0.7 (0.4â1.0) Swaen Dutch licensed herbicide applicators et al., 2004 Nose 0 â Mouth and pharynx 0 â continued
270 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-3 Continued Estimated Exposed Relative Risk Reference Study Population a,b Casesc (95% CI)c Studies Reviewed in Update 2000 Caplan Caseâcontrol study of US men born 1929â1953, all 70 et al., 2000 nasal cancers (carcinomas, plus 11 lymphomas and 5 sarcomas) from CDC (1990a) study population Selected landscaping and forestry occupations 26 1.8 (1.1â3.1) Living or working on farm 23 0.5 (0.3â0.8) Herbicides or pesticides 19 0.7 (0.4â1.3) Phenoxy herbicides 5 1.2 (0.4â3.3) Studies Reviewed in Update 1998 Hooiveld Workers at Dutch chemical factory (lip, oral cavity, et al., 1998 pharynx) All working any time 1955â1985 1 2.3 (0.1â12.4) Cleaned up 1963 explosion 1 7.1 (0.2â39.6) Rix et al., Danish men and women paper mill workers 1998 Buccal cavity (ICD-7 140â144) Men 24 1.0 (0.7â1.5) Women 4 1.5 (0.4â3.8) Pharynx (ICD-7 145â149) Men 15 2.0 (1.1â3.3) Women 2 2.1 (0.2â7.6) Tonsil cancers among pharyngeal cancers 11 Kogevinas IARC cohort (men and women)âWorkers exposed to et al., 1997 any phenoxy herbicide or chlorophenol Oral cavity and pharynx cancer (ICD-9 140â149) 26 1.1 (0.7â1.6) Exposed to TCDD 22 1.3 (0.8â2.0) Not exposed to TCDD 3 0.5 (0.1â1.3) Nose and nasal sinuses cancer (ICD-9 160) 3 1.6 (0.3â4.7) Exposed to TCDD 0 0.0 (0.0â3.5) Not exposed to TCDD 3 3.8 (0.8â11.1) Studies Reviewed in Update 1996 Becher German phenoxy herbicide production workers (included et al., 1996 in the IARC cohort) Buccal cavity, pharynx (ICD-9 140â149) 9 3.0 (1.4â5.6) Tongue 3 * Floor of mouth 2 * Tonsil 2 * Pharynx 2 * Asp et al., Finnish herbicide applicators 1994 Buccal and pharynx (ICD-8 140â149) Incidence 5 1.0 (0.3â2.3) Mortality 0 0.0 (0.0â3.0) âOther Respiratoryâ (ICD-8 160, 161, 163)ânose, larynx, pleura Incidence 4 1.1 (0.3â2.7) Mortality 1 0.5 (0.0â2.9)
CANCER 271 TABLE 6-3 Continued Estimated Exposed Relative Risk Reference Study Population a,b Casesc (95% CI)c Studies Reviewed in VAO Blair et al., White male farmers from 23 stateâdeaths 1984â1988 1993 Lip 21 2.3 (1.4â3.5) Ronco Italian farmers (lip, tongue, salivary glands, mouth, et al., 1992 pharynx)âmortality Self-employed 13 0.9 (*) Employees 4 0.5 (*) Danish self-employed farmersâincidence Lip 182 1.8 (p 0.05) Tongue 9 0.6 (*) Salivary glands 13 0.9 (*) Mouth 14 0.5 (p 0.05) Pharynx 13 0.3 (p 0.05) Nasal cavities and sinuses 11 0.6 (*) Danish farming employeesâincidence Lip 43 2.1 (p 0.05) Tongue 2 0.6 (*) Salivary glands 0 0.0 (*) Mouth 0 0.0 (p 0.05) Pharynx 9 1.1 (*) Nasal cavities and sinuses 5 1.3 (*) Saracci IARC cohortâexposed subcohort (men and women) et al., 1991 Buccal cavity and pharynx (ICD-8 140â149) 11 1.2 (0.6â2.1) Nose and nasal cavities (ICD-8 160) 3 2.9 (0.6â8.5) Zober BASF Aktiengesellschaft accident cohortâ33 cancers et al., 1990 among 247 workers at 34-yr follow-up Squamous-cell carcinoma of tonsil 1 * Wiklund Licensed Swedish pesticide applicatorsâ et al., incidence 1989a Lip 14 1.8 (1.0â2.9) Coggon British MCPA production workers (included in the IARC et al., 1986 cohort) Lip (ICD-9 140) 0 * Tongue (ICD-9 141) 1 1.1 (0.0â6.2) Pharynx (ICD-9 146â149) 1 0.5 (0.0â3.0) Nose (ICD-9 160) 3 4.9 (1.0â14.4) Robinson Northwestern US paper and pulp workers et al., 1986 Buccal cavity and pharynx (ICD-7 140â148) 1 0.1 (0.0â0.7) Nasal (ICD-7 160) 0 â* Wiklund, Swedish men and women agricultural 1983 workersâincidence Lip 508 1.8 (1.6â2.1) Tongue 32 0.4 (0.2â0.6) Salivary glands 68 1.0 (0.7â1.4) Mouth 70 0.6 (0.5â0.8) Throat 84 0.5 (0.4â0.7) Nose and nasal sinuses 64 0.8 (0.6â1.2) continued
272 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-3 Continued Estimated Exposed Relative Risk Reference Study Population a,b Casesc (95% CI)c Hardell Residents of northern Sweden (44 nasal and 27 naso- et al., 1982 pharyngeal cancers) Phenoxy acid exposure 8 2.1 (0.9â4.7) Chlorophenol exposure 9 6.7 (2.8â16.2) Burmeister, Iowa farmersâdeaths 1971â1978 1981 Lip 20 2.1 (p 0.01) ENVIRONMENTAL Studies Reviewed in VAO Bertazzi Seveso residentsâ10-year follow-upâincidence et al., 1993 Buccal cavity (ICD-9 140â149) Zone BâMen 6 1.7 (0.8â3.9) Women 0 â* Zone RâMen 28 1.2 (0.8â1.7) Women 0 â* Nose and nasal cavity (ICD-9 160) Zone RâMen 0 â* Women 2 2.6 (0.5â13.3) VIETNAM VETERANS New Studies ADVA, Australian Vietnam veterans vs Australian 2005a populationâincidence Head and neck 247 1.5 (1.3â1.6) Navy 56 1.6 (1.1â2.0) Army 174 1.6 (1.3â1.8) Air Force 17 0.9 (0.5â1.5) ADVA, Australian Vietnam veterans vs Australian 2005b populationâmortality Head and neck 101 1.4 (1.2â1.7) Navy 22 1.5 (0.9â2.1) Army 69 1.5 (1.1â1.8) Air Force 9 1.1 (0.5â2.0) Nasal 3 0.8 (0.2â2.2) ADVA, Australian conscripted Army National Service Vietnam- 2005c era veterans: deployed vs non-deployed Head and neck Incidence 44 2.0 (1.2â3.4) Mortality 16 1.8 (0.8â4.3) Nasal Mortality 0 0.0 (0.0â48.2) Boehmer Follow-up of CDC Vietnam Experience Cohort (ICD-9 et al., 2004 140â149) 6 *
CANCER 273 TABLE 6-3 Continued Estimated Exposed Relative Risk Reference Study Population a,b Casesc (95% CI)c Studies Reviewed in Update 2004 Akhtar White AFHS subjects vs national rates (buccal cavity) et al., 2004 Ranch Hand veterans Mortalityâall 0 0.0* Incidenceâall 6 0.9 (0.4â1.9) With tours between 1966â1970 6 1.1 (0.5â2.3) Comparison veterans Mortalityâall 1 0.5* Incidenceâall 5 0.6 (0.2â1.2) With tours between 1966â1970 4 0.6 (0.2â1.4) Studies Reviewed in Update 2000 AFHS, Air Force veterans participating in 1997 exam cycle, 2000 Ranch Hands vs Comparisons Oral cavity, pharynx, and larynx 4 0.6 (0.2â2.4) Studies Reviewed in Update 1998 CDVA, Australian Vietnam veterans vs Australian 1997a populationâincidence Lip (ICD-9 140) 0 * Nasopharyngeal cancer (ICD-9 147) 2 0.5 (0.1â1.7) Nasal cavities (ICD-9 160) 2 1.2 (0.1â4.1) CDVA, Australian conscripted Army National Service Vietnam- 1997b era veteransâdeployed vs non-deployed Nasopharyngeal cancer 1 1.3 (0.0â 10) Nasal cavities 0 0 (0.0â 10) Vistainer Michigan Vietnam veterans (lip, oral cavity, pharynx) et al., 1995 Non-blacks 11 1.1 (0.5â1.9) Studies Reviewed in VAO CDC, Caseâcontrol study of US men born 1929â1953 1990a 89 Nasopharyngeal carcinomas Vietnam service 3 0.5 (0.2â1.8) 62 Nasal carcinomas Vietnam service 2 0.7 (0.2â2.9) ABBREVIATIONS: AFHS, Air Force Health Study; CDC, Centers for Disease Control and Pre- vention; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; ICD-9, International Classiï¬cation of Diseases, Ninth Edition; MCPA, methyl-4-chlorophenoxyacetic acid. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohort.
274 VETERANS AND AGENT ORANGE: UPDATE 2006 explicitly reported in the study, but the portion of them that were speciï¬cally lip cancers was analyzed (see below). Using death as the outcome among participants in the AHS, Blair et al. (2005a) reported ï¬ve deaths from buccal-cavity and pharyngeal cancers com- bined in the private applicators, indicating a signiï¬cant reduction in mortality (SMR 0.3, 95% CI 0.1â0.7). There were no deaths from these cancers among spouses of applicators. ât Mannetje et al. (2005) reported results for lip, oral cavity, and pharynx combined (ICD-9 140â149), which represented two deaths from cancer of un- speciï¬ed parts of the mouth (ICD-9 141â145) observed among the production workers and one from nasopharyngeal cancer (ICD-9 147) observed among the sprayers. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pes- ticide users from the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and (4-chloro- 2-methylphenoxy) acetic acid (MCPA). The risk estimate for cancer of the buccal cavity and pharynx was signiï¬cantly reduced (18 cases; SMR 0.34, 95% CI 0.2â0.5). The authors suggested that the healthy-worker effect contributed to the observation of reduced mortality. Reif et al. (1989) performed a series of caseâcontrol analyses on a sample of 19,904 men entered into the New Zealand Cancer Registry from 1980â1984 with an occupation speciï¬ed. They focused on the 134 registrants for whom forestry worker (presumed to be exposed to phenoxyherbicides and chlorophenols) was the most recent occupation. The three forestry workers among the 649 cases with cancer of the buccal cavity did not constitute an excess (odds ratio [OR] 0.71, 95% CI 0.23â2.19). However, two forestry workers among the 49 cases of naso- pharyngeal cancer (OR 5.56, 95% CI 1.59â19.48) did represent a signiï¬cantly increased risk. Environmental Studies No new environmental studies concerning exposure to the compounds of in- terest and oral, nasal, or pharyngeal cancers were published since Update 2004. Vietnam-Veteran Studies The report titled Cancer Incidence in Australian Vietnam Veterans Study 2005 (ADVA, 2005a) noted 247 head and neck cancers, including cancers of the tongue, gum, mouth, palate, salivary glands, tonsil, oropharynx, and nasopharynx. There was a signiï¬cant increase in the incidence of head and neck cancers (SIR 1.48, 95% CI 1.29â1.66). The results were equivalent in Navy veterans (SIR 1.55, 95% CI 1.14â1.95) and Army veterans (SIR 1.55, 95% CI 1.32â1.78), but the association was considerably weaker in Air Force veterans (SIR 0.93, 95% CI 0.54â1.49).
CANCER 275 On the basis of 101 observed deaths from head and neck cancer, The Third Australian Vietnam Veterans Mortality Study 2005 (ADVA, 2005b) reported a signiï¬cant increase in the Vietnam-veteran cohort (SMR 1.44, 95% CI 1.16â 1.73). There were 69 cases of head and neck cancer in the Army veterans (SMR 1.49, 95% CI 1.14â1.84), 22 cases in the Navy veterans (SMR 1.49, 95% CI 0.87â2.10), and 9 in the Air Force veterans (SMR 1.09, 95% CI 0.49â2.03). Those cancers were previously found to be somewhat increased in an earlier mortality study of the same cohort; CDVA (1997a) reported an SMR of 1.2 (95% CI 0.2â4.4) for nasal cancers. In commenting on the statistically signiï¬cant roughly 50 percent increase in both incidence and mortality from head and neck cancers among the Austra- lian Vietnam veterans, the authors noted that these cancers are associated with cigarette-smoking and alcohol use, but neither of these risk factors was measured or adjusted for in the reports. They commented that alcohol consumption is higher among servicemen than in the general population and that if cigarette-smoking were increased in this cohort, it also could explain some of the observed increase in head and neck cancers relative to the incidence in the general population. Another Australian study (ADVA, 2005c), which compared deployed male Army National Service veterans with their non-deployed Vietnam-era counter- parts, also reported on head and neck cancers. There were 44 cases among the deployed and 28 cases among the non-deployed, for an increased relative risk (RR) of 2.02 (95% CI 1.23â3.37) in this design aimed at accounting for factors in which the military subjects differed from the general Australian populace. With 16 deaths among the deployed and 11 among the non-deployed, the ï¬ndings on mortality from head and neck cancers were more equivocal (RR 1.82, 95% CI 0.79â4.33). Mortality due to nasal cancer was also listed in the Australian reports, but the numbers observed were too small for estimation of any stable statistics: three cases in all the Australian Vietnam veterans (ADVA, 2005b) and no deaths from nasal cancer in the deployed and one in the non-deployed (ADVA, 2005c). In the mortality update through 2000 on the Centers for Disease Control and Prevention (CDC) Vietnam Experience Study (VES) comparing deployed and non-deployed Vietnam-era veterans, Boehmer et al. (2004) reported six cases of lip, oral-cavity, or pharynx cancer (ICD-9 140â149) in the deployed and three in the non-deployed, for a crude RR of 2.0. The researchers did not consider the data sufï¬cient for the calculation of risk statistics unless there were at least 10 deaths from cancer of a given type. Biologic Plausibility A recent National Toxicology Program (NTP) study (Yoshizawa et al., 2005a) reported an increase in the incidence of gingival squamous-cell carcinoma in fe-
276 VETERANS AND AGENT ORANGE: UPDATE 2006 male rats treated orally (by gavage) with TCDD at 100 ng/kg 5 days/week for 104 weeks. Incidences of gingival squamous-cell hyperplasia were signiï¬cantly increased in all groups treated at 3â46 ng/kg. In addition, squamous-cell carci- noma in the oral mucosa of the palate was increased. Increased neoplasms of the oral mucosa were previously observed and described as carcinomas of the hard palate and nasal turbinates (Kociba et al., 1978). Kociba et al. (1978) also reported a small increase in the incidence of tongue squamous-cell carcinoma. A similar 2-year study performed in female rats failed to reveal a pathologic effect of TCDD on nasal tissues (Nyska et al., 2005). The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis The new occupational studies of cancers of the oral and nasal cavities or pharynx were generally small and so yielded unstable estimates of risk. Integra- tion of the evidence on this set of cancers is challenging because different studies group cases differently. The signiï¬cant results found in the AHS population of pesticide applicators (the incidence of buccal-cavity cancers in private applicators in the Alavanja study and mortality from buccal-cavity and pharyngeal cancers in the Blair study) were in the direction of deï¬cits rather than excess risk associated with exposure. Studies on Australian Vietnam veterans showed some increases in risk, but the results were not adjusted for cigarette-smoking or alcohol use, both of which are known risk ractors. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and oral, nasal, or pharyngeal cancers. At the request of VA, the committee attempted to ensure that the conditions making up the full array of relevant cancer types had been reviewed and reported on with the greatest appropriate degree of speciï¬city. The results suggested that some of the head and neck cancers that have been considered together in this section starting with the original VAO report might merit more individualized consideration. Such a review is complicated, however, by the fact that a speciï¬c cancer type may have been implicitly subsumed in broader groupings, particu- larly when no cases of the speciï¬c type were observed in a given study. The fol- lowing subsections, therefore, address the cumulative evidence that lip cancer, tongue cancer, or tonsil cancer might individually be associated with exposure to the herbicides used in Vietnam.
CANCER 277 Lip Cancer In the committeeâs review, at VAâs request, for cancers that may have been overlooked, a number of reported results were found speciï¬cally on lip cancer (ICD-9 140). They are evaluated as a group in this section, and information pecu- liar to lip cancer has been incorporated into Table 6-3, which presents the overall epidemiologic ï¬ndings on oral, nasal, and pharyngeal cancers. In addition to the risk factors for oral and pharyngeal cancers discussed above, exposure to sunlight is a risk factor for lip cancer. Conclusions from VAO and Updates This update considers lip cancer independently for the ï¬rst time. Prior up- dates considered lip cancer only as a possible component of the various types of cancer grouped as oral, nasal, and pharyngeal cancers, the evidence on which has been judged to be inadequate to support an association with exposure to the herbicides used in Vietnam. Summary of the Epidemiologic Literature Occupational Studies Burmeister (1981) reported cancer mortality from 1971 to 1978 in Iowa male farmers and non-farmers. Farming was deï¬ned according to the usual occupation as indicated on the death certiï¬cates. Both SMRs and proportional mortality ratios (PMRs) were computed. The SMR for lip cancer was 2.06 (p 0.01); the PMR for white male farmers less than 65 years old was 4.65 (not signiï¬cant), and the PMR for white male farmers 65 years old and older was 1.51 (p 0.05). The combined PMR over all ages was 1.62 (p 0.01). There were 20 lip-cancer deaths in farmers and 11 in non-farmers. There was no speciï¬c exposure information on the participants in the study, beyond that inferred from the indication of usual occupation on the death certiï¬cates. Wiklund (1983) linked Swedenâs National Cancer Registry with information from the 1960 census. The census categorization of occupation was determined for tumors diagnosed in the period 1961â1973. Some 19,490 persons were regis- tered as having agriculture as their economic activity although no direct pesticide or herbicide exposure is necessarily inferred. The results showed 508 cases of lip cancer, leading to an SIR of l.83 (95% CI 1.62â2.05); similarly, for men alone the SIR was 1.82. Wiklund et al. (1989a) studied 20,245 licensed Swedish pesticide applicators whose licenses were issued in 1965â1976. The vast majority of cohort members were men. Overall, the cohort had a signiï¬cantly decreased SIR for all cancers combined and for several speciï¬c cancers. There were no statistically signiï¬cant increases in risk for any cancers or any time trends. For lip cancer, there were 14 observed cases (SIR 1.75, 95% CI 0.96â2.94).
278 VETERANS AND AGENT ORANGE: UPDATE 2006 Blair et al. (1993) analyzed deaths occurring in 23 states in 1984â1988. PMRs were calculated by sex and race for farmers, who were people whose death certiï¬cates indicated farming as their usual occupation and agricultural crop products or livestock as their industry. White men had a PMR of 2.31 (95% CI 1.43â3.53) on the basis of 21 lip-cancer cases. The ï¬ndings for other raceâsex groups were not signiï¬cant and consisted of only one case. The authors noted that their mortality risk estimates in general were more likely to be underestimated than overestimated because of misclassiï¬cation of disease and occupation. Those effects are thought to be more severe than any increase in risk associated with the use of proportional rather than absolute mortality analyses. It should be noted that this study has no speciï¬c data on pesticide or herbicide exposures beyond an indirect inference associated with the death-certiï¬cate occupation. Nordby et al. (2004) reported on a cohort study of lip cancer in farmers in Norway born in 1925â1971. They were followed until 1999 to identify incident cases of lip cancer by using the national cancer registry in Norway. Exposure of cohort members was assessed through proxy measures, such as farm production, weather and fungal forecasts, and pesticide use (not peculiar to any particular agent). The results showed a statistically signiï¬cantly reduced risk of lip cancer associated with exposure to pesticides. The lip-cancer rate among those not re- porting pesticide use was 4.9 per 100,000 person-years, and the corresponding ï¬gure for pesticide users was 3.7. A multivariate model was ï¬tted to examine the effects of pesticide use and other factors, including grain farming, fungal forecasts, horses on the farm, and engagement of the farmer in the construction industry. The RR associated with pesticide use in this model was 0.7 (95% CI 0.4â1.0). The authors speculate that the reduction in risk might be associated with exposure to immunosuppressive mycotoxins, in which case pesticides would reduce the farmersâ burden of exposure by reducing mold growth. There may also be effects of sun exposure in this occupational group. Among the private pesticide applicators in the AHS, Alavanja et al. (2005) report 25 cases of lip cancer (SIR 1.43, 95% CI 0.93â2.11). There were two lip-cancer cases in the spouses of private applicators and three in commercial ap- plicators; the SIR were modestly increased with very wide conï¬dence intervals. Mortality from lip cancer was not reported in the companion AHS study (Blair et al., 2005b). Environmental Studies No new environmental studies concerning exposure to the compounds of interest and lip cancer were published since Update 2004. Vietnam-Veteran Studies The Australian veterans cohort study (CDVA, 1997a) reported that no deaths from lip cancer were observed. The updated study of mortality in Australian Vietnam veterans (ADVA, 2005b) does not mention lip cancer.
CANCER 279 Synthesis The studies reporting on lip cancer that were identiï¬ed by the committeeâs retrospective screen for results on rare cancers in the publications considered previously in the VAO series generally had very low speciï¬city with respect to exposure to the compounds of interest. Exposure status was deï¬ned almost exclusively in terms of occupation, and even the determination of occupation usually could not be regarded as rigorous. In most instances, occupation was not stringently deï¬ned and was ascertained at only one time (for example, in a census or on a death certiï¬cate). Studies that use computer techniques to link records in comprehensive da- tabases, such as those matching entries in tumor registries with compendiums of national censuses, amass large samples that may have the effect of inï¬ating power. Such investigations are useful for generating hypotheses, but suggestive ï¬ndings must be replicated by studies with more reï¬ned designs that are capable of gathering more extensive information about the subjects to use in adjusting for confounders. The certainty of the diagnostic categories may also be dubious when infor- mation is culled directly from death certiï¬cates or other databases. For lip cancer, in particular, it is unclear to what extent this diagnostic category would overlap with non-melanoma skin cancers in the sources from which the information was gathered for the studies discussed here. For lip cancer, it would be important to adjust for smoking and sunlight exposure before inferring that agricultural chemicals (perhaps in the family of phenoxy herbicides) played a role in any observed association in an occupational group. Such adjustment was not part of the analyses conducted in the studies discussed here that reported increased risks of lip cancer in occupational groups that had theoretical exposure to the compounds of interest. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and lip cancer. Tongue Cancer In the committeeâs review, at VAâs request, for cancers that may have been overlooked, a number of reported results were found speciï¬cally on tongue can- cer (ICD-9 141). They are evaluated as a group in this section, and information peculiar to tongue cancer has been incorporated into Table 6-3, which presents the overall epidemiologic ï¬ndings on oral, nasal, and pharyngeal cancers.
280 VETERANS AND AGENT ORANGE: UPDATE 2006 Conclusions from VAO and Updates This update considers tongue cancer independently for the ï¬rst time. Prior updates considered tongue cancer only as a possible component of the various types of cancer grouped as oral, nasal, and pharyngeal cancers, the evidence on which has been judged to be inadequate to support an association with exposure to the herbicides used in Vietnam. Summary of the Epidemiologic Literature Occupational Studies Among the 331,767 Swedish people who received a diagnosis of a malignant tumor in 1961â1973, Wiklund (1983) found 19,490 with agriculture indicated as their economic activity on the Swedish census. Direct pesticide or herbicide exposure cannot necessarily be inferred. The 32 cases of tongue cancer yielded a risk signiï¬cantly below the null ratio of 1 (SIR 0.40, 95% CI 0.24â0.61). The SIR for men alone was 0.35. Coggon et al. (1986) described the mortality and cancer experience of work- ers at a factory that manufactured, formulated, and sprayed MCPA and other phe- noxy acid herbicides. Overall mortality in 5,784 men employed in the company during 1947â1975 was traced until the end of 1983 and was shown to be lower than that in the national population; the picture was similar for cancer mortal- ity. The single observed death due to tongue cancerâvery close to the expected numberâled to an SMR of 0.96 with a very wide CI. An adjustment for the overall difference between urban and rural mortality led to similar results. Green (1991) conducted a cohort mortality study of forestry workers at a public electric utility in Ontario; cohort members had worked for more than 6 months during 1950â1982 and were routinely exposed to herbicides. The general population was used as a comparison. There was no overall excess mortality compared with that in the reference population. Only a single death from tongue cancer was observed; no site-speciï¬c SMR was computed. The authors noted that members of the cohort were generally still young, and at the end of the study fol- low-up period most participants had not reached ages at which the incidence of cancer would usually increase. Consequently, this study may have had relatively low power. The speciï¬c pattern of herbicide use by Ontario Hydro (the study em- ployer) was described in some detail, but there are no direct linkages of exposure to individual study participants. Ronco et al. (1992) reported nine cases of tongue cancer among men self- employed as farmers in Denmark with an SIR of 0.58 and two cases among male farm employees with an SIR of 0.63; neither result is statistically signiï¬cant. There were no incident cases of tongue cancer among Danish women. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and tongue cancer were published since Update 2004.
CANCER 281 Vietnam-Veteran Studies The Australian Veteran Cohort Study (CDVA, 1997a) investigated mortality in Australian veterans who had served in Vietnam. There were 17 deaths from tongue cancer, with a calculated SMR of 2.53. The standardized relative mortality ratio (SRMR), the SMR for a speciï¬c cancer site divided by the SMR for all other causes of death combined, was 2.34 (95% CI 1.46â3.84) and suggested a risk increase relative to the risk of other causes of death. Synthesis Interpretation of the evidence on tongue cancer is constrained by the group- ing of data on them with data on other oral cancers. Most of the studies with information on this speciï¬c tumor site observed only a small number of cases and therefore had unstable estimates of risk. Conclusion On the basis of its evaluation of the epidemiologic evidence reviewed ret- rospectively here on tongue cancer alone, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and tongue cancer. Tonsil Cancer VA asked that the committee undertake a focused examination of what information might be available on cancer of the tonsil (ICD-9 146.0â146.2), which constitutes a portion of the oropharynx (ICD-9 140). Tonsil cancer may also arise in proximal areas of the oral and throat region, including the soft palate (ICD-9 145.3), the adenoid and the pharyngeal tonsil in the posterior pharyngeal wall (ICD-9 147.1), the base of the tongue (ICD-9 141.0), and the lingual tonsil (ICD-9 141.6). Tonsil cancers are usually classiï¬ed as squamous-cell carcinomas, but the cell types found in biopsy tissue occasionally lead oral pathologists to classify some as sarcomas or lymphomas (Mayo Clinic, 2007). Tonsil cancer is somewhat more common in men than in women, and smoking and alcohol may increase the risk. The committee screened the studies that contributed results on the cancer types discussed in prior updates for results on tonsil cancer. The committeeâs ï¬ndings are discussed below, and information peculiar to tonsil cancers has been incorporated into Table 6-3, which presents the overall epidemiologic ï¬ndings on oral, nasal, and pharyngeal cancers.
282 VETERANS AND AGENT ORANGE: UPDATE 2006 Conclusions from VAO and Updates This update considers tonsil cancer independently for the ï¬rst time. Prior updates considered tonsil cancer only as a possible component of the various types of cancer grouped as oral, nasal, and pharyngeal cancers, the evidence on which has been judged to be inadequate to support an association with exposure to the herbicides used in Vietnam. Summary of the Epidemiologic Literature Zober et al. (1990) noted that a squamous-cell carcinoma of the tonsil was among the 33 cancers diagnosed in 247 workers exposed during an accident at the BASF plant in Aktiengesellschaft 34 years earlier. Becher et al. (1996) conducted an occupational cohort study of 2,479 work- ers in four industrial plants in Germany, which did not include the factory reported on by Zober et al. (1990). The factories produced various herbicides, including those known to have been contaminated with TCDD. High dioxin and furan exposures have been documented by blood fat measurements in two of the four plants. In one of the factories where TCDD contamination was so docu- mented, one case of tonsil cancer was observed in a group of buccal-cavity and pharyngeal cancers (ICD-9 140â149), which as a group had a non-signiï¬cantly increased SMR of 1.78. Rix et al. (1998) studied a cohort of 14,362 workers at Danish paper mills employed during 1943â1990. There were 17 cases of pharyngeal cancer (ICD-7 145â148) in the cohort: 15 in men (SIR 1.99, 95% CI 1.11â3.29) and 2 in women. The authors report that 11 of the 17 were in the tonsils, so the RR of tonsil cancers in particular would be about twice the corresponding RR for pharyngeal cancers as a whole. No new environmental or Vietnam-veteran studies concerning exposure to the compounds of interest and tonsil cancer were published since Update 2004. Synthesis Among all the cohort studies of populations potentially exposed to the compounds of interest reviewed by VAO committees, only Rix et al. (1998), Becher et al. (1996), and Zober et al. (1990) speciï¬cally stated an exact number of tonsil-cancer cases observed, as opposed to grouping them with the more general classiï¬cation of oral, nasal, or pharyngeal cancers. The paucity of ï¬nd- ings speciï¬cally related to tonsil cancer is a consequence of the extreme rarity of this type of cancer and its occurrence in an anatomic region whose cancers are generally grouped fairly idiosyncratically. That the tissue type developing into a neoplasm at this location might generate a carcinoma, a lymphoma, or a sarcoma has further constrained the committeeâs ability to assemble a meaning-
CANCER 283 ful body of evidence addressing risk factors for this unusual type of cancer. A caseâcontrol protocol would probably be more effective in determining whether tonsil cancer is associated with exposure to the herbicides used in Vietnam, but we have been unable to locate any publications reporting studies of this design. Anecdotal reports from veterans to VA suggest that the tonsil might be responsive to their exposure experience in Vietnam, but the likelihood of evaluating such an association convincingly is small unless primary research is conducted to address it speciï¬cally. Conclusion The committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and tonsil cancer. CANCERS OF THE DIGESTIVE ORGANS Until this update, VAO committees have reviewed âgastrointestinal tract tu- morsâ as a group consisting of stomach, colorectal, and pancreatic cancers, with esophageal cancer being formally factored in only by Update 2004. These can- cers are often subsumed under âcancers of the digestive organs,â a classiï¬cation that traditionally includes âhepatobiliary cancers,â which have been considered separately by previous VAO committees. With evidence from occupational studies now available, this update and future updates will address cancers of the diges- tive organs individually. This section presents ï¬ndings from reports since the last review that have considered cancers of the digestive organs as a group (ICD-9 150â159), which is in practice too broad for etiologic analyses; it then presents updated and integrated information on individual types of digestive cancer. Esophageal cancer (ICD-9 150), stomach cancer (ICD-9 151), colon cancer (ICD-9 153), rectal cancer (ICD-9 154), and pancreatic cancer (ICD-9 157) are among the most common cancers. ACS estimated that about 219,170 people would receive diagnoses of those cancers in the United States in 2006, and 112,670 people would die from them (Jemal et al., 2006). When other digestive cancers (for example, small intestine, anal, and hepatobiliary) were included, the 2006 estimates for the United States were about 263,060 new diagnoses and 136,180 deaths (Jemal et al., 2006). Collectively, tumors of the digestive organs were expected to account for 19 percent of new diagnoses and 24 percent of cancer deaths in 2006. The average annual incidences of gastrointestinal cancers are presented in Table 6-4. The incidences of stomach, colon, rectal, and pancreatic cancers increase with age. In general, incidence is higher in men than in women and higher in blacks than in whites. Other risk factors for the cancers vary but always include
284 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-4 Average Annual Incidence (per 100,000) of Selected Gastrointestinal Cancers in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Stomach: Men 9.2 8.0 15.9 15. 6 14.0 20.9 25.6 22.8 42.5 Women 4.7 3.6 9.2 6.9 5.7 11.3 10.5 8.5 18.6 Esophagus: Men 9.5 9.5 13.7 16.6 16.2 30.1 23.8 23.9 33.0 Women 1.8 1.3 6.3 3.3 2.8 9.5 5.3 5.0 11.7 Colon (excluding the rectum): Men 35.3 33.7 52.1 59.7 57.5 88.8 99.9 96.3 154.6 Women 27.6 25.3 43.4 43.9 40.7 74.3 71.9 69.3 112.2 Rectum and Rectosigmoid Junction: Men 24.4 23.6 26.8 35.5 35.2 32.9 52.3 51.8 48.5 Women 14.7 13.8 18.9 22.1 21.7 29.7 28.1 27.8 35.9 Liver and Intrahepatic Bile Duct: Men 16.4 12.6 33.8 18.4 13.7 38.2 23.2 17.0 30.5 Women 2.9 2.2 4.9 4.7 3.6 9.2 7.9 5.6 8.9 Pancreas: Men 12.5 12.2 20.3 21.4 20.4 34.7 33.8 33.5 45.5 Women 7.8 7.4 11.4 13.8 13.0 18.1 23.7 22.5 37.6 Small Intestine: Men 3.1 3.0 5.1 5.0 4.7 10.6 5.3 5.2 5.5 Women 1.9 1.7 4.9 2.8 2.9 3.3 4.4 4.2 7.3 Anus, Anal Canal, and Anorectum: Men 2.1 2.0 4.1 2.3 2.5 2.1 3.4 3.5 5.0 Women 2.9 3.2 3.3 3.1 3.2 4.8 3.8 4.2 3.6 Other Digestive Organs: Men 0.6 0.4 0.7 0.8 0.9 0.7 1.1 1.1 1.5 Women 0.6 0.6 0.4 0.9 0.9 1.2 0.9 1.0 0.8 Gallbladder: Men 0.4 0.4 0.5 0.9 0.7 0.7 1.6 1.7 1.5 Women 1.2 1.1 1.6 1.8 1.8 0.9 3.2 3.2 2.8 Other Biliary: Men 1.2 1.0 1.9 2.6 2.5 3.5 4.0 4.0 2.5 Women 1.0 1.0 0.8 1.5 1.4 1.2 3.2 3.4 2.0 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. family history of the same form of cancer, some diseases of the affected organ, and diet. Tobacco use is a risk factor for pancreatic cancer and possibly stomach cancer (Miller et al., 1996). Infection with the bacterium Helicobacter pylori in- creases the risk of stomach cancer. Type 2 diabetes is associated with an increased risk of cancers of the colon and pancreas (ACS, 2006).
CANCER 285 Conclusions from VAO and Updates The committee responsible for VAO concluded that there was limited or sug- gestive evidence of no association between exposure to the compounds of interest and gastrointestinal tract tumors (stomach, colon, rectal, and pancreatic tumors; esophageal tumors are included later). The evidence associated with hepatobili- ary cancers was judged inadequate to support an association with exposure to the compounds of interest. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change those conclusions. Update of the Epidemiologic Literature on All Cancers of the Digestive Organs Occupational Studies Since the last update, three occupational studies have reported data on all gastrointestinal and hepatic sites analyzed collectively. ât Mannetje et al. (2005) completed a mortality study in New Zealand of 813 TCDD-exposed phenoxy her- bicide producers and 699 sprayers whose vital status was followed to 2000 from 1969 and 1973, respectively. Among producers and sprayers, rates of digestive cancers overall (including hepatic tumors, ICD-9 150â159) were not higher than expected (for producers: SMR 1.38, 95% CI 0.77â2.28; for sprayers: SMR 1.15, 95% CI 0.66â1.87). Reported results on speciï¬c tumor sites are discussed in subsections below. Alavanja et al. (2005) reported cancer incidence in a prospective cohort study of private pesticide applicators, commercial applicators, and spouses of farmer applicators followed for an average of 7.2 years. Cancer cases were identiï¬ed through cancer registry ï¬les in North Carolina and Iowa. The incidence of diges- tive system cancers (including liver and gallbladder cancers) was signiï¬cantly lower than expected in private applicators (SIR 0.83, 95% CI 0.76â0.91) and their spouses (SIR 0.85, 95% CI 0.72â0.99). The incidence in commercial ap- plicators was close to the expected (SIR 0.97, 95% CI 0.62â1.44). Blair et al. (2005a) reported cancer mortality in the same prospective cohort study of pesticide applicators and spouses in North Carolina and Iowa. After an average of only 5.3 years of follow-up, a reduction in the overall risk of digestive cancers was reported in the private applicators (SMR 0.7, 95% CI 0.6â0.8) and a more modest reduction in their spouses (SMR 0.9, 95% CI 0.7â1.2). Environmental Studies No new environmental studies concerning exposure to the compounds of interest and digestive system cancers were published since Update 2004.
286 VETERANS AND AGENT ORANGE: UPDATE 2006 Vietnam-Veteran Studies In a set of three reports updating the health status of Australian Vietnam veterans, results concerning possible associations between Vietnam service and gastrointestinal cancers were reported; colorectal and stomach cancers were combined, and hepatobiliary cancers were reported separately. The SIR for gas- trointestinal cancers was 1.05 (95% CI 0.97â1.12) when veterans were compared with the general population of Australia (ADVA, 2005a). Mortality from gastroin- testinal cancers was unaffected (SMR 0.96, 95% CI 0.86â1.06) when veterans were compared with the general population (ADVA, 2005b). A separate report compared the rates of gastrointestinal cancer in deployed and non-deployed National Service Vietnam veterans (ADVA, 2005c); the increase in incidence in the deployed did not reach signiï¬cance (RR 1.06, 95% CI 0.82â1.36), and the RR of death from gastrointestinal cancer was not increased (RR 0.81, 95% CI 0.52â1.24). Pavuk et al. (2005) analyzed the cancer incidence in 1,482 US Air Force veterans who were referent controls for the Ranch Hand subjects in the Air Force Health Study. The veterans had served in Southeast Asia, primarily conducting transport missions while stationed in Taiwan, the Philippines, Guam, Japan, or Thailand. The 24 cases of digestive system cancer (not explicitly deï¬ned) yielded an RR of 1.8 (95% CI 0.8â3.9) on the basis of serum TCDD concentrations (the natural logarithm was used in a Cox model). The highest quartile of TCDD (5.2â54.8 pg/g of lipid) was associated with an RR of digestive system cancer of 3.3 (95% CI 0.9â12.5). In contrast, on the basis of the number of years served in Southeast Asia, the overall RR of digestive system cancer was somewhat more convincingly increased (RR 1.2, 95% CI 1.0â1.4), but the highest quartile for this measure of exposure (3.7â16.4 years) was associated with an RR of 2.1 (95% CI 0.6â7.3). In analyses of Ranch Hand subjects themselves (Akhtar et al., 2004) discussed in Update 2004, there was no suggestion of an association between herbicide exposure in Vietnam and digestive system cancers. Esophageal Cancer Epithelial tumors of the esophagus (squamous-cell carcinomas and adeno- carcinomas) are responsible for more than 95 percent of all esophageal cancers (ICD-9 150); 14,550 newly diagnosed cases and 13,770 deaths were estimated for 2006 (Jemal et al., 2006). The considerable geographic variation in the incidence of esophageal tumors suggests that multifactorial etiology is responsible. Rates of esophageal cancer have been increasing in the last 2 decades. Adenocarcinoma of the esophagus has slowly replaced squamous-cell carcinoma as the most com- mon type of esophageal malignancy in the United States and western Europe (Blot and McLaughlin, 1999). Squamous-cell esophageal carcinoma is seen more commonly in blacks than in whites and in men than in women. Smoking
CANCER 287 and alcohol ingestion are also associated with the development of squamous- cell carcinoma. Smoking and alcohol are less well linked to the development of esophageal adenocarcinoma. The rapid increase in obesity in the United States has been linked to increasing rates of gastroesophageal reï¬ux disease, and the rise in chronic inï¬ammation has been linked to the observed increase in esophageal adenocarcinoma. Conclusions from VAO and Updates This update considers esophageal cancer independently for the ï¬rst time. Prior updates developed a table of results for esophageal cancer, but conclusions about the adequacy of the evidence of its association with herbicide exposure were reached in the context of gastrointestinal tract cancers. Table 6-5 summa- rizes the results of the relevant studies concerning esophageal cancer. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. A JEM was applied to 58,162 individual work histories to estimate exposure to nonvolatile organochlorine compounds (which would include TCDD). Death from esophageal cancer was not more strongly associated with having ever been exposed to nonvolatile organo- chlorine compounds (n 26; SMR 0.78, 95% CI 0.51â1.15) than with having never been exposed (n 27; SMR 0.71, 95% CI 0.41â1.03). In the mortality study of phenoxy herbicide producers and sprayers in New Zealand (ât Mannetje et al., 2005), the numbers of observed and expected deaths from esophageal cancer were so small that the estimated risks in the producer group (SMR 1.94, 95% CI 0.24â7.02) and in the sprayer group (SMR 0.72, 95% CI 0.0â3.99) were in effect indeterminate. In their study of cancer incidence in private and commercial pesticide ap- plicators and in the spouses of the private applicators in the AHS, Alavanja et al. (2005) did not report results separately for esophageal cancer. Reporting on cancer mortality in the same prospective cohort study, Blair et al. (2005a) found death from esophageal cancer to be less frequent than expected in the private applicators (SMR 0.5, 95% CI 0.3â0.9); only one case was observed in their spouses. Lee et al. (2004a) conducted a population-based caseâcontrol study of 170 cases of adenocarcinoma of the stomach and 137 cases of adenocarcinoma of the esophagus during 1988â1993. Controls were randomly selected from the same geographic area. Living on a farm, duration of farming, and having ever used herbicides were not associated with an increased risk of either type of cancer. No indication of increased risk of esophageal cancer was observed in connection with self-reported use of phenoxy herbicides, 2,4,5-T, or 2,4-D.
288 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-5 Selected Epidemiologic StudiesâEsophageal Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean IARC cohort of pulp and paper workers et al., 2006 Exposure to nonvolatile organochlorine compounds Never 27 0.7 (0.4â1.0) Ever 26 0.8 (0.5â1.2) Blair et al., US Agriculture Health Study 2005a Private applicators (men and women) 16 0.5 (0.3â0.9) Spouses of private applicators ( 99% women) 1 0.3 (0.1â1.9) ât Mannetje Phenoxy herbicide producers (men and women) 2 2.0 (0.2â7.0) et al., 2005 Phenoxy herbicide sprayers ( 99% men) 1 0.7 (0.0â4.0) Lee et al., Population-based caseâcontrolâagricultural pesticide 2004a use and adenocarcinoma of the esophagus 137 Insecticides 0.7 (0.4â1.1) Herbicides 0.7 (0.4â1.2) Reif et al., New Zealand forestry workersânested caseâcontrol 1989 (incidence) correspondence 4 1.8 (0.7â4.8) Magnani UK caseâcontrol et al., 1987 Herbicides * 1.6 (0.7â3.6) Chlorophenols * 1.2 (0.7â2.2) Studies Reviewed in Update 1998 Kogevinas IARC cohort (men and women) et al., 1997 Workers exposed to any phenoxy herbicide or chlorophenol 28 1.0 (0.7â1.4) Exposed to TCDD (or higher-chlorinated dioxins) 20 1.3 (0.8â1.9) Not exposed to TCDD (or higher-chlorinated dioxins) 6 0.5 (0.2â1.1) Studies Reviewed in Update 1996 Asp et al., Finnish herbicide applicatorsâincidence 3 1.6 (0.3â4.6) 1994 Finnish herbicide applicatorsâmortality 2 1.3 (0.2â4.7) Studies Reviewed in VAO Ronco et al., Danish farm workersâincidence 1992 MenâSelf-employed 32 0.4 (p 0.05) Employee 13 0.9 (*) WomenâSelf-employed 1 1.4 (*) Family worker 2 0.4 (*) Saracci et al., IARC cohortâexposed subcohort (men and women) 8 0.6 (0.3â1.2) 1991 Coggon British MCPA production workers (included in the et al., 1986 IARC cohort) 8 0.9 (0.4â1.9) Wiklund, Swedish men and women agricultural 1983 workersâincidence 169 0.6 (0.5â0.7)
CANCER 289 TABLE 6-5 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c ENVIRONMENTAL None VIETNAM VETERANS New Studies ADVA, Australian male Vietnam veterans vs Australian 2005a populationâincidence 70 1.2 (0.9â1.5) Navy 19 1.6 (0.9â2.4) Army 40 1.1 (0.7â1.4) Air Force 11 1.5 (0.8â2.8) ADVA, Australian male Vietnam veterans vs Australian 2005b populationâMortality 67 1.1 (0.8â1.3) Navy 13 1.0 (0.5â1.7) Army 42 1.0 (0.7â1.3) Air Force 12 1.5 (0.8â2.6) ADVA, Australian male conscripted Army National Service 2005c Vietnam-era veterans: deployed vs non-deployed Incidence 9 1.9 (0.6â6.6) Mortality 10 1.3 (0.5â3.6) Boehmer Follow-up of CDC Vietnam Experience Cohort 6 1.2 (0.4â4.0) et al., 2004 Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 23 1.2 (0.7â1.7) CDVA, 1997b Australian national service Vietnam veterans 1 1.3 (0.0â 10) ABBREVIATIONS: ADVA, Australian Department of Veteran Affairs; CDVA, Commonwealth De- partment of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; ICD-9, International Classiï¬cation of Diseases, Ninth Edition; MCPA, methyl-4-chloro- phenoxyacetic acid. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. Studies in italics have been superseded by newer studies of the same cohort. Starting with the 19,904 men entered into the the New Zealand Cancer Reg- istry from 1980â1984 with a speciï¬ed occupation, Reif et al. (1989) contrasted the 385 cases of esophageal cancer with the remaining subjects having other types of cancer. Of the 134 cancer registrants for whom forestry worker (with presumed exposure to phenoxyherbicides and chlorophenols) was the most recent occupation, the proportion with esophageal cancer (4 cases; OR 1.77, 95% CI 0.66â4.75) was not signiï¬cantly elevated.
290 VETERANS AND AGENT ORANGE: UPDATE 2006 Magnani et al. (1987) reported a caseâcontrol mortality study of 244 cases of esophageal cancer and 935 controls in the UK. A JEM was used to predict ex- posures to various chemical agents on the basis of job title as indicated on death certiï¬cates. Estimates of risk of esophageal cancer associated with exposure to herbicides (RR 1.6, 95% CI 0.7â3.6) and chlorophenols (RR 1.2, 95% CI 0.7â2.2) were not signiï¬cantly increased. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and esophageal cancer were published since Update 2004. Vietnam-Veteran Studies In reports updating the health status of Australian Vietnam veterans, 70 cases of esophageal cancer were diagnosed (SIR 1.22, 95% CI 0.94â1.51) (ADVA, 2005a), and there were 67 deaths from esophageal cancer (SMR 1.06, 95% CI 0.81â1.32) (ADVA, 2005b). In a separate study of diagnoses and deaths in deployed and non-deployed National Service veterans, the trend toward an increased rate of esophageal cancer remained with an RR of 1.93 (95% CI 0.61â6.59) for incidence and an RR of 1.33 (95% CI 0.50â3.55) for mortality based on nine observed cases (ADVA, 2005c). In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported six esophageal-cancer deaths in the deployed and ï¬ve in the non- deployed (crude rate ratio [CRR], 1.2, 95% CI 0.4â4.0). Biologic Plausibility The committee did not ï¬nd any new studies that supported the biologic plau- sibility of an association of exposure to the compounds of interest and esophageal cancer. The biologic plausibility of the carcinogenicity of the compounds of inter- est in general is summarized at the end of this chapter. Synthesis Previous updates did not review the risk of esophageal cancer separately. Reviewing the epidemiologic studies of esophageal cancer to date yielded no evidence of an increased risk associated with the compounds of interest. The recent updates of the health status of the Australian Vietnam veterans present an interesting but non-signiï¬cant pattern of increased risk of esophageal cancer. No toxicologic studies provide evidence of biologic plausibility of an association between the compounds of interest and tumors of the esophagus. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient
CANCER 291 evidence to determine whether there is an association between exposure to the compounds of interest and esophageal cancer. Stomach Cancer The incidence of stomach cancer (ICD-9 151) increases in people 50â64 years old. ACS estimated that in 2006 13,400 men and 8,880 women would develop new cases of stomach cancer and 6,690 men and 4,740 women would die from it (Jemal et al., 2006). In general, the incidence is higher in men than in women and higher in blacks than in whites. Other risk factors include family history of this cancer, some diseases of the stomach, and diet. Infection with the bacterium Helicobacter pylori increases the risk of stomach cancer. Tobacco use, consumption of salt-preserved food, and a high salt intake may also increase the risk of stomach cancer (Key et al., 2004; Miller et al., 1996). Conclusions from VAO and Updates This update considers stomach cancer independently for the ï¬rst time. Prior updates developed a table of results for stomach cancer, but conclusions about the adequacy of the evidence of its association with herbicide exposure have been reached in the context of gastrointestinal tract cancers. Table 6-6 summarizes the results of the relevant studies concerning stomach cancer. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. A JEM was applied to 58,162 individual work histories to estimate exposure to nonvolatile organochlorine com- pounds (which would include TCDD). Death from stomach cancer was not more strongly associated with having ever been exposed to nonvolatile organochlorine compounds (n 98; SMR 0.89, 95% CI 0.72â1.08) than with having never been exposed (n 146; SMR 0.93, 95% CI 0.79â1.10). In the mortality study of phenoxy herbicide producers and sprayers in New Zealand (ât Mannetje et al., 2005), the numbers of observed and expected deaths from stomach cancer among producers (n 2) and sprayers (n 3) were so small that the estimated risks were in effect indeterminate. In their study of cancer incidence in private and commercial pesticide ap- plicators and the spouses of the private applicators in the AHS, Alavanja et al. (2005) did not report results separately for stomach cancer. Reporting on cancer mortality in the same prospective cohort study, Blair et al. (2005a) found death from stomach cancer to be reduced in the private applicators (SMR 0.5, 95% CI 0.2â1.0) and as expected in their spouses (SMR 1.1, 95% CI 0.3â2.8). Lee et al. (2004a) conducted a population-based caseâcontrol study of 170 cases of adenocarcinoma of the stomach and 137 cases of adenocarcinoma of the esophagus in 1988â1993. Controls were randomly selected from the same
292 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-6 Selected Epidemiologic StudiesâStomach Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 146 0.9 (0.8â1.1) Ever 98 0.9 (0.7â1.1) Alavanja et al., 2005 US Agriculture Health Studyâincidence Private applicators (men and women) 462 0.8 (0.8â0.9) Spouses of private applicators ( 99% women) 161 0.9 (0.7â1.0) Commercial applicators (men and women) 24 1.0 (0.6â1.4) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 10 0.5 (0.2â1.0) Spouses of private applicators ( 99% women) 4 1.1 (0.3â2.8) ât Mannetje et al., Phenoxy herbicide producers (men and 2005 women) 2 1.1 (0.1â4.0) Phenoxy herbicide sprayers ( 99% men) 3 1.4 (0.3â4.0) Lee et al., 2004a Population-based caseâcontrolâ agricultural pesticide use and adenocarcinoma of the stomach 170 Insecticides 0.9 (0.6â1.4) Herbicides 0.9 (0.5â1.4) Torchio et al., 1994 Italian licensed pesticide users 126 0.7 (0.6â0.9) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 13 2.2 (1.3â3.9) Studies Reviewed in Update 2004 Bodner et al., 2003 Dow production workers (included in the IARC cohort and the NIOSH Dioxin Registry) â 1.5 (0.7â2.7) Swaen et al., 2004 Dutch licensed herbicide applicators 3 0.4 (0.1â1.3)d Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) Digestive organs and peritoneum 16 0.7 (0.4â1.2) Studies Reviewed in Update 2000 Steenland et al., 1999 US chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 13 1.0 (0.6â1.8) Hooiveld et al., 1998 Dutch chemical production workers (included in the IARC cohort) 3 1.0 (0.2â2.9)
CANCER 293 TABLE 6-6 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Rix et al., 1998 Danish paper mill workersâincidence Men 48 1.1 (0.8â1.4) Women 7 1.0 (0.4â2.1) Studies Reviewed in Update 1998 Gambini et al., 1997 Italian rice growers 39 1.0 (0.7â1.3) Kogevinas et al., 1997 IARC cohort (men and women) Workers exposed to any phenoxy herbicide or chlorophenol 72 0.9 (0.7â1.1) Workers exposed to TCDD (or higher-chlorinated dioxins) 42 0.9 (0.7â1.2) Workers not exposed to TCDD (or higher-chlorinated dioxins) 30 0.9 (0.6â1.3) Becher et al., 1996 German production workers (included in the IARC cohort) Plant I 12 1.3 (0.7â2.2) Plant II 0 â Plant III 0 â Plant IV 2 0.6 (0.1â2.3) Ott and Zober, 1996 BASF employeesâincidence 3 1.0 (0.2â2.9) TCDD g/kg of body weight 0.1 0 0.0 (0.0â3.4) 0.1â0.99 1 1.3 (0.0â7.0) 1t 2 1.7 (0.2â6.2) Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 4 1.7 (0.5â4.3) 15-year latency 3 1.8 (0.4â5.2) Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 657 1.0 (1.0â1.1) White women 12 1.2 (0.6â2.0) Bueno de Mesquita Dutch phenoxy herbicide workers et al., 1993 (Included in the IARC cohort) 2 0.7 (0.1â2.7) Collins et al., 1993 Monsanto Company workers (included in NIOSH cohort) 0 0.0 (0.0â1.1) Kogevinas et al., 1993 IARC cohortâwomen 1 1.4* Studies Reviewed in VAO Ronco et al., 1992 Danish farm workersâincidence Men 286 0.9* Women 5 1.0* Swaen et al., 1992 Dutch licensed herbicide applicators 1 0.5 (0.0â2.7)d Fingerhut et al., 1991 NIOSHâentire cohort 10 1.0 (0.5â1.9) 1-year exposure; 20-year latency 4 1.4 (0.4â3.5) continued
294 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-6 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Manz et al., 1991 German production workersâmen and women (included in the IARC cohort) Men 12 1.2 (0.6â2.1) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 40 0.9 (0.6â1.2) Wigle et al., 1990 Canadian farmers 246 0.9 (0.8â1.0) Zober et al., 1990 BASF employeesâbasic cohort 3 3.0 (0.8â7.7)e Alavanja et al., 1989 USDA forest or soil conservationists 9 0.7 (0.3â1.3) Henneberger et al., New Hampshire pulp and paper 1989 workers 5 1.2 (0.4â2.8) Solet et al., 1989 US paper and pulp workers 1 0.5 (0.1â3.0) Alavanja et al., 1988 USDA agricultural extension agents 10 0.7 (0.4â1.4) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0 â (0.0â3.7) Thomas, 1987 US ï¬avor and fragrance chemical plant workers 6 4.2 Expected Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 26 0.9 (0.6â1.3) Robinson et al., 1986 Northwestern US paper and pulp workers 17 1.2 (0.8â1.9)e Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) Men 12 1.3* Women 1 0.7* Blair et al., 1983 Florida pesticide applicators 4 3.3 Expected Burmeister et al., 1983 Iowa residentsâfarming exposures 1,812 1.3 (p 0.05) Wiklund, 1983 Swedish male and female agricultural workersâincidence 2,599 1.1 (1.0â1.2)f Burmeister, 1981 Iowa farmers 338 1.1 (p 0.01) Axelson et al., 1980 Swedish railroad workersâtotal exposure 3 2.2* ENVIRONMENTAL Studies Reviewed in Update 2004 Fukuda et al., 2003 Residents of municipalities in Japan with or without waste incineration plants Age-adjusted mortality (100,000) 38.2 7.8 vs in men 39.0 8.8 (p 0.29) Age-adjusted mortality (100,000) in 20.7 5.0 vs women 20.7 5.8 (p 0.92) Studies Reviewed in Update 2002 Revich et al., 2001 Residents of Chapaevsk, Russia Men 59 1.7 (1.3â2.2) Women 45 0.7 (0.5â0.9)
CANCER 295 TABLE 6-6 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zones A, Bâmen 16 0.9 (0.5â1.5) women 11 1.0 (0.6â1.9) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Aâwomen 1 0.9 (0.0â5.3) Zone Bâmen 10 0.8 (0.4â1.5) women 7 1.0 (0.4â2.1) Zone Râmen 76 0.9 (0.7â1.1) women 58 1.0 (0.8â1.3) Svensson et al., 1995 Swedish ï¬shermenâmortality (men and women) East coast 17 1.4 (0.8â2.2) West coast 63 0.9 (0.7â1.2) Swedish ï¬shermenâincidence (men and women) East coast 24 1.6 (1.0â2.4) West coast 71 0.9 (0.7â1.2) Studies Reviewed in Update 1996 Bertazzi et al., 1993 Seveso residentsâ10-year follow-upâincidence Zone Bâmen 7 1.0 (0.5â2.1) women 2 0.6 (0.2â2.5) Zone Râmen 45 0.9 (0.7â1.2) women 25 1.0 (0.6â1.5) Studies Reviewed in VAO Pesatori et al., 1992 Seveso residentsâincidence Zones A, Bâmen 7 0.9 (0.4â1.8) women 3 0.8 (0.3â2.5) Bertazzi et al., 1989a Seveso residentsâ10-year follow-up Zones A, B, Râmen 40 0.8 (0.6â1.2) women 22 1.0 (0.6â1.5) Bertazzi et al., 1989b Seveso residentsâ10-year follow-up Zone Bâmen 7 1.2 (0.6â2.6) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 104 0.9 (0.7â1.1) Navy 28 1.1 (0.7â1.6) Army 66 0.9 (0.7â1.1) Air Force 10 0.7 (0.3â1.3) continued
296 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-6 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 76 0.9 (0.7â1.2) Navy 22 1.3 (0.8â1.8) Army 50 0.9 (0.7â1.2) Air Force 4 0.4 (0.1â1.0) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 11 0.6 (0.2â1.2) Mortality 7 0.7 (0.2â2.0) Pavuk et al., 2005 White Air Force comparison subjects only (digestive system)âincidence Serum TCDD levels (pg/g), based on model with exposure variable loge(TCDD)f Per unit increase of -loge(TCDD) in pg/g 24 1.8 (0.8â3.9) Quartiles (pg/g) 0.4â2.6 4 â* 2.6â3.8 3 1 (0.2â4.8) 3.8â5.2 7 2 (0.5â8.2) 5.2 10 3.3 (0.9â12.5) Number of years served in Southeast Asia (SEA) Per year of service 24 1.2 (1â1.4) Quartiles (years in SEA) 0.8â1.3 4 1.3â2.1 4 1 (0.2â3.8) 2.1â3.7 5 1.1 (0.3â4.2) 3.7â16.4 11 2.1 (0.6â7.3) Boehmer et al., 2004 Follow-up of CDC Vietnam Experience Cohort (stomach) 5 â* Studies Reviewed in Update 2004 Akhtar et al., 2004 Air Force Ranch Hand veteransâ cancer of the digestive system All Ranch Hand veterans Incidence (SIR) 16 0.6 (0.4â1.0) Mortality (SMR) 6 0.4 (0.2â0.9) Veterans, tours 1966â1970âincidence 14 0.6 (0.4â1.1) White Air Force comparison veteransâ cancer of the digestive system All comparison veterans Incidence (SIR) 31 0.9 (0.6â1.2) Mortality (SMR) 14 0.7 (0.4â1.1) Veterans, tours 1966â1970âincidence 24 0.9 (0.6â1.3)
CANCER 297 TABLE 6-6 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 32 1.1 (0.7â1.4) CDVA, 1997b Australian national service Vietnam veterans 4 1.7 (0.3â 10) Studies Reviewed in VAO Breslin et al., 1988 Army Vietnam veterans 88 1.1 (0.9â1.5) Marine Vietnam veterans 17 0.8 (0.4â1.6) Anderson et al., 1986b Wisconsin Vietnam veterans 1 â* ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; NIOSH, National Institute for Occupational Safety and Health; NS, not signiï¬cant; MCPA, 2 methyl-4-chlorophenoxyacetic acid; TCDD, 2,3,7,8-tetrachlo- rodibenzo-p-dioxin; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d Risk estimate is for stomach and small intestine. e 90% CI f 99% CI. g Incidence rates provided in absence of information on exposed cases or estimated relative risk for morbidity. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohort. geographic area. Living on a farm, duration of farming, and having ever used herbicides were not associated with an increased risk of either type of cancer. No indication of an increased risk of stomach cancer was observed in association with self-reported use of phenoxy herbicides (OR 0.8, 95% CI 0.5â1.5), 2,4,5-T (OR 0.7, 95% CI 0.3â1.7), or 2,4-D (OR 0.8, 95% CI 0.4â1.3). Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics re- ports as having high herbicide use, especially of 2,4-D and MCPA. The estimated risk of dying from stomach cancer was signiï¬cantly reduced among the licensed pesticide users (126 cases; SMR 0.72, 95% CI 0.6â0.86) when compared with regional and provincial populations. The authors suggested that the relatively short duration of follow-up and the healthy-worker effect contributed to the ob- servation of a reduction in mortality. Starting with the 19,904 men entered into the the New Zealand Cancer Reg- istry from 1980â1984 with a speciï¬ed occupation, Reif et al. (1989) contrasted the 1,014 cases of stomach cancer with the remaining subjects having other types of cancer. Of the 134 cancer registrants for whom forestry worker (with
298 VETERANS AND AGENT ORANGE: UPDATE 2006 presumed exposure to phenoxyherbicides and chlorophenols) was the most recent occupation, the proportion with stomach cancer (13 cases; OR 2.22, 95% CI 1.26â3.91) was signiï¬cantly elevated. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and stomach cancer were published since Update 2004. Vietnam-Veteran Studies In the three reports updating the health status of Australian Vietnam veterans, 104 diagnoses of stomach cancer (SIR 0.89, 95% CI 0.72â1.07) and 76 deaths (SMR 0.94, 95% CI 0.73â1.15) were reported (ADVA, 2005a,b). No increase was reported in the National Service veteran study that examined the healthy-warrior effect (ADVA, 2005b). In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported ï¬ve stomach-cancer deaths in the deployed and three in the non- deployed. The researchers did not consider the data sufï¬cient for the calculation of risk statistics unless there were at least 10 deaths from a type of cancer. Biologic Plausibility No animal studies have reported an increased incidence of gastrointestinal cancer after exposure to the compounds of interest. However, treatment with TCDD in some animal models (female hairless mice) has been reported to result in hyperplasia of mucous cells in the fundic region of the stomach (Hebert et al., 1990). In addition, a transgenic mouse bearing a constitutively active form of the aryl hydrocarbon receptor (AhR) has been shown to develop stomach tumors (Andersson et al., 2002a). The tumors are neither dysplastic nor metaplastic but are indicative of both squamous and intestinal type metaplasia (Andersson et al., 2005). The validity of the transgenic animal model is indicated by the similarities in the phenotype of the transgenic animal (increased relative weight of the liver and heart, decreased weight of the thymus, and increased expression of the AhR target gene CYP1A1) and animals treated with TCDD (Brunnberg et al., 2006). The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis The risk of stomach cancers has not been reviewed separately in previous updates. Among the newly reviewed studies, only Reif et al. (1989) reported a signiï¬cant relationship, which was between stomach cancer and the rather non- speciï¬c exposure of being a forestry worker. There is some evidence of biologic plausibility in animal models, but the epidemiologic studies to date do not sup- port an association between exposure to the compounds of interest and stomach cancer.
