3
Needs of the Most Vulnerable Adolescents
While the committee is concerned with the needs of all adolescents and with broad policy questions about the delivery of care, the two workshops examined the challenges in care for the most vulnerable groups. Developmental and social needs affect the delivery of health care for any adolescent, and they are of special importance for the care of the most vulnerable adolescents. The workshop presenters highlighted gaps in care for vulnerable adolescents that are of a different order from those that affect young people who are less vulnerable or disadvantaged. Adolescents whose life circumstances are seriously disadvantaged may go years without seeing a doctor, may have serious and multiple untreated physical or mental illnesses, or may live without necessary vaccinations, preventive reproductive, dental, and other care, for example. Moreover, they often need support that bridges the divide between health and social services, if they live in a severely dysfunctional family, are homeless or physically neglected, or for a variety of other reasons.
In planning the community forum, which focused on the experiences of the most vulnerable groups, the committee members faced a dilemma. While they were eager to hear from a variety of adolescents about their experiences, there was time available to hear from only a handful of individuals. Asking any individual to speak on behalf of large numbers of others facing similar circumstances is problematic, and the very young people who are most affected by difficult circumstances—as well as younger adolescents who already may have the least voice in their own
care—may be the least likely to be willing to speak at a public community forum hosted by the National Academies. At the same time, hearing the accounts of adolescents who have themselves experienced the kinds of disadvantage that seriously compromise health care, though anecdotal, was essential to the committee’s goals.
Fortunately, the committee was able to identify several young people, as well as some adults who work directly with disadvantaged adolescents, who provided thoughtful and compelling descriptions of what they have experienced and observed. Their observations provided insights into complex issues that the committee could pursue.
Matthew Morton, who at the age of 22 is the vice chair of the National Council on Youth Policy of the National Network for Youth, described for the audience the most pressing issues he sees facing three groups of adolescents: those in foster care, those in the juvenile justice system, and those who have run away from home or are homeless. His views on the needs of these young people have been shaped by his own childhood, during which he was orphaned and cared for, as he explained, “in a home marked by alcoholism, cocaine addiction, neglect, and occasional police visits.” Shawn Denise Semelsberger, who spent many years in foster care and serves on the board of directors of a crisis intervention center, followed up on Morton’s presentation with her observations about issues that affect adolescents in foster care. Paul Fogle, a college senior who is also a member of the board of the National Youth Leadership Network and has lived with a disability all his life, reflected on particular challenges in providing care for adolescents with disabilities.1
In addition, three adults with many years of experience working with vulnerable people offered their perspectives on providing health care to adolescents who live in the U.S.-Mexico border areas (Salvador Balcorta), unattached or homeless adolescents (Alan Shapiro), and low-income adolescents (Coleen DeFlorimonte). The information provided by these presenters was supplemented by the findings discussed by researchers Abigail English, Robert Garofalo, Kimberly Hoagwood, and Constance Weisner at the research workshop.
ADOLESCENTS IN FOSTER CARE
In 2005 there were nearly 227,000 adolescents (age 12 and older) residing in foster care (U.S. Department of Health and Human Services,
2006).2 Morton explained that the health status of these young people is frequently compromised by such problems as mental disorders, chronic medical conditions that are not properly managed, substance abuse, risky sexual behavior, abuse, and malnutrition (English, Stinnett, and Dunn-Georgiou, 2006). Abigail English described their health care needs, which include comprehensive health assessments, dental care, family planning and prenatal care, mental health services, treatment for substance use and abuse, and oversight of the coordination of the care they receive.
While adolescents in foster care families are generally eligible for Medicaid, they nevertheless often receive inadequate preventive care, oral and mental health services, and treatment for substance abuse.3 Moreover, as adolescents age out of foster care, they often find themselves with no health coverage at all, even though states do have the option of extending Medicaid coverage for them during the period of transition from care to self-sufficient adulthood. The federal Administration for Children and Families has estimated that more than 65,000 adolescents age 16 and older left foster care in 2005, only about 25,000 of whom were ready for complete emancipation (Administration for Children and Families, 2005).
