Introduction
Influenza is a virus that attacks the upper respiratory tract, resulting in an infection that typically lasts one week and is characterized by fever, headache, cough, sore throat, and general malaise. There are three main types of influenza virus: A, B, and C. Type-A strains are the most virulent and have periodically caused global human pandemics. Subtypes of influenza A viruses are categorized according to two specific proteins, Hemagglutinin and Neuraminidase, that appear on the surface of the virus. There are 16 known variants of Hemagglutinin, H1–H16, and 9 known variants of Neuraminidase, N1–N9 (USDA, 2006). Strains of the influenza virus are also categorized according to pathogenicity, the ability to cause disease, as low pathogenic (LP) and highly pathogenic (HP). Approximately 200,000 cases of seasonal influenza are reported in the United States each year, and an estimated 36,000 of these cases end in death (Homeland Security Council [HSC], 2005).
Avian influenza is an infectious disease primarily found in wild, migratory birds and poultry, caused by influenza A strains of the virus. The disease occurs worldwide, and outbreaks have been reported among poultry flocks for years. Strains that cause a high proportion of deaths in affected flocks are referred to as highly pathogenic avian influenza (HPAI). Influenza viruses (e.g., avian, swine, human) are typically species-specific. However, the World Health Organization (WHO) has confirmed instances of human infection with an avian influenza virus on 10 occasions since 1959 (WHO, 2006). In 1997, 18 cases and 6 deaths of humans infected with the H5N1 strain of avian influenza were documented in Hong Kong (WHO, 2006).
Interspecies transmission is possible, because influenza strains can mutate rapidly and acquire genes from other influenza strains. New influenza subtypes emerge in two ways: (1) through re-assortment (antigenic shift) where an animal is simultaneously infected with two different strains and the genetic material of the viruses mix to produce a new hybrid strain; or (2) through adaptive mutation (antigenic drift), wherein an influenza virus undergoes gradual mutation, eventually resulting in the capacity to infect a different animal species (WHO, 2005).
According to WHO, human pandemics result when a new influenza A virus emerges with the capacity to efficiently infect and easily spread between humans. Since 2003, H5N1 has been reported among wild birds in nine southeast Asian countries (Korea, Viet Nam, Japan, Thailand, Cambodia, the Lao People’s Democratic Republic, Indonesia, China, and Malaysia). In 2005, H5N1 was documented among wild birds in Russia, Kazakhstan, Croatia, Romania, and in domestic birds in Ukraine (WHO, 2006). From 2003 to 2006, WHO confirmed 263 cases of human infection and 158 deaths in 10 countries (see Figure 1). The National Institute of Allergy and Infectious Diseases (NIAID) has stated that migratory birds, the poultry trade, and human travel could likely introduce H5N1 into the United States (NIAD, 2007). NIAD notes that when an influenza virus is transmitted across species, it typically results in a “dead end” infection that is not spread from human to human (NIAD, 2007). However, there is increased concern that H5N1 will eventually mutate, allowing for human-to-human transmission.
|
Country |
2003 |
2004 |
2005 |
2006 |
Total |
|||||
|
|
Cases |
Deaths |
Cases |
Deaths |
Cases |
Deaths |
Cases |
Deaths |
Cases |
Deaths |
|
Azerbaijan |
0 |
0 |
0 |
0 |
0 |
0 |
8 |
5 |
8 |
5 |
|
Cambodia |
0 |
0 |
0 |
0 |
4 |
4 |
2 |
2 |
6 |
6 |
|
China |
1 |
1 |
0 |
0 |
8 |
5 |
13 |
8 |
22 |
14 |
|
Djibouti |
0 |
0 |
0 |
0 |
0 |
0 |
1 |
0 |
1 |
0 |
|
Egypt |
0 |
0 |
0 |
0 |
0 |
0 |
18 |
10 |
18 |
10 |
|
Indonesia |
0 |
0 |
0 |
0 |
20 |
13 |
55 |
45 |
75 |
58 |
|
Iraq |
0 |
0 |
0 |
0 |
0 |
0 |
3 |
2 |
3 |
2 |
|
Thailand |
0 |
0 |
17 |
12 |
5 |
2 |
3 |
3 |
25 |
17 |
|
Turkey |
0 |
0 |
0 |
0 |
0 |
0 |
12 |
4 |
12 |
4 |
|
Viet Nam |
3 |
3 |
29 |
20 |
61 |
19 |
0 |
0 |
93 |
42 |
|
Total |
4 |
4 |
46 |
32 |
98 |
43 |
115 |
79 |
263 |
158 |
Figure 1. Confirmed Cases of Human Avian Influenza Infections and Deaths from 2003 to 2006.