CANCER 299 Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and stomach cancer. Colorectal Cancer Colorectal cancers include malignancies of the colon (ICD-9 153) and of the rectum and anus (ICD-9 154); less prevalent tumors of the small intestine (ICD- 9 152) are frequently included in this grouping. Should any ï¬ndings on cancers of the retroperitoneum and other and unspeciï¬ed digestive organs (ICD-9 159) be found, they will be considered in this category. Colorectal cancers account for about 55 percent of digestive tumors; ACS estimated that in 2006 148,610 people would develop new cases and 55,170 would die from the cancers in the United States (ACS, 2006). Excluding basal-cell and squamous-cell skin cancers, colorectal cancer is the third-most common form of cancer both in men and in women. The incidence of colorectal cancer increases with age; it is higher in men than in women and in blacks than in whites. Because it is recommended that all persons over 50 years old receive colon-cancer screening, screening can affect incidence rates. Other risk factors include family history of this form of cancer, some diseases of the intestines, and diet. Type 2 diabetes is associated with an increased risk of cancer of the colon (ACS, 2007a). Conclusions from VAO and Updates This update considers colorectal cancer independently for the ï¬rst time. Prior updates developed tables of results for colon and rectal cancer, but conclusions about the adequacy of the evidence of their association with herbicide exposure have been reached only in the context of gastrointestinal tract cancers. Tables 6-7 and 6-8 summarize the results of the relevant studies concerning colon and rectal cancers, respectively. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. A JEM was applied to 58,162 individual work histories to estimate exposure to nonvolatile organochlorine com- pounds (which would include TCDD). Death from colon cancer was signiï¬cantly decreased among those who had been exposed to nonvolatile organochlorine com- pounds (n 62; SMR 0.74, 95% CI 0.57â0.95) but not among those who had never been exposed (n 106; SMR 1.04, 95% CI 0.85â1.25). Death from rectal
300 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-7 Selected Epidemiologic StudiesâColon Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 106 1.0 (0.9â1.3) Ever 62 0.7 (0.6â1.0) Alavanja et al., 2005 US Agriculture Health Studyâincidence Private applicators (men and women) 208 0.9 (0.8â1.0) Spouses of private applicators ( 99% women) 12 1.2 (0.6â2.1) Commercial applicators (men and women) 87 0.9 (0.7â1.1) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 56 0.7 (0.6â1.0) Spouses of private applicators ( 99% women) 31 1.2 (0.8â1.6) ât Mannetje et al., 2005 Phenoxy herbicide producers (men and women) 2 0.6 (0.0â2.3) Phenoxy herbicide sprayers ( 99% men) 8 1.9 (0.8â3.8) Torchio et al., 1994 Italian licensed pesticide users Large intestine 84 0.6 (0.5â0.7) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 7 0.5 (0.2â1.1) Small intestine 2 5.2 (1.4â18.9) Studies Reviewed in Update 2000 Steenland et al., 1999 US chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 34 1.2 (0.8â1.6)d Hooiveld et al., 1998 Dutch chemical production workers (included in the IARC cohort) 3 1.4 (0.3â4.0) Rix et al., 1998 Danish paper mill workersâincidence Men 58 1.0 (0.7â1.2) Women 23 1.1 (0.7â1.7) Studies Reviewed in Update 1998 Gambini et al., 1997 Italian rice growers 27 1.1 (0.7â1.6) Kogevinas et al., 1997 IARC cohort (men and women) Workers exposed to any phenoxy herbicide or chlorophenol 86 1.1 (0.9â1.3) Exposed to TCDD (or higher- chlorinated dioxins) 52 1.0 (0.8â1.3) Not exposed to TCDD (or higher- chlorinated dioxins) 33 1.2 (0.8â1.6)
CANCER 301 TABLE 6-7 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Becher et al., 1996 German production workers (included in the IARC cohort) Plant I 2 0.4 (0.1â1.4) Plant II 0 â Plant III 1 2.2 (0.1â12.2) Plant IV 0 â Ott and Zober, 1996e BASF employeesâincidence 5 1.0 (0.3â2.3) TCDD g/kg of body weight) 0.1 2 1.1 (0.1â3.9) 0.1â0.99 2 1.4 (0.2â5.1) 1 1 0.5 (0.0â3.0) Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 4 0.8 (0.2â2.1) 15-year latency 4 1.0 (0.3â2.6) Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 2,291 1.0 (0.9â1.0) White women 59 1.0 (0.8â1.3) Bueno de Mesquita Dutch phenoxy herbicide workers (included et al., 1993 in the IARC cohort) 3 1.8 (0.4â5.4) Collins et al., 1993 Monsanto Company workers (included in the NIOSH cohort) 3 0.5 (0.1â1.3) Studies Reviewed in VAO Swaen et al., 1992 Dutch licensed herbicide applicators 4 2.6 (0.7â6.5) Ronco et al., 1992 Danish workersâincidence Menâself-employed 277 0.7 (p 0.05) employee 45 0.6 (p 0.05) Womenâself-employed 14 0.9 (*) employee 112 0.9 (*) family worker 2 0.2 (p 0.05) Fingerhut et al., 1991 NIOSHâentire cohort 25 1.2 (0.8â1.8)d 1-year exposure; 20-year latency 13 1.8 (1.0â3.0)d Manz et al., 1991 German production workers (included in the IARC cohort) 8 0.9 (0.4â1.8) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 41 1.1 (0.8â1.5) Zober et al., 1990b.e BASF employeesâbasic cohort 2 2.5 (0.4â7.8)f Alavanja et al., 1989 USDA forest or soil conservationists 44g 1.5 (1.1â2.0) Henneberger et al., 1989 New Hampshire pulp and paper workers 9 1.0 (0.5â2.0) Solet et al., 1989 US pulp and paper workers 7 1.5 (0.6â3.0) Alavanja et al., 1988 USDA agricultural extension agents 41 1.0 (0.7â1.5) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 4 2.1 (0.6â5.4) continued
302 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-7 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Thomas, 1987 US ï¬avor and fragrance chemical plant workers 4 0.6* Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 19 1.0 (0.6â1.6) Robinson et al., 1986 Northwestern US pulp and paper workers 7 0.4 (0.2â0.7)f Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) Men 10 1.0* Women 1 0.3* Blair et al., 1983 Florida pesticide applicators 5 0.8* Wiklund, 1983 Swedish male and female agricultural workersâincidence 1,332 0.8 (0.7â0.8)h Thiess et al., 1982 BASF production workers 1 0.4* Burmeister, 1981 Iowa farmers 1,064 1.0 (NS) Hardell, 1981 Swedish residents Exposed to phenoxy acids 11 1.3 (0.6â2.8) Exposed to chlorophenols 6 1.8 (0.6â5.3) ENVIRONMENTAL Studies Reviewed in Update 2002 Revich et al., 2001 Residents of Chapaevsk, Russia Men 17 1.3 (0.8â2.2) Women 24 1.0 (0.7â1.5) Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zones A, Bâmen 10 1.0 (0.5â1.9) women 5 0.6 (0.2â1.4) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Aâwomen 2 2.6 (0.3â9.4) Zone Bâmen 5 0.8 (0.3â2.0) women 3 0.6 (0.1â1.8) Zone Râmen 34 0.8 (0.6â1.1) women 33 0.8 (0.6â1.1) Svensson et al., 1995 Swedish ï¬shermenâmortality (men and women) East coast 1 0.1 (0.0â0.7) West coast 58 1.0 (0.8â1.3) Swedish ï¬shermenâincidence (men and women) East coast 5 0.4 (0.1â0.9) West coast 82 1.0 (0.8â1.2)
CANCER 303 TABLE 6-7 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 1996 Bertazzi et al., 1993 Seveso residentsâ10-year follow-upâmorbidity Zone Bâmen 2 0.5 (0.1â2.0) women 2 0.6 (0.1â2.3) Zone Râmen 32 1.1 (0.8â1.6) women 23 0.8 (0.5â1.3) Studies Reviewed in VAO Lampi et al., 1992 Finnish community exposed to chlorophenol contamination (men and women) 9 1.1 (0.7â1.8) Pesatori et al., 1992 Seveso residentsâincidence Zones A, Bâmen 3 0.6 (0.2â1.9) women 3 0.7 (0.2â2.2) Bertazzi et al., 1989a Seveso residentsâ10-year follow-up Zones A, B, Râmen 20 1.0 (0.6â1.5) women 12 0.7 (0.4â1.2) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 376 1.1 (1.0â1.2) Navy 91 1.3 (1.0â1.5) Army 239 1.1 (0.9â1.2) Air Force 47 1.1 (0.8â1.5) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 176 1.0 (0.8â1.1) Navy 49 1.3 (0.9â1.6) Army 107 0.9 (0.7â1.0) Air Force 21 0.9 (0.5â1.3) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 54 0.9 (0.7â1.4) Mortality 29 0.8 (0.5â1.3) Boehmer et al., 2004 Follow-up of CDC Vietnam Experience Cohort (colon, rectum, anus) 9 1.0 (0.4â2.6) Studies Reviewed in Update 2000 AFHS, 2000e Air Force Ranch Hand veterans 7 1.5 (0.4â5.5) AIHW, 1999e Australian Vietnam veteransâmen 188 221 expected (191â251) CDVA, 1998a Australian Vietnam veteransâmen 405j 117 expected (96â138) CDVA, 1998b Australian Vietnam veteransâwomen 1j 1 expected (0â5) continued
304 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-7 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 78 1.2 (0.9â1.5) CDVA, 1997b Australian National Service Vietnam 6 0.6 (0.2â1.5) veterans Studies Reviewed in Update 1996 Dalager et al., 1995 US Vietnam veteransâwomen 4 0.4 (0.1â1.2) Vietnam veteran nurses 4 0.5 (0.2â1.7) Studies Reviewed in VAO Breslin et al., 1988k Army Vietnam veterans 209 1.0 (0.7â1.3) Marine Vietnam veterans 33 1.3 (0.7â2.2) Anderson et al., 1986b Wisconsin Vietnam veterans 6 1.0 (0.4â2.2) ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; AFHS, Air Force Health Study; AIHW, Australian Institute of Health and Welfare; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, methyl-4- chlorophenoxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; NS, not signiï¬cant; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d Colon and small intestine combined. e Colon and rectal cancer results combined. f 90% CI. g p 0.01. h 99% CI. i Incidence rates provided in absence of information on exposed cases or estimated relative risk for morbidity. j Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have cancer of the colon?â k Intestinal and other GI cancer results are combined in this study. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohort. cancer, however, was not more strongly associated with having ever been exposed to nonvolatile organochlorine compounds (n 51; SMR 0.96, 95% CI 0.71â1.26) than with having never been exposed (n 60; SMR 0.87, 95% CI 0.66â1.12). In their prospective cohort study of cancer incidence in private commercial pesticide applicators, Alavanja et al. (2005) found the incidence of rectal cancer signiï¬cantly lower than expected (SIR 0.81, 95% CI 0.65â0.99) and the inci- dence of colon cancer similar to that predicted in the general population (SIR 0.88, 95% CI 0.76â1.01). In commercial applicators, the incidence of colon
CANCER 305 TABLE 6-8 Selected Epidemiologic StudiesâRectal Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 60 0.9 (0.7â1.1) Ever 51 1.0 (0.7â1.3) Alavanja et al., 2005 US Agriculture Health Studyâincidence Private applicators (men and women) 94 0.8 (0.7â1.0) Spouses of private applicators ( 99% women) 23 0.6 (0.4â0.9) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) * * Spouses of private applicators ( 99% women) * * ât Mannetje et al., Phenoxy herbicide producers (men and women) 5 2.5 (0.8â5.7) 2005 Phenoxy herbicide sprayers ( 99% men) 4 1.5 (0.4â3.8) Torchio et al., 1994 Italian licensed pesticide users * * Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 10 1.2 (0.6â2.3) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 5 2.1 (0.7â4.8) Studies Reviewed in Update 2000 Steenland et al., US chemical production workers (included 1999 in the IARC cohort and the NIOSH Dioxin Registry) 6 0.9 (0.3â1.9) Hooiveld et al., Dutch chemical production workers (included in 1998 the IARC Cohort) 1 1.0 (0.0â5.6) Rix et al., 1998 Danish paper mill workersâincidence Men 43 0.9 (0.6â1.2) Women 15 1.5 (0.8â2.4) Studies Reviewed in Update 1998 Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 44 1.1 (0.8â1.4) Exposed to TCDD (or higher-chlorinated dioxins) 29 1.3 (0.9â1.9) Not exposed to TCDD (or higher- chlorinated dioxins) 14 0.7 (0.4â1.2) Becher et al., 1996 German production workers (included in the IARC Cohort) Plant I 6 1.9 (0.7â4.0) Plant II 0 â Plant III 0 â Plant IV 1 0.9 (0.0â4.9) continued
306 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-8 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 0 â 15-year latency 0 â Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 367 1.0 (0.9â1.1) White women 4 0.5 (0.1â1.3) Bueno de Mesquita Dutch phenoxy herbicide workers (included in et al., 1993 the IARC cohort) 0 0 (0.0â4.3) Studies Reviewed in VAO Ronco et al., 1992 Danish workersâincidence Menâself-employed 309 0.8 (p 0.05) employee 55 0.8 (*) Womenâself-employed 5 0.6 (*) employee 55 0.8 (*) family worker 2 0.4 (*) Fingerhut et al., NIOSHâentire cohort 5 0.9 (0.3â2.1) 1991 1-year exposure; 20-year latency 2 1.2 (0.4â4.2) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 24 1.1 (0.7â1.6) Alavanja et al., 1989 USDA forest or soil conservationists 9 1.0 (0.5â1.9) Henneberger et al., New Hampshire pulp and paper workers 1 0.4 (0.0â2.1) 1989 Alavanja et al., 1988 USDA agricultural extension agents 5 0.6 (0.2â1.3) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 1 1.7 (0.0â9.3) Thomas, 1987 US ï¬avor and fragrance chemical plant workers 6 2.5* Coggon et al., 1986 British MCPA chemical workers (included in the IARC cohort) 8 0.6 (0.3â1.2) Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) Men 14 1.5* Women 2 1.0* Blair et al., 1983 Florida pesticide applicators 2 1.0* Wiklund, 1983 Swedish male and female agricultural workersâincidence 1,083 0.9 (0.9â1.0)d ENVIRONMENTAL Studies Reviewed in Update 2002 Revich et al., 2001 Residents of Chapaevsk, Russia Men 21 1.5 (1.0â2.4) Women 24 0.9 (0.6â1.4)
CANCER 307 TABLE 6-8 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zones A, Bâmen 9 2.4 (1.2â4.6) women 3 1.1 (0.4â3.5) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Bâmen 7 2.9 (1.2â5.9) women 2 1.3 (0.1â4.5) Zone Râmen 19 1.1 (0.7â1.8) women 12 0.9 (0.5â1.6) Svensson et al., Swedish ï¬shermenâmortality (men and 1995 women) East coast 4 0.7 (0.2â1.9) West coast 31 1.0 (0.7â1.5) Swedish ï¬shermenâincidence (men and women) East coast 9 0.9 (0.4â1.6) West coast 59 1.1 (0.8â1.4) Studies Reviewed in Update 1996 Bertazzi et al., 1993 Seveso residentsâ10-year follow-upâincidence Zone Bâmen 3 1.4 (0.4â4.4) women 2 1.3 (0.3â5.4) Zone Râmen 17 1.1 (0.7â1.9) women 7 0.6 (0.3â1.3) Studies Reviewed in VAO Pesatori et al., 1992 Seveso residentsâincidence Zones A, Bâmen 3 1.2 (0.4â3.8) women 2 1.2 (0.3â4.7) Bertazzi et al., Seveso residentsâ10-year follow-up 1989a Zones A, B, Râmen 10 1.0 (0.5â2.0) women 7 1.2 (0.5â2.7) Bertazzi et al., Seveso residentsâ10-year follow-up 1989b Zone Bâmen 2 1.7 (0.4â7.0) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 234 1.0 (0.9â1.1) Navy 54 1.1 (0.8â1.4) Army 152 1.0 (0.8â1.1) Air Force 28 1.0 (0.6â1.4) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 69 0.9 (0.7â1.1) Navy 13 0.8 (0.4â1.4) Army 44 0.9 (0.6â1.1) Air Force 12 1.3 (0.6â2.2) continued
308 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-8 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 46 1.4 (0.9â2.2) Mortality 10 1.8 (0.6â5.6) Boehmer et al., 2004 Follow-up of CDC Vietnam Experience Cohort (colon, rectum, anus) 9 1.0 (0.4â2.6) Studies Reviewed in Update 2000 AFHS, 2000f Air Force Ranch Hand veterans 7 1.5 (0.4â5.5) AIHW, 1999f Male Australian Vietnam veterans 188 221 expected (191â251) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 16 0.6 (0.4â1.0) CDVA, 1997b Australian National Service Vietnam veterans 3 0.7 (0.2â9.5) Studies Reviewed in VAO Anderson et al., Wisconsin Vietnam veterans 1 â 1986 ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; AFHS, Air Force Health Study; AIHW, Australian Institute of Health and Welfare; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, methyl-4-chlorophenoxyacetic acid; NIOSH, National Institute for Oc- cupational Safety and Health; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d 99% CI. e Incidence rates provided in absence of information on exposed cases or estimated relative risk for morbidity. f Colon and rectal cancer results combined. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohort. cancer (SIR 1.20, 95% CI 0.62â2.10) and of rectal cancer (SIR 1.25, 95% CI 0.50â2.58) remained insigniï¬cant. In the same cohort, Blair et al. (2005a) found the rate of colon-cancer death reduced in the private applicators (SMR 0.7, 95% CI 0.6â1.0) but slightly increased in their spouses (SMR 1.2, 95% CI 0.8â1.6). Mortality from rectal cancer was not reported separately. In the mortality study of phenoxy herbicide producers and sprayers in New Zealand (ât Mannetje et al., 2005), the data on colon-cancer death (SMR 0.62,
CANCER 309 95% CI 0.08â2.25) and rectal-cancer death (SMR 2.45, 95% CI 0.79â5.73) among producers were indeterminate. In the sprayer group, there were non- signiï¬cant excesses of cancer deaths from both colon cancer (SMR 1.94, 95% CI 0.84â3.83) and rectal cancer (SMR 1.47, 95% CI 0.40â3.76). Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and MCPA. The esti- mated risk of cancer of the large intestine was reduced (84 cases; SMR 0.57, 95% CI 0.45â0.71). Reif et al. (1989) performed a series of caseâcontrol analyses on a sample of 19,904 men entered into the New Zealand Cancer Registry from 1980â1984 with an occupation speciï¬ed. They focused on the 134 registrants for whom forestry worker (presumed to be exposed to phenoxyherbicides and chlorophenols) was the most recent occupation. Two forestry workers among 63 cases of cancer of the small intestine (OR 5.22, 95% CI 1.44â18.88) represented a signiï¬cantly increased risk. The seven forestry workers among the 2,043 cases of colon cancer (OR 0.51, 95% CI 0.24â1.09) and the 10 forestry workers among the 1,376 rectal cancer cases (OR 1.22, 95% CI 0.64â2.34) did not constitute excesses. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and colorectal cancer were published since Update 2004. Vietnam-Veteran Studies The 2005 report updating the cancer incidence of Australian Vietnam veterans (ADVA, 2005a) noted a slight increase in the inci- dence of colon cancer (SIR 1.13, 95% CI 1.01â1.24), but no excess of deaths from colon cancer was observed (SMR 0.98, 95% CI 0.83â1.12). The report did not include speciï¬c information on the incidence of rectal cancers, but a slight increase in deaths from colorectal cancer was observed (SMR 0.96, 95% CI 0.86â1.06). The incidence of colorectal cancers among deployed National Service veterans (RR 1.13, 95% CI 0.86â1.46) was not increased when compared with that in non-deployed troops, and no excess colorectal deaths were observed (RR 0.80, 95% CI 0.48â1.30) (ADVA, 2005c). In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported nine deaths from cancer of the colon, rectum, or anus (ICD-9 153â154) in the deployed and eight in the non-deployed (CRR 1.02, 95% CI 0.39â2.64). Biologic Plausibility No animal studies have reported an increased incidence of colorectal can- cer after exposure to the compounds of interest. The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter.
310 VETERANS AND AGENT ORANGE: UPDATE 2006 Synthesis Previous updates have not reviewed the risk of colorectal cancers separately. There has been no evidence to suggest an association between the compounds of interest and colorectal cancer in the epidemiologic studies reviewed to date. The only signiï¬cant increase in intestinal cancers noted in this update was the reported result concerning cancer of the small intestine that was based on cases in two exposed people (Reif et al., 1989); this is a very uncommon tumor type that is reported here for completeness of coverage with the more common cancers of the large intestine and rectum. There is no evidence of biologic plausibility of an association between exposure to any of the compounds of interest and the development of tumors of the colon or rectum. Overall, the available evidence does not support an association between the compounds of interest and colorectal cancer. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and colorectal cancer. Hepatobiliary Cancers Hepatobiliary cancers include cancers of the liver (ICD-9 155.0, 155.2) and the intrahepatic bile duct (ICD-9 155.1). ACS estimated that in 2006 12,600 men and 5,910 women would receive diagnoses of liver or intrahepatic bile duct cancer in the United States and 10,840 men and 5,360 women would die from those cancers (ACS, 2006). Gallbladder cancer and extrahepatic bile duct cancer (ICD-9 156) are fairly uncommon, but they are often grouped with liver cancers when they are addressed. In the United States, liver cancers account for about 1.3 percent of new cancer cases and 1.2 percent of cancer deaths. Misclassiï¬cation of metastatic cancers as primary liver cancer can lead to overestimation of the number of deaths attributable to liver cancer (Percy et al., 1990). In developing countries, especially those in sub-Saharan Africa and Southeast Asia, liver cancers are common and are among the leading causes of death. The known risk factors for liver cancer include chronic infection with hepatitis B or C virus and exposure to the carcinogens aï¬atoxin and vinyl chloride. Alcohol cirrhosis and obesity- associated metabolic syndrome may also contribute to the risk of liver cancer. In the general population, the incidence of liver and intrahepatic bile duct cancer increases slightly with age; at the ages of 50â64 years, it is greater in men than
CANCER 311 in women and greater in blacks than in whites. The average annual incidence of hepatobiliary cancers is shown in Table 6-4. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and hepatobiliary cancers. Additional in- formation available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-9 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. The SMR for liver cancer was not associated with a JEM-based estimate of exposure to nonvolatile organochlo- rine compounds (never exposed: 27 cases; SMR 0.87, 95% CI 0.57â1.27; ever exposed: 16 cases; SMR 0.69, 95% CI 0.40â1.13). Alavanja et al. (2005) reported cancer incidence in a prospective cohort study of private pesticide applicators, commercial applicators, and spouses of the private applicators. The risk of liver cancer was effectively unity for the private applicators (SIR 0.98, 95% CI 0.68â1.37) and for their spouses (SIR 0.86, 95% CI 0.17â2.51), as was the risk of gallbladder cancer in the spouses (SIR 0.85, 95% CI 0.17â2.48). An excess of gallbladder cancers (n 8) in the applica- tors approached signiï¬cance (SIR 2.26, 95% CI 0.87â4.45). Blair et al. (2005a) reported cancer mortality in the same prospective cohort of pesticide applicators and spouses in North Carolina and Iowa. In the applica- tors, mortality from liver cancer was reduced (SMR 0.6, 95% CI 0.2â1.1), but three cases of gallbladder cancer generated an increased risk estimate (SMR 2.0, 95% CI 0.4â5.7). In their spouses, the risks of death from liver cancer (SMR 1.7, 95% CI 0.4â4.3) and gallbladder cancer (SMR 1.3, 95% CI 0.1â4.6) were not increased. In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers from 1969 and 1973, respectively, through 2000. The data on the risk of death from hepatic cancer (ICD-9 155) were uninformative; one death occurred in the producer group and none in the sprayer group. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics re- ports as having high herbicide use, especially of 2,4-D and MCPA. The estimated risk of death from liver cancer was signiï¬cantly reduced in this cohort (15 cases; SMR 0.56, 95% CI 0.31â0.92) when compared with the expected mortality for
312 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-9 Selected Epidemiologic StudiesâHepatobiliary Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 27 0.9 (0.6â1.3) Ever 16 0.7 (0.4â1.1) Alavanja et al., 2005 US Agriculture Health Studyâincidence Liver Private applicators (men and women) 35 1.0 (0.7â1.4) Spouses of private applicators ( 99% women) 3 0.9 (0.2â2.5) Commercial applicators (men and women) â 0.0 (0.0â4.2) Gallbladder Private applicators (men and women) 8 2.3 (1.0â4.5) Spouses of private applicators ( 99% women) 3 0.9 (0.2â2.5) Commercial applicators (men and women) â 0.0 (0.0â35.8) Blair et al., 2005a US Agriculture Health Study Liver Private applicators (men and women) 8 0.6 (0.2â1.1) Spouses of private applicators ( 99% women) 4 1.7 (0.4â4.3) Gallbladder Private applicators (men and women) 3 2.0 (0.4â5.7) Spouses of private applicators ( 99% women) 2 1.3 (0.1â4.6) ât Mannetje et al., New Zealand phenoxy herbicide workers 2005 (ICD-9 155) Producers (men and women) 1 1.6 (0.0â8.8) Sprayers ( 99% men) 0 0.0 (0.0â4.2) Torchio et al., 1994 Italian licensed pesticide users Liver 15 0.6 (0.3â0.9) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) Liver 1 0.8 (0.1â5.8) Gallbladder 3 4.1 (1.4â12.0) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 0 â Studies Reviewed in Update 2000 Steenland et al., 1999 US chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 7 0.9 (0.4â1.6)
CANCER 313 TABLE 6-9 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Rix et al., 1998 Danish paper mill workersâincidence Liverâmen 10 1.1 (0.5â2.0) women 1 0.6 (0.0â3.2) Gallbladderâmen 9 1.6 (0.7â3.0) women 4 1.4 (0.4â3.7) Studies Reviewed in Update 1998 Gambini et al., 1997 Italian rice growers 7 1.3 (0.5â2.6) Kogevinas et al., 1997 IARC cohort (men and women) Workers exposed to any phenoxy herbicide or chlorophenol 15 0.7 (0.4â1.2) Workers exposed to TCDD (or higher- chlorinated dioxins) 12 0.9 (0.5â1.5) Workers not exposed to TCDD (or higher- chlorinated dioxins) 3 0.4 (0.1â1.2) Becher et al., 1996 German production workers (included in the IARC cohort) 1 1.2 (0.0â6.9) Ott and Zober, 1996 BASF employeesâincidence 2 2.1 (0.3â7.5) TCDD g/kg of body weight) 0.1 1 2.8 (0.1â15.5) 0.1â0.99 0 0.0 (0.0â15.4) 1 1 2.8 (0.1â15.5) Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 0 â* 15-year latency 0 â* Studies Reviewed in Update 1996 Asp et al., 1994 Finnish herbicide applicatorsâincidence 3 0.9 (0.2â2.6) Finnish herbicide applicatorsâmortality 2 0.6 (0.1â2.2) Blair et al., 1993 US farmers in 23 states White men 326 1.0 (0.9â1.1) White women 6 0.7 (0.3â1.6) Collins et al., 1993 Monsanto Company 2,4-D production workers (Included in NIOSH cohort) 2 1.4 (0.2â5.2) Studies Reviewed in VAO Ronco et al., 1992 Danish farm workersâincidence Liver Menâself-employed 23 0.4 (p 0.05) employee 9 0.8 (*) Womenâfamily worker 5 0.5 (*) Gallbladder Menâself-employed 35 0.8 (*) employee 7 0.8 (*) Womenâself-employed 7 2.7 (p 0.05) employee 1 0.7 (*) family worker 17 1.0 (*) continued
314 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-9 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Fingerhut et al., 1991 NIOSHâentire cohort (liver and biliary) 6 1.2 (0.4â2.5) 1-year exposure; 20-year latency 1 0.6 (0.0â3.3) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 4 0.4 (0.1â1.1) Solet et al., 1989 US pulp and paper workers 2 2.0 (0.2â7.3) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0 1.2 (*) Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) Men 3 1.0 (*) Women 0 â Hardell et al., 1984 Swedish residentsâincidence and mortality combined 102 1.8 (0.9â4.0) Wiklund, 1983 Swedish male and female agricultural workersâincidence Liver (primary) 103 0.3 (0.3â0.4)d Biliary passages 169 0.6 (0.5â0.7) Liver (unspeciï¬ed) 67 0.9 (0.7â1.3) Zack and Suskind, Monsanto Company production workers 1980 (Included in NIOSH cohort) 0 â* ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zone A, Bâmen (liver, gallbladder) 6 0.5 (0.2â1.0) (liver) 6 0.5 (0.2â1.1) women (liver, gallbladder) 7 1.0 (0.5â2.2) (liver) 6 1.3 (0.6â2.9) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Bâmen (liver, gallbladder) 4 0.6 (0.2â1.4) (liver) 4 0.6 (0.2â1.6) women (liver, gallbladder) 4 1.1 (0.3â2.9) (liver) 3 1.3 (0.3â3.8) Zone Râmen (liver, gallbladder) 35 0.7 (0.5â1.0) (liver) 31 0.7 (0.5â1.0) women (liver, gallbladder) 25 0.8 (0.5â1.3) (liver) 12 0.6 (0.3â1.1)
CANCER 315 TABLE 6-9 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Svensson et al., 1995 Swedish ï¬shermenâmortality (men and women) East coast 1 0.5 (0.0â2.7) West coast (liver and bile ducts) 9 0.9 (0.4â1.7) Swedish ï¬shermenâincidence (men and women) East coast 6 1.3 (0.5â2.9) West coast (liver and bile ducts) 24 1.0 (0.6â1.5) Studies Reviewed in Update 1996 Bertazzi et al., 1993 Seveso residentsâ10-year follow-upâincidence Zone Bâmen (liver) 4 2.1 (0.8â5.8) (gallbladder) 1 2.3 (0.3â17.6) women (gallbladder) 4 4.9 (1.8â13.6) Zone Râmen (liver) 3 0.2 (0.1â0.7) (gallbladder) 3 1.0 (0.3â3.4) women (liver) 2 0.5 (0.1â2.1) (gallbladder) 7 1.0 (0.5â2.3) Cordier et al., 1993 Military service in South Vietnam for 10 years after 1960 11 8.8 (1.9â41.0) Studies Reviewed in VAO Pesatori et al., 1992 Seveso residentsâincidence Zone A, Bâmen (liver) 4 1.5 (0.5â4.0) (gallbladder) 1 2.1 (0.3â15.6) women (liver) 1 1.2 (0.2â9.1) (gallbladder) 5 5.2 (2.1â13.2) Zone Râmen (liver) 8 0.5 (0.2â0.9) (gallbladder) 3 1.0 (0.3â3.4) women (liver) 5 0.8 (0.3â2.1) (gallbladder) 7 1.0 (0.5â2.3) Bertazzi et al., 1989b Seveso residentsâ10-year follow-up Zone Aâwomen (gallbladder) 1 12.1 (1.6â88.7) Zone Bâmen (liver) 3 1.2 (0.4â3.8) women (gallbladder) 2 3.9 (0.9â16.2) Zone Râmen (liver) 7 0.4 (0.2â0.8) women (liver) 3 0.4 (0.1â1.4) (gallbladder) 5 1.2 (0.5â3.1) Hoffman et al., 1986 Residents of Quail Run Mobile Home Park (men and women) 0 * continued
316 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-9 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 27 0.7 (0.4â1.0) Navy 8 1.0 (0.4â1.9) Army 18 0.7 (0.4â1.1) Air Force 1 0.2 (0.0â1.2) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality (liver and gallbladder) 48 0.9 (0.6â1.1) Navy 11 1.0 (0.5â1.7) Army 33 0.9 (0.6â1.2) Air Force 4 0.6 (0.2â1.5) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 2 2.5 (0.1â147.2) Mortality (liver and gallbladder) 4 2.5 (0.4â27.1) Boehmer et al., 2004 Follow-up of CDC Vietnam Experience 5 â* Cohort (liver) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 2 1.6 (0.2â11.4) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans Liver 8 0.6 (0.2â1.1) Gallbladder 5 1.3 (0.4â2.8) CDVA, 1997b Australian National Service Vietnam veterans 1 â* Studies Reviewed in VAO CDC, 1990a US men born 1921â1953 8 1.2 (0.5â2.7) Breslin et al., 1988 Army Vietnam veterans (liver and bile duct) 34 1.0 (0.8â1.4) Marine Vietnam veterans (liver and bile duct) 6 1.2 (0.5â2.8) Anderson et al., 1986b Wisconsin Vietnam veterans 0 â* ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; CDC, Centers for Disease Control and Prevention; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; NIOSH, National Institute for Occupational Safety and Health, TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d 99% CI. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohort.
CANCER 317 the regional and provincial population. The authors suggested that the relatively short duration of follow-up and the healthy-worker effect contributed to the ob- servation of reduced mortality. Reif et al. (1989) performed a series of caseâcontrol analyses on a sample of 19,904 men entered into the New Zealand Cancer Registry from 1980â1984 with an occupation speciï¬ed. They focused on the 134 registrants for whom forestry worker (presumed to be exposed to phenoxyherbicides and chlorophenols) was the most recent occupation. A single forestry worker among the 184 cases with cancer of the liver did not constitute an excess (OR 0.81, 95% CI 0.11â5.8). However, three forestry workers were among the 120 cases of gallbladder cancer (OR 4.13, 95% CI 1.42â12.04) in the cohort. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and hepatobiliary cancer were published since Update 2004. Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported ï¬ve deaths from cancer of the liver or in- trahepatic bile ducts (ICD-9 155) in the deployed and three in the non-deployed. The researchers did not consider the data sufï¬cient for the calculation of risk statistics unless there were at least 10 deaths from a type of cancer. A set of three reports updating the health status of Australian Vietnam vet- erans noted results concerning possible associations between Vietnam service and the incidence of liver cancer and mortality from liver and gallbladder cancer. The incidence of liver cancer was lower in Vietnam veterans than in the general population (SIR 0.70, 95% CI 0.44â0.97) (ADVA, 2005a), and there was no increase in the risk of death from liver or gallbladder cancer (SMR 0.88, 95% CI 0.63â1.13) (ADVA, 2005b). In a third report on the potential for a healthy- warrior effect, there were too few incident cases of liver cancer (n 2) to calcu- late stable estimates (RR 2.50, 95% CI 0.13â147); that was also the case for mortality from liver or gallbladder cancer (n 4; RR 2.45, 95% CI 0.35â27.06) (ADVA, 2005c). Biologic Plausibility A recent study used a mouse model bearing a constitutively active form of the AhR to examine the role of the AhR in promotion of hepatocarcinogenesis; treatment with the tumor initiator N-nitrosodiethylamine resulted in an increase in hepatic tumors that was signiï¬cantly greater than that observed in the wild-type mice (Moennikes et al., 2004). The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter.
318 VETERANS AND AGENT ORANGE: UPDATE 2006 Synthesis In this update, no new reports of a deï¬nitive link between exposure to the compounds of interest and hepatobiliary tumors were found. One study suggested a reduced risk of hepatic cancers in veteran populations, and one suggested an in- creased risk of cancer of the gallbladder among forestry workers. However, given the relatively low incidence of hepatobiliary cancers in Western populations, the evidence from epidemiologic studies remains inadequate to link the compounds of interest with hepatobiliary cancer. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and hepatobiliary cancer. The evidence regarding associa- tion is drawn from occupational and other studies in which subjects were exposed to a variety of herbicides and herbicide components. Although several of those studies involved sizable cohorts, hepatobiliary cancers are rare, and the power of the studies to detect an increase in incidence is low. Pancreatic Cancer The incidence of pancreatic cancer (ICD-9 157) increases with age. ACS estimated that 17,150 men and 16,580 women would develop pancreatic cancer in the United States in 2006 and that 16,090 men and 16,210 women would die from it (Jemal et al., 2006). The incidence is higher in men than in women and higher in blacks than in whites. Other risk factors include family history, diet, and tobacco use; the incidence is about twice as high in smokers as in nonsmokers (Miller et al., 1996). Chronic pancreatitis, obesity, and type 2 diabetes are also associated with an increased risk of pancreatic cancer (ACS, 2006). Conclusions from VAO and Updates This update considers pancreatic cancer independently for the ï¬rst time. Prior updates developed tables of results for pancreatic cancer, but conclusions about the adequacy of the evidence of its association with herbicide exposure have been reached in the context of gastrointestinal tract cancers. Table 6-10 sum- marizes the results of the relevant studies concerning pancreatic cancer. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. The SMR for pancreatic cancer
CANCER 319 TABLE 6-10 Selected Epidemiologic StudiesâPancreatic Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 67 0.8 (0.7â1.1) Ever 69 1.1 (0.9â1.4) Alavanja et al., 2005 US Agriculture Health Studyâincidence Private applicators (men and women) 46 0.7 (0.5â1.0) Spouses of private applicators ( 99% women) 20 0.9 (0.6â1.4) Commercial applicators (men and women) 3 1.1 (0.2â3.2) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 29 0.6 (0.4â0.9) Spouses of private applicators ( 99% women) 10 0.7 (0.3â1.2) ât Mannetje et al., 2005 Phenoxy herbicide producers (men and women) 3 2.1 (0.4â6.1) Phenoxy herbicide sprayers ( 99% men) 0 0.0 (0.0â2.1) Torchio et al., 1994 Italian licensed pesticide users 32 0.7 (0.5â1.0) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 6 1.8 (0.8â4.1) Magnani et al., 1987 UK caseâcontrol Herbicides * 0.7 (0.3â1.5) Chlorophenols * 0.8 (0.5â1.4) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 5 1.2 (0.4â2.7) Studies Reviewed in Update 2000 Ojajärvi et al., 2000 Meta-analysis of 161 populations 127 MRR 1.0 (0.8â1.3) Steenland et al., 1999 US chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 16 1.0 (0.6â1.6) Hooiveld et al., 1998 Dutch chemical production workers (included in the IARC cohort) 4 2.5 (0.7â6.3) Rix et al., 1998 Danish paper mill workersâincidence Men 30 1.2 (0.8â1.7) Women 2 0.3 (0.0â1.1) Studies Reviewed in Update 1998 Gambini et al., 1997 Italian rice growers 7 0.9 (0.4â1.9) continued
320 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-10 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Kogevinas et al., 1997 IARC cohort (men and women) Workers exposed to any phenoxy herbicide or chlorophenol 47 0.9 (0.7â1.3) Exposed to TCDD (or higher- chlorinated dioxins) 30 1.0 (0.7â1.4) Not exposed to TCDD (or higher- chlorinated dioxins) 16 0.9 (0.5â1.4) Becher et al., 1996 German production workers (included in the IARC cohort) Plant I 2 0.6 (0.1â2.3) Plant II 0 â Plant III 0 â Plant IV 2 1.7 (0.2â6.1) Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 2 0.7 (0.1â2.7) 15-year latency 2 0.9 (0.1â3.3) Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 1,133 1.1 (1.1â1.2) White women 23 1.0 (0.6â1.5) Bueno de Mesquita Dutch phenoxy herbicide workers (included 3 2.2 (0.5â6.3) et al., 1993 in the IARC cohort) Studies Reviewed in VAO Ronco et al., 1992 Danish farm workersâincidence Menâself-employed 137 0.6 (p 0.05) employee 23 0.6 (p 0.05) Womenâself-employed 7 1.2 (*) employee 4 1.3 (*) family worker 27 0.7 (p 0.05) Swaen et al., 1992 Dutch licensed herbicide applicators 3 2.2 (0.4â6.4) Fingerhut et al., 1991 NIOSHâentire cohort 10 0.8 (0.4â1.6) 1-year exposure; 20-year latency 4 1.0 (0.3â2.5) Saracci et al., 1991 IARC cohortâexposed subcohort (men and 26 1.1 (0.7â1.6) women) Alavanja et al., 1989 USDA forest or soil conservationists 22 1.5 (0.9â2.3) Henneberger et al., 1989 New Hampshire paper and pulp workers 9 1.9 (0.9â3.6) Solet et al., 1989 US pulp and paper workers 1 0.4 (0.0â2.1) Alavanja et al., 1988 USDA agricultural extension agents 21 1.3 (0.8â1.9) Thomas, 1987 US ï¬avor and fragrance chemical plant 6 1.4* workers Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 9 0.7 (0.3â1.4) Robinson et al., 1986 Northwestern US paper and pulp workers 4 0.3 (0.1â0.8)d
CANCER 321 TABLE 6-10 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) Men 3 0.6* Women 0 â Blair et al., 1983 Florida pesticide applicators 4 4.0 Expected* Wiklund, 1983 Swedish male and female agricultural workersâincidence 777 0.8 (0.8â0.9)e Burmeister, 1981 Iowa farmers 416 1.1* ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zones A, Bâmen 4 0.7 (0.3â1.9) women 1 0.3 (0.0â2.0) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Aâmen 1 1.9 (0.0â10.5) Zone Bâmen 2 0.6 (0.1â2.0) women 1 0.5 (0.0â3.1) Zone Râmen 20 0.8 (0.5â1.2) women 11 0.7 (0.4â1.3) Svensson et al., 1995 Swedish ï¬shermenâmortality (men and women) East coast 5 0.7 (0.2â1.6) West coast 33 0.8 (0.6â1.2) Swedish ï¬shermenâincidence (men and women) East coast 4 0.6 (0.2â1.6) West coast 37 1.0 (0.7â1.4) Studies Reviewed in VAO Pesatori et al., 1992 Seveso residentsâincidence Zones A, Bâmen 2 1.0 (0.3â4.2) women 1 1.6 (0.2â12.0) Bertazzi et al., 1989a Seveso residentsâ10-year follow-up Zones A, B, Râmen 9 0.6 (0.3â1.2) women 4 1.0 (0.3â2.7) Bertazzi et al., 1989b Seveso residentsâ10-year follow-up Zone Bâmen 2 1.1 (0.3â4.5) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 86 1.2 (0.9â1.4) Navy 14 0.9 (0.5â1.5) Army 60 1.2 (0.9â1.5) Air Force 12 1.3 (0.7â2.3) continued
322 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-10 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 101 1.2 (1.0â1.5) Navy 18 1.0 (0.6â1.6) Army 71 1.3 (1.0â1.6) Air Force 11 1.1 (0.5â1.8) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 17 2.5 (1.0â6.3) Mortality 19 3.1 (1.3â8.3) Boehmer et al., 2004 Follow-up of CDC Vietnam Experience 5 1.0 (0.3â3.5) Cohort Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 38 1.4 (0.9â1.8) CDVA, 1997b Australian National Service Vietnam veterans 6 1.5 Studies Reviewed in Update 1996 Dalager et al., 1995 US Vietnam veteransâwomen 7 2.8 (0.8â10.2) Vietnam veteran nurses 7 5.7 (1.2â27.0) Visintainer et al., 1995 Michigan Vietnam veterans 14 1.0 (0.6â1.7) Studies Reviewed in VAO Thomas et al., 1991 US Vietnam veteransâwomen 5 2.7 (0.9â6.2) Breslin et al., 1988 Army Vietnam veterans 82 0.9 (0.6â1.2) Marine Vietnam veterans 18 1.6 (0.5â5.8) Anderson et al., 1986b Wisconsin Vietnam veterans 4 â ABBREVIATIONS: ADVA, Australian Department of Veteran Affairs; CDVA, Commonwealth De- partment of Veteransâ Affairs; CI, conï¬dence interval; IARC; International Agency for Research on Cancer; MCPA, methyl-4-chlorophenoxyacetic acid; NIOSH, National Institute for Occupa- tional Safety and Health; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d 90% CI. e 99% CI. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohort. was not associated with a JEM-based estimate of exposure to nonvolatile organo- chlorine compounds (never exposed: 67 cases; SMR 0.84, 95% CI 0.65â1.06; ever exposed: 69 cases; SMR 1.12, 95% CI 0.87â1.42). In the AHS study of cancer incidence, Alavanja et al. (2005) reported a slight decrease in the incidence of pancreatic cancer in private applicators (SIR
CANCER 323 0.73, 95% CI 0.53â0.97) and no increase in their spouses (SIR 0.92, 95% CI 0.56â1.42). In the commercial applicators, the ï¬ndings on pancreatic cancer were indeterminate; there were only three cases. In investigating cancer mortality in the same prospective cohort study of private pesticide applicators and their spouses, Blair et al. (2005a) found that the rates of pancreatic cancer were reduced in both the applicators (SMR 0.6, 95% CI 0.4â0.9) and their spouses (SMR 0.7, 95% CI 0.3â1.2). The similarity to the results reported by Alavanja et al. (2005) is not unexpected, because median survival of pancreatic cancer is only about 3â6 months. In the mortality study of phenoxy herbicide producers and sprayers in New Zealand (ât Mannetje et al., 2005), only three cases of pancreatic cancer were observed in the producer group and none in the sprayer group. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and MCPA. The esti- mated risk of pancreatic cancer was signiï¬cantly reduced (32 cases; SMR 0.7, 95% CI 0.48â0.99). The authors suggested that the relatively short duration of follow-up and the healthy-worker effect contributed to the observation of reduced mortality. Starting with the 19,904 men entered into the the New Zealand Cancer Reg- istry from 1980â1984 with a speciï¬ed occupation, Reif et al. (1989) contrasted the 571 cases of pancreatic cancer with the remaining subjects having other types of cancer. Of the 134 cancer registrants for whom forestry worker (with presumed exposure to phenoxy herbicides and chlorophenols) was the most recent occupa- tion, the proportion with pancreatic cancer was not signiï¬cantly elevated (6 cases; OR 1.79, 95% CI 0.79â4.05). Magnani et al. (1987) reported a caseâcontrol mortality study of 343 pancre- atic-cancer cases and 1,315 controls in the United Kingdom. A JEM was used to predict exposures to various chemical agents on the basis of job title as indicated on the death certiï¬cates. Estimated risks of pancreatic cancer associated with exposure to herbicides (RR 0.7, 95% CI 0.3â1.5) and chlorophenols (RR 0.8, 95% CI 0.5â1.4) were not signiï¬cantly increased. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and pancreatic cancer were published since Update 2004. Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported ï¬ve pancreatic-cancer deaths in the de- ployed and ï¬ve in the non-deployed (CRR 1.02, 95% CI 0.29â3.53). A set of three reports updating the health status of Australian Vietnam vet- erans noted 86 cases of pancreatic cancer (SIR 1.15, 95% CI 0.91â1.40) (ADVA, 2005a) and 101 deaths (SMR 1.21, 95% CI 0.97â1.45) (ADVA,
324 VETERANS AND AGENT ORANGE: UPDATE 2006 2005b). However, in the report on the health of National Service veterans and non-deployed troops, the incidence of pancreatic cancer was much higher in deployed National Service veterans than in non-deployed veterans (RR 2.46, 95% CI 1.04â6.27), and mortality from pancreatic cancer was also higher (RR 3.13, 95% CI 1.31â8.26) (ADVA, 2005c). Information on the smoking status of neither National Service veterans nor non-deployed troops was available, but the investigators postulate that given the increased rates of lung, head, and neck cancers in the National Service veterans, those veterans might have higher rates of smoking than the non-deployed controls (ADVA, 2005c). Biologic Plausibility A 2-year study of female rats has reported increased incidences of pancre- atic adenomas and carcinomas after treatment at the highest dose of TCDD (100 ng/kg per day) (Nyska et al., 2004). Chronic active inï¬ammation, acinar-cell vacuolation, and an increase in proliferation of the acinar cells surrounding the vacuolated cells have been observed (Yoshizawa et al., 2005b). Synthesis The increased rates of pancreatic cancer among Australian Vietnam National Service veterans could be associated with increased rates of smoking and cannot be attributed to exposure to the compounds of interest. All other reports have been largely negative except the report of seven cases of pancreatic cancer (RR 5.7, 95% CI 1.2â27) in US Vietnam female nurse veterans (Dalager et al., 1995). Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and pancreatic cancer. Conclusions on All Cancers of the Digestive Organs The original VAO report (IOM, 1994) considered âgastrointestinal tract tu- morsâ as a groupâwhich explicitly included stomach, colon, rectal, and pancre- atic cancersâand concluded that there was suggestive evidence of no association with herbicide exposure. Cumulative results tables have been maintained for these four cancer sites, and another was added for esophageal cancer in Update 2004, but until now a global conclusion has been reached on gastrointestinal cancers overall while cancers associated with the liver have been considered sepa- rately. The committee decided to appraise the evidence separately for esophageal,
CANCER 325 stomach, colorectal, pancreatic, and hepatobiliary cancer to address VAâs concern that all types of cancer be reported on with the greatest degree of speciï¬city pos- sible and to implement its own conviction that the tissues along the span of the digestive tract are likely to vary in their risk factors and responses to carcinogens. Drawing discrete conclusions is somewhat complicated because reported results on those sites are grouped in a variety of ways that may be inï¬uenced by the nature of the observed results in a given study. For each of the cancer types previously grouped as âgastrointestinal tract tumorsâ with a categorization of limited or suggestive evidence of no association with exposure to the compounds of interest, this committee does conclude, how- ever, that there is inadequate or insufï¬cient evidence to support an association. There is not enough evidence to support an assertion about association, either positive or negative, with phenoxy herbicides or dioxin; and virtually no data are available on human response to cacodylic acid or picloram, so an assertion of no association with these two substances is not sustainable either. LARYNGEAL CANCER ACS estimated that 7,700 men and 1,810 women would receive diagnoses of cancer of the larynx (ICD-9 161) in the United States in 2006 and 2,950 men and 790 women would die from it (Jemal et al., 2006). Those numbers constitute a little more than 0.7 percent of new cancer diagnoses and deaths. The incidence of cancer of the larynx increases with age, and it is more common in men than in women, with a sex ratio in the United States of about 4:1 among persons 50â64 years old. The average annual incidence of laryngeal cancer is shown in Table 6-11. Established risk factors for laryngeal cancer are tobacco and alcohol use, which are independent and act synergistically. Occupational exposuresâlong and intense exposures to wood dust, paint fumes, and some chemicalsâalso could increase risk (ACS, 2007b). An IOM committee (2006) recently concluded that asbestos is a causal factor in laryngeal cancer (IOM, 2006); infection with human TABLE 6-11 Average Annual Cancer Incidence (per 100,000) of Laryngeal Cancer in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 10.4 9.7 21.9 15.8 15.4 28.3 24.1 24.4 38.0 Women 2.2 2.2 4.1 3.5 3.4 6.8 5.1 5.1 10.1 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
326 VETERANS AND AGENT ORANGE: UPDATE 2006 papilloma virus (HPV) might also raise the risk of laryngeal cancer (Hobbs and Burchall, 2004). Conclusions from VAO and Updates The committee responsible for VAO concluded that there was limited or suggestive evidence of an association between exposure to at least one of the compounds of interest and laryngeal cancer. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-12 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. The SMR for cancer of the larynx was not as- sociated with a JEM-based estimate of exposure to nonvolatile organochlorine compounds (never exposed: 18 cases; SMR 0.92, 95% CI 0.54â1.45; ever exposed: 20 cases; SMR 1.23, 95% CI 0.75â1.90). In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers from 1969 and 1973, respectively, through 2000. Laryngeal cancers were grouped with re- spiratory cancers (ICD-9 160â165; n 13); from the results for the subcategories, âtrachea, bronchus, lungâ (ICD-9 162; n 12) and âotherâ (ICD-9 163â165; n 1), it is evident that no laryngeal cancer deaths (ICD-9 161) were observed in either the producer or the sprayer group. Torchio et al. (1994) reported on the mortality experience of a cohort of 23,401 male farmers in the Piedmont area of Italy from the time they registered to use agricultural pesticides (1970â1974) through 1986. Those provinces are characterized by higher use of herbicides, particularly 2,4-D and MCPA, than the rest of the country. Mortality from laryngeal cancer was signiï¬cantly lower in the farmers than in the regional population (SMR 0.46, 95% CI 0.30â0.67). Reif et al. (1989) performed a series of caseâcontrol analyses on the sample of 19,904 people with speciï¬ed occupations among the 24,762 men 20 years old or older entered from 1980 to 1984 into the the New Zealand Cancer Registry. The focus of their study was on the 134 for whom forestry work was the most recent occupation listed. For each type of cancer, those with any other type of cancer were used as controls. Of 303 people with laryngeal cancer, two had most recently been forestry workers (OR 1.14, 95% CI 0.28â4.65).
CANCER 327 TABLE 6-12 Selected Epidemiologic StudiesâLaryngeal Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 18 0.9 (0.5â1.5) Ever 20 1.2 (0.8â1.9) ât Mannetje et al., Phenoxy herbicide producers (men and women) 0 * 2005 Phenoxy herbicide sprayers ( 99% men) 0 * Torchio et al., 1994 Italian farmers licensed to use pesticides 25 0.5 (0.3â0.7) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 2 1.1 (0.3â4.7) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 1 1.0 (0.0â5.1) Studies Reviewed in Update 2002 Thörn et al., 2000 Swedish lumberjacks exposed to phenoxyacetic herbicides Foremenâincidence 0 * Studies Reviewed in Update 1998 Gambini et al., 1997 Italian rice growers 7 0.9 (0.4â1.9) Kogevinas et al., IARC cohort (men and women) 21 1.6 (1.0â2.5) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 21 1.6 (1.0â2.5) Exposed to TCDD (or higher-chlorinated dioxins) 15 1.7 (1.0â2.8) Not exposed to TCDD (or higher-chlorinated dioxins) 5 1.2 (0.4â2.9) Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 2 2.9 (0.3â10.3) 0-year latency 2 2.9 (0.4â10.3) 15-year latency 1 â Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 162 0.7 (0.6â0.8) White women 0 â (0.0â3.3) Studies Reviewed in VAO Fingerhut et al., NIOSHâentire cohort 7 2.1 (0.8â4.3) 1991 1-year exposure, 20-year latency 3 2.7 (0.6â7.8) Manz et al., 1991 German production workersâmen and women (included in the IARC cohort) 2 2.0 (0.2â7.1) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 8 1.5 (0.6â2.9) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 1 3.0 (0.0â16.8) continued
328 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-12 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 4 2.3 (0.5â4.5) ENVIRONMENTAL Studies Reviewed in Update 2002 Revich et al., 2001 Residents of Chapaevsk, Russia Men 13 2.3 (1.2â3.8) Women 1 0.1 (0.0â0.6) Studies Reviewed in Update 2000 Bertazzi et al., 2001d Seveso residentsâ20-year follow-up Zone A, Bâmen 64 1.3 (1.0â1.6) women 5 0.7 (0.3â1.7) Bertazzi et al., 1998e Seveso residentsâ15-year follow-up Zone Bâmen 40 1.2 (0.9â1.7) women 2 0.5 (0.1â2.0) Zone Râmen 208 0.9 (0.8â1.1) women 35 1.1 (0.8â1.5) VIETNAM VETERANS New Studies ADVA, 2005a Australian Vietnam veterans vs Australian populationâincidence 97 1.5 (1.2â1.8) Navy 21 1.5 (0.9â2.1) Army 69 1.6 (1.2â1.9) Air Force 7 0.8 (0.3â1.7) ADVA, 2005b Australian Vietnam veterans vs Australian populationâmortality 28 1.1 (0.7â1.5) Navy 6 1.1 (0.4â2.4) Army 19 1.1 (0.7â1.7) Air Force 3 0.8 (0.2â2.5) ADVA, 2005c Australian men conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 8 0.7 (0.2â1.6) Mortality 2 0.4 (0.0â2.4) Boehmer et al., 2004 CDC Vietnam Experience Cohort 0 0 (*) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans Oral cavity, pharynx, and larynx 4 0.6 (0.2â2.4) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 12 1.3 (0.7â2.2) CDVA, 1997b Australian National Service Vietnam veterans 0 0 (0â 10)
CANCER 329 TABLE 6-12 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Watanabe and Kang, Army Vietnam veterans compared with US men 50 1.3* 1996 Marine Vietnam veterans 4 0.7* Army Vietnam veterans 50 1.4e ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, methyl-4- chlorophenoxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d Report did not separate laryngeal from lung and other respiratory cancers. e Statistically signiï¬cant with the 95% CI not including 1.0. * Information not provided by study authors. Studies in italics have been superseded by newer studies of the same cohorts. Environmental Studies No relevant environmental studies concerning exposure to the compounds of interest and laryngeal cancer were published since Update 2004. Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported no deaths from laryngeal cancer in the deployed and two in the non- deployed. (The researchers estimated rate ratios only for sites of cancer with 10 or more deaths.) A series of reports providing updates on the health status of Australian Vietnam veterans found a signiï¬cant association with the incidence of laryngeal cancer (SIR 1.46, 95% CI 1.17â1.75) (ADVA, 2005a) but not with mortality from laryngeal cancer (SMR 1.09, 95% CI 0.69â1.49) (ADVA, 2005b) when comparing veterans with the general population. When Australian veterans de- ployed to Vietnam were compared with those not deployed there, however, both laryngeal-cancer incidence and mortality were non-signiï¬cantly reduced (RR 0.65, 95% CI 0.24â1.60 and RR 0.42, 95% CI 0.04â2.37, respectively [ADVA, 2005c]).
330 VETERANS AND AGENT ORANGE: UPDATE 2006 Biologic Plausibility No animal studies have identiï¬ed an association between exposure to the compounds of interest and an increased incidence of laryngeal cancer. The bio- logic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Only three reports (all on Australian Vietnam veterans) published since Up- date 2004 provided any useful data regarding the association between exposure to the compounds of interest and laryngeal cancer. Only in the study of cancer incidence compared with the general population was the rate of laryngeal cancer convincingly increased (ADVA, 2005a), but the study that included a reference group for comparing Vietnam-era veterans did not support the hypothesis that the increase was associated with having been in Vietnam (ADVA, 2005a). The conclusion that there is limited or suggestive evidence of an association between exposure to the compounds of interest and laryngeal cancer is not affected by the results of the new studies. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is limited or suggestive evi- dence of an association between exposure to at least one compound of interest and laryngeal cancer. LUNG CANCER Lung cancer (carcinomas of the lung and bronchus, ICD-9 162.2â162.9) is the leading cause of cancer death in the United States. ACS estimated that 92,700 men and 81,770 women would receive diagnoses of lung cancer in the United States in 2006 and about 90,330 men and 72,130 women would die from it (Jemal et al., 2006). Those numbers represent roughly 12.5 percent of new cancer diag- noses and 29 percent of cancer deaths in 2006. The principal types of lung neo- plasms are identiï¬ed collectively as bronchogenic carcinoma (the bronchi are the two main branches of the trachea) and carcinoma of the lung. The trachea (ICD-9 162.0) is frequently grouped with the lung and bronchus under ICD-9 162. The lung is also a common site of the development of metastatic tumors. In men and women, the incidence of lung cancer increases greatly beginning at about the age of 40 years. The incidence in people 50â54 years old is double that in people 45â49 years old, and it doubles again in those 55â59 years old. The incidence is consistently higher in black men than in women or white men.
CANCER 331 The average annual incidence of lung cancer in the United States is shown in Table 6-13. ACS estimates that more than 90 percent of lung cancers in men are attrib- utable to tobacco use (ACS, 1998). Smoking increases the risk of all histologic types of lung cancer, although the associations with squamous-cell and small-cell carcinomas are strongest. Other risk factors include exposure to asbestos, ura- nium, vinyl chloride, nickel chromates, coal products, mustard gas, chloromethyl ethers, gasoline, diesel exhaust, and inorganic arsenic (this does not imply that cacodylic acid, which is a metabolite of inorganic arsenic, can also be assumed to be a risk factor). Important environmental risk factors include exposure to tobacco smoke and radon (ACS, 2007c). Conclusions from VAO and Updates The committee responsible for VAO concluded that there was limited or sug- gestive evidence of an association between exposure to at least one compound of interest and lung cancer. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-14 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. The SMR of lung cancer was not associated with a JEM-based estimate of exposure to nonvolatile organochlorine compounds (never exposed: 356 cases; SMR 0.98, 95% CI 0.88â1.08; ever exposed: 314 cases; SMR 1.04, 95% CI 0.93â1.17). TABLE 6-13 Average Annual Incidence (per 100,000) of Lung and Bronchial Cancer in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 58.9 54.0 123.2 123.1 114.2 244.5 230.6 224.9 362.8 Women 46.7 47.0 67.0 96.0 98.2 125.5 159.3 168.3 177.6 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
332 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-14 Selected Epidemiologic StudiesâLung and Bronchus Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workersâ exposure to nonvolatile organochlorine compounds Lung (ICD-9 162) Never 356 1.0 (0.9â1.1) Ever 314 1.0 (0.9â1.2) Pleura (ICD-9 163) Never 17 2.8 (1.6â4.5) Ever 4 0.8 (0.2â2.0) Other Respiratory (ICD-9 164â165) Never 8 2.1 (0.9â4.2) Ever 2 0.7 (0.1â2.4) Alavanja et al., 2005 US Agriculture Health Studyâincidence (lung) Private applicators (men and women) 266 0.5 (0.4â0.5) Spouses of private applicators ( 99% women) 68 0.4 (0.3â0.5) Commercial applicators (men and women) 12 0.6 (0.3â1.0) Blair et al., 2005a US Agriculture Health Study (lung) Private applicators (men and women) 129 0.4 (0.3â0.4) Years handled pesticides 10 years 25 0.4* (p 0.05) 10 years 80 0.3* (p 0.05) Spouses of private applicators ( 99% women) 29 0.3 (0.2â0.5) ât Mannetje et al., New Zealand phenoxy herbicide workers 2005 (trachea, bronchus, lung) Producers (men and women) 12 1.4 (0.7â2.4) Sprayers ( 99% men) 5 0.5 (0.2â1.1) Torchio et al., 1994 Italian licensed pesticide users 155 0.5 (0.4â0.5) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 30 1.3 (0.8â1.9) Studies Reviewed in Update 2004 Bodner et al., 2003 Dow chemical production workersâ lung (included in the IARC cohort and the NIOSH Dioxin Registry) 54 0.8 (0.6â1.1) Swaen et al., 2004 Dutch licensed herbicide applicators (trachea and lung) 27 0.7 (0.5â1.0) Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4âD production workers (included in the IARC cohort and the NIOSH Dioxin Registry) Respiratory system 31 0.9 (0.6â1.3)
CANCER 333 TABLE 6-14 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Thörn et al., 2000 Swedish lumberjacks exposed to phenoxy herbicides Foremenâincidence (bronchus and lung) 1 4.2 (0.1â23.2) Studies Reviewed in Update 2000 Steenland et al., 1999 US chemical production workersâlung (included in the IARC cohort and the NIOSH Dioxin Registry) 125 1.1 (0.9â1.3) Studies Reviewed in Update 1998 Gambini et al., 1997 Italian rice growers (lung) 45 0.8 (0.6â1.1) Kogevinas et al., 1997 IARC cohort (men and women, lung) Workers exposed to any phenoxy herbicide or chlorophenol 380 1.1 (1.0â1.2) Exposed to TCDD (or higher- chlorinated dioxins) 225 1.1 (1.0â1.3) Not exposed to TCDD (or higher- chlorinated dioxins) 148 1.0 (0.9â1.2) Becher et al., 1996 German production workers (included in the IARC cohort) (lung) 47 1.4 (1.1â1.9) Ott and Zober, 1996 BASF employeesâincidence Respiratory system 13 1.2 (0.6â2.0) TCDD ( g/kg of body weight) 0.1â0.99 2 0.7 (0.1â2.5) 1 8 2.0 (0.9â3.9) Lung or bronchus 11 1.1 (0.6â2.0) TCDD ( g/kg of body weight) 0.1â0.99 2 0.8 (0.1â2.8) 1 8 2.2 (1.0â4.3) Ramlow et al., 1996 Dow pentachlorophenol production workersârespiratory system (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 18 1.0 (0.6â1.5) 15-year latency 17 1.1 (0.6â1.8) Studies Reviewed in Update 1996 Asp et al., 1994 Finnish herbicide applicators 1972â1989 (trachea, bronchus, lung) Incidence 39 0.9 (0.7â1.3) Mortality 37 1.0 (0.7â1.4) Blair et al., 1993 US farmers from 23 states (lung) White men 6,473 0.9 (0.9â0.9) White women 57 0.8 (0.6â1.1) Bloemen et al., 1993 Dow 2,4-D production workersârespiratory system (included in the IARC cohort and the NIOSH Dioxin Registry) 9 0.8 (0.4â1.5) continued
334 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-14 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Kogevinas et al., 1993 IARC cohort, women (lung)âincidence 2 1.4 (0.2â4.9) Lynge, 1993 Danish production workers, men (lung)â incidence (included in the IARC cohort) 13 1.6 (0.9â2.8) Studies Reviewed in VAO Bueno de Mesquita Dutch phenoxy herbicide workers (included et al., 1993 in the IARC cohort) (trachea, bronchus, lung) 9 0.8 (0.4â1.5) Swaen et al., 1992 Dutch herbicide applicators (trachea and lung) 12 1.1 (0.6â1.9) Coggon et al., 1991 British phenoxy herbicide workers (lung) (included in the IARC cohort) 19 1.3 (0.8â2.1) Workers with exposure above background levels 14 1.2 (0.7â2.1) Fingerhut et al., 1991 NIOSHâentire cohort (trachea, bronchus, lung) 89 1.1 (0.9â1.4) 1-year exposure; 20-year latency 40 1.4 (1.0â1.9) Green, 1991 Herbicide sprayers in Ontario (lung) 5 * Manz et al., 1991 German production workers, men (lung) (included in the IARC cohort) 26 1.7 (1.1â2.4) Saracci et al., 1991 IARC cohort, men and women (trachea, bronchus, lung) 173 1.0 (0.9â1.2) McDufï¬e et al., 1990 Saskatchewan farmers applying herbicides (lung) 103 0.6 (* NS) Zober et al., 1990 BASF employees (trachea, bronchus, lung)âincidence 4 2.0 (0.7â4.6) Bender et al., 1989 Herbicide sprayers in Minnesota (trachea, bronchus, lung) 54 0.7 (0.5â0.9) Wiklund et al., 1989a Swedish pesticide applicators (trachea, bronchus, lung) 38 0.5 (0.4â0.7) Bond et al., 1988 Dow 2,4-D production workersâlung (included in the IARC cohort and the NIOSH Dioxin Registry) 8 1.0 (0.5â2.0) Low cumulative exposure 1 0.7 (* NS) Medium cumulative exposure 2 1.0 (* NS) High cumulative exposure 5 1.7 (* NS) Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) (lung, pleura, and retroperitoneal) 117 1.2 (1.0â1.4) Background exposure 39 1.0 (0.7â1.4) Low-grade exposure 35 1.1 (0.8â1.6) High-grade exposure 43 1.3 (1.0â1.8) Lynge, 1985 Danish production workersâlung, incidence (included in the IARC cohort) Men 38 1.2* Women 6 2.2*
CANCER 335 TABLE 6-14 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Blair et al., 1983 Licensed pesticide applicators in Florida, lawn and ornamental pest category only (lung) 7 0.9* Axelson et al., 1980 Swedish herbicide sprayers (lung) 3 1.4* ENVIRONMENTAL Studies Reviewed in Update 2004 Fukuda et al., 2003 Residents of municipalities in Japan with vs without waste incineration plants (lung) Age-adjusted mortality (100,000), men 39.0 6.7 vs 41.6 9.1 (p 0.001) Age-adjusted mortality (100,000), women 13.7 3.8 vs 14.3 4.6 (p 0.11) Studies Reviewed in Update 2002 Revich et al., 2001 Residents of Chapaevsk, Russia (lung) Men 168 3.1 (2.6â3.5) Women 40 0.4 (0.3â0.6) Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-upâ incidence (lung) Zones A, Bâmen 57 1.3 (1.0â1.7) women 4 0.6 (0.2â1.7) Bertazzi et al., 1998 Seveso residentsâ15-year follow-upâ incidence (lung) Zone Aâmen 4 1.0 (0.4â2.6) Zone Bâmen 34 1.2 (0.9â1.7) women 2 0.6 (0.1â2.3) Zone Râmen 176 0.9 (0.8â1.1) women 29 1.0 (0.7â1.6) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-upâ incidence (lung) Zone Aâmen 4 1.0 (0.3â2.5) Zone Bâmen 34 1.2 (0.9â1.7) women 2 0.6 (0.1â2.1) Zone Râmen 176 0.9 (0.8â1.0) women 29 1.0 (0.7â1.5) Svensson et al., 1995 Swedish ï¬shermen East coast (lung and larynx) 16 0.8 (0.5â1.3) West coast (lung and larynx) 77 0.9 (0.7â1.1) continued
336 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-14 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in VAO Bertazzi et al., 1993 Seveso residentsâ10-year follow-upâ incidence (trachea, bronchus, lung) Zone Aâmen 2 0.8 (0.2â3.4) Zone Bâmen 18 1.1 (0.7â1.8) Zone Râmen 96 0.8 (0.7â1.0) women 16 1.5 (0.8â2.5) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 576 1.2 (1.1â1.3) Branch of Service Navy 141 1.4 (1.2â1.7) Army 372 1.2 (1.1â1.3) Air Force 63 1.0 (0.7â1.2) Histologic type Adenocarcinoma 188 1.5 (1.2â1.7) Squamous 152 1.2 (1.0â1.4) Small-cell 87 1.2 (0.97â1.5) Large-cell 79 1.1 (0.8â1.3) Other 70 1.1 (0.8â1.3) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 544 1.2 (1.1â1.3) Branch of service Navy 135 1.4 (1.2â1.6) Army 339 1.1 (1.0â1.6) Air Force 71 1.1 (0.9â1.4) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence (1982â2000) 78 2.4 (1.6â3.5) Histologic type Adenocarcinoma 27 2.7 (1.3â5.6) Squamous 19 5.0 (1.8â17.0) Small-cell 14 2.1 (0.9â5.5) Large-cell 8 1.1 (0.4â3.3) Other 10 1.8 (0.6â5.5) Mortality (1966â2001) 67 1.8 (1.2â2.7)
CANCER 337 TABLE 6-14 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Pavuk et al., 2005 White Air Force comparison subjects only (respiratory system)âincidence Serum TCDD levels (pg/g), based on model with exposure variable loge(TCDD)d Per unit increase of âloge(TCDD) in pg/g 36 1.7 (0.9â3.2) Quartiles (pg/g) 0.4â2.6 6 1.0 2.6â3.8 8 1.1 (0.3â3.4) 3.8â5.2 9 1.2 (0.4â3.5) 5.2 13 1.9 (0.7â5.5) Number of years served in Southeast Asia (SEA) Per year of service 36 1.1 (0.9â1.2) Quartiles (years in SEA) 0.8â1.3 8 1.0 1.3â2.1 4 0.5 (0.2â1.8) 2.1â3.7 11 0.7 (0.3â2.0) 3.7â16.4 13 0.7 (0.3â2.0) Boehmer et al., 2004 Follow-up of CDC Vietnam Experience Cohort (trachea, bronchus, lung) 41 1.0 (0.6â1.5) Low pay grade at time of discharge * 1.6 (0.9â3.0) High pay grade at time of discharge * 0.8 (0.6â1.1) Studies Reviewed in Update 2004 Akhtar et al., 2004 White AFHS subjects vs national rates (respiratory system) Ranch Hand veterans Mortalityâall 21 0.9 (0.6â1.3) Incidenceâall 33 1.1 (0.8â1.6) With tours between 1966â1970 26 1.1 (0.7â1.6) Comparison veterans Mortalityâall 38 1.1 (0.8â1.5) Incidenceâall 48 1.2 (0.9â1.6) With tours between 1966â1970 37 1.2 (0.9â1.6) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans (lung and bronchus) 10 3.7(0.8â17.1) AIHW, 1999 Australian Vietnam veteransâValidation 65 expected study (lung) 46e (49â81) CDVA, 1998a 65 expected Australian Vietnam veterans (lung) 120 (49â89) Studies Reviewed in Update 1998 CDVA, 1997a Australian Vietnam veterans (lung) 212 1.3 (1.1â1.4) CDVA, 1997b Australian National Service Vietnam veterans (lung) 27 2.2 (1.1â4.3) continued
338 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-14 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Dalager and Kang, Army Chemical Corps veterans (respiratory 1997 system) 11 1.4 (0.4â5.4) Mahan et al., 1997 Caseâcontrol of Vietnam-era Vietnam veteransâincidence (lung) 134 1.4 (1.0â2.0) Watanabe and Kang, US Army and Marine Corps Vietnam 1996 veterans (lung) Army Vietnam service 1,139 1.1* (p 0.05) Non-Vietnam 1,141 1.1* (p 0.05) Marine Vietnam service 215 1.2 (1.0â1.3) Non-Vietnam 77 0.9* Watanabe and Kang, Marine Vietnam service vs non-Vietnam 1995 (lung) 42 1.3 (0.8â2.1) ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; AIHW, Australian Institute of Health and Welfare; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; MCPA, methyl- 4-chlorophenoxyacetic acid; NS, not signiï¬cant; PCDD, polychlorinated dibenzodioxin; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d The original paper implied that the exposure metric for TCDD was based on actual measured serum levels of TCDD. Subsequent correspondence between the Committee and the investigators indicated that the metric was actually transformed using the natural logarithm of TCDD. e Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have lung cancer?â * Information not provided by study authors. Studies in italics have been superseded by newer studies of the same cohorts. Publications arising from the US AHS have provided ï¬ndings on the risk of lung cancer in farmers (private pesticide applicators), their spouses, and commer- cial pesticide applicators, but no results peculiar to any of the herbicides under consideration here have been published. Blair et al. (2005a) reported that farmers and their spouses both had mortality from lung cancer substantially lower than the general population of Iowa and North Carolina, with rate ratios of around 0.4 (see Table 6-14). Such low mortality may have been due to chance, the healthy-worker effect, lower consumption of tobacco, increased level of exercise, or the protec- tive effect of endotoxins to which many agricultural workers may be exposed. In a publication on the incidence of lung cancer through 2001, Alavanja et al. (2004) stated, without giving quantitative results, that the farmers had a markedly lower incidence of lung cancer than the general populations of their states, which
CANCER 339 might be largely attributable to low rates of smoking; 2,4-D was not among the chemicals for which speciï¬c rate ratios were provided, although it was implicit that 2,4-D exposure had been analyzed for any association with the occurrence of lung cancer. A later publication on cancer incidence from recruitment through 2002 (Alavanja et al., 2005) presented ï¬ndings on subgroups (farmers, their spouses, and commercial applicators; see Table 6-14), none of which showed an increased risk of lung cancer. In a cohort study in New Zealand, ât Mannetje et al. (2005) found that mortality from cancer of the trachea, bronchus, or lung (ICD-9 162) showed a non-signiï¬cant excess (SMR 1.4, 95% CI 0.7â2.4) in phenoxy herbicide pro- ducers, who also had potential exposure to dioxins. Among phenoxy herbicide sprayers, however, the estimated risk was lower than expected (SMR 0.5, 95% CI 0.2â1.1). Torchio et al. (1994) reported on the mortality experience of a cohort of 23,401 male farmers in the Piedmont area of Italy from the time when they reg- istered to use agricultural pesticides (1970â1974) through 1986. The provinces in that area are characterized by higher use of herbicides, particularly 2,4-D and MCPA, than the rest of the country. The estimated risk of lung cancer was signiï¬cantly reduced (155 cases; SMR 0.45, 95% CI 0.38â0.52). The authors suggested that the relatively short duration of follow-up and the healthy-worker effect contributed to the observation of reduced mortality. Reif et al. (1989) performed a series of caseâcontrol analyses on the sample of 19,904 people with speciï¬ed occupations among the 24,762 men 20 years old or older entered from 1980 to 1984 into the the New Zealand Cancer Registry. The focus of their study was on the 134 for whom forestry work was the most recent occupation listed. For each type of cancer, the registrants with any other type of cancer were used as controls. Of 4,224 people with lung cancer, 30 had most recently been forestry workers (OR 1.27, 95% CI 0.84â1.91). Environmental Studies No new environmental studies concerning exposure to the compounds of interest and respiratory cancer were published since Update 2004. Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) did not ï¬nd any excess risk of mortality from lung cancer in the entire cohort (CRR 0.94, 95% CI 0.62â1.48) but did observe an association in veterans who were classiï¬ed as having a low pay grade at the time of discharge (RR 1.64, 95% CI 0.94â2.89). When the ï¬rst ï¬ndings of the study (Boyle et al., 1987) were considered in VAO, mortality had been too low to support any conclusions. Pavuk et al. (2005) analyzed the incidences of several types of cancer in
340 VETERANS AND AGENT ORANGE: UPDATE 2006 subjects in the comparison group in the AFHS in 1982â2003 in terms of their serum TCDD concentrations and the number of years served in Southeast Asia. Their work extends to people with lower TCDD exposures the analyses of can- cer incidences observed in the Ranch Hand subjects themselves (Akhtar et al., 2004), which were considered in Update 2004. In those analyses, cancers of the lung were included with other cancers of the ârespiratory system.â There was a non-signiï¬cant increase in the incidence of cancer of the respiratory tract with increased serum TCDD (RR 1.7 per unit increase in loge[TCDD concentration in picograms per gram], 95% CI 0.9â3.2). However, there was no evidence of an association between the number of years of service in Southeast Asia and the incidence of respiratory cancer (see Table 6-14 for a comparison of the risks estimated for the quartiles of TCDD concentrations with the number of years served in Southeast Asia). The recent update of the health experience of Australian Vietnam veterans showed signiï¬cant associations with the incidence of lung cancer (SIR 1.23, 95% CI 1.13â1.33) (ADVA, 2005a) and mortality (SMR 1.18, 95% CI 1.08â 1.28) (ADVA, 2005b) when all Vietnam veterans (all male, all branches, âdefence forces,â and âCitizen Military Forcesâ) were compared with the general popula- tion of Australia. When conscripted male Army veterans deployed to Vietnam (National Service veterans) were compared with their non-deployed counterparts (National Service non-veterans), the increase in the incidence of lung cancer was more pronounced (SIR 2.35, 95% CI 1.60â3.49) (ADVA, 2005c). The lat- ter analysis makes use of the presumably more comparable reference group of other veterans and may account for the underestimation of rate ratios obtained when the general population is used (the healthy-warrior effect). There was some variation in rate ratios with branch of service for both incidence of lung cancer (ADVA, 2005a) and mortality from it (ADVA, 2005b); increases were most pro- nounced in the Navy, substantial in the Army, and equivocal in the Air Force (see Table 6-14). Rate ratios of some histologic subtypes, especially adenocarcinomas and squamous-cell carcinomas, were higher. Biologic Plausibility As noted in previous VAO reports, there is evidence of increased incidence of squamous-cell carcinoma of the lung in male and female rats exposed to TCDD at high concentrations (Kociba et al., 1978; Van Miller et al., 1977). A more recent study reported a signiï¬cant increase in cystic keratinizing epitheliomas in female rats exposed to TCDD for 2 years (NTP, 2006), and increases in the incidences of bronchiolar metaplasia, acinar vacuolization, and inï¬ammation were observed in the high-dose (100-ng/kg) group. A recent 2-year study of F344 rats exposed to cacodylic acid at 0â100 ppm and B6C3F1 mice exposed at 0â500 ppm failed to detect neoplasms in the lung at any dose (Arnold et al., 2006); this ï¬nding is consistent with that of previous studies. However, exposure to cacodylic acid has previously been shown to in-
CANCER 341 crease tumor multiplicity in mouse strains susceptible to developing lung tumors (for example, A/J strain; Hayashi et al., 1998) or mice pretreated with an intitiat- ing agent (4-nitroquinoline 1-oxide; Yamanaka et al., 1996). The data indicate that cacodylic acid may act as a tumor promoter in the lung. The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis The evidence remains inconclusive but suggestive of an association between exposure to at least one compound of interest and the risk of developing or dying from lung cancer. The best evidence comes from studies of heavily exposed occu- pational cohorts. The latest ï¬ndings from the US AFHS suggest an increase in risk with concentration of serum TCDD even in the subjects who made up the comparison group, whose TCDD exposure was considerably lower than that of the main Ranch Hand group. The American and Australian cohort studies of Viet- nam veterans, which presumably cover a large proportion of exposed soldiers, show higher than expected incidence of and mortality from lung cancer. The main limitations of those studies are that there was no assessment of exposure, as there was in, for example, the Ranch Hand study, and that some potential confound- ing variables, notably smoking, could not be accounted for. It is unlikely that the distribution of smoking would differ greatly between veteran cohorts, so the likelihood of important confounding by smoking is probably low. Those studies therefore lend support to the ï¬ndings of the Ranch Hand study. The method- ologically sound US AHS did not show any increased risks of lung cancer, but, although there was substantial 2,4-D exposure in this cohort (Blair et al., 2005b), dioxin exposure of these contemporary farmers was probably negligible. The evi- dence from occupational studies remains inconsistent; for example, in the study by Bodner et al. (2003), no excess risks of lung cancer in chemical-company employees were found, but these results must be weighed against results in pre- viously reviewed occupational cohorts that did show evidence of an association (Becher et al., 1996; Ott and Zober, 1996; Steenland et al., 1999). Also supportive of an association are the numerous lines of mechanistic evidence, discussed in the section on biologic plausibility, which provide fur- ther support for the conclusion that the evidence of an association is limited or suggestive. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is limited or suggestive evidence of an association between exposure to at least one compound of interest and carcinomas of the lung, bronchus, and trachea.