Shawn Denise Semelsberger provided a firsthand account of how difficult it can be for young people to navigate the system of health care services. Now 21 years old and an advocate for adolescents in foster care, Semelsberger has been in foster care herself and has only recently been responsible for negotiating her health care and Medicaid coverage entirely on her own. Her account of a frustrating and confusing process of supplying documentation, filling out forms, resubmitting an application that had been lost by administrators, and interacting with an array of individuals who often gave her conflicting information about her eligibility demonstrated the challenges adolescents can face as they make the transition out of foster care. She pointed out that the obstacles to obtaining coverage and care to which they are entitled could overwhelm many adolescents. Many more face gaps in coverage because they earn slightly more than the cutoff for Medicaid eligibility but are not covered by employers and cannot afford the alternatives available through community colleges or other sources.
ADOLESCENTS IN THE JUVENILE JUSTICE SYSTEM
In 2003, 2.2 million adolescents under age 18 were arrested, and in that year 97,000 were held in juvenile residential facilities, according to figures supplied by Morton (Office of Juvenile Justice and Delinquency Prevention, 2006). English supplemented this description, noting that that minorities and low-income adolescents are overrepresented in this group. These adolescents have the same range of health needs as any other group—as well as a high rate of problems with mental health and substance abuse—but two factors limit their access to care. First, the care they receive through the juvenile justice system is often inadequate. Morton cited as one example a finding that the 5,000 adolescents who pass through the juvenile justice system in New York City annually are cared for by one full-time doctor and a staff of mostly part-time physician assistants and nurses (von Zeilbauer, 2005).
Second, states have the option to suspend adolescent’s health coverage under Medicaid when they enter the juvenile justice system because they do not receive federal financial assistance for adolescents in these circumstances. Where Medicaid coverage has been terminated, it can be very difficult for young people to reactivate their coverage once they leave the juvenile justice system. Moreover, Morton explained, many juvenile justice systems do little to help adolescents reactivate their coverage or make other connections with the social services that can help them address their health and emotional problems once they leave the system.
RUNAWAY AND HOMELESS ADOLESCENTS
Perhaps the group of adolescents most disconnected from services and support consists of those who run away from home or are homeless for other reasons, as explained by both Morton and Alan Shapiro, a physician who works in a Community Pediatric Program run by the Children’s Hospital at Montefiore in the Bronx borough of New York City. According to the Centers for Disease Control and Prevention (CDC), some 1.6 million adolescents run away or become homeless every year in the United States (Robertson and Toro, 1999), and 68 percent of this group are young people ages 15 to 17. Counting these adolescents is difficult, as English noted, in part because the definitions of both adolescent and homelessness are not precise, and also because these populations are often in transition. And the primary sources for counts of homeless adolescents are providers of services, so homeless adolescents who do not receive services are not included. Morton also noted that the absence of more recent counts of this population is indicative of the extent to which this group is overlooked.
Programs exist around the country to provide emergency shelter as well as social and medical services for these adolescents. However, they
are not sufficient to locate and serve the numbers of adolescents who need them. These young people may lack health insurance and a stable home (and thus medical records and parental permission for treatment), and they often lack access to any health care at all, despite their particular vulnerability to health problems associated with life on the street, such as substance abuse and sexually transmitted diseases. The health of homeless adolescents with chronic medical conditions, such as diabetes or positive HIV status, is at particular risk because it is very difficult for them to take critical medications regularly.
As one report on homeless adolescents has shown, these adolescents often must choose from “a short list of survival strategies,” such as gang membership, drug sales, or paid sex, which have serious health consequences (New York City Association of Homeless and Street-Involved Youth Organizations, 2005). Their health is often further compromised by inadequate sleep, poor nutrition, and exposure to the elements.
Shapiro illustrated these points with a snapshot of five patients—all homeless—whom he had recently treated: a young woman who was diabetic; a 19-year-old who is addicted to cocaine, has been diagnosed with bipolar disease, and engages in “survival sex”; an HIV-positive gay young man; an 18-year-old mother who brought her infant in for a checkup; and a young woman who had recently emigrated from Central America who had been abused and is battling alcoholism and depression. While shockingly sad, these cases are typical of those who seek care from the center at which Shapiro works—and, he suggested, countless others around the country.