NOTE: The total number of cases includes number of deaths. For current figures refer to http://www.pandemicflu.gov/index.html (WHO, 2007).
On October 23, 2006, the Disasters Roundtable of the National Academies convened a workshop on Citizen Engagement in Emergency Planning for a Flu Pandemic to explore the roles and needs of the citizenry in pandemic influenza preparedness planning. The workshop was organized in cooperation with the Board on Population Health and Public Health Practice of the Institute of Medicine (IOM).
Session I:
Why Worry About Pandemic Flu?
Panelists: Eric Toner, Center for Biosecurity, University of Pittsburgh Medical Center; Bruce Gellin, National Vaccine Program Office, Department of Health and Human Services (HHS); Joshua Sharfstein, Department of Health, Baltimore
National Plans for Confronting a Pandemic Flu
Pandemic influenza predictions are based on the three pandemics of the twentieth century: the 1918-1919 Spanish Flu (responsible for 40 million deaths), the 1957-1958 Asian Flu (responsible for more than 2 million deaths), and the 1968-1969 Hong Kong Flu (responsible for approximately 1 million deaths). Panelist Eric Toner, senior associate with the Center for Biosecurity of the University of Pittsburgh Medical Center, noted that the Department of Health and Human Services (HHS), in preparation for a potential influenza pandemic, has established two planning scenarios, based on the 1918 (extreme) and 1957 (mild) influenza pandemics (see Figure 2). Toner reported that in both scenarios, one-third of the U.S. population will become ill and 50 percent of those infected will require medical attention. As many as 1.5 million people will require intensive care. The distinction between the two scenarios is the level of demand for care that hospitals across the nation will experience during an influenza pandemic. Toner stated that there are less than 100,000 intensive care unit (ICU) beds available in U.S. hospitals and noted that ICU beds and ventilators are almost always in use under normal operating conditions. Diverting ICU
beds and ventilators for influenza patients would adversely impact other patients that would normally need these services. “In the severe scenario, we need twice as many hospital beds as exist, five times as many ICU beds, and twice as many ventilators than are currently available just to treat flu patients,1” remarked Toner. Additional resources will be needed to treat patients with other health needs.
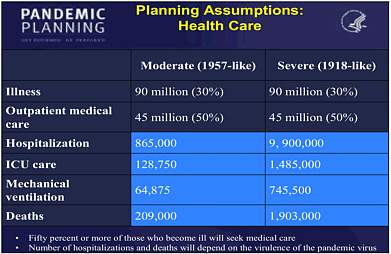
Figure 2. Health and Human Services Influenza Pandemic Scenarios (HHS, 2005).
Bruce Gellin, director of HHS’ National Vaccine Program Office, detailed steps that the federal government has taken to plan for an influenza pandemic in the United States. The Homeland Security Council (HSC) released the National Strategy for Pandemic Influenza in November 2005, followed by its Implementation Plan in May 2006. HHS also released its Pandemic Influenza Plan in 2005. Gellin reported that Michael O. Leavitt, Secretary of Health and Human Services, has also convened summits hosted by governors in states across the country to stress the importance of a pandemic influenza threat and encourage states and localities to engage in preparedness activities.
