3
Sensitization and Chronic Beryllium Disease
It is well established that beryllium causes sensitization (BeS) and chronic beryllium disease (CBD). This chapter provides an overview of the literature relevant to assessing the risks of those conditions associated with occupational exposure to beryllium. We first review the epidemiologic literature on BeS and CBD. The current clinical description of CBD is presented next with diagnosis, testing, and management approaches. That is followed by a discussion of what is known about the pathogenesis and mode of action of CBD and about genetic factors that confer susceptibility to it. Finally, we consider the development of animal models to study CBD.
EPIDEMIOLOGY AND CLINICAL DISEASE
Exposure to beryllium can cause two distinct types of pulmonary disease, a pneumonitis referred to as acute beryllium disease and a chronic granulomatous disease called CBD. Acute beryllium disease, first reported in the 1930s, was observed in beryllium workers and was characterized by the onset of respiratory symptoms usually over several weeks. Chest radiographic descriptions were those of initial diffuse haziness, followed by lung infiltrates and nodules. Most patients recovered over several months with appropriate treatment and removal from exposure, but recurrences occurred on repeat exposure (Van Ordstrand et al. 1945). Several fatalities were reported, and pathologic changes in those cases showed edema, infiltration with mononuclear inflammatory cells, alveolar cell proliferation or desquamation, and the absence of granulomas (Freiman and Hardy 1970). The incidence of acute beryllium disease decreased after respiratory exposures to beryllium were controlled in the plant (Van Ordstrand et al. 1945). The mechanism of a dose-related toxic pneumonitis has been postulated, although immune or hypersensitivity responses are also possible. Acute beryllium disease has rarely been reported over the last several decades. CBD, however, despite substantial reductions in beryllium respiratory exposures, continues to occur in exposed workers. The pathogenesis of CBD involves a lymphocyte-mediated immune response (delayed hypersensitivity) to beryllium that leads to noncaseating granulomatous lesions. CBD affects primarily the lungs, although granulomas can also occur in other organs, such as skin, liver, and spleen. BeS precedes the development of CBD and is detected on the basis of the in vitro response of lymphocytes to beryllium in the beryllium lymphocyte proliferation test (BeLPT). Historically, CBD was diagnosed when it presented with progressive respiratory symptoms, such systemic complaints as fatigue, and radiographic and lung-function abnormalities. Screening healthy workers with the BeLPT has enabled the detection of BeS in asymptomatic exposed workers and the
earlier diagnosis of CBD and has changed the clinical spectrum of CBD. This section reviews the recent epidemiologic literature on BeS and CBD and their clinical presentation, diagnosis, and management.
Epidemiologic Literature
CBD was first reported in the United States in the early 1940s by Van Ordstrand et al. (1943), Kress and Crispell (1944), and Hardy and Tabershaw (1946). Cases were observed in industrial plants that were refining and manufacturing beryllium metal and beryllium alloys and in plants manufacturing fluorescent light bulbs. By 1948, the known cases totaled more than 400, and the basic clinical features of the disease were understood. It was established that the risk of disease among beryllium workers rose with the intensity of airborne exposure and that risk varied with the physicochemical properties of the beryllium exposure (Machle et al. 1948; see Chapter 2 for more information). From the late 1940s into the 1960s, there were also outbreaks of CBD caused by air pollution around beryllium refineries in Ohio and Pennsylvania and outbreaks in family members of beryllium-factory workers, presumably caused by contaminated clothing (Hardy 1980). Although there was a clear relationship between the air concentration of beryllium and the risk of CBD in areas close to the factories, the disease rates outside the plant were higher than expected (Eisenbud et al. 1949; Lieben and Metzner 1959).
The risk of CBD in workers exposed during the 1940s and 1950s has been estimated to be 1-10% (Eisenbud and Lisson 1983), although there is considerable uncertainty because most of the studies in that era did not use well-defined cohorts or have adequate followup.
Sterner and Eisenbud (1951) first proposed an immunologic mechanism of CBD in 1951. Their evidence was largely circumstantial, but their inference was correct. They based their hypothesis on several pieces of evidence: the highly variable incidence in different groups of workers, the surprisingly high risk in neighborhoods whose exposures appeared to be low, the sometimes rapid onset of disease after exposure, and the failure to observe an association between the amount of beryllium in lung autopsy specimens and the extent of lung damage.
From the 1940s through the 1960s, the Atomic Energy Commission (AEC) was the primary user of beryllium in the U.S. economy. In 1949, AEC’s occupational hygienists recommended an air standard of 2 μg/m3 as an 8-h time-weighted average and a peak standard of 25 μg/m3 (Eisenbud 1982). Before the widespread application of the BeLPT, it appeared that strict adherence to those standards might adequately protect workers from CBD. However, it is now clear that CBD occurs in factories that have beryllium aerosol concentrations consistently below 2 μg/m3 (Kreiss et al. 2007).
The development of the BeLPT changed case-finding tools used in CBD epidemiology studies from chest radiographs and spirometry to the identification of BeS with a blood test, followed up with biopsy as well as clinical examination. This change created a fundamental non-comparability in the clinical and epidemiology literature pre- and post-BeLPT development, which (along with reduced exposures) has been associated with identification of clinically milder cases of CBD compared with the older clinical and epidemiologic literature. There appears to be a consensus in the field that a case series of CBD identified in exposed workers by BeLPT and confirmed with biopsy provides more specificity in diagnosis compared with tools such as chest radiographs and spirometry. Unfortunately, there are no studies that formally document this impression. For this reason, in its review of the epidemiologic evidence, the committee decided to focus primarily on the epidemiologic studies of CBD that include the use of the BeLPT. The committee took into account the results of the older epidemiology studies along with clinical studies and case series describing clinically diagnosed CBD in the pre-BeLPT era to inform other sections of this chapter (see sections on “Presentation, Diagnosis and Testing of CBD” and “Natural History and Management”).
In a recent review, Kreiss et al. (2007) summarized 12 studies (with overlapping populations) in which CBD prevalence was assessed cross-sectionally and ranged from 0.1% to nearly 8% (Table 3-1). Those data reflect exposures to workers decades after the recognition of the disease and indicate that many workers are still being exposed to concentrations of beryllium that put them at risk. The high
TABLE 3-1 Summary of Recent Epidemiologic Studies of Chronic Beryllium Disease
|
|
|
Prevalence |
Exposure-Response Relationship?a |
|
|
|
Reference |
Study Type |
BeS |
CBD |
Comments |
|
|
Mining and extraction |
|||||
|
Deubner et al. 2001a |
Cross-sectional |
4.0% |
1.3% |
No |
|
|
Beryllium metal processing and alloy production |
|||||
|
Kreiss et al. 1997 |
Cross-sectional |
9.4% |
4.6% |
No |
|
|
Newman et al. 2001 |
Longitudinal |
9.4% |
5.5% |
No |
|
|
Kelleher et al. 2001 |
Case-control |
N/A |
N/A |
Yes |
|
|
Rosenman et al. 2005 |
Cross-sectional |
14.6% |
7.6% |
No |
|
|
Beryllia ceramics |
|||||
|
Kreiss et al. 1993a |
Cross-sectional |
1.6% |
1.8% |
No |
|
|
Kreiss et al. 1996 |
Cross-sectional |
5.9% |
4.4% |
Yes |
|
|
Henneberger et al. 2001 |
Cross-sectional |
9.9% |
5.3% |
Yes |
|
|
Cummings et al. 2007 |
Longitudinal |
N/A |
N/A |
Yes |
|
|
Beryllium-copper alloy processing and distribution |
|||||
|
Schuler et al. 2005 |
Cross-sectional |
6.5% |
3.9% |
No |
|
|
Stanton et al. 2006 |
Cross-sectional |
1.1% |
1.1% |
No |
Workers in three distribution centers |
|
Nuclear-weapons industry |
|||||
|
Rocky Flats nuclear weapons facility |
|||||
|
Kreiss et al. 1989 |
Cross-sectional |
11.8% |
7.8% |
No |
Production and research and development machinists only |
|
Kreiss et al. 1993b |
Cross-sectional |
1.9% |
1.7% |
No |
Stratified random sample with probable beryllium exposure |
|
Stange et al. 1996b |
Longitudinal |
2.4% |
0.7% |
No |
Current and former workers |
|
Stange et al. 2001 |
Longitudinal |
4.5% |
1.6% |
No |
Current and former workers (including workers in Stange et al. 1996b) |
|
Sackett et al. 2004 |
Cross-sectional |
0.8% |
0.1% |
No |
Decontamination and decommissioning workers only |
|
Viet et al. 2000 |
Case-control |
N/A |
N/A |
Yes |
Current and former workers |
|
Hanford Nuclear Reservation, Oak Ridge Reservation, and Savannah River site |
|||||
|
Welch et al. 2004 |
Cross-sectional |
1.4% |
0.1% |
No |
Construction-trade workers |
|
aNo = no evidence of exposure-response was provided by the paper; Yes = evidence of increased prevalence or risk with increasing exposure. SOURCE: Adapted from Kreiss et al. 2007. Adapted table reprinted with permission; copyright 2007, Annual Review of Public Health. |
|||||
prevalences of BeS and CBD in the studies by Kreiss et al. (1997, 1998), Henneberger et al. (2001), Newman et al. (2001), and Rosenman et al. (2005) are at least partly explained by higher ambient airborne concentrations of beryllium in these facilities. The newer epidemiologic studies have benefited from the ability to detect BeS with the BeLPT, and their results indicate that in general the prevalence of BeS is higher than that of clinically confirmed CBD, although the difference varies widely. The differing ratios of BeS to CBD among studies are probably strongly affected by the extent of followup of former workers, the time elapsed since initial exposures, and the physical form and intensity of exposure.
It is very difficult to estimate the “background” risk of CBD. Although there is natural background exposure to beryllium in soils, air, food, and water, the committee knows of no studies that have attempted to identify cases from “natural” sources. There have been case reports of CBD in people
with incidental or inconsequential exposure to beryllium, but such reports are of limited use in estimating background risk. It is also likely that many cases of CBD are mistakenly diagnosed as sarcoidosis, and without a known source of exposure, and lacking a BeLPT, there is no way to distinguish these CBD cases from sarcoid.
The recent literature on BeS and CBD in different sectors of the beryllium industry is briefly summarized below. The division into sectors may be useful because it roughly corresponds to the physicochemical forms of beryllium to which workers are exposed. There are a number of methodologic issues and differences between the epidemiologic studies, including study designs, number of study participants, how exposures were quantified, diversity of physicochemical form of beryllium, genetic susceptibility to CBD, and the healthy worker effect. In its second report, the committee will provide an expanded discussion of these issues and how they limit the interpretability of the epidemiologic studies.
Beryllium Mining and Extraction
There is some information on the risk of CBD in workers in beryllium mining and extraction. In the United States, beryllium ore is mined in a single facility in Utah; substantial mineral resources also exist in China, Russia, and elsewhere. The U.S. facility has been studied twice: by Rom et al. (1983), who reported on worker health surveys in 1979 and 1982, and more recently by Deubner et al. (2001a). The Rom et al. study used an early version of the BeLPT, and its results are difficult to interpret. The Deubner et al. study appears to provide a more reliable assessment of the risk in mining and extraction.
Bertrandite ore (containing an average of 0.23% beryllium) is mined at the Utah facility, and an extraction mill at the same site produces beryllium hydroxide, which is shipped elsewhere to be made into beryllium oxide ceramics and beryllium metal. The same facility extracts beryllium from beryl ore (3.6-5.0% beryllium) that is mined abroad. A medical screening in 1996 included the BeLPT. Seventy-five of 87 (86%) workers in the facility were tested, and 12 refused to be tested. The single worker found to have CBD had substantial exposure to beryllium in another facility. Three beryllium-sensitized workers had worked only in the facility under study. It is not possible from the data given to conclude that there is no risk in mining and extraction. The paper does not permit an analysis that separates mine from mill workers, so it is not possible to estimate the prevalence or risk of sensitization separately for the two activities—mining, in which exposure is exclusively to highly dilute ores, and extraction, in which beryllium salts are present. It appears that there may be a lower risk of sensitization in mining and extraction than in other phases of production, but confidence in this finding is limited by the small numbers, limited participation, and inability to separate exposures in mining and in extraction.
Beryllium Metal Processing and Alloy Production
The beryllium-metal processing and -alloy production facilities have provided important data on risks of BeS and CBD and the relationships between the two (Kreiss et al. 1997; Newman et al. 2001; Rosenman et al. 2005). The relevant studies involved cross-sectional screening of a working population, and each found both BeS and CBD (Table 3-1).