Shapiro presented a diagram to illustrate his view of both the most common reasons why adolescents end up homeless or “throwaway” and the factors that place them at increased risk (see Figure 3-1). He distinguishes intrinsic problems—the most significant of which is the family—from extrinsic causes. Not only are these adolescents mostly from impoverished families, but they are also extremely likely to have been physically, sexually, or emotionally abused. Parental neglect or rejection—because of intolerance of homosexuality or teen pregnancy or just because of family dysfunction—is a frequent factor. The foster care and juvenile justice systems are extrinsic factors, in that young people who are in trouble often encounter even worse problems with the systems that are intended to help them.
Given the combinations of problems these adolescents face, they are frequently drawn to such programs as the one Shapiro described, viewing them as a kind of home. He noted that many young people tend to return regularly even when they have no medical needs because “we are their parents, we are their relatives.” His broader point was that almost any health problem and clinical outcome one might examine looks worse for
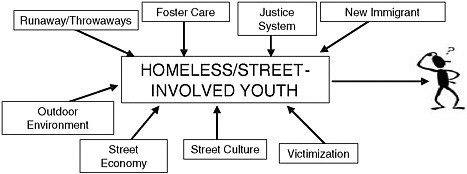
FIGURE 3-1 Factors contributing to and fostering homelessness and street involvement in youth.
SOURCE: From presentation by Alan Shapiro at A National Community Forum on Adolescent Health Care, Nov. 6, 2006.
homeless adolescents than for others. Preventing homelessness would be the best way to improve health outcomes for these adolescents, regardless of any other factor.
Short of eliminating homelessness, Shapiro had a number of specific recommendations for improving care to this population:
-
Insurance eligibility should be expanded to cover 21- to 24-year-olds. Enrollment should be easier—the required procedures should reflect the realities of homeless life.
-
Mental health and substance abuse services for adolescents should be significantly expanded.
-
Interagency task forces should provide oversight and coordination—so that components of the system, such as justice system discharge programs, supported independent living, and aftercare safety nets, can work together to meet adolescents’ needs.
LOW-INCOME ADOLESCENTS
Poverty, a factor that can exacerbate other problems that adolescents may face, is also a challenging circumstance on its own that often limits access to high-quality health care. Coleen DeFlorimonte, a pediatric nurse practitioner with the Woodson Adolescent Wellness Center in Washington, DC, described the needs she sees in a group whose primary shared characteristic is poverty. Run jointly by the District of Columbia Department of Health, the Maternal and Family Health Administration, and the DC public school system, the Woodson program provides comprehensive
health care, dental care, pregnancy prevention, and health education to adolescents. Housed in a public high school, the program depends for its success on a close relationship with the school’s administrators.
The population at Woodson Senior High School is disadvantaged: 65 percent are eligible for free or reduced price lunch. Tests scores are low, and the dropout rate is high. Nearly 500 students (out of 561 who are eligible) visited the clinic one or more times in the past year for health problems, and another 244 visits involved mental health problems. Among the most common services requested at the clinic are required vaccinations, sports physicals, treatment for sexually transmitted diseases, HIV counseling, contraceptive management, laboratory testing for such diseases as sickle cell anemia, and dental services. The clinic finds itself not only providing basic primary care services but also addressing problems, particularly violence, which are especially prevalent in large urban areas.
DeFlorimonte identified two principal challenges in the care available to these young people. First, the programs themselves often struggle financially. As Shapiro also noted, they bring in almost no revenue and are dependent on external funding from a combination of sources, although they face the same costs—for laboratory tests and medications, for example—that other kinds of medical facilities do. There are not enough such programs, and existing ones often have insufficient staff and resources for all the needs they see in the communities they serve. Second, the staff in many programs struggle to forge relationships with some of the adolescents most in need of their services. DeFlorimonte would like to see young people more involved in planning and running these programs so that they can more easily reach this challenged population. This may be particularly important because, in her experience, it is very difficult to engage the parents of adolescents in their children’s medical care.