Gellin addressed HHS efforts to strengthen pandemic response in the areas of vaccine and antivirals.2 He noted that because influenza viruses are constantly mutating, we cannot reliably predict the strain that will infect people. Consequently, vaccines cannot be stockpiled in advance. Toner added that because vaccines are manufactured using slow and antiquated production technology, it will take between 6 to 12 months to produce enough vaccine for most of the U.S. population, once a pandemic begins. HHS’ Pandemic Influenza Plan calls for vaccine production to begin once human-to-human transmission of avian influenza is reported in any nation. Gellin reported that the Strategic National Stockpile is working to amass a supply of the antiviral oseltamivir phosphate, marketed as Tamiflu®, an oral Neuraminidase
inhibitor for influenza A. He stated that HHS has purchased 26 million treatment courses3 of Tamiflu® and should have 30 million by early 2007. According to Gellin, HHS plans to stockpile sufficient quantities of Tamiflu® to treat at least 25 percent of the people that are expected to become ill. This would require the preparation and stockpiling of 75 million antiviral courses and an additional 6 million to help contain the disease, according to Gellin. To aid states and localities in their preparations, HHS allows states to purchase Tamiflu® at federally negotiated rates with an additional 25 percent discount. Gellin cautioned that antivirals should not be viewed as a panacea, noting that influenza viruses can develop resistance to Tamiflu®. He also reported that the necessary dosage and duration of antiviral treatment varies between influenza strains. Moreover, the timing of prophylaxis is critical, Gellin added; the antiviral must be administered within 48 hours of infection to be effective.
Local Expectations and Readiness for Pandemic Flu
Pandemic response also includes disease containment efforts such as possible quarantines, travel restrictions, social distancing (e.g., school and workplace closures, canceling mass assemblies), and infection control (e.g., use of gloves, masks, hand washing) to mitigate the spread of the disease. As Commissioner of Health for Baltimore, Maryland, Joshua Sharfstein stated that he is concerned with maintaining Baltimore’s critical infrastructure systems during a pandemic. To address this concern, his department is engaged in “continuity of operations” planning to determine which positions are essential to the city’s operations. Sharfstein commented that in a pandemic it may be necessary to shift staff members into different positions as part of the emergency response. “The key public health approach that we’re trying to take is to use the regular functions of the public health department to develop capacity,” stated Sharfstein.
Sharfstein indicated that he is also working to engage the 651,154 citizens of Baltimore through various public health initiatives. He stated that Baltimore participates in the Center for Disease Control and Prevention (CDC) City Readiness Initiative (CRI), a program that aims to increase the capacity of cities to deliver medication and medical supplies quickly during a large-scale public health emergency. According to Sharfstein, Baltimore has also launched campaigns like B’More Prepared to encourage citizen involvement in emergency preparedness and has used recent Hepatitis B and Varicella (chickenpox) vaccination requirements for 5th and 9th grade school children as an opportunity to educate parents about the importance of vaccinations.
In the discussion that followed the panel, workshop participants noted that some private enterprises have initiated antiviral stockpiles independently of the Strategic National Stockpile and these enterprises are determining their own priority guidelines as to who should receive treatment. Antivirals such as Tamiflu® are available for purchase online, and these purchases are not tracked by local and state governments. Consequently, local officials may not have an accurate account of the amount of antivirals stockpiled in their jurisdictions. Sharfstein commented that this issue has been raised in Baltimore, and some have suggested establishing an influenza vaccine buy-back program that would entail registering corporate purchases and offering a potential refund for unused vaccine. Such an effort could potentially assist cities and states in coordinating their vaccination programs.
Session II:
Government and Health Professionals Cannot Go It Alone in a Large-Scale Health Crisis
Panelists: Judith W. Leavitt, School of Medicine, University of Wisconsin-Madison; Jason Corburn, Columbia University; Susan Chu, Flu Wiki
Public Resistance or Cooperation? A Tale of Smallpox in Two Cities
Judith Leavitt, professor of medical history, history of science, and women’s studies at the University of Wisconsin-Madison, presented “two historical extremes” of public reaction to efforts undertaken by public health departments in response to pandemic outbreaks. Focusing on Milwaukee, Wisconsin’s experience with Smallpox in 1894, and the Spanish Flu in 1918, and Smallpox in New York City in 1947, Leavitt demonstrated the importance of public engagement in pandemic response.