The study by Newman et al. (2001) is valuable because the same population was studied in a later case-control analysis (Kelleher et al. 2001) to investigate exposure-risk relationships that go beyond the prevalence data presented in most studies. Those studies were conducted in a beryllium-metal machining facility that experienced an index CBD case in 1995. The plant opened in 1969, and extensive environmental measurements were taken throughout the plant’s history. Beginning in 1995, BeLPT screening was conducted on all workers, with retesting 2 years later. All 235 eligible workers were tested in 1995-1997, and 15 (6.4%) were beryllium-sensitized. Of the 15 sensitized workers, 12 completed clinical evaluations, and nine were found to have CBD. The onset of sensitization was sometimes very short—3 months or less in four of the 15.
To investigate exposure-response relationships, 20 workers with BeS (n = 7) or CBD (n = 13) were compared with 206 at-risk workers who had neither condition in a case-control analysis (Kelleher et al. 2001). Exposure assessments for cases and controls were conducted by using personal exposure data that had been gathered with a size-selective impactor in the breathing zone. Cumulative and average lifetime exposures were calculated for particles in two sizes: less than 6 μm and less than 1 μm. There was evidence that case subjects were more highly exposed than controls in terms of both total exposure and the two size ranges. For example, cumulative exposure to particles smaller than 1 μm was associated with the prevalence of BeS or CBD when prevalence was compared across three exposure groups; when compared with those who had low cumulative exposure (less than 0.09 μg/m3), the odds ratio (OR) for those with medium exposure (0.09-1.87 μg/m3) was 1.85, and for high exposure (over 1.87 μg/m3) the OR was 2.46. Confidence intervals were rather wide because of the small numbers of cases, but a clear trend was evident.
Beryllium Oxide Ceramics
Beryllium oxide ceramics production workers in two facilities have been studied: one that produced ceramics until 1975 (Kreiss et al. 1993a), and a second that still produces them (Kreiss et al. 1996; Henneberger et al. 2001; Cummings et al. 2007).
Those studies are among the best sources of evidence of the risk of BeS associated with low exposure. The plant that still produces ceramics has monitored workers closely for the onset of sensitization (and for CBD among those who become sensitized) over about 10 years. The facility has also engaged in increasingly elaborate control procedures in an attempt to eliminate the risk of sensitization. BeS screening with the BeLPT was first conducted in 1992, when eight of 136 screened workers (5.9%) were found to be sensitized. Six of the eight had CBD as evidenced by granulomas in biopsied lung tissue. The highest risk was in machining, which had higher average mass concentrations of beryllium in air than other jobs. At the initial 1992 screening, the prevalence of BeS was higher in machinists (14.3%) than in all other workers (1.2%). After the survey, the company undertook engineering controls to reduce airborne exposures over the period 1993-1996. Employment increased in 1996, and a second BeLPT screening was conducted in 1998. A detailed assessment of airborne exposures was also carried out at the same time. Overall, 15 of 151 (9.9%) screened workers had BeS in 1998. Those results are best understood by looking separately at two groups: long-term workers who had been employed before the first screening in 1992 and short-term workers who were hired after it. The short-term workers had experienced only recent exposure to beryllium, and their exposure-risk experience was less likely to have been biased by loss to followup than that of the long-term workers. But the prevalence of BeS was similar in the two groups: 10.4% in 77 long-term workers and 9.5% in 74 short-term workers. The investigators observed that short-term workers with “low” mean exposure (0.05-0.28 μg/m3) had a lower prevalence of sensitization (5%) than those with higher exposure (0.29-4.4 μg/m3) (14%). That fairly large difference in prevalence was based on very small numbers: 39 workers with low exposure and 35 with high exposure.
Concluding that the recently installed ventilation controls had not reduced the prevalence of sensitization, the company embarked on a second, much more elaborate control strategy, including careful attention to elimination of skin contact, stricter control of airborne exposures, and reduction of the resuspension of settled particles. From 2000 on, as new workers were hired, they received baseline sensitization tests so that the incidence of sensitization could be quantified prospectively. Cummings et al. (2007) assessed the effectiveness of the post-2000 exposure-control program by comparing the incidence of sensitization in workers hired from 2000 to 2004 with the incidence in those hired from 1993 to 1998. From 2000 to 2004, 126 workers were hired, and most contributed a baseline result and at least one postbaseline test result. The results were compared with those of the 69 workers tested in the 1998 survey. The two groups of workers were of similar mean age (37 and 35 years, respectively), and both had mean tenures of 16 months. The incidence of BeS among those hired in 2000-2004 was 0.7 case per
1,000 person-months, and the incidence in the group hired earlier was 5.6 cases per 1,000 person-months. Again, although that is a large difference, it was based on very small numbers: one case in 1,480 person-months vs six cases in 1,081 person-months, respectively.
It appears from the Cummings et al. paper that an elaborate control program, including scrupulous attention to skin contact, inhalation exposure, and dust control throughout the facility, was effective at reducing (but not eliminating) the risk of sensitization. The comparison of the first (1992) and second (1998) surveys suggested that engineering control of airborne exposure alone was not sufficient to eliminate the risk of sensitization (Henneberger et al. 2001).
Copper-Beryllium Alloy Processing and Distribution
Case reports document the occurrence of CBD in workers exposed to 2% beryllium-copper alloy (Balkissoon and Newman 1999), but the case subjects had experienced substantial exposure through grinding, heating, and cutting operations. Two studies of beryllium-copper alloy processing and distribution facilities have provided data on risks of BeS and CBD and the relationships between them (Schuler et al. 2005; Stanton et al. 2006). A study of beryllium-copper distribution-center workers provided some information on the risk to those with more modest exposure (Stanton et al. 2006). Some processing of beryllium-copper strip and rod took place at these facilities, including sawing, heat treating, welding, and slitting; but dust- and fume-generating activities should have been lower than in beryllium manufacturing facilities. Exposure-monitoring data confirmed the generally low airborne exposures: the median concentration of 393 full-shift personal samples was 0.03 μg/m3, 97% of the values were less than 0.2 μg/m3, and no samples exceeded 2 μg/m3. Of the 100 current workers invited to participate in a cross-sectional health survey, 88 agreed; one was found to be sensitized to beryllium and, after clinical examination, found to have CBD. That worker had spent 22 years in a production-support job as a shipper and receiver.
That case and others (Kreiss et al. 1993a,b, 1996) indicate that CBD can occur in workers exposed at well below an air concentration of 2 μg/m3.
Nuclear-Weapons Production and Cleanup
A series of studies have investigated BeS and CBD in workers in nuclear-weapons production facilities, including the cleanup of those plants (Kreiss et al. 1989, 1993b; Stange et al. 1996b, 2001; Viet et al. 2000; Sackett et al. 2004; Welch et al. 2004). The U.S. Department of Energy conducts health surveillance of workers potentially exposed to beryllium at its facilities, and the surveillance data form the basis of this set of studies. Results of surveillance at the Rocky Flats nuclear weapons facility near Denver have been presented (Kreiss et al. 1989, 1993b; Stange et al. 1996b, 2001, 2004; Viet et al. 2000; Sackett et al. 2004). Welch et al. (2004) studied construction workers at three other facilities: in Hanford, Washington; Oak Ridge, Tennessee; and Savannah River, South Carolina. Those studies were all cross-sectional and based on health surveys of various worker cohorts. They share many of the limitations of other beryllium epidemiologic studies, including refusals to participate, loss to followup, and inadequate exposure data or inadequate ability to link exposure data to specific study participants. Despite their limitations, they provide useful data on risks in a fairly large and diverse group of workers in the nuclear industry.
BeS and CBD were reported in each of the studies in workers who handled beryllium metal and alloy and in those who performed various tasks involved in cleaning up former weapons facilities where beryllium was handled. Cross-sectional prevalences of BeS were 0.8-11.8% and of CBD were 0.1-7.8%.
Viet et al. (2000) used the surveillance and exposure monitoring data from Rocky Flats to investigate exposure-risk relationships. They conducted a case-control sampling of the surveyed cohort, choosing as case subjects all those who had been identified with BeS or clinically diagnosed CBD.
Controls were chosen by 1:1 sampling and matching to cases on age, sex, race, and smoking. There were 74 cases of BeS without evidence of CBD and 50 cases of CBD. For each case and control, a lifetime beryllium-exposure history was constructed by using job-history information combined with estimates of exposure in each job based on fixed-area samples. Although the number of air samples was very large, the samples were not taken in the workers’ breathing zones but rather at fixed locations throughout the workplace. One would expect a certain amount of exposure misclassification from this monitoring system. The resulting error may have reduced the strength of the association between exposure and risk.
Cumulative and average exposure estimates were fit to case-control status in logistic-regression models. There was strong evidence of increasing risk of CBD with increasing beryllium exposure, particularly as measured by cumulative exposure. The evidence of an association with BeS was not as strong. Although the cross-sectional nature of the study limited risk prediction in important ways, the authors estimated that there was a 0.5% risk of CBD at the current standard of 2 μg/m3.
Longitudinal Studies of Progression of BeS
Only a few studies have investigated the progression of BeS to CBD. They have been small and varied in design, exposure setting, length of followup, and diagnostic evaluation. In one of the earliest clinical studies to use the BeLPT, Rom et al. (1983) reported that 13 of 82 beryllium mining and milling workers had BeS. None of sensitized workers developed CBD over the following 3 years, and some showed possible reversal of sensitization. However, the initial diagnosis of BeS was based on only one positive result of an early version of the BeLPT, so it is difficult to interpret (see discussion of the BeLPT later in this chapter).
More recently surveillance studies of current and former workers at Rocky Flats have found that about 3.3% (172 of 5,173) of workers were sensitized to beryllium on initial screening; about 40% (74 of 172) of the sensitized workers were diagnosed with CBD (Stange et al. 1996b, 2001). Repeat evaluation of 2,891 workers 3 years later identified an additional 63 (2.2%) workers with BeS, seven of whom had CBD (Stange et al. 2001). Thus, 4.54% of screened workers had BeS. Machinists were at highest risk for CBD (11.4%). Additional long-term followup is needed to determine what proportion of the remaining workers with BeS will progress to CBD.
Newman et al. (2005) followed a cohort of 55 patients with BeS at 2-year intervals for a mean followup of 4.8 years to determine progression to CBD. BeS was defined on the basis of a positive BeLPT and no evidence of pathologic changes (granulomas or mononuclear cell infiltrates) on transbronchial biopsy. CBD was defined on the basis of evidence of BeS and pathologic changes. Of the 55 patients with BeS, 17 (31%) developed CBD within an average followup period of 3.8 years; machinists had the highest likelihood of progression to CBD. The authors estimated that BeS progresses to CBD at a rate of 6-8% per year after diagnosis. For a 6-year followup period, the progression rate was estimated at 3.2-9.2% per year. The likelihood of progression from BeS to CBD was associated with loss of lung function and the presence of a higher percentage of lymphocytes in BAL fluid than sensitized patients on baseline evaluation.
The longitudinal studies are consistent with the larger cross-sectional literature in showing that in most settings workers with BeS are at high risk for CBD but that the risk is variable.
Risk Posed by Low-Level Environmental Exposure
CBD has occurred in people thought to have trivial, unrecognized, or brief exposure to beryllium. Examples include secretaries, security guards, end-product inspectors, and workers hired years after beryllium operations ceased (Kreiss et al. 1993a,b, 1996; Eisenbud and Lisson 1983). Family members of beryllium workers have developed CBD thought to have occurred from contact with contaminated clothing (Lieben and Metzner 1959; Eisenbud and Lisson 1983; Newman and Kreiss 1992). Although in
some of those cases it is not possible to rule out some occupational exposure, the overall picture is that people can develop CBD from beryllium exposures that would generally be considered incidental.
Cases of CBD have also been reported in residents of communities that surround beryllium manufacturing facilities. Although they are considered “community cases,” the exposures occurred before controls were instituted in the 1970s to reduce beryllium emissions into the air of surrounding communities, and some exposures were probably comparable with current occupational exposures or the “incidental” exposures noted above. It can also be difficult to rule out occupational exposure in some of those cases (Lieben and Metzner 1959; Dattoli et al. 1964; Lieben and Williams 1969; Newman and Kreiss 1992). On the basis of estimates of community exposure around one such plant, the U.S. Environmental Protection Agency set a community standard of 0.01 μg/m3 in air averaged over a 30-day period (40 CFR Sec. 61.32).
Risk Posed by Skin Exposure
It has been presumed that the respiratory tract is the key route of exposure to beryllium, and research and prevention have focused almost exclusively on airborne exposure. However, BeS and CBD have persisted despite substantial reductions in respiratory exposures, and attention has recently focused on the role of skin exposure in BeS and CBD (Day et al 2007; Kreiss et al. 2007). As discussed above, several lines of evidence suggest that skin exposure may contribute to BeS and CBD and that reducing such exposure may reduce the risk of sensitization.