ADOLESCENTS WITH DISABILITIES
A group that faces many of the challenges related to health care already described, as well as some additional ones, is adolescents with disabilities, including learning disabilities, speech and language impairments, and a host of other physical and mental impairments. Paul Fogle offered some perspective on their needs. His involvement with the National Youth Leadership Network—a group that works to develop leadership skills in adolescents with disabilities—as well as his comments at the community forum were shaped by his own experiences growing up with a congenital neurological malformation that has required ongoing medical attention.
From Fogle’s perspective, two critical concerns face adolescents with disabilities. First, these young people need support in learning to take responsibility for their own care and decisions about their care at early
ages, to prepare them to take over this responsibility to the extent that they can when they reach adulthood. Making this happen entails both education, to help adolescents fully understand the nature of their disabilities and the challenges they are likely to face, and opportunities for guided decision making as they get older. Fogle observed that many doctors he has seen addressed themselves solely to his parents, as if he were not present.
Second, adolescents with disabilities often face very significant problems with continuity of health coverage, especially as they reach the ages of 18 or 21 and are no longer eligible for coverage under their parents’ policies or other coverage available to minors. Many young people end up institutionalized, he observed, even though they could live independently with the right supports, because the coverage they have is not sufficiently flexible to encompass alternative arrangements. Finally, transportation can be a significant obstacle for those with disabilities, and families may not be in a position to provide all that is needed. For adolescents who want to be as independent as possible and are otherwise able to do so, this obstacle exacerbates difficulties they have in coordinating care from multiple providers.
ADOLESCENTS WITH MENTAL ILLNESS
Mental health and substance use disorders are prevalent among adolescents in the United States, as Kimberly Hoagwood (Columbia University) explained. Looking just at the prevalence rates of several of the most common mental disorders in school-age children and adolescents demonstrates how many young people are affected: depression/bipolar disorder, 7.8 percent; anxiety, 8.0 percent; disruptive disorders, 5.6 percent, attention deficit hyperactivity disorder, 5.0 percent; substance use disorders, 7.7 percent, and autism/pervasive developmental disorder, 0.5 percent (Office of the Surgeon General, 1999). A significant body of research has explored the efficacy of various treatments for these and other common mental disorders of adolescence. Meta-analyses of the effects of psychosocial treatments, hundreds of clinical trials on the safety and efficacy of psychotropic medications for adolescents, and other work offer some clear guidelines for the treatment of adolescents (selected examples of meta-analyses are Burns and Hoagwood, 2002; Burns, Hoagwood, and Mrazek, 1999; U.S. Public Health Service, 1999; Weisz, 2004).
Despite this research, adolescents with these conditions are not, by and large, receiving the care they need. Hoagwood described a system in which standards for effective care have been developed almost completely in isolation from models for delivering care. The result of this situation is that effective treatments for most disorders are not supported by
the structures through which mental health care is delivered. For example, nonspecialty sectors, including schools, primary care, child welfare, and juvenile justice, are the default system for adolescents with mental health needs, but they are not set up to identify and meet these needs.
Adolescents tend to receive their health care in multiple and nonspecialist settings, with little coordination among providers, Hoagwood explained. Young people and their families must patch together services available to them from various sources. Factors such as distrust for professionals, concerns about losing custody, and the experience of blame for serious problems may discourage families from taking advantage of services that are available. Psychotherapeutic treatments (communication sessions between a patient and a trained therapist) that have been found to be effective at improving outcomes in research settings have proved far less effective when offered in routine clinical settings (Weisz et al., 1995). While information about evidence-based treatments is often disseminated rapidly among practitioners, the process is not systematic. Some states have focused on ensuring that adolescents receive the mental health care that has been demonstrated to be most effective—Hoagwood cited 12 states that have worked to implement this goal.4 In others, the care may be haphazard. Given that situation, she observed that recent efforts in schools, primary care settings, home-based services, and family-based services may offer the most promise for implementing research-based practice with adolescents. Studying models and adopting strategies for delivering specific therapies in particular settings to certain populations of adolescents may help make treatments more effective in a clinical setting. Such policies as incentives that promote the monitoring of outcomes for patients and wider dissemination of new treatments (some of which involves proprietary material) could also be effective in the implementation of evidence-based practices in clinical settings.