342 VETERANS AND AGENT ORANGE: UPDATE 2006 BONE AND JOINT CANCER ACS (2006) estimated that about 1,500 men and 1,260 women would re- ceive diagnoses of bone or joint cancer (ICD-9 170) in the United States in 2006 and that 730 men and 530 women would die from these cancers. Primary bone cancers are among the least common malignancies, but the bones are frequent sites of tumors secondary to cancers that have metastasized. Only primary bone cancer is considered here. The average annual incidence of bone and joint cancer is shown in Table 6-15. Bone cancer is more common in teenagers than in adults. It is rare among people in the age groups of most Vietnam veterans (50â64 years). Among the risk factors for adultsâ contracting of bone or joint cancer are exposure to ionizing radiation in treatment for other cancers and a history of some non-cancer bone diseases, including Pagetâs disease. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and bone and joint cancer. Additional in- formation available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-16 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers from 1969 and 1973, respectively, through 2000. No deaths from bone and joint cancer (ICD-9 170) were observed in either the producer or sprayer group. TABLE 6-15 Average Annual Incidence (per 100,000) of Bone and Joint Cancer in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 0.9 0.9 0.7 1.1 1.2 1.1 1.4 1.5 1.0 Women 0.9 1.0 0.4 0.9 1.1 0.3 1.0 1.0 0.4 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
CANCER 343 TABLE 6-16 Selected Epidemiologic StudiesâBone and Joint Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies Merletti et al., 2006 Association of occupational exposure and risk 18 2.6 (1.5â4.6) of bone sarcoma ât Mannetje et al., Phenoxy herbicide producers and sprayers 0 â 2005 (men and women) Torchio et al., 1994 Italian licensed pesticide users 10 0.8 (0.4â1.4) Reif et al., 1989 New Zealand forestry workersânested 1 1.7 (0.2â13.3) caseâcontrol (incidence) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licenced herbicide applicators 0 â Studies Reviewed in Update 2000 Rix et al., 1998 Danish paper mill workersâincidence Men 1 0.5 (0.0â2.7) Women 0 â Studies Reviewed in Update 1998 Gambini et al., 1997 Italian rice growers 1 0.5 (0.0â2.6) Hertzman et al., 1997 British Columbia sawmill workers Mortality 5 1.3 (0.5â2.7) Incidence 4 1.1 (0.4â2.4) Kogevinas et al., 1997 IARC cohort (men and women) 5 1.2 (0.4â2.8) Workers exposed to any phenoxy herbicide 5 1.2 (0.4â2.7) or chlorophenol Exposed to TCDD (or higher-chlorinated 3 1.1 (0.2â3.1) dioxins) Not exposed to TCDD (or higher- 2 1.4 (0.2â5.2) chlorinated dioxins) Ramlow et al., 1996 Dow pentachlorophenol production workers 0 * (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 0 â 15-year latency 0 â Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 49 1.3 (1.0â1.8) White women 1 1.2 (0.0â6.6) Collins et al., 1993 Monsanto Company workers (included in the 2 5.0 (0.6â18.1) NIOSH cohort) Studies Reviewed in VAO Ronco et al., 1992 Danish and Italian farm workers Male Danish farmers 9 0.9* Female Danish farmers 0 * Fingerhut et al., 1991 NIOSHâentire cohort 2 2.3 (0.3â8.2) 1-year exposure, 20-year latency 1 5.5 (0.1â29.0) Zober et al., 1990 BASF employeesâbasic cohort 0 0 (0.0â65.5) continued
344 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-16 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Bond et al., 1988 Dow 2,4-D production workers (included in the 0 â (0.0â31.1) IARC cohort and the NIOSH Dioxin Registry) Coggon et al., 1986 British MCPA production workers (included in 1 0.9 (0.0â5.0) the IARC cohort) Wiklund, 1983 Swedish male and female agricultural 44 1.0 (0.6â1.4)d workersâincidence Burmeister, 1981 Iowa farmers 56 1.1 (NS) ENVIRONMENTAL Studies Reviewed in Update 2002 Revich et al., 2001 Residents of Chapaevsk, Russia Mortality standardized to Samara Region (bone, soft-tissue cancer) Men 7 2.1 (0.9â4.4) Women 7 1.4 (0.6â3.0) Studies Reviewed in Update 2000 Bertazzi et al., 1998 Seveso residentsâ15-year follow-up Zone Bâwomen 1 2.6 (0.3â19.4) Zone Râmen 2 0.5 (0.1â2.0) women 7 2.4 (1.0â5.7) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Bâwomen 1 2.6 (0.0â14.4) Zone Râmen 2 0.5 (0.1â1.7) women 7 2.4 (1.0â4.9) VIETNAM VETERANS Studies Reviewed in Update 1998 Clapp, 1997 Massachusetts Vietnam veterans 4 0.9 (0.1â11.3) AFHS, 1996 Air Force Ranch Hand veterans 0 * Studies Reviewed in VAO Breslin et al., 1988 Army Vietnam veterans 27 0.8 (0.4â1.7) Marine Vietnam veterans 11 1.4 (0.1â21.5) Anderson et al., 1986b Wisconsin Vietnam veterans 1 * Lawrence et al., 1985 New York Vietnam veterans 8 1.0 (0.3â3.0) ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; AFHS, Air Force Health Study; CI, con- ï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, methyl-4-chlorophen- oxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; NS, not signiï¬cant; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d 99% CI. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts.
CANCER 345 Merletti et al. (2006) reported results from a multicenter caseâcontrol study conducted in seven European countries in 1995â1997 and focused on rare cancers, including bone sarcomas. A total of 96 cases were identiï¬ed, and controls were selected in at least a 1:4 ratio and matched on the basis of age group, sex, and region. Exposure was determined indirectly solely on the basis of self-reported job titles. Although risk was signiï¬cantly increased in those who reported use of pesticides, insecticides, or herbicides, no data are given with respect to the speciï¬c compounds of interest to this report. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics re- ports as having high herbicide use, especially of 2,4-D and MCPA. The estimated risk of bone cancer was reduced (10 cases; SMR 0.75, 95% CI 0.36â1.38). Starting with the 19,904 men entered into the the New Zealand Cancer Reg- istry from 1980â1984 with a speciï¬ed occupation, Reif et al. (1989) contrasted the 49 cases of bone cancer with the remaining subjects having other types of cancer. Of the 134 cancer registrants for whom forestry worker (with presumed exposure to phenoxy herbicides and chlorophenols) was the most recent occupa- tion, the proportion with bone cancer (1 case; OR 1.72, 95% CI 0.22â13.30) was not signiï¬cantly elevated. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and bone and joint cancer were published since Update 2004. Vietnam-Veteran Studies The AFHS completed the report on its scheduled 2002 follow-up examina- tion of participants. The examination included questionnaires, physical examina- tions, and clinical assessments, all of which were used to ascertain bone-cancer risk in participants. Too few events were observed in the cohort to allow assess- ment of the risk. The Third Australian Vietnam Veterans Mortality Study 2005 assessed mor- tality in Australian Vietnam veterans in all branches of service. Mortality ex- perience (through 2001) in the veterans was compared with that in the general population of Australia. However, too few cases of bone cancer were observed in the cohort to allow assessment of RR. Biologic Plausibility No animal studies reported an increased incidence of bone and joint cancers after exposure to the compounds of interest. The biologic plausibility of the car- cinogenicity of the compounds of interest in general is summarized at the end of this chapter.
346 VETERANS AND AGENT ORANGE: UPDATE 2006 Synthesis Results of several pertinent studies have been published since the previous update and were noted above. The studies either reported a non-signiï¬cant in- crease in risk of bone and joint cancer, observed too few events to estimate RR adequately, or did not present data that sufï¬ciently linked observed results to speciï¬c compounds of interest to this report. Thus, the new results add little to the previous body of results, summarized in Table 6-16, that taken together do not indicate an association between exposure to the compounds of interest and bone cancer. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and bone cancer. That conclusion is based on occupational and environmental studies in which subjects were exposed to a variety of herbi- cides and herbicide mixtures. SOFT-TISSUE SARCOMAS Soft-tissue sarcoma (STS) (ICD-9 164.1, 171) arises in soft somatic tis- sues within and between organs. Three of the most common types of STSâ liposarcoma, ï¬brosarcoma, and rhabdomyosarcomaâoccur in similar numbers in men and women. Because of the diverse characteristics of STS, accurate diagnosis and classiï¬cation can be difï¬cult. ACS estimated that in 2006 about 5,720 men and 3,810 women would receive diagnoses of STS in the United States and that about 1,830 men and 1,670 women would die from it (ACS, 2006). The average annual incidence of STS is shown in Table 6-17. TABLE 6-17 Average Annual Incidence (per 100,000) of Soft-Tissue Sarcoma (Including Malignant Neoplasms of the Heart) in United States a 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 4.2 4.3 4.3 5.0 4.9 6.7 6.7 7.3 3.5 Women 2.9 3.1 3.1 4.2 4.0 7.1 5.1 4.8 7.7 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
CANCER 347 Among the risk factors for STS are exposure to ionizing radiation during treatment for other cancers and some inherited conditions, including Gardnerâs syndrome, Li-Fraumeni syndrome, and neuroï¬bromatosis. Several chemical exposures have been identiï¬ed as possible risk factors (Zahm and Fraumeni, 1997). Conclusions from VAO and Updates The committee responsible for VAO judged that the strong ï¬ndings in the IARC and NIOSH cohorts, plus extensive Scandinavian caseâcontrol studies, complemented by consistency in preliminary reports on the Seveso population and one statistically signiï¬cant ï¬nding in a state study of Vietnam veterans, con- stituted sufï¬cient information to determine that there is an association between exposure to at least one of the compounds of interest and STS. Additional infor- mation available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-18 summarizes the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. Mortality rates for soft-tissue sarcoma stan- dardized with the national rates of the 11 contributing countries did not indicate any association to nonvolatile organochlorine compounds, including TCDD (ever exposed: 4 cases, SMR 0.80, 95% CI 0.22â2.04; never exposed: 8 cases, SMR 1.22, 95% CI 0.53â2.41) as derived using a JEM approach. In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers from 1969 and 1973, respectively, through 2000. A single death from STS (ICD-9 171) was observed (0.23 expected) in the sprayer group. In a prospective cohort study of private pesticide applicators, commercial applicators, and spouses of the private applicators, Alavanja et al. (2005) reported 10 and 3 incident cases of âsoft tissueâ cancer in the private applicators (SIR 0.65, 95% CI 0.31â1.20) and their spouses (SIR 0.48, 95% CI 0.10â1.41), respectively, and none among the commercial applicators; those results led to non-signiï¬cant risk estimates below the null. In a study of cancer mortality in the same prospective cohort, Blair et al. (2005a) reported four and three deaths from âsoft tissueâ cancer in the pesticide applicators (SMR 0.7, 95% CI 0.2â1.8) and their spouses (SMR 1.4, 95% CI 0.3â4.1), respectively. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics re-
348 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-18 Selected Epidemiologic StudiesâSoft-Tissue Sarcoma Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 8 1.2 (0.5â2.4) Ever 4 0.8 (0.2â2.0) Alavanja et al., 2005 US Agriculture Health Studyâincidence Private applicators (men and women) 10 0.7 (0.3â1.2) Spouses of private applicators ( 99% women) 3 0.5 (0.1â1.4) Commercial applicators (men and women) â 0.0 (0â3.8) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 4 0.7 (0.2â1.8) Spouses of private applicators ( 99% women) 3 1.4 (0.3â4.1) ât Mannetje et al., Phenoxy herbicide producers (men and 2005 women) 0 0.0 (0.0â19.3) Phenoxy herbicide sprayers ( 99% men) 1 4.3 (0.1â23.8) Torchio et al., 1994 Italian licensed pesticide users 2 1.0 (0.1â3.5) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 4 3.2 (1.2â9.0) Studies Reviewed in Update 2004 Bodner et al., 2003 Dow chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 2 2.4 (0.3â8.6) Studies Reviewed in Update 2000 Steenland et al., 1999 US chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0 * Hooiveld et al., 1998 Dutch chemical production workers (included in the IARC cohort) 0 * Rix et al., 1998 Danish paper mill workersâincidence Women employed in sorting and packing 8 4.0 (1.7â7.8) Men employed in sorting and packing 12 1.2 (0.6â2.0) Studies Reviewed in Update 1998 Hertzman et al., 1997 Canadian sawmill workers 11 1.0 (0.6â1.7) Kogevinas et al., 1997 IARC cohort (men and women) Workers exposed to any phenoxy herbicide or chlorophenol 9 2.0 (0.9â3.8) Exposed to TCDD (or higher- chlorinated dioxins) 6 2.0 (0.8â4.4) Not exposed to TCDD (or higher- chlorinated dioxins) 2 1.4 (0.2â4.9)
CANCER 349 TABLE 6-18 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Ott and Zober, 1996 BASF employeesâincidence 0 0.2 expected Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0 0.2 expected Studies Reviewed in Update 1996 Kogevinas et al., 1995 IARC cohortâincidence (men and women) 11 * Mack, 1995 US cancer registry data (SEER program) review Men 3,526 * Women 2,886 * Blair et al., 1993 US farmers in 23 states 98 0.9 (0.8â1.1) Lynge, 1993 Danish production workersâupdated incidence for men and women (included in the IARC cohort) 5 2.0 (0.7â4.8) Kogevinas et al., 1992 IARC cohort (men and women) 10â19 years since ï¬rst exposure 4 6.1 (1.7â15.5) Studies Reviewed in VAO Bueno de Mesquita Dutch phenoxy herbicide workers (included et al., 1993 in the IARC cohort) 0 0.0 (0.0â23.1) Hansen et al., 1992 Danish gardenersâincidence (men and women) Male gardeners 3 5.3 (1.1â15.4) Smith and Australia residents 30 1.0 (0.3â3.1) Christophers, 1992 Fingerhut et al., 1991 NIOSH cohortâentire cohort 4 3.4 (0.9â8.7) 1-year exposure, 20-year latency 3 9.2 (1.9â27.0) Manz et al., 1991 German production workersâmen and women (included in the IARC cohort) 0 * Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 4 2.0 (0.6â5.2) Zober et al., 1990 BASF employeesâbasic cohort 0 * Alavanja et al., 1989 USDA forest and soil conservationists 2 1.0 (0.1â3.6) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0 * Wiklund et al., 1988, Swedish agricultural workers (men and 1989b women) 7 0.9 (0.4â1.9) Woods et al., 1987 Washington State residentsâincidence High phenoxy exposure * 0.9 (0.4â1.9) Self-reported chloracne * 3.3 (0.8â14.0) Coggon et al., 1986 British MCPA chemical workers (included in the IARC cohort) 1 1.1 (0.03â5.9) Hoar et al., 1986 Kansas residentsâincidence All farmers 95 1.0 (0.7â1.6) Farm use of herbicides 22 0.9 (0.5â1.6) continued
350 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-18 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Smith and Pearce, Reanalysis of New Zealand workers 133 1.1 (0.7â1.8)d 1986 Vineis et al., 1986 Italian rice growers Among all living women 5 2.4 (0.4â16.1) Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) Men 5 2.7 (0.9â6.3) Women 0 * Balarajan and Agricultural workers in England Acheson, 1984 Overall 42 1.7 (1.0â2.9) Those under 75 years old 33 1.4 (0.8â2.6) Smith et al., 1984 Update of New Zealand workers 17 1.6 (0.7â3.8)d Blair et al., 1983 Florida pesticide applicators 0 * Smith et al., 1983 New Zealand workers exposed to herbicides 17 1.6 (0.8â3.2)d Hardell, 1981 Swedish residents Exposed to phenoxy acids 13 5.5 (2.2â13.8) Exposed to chlorophenols 6 5.4 (1.3â22.5) Eriksson et al., 1979, Swedish workers 25 (2.5â10.4) 1981 5:1 matched ENVIRONMENTAL New Studies Pahwa et al., 2006 Any phenoxy herbicide 46 1.10 (0.7â1.5) 2,4-D 41 0.96 (0.6â1.5) Mecoprop 12 0.98 (0.5â1.9) MCPA 12 1.08 (0.5â2.2) Studies Reviewed in Update 2004 Tuomisto et al., 2004 Finnish STS patients and controls 110 Quintile 2 (median tissue concentration 20 ng/kg WHO-TEQ) * 0.4 (0.2â1.1) Quintile 5 (median tissue concentration ~60 ng/kg WHO-TEQ) * 0.7 (0.2â2.0) Comba et al., 2003 Residents near an industrial-waste incinerator in Mantua, Italyâincidence Residence within 2 km of incinerator 5 31.4 (5.6â176.1) Studies Reviewed in Update 2002 Costani et al., 2000 Residents near a chemical plant in Mantua, Italyâincidence 20 2.3 (1.3â3.5) Studies Reviewed in Update 2000 Bertazzi et al., 2001 Sevesoâ20-year follow-up (men and women) 0 * Viel et al., 2000 Residents near a French solid-waste incineratorâincidence Spatial cluster 45 1.4 (p 0.004) 1994â1995 12 3.4 (p 0.008) Bertazzi et al., 1998 Sevesoâ15-year follow-up (men and women) Zone Râmen 4 2.1 (0.7â6.5)
CANCER 351 TABLE 6-18 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up (men and women) Zone Râmen 4 2.1 (0.6â5.4) Gambini et al., 1997 Italian rice growers 1 4.0 (0.1â22.3) Svensson et al., 1995 Swedish ï¬shermenâincidence (men and women) West coast 3 0.5 (0.1â1.4) Studies Reviewed in Update 1996 Bertazzi et al., 1993 Seveso residentsâ10-year follow-upâmorbidity Zone Râmen 6 2.8 (1.0â7.3) women 2 1.6 (0.3â7.4) Studies Reviewed in VAO Lampi et al., 1992 Finnish community exposed to chlorophenol contamination (men and women) 6 1.6 (0.7â3.5) Bertazzi et al., 1989a Seveso residentsâ10-year follow-up Zone A, B, Râmen 2 5.4 (0.8â38.6) women 1 2.0 (0.2â1.9) Bertazzi et al., 1989b Seveso residentsâ10-year follow-up Zone Râmen 2 6.3 (0.9â45.0) Zone Bâwomen 1 17.0 (1.8â163.6) VIETNAM VETERANS New Studies ADVA, 2005a Australian Vietnam veterans vs Australian populationâincidence 35 1.0 (0.7â1.3) Navy 6 0.8 (0.3â1.7) Army 29 1.2 (0.8â1.6) Air Force 0 0.0 (0.0â1.1) ADVA, 2005b Australian Vietnam veterans vs Australian populationâmortality 12 0.8 (0.4â1.3) Navy 3 0.9 (0.2â2.4) Army 9 0.8 (0.4â1.5) Air Force 0 0.0 (0.0â2.3) ADVA, 2005c Australian men conscripted Army National Service Vietnam-era veteransâdeployed vs non-deployed Incidence 10 1.0 (0.4â2.4) Mortality 3 0.5 (0.1â2.0) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 1 0.8 (0.1â12.8) AIHW, 1999 Male Australian Vietnam veterans 14 27 expected (17â37) CDVA, 1998a Male Australian Vietnam veterans 398e 27 expected (17â37) continued
352 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-18 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c CDVA, 1998b Female Australian Vietnam veterans 2e 0 expected (0â4) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 9 1.0 (0.4â1.8) CDVA, 1997b Australian National Service Vietnam veterans 2 0.7 (0.6â4.5) Clapp, 1997 Massachusetts Vietnam Veterans 18 1.6 (0.5â5.4) AFHS, 1996 Ranch Hand veterans 0 * Watanabe and Kang, US Marines in Vietnam 0 * 1995 Studies Reviewed in Update 1996 Visintainer et al., Michigan Vietnam veterans 8 1.1 (0.5â2.2) 1995 Studies Reviewed in VAO Watanabe et al., 1991 Army Vietnam veterans 43 1.1 Marine Vietnam veterans 11 0.7 Bullman et al., 1990 Army I Corps Vietnam veterans 10 0.9 (0.4â1.6) Michalek et al., 1990 Ranch Hand veterans 1 * Comparisons 1 * Breslin et al., 1988 Army Vietnam veterans 30 1.0 (0.8â1.2) Marine Vietnam veterans 8 0.7 (0.4â1.3) Kogan and Clapp, Vietnam veterans in Massachusetts 9 5.2 (2.4â11.1) 1988 Fett et al., 1987 Australian Vietnam veterans 1 1.3 (0.1â20.0) Anderson et al., 1986b Wisconsin Vietnam veterans 4 * Breslin et al., 1986 US Vietnam veterans Army 30 1.0* Marines 8 0.7* Kang et al., 1986 Vietnam veterans vs. Vietnam-era veterans 86 0.8 (0.6â1.1) Lawrence et al., 1985 New York State Vietnam veterans 2 1.1 (0.2â6.7) Greenwald et al., New York State Vietnam veterans 10 0.5 (0.2â1.3) 1984 ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Veteran Affairs; AFHS, Air Force Health Study; AIHW, Australian Institute of Health and Welfare; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, methyl-4-chlorophenoxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; SEER, Surveillance, Epidemiology, and End Results Program; STS, soft-tissue sarcoma; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin; WHO-TEQ, toxicity equivalency as deï¬ned by the World Health Organization. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d 90% CI. e Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have soft-tissue sarcoma?â * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts.
CANCER 353 ports as having high herbicide use, especially of 2,4-D and MCPA. The estimated risk of cancer of the connective soft tissue was not increased (two cases; SMR 0.95, 95% CI 0.11â3.45). Reif et al. (1989) performed a series of caseâcontrol analyses on the sample of 19,904 people with speciï¬ed occupations among the 24,762 men 20 years old or older entered into the the New Zealand Cancer Registry in 1980â1984. The focus of their study was on the 134 for whom forestry work was the most recent occupation listed. For each type of cancer, the people with any other type of can- cer were used as controls. Of 142 people with STS, four had most recently been forestry workers (OR 3.24, 95% CI 1.17â8.98). Environmental Studies In the caseâcontrol study of men living in six Canadian provinces, Pahwa et al. (2006) investigated whether exposure to phenoxy herbicides and other pesticides was associated with the incidence of STS. (The results of the study in terms of farm work or residence were reported in Pahwa et al. [2003], which has not been previously reviewed in this series, but the current citation more speciï¬- cally addresses the VAO charge.) Interviews were completed with 357 men who received new diagnoses of STS in 1991â1994 and with 1,506 control subjects. No associations were found with any exposures to phenoxy herbicides (OR 1.07, 95% CI 0.80â1.44), to 2,4-D (OR 0.97, 95% CI 0.71â1.32), to mecoprop (2-[2-methyl-4-chlorophenoxy]propanoic acid) (OR 1.40, 95% CI 0.86â2.25), or to MCPA (OR 1.05, 95% CI 0.54â2.02). Vietnam-Veteran Studies In a set of three reports updating the health status of Australian Vietnam veterans, no associations between Vietnam service and cancers of connective soft tissue were found in comparing veterans with the general population of Austra- lia in incidence (SIR 0.99, 95% CI 0.66â1.31) (ADVA, 2005a) and mortality (SMR 0.75, 95% CI 0.38â1.28) (ADVA, 2005b). When conscripted male Army veterans deployed to Vietnam (National Service veterans) were compared with their non-deployed counterparts (National Service non-veterans), no increases were found in the incidence of STS (SIR 0.99, 95% CI 0.39â2.44) or mortality from it (SMR 0.48, 95% CI 0.08â2.01) (ADVA, 2005c). Biologic Plausibility In a 2 year study, dermal application of TCDD to Swiss-Webster mice led to an increase in ï¬brosarcomas in the female mice, but not male mice (NTP, 1982b). There is some concern that the increase in ï¬brosarcomas may be associated with the treatment protocol, rather than due to the treatment with TCDD. The NTP gavage study (1982a) also found elevated incidences of ï¬brosarcomas in male
354 VETERANS AND AGENT ORANGE: UPDATE 2006 and female rats and in female mice (as VAO also reported; but Update 2004 said there were no animal data speciï¬cally supporting STS). The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Previous committees have concluded that the occupational, environmen- tal, and Vietnam-veteran studies showed sufï¬cient evidence to link herbicide exposure to STS. Three new studies did not ï¬nd associations with STS, but the statistical power to detect excess risks in these small cohorts of phenoxy herbi- cide producers and sprayers was low; furthermore, the populations in the United States, Canada, and Italy were exposed to contemporary phenoxy herbicides unlikely to contain TCDD. The ï¬ndings of a sizable multinational investigation of paper and pulp workers were indeterminant for the rather nonspeciï¬c exposure ânonvolatile organochlorines,â but an occupational analysis of those entered into the New Zealand Cancer Registry in the early 1980s did ï¬nd a strong association between STS and having been a forestry worker. The studies of Australian vet- erans did not show any evidence of increased risks among deployed soldiers, but the power to detect excess risk was low and there were no data regarding actual exposures. The committee did not ï¬nd that these new data justiï¬ed modifying the previous conclusion. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is sufï¬cient evidence of an asso- ciation between exposure to at least one of the compounds of interest and STS. SKIN CANCERâMELANOMA Skin cancers are generally divided into two broad categories: neoplasms that develop from melanocytes (malignant melanoma, or simply melanoma) and neoplasms that do not. Non-melanoma skin cancers (primarily basal-cell and squamous-cell carcinomas) have a far higher incidence than melanoma but are considerably less aggressive and therefore more treatable. The average annual incidence of melanoma is shown in Table 6-19. The committee responsible for Update 1998 ï¬rst chose to address melanoma studies separately from those of non-melanoma skin cancer. Some researchers report results by combining all types of skin cancer without specifying type. The present committee believes that such information is not interpretable (although there is a supposition that mortality ï¬gures refer predominantly to melanoma and sizable incidence ï¬gures refer to non-melanoma skin cancer). Therefore, the committee is interpreting data
CANCER 355 TABLE 6-19 Average Annual Cancer Incidence (per 100,000) of Skin Cancers (Excluding Basal- and Squamous-Cell Cancers) in United States a 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age Melanomas All All All of the Skin Races White Black Races White Black Races White Black Men 32.4 38.6 0.5 45.4 52.7 1.1 55.4 64.8 3.5 Women 24.6 30.0 0.2 26.9 32.2 1.8 28.6 34.6 1.2 SEER incidence data are not available for non-melanoma skin cancer. a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. only on results that are speciï¬ed as applying to melanoma or to non-melanoma skin cancer. ACS estimated that about 34,260 men and 27,930 women would receive diagnoses of cutaneous melanoma (ICD-9 172) in the United States in 2006 and 5,020 men and 2,890 women would die from it (Jemal et al., 2006). More than a million cases of non-melanoma skin cancer (ICD-9 173), primarily basal-cell and squamous-cell carcinomas, are diagnosed in the United States each year (ACS, 2006); it is not required to report them to registries, so the numbers of cases are not as precise as those of other cancers. ACS reports that although melanoma accounts for only about 4 percent of skin-cancer cases, it is responsible for about 79 percent of skin-cancer deaths (2006). It estimates that 1,000â2,000 people die each year from non-melanoma skin cancer. Melanoma occurs more frequently in fair-skinned people than in dark-skinned people; the risk in whites is roughly 20 times that in dark-skinned blacks. The incidence increases with age, although more strikingly in men than in women. Other risk factors include the presence of certain moles on the skin, suppression of the immune system, and excessive exposure to ultraviolet (UV) radiation, typically from the sun. A family history of the disease has been identiï¬ed as a risk factor, but it is unclear whether that is attributable to genetic factors or to similarities in skin type and sun exposure patterns. Excessive exposure to UV radiation is the most important risk factor for non-melanoma skin cancer, although some skin diseases and chemical exposures have also been identiï¬ed as potential risk factors. Exposure to inorganic arsenic is a risk factor for skin cancer (this does not imply that cacodylic acid, which is a metabolite of inorganic arsenic, can also be assumed to be a risk factor). Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between
356 VETERANS AND AGENT ORANGE: UPDATE 2006 exposure to the compounds of interest and skin cancer. Additional information available to the committee responsible for Update 1996 did not change that con- clusion. The Update 1998 committee considered the literature on melanoma sepa- rately from that of non-melanoma skin cancer. It found that there was inadequate or insufï¬cient information to determine whether there is an association between the compounds of interest and melanoma. The Update 2000, Update 2002, and Update 2004 committees concurred with the ï¬ndings of the Update 1998 com- mittee. Table 6-20 summarizes the relevant melanoma studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. A JEM was applied to 58,162 individual work histories to estimate exposure to nonvolatile organochlorine compounds (which would include TCDD). Death from melanoma was not more strongly associated with having ever been exposed to nonvolatile organochlorine compounds (n 21; SMR 1.17, 95% CI 0.72â1.78) than with having never been exposed (n 20; SMR 0.82, 95% CI 0.5â1.27). The study by ât Mannetje et al. (2005) is an extension of a cohort study in New Zealand, which is part of an IARC international study of phenoxy herbicide producers and sprayers. Their report describes follow-up from 1969 to 2000 of 813 herbicide producers and 699 sprayers who were classiï¬ed as exposed to dioxin and phenoxy herbicides. SMRs were computed relative to general New Zealand standards. No cases of melanoma were observed in the production workers, and only one in the sprayers; the estimated SMRs were therefore very unstable and had wide conï¬dence intervals. In reporting on cancer incidence in the AHS cohort, Alavanja et al. (2005) found that the spouse group showed a signiï¬cant excess of melanoma, with 67 observed cases (SIR 1.64, 95% CI 1.27â2.09). Such an excess was not seen in the private applicators (SIR 0.95, 95% CI 0.78â1.16) or the commercial ap- plicators (SIR 1.05, 95% CI 0.42â2.17). Melanoma was the only cancer type observed to have a signiï¬cantly increased risk in the spouses. The authors consid- ered that result to be âunexpectedâ and commented that a high percentage of farm spouses engage in outdoor work that involves substantial exposure to sunlight. Blair et al. (2005a) studied mortality in the AHS cohorts of private applica- tors (mostly farmers) and their spouses. In the private applicators, there were 13 deaths from melanoma (SMR 0.7, 95% CI 0.4â1.3). In the spouses, there were two deaths from melanoma (SMR 0.4, 95% CI 0.1â1.6). The increase in mela- noma incidence observed among the AHS spouses is not yet reï¬ected in mortality from melanoma, but the cohort has very low overall mortality compared with the
CANCER 357 TABLE 6-20 Selected Epidemiologic StudiesâMelanoma Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b OCCUPATIONAL New Studies McLean et al., IARC cohort of pulp and paper workers 2006 Exposure to nonvolatile organochlorine compounds Never 20 0.8 (0.5â1.3) Ever 21 1.2 (0.7â1.8) Alavanja et al., US Agriculture Health Studyâincidence 2005 Private applicators (men and women) 100 1.0 (0.8â1.2) Spouses of private applicators ( 99% women) 67 1.6 (1.3â2.1) Commercial applicators (men and women) 7 1.1 (0.4â2.2) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 13 0.7 (0.4â1.3) Spouses of private applicators ( 99% women) 2 0.4 (0.1â1.6) ât Mannetje et al., Phenoxy herbicide producers (men and women) 0 0.0 (0.0â3.0) 2005 Phenoxy herbicide sprayers ( 99% men) 1 0.6 (0.0â3.4) Torchio et al., Italian licensed pesticide users 9 1.2 (0.6â2.3) 1994 Magnani et al., UK caseâcontrol 1987 Herbicides * 1.2 (0.4â4.0) Chlorophenols * 0.9 (0.4â2.3) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators Melanoma, squamous-cell carcinoma, and unknown skin cancer (mortality presumably attributable to melanoma) 5 3.6 (1.2â8.3) Studies Reviewed in Update 2002 Thörn et al., 2000 Swedish lumberjack workers exposed to phenoxyacetic herbicidesâincidence Women 1 3.5 (0.1â19.2) Men 0 â Studies Reviewed in Update 2000 Hooiveld et al., Dutch chemical production workers (included in 1998 the IARC cohort) 1 2.9 (0.1â15.9) Studies Reviewed in Update 1998 Hertzman et al., British Columbia sawmill workers 1997 Incidence 38 1.0 (0.7â1.3) Mortality 17 1.4 (0.9â2.0) Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 9 0.6 (0.3â1.2) Exposed to TCDD (or higher-chlorinated dioxins) 5 0.5 (0.2â3.2) Not exposed to TCDD (or higher- chlorinated dioxins) 4 1.0 (0.3â2.4) continued
358 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-20 Continued Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 244 1.0 (0.8â1.1) White women 5 1.1 (0.4â2.7) Lynge, 1993 Danish production workersâupdated incidence (included in the IARC cohort) 4 4.3 (1.2â10.9) Studies Reviewed in VAO Ronco et al., 1992 Danish workersâincidence Men 72 0.7 (p 0.05) Women 5 1.2* Wigle et al., 1990 Canadian farmers 24 1.1 (0.7â1.6) Wiklund, 1983 Swedish male and female agricultural workersâincidence 268 0.8 (0.7â1.0)c ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., Seveso residentsâ20-year follow-up 2001 Zones A, Bâmen 1 1.5 (0.2â12.5) women 2 1.8 (0.4â7.3) Schreinemachers, Rural or farm residents of Minnesota, Montana, 2000 and North and South Dakota Menâcounties with high wheat acreage 41 0.8 (0.6â1.1) medium wheat acreage 50 0.8 (0.6â1.1) Womenâcounties with high wheat acreage 29 0.7 (0.5â1.2) medium wheat acreage 59 1.2 (0.9â1.8) Studies Reviewed in Update 1998 Bertazzi et al., Seveso residentsâ15-year follow-up 1997 Zone Aâwomen 1 9.4 (0.1â52.3) Zone Râmen 3 1.1 (0.2â3.2) women 3 0.6 (0.1â1.8) Svensson et al., Swedish ï¬shermen (men and women) 1995 East coast Incidence 0 0.0 (0.0â0.7) Mortality 0 0.0 (0.0â1.7) West coast Incidence 20 0.8 (0.5â1.2) Mortality 6 0.7 (0.3â1.5) Studies Reviewed in VAO Bertazzi et al., Seveso residentsâ10-year follow-up 1989a Zones A, B, Râmen 3 3.3 (0.8â13.9) women 1 0.3 (0.1â2.5)
CANCER 359 TABLE 6-20 Continued Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 756 1.3 (1.2â1.4) Navy 173 1.4 (1.2â1.6) Army 510 1.2 (1.2â1.4) Air Force 73 1.4 (1.1â1.7) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 111 1.1 (0.9â1.3) Navy 35 1.6 (1.0â2.1) Army 66 1.0 (0.7â1.2) Air Force 10 1.0 (0.5â1.8) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veteransâdeployed vs non-deployed Incidence 204 1.1 (0.9â1.4) Mortality 14 0.6 (0.3â1.1) Pavuk et al., 2005 White Air Force comparison subjects onlyâincidence Serum TCDD levels (pg/g), based on model with exposure variable loge(TCDD)d Per unit increase of âloge(TCDD) in pg/g 25 2.7 (1.1â6.3) Quartiles (pg/g) 0.4â2.6 3 1.0 2.6â3.8 5 2.1 (0.4â11) 3.8â5.2 8 3.2 (0.7â15.5) 5.2 9 3.6 (0.7â17.2) Number of years served in Southeast Asia (SEA) Per year of service 25 1.1 (0.9â1.3) Quartiles (years in SEA) 0.8â1.3 3 1.0 1.3â2.1 4 1.9 (0.3â10.3) 2.1â3.7 8 3.2 (0.7â15.3) 3.7â16.4 10 4.1 (0.9â19.7) Boehmer et al., Follow-up of CDC Vietnam Experience Cohort 6 1.4 (0.4â4.9) 2004 continued
360 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-20 Continued Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b Studies Reviewed in Update 2004 Akhtar et al., 2004 AFHS subjects vs national rates White AFHS Ranch Hand veterans Mortalityâall * Incidenceâall 17 2.3 (1.4â3.7) With tours between 1966â1970 16 2.6 (1.5â4.1) White AFHS comparison veterans Mortalityâall * Incidenceâall 15 1.5 (0.9â2.4) With tours between 1966â1970 12 1.5 (0.8â2.6) White AFHS subjectsâincidence Who spent at most 2 years in SEA Per unit increase of âloge(TCDD) in pg/g 14 2.2 (1.3â3.9) Comparison group 3 1.0 Ranch Hand 10 TCDD pg/g in 1987 4 3.0 (0.5â16.8) 118.5 TCDD pg/g at end of service 4 7.4 (1.3â41.0) 118.5 TCDD pg/g at end of service 3 7.5 (1.1â50.2) Only Ranch Hands with 100% service in Vietnam and comparisons with 0% service in Vietnam Per unit increase of âloge(TCDD) in pg/g 14 1.7 (1.0â2.8) Comparison group 2 1.0 Ranch Hand 10 TCDD pg/g in 1987 5 3.9 (0.4â35.3) 118.5 TCDD pg/g at end of service 4 7.2 (0.9â58.8) 118.5 TCDD pg/g at end of service 3 5.5 (0.6â46.1) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veteransâincidence 16 1.8 (0.8â3.8) Ketchum et al., Ranch Hand (RH) veterans and comparisons 1999 through June 1997âincidence Comparisons 9 1.0 RH background-exposure 4 1.1 (0.3â4.5) RH low-exposure 6 2.6 (0.7â9.1) RH high-exposure 2 0.9 (0.2â5.6) AIHW, 1999 Australian Vietnam veterans (validation study) 380 expected âincidence 483 (342â418) CDVA, 1998a Australian Vietnam veterans (men)âincidence 2,689e 380 expected (342â418) CDVA, 1998b Australian Vietnam veterans 7e 3 expected (women)âincidence (1â8) Studies Reviewed in Update 1998 CDVA, 1997a Australian Vietnam veterans (men) 51 1.3 (0.9â1.7) CDVA, 1997b Australian National Service Vietnam veterans 16 0.5 (0.2â1.3) Clapp, 1997 Massachusetts Vietnam veteransâincidence 21 1.4 (0.7â2.9)
CANCER 361 TABLE 6-20 Continued Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b Studies Reviewed in VAO Wolfe et al., 1990 Air Force Ranch Hand veteransâincidence 4 1.3 (0.3â5.2) Breslin et al., 1988 Army Vietnam veterans 145 1.0 (0.9â1.1) Marine Vietnam veterans 36 0.9 (0.6â1.5) ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin. a Cohorts are male and the endpoint is mortality unless otherwise noted. b Given when available. c 99% CI. d The original paper implied that the exposure metric for TCDD was based on actual measured serum levels of TCDD. Subsequent correspondence between the Committee and the investigators indicated that the metric was actually transformed using the natural logarithm of TCDD. e Self-reported medical history. Answer to question: Since your ï¬rst day of service in Vietnam, have you been told by a doctor that you have melanoma? â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts. general population. The numbers of melanoma deaths observed in this study are small, and the conï¬dence intervals are relatively wide. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics re- ports as having high herbicide use, especially of 2,4-D and MCPA. The estimated risk of melanoma was not signiï¬cantly increased (nine cases; SMR 1.21, 95% CI 0.56â2.29). Magnani et al. (1987) conducted a caseâcontrol mortality study of 99 people with melanoma and 361 controls in the United Kingdom. A JEM was used to predict exposures to various chemical agents on the basis of job title as indicated on the death certiï¬cates. Estimated risks of melanoma associated with exposure to herbicides (RR 1.2, 95% CI 0.4â4.0) and chlorophenols (RR 0.9, 95% CI 0.4â2.3) were not signiï¬cantly increased. For completeness, we note here a letter to the editor by Kennedy et al. (2005). It is not evident that it was peer-reviewed, which is a standard require- ment for inclusion in the present committeeâs evidentiary database of nongovern- ment reports, but no other publications on the Leiden Skin Cancer Study could be found mentioning herbicides. The letter describes results from a caseâcontrol study of squamous-cell carcinoma, basal-cell carcinoma, and melanoma without providing any details about the selection of cases and controls. Data on only male subjects were reported because relevant exposures of women were rare. Of the
362 VETERANS AND AGENT ORANGE: UPDATE 2006 47 men with melanoma, only one reported ever being exposed to herbicides. The data are insufï¬cient to support a stable RR estimate, but the authors did document a signiï¬cant risk of melanoma in men exposed to arsenic (RR 7.1), although apparently neither organic nor in the form of a herbicide, as would be of inter- est for the VAO reports. Even if it were eligible for inclusion, the paper would provide little information on the potential for an association between exposure to herbicides and melanoma. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and melanoma were published since Update 2004. Vietnam-Veteran Studies Pavuk et al. (2005) reported on cancer incidence from 1982 to 2003 in the comparison group in the Air Force Health Study (AFHS). Those Air Force veterans had served in Southeast Asia but had not been involved in spraying her- bicides during the Vietnam War, as had the Ranch Hand veterans who were the AFHS primary subjects. Of the roughly 1,800 comparison subjects enrolled in the course of the AFHS, 1,482 had serum TCDD readings used as the basis of the analyses presented here. The median TCDD concentration in the Southeast Asia comparison group (sampled in 1987) was 3.8 pg/g of lipid, and the values in the highest quartile ranged from 5.2 to 54.8 pg/g. The serum TCDD concentrations in the comparison subjects overlapped considerably with those in the Ranch Hand veterans, 43.2 percent of whom had TCDD readings in 1987 of less than 10 pg/g (see Akhtar et al., 2004). The 25 cases of melanoma were distributed as three, ï¬ve, eight, and nine cases over the quartiles with increasing TCDD. Using the lowest quartile as the referent group for the other three quartiles of Southeast Asia comparison subjects, the second, third, and fourth quartiles of serum TCDD showed increasing RRs of 2.1 (95% CI 0.4â11), 3.2 (95% CI 0.7â15.5), and 3.6 (95% CI 0.7â17.2), re- spectively. The committeeâs correspondence with the authors conï¬rmed that the reported signiï¬cant doseâresponse relationship was based on a model that used natural-logarithm transformation of the continuous variable, individual serum TCDD concentration (slope per ln [TCDD], 2.7, 95% CI 1.1â6.3; p 0.02). The results were adjusted for a number of other risk factors, including military occupation, year of birth, number of years served in Southeast Asia, body-mass index (BMI), skin reaction to sunlight exposure, and eye color. An analogous analysis on the numbers of years that each person had served in Southeast Asia did not yield a signiï¬cant association with the risk of melanoma (slope per year in Southeast Asia, 1.1, 95% CI 0.9â1.3; p 0.46). Thus, an increase in the oc-
CANCER 363 currence of melanoma was found to be more speciï¬cally associated with TCDD exposure than with service in Southeast Asia. In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported six melanoma deaths in the deployed and four in the non-deployed (CRR 1.39, 95% CI 0.39â4.93). A statistically signiï¬cant increase in melanoma incidence in male Australian Vietnam veterans was found in comparison with the general Australian popula- tion (ADVA, 2005a) on the basis of 756 observed cases (SIR 1.32, 95% CI 1.23â1.41). When the analysis was stratiï¬ed over the Army, Navy, and Air Force, similar signiï¬cant associations with the incidence of melanoma were observed in all three branches of service. A potential confounder in the study is exposure to sunlight. The mortality experience of the above group of male Australian Vietnam vet- erans through 2001 was analyzed, again by using the rate observed in Australian men in general as the standard (ADVA, 2005b). The 111 deaths from melanoma in all the veterans showed a statistically non-signiï¬cant increase (SMR 1.10, 95% CI 0.90â1.31). On the basis of 35 deaths from melanoma, mortality was signiï¬cantly increased in the veterans who had served in the Navy (SMR 1.56, 95% CI 1.04â2.08), but the ï¬ndings were neutral for those who had served in the Army or Air Force. A different Australian study (ADVA, 2005c) compared deployed male Army National Service veterans with non-deployed Vietnam-era veterans. That com- parison has the advantage of contrasting health outcomes in groups of men who were of similar age, health, and ï¬tness at the time of enlistment but who differed primarily in Vietnam experience. On the basis of 204 incident cases of and 14 deaths from melanoma in the deployed veterans, neither incidence (SIR 1.13, 95% CI 0.93â1.37) nor mortality (SMR 0.56, 95% CI 0.28â1.08) was increased in comparison with the non-deployed veterans. Biologic Plausibility No animal studies have reported an increased incidence of melanoma after exposure to the compounds of interest. The biologic plausibility of the carcino- genicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis On the whole, the new occupational studies of melanoma were small and could not provide stable estimates of RR associated with herbicide exposure. The Alavanja study had a suggestive result in one subgroup (the female spouses of the private applicators), which the authors had not expected. Increased risks
364 VETERANS AND AGENT ORANGE: UPDATE 2006 in contemporary users of phenoxy herbicides would not be expected, however, if TCDD were the agent responsible for any increase in melanoma. Occupational studies reviewed previously by the VAO committees have shown a wide range of estimated RRs of melanoma, with only a few results sug- gesting an increase in the risk of melanoma in workers potentially exposed to the components of the herbicides sprayed in Vietnam. With respect to melanoma mortality, only the ï¬nding of Swaen et al. (2004) based on ï¬ve skin-cancer deaths in Dutch herbicide applicators was statistically signiï¬cant (SMR 3.5, 95% CI 1.2â8.3), and even this result did not explicitly exclude non-melanoma skin can- cer. The pooled international IARC cohort (Kogevinas et al., 1997) provides the most comprehensive analysis of cancer mortality in phenoxy herbicide producers and sprayers, with or without concurrent TCDD exposure, but there were only nine melanoma deaths in all the people exposed to phenoxy herbicides and no suggestion of an increased risk with or without TCDD exposure. On the basis of four exposed cases, Lynge (1993) reported a signiï¬cant increase in the incidence of melanoma (SIR 4.3, 95% CI 1.2â10.9) in the cohort of Danish phenoxy her- bicide producers (whose mortality experience was included in the non-signiï¬cant ï¬ndings on the IARC cohort overall). The limited ï¬ndings concerning mortality 20 years after environmental ex- posure arising from the Seveso accident (Bertazzi et al., 2001) show modest increases in the estimated risks in both men (SMR 1.5, 95% CI 0.2â12.5) and women (SMR 1.8, 95% CI 0.4â7.3) who resided closest to the release (in Zones A and B), but these estimates, being based on only one and two deaths from melanoma, respectively, are extremely unstable. The newly published studies of Australian servicemen who served in Viet- nam show some indication of increases in the occurrence of melanoma, but the overall interpretation is not straightforward. The incidence of melanoma is sig- niï¬cantly increased in all male Australian Vietnam veterans in comparison with the general population (ADVA, 2005a). In the parallel study of mortality in the servicemen relative to the Australian population (ADVA, 2005b), the increase in melanoma risk is signiï¬cant only in those serving in the Navy (SIR 1.6, 95% CI 1.0â2.1), who might also have had more sunlight exposure. The third Australian study (ADVA, 2005c), comparing deployed and non-deployed National Service veterans (male Army conscripts) with respect to both melanoma incidence and mortality, does not support an effect of deployment (as used as a surrogate for herbicide exposure). The mortality update on the CDC VES (Boehmer et al., 2004) does contain a somewhat, but not signiï¬cantly, higher incidence of mela- noma in deployed than in non-deployed Vietnam-era veterans (SMR 1.39, 95% CI 0.39â4.93). The most persuasive evidence comes from the AFHS. The positive ï¬ndings of an association between TCDD exposure and melanoma presented in Akhtar et al. (2004) are extended down into serum concentrations in the Southeast Asia comparison group in the analyses of Pavuk et al. (2005). Increases in melanoma
CANCER 365 risk in people in the second, third, and fourth quartiles of serum TCDD concen- trations were seen in comparison with the lowest quartile. The overall slope of a doseâresponse curve in an analytic model based on the logarithm of the continu- ous variableâeach personâs serum TCDD concentrationâwas also statistically signiï¬cant. In Akhtar et al. (2004), the ï¬ndings on melanoma incidence in the Ranch Hand veterans were similarly signiï¬cantly increased; they were stronger and more TCDD-speciï¬c than for any other type of cancer. Melanoma diagnoses are known to increase with screening, as was conducted in the AFHS, but this factor is less likely to bias the estimated risks when the comparison is internal, as in the AFHS reports. It is compelling that a signiï¬cant doseâresponse relationship is found when analysis is based on individual readings for the continuous variable (serum TCDD) that is generally regarded as the most precise indicator of herbicide exposure in Vietnam. The analyses in Akhtar et al. (2004) and Pavuk et al. (2005) involve interpretations that were not part of the original study design, but, given some of the insights that have been gained in the course of the AFHS, such approaches may be justiï¬ed. The results in those two publications would be more useful if they were presented in a more transparent fashion. In summary, although the collateral evidence from studies of other occupa- tional and environmental populations is inconsistent, signiï¬cant associations have been demonstrated in studies of populations with well-characterized exposures to the compounds of interest (Lynge, 1993; Swaen et al., 2004); they provide evidence of an association with melanoma that may be limited by the possibility of bias or chance. The ï¬ndings of the ADVA (2005a,b,c) in Australian Vietnam veterans are limited by internal inconsistency. The increase in mortality reported by the CDC VES (Boehmer et al., 2004) is consistent but far from signiï¬cant. The results of the AFHS have long been anticipated as the most directly pertinent to the experience of US Vietnam veterans, so the committee was im- pressed by recent reports (Akhtar et al., 2004; Pavuk et al., 2005) of a strong doseâresponse relationship between serum TCDD concentrations and melanoma in this population. Some members of the committee were concerned, however, that the ï¬ndings of the AFHS have not been presented in a complete and sys- tematic fashion. For example, the follow-up for the analysis of the Ranch Hand subjects (Akhtar et al., 2004) represents ï¬ndings only up to 1999 (not including results of the ï¬nal examination cycle), whereas the report on the Southeast Asia comparison group (Pavuk et al., 2005) includes diagnoses through 2003. The cross-sectional report (AFHS, 2005) does not provide a deï¬nitive statement of cumulative melanoma diagnoses observed in the Ranch Hand subjects through 2003 to match the data analyzed for the Southeast Asia comparison group in Pavuk et al. (2005), but the stated prevalences in the ï¬nal examination cycle sug- gest that new melanoma diagnoses in the comparison subjects greatly exceeded those in Ranch Hand subjects (see Table 4-4 in Chapter 4). The committee there- fore endorses further evaluation and longitudinal analysis of the entire data set
366 VETERANS AND AGENT ORANGE: UPDATE 2006 on cancer outcomes generated in the important AFHS population. The AFHS is of questionable central relevance to the committeeâs charge, but it had a persist- ing concern that there was little suggestion of an association in other relevant populations. The committee members agreed that the two published articles from the AFHS (Akhtar et al., 2004; Pavuk et al., 2005) were very strong ï¬ndings based on TCDD measurements in a study population of prime interest. Several could not, however, agree to move melanoma into the limited or suggestive category, given the paucity of support from other investigated populations. Another re- straining concern was the hint in the report (AFHS, 2005) on those attending the ï¬nal AFHS examination that many more new melanomas were diagnosed among the comparison veterans than in the Ranch Hand subjects, which might produce quite different results if the analyses in Akhtar et al. (2004) were rerun on the ï¬nal data set. Conclusion After extensive deliberation concerning new evidence and the results of stud- ies reviewed in previous updates, the committee was unable to reach consensus as to whether the evidence concerning an association between exposure to the com- pounds of interest and melanoma met the criteria for being considered limited or suggestive or this health outcome should remain in the inadequate or insufï¬cient classiï¬cation primarily because the suggestive ï¬ndings are almost exclusively from the AFHS, whose ï¬nal data on both the Ranch Hand and comparison sub- jects have not yet been analyzed in a satisfactory and uniform manner. SKIN CANCERâBASAL-CELL AND SQUAMOUS-CELL CANCER (NON-MELANOMA) The preceding section on melanoma presented background information on non-melanoma skin cancer. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and skin cancer, and additional informa- tion available to the committee responsible for Update 1996 did not change that conclusion. The Update 1998 committee considered the literature on non- melanoma skin cancer separately from that on melanoma and concluded that there was inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and basal-cell or squamous-cell cancer. The Update 2000 and Update 2002 committees concurred with that conclusion. Table 6-21 summarizes the relevant studies.
CANCER 367 TABLE 6-21 Selected Epidemiologic StudiesâNon-Melanoma (basal- and squamous-cell) Skin Cancer Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b OCCUPATIONAL New Studies Torchio et al., 1994 Italian licensed pesticide users 3 0.6 (0.1â1.8) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators Melanoma, squamous-cell carcinoma, and unknown skin cancer (mortality presumable attributable to melanoma) 5 3.6 (1.2â8.3) Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) Non-melanoma skin cancer 0 â Thörn et al., 2000 Swedish lumberjacks exposed to phenoxyacetic herbicidesâincidence Foremen 1 16.7 (0.2â92.7) Studies Reviewed in Update 1998 Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 4 0.9 (0.3â2.4) Exposed to TCDD (or higher-chlorinated dioxins) 4 1.3 (0.3â3.2) Not exposed to TCDD (or higher- chlorinated dioxins) 0 â* Zhong and Rafnsson, Icelandic pesticide users (men and 1996 womenâincidence) Men 5 2.8 (0.9â6.6) Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 425 1.1 (1.0â1.2) White women 6 1.0 (0.4â2.1) Studies Reviewed in VAO Ronco et al., 1992 Danish workersâincidence Menâself-employed 493 0.7 (p 0.05) employee 98 0.7 (p 0.05) Womenâself-employed 5 0.3 (p 0.05) employee 10 0.9 (*) family worker 90 0.6 (p 0.05) Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 3 3.1 (0.6â9.0) continued
368 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-21 Continued Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b ENVIRONMENTAL Studies Reviewed in Update 1998 Gallagher et al., 1996 Alberta, Canada, residentsâsquamous-cell carcinoma (incidence) All herbicide exposure 79 1.5 (1.0â2.3) Low herbicide exposure 33 1.9 (1.0â3.6) High herbicide exposure 46 3.9 (2.2â6.9) Alberta, Canada, residentsâbasal-cell carcinoma All herbicide exposure 70 1.1 (0.8â1.7) Svensson et al., 1995 Swedish ï¬shermen East coast Incidence 22 2.3 (1.5â3.5) Mortality 0 0.0 (0.0â15.4) West coast Incidence 69 1.1 (0.9â1.4) Mortality 5 3.1 (1.0â7.1) Studies Reviewed in Update 1996 Bertazzi et al., 1993 Seveso residentsâ10-year follow-up (incidence) Zone Aâmen 1 2.4 (0.3â17.2) women 1 3.9 (0.5â28.1) Zone Bâmen 2 0.7 (0.2â2.9) women 2 1.3 (0.3â5.1) Zone Râmen 20 1.0 (0.6â1.6) women 13 1.0 (0.6â1.9) Studies Reviewed in VAO Pesatori et al., 1992 Seveso residentsâincidence Zones A, Bâmen 3 1.0 (0.3â3.0) women 3 1.5 (0.5â4.9) Zone Râmen 20 1.0 (0.6â1.6) women 13 1.0 (0.5â1.7) Wiklund, 1983 Swedish agricultural workersâincidence 708 1.1 (1.0â1.2)c
CANCER 369 TABLE 6-21 Continued Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b VIETNAM VETERANS New Studies Pavuk et al., 2005 White Air Force comparison subjects only (basal and squamous cell)âincidence Serum TCDD levels (pg/g), based on model with exposure variable loge(TCDD)d Per unit increase of âloge(TCDD) in pg/g 253 1.2 (0.9â1.4) Quartiles (pg/g) 0.4â2.6 50 * 2.6â3.8 59 1.2 (0.8â1.8) 3.8â5.2 71 1.5 (1.1â2.3) 5.2 73 1.4 (0.9â2.0) Number of years served in Southeast Asia (SEA) Per year of service 253 1 (0.9 â1.1) Quartiles (years in SEA) 0.8â1.3 55 * 1.3â2.1 50 0.9 (0.6â1.4) 2.1â3.7 73 1.1 (0.8â1.6) 3.7â16.4 75 1.2 (0.8â1.7) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veteransâincidence Basal-cell carcinoma 121 1.2 (0.9â1.6) Squamous-cell carcinoma 20 1.5 (0.8â2.8) CDVA, 1998a Australian Vietnam veteransâmen (incidence) 6,936e ** CDVA, 1998b Australian Vietnam veteransâwomen (incidence) 37e ** Studies Reviewed in VAO Wolfe et al., 1990 Air Force Ranch Hand veteransâincidence Basal-cell carcinoma 78 1.5 (1.0â2.1) Squamous-cell carcinoma 6 1.6 (0.5â5.1) ABBREVIATIONS: AFHS, Air Force Health Study; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval. a Cohorts are male unless otherwise noted. b Given when available. c 99% CI. d The original paper implied that the exposure metric for TCDD was based on actual measured serum levels of TCDD. Subsequent correspondence between the Committee and the investigators indicated that the metric was actually transformed using the natural logarithm of TCDD. e Self-reported medical history. Answer to question: Since your ï¬rst day of service in Vietnam, have you been told by a doctor that you have other skin cancers (basal-cell carcinoma, squamous-cell carcinoma)? * Information not provided by study authors. Studies in italics have been superseded by newer studies of the same cohorts.
370 VETERANS AND AGENT ORANGE: UPDATE 2006 Update of the Epidemiologic Literature Occupational Studies In reporting on cancer incidence in the AHS cohort, Alavanja et al. (2005) did not consider non-melanoma skin cancers, because they are not systematically registered in Iowa or North Carolina. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics re- ports as having high herbicide use, especially of 2,4-D and MCPA. The estimated risk of skin cancer other than melanoma was not increased (three cases; SMR 0.6, 95% CI 0.12â1.75). As in the section above on melanoma, we note here a letter to the editor by Kennedy et al. (2005) although it apparently was not peer-reviewed. They reported the frequency of exposure to herbicides of 103 men with squamous-cell carcinoma, 171 with nodular basal-cell carcinoma, and 78 with superï¬cial mul- tifocal basal-cell carcinoma. Separate exposure rates for cases and controls were not reported in their caseâcontrol study. The ORs for herbicide exposure were 0.8 for squamous-cell carcinoma, 0.6 for nodular basal-cell carcinoma, and 0.5 for superï¬cial multifocal basal-cell carcinoma; all have wide conï¬dence intervals, and none is statistically signiï¬cant. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and non-melanoma skin cancer were published since Update 2004. Vietnam-Veteran Studies Focusing only on the Southeast Asia comparison subjects in the AFHS, Pavuk et al. (2005) reported 253 cases of basal-cell and squamous-cell carci- noma and an overall RR of 1.2 (95% CI 0.9â1.4) when the second, third, and fourth quartiles combined were compared with the ï¬rst quartile for serum TCDD concentrations. A signiï¬cant excess (based on 71 cases) was found for the third quartile (RR 1.5, 95% CI 1.1â2.3; p 0.03). The RR for the fourth quartile was 1.4, but it did not achieve statistical signiï¬cance. The overall doseâresponse relationship in a model that considered individual values for serum TCDD was not statistically signiï¬cant. Those results were adjusted for a number of other risk factors, including military occupation, year of birth, number of years served in Southeast Asia, BMI, skin reaction to sunlight exposure, and eye color.