According to Leavitt, Milwaukee citizens rioted for a month in response to the health department’s policies of vaccination and social distancing in response to the 1894 outbreak of Smallpox. Smallpox was reported throughout the city, but was primarily concentrated on the Southside, which was heavily populated by German and Polish immigrants. Health Commissioner Walter Kempster implemented a response plan of vaccinations and isolation of the infected either at home or in the Milwaukee Isolation Hospital, which lacked running water and sewer connections. Leavitt reported that native-born white, middle-class Milwaukeeans were allowed to remain in their homes, while immigrants were forcibly removed and sent to the isolation hospital. Consequently, Smallpox spread widely and went unreported on the Southside of Milwaukee. The immigrant community opposed the forcible removal of their children from their homes and eventually rioted. Leavitt characterized the public health department’s response as one of discriminatory strong-arm tactics that did not involve community input or rely on consensus-building.
The Milwaukee public health department’s pandemic response to the 1918 Spanish Flu outbreak was met with considerably less public resistance due to Health Commissioner George Ruhland’s active involvement of community actors. Leavitt noted that Ruhland encouraged physicians to report cases of influenza, appointed an advisory committee of physicians and businessmen, and engaged the city’s volunteer and religious organizations. Ruhland also implemented an extensive public education campaign, publishing health department articles in newspapers and distributing pamphlets and placards throughout Milwaukee. In contrast to Kempster, Ruhland reached immigrants by printing health advisories in three languages. According to Leavitt, Ruhland’s use of the media and community organizations encouraged Milwaukeeans to comply with social distancing measures (e.g., closing schools, canceling public meetings) to quell the disease.
New York City’s experience with Smallpox in 1947 mirrored the Milwaukee public health department’s handling of the 1918 Spanish Flu. Leavitt stated that Smallpox had not been reported in New York City since the 1920s. As a result, in 1947, New York’s population was unfamiliar with the disease and few had been vaccinated. Health Commissioner Israel Weinstein launched a vaccination campaign that resulted in the voluntary vaccination of 6.5 million New Yorkers. Leavitt attributed the success—4,000 cases and 900 deaths were predicted, but only 12 cases and 2 deaths were reported—to Weinstein’s public education efforts. Reviewing Milwaukee’s experience with pandemic diseases in 1894 and 1918 and New York’s Smallpox outbreak in 1947, Leavitt concluded that “coercion, historically, has not been as effective as education.”
Street Science: Why Public Health Professionals Need the Public
Jason Corburn, assistant professor in the urban planning program at Columbia University, concurred with Leavitt on the importance of community involvement in public health response. Referring to his research on the environmental health of the Greenpoint-Williamsburg neighborhood of Brooklyn, New York, Corburn championed the “co-production” of expertise through active engagement with community members by researchers and public health officials. Corburn detailed the evolution of the Environmental Protection Agency’s (EPA) assessment of the neighborhood in response to environmental health concerns. He reported that as much as 50 percent of Brooklyn’s waste is transported through the neighborhood daily. In 1999, in response to concerns about air pollution, lead poisoning, and high incidences of asthma, EPA included Greenpoint-Williamsburg as a case study in its Cumulative Exposure Project (CEP), which was initially launched in 1994. According to Corburn, EPA’s efforts did not fully consider the demographic composition of the neighborhood or its cultural practices. For example, EPA’s dietary assessment of the community was based on a National Health and Nutrition Examination Survey (NHNES) of a “standard” northeastern urban diet. Yet Corburn characterized Greenpoint-Williamsburg as a low-income community primarily comprised of Polish and Slavic immigrants, Latinos, and Hasidic Jews. Corburn remarked that some Greenpoint-Williamsburg residents were eating subsistence diets of East River fish due to poverty and cultural tradition; as such, EPA’s dietary assessment would have missed actual practice without community input. According to Corburn, community members struggled to get EPA to acknowledge the value that their knowledge could add to EPA’s assessment. “Engaging community members and their knowledge about how they move through the world, and what they know about their disease management and exposure risks in their community can contribute to better science and policy,” remarked Corbun.