ADOLESCENTS WITH SUBSTANCE USE DISORDERS
Adolescents with substance use disorders face multiple challenges in getting the care they need. Most insurance plans lack coverage for substance use disorders. Even in the minority of cases in which mental health coverage is otherwise adequate, substance use disorders are often not covered. Moreover, as Constance Weisner (University of California, San Francisco) explained, adolescents tend not to seek treatment of these disorders until they become severe and more difficult to treat than if the patient had been evaluated at an earlier stage.
Substance use disorders have a big impact on long-term health for adolescents. Young people in alcohol and drug treatment have significantly higher prevalence of a variety of medical conditions, including asthma, injuries, sleep disorders, pain conditions (e.g., headaches, arthritis, back and neck pain), and sexually transmitted diseases. They also have higher rates of other mental health problems, such as depression, anxiety disorder, eating disorders, and conduct disorders. They are more likely than other adolescents to engage in high-risk behaviors, such as injecting drugs and sharing needles, and unprotected and other risky sexual behavior.
Many factors may prevent adolescents with substance use problems from being identified, diagnosed, or treated. Fear of stigma and embarrassment may prevent them and their parents from seeking care, and they may not be certain where they should go for care. Diagnosis can also be subjective. Practitioners, however, miss opportunities to screen and identify adolescents with these problems, Weisner pointed out. One study of adolescents who ultimately were treated for chemical dependence found that 90 percent of them had a primary care visit in the 24 months prior to entering treatment without recognition of the disorder, and over half of the young people had a visit within the previous 3 months. Half had a visit with a psychiatrist within the 24-month period, and a third had one within 3 months prior to beginning their treatment. Smaller but still significant numbers made emergency room visits—all of these were missed opportunities to address a significant health problem (Sterling et al., 2004).
Although screening for risky behaviors in primary care settings is recommended by the American Medical Association, the American Academy of Pediatrics, and the Institute of Medicine (see for example, the description of one such tool in Box 3-1, the CRAFFT screening test for adolescent substance abuse), Weisner reported that relatively few providers do so. Among the reasons they give for not screening their patients are time constraints, concerns about confidentiality, lack of awareness of resources for patients, and lack of awareness of effective treatments (see Box 3-1).
Once problems are identified, a range of treatments is available, which have been the subject of a significant body of research. While many research questions remain—about the comparative effectiveness of different programs, for example—Weisner made clear that practitioners have many evidence-based options (selected research: Dasinger, Shane, and Martinovich, 2004; Deas and Thomas, 2001; Liddle and Dakof, 1995; Liddle et al., 2004; Waldron and Kaminer, 2004; Winters, 1999). Key elements of effective treatment that have emerged from this research include assessment and monitoring; a comprehensive, integrated approach; family involvement; developmental appropriateness; and continuing care.
|
BOX 3-1 CRAFFT: A Brief Screening Test for Adolescent Substance Abuse C Have you ever ridden in a CAR driven by someone (including yourself) who was “high” or had been using alcohol or drugs? R Do you ever use alcohol or drugs to RELAX, feel better about yourself, or fit in? A Do you ever use alcohol or drugs while you are by yourself, ALONE? F Do your family or FRIENDS ever tell you that you should cut down on your drinking or drug use? F Do you ever FORGET things you did while using alcohol or drugs? T Have you gotten into TROUBLE while you were using alcohol or drugs? SOURCE: Knight et al. (2002). |
This last point is especially important, in Weisner’s view, because while many programs are effective in the short term, these disorders are likely to recur and patients need long-term monitoring and follow-up for chronic conditions.
Weisner suggested modeling a system that effectively addresses substance use problems as one in which clinicians:
-
make use of effective links among primary care, specialty care, and community agencies to offer all available resources to patients;
-
use illness self-management practices;
-
screen for all comorbid conditions;
-
routinely ask patients and families for permission to share clinical information with other providers; and
-
make use of evidence-based care and coordination.
She further recommended that health plans cover screening and care for these disorders and support the coordination of information and care, perhaps using electronic record-keeping.