CANCER 371 Biologic Plausibility Studies in mice that have been designed to determine carcinogenic actions of TCDD generally support the idea that TCDD promotes the formation of skin papillomas and squamous-cell carcinomas (Dunson et al., 2000; Poland et al., 1982; Wyde et al., 2004). However, the observation of the tumor-promoting ef- fects of TCDD only in speciï¬c strains (the genetically initiated TgAc [Dunson et al., 2000; Wyde et al., 2004] and the hairless strain [Hebert et al., 1990; Poland et al., 1982] but not such strains as the ICR strain [Wu et al., 2004]) indicates that activation of multiple carcinogenic pathways is required. Similar studies performed in the Syrian golden hamster revealed that treatment with TCDD alone was sufï¬cient for the development of squamous-cell carcinomas of the facial skin (Rao et al., 1988). Cacodylic acid is a well-known skin carcinogen in humans, but studies in animal models have failed to demonstrate its carcinogenic action in the skin (Cohen et al., 2006). The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis The new results in the Pavuk et al. study, although intriguing, demonstrate only a small RR that is not statistically signiï¬cant, and the doseâresponse rela- tionship also is not statistically signiï¬cant. The only statistically signiï¬cant result was found in the third, rather than the fourth, quartile of exposure to TCDD, although similar estimated risks were found in the second and fourth quartiles. On the basis of the new studies and in accord with the results of reports previ- ously assessed, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and basal-cell or squamous-cell cancer. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and basal-cell or squamous-cell cancer. BREAST CANCER Breast cancer (ICD-9 174 for women, ICD-9 175 for men) is the second- most common type of cancer (after non-melanoma skin cancer) in women in the United States. ACS estimated that 212,920 women would receive diagnoses of breast cancer in the United States in 2006 and that 40,970 would die from it
372 VETERANS AND AGENT ORANGE: UPDATE 2006 (Jemal et al., 2006). Overall, those numbers represent about 31 percent of the new cancers and 15 percent of cancer deaths in women. Incidence data on breast cancer are presented in Table 6-22. Breast-cancer incidence generally increases with age. In the age groups of most Vietnam veterans, the incidence is higher in whites than in blacks. Estab- lished risk factors other than age include personal or family history of breast cancer and some characteristics of reproductive historyâspeciï¬cally, early men- arche, late onset of menopause, and either no pregnancies or ï¬rst full-term preg- nancy after the age of 30 years. A pooled analysis of six large-scale prospective studies of invasive breast cancer showed that alcohol consumption over the range of consumption reported by most women was associated with a linear increase in incidence in women (Smith-Warner et al., 1998). The potential of other personal behavioral and environmental factors (including exogenous hormones) to affect breast-cancer incidence is being studied extensively. Most of the roughly 10,000 female Vietnam veterans who were potentially exposed to herbicides in Vietnam are approaching or have recently reached menopause. Given the high incidence of breast cancer among older and post- menopausal women in general, on the basis of demographics alone it is expected that the breast-cancer burden in female Vietnam veterans will increase in the near future. Breast cancer occurs primarily in women, and the vast majority of breast- cancer epidemiologic studies involve women, but it also occurs in men (ACS, 2006). Reported instances of male breast cancer are noted, but the committeeâs conclusions are based on the studies in women. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and breast cancer. Additional information TABLE 6-22 Average Annual Incidence (per 100,000) of Breast Cancer in Women in the United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 1.34 1.35 2.17 2.7 2.4 6.4 3.8 4.0 5.5 Women 249.0 258.1 227.6 327.2 340.6 281.3 388.4 408.3 333.1 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
CANCER 373 available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-23 summarizes the relevant research. Update of the Epidemiologic Literature Occupational Studies Three reports on breast-cancer risk in spouses in the AHS have been pub- lished since Update 2004. Alavanja et al. (2005) identiï¬ed 474 cases of breast cancer diagnosed through 2002 in the 32,347 spouses of pesticide applicators. No excess breast cancer was observed compared with the general population of North Carolina and Iowa (SIR 0.99, 95% CI 0.90â1.08). It is unclear whether an association between the compounds of interest and breast-cancer risk, if one existed, would be strong enough to increase the estimated risk in such a broadly categorized exposure group. Engel et al. (2005) later conducted more detailed analyses on breast cancer in the same women in relation to type of chemical ex- posure. The association was null for exposure to phenoxy herbicides as a broad category, considering either direct chemical use by the women (RR 0.8, 95% CI 0.6â1.1) or use by the husbands of women who did not apply the chemicals themselves (RR 1.1, 95% CI 0.7â1.8). The results did not vary with duration of exposure, menopausal status, or state of residence (North Carolina vs Iowa). When exposure to 18 speciï¬c herbicides was considered, a signiï¬cant increase in risk was seen only in women whose husbands used trichlorophenoxy propionic acid (2,4,5-TP) (RR 2.0, 95% CI 1.2â3.2). Results for 2,4-D and 2,4,5-T were null. Blair et al. (2005a) analyzed cancer mortality for 1994â2000 in the same cohort and reported no increase in risk of death from breast cancer in the AHS spouses (SMR 0.9, 95% CI 0.7â1.1); the few women among the private ap- plicators had a similar risk with wider conï¬dence limits. Again, in this analysis the use of broad exposure categories could mask an association with the speciï¬c herbicides of interest. In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers from 1969 and 1973, respectively, through 2000. One woman and one man died from breast cancer in the producer group and none of the sprayers. Estimation of breast- cancer risk in this cohort is extremely imprecise because of the small numbers. Mills and Yang (2005) conducted a caseâcontrol study in Hispanic agricul- tural workers in California. They estimated breast-cancer risk in relation to union work histories and pesticide use as recorded in state databases. They considered 13 speciï¬c chemicals, including 2,4-D. With non-exposed women as the referent group, no association with 2,4-D use was seen in women who had breast cancer diagnosed in 1988â1994. For cases diagnosed in the later period of observation (1995â2001), however, high exposure to 2,4-D was associated with a signiï¬cant
374 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-23 Selected Epidemiologic StudiesâBreast Cancer Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a OCCUPATIONAL New Studies McLean et al., IARC cohort of pulp and paper workers 2006 Exposure to nonvolatile organochlorine compounds Never 21 0.9 (0.6â1.4) Ever 32 0.9 (0.6â1.3) Alavanja et al., US Agriculture Health Studyâincidence 2005 Private applicators (men and women) 27 1.1 (0.7â1.6) Spouses of private applicators ( 99% women) 474 1.0 (0.9â1.1) Commercial applicators (men and women) 1 0.6 (0.1â3.5) Blair et al., 2005a US Agriculture Health Studyâmortality Private applicators (men and women) 3 0.9 (0.2â2.7) Spouses of private applicators ( 99% women) 54 0.9 (0.7â1.1) Engel et al., 2005 US Agriculture Health Study, wives of private applicatorsâincidence Wives own use of phenoxy herbicides 41 0.8 (0.6â1.1) 2,4-D 41 0.8 (0.6â1.1) Husbandsâ use of phenoxy herbicides 110 1.1 (0.7â1.8) 2,4-D 107 0.9 (0.6â1.4) 2,4,5-T 44 1.3 (0.9â1.9) 2,4,5-TP 19 2.0 (1.2â3.2) Mills and Yang, Hispanic agricultural farm workers (women) 2005 Cancer diagnosis 1987â1994 Low 2,4-D use 12 0.6 (0.2â1.9) High 2,4-D use 8 0.6 (0.2â1.7) Cancer diagnosis 1995â2001 Low 2,4-D use 19 2.2 (1.0â4.9) High 2,4-D use 21 2.1 (1.1â4.3) ât Mannetje et al., Phenoxy herbicide producers (men and women) 2005 Women 1 1.3 (0.0â7.2) Men 1 32 (0.8â175) Phenoxy herbicide sprayers ( 99% men) 0 0.0 (*) Studies Reviewed in Update 2000 Duell et al., 2000 Female farm workers and residents in North Carolina Used pesticides in the garden 228 2.3 (1.7â3.1) Laundered clothes for pesticide user 119 4.1 (2.8â5.9) Studies Reviewed in Update 1998 Kogevinas et al., IARC cohort 1997 Women (identical with Manz et al., 1991) 9 2.2 (1.0â4.1) Men 2 2.6 (0.3â9.3)
CANCER 375 TABLE 6-23 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states Menâwhite 18 0.7 (0.4â1.2) nonwhite 4 1.7 (0.5â4.4) Womenâwhite 71 1.0 (0.8â1.3) nonwhite 30 0.7 (0.5â1.0) Kogevinas et al., IARC cohortâwomen 7 0.9 (0.4â1.9) 1993 Studies Reviewed in VAO Ronco et al., 1992 Danish and Italian farm workers Male farmers 5 0.5* Female farmers 41 0.9* Female family workers 429 0.8 (p 0.05) Manz et al., 1991 German production workersâmen and women (included in the IARC cohort) Women 9 2.2 (1.0â4.1) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) Men 2 3.5 (0.4â12.5) Women 1 0.3 (0.0â1.7) Lynge, 1985 Danish male and female production workersâ incidence (included in the IARC cohort) Women 13 0.9* Wiklund, 1983 Swedish male and female agricultural workersâincidence 444 0.8 (0.7â0.9)b ENVIRONMENTAL New Studies Reynolds et al., Women undergoing breast biopsies in San 2005 Francisco area hospitalsâ79 breastâcancer cases vs 52 controls with benign breast conditionsâincidence Total TEQs (pg/g) in adipose breast tissue 14.0 24 1.0 14.1â20.9 22 0.7 (0.3â1.9) 21.0 33 0.3 (0.3â2.0) p-trend 0.99 Reynolds et al., California Teachers Study cohort 2004 Residential proximity to use of âendocrine disruptorsâ (including 2,4âD and cacodylic acid) Quartiles of use (lb/mi2) 1 1,027 1.0 1â21 274 1.0 (0.8â1.1) 22â323 114 0.9 (0.7â1.1) 324 137 1.0 (0.9â1.3) continued
376 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-23 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Studies Reviewed in Update 2002 Warner et al., 2002 Seveso Womenâs Health Studyâ981 women who were infants to age 40 when exposedâincidence With 10-fold increase in TCDD level 15 2.1 (1.0â4.6) Revich et al., 2001 Residents of Chapaevsk, Russiaâwomen 58 2.1 (1.6â2.7) Holford et al., 2000 Patients at Yale-New Haven hospital with breast-related surgery; dioxin-like congener 156 * 0.9 (0.8â1.0) Studies Reviewed in Update 2000 Bertazzi et al., Seveso residentsâ20-year follow-up 2001 Zone A, Bâwomen 14 0.7 (0.4â1.3) Bagga et al., 2000 Women receiving medical care in Woodland Hills, California 73 NS Demers et al., 2000 Women in Quebec Cityânewly diagnosed 314 NS Høyer et al., 2000 Female participants of Copenhagen City Heart 195 Overall survival Study RR 2.8 (1.4â5.6) Studies Reviewed in Update 1998 Bertazzi et al., Seveso residentsâ15-year follow-up 1997 Zone Aâwomen 1 0.6 (0.0â3.1) Zone Bâwomen 9 0.8 (0.4â1.5) Zone Râwomen 67 0.8 (0.6â1.0) Studies Reviewed in Update 1996 Bertazzi et al., Seveso residentsâ10-year 1993 follow-upâincidence Zone Aâwomen 1 0.5 (0.1â3.3) Zone Bâwomen 10 0.7 (0.4â1.4) Zone Râwomen 106 1.1 (0.9â1.3) men 1 1.2 (0.1â10.2) Studies Reviewed in VAO Bertazzi et al., Seveso residentsâ10-year follow-up 1989b Zone Aâwomen 1 1.1 (0.1â7.5) Zone Bâwomen 5 0.9 (0.4â2.1) Zone Râwomen 28 0.6 (0.4â0.9) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 7 0.9 (0.4â1.9) Navy 1 0.6 (0.0â3.3) Army 5 1.0 (0.3â2.2) Air Force 1 1.1 (0.0â6.3)
CANCER 377 TABLE 6-23 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 4 2.2 (0.6â5.4) Navy 1 2.5 (0.0â13.5) Army 3 2.5 (0.5â7.2) Air Force 0 0.0 (0.0â14.6) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veteransâdeployed vs non-deployed 0 â Incidence 0 0.0 (0.0â2.4) Mortality * Boehmer et al., Follow-up of CDC Vietnam Experience Cohort 0 â 2004 Studies Reviewed in Update 2002 Kang et al., 2000 Female Vietnam veterans 170 1.2 (0.9â1.5) Studies Reviewed in Update 2000 CDVA, 1998b Australian Vietnam veteransâwomen 17c 5 expected (2â11) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veteransâmen 3 5.5 (1.0â 10.0) Studies Reviewed in Update 1996 Dalager et al., 1995 Female US Vietnam veterans 26 1.0 (0.6â1.8) Studies Reviewed in VAO Thomas et al., Female US Vietnam veterans 17 1.2 (0.6â2.5) 1991 ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; CI, conï¬dence interval; IARC, Inter- national Agency for Research on Cancer; NS, not signiï¬cant; PCB, polychlorinated biphenyls; RR, relative risk; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin; TEQ, toxicity equivalency. a Given when available. b 99% CI. c Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have breast cancer?â * Information not provided by study authors. Studies in italics have been superseded by newer studies of the same cohorts. increase in breast cancer (OR 2.14, 95% CI 1.06â4.32), and low exposure was associated with a similar increase (OR 2.16, 95% CI 0.95â4.93). It is not clear why a positive association was apparent only in the later years of observation, but it is conceivable that risk increased as latency and exposure duration increased. Individual-level data on established breast-cancer risk factors were not available; county-level data on fertility and socioeconomic status were used as surrogates in adjusted analyses. That is an important limitation in a breast-cancer study because misclassiï¬cation of established risk factors as covariates can introduce substantial
378 VETERANS AND AGENT ORANGE: UPDATE 2006 bias. However, fertility rates by county were inversely associated with breast- cancer risk in subjects in this study, so this ecologic variable might have been capturing some of the confounding that could occur because of different repro- ductive patterns between cases and controls. The strengths of this studyâwhich bears on 2,4-D exposure only, not dioxinsâinclude the use of a comprehensive statewide cancer registry for ascertainment of breast-cancer status and unbiased exposure estimation because of linkage of individual work records to a detailed database on agricultural chemical use. Environmental Studies Reynolds et al. (2004) used a geographic information system (GIS) to link data on pesticide use to residential histories of women in the California Teach- ers Study cohort. Two compounds of interest, 2,4-D and cacodylic acid, were included among 34 chemicals in a category labeled endocrine disruptors but were not addressed in any speciï¬c analyses. Residential proximity to use of chemicals in the entire category was not associated with breast-cancer risk (for the heaviest vs the lowest exposure intensity, RR was 1.03, 95% CI 0.86â1.25). It is not clear how many subjects in the analysis had substantial exposure to the compounds. In another GIS analysis, Brody et al. (2004) compared residential proximity to pesticide sources in people with breast cancer and controls in Massachusetts. No associations were observed; however, the relevance of the study is limited by uncertainty in the extent of exposure to any of the compounds of interest. Mills and Yang (2006) computed RRs of breast cancer among Latina women in California according to countywide data on pesticide use. Signiï¬cant increases in risk were reported in association with two organochlorines (methoxychlor and toxaphene); however, risk estimates were not provided for any of the speciï¬c compounds of interest. The analysis carries less weight than the previously de- scribed study on Latina farm workers by the same authors because, although the number of breast cancers is much greater, the proportion of women signiï¬cantly exposed to the chemicals is much lower. Three recent studies are noteworthy for having measured organochlorines in adipose tissue in breast-cancer cases and controls, although two of them are not very informative, because of lack of focus on the speciï¬c compounds of interest. The ï¬rst, a methodologic study by Petreas et al. (2004), is discussed in Chapter 5 in connection with exposure considerations. Raaschou-Nielsen et al. (2005) compared 409 postmenopausal Danish women with breast cancer to an equal number of matched controls selected from a large research cohort. Fourteen pesticides and 18 polychlorinated biphenyl (PCB) congeners were measured in adipose tissue from the buttocks; women with higher adipose-tissue concentrations of the compounds did not have a higher risk of breast cancer. In fact, the study found strong inverse associations with risk of estrogen-receptor-negative breast cancer in women with the highest concentra-
CANCER 379 tions of total PCBs and several organochlorine pesticides (p 0.007 for trend across quartiles of total PCBs). The investigators speculate that the inverse as- sociations could have resulted from higher ï¬sh consumption by controls or from more rapid metabolic conversion of precursors to proximal carcinogens by the women with cancer. The study is noteworthy because of its size and because it is the ï¬rst to use adipose-tissue organochlorines in a prospective analysis of breast- cancer risk. However, its relevance for the purposes of the present committee is limited by the lack of TCDD measurement and by the extreme weakness of the dioxin-like activity of the PCB congeners. Reynolds et al. (2005) measured dioxin in breast adipose tissue obtained from 79 women with breast cancer and 52 controls with benign breast conditions. They found no associations between any of 17 polychlorinated dibenzodioxins and dibenzofurans with substitutions in the 2, 3, 7, or 8 positions. When all mea- sured compounds were combined as international toxic equivalent units, the OR for the highest tertile vs the lowest was 0.73 (95% CI 0.27â1.95). Although small and lacking in statistical power, the study is unique in its focus on the target-organ exposure and the speciï¬c compounds of interest. Vietnam-Veteran Studies In the mortality update of the CDC VES of only male subjects through 2000, Boehmer et al. (2004) reported a single case of breast cancer in the non-deployed. Similarly, the updates on the health status of Australian Vietnam veterans reported only on male veterans but included scattered breast-cancer cases. No increase was seen when veterans were compared with the general population of Australia in incidence (SIR 0.90, 95% CI 0.36â1.86) (ADVA, 2005a), but four deaths produced a non-signiï¬cant increase in mortality (SMR 2.15, 95% CI 0.58â5.42) (ADVA, 2005b). In the comparison of deployed with non-deployed Vietnam vet- erans (ADVA, 2005c), only two breast-cancer cases were identiï¬ed, both in the non-deployed, and no deaths from this type of cancer. Biologic Plausibility All the experimental evidence indicates that 2,4-D, 2,4,5-T, and TCDD are weakly genotoxic if at all. However, TCDD is a demonstrated carcinogen in animals and is classiï¬ed as a human carcinogen because of its ability to act as a strong tumor promoter. The possible general mechanisms by which TCDD may exert those effects are discussed in Chapter 3. With respect to breast cancer, studies performed in laboratory animals (Sprague-Dawley rats) indicate that the effect of TCDD may depend on the age of the animal. For example, TCDD exposure was found to inhibit mammary-tumor growth in the adult rat (Holcombe and Safe, 1994) but to increase tumor growth in the neonatal rat (21 days old) (Desaulniers et al., 2001). Other studies have
380 VETERANS AND AGENT ORANGE: UPDATE 2006 failed to demonstrate a TCDD effect on mammary-tumor incidence or growth (Desaulniers et al., 2004). Those observations may indicate a close association between the development of mammary cancers and mammary gland differentiation. Agents capable of disrupting the ability of the normal mammary epithelial cell to enter or maintain its appropri- ate status (a proliferative, differentiated, apoptotic state), to maintain its appropriate architecture, or to alter key hormone (estrogen) signaling are likely to act as carci- nogenic agents (Fenton, 2006; McGee et al., 2006). In that light, it is interesting that postnatal exposure of pregnant rats to TCDD has been found to alter proliferation and differentiation of the mammary gland (Birnbaum and Fenton, 2003; Vorderstrasse et al., 2004). Thus, the effect of TCDD may depend on the timing of the exposure and may affect mammary-tumor development only if the exposure occurs during a speciï¬c window during mammary development. The breast is the only human organ that does not fully differentiate until it becomes ready for use; nulliparous women have less-differentiated breast lobules, which are presumably more vulnerable to carcinogenesis. The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Recent results from the AHS cohort generally do not support the hypoth- esis that exposure to the compounds in Agent Orange increases breast-cancer incidence or mortality in women, although exposure to the speciï¬c compounds of interest was not speciï¬ed. Increased risks observed in one subgroup whose husbands worked with 2,4,5-TP will require further study and conï¬rmation; this ï¬nding could have arisen by chance. Recent studies of environmental exposure found null associations; however, exposures were of questionable relevance. Two studies of organochlorine concentrations in adipose tissue failed to ï¬nd any evi- dence of increased risk in association with higher adipose concentrations; in fact, the more relevant study found the risk in the highest tercile of dioxin concentra- tions in breast fat was lower than in the lowest tercile of dioxin concentrations, although not signiï¬cantly so. One study published since the last update does provide some evidence of an association between exposure to 2,4-D and breast-cancer risk in female farm- workers in California (Mills and Yang, 2005). The study is limited by lack of detailed information on potential confounding factors and lack of evidence of a doseâresponse relationship, but it is large and the investigators were able to estimate individual exposures by linking work histories to an extensive database on pesticide use. The committee considered the new information in the context of the cumula- tive data from studies reviewed in previous updates. Results of several prior stud- ies lend support to the hypothesis that there is an association between exposure to
CANCER 381 the compounds of interest, speciï¬cally, studies by Kogevinas et al. (1997), Kang et al. (2000), Revich et al. (2001), and Warner et al. (2002). The ï¬rst of those studies is a mortality study of a large multinational cohort of workers exposed to phenoxy herbicides or chlorophenols in manufacturing or spraying (Kogevinas et al., 1997). In women speciï¬cally exposed to TCDD and higher chlorinated dioxins, there were nine deaths from breast cancer vs 4.17 expected (SMR 2.16, 95% CI 0.99â4.10), whereas there was no appreciable risk in other women in the cohort. All nine deaths occurred in the German her- bicide plant that accounted for most of the exposure of women to TCDD. The breast-cancer SMR for this plant alone was 2.84 (95% CI 1.30â5.39). There were also two deaths from breast cancer in the multinational cohort in men exposed to TCDD and higher chlorinated dioxins; this is more than expected for this rare tumor, but such a result could have arisen by chance. Kang et al. (2000) reported an increased OR for breast cancer in a cross- sectional study comparing female Vietnam veterans with non-Vietnam veterans (multivariate OR 1.18, 95% CI 0.91â1.51). Revich et al. (2001) calculated SMRs for women occupationally or environ- mentally exposed to dioxins in Chapaevsk, Russia, the site of a large chemical plant. Substantially increased concentrations of dioxins were measured in soil, drinking water, and breast milk in Chapaevsk and in the serum of people who worked in the factory or lived nearby. The SMR for breast cancer in the town of Chapaevsk, with 58 observed deaths and expected numbers based on rates for the entire region, was signiï¬cantly increased (SMR 2.1, 95% CI 1.6â2.7). That result has limited weight because women in the town were exposed to numerous toxic chemicals, and, although widespread contamination with dioxin was docu- mented, it is difï¬cult to attribute the breast-cancer excess to dioxins alone. Finally, in a study of women exposed in Seveso (Warner et al., 2002), there was a signiï¬cant association between lipid-adjusted serum TCDD concentrations and breast-cancer incidence (RR 2.1 for a 10-fold increase in serum TCDD, 95% CI 1.0â4.6). The study found no difference in the risk estimate after com- prehensive adjustment for established or potential breast-cancer risk factors. It is important to note that the Seveso Womenâs Cohort Study ascertained breast- cancer status 20â22 years after the Seveso explosion by interview followed by medical-record veriï¬cation; the study did not include three women who had already died from breast cancer before the interviews took place. The committee believes that the recent data from the study by Mills and Yang (2005), although not persuasive in themselves, lend additional weight to an association between the relevant herbicide exposures and breast-cancer risk. This study has reasonable size and relatively speciï¬c exposure information but is limited chieï¬y by the data available to control for confounding. Among the four earlier studies contributing to the committeeâs view, two have highly speciï¬c exposure data (related to occupational exposure to phenoxy herbicides and to Seveso), one reports an increased risk in women living in an area with
382 VETERANS AND AGENT ORANGE: UPDATE 2006 documented heavy dioxin contamination (Chapaevsk), and one reports an in- creased risk in female Vietnam veterans that does not achieve the conventional level of statistical signiï¬cance. Each study has limitations or weaknesses that keep its conclusions about the association in question from being deï¬nitive. Some members of the committee considered the body of evidence as a whole to be suggestive of an association; for others, the few modestly positive results associated with a diversity of exposures suggested chance ï¬ndings rather than a coherent picture. Further laboratory and epidemiologic work on this association should be pursued. The main reason for the unresolved division in the committeeâs opinion concerning the adequacy of the available evidence to support an association be- tween breast cancer and exposure to the components of the herbicides sprayed in Vietnam was differing individual views about the speciï¬city and relevance of the studied exposures for the population of primary concern to the committee, Viet- nam veterans. Overall, the committee was impressed by the positive results from Seveso, but several members considered this a very small sample upon which to anchor an association. The degree to which the proï¬le of chemicals contributing to total toxicity equivalency (TEQ) in the more positive epidemiologic studies dif- fered from that of Vietnam veterans diminished the conviction of some members that these results constituted fully relevant evidence. Conclusion After extensive deliberation concerning the new evidence and the results of studies reviewed in previous updates, the committee was unable to reach consensus as to whether the evidence of an association between exposure to the compounds of interest and breast cancer met the criteria for being considered limited or suggestive or whether concerns about chance, bias, and confounding remained so substantial that breast cancer should remain in the inadequate or insufï¬cient classiï¬cation. CANCERS OF THE FEMALE REPRODUCTIVE SYSTEM This section addresses cancers of the cervix (ICD-9 180), endometrium (also referred to as the corpus uteri; ICD-9 182.0â182.1, 182.8), and ovary (ICD-9 183.0). Other cancers of the female reproductive system that are infrequently reported separately are unspeciï¬ed cancers of the uterus (ICD-9 179), placenta (ICD-9 181), fallopian tube and other uterine adnexa (ICD-9 183.2â183.9), and other female genital organs (ICD-9 184); any ï¬ndings on these cancers would be included in this section. It also presents statistics on other cancers of the female reproductive system. ACS estimates of the numbers of new female reproductive- system cancers in the United States in 2006 are presented in Table 6-24, with
CANCER 383 genital-system cancers representing roughly 11 percent of new cancer cases and 10 percent of cancer deaths in women (Jemal et al., 2006). The incidences of and risk factors for those diseases vary (Table 6-25). Cer- vical cancer occurs more often in blacks than in whites, whereas whites are more likely to develop endometrial and ovarian cancer. The incidence of endometrial and ovarian cancer is increased among older women and among those with posi- tive family histories. Use of unopposed estrogen hormone therapy and obesity, which increases endogenous concentrations of estrogen, both increase the risk of endometrial cancer. HPV infection, particularly infection with HPV types 16 and 18, is the most important risk factor for cervical cancer. Use of oral contraceptives is associated with a substantial reduction in the risk of ovarian cancer. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between ex- posure to the compounds of interest and female reproductive cancers. Additional information available to the committees responsible for Update 1996, Update TABLE 6-24 Estimates of New Cases and Deaths in 2004 in United States for Selected Cancers of the Female Reproductive Systema Site New Cases Deaths Cervix 9,710 3,700 Endometrium 41,200 7,350 Ovary 20,180 15,310 Other female genital 2,420 2,420 a ACS (2006). TABLE 6-25 Average Annual Incidence (per 100,000) of Female Genital System Cancers in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black All genital sites 85.5 89.5 61.7 119.3 126.3 80.0 151.1 156.5 145.3 Cervix 11.7 10.9 15.3 11.8 10.8 17.8 13.2 11.4 25.8 Endometrium 45.5 48.8 24.6 68.6 73.7 36.6 88.6 93.0 77.1 Ovary 22.8 24.2 15.1 31.5 33.9 17.8 39.3 42.0 30.7 Other genital organs 1.1 1.1 0.6 1.5 1.7 0.9 2.7 2.6 1.2 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
384 VETERANS AND AGENT ORANGE: UPDATE 2006 1998, Update 2000, Update 2002, and Update 2004 did not change that conclu- sion. Tables 6-26, 6-27, and 6-28 summarize the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies In the analysis of cancer incidence in the AHS, Alavanja et al. (2005) re- ported an excess of ovarian cancer in pesticide applicators (SIR 2.97, 95% CI 1.28â5.85) but a signiï¬cantly reduced incidence in spouses of farmer applicators (SIR 0.55, 95% CI 0.38â0.78). Blair et al. (2005a) observed parallel results for mortality in the same cohort: death from ovarian cancer was increased in applicators (on the basis of only four deaths) but not in farmer spouses. Neither incidence of nor mortality from other female reproductive cancers (combined) was reported to be increased in the analyses. No new environmental or Vietnam-veteran studies concerning exposure to the compounds of interest and female reproductive cancer were published since Update 2004. Biologic Plausibility No animal studies have reported an increased incidence of female reproduc- tive cancer after exposure to the compounds of interest. One study (Kociba et al., 1978), however, showed a reduced incidence of uterine tumors in rats fed TCDD at 0.1 mg/kg of diet for 2 years. The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Two analyses of the same cohort found increased incidence of and mortality from ovarian cancer in women who had been engaged in pesticide application. The weight of those studies for the present purposes is limited by the lack of de- tail on chemical exposures and the absence of data that would allow for control of confounding. Future studies of ovarian cancer should be watched carefully, particularly studies that use biomarkers of exposure or more detailed chemical- exposure histories.
CANCER 385 TABLE 6-26 Selected Epidemiologic StudiesâCervical Cancers Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a OCCUPATIONAL Studies Reviewed in Update 1998 Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 3 1.1 (0.2â3.3) Exposed to TCDD (or higher-chlorinated dioxins 0 0.0 (0.0â3.8) Not exposed to TCDD (or higher- chlorinated dioxins) 3 1.8 (0.4â5.2) Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states Whites 6 0.9 (0.3â2.0) Nonwhites 21 2.0 (1.3â3.1) Lynge, 1993 Danish phenoxy herbicide workers 7 3.2 (1.3â6.6) Studies Reviewed in VAO Wiklund, 1983 Swedish men and women agricultural workersâincidence 82 0.6 (0.4â0.8)b Ronco et al., 1992 Danish self-employed farm farmersâincidence Self-employed farmers 7 0.5 (p 0.05) Family workers 100 0.5 (p 0.05) Employees 12 0.8* ENVIRONMENTAL Studies Reviewed in Update 2002 Revich et al., 2001 Residents of Chapaevsk, Russia 13 1.8 (1.0â3.1) VIETNAM VETERANS Studies Reviewed in Update 2002 Kang et al., 2000 Female Vietnam veterans 57 1.1 (0.7â1.7) Studies Reviewed in Update 2000 CDVA, 1998b Australian Vietnam veteransâwomen 8c 1 expected (0â5) ABBREVIATIONS: CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence inter- val; IARC, International Agency for Research on Cancer. a Given when available. b 99% CI. c Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have cancer of the cervix?â * Information not provided by study authors.
386 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-27 Selected Epidemiologic StudiesâUterine Cancers Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a OCCUPATIONAL Studies Reviewed in Update 1998 Kogevinas et al., 1997 IARC cohort (includes cancers of the endometrium) Workers exposed to any phenoxy herbicide or chlorophenol 4 2.3 (0.6â5.9) Exposed to TCDD (or higher- chlorinated dioxins 3 3.4 (0.7â10.0) Not exposed to TCDD (or higher- chlorinated dioxins) 1 1.2 (0.0â6.5) Studies Reviewed in VAO Blair et al., 1993 US farmers in 23 states Whites 15 1.2 (0.7â2.1) Nonwhites 17 1.4 (0.8â2.2) Ronco et al., 1992 Danish self-employed farm farmersâincidence Self-employed farmers 8 0.6* Family workers 103 0.8 (p 0.05) Employees 9 0.9* Wiklund, 1983 Swedish men and women agricultural workersâincidence 135 0.9 (0.7â1.1)b ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zones A, Bâwomen 2 0.5 (0.1â1.9) Weiderpass et al., 2000 Swedish women 154 1.0 (0.6â2.0) Bertazzi et al., 1998 Seveso residentsâ15-year follow-up Zone Bâwomen 1 0.3 (0.0â2.4) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Bâwomen 1 0.3 (0.0â1.9) Zone Râwomen 27 1.1 (0.8â1.7) VIETNAM VETERANS Studies Reviewed in Update 2002 Kang et al., 2000 Female Vietnam veterans 41 1.0 (0.6â1.6) Studies Reviewed in Update 2000 CDVA, 1998b Australian Vietnam veteransâwomen 4c 1 expected (0â5)
CANCER 387 TABLE 6-27 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Studies Reviewed in Update 1996 Dalager et al., 1995 Female Vietnam veterans 4 2.1 (0.6â5.4) ABBREVIATIONS: CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer. a Given when available. b 99% CI. c Self-reported medical history. Answer to question: Since your ï¬rst day of service in Vietnam, have you been told by a doctor that you have uterine cancer? * Information not provided by study authors. Studies in italics have been superseded by newer studies of the same cohorts. TABLE 6-28 Selected Epidemiologic StudiesâOvarian Cancer Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a OCCUPATIONAL New Studies Alavanja et al., 2005 US Agriculture Health Studyâincidence Private applicators (men and women) 8 3.0 (1.3â5.9) Spouses of private applicators ( 99% women) 32 0.6 (0.4â0.8) Commercial applicators (men and women) 0 0.0 (0.0â16.0) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 4 3.9 (1.1â10.1) Spouses of private applicators ( 99% women) 13 0.7 (0.4â1.2) Studies Reviewed in Update 1998 Kogevinas et al., 1997 IARC cohort Workers exposed to any phenoxy herbicide or chlorophenol 1 0.3 (0.0â1.5) Exposed to TCDD (or higher-chlorinated dioxins 0 0.0 (0.0â2.6) Not exposed to TCDD (or higher- chlorinated dioxins) 1 0.5 (0.0â2.5) Studies Reviewed in Update 1996 Kogevinas et al., 1993 IARC cohort 1 0.7* Studies Reviewed in VAO Ronco et al., 1992 Danish self-employed farmersâincidence Self-employed farmers 12 0.9* Family workers 104 0.8 (p 0.05) Employees 5 0.5* Donna et al., 1984 Female residents near Alessandria, Italy 18 4.4 (1.9â16.1) continued
388 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-28 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zones A, Bâwomen 3 0.7 (0.2â2.0) Bertazzi et al., 1998 Seveso residentsâ15-year follow-up Zone Aâwomen 1 2.3 (0.3â16.5) Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Aâwomen 1 2.3 (0.0â12.8) Zone Râwomen 21 1.0 (0.6â1.6) VIETNAM VETERANS Studies Reviewed in Update 2002 Kang et al., 2000 Female Vietnam veterans 16 1.8 (0.7â4.6) Studies Reviewed in Update 2000 CDVA, 1998b Australian Vietnam veteransâwomen 1b 0 expected (0â4) ABBREVIATIONS: CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer. a Given when available. b Self-reported medical history. Answer to question: Since your ï¬rst day of service in Vietnam, have you been told by a doctor that you have ovarian cancer? * Information not provided by study authors. Studies in italics have been superseded by newer studies of the same cohorts. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and uterine, ovarian, or cervical cancer. PROSTATE CANCER ACS estimated that 234,460 new cases of prostate cancer (ICD-9 185) would be diagnosed in the United States in 2006 and that 27,350 men would die from it (Jemal et al., 2006). That makes prostate cancer the second-most common cancer in men (after non-melanoma skin cancers); it is expected to account for about 33 percent of new cancer diagnoses and 9 percent of cancer deaths in men in 2006. The average annual incidence of prostate cancer is shown in Table 6-29. Incidence varies dramatically with age and race. The risk more than doubles between the ages of 50â54 years and 55â59 years, and it nearly doubles again
CANCER 389 TABLE 6-29 Average Annual Incidence (per 100,000) of Prostate Cancer in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black 146.6 140.6 278.0 356.1 342.9 648.6 620.6 609.2 1,043.0 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. between the ages of 55â59 years and 60â64 years. As a group, American black men have the highest recorded incidence of prostate cancer in the world (Miller et al., 1996). Their risk is roughly twice that in whites in the United States, 5 times that in Alaska natives, and nearly 8.5 times that in Korean Americans. Little is known about the causes of prostate cancer. Other than race and age, risk factors include a family history of the disease and possibly some elements of the Western diet, such as high consumption of animal fats. The study of the incidence of and mortality from prostate cancer is com- plicated by trends in screening for the disease. The recent introduction and widespread adoption of prostate-speciï¬c antigen (PSA) for screening have led to improved detection and thus to reports of increased incidence in the United States. The long-term inï¬uence of better screening on incidence and mortality, however, is difï¬cult to predict for any country or population, and it will depend on the rapidity with which the screening tool is adopted, its differential use in men of various ages, and the aggressiveness of tumors detected early with this test (Gann, 1997). Because exposure to PSA testing is such a strong determinant of prostate-cancer incidence, epidemiologic studies must be careful to exclude differential PSA testing as an explanation of a difference in risk observed between two populations. Prostate cancer tends not to be fatal, so mortality studies might miss an in- creased incidence of the disease. Findings that show an association between an exposure and prostate-cancer mortality should be examined closely to determine whether the exposed group might have had poorer access to treatment that would have increased the likelihood of survival. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was limited or suggestive evidence of an association between exposure to the compounds of interest and prostate cancer. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Up- date 2004 did not change that conclusion. Table 6-30 summarizes results of the relevant studies, including morbidity and mortality studies. The type, quality, and
390 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-30 Selected Epidemiologic StudiesâProstate Cancer Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 117 0.9 (0.7â1.0) Ever 84 0.9 (0.7â1.2) Alavanja et al., 2005 US Agriculture Health Studyâincidence Private applicators (men and women) 1,046 1.3 (1.2â1.3) Spouses of private applicators ( 99% women) 5 1.2 (0.4â2.8) Commercial applicators (men and women) 41 1.4 (1.0â1.9) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 48 0.7 (0.5â0.8) Spouses of private applicators ( 99% women) 0 0.0 (0â1.6) ât Mannetje et al., 2005 Phenoxy herbicide producers (men and women) 1 0.4 (0.0â2.1) Phenoxy herbicide sprayers ( 99% men) 2 0.6 (0.1â2.2) Torchio et al., 1994 Italian licensed pesticide users 66 1.0 (0.7â1.2) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 12 0.7 (0.4â1.3) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 6 1.0 (0.4â2.2) Alavanja et al., 2003 US Agriculture Health Studyâ Pesticide appliers from Iowa and North Carolinaâincidence 566 1.1 (1.1â1.2) Bodner et al., 2003 Dow chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) â 1.7 (1.0â2.6) Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 7 1.3 (0.5â2.8) Thörn et al., 2000 Swedish lumberjacks exposed to phenoxyacetic herbicides Foremenâincidence 2 4.7 (*) Male lumberjacksâincidence 3 0.9 (*)
CANCER 391 TABLE 6-30 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Studies Reviewed in Update 2000 Sharma-Wagner et al., Swedish citizens 2000 Agriculture and stock raising 6,080 1.1 (1.0â1.1) (p 0.01) Farmers, foresters, and gardeners 5,219 1.1 (1.0â1.1) (p 0.01) Paper mill workers 304 0.9 (0.8â1.0) Pulp grinding 39 1.4 (1.0â1.9) (p 0.05) Fleming et al., 1999a Florida pesticide appliers 353 1.9 (1.7â2.1) Fleming et al., 1999b Florida pesticide appliers 64 2.4 (1.8â3.0) Steenland et al., 1999 US chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 28 1.2 (0.8â1.7) Dich and Wiklund, 1998 Swedish pesticide appliers 401 1.1 (1.0â1.2) Born 1935 or later 7 2.0 (0.8â4.2) Born before 1935 394 1.1 (1.0â1.2) Studies Reviewed in Update 1998 Gambini et al., 1997 Italian rice growers 19 1.0 (0.6â1.5) Hertzman et al., 1997 Canadian sawmill workers Morbidity 282 1.0 (0.9â1.1) Mortality from male genital tract cancers 116 1.2 (1.0â1.4) Kogevinas et al., 1997 IARC cohort (men and women) Workers exposed to any phenoxy herbicide or chlorophenol 68 1.1 (0.9â1.4) Exposed to TCDD (or higher- chlorinated dioxins 43 1.1 (0.8â1.5) Not exposed to TCDD (or higher- chlorinated dioxins) 25 1.1 (0.7â1.6) Becher et al., 1996 German production workers (included in the IARC cohort) 9 1.3* Ott and Zober, 1996 BASF employeesâincidence TCDD g/kg of body weight) 0.1 4 1.1 (0.3â2.8) 0.1â0.99 1 1.1 (0.0â5.9) Zhong and Rafnsson, 1996 Icelandic pesticide users 10 0.7 (0.3â1.3) Studies Reviewed in Update 1996 Asp et al., 1994 Finnish herbicide applicators Incidence 6 0.4 (0.1â0.8) Mortality 5 0.8 (0.3â1.8) Blair et al., 1993 US farmers in 23 states (men and women) Whites 3,765 1.2 (1.1â1.2) Nonwhites 564 1.1 (1.1â1.2) continued
392 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-30 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Bueno de Mesquita et al., Dutch phenoxy herbicide workers 1993 (included in the IARC cohort) 3 2.6 (0.5â7.7) Collins et al., 1993 Monsanto Company workers (included in the NIOSH cohort) 9 1.6 (0.7â3.0) Studies Reviewed in VAO Morrison et al., 1993 Canadian farmers, 45â69 years old, no employees, or custom workers, sprayed 250 acres 20 2.2 (1.3â3.8) Ronco et al., 1992 Danish workersâincidence Menâself-employed 399 0.9 (p 0.05) employee 63 0.8 (p 0.05) Swaen et al., 1992 Dutch licensed herbicide applicators 1 1.3 (0.0â7.3) Fingerhut et al., 1991 NIOSHâentire cohort 17 1.2 (0.7â2.0) 1-year exposure; 20-year latency 9 1.5 (0.7â2.9) Manz et al., 1991 German production workersâmen and women (included in the IARC cohort) 7 1.4 (0.6â2.9) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 30 1.1 (0.8â1.6) Zober et al., 1990 BASF employeesâbasic cohort 0 * (0.0â6.1)b Alavanja et al., 1989 USDA forest conservationists * 1.6 (0.9â3.0) Soil conservationists * 1.0 (0.6â1.8) Henneberger et al., 1989 New Hampshire pulp and paper workers 9 1.0 (0.5â1.9) Solet et al., 1989 US paper and pulp workers 4 1.1 (0.3â2.9) Alavanja et al., 1988 USDA agricultural extension agents * 1.0 (0.7â1.5) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 1 1.0 (0.0â5.8) Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 18 1.3 (0.8â2.1) Robinson et al., 1986 Northwestern US paper and pulp workers 17 1.2 (0.7â1.7)b Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) 9 0.8* Blair et al., 1983 Florida pesticide applicators 2 3.8 expected Burmeister et al., 1983 Iowa residentsâfarm exposures 4,827 1.2 (p 0.05) Wiklund, 1983 Swedish male and female agricultural workers 3,890 1.0 (0.9â1.0)c Burmeister, 1981 Iowa farmers 1,138 1.1 (p 0.01) ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zones A, Bâmen 8 1.1 (0.5â2.2)
CANCER 393 TABLE 6-30 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Studies Reviewed in Update 1998 Bertazzi et al., 1997 Seveso residentsâ15-year follow-up Zone Bâmen 6 1.2 (0.5â2.7) Zone Râmen 39 1.2 (0.8â1.6) Svensson et al., 1995 Swedish ï¬shermenâmortality East coast 12 1.0 (0.5â1.8) West coast 123 1.1 (0.9â1.3) Swedish ï¬shermenâincidence East coast 38 1.1 (0.8â1.5) West coast 224 1.0 (0.9â1.1) Studies Reviewed in Update 1996 Bertazzi et al., 1993 Seveso residentsâ10-year follow-upâincidence Zone Râmen 16 0.9 (0.5â1.5) Studies Reviewed in VAO Pesatori et al., 1992 Seveso residentsâincidence Zones A, Bâmen 4 1.4 (0.5â3.9) Zone Râmen 17 0.9 (0.6â1.5) Bertazzi et al., 1989a Seveso residentsâ10-year follow-up Zones A, B, Râmen 19 1.6 (1.0â2.7) Bertazzi et al., 1989b Seveso residentsâ10-year follow-up Zone Bâmen 3 2.2 (0.7â6.9) Zone Râmen 16 1.6 (0.9â2.7) VIETNAM VETERANS New Studies Leavy et al., 2006 606 Prostate cancer cases in Western Australia Vietnam service 25 2.1 (0.9â5.1) continued
394 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-30 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Pavuk et al., 2006 AFHS subjectsâincidence 20-yr cumulative TCDD (ppt-yr) Comparison group 81 1.0 RH low ( 434 ppt-yr) 31 1.0 (0.7â1.6) RH high ( 434 ppt-yr) 28 1.2 (0.8â1.9) p-trend 0.42 Last tour in SEA before 1969 (heavy spraying) Yes Comparison group 17 1.0 RH low ( 434 ppt-yr) 9 1.0 (0.4â2.3) RH high ( 434 ppt-yr) 15 2.3 (1.1â4.7) p-trend 0.04 No Comparison group 64 1.0 RH low ( 434 ppt-yr) 22 1.1 (0.7â1.8) RH high ( 434 ppt-yr) 13 0.9 (0.5â1.6) p-trend 0.75 Less than 2 years served in SEA Yes Comparison group 16 1.0 RH low ( 434 ppt-yr) 20 1.9 (1.0â3.7) RH high ( 434 ppt-yr) 14 2.2 (1.0â4.5) p-trend 0.03 No Comparison group 65 1.0 RH low ( 434 ppt-yr) 11 0.8 (0.4â1.5) RH high ( 434 ppt-yr) 14 1.1 (0.6â1.9) p-trend 0.89 ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 692 1.3 (1.2â1.3) Navy 137 1.2 (1.0â1.4) Army 451 1.8 (1.2â1.4) Air Force 104 1.3 (1.0â1.5) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 107 1.2 (1.0â1.5) Navy 22 1.3 (0.8â1.8) Army 65 1.2 (0.9â1.5) Air Force 19 1.4 (0.8â2.1) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veteransâdeployed vs non-deployed Incidence 65 1.2 (0.9â1.5) Mortality 0 0.0 (0.0â0.7)
CANCER 395 TABLE 6-30 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Pavuk et al., 2005 White Air Force comparison subjects onlyâincidence Serum TCDD levels (pg/g), based on model with exposure variable loge(TCDD)d Per unit increase of âloge(TCDD) in pg/g 83 1.1 (0.7â1.5) Quartiles (pg/g) 0.4â2.6 13 1.0 2.6â3.8 24 1.7 (0.8â3.3) 3.8â5.2 24 1.5 (0.7â2.9) 5.2 22 1.2 (0.6â2.4) Number of years served in Southeast Asia (SEA) Per year of service 83 1.1 (1.0â1.2) Quartiles (years in SEA) 0.8â1.3 8 1.0 1.3â2.1 11 1.3 (0.5â3.2) 2.1â3.7 28 2.2 (1.0â4.9) 3.7â16.4 36 2.4 (1.1â5.2) Boehmer et al., 2004 Follow-up of CDC Vietnam Experience Cohort 1 0.4 continued
396 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-30 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Studies Reviewed in Update 2004 Akhtar et al., 2004 AFHS subjects vs national rates White AFHS Ranch Hand veterans Mortalityâall 2 0.7 (0.1â2.3) Incidenceâall 36 1.5 (1.0â2.0) With tours between 1966â1970 34 1.7 (1.2â2.3) White AFHS comparison veterans Mortalityâall 3 0.8 (0.2â2.1) Incidenceâall 54 1.6 (1.2â2.1) With tours between 1966â1970 42 1.6 (1.2â2.2) White AFHS subjectsâincidence Who spent at most 2 years in SEA Per unit increase of âloge(TCDD) in pg/g 28 1.5 (0.9â2.4) Comparison group 7 1.0 Ranch Hand 10 TCDD pg/g in 1987 10 1.5 (0.5â4.4) 118.5 TCDD pg/g at end of service 6 2.2 (0.7â6.9) 118.5 TCDD pg/g at end of service 5 6.0 (1.4â24.6) Only Ranch Hands with 100% service in Vietnam and comparisons with 0% service in Vietnam Per unit increase of âloge(TCDD) in pg/g 20 1.1 (0.6â1.8) Comparison group 3 1.0 Ranch Hand 10 TCDD pg/g in 1987 9 2.5 (0.4â16.1) 118.5 TCDD pg/g at end of service 4 2.4 (0.4â16.0) 118.5 TCDD pg/g at end of service 4 4.7 (0.8â29.1) Giri et al., 2004 Veterans using the DVA Medical Center in Ann Arbor, MI All cases 11 OR 2.1 (0.8â5.2) Cases in white veterans only * OR 2.7 (0.9â8.2) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 26 0.7 (0.4â1.3) AIHW, 1999 Australian Vietnam veterans (validation 212 147 expected study) (123â171) CDVA, 1998a Australian Vietnam veterans 428e 147 expected (123â171)
CANCER 397 TABLE 6-30 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Studies Reviewed in Update 1998 Clapp, 1997 Massachusetts Vietnam veteransâincidence Exposed cancers 15 0.8 (0.4â1.6) CDVA, 1997a Australian military Vietnam veterans 36 1.5 (1.0â2.0) AFHS, 1996 Air Force Ranch Hand veterans 2 0.6 expected Watanabe and Kang, 1996 US Army and Marine Corps Vietnam veterans Army Vietnam Service 58 1.1* Non-Vietnam 1.0 1.2*f Marine Vietnam Service 9 1.2* Non-Vietnam 6 1.3* Studies Reviewed in Update 1996 Visintainer et al., 1995 Michigan Vietnam veterans Male genital systemâall races 19 1.1 (0.6â1.7) Studies Reviewed in VAO Breslin et al., 1988 Army Vietnam veterans 30 0.9 (0.6â1.2) Marine Vietnam veterans 5 1.3 (0.2â10.3) Anderson et al., 1986b Wisconsin Vietnam veterans 0 â ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; AIHW, Australian Institute of Health and Welfare; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; DVA, Department of Veterans Affairs; IARC, International Agency for Research on Cancer; MCPA, methyl-4-chloro- phenoxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; OR, odds ratio; RH, Ranch Hand; SEA, Southeast Asia; USDA, US Department of Agriculture. a Given when available. b 90% CI. c 99% CI. d The original paper implied that the exposure metric for TCDD was based on actual measured serum levels of TCDD. Subsequent correspondence between the committee and the investigators indicated that the metric was actually transformed using the natural logarithm of TCDD. e Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have prostate cancer?â f Statistically signiï¬cant with the 95% CI not including 1.0. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts.
398 VETERANS AND AGENT ORANGE: UPDATE 2006 speciï¬city of each study must be considered in the interpretation and weighing of evidence. Because of study heterogeneity, simply examining all the estimated risks in the table together will not yield a good assessment of the risks. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers with exposure to nonvolatile organochlorine compounds potentially contaminated with TCDD. On the basis of a JEM, the SMR of prostate cancer among men who were ever exposed to nonvolatile or- ganochlorine compounds was not increased (SMR 0.93, 95% CI 0.74â1.15). Alavanja et al. (2005) updated their prostate-cancer incidence data on a cohort of private and commercial pesticide applicators who were participants in the AHS. The incidence of prostate cancer was signiï¬cantly increased in the private applicators, who were mostly farmers (SIR 1.26, 95% CI 1.18â1.33) and increased with borderline signiï¬cance in the commercial applicators (SIR 1.37, 95% CI 0.98â1.86). A separate report from the AHS examined associations between cumulative exposure to speciï¬c chemicals and prostate-cancer mortality (Blair et al., 2005a). Positive associations were observed with several pesticides in applicators with a family history of prostate cancer and a signiï¬cantly increased risk in all cohort members with highest exposure to the fumigant methyl bromide. There were no associations between general herbicide exposure and prostate-cancer risk; how- ever, exposure to phenoxy herbicides or dioxin was not reported speciï¬cally. An analysis of mortality in the private applicators in the AHS cohort also appeared recently (Blair et al., 2005a). In contrast with the results on incident prostate cancer, mortality from prostate cancer was signiï¬cantly reduced in these applicators compared with the general population (SMR 0.7, 95% CI 0.5â0.8). The relation between exposure to groups of chemicals and mortality was not reported, and the number of deaths available in the AHS for such an analysis is small. Possible explanations of the higher incidence of and lower mortality from prostate cancer in the AHS than in the general population are greater access of cohort members to early detection through PSA screening and greater adoption of aggressive treatment, although their effects on mortality from prostate cancer are not established. In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers from 1969 and 1973, respectively, through 2000. Although the exposures in this cohort are substantial and highly relevant, the number of deaths due to prostate cancer was too small to provide useful risk estimates. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide
CANCER 399 users in the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and MCPA. The esti- mated risk of prostate cancer was not increased (66 cases; SMR 0.96, 95% CI 0.74â1.22). Starting with the 19,904 men entered into the the New Zealand Cancer Reg- istry from 1980â1984 with a speciï¬ed occupation, Reif et al. (1989) contrasted the 2,435 cases of prostate cancer with the remaining subjects having other types of cancer. Of the 134 cancer registrants for whom forestry worker (with presumed exposure to phenoxy herbicides and chlorophenols) was the most recent occupa- tion, the proportion with prostate cancer (12 cases; OR 0.72, 95% CI 0.39â1.31) was not signiï¬cantly elevated. Environmental Studies No new relevant environmental studies concerning exposure to the com- pounds of interest and prostate cancer were published since Update 2004. Vietnam-Veteran Studies Two reports on prostate-cancer risk in the AFHS were published since Up- date 2004. A recent publication from Pavuk et al. (2006) focuses solely on pros- tate cancer in contrast with earlier analyses (Akhtar et al., 2004; Pavuk et al., 2005) and uses information on serum TCDD concentration and years of service in Southeast Asia in both the Ranch Hand and comparison subcohorts. They found no increase in prostate cancer in the Ranch Hand veterans compared with the comparison cohort and no overall association between cumulative serum TCDD and prostate-cancer risk in the Ranch Hand group. In contrast with the compari- son veterans, Ranch Hand veterans had no evidence of higher prostate-cancer risk with longer Southeast Asia service. However, more detailed results showed that prostate-cancer risk was signiï¬cantly higher in Ranch Hand veterans who had high TCDD and served in Southeast Asia for less than 2 years, or before 1969, than in the control subcohort of Air Force veterans. The authors postulate that those results could be explained by a low risk in comparison veterans who had shorter and earlier service, but further analyses to test this were not presented. Dioxin exposure was presumed to be higher in the Ranch Hand veterans before 1969, and combining this characteristic with serum TCDD concentration might provide more accurate classiï¬cation of men with truly high exposure and thus reveal an association if one exists. Additional analyses, with different referent groups and simultaneous adjustment for timing and duration of service and serum TCDD, would be helpful, but the data available so far are probably too sparse to provide ï¬nely detailed risk estimates. In a slightly earlier article (Pavuk et al., 2005), prostate cancer was among the cancers whose incidences were analyzed only in the comparison group in the
400 VETERANS AND AGENT ORANGE: UPDATE 2006 Ranch Hand studyâa group presumably not directly exposed to Agent Orange. The authors found a signiï¬cant increase in prostate-cancer risk in relation to length of service in Southeast Asia, but not to serum TCDD concentration. Those in the highest quartile of length of Southeast Asia service (3.7â16.4 years) had more than twice the risk (RR 2.4, 95% CI 1.1â5.2) of those in the lowest quartile (0.8â1.3 years). There was evidence of a signiï¬cant interaction between serum TCDD and years of Southeast Asia service in cancer risk at all sites; however, no such interaction was observed speciï¬cally in prostate cancer. Serum TCDD concentrations in this cohort, which was not directly exposed to Agent Orange, were considerably lower than those in the Ranch Hand veterans; moreover, there was no association between serum TCDD and years served in Southeast Asia. An even earlier study of both the Ranch Hand and AFHS comparison veter- ans (Akhtar et al., 2004), discussed in Update 2004, had reported that prostate- cancer risk in both groups was higher than that in the general US white population (SIR 1.62 and 1.46, respectively). The differences between the results of that study and the more recent analyses by Pavuk et al. (2005, 2006) are most likely explained by a higher prostate-cancer risk among all veterans who served in Southeast Asia than in the general population; that conclusion would be supported by the observation that prostate-cancer risk in men in the AHFS comparison group, who were not knowingly exposed to herbicides, appeared to increase as length of service in Southeast Asia increased (Pavuk et al., 2005). In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported one prostate-cancer death in the deployed and three in the non-deployed. They did not consider the data sufï¬cient for the calculation of risk estimates un- less there were at least 10 deaths from a given type of cancer. In a set of three reports updating the health status of Australian Vietnam veter- ans, results were reported concerning a possible association between Vietnam ser- vice and prostate-cancer risk. The ï¬rst report, on cancer incidence, identiï¬ed 692 prostate cancers in Vietnam veteransâfor a small but signiï¬cant increase in inci- dence compared with that in the general Australian male population (SIR = 1.25, 95% CI 1.16â1.34) (ADVA, 2005a). The second, on mortality (ADVA, 2005b), included 107 deaths due to prostate cancer, and mortality was similarly increased (SMR 1.23, 95% CI 0.99â1.46). Incidence and mortality were increased by about the same degree in veterans who served in the Navy, Army, and Air Force, so a generalized exposure or risk factor might have been responsible. To deal with the possibility of a healthy-worker effect in the Australian veterans, a third report compared men deployed to Vietnam with a National Service cohort that was not deployed (ADVA, 2005c). The results indicate that the incidence of prostate cancer was similar in the deployed and non-deployed groups; there were too few deaths due to prostate cancer to permit stable risk estimates. Leavy et al. (2006) reported the results of a caseâcontrol study that included 606 people with prostate cancer and 471 controls in Western Australia. A self- report of having served in Vietnam was associated with a non-signiï¬cant increase
CANCER 401 in risk (OR 2.12, 95% CI 0.88â5.06). The low prevalence of reported service in Vietnam (1.6% of controls) resulted in low statistical power of this analysis. Biologic Plausibility Prostate cells and prostatic-cancer cell lines are responsive to TCDD in induc- tion of various genes, including those involved in drug metabolism. Simanainen et al. (2004b) used different rat lines (TCDD-resistant Hans/Wistar and TCDD- sensitive Long Evans) and showed that TCDD treatment resulted in a signiï¬cant decrease in the weight of prostate lobes; however, the effect did not appear to be line-speciï¬c. In contrast, the TCDD reduction in sperm does appear to be line-speciï¬c and not fully related to the effects of TCDD on serum testosterone (Simanainen et al., 2004a). TCDD effects appear to occur through actions on the urogenital sinus (Lin et al., 2004). In utero and lactational exposure to TCDD appears to retard the aging process in the prostate (Fritz et al., 2005). The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Studies reported since the last update, which are based on occupational cohorts and Vietnam veterans, continue to be limited by nonspeciï¬c exposure information, low statistical power, or both. The increased incidence of prostate cancer in chemical applicators in the AHS is of considerable interest and could yield more relevant risk estimates in the future if the number of men with expo- sures to the compounds of interest is large enough. Updated analyses from the AFHS conï¬rm an association between length of service in Southeast Asia and prostate-cancer incidence in the comparison subcohort. The association appears to be unrelated to serum TCDD concentration and suggests that other factors related to service in Southeast Asia could be responsible. Prostate-cancer risk was not related to serum TCDD in the Ranch Hand veterans either, and subgroup analyses, which suggest increased risk in the men with both higher TCDD and earlier or shorter service in Southeast Asia, cannot now be clearly interpreted. Although the associations are not large, several studies provide evidence of a small increase in morbidity or mortality due to prostate cancer. The evidence regarding association is drawn from occupational studies in which subjects were exposed to a variety of pesticides, herbicides, and herbicide components and from studies of Vietnam veterans. Since Update 2004, however, new evidence has emerged that service in Vietnam itself may be associated with a higher risk of prostate cancer. Although the explanations for that are unclear, the possibility needs to be taken into account in interpreting studies that bear on the relationship of Agent Orange exposure to prostate cancer.
402 VETERANS AND AGENT ORANGE: UPDATE 2006 Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is limited or suggestive evidence of an association between exposure to at least one of the compounds of interest and prostate cancer. TESTICULAR CANCER ACS estimated that 8,250 men would receive diagnoses of testicular cancer (ICD-9 186.0â186.9) in the United States in 2006 and that 370 men would die from it (Jemal et al., 2006). Other cancers of the male reproductive system that are infrequently reported separately are cancers of the penis and other male genital organs (ICD-9 187). The average annual incidence of testicular cancer is shown in Table 6-31. Testicular cancer occurs more often in men younger than 40 years old than in older men. On a lifetime basis, the risk in white men is about 4 times that in black men. Cryptorchidism (undescended testes) is a major risk factor for testicu- lar cancer. Family history of the disease also appears to be a risk factor. Several other hereditary, medical, and environmental risk factors have been suggested, but the results of research are inconsistent (Bosl and Motzer, 1997). Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between ex- posure to the compounds of interest and testicular cancer. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-32 summarizes the results of the relevant studies. TABLE 6-31 Average Annual Incidence (per 100,000) of Testicular Cancer in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black 3.8 4.4 1.2 2.0 2.2 1.8 1.6 1.7 1.0 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
CANCER 403 TABLE 6-32 Selected Epidemiologic StudiesâTesticular Cancer Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 2 1.1 (0.1â4.1) Ever 5 3.6 (1.2â8.4) Alavanja et al., 2005 US Agriculture Health Studyâincidence Private applicators (men and women) 23 1.1 (0.7â1.6) Spouses of private applicators ( 99% women) â 0.0 (0.0â50.2) Commercial applicators (men and women) 4 1.2 (0.3â3.2) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 0 â* Spouses of private applicators ( 99% women) 0 â* Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 6 1.0 (0.4â2.6) Studies Reviewed in Update 2002 Burns et al., 2001 Dow chemical production workers 1 2.2 (0.0â12.5) Studies Reviewed in Update 2000 Fleming et al., 1999b Florida pesticide appliers 23 2.5 (1.6â3.7) Hardell et al., 1998 Swedish workers exposed to herbicides 4 0.3 (0.1â1.0) Studies Reviewed in Update 1998 Hertzman et al., 1997 British Columbia sawmill workers Mortality 116b 1.0 (0.8â1.1) Incidence 18 1.0 (0.6â1.4) Kogevinas et al., 1997 IARC cohort 7 1.3 (0.5â2.7) Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0 â* Zhong and Rafnsson, Icelandic pesticide users 2 1.2 (0.1â4.3) 1996 Studies Reviewed in Update 1996 Blair et al., 1993 US farmers in 23 states White men 32 0.8 (0.6â1.2) Nonwhite men 6 1.3 (0.5â2.9) Studies Reviewed in VAO Ronco et al., 1992 Danish workersâincidence Menâself-employed 74 0.9 (*) employee 23 0.6 (p 0.05) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 7 2.3 (0.9â4.6) continued
404 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-32 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 1 4.6 (0.0â25.7) Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 4 2.2 (0.6â5.7) Wiklund, 1983 Swedish male and female agricultural workersâincidence 101 1.0 (0.7â1.2)c ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zone A, Bâmen 17 1.0 (0.6â1.7) Bertazzi et al., 1998 Seveso residentsâ15-year follow-up (genitourinary tract) Zone Bâmen 10 1.0 (0.5â1.8) Zone Râmen 73 1.0 (0.8â1.3) Studies Reviewed in Update 1996 Bertazzi et al., 1993 Seveso residentsâ10-year follow-upâincidence Zone Bâmen 1 1.0 (0.1â7.5) Zone Râmen 9 1.4 (0.7â3.0) Studies Reviewed in VAO Pesatori et al., 1992 Seveso residentsâincidence Zones A, Bâmen 1 0.9 (0.1â6.7) Zone Râmen 9 1.5 (0.7â3.0) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 54 0.9 (0.6â1.1) Navy 17 1.2 (0.7â1.8) Army 34 0.8 (0.5â1.0) Air Force 3 0.8 (0.2â2.3) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 14 0.9 (0.4â1.4) Navy 3 0.8 (0.2â2.4) Army 10 0.9 (0.4â1.7) Air Force 0 0.0 (0.0â3.3) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veteransâdeployed vs non-deployed Incidence 17 0.7 (0.4â1.2) Mortality 4 0.8 (0.2â2.0) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 3 â* AIHW, 1999 Australian Vietnam veterans 59 110 expected (89â139)
CANCER 405 TABLE 6-32 Continued Estimated Exposed Relative Risk Reference Study Population Casesa (95% CI)a CDVA, 1998a Australian Vietnam veterans 151d 110 expected (89â131) Studies Reviewed in Update 1998 Clapp, 1997 Massachusetts Vietnam veteransâincidence 30 1.2 (0.4â3.3) CDVA, 1997a Australian military Vietnam veterans 4 (NS) CDVA, 1997b Australian National Service Vietnam veterans 1 1.3 Dalager and Kang, Army Chemical Corps veterans 2 4.0 (0.5â14.5) 1997 Watanabe and Kang, Army Vietnam service 114 1.1* 1996 MarineVietnam service 28 1.0* Studies Reviewed in Update 1996 Bullman et al., 1994 Navy veterans 12 2.6 (1.1â6.2) Studies Reviewed in VAO Tarone et al., 1991 Patients at three Washington, DC, area hospitals 31 2.3 (1.0â5.5) Watanabe et al., 1991 Army Vietnam veterans 109 1.2 (NS) Marine Vietnam veterans 28 0.8 (NS) Breslin et al., 1988 Army Vietnam veterans 90 1.1 (0.8â1.5) Marine Vietnam veterans 26 1.3 (0.5â3.6) Anderson et al., 1986 Wisconsin Vietnam veterans 9 1.0 (0.5â1.9) ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; AIHW, Australian Institute of Health and Welfare; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, methyl-4-chlorophenoxyacetic acid; NS, not signiï¬cant. a Given when available. b Male genital cancers. c 99% CI. d Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have cancer of the testis?â * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts. Update of the Epidemiologic Literature Occupational Studies In the study by McLean et al. (2006) of mortality in a multinational IARC cohort of 60,468 pulp and paper industry workers, testicular cancer was not con- sidered separately; however, deaths attributed to all male genital cancers were increased among men who were ever exposed to nonvolatile organochlorine com- pounds potentially contaminated with TCDD. On the basis of only ï¬ve deaths, the SMR was 3.60 (95% CI 1.17â8.40).
406 VETERANS AND AGENT ORANGE: UPDATE 2006 Alavanja et al. (2005) found no evidence of a signiï¬cant increase in testicular- cancer risk in the AHS cohorts of private pesticide applicators (SIR 1.05, 95% CI 0.67â1.58) and commercial applicators (SIR 1.24, 95% CI 0.33â3.17). After investigating the mortality experience of those cohorts, Blair et al. (2005a) reported no deaths from testicular cancer. Starting with the 19,904 men entered into the the New Zealand Cancer Reg- istry from 1980â1984 with a speciï¬ed occupation, Reif et al. (1989) contrasted the 399 cases of testicular cancer with the remaining subjects having other types of cancer. Of the 134 cancer registrants for whom forestry worker (with presumed exposure to phenoxy herbicides and chlorophenols) was the most recent occupa- tion, the proportion with testicular cancer was not elevated (6 cases; OR 0.99, 95% CI 0.38â2.61). Environmental Studies No new environmental studies concerning exposure to the compounds of interest and testicular cancer were published since Update 2004. Vietnam-Veteran Studies A set of three reports updating the health status of Australian Vietnam veter- ans reported results on a possible association between Vietnam service and tes- ticular cancer. The risk of testicular cancer in the veterans was non-signiï¬cantly reduced compared with that in the general population (SMR 0.87, 95% CI 0.63â1.10) (ADVA, 2005a), as was mortality (SMR 0.85, 95% CI 0.43â1.39) (ADVA, 2005b). The possibility of a healthy-warrior effect was investigated in a separate study that compared the rates of testicular cancer in deployed and non- deployed Vietnam veterans (ADVA, 2005c). Again, based on relatively few cases, the risks for both incidence of and mortality from testicular cancer were slightly lower in the deployed. Biologic Plausibility No animal studies have reported an increased incidence of testicular cancer after exposure to the compounds of interest. The biologic plausibility of the car- cinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis The evidence from epidemiologic studies is inadequate to link herbicide exposure and testicular cancer. The relative rarity of this cancer makes it difï¬cult to develop risk estimates with any precision. Most cases occur in men 25â35
CANCER 407 years old, and men who have received such a diagnosis could be excluded from military service; this could explain the slight reduction in risk observed in some veteran studies. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and testicular cancer. BLADDER CANCER Bladder cancer (ICD-9 188) is the most common urinary tract cancer. Can- cers of the urethra, paraurethral glands, and other and unspeciï¬ed urinary cancers (ICD-9 189.3â189.9) are infrequently reported separately; any ï¬ndings on these cancers would be reported in this section. ACS estimated that 44,690 men and 16,730 women would receive a diagnosis of bladder cancer in the United States in 2006 and that 8,990 men and 4,070 women would die from it (Jemal et al., 2006). In men, in whom this cancer is about twice as common as it is in women, those numbers represent about 6 percent of new cancer diagnoses and 3 percent of cancer deaths. Overall, bladder cancer is fourth in incidence among men in the United States. Bladder-cancer risk rises rapidly with age. In men in the age groups that characterize most Vietnam veterans, bladder-cancer incidence is about twice as high in whites as in blacks. The average annual incidence of urinary bladder cancer is shown in Table 6-33. The most important known risk factor for bladder cancer is tobacco use, which accounts for about half the bladder cancers in men and one-third of them in women (Miller et al., 1996). Occupational exposure to aromatic amines (also TABLE 6-33 Average Annual Incidence (per 100,000) of Bladder Cancer in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 24.0 26.2 15.7 48.0 53.1 30.1 84.2 93.7 45.5 Women 7.4 8.4 4.7 14.0 15.8 8.9 23.5 26.7 14.5 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
408 VETERANS AND AGENT ORANGE: UPDATE 2006 called arylamines), polycyclic aromatic hydrocarbons, and some other organic compounds used in the rubber, leather, textile, paint-products, and printing in- dustries is associated with higher incidence. In some parts of Africa and Asia, infection with the parasite Schistosoma hæmatobium contributes to the high incidence. Exposure to inorganic arsenic is also a risk factor for bladder cancer. Al- though cacodylic acid is a metabolite of inorganic arsenic as discussed in Chapter 3, the data are insufï¬cient to conclude that studies of inorganic-arsenic exposure are directly relevant to exposure to cacodylic acid, so the literature on inorganic arsenic is not considered in this section. Conclusions from VAO and Updates The committees responsible for VAO and Update 1996 concluded that there was limited or suggestive evidence of no association between exposure to the compounds of interest and urinary bladder cancer. Additional information avail- able to the committee responsible for Update 1998 led it to change that conclu- sion to one of inadequate or insufï¬cient information to determine whether there is an association. The Update 2000, Update 2002, and Update 2004 committees did not change that conclusion. Table 6-34 summarizes the results of the relevant studies. Update of Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers exposed to nonvolatile organochlorines poten- tially contaminated with TCDD. No excess in mortality due to bladder cancer was observed in men who were ever exposed to nonvolatile organochlorines in this cohort (SMR 1.09, 95% CI 0.79â1.46). In the report by Alavanja et al. (2005) on cancer incidence in the AHS pro- spective cohorts of private pesticide applicators, commercial applicators, and the spouses of the private farmer applicators, statistics are presented for âurinary sys- tem cancers,â presumably including bladder and kidney cancers. The incidence of this group of cancers was signiï¬cantly lower than expected in private applicators (SIR 0.65, 95% CI 0.56â0.75), non-signiï¬cantly reduced in their spouses (SIR 0.69, 95% CI 0.40â1.11), and roughly equivalent to that in the general popula- tion in the commercial applicators (SIR 1.08, 95% CI 0.57â1.84). In a study of cancer mortality in the same prospective AHS cohorts of pes- ticide applicators and spouses in North Carolina and Iowa, Blair et al. (2005a) reported bladder cancers separately; neither group showed any indication of increased mortality from bladder cancer.