Decades ago, workers developed contact dermatitis from skin exposure to soluble beryllium salts, which was confirmed with beryllium skin patch testing (Curtis 1951). Patch testing was developed as a diagnostic test for CBD but was discontinued because of concerns that such testing itself could cause BeS or worsen CBD (Curtis 1959).
The question of whether less soluble particulate forms of beryllium (metal, oxides, and alloys) that are the primary media of work exposure can penetrate human skin has been raised (see Chapter 2). An increased risk of CBD has been reported in workers who have skin lesions, which presumably increase uptake of beryllium (Johnson et al. 2001; Schuler et al. 2005). As noted earlier, particulate forms of beryllium, like such other particles as titanium dioxide and polystyrene latex spheres, may be able to penetrate normal human skin (Tan et al. 1996; Tinkle et al. 2003). BeS has also been produced in mice by skin exposure to beryllium oxide particles (Tinkle et al. 2003).
The epidemiologic literature demonstrating weak relationships between air exposure and response and new cases of BeS and CBD despite reductions in air concentrations (to below the current standard of 2 μg/m3) have been used to support a role of skin exposure in BeS (Henneberger et al. 2001; Cummings et al. 2007). Cummings et al. (2007) described the effects of a comprehensive prevention program in one beryllium oxide ceramics plant targeted at both respiratory and dermal protection (details of which were provided earlier in this chapter). The program included extensive use of personal protective equipment (PPE) and administrative changes geared to reducing beryllium in the air, on all work surfaces, and on skin. After implementation, the rate of BeS was substantially reduced.
Most epidemiologic studies have not attempted to measure skin exposure for estimating exposure-response relationships, so the effectiveness of PPE is unclear. A recent exposure assessment at a copper-beryllium alloy facility documented beryllium contamination of work surfaces and gloves and exposure of skin on the neck and face and under gloves (Day et al. 2007). Air beryllium concentrations correlated strongly with the degree of contamination of work surfaces, and concentrations on work surfaces, gloves, and skin also correlated.
In addition to the beryllium literature, there is evidence that skin exposure to other occupational and environmental sensitizers, such as isocyanates, may lead to systemic sensitization that can progress to lung disease if there is also respiratory exposure (Bello et al. 2006; Day et al. 2007). The potential importance of skin exposure is also supported by the role of skin in the development of other systemic, as well as dermatologic, immune diseases.
For immune-mediated diseases, such as CBD and asthma, skin as a potential route of exposure and sensitization has several important implications for pathogenesis, risk factors, diagnosis, and prevention. Some forms of exposure may make beryllium more bioavailable to the skin (soluble metals and liquids) and others more bioavailable to the lung (respirable particles and vapors); the hazard associated with beryllium may depend on its route of entry. If skin exposure can lead to sensitization, regulatory standards based on air concentrations, even if very low, may not prevent sensitization or eliminate the risk of disease.
Clinical Literature
There is a large body of clinical information on BeS and CBD. This section first reviews the literature on diagnosis of and testing for BeS; then describes the clinical presentation and diagnosis of and testing for CBD; discusses the natural history of CBD and its management; and describes the use of the BeLPT in surveillance of beryllium workers.
Diagnosis of and Testing for BeS
As described above, beryllium causes chronic granulomatous disease in the lung associated with the presence of lymphocytes that specifically respond to the presence of beryllium in the lung. Prior to the advent of the BeLPT, the diagnosis of CBD was based on clinical presentation and clinical diagnosis. In the 1970s and 1980s, researchers identified that lymphocytes from blood or the lung of individuals with CBD proliferated in the presence of beryllium in vitro. This response was refined and developed into what we know now as the BeLPT. The use of the BeLPT allows the identification of BeS in the absence of CBD.
BeS is not a disease in its own right and has no symptoms, but is important because it identifies a subgroup of exposed workers who are at risk of developing CBD. The diagnosis of BeS requires confirmation of an abnormal BeLPT with a second abnormal test. The BeLPT is now used as part of the diagnosis of CBD, for screening of asymptomatic workers or former workers for both BeS and CBD, and for surveillance to identify patterns of exposure to beryllium in the workplace.
The test involves an in vitro challenge of either BAL or peripheral blood lymphocytes with beryllium salts. In beryllium-responsive people, the challenge induces an oligoclonal proliferation of sensitized lymphocytes measured on the basis of uptake of tritiated thymidine. Somewhat different protocols and criteria have been used, but BeLPT testing is becoming more standardized in the few laboratories in the United States that do it.
The test is performed by placing cells in primary culture in the presence and absence of beryllium sulfate, typically across a 3-log range of salt concentrations. Cell proliferation is measured according to the incorporation of tritiated thymidine into the dividing cells (typically after 3, 5, and 7 days in culture). Results are expressed as a "stimulation index": the ratio of the radioactivity counts per minute in cells stimulated by beryllium salts divided by the counts per minute in unstimulated cells. Each laboratory sets its own normal range for the test on the basis of data from normal nonexposed control subjects. A test is typically considered positive if two stimulation indexes are increased. The BeLPT, like other cell-culture assays, is associated with intratest, intertest, and interlaboratory variability; therefore, a positive, or abnormal, BeLPT result is generally confirmed with a second analysis, either by testing of the same blood sample in a different laboratory or by testing of a later sample before the subject is considered sensitized.
The BeLPT of peripheral blood or BAL cells is used as part of the diagnostic workup of patients who have interstitial lung disease and possible beryllium exposure when CBD is in the differential diagnosis. A positive BeLPT result differentiates CBD from other lung diseases (such as sarcoidosis, chronic obstructive pulmonary disease, and hypersensitivity pneumonitis). Almost all patients with CBD have a positive BeLPT result when peripheral blood or BAL cells are used, whereas patients with
sarcoidosis or other interstitial lung diseases do not. Thus, the BeLPT is very specific in this setting. Although some workers with an abnormal BeLPT do not have CBD, a confirmed abnormal blood BeLPT result is considered a strong predictor of CBD among workers with known exposure to beryllium. Several studies have reported that CBD is diagnosed in 50% or more of the screened workers with two abnormal blood BeLPT results (Newman et al. 2001). The conversion rate from BeS to CBD in one cohort of workers followed for a mean of 4.8 years was between 6% and 8% per year (Newman et al. 2005). More followup time is needed to see what the final lifetime risk is for this group. Nevertheless, the presence of BeS as measured with the blood BeLPT indicates a high probability of developing CBD in workers in beryllium production facilities.
Interlaboratory variation in the blood BeLPT test has been described (Deubner et al. 2001b). Stange at al. (2004) presented data on a comparison of four laboratories in the United States that perform the BeLPT. Over 7,300 split samples were sent to the four laboratories, and each sample was tested at two. When one laboratory recorded an abnormal BeLPT, the likelihood that a second laboratory would find the sample abnormal was 26.2%, 39.7%, and 32.4% in the laboratories that tested more than 200 samples. (The fourth laboratory, which tested only 123 samples, had a higher agreement, 61.8%, but this rate was based on a relatively small number of samples.) When the comparison was restricted to people known to be sensitized (those who had two abnormal BeLPT results), a repeat sample in another laboratory had a likelihood of 80.4-91.9% of being found abnormal. In part because of potential interlaboratory variation, surveillance programs typically require two separate positive BeLPT results to determine BeS—a requirement that decreases the sensitivity of the test but increases the specificity.
New approaches based on flow cytometric analysis of CD4+ T cells that respond to beryllium (Farris et al. 2000; Milovanova et al. 2004; Milovanova 2007) and the detection of beryllium-specific cytokine-secreting T cells with enzyme-linked immunosorbant spot assay (Pott et al. 2005) are under development.
Presentation and Diagnosis of and Testing for CBD
Clinically, CBD can be difficult to distinguish from sarcoidosis and other interstitial lung diseases, especially if, as is common, the history of beryllium exposure is not obtained. Since its pathogenesis involves a beryllium-specific, cell-mediated immune response, CBD cannot occur without sensitization. Thus, the clinical definition of CBD has evolved with the development of the BeLPT. Symptoms of CBD include dyspnea, cough, fatigue, anorexia, weight loss, chest pain, and arthralgia, or cases may be asymptomatic. Physical examination findings can be normal or include bibasilar crackles and, less commonly, lymphadenopathy, skin lesions, hepatosplenomegaly, and clubbing. Signs of pulmonary hypertension can be found in severe long-standing disease (Stoeckle et al. 1969). The clinical course of the disease can be variable. Systemic manifestations of CBD are less common than those of sarcoidosis and include increases in serum gamma globulin and erythrocyte sedimentation rate, erythrocytosis, hyperuricemia, and reversible hypercalcemia and hypercalcinuria. Renal calculi have also been reported (Stoeckle et al. 1969).
The current criteria for diagnosing CBD include all the following (Pappas and Newman 1993; Maier et al. 1999; Saltini et al. 2001; Amicosante et al. 2005):
-
History of or evidence of beryllium exposure.
-
Evidence of an immune response to beryllium, that is, positive responses in blood or BAL BeLPT tests or positive skin patch test (seldom performed in clinical practice). Those responses can also be considered evidence of exposure if exposure history cannot be ascertained.
-
Nonnecrotizing granulomata on lung biopsy.
A clinical evaluation for CBD generally includes spirometry, measurement of lung volume and diffusion capacity, chest radiography, and, if clinically indicated, a high-resolution computed tomography
(HRCT) scan of the chest. For a person with a high likelihood of CBD or with abnormalities in the tests that suggest the presence of interstitial lung disease, the current clinical recommendation is to undertake BAL and transbronchial biopsy. In a clinical setting, the decision of whether to perform lavage and biopsy is made case by case. When a lung biopsy has not been done or is not possible, a presumptive diagnosis of CBD can be based on the presence of an immune response and radiographic findings (chest radiograph or HRCT scan) of diffuse small opacities.
CBD presents as a clinical spectrum in sensitized people that ranges from the presence of granulomas on lung biopsy without respiratory symptoms, radiographic abnormalities, or decrements in pulmonary-function or exercise tests to end-stage lung disease with severe dyspnea, severe pulmonary function changes, radiographic changes, arterial oxygen desaturation, and cor pulmonale. Between those extremes, there may be mild to severe changes in one or more of the tests. Many of the symptoms, radiographic changes, and pulmonary-function test findings in CBD are nonspecific and can be due to other conditions, so other explanations of such findings need to be considered. Conversely, pulmonary-function test results that are considered normal on the basis of predicted values in a patient with CBD may not be truly normal for that person and could reflect a substantial decline in lung volumes or carbon monoxide diffusing capacity (DLCO) in the person but still fall above the lower limit for “normal.” Such changes may be apparent only if serial pulmonary-function test results are available with a true baseline for the patient. Thus, it can be difficult to determine whether mild disease is truly “subclinical” or constitutes a clinically significant effect; although the term subclinical CBD has been used (Kriebel et al. 1988; Newman 1996), it has not been clearly defined, and other terms have also been used, such as early CBD (Rossman 1996) and surveillance CBD (Pappas and Newman 1993).
Histopathology
The largest study of the histopathology of CBD examined 124 cases of CBD from the Beryllium Case Registry (Freiman and Hardy 1970). Patterns of diffuse noncaseating granulomas with various degrees of mononuclear-cell interstitial infiltrates were described in the lung-biopsy specimens from those patients. Giant cells, asteroid bodies within giant cells, and calcific inclusions were also noted. About half the cases had accompanying moderate to advanced interstitial fibrosis. The authors reported that patients with slight or absent cellular infiltration and with well-formed granulomas appeared to have a better prognosis. More recent studies have confirmed the histopathologic pattern of noncaseating granulomas, mononuclear-cell interstitial infiltrates, and interstitial fibrosis in lung specimens from transbronchial biopsies of patients with CBD (Newman et al.1989). The pathologic findings are not specific for CBD and may occur in other lung diseases, including sarcoidosis. In addition to noncaseating granulomas in the lung, extrapulmonary granulomas have been described in skin, liver, lymph nodes, and muscle in patients with CBD (Stoeckle et al. 1969).
Bronchoscopy, BAL, and Biopsy
Bronchoscopy with BAL and transbronchial biopsy is generally recommended for diagnosing CBD but is not without risk. Transbronchial lung biopsies are performed to determine the presence of nonnecrotizing granulomas and interstitial infiltration; fibrosis and coalescence into nodules may also be seen. The granulomas are histologically indistinguishable from those due to other granulomatous disorders, such as sarcoidosis and a granulomatous response to infection (without caseation). Biopsy samples should be stained to exclude infection.