Pandemic Risk Communication in the Internet Age
The proliferation of the Internet and its increased use by the public worldwide has created new tools to engage and inform the public about a potential influenza pandemic. Retired physician Susan Chu remarked that the nonprofit Flu Wiki Forum, which she moderates from the United Kingdom, serves as an online clearinghouse for pandemic influenza preparedness and education. Chu characterized the Forum as an “experiment in community public health planning with the objective of harnessing the information and intellectual resources of the vast network of individuals working online to solve the complex interrelated problems that an influenza pandemic would present.” She stated that the Forum is highly interactive, rather than just a one-way communication channel, and noted that it involves both information dissemination and information gathering from numerous external sources. Individuals are encouraged to submit content for inclusion on the Web site, according to Chu. She also noted that the activities of the Forum are driven largely by its users. In response to requests from its users, the Forum designated the week of October 3, 2005, as Pandemic Flu Awareness Week and launched the campaign again in October 2006.
According to Chu, Web sites such as Flu Wiki empower the public to become actively involved in pandemic preparedness. She noted that individuals who access the site can track reported cases of H5N1 infection globally, follow changes in international healthcare policies, share concerns, and educate their communities about pandemic influenza preparedness.
In the discussions that followed the panel, workshop participants stressed the importance of engaging the public before the advent of an influenza pandemic. Participants commented that honest, clear and open communication by public health officials to the public is essential in maintaining the public’s trust.
Session III:
When Does Citizen Engagement Work Best? Lessons Learned from Research and Experience
Panelists: Elaine Chatigny, Public Health Agency of Canada (PHAC); Kathleen R. Stratton, Board on Population Health and Public Health Practice, IOM; Gail Bingham, RESOLVE, Inc.
Citizen Consultations in Setting National Public Health Priorities
The Public Health Agency of Canada (PHAC) was established in September 2004 as a stand-alone agency in response to the Severe Acute Respiratory Syndrome (SARS) outbreak reported in Canada from February 23, 2003 to July 2, 2003. The PHAC is charged with helming Canada’s federal efforts to prevent disease and promote and protect national and international public health. According to Elaine Chatigny, director general of the Communications Directorate, PHAC views public engagement as a pivotal component of its planning efforts. Engaging the public ensures that proposed public health policies reflect the societal values of Canada’s diverse population. Public engagement also lends PHAC’s actions legitimacy. Chatigny remarked that establishing and maintaining credibility and public trust is essential. She noted that public health decisions are made within a shifting political context that changes with each election cycle.
Chatigny and her colleagues at PHAC chose to build upon the experience gleaned from Health Canada’s previous efforts to encourage public engagement, which resulted in the Policy Toolkit for Public Involvement in Decision Making. In addition, following 22 roundtables and consultations, 10 Health Goals for Canada were issued. According to Chatingy, PHAC aims to leverage the lessons learned from Health Canada’s efforts in its plans for pandemic influenza preparedness. To that end, PHAC has developed a strategy for public engagement that centers on educating the public about antivirals for prophylaxis. Chatigny reported that PHAC would convene a series of 10 dialogues and a rollout event from November 2006 through January 2007, to engage citizens, targeted groups, national stakeholders, and First Nations communities. She stated that the operationalization and enactment of public engagement can be a particularly protracted process for PHAC. Each strategy and plan must be approved at the federal, provincial, and territorial levels. Chatigny commented that public engagement at the local level in Canada is particularly challenging because hundreds of languages are spoken in some of the provinces, while the Canadian federal government only recognizes English and French. Consequently, pandemic influenza information should be prepared in numerous languages in order to reach the entire community. Chatingy concluded that public engagement is an immense but necessary endeavor to ensure that the concerns and needs of all citizens are incorporated into pandemic influenza preparedness policies and activities.