CANCER 409 TABLE 6-34 Selected Epidemiologic StudiesâBladder Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 50 1.0 (0.7â1.3) Ever 43 1.1 (0.8â1.5) Alavanja et al., US Agriculture Health Study (urinary 2005 system)âincidence Private applicators (men and women) 184 0.7 (0.6â0.8) Spouses of private applicators ( 99% women) 17 0.7 (0.4â1.1) Commercial applicators (men and women) 13 1.1 (0.6â1.8) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 7 0.4 (0.1â0.7) Spouses of private applicators ( 99% women) 2 0.8 (0.1â2.7) ât Mannetje et al., Phenoxy herbicide producers (men and women) 0 â* 2005 Phenoxy herbicide sprayers ( 99% men) 0 â* Torchio et al., 1994 Italian licensed pesticide users 31 0.5 (0.4â0.8) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 4 0.7 (0.3â1.8) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 2 0.7 (0.1â2.4) Bodner et al., 2003 Dow chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) â 0.7 (0.1â2.0) Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 1 0.5 (0.1â2.8) Studies Reviewed in Update 2000 Steenland et al., US chemical production workers (included in the 1999 IARC cohort and the NIOSH Dioxin Registry) Total cohort 16 2.0 (1.1â3.2) High-exposure cohort 6 3.0 (1.4â8.5) Hooiveld et al., Dutch chemical production workers (included in 1998 the IARC cohort) Total cohort 4 3.7 (1.0â9.5) Accidentally exposed subcohort 1 2.8 (0.1â15.5) Studies Reviewed in Update 1998 Hertzman et al., Canadian sawmill workers 1997 Mortality 33 0.9 (0.7â1.2) Incidence 94 1.0 (0.8â1.2) continued
410 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-34 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 34 1.0 (0.7â1.5) Exposed to TCDD (or higher-chlorinated dioxins) 24 1.4 (0.9â2.1) Not exposed to TCDD (or higher- chlorinated dioxins) 10 0.7 (0.3â1.2) Ott and Zober, BASF employees (bladder or kidney)âincidence 2 1.4 (0.4â3.2) 1996 Studies Reviewed in Update 1996 Asp et al., 1994 Finnish herbicide applicatorsâincidence 12 1.6 (0.8â2.8) Bueno de Mesquita Dutch phenoxy herbicide workers (included in et al., 1993 the IARC cohort) 1 1.2 (0.0â6.7) Collins et al., 1993 Monsanto Company workers (included in the IARC cohort) Bladder and other urinary 16d 6.8 (3.9â11.1) Studies Reviewed in VAO Ronco et al., 1992 Danish workersâincidence Menâself-employed 300 0.6 (p 0.05) employee 70 0.7 (p 0.05) Womenâself-employed 1 0.2 (*) employee 2 0.6 (*) family worker 25 0.6 (p 0.05) Fingerhut et al., NIOSHâentire cohort (bladder and other) 9 1.6 (0.7â3.0) 1991 1-year exposure; 20-year latency 4 1.9 (0.5â4.8) Green, 1991 Herbicide sprayers in Ontario Diseases of the genitourinary system 1 1.0 (0.0â5.6) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 13 0.8 (0.4â1.4) Zober et al., 1990 BASF employeesâbasic cohort 0 â (0.0â15.0) Alavanja et al., USDA forest or soil conservationists 8 0.8 (0.3â1.6) 1989 Henneberger et al., New Hampshire pulp and paper workers 4 1.2 (0.3â3.2) 1989 Alavanja et al., USDA agricultural extension agents 8 0.7 (0.4â1.4) 1988 Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin registry) 0 â (0â7.2) Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 8 0.9 (0.4â1.7) Robinson et al., Northwestern US paper and pulp workers 8 1.2 (0.6â2.6) 1986 Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) 11 0.8 (*) Blair et al., 1983 Florida pesticide applicators 3 1.6 (*) Burmeister, 1981 Iowa farmers 274 0.9 (NS)
CANCER 411 TABLE 6-34 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c ENVIRONMENTAL Studies Reviewed in Update 2002 Revich et al., 2001 Residents of Chapaevsk, Russia (urinary organs) Men 31 2.6 (1.7â3.6) Women 17 0.8 (0.5â1.3) Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zone A, Bâmen 6 1.2 (0.5â2.7) Schreinemachers, Rural or farm residents of Minnesota, Montana, 2000 and North and South Dakota Menâcounties with high wheat acreage 129 0.9 (0.7â1.1) medium wheat acreage 147 0.8 (0.7â1.0) Womenâcounties with high wheat acreage 59 1.1 (0.8â1.6) medium wheat acreage 67 1.1 (0.8â1.5) Bertazzi et al., Seveso residentsâ15-year follow-up 1998 Zone Bâmen 1 2.4 (0.3â16.8) women 3 0.9 (0.3â3.0) Zone Râmen 21 0.9 (0.6â1.5) women 4 0.6 (0.2â1.8) Studies Reviewed in Update 1998 Gambini et al., Italian rice growers 12 1.0 (0.5â1.8) 1997 Svensson et al., Swedish ï¬shermenâmortality (men and women) 1995 East coast 5 1.3 (0.4â3.1) West coast 20 1.0 (0.6â1.6) Swedish ï¬shermenâincidence (men and women) East coast 10 0.7 (0.4â1.3) West coast 55 0.9 (0.7â1.1) Studies Reviewed in VAO Pesatori et al., Seveso residentsâincidence 1992 Zones A, Bâmen 10 1.6 (0.9â3.1) women 1 0.9 (0.1â6.8) Zone Râmen 39 1.0 (0.7â1.4) women 4 0.6 (0.2â1.5) Lampi et al., 1992 Finnish community exposed to chlorophenol contamination (men and women) 14 1.0 (0.6â1.9) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 164 1.0 (0.9â1.2) Navy 34 1.0 (0.7â1.4) Army 104 1.0 (0.8â1.2) Air Force 26 1.3 (0.8â1.8) continued
412 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-34 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 22 0.7 (0.4â1.0) Navy 4 0.6 (0.2â1.6) Army 13 0.7 (0.3â1.1) Air Force 5 1.1 (0.4â2.5) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 19 0.7 (0.4â1.1) Mortality 1 0.3 (0.0â1.7) Boehmer et al., Follow-up of CDC Vietnam Experience Cohort 1 â* 2004 Studies Reviewed in Update 2004 Akhtar et al., 2004 AFHS subjects vs national rates White AFHS Ranch Hand veterans MortalityâAll 1 0.9 (*) IncidenceâAll 14 1.1 (0.6â1.7) With tours between 1966â1970 14 1.3 (0.7â2.1) White AFHS comparison veterans MortalityâAll 1 0.6 (*) IncidenceâAll 8 0.4 (0.2â0.8) With tours between 1966â1970 4 0.3 (0.1â0.7) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans Bladder and kidney 11 3.1 (0.9â11.0) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 11 1.1 (0.6â1.9) CDVA, 1997b Australian National Service Vietnam veterans 1 0.6 (*) Clapp, 1997 Massachusetts Vietnam veterans 80 0.6 (0.2â1.3) Studies Reviewed in VAO Breslin et al., 1988 Army Vietnam veterans 9 0.6 (0.3â1.2) Marine Vietnam veterans 4 2.4 (0.1â66.4) Anderson et al., Wisconsin Vietnam veterans 1 â* 1986 ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, methyl-4-chlorophenoxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; NS, not signiï¬cant; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d Many of the employees studied were also exposed to 4-aminobiphenyl, a known bladder carcinogen. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts.
CANCER 413 In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers from 1969 and 1973, respectively, through 2000. No deaths from bladder cancer (ICD-9 188) were observed in the producers or sprayers. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and MCPA. The esti- mated risk of bladder cancer was signiï¬cantly reduced (31 cases; SMR 0.54, 95% CI 0.37â0.78). The authors suggested that the relatively short duration of follow-up and the healthy-worker effect contributed to the observed reduction in mortality. Starting with the 19,904 men entered into the the New Zealand Cancer Reg- istry from 1980â1984 with a speciï¬ed occupation, Reif et al. (1989) contrasted the 912 cases of bladder cancer with the remaining subjects having other types of cancer. Of the 134 cancer registrants for whom forestry worker (with presumed exposure to phenoxy herbicides and chlorophenols) was the most recent occupa- tion, the proportion with bladder cancer (4 cases; OR 0.68, 95% CI 0.25â1.84) was not elevated. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and bladder cancer were published since Update 2004. Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported one bladder-cancer death in the deployed and two in the non-deployed. They did not consider the data sufï¬cient for the calculation of risk estimates un- less there were at least 10 deaths from cancer of a given type. A set of three reports updating the health status of Australian Vietnam veter- ans presented results concerning a possible association between Vietnam service and bladder cancer. Compared with the general population, the Australian veter- ans did not have an increased incidence (ADVA, 2005a) of bladder cancer (SIR 1.04, 95% CI 0.88â1.20), whereas mortality (ADVA, 2005b) from bladder cancer was reduced with borderline statistical signiï¬cance (SMR 0.71, 95% CI 0.42â 1.01). The possibility that that was attributable to a healthy-warrior effect was investigated in a separate study that compared rates of bladder cancer in deployed and non-deployed Vietnam veterans (ADVA, 2005c). Bladder-cancer incidence was marginally lower in deployed veterans (SIR 0.63, 95% CI 0.34â1.11); there were too few deaths from bladder cancer to permit reliable risk estimates.
414 VETERANS AND AGENT ORANGE: UPDATE 2006 Biologic Plausibility In laboratory animals, cacodylic acid has been shown to induce primarily bladder tumors (Cohen et al., 2006). In a study of male F344 rats, cacodylic acid administered in drinking water resulted in formation of bladder tumors at the highest concentrations (50 and 200 ppm) (Wei et al., 2002). In another report (Arnold et al., 2006), administration of cacodylic acid in the diet resulted in formation of papillomas and carcinomas in the bladders of both female and male F344 rats but not B6C3F1 mice. No studies have reported an increased incidence of urinary bladder cancer in TCDD-treated animals. The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Available analyses of an association between exposure to the compounds of interest and bladder-cancer risk are characterized by low precision because of the small numbers, low exposure speciï¬city, and lack of ability to control for confounding. No new data have emerged since Update 2004 to alter the conclusion that the cumulative evidence of such an association is inadequate or insufï¬cient. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and bladder cancer. RENAL CANCER Cancers of the kidney (ICD-9 189.0) and renal pelvis (ICD-9 189.1) are often grouped in epidemiologic studies; cancer of the ureter (ICD-9 189.2) is also included sometimes. Although diseases of those organs have different char- acteristics and could have different risk factors, there is some logic to grouping them: the structures are all exposed to ï¬lterable compounds, such as polycyclic aromatic hydrocarbons, that appear in urine. ACS estimated that 24,650 men and 14,240 women would receive diagnoses of renal cancer (ICD-9 189.0, 189.1) in the United States in 2006 and that 8,130 men and 4,710 women would die from it (Jemal et al., 2006). Those ï¬gures represent 2â3 percent of all new cancer diagnoses and cancer deaths. The average annual incidence of renal cancer is shown in Table 6-35.
CANCER 415 TABLE 6-35 Average Annual Incidence (per 100,000) of Kidney and Renal Pelvis Cancer in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 22.7 22.5 33.5 35.7 35.6 45.3 54.4 55.5 61.1 Women 10.9 11.1 13.2 18.3 18.9 19.6 24.5 25.2 33.1 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. Renal cancer is twice as common in men as in women. In the age groups that include most Vietnam veterans, black men have a higher incidence than white men. With the exception of Wilmsâ tumor (which is more likely to occur in chil- dren), renal cancer is more common in people over 50 years old. Tobacco use is a well-established risk factor for renal cancer. People with some rare syndromesânotably, von Hippel-Lindau syndrome and tuberous sclerosisâare at higher risk. Other potential risk factors include obesity, heavy acetaminophen use, kidney stones, and occupational exposure to asbestos, cad- mium, and organic solvents. Fireï¬ghters, who are routinely exposed to numerous pyrolysis products, are in a known higher-risk group. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and renal cancer. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-36 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers with exposure to organochlorine compounds potentially contaminated with TCDD. The SMR of kidney cancer was signiï¬- cantly lower than expected in workers who were ever exposed to nonvolatile organochlorine compounds (SMR 0.53, 95% CI 0.31â0.83). As noted above in the section on bladder cancer, Alavanja et al. (2005) pre- sented ï¬ndings on the incidence of âurinary system cancers,â presumably includ-
416 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-36 Selected Epidemiologic StudiesâRenal Cancer Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 41 0.9 (0.7â1.3) Ever 18 0.5 (0.3â0.8) ât Mannetje et al., Phenoxy herbicide producers (men and women) 1 1.2 (0.0â6.6) 2005 Phenoxy herbicide sprayers ( 99% men) 3 2.7 (0.6â8.0) Torchio et al., 1994 Italian licensed pesticide users 16 0.6 (0.4â1.0) Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 2 0.6 (0.2â2.3) Magnani et al., UK caseâcontrol 1987 Herbicides * 1.3 (0.6â3.1) Chlorophenols * 0.9 (0.4â1.9) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 4 1.3 (0.4â3.4) Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 2 0.9 (0.1â3.3) Studies Reviewed in Update 2000 Steenland et al., US chemical workers (included in the IARC 1999 cohort and the NIOSH Dioxin Registry) 13 1.6 (0.8â2.7) Hooiveld et al., Dutch chemical production workers (included in 1998 the IARC cohort) Total cohortâkidney cancer 4 4.1 (1.1â10.4) Total cohortââurinary organsâ 8 3.9 (1.7â7.6) Studies Reviewed in Update 1998 Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 29 1.1 (0.7â1.6) Exposed to TCDD (or higher-chlorinated dioxins) 26 1.6 (1.1â2.4) Not exposed to TCDD (or higher- chlorinated dioxins) 3 0.3 (0.1â0.9) Studies Reviewed in Update 1996 Mellemgaard et al., Danish Cancer Registry patients 1994 Occupational herbicide exposure among men 13 1.7 (0.7â4.3) Occupational herbicide exposure among women 3 5.7 (0.6â58.0) Blair et al., 1993 US farmers in 23 states White men 522 1.1 (1.0â1.2) White women 6 0.8 (0.3â1.7)
CANCER 417 TABLE 6-36 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in VAO Ronco et al., 1992 Danish workersâincidence Menâself-employed 141 0.6 (p 0.05) employee 18 0.4 (p 0.05) Womenâself-employed 4 0.9 (*) employee 3 1.0 (*) family worker 30 0.8 (*) Fingerhut et al., NIOSH cohortâentire cohort 8 1.4 (0.6â2.8) 1991 1-year exposure, 20-year latency 2 1.1 (0.1â3.8) Manz et al., 1991 German production workersâmen and women (Included in the IARC cohort) 3 1.6 (0.3â4.6) Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 11 1.0 (0.5â1.7) Alavanja et al., USDA forest conservationists * 1.7 (0.5â5.5) 1989 Soil conservationists * 2.4 (1.0â5.9) Henneberger et al., New Hampshire paper and pulp workers 3 1.5 (0.3â4.4) 1989 Alavanja et al., USDA agricultural extension agents * 1.7 (0.9â3.3) 1988 Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0 * (0.0â6.2) Robinson et al., 1986 Northwestern US paper and pulp workers 6 1.2 (0.5â3.0) Coggon et al., 1986 British MCPA production workers (included in the IARC cohort) 5 1.0 (0.3â2.3) Lynge, 1985 Danish production workersâincidence 3 0.6* Blair et al., 1983 Florida pesticide applicators 1 0.5* Wiklund, 1983 Swedish agricultural workers (men and women) 775 0.8 (0.7â0.9)d Burmeister, 1981 Iowa farmers 178 1.1 (NS) ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zone A, Bâmen 3 0.8 (0.3â2.6) women 3 1.8 (0.6â5.8) Schreinemachers, Rural or farm residents of Minnesota, Montana, 2000 and North and South Dakota Menâcounties with high wheat acreage 129 1.0 (0.8â1.3) medium wheat acreage 147 1.0 (0.8â1.2) Womenâcounties with high wheat acreage 90 1.1 (0.8â1.4) medium wheat acreage 85 0.9 (0.7â1.2) continued
418 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-36 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 1996 Bertazzi et al., Seveso residentsâ10-year follow-up (kidney and 1993 other urinary organs)âincidence Zone Râmen 10 0.9 (0.4â1.7) women 7 1.2 (0.5â2.7) Studies Reviewed in VAO Pesatori et al., Seveso residentsâincidence 1992 Zones A, Bâmen 0 â* women 1 1.1 (0.2â8.1) Zone Râmen 11 0.9 (0.5â1.7) women 7 1.2 (0.5â2.6) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 125 1.0 (0.8â1.2) Navy 34 1.3 (0.9â1.7) Army 77 0.9 (0.7â1.1) Air Force 14 1.1 (0.6â1.8) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 50 1.0 (0.7â1.2) Navy 12 1.1 (0.6â1.9) Army 33 0.9 (0.6â1.3) Air Force 5 0.8 (0.3â1.8) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veteransâdeployed vs non-deployed Incidence 19 0.7 (0.4â1.0) Mortality 4 0.4 (0.1â1.1) Boehmer et al., Follow-up of CDC Vietnam Experience Cohort 1 â* 2004 Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 11 3.1 (0.9â11.0) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 22 1.2 (0.7â1.8) CDVA, 1997b Australian National Service Vietnam veterans 3 3.9 (*) Studies Reviewed in Update 1996 Visintainer et al., Michigan Vietnam veterans 21 1.4 (0.9â2.2) 1995 Studies Reviewed in VAO Breslin et al., 1988 Army Vietnam veterans 55 0.9 (0.5â1.5) Marine Vietnam veterans 13 0.9 (0.5â1.5) Kogan and Clapp, Massachusetts Vietnam veterans 9 1.8 (1.0â3.5) 1988
CANCER 419 TABLE 6-36 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Anderson et al., Wisconsin Vietnam veterans 2 â* 1986 ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, methyl-4-chlorophenoxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; NS, not signiï¬cant; SMR, standardized mortality ratio; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d 99% CI. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts. ing both bladder and kidney cancers, in the AHS cohorts. The incidence of that group of cancers was signiï¬cantly lower than expected in private applicators but not different from expected in their spouses or commercial pesticide applicators. In the companion mortality study, Blair et al. (2005a) reported ï¬ndings only on bladder cancers. In the mortality study of phenoxy herbicide producers and sprayers in New Zealand (ât Mannetje et al., 2005), the risk of renal cancer (ICD-9 189) could not be reliably estimated, because there were too few cases. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and MCPA. The esti- mated risk of kidney cancer was not increased (16 cases; SMR 0.63, 95% CI 0.36â1.02). Starting with the 19,904 men entered into the the New Zealand Cancer Reg- istry from 1980â1984 with a speciï¬ed occupation, Reif et al. (1989) contrasted the 542 cases of kidney cancer with the remaining subjects having other types of cancer. Of the 134 cancer registrants for whom forestry worker (with presumed exposure to phenoxy herbicides and chlorophenols) was the most recent occupa- tion, the proportion with kidney cancer (2 cases; OR 0.58, 95% CI 0.15â2.30) was not elevated.
420 VETERANS AND AGENT ORANGE: UPDATE 2006 Magnani et al. (1987) reported a caseâcontrol mortality study of 147 people with kidney cancer and 556 controls in the United Kingdom. A JEM was used to predict exposures to various chemical agents on the basis of job title as indicated on death certiï¬cates. The estimated risks of kidney cancer associated with expo- sure to herbicides (RR 1.3, 95% CI 0.6â3.1) and chlorophenols (RR 0.9, 95% CI 0.4â1.9) were not signiï¬cantly increased. Environmental Studies No new studies concerning exposure to the compounds of interest and renal cancer were published since Update 2004. Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported one renal-cancer death in the deployed and eight in the non-deployed. They did not consider the data sufï¬cient for the calculation of risk estimates un- less there were at least 10 deaths from cancer of a given type. A set of three reports updated the health status of Australian Vietnam veter- ans presented results concerning a possible association between Vietnam service and renal cancer. The risk of renal cancer in the veterans was not given numeri- cally but in graphs and appeared to be close to that in the general population of Australia (ADVA, 2005a); mortality results were similar (ADVA, 2005b). The possibility that those results were attributable to a healthy-warrior effect was investigated in a separate study that compared rates of renal cancer in deployed and non-deployed Vietnam veterans (ADVA, 2005c); the incidence was somewhat lower in deployed veterans (SIR 0.59, 95% CI 0.32â1.04), and there were too few renal-cancer deaths to permit reliable analysis. Biologic Plausibility No animal studies have reported an increased incidence of renal cancer after exposure to the compounds of interest. The biologic plausibility of the carcino- genicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Available analyses of an association between exposure to the compounds of interest and renal-cancer risk are limited by the small number of cases and lack of exposure speciï¬city. No new data have emerged since Update 2004 to alter that committeeâs conclusion that the evidence is inadequate or insufï¬cient to determine whether there is an association.
CANCER 421 Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and renal cancer. CANCERS OF THE EYE AND ORBIT ACS estimated that 1,230 men and 1,130 women would receive diagnoses of eye cancers (ICD-9 190) in the United States in 2006 and that 110 men and 120 women would die from it (Jemal et al., 2006). Conclusions from VAO and Updates In response to VAâs request that the present committee scan the literature considered by previous VAO committees for overlooked rare cancers, retroac- tive consideration has been given to ocular cancer in this update. In the course of this review, it was noted that eye cancers are often grouped with brain cancers. The few results reported speciï¬cally on cancers of the eye are discussed below, and their ï¬ndings incorporated into Table 6-38, which contains the cumulative results on brain cancer. Future updates will include eye and orbit cancer with brain cancer. Update of the Epidemiologic Literature Occupational Studies Wiklund (1983) found 93 cases of eye cancer diagnosed in 1961â1973 in people who declared themselves to be agricultural workers in the Swedish census. The SIR was 1.13 (95% CI 0.85â1.47), 1.14 in men. In a mortality study of 878 Dow chemical workers potentially exposed to 2,4-D in 1945â1983, Bond et al. (1988) noted that there were no cases of eye cancer, whereas 0.2 case was expected. In a mortality study of workers with pos- sible pentachlorophenol exposure followed from 1940 to 1989, Ramlow et al. (1996) reported that no cases of eye cancer were observed, but less than 0.1 case was expected. Ronco et al. (1992) observed 19 cases of eye cancer in people self-employed as farmers in the Danish census (SIR 0.91) and 6 in farming employees (SIR 1.34). Neither result was statistically signiï¬cant. No deaths from eye cancer were reported in their similar cancer-mortality study in Italy. Blair et al. (1993) used death-certiï¬cate information on farmers in 23 states in 1984â1988. There were 17 cases of eye cancer in white men and none in any
422 VETERANS AND AGENT ORANGE: UPDATE 2006 other group. The PMR for eye cancer in white men was 1.58 (95% CI 0.92â2.52). High exposure to sunlight generically associated with farming may be a con- founding factor. The report by Alavanja et al. (2005) on cancer incidence in the AHS pro- spective cohorts of private pesticide applicators, commercial applicators, and the spouses of the private applicators does not mention eye cancers except for their possible inclusion in âbrain and central nervous system cancers,â In the compan- ion study on cancer mortality in the same prospective AHS cohorts of applicators and their spouses, Blair et al. (2005a) report two deaths from eye cancer in the private applicators (SMR 2.1, 95% CI 0.2â7.6) and one eye-cancer death in their spouses (SMR 3.7, 95% CI 0.1â20). In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers through 2000. No deaths from eye cancer were observed in either group. Environmental Studies Schreinemachers (2000) carried out a study in Minnesota, North Dakota, South Dakota, and Montana in which acreage under wheat was used as a surrogate for exposure to chlorophenoxy herbicides; the rationale was that in these states more than 90 percent of spring wheat and 30 percent of winter wheat was treated with these herbicides. Cancer mortality was examined during 1980â1999 for selected counties characterized by extent of agriculture and percentage of population that was rural. For eye cancers, the counties were divided into two groups of relatively high or low wheat acreage because of the small number of cases involved. In men, 15 cases were observed, for an SMR of 1.95 (95% CI 0.69â5.47). In women, 18 cases were observed, for an SMR of 2.77 (95% CI 1.00â7.63), which was of bor- derline signiï¬cance. Vietnam-Veteran Studies Cancer Incidence in Australian Vietnam Veterans (ADVA, 2005a) reported 27 cases of eye cancer (SIR 1.75, 95% CI 1.09â2.41); veterans of unknown status were excluded. When results were broken down by branch of service, the Navy Vietnam veterans experienced an SIR that was described as âsubstan- tially lower than expectedââ0.60 (95% CI 0.07â2.16). In Army veterans, there were 21 cases, for an SIR of 1.99 (95% CI 1.14â2.84). The Air Force veterans experienced 4 cases, giving an SIR of 2.61 (95% CI 0.71â6.69). In deriving all those results, veterans of unknown status were excluded. Similar SIRs were seen when the researchers included the two observed cases of eye cancer in veterans of unknown status in their calculations. The report speciï¬es that most of the eye cancers were melanomas. Increased exposure to ultraviolet radiation in sunlight is postulated as a likely cause of the increased risk of eye melanomas.
CANCER 423 The Third Australian Vietnam Veterans Mortality Study 2005 (ADVA, 2005b) extended the 1997 mortality study of Australian servicemen with follow-up to the end of 2001. Mortality is compared through the SMR statistic with the expected number of deaths among male Australians of the same age during the relevant period. In Army Vietnam veterans, there were ï¬ve cases of eye cancer, which led to a statistically signiï¬cant SMR of 3.43 (95% CI 1.09â7.85). An analysis was also carried out to investigate eye-cancer mortality. The SMR was signiï¬- cantly increased in 1980â1990 on the basis of three observed cases (5.40, 95% CI 1.10â15.5). In 1963â1979 and 1991â2001, the SMRs were not signiï¬cantly increased on the basis of one and two cases, respectively. Australian National Service Vietnam Veterans: Mortality and Cancer In- cidence 2005 (ADVA, 2005c) compared National Service veterans and non- veterans. There were 11 cases observed in the deployed versus eight expected, and eight in the non-deployed versus 11 expected. The RR of eye cancer in deployed compared with non-deployed was 1.85 (95% CI 0.68â5.29). Synthesis Most of the epidemiologic studies of ï¬ndings on eye cancer alone reported few or no cases, were of low power, and had statistically non-signiï¬cant results. The studies with the largest numbers of cases (for example, Schreinemachers, 2000; Wiklund, 1983) did not indicate signiï¬cant increases in risk associated with herbicide exposure. Some analyses of the Australian Vietnam veterans showed excess risk, but it was probably due to excess exposure to UV radiation, which was not adjusted for. It should be noted that eye cancer is sometimes reported in a combined category with brain cancers. Conclusion The sparse data on the occurrence of eye cancer separately constitute inad- equate or insufï¬cient evidence to determine whether there is an association be- tween exposure to the compounds of interest and eye cancer. Any future ï¬ndings for this cancer site will be tracked with results on brain cancer. BRAIN CANCER âBrain and other nervous system cancersâ (ICD-9 191â192) involve the cen- tral nervous system (CNS) and include tumors of the brain and spinal cord, the cranial nerves, and the meninges (the outer covering of the brain and spinal cord). Any of the cell types in the CNS can produce cancer. Tumors of the peripheral nerves and autonomic nervous system are considered âsoft-tissueâ tumors (ICD-9 171). Most cancers in the CNS originate in other parts of the body, such as the
424 VETERANS AND AGENT ORANGE: UPDATE 2006 lung or breast, but have metastasized to the brain or spinal cord. This section focuses on cancers that originate in the CNS. In addressing VAâs request that gaps in the full array of cancer ICD codes present in the conclusions of prior updates be ï¬lled, it was noted that cancer of the eye (ICD-9 190), when reported, is often grouped with brain cancer. Cancer of the eye is considered retrospectively in the previous section; in future updates, ï¬nd- ings concerning cancer of the eye will be tracked with results on brain cancer. The average annual incidence of CNS cancer is shown in Table 6-37. About 95 percent of cases derive from brain, cranial nerves, and cranial meninges. In adults over 45 years old, about 90 percent of tumors that originate in the brain are gliomasâastrocytoma, ependymoma, oligodendroglioma, or glioblastoma multiforme. Astrocytoma is the most common; glioblastoma multiforme has the worst prognosis. Meningioma accounts for 20â40 percent of CNS cancers. It tends to occur in middle age and more commonly in women. Most meningiomas are benign and can be removed surgically. ACS estimated that about 10,730 men and 8,090 women would receive diagnoses of brain and other nervous system cancers in the United States in 2006 and that 7,260 men and 5,560 women would die from them (Jemal et al., 2006). Those numbers represent about 1.3 percent of new cancer diagnoses and 2.3 percent of cancer deaths. In reviewing the descriptive epidemiology of these cancers, it is important to recognize the variation in which speciï¬c cancers are included in published reports, often distinguished by a focus on benign or malignant cancers. Another variation is whether cancer from related tissues (such as the pituitary and the eye) is included. Various types of cancer are usually grouped; although this may bias results in unpredictable ways, the most likely consequence is dilution of risk estimates toward the null. The only well-established environmental risk factor for brain tumors is ex- posure to high doses of ionizing radiation (ACS, 2007d; Wrensch et al., 2002). Other environmental exposuresâsuch as to vinyl chloride, petroleum products, and electromagnetic ï¬eldsâare unproved as risk factors. The causes of most cancers of the brain and nervous system are not known. TABLE 6-37 Average Annual Incidence (per 100,000) of Brain and Other Nervous System Cancers in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 9.2 10.1 4.8 12.7 14.0 8.9 17.5 19.7 8.5 Women 6.4 7.3 3.5 8.8 9.3 7.1 9.8 11.1 4.0 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003.
CANCER 425 Conclusions from VAO and Updates The committee responsible for VAO concluded that there was limited or sug- gestive evidence of no association between exposure to the compounds of interest and brain cancer. The committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-38 summarizes the results of the relevant studies. Update of Epidemiologic Literature Occupational Studies Several additional studies concerning a possible association between occupa- tional exposure to the compounds of interest and brain cancer have come to the attention of the committee. Some were published before Update 2004 but were not reviewed previously. McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. The SMR of brain cancer was not associated with a JEM-based estimate of exposure to nonvolatile organochlorine compounds (never exposed: 44 cases; SMR 1.02, 95% CI 0.74â1.37; ever exposed: 28 cases; SMR 0.80, 95% CI 0.53â1.15). ât Mannetje et al. (2005) reported on the mortality experience of a New Zealand cohort of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers from 1969 and 1973, respectively, through 2000. One death from brain cancer (ICD-9 191) was observed in each group and yielded unstable risk esti- mates less than 1. Alavanja et al. (2005) reported on a cohort of agricultural pesticide appli- cators and their spouses in the AHS, using data from the brain-cancer registry of North Carolina and Iowa. Estimates of association with CNS cancer were reported for 4,916 commercial applicators (ï¬ve cases; SIR 1.85, 95% CI 0.59â 4.31), 52,395 private applicators (33 cases; SIR 0.80, 95% CI 0.55â1.12), and 32,347 spouses of private applicators (15 cases; SIR 0.90, 95% CI 0.51â1.49). The estimated risk in applicators was moderately increased, but the increase was not statistically signiï¬cant. In a corresponding mortality report from the AHS (Blair et al., 2005a), the ï¬ndings were non-signiï¬cant for private applicators (SMR 1.1, 95% CI 0.5â1.8) and their spouses (SMR 0.7, 95% CI 0.6â1.0). Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics reports as having have high herbicide use, especially of 2,4-D and MCPA. The estimated risk of CNS cancer was signiï¬cantly reduced (15 cases; SMR 0.53, 95% CI 0.3â0.9). The authors suggested that the short duration of follow-up and the healthy-worker effect contributed to the observed reduction in mortality.
426 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-38 Selected Epidemiologic StudiesâBrain Tumors Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., 2006 IARC cohort of pulp and paper workers Exposure to nonvolatile organochlorine compounds Never 44 1.0 (0.7â1.4) Ever 28 0.8 (0.5â1.2) Alavanja et al., US Agriculture Health Studyâincidence 2005 Private applicators (men and women) 33 0.8 (0.6â0.8) Spouses of private applicators ( 99% women) 15 0.9 (0.5â1.4) Commercial applicators (men and women) 5 1.9 (0.6â4.3) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 19 0.7 (0.4â1.1) Years handled pesticides 10 years 5 0.9 (* NS) 10 years 12 0.6 (* NS) Spouses of private applicators ( 99% women) 11 1.1 (0.5â1.8) Carreon et al., 2005 Women Arsenicals 13 1.0 (0.5â1.9) Phenoxy herbicides 25 0.9 (0.5â1.5) 2,4-D 24 0.9 (0.5â1.6) Lee et al., 2005 Nebraska caseâcontrol studyâincidence (gliomas) Phenoxy herbicidesâcombined reports (identical to results for 2,4-D speciï¬cally) 32 1.8 (1.0â3.3) By self 7 0.6 (0.2â1.6) By proxy 25 3.3 (1.5â7.2) 2,4,5-Tâcombined reports 7 1.3 (0.5â3.6) By self 2 0.4 (0.1â2.3) By proxy 5 2.7 (0.7â9.8) NIOSH Upper Midwest Health Studyâcaseâcontrol ât Mannetje et al., New Zealand phenoxy herbicide workers 2005 Phenoxy herbicide producers (men and women) 1 0.8 (0.0â4.6) Phenoxy herbicide sprayers ( 99% men) 1 0.6 (0.0â3.4) Ruder et al., 2004 Men Arsenicals 15 0.7 (0.4â1.4) Phenoxy herbicides 67 0.9 (0.6â1.2) 2,4-D * * Torchio et al., 1994 Italian licensed pesticide users Brain and nervous system 15 0.5 (0.3â0.9) Eye 4 2.4 (0.7â6.1) Reif et al., 1989 Caseâcontrol study on all men with occupation indicated entered into New Zealand Cancer Registry 1980â1984 (brain or CNS cancers) Forestry workers 4 1.2 (0.4â3.3)
CANCER 427 TABLE 6-38 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Magnani et al., UK caseâcontrol, JEM used on occupation given 1987 on death certiï¬cate Herbicides * 1.2 (0.7â2.1) Chlorophenols * 1.1 (0.7â1.8) Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 4 1.6 (0.4â4.1) Bodner et al., 2003 Dow chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) * 0.6 (0.1â1.8)d Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 3 1.1 (0.2â3.2) Thörn et al., 2000 Swedish lumberjacks exposed to phenoxy acetic herbicides Foremanâincidence 0 * Studies Reviewed in Update 2000 Steenland et al., US chemical workers (included in the IARC 1999 cohort and the NIOSH Dioxin Registry) 8 0.8 (0.4â1.6)d Studies Reviewed in Update 1998 Gambini et al., Italian rice growers 4 0.9 (0.2â2.3)d 1997 Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 22 0.7 (0.4â1.0) Exposed to TCDD (or higher-chlorinated dioxins) 12 0.6 (0.3â1.1) Not exposed to TCDD (or higher- chlorinated dioxins) 10 0.8 (0.4â1.5) Becher et al., 1996 German production workers (included in the IARC cohort)âcohort I 3 2.3 (0.5â6.8) Ramlow et al., 1996 Dow pentachlorophenol production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 1 *d 15-year latency 1 *d Studies Reviewed in Update 1996 Asp et al., 1994 Finnish herbicide applicators (eye and brain) Incidence 3 0.7 (0.1â2.0) Mortality 3 1.2 (0.3â3.6) Dean, 1994 Irish farmers and farm workers Men 195 â* Women 72 â* Blair et al., 1993 US farmers in 23 states White men 447 1.2 (1.1â1.3) White women 9 1.1 (0.5â2.1) continued
428 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-38 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in VAO Morrison et al., Farmers in Canadian prairie province 1992 250 acres sprayed with herbicides 24 0.8 (0.5â1.2) Ronco et al., 1992 Danish and Italian farm workers Male Danish farmersâincidence 194 1.1*d Female Danish farmersâincidence 5 1.0*d Swaen et al., 1992 Dutch licensed herbicide applicators 3 3.2 (0.6â9.3) Fingerhut et al., NIOSH cohortâentire cohort 1991 1-year exposure; 20-year latency 2 1.1 (0.1â3.8)d Saracci et al., 1991 IARC cohortâexposed subcohort (men and women) 6 0.4 (0.1â0.8) Wigle et al., 1990 Canadian farmers 96 1.0 (0.8â1.3) Alavanja et al., USDA forest or soil conservationists 6 1.7 (0.6â3.7) 1989 Henneberger et al., New Hampshire pulp and paper workers 2 1.2 (0.1â4.2) 1989 Alavanja et al., USDA agricultural extension agents * 1.0 (0.4â2.4) 1988 Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) Brain and other system tissues 0 * (0.0â4.1) Musicco et al., Brain tumor patients from Milan, Italy (male and 1988 female farmers) 61 1.6 (1.1â2.4) Coggon et al., 1986 British MCPA chemical workers (included in the IARC cohort) 11 1.2 (0.6â2.2)d Robinson et al., Northwestern US paper and pulp workers 4 0.6 (0.2â2.1) 1986 Lynge, 1985 Danish production workersâincidence (included in the IARC cohort) 4 0.7* Blair et al., 1983 Florida pesticide applicators 5 2.0* Burmeister, 1981 Iowa farmers 111 1.1 (*NS) ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., 2001 Seveso residentsâ20-year follow-up Zone A, Bâmen 1 0.4 (0.1â3.0) women 3 1.9 (0.6â6.0) Schreinemachers, Rural or farm residents of Minnesota, Montana, 2000 and North and South Dakota Menâcounties with high wheat acreage 130 1.1 (0.9â1.4)d medium wheat acreage 131 0.9 (0.8â1.2)d Womenâcounties with high wheat acreage 95 1.2 (0.9â1.5)d medium wheat acreage 94 1.0 (0.7â1.2)d
CANCER 429 TABLE 6-38 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Bertazzi et al., Seveso residentsâ15-year follow-up 1998 Zone Bâmen 1 0.8 (0.1â5.5) women 3 3.2 (1.0â10.3) Zone Râmen 12 1.3 (0.7â2.5) women 8 1.1 (0.5â2.4) Studies Reviewed in Update 1998 Svensson et al., Swedish ï¬shermenâmortality (men and women) 1995 East coast 2 0.6 (0.1â2.1) West coast 15 1.1 (0.6â1.7) Swedish ï¬shermenâincidence (men and women) East coast 3 0.5 (0.1â1.5) West coast 24 0.9 (0.6â1.4) Studies Reviewed in Update 1996 Bertazzi et al., Seveso residentsâ10-year follow-upâincidence 1993 Zone Râmen 6 0.6 (0.3â1.4) women 6 1.4 (0.6â3.4) Studies Reviewed in VAO Pesatori et al., Seveso residentsâincidence 1992 Zones A, Bâwomen 1 1.5 (0.2â11.3) Zone Râmen 6 0.6 (0.3â1.4) women 5 1.2 (0.4â3.0) Bertazzi et al., Seveso residentsâ10-year follow-up 1989a Zones A, B, Râmen 5 1.2 (0.4â3.1) women 5 2.1 (0.8â5.9) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence (brain) 97 1.1 (0.9â1.2) Navy 24 1.2 (0.7â1.7) Army 63 1.0 (0.8â1.3) Air Force 10 1.1 (0.6â2.1) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality (brain and CNS) 99 1.0 (0.8â1.1) Navy 23 1.0 (0.6â1.4) Army 66 0.9 (0.7â1.2) Air Force 9 0.9 (0.4â1.6) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veteransâdeployed vs non- deployed (brain and CNS) Incidence (1982â2000) 23 1.4 (0.7â2.6) Mortality (1966â2001) 27 1.6 (0.9â3.1) Boehmer et al., Follow-up of CDC Vietnam Experience Cohort 2004 (meninges, brain, other CNS) 9 1.2 (0.4â3.2) continued
430 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-38 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 2004 Akhtar et al., 2004 White AFHS subjects vs national rates Ranch Hand veterans Mortalityâall (CNS) 3 1.3 (0.3â3.6) Incidenceâall (brain and nervous system) 5 1.8 (0.7â4.1) With tours between 1966â1970 5 2.2 (0.8â4.8) Comparison veterans Mortalityâall (CNS) 1 0.3 (*) Incidenceâall (brain and nervous system) 2 0.5 (0.1â1.8) With tours between 1966â1970 2 0.7 (0.1â2.3) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 39 1.1 (0.7â1.4) CDVA, 1997b Australian National Service Vietnam veterans 13 1.4 Dalager and Kang, Army Chemical Corps veterans 2 1.9eâ 1997 Studies Reviewed in Update 1996 Dalager et al., 1995 US Vietnam veteransâwomen 4 1.4 (0.4â3.7) Visintainer et al., Michigan Vietnam veterans 36 1.1 (0.8â1.5) 1995 Boyle et al., 1987 Vietnam Experience Study 3 â* Studies Reviewed in VAO Thomas and Kang, Army Chemical Corps Vietnam veterans 2 * 1990 Breslin et al., 1988 Army Vietnam veterans 116 1.0 (0.3â3.2) Marine Vietnam veterans 25 1.1 (0.2â7.1) Anderson et al., Wisconsin Vietnam veterans 8 0.8 (0.3â1.5) 1986 Lawrence et al., New York Vietnam veterans 4 0.5 (0.2â1.5)d 1985 ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; CI, conï¬dence interval; CNS, central nervous system; IARC, International Agency for Research on Cancer; MCPA, methyl-4-chlorophenoxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; NS, not signiï¬cant; TCDD, 2,3,7,8- tetrachlorodibenzo-p-dioxin; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d Brain and central nervous system combined. e Crude rate ratio of Vietnam to non-Vietnam veterans. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts.
CANCER 431 Reif et al. (1989) performed a series of caseâcontrol analyses on a sample of 19,904 men entered into the New Zealand Cancer Registry from 1980â1984 with an occupation speciï¬ed. They focused on the 134 registrants for whom forestry worker (presumed to be exposed to phenoxy herbicides and chlorophenols) was the most recent occupation. The brain cancer risk associated with having been a forestry worker (four cases, OR 1.19, 95% CI 0.44â3.25) was not signiï¬cantly increased. Lee et al. (2005) reported a caseâcontrol study (251 cases and 498 con- trols) in Nebraska to investigate an association between agricultural pesticide exposure reported by subjects (24 percent of cases and 40 percent of controls) or their proxy respondents (76 percent of cases and 60 percent of controls) and adult glioma. When self-reports and proxy reports were combined, the estimated risk of glioma associated with exposure to 2,4-D (32 cases; OR 1.8, 95% CI 1.0â3.3) was identical with that associated with exposure to phenoxy herbicides in general; the ï¬ndings on 2,4,5-T (seven cases; OR 1.3, 95% CI 0.5â3.6) were much sparser. The strengths of the study were case ascertainment and diagnostic certainty. The need to rely on proxy responses for most subjects was a limita- tion that arose out of interviews being conducted during 1992â1994 whereas the diagnoses occurred in 1988â1993. The pronounced and systematic discrepancy (see Table 6-38) between the results on subject-reported exposure (reduced ORs) and proxy-reported exposure (signiï¬cantly increased ORs), however, underscores concern about recall bias and casts doubt on any interpretations. Investigators in the NIOSH Upper Midwest Health Study reported caseâ control studies of women (Carreon et al., 2005; 341 cases and 528 controls) and men (Ruder et al., 2004; 457 cases and 648 controls). Estimated risks of intracranial glioma associated with reported exposure to arsenicals, organochlo- rines, phenoxy herbicides, or 2,4-D ranged from 0.7 to 1.5; none was statistically signiï¬cant. Magnani et al. (1987) reported a caseâcontrol mortality study (432 cases of brain cancer and 1,603 controls) in the United Kingdom. A JEM was used to predict exposure to various chemical agents on the basis of job title as indicated on death certiï¬cates. Estimated risks of brain cancer associated with exposure to herbicides (RR 1.2, 95% CI 0.7â2.1) and chlorophenols (RR 1.1, 95% CI 0.7â1.8) were not signiï¬cantly increased. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and brain cancer were published since Update 2004. Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported nine deaths from cancers of the meninges, brain, or other parts of the
432 VETERANS AND AGENT ORANGE: UPDATE 2006 CNS (ICD-9 191â192) in the deployed and seven in the non-deployed (CRR 1.19, 95% CI 0.44â3.20). Pavuk et al. (2005) reported on the risk of cancer in the comparison group of the Ranch Hand cohort study. Only one case of brain or other CNS cancer was reported; the sparseness of the data preclude risk estimation. The Australian Vietnam Veterans Mortality and Cancer Incidence Stud- ies (ADVA, 2005a,b) reported the risk of brain cancer in a cohort of 59,179 servicemen. The estimated risks of brain cancer (97 cases; SIR 1.07, 95% CI 0.85â1.28) and brain-cancer mortality (99 cases; SMR 0.95, 95% CI 0.76â1.13) were not signiï¬cantly associated with service in Vietnam. The possibility that the comparisons with the general population might be inï¬uenced by a healthy-warrior effect was investigated in a separate study that compared the rates of brain and CNS cancer in deployed and non-deployed Vietnam veterans (ADVA, 2005c). Brain-cancer incidence (RR 1.36, 95% CI 0.73â2.56) and mortality (RR 1.64, 95% CI 0.89â3.09) were not signiï¬cantly associated with deployment in Vietnam. Biologic Plausibility No animal studies have reported an association between exposure to the compounds of interest and brain cancer. The biologic plausibility of the carci- nogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Since Update 2004, several relevant studies have been identiï¬ed, including cohort and caseâcontrol designs. Many studies rely on surrogate indicators of ex- posure, such as occupational titles, but several estimated exposure to one or more of the compounds of interest on the basis of a JEM or self-reported exposure his- tory. Most used cancer-registry data with a high degree of diagnostic certainty. The signiï¬cant association between occupational exposure to the compounds of interest (2,4-D and phenoxy herbicides) and brain cancer reported in the caseâcontrol study by Lee et al. (2005) was severely compromised by the marked difference between self-reported data and proxy-reported data. The cohort study by Alavanja et al. (2005) reported an increased risk in commercial herbicide applicators who were exposed to some of the compounds of interest, but the in- crease was not statistically signiï¬cant. And two studies reviewed in prior updates report non-signiï¬cant increases in risk in herbicide applicators who were exposed to the compounds of interest (Blair et al., 1983; Swaen et al., 2004). Particularly noteworthy are the increased incidence of and mortality from brain cancer (two to three times those in the comparison groups) in exposed cohorts in both the Air
CANCER 433 Force Ranch Hands (Akhtar et al., 2004) and the Army Chemical Corps (Dalager and Kang, 1997). Most of the relevant prior cohort studies do not show substantial risk dif- ferences from the null hypothesis, but this may reï¬ect the limited power of the cohort method to identify risk differences in rare diseases, such as brain cancer. With the accumulation of ï¬ndings that deviate from consistency with the null hypothesis, however, the present committee can no longer retain the original VAO committeeâs conclusion that the available evidence is suggestive of no association. Conclusion On the basis of detailed evaluation of the epidemiologic evidence from new and previously reported studies of populations with potential exposure to the compounds of interest, the committee concludes that the categorization in prior updates (limited or suggestive evidence of no association) should be revised to inadequate or insufï¬cient to determine whether there is an association between exposure to the compounds of interest and brain cancer and other nervous system cancers. ENDOCRINE CANCERS Cancers of the endocrine system as grouped by the SEER program (see Table B-2 in Appendix B) represent a disparate group of ICD codes: thymus cancer (ICD-9 164.0), thyroid cancer (ICD-9 193), and other endocrine cancer (ICD-9 194). ACS estimated that 7,590 men and 22,590 women would receive diagnoses of thyroid cancer in the United States in 2006 and that 630 men and 870 women would die from it (Jemal et al., 2006). It also estimated that 1,100 men and 980 women would receive diagnoses of other endocrine cancer in 2006 and that 390 men and 400 women would die from it (Jemal et al., 2006). Incidence data on cancers of the endocrine system are presented in Table 6-39. Thyroid cancer is the most prevalent of the endocrine cancers. Many types of tumors can develop in the thyroid gland; most are benign. The thyroid gland con- tains two main types of cells: follicle cells that make and store thyroid hormone and that make thyroglobulin and C cells that make the hormone calcitonin, which helps to regulate calcium metabolism. Different cancers can develop from each kind of cell, and the classiï¬cation of thyroid cancer is still evolving (Liu et al., 2006). The several types into which thyroid cancer is currently classiï¬ed differ in their seriousness. Papillary carcinoma is the most common and usually affects women of childbearing age; it metastasizes slowly and is the least malignant type of thyroid cancer. Follicular carcinoma accounts for about 30 percent of all
434 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-39 Average Annual Incidence (per 100,000) of Endocrine System in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 7.8 8.1 8.0 10.4 10.8 5.7 11.6 11.8 6.0 Women 21.3 21.6 12.6 19.8 19.4 16.1 19.7 20.3 16.1 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. cases and has a greater rate of recurrence and metastasis. Medullary carcinoma is a cancer of nonthyroid cells in the thyroid gland and tends to occur in fami- lies; it requires different treatment from other types of thyroid cancer. Anaplastic carcinoma (also called giant-cell and spindle-cell cancer) is rare but is the most malignant form of thyroid cancer; it does not respond to radioiodine therapy and metastasizes quickly, invading such nearby structures as the trachea, causing compression and breathing difï¬culties. Thyroid cancer can occur in all age groups. People who have had radiation therapy directed at the neck are at higher risk. That therapy was commonly used in the 1950s to treat enlarged thymus glands, adenoids, and tonsils and to treat skin disorders. People who received radiation therapy as children have a higher incidence of thyroid cancer. Other risk factors are a family history of thyroid cancer and chronic goiter. Conclusions from VAO and Updates The present update is the ï¬rst to consider endocrine cancers as constituting a separate cancer type. Thus, there is no conclusion from prior VAO committees related to an association between exposure to the compounds of interest and en- docrine cancers. That the committee responsible for VAO and the committees re- sponsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not consider endocrine cancers separately is a reï¬ection of the rarity of thyroid and other endocrine cancers. The present committee searched for studies of rare cancers and identiï¬ed a number of relevant studies that reported thyroid cancer, in some cases grouped with other endocrine cancers, in populations po- tentially exposed to the compounds of interest. A number of the studies identiï¬ed had been considered in VAO or previous updates with respect to endpoints other than thyroid cancer. Those earlier studies are considered below in chronologic order, followed by comments on newer reports identiï¬ed by the current commit- tee. Table 6-40 summarizes the pertinent results of the relevant studies.
CANCER 435 TABLE 6-40 Selected Epidemiologic StudiesâEndocrine Cancers (thyroid, thymus, and other) Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b OCCUPATIONAL Alavanja et al., US Agriculture Health Studyâincidence (thyroid 2005 and other endocrine) Private applicators (men and women) 29 1.3 (0.8â1.8) Spouses of private applicators ( 99% women) 24 0.9 (0.5â1.4) Commercial applicators (men and women) 3 1.6 (0.3â5.0) ât Mannetje et al., Phenoxy herbicide producers (men and women) 0 * 2005 Phenoxy herbicide sprayers ( 99% men) 0 * Blair et al., 2004 US Agriculture Health Studyâmortality (thyroid) Private applicators (men and women) 3 1.8 (0.4â5.3) Spouses of private applicators ( 99% women) 0 0.0 (0.0â2.2) Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol (thyroid, ICD-9 193) 4 1.7 (0.5â4.3) Exposed to TCDD (or higher-chlorinated dioxins) 2 1.4 (0.2â4.9) Not exposed to TCDD (or higher- chlorinated dioxins) 2 2.2 (0.3â7.9) Workers exposed to any phenoxy herbicide or chlorophenol (other endocrine organs, ICD-9 194) 5 3.6 (1.2â8.4) Exposed to TCDD (or higher-chlorinated dioxins) 2 2.3 (0.3â8.1) Not exposed to TCDD (or higher- chlorinated dioxins) 3 6.4 (1.3â18.7) Ramlow et al., Dow cohort of pentachlorophenol factory 1996 workers employed between 1940 and 1989 at Michigan Division 0 â Zhong and Icelandic men and women exposed to agricultural Rafnsson, 1996 pesticides, primarily 2,4-Dâincidence (other endocrine organs, ICD-9 194) 2 1.3 (0.1â4.7) Asp et al., 1994 Finnish phenoxy herbicide applicatorsâ Incidence (thyroid and other endocrine) No latency 2 1.9 (0.3â7.0) 10-year latency 2 2.4 (0.3â8.6) 15-year latency 2 3.4 (0.4â12.2) Mortality (thyroid) No latency 1 3.8 (0.1â21.3) 10-year latency 1 4.7 (0.1â26.4) 15-year latency 1 6.5 (0.2â36.2) Blair et al., 1993 US farmers in 23 states (thyroid) White men 39 1.3 (1.0â1.8) White women 1 0.8 (0.0â4.4) continued
436 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-40 Continued Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b Hallquist et al., Caseâcontrol study of male and female thyroid 1993 cancers from Swedish Cancer Registry, 1980â1989 Phenoxy herbicide exposure 3 0.5 (0.0â2.0) Chlorophenol exposure 4 2.8 (0.5â18) Ronco et al., 1992 Danish workersâincidence Menâself-employed 13 0.7 (*) employee 5 1.1 (*) Womenâself-employed 1 1.3 (*) employee 1 1.4 (*) family worker 15 1.7 (p 0.05) Green, 1991 Cohort mortality study of forestry workers exposed to phenoxy acid herbicides 1 * Wiklund et al., Cancer risk in licensed pesticide applicators in 1989 Sweden 6 1.1 (0.4â2.4) Bond et al., 1988 Workers engaged in manufacture of phenoxy herbicides 0 * Coggon et al., 1986 British MCPA procuction workers (included in IARC cohort) (thyroid) 1 1.8 (0.4â9.8) Wiklund, 1983 Male and female Swedish agricultural workersâincidence Thyroid 126 0.9 (0.7â1.1) Other endocrine gland 117 0.7 (0.5â0.9) ENVIRONMENTAL Schreinemachers, Rural or farm residents of Minnesota, Montana, 2000 and North and South Dakota Thyroid (ICD-9 193) Menâcounties with high wheat acreage 10 1.9 (0.8â4.6) medium wheat acreage 9 1.5 (0.6â3.6) Womenâcounties with high wheat acreage 13 0.9 (0.5â1.9) medium wheat acreage 12 0.8 (0.4â1.6) Thymus and other endocrine glands (ICD-9 164.0, 194) Menâcounties with high wheat acreage 8 1.4 (0.6â3.6) medium wheat acreage 5 0.8 (0.3â2.4) Womenâcounties with high wheat acreage * * medium wheat acreage * * Bertazzi et al., 1998 Cancer mortality in populations following Seveso accident Zone A * * Zone Bâmen 1 4.9 (0.6â39.0) women 1 3.2 (0.4â24.5) Zone Râmen 0 â women 2 0.8 (0.2â3.6)
CANCER 437 TABLE 6-40 Continued Estimated Exposed Relative Risk Reference Study Populationa Casesb (95% CI)b VIETNAM VETERANS ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence (thyroid) 17 0.6 (0.3â0.9) Navy 3 0.5 (0.1â1.3) Army 11 0.5 (0.3â1.0) Air Force 3 1.2 (0.2â3.5) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality (thyroid) 2 0.5 (0.0â1.8) Navy 1 1.2 (0.0â6.5) Army 1 0.4 (0.0â2.0) Air Force 0 0.0 (0.0â7.8) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veteransâdeployed vs non-deployed Incidence (thyroid) 4 0.6 (0.1â2.2) Mortality (thyroid) 1 1.2 (0.0â91.7) Breslin et al., 1988 Veterans with service in Vietnam vs era veterans (thyroid and other endocrine, ICD-9 193â194) Army 15 0.6 (0.3â1.2) Marine Corp 4 0.6 (0.1â3.4) Clapp, 1997 Massachusetts male Vietnam veterans vs era veteransâincidence 1988â1993 (thyroid) 4 1.2 (0.3â4.5) ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- eran Affairs; AFHS, Air Force Health Study; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; MCPA, 2-methyl-4-chlorophenoxyacetic acid; NIOSH, National Institute for Occupational Safety and Health; NS, not signiï¬cant; TCDD, 2,3,7,8-tetrachlorodibenzo-p-dioxin. a Results are for mortality and for men unless otherwise speciï¬ed. b Given when available. * Information not provided by study authors. â Denoted by a dash in the original study.
438 VETERANS AND AGENT ORANGE: UPDATE 2006 Update of the Epidemiologic Literature Occupational Studies Wiklund (1983) investigated cancer incidence from 1961 to 1973 in men and women who indicated in the 1960 Swedish census that their economic activity was agricultural. The Swedish Cancer Registry recorded 126 cases of thyroid cancer and 117 cases of other endocrine cancer in this occupational group and found no indication of an increase in risk of either sort of endocrine cancer. Coggon et al. (1986) examined mortality of workers in the United Kingdom exposed to 2-methylchlorophenoxy acid during its manufacture. The study cohort consisted of 4,078 men employed by the company at its factory or spray depots in 1947â1975. The cohort was identiï¬ed from personnel records, and people were classiï¬ed as exposed to high, low, or background concentrations on the basis of job titles and dates of employment. Members of the cohort were traced through the National Health Service Registry. There were 1,039 deaths in the cohort, including only one from cancer of the thyroid. Bond et al. (1988) examined mortality in Dow chemical workers engaged in the manufacture of phenoxy herbicides at any time from 1948 to 1983. Mortality was compared with that in all other male workers in the same company location but not engaged in herbicide production. No thyroid cancers were observed. Wiklund et al. (1989a) reported cancer risk in licensed pesticide applicators in Sweden. The pesticides used were based on occupation and included herbi- cides. The cohort included 20,245 people who had applied for a license to apply pesticides during 1965â1976. The cohort was followed in the cancer registry until 1982. Six deaths were attributed to thyroid cancer, for a non-signiï¬cant SIR of 1.10 (95% CI 0.4â2.39). Green (1991) conducted a cohort mortality study of Ontario forestry work- ers exposed to phenoxy acid herbicides. The cohort included workers employed at a public electric utility for at least 6 months during 1950â1982 and routinely exposed to herbicides, including phenoxy acid herbicides. The cohort consisted of 1,222 men, and the male population of Ontario was used as the reference group. One death from thyroid cancer was reported. SMRs were calculated for all neoplasms, and not speciï¬cally for thyroid cancer. Ronco et al. (1992) used database linkage to investigate thyroid-cancer in- cidence in Danish farmers and farm workers. A cohort of farmers of both sexes, 15â74 years old, was identiï¬ed in the 1970 census in the Danish Occupational Cancer Registry and followed for 10 years. Categories of farmers were male self- employed, male employee, female self-employed, female employee, and female family worker. There were 13 cases in the self-employed males and ï¬ve in the male employees, for SIRs of 0.70 and 1.13, respectively (not signiï¬cant at p 0.05). In the women, there was one case each in the self-employed and employee groups and 15 cases in the family-worker group, for an SIR of 1.67 (p 0.05).