BAL is usually obtained by washing the middle lobe or lingula, and the fluid is sent for analysis of total and differential cell counts (to identify the presence of lymphocytosis), for culturing (to exclude infection as a cause of granulomatous changes), and to a specialized laboratory for a BeLPT on the BAL
cells (rapid processing of the fluid with a specialized technique is needed) (Rossman et al. 1988; Newman et al. 1989).
BAL typically shows lymphocytosis with varied percentages of lymphocytes (Rossman et al. 1988; Newman et al. 1989). The percentage of BAL lymphocytes may correlate with physiologic and radiographic disease severity. In some cases of subjects with BeS and biopsy-confirmed CBD, BAL may show normal percentages of lymphocytes (Newman et al. 2005). Because of the association between cigarette smoking and increases in alveolar macrophages, cigarette smoking may obscure BAL lymphocytosis (Newman et al. 2005).
Pulmonary-Function Testing
Results of pulmonary-function testing in patients with CBD are variable; they include showing restrictive, obstructive, mixed-pattern, or isolated impairment in lung diffusion capacity. Milder cases can have minimal or no physiologic abnormalities. Sensitive physiologic measures have been reported to be increased ratio of dead space to tidal volume (VD/VT) on exercising (Pappas and Newman 1993) and an increased alveolar-arterial oxygen (A-a) gradient on exercising (Daniloff et al. 1997), both reflecting impaired gas exchange. Increased A-a gradient on exercising has also shown good correlation with HRCT-scan indications of CBD (Daniloff et al. 1997). In more advanced cases, decreased DLCO, restriction, airflow obstruction, and arterial hypoxemia may be present alone or in combination.
An early report from Andrews et al. (1969) of 41 patients studied for an average of 23 years after initial beryllium exposure showed a restrictive defect (20%), reduced diffusing capacity (normal lung volumes and air-flow rates but reduced DLCO) (36%), and an obstructive defect (39%); 5% were normal. The authors reported that the obstructive pattern occurred in both smokers and nonsmokers and was associated with peribronchial granulomas.
In a report of 12 patients with new diagnoses of CBD, pulmonary-function abnormalities were mild (Newman et al. 1989). One patient had restriction, and two former smokers had mild obstruction. Of the 12 patients, 11 had diffusing capacity that was normal when corrected for lung volume. Gas exchange on maximal exercise was normal in six of the nine patients tested.
A study of 21 patients with CBD (defined as beryllium exposure, consistent biopsy results, and abnormal BeLPT results) identified through screening at their plants showed that 14 had normal pulmonary-function test results and 10 had normal physiologic measures on maximal exercise (Pappas and Newman 1993). Four had airflow obstruction, two had mixed obstruction and restriction, and one had abnormal DLCO per liter of alveolar volume (VA). The 11 with abnormal exercise physiologic results showed either increased VD/VT on exercise, abnormal gas exchange, or both. The group of 15 CBD patients referred because of symptoms or radiographic abnormalities showed similar results, although fewer of them had normal pulmonary-function test results and exercise physiologic results, their DLCO/VA was lower, and they showed evidence of reduced exercise tolerance in addition to abnormalities in VD/VT and gas exchange.
Chest Radiography
Radiographic findings in CBD were first described as diffuse densities and hilar adenopathy (Weber et al. 1965; Stoeckle et al. 1969; Hasan and Kazemi 1974). Contraction of lobes with hyperinflation of adjacent lobes, calcifications in parenchymal densities and hilar nodes, pneumothorax, cysts, bullae, and linear scars were also described in advanced cases.
More recent studies of CBD that used the International Labour Organization classification system have described mainly diffuse, symmetric small opacities that were rounded, irregular, and of mixed patterns (Aronchick et al. 1987; Newman et al. 1994). Hilar adenopathy (always associated with interstitial abnormalities) was observed in 35-40% of people who had abnormal chest radiographs. Less
common plain-film findings included coalescence of small opacities, linear scars, emphysematous bullae, retraction, distortion of lung architecture, and pleural thickening. Of those with biopsy-proven noncaseating granulomas, 46% had normal chest radiographs (Newman et al. 1994). The radiographic features of CBD are nonspecific and occur in other lung diseases, including sarcoidosis.
HRCT scanning of the chest is more sensitive than plain chest radiography in identifying abnormalities in patients with CBD. However, HRCT scans showing no signs consistent with CBD have been reported in 25% of patients with biopsy-proven noncaseating granulomas (Newman et al. 1994). The most common HRCT findings in CBD are nodules and septal thickening. Other findings include ground-glass attenuation, pleural irregularity, bronchial-wall thickening, and hilar and mediastinal adenopathy. Honeycombing has been reported in clinically severe cases (Newman et al. 1994). The HRCT appearances of CBD are nonspecific and occur in other lung diseases, including sarcoidosis. In a study by Daniloff et al. (1997), there was a significant correlation between HRCT changes and impaired gas exchange on exercise.
Additional and New Tests
Newer tests and approaches for improving the diagnosis of CBD and elucidating disease progression are being developed. For example, measuring neopterin concentrations in peripheral blood has been proposed as a diagnostic adjunct that may correlate with CBD severity or progression (Harris et al. 1997; Maier et al. 2003a). A beryllium-stimulated neopterin test has been reported to have a sensitivity of 80-90% and a specificity of 87-100% (Maier et al. 2003a). Another proposed biomarker is beryllium-specific cytokine-secreting T cells (secreting IFγ and IL-2) that are detected in peripheral blood in an enzyme-linked immunosorbent spot assay (Pott et al. 2005). Such T-cell cytokine assays may help to differentiate BeS from CBD (Tinkle et al. 1997). Another proposed approach has been the use of induced sputum as an alternative to BAL fluid (Fireman et al. 1999), but the data are insufficient to evaluate this.
Natural History and Management
As noted earlier, CBD has a clinical spectrum that can range from evidence of BeS and granulomas of the lung without clinically significant symptoms or deficits in lung function to end-stage lung disease. Little has been published on the progression of CBD from the asymptomatic form to functionally significant lung disease. The risk factors and time course have not been clearly delineated. Progression from asymptomatic to symptomatic disease in people now under surveillance has been suggested to be generally slow. Possible risk factors for progression that have not been systematically assessed include smoking status, race, sex, genetic factors, exposure duration, magnitude and type of beryllium exposure (including particle size and solubility), concurrent exposures, and life stresses, such as pregnancy and lactation, combat, and surgery (Newman 1996). Newman (1996) emphasized the need for prospective studies of the natural history of BeS and subclinical CBD. In his clinical experience, the sequence of events for those with progression has been from BeS to gradual emergence of chronic inflammation in the lung, pathologic alterations, measurable physiologic derangement (demonstrated by pulmonary function and gas exchange), more severe lung disease, and finally death in some cases. Rossman (1996) also reported that in his clinical practice an annual assessment of CBD patients is performed that includes a history, physical examination, chest radiography, pulmonary-function tests, and exercise-physiology tests to detect early lung damage. In a cohort of 55 patients with BeS followed for 1-11 years, 31% developed CBD in an average of 3.8 years (range, 1-9.5 years), but only one received oral steroid therapy, suggesting that most cases had generally mild disease in this time period (Newman et al. 2005). Longer followup will be needed to determine outcome for those with surveillance-detected CBD on a long-term basis.
Management of CBD is modeled on the management of sarcoidosis. Oral corticosteroid treatment is initiated in patients who have evidence of progressive disease, although progressive disease is not well defined. In advanced cases of CBD (those with respiratory symptoms and deteriorating pulmonary function that are considered as probably due to CBD), standard clinical practice includes the use of corticosteroids. In cases of CBD without physiologic impairment, whose diagnosis is usually based on transbronchial biopsy, the general approach to management is periodic re-evaluation to look for deterioration in symptoms, pulmonary-function test results, or chest radiographs, typically every 1-2 years. The decision to institute treatment with corticosteroids or other anti-inflammatory agents is made case by case.
Older reports, which appeared when beryllium concentrations were much higher, indicated that deterioration can be rapid after the development of clinical disease. Hardy and Tabershaw (1946) followed 17 cases in young workers (age at symptom onset, 20-38 years) and described progression to death in five patients within 1-2 years. Improvement was noted in several workers, but the others had continuing severe disease that progressed rapidly in many cases. In some cases, exacerbation and remission were described. In others, a stable condition that lasted for years was followed by deterioration. Deterioration was described as worsening dyspnea, worsening lung function, worsening radiographic abnormalities, and in some cases the signs and symptoms of pulmonary hypertension and cor pulmonale. One patient returned to normal (with regard to symptoms and radiographic findings) after treatment with adrenocorticotropin (Stoeckle et al. 1969).
A more recent report of siblings with CBD showed clinical features similar to those reported earlier with progressive worsening of disease over 6 years despite steroid treatment (Tarlo et al. 2001). Since the report was published, one sibling has died and the other has become oxygen-dependent. A third co-worker also has end-stage lung disease and has been assessed for heart-lung transplantation (case presentation at International Beryllium Meeting in Montreal 2005), and a fourth worker identified in the last year also has clinical disease requiring steroid therapy despite a BeLPT surveillance program (S. Tarlo, University of Toronto, personal commun., April 23, 2007).
There is also an absence of published data on socioeconomic effects of sensitization and disease. Recommendations have been made that sensitized people minimize further occupational exposure to beryllium (Infante and Newman 2004), and published recommendations have advised avoidance for those with CBD. Implementation of those recommendations might be expected to result in job loss or reduction in income. In addition, even for those without clinical disease, the diagnosis of subclinical CBD or BeS may be associated with psychosocial stress or loss of income. A case presentation at the 2005 International Beryllium Disease Conference in Montreal described a young man with subclinical disease that resulted in job loss, major reactive depression, and unemployment (S. Tarlo, University of Toronto, personal commun., April 23, 2007). However, evaluation of the psychosocial and socioeconomic implications of receiving a diagnosis of BeS or subclinical disease is beyond the scope of the present committee’s task.
Extrapulmonary Disease
Like sarcoidosis, CBD can have extrapulmonary manifestations; they are less common than in sarcoidosis, but few studies have systematically characterized them. Patch testing with soluble beryllium salts has confirmed skin sensitization to beryllium, and skin lesions were reported in workers exposed to beryllium salts (Kreiss et al. 2007) but much less commonly in workers exposed to beryllium metal particles and dusts. Reported cutaneous manifestations of beryllium exposure include dermal granulomas and irritant and allergic contact dermatitis (Curtis 1951; Vilaplana et al. 1992; Berlin et al. 2003). The prevalence of those beryllium-related skin conditions appears to be relatively low, but epidemiologic studies have focused almost exclusively on BeS or CBD and given little attention to skin symptoms and disease.
Surveillance of Beryllium-Exposed Workers with the BeLPT
When used on a population basis, rather than as a screening or diagnostic test, the BeLPT has been shown to be useful for identifying facilities or jobs that pose substantial risk. Medical surveillance with the BeLPT appears to be more sensitive than traditional air sampling because BeS can occur at extremely low air concentrations and also possibly from skin exposure, for which there are no standard monitoring or regulatory guidelines (Stange et al. 2004; Day et al. 2006; Kreiss et al. 2007).
Any test that is used in medical surveillance needs to have acceptable sensitivity, specificity, and predictive value. Since a diagnosis of BeS is usually followed by additional diagnostic testing for CBD with attendant risk and expense, such a diagnosis must have an acceptable positive predictive value (PPV) and so a limited number of false positive tests. Not all abnormal BeLPT results are confirmed by a second test on the same person or even on the same blood sample. Stange et al. (2004) reported on variation between laboratories when a blood sample was split and sent to two laboratories simultaneously. The range of agreement on abnormal results was 26.2-61.8% depending on the laboratories being compared; even between the laboratories with the highest agreement, 38.2% of abnormal BeLPT results were not confirmed by the second laboratory. Because a diagnosis of BeS can lead to additional testing, including biopsy, the clinical definition of sensitization requires a confirmation of an abnormal BeLPT with a second abnormal test (a “confirmed abnormal”); this reduces sensitivity while raising specificity. A “false positive” diagnosis of BeS would then only occur if the BeLPT were confirmed abnormal. An unconfirmed abnormal BeLPT is not a false positive using this definition. It is theoretically possible that someone could have a confirmed abnormal BeLPT but not be sensitized to beryllium, but there is no other test to measure sensitization to beryllium, so it is not possible to identify these cases with any confidence. The available evidence suggests that such false positives are rare. For example, of 458 employees at Rocky Flats who were either new hires or standing employees with no known exposure to beryllium, none had a confirmed positive result (Stange et al. 2004). Silveira et al. (2003) combined data on three sites and found no confirmed positive results in over 1,000 “unexposed” people screened. Any estimate of the rate of a confirmed abnormal BeLPT in people with no exposure to beryllium is confounded by the fact that CBD (and hence a sensitivity to beryllium) has been found after relatively low exposures, and that there is no independent measure of beryllium exposure. If a person with no known exposure to beryllium has a confirmed positive BeLPT, might it be possible that he had occult exposure? Or if a job is thought to involve beryllium exposure in part because of surveillance using the BeLPT, might that job be inappropriately classified with a “false positive” BeLPT? The committee will address such questions in the second report, as part of the discussion of the usefulness of the BeLPT for medical surveillance.