Involving Citizens and Stakeholders in Select Vaccine Policy Decisions
Throughout the workshop’s proceedings, several participants expressed concerns about the ethical issues involved in deciding which groups will and will not be vaccinated in the advent of an influenza pandemic. Kathleen Stratton, program officer at the Institute of Medicine (IOM), recounted the misgivings of parent groups about their exclusion from the decision-making process when they learned that thimerosal, a mercury-containing preservative, had been used in vaccines once commonly administered to school children. While studies by IOM have concluded that there is no direct link between mercury and autism in children, Stratton reported that parent groups were incensed that they were not involved in the policymaking process.
In an effort to involve the public in vaccine policy decisions that have been and will be made in relation to pandemic influenza, IOM has established the Vaccine Policy Analysis Collaborative (VPACE) as a
conduit for citizen engagement with national stakeholders (e.g., American Academy of Pediatrics, American Medical Association, Advisory Committee on Immunization Practices, CDC, HHS, state and territorial health officials). Stratton noted that the public cannot be involved in every decision. For example, the public is not involved in the annual decision-making process to determine which of the three most prominent influenza virus strains should be incorporated into the seasonal vaccine. However, Stratton believes that there are many other vaccine decisions that do not involve such technical issues and could benefit from citizen input.
To help determine how to effectively involve the public in vaccine policy decisions, VPACE launched the Public Engagement Pilot Project on Pandemic Influenza (PEPPPI). PEPPPI is a consortium of organizations, including the IOM, HHS, CDC, the Keystone Center, the University of Georgia, the Atlanta Journal-Constitution, Georgia Department of Health, and the states of Massachusetts, Nebraska, and Oregon. The consortium is tasked with determining how to prioritize groups in the early stages of a pandemic when vaccine will be in short supply. According to Stratton, PEPPPI has included new stakeholders, for example critics of federal vaccine policy that have previously not had a voice in the policy process. PEPPPI’s stakeholders met twice in the summer of 2005 in Washington, D.C., to develop a framework for citizen engagement on vaccine distribution strategies and priorities. Citizens were then given an opportunity to express their concerns in Atlanta, Georgia, and provide feedback in Boston, Massachusetts; Omaha, Nebraska; and Portland, Oregon. Stratton reported that the response to PEPPPI’s efforts was generally supportive and served to highlight concerns that had not been considered.
Citizen Voices on Pandemic Flu Choices, a final summary of PEPPPI’s activities and findings, was submitted to HHS in December 2005. The central ethical issues that were raised included concerns about the powers of the state versus the liberties of citizens and the ability of the public to trust statements made by the government, as well as the fair distribution of vaccines and antivirals. Stratton noted that trust and fairness are intertwined, as public trust of government authority may be undermined by perceptions that vaccination priorities are unfair. PEPPPI concluded that it would be most efficient to initially distribute influenza vaccines to groups at the highest risk, as well as children, and then subsequent distribution could be based on a lottery system and a system of “first-come, first-served.” Stratton noted that decisions that prioritize groups over others must ultimately be made by government officials. Public engagement would ensure that these decisions are perceived as fair and just.
Importance of Collaborative Knowledge
Chatigny and Stratton demonstrated the difficulties that public engagement poses for policy decision-making. Namely, heterogeneous communities are comprised of groups and organizations with differing concerns and objectives. As such, a top-down approach to public policy is often met with resistance by community members. As president of RESOLVE, a nonprofit public policy, consensus-building organization, Gail Bingham has more than 30 years of experience facilitating and mediating dialogues between different stakeholders on a variety of issues. Relying on experience documented in Resolving Environmental Disputes: A Decade of Experience, Bingham stated that in 78 percent of the cases that she has examined, consensus was reached in instances where decision makers engaged the public in advance of policy enactment. Echoing Corburn, Bingham stressed the importance of collaborative knowledge. She stated that collaboration and consensus-building efforts can be initiated in advance of the potential kinds of conflicts highlighted by Leavitt. “At the community level, the public knows more than policymakers about community networks,” remarked Bingham.