CANCER 439 The lack of reliable exposure data precludes drawing further conclusions from the study. A similar approach to evaluating cancer mortality within 6 months after the declaration of a farming occupation on the 1981 Italian census did not generate useful ï¬ndings. Blair et al. (1993) used information from death certiï¬cates from 1984â1988 to assess cancer mortality in farmers in 23 states. There were 39 cases of thy- roid cancer in a population of 119,648 white men, for a PMR of 1.34 (95% CI 0.95â1.83). There was one case each in white women, nonwhite women, and nonwhite men. There was no exposure assessment in the study, and the authors note possible limitations due to the PMR methodology. Hallquist et al. (1993) examined the possibility of an association between occupational exposures and thyroid cancer in a caseâcontrol study. The study involved 180 cases drawn from the Swedish Cancer Registry; the people with cancer were 20â70 years old at diagnosis during the period 1980â1989. Diag- nosis was conï¬rmed histologically. There were 360 controls, two for each case, matched on age and sex, drawn from the National Population Registry and in the same regions as the cases. Residence, occupation, and exposures were deter- mined by questionnaire with telephone follow-up. At the time of study, subjects were 123 women and 48 men, and controls were 240 women and 85 men; 9 subjects and 34 controls refused to participate and one control died before being interviewed for the study. Three subjects and 10 controls reported exposure to phenoxy herbicides, for an OR of 0.5 (95% CI 0.01â2.0). Four subjects and three controls were exposed to chlorophenols, which can contain dioxins (OR 2.8, 95% CI 0.5â18); the increase was not signiï¬cant. Asp et al. (1994) reported on a cohort of Finnish chlorophenoxy herbicide applicators that had been assembled in 1972 from personnel records of Finnish employers involved in brush wood control. 2,4-D and 2,4,5-T were used almost exclusively from the middle 1950s to the 1970s. The two herbicides were used in a 2:1 mixture of 2,4-D to 2,4,5-T. Four of the ï¬ve 2,4,5-T preparations used during the period contained TCDD at 0.1â0.95 mg/kg of herbicide. The use of 2,4,5-T has been suspended since 1980, and exposure since then has been to 2,4-D and MCPA. The original cohort included 1,971 men who had been exposed to phenoxy herbicides for at least 2 weeks during 1955â1971. At the beginning of 1972, the cohort included 1,909 men. Mortality in the cohort was followed to the end of 1989. Cancer incidence was followed from 1972 to the end of 1979. There was a single death from thyroid cancer and an additional incident endocrine can- cer case; both occurred at least 15 years after the start of exposure. The estimated risks were high but non-signiï¬cant, and the results are generally uninformative. Ramlow et al. (1996) examined mortality in a cohort of pentachlorophenol factory workers employed during 1940â1989 at the Dow Chemical Michigan Division. The cohort is a subset of the larger Dow cohort that was potentially exposed to dioxin. Census lists from the division were used to measure the po- tential for exposure to herbicides and pentachlorophenol. Some 2,192 workers
440 VETERANS AND AGENT ORANGE: UPDATE 2006 were identiï¬ed, and job titles were used to determine potential dioxin exposure. Exposure assessment included a detailed description of dioxin exposure; expo- sure assessments in the Dow study were discussed more extensively elsewhere (Ott et al., 1987). No deaths from thyroid cancer were identiï¬ed in the cohort, which was followed for 15 years. Zhong and Rafnsson (1996) examined a cohort in Iceland of 2,449 people (1,860 men and 589 women) who had encountered pesticides in different ways. Cohort members were classiï¬ed according to types of activity considered to re- sult in different exposures to pesticides. Exposure was estimated on the basis of amounts of pesticides sold for agricultural purposes during 1976â1993 according to Icelandic records that include amounts of speciï¬c chemicals sold. The most- used chemical was 2,4-D; about twice as much of it was used as of the next-most used. 2,4,5-T was used, but it was the least used chemical in the registry. In the cohort, there were two cases of endocrine cancer (ICD-9 194) (SIR 1.29, non- signiï¬cant, 95% CI 0.14â4.66). Kogevinas et al. (1997) examined cancer mortality in workers exposed to phenoxy herbicides, chlorophenols, and dioxins in a large international cohort study. The study included 21,863 male and female workers in 36 cohorts ex- posed to the chemicals in 12 countries. The study was coordinated by IARC. Subjects were followed from 1939 to 1992. In all the workers exposed to any phenoxy herbicides or chlorophenols, there were four deaths from thyroid cancer (SMR 1.65, 95% CI 0.45â4.32) and ï¬ve from other endocrine cancers (SMR 3.60, 95% CI 1.17â8.39). When the sample was partitioned into those who had and those who had not been exposed to TCDD, the increases in risk were more pronounced in those who had not been exposed to TCDD (thyroid-cancer SMR 2.17, 95% CI 0.26â7.85; other endocrine cancer SMR 6.38, 95% CI 1.32â18.65). In New Zealand, ât Mannetje et al. (2005) followed the mortality experience of 813 TCDD-exposed phenoxy herbicide producers and 699 sprayers through 2000. No deaths from thyroid cancer (ICD-9 193) or other endocrine cancer (ICD-9 194) were observed in either group. Alvanja et al. (2005) published a report on a cohort of agricultural pesticide applicators and their spouses in the AHS using data from cancer registries of North Carolina and Iowa. They reported three cases of thyroid and other endo- crine cancers in 4,916 commercial applicators (SIR 1.58, 95% CI 0.34â4.99), 29 cases in 52,395 private applicators (SIR 1.29, 95% CI 0.77â1.76), and 24 cases in 32,347 spouses of private applicators (SIR 0.91, 95% CI; 0.54â1.44). The estimated risks in commercial applicators and private applicators were slightly increased, but none of the estimated risks was statistically signiï¬cant. Blair et al. (2005a) examined mortality in the same AHS prospective cohort of private pesticide applicators and their spouses. In the private applicators, there were three deaths speciï¬cally from thyroid cancer (SMR 1.8, 95% CI 0.4â5.3);
CANCER 441 there was no mention of other endocrine cancers. There were no deaths from any type of endocrine cancers in the spouses. Environmental Studies Bertazzi et al. (1998) summarized cancer mortality in populations in the dif- ferent zones of exposure after the Seveso accident. Mortality was examined in residents in Zone A (high exposure; 805 people) and Zone B (medium exposure; 5,942 people), and Zone R (low exposure; 38,625 people). There were no deaths from thyroid cancer in Zone A from 1976 to 1991. In Zone B, there was one death from thyroid cancer in men and one in women; these resulted in unstable estimates of increased risk. In Zone R, there were two deaths from thyroid cancer in women but none in men. A study by Schreinemachers (2000) examined cancer mortality in four wheat-producing states: Minnesota, North Dakota, South Dakota, and Montana. Acreage devoted to raising wheat in counties in those states was used as a sur- rogate for exposure to chlorophenoxy herbicides; the rationale was that in those states more that 90 percent of spring wheat and 30 percent of winter wheat were treated with chlorophenoxy herbicides. Cancer mortality was examined during 1980â1999 in selected counties according to wheat acreage per county and the percentage of the population that was rural. Age-standardized mortality rate ratios showed an increasing trend for thyroid-cancer death in white men over 65 years old in the tertiles based on wheat acreage, with eight cases and an SRR of 2.54 (95% CI 0.88â7.35) in the highest tertile. In white women over 65 years old, there were 13 cases, for an SRR of 1.55 (95% CI of 0.88â7.35). The results suggest hypotheses but present the difï¬culty of uncertainty as to whether results for counties hold for individuals. Vietnam-Veteran Studies Anderson et al. (1986a) examined mortality in Vietnam veterans in Wiscon- sin. Vietnam veterans were compared with veterans who did not serve in Vietnam. No death from thyroid cancer was recorded in the Vietnam veterans. In a proportionate mortality study of Army and Marine Corps Vietnam vet- erans, Breslin et al. (1988) examined a sample of 52,253 men who had served in the corps during 1965â1973 and who died during 1965â1982. The cause of death was ascertained for 51,421. Of these, 24,235 had served in Vietnam. Thyroid and other endocrine cancers were grouped. There were 15 deaths in army personnel and four in marine personnel. The PMRs were 0.59 and 0.57, respectively. Clapp (1997) evaluated male veterans in Massachusetts for cancer incidence, using data from the Massachusetts Cancer Registry. Over the period 1988â1993, 245 cases of cancer were reported in Vietnam veterans and 999 cases in Vietnam- era veterans. The age-adjusted OR for thyroid cancer (4 cases in the Vietnam
442 VETERANS AND AGENT ORANGE: UPDATE 2006 veterans and 13 in the Vietnam-era veterans) was 1.2 (95% CI 0.3â4.5), which is not statistically signiï¬cant. A set of reports updating the health status of Australian Vietnam veterans (ADVA 2005a,b,c), including thyroid cancer, covered a possible association be- tween Vietnam service and thyroid cancer. In a comparison of veterans with the general population of Australia, the SIR was 0.57 (95% CI 0.33â0.92) (ADVA, 2005a), and the SMR was 0.51 (95% CI 0.03â1.78) (ADVA, 2005b). The pos- sibility that the results were attributable to a healthy-warrior effect was investi- gated in a separate study that compared rates of thyroid cancer in deployed and non-deployed Vietnam veterans (ADVA, 2005c); the decrease in incidence in the deployed did not reach signiï¬cance (RR 0.14, 95% CI 0.63â2.24), and the RR of thyroid-cancer mortality based on a single death in each group of veterans was close to 1 with an extremely wide conï¬dence range (RR 1.17, 95% CI 0.01â91.69). Biologic Plausibility The NTP conducted carcinogenesis bioassays in Osborne-Mendel rats and B6C3F1 mice exposed to TCDD by gavage (NTP, 1982a). The incidence of follicular-cell adenoma, but not of carcinoma, increased with increasing TCDD dose in both male and female rats; the increase was signiï¬cant in male but not female rats. There was a signiï¬cant increase in follicular-cell adenoma in female but not male mice. The NTP carried out a similar study in female Sprague-Daw- ley rats more recently (NTP, 2006). Walker et al. (2006) compared the resulting data from that and another study of chronic toxicity and carcinogenicity of TCDD in female Sprague-Dawley rats. They compared the recent results of the NTP assessment and the results of the Dow Chemical assessment of TCDD carcino- genicity. In the NTP and Dow studies, the incidence of thyroid cancer (C-cell adenoma and carcinoma) decreased with increasing dose of TCDD. However, an increased incidence of minimal thyroid follicular-cell hypertrophy was noted in rats given TCDD at 22 ng/kg of body weight or greater. As indicated in Chapter 3, 2,4-D and 2,4,5-T are at most only weakly muta- genic or carcinogenic. No studies that addressed a possible association between exposure to those herbicides and thyroid cancer in animal models have been identiï¬ed. Synthesis Several relevant studiesâincluding cohort studies, environmental studies, and Vietnam-veteran studiesâare considered here for the ï¬rst time in the series of VAO reports. They show low thyroid-cancer incidence and cancer mortality in various populations. The studies assessed exposure to one or more of the com- pounds of interest although the metrics often were based on surrogate indicators
CANCER 443 or self-reported exposure. Some of the cohort studies used cancer-registry data with a high degree of diagnostic certainty. Several of the studies show somewhat increased risks of thyroid or other endocrine cancers in association with the com- pounds of interest. Of the studies with any indication of statistical signiï¬cance, Blair et al. (1993) and Ronco et al. (1992) both had mixed results; the authors were conducting analyses on large samples whose exposure was no better char- acterized than âagricultural workerâ on a death certiï¬cate or census response, whereas in the IARC cohort (Kogevinas et al., 1997), the risks of endocrine can- cers were lower in phenoxy herbicide workers who also had exposure to TCDD. Most showed no substantial risk differences in association with the components of Agent Orange. Many of the studies had very small numbers of cases, and their limitations preclude risk estimation. There were no signiï¬cant ï¬ndings in Vietnam-veteran studies. Thus, the studies reviewed do not provide sufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and thyroid cancer. Conclusion On the basis of its evaluation of the epidemiologic evidence reviewed here, the committee concludes that there is insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and thyroid or other endocrine cancers. NON-HODGKINâS LYMPHOMA Non-Hodgkinâs lymphoma (NHL, ICD-9 200.0â200.8, 202.0â202.2, 202.8â 202.9) is the more common of the two primary types of cancer of the lymphatic system. ACS estimated that 30,680 men and 28,190 women would receive di- agnoses of NHL in the United States in 2006 and that 10,000 men and 8,840 women would die from it (Jemal et al., 2006). Collectively, lymphomas (which include Hodgkinâs disease) are the ï¬fth-most common form of cancer in the United States. The incidence of NHL is uniformly higher in men than in women and typically higher in whites than in blacks. In the groups that characterize most Vietnam veterans, incidence increases with age. Average annual incidences are shown in Table 6-41. The causes of NHL are poorly understood. People with suppressed or com- promised immune systems are known to be at higher risk, and some studies show increased incidence in people with HIV, human T-cell lymphotropic virus, Epstein-Barr virus, and gastric Helicobacter pylori infections. Behavioral, oc- cupational, and environmental risk factors also have been proposed (Blair et al., 1997). Chronic lymphocytic leukemia (CLL) and hairy-cell leukemia share many traits with NHL (for example, immunohistochemical traits and B-cell origin); it
444 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-41 Average Annual Incidence (per 100,000) of Non-Hodgkinâs Lymphoma in United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All White Black All White Black All White Black Races Races Races Men 26.7 28.4 24.1 37.6 38.8 38.2 52.0 55.0 37.5 Women 18.2 18.4 18.7 28.3 29.2 24.4 38.2 41.5 25.4 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. may progress to an acute aggressive form of NHL). CLL is discussed separately after the general section on leukemia. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was sufï¬cient evidence to support an association between exposure to at least one of the com- pounds of interest and NHL. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-42 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. A JEM was applied to 58,162 individual work histories to estimate exposure to nonvolatile organochlorine compounds (which would include TCDD). Death from NHL was not more strongly associated with having ever been exposed to nonvolatile organochlorine compounds (n 25; SMR 0.86, 95% CI; 0.55â1.26) than with having never been exposed (n 35; SMR 0.93, 95% CI 0.65â1.30). Two reports from the US AHS (Alavanja et al., 2005; Blair et al., 2005a) provided ï¬ndings on the incidence of and mortality from NHL among pesticide applicators, commercial applicators, and their spouses, but no results on any of the speciï¬c herbicides under consideration were published. As delineated in Table 6-42, no associations were observed between those occupational categories and NHL. No associations were found in the cohort study of New Zealand phenoxy producers and sprayers (ât Mannetje et al., 2005), in which a single death from
CANCER 445 TABLE 6-42 Selected Epidemiologic StudiesâNon-Hodgkinâs Lymphoma Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies Chiu et al., 2006 Nebraska residents, NHL reclassiï¬ed according (based on Zahm to speciï¬c chromosomal translocation et al., 1990, 1993) (t[14;18][q32;q21]) Translocation present in cases Herbicides 25 2.9 (1.1â7.9) Translocation absent in cases Herbicides 22 0.7 (0.3â1.2) McLean et al., IARC cohort of pulp and paper workers 2006 Exposure to nonvolatile organochlorine compounds Never 35 0.9 (0.7â1.3) Ever 25 0.9 (0.6â1.3) Alavanja et al., US Agriculture Health Studyâincidence 2005 Private applicators (men and women) 114 1.0 (0.8â1.2) Spouses of private applicators ( 99% women) 42 0.9 (0.6â1.2) Commercial applicators (men and women) 6 1.0 (0.4â2.1) Pooled analyses of caseâcontrol studies conducted in Iowa, Minnesota, Kansas, Nebraska, 1980s Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 33 0.9 (0.6â1.2) Spouses of private applicators ( 99% women) 16 1.2 (0.7â2.0) Fritschi et al., 2005 Population-based caseâcontrol study in New South Wales, Australia, 2000â2001 Phenoxy herbicides Non-substantial exposure 10 0.7 (0.3â1.7) Substantial exposure 5 1.8 (0.4â7.4) Mills et al., 2005 Nested caseâcontrol analyses of Hispanic workers in cohort of 139,000 California United Farm Workers Ever used 2,4-D * 3.8 (1.9â7.8) ât Mannetje et al., Phenoxy herbicide producers (men and women) 1 0.9 (0.0â4.9) 2005 Phenoxy herbicide sprayers ( 99% men) 1 0.7 (0.0â3.8) Chiu et al., 2004 Herbicide usage Farmers 294 1.2 (1.0â1.5) Non-farmers 273 1.0 (0.8â1.2) Lee et al., 2004b Asthmatics Herbicide exposureâphenoxyacetic acid 17 1.3 (0.7â2.4) Exposures among farmers 2,4-D 17 1.3 (0.7â2.5) 2,4,5-T 7 2.2 (0.8â6.1) continued
446 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-42 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Non-asthmatics Herbicide exposureâphenoxyacetic acid 176 1.0 (0.8â1.3) Exposures among farmers 2,4-D 172 1.0 (0.8â1.3) 2,4,5-T 36 1.1 (0.7â1.8) Hardell et al., 2002 Pooled analysis of Swedish caseâcontrol studies of NHL and of hairy cell leukemia Herbicide exposure 77 1.8 (1.3â2.4) Phenoxyacetic acids 64 1.7 (1.2â2.3) MCPA 21 2.6 (1.4â4.9) 2,4-D and 2,4,5-T 48 1.5 (1.0â2.2) Other 15 2.9 (1.3â6.4) Torchio et al., Italian licensed pesticide users 15 0.9 (0.5â1.5) 1994 Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 7 1.8 (0.9â4.0) Studies Reviewed in Update 2004 Bodner et al., 2003 Dow chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) â 1.4 (0.6â2.7) Miligi et al., 2003 Residents from 11 different areas in Italy Phenoxy acid herbicides exposure Men 18d 1.0 (0.5â2.0) Women 11d 1.3 (0.5â3.7) 2,4âD exposure Men 6d 0.7 (0.3â0.19) Women 7d 1.5 (0.4â5.7) Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 3 1.0 (0.2â2.9) Thörn et al., 2000 Swedish lumberjacks exposed to phenoxyacetic herbicidesâincidence 2 2.3 (0.3â8.5) Studies Reviewed in Update 2000 Steenland et al., US chemical production workers (included in the 1999 IARC cohort and the NIOSH Dioxin Registry) 12 1.1 (0.6â1.9) Hooiveld et al., Dutch phenoxy herbicide workers (included in 1998 the IARC cohort) 3 3.8 (0.8â11.0) Studies Reviewed in Update 1998 Gambini et al., Italian rice growers 4 1.3 (0.3â3.3) 1997 Keller-Byrne et al., Farmers in central United States 1.3 (1.2â1.6) 1997
CANCER 447 TABLE 6-42 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 34 1.3 (0.9â1.8) Exposed to TCDD (or higher-chlorinated dioxins) 24 1.4 (0.9â2.1) Not exposed to TCDD (or higher- chlorinated dioxins) 9 1.0 (0.5â1.9) Becher et al., 1996 German production workers (included in the IARC cohort) 6 3.3 (1.2â7.1) Nanni et al., 1996 Italian farming and animal-breeding workersâ incidence (men and women) 3d 1.4 (0.4â5.7) Ramlow et al., Dow pentachlorophenol production workers 1996 (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 7e 1.4 (0.6â2.9) 15-year latency 5e 1.3 (0.4â3.1) Amadori et al., Italian farming and animal-breeding workersâ 1995 incidence (men and women) 164 1.8 (1.2â2.6) Studies Reviewed in Update 1996 Kogevinas et al., IARC cohortâincidence (men and women) 1995 Exposed to 2,4,5-T 10 1.9 (0.7â4.8) Exposed to TCDD 11 1.9 (0.7â5.1) Asp et al., 1994 Finnish herbicide applicators Incidence 1 0.4 (0.0â2.0) Dean, 1994 Irish farmers and farm workers Men 244d â Women 84d â Hardell et al., 1994 Umea (Sweden) Hospital patientsâincidence Exposure to phenoxy herbicides 25 5.5 (2.7â11.0) Exposure to chlorophenols 35 4.8 (2.7â8.8) Morrison et al., Farm operators in three Canadian provinces 1994 All farm operators * 0.8 (0.7â0.9) Highest quartile of herbicides sprayed 19 2.1 (1.1â3.9) Highest quartile of herbicides sprayed relative to no spraying 6 3.0 (1.1â8.1) Blair et al., 1993 US farmers from 23 states (white men) 843 1.2 (1.1â1.3) Bloemen et al., Dow 2,4-D production workers (included in the 1993 IARC cohort and the NIOSH Dioxin Registry) 2 2.0 (0.2â7.1) Bueno de Mesquita Dutch phenoxy herbicide workers (included in et al., 1993 the IARC cohort) 2 3.0 (0.4â10.8) Lynge, 1993 Danish male and female production workers (included in the IARC cohort)âupdated incidence Exposure to phenoxy herbicides (men) 10 1.7 (0.5â4.5) continued
448 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-42 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Persson et al., Swedish NHL patients 1993 Exposure to phenoxy herbicides 10 2.3 (0.7â7.2) Occupation as lumberjack 9 6.0 (1.1â31.0) Zahm et al., 1993 Women from eastern Nebraska farms 119 1.0 (0.7â1.4) Kogevinas et al., IARC cohort (men and women) 1992 Workers exposed to any phenoxy herbicide or chlorophenol 11 1.0 (0.5â1.7) Studies Reviewed in VAO Hansen et al., 1992 Danish gardeners (men and women)âincidence 8 2.0 (0.9â3.9) Ronco et al., 1992 Danish farm workersâincidence 147 1.0 (*) Italian farm workersâmortality 14 1.3 (*) Smith and Australian residents Christophers, 1992 Exposure 1 day 15 1.5 (0.6â3.7) Exposure 30 days 7 2.7 (0.7â9.6) Swaen et al., 1992 Dutch herbicide applicators 0 â Vineis et al., 1991 Residents of selected Italian provinces Male residents of contaminated areas * 2.2 (1.4â3.5) Wigle et al., 1990 Canadian farmers All farmers 103 0.9 (0.8â1.1) Spraying herbicides on 250 acres 10 2.2 (1.0â4.6) Zahm et al., 1990 Eastern Nebraska residents Ever done farm work 147 0.9 (0.6â1.4) Ever mixed or applied 2,4-D 43 1.5 (0.9â2.5) Alavanja et al., USDA forest or soil conservationists 22 2.4 (1.5â3.6) 1989 Corrao et al., 1989 Italian farmers licensed to apply pesticides Licensed pesticide users and nonusers 45f 1.4 (1.0â1.9) Farmers in arable land areas 31 1.8 (1.2â2.5) LaVecchia et al., Residents of the Milan, Italy, area (men and 1989 women) Agricultural occupations * 2.1 (1.3â3.4) Persson et al., Ãrebro (Sweden) Hospital (men and women) 1989 Exposed to phenoxy acids 6 4.9 (1.0â27.0) Wiklund et al., Swedish pesticide applicators (men and women) 27 1.1 (0.7â1.6) 1989b Alavanja et al., USDA agricultural extension agents * 1.2 (0.7â2.3) 1988 Dubrow et al., Hancock County, Ohio residentsâfarmers 15 1.6 (0.8â3.4) 1988 Olsson and Brandt, Lund (Sweden) Hospital patients 1988 Exposed to herbicides * 1.3 (0.8â2.1) Exposed to chlorophenols * 1.2 (0.7â2.0)
CANCER 449 TABLE 6-42 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Wiklund et al., Swedish agricultural and forestry workers (men 1988 and women) Workers in land or animal husbandry 1.0 (0.9â1.1) Timber cutters 0.9 (0.7â1.1) Pearce et al., 1987 New Zealand residents Farming occupations 33 1.0 (0.7â1.5) Fencing work 68 1.4 (1.0â2.0) Woods et al., 1987 Washington state residents Phenoxy herbicide use * 1.1 (0.8â1.4) Chlorophenol use * 1.0 (0.8â1.2) Farming occupations * 1.3 (1.0â1.7) Forestry herbicide appliers * 4.8 (1.2â19.4) Hoar et al., 1986 Kansas residents Farmers compared with non farmers 133 1.4 (0.9â2.1) Farmers using herbicides 21 days/year 7 6.0 (1.9â19.5) Pearce et al., 1986 New Zealand residentsâagricultural sprayers 19g 1.5 (0.7â3.3) Pearce et al., 1985 New Zealand residents with agricultural occupations, 20â64 years old 224 1.4 (0.9â2.0) Burmeister et al., Iowa residentsâfarming exposures 1,101 1.3 (*) 1983 Wiklund, 1983 Swedish male and female agricultural workersâincidence 476 1.1 (0.9â1.2) Cantor, 1982 Wisconsin residentsâfarmers 175 1.2 (1.0â1.5) Riihimaki et al., Finnish herbicide applicators 0 â 1982 Hardell et al., Umea (Sweden) Hospital patientsâincidence 1981 Exposed to phenoxy acids 41 4.8 (2.9â8.1)f Exposed to chlorophenols 50 4.3 (2.7â6.9)f ENVIRONMENTAL New Studies Hartge et al., 2005 NCI SEER caseâcontrol study (Iowa, Los Angeles County, Detroit, Seattle) 1998â2000 Exposures to 2,4-D in carpet dust (ng/g) Under detection limit 147 1 500 257 1.1 (0.8â1.6) 500â999 86 0.9 (0.6â1.5) 1000â9999 165 0.7 (0.5â1.0) 10000 24 0.8 (0.4â1.7) continued
450 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-42 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Kato et al., 2004 Population-based caseâcontrol study in upstate New York state, women, 20â79 years of age, 1995â1998 Home usage only of herbicides/pesticides (times) 0 231 1 1â4 33 0.9 (0.5â1.5) 5â17 30 0.7 (0.4â1.3) 18â39 27 1.0 (0.6â1.7) 40 40 0.9 (0.5â1.5) Studies Reviewed in Update 2004 Floret et al., 2003 Residents near a French municipal solid-waste incinerator High-exposure category 31 2.3 (1.4â3.8) Studies Reviewed in Update 2002 Hardell et al., 2001 Caseâcontrol study of NHLâTEQ 27.8 and EA 80 8 2.8 (0.5â18.0) McDufï¬e et al., Caseâcontrol study of NHL in Canada 2001 Exposed to phenoxy herbicides 131 1.4 (1.1â1.8) 2,4-D 111 1.3 (1.0â1.7) Mecoprop 53 2.3 (1.6â3.4) Studies Reviewed in Update 2000 Bertazzi et al., Seveso residentsâ20-year follow-up 2001 Zone A,Bâmen 4 1.8 (0.7â4.9) women 3 1.2 (0.4â3.9) Schreinemachers, Rural or farm residents of Minnesota, Montana, 2000 and North and South Dakota Menâcounties with high wheat acreage 176h 0.9 (0.8â1.1) medium wheat acreage 186h 0.8 (0.7â1.0) Womenâcounties with high wheat acreage 162h 1.0 (0.8â1.2) medium wheat acreage 202h 1.0 (0.8â1.2) Viel et al., 2000 Residents near a French solid-waste incineratorâincidence Spatial cluster 286 1.3 (p 0.001) 1991â1994 109 1.8 (p 0.001) Studies Reviewed in Update 1998 Bertazzi et al., Seveso residentsâ15-year follow-up 1997 Zone Bâmen 2 1.5 (0.2â5.3) Zone Râmen 10 1.1 (0.5â2.0) women 8 0.9 (0.4â1.7)
CANCER 451 TABLE 6-42 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 1996 Bertazzi et al., Seveso residentsâ10-year follow-upâincidence 1993 Zone Bâmen 3 2.3 (0.7â7.4) women 1 0.9 (0.1â6.4) Zone Râmen 12 1.3 (0.7â2.5) women 10 1.2 (0.6â2.3) Studies Reviewed in VAO Lampi et al., 1992 Finnish community exposed to chlorophenol contamination (men and women) 16 2.8 (1.4â5.6) Pesatori et al., Seveso residentsâincidence 1992 Zones A, Bâmen 3 1.9 (0.6â6.1) women 1 0.8 (0.1â5.5) Zone Râmen 13 1.4 (0.7â2.5) women 10 1.1 (0.6â2.2) Bertazzi et al., Seveso residentsâ10-year follow-up 1989b Zone Bâwomen 2 1.0 (0.3â4.2) Zone Râmen 3 1.0 (0.3â3.4) women 4 1.6 (0.5â4.7) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 126 0.7 (0.6â0.8) Navy 31 0.8 (0.5â1.0) Army 86 0.7 (0.5â0.8) Air Force 9 0.8 (0.2â0.9) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 70 0.8 (0.6â1.0) Navy 10 0.5 (0.3â0.9) Army 52 0.9 (0.6â1085) Air Force 8 1.1 (0.4â1.6) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 35 1.1 (0.7â1.9) Mortality 21 1.4 (0.7â2.8) Boehmer et al., Vietnam Experience Cohort 6 0.9 (0.3â2.9) 2004 Studies Reviewed in Update 2004 Akhtar et al., 2004 White Air Force Ranch Hand veterans Lymphopoetic leukemia Ranch Hand Veteransâincidence 10 0.9 (0.4â1.5) Comparison Air Force Veteransâincidence 9 0.6 (0.3â1.0) continued
452 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-42 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 1 0.2 (0.0â2.6) AIHW, 1999 Australian Vietnam veterans 62 48 expected (34â62) CDVA, 1998a Australian Vietnam veteransâmen 137i 48 expected (34â62) CDVA, 1998b Australian Vietnam veteransâwomen 2i 0 expected (0â4) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans NHL deaths, 1980â1994 33 0.9 (0.6â1.2) Watanabe and Marine Vietnam veterans 46 1.7 (1.2â2.2) Kang, 1996 Studies Reviewed in Update 1996 Visintainer et al., Michigan Vietnam veterans 32 1.5 (1.0â2.1) 1995 Studies Reviewed in VAO Clapp et al., 1991 Massachusetts Vietnam veterans 1.2 (0.6â2.4) Dalager et al., Vietnam veterans diagnosed with NHL 100 1.0 (0.7â1.5) 1991 OâBrien et al., Army enlisted Vietnam veterans 7j 1.8 1991 Thomas et al., Women Vietnam veterans 3 1.3 (0.3â1.8) 1991 Watanabe et al., Army Vietnam veterans 1991 vs Army non-Vietnam veterans 140 0.8 (*) vs all non-Vietnam veterans 140 0.9 (*) Marine Vietnam veterans vs Marine non-Vietnam veterans 42 1.8 (1.3â2.4) vs all non-Vietnam veterans 42 1.2 (*) CDC, 1990b US Vietnam veterans born 1921â1953 99 1.5 (1.1â2.0) Army Vietnam veterans 45 1.2 (0.8â1.8) Marine Vietnam veterans 10 1.8 (0.8â4.3) Air Force Vietnam veterans 12 1.0 (0.5â2.2) Navy Vietnam veterans 32 1.9 (1.1â3.2) Blue-water Navy Vietnam veterans 28 2.2 (1.2â3.9) Michalek et al., Air Force Ranch Hand veteran mortality 0 * 1990 Wolfe et al., 1990 Air Force Ranch Hand veteran morbidity 1 * Breslin et al., 1988 Army Vietnam veterans 108 0.8 (0.6â1.0) Marine Vietnam veterans 35 2.1 (1.2â3.8) Garland et al., Navy enlisted personnel 1974â1983 68 0.7 (0.5â0.9) 1988
CANCER 453 TABLE 6-42 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Burt et al., 1987 Army combat Vietnam veterans 39 1.1 (0.7â1.5) Marine combat Vietnam veterans 17 3.2 (1.4â7.4) Army Vietnam veterans (service 1967â1969) 64 0.9 (0.7â1.3) Marine Vietnam veterans (service 1967â1969) 17 2.5 (1.1â5.8) Fett et al., 1987 Australian Vietnam veterans 4 1.8 (0.4â8.0) Anderson et al., Wisconsin Vietnam veterans (includes 1986b lymphosarcoma and reticulosarcoma) 4 â Holmes et al., West Virginia Vietnam veterans vs West Virginia 1986 Vietnam-era veterans 2 1.1 (*) Lawrence et al., New York Vietnam veterans vs New York 1985 Vietnam-era veterans 10f 1.0 (0.4â2.2) ABBREVIATIONS: 2,4,5-T, 2,4,5-trichlorophenoxyacetic acid, 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Veteran Affairs; AFHS, Air Force Health Study; AIHW, Aus- tralian Institute of Health and Welfare; CDC, Centers for Disease Control and Prevention; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; EA, Epstein-Barr virus early antigen; IARC, International Agency for Research on Cancer; NHL, non-Hodgkinâs lymphoma; SIR, standard incidence ratio; SMR, standardized mortality ratio; TCDD, 2,3,7,8-tetrachlorodibenzo-p- dioxin; TEQ, toxicity equivalency; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d Includes NHL and chronic lymphocytic leukemia combined. e Includes all lymphomas combined. f Includes lymphoma and Hodgkinâs disease. g Only NHL other than lymphosarcoma and reticulosarcoma (ICD-9 202). h Includes lymphosarcoma, reticulum cell sarcoma including other lymphoma i Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have NHL?â j NHL, four living cases and three deaths originally reported in the CDC Vietnam Experience Study (Boyle et al., 1987). * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts. NHL (ICD-9 200, 202) was observed in the producer group and one death in the sprayer group. A subcohort comprising Hispanic workers drawn from a larger cohort of 139,000 California members of the United Farm Workers of America (UFW) was reanalyzed with a nested caseâcontrol design (Mills et al., 2005). A total of 60 people with NHL (45 men and 15 women) were identiï¬ed, and each case was matched to ï¬ve control subjects drawn from the original cohort on sex, year of birth, and ethnicity (all were of Hispanic origin). A strong association between
454 VETERANS AND AGENT ORANGE: UPDATE 2006 use of 2,4-D and NHL was found (OR 3.80, 95% CI 1.85â7.81); much higher excess risks were found for extranodal cancer (n 22; OR 9.73, 95% CI 2.68â 35.3) than for nodal NHL (n 38; OR 2.29, 95% CI 0.90â5.82). The incidence was signiï¬cantly increased in both men (n 45; OR 3.79, 95% CI 1.58â9.11) and women (n 15; OR 5.23, 95% CI 1.30â20.9). Fritschi and collaborators (2005) conducted a population-based caseâcontrol study in 2000â2001 in men and women 20â74 years old living in New South Wales, Australia. Case subjects were identiï¬ed with the Central Cancer Registry of New South Wales, and control subjects were selected randomly from electoral rolls that represented almost 100 percent of Australian citizens. Equal numbers of cases and controls (694 of each) were selected, and response rates were around 69 percent for cases and 54 percent for controls. On the basis of detailed ques- tions asked of subjects, occupational exposure to pesticides and herbicides was assessed by a team of industrial hygienists who were unaware of the subjectsâ case status. For âsubstantialâ exposure to phenoxy herbicides, an OR of 1.75 was found (ï¬ve exposed case subjects, 95% CI 0.42â7.38). Chiu et al. (2004) and Lee et al. (2004b) conducted a pooled (combined) analysis of two caseâcontrol studies that were carried out in three midwest- ern American states: Iowa and Minnesota (Cantor et al., 1992) and Nebraska (Zahm et al., 1990). In the IowaâMinnesota component of the study, 530 white male case subjects 30 years old and older were identiï¬ed in 1980â1983; in the Nebraska component, 346 male and female case subjects 21 years old and older were identiï¬ed in 1983â1986. Control subjects were frequency-matched to case subjects by age, sex, and race. Two sampling frames were used to select control subjects: for cases 20â64 years old, random-digit dialing was used; for older control subjects, ï¬les from the Health Care Financing Administration were used (2,357 controls). Response rates for case subjects were about 90 percent and for controls 78 percent (Iowa and Minnesota) to 85 percent (Nebraska). In-depth interviews provided information on self-reported use of pesticides and herbicides. Risks were increased by 20 percent in farmers by use of herbicides (OR 1.2, 95% CI 1.0â1.5) but not in non-farmers. In asthmatics, risks were increased by exposure to 2,4-D (OR 1.3, 95% CI 0.7â2.5) and 2,4,5-T (OR 2.2, 95% CI 0.8â6.1), but the conï¬dence intervals were broad and included unity. According to the study authors, there was limited statistical power to investigate interactions by asthma status. A recent analysis of the data from Nebraska (Chiu et al., 2006, based on Zahm et al., 1990, 1993) was used to determine risks of types of NHL. Spe- ciï¬cally, tissue samples were analyzed according to the presence of a speciï¬c chromosomal translocation (t[14;18][q32;q21]), and only 172 of 385 cases were included. Exposure to herbicides was found to confer a signiï¬cantly higher risk (OR 2.9, 95% CI 1.1â7.9) in subjects who had the translocation but not in those who did not (OR 0.7, 95% CI 0.3â1.2). Hardell et al. (2002) conducted a pooled analysis of two caseâcontrol stud-
CANCER 455 ies (that were not consider in previous VAO reports), one of NHL (Hardell and Eriksson, 1999) and one speciï¬cally of a rare form of NHL, hairy cell leukemia (Nordstrom et al., 1998). The increased risk associated with exposure to phenoxy herbicides (OR 1.65, 95% CI 1.16â2.34) was more strongly associated speciï¬- cally with exposure to MCPA (OR 2.62, 95% CI 1.40â4.88) than to 2,4-D and 2,4,5-T (OR 1.48, 95% CI 0.99â2.20), and the overall association with herbi- cides (OR 1.75, 95% CI 1.26â2.42) was stronger for âother herbicidesâ (OR 2.90, 95% CI 1.34â6.37). Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and MCPA. The SMR for death from NHL was not signiï¬cantly increased (15 cases; SMR 0.9, 95% CI 0.52â1.52). Reif et al. (1989) performed a series of caseâcontrol analyses on the sample of 19,904 people with speciï¬ed occupations among the 24,762 men 20 years old or older entered into the the New Zealand Cancer Registry from 1980 to 1984. The focus of their report was on the 134 for whom forestry work was the most recent occupation listed. For each type of cancer, people with any other type of cancer were used as controls. Of 535 people with NHL, seven had most recently been forestry workers (OR 1.84, 95% CI 0.85â3.97). Environmental Studies Hartge et al. (2005) conducted a population-based caseâcontrol study of NHL, identifying cases from four SEER registries (Iowa, Los Angeles County, Detroit, and Seattle) during the period 1998â2000. (The data were also addressed in Colt et al. [2005], and the study was reanalyzed by Lee et al. [2006].) Control subjects were frequency-matched to case subjects by age, sex, race, and SEER center. Two sampling frames were used to select control subjects: for cases 20â64 years old, random-digit dialing was used; for older subjects, Medicare ï¬les were used. The authors investigated residential exposure to pesticides and herbicides in detailed in-person interviews. They also analyzed carpet dust for pesticides. Response rates for cases were 59 percent and for controls 59 percent; responses yielded data on 1,321 cases and 1,057 controls. No associations with 2,4-D in carpet dust were found. In a subset of 100 cases and 100 control subjects whose serum concentrations were determined, De Roos et al. (2005) found a marginal association (p 0.06) with TEQs overall of PCBs, furans, and dioxins but not dioxins alone. Kato et al. (2004) conducted an incident, population-based, caseâcontrol study in upstate New York of women 20â79 years old who received a diagno- sis of NHL or died from it in 1995â1998. Case subjects were identiï¬ed in the New York state cancer registry, and linkages with state death certiï¬cates were conducted. Control subjects were selected from driverâs-license ï¬les (for people
456 VETERANS AND AGENT ORANGE: UPDATE 2006 under 65 years old) and Health Care Financing Administration records (for people at least 65 years old). Response rates were 56 percent for cases, 30 percent for controls identiï¬ed from driverâs-license ï¬les, and 67 percent for controls identi- ï¬ed from ï¬nancial records. Next of kin were interviewed as surrogate respondents (20.5 percent for cases and 3.2 percent for controls). The lack of comparability in interviewing subjects is a cause of concern. Subjects were asked about occu- pational and home use of herbicides and pesticides, and no associations were found with the use of the combination âherbicides/pesticides.â McDufï¬e et al. (2005) reported a reanalysis of data gathered in the Cross Canada Study of Pesticides and Health (McDufï¬e et al., 2001, as described in Update 2002). That caseâcontrol study identiï¬ed men with new diagnoses of NHL in 1991â1994 in cancer registries of six Canadian provinces and through active ascertainment; 513 were interviewed. Frequency matching by age and province was used in enrolling 1,506 control subjects. There was evidence of an association with any exposure to 2,4-D (OR 1.25, 95% CI 0.96â1.62) and any phenoxy herbicide (OR 1.45, 95% CI 1.13â1.87), although the excess risks posed by exposure to 2,4-D may have been due to concomitant exposure to DEET (OR 1.17, 95% CI 0.84â1.64). Vietnam-Veteran Studies In a follow-up of the CDC VES, Boehmer et al. (2004) compared the mortal- ity experience of US Vietnam veterans with that of non-veterans and did not ï¬nd an increased rate ratio for death from NHL (CRR 0.94, 95% CI 0.30â2.93). A set of three reports updating the health status of Australian Vietnam veter- ans noted negative associations between Vietnam service and NHL in comparing veterans with the general population of Australia with respect to incidence (SIR 0.67, 95% CI 0.55â0.79) (ADVA, 2005a) and mortality (SMR 0.78, 95% CI 0.60â0.96) (ADVA, 2005b). A separate study compared rates of NHL in deployed and non-deployed Vietnam veterans (ADVA, 2005c); the increases in incidence (RR 1.17, 95% CI 0.72â1.89) and mortality (RR 1.42, 95% CI 0.73â2.80) in the deployed did not approach signiï¬cance. Biologic Plausibility Increased rates of lymphoma have been reported in female B6C3F mice exposed to TCDD at 1 mg/kg of body weight via gavage twice a week for 2 years (NTP, 1982a). Subsequently, animal studies have not shown an increase in lymphoma in TCDD-exposed animals. The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter.
CANCER 457 Synthesis In previous VAO reports, the evidence was found to be sufï¬cient to support an association between exposure to at least one of the compounds of interest and NHL. Most of the evidence suggests that 2,4-D or 2,4,5-T, rather than TCDD, is responsible for the associations observed in occupational cohorts. For instance, the main cohorts with TCDD exposure, but not herbicide exposure, do not have increased rates of NHL. Some of the new reports of occupational and environ- mental studies (Chiu et al., 2004; Lee et al., 2004b; McDufï¬e et al., 2005; Mills et al., 2005) support the previous VAO committeeâs ï¬ndings, and others do not. Speciï¬cally, the newly reported papers from the US AHS (Alavanja et al., 2005; Blair et al., 2005a) do not provide speciï¬c information on the herbicides of interest, and there was no evidence of association in the New Zealand phenoxy herbicide producers and sprayers (ât Mannetje et al., 2005), although statistical power was extremely low in the latter small study. The UFW study showed a strong association between use of 2,4-D and NHL. The occupational caseâcontrol studies in New South Wales (Fritschi et al., 2005) showed a positive association, but the number of exposed cases was low. The pooled analyses of previously con- ducted caseâcontrol studies also suggested increased risks posed by exposure to herbicides. The American amd Australian Vietnam-veteran studies, in which there was no speciï¬c assessment of exposure, did not indicate that Vietnam veterans had higher rates of NHL than comparison populations. Conclusions On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is sufï¬cient evidence of an as- sociation between exposure to at least one of the compounds of interest and NHL. The evidence is drawn from occupational and other studies in which subjects were exposed to a variety of herbicides and herbicide components. HODGKINâS DISEASE Hodgkinâs disease (HD) (ICD-9 201) is distinct from NHL in its cell of ori- gin, its demographics, and its genetics. ACS estimated that 4,190 men and 3,610 women would receive diagnoses of HD in the United States in 2006 and that 770 men and 720 women would die from it (Jemal et al., 2006). The average annual incidence is shown in Table 6-43. The possibility that HD has an infectious etiology has been a topic of discus- sion since its earliest description. An increased incidence in people with a history of infectious mononucleosis has been observed in some studies, and a link with Epstein-Barr virus has been proposed. In addition to the occupational associations discussed below, higher rates of the disease have been observed in people who have suppressed or compromised immune systems.
458 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-43 Average Annual Incidence (per 100,000) of Hodgkinâs Disease in the United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black Men 2.8 3.0 3.1 2.7 2.6 3.5 3.6 3.8 2.5 Women 1.8 1.9 1.6 1.5 1.7 1.2 2.3 2.4 0.8 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. Conclusions from VAO and Updates The committee responsible for VAO determined that there was sufï¬cient information to support an association between exposure to the compounds of interest and HD. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-44 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. A JEM was applied to 58,162 individual work histories to estimate exposure to nonvolatile organochlorine compounds (which would include TCDD). Death from HD was signiï¬cantly increased in those who had ever been exposed to nonvolatile organochlorine compounds (n 17; SMR 1.76, 95% CI 1.02â2.82) but not in those who had never been exposed (n 7; SMR 0.58, 95% CI 0.23â1.19). Two reports from the US AHS (Alavanja et al., 2005; Blair et al., 2005a) found no excess risks of HD among pesticide applicators, commercial applica- tors, and their spouses, but the numbers of cases were very small. No results on any of the speciï¬c herbicides of interest were published (see Table 6-46). In their small cohort of New Zealand phenoxy herbicide producers and sprayers, ât Mannetje et al. (2005) found only one case of HD. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and MCPA. The esti- mated risk of HD was not signiï¬cantly increased (11 cases; SMR 0.95, 95% CI 0.47â1.69).
CANCER 459 TABLE 6-44 Selected Epidemiologic StudiesâHodgkinâs Disease Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., IARC cohort of pulp and paper workers 2006 Exposure to nonvolatile organochlorine compounds Never 7 0.6 (0.2â1.2) Ever 17 1.8 (1.0â2.8) Alavanja et al., US Agriculture Health Studyâincidence 2005 Private applicators (men and women) 11 0.9 (0.4â1.6) Spouses of private applicators ( 99% women) 4 0.7 (0.2â1.9) Commercial applicators (men and women) 1 0.8 (0.1â4.2) Blair et al., 2005a US Agriculture Health Study 3 1.1 (0.2â3.3) Private applicators (men and women) 3 1.7 (0.3â4.8) Spouses of private applicators ( 99% women) 0 0.0 (0.0â2.5) ât Mannetje et al., Phenoxy herbicide producers (men and women) 1 5.6 (0.1â31.0) 2005 Phenoxy herbicide sprayers ( 99% men) 0 0.0 (0.0â16.1) Torchio et al., Italian licensed pesticide users 11 1.0 (0.5â1.7) 1994 Studies Reviewed in Update 2004 Swaen et al., 2004 Dutch licensed herbicide applicators 0 â Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 1 1.5 (0.0â8.6) Studies Reviewed in Update 2000 Steenland et al., US chemical production workers (included in the 1999 IARC cohort and the NIOSH Dioxin Registry) 3 1.1 (0.2â3.2) Hooiveld et al., Dutch chemical production workers (included in 1998 the IARC cohort) 1 3.2 (0.1â17.6) Rix et al., 1998 Danish paper mill workersâincidence Men 18 2.0 (1.2â3.2) Women 2 1.1 (0.1â3.8) Studies Reviewed in Update 1998 Gambini et al., Italian rice growers 1 0.7 (0.0â3.6) 1997 Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 10 1.0 (0.5â1.8) Exposed to TCDD (or higher-chlorinated dioxins) 8 1.3 (0.6â2.5) Not exposed to TCDD (or higher- chlorinated dioxins) 1 0.3 (0.0â1.5) Becher et al., 1996 German production workers (included in the IARC cohort) 0 â continued
460 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-44 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Ramlow et al., Dow pentachlorophenol production workers 1996 (included in the IARC cohort and the NIOSH Dioxin Registry) 0 â Waterhouse et al., Residents of Tecumseh, Michigan 13 2.0 (1.1â3.4) 1996 Studies Reviewed in Update 1996 Asp et al., 1994 Finnish herbicide applicators 2 1.7 (0.2â6.0) Blair et al., 1993 US farmers in 23 states 56 1.0 (0.8â1.3) Kogevinas et al., IARC cohortâincidence, women 1 * 1993 Persson et al., Swedish NHL patientsâexposure to phenoxy 5 7.4 (1.4â40.0)d 1993 herbicides Kogevinas et al., IARC cohort (men and women) 3 0.6 (0.1â1.7) 1992 Studies Reviewed in VAO Eriksson and Swedish Cancer Registry patients Karlsson, 1992 Sawmill workers 10 2.2* Farmers 97 1.2* Forestry workers 35 1.2* Horticulture workers 11 1.2* Ronco et al., 1992 Danish workersâincidence Menâself-employed 27 0.6 (p 0.05) employee 13 1.0 (*) Womenâself-employed 1 1.1 (*) employee 1 1.2 (*) family worker 9 0.9 (*) Swaen et al., 1992 Dutch licensed herbicide applicators 1 3.3 (0.04â18.6) Fingerhut et al., NIOSH cohortâentire cohort 3 1.2 (0.3â3.5) 1991 1-year exposure, 20-year latency 1 2.8 (0.1â15.3) Green, 1991 Ontario herbicide sprayers 0 * Saracci et al., IARC cohortâexposed subcohort (men and 1991 women) 2 0.4 (0.1â1.4) Zober et al., 1990 BASF employeesâbasic cohort 0 * Alavanja et al., 1989 USDA forest or soil conservationists 4 2.2 (0.6â5.6) LaVecchia et al., Residents of the Milan, Italy, area (men and 1989 women) Agricultural occupations * 2.1 (1.0â3.8) Chemical industry occupations * 4.3 (1.4â10.2) Persson et al., Orebro (Sweden) Hospital patients (men and 1989 women) Farming 6 1.2 (0.4â3.5)d Exposed to phenoxy acids 4 3.8 (0.7â21.0)d Wiklund et al., Swedish pesticide applicators 15 1.5 (0.8â2.4) 1989b
CANCER 461 TABLE 6-44 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Alavanja et al., USDA agricultural extension agents 1988 PMR analysis 6 2.7 (1.2â6.3) Caseâcontrol analysis 6 1.1 (0.3â3.5) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 1 2.7 (0.0â14.7) Dubrow et al., Hancock County, Ohio residentsâfarmers 3 2.7* 1988 Wiklund et al., Swedish agricultural and forestry workers (men 1988 and women) Workers in land or animal husbandry 242 1.0 (0.9â1.2) Workers in silviculture 15 2.3 (1.3â3.7) Hoar et al., 1986 Kansas residents All farmers 71 0.8 (0.5â1.2) Using herbicides (phenoxy acids and others) 28 0.9 (0.5â1.5) Using herbicides 20 days/year 3 1.0 (0.2â4.1) Using herbicides 15 years 10 1.2 (0.5â2.6) Pearce et al., 1985 New Zealand residents with agricultural occupations, ages 20â64 107 1.1 (0.6â2.0) Hardell and Umea (Sweden) Hospital patientsâincidence Bengtsson, 1983 Exposed to phenoxy acids 14 5.0 (2.4â10.2) Exposed to high-grade chlorophenols 6 6.5 (2.2â19.0) Exposed to low-grade chlorophenols 5 2.4 (0.9â6.5) Wiklund, 1983 Swedish male and female agricultural workersâincidence 226 1.0 (0.9â1.2)e Riihimaki et al., Finnish herbicide applicators 0 * 1982 Burmeister, 1981 Iowa farmers 47 1.2 (NS) Hardell et al., Umea (Sweden) Hospital patientsâincidence 1981 Exposed to phenoxy acids 41 4.8 (2.9â8.1)f Exposed to chlorophenols 50 4.3 (2.7â6.9)f ENVIRONMENTAL New Studies Pahwa et al., 2006 Canadian men ( 19 years of age) from 1 of 6 Canadian provinces Any phenoxy herbicide 65 1.0 (0.7â1.4) 2,4-D 57 1.0 (0.7â1.4) Mecoprop 20 1.3 (0.7â2.2) MCPA 11 1.2 (0.6â2.6) Studies Reviewed in Update 2000 Bertazzi et al., Seveso residentsâ20-year follow-up 2001 Zone A, Bâmen 2 2.6 (0.6â10.9) women 2 3.7 (0.9â16.0) continued
462 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-44 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Schreinemachers, Rural or farm residents of Minnesota, Montana, 2000 and North and South Dakota Menâcounties with high wheat acreage 14 0.8 (0.4â1.5) medium wheat acreage 32 1.8 (1.1â2.9) Womenâcounties with high wheat acreage 14 0.9 (0.4â1.7) medium wheat acreage 19 1.0 (0.6â1.9) Viel et al., 2000 Residents around a French municipal solid-waste incineratorâincidence 9 1.5 (NS) Studies Reviewed in Update 1998 Bertazzi et al., Seveso residentsâ15-year follow-up 1997 Zone Bâmen 2 3.3 (0.4â11.9) women 2 6.5 (0.7â23.5) Zone Râwomen 4 1.9 (0.5â4.9) Studies Reviewed in Update 1996 Bertazzi et al., Seveso residentsâ10-year follow-upâincidence 1993 Zone Bâmen 1 1.7 (0.2â12.8) women 1 2.1 (0.3â15.7) Zone Râmen 4 1.1 (0.4â3.1) women 3 1.0 (0.3â3.2) VIETNAM VETERANS New Studies ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 51 2.1 (1.5â2.6) Navy 7 1.3 (0.5â2.6) Army 40 2.3 (1.6â3.0) Air Force 4 2.1 (0.6â5.3) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 13 0.9 (0.5â1.5) Navy 2 0.6 (0.1â2.1) Army 11 1.1 (0.5â1.9) Air Force 0 0.0 (0.0â2.9) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 12 0.9 (0.4â2.0) Mortality 4 1.7 (0.3â11.8) Boehmer et al., Vietnam Experience Cohort 2 0.9 (*) 2004
CANCER 463 TABLE 6-44 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 2004 Akhtar et al., 2004 White Air Force Ranch Hand veterans Lymphopoietic leukemia Ranch Hand Veteransâincidence 10 0.9 (0.4â1.5) Comparison Air Force Veteransâincidence 9 0.6 (0.3â1.0) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 1 0.3 (0.0â3.2) Studies Reviewed in Update 1998 Watanabe and Marine Vietnam veterans 25 1.9 (1.2â2.7) Kang, 1996 Studies Reviewed in Update 1996 Visintainer et al., Michigan Vietnam veterans 20 1.1 (0.7â1.8) 1995 Studies Reviewed in VAO Watanabe et al., Army Vietnam veterans 1991 vs Army non-Vietnam veterans 116 1.0 (*) vs all non-Vietnam veterans 116 1.1 (*) Marine Vietnam veterans vs Marine non-Vietnam veterans 25 1.9 (*) vs all non-Vietnam veterans 25 1.0 (*) CDC, 1990a US men born 1921â1953 Vietnam veterans 28 1.2 (0.7â2.4) Army 12 1.0 (0.5â2.0) Marine 4 1.7 (0.5â5.9) Air Force 5 1.7 (0.6â4.9) Navy 7 1.1 (0.4â2.6) Michalek et al., Air Force Ranch Hand veteran mortality 0 â* 1990; Wolfe et al., 1990 Breslin et al., 1988 Army Vietnam veterans compared with Vietnam- era Army veterans 92 1.2 (0.7â1.9) Marine Vietnam veterans compared with Marine Vietnam-era veterans 22 1.3 (0.7â2.6) Boyle et al., 1987 Vietnam Experience Study 0 â* Fett et al., 1987 Australian Vietnam veterans 0 â* Anderson et al., Wisconsin Vietnam veterans 4 â* 1986b Holmes et al., West Virginia Vietnam veterans compared with 1986 West Virginia Vietnam-era veterans 5 8.3 (2.7â19.5) continued
464 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-44 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Lawrence et al., New York Vietnam veterans compared with 1985 New York Vietnam-era veterans 10e 1.0 (0.4â2.2)g ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Vet- erans Affairs; AFHS, Air Force Health Study; CDC, Centers for Disease Control and Prevention; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; NHL, Non-Hodgkinâs Lymphoma; NIOSH, National Institute for Occupational Safety and Health; NS, not signiï¬cant; PMR, proportionate-mortality ratio; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d 90% CI. e 99% CI. f Includes both NHL and HD. g Includes both lymphoma and HD. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts. Environmental Studies In the Cross Canada Study of Pesticides and Health, Pahwa et al. (2006) investigated the possibility of an association between exposure to phenoxy herbi- cides and other pesticides and HD. Interviews were conducted with 316 men with newly diagnosed HD in 1991â1994, and their exposures were compared with those of 1,506 control subjects. No associations were found with any exposure to phenoxy herbicides (OR 0.99, 95% CI 0.70â1.38), 2,4-D (OR 0.96, 95% CI 0.67â1.37), mecoprop (OR 1.26, 95% CI 0.72â2.21), or MCPA (OR 1.24, 95% CI 0.60â2.60). Vietnam-Veteran Studies In an update of mortality in the cohorts of the CDC VES through 2000, Boehmer et al. (2004) reported two deaths from HD in deployed veterans and two in non-deployed veterans. A set of three reports updating the health status of Australian Vietnam veter- ans noted a signiï¬cant association of service in Vietnam with HD in comparing male veterans with the general population of Australia with respect to incidence (SIR 2.05, 95% CI 1.49â2.61) (ADVA, 2005a) but not mortality (SMR 0.89, 95% CI 0.46â1.49) (ADVA, 2005b). In another analysis comparing rates of HD in deployed and non-deployed Vietnam veterans (ADVA, 2005c), the incidence
CANCER 465 rate ratio was 0.90 (95% CI 0.39â1.97), and the mortality rate ratio was 1.72 (95% CI 0.29â11.77). Biologic Plausibility No animal studies have shown an association between exposure to the com- pounds of interest and HD. It is not clear whether true HD even develops in rats and mice. The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis The relative rarity of HD complicates the evaluation of epidemiologic stud- ies that address it. However, earlier studies carried out in Sweden (for example, the work of Hardell and colleagues) were well conducted and included excellent characterization of exposure. The committee believes that the small amount of additional information in the present report does not contradict these ï¬ndings, especially given that most studies had low statistical power. Although it has not been demonstrated as clearly as for NHL, a positive association between the com- pounds of interest and the development of HD is biologically plausible because of their common lymphoreticular origin and common risk factors. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is sufï¬cient evidence of an asso- ciation between exposure to at least one of the compounds of interest and HD. MULTIPLE MYELOMA Multiple myeloma (ICD-9 203.0) is characterized by the proliferation of bone marrow stem cells that results in an excess of neoplastic plasma cells and in the production of excess abnormal proteins, usually fragments of immuno- globulins. Multiple myeloma is sometimes grouped with other immunoprolifera- tive neoplasms (ICD-9 203.8). ACS estimated that 9,250 men and 7,320 women would receive diagnoses of multiple myeloma in the United States in 2006 and that 5,680 men and 5,630 women would die from it (Jemal et al., 2006). The average annual incidence of multiple myeloma is shown in Table 6-45. The incidence of multiple myeloma is highly age-dependent, with a rela- tively low rate in people under 40 years old. The incidence is slightly higher in men than in women, and the difference becomes more pronounced with age. An increased incidence of multiple myeloma has been observed in several occupational groups, including farmers and other agricultural workers and those
466 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-45 Average Annual Incidence (per 100,000) of Multiple Myeloma in the United Statesa 50â54 Years of Age 55â59 Years of Age 64 Years of Age All All All Races White Black Races White Black Races White Black Men 7.0 6.3 15.2 11.4 10.3 26.5 17.9 17.3 32.5 Women 4.8 4.0 12.6 8.2 7.5 15.2 12.2 10.3 29.9 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. with workplace exposure to rubber, leather, paint, and petroleum (Riedel et al., 1991). People with high exposure to ionizing radiation and those who suffer from other plasma-cell diseases, such as monoclonal gammopathy of unknown signiï¬cance or solitary plasmacytoma, are also at greater risk. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was limited or suggestive evidence of an association between exposure to the compounds of interest and multiple myeloma. Additional information available to the commit- tees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-46 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. A JEM was applied to individual work histories to estimate exposure to nonvolatile organochlorine compounds (which would include TCDD). Multiple myeloma was not more strongly associated with hav- ing ever been exposed to nonvolatile organochlorine compounds (n 20; SMR 1.07, 95% CI 0.66â1.66) than with having never been exposed (n 21; SMR 0.83, 95% CI 0.51â1.27). Two reports from the US AHS (Alavanja et al., 2005; Blair et al., 2005a) provided ï¬ndings on multiple myeloma in pesticide applicators, commercial applicators, and their spouses, but no results on any of the speciï¬c herbicides under consideration were published. A higher incidence of multiple myeloma than expected was found in private applicators (43 cases; SIR 1.34, 95% CI 0.97â1.81) (Blair et al., 2005a).
CANCER 467 TABLE 6-46 Selected Epidemiologic StudiesâMultiple Myeloma Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., IARC cohort of pulp and paper workers 2006 Exposure to nonvolatile organochlorine compounds Never 21 0.8 (0.5â1.3) Ever 20 1.1 (0.7â1.7) Alavanja et al., US Agriculture Health Studyâincidence 2005 Private applicators (men and women) 43 1.3 (1.0â1.8) Spouses of private applicators ( 99% women) 13 1.1 (0.6â1.9) Commercial applicators (men and women) 0 0.0 (0.0â2.7) Blair et al., 2005a US Agriculture Health Study Private applicators (men and women) 11 0.6 (0.3â1.2) Spouses of private applicators ( 99% women) 5 0.9 (0.3â2.1) ât Mannetje et al., Phenoxy herbicide producers (men and women) 3 5.5 (1.1â16.1) 2005 Phenoxy herbicide sprayers ( 99% men) 0 0.0 (0.0â5.3) Torchio et al., Italian licensed pesticide users 5 0.4 (0.1â1.0) 1994 Reif et al., 1989 New Zealand forestry workersânested caseâcontrol (incidence) 1 0.5 (0.1â3.7) Studies Reviewed in Update 2004 Swaen et al., 2004 Dow chemical production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 3 2.1 (0.4â6.1) Studies Reviewed in Update 2002 Burns et al., 2001 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 1 0.8 (0.0â4.5) Thörn et al., 2000 Swedish lumberjacks exposed to phenoxyacetic herbicidesâincidence 0 â Studies Reviewed in Update 2000 Steenland et al., US chemical production workers (included in the 1999 IARC cohort and the NIOSH Dioxin Registry) 10 2.1 (1.0â3.8) Hooiveld et al., Dutch phenoxy herbicide workers (included in 1998 the IARC cohort) 0 0.0* Studies Reviewed in Update 1998 Gambini et al., Italian rice growers 0 â* 1997 Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 17 1.3 (0.8â2.1) Exposed to TCDD (or higher-chlorinated dioxins) 9 1.2 (0.6â2.3) Not exposed to TCDD (or higher- chlorinated dioxins) 8 1.6 (0.7â3.1) continued
468 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-46 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Becher et al., German production workers (included in the 1996 IARC cohort) Plant I 3 5.4 (1.1â15.9) Studies Reviewed in Update 1996 Asp et al., 1994 Finnish herbicide applicators Incidence 2 1.5 (0.2â5.2) Mortality 3 2.6 (0.5â7.7) Dean, 1994 Irish farmers and farm workers (men and women) Men 171 1.0* Semenciw et al., Farmers in Canadian prairie provinces 160 0.8 (0.7â1.0) 1994 Blair et al., 1993 US farmers in 23 states 413 1.2 (1.0â1.3) Brown et al., 1993 Iowa residents who used pesticides or herbicides 111 1.2 (0.8â1.7) Lynge, 1993 Danish production workersâupdated incidence (included in the IARC cohort) Men 0 * Women 2 12.5 (1.5â45.1) Zahm et al., 1992 Eastern Nebraska users of herbicides Men 8 0.6 (0.2â1.7) Women 10 2.3 (0.8â7.0) Eastern Nebraska users of insecticides Men 11 0.6 (0.2â1.4) Women 21 2.8 (1.1â7.3) Studies Reviewed in VAO Eriksson and Residents of northern Sweden 20 2.2 (1.2â4.7)d Karlsson, 1992 Swaen et al., 1992 Dutch herbicide applicators 3 8.2 (1.6â23.8) Fingerhut et al., NIOSH cohortâentire cohort 5 1.6 (0.5â3.9) 1991 1-year exposure, 20-year latency 3 2.6 (0.5â7.7) Saracci et al., IARC cohortâexposed subcohort (men and 1991 women) 4 0.7 (0.2â1.8) Alavanja et al., USDA forest or soil conservationists 6 1.3 (0.5â2.8) 1989 Boffetta et al., ACS Prevention Study II subjects 12 2.1 (1.0â4.2) 1989 Farmers using herbicides or pesticides 8 4.3 (1.7â10.9) LaVecchia et al., Residents of the Milan, Italy, area (men and 1989 women) Agricultural occupations * 2.0 (1.1â3.5) Morris et al., 1986 Residents of four SEER areas 2.9 (1.5â5.5) Pearce et al., 1986 New Zealand residentsâagricultural sprayers Use of agricultural spray 16 1.3 (0.7â2.5) Likely sprayed 2,4,5-T 14 1.6 (0.8â3.1) Cantor and Blair, Wisconsin residentsâfarmers in counties with 1984 highest herbicide use * 1.4 (0.8â2.3)
CANCER 469 TABLE 6-46 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Burmeister et al., Iowa residentsâfarming exposures 1983 Born 1890â1900 * 2.7 (p 0.05) Born after 1900 * 2.4 (p 0.05) Riihimaki et al., Finnish herbicide applicators 1 (0.2 expected) 1982 ENVIRONMENTAL New Studies Pahwa et al., 2006 Canadian men ( 19 years of age) from 1 of 6 Canadian provinces Any phenoxy herbicide 62 1.2 (0.8â1.8) 2,4-D 59 1.3 (0.9â1.9) Mecoprop 16 1.2 (0.7â2.8) MCPA 7 0.5 (0.2â1.2) Studies Reviewed in Update 2000 Bertazzi et al., Seveso residentsâ20-year follow-up 2001 Zone A, Bâmen 1 0.6 (0.1â4.3) women 4 3.2 (1.2â8.8) Schreinemachers, Rural or farm residents of Minnesota, Montana, 2000 and North and South Dakota Menâcounties with high wheat acreage 75 0.8 (0.6â1.0) medium wheat acreage 108 1.0 (0.8â1.3) Womenâcounties with high wheat acreage 77 1.0 (0.7â1.3) medium wheat acreage 91 1.0 (0.8â1.3) Studies Reviewed in Update 1998 Bertazzi et al., Seveso residentsâ15-year follow-up 1997 Zone Bâmen 1 1.1 (0.0â6.2) women 4 6.6 (1.8â16.8) Zone Râmen 5 0.8 (0.3â1.9) women 5 1.0 (0.3â2.3) Studies Reviewed in Update 1996 Bertazzi et al., Seveso residentsâ10-year follow-upâincidence 1993 Zone Bâmen 2 3.2 (0.8â13.3) women 2 5.3 (1.2â22.6) Zone Râmen 1 0.2 (0.0â1.6) women 2 0.6 (0.2â2.8) Studies Reviewed in VAO Pesatori et al., Seveso residentsâincidence 1992 Zones A, Bâmen 2 2.7 (0.6â11.3) women 2 4.4 (1.0â18.7) Zone Râmen 1 0.2 (0.0â1.5) women 3 0.9 (0.3â3.1) VIETNAM VETERANS New Studies Boehmer et al., Vietnam Experience Cohort 1 0.4 (*) 2004 continued
470 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-46 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c ADVA, 2005a Australian male Vietnam veterans vs Australian populationâincidence 31 0.7 (0.437â0.9) Navy 4 0.4 (0.1â1.0) Army 21 0.7 (0.4â1.0) Air Force 6 1.1 (0.4â2.4) ADVA, 2005b Australian male Vietnam veterans vs Australian populationâmortality 24 0.9 (0.5â1.2) Navy 3 0.5 (0.1â1.5) Army 15 0.8 (0.4â1.3) Air Force 6 1.7 (0.6â3.6) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veteransâdeployed vs non-deployed Incidence 8 2.1 (0.7â6.0) Mortality 5 0.9 (0.2â3.4) Studies Reviewed in Update 2004 Akhtar et al., 2004 White Air Force Vietnam Veterans Lymphopoetic leukemia Ranch Hand Veteransâincidence 10 0.9 (0.4â1.5) Comparison Air Force Veteransâincidence 9 0.6 (0.3â1.0) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 2 0.7 (0.1â5.0) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 6 0.6 (0.2â1.3) CDVA, 1997b Australian military Vietnam veterans 0 Watanabe and Army Vietnam veterans 36 0.9* Kang, 1996 Marine Vietnam veterans 4 0.6* Studies Reviewed in VAO Breslin et al., Army Vietnam veterans 18 0.8 (0.2â2.5) 1988 Marine Vietnam veterans 2 0.5 (0.0â17.1) ABBREVIATIONS: 2,4-D, 2,4-dichlorophenoxyacetic acid; ACS, American Cancer Society; ADVA, Australian Department of Veterans Affairs; AFHS, Air Force Health Study; CI, conï¬dence interval; IARC, International Agency for Research on Cancer; NIOSH, National Institute for Occupational Safety and Health; SEER, Surveillance, Epidemiology, and End Results program; TCDD, 2,3,7,8- tetrachlorodibenzo-p-dioxin; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. d 90% CI. * Information not provided by study authors. â Denoted by a dash in the original study. Studies in italics have been superseded by newer studies of the same cohorts.
CANCER 471 In the cohort study of New Zealand phenoxy herbicide producers and spray- ers (ât Mannetje et al., 2005), the sole signiï¬cant ï¬nding reported was higher mortality from multiple myeloma among producers than expected (three deaths; SMR 5.51, 95% CI 1.14â16.1). No deaths from multiple myeloma were ob- served in the sprayers. Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics reports as having high herbicide use, especially of 2,4-D and MCPA. The esti- mated risk of multiple myeloma was signiï¬cantly reduced (ï¬ve cases; SMR 0.42, 95% CI 0.14â0.99). The authors suggested that the relatively short dura- tion of follow-up and the healthy-worker effect contributed to the observation of reduced mortality. Reif et al. (1989) performed a series of caseâcontrol analyses of the sample of 19,904 people with speciï¬ed occupations among the 24,762 men 20 years old or older entered into the the New Zealand Cancer Registry in 1980â1984. Their focus was on the 134 for whom forestry work was the most recent occupation listed. For each type of cancer, the people with any other type of cancer were used as controls. Of 295 people with multiple myeloma, only one had most recently been a forestry worker (OR 0.53, 95% CI 0.08â3.72). Environmental Studies In a caseâcontrol study of 342 men with new diagnoses of multiple myeloma in 1991â1994 and 1,506 controls in six Canadian provinces, Pahwa et al. (2006) investigated whether exposure to phenoxy herbicides and other pesticides was associated with multiple myeloma. Suggestions of positive associations were found with any exposure to phenoxy herbicides (OR 1.25, 95% CI 0.93â1.68) or 2,4-D (OR 1.21, 95% CI 0.89â1.65), but the conï¬dence intervals all included unity; a 66% increase in incidence was found in association with exposure to mecoprop (OR 1.66, 95% CI 1.02â2.71); and no association was found in asso- ciation with exposure to MCPA (OR 0.71, 95% CI 0.32â1.58). In analyses of the subset of subjects who worked or lived on farms, the association with expo- sure to those phenoxy herbicides was similar, but the association with mecoprop was reduced (OR 1.21, 95% CI 0.65â2.27). Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported one death from multiple myeloma in deployed veterans and one in non- deployed veterans. A set of three reports updating the health status of Australian Vietnam vet- erans noted no associations between Vietnam service and multiple myeloma in comparing veterans with the general population of Australia with respect to inci- dence (SIR 0.66, 95% CI 0.43â0.90) (ADVA, 2005a) or mortality (SMR 0.86,
472 VETERANS AND AGENT ORANGE: UPDATE 2006 95% CI 0.52â1.20) (ADVA, 2005b). A separate study compared the rates of multiple myeloma in deployed and non-deployed Vietnam veterans (ADVA, 2005c); the incidence of multiple myeloma in deployed veterans was increased (RR 2.19, 95% CI 0.76â5.98), but mortality from multiple myeloma was not increased (RR 0.90, 95% CI 0.22â3.29). Biologic Plausibility No animal studies have reported an association between exposure to the compounds of interest and multiple myeloma. The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis The study by ât Mannetje et al. (2005) of an occupational group in New Zea- land that was involved in the production of phenoxy herbicides and the US AHS (Alavanja et al., 2005) showed higher than expected risks of multiple myeloma. The main limitation of the report of the US AHS is that it did not present ï¬ndings on any of the compounds of interest, although subjects in the study were indeed exposed to 2,4-D. An environmental caseâcontrol study in Canada suggested small excess risks, but the conï¬dence intervals were broad. Recent studies of Australian Vietnam veterans suggested a higher risk of multiple myeloma in male Army veterans deployed to Vietnam than in their non-deployed counterparts. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is limited or suggestive evidence of an association between exposure to at least one of the compounds of interest and multiple myeloma. AL AMYLOIDOSIS The committee has moved the section on AL amyloidosis from its position in previous VAO updates, where it was grouped with a variety of non-neoplastic health conditions, to put it closer to related conditions, such as multiple myeloma and some types of B-cell lymphoma. The conditions share several biologic fea- tures, most notably clonal hyperproliferation of B-cell-derived plasma cells and production of abnormal amounts of immunoglobulins. The primary feature of amyloidosis (ICD-9 277.3) is the accumulation and deposition in various tissues of insoluble protein, historically termed amyloid. A wide spectrum of disease can stem from this; excessive amyloid protein can have limited clinical consequences or can produce severe, rapidly progressive
CANCER 473 multiple-organ-system dysfunction. Annual incidence is estimated at 1/100,000; there are about 2,000 new cases each year in the United States. Amyloidosis occurs mainly in people 50 70 years old and occurs more often in men than in women (Solomon, 1999). Amyloid protein accumulates in the extracellular spaces of various tissues, often affecting multiple organ systems. The pattern of organ involvement depends on the nature of the protein; some amyloid proteins are more ï¬brillogenic than others. Amyloidosis is classiï¬ed according to the biochemical properties of the ï¬bril-forming protein, with the letter A (for amyloid) as the ï¬rst designation. AL amyloidosis is the most common form of amyloidosis; the L indicates that the amyloid protein is derived from immunoglobin light chains. That links AL amy- loidosis with other B-cell disorders that involve overproduction of immunoglobin, such as multiple myeloma and some types of B-cell lymphomas. AL amyloidosis results from the abnormal overproduction of immunoglobu- lin light chain protein from a monoclonal population of plasma cells. Clinical ï¬ndings can include excessive AL protein or immunoglobulin fragments in the urine or serum, renal failure with nephrotic syndrome, liver failure with hepato- megaly, heart failure with cardiomegaly, marcroglossia, carpal tunnel syndrome, and peripheral neuropathy. Bone marrow biopsies commonly show an increased density of plasma cells, suggesting a premalignant state. Historically, that test emphasized routine histochemical analysis, but modern immunocytochemistry and ï¬ow cytometry now commonly identify monoclonal populations of plasma cells with molecular techniques. AL amyloidosis can progress rapidly and is often far advanced by the time it is diagnosed (Buxbaum, 2004). Conclusions from VAO and Updates The VA identiï¬ed AL amyloidoisis as of concern after the publication of Update 1998. AL amyloidosis was considered by the committees responsible for Update 2000, Update 2002, and Update 2004. Those committees concluded that there was inadequate or insufï¬cient evidence to determine whether there is an as- sociation between exposure to the compounds of interest and AL amyloidosis. Update of the Epidemiologic Literature Because it is a rare condition, there is little epidemiologic literature speciï¬- cally on AL amyloidosis. Cohen et al. (2004) describe a series of six patients with AL amyloidosis in association with NHL; risk could not be estimated, because the study design did not include a control group for comparison, but the report indicates that the two conditions are closely related. Rajkumar et al. (2006) review the relationship between AL amyloidosis and other plasma cell disorders. They describe AL amyloidosis as a clonal plasma cell disorder characterized by low tumor burden but profound multisystemic disease.