The ultimate question is how well the BeLPT predicts CBD. The usefulness of a screening test can be described according to its sensitivity, its specificity, its PPV, and its negative predictive value. Sensitivity is a measure of how well the test detects true positives, and specificity is a measure of how well it detects true negatives. The PPV is a measure of how many of those who test positive have the underlying condition; it is the ratio of true positives to all positives. A test with very good sensitivity and specificity may not have a good PPV if the disease prevalence is low in the population being screened. For example, a test whose sensitivity is 99.9% and whose specificity is 99.9% is an excellent test. If we use this test in a population of 1,000,000 of whom 1% have the disease for which we are screening, we will detect 9,990 with the disease and miss 10 with the disease. However, we will also have 990 false positives, and a PPV of 91%. As the specificity of the test declines, or the underlying prevalence of disease declines, so does the PPV. In one study that specifically addressed a beryllium-exposed population, Deubner et al. (2001b) calculated the PPV of the blood BeLPT in the Brush-Wellman workforce and reported that a single unconfirmed test had a PPV for CBD of 39%, a confirmed abnormal result had a PPV for CBD of 45%, and a split sample reported as abnormal in two laboratories had a PPV of 49%.
Those results came from populations of workers with on-going exposure to beryllium. Some studies suggest that as exposure declines the incidence of sensitization may decline less than the incidence of CBD in a population; this would mean that the predictive value of the blood BeLPT for CBD may be
lower in workers with low or intermittent exposure to beryllium than in the populations discussed above. Stange et al. (2001) described the prevalence of BeS and CBD in workers at Rocky Flats tested through on-going beryllium surveillance. As years of exposure increased, the proportion of those examined who had CBD also increased, but the proportion of sensitization without CBD did not increase. The CBD prevalence increased from 0.5% in male workers with less than 5 years of employment to 3.7% in those with 20-25 years of employment. The prevalence of sensitization without CBD was 3% in workers with less than 5 years at the plant and was at most 4% in groups with more years of exposure. The ratio of people with CBD to all sensitized people (with and without CBD) is the PPV of the BeLPT; because there can be a long latency between BeS and CBD, the ratio will change with increasing length of followup. Overall, the PPV was 35% in the Rocky Flats workers described by Stange et al.; about one-third of those who were sensitized also had CBD. The PPV was 14% in workers with less than 5 years of employment at Rocky Flats and increased to 65% in workers with more than 20 years of work at the facility. The incidence of CBD varied among groups; for example, it was 23% in the scientists and engineers who were sensitized and 73% in the machinists.
PATHOGENESIS AND MECHANISMS OF ACTION
As early as 1951, Sterner and Eisenbud proposed that CBD was an immune-mediated hypersensitivity reaction directed against the inhaled beryllium antigen. Even the earliest accounts of the disease described it as hypersensitivity of delayed onset, which fits with the present understanding of the cellular immune mechanisms underlying CBD. Although alterations in humoral immune characteristics have been described in CBD patients (Resnick et al. 1970; Cianciara et al. 1980), by and large the immunopathology of the disease involves cellular immune mechanisms. The understanding of the immunologic basis of CBD and the immunopathogenic mechanisms that contribute to it has advanced, but many questions about the details of interactions between exposure and host factors that are manifested as disease in some people remain. The literature of CBD is extensive, and this section consists of a selective review of the primary pertinent literature that has shaped current understanding of the immune mechanisms involved and of genetic factors that might contribute to susceptibility to the disease.
CBD is a systemic granulomatous disorder that affects the lungs predominantly. The mechanism underlying CBD pathogenesis involves an immune response to beryllium (Figure 3-1). In this context, CD4+ T lymphocytes recognize beryllium as an antigen that triggers cell proliferation and release of cytokines and inflammatory mediators. The release of inflammatory mediators results in an accumulation of mononuclear-cell infiltrates and fibrosis that lead to the lesion typical of the disease—a noncaseating granuloma.
Critical Role of CD4+ T Cells
Beryllium acts as a major histocompatability complex (MHC) class II restricted antigen stimulating the proliferation and accumulation of beryllium-specific CD4+ T cells in the lungs (Saltini et al. 1989, 1990). Two observations illustrate the primary importance of CD4+ T cells in the pathogenesis of CBD: the development of granulomatous inflammation in the lung is associated with the accumulation of CD4+ T cells in the BAL fluid, and sensitization to beryllium is detected in the ability of CD4+ T cells to proliferate in response to beryllium salts in culture.
The immunobiology believed to be associated with CBD provides a diagnostic test for BeS. As noted earlier, the BeLPT involves an in vitro challenge of either BAL-derived or peripheral blood-derived mononuclear cells with beryllium salts. In beryllium-responsive people, the challenge induces an oligoclonal proliferation of sensitized lymphocytes that is measured in a standard assay in which tritiated-thymidine incorporation occurs in proportion to DNA synthesis and blastogenesis (Rossman et al. 1988; Kreiss et al. 1989).
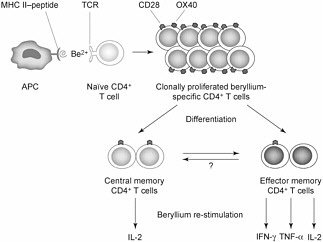
FIGURE 3-1 Immune response to beryllium. Source: Fontenot and Maier 2005. Reprinted with permission; copyright 2005, Trends in Immunology.
Because beryllium drives the proliferation and expansion of CD4+ T cells in an antigen-restricted manner, T-cell lines and clones have been derived from the BAL fluid and blood of CBD patients. There are important differences between the antigen-specific T-cell clones found in the lungs of CBD patients and those in the circulation of beryllium-sensitized people, and the differences may have implications for the progression from BeS to CBD. For example, the T-cell receptor (TCR) repertoire of beryllium-reactive peripheral blood cells appears to be more diverse than that in the lungs of CBD patients (Fontenot et al. 1999). That suggests that a subset of T-cell clones expressing homologous TCRs has pathogenic potential. In many people, particularly CBD patients in the ceramics industry exposed to beryllium oxides, the T cells found in the BAL fluid express TCRBV3 genes with identical or homologous complementary-determining region 3 sequences. As further evidence that these are oligoclonal expansions, the beryllium-responsive T cells coexpress only a few homologous TCRα genes (Fontenot et al. 1999). That means that there is selective expansion or accumulation of some CD4+ T-cell subsets in the lungs of CBD patients. The selectivity is probably related to the antigenicity of beryllium and probably provides clues to conventional antigen peptides that are modified by beryllium.
Antigen Processing and Presentation of Beryllium
As discussed above, sensitization to beryllium can be readily demonstrated in the ability of CD4+ T cells to proliferate in response to beryllium salts in culture. The proliferative response has characteristics of a response to antigen, but the nature of the antigen recognized by CD4+ T cells is not known. In studies with mouse lymphocytes, Newmann and Campbell (1987) reported that beryllium sulfate was mitogenic for B lymphocytes but not T lymphocytes. The potential for endotoxin contamination of the beryllium-salt preparation to drive this polyclonal B-cell response was not addressed by Newmann and Campbell. On the basis of many human studies, it is reasonable to conclude that beryllium is not a mitogen for human lymphocytes. Proliferation of beryllium-specific CD4+ T cells requires the engagement of clonotypic TCRs with an unknown beryllium antigen bound by MHC class II molecules on the surface of antigen-presenting cells.
The physiochemical properties of beryllium ions offer few clues that lead to a better understanding of its immunogenicity. The immunogenicity of beryllium probably lies mainly in its ability to haptenate, and thereby alter the structure of peptides occupying the antigen-binding cleft of MHC class-II molecules. Other metal ions including nickel, cobalt, mercury, and gold may elicit T cell reactivity by similar mechanisms (Lawrence and McCabe 2002); however, the specific peptides and MHC molecules involved in all cases are different than those attributed to immune reactivity to beryllium. As with these immune reactivities to other metal:pMHC, the response to beryllium:pMHC is exquisitely specific and lacks crossreactivity with other metal:MHC complexes.
Knowing that susceptibility to CBD was associated with particular alleles of the class II human leukocyte antigen-DP (HLA-DP) molecule, Fontenot et al. (2000) examined whether the CD4+ T-cell proliferation accompanying CBD involved the presentation of beryllium by HLA-DP. Beryllium-specific T-cell lines isolated from the lungs of CBD patients showed that the response to beryllium was almost completely and selectively blocked by monoclonal antibodies directed at HLA-DP. Additional studies with fibroblasts engineered to express only specific HLA-DP alleles demonstrated that the response to beryllium was restricted to haplotypes previously implicated in susceptibility to the disease. Hence, beryllium presentation by some HLA-DP alleles to CD4+ T cells is the underlying mechanistic basis of CBD. Analysis of the amino acid residues shared by HLA-DP alleles that present beryllium revealed that those possessing a negatively charged glutamic acid residue at the 69th position of the β chain were especially capable of inducing a T-cell response (Richeldi et al. 1993; Wang et al. 1999; Lombardi et al. 2001; Fontenot et al. 2000; Bill et al. 2005). Not all CBD patients have a Glu69 containing HLA-DP allele. Indeed, the early work by Fontenot et al. (2000) demonstrated that anti-HLA-DR reagents partially inhibited T cell responsiveness to beryllium in some cases. Recent work by Bill et al. (2005) reported an increased frequency of HLA-DR13 in some CBD patients lacking a Glu69 HLA-DP allele. These HLA-DR13 alleles possess a glutamic acid at position 71 of the β-chain (which corresponds to position 69 of HLA-DP). Beryllium presentation to CD4+ T cells can occur through an alternate HLA-DR Glu71 pathway that is capable of inducing beryllium-specific proliferation and IFN-γ production by CD4+ T cells. Genetic susceptibility to CBD is discussed later in this chapter.
Amicosante et al. (2001) conducted beryllium-binding assays with purified soluble HLA-DP molecules and beryllium sulfate and showed that the HLA-DPβGlu69 residue played a role in beryllium binding. Whether that involves a direct interaction between Glu69 and beryllium ions or beryllium modifies an unknown peptide that then preferentially interacts with the HLA-DPβGlu69 alleles is unknown (reviewed by Amicosante and Fontenot [2006]). Homozygosity, as opposed to heterozygosity, in the expression of the HLA-DPβGlu69 supratypic variant allele did not impart increased responsiveness, so the cell-surface density of class II molecules charged with beryllium-modified antigenic peptides does not dictate the intensity of responsiveness (Amicosante et al. 2005).
The nature of the beryllium antigen remains one of the key issues that requires further study with respect to the immunopathogenesis of CBD. Amicosante et al. (2001) demonstrated that beryllium binds to HLA-DPβGlu69 at a pH of 5.0 as well as at a pH of 7.5. The pH 5.0 mimics the acidic microenvironment where peptides are loaded onto HLA class II molecules, whereas, pH 7.5 represents the extracellular pH where beryllium might bind to HLA-DP molecules directly at the cell surface. That beryllium binds to HLA-DPβGlu69 at a pH of 7.5 suggests that it binds to HLA-DP in the absence of antigen processing. Furthermore, Fontenot et al. (2006a) demonstrated that paraformaldehyde-fixed beryllium-pulsed antigen-presenting cells stimulated the proliferation of CD4+ T-cell lines derived from the lungs of CBD patients. That suggests that the presentation of soluble beryllium does not require antigen processing. Although direct antigen presentation of beryllium from soluble beryllium salts may occur, Stefaniak et al. (2005) reported that dissolution of beryllium oxide particles in macrophage phagolysosomes may be an important source of dissolved beryllium for input to the cell-mediated immune reaction characteristic of beryllium disease. The physiochemical state of beryllium (i.e., single constituent versus multi-constituent material) influences its bioavailability, which may be tied to its ability to initiate or sustain immune reactivity to beryllium. Stefaniak et al. (2006) found that the dissolution rate stimulated by phagolysosomal fluid was greater for beryllium-copper-alloy fume than for
beryllium oxide, suggesting that the physiochemical form of beryllium encountered in the workplace may have a bearing on initiating the sensitization process. Beryllium complexed with ferritin may be an important source of beryllium uptake by macrophages (Sawyer et al. 2004a). The uptake of beryllium may lead to aberrant apoptotic processes and the release of beryllium ions, which will continue the stimulation of T-cell activation (Sawyer et al. 2000; Kittle et al. 2002; Sawyer et al. 2004a). Beryllium uptake may be accompanied by oxidative stress and generation of reactive oxygen species that lead to the apoptotic response (Sawyer et al. 2005). It has been hypothesized that the interaction between the innate and acquired immune systems leads to the cyclical rerelease of beryllium into the lungs, where it elicits proinflammatory cytokine production and T-cell proliferation (Sawyer et al. 2002).