In the discussions that followed the panel, participants stressed the importance of building, and in some cases restoring, public trust in public health policies and government agencies. Panelists acknowledged that this is an important and ongoing endeavor.
Session IV:
Projections on a Potential Influenza Pandemic
Panelists: Gabor Kelen, Johns Hopkins University; Randy Rowel, Morgan State University; Darlene Sparks Washington, American Red Cross; Susan Messina, Citizen-Activist
In the final workshop session, Disasters Roundtable Steering Committee member Monica Schoch-Spana moderated a collaborative discussion with four panelists that were asked to contemplate the likely conditions that communities across the United States would experience under severe pandemic influenza conditions. Schoch-Spana presented a scenario in which a virulent influenza strain has an attack rate of 25 percent, all members of her hypothetical community are vulnerable to the disease, vaccines are unavailable, epidemiologists have predicted an 8-week crisis, and hospitals face increased demand for their services at the same time that fewer staff can work due to personal illness, having to care for sick family members, or concern about bringing home contagion. The scenario highlighted a key dilemma for communities during a severe pandemic—how to care for large numbers of ill people when hospitals are overwhelmed. This situation presented a concrete problem with which to explore the social value of greater public involvement in pandemic preparedness in advance of an actual event.
Gabor Kelen, director of research and program director of the Emergency Medicine Residency at Johns Hopkins University, suggested that hospital emergency rooms will not be involved in treatment in order to avoid the risk of infecting other patients seeking emergency care. Instead, he recommended setting up staging grounds outside of a hospital setting to determine which patients need to be hospitalized. According to Kelen, as much as 70 percent of the patients currently hospitalized can be released for a 72-hour period without compromising their care.4 As such, there would be space in hospitals to treat influenza patients. How long that space could be made available (in the face of the reduced staffing brought on by the influenza outbreak and over the full crisis period) and how well a community could care for those people discharged early from the hospital were not explicated in Kelen's remarks. He noted that the majority of influenza patients will not and should not be treated in hospitals. Kelen also highlighted the importance of using an all-hazards approach to pandemic influenza preparedness, as the U.S. public healthcare system faces similar concerns when addressing the threat of potential acts of bioterrorism.
Randy Rowel, assistant professor in the School of Public Health and Policy at Morgan State University, noted that following the federal, state, and local response in the Gulf Coast to Hurricane Katrina in 2005, a high level of distrust exists in many communities. Consequently, many individuals may ignore advisories and go to the emergency rooms for treatment. If refused and redirected to staging areas, they may perceive these policies as discriminatory.
Citizen activist Susan Messina remarked that in such a scenario her first concern would be for the health of her children and members of her community. Messina remarked that as a citizen she would want to take an active role in pandemic influenza response. If hospital beds were unavailable, she would offer the bed in her finished basement.
Darlene Sparks Washington, director of preparedness and team lead for Influenza Pandemic Planning at the American Red Cross, stated that in this scenario the 775 local chapters spread across the United States would be charged with responding to the event. The American Red Cross is currently involved in preevent planning activities that include polling communities to ascertain the public’s expectations of the American Red Cross during an outbreak, reported Washington.
Schoch-Spana also asked the panelists to consider the value of engaging the public in advance of an influenza pandemic. Kelen stated that engaging the public in advance would serve to stem concerns about discrimination and dissatisfaction with public health response by establishing realistic expectations. Washington stressed the importance of building a culture of preparedness. According to Washington, pandemic influenza preparedness among the public needs to be included in the general preparedness activities that households undertake for hazards like house fires. Messina concurred that public engagement is important and that the public needs to be involved in policy decisions. However, she noted that many members of the public may not yet be educated enough about the issues raised by pandemic influenza and that some input may not be useful and hence need to be balanced with the perspective of experts. Messina also cautioned against involving the public as a shield to excuse unpopular policy decisions.