474 VETERANS AND AGENT ORANGE: UPDATE 2006 No new occupational, environmental, or Vietnam-veteran studies concerning exposure to the compounds of interest and amyloidosis of any sort were published since Update 2004. Biologic Plausibility A 1979 study reported AL amyloidosis in association with chronic skin le- sions in Swiss mice after chronic exposure to TCDD (Toth et al., 1979). That ï¬nding has not been reported in later studies of TCDD carcinogenicity in mice or rats. The observation of common chromosomal abnormalities in AL amyloidosis and multiple myeloma (Harrison et al., 2002) and of âprogressionâ from AL amyloidosis to multiple myeloma (Rajkumar et al., 1998) support the biologic plausibility of linking AL amyloidosis with multiple myeloma. It is known that AL amyloidosis is associated with B-cell diseases and roughly 15â20 percent of the time it occurs with multiple myeloma. Other diagnoses associated with AL amyloidosis include B-cell lymphomas (Cohen et al., 2004), monoclonal gammopathies, agammaglobulinemia, and monoclonal gammopathy of undetermined signiï¬cance (Rajkumar et al., 2006). Thus, AL amyloidosis can result from such medical conditions as multiple myeloma and B-cell lymphomas for which there is evidence of association with exposure to the compounds of interest. Synthesis AL amyloidosis is a very rare condition, and it is not likely that popula- tion-based epidemiology will ever provide substantial direct evidence regarding its causation. However, the biologic and pathophysiologic features linking AL amyloidosis, multiple myeloma, and some types of B-cell lymphomasâmost notably clonal hyperproliferation of plasma cells and abnormal immunoglobulin productionâindicate that AL amyloidosis is pathophysiologically related to those conditions. Conclusion On the basis of its evaluation of the evidence reviewed here and in previ- ous VAO reports, the committee concludes that there is limited or suggestive evidence of an association between exposure to the compounds of interest and AL amyloidosis. LEUKEMIA There are four primary types of leukemia (ICD-9 202.4, 203.1, 204.0â204.9, 205.0â205.9, 206.0â206.9, 207.0â207.2, 207.8, 208.0â208.9): acute and chronic
CANCER 475 lymphocytic leukemia and acute and chronic myelogenous (or granulocytic) leukemia. Acute myelogenous leukemia (ICD-9 205) is also commonly called acute myeloid leukemia or acute nonlymphocytic leukemia. There are numerous subtypes of AML; for consistency, the present report uses acute myelogenous leukemia, or AML, regardless of designations in the source materials. ACS estimated that 20,000 men and 15,070 women would receive diagnoses of some form of leukemia in the United States in 2006 and that 12,470 men and 9,810 women would die from it (Jemal et al., 2006). Collectively, leukemia was expected to account for 2.5 percent of all new diagnoses of cancer and 3.9 percent of deaths from cancer in 2006. The different forms of leukemia have different patterns of incidence and, in some cases, different risk factors. The incidences of the various forms of leukemia are presented in Table 6-47. In adults, acute leukemia is nearly always in the form of AML; see the mate- rial below speciï¬cally about AML for more background information about this hematopoietic neoplasm. TABLE 6-47 Average Annual Incidence (per 100,000) of Leukemias in the United Statesa 50â54 Years of Age 55â59 Years of Age 60â64 Years of Age All All All Races White Black Races White Black Races White Black All Leukemias Men 12.6 12.8 11.3 21.0 22.3 16.6 32.8 34.2 26.5 Women 7.8 8.0 5.9 12.0 12.2 10.7 17.5 18.6 11.7 Acute Lymphocytic Leukemia Men 1.0 1.0 1.2 1.0 1.0 1.1 1.5 1.4 1.0 Women 0.7 0.6 1.0 1.0 1.1 0.6 0.6 0.5 0.4 Acute Myeloid Leukemia Men 3.2 3.2 2.4 5.4 5.7 3.5 9.1 9.2 8.5 Women 2.8 2.8 1.6 4.3 4.2 3.6 5.8 5.8 5.6 Chronic Lymphocytic Leukemia Men 5.0 5.4 4.8 9.3 10.2 6.7 14.7 15.6 11.0 Women 2.0 2.2 1.0 4.1 4.5 3.0 6.4 7.3 2.0 Chronic Myeloid Leukemia Men 1.8 1.7 1.5 2.2 2.2 1.8 3.8 3.9 2.5 Women 1.2 1.3 1.0 1.3 1.3 1.5 2.4 2.5 1.2 All Other Leukemiab Men 0.4 0.3 0.2 0.8 0.6 2.5 1.2 1.3 1.5 Women 0.3 0.3 0.6 0.6 0.5 0.6 1.0 1.0 0.8 a SEER (Surveillance, Epidemiology, and End Results program) nine standard registries, crude age- speciï¬c rates, 1999â2003. b Includes leukemic reticuloendotheliosis (hairy-cell leukemia), plasma-cell leukemia, monocytic leukemia, and acute and chronic erythremia and erythroleukemia.
476 VETERANS AND AGENT ORANGE: UPDATE 2006 Acute lymphocytic leukemia (ALL) is a disease of the young and of people over 70 years old. It is relatively uncommon in the age groups that include most Vietnam veterans. The lifetime incidence of ALL is slightly higher in whites than in blacks and higher in men than in women. Exposure to high doses of ionizing radiation is a known risk factor for ALL, but there is little consistent evidence on other factors. CLL shares many traits with lymphomas (such as immunohistochemistry, B-cell origin, and progression to an acute, aggressive form of NHL), so the com- mittee reviews it below separately from the other leukemias. The incidence of chronic myelogenous leukemia (CML) increases steadily with age in people over 30 years old. Its lifetime incidence is roughly equal in whites and blacks and is slightly higher in men than in women. CML accounts for about one-ï¬fth of the cases of leukemia among people in the age groups that include most Vietnam veterans. It is associated with an acquired chromosomal abnormality known as the Philadelphia chromosome, for which exposure to high doses of ionizing radiation is a known risk factor. Little is known about the risk factors associated with other forms of leuke- mia. However, two human retroviruses have been linked to human leukemias: HTLV-1 appears to cause adult T-cell leukemia or lymphoma, and HTLV-2 has been linked to hairy-cell leukemia, but with less deï¬nitive data. Conclusions from VAO and Updates The committee responsible for VAO concluded that there was inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and leukemia. Additional information available to the committees responsible for Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004 did not change that conclusion. Table 6-48 summarizes the results of the relevant studies. Update of the Epidemiologic Literature Occupational Studies McLean et al. (2006) reported on a multinational IARC cohort of 60,468 pulp and paper industry workers. A JEM was applied to individual work histories to estimate exposure to nonvolatile organochlorine compounds (which would include TCDD). The occurrence of leukemia was not more strongly associated with having ever been exposed to nonvolatile organochlorine compounds (n 35; SMR 0.89, 95% CI 0.62â1.24) than with having never been exposed (n 49; SMR 0.95, 95% CI 0.70â1.26). Two reports of the US AHS (Alavanja et al., 2005; Blair et al., 2005a) pre- sented no results on any of the speciï¬c herbicides under consideration but noted
CANCER 477 TABLE 6-48 Selected Epidemiologic StudiesâLeukemia Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies McLean et al., IARC cohort of pulp and paper workers 2006 Exposure to nonvolatile organochlorine compounds Never 49 1.0 (0.7â1.3) Ever 35 0.9 (0.6â1.2) Alavanja et al., US Agriculture Health Studyâincidence 2005 Private applicators (men and women) 70 0.9 (0.7â1.2) Spouses of private applicators ( 99% women) 17 0.7 (0.4â1.2) Commercial applicators (men and women) 4 0.9 (0.3â2.4) Blair et al., US Agriculture Health Study 2005a Private applicators (men and women) 27 0.8 (0.5â1.1) Spouses of private applicators ( 99% women) 14 1.4 (0.8â2.4) Mills et al., 2005 Cohort study of 139,000 United Farm Workers, with nested caseâcontrol analyses restricted to Hispanic workers in California Ever used 2,4-D Total leukemia * 1.0 (0.4â2.6) Lymphocytic leukemia * 1.5 (0.3â6.6) Granulocytic (myelogenous) leukemia * 1.3 (0.3â5.4) ât Mannetje Phenoxy herbicide producers (men and women) 0 0.0 (0.0â5.3) et al., 2005 Phenoxy herbicide sprayers ( 99% men) (myelogenous leukemia) 1 1.2 (0.0â6.4) Hertzman et al., British Columbia sawmill worker with 1997 chlorophenate process (more hexa-, hepta-, and octa CDDs than TCDD), all leukemiasâincidence 47 1.2 (0.9â1.5) ALL 2 1.0 (0.2â3.1) CLL 24 1.7 (1.2â2.4) AML 5 0.8 (0.3â1.7) CML 7 1.1 (0.5â2.0) Other and unspeciï¬ed 5 0.5 (0.2â1.0) Torchio et al., Italian licensed pesticide users 27 0.8 (0.5â1.1) 1994 Reif et al., 1989 Caseâcontrol study on all men with occupation indicated entered into New Zealand Cancer Registry 1980â1984 (all leukemias) Forestry workers 4 1.0 (0.4â2.6) AML 3 2.2 (*) Studies Reviewed in Update 2004 Miligi et al., Caseâcontrol of residents of 11 areas in Italyâ 2003 incidence of leukemia excluding CLL Exposure to phenoxy herbicides 2.1 (0.7â6.2) Swaen et al., Dutch licensed herbicide applicatorsâmortality 3 1.3 (0.3â3.7) 2004 continued
478 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-48 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 2002 Burns et al., Dow 2,4-D production workers (included in the 2001 IARC cohort and the NIOSH Dioxin Registry) Lymphopoietic mortality in workers with high 2,4-D exposure 4 1.3 (0.4â3.3) Thörn et al., Swedish lumberjacks exposed to phenoxyacetic 2000 herbicides 0 â Studies Reviewed in Update 2000 Steenland et al., US chemical production workers (included in the 1999 IARC cohort and the NIOSH Dioxin registry) 10 0.8 (0.4â1.5) Hooiveld et al., Dutch chemical production workers (included in 1998 the IARC cohort) 1 1.0 (0.0â5.7) Rix et al., 1998 Danish paper mill workersâincidence Men 20 0.8 (0.5â1.2) Women 7 1.3 (0.5â2.7) Studies Reviewed in Update 1998 Gambini et al., Italian rice growers 4 0.6 (0.2â1.6) 1997 Kogevinas et al., IARC cohort (men and women) 1997 Workers exposed to any phenoxy herbicide or chlorophenol 34 1.0 (0.7â1.4) Exposed to TCDD (or higher-chlorinated dioxins) 16 0.7 (0.4â1.2) Not exposed to TCDD (or higher-chlorinated dioxins) 17 1.4 (0.8â2.3) Becher et al., German chemical production workers (included in 1996 the IARC cohort)âCohort I 4 1.8 (0.5â4.7) Ramlow et al., Dow pentachlorophenol production workers 1996 (included in the IARC cohort and the NIOSH Dioxin Registry) 0-year latency 2 1.0 (0.1â3.6) 15-year latency 1 â Waterhouse Residents of Tecumseh, Michiganâincidence et al., 1996 All leukemias Men 42 1.4 (1.0â1.9) Women 32 1.2 (0.9â1.8) CLL 10 1.4 (1.0â1.9) Amadori et al., Italian farming and animal-breeding workers 1995 Farmers 5 1.6 (0.5â5.2) Farmer-breeders 10 3.1 (1.1â8.3)
CANCER 479 TABLE 6-48 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 1996 Asp et al., 1994 Finnish herbicide applicators Mortality 2 (*) Lymphatic 1 0.9 (0.0â5.1) Myelogenous 1 0.7 (0.0â3.7) Incidence Lymphatic 3 1.0 (0.2â3.0) Semenciw et al., Farmers in Canadian prairie provinces 357 0.9 (0.8â1.0) 1994 Lymphatic 132 0.9 (0.8â1.1) Myelogenous 127 0.8 (0.7â0.9) Blair et al., 1993 US farmers in 23 states White men 1,072 1.3 (1.2â1.4) White women 24 1.5 (0.9â2.2) Kogevinas et al., IARC cohort (women only, myelogenous 1993 leukemia) 1 2.0 (0.2â7.1) Studies Reviewed in VAO Bueno de Dutch phenoxy herbicide workers (included in the Mesquita et al., IARC cohort) 1993 Leukemia and aleukemia (ICD-9 204â207) 2 2.2 (0.3â7.9) Myelogenous leukemia (ICD-8 205) 2 4.2 (0.5â15.1) Hansen et al., Danish gardenersâincidence 1992 All gardenersâCLL 6 2.5 (0.9â5.5) all other types of leukemia 3 1.2 (0.3â3.6) MenâCLL 6 2.8 (1.0â6.0) all other types of leukemia 3 1.4 (0.3â4.2) Ronco et al., Danish workersâincidence 1992 Menâself-employed 145 0.9 (*) employee 33 1.0 (*) Womenâself-employed 8 2.2 (p 0.05) employee 3 1.3 (*) family worker 27 0.9 (*) Fingerhut et al., NIOSHâentire cohort 6 0.7 (0.2â1.5) 1991 Saracci et al., IARC cohortâexposed subcohort (men and 1991 women) 18 1.2 (0.7â1.9) continued
480 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-48 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Brown et al., Caseâcontrol on white men in Iowa and 1990 Minnesota, all types of leukemiaâincidence 578 Ever farmed 335 1.2 (1.0â1.5) AML 81 1.2 (0.8â1.8) CML 27 1.1 (0.6â2.0) CLL 156 1.4 (1.1â1.9) ALL 7 0.9 (0.3â2.5) Myelodysplasias 32 0.8 (0.5â1.4) Any herbicide use 157 1.2 (0.9â1.6) AML 39 1.3 (0.8â2.0) CML 16 1.3 (0.7â2.6) CLL 74 1.4 (1.0â2.0) ALL 2 0.5 (0.1â2.2) Myelodysplasias 10 0.7 (0.3â1.5) Phenoxy acid use 120 1.2 (0.9â1.6) 2,4-D use 98 1.2 (0.9â1.6) 2,4,5-T use 22 1.3 (0.7â2.2) First use 20 years prior 11 1.8 (0.8â4.0) MCPA 11 1.9 (0.8â4.3) First use 20 years prior 5 2.4 (0.7â8.2) Wigle et al., 1990 Canadian farmers 138 0.9 (0.7â1.0) Zober et al., BASF employees at plant with 1953 explosion 1990 All 3 cohorts (n 247) 1 1.7* Cohort 3 1 5.2 (0.4â63.1) Incident case of AML in Cohort 1 Alavanja et al., USDA agricultural extension agents 23 1.9 (1.0â3.5) 1988 Lymphatic * 2.1 (0.7â6.4) Trend over years worked (p 0.01) Myelogenous * 2.8 (1.1â7.2) Trend over years worked (p 0.01) Bond et al., 1988 Dow 2,4-D production workers (included in the IARC cohort and the NIOSH Dioxin Registry) 2 3.6 (0.4â13.2)d Blair and White, 1,084 leukemia deaths in Nebraska 1957â1974 1985 Farmerâusual occupation on death certiï¬cate 1.3 (p 0.05) 99 ALLs * 1.3 (*) 248 CLLs * 1.7 (p 0.05) 105 unspeciï¬ed lymphatics * 0.9 (*) 235 AMLs * 1.2 (*) 96 CMLs * 1.1 (*) 39 unspeciï¬ed myelogenous * 1.0 (*) 39 acute monocytics * 1.9 (*) 52 acute unspeciï¬ed leukemias * 2.4 (*) 65 unspeciï¬ed leukemias * 1.2 (*)
CANCER 481 TABLE 6-48 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Burmeister et al., 1,675 leukemia deaths in Iowa 1968â1978 1982 Farmerâusual occupation on death certiï¬cate 1.2 (p 0.05) ALL 28 0.7 (0.4â1.2) CLL 132 1.7 (1.2â2.4) Lived in one of 33 counties with highest herbicide use * 1.9 (1.2â3.1) Unspeciï¬ed lymphatic 64 1.7 (1.0â2.7) AML 86 1.0 (0.8â1.5) CML 46 1.0 (0.7â1.7) Unspeciï¬ed myelogenous 36 0.8 (0.5â1.4) Acute monocytic 10 1.1 (0.4â2.6) Unspeciï¬ed leukemia 31 1.1 (0.6â2.0) ENVIRONMENTAL Studies Reviewed in Update 2002 Revich et al., Residents of Chapaevsk, Russia 2001 Mortality standardized to Samara Region Men 11 1.5 (0.8â2.7) Women 15 1.5 (0.8â2.4) Studies Reviewed in Update 2000 Bertazzi et al., Seveso residentsâ20-year follow-up 2001 Zones A, Bâmen 9 2.1 (1.1â4.1) women 3 1.0 (0.3â3.0) Rural or farm residents of Minnesota, Montana, North Dakota, South Dakota Menâcounties with wheat acreage 23,000â110,999 246 1.0 (0.8â1.1) Menâcounties with wheat acreage 111,000 248 1.1 (1.0â1.3) Womenâcounties with wheat acreage 23,000â110,999 183 1.0 (0.8â1.2) Womenâcounties with wheat acreage 111,000 146 0.9 (0.8â1.2) Bertazzi et al., Seveso residentsâ15-year follow-up 1998 Zone Bâmen 7 3.1 (1.4â6.7) women 1 0.6 (0.1â4.0) Zone Râmen 12 0.8 (0.4â1.5) women 12 0.9 (0.5â1.6) Studies Reviewed in Update 1998 Bertazzi et al., Seveso residentsâ15-year follow-up 1997 Zone Bâmen 7 3.1 (1.3â6.4) women 1 0.6 (0.0â3.1) Zone Râmen 12 0.8 (0.4â1.4) women 12 0.9 (0.4â1.5) continued
482 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-48 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c Studies Reviewed in Update 1996 Swensson et al., Swedish ï¬shermen 1995 All leukemiasâmortality East coast (higher serum TEQs) 5 1.4 (0.5â3.2) West coast (lower serum TEQs) 24 1.0 (0.6â1.5) Lymphocyticâincidence East coast (higher serum TEQs) 4 1.2 (0.3â3.3) West coast (lower serum TEQs) 16 1.3 (0.8â2.2) Myelogenousâincidence East coast (higher serum TEQs) 2 0.9 (0.1â3.1) West coast (lower serum TEQs) 6 0.5 (0.2â1.1) Bertazzi et al., Seveso residentsâ10-year follow-upâincidence 1993 Zone Bâmen 2 1.6 (0.4â6.5) Myelogenous leukemia (ICD-9 205) 1 2.0 (0.3â14.6) women 2 1.8 (0.4â7.3) Myelogenous leukemia (ICD-9 205) 2 3.7 (0.9â15.7) Zone Râmen 8 0.9 (0.4â1.9) Myelogenous leukemia (ICD-9 205) 5 1.4 (0.5â3.8) women 3 0.4 (0.1â1.2) Myelogenous leukemia (ICD-9 205) 2 0.5 (0.1â2.1) Studies Reviewed in VAO Bertazzi et al., Seveso residentsâ10-year follow-up 1992 Zones A, B, Râmen 4 2.1 (0.7â6.9) women 1 2.5 (0.2â27.0) VIETNAM VETERANS New Studies ADVA, 2005a Australian Vietnam veterans vs Australian populationâincidence All branches 130 1.1 (1.0â1.4) Lymphocytic leukemia 72 1.4 (1.1â1.7) Myelogenous leukemia 54 1.0 (0.8â1.3) Navy 35 1.5 (1.0â2.0) Lymphocytic leukemia 14 1.3 (0.7â2.1) Myelogenous leukemia 19 1.7 (1.0â2.6) Army 80 1.1 (0.8â1.3) Lymphocytic leukemia 50 1.4 (1.0â1.8) Myelogenous leukemia 28 0.8 (0.5â1.1) Air Force 15 1.2 (0.7â2.0) Lymphocytic leukemia 8 1.4 (0.6â2.7) Myelogenous leukemia 7 1.3 (0.5â2.6)
CANCER 483 TABLE 6-48 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c ADVA, 2005b Australian Vietnam veterans vs Australian populationâmortality All branches 84 1.0 (0.8â1.3) Lymphocytic leukemia 24 1.2 (0.7â1.7) Myelogenous leukemia 55 1.1 (0.8â1.3) Navy 17 1.3 (0.8â1.8) Lymphocytic leukemia 4 0.2 (0.0â1.2) Myelogenous leukemia 11 1.6 (0.9â2.5) Army 48 0.1 (0.7â1.2) Lymphocytic leukemia 17 1.3 (0.7â2.0) Myelogenous leukemia 30 0.8 (0.5â1.1) Air Force 14 1.6 (0.8â2.6) Lymphocytic leukemia 6 2.7 (1.0â5.8) Myelogenous leukemia 8 1.3 (0.5â2.5) ADVA, 2005c Australian male conscripted Army National Service Vietnam-era veterans: deployed vs non-deployed Incidence 16 0.6 (0.3â1.1) Lymphocytic leukemia 9 0.8 (0.3â2.0) Myelogenous leukemia 7 0.5 (0.2â1.3) Mortality 11 0.6 (0.3â1.3) Lymphocytic leukemia 2 0.4 (0.0â2.4) Myelogenous leukemia 8 0.7 (0.3â1.7) Boehmer et al., Vietnam Experience Cohort 8 1.0 (0.4â2.5) 2004 Studies Reviewed in Update 2004 Akhtar et al., White Air Force Ranch Hand veteransâ 2004 lymphopoietic cancersâ All Ranch Hand veterans Incidence (SIR) 10 0.9 (0.4â1.5) Mortality (SMR) 6 1.0 (0.4â2.0) Veterans with tours between 1966â1970âincidence 7 0.7 (0.3â1.4) White Air Force Comparison veteransâ lymphopoietic cancersâ All comparison veterans Incidence (SIR) 9 0.6 (0.3â1.0) Mortality (SMR) 5 0.6 (0.2â1.2) Veterans with tours between 1966â1970âincidence 4 0.3 (0.1â0.8) Studies Reviewed in Update 2000 AFHS, 2000 Air Force Ranch Hand veterans 2 0.7 (0.1â5.0) AIHW, 1999 Australian Vietnam veterans 27 26 expected (16â36) CDVA, 1998a Australian Vietnam veteransâmen 64e 26 expected (16â36) continued
484 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-48 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c CDVA, 1998b Australian Vietnam veteransâwomen 1e 0 expected (0â4) Studies Reviewed in Update 1998 CDVA, 1997a Australian military Vietnam veterans 33 1.3 (0.8â1.7) Dalager and Army Chemical Corps veterans 1.0 (0.1â3.8) Kang, 1997 Studies Reviewed in Update 1996 Visintainer et al., Michigan Vietnam veterans 30 1.0 (0.7â1.5) 1995 ABBREVIATIONS: 2,4,5-T, 2,4,5-trichlorophenoxyacetic acid, 2,4-D, 2,4-dichlorophenoxyacetic acid; ADVA, Australian Department of Veterans Affairs; AFHS, Air Force Health Study; AIHW, Aus- tralian Institute of Health and Welfare; CDVA, Commonwealth Department of Veteransâ Affairs; CI, conï¬dence interval; CLL, chronic lymphocytic leukemia; IARC, International Agency for Research on Cancer; TEQ, toxicity equivalency; USDA, US Department of Agriculture. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. dp 0.01. e Self-reported medical history. Answer to question: âSince your ï¬rst day of service in Vietnam, have you been told by a doctor that you have leukemia?â * Information not provided by study authors. â Denoted by a dash in the original study. â Lymphopoietic cancers comprise all of the forms of lymphoma (including Hodgkinâs Disease and non-Hodgkinâs lymphoma) and leukemia (ALL, AML, CLL, CML). Studies in italics have been superseded by newer studies of the same cohorts. no increases in the incidence of or mortality from leukemia in pesticide applica- tors, commercial applicators, or their spouses (Table 6-44). ât Mannetje et al. (2005) found only one case of leukemia, speciï¬ed as a myelogenous tumor (ICD-9 205), in their small cohort of phenoxy herbicide producers and sprayers. A subcohort of Hispanic workers drawn from a larger cohort of 139,000 California UFW members was assembled for a nested caseâcontrol study (Mills et al., 2005). A total of 51 people with leukemia (35 men and 16 women; 23 lym- phocytic, 20 granulocytic, and 8 other) were identiï¬ed. Control subjects (in a 5:1 ratio) matched by sex, ethnicity, and age were drawn from the UFW cohort by using incidence density sampling. Exposure to pesticides and herbicides was determined by linking the subjectsâ job titles to records of pesticide application in the California Department of Pesticide Regulation. Use of 2,4-D was not found to be associated with all types of leukemia (OR 1.03, 95% CI 0.41â2.61) or with leukemias speci- ï¬ed as having arisen from myelogenous or lymphocytic cell lines.
CANCER 485 Torchio et al. (1994) reported on a cohort of 23,401 Italian licensed pesticide users in the Piedmont region, which the Italian National Institute of Statistics re- ports as having high herbicide use, especially of 2,4-D and MCPA. The estimated risk of leukemia was not increased (27 cases; SMR 0.75, 95% CI 0.49â1.08). Reif et al. (1989) performed a series of caseâcontrol analyses on the sample of 19,904 people with speciï¬ed occupations among the 24,762 men 20 years old or older entered into the New Zealand Cancer Registry during 1980â1984. The focus of their report was on the 134 for whom forestry work was the most recent occupation listed. For each type of cancer, people with any other type of cancer were used as controls. Of 534 people with leukemia, 4 had most recently been forestry workers (OR 0.96, 95% CI 0.36â2.61). Environmental Studies No relevant environmental studies concerning a possible association between exposure to the compounds of interest and leukemia were published since those reviewed in Update 2004. Vietnam-Veteran Studies In the mortality update of the CDC VES through 2000, Boehmer et al. (2004) reported eight deaths from leukemia in both the deployed and non-deployed vet- erans (CRR 0.95, 95% CI 0.36â2.53). A set of three reports updating the health status of Australian Vietnam vet- erans noted non-signiï¬cantly increased risks of leukemia after Vietnam service in comparing veterans with the general population of Australia with respect to incidence (SIR 1.88, 95% CI 0.98â1.38) (ADVA, 2005a) and mortality (SMR 1.07, 95% CI 0.84â1.30) (ADVA, 2005b). A separate study compared rates of leukemia in deployed and non-deployed Vietnam veterans (ADVA, 2005c); no increased risks of leukemia (RR 0.60, 95% CI 0.31â1.13) or leukemia mortal- ity (RR 0.61, 95% CI 0.27â1.30) were seen in the deployed. The reports on the Australian Vietnam veterans also presented risks broken down by leukemia type (see Table 6-49); only in CLL did the veterans have a signiï¬cant increase over the general public (ADVA, 2005a). Biologic Plausibility Male rats fed TCDD at a dose of 1 ng/kg of body weight per week for 78 weeks and sacriï¬ced at week 95 of the study showed an increased incidence of lymphocytic leukemia (Van Miller et al., 1977), but female rats and mice of both sexes did not show increased incidences. Later studies of TCDDâs carcinogenicity have not shown an increased incidence of leukemia in mice or rats.
486 VETERANS AND AGENT ORANGE: UPDATE 2006 Two recent in vitro studies suggest that TCDD exposure does not promote leukemia. van Grevenynghe et al. (2006) reported that proliferation of cultured human bone marrow stem cells (the source of leukemic cells) was not inï¬uenced by addition of TCDD to the culture medium. And Mulero-Navarro et al. (2006) reported that the AhR promoter is silenced in ALLâan effect that could lead to reduced expression of the receptor that binds TCDD and mediates its toxicity. No reports of animal studies have noted an increased incidence of leukemia after exposure to the phenoxy herbicides or other compounds of interest. Synthesis The new studies from the US AHS and on Vietnam veterans did not provide any new evidence of an association between exposure to the compounds of inter- est and leukemia, although it is important to recognize that analyses of possible effects of exposure to TCDD and other compounds of interest were not reported. Exposure to 2,4-D was assessed in UFW members, but no association with leu- kemia incidence was found. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is inadequate or insufï¬cient evidence to determine whether there is an association between exposure to the compounds of interest and leukemias other than CLL. Chronic Lymphocytic Leukemia In the proposed World Health Organization classiï¬cation of non-Hodgkinâs lymphoid neoplasms CLL (ICD-9 204.1) and its lymphomatous form, small-cell lymphocytic lymphoma, are mature B-cell neoplasms (IARC, 2001). ACS esti- mated that about 6,280 men and 3,740 women would receive diagnoses of CLL in the United States in 2006 and that 2,590 men and 2,070 women would die from it (Jemal et al., 2006). Nearly all cases occur after the age of 50 years. For average annual incidence, see Table 6-47. The requirements for diagnosis of CLL include an absolute peripheral-blood lymphocyte count of more than 10 à 109 per liter, a predominant population of mature-looking lymphocytes, and hypercellular or normal cellular bone marrow that contains more than 30 percent lymphocytes. The malignant cells in CLL exhibit a characteristic membrane phenotype with coexpression of pan-B-cell an- tigensâincluding CD19, CD20, and CD23âwith CD5. However, the cell surface membranes express only weak surface-membrane immunoglobulin. Patients with CLL are staged according to the Rai classiï¬cation: stage 0, clinical features of lymphocytes in the blood and marrow only; stage I or II (intermediate risk), lymphocytosis, lymphadenopathy, and splenomegaly with
CANCER 487 or without hepatomegaly; and stage III or IV (high risk), lymphocytosis and either anemia or thrombocytopenia or both. The most consistent abnormal ï¬nd- ing at initial diagnosis is lymphadenopathyâfrom small lymph nodes to nodes as large as an orange. Patients with large lymphadenopathy, white-cell counts higher than 100 à 109 per liter, or thrombocytopenia require therapy. The dis- ease is complicated by autoimmune anemias and recurrent infection because of hypogammaglobulinemia. Diffuse small-cell lymphocytic lymphoma is the term for the condition of pa- tients who have lymphomatous CLL. Patients seek medical attention for painless generalized lymphadenopathy that in many cases has lasted for several years. Un- like the situation in CLL, the peripheral blood may be normal or reveal only mild lymphocytosis. However, the bone marrow has abnormal cells in 75â95 percent of cases. Both small-cell lymphocytic lymphoma and CLL can transform into aggressive NHL, known as Richterâs syndrome. Richterâs syndrome is character- ized by diffuse large-cell lymphoma or its immunoblastic variant. It is resistant to current therapies, and the median survival is about 6 months. Hairy-cell leukemia has recently been classiï¬ed as a rare form of CLL (AJCC, 2002). Conclusions from VAO and Updates Update 2002 was the ï¬rst to discuss CLL separately from other leukemias. The epidemiologic studies indicated that farming, especially with exposure to 2,4-D and 2,4,5-T, is associated with signiï¬cant mortality from CLL. Many more studies support the hypothesis that herbicide exposure can contribute to NHL risk. Most cases of CLL and NHL reï¬ect malignant transformation of B- lymphocyte progenitor cells, so these diseases could have a common etiology. Studies reviewed in Update 2002 and Update 2004 and in the present report are summarized in Table 6-49. Update of the Epidemiologic Literature Occupational Studies In the review responding to VAâs request that all evidence on AML be as- sessed in this update, the committee noted a large study of sawmill workers in which the dioxin exposure from chlorophenols tended to involve less TCDD than hexachlorinated, heptachlorinated, and octachlorinated dioxins. Hertzman et al. (1997) reported on cancer incidence in 1969â1989 in a cohort of 23,829 workers in 11 sawmills in British Columbia that used chlorophenate. The risk of all types of leukemias neared signiï¬cance (SIR 1.18, 95% CI 0.91â1.50), which was dominated largely by 24 cases of CLL (SIR 1.67, 95% CI 1.16â2.36).
488 VETERANS AND AGENT ORANGE: UPDATE 2006 TABLE 6-49 Selected Epidemiologic StudiesâChronic Lymphocytic Leukemia Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c OCCUPATIONAL New Studies Hertzman et al., British Columbia sawmill worker with 1997 chlorophenate process (more hexa-, hepta-, and octa CDDs than TCDD), all leukemiasâincidence 47 1.2 (0.9â1.5) ALL 2 1.0 (0.2â3.1) CLL 24 1.7 (1.2â2.4) AML 5 0.8 (0.3â1.7) CML 7 1.1 (0.5â2.0) Other and unspeciï¬ed 5 0.5 (0.2â1.0) Studies Reviewed in Update 1998 Waterhouse et al., Residents of Tecumseh, Michiganâincidence 1996 (men and women) 10 1.8 (0.8â3.2) Amadori et al., Workers in northeast Italy (men and women) 1995 Farming and animal-breeding workers 15 2.3 (0.9â5.8) Farming workers only 5 1.6 (0.5â5.2) Animal-breeding workers only 10 3.1 (1.1â8.3) Studies Reviewed in VAO Hansen et al., Danish gardeners (men and women) 1992 All gardeners 6 2.5 (0.9â5.5) Male gardeners 6 2.8 (1.0â6.0) Brown et al., 1990 Residents of Iowa and Minnesota Ever farmed 156 1.4 (1.1â1.9) Any herbicide use 74 1.4 (1.0â2.0) Blair and White, 1,084 leukemia deaths in Nebraska 1957â1974 1985 Farmerâusual occupation on death certiï¬cate * 1.3 (p 0.05) 248 CLLs * 1.7 (p 0.05) Burmeister et al., 1,675 leukemia deaths in Iowa 1968â1978 1982 Farmerâusual occupation on death certiï¬cate 1.2 (p 0.05) CLL 132 1.7 (1.2â2.4) Lived in 33 counties with highest herbicide use * 1.9 (1.2â3.1) ENVIRONMENTAL Studies Reviewed in Update 2000 Bertazzi et al., Seveso residentsâ20-year follow-up 2001 Lymphatic leukemia Zones A, Bâmen 2 1.6 (0.4â6.8) women 0 â
CANCER 489 TABLE 6-49 Continued Estimated Exposed Relative Risk Reference Study Populationa,b Casesc (95% CI)c VIETNAM VETERANS New Studies ADVA, 2005a Australian Vietnam veterans vs Australian populationâincidence All branches 58 1.20 (0.7â1.7) Navy 12 1.51 (0.8â2.6 Army 42 1.68 (1.2â2.2) Air Force 4 0.87 (0.2â2.2) ABBREVIATIONS: ADVA, Australian Department of Veterans Affairs. a Table shows mortality unless otherwise noted. b Cohorts are male unless otherwise noted. c Given when available. â Denoted by a dash in the original study. Environmental Studies No new environmental studies concerning exposure to the compounds of interest and CLL were published since Update 2004. Vietnam-Veteran Studies An increase in the incidence of CLL was observed in the comparison be- tween Australian Vietnam veterans and the general public (SIR 1.55, 95% CI 1.15â1.95) (ADVA, 2005a). Only in the group of Army veterans was a signiï¬- cant effect shown (SIR 1.68, 95% CI 1.18â2.19), although the rate was also increased in the smaller group of Navy veterans (SIR 1.51, 95% CI 0.78â2.63). In the corresponding mortality study (ADVA, 2005b), cases of lymphocytic leukemia were too few to separate into acute and chronic types. In the study that compared the incidence of CLL in deployed and non-deployed Australian forces (ADVA, 2005c), no increase was found in the deployed (RR 0.90, 95% CI 0.31â2.45); again, there were too few deaths from lymphocytic leukemia to analyze acute and chronic types separately. Biologic Plausibility No animal studies have reported an increase speciï¬cally in the incidence of CLL after exposure to the compounds of interest. However, given the similarities
490 VETERANS AND AGENT ORANGE: UPDATE 2006 between CLL and B-cell lymphomas, a similar argument for biologic plausibil- ity can be made. An increased incidence of lymphoma was reported in female B6C3F mice exposed to TCDD at 1 mg/kg of body weight via gavage twice a week for 2 years (NTP, 1982a). The ï¬nding was conï¬rmed and extended in recent NTP studies in which a dose-related increase in the incidence of lymphoma was observed in female mice given TCDD orally at 0.04, 0.2, or 2.0 g/kg twice a week for 104 weeks. Laboratory animal studies of 2,4-D found no induction of lymphomas. (See Chapter 3 for more information on 2,4-D toxicity.) The biologic plausibility of the carcinogenicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Although considerably more studies support the hypothesis that herbicide ex- posure can contribute to the development of NHL, exposure to 2,4-D and 2,4,5-T also appears to be associated with the occurrence of CLL. Malignant transforma- tion of B-lymphocyte progenitor cells is apparent in most cases of CLL and NHL, so it is plausible that these diseases could have a common etiology. Conclusion On the basis of its evaluation of the evidence reviewed here and in previous VAO reports, the committee concludes that there is sufï¬cient evidence of an as- sociation between exposure to the compounds of interest and CLL. Acute Myelogenous Leukemia In adults, acute leukemia is nearly always in the form of AML (ICD-9 205.0, 207.0, 207.2). ACS estimated that about 6,350 men and 5,580 women would receive new diagnoses of AML in the United States in 2006 and that 5,090 men and 3,950 women would die from it (Jemal et al., 2006). Seven distinct morpho- logic groups were described in the FrenchâAmericanâBritish (FAB) classiï¬cation system. FAB M-0 and M-1 without maturation are characterized by the presence of Auer rods in the leukemic cell. FAB M-2 myelogenous leukemia with matu- ration also has Auer rods and is more likely to have chromosomal abnormali- ties. FAB M-3 progranulocytic leukemia has distinct morphologic, clinical, and cytogenetic features that include a tendency toward disseminated intravascular coagulation. FAB M-4 myelomonocytic leukemia is characterized by a mixture of large myeloid and monocytic elements. Some patients have prominent eosino- philia. Patients who present with the FAB categories M-2 to M-4 generally are 30â40 years old and experience a favorable outcome of induction chemotherapy. Patients with FAB M-5, monocytic leukemia; FAB M-6, erythroleukemia; or FAB
CANCER 491 M-7, megakaryocytic leukemia, often are over 60 years old, and the prognosis generally is poor. AML is the most common leukemia among adults; its incidence increases steadily with age in people over 40 years old. In the age groups that typically in- clude Vietnam veterans, AML makes up roughly one-fourth of cases of leukemia in men and one-third in women. Overall, AML is slightly more common in men than in women. Risk factors associated with an increased risk of AML include high doses of ionizing radiation, occupational exposure to benzene, and exposure to some medications used in cancer chemotherapy (such as melphalan). Fanconiâs anemia and Down syndrome are associated with an increased risk of AML, and tobacco use is thought to account for about 20 percent of AML cases. Conclusions from VAO and Updates In this update, at the request of VA, AML is being considered as an inde- pendent cancer type to determine whether there is evidence that its occurrence is associated with exposure to the herbicides sprayed in Vietnam. The search strategies that have been in use since the VAO project was under- taken in the Institute of Medicine would have identiï¬ed any articles addressing AML speciï¬cally and articles that reported on leukemia in general. All the studies previously reviewed in this series with respect to leukemia were revisited to locate any reported results speciï¬cally on AML. Perhaps the complexity of the leukemia classiï¬cation systems and the fact that they have been in ï¬ux throughout the 20th century have caused epidemiologists to question whether diagnoses of speciï¬c leukemia types made over decades could be compiled and reliably reallocated to appropriate types for analysis. For whatever reasons, virtually no usable informa- tion on types of leukemia has been reported in the epidemiologic literature on cohorts reviewed to date. Occasionally, leukemia is partitioned into lymphocytic and myelogenous (Alavanja et al., 1988; Asp et al., 1994; Bertazzi et al., 1993; Bueno de Mesquita et al., 1993; Kogevinas et al., 1993; Semenciw at al., 1994; Svensson et al., 1995), but no instances of partitioning into acute and chronic were observed. Findings characterized in both respects are extremely uncom- mon (Green, 1991; Hertzman et al., 1997; Reif et al., 1989; Zober et al., 1990). These instances are likely to occur without associated statistics and for such small numbers of cases would not be useful. The rarity of individual speciï¬c leukemias makes them a more suitable topic for the caseâcontrol design, but the committee found only a small number of studies that followed such a protocol and yielded results for AML (Blair and White, 1985; Brown et al. 1990; Burmeister et al., 1982). The statistics that are available for AML in particular have been entered with the results for leukemia overall in Table 6-48. Green (1991) noted that the one case of leukemia observed in the 17 people who died from cancer in a cohort of 1,222 forestry workers who worked with phe-
492 VETERANS AND AGENT ORANGE: UPDATE 2006 noxy herbicides and picloram was AML. In reporting on the 534 men entered in the New Zealand Cancer Registry from 1980â1984 with a diagnosis of leukemia, Reif et al. (1989) mentioned that, of the four cases who were forestry workers, three had AML, giving an elevated risk in association with that occupation (OR 2.24) that was characterized as being âimprecise.â In describing the cohort of 247 at the BASF plant that had an explosion in 1953, Zober et al. (1990) mentioned only that there was an incident case of AML. Kogevinas et al. (1993) mentioned one death from myelogenous leukemia in the 701 women in the IARC cohort, for an increased risk estimate with a very wide conï¬dence range (SMR 1.96, 95% CI 0.24â7.08). The ï¬ndings of Asp et al. (1994) on leukemia incidence and mortality in 1,909 Finnish phenoxy herbicide applicators were so sparse that partitioning into lymphocytic and myelogenous types was unilluminating. The observation by Bueno de Mesquita et al. (1993) that both the leukemia deaths ob- served in their cohort of Dutch chemical workers involved the myeloid cell type practically doubled the estimated risk (SMR 4.17, 95% CI 0.50â15.05), but the conï¬dence interval remained exceedingly large. The situation was similar when Bertazzi et al. (1993) distinguished between myelogenous and lymphocytic leu- kemias in the 10-year follow-up of morbidity in the Seveso cohort. Svensson et al. (1995) reported separately on the incidence of lymphocytic and myelogenous leukemias in ï¬shermen residing on the east and west coasts of Sweden; on the basis of a modest number of cases, the incidence of neither type of leukemia dif- fered from no effect, but the estimated risks of lymphatic leukemias were greater than 1, and those of the myelogenous type fell below 1. A cohort of farmers in Alberta, Saskatchewan, and Manitoba was deï¬ned by identiï¬cation of speciï¬ed occupation in the 1971 Canadian census and linked to the Canadian Mortality Data Base (Semenciw et al., 1994). Findings based on 357 leukemia deaths (SMR 0.85, 95% CI 0.77â0.95) were robust enough that they could be usefully partitioned to yield a signiï¬cantly reduced risk of myelogenous leukemias (SMR 0.78, 95% CI 0.65â0.93) but not lymphatic leukemias (SMR 0.94, 95% CI 0.79â1.12). In the leukemia results on agricultural extension workers (Alavanja et al., 1988), the phenomenon was similar, but the message was reversed. The signiï¬- cant increase in leukemias overall (SMR 1.92, 95% CI 1.04â3.54) was intensi- ï¬ed when the analysis was restricted to myelogenous leukemias (SMR 2.80, 95% CI 1.09â7.19). Hertzman et al. (1997) reported on the cancer incidence in 1969â1989 in a cohort of 23,829 workers in 11 sawmills in British Columbia that used chloro- phenate, which tends to be contaminated with hexachlorinated, heptachlorinated, and octachlorinated, rather than tetrachlorinated, dioxins. The risk of all types of leukemias neared signiï¬cance (SIR 1.18, 95% CI 0.91â1.50) and was domi- nated by 24 cases of CLL (SIR 1.67, 95% CI 1.16â2.36); the ï¬ve cases of AML, however, did not indicate an increased risk (SIR 0.81, 95% CI 0.32â1.70). For every white man 30 years old or older who died of any type of leukemia
CANCER 493 in Nebraska in 1957â1974, Blair and White (1985) selected two non-leukemia deaths matched on sex, race, county of residence, age at death (within 2 years), and calendar year of death. Usual occupations were obtained from death certiï¬- cates, and 1,084 of the people with leukemia were coded as farmers (farm owners, tenants, or laborers), for a risk ratio of 1.25, which was said to be signiï¬cant at the 0.05 level. When the risks of nine different leukemia types were calculated, only the risk of CLL (OR 1.67) was signiï¬cantly increased; the estimated risk of AML in 235 farmers was 1.18. Burmeister et al. (1982) conducted an analogous investigation of the as- sociation between a usual occupation of farming and death from leukemia in 1968â1978 in Iowa. There was an increased risk of leukemias overall (OR 1.24; p 0.05), but no increase in risk was associated with AML in particular. Brown et al. (1990) not only broke down leukemia cases by type but provided a substantial amount of information on the use of speciï¬c phenoxy herbicides and AML and CLL. A companion caseâcontrol study was conducted on lympho- mas. Screening of white men 30 years old or older in the Iowa Tumor Registry (March 1981âOctober 1983) and a surveillance network established for this study in Minnesota (October 1980âSeptember 1982) identiï¬ed 578 newly diagnosed cases of leukemia. Stratifying on age, vital status, and state assembled a popula- tion-based sample of 1,245 white men without lymphohematopoietic cancer. Detailed information on personal habits, family medical history, and occupation (particularly farming and aspects of pesticide use) was gathered from in-person interviews conducted with the subjects or close relatives. For leukemias overall, the results suggested an association with phenoxy herbicide use (SIR 1.2, 95% CI 0.9â1.6). For AML in particular, the association with having ever used herbi- cides (SIR 1.3, 95% CI 0.8â2.0) was slightly more pronounced than that with having ever lived on a farm (SIR 1.2, 95% CI 0.8â1.8). Update of the Epidemiologic Literature In light of the overall paucity of information on a possible association be- tween exposure to the herbicides sprayed in Vietnam and AML speciï¬cally, the information published on this subject since Update 2004 is relatively rich. Occupational Studies In their small cohort of phenoxy herbicide producers and sprayers, ât Mannetje et al. (2005) found a single case of leukemia, which was speciï¬ed as myeloid (ICD-9 205). Environmental Studies No new environmental studies concerning the com- pounds of interest and AML were published since Update 2004. Vietnam-Veteran Studies The reports on the Australian Vietnam veterans (ADVA, 2005a,b,c) were unusual in presenting risks broken down by leukemia type
494 VETERANS AND AGENT ORANGE: UPDATE 2006 (see Table 6-49). Compared with the incidence in the general public (SIR 1.04, 95% CI 0.67â1.42) (ADVA, 2005a) or non-deployed veterans (RR 0.30, 95% CI 0.06â1.11) (ADVA, 2005c), the incidence of AML in deployed veterans was not perceptibly increased. With respect to mortality, however, the ï¬ndings for leukemia were broken down only to the level of lymphocytic versus myelogenous but not speciï¬cally for AML (ADVA, 2005b,c). Biologic Plausibility No animal studies have reported an increase in the incidence of AML after exposure to the compounds of interest. The biologic plausibility of the carcino- genicity of the compounds of interest in general is summarized at the end of this chapter. Synthesis Taken together, the occupational, environmental, and veteran studies are limited by the paucity of reports related to the types of leukemia and to AML in particular. In concluding its review of the available ï¬ndings related to the occurrence of AML in veterans exposed to the herbicides sprayed in Vietnam, the committee notes the ï¬nding in Update 2000 of limited or suggestive evidence of an associa- tion between exposure to the compounds of interest and AML in the children of Vietnam veterans and the reversal of the ï¬nding in Acute Myelogenous Leukemia (2002). The recognition of an error in a key publication and new information on the illness resulted in reclassiï¬cation of AML in children to inadequate evidence to determine whether there is an association. Conclusion The committee concludes that there is inadequate or insufï¬cient information to determine whether there is an association between exposure to the compounds of interest and AML or other speciï¬c types of leukemia except CLL. SUMMARY Biologic Plausibility The biologic plausibility of an association between exposure to the com- pounds of interest and human cancers is summarized as follows. The studies con- sidered in this chapter with respect to biologic plausibility have been restricted primarily to those performed in laboratory animals (rats, mice, hamsters, and monkeys). Mechanistic studies pertaining to the possible carcinogenic actions of the compounds of interest have been described in Chapter 3. The evidence
CANCER 495 obtained from cellular and molecular studies indicates that a connection between human exposure to TCDD and cancers is biologically plausible. In considering the relevance of the studies in laboratory animals to the effect that human expo- sure to TCDD (and other compounds of interest) may have on the development of cancers in the veterans of the Vietnam War, a few notes of caution should be observed. First, the effects of TCDD vary widely among species. For example, there are differences among various experimental animals in susceptibility to a number of TCDD-induced effects, and the sites at which tumors are induced vary among species. Second, the exposures used in the animal studies may or may not appropriately represent human exposures (discussed in Chapter 3). Third, the dose or body burden that would be expected to affect either the incidence or the progression of a speciï¬c human cancer signiï¬cantly is not clear. Fourth, given that human cancers are complex diseases most frequently observed in the aging population and inï¬uenced by genetic, dietary, hormonal, and environmental fac- tors, it is not yet clear whether the studies have been performed in a manner that appropriately models the development of the speciï¬c human cancers of interest. With respect to 2,4-D, 2,4,5-T, and picloram, several studies have been performed in laboratory animals. In general, the results were negative, although some of them would not meet current standards for cancer bioassays; others pro- duced equivocal results. Thus, it is impossible to have conï¬dence in conclusions regarding the carcinogenicity of those compounds. Most of the evidence indicates that 2,4-D is genotoxic only at very high concentrations. Although 2,4,5-T was shown to increase the formation of DNA adducts by cytochrome P450-derived metabolites of benzo[a]pyrene, most available evidence indicates that 2,4,5-T is genotoxic only at high concentrations. There is some evidence that cacodylic acid is carcinogenic. Studies per- formed in laboratory animals have shown that it can induce neoplasms of the kid- ney (Yamamoto et al., 1995) and bladder (Arnold et al., 2006; Wei et al., 2002). In the lung, treatment with cacodylic acid induced formation of neoplasms when administered to mouse strains that are genetically susceptible to them (Hayashi et al., 1998). Other studies have used the two-stage model of carcinogenesis in which animals are exposed ï¬rst to a known genotoxic agent and then to a sus- pected tumor-promoting agent. With that model, cacodylic acid has been shown to act as a tumor-promoter with respect to lung cancer (Yamanaka et al., 1996). A number of health agencies have concluded that TCDD is a human carcino- gen. Studies in laboratory animals in which only TCDD has been administered have reported that TCDD can increase the incidence of a number of neoplasms, most notably of the liver, lung, thyroid, and oral mucosa (Kociba et al., 1978; NTP, 2006). Some studies have used the two-stage model of carcinogenesis and shown that TCDD can act as a tumor promoter to increase the incidence of ovar- ian (Davis et al., 2000), liver (Beebe et al., 1995), and skin cancers (Wyde et al., 2004). When Cheng et al. (2006) applied the concentration- and age-dependent elimination model of Aylward and colleagues (2005) in estimating the cancer risk associated with occupational TCDD exposure in the NIOSH cohort, they found
496 VETERANS AND AGENT ORANGE: UPDATE 2006 that the model predicted cumulative serum TCDD concentrations four to ï¬ve times higher than those obtained with the ï¬rst-order elimination model and an 8.7-year ï¬xed-half-life model. As to the mechanisms by which TCDD exerts its carcinogenic effects, it is thought to act primarily as a tumor promoter. In many of the animal studies reviewed, treatment with TCDD has resulted in hyperplasia and/or metaplasia of epithelial tissues. In addition, in both laboratory animals and cultured cells, TCDD has been shown to exhibit a wide array of effects on growth regulation, hormone systems, and other factors associated with the regulation of cellular processes that involve growth, maturation, and differentiation. Thus, it may be that TCDD (and perhaps other compounds of interest) may increase the incidence or progression of human cancers through an interplay between multiple cellular factors. Tissue-speciï¬c protective cellular mechanisms may also affect the response to TCDD and further complicate our understanding of its carcino- genic effects. In conclusion, the evidence indicates that a connection between TCDD and cacodylic acid and cancer in humans is, in general, biologically plausible. Experi- ments with 2,4-D, 2,4,5-T, and picloram in animals and cells have not provided a strong biologic basis for the presence or absence of carcinogenic effects. Con- siderable uncertainty remains about how to apply the available information to the evaluation of the carcinogenic potential of herbicide or TCDD exposure in Vietnam veterans. Conclusions The committee had four categories available to classify the strength of the evidence from the occupational, environmental, and veteran studies reviewed regarding an association between exposure to the compounds of interest and each of the kinds of cancer studied. In categorizing diseases according to the strength of the evidence, the committee applied the same criteria (discussed in Chapter 2) that were used in VAO, Update 1996, Update 1998, Update 2000, Update 2002, and Update 2004. To be consistent with the charge to the committee by the Sec- retary of Veterans Affairs in Public Law 102-4 and with accepted standards for scientiï¬c reviews, the committee distinguished among the four conclusions on the basis of statistical association, not causality. Despite extensive consideration of all the evidence available, the committee could not reach consensus on whether breast cancer and melanoma skin cancer satisfy the criteria for inclusion in the category of limited or suggestive evidence of an association or should be retained in the category of inadequate or insuf- ï¬cient evidence to determine whether there is an association. Health Outcomes with Sufï¬cient Evidence of an Association For outcomes in this category, a positive association with at least one of the compounds of interest must be observed in studies in which chance, bias, and
CANCER 497 confounding can be ruled out with reasonable conï¬dence. The committee re- garded evidence from several small studies that were free of bias and confounding and that showed an association that was consistent in magnitude and direction as sufï¬cient evidence of an association. Previous VAO committees found sufï¬cient evidence of an association be- tween exposure to at least one of the compounds of interest and four kinds of cancer: STS, NHL, HD, and CLL. The scientiï¬c literature continues to support the classiï¬cation of those four cancers in the category of sufï¬cient evidence. Health Outcomes with Limited or Suggestive Evidence of an Association For outcomes in this category, the evidence must suggest an association with at least one of the compounds of interest that could be limited because chance, bias, or confounding could not be ruled out with conï¬dence. A high-quality study may have demonstrated a strong positive association amid a ï¬eld of less convinc- ing positive ï¬ndings, or, more often, several studies yielded positive results, but the results of other studies were inconsistent. Previous VAO committees found limited or suggestive evidence of an associ- ation between exposure to at least one of the compounds of interest and laryngeal cancer; cancer of the lung, bronchus, or trachea; prostatic cancer; and multiple myeloma. The literature continues to support the classiï¬cation of those diseases in the category of limited or suggestive evidence. The evidence of an association between the chemicals of interest and AL amyloidosis was found to be limited or suggestive on the basis primarily of biologic similarities to multiple myeloma. The committee could not reach consensus on whether breast cancer and mel- anoma skin cancer satisfy the criteria for inclusion in the category of limited or suggestive evidence of an association or should be retained in the category of in- adequate or insufï¬cient evidence to determine whether there is an association. Health Outcomes with Inadequate or Insufï¬cient Evidence to Determine Whether There Is an Association This is the default category for any disease outcome for which there is no information upon which to base even a discussion. For many of the kinds of can- cer reviewed by the committee, some scientiï¬c data were available, but they were inadequate or insufï¬cient in terms of quality, consistency, or statistical power to support a conclusion of the presence or absence of an association. Some studies fail to control for confounding or to provide adequate exposure assessment. In addition to any speciï¬c kinds of cancer that have not been directly addressed in the present report, this category includes hepatobiliary cancer (cancer of the liver, gallbladder, and bile ducts); cancer of the buccal cavity, pharynx, and nose; bone and joint cancer, non-melanoma skin cancer (including basal-cell carcinoma and squamous-cell carcinoma); cancer of the male and female reproductive systems (excluding prostate cancer); urinary bladder cancer; renal cancer (cancer of the
498 VETERANS AND AGENT ORANGE: UPDATE 2006 kidney and renal pelvis); and the various forms of leukemia other than CLL. Some kinds of cancer (cancer of the brain, colon, rectum, stomach, and pancreas) previously deemed to have limited or suggestive evidence of no association have been moved to this category. The committee could not reach consensus on whether breast cancer and mel- anoma skin cancer satisfy the criteria for inclusion in the category of limited or suggestive evidence of an association or should be retained in the category of in- adequate or insufï¬cient evidence to determine whether there is an association. Health Outcomes with Limited or Suggestive Evidence of No Association For outcomes in this category, several adequate studies covering the full known range of human exposure are consistent in not showing a positive associa- tion with exposure to one of the compounds of interest. The studies have rela- tively narrow conï¬dence intervals. A conclusion of âno associationâ is inevitably limited to the conditions, magnitude of exposure, and length of observation of the available studies. The possibility of a very small increase in risk associated with a given exposure can never be excluded. Inclusion in this category does, how- ever, presume evidence of lack of association between each of the compounds of interest and a particular health outcome, but there has been virtually no cancer epidemiology speciï¬cally evaluating the consequences of exposure to picloram or cacodylic acid. Previous VAO committees found a sufï¬cient number and variety of well- designed studies to conclude that there was limited or suggestive evidence of no association between the compounds of interest and a small group of cancer types: gastrointestinal tumors (of the colon, rectum, stomach, and pancreas) and brain tumors. In light of the presumption noted above and re-evaluation of previously reviewed evidence, those types of cancer have been reclassiï¬ed as having inad- equate or insufï¬cient evidence to determine whether there is an association. On the basis of evaluation of the scientiï¬c literature, no additional types of cancer satisfy the criteria for inclusion in this category. REFERENCES1 ACS (American Cancer Society). 1998. Cancer Facts and Figures. http://www.cancer.org/statistics/ cff98/graphicaldata.html (Accessed March 12). ACS. 2006. Cancer Facts and Figures 2006. Atlanta, GA: American Cancer Society. http://www. cancer.org/downloads/STT/CAFF2006PWSecured.pdf (Accessed March 6, 2007). 1Throughout the report the same alphabetic indicator following year of publication is used con- sistently for the same article when there were multiple citations by the same ï¬rst author in a given year. The convention of assigning the alphabetic indicator in order of citation in a given chapter is not followed.
CANCER 499 ACS. 2007a. What Are the Risk Factors for . . . http://www.cancer.org/docroot/CRI/content/CRI_2_ 4_2X_What_are_the_risk_factors_for... (Accessed September 18, 2007). ACS. 2007b. What Are the Risk Factors for . . . http://www.cancer.org/docroot/CRI/content/CRI_2_2_ 2X_What_causes_laryngeal_and_hypopharyngeal_cancers... (Accessed September 18, 2007). ACS. 2007c. What Are the Risk Factors for . . . http://www.cancer.org/docroot/CRI/content/CRI_2_ 2_2x_What_Causes... (Accessed September 1, 2007). ACS. 2007d. What Are the Risk Factors for . . . http://www.cancer.org/docroot/CRI/content/CRI_2_ 4_2X_What_are_the_risk_factors_for_brain... (Accessed September 18, 2007). ADVA (Australia, Department of Veteransâ Affairs). 2005a. Cancer Incidence in Australian Vietnam Veteran Study 2005. Canberra, Australia: Department of Veteransâ Affairs. ADVA. 2005b. The Third Australian Vietnam Veterans Mortality Study 2005. Canberra, Australia: Department of Veteransâ Affairs. ADVA. 2005c. Australian National Service Vietnam Veterans: Mortality and Cancer Incidence 2005. Canberra, Australia: Department of Veteransâ Affairs. AFHS (Air Force Health Study). 1996. An Epidemiologic Investigation of Health Effects in Air Force Personnel Following Exposure to Herbicides. Mortality Update 1996. Brooks AFB, TX: Epide- miologic Research Division. Armstrong Laboratory. AL/AO-TR-1996-0068. 31 pp. AFHS. 2000. An Epidemiologic Investigation of Health Effects in Air Force Personnel Following Exposure to Herbicides. 1997 Follow-up Examination and Results. Reston, VA: Science Ap- plication International Corporation. F41624â96âC1012. AFHS. 2005. An Epidemiologic Investigation of Health Effects in Air Force Personnel Following Exposure to Herbicides. 1997 Follow-up Examination and Results. Brooks AFB, TX: Epidemio- logic Research Division. Armstrong Laboratory. AFRL-HE-BR-SR-2005-0003. AIHW (Australian Institute of Health and Welfare). 1999. Morbidity of Vietnam Veterans: A Study of the Health of Australiaâs Vietnam Veteran Community, Volume 3: Validation Study. Canberra. AJCC (American Joint Committee on Cancer). 2002. Lymphoid neoplasms. AJCC Cancer Staging Manual, 6th Edition. New York: Springer-Verlag. Pp. 393â406. Akhtar FZ, Garabrant DH, Ketchum NS, Michalek JE. 2004. Cancer in US Air Force veterans of the Vietnam War. Journal of Occupational and Environmental Medicine 46(2):123â136. Alavanja MC, Blair A, Merkle S, Teske J, Eaton B. 1988. Mortality among agricultural extension agents. American Journal of Industrial Medicine 14(2):167â176. Alavanja MC, Blair A, Merkle S, Teske J, Eaton B, Reed B. 1989. Mortality among forest and soil conservationists. Archives of Environmental Health 44:94â101. Alavanja MC, Samanic C, Dosemeci M, Lubin J, Tarone R, Lynch CF, Knott C, Thomas K, Hoppin JA, Barker J, Coble J, Sandler DP, Blair A. 2003. Use of agricultural pesticides and pros- tate cancer risk in the Agricultural Health Study cohort. American Journal of Epidemiology 157(9):800â814. Alavanja MC, Dosemeci M, Samanic C, Lubin J, Lynch CF, Knott C, Barker J, Hoppin JA, Sandler DP, Coble J, Thomas K, Blair A. 2004. Pesticides and lung cancer risk in the Agricultural Health Study cohort. American Journal of Epidemiology 160(9):876â885. Alavanja MCR, Sandler DP, Lynch CF, Knott C, Lubin JH, Tarone R, Thomas K, Dosemeci M, Barker J, Hoppin JA, Blair A. 2005. Cancer incidence in the Agricultural Health Study. Scandinavian Journal of Work, Environment and Health 31(Suppl 1):39â45. Amadori D, Nanni O, Falcini F, Saragoni A, Tison V, Callea A, Scarpi E, Ricci M, Riva N, Buiatti E. 1995. Chronic lymphocytic leukaemias and non-Hodgkinâs lymphomas by histological type in farming-animal breeding workers: A population caseâcontrol study based on job titles. Oc- cupational and Environmental Medicine 52(6):374â379. Anderson HA, Hanrahan LP, Jensen M, Laurin D, Yick W-Y, Wiegman P. 1986a. Wisconsin Vietnam Veteran Mortality Study: Proportionate Mortality Ratio Study Results. Madison: Wisconsin Division of Health.
500 VETERANS AND AGENT ORANGE: UPDATE 2006 Anderson HA, Hanrahan LP, Jensen M, Laurin D, Yick W-Y, Wiegman P. 1986b. Wisconsin Vietnam Veteran Mortality Study: Final Report. Madison: Wisconsin Division of Health. Andersson E, Nilsson R, Toren K. 2002b. Gliomas among men employed in the Swedish pulp and paper industry. Scandinavian Journal of Work, Environment and Health 28(5):333â340. Andersson P, McGuire J, Rubioi C, Gradin K, Whitelaw ML, Pettersson S, Hanberg A, Poellinger L. 2002a. A constitutively active dioxin/aryl hydrocarbon receptor induces stomach tumors. Proceedings of the National Academy of Sciences of the United States 99(15):9990â9995. Andersson P, Rubio C, Poellinger L, Hanberg A. 2005. Gastric hamartomatous tumours in a transgenic mouse model expressing an activated dioxin/Ah receptor. Anticancer Research 25(2A):903â911. Arnold LL, Eldan M, Nyska A, van Gemert M, Cohen SM. 2006. Dimethylarsinic acid: Re- sults of chronic toxicity/oncogenicity studies in F344 rats and in B6C3F1 mice. Toxicology 223(1-2):82â100. Asp S, Riihimaki V, Hernberg S, Pukkala E. 1994. Mortality and cancer morbidity of Finnish chlorophenoxy herbicide applicators: an 18-year prospective follow-up. American Journal of Industrial Medicine 26(2):243â253. Axelson O, Sundell L, Andersson K, Edling C, Hogstedt C, Kling H. 1980. Herbicide exposure and tumor mortality. An updated epidemiologic investigation on Swedish railroad workers. Scandi- navian Journal of Work, Environment and Health 6(1):73â79. Aylward LL, Brunet RC, Starr TB, Carrier G, Delzell E, Cheng H, Beall C. 2005. Exposure recon- struction for the TCDD-exposed NIOSH cohort using a concentration- and age-dependent model of elimination. Risk Analysis 25(4):945â956. Bagga D, Anders KH, Wang HJ, Roberts E, Glaspy JA. 2000. Organochlorine pesticide content of breast adipose tissue from women with breast cancer and control subjects. Journal of the Na- tional Cancer Institute 92(9):750â753. Balarajan R, Acheson ED. 1984. Soft tissue sarcomas in agriculture and forestry workers. Journal of Epidemiology and Community Health 38(2):113â116. Becher H, Flesch-Janys D, Kauppinen T, Kogevinas M, Steindorf K, Manz A, Wahrendorf J. 1996. Cancer mortality in German male workers exposed to phenoxy herbicides and dioxins. Cancer Causes and Control 7(3):312â321. Beebe LE, Fornwald LW, Diwan BA, Anver MR, Anderson LM. 1995. Promotion of N-nitroso- diethylamine-initiated hepatocellular tumors and hepatoblastomas by 2,3,7,8-tetrachloro- dibenzo-p-dioxin or Aroclor 1254 in C57BL/6, DBA/2, and B6D2F1 mice. Cancer Research 55(21):4875â4880. Bender AP, Parker DL, Johnson RA, Scharber WK, Williams AN, Marbury MC, Mandel JS. 1989. Minnesota highway maintenance worker study: Cancer mortality. American Journal of Indus- trial Medicine 15(5):545â556. Bertazzi PA, Zocchetti C, Pesatori AC, Guercilena S, Sanarico M, Radice L. 1989a. Mortality in an area contaminated by TCDD following an industrial incident. Medicina Del Lavoro 80(4):316â329. Bertazzi PA, Zocchetti C, Pesatori AC, Guercilena S, Sanarico M, Radice L. 1989b. Ten-year mor- tality study of the population involved in the Seveso incident in 1976. American Journal of Epidemiology 129(6):1187â1200. Bertazzi PA, Zocchetti C, Pesatori AC, Guercilena S, Consonni D, Tironi A, Landi MT. 1992. Mor- tality of a young population after accidental exposure to 2,3,7,8-tetrachlorodibenzodioxin. International Journal of Epidemiology 21(1):118â123. Bertazzi A, Pesatori AC, Consonni D, Tironi A, Landi MT, Zocchetti C. 1993. Cancer incidence in a population accidentally exposed to 2,3,7,8-tetrachlorodibenzo-para-dioxin. Epidemiology 4(5):398â406.
CANCER 501 Bertazzi PA, Zochetti C, Guercilena S, Consonni D, Tironi A, Landi MT, Pesatori AC. 1997. Dioxin exposure and cancer risk: a 15-year mortality study after the âSeveso accident.â Epidemiology 8(6):646â652. Bertazzi PA, Bernucci I, Brambilla G, Consonni D, Pesatori AC. 1998. The Seveso studies on early and long-term effects of dioxin exposure: A review. Environmental Health Perspectives 106(Suppl 2):625â633. Bertazzi PA, Consonni D, Bachetti S, Rubagotti M, Baccarelli A, Zocchetti C, Pesatori AC. 2001. Health effects of dioxin exposure: A 20-year mortality study. American Journal of Epidemiol- ogy 153(11):1031â1044. Birnbaum LS, Fenton SE. 2003. Cancer and developmental exposure to endocrine disruptors. Envi- ronmental Health Perspectives 111(4):389â394. Blair A, Kazerouni N. 1997. Reactive chemicals and cancer. Cancer Causes and Control 8(3): 473â490. Blair A, White DW. 1985. Leukemia cell types and agricultural practices in Nebraska. Archives of Environmental Health 40(4):211â214. Blair A, Grauman DJ, Lubin JH, Fraumeni JF Jr. 1983. Lung cancer and other causes of death among licensed pesticide applicators. Journal of the National Cancer Institute 71(1):31â37. Blair A, Dosemeci M, Heineman EF. 1993. Cancer and other causes of death among male and female farmers from twenty-three states. American Journal of Industrial Medicine 23(5):729â742. Blair A, Zahm SH, Cantor KP, Ward MH. 1997. Occupational and environmental risk factors for chronic lymphocytic leukemia and non-Hodgkinâs lymphoma. In: Marti GE, Vogt RF, Zenger VE, eds. Proceedings of the USPHS Workshop on Laboratory and Epidemiologic Approaches to Determining the Role of Environmental Exposures as Risk Factors for B-Cell Chronic Lympho- cytic and Other B-Cell Lymphoproliferative Disorders. US Department of Health and Human Services, Public Health Service. Blair A, Sandler DP, Tarone R, Lubin J, Thomas K, Hoppin JA, Samanic C, Coble J, Kamel F, Knott C, Dosemeci M, Zahm SH, Lynch CF, Rothman N, Alavanja MC. 2005a. Mortality among participants in the Agricultural Health Study. Annals of Epidemiology 15(4):279â285. Blair A, Sandler D, Thomas K, Hoppin JA, Kamel F, Coble J, Lee WJ, Rusiecki J, Knott C, Dosemeci M, Lynch CF, Lubin J, Alavanja M. 2005b. Disease and injury among participants in the Agri- cultural Health Study. Journal of Agricultural Safety and Health 11(2):141â150. Bloemen LJ, Mandel JS, Bond GG, Pollock AF, Vitek RP, Cook RR. 1993. An update of mortality among chemical workers potentially exposed to the herbicide 2,4-dichlorophenoxyacetic acid and its derivatives. Journal of Occupational Medicine 35(12):1208â1212. Blot WJ, McLaughlin JK. 1999. The changing epidemiology of esophageal cancer. Seminars in Oncology 26(5 Suppl 15):2â8. Bodner KM, Collins JJ, Bloemen LJ, Carson ML. 2003. Cancer risk for chemical workers ex- posed to 2,3,7,8-tetrachlorodibenzo-p-dioxin. Occupational and Environmental Medicine 60(9):672â675. Boehmer TK, Flanders WD, McGeehin MA, Boyle C, Barrett DH. 2004. Postservice mortality in Vietnam veterans: 30-year follow-up. Archives of Internal Medicine 164(17):1908â1916. Boffeta P, Stellman SD, Garï¬nkel L. 1989. A caseâcontrol study of multiple myeloma nested in the American Cancer Society prospective study. International Journal of Cancer 43(4):554â559. Bond GG, Wetterstroem NH, Roush GJ, McLaren EA, Lipps TE, Cook RR. 1988. Cause speciï¬c mor- tality among employees engaged in the manufacture, formulation, or packaging of 2,4-dichloro- phenoxyacetic acid and related salts. British Journal of Industrial Medicine 45(2):98â105. Bosl GJ, Motzer RJ. 1997. Testicular germ-cell cancer. New England Journal of Medicine 337(4): 242â253.