The beryllium-antigen-presenting cells themselves have not been well defined (L.A. Maier, National Jewish Medical and Research Center, personal commun., April 5, 2007). They may be macrophages, dendritic cells, or other professional antigen-presenting cells. Recently, self-presentation of beryllium by HLA-DP-expressing BAL CD4+ T cells has been reported (Fontenot et al. 2006b). Self-presentation by BAL T cells in the granuloma results in activation-induced cell death, which may lead to the oligoclonality of the T-cell populations characteristic of CBD.
Th1 Cytokine Secretion by Beryllium-Specific T Cells
The CD4+ T cells that accumulate in the lungs of CBD patients exhibit a Th1 phenotype and secrete such cytokines as IL-2, IFN-γ, and TNF-α (Tinkle and Newman 1997; Tinkle et al. 1997; Fontenot et al. 2002). Bost et al. (1994) were the first to show that alveolar macrophages from CBD patients produced increased concentrations of mRNAs for TNF-α and IL-6 but not IL-1β, and the increase in mRNA was accompanied by an increase in TNF-α in BAL fluid. Tinkle et al. (1996) extended those observations and showed that the cytokines were released in response to beryllium stimulation and contributed to the unchecked inflammatory responses of effector macrophages and lymphocytes that are characteristic of the disease. The frequency of beryllium-specific Th1-cytokine-secreting CD4+ T cells in the blood of beryllium-exposed people may prove to be a useful biomarker in discriminating between BeS and progression to CBD (Pott et al. 2005). The release of chemokines, including MIP-1α and GRO-1, may also lead to the migration of lymphocytes to the lung and the formation of the microenvironment that contributes to the development of CBD (Hong-Geller et al. 2006). The polarized Th1-like response to beryllium results in macrophage activation, accumulation, and aggregation and to the perpetuation of granulomatous inflammation seen in CBD.
Beryllium-Sensitization Progression to Chronic Beryllium Disease
The immunologic mechanisms underlying the progression from BeS to CBD are not well understood. Beryllium-sensitized people demonstrate a beryllium-specific immune response and show no evidence of lung disease. In contrast, CBD is characterized by granulomatous inflammation and the accumulation of beryllium-responsive CD4+ T cells in the lung.
As mentioned above, the development of granulomatous inflammation in the lung is associated with the accumulation of CD4+ T cells in BAL fluid. Saltini et al. (1989, 1990) showed that increased frequency of mononuclear cells (macrophages and lymphocytes) in BAL fluid was a characteristic of CBD. Most of the BAL lymphocytes were CD4+ T cells, the majority of which express markers consistent with an effector-memory T-cell (TEM-cell) phenotype (such as CD45ROhi, CD62Llo, and CCR7lo). These TEM cells recognize the beryllium antigen in a CD28-costimulation-independent fashion, unlike beryllium-reactive cells in the periphery that require CD28 costimulation (Fontenot et al. 2003). A recent report by Palmer et al. (2007) extends that analysis of phenotypic characterization of CD4+ subsets implicated in CBD by showing that expression of the CD57 marker is associated with inflammation and functional competence of the T cells in the lung.
Progression from BeS to CBD is characterized by an increase in the frequency of beryllium-specific, Th1 cytokine secreting CD4+ T cells in the lung and granulomatous tissue. There appear to be important differences between beryllium-reactive memory CD4+ T cells found in the lung and the peripheral blood of CBD patients (Fontenot et al. 2003). These differences include maturational differences in the memory T cell compartment as indicated by CD28 costimulation dependence of the CD4+ beryllium-specific T cells in the periphery and dissociation between Th1 cytokine secretion and lymphoproliferation in the periphery. Fontenot et al. (2005) compared the memory-cell phenotype of beryllium-reactive cells from CBD and BeS subjects and found that progression from sensitization to disease was associated with a differentiation of memory cells to an effector cell phenotype (i.e., TEM). Thus, an accounting of the frequency of TEM cells in the blood of sensitized people may provide a means of monitoring disease progression. In other words, the beryllium-reactive CD4+ T cells in the lungs of CBD patients are more differentiated than those in the blood of BeS people. Understanding the functional differences in CD4+ T cells between the two compartments may be the key to understanding the immunopathogenesis of CBD and conversion from BeS and may lead to the development of biomarkers to identify people at greatest risk.
GENETIC SUSCEPTIBILITY
As noted earlier in this chapter, not all people exposed to beryllium become sensitized, and not all who do progress to develop CBD. Development of CBD appears to depend not only on the history of exposure to beryllium but also on the genotype and phenotype of the person exposed. Attempts to identify the genetic components involved in susceptibility have centered primarily on the definition of CBD as a cell-mediated MHC class II restricted inflammatory disease. Accordingly, most studies have focused on specific genetic polymorphisms in MHC class II and proinflammatory genes, and a few others have considered the role of TCR expression repertoires and other potential modifier genes.
Human Leukocyte Antigen Class II
In humans, the most gene-dense and polymorphic region of the genome is the MHC, which resides on chromosome 6p21.31. At the centromeric end of the MHC, spanning about 800 kilobases of DNA, sits the classical class II region (Acton 2001). It codes for HLA-DP, HLA-DQ, and HLA-DR—three heterodimeric proteins with limited tissue distribution (for example, to macrophages, monocytes, dendritic cells, and B lymphocytes) that are involved in antigen presentation and processing. The notion of a role of these genes in CBD arose from experiments that used lymphocytes derived from blood and BAL fluid of patients with the disease. Several studies demonstrated that antibodies directed against class II molecules blocked proliferation of those lymphocytes in response to beryllium stimulation. The studies led to the idea that some HLA class II molecules may bind to beryllium and present it to T cells. Each class II molecule consists of an α chain and a β chain, and the α1 and β1 domains of these chains, respectively, form the peptide-binding domain of each molecule. Genes coding for those domains, which can be highly polymorphic, have been attractive candidates in genetic-association studies of CBD. Functional studies have also been used to study whether identified polymorphisms will result in differences in binding affinity and specificity for beryllium.
HLA-DP
In the HLA-DP heterodimer, the β chain displays far more polymorphism than the α chain. Some 23 alleles of HLA-DPα1 and 126 alleles of HLA-DPβ1 have been described as of April 2007 (EBI 2007). In a seminal study, Richeldi et al. (1993) first demonstrated the role of variants in the HLA-DPβ1 domain
in CBD. That remains the best-studied and strongest genetic association in this disease. They identified 33 CBD patients defined by a history of occupational exposure, x-ray abnormalities, abnormal lung function, presence of granulomas, and a positive BeLPT result. The patients had a higher frequency of the HLA-DPB*0201 allele than 44 similarly exposed workers who had no manifestations of CBD (52% vs 18%) and a lower frequency of the DPB*0401 allele (27% vs 68%). The two alleles differ at position 69, where HLA-DPB*0201 has the amino acid glutamic acid instead of lysine. Further analysis showed that when all the alleles were considered, this Glu69 single-nucleotide polymorphism (GAG instead of AAG) was expressed in 97% of the CBD patients examined and 30% of the controls. HLA-DPB1 Glu69 appeared to be a definitive marker of susceptibility to beryllium disease.
Later studies, many by the same group, have reaffirmed the predominant role of the Glu69 variant in CBD but have suggested that its frequency is lower than originally thought (see Table 3-2). For example, Saltini et al. (2001) found HLA-DPB1 Glu69 to be present in only 73% of 22 cases studied. Given the relatively small samples involved in the studies, such a discrepancy is to be expected.
HLA-DP1 Glu69 and Sensitization
The original Richeldi et al. (1993) study left open the question of whether HLA-DP1 Glu69 was a marker of an immune response to beryllium, specifically recognition and presentation, or simply a marker of disease susceptibility. Several studies have now evaluated HLA-DP1 Glu69 in BeS rather than in CBD itself. Wang et al. (2001) found the Glu69 substitution in 22 (88%) of 25 BeS people but in only 61 (37%) of 163 nonsensitized people. One study reported a much lower frequency of Glu69 in BeS subjects than in CBD subjects (Salitini et al. 2001), but other, larger studies have confirmed the initial finding and have shown Glu69 frequency to be similar in people with BeS and those with CBD (Rossman et al. 2002; Maier et al. 2003b; McCanlies et al. 2004).
HLA-DPB1 Glu69 is present in up to 48% of beryllium-exposed people without CBD (McCanlies et al. 2003). Given the low frequency of the disease, that implies that most people with the Glu69 substitution do not develop the disease. Their failure to get CBD may be due in part to undocumented differences in workplace exposure to beryllium, co-exposure to other environmental factors, or an inability to identify people in the early stages of the disease. Alternatively, other genetic considerations may be important. Using allele-specific DNA sequencing, Wang et al. (1999) showed that the specific allele carrying the Glu69 might be important. The most common HLA-DPB1 Glu69 allele is *0201; however, in a comparison of 20 people with CBD and 75 controls, the strongest association with CBD was found with the rarer non-*0201 Glu69 alleles. Furthermore, the specific alleles for the α chain (HLA-DPA1) in the HLA-DPB1 Glu69 carriers were associated with disease development. The disparity in the importance of HLA-DPB1*0201 between this study and that of Richeldi et al. (1993) was attributed to the small number of probes and the less sensitive technique (partial regional group-specific hybridization) used in the earlier study. Wang et al. (2001) studied the role of the alleles in BeS in a followup study of the same 20 CBD patients, 25 patients with positive BeLPT results but without CBD, and 163 BeLPT-negative controls. The frequency of the rare non-*0201 Glu69 alleles was higher in BeS subjects (52%) than in controls (13%) and appeared lower than in CBD patients although this was not statistically significant. In particular, HLA-DPB1*1701 was overrepresented in CBD (30%) and BeS (16%) groups but rare in the controls (2%). Although those results are suggestive, there have been some concerns about misclassification of subjects. However, studies by Rossman et al. (2002) and Maier et al. (2003b) have largely confirmed that the HLA-DPB1 non-*0201 Glu69 allele is more prevalent than the more common HLA-DPB1*0201 in both CBD and BeS. One study found no differences between BeS subjects and controls (Saltini et al. 2001), but it had a smaller study population and this smaller group was included in other genetic studies.
Using computational chemistry and molecular modeling, Weston et al. (2005) studied the HLA-DPB1 gene variants that were shown to code for Glu69. They assigned odds ratios for specific alleles on the basis of the studies cited above and found a strong correlation between the reported hierarchic order of
risk of CBD and the predicted surface electrostatic potential and charge of the corresponding isotypes. They concluded that alleles associated with the most negatively charged proteins carry the greatest risk of BeS and CBD.
Another unresolved issue is whether copy number affects sensitization and disease. In the studies by Wang et al. (1999, 2001), HLA-DPB1 Glu69 homozygotes were seen only at very low frequencies in the control groups (1.3-3%) but at 24% and 30% in BeS and CBD groups, respectively. Maier et al.