In the discussions that followed the panel, workshop participants expressed concerns about issues of handling mass deaths and disposing of human remains during an influenza pandemic. Messina stated that her colleagues in national hospice and palliative care are engaged in emergency planning to address the grief counseling needs that may result from mass casualties of the disease. Participants noted that many communities have specific funereal rituals and rites that may include taboos against mass burials. Workshop participants also noted that there are a limited number of medical examiners operating in the United States.
Closing Remarks
Disasters Roundtable Steering Committee chair William Hooke remarked that pandemic influenza presents many of the challenges presented by natural hazards and disasters. He also stated that all disasters exacerbate preexisting social inequities. Hooke advised participants not to consider pandemic influenza preparations in a vacuum. He noted that several speakers and participants had previously stated that the public will continue to need treatment for other ailments during a pandemic. Hooke suggested that it is also likely that the United States will be faced with other disasters while responding to pandemic influenza.
Bibliography
Bingham, Gail. 1986. Resolving Environmental Disputes: A Decade of Experience. Conservation Foundation. Washington, D.C.
Center for Disease Control and Prevention (CDC). 2006. Center for Disease Control and Prevention FluSurge 2.0. Available online at http://www.cdc.gov/flu/tools/flusurge/. Accessed April 10, 2007.
Health and Human Services (HHS). 2005. HHS Pandemic Influenza Preparedness Plan. Available online at http://www.hhs.gov/pandemicflu/plan/pdf/HHSPandemicInfluenzaPlan.pdf. Accessed April 10, 2007.
HHS. 2005b. Citizen Voices on Pandemic Flu Choices: A Report of the Public Engagement Pilot Project on Pandemic Influenza. Available online at http://www.hhs.gov/nvpo/PEPPPI/PEPPPICompleteFinalReport.pdf. Accessed February 12, 2007.
Homeland Security Council (HSC). 2005. National Strategy for Pandemic Influenza. Available online at http://www.whitehouse.gov/homeland/pandemic-influenza.html. Accessed February 9, 2007.
HSC. 2006. National Strategy for Pandemic Influenza: Implementation Plan. Available online at http://www.whitehouse.gov/homeland/nspi_implementation.pdf. Accessed February 9, 2007.
National Institute of Allergy and Infectious Diseases (NIAID). 2007. Questions and Answers: H5N1 Avian Flu Vaccine Trials. Available online at http://www3.niaid.nih.gov/news/newsreleases/2005/H5N1QandA.htm. Accessed February 9, 2007.
National Research Council (NRC). 2001. Immunization Safety Review: Thimerosal-Containing Vaccines and Neurodevelopmental Disorders. Available online at http://books.nap.edu/catalog/10208.html. Accessed February 9, 2007.
NRC. 2004. Immunization Safety Review: Influenza Vaccines and Neurological Complications. The National Academies Press, Washington, DC. Available online at http://books.nap.edu/catalog/10822.html. Accessed February 9, 2007.
U.S. Department of Agriculture (USDA). 2006. Avian Influenza: Protecting the United States. USDA Preparations and Response. Available online at http://www.usda.gov/documents/AvianFluBrochure.pdf. Accessed February 9, 2007.
World Health Organization (WHO). 2005. WHO Outbreak Communication: WHO Handbook for Journalists 2005. Available online at http://www.who.int/csr/don/Handbook_influenza_pandemic_dec05.pdf. Accessed February 9, 2007.
WHO. 2006. Avian influenza ("bird flu")-Fact sheet February 2006. Available online at http://www.who.int/mediacentre/factsheets/avian_influenza/en/. Accessed February 9, 2007.
WHO. 2007. Cumulative Number of Confirmed Human Cases of Avian Influenza A/(H5N1) Reported to WHO. Available online at http://www.who.int/csr/disease/avian_influenza/country/cases_table_2007_04_02/en/index.html. Accessed April 5, 2007.