502 VETERANS AND AGENT ORANGE: UPDATE 2006 Boyle C, Decouï¬e P, Delaney RJ, DeStefano F, Flock ML, Hunter MI, Joesoef MR, Karon JM, Kirk ML, Layde PM, McGee DL, Moyer LA, Pollock DA, Rhodes P, Scally MJ, Worth RM. 1987. Postservice Mortality Among Vietnam Veterans. Atlanta, GA: Centers for Disease Control. CEH 86-0076. 143 pp. Breslin P, Lee Y, Kang H, Burt V, Shepard BM. 1986. A Preliminary Report: The Vietnam Vet- erans Mortality Study. Washington, DC: Veterans Administration, Ofï¬ce of Environmental Epidemiology. Breslin P, Kang H, Lee Y, Burt V, Shepard BM. 1988. Proportionate mortality study of US Army and US Marine Corps veterans of the Vietnam War. Journal of Occupational Medicine 30(5):412â419. Brody JG, Aschengrau A, McKelvey W, Rudel RA, Swartz CH, Kennedy T. 2004. Breast cancer risk and historical exposure to pesticides from wide-area applications assessed with GIS. Environ- mental Health Perspectives 112(8):889â897. Brown LM, Blair A, Gibson R, Everett GD, Cantor KP, Schuman LM, Burmeister LF, Van Lier SF, Dick F. 1990. Pesticide exposures and other agricultural risk factors for leukemia among men in Iowa and Minnesota. Cancer Research 50(20):6585â6591. Brown LM, Burmeister LF, Everett GD, Blair A. 1993. Pesticide exposures and multiple myeloma in Iowa men. Cancer Causes and Control 4(2):153â156. Brunnberg S, Andersson P, Lindstam M, Paulson I, Poellinger L, Hanberg A. 2006. The constitutively active Ah receptor (CA-Ahr) mouse as a potential model for dioxin exposureâeffects in vital organs. Toxicology 224(3):191â201. Bueno de Mesquita HB, Doornbos G, Van der Kuip DA, Kogevinas M, Winkelmann R. 1993. Oc- cupational exposure to phenoxy herbicides and chlorophenols and cancer mortality in the Netherlands. American Journal of Industrial Medicine 23(2):289â300. Bullman TA, Kang HK, Watanabe KK. 1990. Proportionate mortality among US Army Vietnam vet- erans who served in Military Region I. American Journal of Epidemiology 132(4):670â674. Bullman TA, Watanabe KK, Kang HK. 1994. Risk of testicular cancer associated with surrogate measures of Agent Orange exposure among Vietnam veterans on the Agent Orange Registry. Annals of Epidemiology 4(1):11â16. Burmeister LF. 1981. Cancer mortality in Iowa farmers, 1971â1978. Journal of the National Cancer Institute 66(3):461â464. Burmeister LF, Van Lier SF, Isacson P. 1982. Leukemia and farm practices in Iowa. American Journal of Epidemiology 115(5):720â728. Burmeister LF, Everett GD, Van Lier SF, Isacson P. 1983. Selected cancer mortality and farm practices in Iowa. American Journal of Epidemiology 118(1):72â77. Burns CJ, Beard KK, Cartmill JB. 2001. Mortality in chemical workers potentially exposed to 2,4- dichlorophenoxyacetic acid (2,4-D) 1945â1994: An update. Occupational and Environmental Medicine 58(1):24â30. Burt VL, Breslin PP, Kang HK, Lee Y. 1987. Non-Hodgkinâs Lymphoma in Vietnam Veterans. Depart- ment of Medicine and Surgery, Veterans Administration, 33 pp. Buxbaum JN. 2004. The systemic amyloidoses. Current Opinion in Rheumatology 16(1):67â75. Cantor KP. 1982. Farming and mortality from non-Hodgkinâs lymphoma: A caseâcontrol study. International Journal of Cancer 29(3):239â247. Cantor KP, Blair A. 1984. Farming and mortality from multiple myeloma: A caseâcontrol study with the use of death certiï¬cates. Journal of the National Cancer Institute 72(2):251â255. Cantor KP, Blair A, Everett G, Gibson R, Burmeister LF, Brown LM, Schuman L, Dick FR. 1992. Pesticides and other agricultural risk factors for non-Hodgkinâs lymphoma among men in Iowa and Minnesota. Cancer Research 52(9):2447â2455. Caplan LS, Hall HI, Levine RS, Zhu K. 2000. Preventable risk factors for nasal cancer. Annals of Epidemiology 10(3):186â191.
CANCER 503 Carreon T, Butler MA, Ruder AM, Waters MA, Davis-King KE, Calvert GM, Schulte PA, Connally B, Ward EM, Sanderson WT, Heineman EF, Mandel JS, Morton RF, Reding DJ, Rosenman KD, Talaska G, Cancer B. 2005. Gliomas and farm pesticide exposure in women: The Upper Midwest Health Study. Environmental Health Perspectives 113(5):546â551. CDC (Centers for Disease Control and Prevention). 1990a. The association of selected cancers with service in the US military in Vietnam. III. Hodgkinâs disease, nasal cancer, nasopharyngeal cancer, and primary liver cancer. The Selected Cancers Cooperative Study Group. Archives of Internal Medicine 150(12):2495â2505. CDC. 1990b. The association of selected cancers with service in the US military in Vietnam. I. Non- Hodgkinâs lymphoma. Archives of Internal Medicine 150:2473â2483. CDVA (Commonwealth Department of Veteransâ Affairs). 1997a. Mortality of Vietnam Veterans: The Veteran Cohort Study. A Report of the 1996 Retrospective Cohort Study of Australian Vietnam Veterans. Canberra, Australia: Department of Veteransâ Affairs. CDVA. 1997b. Mortality of National Service Vietnam Veterans: A Report of the 1996 Retrospective Cohort Study of Australian Vietnam Veterans. Canberra, Australia: Department of Veteransâ Affairs. CDVA. 1998a. Morbidity of Vietnam Veterans: A Study of the Health of Australiaâs Vietnam Veteran Community. Volume 1: Male Vietnam Veterans Survey and Community Comparison Outcomes. Canberra, Australia: Department of Veteransâ Affairs. CDVA. 1998b. Morbidity of Vietnam Veterans: A Study of the Health of Australiaâs Vietnam Veteran Community. Volume 2: Female Vietnam Veterans Survey and Community Comparison Out- comes. Canberra, Australia: Department of Veteransâ Affairs. Chen YC, Su HJ, Guo YL, Hsueh YM, Smith TJ, Ryan LM, Lee MS, Christiani DC. 2003. Arsenic methylation and bladder cancer risk in Taiwan. Cancer Causes and Control 14(4):303â310. Cheng H, Aylward L, Beall C, Starr TB, Brunet RC, Carrier G, Delzell E. 2006. TCDD exposure- response analysis and risk assessment. Risk Analysis 26(4):1059â1071. Chiu BC, Weisenburger DD, Zahm SH, Cantor KP, Gapstur SM, Holmes F, Burmeister LF, Blair A. 2004. Agricultural pesticide use, familial cancer, and risk of non-Hodgkin lymphoma. Cancer Epidemiology, Biomarkers and Prevention 13(4):525â531. Chiu BC, Dave BJ, Blair A, Gapstur SM, Zahm SH, Weisenburger DD. 2006. Agricultural pesticide use and risk of t(14;18)-deï¬ned subtypes of non-Hodgkin lymphoma. Blood 108(4):1363â1369. Clapp RW. 1997. Update of cancer surveillance of veterans in Massachusetts, USA. International Journal of Epidemiology 26(3):679â681. Clapp RW, Cupples LA, Colton T, Ozonoff DM. 1991. Cancer surveillance of veterans in Massachu- setts, 1982â1988. International Journal of Epidemiology 20(1):7â12. Cocco P, Heineman EF, Dosemeci M. 1999. Occupational risk factors for cancer of the central nervous system (CNS) among US women. American Journal of Industrial Medicine 36(1):70â74. Coggon D, Pannett B, Winter PD, Acheson ED, Bonsall J. 1986. Mortality of workers exposed to 2-methyl-4-chlorophenoxyacetic acid. Scandinavian Journal of Work, Environment and Health 12(5):448â454. Coggon D, Pannett B, Winter P. 1991. Mortality and incidence of cancer at four factories making phenoxy herbicides. British Journal of Industrial Medicine 48(3):173â178. Cohen AD, Zhou P, Xiao Q, Fleisher M, Kalakonda N, Akhurst T, Chitale DA, Moscowitz MV, Dhodapkar J, Teruya-Feldstein D, Filippa D, Comenzo RL. 2004. Systemic AL amyloidosis due to non-Hodgkinâs lymphoma: An unusual clinicopathologic association. British Journal of Haematology 124:309â314. Cohen SM, Arnold LL, Eldan M, Lewis AS, Beck BD. 2006. Methylated arsenicals: the implications of metabolism and carcinogenicity studies in rodents to human risk assessment. Critical Reviews in Toxicology 36(2):99â133.
504 VETERANS AND AGENT ORANGE: UPDATE 2006 Collins JJ, Strauss ME, Levinskas GJ, Conner PR. 1993. The mortality experience of workers exposed to 2,3,7,8-tetrachlorodibenzo-p-dioxin in a trichlorophenol process accident. Epidemiology 4(1):7â13. Colt JS, Severson RK, Lubin J, Rothman N, Camann D, Davis S, Cerhan JR, Cozen W, Harge P. 2005. Organochlorines in carpet dust and non-Hodgkin lymphoma. Epidemiology 16(4):516â525. Comba P, Ascoli V, Belli S, Benedetti M, Gatti L, Ricci P, Tieghi A. 2003. Risk of soft tissue sarcomas and residence in the neighbourhood of an incinerator of industrial wastes. Occupational and Environmental Medicine 60(9):680â683. Cordier S, Le TB, Verger P, Bard D, Le CD, Larouze B, Dazza MC, Hoang TQ, Abenhaim L. 1993. Viral infections and chemical exposures as risk factors for hepatocellular carcinoma in Vietnam. International Journal of Cancer 55(2):196â201. Corrao G, Caller M, Carle F, Russo R, Bosia S, Piccioni P. 1989. Cancer risk in a cohort of licensed pesticide users. Scandinavian Journal of Work, Environment and Health 15(3):203â209. Costani G, Rabitti P, Mambrini A, Bai E, Berrino F. 2000. Soft tissue sarcomas in the general popula- tion living near a chemical plant in northern Italy. Tumori 86(5):381â383. Dalager NA, Kang HK. 1997. Mortality among Army Chemical Corps Vietnam veterans. American Journal of Industrial Medicine 31(6):719â726. Dalager NA, Kang HK, Burt VL, Weatherbee L. 1991. Non-Hodgkinâs lymphoma among Vietnam veterans. Journal of Occupational Medicine 33(7):774â779. Dalager NA, Kang HK, Thomas TL. 1995. Cancer mortality patterns among women who served in the military: The Vietnam experience. Journal of Occupational and Environmental Medicine 37(3):298â305. Davis BJ, McCurdy EA, Miller BD, Lucier GW, Tritscher AM. 2000. Ovarian tumors in rats induced by chronic 2,3,7,8-tetrachlorodibenzo-p-dioxin treatment. Cancer Research 60(19):5414â5419. Dean G. 1994. Deaths from primary brain cancers, lymphatic and haematopoietic cancers in agri- cultural workers in the Republic of Ireland. Journal of Epidemiology and Community Health 48(4):364â368. Demers A, Ayotte P, Brisson J, Dodin S, Robert J, Dewailly E. 2000. Risk and aggressiveness of breast cancer in relation to plasma organochlorine concentrations. Cancer Epidemiology, Biomarkers and Prevention 9(2):161â166. Demers A, Ayotte P, Brisson J, Dodin S, Robert J, Dewailly E. 2002. Plasma concentrations of poly- chlorinated biphenyls and the risk of breast cancer: A congener-speciï¬c analysis. American Journal of Epidemiology 155(7):629â635. Demers PA, Boffetta P, Kogevinas M, Blair A, Miller BA, Robinson CF, Roscoe RJ, Winter PD, Colin D, Matos E, et al. 1995. Pooled reanalysis of cancer mortality among ï¬ve cohorts of workers in wood-related industries. Scandinavian Journal of Work, Environment and Health 21(3):179â190. De Roos AJ, Hartge P, Lubin JH, Colt JS, Davis S, Cerhan JR, Severson RK, Cozen W, Patterson DG Jr, Needham LL, Rothman N. 2005. Persistent organochlorine chemicals in plasma and risk of non-Hodgkinâs lymphoma. Cancer Research 65(23):11214â11226. Desaulniers D, Leingartner K, Russo J, Perkins G, Chittim BG, Archer MC, Wade M, Yang J. 2001. Modulatory effects of neonatal exposure to TCDD or a mixture of PCBs, p,p -DDT, and p-p - DDE on methylnitrosourea-induced mammary tumor development in the rat. Environmental Health Perspectives 109:739â747. Desaulniers D, Leingartner K, Musicki B, Cole J, Li M, Charboneau M, Tsang BK. 2004. Lack of effects of postnatal exposure to a mixture of aryl hydrocarbon-receptor agonists on the devel- opment of methylnitrosourea-induced mammary tumors in Sprague-Dawley rats. Journal of Toxicology and Environmental Health, Part A 67(18):1457â1475. Dich J, Wiklund K. 1998. Prostate cancer in pesticide applicators in Swedish agriculture. Prostate 34(2):100â112.
CANCER 505 Donna A, Betta P-G, Robutti F, Crosignani P, Berrino F, Bellingeri D. 1984. Ovarian mesothelial tumors and herbicides: A caseâcontrol study. Carcinogenesis 5(7):941â942. Dubrow R, Paulson JO, Indian RW. 1988. Farming and malignant lymphoma in Hancock County, Ohio. British Journal of Industrial Medicine 45(1):25â28. Duell EJ, Millikan RC, Savitz DA, Newman B, Smith JC, Schell MJ, Sandler DP. 2000. A popula- tion-based caseâcontrol study of farming and breast cancer in North Carolina. Epidemiology 11(5):523â531. Dunson DB, Haseman JK, van Birgelen AP, Stasiewicz S, Tennant RW. 2000. Statistical analysis of skin tumor data from Tg.AC mouse bioassays. Toxicological Sciences 55(2):293â302. Engel LS, Hill DA, Hoppin JA, Lubin JH, Lynch CF, Pierce J, Samanic C, Sandler DP, Blair A, Alavanja MC. 2005. Pesticide use and breast cancer risk among farmersâ wives in the Agricul- tural Health Study. American Journal of Epidemiology 161(2):121â135. Eriksson M, Karlsson M. 1992. Occupational and other environmental factors and multiple myeloma: A population based caseâcontrol study. British Journal of Industrial Medicine 49(2):95â103. Eriksson M, Hardell L, Berg NO, Moller T, Axelson O. 1979. Caseâcontrol study on malignant mesenchymal tumor of the soft tissue and exposure to chemical substances. Lakartidningen 76(44):3872â3875. Eriksson M, Hardell L, Berg NO, Moller T, Axelson O. 1981. Soft-tissue sarcomas and expo- sure to chemical substances: A case-referent study. British Journal of Industrial Medicine 38(1):27â33. Fenton SE. 2006. Endocrine-disrupting compounds and mammary gland development: Early exposure and later life consequences. Endocrinology 147(6):S18âS24. Fett MJ, Nairn JR, Cobbin DM, Adena MA. 1987. Mortality among Australian conscripts of the Viet- nam conï¬ict era. II. Causes of death. American Journal of Epidemiology 125(15):878â884. Fingerhut MA, Halperin WE, Marlow DA, Piacitelli LA, Honchar PA, Sweeney MH, Greife AL, Dill PA, Steenland K, Suruda AJ. 1991. Cancer mortality in workers exposed to 2,3,7,8-tetrachloro- dibenzo-p-dioxin. New England Journal of Medicine 324(4):212â218. Fleming LE, Bean JA, Rudolph M, Hamilton K. 1999a. Mortality in a cohort of licensed pesticide applicators in Florida. Journal of Occupational and Environmental Medicine 56(1):14â21. Fleming LE, Bean JA, Rudolph M, Hamilton K. 1999b. Cancer incidence in a cohort of licensed pesticide applicators in Florida. Journal of Occupational and Environmental Medicine 41(4): 279â288. Floret N, Mauny F, Challier B, Arveux P, Cahn J-Y, Viel J-F. 2003. Dioxin emissions from a solid waste incinerator and risk of non-Hodgkin lymphoma. Epidemiology 14(4):392â398. Fritschi L, Benke G, Hughes AM, Kricker A, Turner J, Vajdic CM, Grulich A, Milliken S, Kaldor J, Armstrong BK. 2005. Occupational exposure to pesticides and risk of non-Hodgkinâs lym- phoma. American Journal of Epidemiology 162(9):849â857. Fritz WA, Lin TM, Moore RW, Cooke PS, Peterson RE. 2005. In utero and lactational 2,3,7,8- tetrachlorodibenzo-p-dioxin exposure: Effects on the prostate and its response to castration in senescent C57BL/6J mice. Toxicological Sciences 86(2):387â395. Fukuda Y, Nakamura K, Takano T. 2003. Dioxins released from incineration plants and mortality from major diseases: An analysis of statistical data by municipalities. Journal of Medical and Dental Sciences 50(4):249â255. Gallagher RP, Bajdik CD, Fincham S, Hill GB, Keefe AR, Coldman A, McLean DI. 1996. Chemical exposures, medical history, and risk of squamous and basal cell carcinoma of the skin. Cancer Epidemiology, Biomarkers and Prevention 5(6):419â424. Gambini GF, Mantovani C, Pira E, Piolatto PG, Negri E. 1997. Cancer mortality among rice growers in Novara Province, northern Italy. American Journal of Industrial Medicine 31(4):435â441. Gann PH. 1997. Interpreting recent trends in prostate cancer incidence and mortality. Epidemiology 8(2):117â120.
506 VETERANS AND AGENT ORANGE: UPDATE 2006 Garland FC, Gorham ED, Garland CF, Ferns JA. 1988. Non-Hodgkinâs lymphoma in US Navy per- sonnel. Archives of Environmental Health 43(6):425â429. Giri VN, Cassidy AE, Beebe-Dimmer J, Smith DC, Bock CH, Cooney KA. 2004. Association be- tween Agent Orange and prostate cancer: A pilot caseâcontrol study. Urology 63(4):757â760; discussion 760â761. Green LM. 1991. A cohort mortality study of forestry workers exposed to phenoxy acid herbicides. British Journal of Industrial Medicine 48(4):234â238. Greenwald P, Kovasznay B, Collins DN, Therriault G. 1984. Sarcomas of soft tissues after Vietnam service. Journal of the National Cancer Institute 73(5):1107â1109. Hallquist A, Hardell L, Degerman A, Boquist L. 1993. Occupational exposures and thyroid cancer: Results of a caseâcontrol study. European Journal of Cancer Prevention 2(4):345â349. Hansen ES, Hasle H, Lander F. 1992. A cohort study on cancer incidence among Danish gardeners. American Journal of Industrial Medicine 21(5):651â660. Hardell L. 1981. Relation of soft-tissue sarcoma, malignant lymphoma and colon cancer to phenoxy acids, chlorophenols and other agents. Scandinavian Journal of Work, Environment and Health 7(2):119â130. Hardell L, Bengtsson NO. 1983. Epidemiological study of socioeconomic factors and clinical ï¬nd- ings in Hodgkinâs disease, and reanalysis of previous data regarding chemical exposure. British Journal of Cancer 48(2):217â225. Hardell L, Ericksson M. 1999. A caseâcontrol study of non-Hodgkin lymphoma and exposure to pesticides. Cancer 85(6):1353â1360. Hardell L, Eriksson M, Lenner P, Lundgren E. 1981. Malignant lymphoma and exposure to chemicals, especially organic solvents, chlorophenols and phenoxy acids: A caseâcontrol study. British Journal of Cancer 43:169â176. Hardell L, Johansson B, Axelson O. 1982. Epidemiological study of nasal and nasopharyngeal cancer and their relation to phenoxy acid or chlorophenol exposure. American Journal of Industrial Medicine 3(3):247â257. Hardell L, Bengtsson NO, Jonsson U, Eriksson S, Larsson LG. 1984. Aetiological aspects on primary liver cancer with special regard to alcohol, organic solvents and acute intermittent porphyria: An epidemiological investigation. British Journal of Cancer 50(3):389â397. Hardell L, Eriksson M, Degerman A. 1994. Exposure to phenoxyacetic acids, chlorophenols, or or- ganic solvents in relation to histopathology, stage, and anatomical localization of non-Hodgkinâs lymphoma. Cancer Research 54(9):2386â2389. Hardell L, Nasman A, Ohlson CG, Fredrikson M. 1998. Caseâcontrol study on risk factors for tes- ticular cancer. International Journal of Oncology 13(6):1299â1303. Hardell L, Lindström G, van Bavel B, Hardell K, Linde A, Carlberg M, Liljegren G. 2001. Adipose tis- sue concentrations of dioxins and dibenzofurans, titers of antibodies to Epstein-Barr virus early antigen and the risk for non-Hodgkinâs lymphoma. Environmental Research 87(2):99â107. Hardell L, Eriksson M, Nordstrom M. 2002. Exposure to pesticides as risk factor for non-Hodgkinâs lymphoma and hairy cell leukemia: Pooled analysis of two Swedish caseâcontrol studies. Leu- kemia and Lymphoma 43(5):1043â1049. Harrison CJ, Mazzullo H, Ross FM, Cheung KL, Gerrard G, Harewood L, Mehta A, Lachmann HJ, Hawkins PN, Orchard KH. 2002. Translocations of 14q32 and deletions of 13q14 are com- mon chromosomal abnormalities in systemic amyloidosis. British Journal of Haematology 117(2):427â435. Hartge P, Colt JS, Severson RK, Cerhan JR, Cozen W, Camann D, Zahm SH, Davis S. 2005. Resi- dential herbicide use and risk of non-Hodgkin lymphoma. Cancer Epidemiology, Biomarkers and Prevention 14(4):934â937.
CANCER 507 Hayashi H, Kanisawa M, Yamanaka K, Ito T, Udaka N, Ohji H, Okudela K, Okada S, Kitamura H. 1998. Dimethylarsinic acid, a main metabolite of inorganic arsenics, has tumorigenicity and progression effects in the pulmonary tumors of A/J mice. Cancer Letters 125(1-2):83â88. Hayes RB. 1997. The carcinogenicity of metals in humans. Cancer Causes and Control 8(3): 371â385. Hebert CD, Harris MW, Elwell MR, Birnbaum LS. 1990. Relative toxicity and tumor-promoting abil- ity of 2,3,7,8-tetrachlorodibenzo-p-dioxin (TCDD), 2,3,4,7,8-pentachlorodibenzofuran (PCDF), and 1,2,3,4,7,8-hexachlorodibenzofuran (HCDF) in hairless mice. Toxicology and Applied Pharmacology 102(2):362â377. Henneberger PK, Ferris BG Jr, Monson RR. 1989. Mortality among pulp and paper workers in Berlin, New Hampshire. British Journal of Industrial Medicine 46(9):658â664. Hertzman C, Teschke K, Ostry A, Hershler R, Dimich-Ward H, Kelly S, Spinelli JJ, Gallagher RP, McBride M, Marion SA. 1997. Mortality and cancer incidence among sawmill workers exposed to chlorophenate wood preservatives. American Journal of Public Health 87(1):71â79. Hoar SK, Blair A, Holmes FF, Boysen CD, Robel RJ, Hoover R, Fraumeni JF. 1986. Agricultural herbicide use and risk of lymphoma and soft-tissue sarcoma. Journal of the American Medical Association 256(9):1141â1147. Hobbs CG, Birchall MA. 2004. Human papillomavirus infection in the etiology of laryngeal carci- noma. Current Opinion in Otolaryngology and Head and Neck Surgery 12(2):88â92. Hoffman RE, Stehr-Green PA, Webb KB, Evans RG, Knutsen AP, Schramm WF, Staake JL, Gibson BB, Steinberg KK. 1986. Health effects of long-term exposure to 2,3,7,8-tetrachlorodibenzo-p- dioxin. Journal of the American Medical Association 255(15):2031â2038. Holcombe M, Safe S. 1994. Inhibition of 7,12-dimethylbenzanthracene-induced rat mammary tumor growth by 2,3,7,8-tetrachlorodibenzo-p-dioxin. Cancer Letters 82(1):43â47. Holford TR, Zheng T, Mayne ST, Zahm SH, Tessari JD, Boyle P. 2000. Joint effects of nine polychlo- rinated biphenyl (PCB) congeners on breast cancer risk. International Journal of Epidemiology 29(6):975â982. Holmes AP, Bailey C, Baron RC, Bosanac E, Brough J, Conroy C, Haddy L. 1986. West Virginia Department of Health Vietnam-Era Veterans Mortality Study: Preliminary Report. Charlestown: West Virginia Health Department. Hooiveld M, Heederik DJ, Kogevinas M, Boffetta P, Needham LL, Patterson DG Jr, Bueno de Mesquita HB. 1998. Second follow-up of a Dutch cohort occupationally exposed to phenoxy herbicides, chlorophenols, and contaminants. American Journal of Epidemiology 147(9):891â901. Høyer AP, Jørgensen T, Brock JW, Grandjean P. 2000. Organochlorine exposure and breast cancer survival. Journal of Clinical Epidemiology 53(3):323â330. IARC (International Agency for Research on Cancer). 2001. Pathology and genetics of tumours of the haemopoietic and lymphoid tissues. In: Jaffe NL, Harris H, Stein, Vardiman JW, eds. World Health Organization, IARC. IOM (Institute of Medicine). 1994. Veterans and Agent Orange Health Effects of Herbicides Used in Vietnam. Washington, DC: National Academy Press. IOM. 1996. Veterans and Agent Orange: Update 1996. Washington, DC: National Academy Press. IOM. 1999. Veterans and Agent Orange: Update 1998. Washington, DC: National Academy Press. IOM. 2001. Veterans and Agent Orange: Update 2000. Washington, DC: National Academy Press. IOM. 2003. Veterans and Agent Orange: Update 2002. Washington, DC: The National Academies Press. IOM. 2005. Veterans and Agent Orange: Update 2004. Washington, DC: The National Academies Press. IOM. 2006. Asbestos: Selected Cancers. Washington, DC: The National Academies Press. Jemal A, Siegel R, Ward E, Murray T, Xu J, Smigal C, Thun MJ. 2006. Cancer statisticsâ2006. CA: A Cancer Journal for Clinicians 56(2):106â130. http://www.cancer.org/downloads/STT/CAFF- 2006PWSecured.pdf (Accessed March 6, 2007)].
508 VETERANS AND AGENT ORANGE: UPDATE 2006 Kang HK, Weatherbee L, Breslin PP, Lee Y, Shepard BM. 1986. Soft tissue sarcomas and military service in Vietnam: A case comparison group analysis of hospital patients. Journal of Occupa- tional Medicine 28(12):1215â1218. Kang HK, Mahan CM, Lee KY, Magee CA, Selvin S. 2000. Prevalence of gynecologic cancers among female Vietnam veterans. Journal of Occupational and Environmental Medicine 42(11): 1121â1127. Kato I, Watanabe-Meserve H, Koenig KL, Baptiste MS, Lillquist PP, Frizzera G, Burke JS, Moseson M, Shore RE. 2004. Pesticide product use and risk of non-Hodgkin lymphoma in women. En- vironmental Health Perspectives 112(13):1275â1281. Keller-Byrne JE, Khuder SA, Schaub EA, McAfee O. 1997. A meta-analysis of non-Hodgkinâs lym- phoma among farmers in the central United States. American Journal of Industrial Medicine 31(4):442â444. Kennedy C, Bajdik CD, Willemze R, Bouwes Bavinck JN. 2005. Chemical exposures other than ar- senic are probably not important risk factors for squamous cell carcinoma, basal cell carcinoma and malignant melanoma of the skin. British Journal of Dermatology 152(1):194â197. Ketchum NS, Michalek JE, Burton JE. 1999. Serum dioxin and cancer in veterans of Operation Ranch Hand. American Journal of Epidemiology 149(7):630â639. Key TJ, Schatzkin A, Willett WC, Allen NE, Spencer EA, Travis RC. 2004. Diet, nutrition and the prevention of cancer. Public Health Nutrition 7(1A):187â200. Kociba RJ, Keys DG, Beyer JE, Careon RM, Wade CE, Dittenber DA, Kalnins RP, Frauson LE, Park CN, Barnar SD, Hummel RA, Humiston CG. 1978. Results of a two-year chronic toxicity and oncogenicity study of 2,3,7,8-tetrachlorodibenzo-p-dioxin in rats. Toxicology and Applied Pharmacology 46:279â303. Kogan MD, Clapp RW. 1988. Soft tissue sarcoma mortality among Vietnam veterans in Massachu- setts, 1972 to 1983. International Journal of Epidemiology 17(1):39â43. Kogevinas M, Saracci R, Bertazzi PA, Bueno de Mesquita BH, Coggon D, Green LM, Kauppinen T, Littorin M, Lynge E, Mathews JD, Neuberger M, Osman J, Pearce N, Winkelmann R. 1992. Cancer mortality from soft-tissue sarcoma and malignant lymphomas in an international cohort of workers exposed to chlorophenoxy herbicides and chlorophenols. Chemosphere 25:1071â1076. Kogevinas M, Saracci R, Winkelmann R, Johnson ES, Bertazzi PA, Bueno de Mesquita BH, Kauppinen T, Littorin M, Lynge E, Neuberger M. 1993. Cancer incidence and mortality in women occu- pationally exposed to chlorophenoxy herbicides, chlorophenols, and dioxins. Cancer Causes and Control 4(6):547â553. Kogevinas M, Kauppinen T, Winkelmann R, Becher H, Bertazzi PA, Bas B, Coggon D, Green L, Johnson E, Littorin M, Lynge E, Marlow DA, Mathews JD, Neuberger M, Benn T, Pannett B, Pearce N, Saracci R. 1995. Soft tissue sarcoma and non-Hodgkinâs lymphoma in workers exposed to phenoxy herbicides, chlorophenols and dioxins: Two nested caseâcontrol studies. Epidemiology 6(4):396â402. Kogevinas M, Becher H, Benn T, Bertazzi PA, Boffetta P, Bueno de Mesquita HB, Coggon D, Colin D, Flesch-Janys D, Fingerhut M, Green L, Kauppinen T, Littorin M, Lynge E, Mathews JD, Neuberger M, Pearce N, Saracci R. 1997. Cancer mortality in workers exposed to phenoxy herbicides, chlorophenols, and dioxins. An expanded and updated international cohort study. American Journal of Epidemiology 145(12):1061â1075. Lampi P, Hakulinen T, Luostarinen T, Pukkala E, Teppo L. 1992. Cancer incidence following chlo- rophenol exposure in a community in southern Finland. Archives of Environmental Health 47(3):167â175. LaVecchia C, Negri E, DâAvanzo B, Franceschi S. 1989. Occupation and lymphoid neoplasms. British Journal of Cancer 60(3):385â388. Lawrence CE, Reilly AA, Quickenton P, Greenwald P, Page WF, Kuntz AJ. 1985. Mortality patterns of New York State Vietnam veterans. American Journal of Public Health 75(3):277â279.
CANCER 509 Leavy J, Ambrosini G, Fritschi L. 2006. Vietnam military service history and prostate cancer. BMC Public Health 6:75. Lee WJ, Lijinsky W, Heineman EF, Markin RS, Weisenburger DD, Ward MH. 2004a. Agricultural pesticide use and adenocarcinomas of the stomach and oesophagus. Occupational and Environ- mental Medicine 61(9):743â749. Lee WJ, Cantor KP, Berzofsky JA, Zahm SH, Blair A. 2004b. Non-Hodgkinâs lymphoma among asthmatics exposed to pesticides. International Journal of Cancer 111(2):298â302. Lee WJ, Colt JS, Heineman EF, McComb R, Weisenburger DD, Lijinsky W, Ward MH. 2005. Agricultural pesticide use and risk of glioma in Nebraska, United States. Occupational and Environmental Medicine 62(11):786â792. Lee WJ, Purdue MP, Stewart P, Schenk M, De Roos AJ, Cerhan JR, Severson RK, Cozen W, Hartge P, Blair A. 2006. Asthma history, occupational exposure to pesticides and the risk of non- Hodgkinâs lymphoma. International Journal of Cancer 118(12):3174â3176. Lin TM, Rasmussen NT, Moore RW, Albrecht RM, Peterson RE. 2004. 2,3,7,8-Tetrachlorodibenzo- p-dioxin inhibits prostatic epithelial bud formation by acting directly on the urogenital sinus. Journal of Urology 172(1):365â368. Liu J, Singh B, Tallini G, Carlson DL, Katabi N, Shaha A, Tuttle RM, Ghossein RA. 2006. Follicular variant of papillary thyroidcarcinoma: A clinicopathologic study of a problematic entity. Cancer 107:1255â1264. Lynge E. 1985. A follow-up study of cancer incidence among workers in manufacture of phenoxy herbicides in Denmark. British Journal of Cancer 52(2):259â270. Lynge E. 1993. Cancer in phenoxy herbicide manufacturing workers in Denmark, 1947â87âAn update. Cancer Causes and Control 4(3):261â272. Mack TM. 1995. Sarcomas and other malignancies of soft tissue, retroperitoneum, peritoneum, pleura, heart, mediastinum, and spleen. Cancer 75(1):211â244. Magnani C, Coggon D, Osmond C, Acheson ED. 1987. Occupation and ï¬ve cancers: A caseâcontrol study using death certiï¬cates. British Journal of Industrial Medicine 44(11):769â776. Mahan CM, Bullman TA, Kang HK, Selvin S. 1997. A caseâcontrol study of lung cancer among Vietnam veterans. Journal of Occupational and Environmental Medicine 39(8):740â747. Manz A, Berger J, Dwyer JH, Flesch-Janys D, Nagel S, Waltsgott H. 1991. Cancer mortality among workers in chemical plant contaminated with dioxin. Lancet 338(8773):959â964. Mayo Clinic. 2007. Tonsil Diagnosis. http://www.mayoclinic.org/tonsil-cancer/diagnosis.html (Ac- cessed February 9, 2007). McDufï¬e HH, Klaassen DJ, Dosman JA. 1990. Is pesticide use related to the risk of primary lung cancer in Saskatchewan? Journal of Occupational Medicine 32(10):996â1002. McDufï¬e HH, Pahwa P, McLaughlin JR, Spinelli JJ, Fincham S, Dosman JA, Robson D, Skinnider LF, Choi NW. 2001. Non-Hodgkinâs lymphoma and speciï¬c pesticide exposures in men: Cross-Canada study of pesticides and health. Cancer Epidemiology, Biomarkers and Prevention 10(11):1155â1163. McDufï¬e HH, Pahwa P, Robson D, Dosman JA, Fincham S, Spinelli JJ, McLaughlin JR. 2005. Insect repellents, phenoxyherbicide exposure, and non-Hodgkinâs lymphoma. Journal of Occupational and Environmental Medicine 47(8):806â816. McGee SF, Lanigan F, Gilligan E, Groner B. 2006. Mammary gland biology and breast cancer. Conference on Common Molecular Mechanisms of Mammary Gland Development and Breast Cancer Progression. EMBO Reports 7(11):1084â1088. McLean D, Pearce N, Langseth H, Jäppinen P, Szadkowska-Stanczyk I, Person B, Wild P, Ki- shi R, Lynge E, Henneberger P, Sala M, Teschke K, Kauppinen T, Colin D, Kogevinas M, Boffetta. 2006. Cancer mortality in workers exposed to organochlorine compounds in the pulp and paper industry: An international collaborative study. Environmental Health Perspectives 114(7):1007â1012.
510 VETERANS AND AGENT ORANGE: UPDATE 2006 Mellemgaard A, Engholm G, McLaughlin JK, Olsen JH. 1994. Occupational risk factors for renal-cell carcinoma in Denmark. Scandinavian Journal of Work, Environment and Health 20(3):160â165. Merletti F, Richiardi L, Bertoni F, Ahrens W, Buemi A, Costa-Santos C, Eriksson M, Guenel P, Kaerlev L, Jockel K-H, Llopis-Gonzalez A, Merler E, Miranda A, Morales-Suarez-Varela MM, Olsson H, Fletcher T, Olsen J. 2006. Occupational factors and risk of adult bone sarcomas: A multicentric caseâcontrol study in Europe. International Journal of Cancer 118(3):721â727. Michalek JE, Wolfe WH, Miner JC. 1990. Health status of Air Force veterans occupationally ex- posed to herbicides in Vietnam. II. Mortality. Journal of the American Medical Association 264(14):1832â1836. Miligi L, Costantini AS, Bolejack V, Veraldi A, Benvenuti A, Nanni O, Ramazzotti V, Tumino R, Stagnaro E, Rodella S, Fontana A, Vindigni C, Vineis P. 2003. Non-Hodgkinâs lymphoma, leu- kemia, and exposures in agriculture: Results from the Italian Multicenter CaseâControl Study. American Journal of Industrial Medicine 44:627â636. Miller BA, Kolonel LN, Bernstein L, Young JL Jr, Swanson GM, West D, Key CR, Liff JM, Glover CS, Alexander GA, et al. (eds). 1996. Racial/Ethnic Patterns of Cancer in the United States 1988â1992. Bethesda, MD: National Cancer Institute. NIH Pub. No. 96-4104. Mills PK, Yang R. 2005. Breast cancer risk in Hispanic agricultural workers in California. Interna- tional Journal of Occupational and Environmental Health 11(2):123â131. Mills PK, Yang R. 2006. Regression analysis of pesticide use and breast cancer incidence in California Latinas. Journal of Environmental Health 68(6):15â22 and 43â44. Mills PK, Yang R, Riordan D. 2005. Lymphohematopoietic cancers in the United Farm Workers of America (UFW), 1988â2001. Cancer Causes and Control 16(7):823â830. Moennikes O, Loeppen S, Buchmann A, Andersson P, Ittrich C, Poellinger L, Schwarz M. 2004. A constitutively active dioxin/aryl hydrocarbon receptor promotes hepatocarcinogenesis in mice. Cancer Research 64(14):4707â4710. Morris PD, Koepsell TD, Daling JR, Taylor JW, Lyon JL, Swanson GM, Child M, Weiss NS. 1986. Toxic substance exposure and multiple myeloma: A caseâcontrol study. Journal of the National Cancer Institute 76(6):987â994. Morrison H, Semenciw RM, Morison D, Magwood S, Mao Y. 1992. Brain cancer and farming in western Canada. Neuroepidemiology 11(4-6):267â276. Morrison H, Savitz D, Semenciw RM, Hulka B, Mao Y, Morison D, Wigle D. 1993. Farming and prostate cancer mortality. American Journal of Epidemiology 137(3):270â280. Morrison HI, Semenciw RM, Wilkins K, Mao Y, Wigle DT. 1994. Non-Hodgkinâs lymphoma and agricultural practices in the prairie provinces of Canada. Scandinavian Journal of Work, Envi- ronment, and Health 20(1):42â47. Mulero-Navarro S, Carvajal-Gonzalez JM, Herranz M, Ballestar E, Fraga MF, Ropero S, Esteller M, Fernandez-Salguero PM. 2006. The dioxin receptor is silenced by promoter hypermethylation in human acute lymphoblastic leukemia through inhibition of Sp1 binding. Carcinogenesis 27(5):1099â1104. Musicco M, Sant M, Molinari S, Filippini G, Gatta G, Berrino F. 1988. A caseâcontrol study of brain gliomas and occupational exposure to chemical carcinogens: The risks to farmers. American Journal of Epidemiology 128:778â785. Nanni O, Amadori D, Lugaresi C, Falcini F, Scarpi E, Saragoni A, Buiatti E. 1996. Chronic lympho- cytic leukaemias and non-Hodgkinâs lymphomas by histological type in farming-animal breed- ing workers: A population caseâcontrol study based on a priori exposure matrices. Occupational and Environmental Medicine 53(10):652â657. Navas-Acien A, Pollan M, Gustavsson P, Plato N. 2002. Occupation, exposure to chemicals and risk of gliomas and meningiomas in Sweden. American Journal of Industrial Medicine 42(3):214â227.
CANCER 511 NCI (National Cancer Institute). 2006. Surveillance, Epidemiology, and End Results (SEER) In- cidence and US Mortality Statistics: SEER IncidenceâCrude Rates for White/Black/Other 1973â2002. http://seer.cancer.gov/canques/ (Accessed June 15, 2006). Nordby KC, Andersen A, Kristensen P. 2004. Incidence of lip cancer in the male Norwegian agricul- tural population. Cancer Causes and Control 15(6):619â626. Nordstrom M, Hardell L, Magnuson A, Hagberg H, Rask-Andersen A. 1998. Occupational exposures, animal exposures and smoking as risk factors for hairy cell leukemia evaluated in a caseâcontrol study. British Journal of Cancer 77(11):2048â2052. NTP (National Toxicology Program). 1982a. Technical Report Series No. 209. Carcinogenesis Bio- assay of 2,3,7,8-Tetrachlorodibenzo-p-dioxin (CAS No. 1746-01-6) in Osborne-Mendel Rats and B6c3F1 Mice (Gavage Study). NIH Publication No. 82-1765. 195 pp. National Toxicology Program, Research Triangle Park, NC, and Bethesda, MD. NTP. 1982b. Technical Report Series No. 201. Carcinogenesis Bioassay of 2,3,7,8-Ttetrachloro- dibenzo-p-dioxin (CAS No. 1746-01-6) in Swiss-Webster Mice (Dermal Study). National Toxi- cology Program. Research Triangle Park, NC, and Bethesda, MD. NTP. 2006. NTP Technical Report on the Toxicology and Carcinogenesis Studies of 2,3,7,8-Tetra- chlorodibenzo-p-dioxin (TCDD) (CAS No. 1746-01-6) in Female Harlan Sprague-Dawley Rats (Gavage Studies). Issue 521:4â232. National Toxicology Program, Research Triangle Park, NC, and Bethesda, MD. Nyska A, Jokinen MP, Brix AE, Sells Dm, Wyde ME, Orzech D, Haseman JK, Flake G, Walker NJ. 2004. Exocrine pancreatic pathology in female Harlan Sprague-Dawley rats after chronic treatment with 2,3,7,8-tetrachlorodibenzo-p-dioxin and dioxin-like compounds. Environmental Health Perspectives 112(8):903â909. Nyska A, Yoshizawa K, Jokinen MP, Brix AE, Sells DM, Wyde ME, Orzech DP, Kissling GE, Walker NJ. 2005. Olfactory epithelial metaplasia and hyperplasia in female Harlan Sprague- Dawley rats following chronic treatment with polychlorinated biphenyls. Toxicologic Pathology 33(3):371â377. OâBrien TR, Decouï¬e P, Boyle CA.1991. Non-Hodgkinâs lymphoma in a cohort of Vietnam veterans. American Journal of Public Health 81:758â760. Ojajärvi IA, Partanen TJ, Ahlbom A, Boffetta P, Hakulinen T, Jourenkova N, Kauppinen TP, Kogevinas M, Porta M, Vainio HU, Weiderpass E, Wesseling CH. 2000. Occupational exposures and pan- creatic cancer: a meta-analysis. Occupational and Environmental Medicine 57:316â324. Olsson H, Brandt L. 1988. Risk of non-Hodgkinâs lymphoma among men occupationally exposed to organic solvents. Scandinavian Journal of Work, Environment and Health 14:246â251. Ott MG, Zober A. 1996. Cause speciï¬c mortality and cancer incidence among employees exposed to 2,3,7,8-TCDD after a 1953 reactor accident. Occupational and Environmental Medicine 53:606â612. Pahwa P, McDufï¬e HH, Dosman J, Robson D, McLaughlin JR, Spinelli JJ, Fincham S. 2003. Ex- posure to animals and selected risk factors among Canadian farm residents with Hodgkinsâ disease, multiple myeloma, or soft tissue sarcoma. Journal of Occupational and Environmental Medicine 45(8):857â868. Pahwa P, McDufï¬e HH, Dosman JA, McLaughlin JR, Spinelli JJ, Robson D, Fincham S. 2006. Hodgkin lymphoma, multiple myeloma, soft tissue sarcomas, insect repellents, and phenoxy- herbicides. Journal of Occupational and Environmental Medicine 48(3):264â274. Pavuk M, Michalek JE, Schecter A, Ketchum NS, Akhtar FZ, Fox KA. 2005. Did TCDD exposure or service in Southeast Asia increase the risk of cancer in Air Force Vietnam veterans who did not spray Agent Orange? Journal of Occupational and Environmental Medicine 47(4):335â342. Pavuk M, Michalek JE, Ketchum NS. 2006. Prostate cancer in US Air Force veterans of the Vietnam War. Journal of Exposure Science and Environmental Epidemiology 16(2):184â190.
512 VETERANS AND AGENT ORANGE: UPDATE 2006 Pearce NE, Smith AH, Fisher DO. 1985. Malignant lymphoma and multiple myeloma linked with agricultural occupations in a New Zealand cancer registry-based sudy. American Journal of Epidemiology 121:225â237. Pearce NE, Smith AH, Howard JK, Sheppard RA, Giles HJ, Teague CA. 1986. Non-Hodgkinâs lymphoma and exposure to phenoxyherbicides, chlorophenols, fencing work, and meat works employment: A caseâcontrol study. British Journal of Industrial Medicine 43:75â83. Pearce NE, Sheppard RA, Smith AH, Teague CA. 1987. Non-Hodgkinâs lymphoma and farming: An expanded caseâcontrol study. International Journal of Cancer 39:155â161. Percy C, Ries GL, Van Holten VD. 1990. The accuracy of liver cancer as the underlying cause of death on death certiï¬cates. Public Health Reports 105:361â368. Persson B, Dahlander AM, Fredriksson M, Brage HN, Ohlson CG, Axelson O. 1989. Malignant lym- phomas and occupational exposures. British Journal of Industrial Medicine 46:516â520. Persson B, Fredriksson M, Olsen K, Boeryd B, Axelson O. 1993. Some occupational exposures as risk factors for malignant lymphomas. Cancer 72:1773â1778. Pesatori AC, Consonni D, Tironi A, Landi MT, Zocchetti C, Bertazzi PA. 1992. Cancer morbidity in the Seveso area, 1976â1986. Chemosphere 25:209â212. Petreas M, Smith D, Hurley S, Jeffrey SS, Gilliss D, Reynolds P. 2004. Distribution of persistent, lipid-soluble chemicals in breast and abdominal adipose tissues: Lessons learned from a breast cancer study. Cancer Epidemiology, Biomarkers and Prevention 13(3):416â424. Poland A, Palen D, Glover E. 1982. Tumour promotion by TCDD in skin of HRS/J hairless mice. Nature 300(5889):271â273. Raaschou-Nielsen O, Pavuk M, LeBlanc A, Dumas P, Philippe Weber J, Olsen A, Tjonneland A, Overvad K, Olsen JH. 2005. Adipose organochlorine concentrations and risk of breast cancer among postmenopausal Danish women. Cancer Epidemiology, Biomarkers and Prevention 14(1):67â74. Rajkumar SV, Gertz MA, Kyle RA. 1998. Primary systemic amyloidosis with delayed progression to multiple myeloma. Cancer 82(8):1501â1505. Rajkumar SV, Dispenzieri A, Kyle RA. 2006. Monoclonal gammopathy of undetermined signiï¬cance, Waldenstrom macroglobulinemia, AL amyloidosis, and related plasma cell disorders: Diagnosis and treatment. Mayo Clinic Proceedings 81(5):693â703. Ramlow JM, Spadacene NW, Hoag SR, Stafford BA, Cartmill JB, Lerner PJ. 1996. Mortality in a cohort of pentachlorophenol manufacturing workers, 1940â1989. American Journal of Indus- trial Medicine 30:180â194. Rao MS, Subbarao V, Prasad JD, Scarpelli DG. 1988. Carcinogenicity of 2,3,7,8-tetrachloridibenzo- p-dioxin in the Syrian golden hamster. Carcinogenesis 9(9):1677â1679. Reif JS, Pearce N, Fraser J. 1989. Occupational risks of brain cancer: A New Zealand cancer registry- based study. Journal of Occupational Medicine 31(10):863â867. Revich B, Aksel E, Ushakova T, Ivanova I, Zhuchenko N, Klyuev N, Brodsky B, Sotskov Y. Dioxin exposure and public health in Chapaevsk, Russia. Chemosphere 43(4-7):951â966. Reynolds P, Hurley SE, Goldberg DE, Anton-Culver H, Bernstein L, Deapen D, Horn-Ross PL, Peel D, Pinder R, Ross RK, West D, Wright WE, Ziogas A. 2004. Residential proximity to agri- cultural pesticide use and incidence of breast cancer in the California Teachers Study cohort. Environmental Research 96(2):206â218. Reynolds P, Hurley SE, Petreas M, Goldberg DE, Smith D, Gilliss D, Mahoney ME, Jeffrey SS. 2005. Adipose levels of dioxins and risk of breast cancer. Cancer Causes and Control 16(5):525â535. Riedel D, Pottern LM, Blattner WA. 1991. Etiology and epidemiology of multiple myeloma. In: Wiernick PH, Camellos G, Kyle RA, Schiffer CA, eds. Neoplastic Disease of the Blood and Blood Forming Organs. New York: Churchill Livingstone.
CANCER 513 Riihimaki V, Asp S, Hernberg S. 1982. Mortality of 2,4-dichlorophenoxyacetic acid and 2,4,5-trichlo- rophenoxyacetic acid herbicide applicators in Finland: First report of an ongoing prospective cohort study. Scandinavian Journal of Work, Environment and Health 8:37â42. Rix BA, Villadsen E, Engholm G, Lynge E. 1998. Hodgkinâs disease, pharyngeal cancer, and soft tissue sarcomas in Danish paper mill workers. Journal of Occupational and Environmental Medicine 40(1):55â62. Robinson CF, Waxweiler RJ, Fowler DP. 1986. Mortality among production workers in pulp and paper mills. Scandinavian Journal of Work, Environment and Health 12:552â560. Robinson CF, Schnorr TM, Cassinelli RT, Calvert GM, Steenland K, Gersic CM, Schubauer-Bergian MK. 2006. Tenth Revision U.S. Mortality Rates: For Use with the NIOSH Life Table Analysis System. Journal of Occupational and Environmental Medicine 48(7):662â667. Ronco G, Costa G, Lynge E. 1992. Cancer risk among Danish and Italian farmers. British Journal of Industrial Medicine 49:220â225. Ruder AM, Waters MA, Butler MA, Carreon T, Calvert GM, Davis-King KE, Schulte PA, Sanderson WT, Ward EM, Connally LB, Heineman EF, Mandel JS, Morton RF, Reding DJ, Rosenman KD, Talaska G. 2004. Gliomas and farm pesticide exposure in men: The Upper Midwest Health Study. Archives of Environmental Health 59(12):650â657. Saracci R, Kogevinas M, Bertazzi PA, Bueno de Mesquita BH, Coggon D, Green LM, Kauppinen T, LâAbbe KA, Littorin M, Lynge E, Mathews JD, Neuberger M, Osman J, Pearce N, Winkelmann R. 1991. Cancer mortality in workers exposed to chlorophenoxy herbicides and chlorophenols. Lancet 338:1027â1032. Schreinemachers DM. 2000. Cancer mortality in four northern wheat-producing states. Environmental Health Perspectives 108(9):873â881. Semenciw RM, Morrison HI, Morison D, Mao Y. 1994. Leukemia mortality and farming in the prairie provinces of Canada. Canadian Journal of Public Health 85:208â211. Sharma-Wagner S, Chokkalingam AP, Malker HS, Stone BJ, McLaughlin JK, Hsing AW. 2000. Occupation and prostate cancer risk in Sweden. Journal of Occupational and Environmental Medicine 42(5):517â525. Simanainen U, Adamsson A, Tuomisto JT, Miettinen HM, Toppari J, Tuomisto J, Viluksela M. 2004a. Adult 2,3,7,8-tetrachlorodibenzo-p-dioxin (TCDD) exposure and effects on male re- productive organs in three differentially TCDD-susceptible rat lines. Toxicological Sciences 81(2):401â407. Simanainen U, Haavisto T, Tuomisto JT, Paranko J, Toppari J, Tuomisto J, Peterson RE, Viluksela M. 2004b. Pattern of male reproductive system effects after in utero and lactational 2,3,7,8- tetrachlorodibenzo-p-dioxin (TCDD) exposure in three differentially TCDD-sensitive rat lines. Toxicological Sciences 80(1):101â108. Smith AH, Pearce NE. 1986. Update on soft tissue sarcoma and phenoxyherbicides in New Zealand. Chemosphere 15:1795â1798. Smith AH, Fisher DO, Giles HJ, Pearce NE. 1983. The New Zealand soft tissue sarcoma caseâcontrol study: Interview ï¬ndings concerning phenoxyacetic acid exposure. Chemosphere 12:565â571. Smith AH, Pearce NE, Fisher DO, Giles HJ, Teague CA, Howard JK. 1984. Soft tissue sarcoma and exposure to phenoxyherbicides and chlorophenols in New Zealand. Journal of the National Cancer Institute 73:1111â1117. Smith JG, Christophers AJ. 1992. Phenoxy herbicides and chlorophenols: A caseâcontrol study on soft tissue sarcoma and malignant lymphoma. British Journal of Cancer 65:442â448. Smith-Warner SA, Spiegelman D, Yaun SS, van den Brandt PA, Folsom AR, Goldbohm RA, Graham S, Holmberg L, Howe GR, Marshall JR, Miller AB, Potter JD, Speizer FE, Willett WC, Wolk A, Hunter DJ. 1998. Alcohol and breast cancer in women: A pooled analysis of cohort studies. Journal of the American Medical Association 279(7):535â540. Solet D, Zoloth SR, Sullivan C, Jewett J, Michaels DM. 1989. Patterns of mortality in pulp and paper workers. Journal of Occupational Medicine 31:627â630.
514 VETERANS AND AGENT ORANGE: UPDATE 2006 Solomon A. 1999. What is amyloidosis? Myeloma Today 3(2). http://myeloma.org/MyelomaToday/ Volume2/Number3/imf_asa.html (Accessed December 19, 2000). Steenland K, Piacitelli L, Deddens J, Fingerhut M, Chang LI. 1999. Cancer, heart disease, and diabe- tes in workers exposed to 2,3,7,8-tetrachlorodibenzo-p-dioxin. Journal of the National Cancer Institute 91(9):779â786. Svensson BG, Mikoczy Z, Stromberg U, Hagmar L. 1995. Mortality and cancer incidence among Swedish ï¬shermen with a high dietary intake of persistent organochlorine compounds. Scandi- navian Journal of Work, Environmental and Health 21(2):106â115. Swaen GMH, van Vliet C, Slangen JJM, Sturmans F. 1992. Cancer mortality among licensed herbi- cide applicators. Scandinavian Journal of Work, Environment and Health 18:201â204. Swaen GM, van Amelsvoort LG, Slangen JJ, Mohren DC. 2004. Cancer mortality in a cohort of li- censed herbicide applicators. International Archives of Occupational and Environmental Health 77(4):293â295. ât Mannetje A, McLean D, Cheng S, Boffetta P, Colin D, Pearce N. 2005. Mortality in New Zealand workers exposed to phenoxy herbicides and dioxins. Occupational and Environmental Medicine 62(1):34â40. Tarone RE, Hayes HM, Hoover RN, Rosenthal JF, Brown LM, Pottern LM, Javadpour N, OâConnell KJ, Stutzman RE. 1991. Service in Vietnam and risk of testicular cancer. Journal of the National Cancer Institute 83:1497â1499. Thiess AM, Frentzel-Beyme R, Link R. 1982. Mortality study of persons exposed to dioxin in a trichlorophenol-process accident that occurred in the BASF AG on November 17, 1953. Ameri- can Journal of Industrial Medicine 3:179â189. Thomas TL. 1987. Mortality among ï¬avour and fragrance chemical plant workers in the United States. British Journal of Industrial Medicine 44:733â737. Thomas TL, Kang HK. 1990. Mortality and morbidity among Army Chemical Corps Vietnam veter- ans: a preliminary report. American Journal of Industrial Medicine 18:665â673. Thomas TL, Kang H, Dalager N. 1991. Mortality among women Vietnam veterans, 1973â1987. American Journal of Epidemiology 134:973â980. Thörn à , Gustavsson P, Sadigh J, Westerlund-Hännerstrand B, Hogstedt C. 2000. Mortality and can- cer incidence among Swedish lumberjacks exposed to phenoxy herbicides. Occupational and Environmental Medicine 57:718â720. Toth K, Somfai-Relle S, Sugar J, Bence J. 1979. Carcinogenicity testing of herbicide 2,4,5-trichlo- rophenoxyethanol containing dioxin and of pure dioxin in Swiss mice. Nature 278(5704): 548â549. Torchio P, Lepore AR, Corrao G, Comba P, Settimi L, Belli S, Magnani C, di Orio F. 1994. Mor- tality study on a cohort of Italian licensed pesticide users. Science of the Total Environment 149(3):183â191. Tuomisto JT, Pekkanen J, Kiviranta H, Tukiainen E, Vartiainen T, Tuomisto J. 2004. Soft-tissue sar- coma and dioxin: A caseâcontrol study. International Journal of Cancer 108(6):893â900. US Census. 1999. Statistical Abstract of the United States: 1999, 119th Edition. Washington, DC: US Bureau of the Census. van Grevenynghe J, Bernard M, Langouet S, Le Berre C, Fest T, Fardel O. 2005. Human CD34- positive hematopoietic stem cells constitute targets for carcinogenic polycyclic aromatic hydro- carbons. Journal of Pharmacology and Experimental Therapeutics 314(2):693â702. Van Miller JP, Lalich JJ, Allen JR. 1977. Increased incidence of neoplasms in rats exposed to low levels of 2,3,7,8-tetrachlorodibenzo-p-dioxin. Chemosphere 9:537â544. Viel JF, Arveux P, Baverel J, Cahn JY. 2000. Soft-tissue sarcoma and non-Hodgkinâs lymphoma clusters around a municipal solid waste incinerator with high dioxin emission levels. American Journal of Epidemiology 152(1):13â19.
CANCER 515 Vineis P, Terracini B, Ciccone G, Cignetti A, Colombo E, Donna A, Mafï¬ L, Pisa R, Ricci P, Zanini E, Comba P. 1986. Phenoxy herbicides and soft-tissue sarcomas in female rice weeders. A population-based case-referent study. Scandinavian Journal of Work, Environment and Health 13:9â17. Vineis P, Faggiano F, Tedeschi M, Ciccone G. 1991. Incidence rates of lymphomas and soft-tissue sarcomas and environmental measurements of phenoxy herbicides. Journal of the National Cancer Institute 83:362â363. Visintainer PF, Barone M, McGee H, Peterson EL. 1995. Proportionate mortality study of Vietnam-era veterans of Michigan. Journal of Occupational and Environmental Medicine 37(4):423â428. Vorderstrasse BA, Fenton SE, Bohn AA, Cundiff JA, Lawrence BP. 2004. A novel effect of dioxin: Exposure during pregnancy severely impairs mammary gland differentiation. Toxicological Sciences 78(2):248â257. Walker NJ, Wyde ME, Fischer LJ, Nyska A, Bucher JR. 2006. Comparison of chronic toxicity and carcinogenicity of 2,3,7,8-tetrachlorodibenzo-p-dioxin (TCDD) in 2-year bioassays in female Sprague-Dawley rats. Molecular Nutrition and Food Research 50(10):934â944. Warner M, Eskenazi B, Mocarelli P, Gerthoux PM, Samuels S, Needham L, Patterson D, Brambilla P. 2002. Serum dioxin concentrations and breast cancer risk in the Seveso Womenâs Health Study. Environmental Health Perspectives 110(7):625â628. Watanabe KK, Kang HK. 1995. Military service in Vietnam and the risk of death from trauma and selected cancers. Annals of Epidemiology 5:407â412. Watanabe KK, Kang HK. 1996. Mortality patterns among Vietnam veterans: A 24-year retrospective analysis. Journal of Occupational and Environmental Medicine 38(3):272â278. Watanabe KK, Kang HK, Thomas TL. 1991. Mortality among Vietnam veterans: With methodological considerations. Journal of Occupational Medicine 33:780â785. Waterhouse D, Carman WJ, Schottenfeld D, Gridley G, McLean S. 1996. Cancer incidence in the rural community of Tecumseh, Michigan: A pattern of increased lymphopoietic neoplasms. Cancer 77(4):763â770. Wei M, Wanibuchi H, Morimura K, Iwai S, Yoshida K, Endo G, Nakae D, Fukushima S. 2002. Carci- nogenicity of dimethylarsinic acid in make F344 rats and genetic alterations in incuded urinary bladder tumors. Carcinogenesis 23(8):1387â1397. Weiderpass E, Adami HO, Baron JA, Wicklund-Glynn A, Aune M, Atuma S, Persson I. 2000. Or- ganochlorines and endometrial cancer risk. Cancer Epidemiology, Biomarkers and Prevention 9:487â493. Wigle DT, Semenciw RB, Wilkins K, Riedel D, Ritter L, Morrison HI, Mao Y. 1990. Mortality study of Canadian male farm operators: Non-Hodgkinâs lymphoma mortality and agricultural practices in Saskatchewan. Journal of the National Cancer Institute 82:575â582. Wiklund K. 1983. Swedish agricultural workers: A group with a decreased risk of cancer. Cancer 51:566â568. Wiklund K, Lindefors BM, Holm LE. 1988. Risk of malignant lymphoma in Swedish agricultural and forestry workers. British Journal of Industrial Medicine 45:19â24. Wiklund K, Dich J, Holm LE, Eklund G. 1989a. Risk of cancer in pesticide applicators in Swedish agriculture. British Journal of Industrial Medicine 46:809â814. Wiklund K, Dich J, Holm LE. 1989b. Risk of soft tissue sarcoma, Hodgkinâs disease and non-Hodgkinâs lymphoma among Swedish licensed pesticide applicators. Chemosphere 18:395â400. Wolfe WH, Michalek JE, Miner JC, Rahe A, Silva J, Thomas WF, Grubbs WD, Lustik MB, Karrison TG, Roegner RH, Williams DE. 1990. Health status of Air Force veterans occupationally ex- posed to herbicides in Vietnam. I. Physical health. Journal of the American Medical Association 264:1824â1831. Woods JS, Polissar L, Severson RK, Heuser LS, Kulander BG. 1987. Soft tissue sarcoma and non- Hodgkinâs lymphoma in relation to phenoxy herbicide and chlorinated phenol exposure in western Washington. Journal of the National Cancer Institute 78:899â910.
516 VETERANS AND AGENT ORANGE: UPDATE 2006 Wrensch M, Minn Y, Chew T, Bondy M, Berger MS. 2002. Epidemiology of primary brain tumors: Current concepts and review of the literature. Neuro-Oncology 4(4):278â299. Wu CH, Chen HL, Su HJ, Lee CC, Shen KT, Ho WL, Ho SY, Ho YS, Wang YJ. 2004. The topical application of 2,3,7,8-tetrachlorodibenzo-p-dioxin lacks skin tumor-promoting potency but induces hepatic injury and tumor necrosis factor-alpha expression in ICR male mice. Food and Chemical Toxicology 42(8):1217â1225. Wyde ME, Braen AP, Hejtmancik M, Johnson JD, Toft JD, Blake JC, Cooper SD, Mahler J, Vallant M, Bucher JR, Walker NJ. 2004. Oral and dermal exposure to 2,3,7,8-tetrachlorodibenzo-p-dioxin (TCDD) induces cutaneous papillomas and squamous cell carcinomas in female hemizygous Tg.AC transgenic mice. Toxicological Sciences 82(1):34â45. Yamamoto S, Konishi Y, Matsuda T, Murai T, Shibata MA, Matsui-Yuasa I, Otani S, Kuroda K, Endo G, Fukushima S. 1995. Cancer incidence by an organic arsenic compound, dimethylarsinic acid (cacodylic acid), in F344/DuCrj rats after pretreatment with ï¬ve carginogens. Cancer Research 55(6):1271â1276. Yamanaka K, Ohtsubo K, Hasegawa A, Hayashi H, Ohji H, Kanisawa M, Okada S. 1996. Exposure to dimethylarsinic acid, a main metabolite of inorganic arsenics, strongly promotes tumorigenesis initiated by 4-nitroquinoline 1-oxide in the lungs of mice. Carcinogenesis 17(4):767â770. Yoshizawa K, Walker NJ, Jokinen MP, Brix AE, Sells DM, Marsh T, Wyde ME, Orzech D, Haseman JK, Nyska A. 2005a. Gingival carcinogenicity in female Harlan Sprague-Dawley rats follow- ing two-year oral treatment with 2,3,7,8-tetrachlorodibenzo-p-dioxin and dioxin-like com- pounds. Toxicological Sciences 83(1):64â77 [erratum appears in Toxicological Sciences 2005; 83(2):405â406]. Yoshizawa K, Marsh T, Foley JF, Cai B, Peddada S, Walker NJ, Nyska A. 2005b. Mechanisms of exocrine pancreatic toxicity induced by oral treatment with 2,3,7,8-tetrachlorodibenzo-p-dioxin in female Harlan Sprague-Dawley rats. Toxicological Sciences 85(1):594â606. Zack JA, Suskind RR. 1980. The mortality experience of workers exposed to tetrachlorodibenzo- dioxin in a trichlorophenol process accident. Journal of Occupational Medicine 22:11â14. Zahm SH, Fraumeni JF Jr. 1997. The epidemiology of soft tissue sarcoma. Seminars in Oncology 24(5):504â514. Zahm SH, Weisenburger DD, Babbitt PA, Saal RC, Vaught JB, Cantor KP, Blair A. 1990. A caseâ control study of non-Hodgkinâs lymphoma and the herbicide 2,4-dichlorophenoxyacetic acid (2,4-D) in eastern Nebraska. Epidemiology 1:349â356. Zahm SH, Blair A, Weisenburger DD. 1992. Sex differences in the risk of multiple myeloma associ- ated with agriculture (2). British Journal of Industrial Medicine 49:815â816. Zahm SH, Weisenburger DD, Saal RC, Vaught JB, Babbitt PA, Blair A. 1993. The role of agricultural pesticide use in the development of non-Hodgkinâs lymphoma in women. Archives of Environ- mental Health 48:353â358. Zhong Y, Rafnsson V. 1996. Cancer incidence among Icelandic pesticide users. International Journal of Epidemiology 25(6):1117â1124. Zober A, Messerer P, Huber P. 1990. Thirty-four-year mortality follow-up of BASF employees exposed to 2,3,7,8-TCDD after the 1953 accident. International Archives of Occupational and Environmental Health 62:139â157.