TABLE 3-2 Summary of Association Studies on HLA-DPB1 Glu69 and TNF-α As Susceptibility Factors in Chronic Beryllium Disease and Beryllium Sensitization
|
Author |
|
N |
Frequency |
Homozygocity |
Alleles |
|
|
HLA-DPB1 Glu69 |
|
|
|
|
Glu69 |
|
|
Richeldi et al. 1993 |
CBD |
33 |
97% |
N/A |
0201: 52% |
|
|
|
Controls |
44 |
30% |
|
18% |
|
|
Richeldi et al. 1997 |
CBD |
6 |
83% |
|
|
|
|
|
Controls |
121 |
30% |
|
|
|
|
Wang et al. 1999 |
CBD |
20 |
95% |
30% |
0201: 42% |
Non-0201: 80% |
|
|
Controls |
34 |
45% |
1.3% |
68% |
|
|
Saltini et al. 2001 |
CBD |
22 |
73% |
N/A |
0201: 36% |
Non-0201: 41% |
|
|
BeS |
23 |
39% |
|
22% |
17% |
|
|
Controls |
93 |
40% |
|
29% |
11% |
|
Wang et al. 2001 |
BeS |
25 |
88% |
24% |
0201: 44% |
Non-0201: 52% |
|
|
Controls |
163 |
38% |
3% |
25% |
13% |
|
Rossman et al. 2002 |
CBD |
25 |
84% |
Not associated with CBD |
Non-0201: associated with CBD vs. controls |
|
|
|
BeS |
30 |
90% |
|||
|
|
Controls |
82 |
47% |
(data not shown) |
|
|
|
Maier et al. 2003 |
CBD |
104 |
86% |
26% |
0201: 39% |
Non-0201: 63% |
|
|
BeS |
50 |
85% |
15% |
40% |
56% |
|
|
Controls |
125 |
38% |
1.7% |
24% |
14% |
|
McCanlies et al. 2004 |
CBD |
90 |
82% |
21% |
N/A |
|
|
|
BeS |
64 |
68% |
16% |
|
|
|
|
Controls |
727 |
33% |
4% |
|
|
|
TNF-α-308 |
|
|
|
|
Other Polymorphisms |
|
|
Saltini et al. 2001 |
BeS and CBD |
45 |
51% |
|
N/A |
|
|
|
Controls |
93 |
16% |
|
|
|
|
Dotti et al. 2004 |
BeS and CBD |
73 |
27% |
|
TNF-α-1031, -863, -238; all not associated vs. controls; TNF-α-857T increased in CBD |
|
|
|
Controls |
43 |
5.8% |
|
||
|
Gaede et al. 2005 |
Europe/Israel CBD |
13 |
15% |
0% |
N/A |
|
|
|
Controls |
216 |
34% |
4.6% |
|
|
|
|
United States CBD |
39 |
44% |
13% |
|
|
|
|
Controls |
67 |
16% |
1.5% |
|
|
|
McCanlies et al. 2007 |
CBD |
91 |
29% |
2.2% |
TNF-α-238: |
8.9% |
|
|
BeS |
63 |
38% |
6.4% |
|
13% |
|
|
Controls |
722 |
28% |
2.6% |
|
12% |
|
Sato et al. 2007 |
CBD |
147 |
30% |
0% |
TNF-α-1031, -863, -857, -238; all not associated vs. controls |
|
|
|
BeS |
112 |
36% |
2.5% |
||
|
|
Controls |
323 |
30% |
2.3% |
||
(2003b) showed a similar frequency (26%) in CBD patients and concluded that Glu69 homozygosity conferred the greatest risk for CBD; however, they did not find that it was a risk factor for BeS. That led to the conclusion that Glu69 homozygosity may be important in disease progression. McCanlies et al. (2004), in a study of 884 beryllium workers (90 with CBD and 64 with BeS), also found increased HLA-DPB1 Glu69 homozygosity in those with CBD (21%) or BeS (16%). However, they argued that because the HLA-DPB1 Glu69 genotypic distribution among CBD cases did not conform to Hardy-Weinberg population laws but did for BeS and controls, it is the presence of those alleles rather than homozygosity itself that confers risk. The mechanism by which homozygosity would enhance an immune response is unclear. Further complicating the issue is the finding that expression of HLA-DP Glu69 in the BeLPT determines higher T-cell proliferation rates but that homozygotes do not show greater proliferation than heterozygotes (Amicosante et al. 2005).
Gene-Environment Interaction
In a cross-sectional study of 127 workers, Richeldi et al. (1997) found that CBD was 8 times more likely in machinists (workers with greater exposure to beryllium) with HLA-DPB1 Glu69 than in those without this variant and was 7 times more prevalent than in nonmachinists with HLA-DPB1 Glu69. Those results suggest a potent additive gene-environment interaction, but the number of cases was very small (six), and this issue has yet to be addressed adequately in a larger setting.
HLA-DQ and HLA-DR
The original report that identified the importance of HLA-DPB1 Glu69 in CBD found no relationship between CBD and HLA-DR or HLA-DQ (Richeldi et al. 1993). However, because a significant number of CBD patients (3-27%) do not have Glu69, other MHC class II molecules have been investigated. The huge number of alleles involved, the small populations studied, and the relative lack of appropriate tools have limited the studies, and their results have been equivocal. The most consistent finding has been an increased frequency of HLA-DR13 alleles in those lacking HLA-DPB1 Glu69 (Rossman et al. 2002; Maier et al. 2003b; Amicosante et al. 2005). Support for this association comes from the finding that those with the alleles have a glutamic acid at position 71 of the β chain, which corresponds to Glu69 of HLA-DP. Functional experiments show that this Glu71 is essential for beryllium presentation by HLA-DR to CD4+ T cells (Bill et al. 2005).
Associations between HLA-DQ markers and BeS or CBD in people lacking HLA-DPB1 Glu69 have been reported, but they have been attributed primarily to linkage disequilibrium with HLA-DR (Amicosante et al. 2005; Maier et al. 2003b).
Tumor-Necrosis Factor-α (TNF-α)
The gene for TNF-α is telomeric to the class II loci. This proinflammatory cytokine is thought to play a key role in CBD. High ![]() concentrations have been associated with more severe pulmonary disease in CBD. In addition, beryllium stimulation of CD4+ T cells from the BAL fluid of CBD patients, but not BeS or sarcoidosis patients, will potentially induce TNF-α production (Sawyer et al. 2004b). (Sawyer et al. 2004b). The process appears to be transcription-dependent, in that beryllium exposure specifically upregulates the AP-1 and NF-κB transcription factors (Sawyer et al. 2007). Accordingly, several studies have evaluated functional polymorphisms in the promoter of the
concentrations have been associated with more severe pulmonary disease in CBD. In addition, beryllium stimulation of CD4+ T cells from the BAL fluid of CBD patients, but not BeS or sarcoidosis patients, will potentially induce TNF-α production (Sawyer et al. 2004b). (Sawyer et al. 2004b). The process appears to be transcription-dependent, in that beryllium exposure specifically upregulates the AP-1 and NF-κB transcription factors (Sawyer et al. 2007). Accordingly, several studies have evaluated functional polymorphisms in the promoter of the ![]() gene and their role in BeS and CBD.
gene and their role in BeS and CBD.
The most commonly studied is the polymorphism with a G to A transition at the -308 position, which has been shown by many to be associated with increased TNF-α production and disease severity in
a variety of conditions. In a small study, Maier et al. (2001) confirmed that this polymorphism was also associated with increased beryllium-stimulated BAL-cell TNF-α production by studying CBD patients who had been classified as “high” (n = 20) or “low” (n = 10) TNF-α producers. Saltini et al. (2001) saw associations between the TNF-308A polymorphism and both BeS and CBD in a population of 639 workers. In a followup study of the same cohort, Dotti et al. (2004) extended those results and reported that TNF-308A alleles were more prominent in the 73 subjects with either BeS or CBD (26.7%) than in the 43 controls (5.8%). Moreover, a similar association was also observed for another polymorphism, TNF-857T. Gaede et al. (2005) suggested that genetic background might also play a role in the importance of the TNF-308 allele. They reported that the high TNF-α-producing variant was present at increased frequency in CBD patients in the United States but not in those in Europe and Israel, but it is likely that the two groups had different beryllium exposure and disease severity.
Recent large-scale studies have cast doubt on earlier findings of the importance of ![]() polymorphisms in CBD. McCanlies et al. (2007) found no relationship between CBD and either TNF-308 or TNF-238 in a large population-based study (886 beryllium workers, including 92 with CBD and 64 with BeS). Furthermore, contrary to previous reports by one group (Saltini et al. 2001; Amicosanti et al. 2001; Rogliani et al. 2004), no interaction between HLA-DP1 Glu69 and either allele could be seen. Similarly, in probably the most thorough examination of the question to date, Sato et al. (2007) compared CBD patients (n = 147), BeS subjects (n = 112), and healthy beryllium-exposed controls (n = 323) and studied five TNF-promoter single-nucleotide polymorphisms (including all those studied previously) and six relevant haplotypes. They reported that although some alleles and haplotypes might be associated with constitutive and beryllium-stimulated BAL-cell
polymorphisms in CBD. McCanlies et al. (2007) found no relationship between CBD and either TNF-308 or TNF-238 in a large population-based study (886 beryllium workers, including 92 with CBD and 64 with BeS). Furthermore, contrary to previous reports by one group (Saltini et al. 2001; Amicosanti et al. 2001; Rogliani et al. 2004), no interaction between HLA-DP1 Glu69 and either allele could be seen. Similarly, in probably the most thorough examination of the question to date, Sato et al. (2007) compared CBD patients (n = 147), BeS subjects (n = 112), and healthy beryllium-exposed controls (n = 323) and studied five TNF-promoter single-nucleotide polymorphisms (including all those studied previously) and six relevant haplotypes. They reported that although some alleles and haplotypes might be associated with constitutive and beryllium-stimulated BAL-cell ![]() production, they were not risk factors for either CBD or BeS. The discrepancies between past studies showing associations and the more recent studies may be due to misclassification, exposure differences, linkage disequilibrium between HLA-DRB1 and
production, they were not risk factors for either CBD or BeS. The discrepancies between past studies showing associations and the more recent studies may be due to misclassification, exposure differences, linkage disequilibrium between HLA-DRB1 and ![]() genes, or statistical power.
genes, or statistical power.
Other Modifier Genes
Despite the assumption that CBD is a multigenetic disease, few genes outside the MHC loci have been carefully studied. Maier et al. (1999) studied polymorphisms in the gene for angiotensin-1 converting enzyme (ACE), a vasodilatory proinflammatory peptide, because of the observation that serum ACE activity is associated with CBD severity (Newman et al. 1992). They did not find any differences in ACE genotype between CBD patients and controls, nor did they find any statistically significant associations between ACE genotype and markers of disease severity or the BeLPT. Gaede et al. (2005) did find an association between polymorphisms in the transforming growth factor β1 (TGF-β1) gene and CBD; the polymorphism was found in 59 CBD patients compared with 164 healthy beryllium-exposed controls. However, TGF-β has not been measured in serum or BAL fluid of CBD patients, so the functional relevance of the association is unknown. Bekris et al. (2006) compared 29 healthy beryllium-exposed people, 27 BeS subjects, and 30 CBD subjects and observed associations between functional polymorphisms in the gene for glutamate cysteine ligase (GCLC TNR 7/7 and GCLM-588 C/C), an enzyme involved in glutathione synthesis, and CBD but not BeS. Because CBD is characterized by a Th1 cytokine response in the lungs and increased glutathione is thought to favor a Th1 response and is observed in the lungs of CBD patients, the results are functionally plausible, but they need to be confirmed in larger studies.
Recent gene-expression studies of beryllium-naive peripheral-blood mononuclear cells stimulated with beryllium have shown upregulated expression in many inflammation-related genes (Hong-Geller et al. 2006). Similar studies of CBD lung tissues will provide likely candidates.
ANIMAL MODELS OF PULMONARY IMMUNOTOXICITY
Beginning in the early 1950s, numerous studies in several animal species were conducted with beryllium in different chemical forms and administered by different routes.
Hall et al. (1950) repeatedly exposed six species (cats, dogs, guinea pigs, monkeys, rabbits, and rats) to four types of beryllium oxide powders that varied in calcination and chemical form—BeSO4•4H2O fired at 1,350°C, BeSO4•4H2O fired at 1,150°C, BeO•2H2O fired at 1,150°C, and Be4O(C2H3O2)6 fired at 400°C—in a dust-dispersion chamber. Hematologic and pulmonary effects of all the test agents in all the species were observed. Rats showed the highest acute toxicity. Beryllium oxide fired at 400°C was the most toxic, probably because of its small particle size (mass mean of 3 μm) and more extensive distribution.
Stokinger et al. (1950) tested 11 species with repeated 6-h exposures to beryllium sulfate at 1-100 mg/m3 in inhalation chambers. Concentrations of 50 mg/m3 and greater were lethal in most of the species. Two response phases seemed to occur: an acute phase, in which animals died within days or weeks, and a delayed phase, in which animals showed increasingly severe changes (anemia, weight loss, and histopathologic lesions in the lungs) over months that sometimes resulted in death.
In a study of female rhesus monkeys (Schepers 1964), beryllium fluoride was found to be more toxic than beryllium sulfate or beryllium phosphate. Weight loss, apathy or malaise, dyspnea, and death from chemical pneumonitis were reported. Pulmonary inflammation, edema, and emphysema were also evident.
Robinson et al. (1968) examined lung histopathology in two dogs exposed to dusts containing a mixture of beryllium oxide (50%), beryllium fluoride (40%), and beryllium chloride (10%) at 115 mg/m3 for 20 min. Small perivascular granulomatous lesions were detected in the lungs after 3 years. The lesions were said to be typical of a foreign-body reaction.
The possibility that adrenal cortical imbalance (an effect sometimes triggered during pregnancy, surgery, or infection) can induce CBD was investigated by Clary et al. (1972). The distribution of radioactive beryllium oxide and beryllium sulfate instilled in the lungs of guinea pigs (strain 13 and albino) and mice (albino) was evaluated after treatment with metyrapone, a disruptor of corticosteroid synthesis (inhibition of 11β-hydroxylation). When adrenal function was altered, there was increased accumulation of beryllium in the liver and decreased accumulation in bone. Effects were greater in male mice than in female mice.
Clary et al. (1975) used beryllium oxide to examine the effect of adrenal stimulation caused by multiple pregnancies on the onset of CBD in male and female rats. The absence of an effect on beryllium oxide distribution or on the onset of CBD suggested that adrenal stimulation does not play a role in CBD.
Marx and Burrel (1973) found that Hartley guinea pigs could be sensitized to beryllium sulfate by repeated—but not single—intradermal injections, which led to positive skin tests. Migration-inhibitory-factor (MIF) production was correlated with positive skin tests, and it was suggested that reactivity to beryllium is associated with classic delayed hypersensitivity.
Eskenasy (1979) sensitized rabbits with intramuscular injections of 10 mg of beryllium sulfate in Freund’s adjuvant. Intradermal and intratracheal challenges led to skin and lung granulomas, respectively.
In another study, rabbits intradermally immunized with beryllium sulfate (100 μg) developed delayed hypersensitivity reactions and skin granulomas when challenged (1-10 μg). MIF production in BAL cells was increased at doses of 5 and 10 μg. Beryllium was toxic to macrophages at doses greater than 10 μg. Popliteal lymph nodes were negative for beryllium-induced lymphocyte proliferation (Kang et al. 1977).
Barna et al. (1981) induced granulomatous lung disease in Hartley and strain 2 guinea pigs by administering injections of 10 mg of beryllium oxide intratracheally. Blood lymphocytes showed significant blast transformation when challenged with beryllium sulfate. Tolerance to the responses was achieved with intravenous or oral exposure to beryllium sulfate. The response was also mitigated by treatment with prednisone, L-asparaginase, or cytoxan. Sensitized guinea pigs had positive delayed-
hypersensitivity skin tests. Granulomatous lung disease was not induced by beryllium oxide in strain 13 guinea pigs; it was suggested that strain 2 animals had a genetic predisposition.
Goel et al. (1980) fed male albino rats 20 mg of beryllium nitrate every 3 days for 10 weeks. The lungs of exposed rats had histopathologic changes indicative of granuloma and inflammation.
Hart et al. (1984) examined the biochemical, cytologic, and histologic alterations in the lungs of F344 rats exposed for 1 h to an aerosol of beryllium oxide fired at 560°C. The initial lung burden of beryllium was 500 ng. Lung inflammation was detected by day 2. In BAL fluid, lipids, enzymes, and total proteins were increased and macrophage phagocytosis was reduced.
Increases in lactate dehydrogenase, alkaline phosphatase, acid phosphatase, and albumin were found in the BAL fluid of male F344 rats and Balb/C mice exposed nose-only to beryllium sulfate for 1 h (rats at 3.3 or 7 μg/L and mice at 7.2 μg/L). Time-dependent increases in those markers of lung damage were observed. Lactate dehydrogenase peaked on day 8 in rats and on day 3 in mice, and albumin peaked on day 5 in both species (Sendelback and Witschi 1987).
Votto et al. (1987) examined a rat model for beryllium sulfate-induced granulomas by using an ovalbumin and Freund’s adjuvant emulsion. F344 rats were immunized with beryllium sulfate and then given subcutaneous booster injections every 2 weeks. Pulmonary granulomas surrounded by lymphocyte cuffs were found after 6 weeks. Immunohistochemical study of lung tissue showed an increase in helper-T subsets and B cells. Lymphocyte populations in BAL fluid did not correlate with those in lung tissue.
Sendelbach et al. (1989) examined histopathologic changes in male rats exposed nose-only to beryllium sulfate for 1 h at 4.05 μg of beryllium per liter. Focal interstitial pneumonitis was detected with an increase in interstitial and alveolar macrophages. Enzyme activity in BAL fluid was increased for up to 3 months and appeared to correlate with the severity of histopathology.
Several lines of research were pursued at the Inhalation Toxicology Research Institute to develop animal models of beryllium-induced lung disease (see Finch et al. 1996 for an overview). Haley et al. (1989) developed a beagle model of beryllium-induced granulomatous lung disease with beryllium oxide calcined at 500°C or 1,000°C. Lung burdens of beryllium achieved were 18 and 42 μg/kg for the 500°C beryllium and 18 and 48 μg/kg for the 1,000°C beryllium. Peribronchiolar and perivascular changes in the lungs that progressed to microgranulomas and granulomatous pneumonia were observed. The changes were more severe in dogs exposed to the 500°C beryllium. The percentages and total numbers of lymphocytes in BAL fluid were increased after 3 months in dogs treated with 500°C beryllium but not in dogs treated with 1,000°C beryllium. Peripheral blood lymphocytes responded to beryllium challenge in vitro in all four treatment groups after 6-7 months, but positive results for lung lymphocytes were observed only in the group with high lung burdens of 500°C beryllium. The granulomatous lung response was reported to be similar to that observed in humans, but the responses appeared to resolve within a year after the single treatment.
In a followup to that study, Haley et al. (1992) exposed the same dogs to the same forms of beryllium oxide 2.5 years after the first exposure to achieve lung burdens of 17 or 50 μg/kg. Lung pathologic effects, particle clearance, and immune sensitization of peripheral blood leukocytes were monitored. Beryllium-induced proliferation of blood lymphocytes was noted from day 30. Inconsistent results were observed with lung lymphocytes cultured with bovine serum, but when cells were cultured with dog serum, increases in blood and lung lymphocytes were observed. The authors concluded that “[beryllium]-induced granulomatous and fibrotic lung lesions are accompanied by [beryllium]-specific immune responses within the lung but these changes do not appear to be cumulative if enough time has elapsed between exposures” (p. 400).
Haley et al. (1990) studied the acute toxicity of beryllium metal after a single nose-only exposure of F344 rats (at 800 μg/m3 for 50 min). Rats developed acute, necrotizing, hemorrhagic, exudative pneumonitis and intra-alveolar fibrosis that peaked on day 14. BAL fluid had increased numbers of inflammatory cells and enzyme concentrations. The authors concluded that human CBD is “an immunologically mediated granulomatous lung disease, whereas beryllium-induced lung lesions in rats appear to be due to direct chemical toxicity and foreign-body-type reactions” (p. 767).
Finch et al. (1994) studied the acute and chronic effects of beryllium metal administered nose-only to F344 rats to achieve lung burdens of 0.32-100 μg. Sacrifices were performed periodically for up to a year after exposure. The lowest lung burden of beryllium that induced pulmonary toxicity (inflammation and alveolar epithelial hyperplasia) was 1.8 μg. At burdens of 10 and 100 μg, particle clearance from the lung was reduced, and pulmonary inflammation was observed. Lung lesions (fibrosis, chronic inflammation, and epithelial hyperplasia) were evident in the 100-μg group after 8 days of exposure. BAL fluid from rats with histologic alterations had general increases in total numbers of cells, neutrophils, proteins, and enzymes.
Mouse models of beryllium-induced pulmonary granuloma were investigated by Huang et al. (1992). A/J mice were immunized with three subcutaneous injections of 5-50 μg of beryllium sulfate in syngeneic serum, bovine serum albumin, or Freund’s adjuvant and then intratracheally challenged with 1-5 μg of beryllium sulfate. Granulomas were found only in mice treated with beryllium sulfate in syngeneic serum. Microgranulomas were observed after 4 weeks, and granulomatous lesions and perivascular lymphoid accumulations were seen after 8 weeks. However, those lesions regressed within 20 weeks. Inflammatory cells, especially Mac-1-positive macrophages, were increased in the BAL fluid. T cells mediating delayed hypersensitivity were also detected after 1-8 weeks. In vitro evidence of BeS was found only in mice sensitized with beryllium sulfate in serum. Similar experiments with beryllium sulfate in BALB/c and C57BL/6 mice did not produce any lung granulomas, nor were granulomas induced in nonimmunized mice treated with a single intratracheal instillation of beryllium oxide.
Haley et al. (1994) conducted studies in cynomolgus monkeys given beryllium oxide (calcined at 500°C) or beryllium metal by bronchoscopic instillation. Lymphocytes were increased in the BAL fluid after 14, 30, or 90 days in monkeys treated with beryllium metal and after 60 days in monkeys treated with beryllium oxide. BAL lymphocytes from monkeys exposed to beryllium metal, but not to beryllium oxide, responded positively in the BeLPT. The lungs of monkeys treated with beryllium metal showed inflammation, interstitial fibrosis, and type II cell hyperplasia. Some also had discrete immune granulomas. Lesions were found less frequently and were less severe in monkeys treated with beryllium oxide.
Nikula et al. (1997) demonstrated chronic granulomatous pneumonia and lymphocytic responses induced in A/J and C3H/HeJ mice by inhalation of beryllium metal (at 1,030 mg/m3 for 90 min). Granulomas, epithelial hyperplasia, and inflammatory cells were detected in the lungs of both strains of mice at 28 weeks. T-cell proliferation responses in the spleen, lymph nodes, and peripheral blood evaluated in vitro did not differ between beryllium-treated and control mice. There was an increase in CD4+ cells in the lungs of treated mice. The authors suggested that their model of CBD was associated with T-cell delayed hypersensitivity and not a foreign-body reaction that is seen in rats.
Pfeifer et al. (1994) compared the histopathologic findings of sarcoidosis and berylliosis in F1 mice (C57BL/6 × DBA/2) given intraperitoneal injections of beryllium sulfate at 3 mg/kg. There was an increase in the formation of reactive oxygen intermediates by murine peritoneal exudate cells and a decrease in T-cell responses to concanavalin A by spleen cells. The authors concluded that although no granulomas were detected, there were similarities between sarcoidosis and beryllium disease in that macrophages were activated in the peritoneum and there was systemic immunosuppression.
Finch et al. (1998a) exposed C3H/HeJ mice to beryllium-metal aerosols to achieve lung burdens of 1.7-34 μg. Particle clearance was impaired at 12 and 34 μg through day 196. Increased numbers of inflammatory cells and enzyme concentrations were detected in the BAL fluid of mice with the two highest lung burdens (12 and 34 μg). Granulomatous pneumonia was seen histologically beginning on day 8 in the high-dose groups and on day 15 in the 2.6-μg group.
Benson et al. (2000) performed biodistribution studies in C3H/HeJ mice given particles of beryllium metal or beryllium-copper alloy (2% beryllium, 98% copper) intratracheally. The alloy was given at 12.5, 25, or 100 μg, and beryllium metal was given at 2 or 8 μg. That acute lung toxicity and death were associated with the alloy but not the metallic beryllium powder suggested copper toxicity. Pulmonary clearance of beryllium was found to be much slower than clearance of copper.
Because mice do not have susceptibility alleles equivalent to those found in humans, new knock-in mouse models with human alleles associated with a range of BeS/CBD risk are being developed that may be useful in experimental study of beryllium dose-response, beryllium type and characteristics conferring risk, dose rate, and therapeutic approaches to beryllium disease.
SUMMARY
Historically, CBD is the noncancer health end point on which occupational exposure limits are based. The epidemiologic evidence shows that the long-standing limit of 2 μg/m3 is inadequate for preventing CBD. The studies have also shown that the risk of CBD in workers depends on the industry, process, and physicochemical form of beryllium being handled. In general, BeS should be regarded as an early marker of disease that is likely to progress to CBD, although the timing and probability of progression are not well-defined. There is growing evidence that skin exposure may be an important contributor to sensitization and development of CBD.
The use of the BeLPT and worker surveillance programs now allow earlier identification of people who are sensitized and who are at risk of CBD. It is clear from animal and human data that susceptibility to CBD has a genetic component and, as noted in Chapter 2, the physiochemical properties of the beryllium and the route of exposure also play a role.
There are currently no adequate animal models of CBD. However, efforts are under way to create mouse models with human alleles associated with a range of BeS and CBD risk that may be useful in experimental study of beryllium dose-response, beryllium type and characteristics conferring risk, dose rate, and therapeutic approaches to beryllium diseases.
In its second report, the committee will evaluate critical health end points on which to base chronic inhalation exposure levels, and consider how susceptibility to CBD should be factored into a risk assessment. The committee will also discuss aspects of the use of the BeLPT in routine surveillance and medical monitoring, including the value of the BeLPT in predicting CBD, protocols for further followup tests after a positive BeLPT result, the likelihood of developing CBD after a true positive test, and a standardized method for achieving consistent test results in different laboratories.




