LESBIAN, GAY, BISEXUAL, TRANSGENDER, OR QUESTIONING ADOLESCENTS
One group that is often overlooked in the design of health care services is the estimated three to eight percent of the adolescent population
who are lesbian, gay, bisexual, transgender, or questioning their sexual orientation, or LGBTQ, as Robert Garofalo (Children’s Memorial Hospital) explained. While these adolescents are found in all communities and types of medical practices, they are not a homogeneous group and only limited research is available on their health status and health care needs. What is available is a significant body of data on risk behaviors, especially among urban young men, related to HIV infection and AIDS. However, because few groups of clinicians have a special interest in adolescents, and perhaps also because of stigma sometimes associated with these issues, very few data have been collected about young women or about transgender, bisexual, and questioning adolescents.5
LGBTQ adolescents have a disproportionate risk of health problems related to risk behaviors, including suicide attempts, drug use, and high-risk sexual behaviors, as well as a high rate of nonmedical problems, such as school truancy and dropout that can contribute to high-risk choices (Garofalo, et al., 1998). They also are more likely to engage in multiple risk behaviors than are other adolescents. Their care is complicated both by a lack of training for practitioners and by the discomfort they may have with revealing their sexual identity, particularly in the presence of their parents. Garofalo advocated an approach to their care that focuses less on their risk factors or their feelings about disclosing their sexual identity and more on the strengths they are likely to have, such as pride, self-determination, and resilience.
He described the Broadway Youth Center in Chicago, a program opened in 2004 by the Howard Brown Health Center, which serves LGBTQ adults, to focus on the needs of LGBTQ and homeless adolescents. The center serves between 4,000 and 5,000 adolescents per year and offers comprehensive services, including housing assistance; case management; medical care and counseling; food, showers, and laundry; general education development and job training; and mentorship. The program has successfully engaged many adolescents, and Garofalo expressed the hope that the stigma experienced by these young people will decrease and that training for practitioners around these issues will improve so that these adolescents can get the care they need in any health care setting. Significant work remains to be done—Garofalo cited a 1998 study of pediatricians in the Washington, DC, area, showing that these practitioners had many misconceptions about LGBTQ adolescents and had reservations about raising the issue (East and El Rayess, 1998). A total of 68 percent
reported that they did not raise questions about sexual orientation in taking medical histories. A big step forward, Garofalo added, would be the inclusion of questions about sexual identity in large-scale surveys, as well as other research on adolescents in this group.
ADOLESCENTS WHO LIVE IN U.S.-MEXICO BORDER COMMUNITIES
Salvador Balcorta, a social worker and chief executive of the Centro de Salud Familiar La Fe, Inc., in El Paso, Texas, described the health care issues facing a group of adolescents in border communities, whose needs are not very familiar to many Americans. This group is much larger than many people may realize. The 6.7 million residents of border county areas make up 2.2 percent of the nation’s population. Of these residents, 1.8 million, or 27 percent, are under 18, which means that if the border region is compared with U.S. states, it ranks among those with the highest percentages of total population who are children and adolescents (Annie E. Casey Foundation, 2005).6
Balcorta spoke passionately as he sketched a portrait of life for the adolescents who live on the border, a group that includes not only Mexican Americans and immigrants from other Central American countries, but also legal and illegal residents. These adolescents are even less likely to complete high school than Hispanic students nationwide, for example, although Hispanics are already less likely to graduate than any other group (Annie E. Casey Foundation, 2005). Extreme poverty in the region, as well as an active drug trade, mean high rates of substance use for adolescents in border areas, and the influence of gangs is difficult for them to avoid.
These adolescents have a high rate of incarceration or residential placement, and 60 percent of those incarcerated come from low-income families. In addition, among those incarcerated at the Texas Youth Commission, 34 percent say they are members of a gang, 46 percent have a high need for drug treatment, 41 percent have severe mental health problems, and 36 percent have been abused or neglected (Texas Youth Commission, 2007).
There is also a high rate of adolescent pregnancy among the general border population. Texas has the highest rate of any state (15 versus 12 percent nationally), and the rate among border residents is even higher, 17 percent (Annie E. Casey Foundation, 2005). Border adolescents also tend to face this problem at very young ages—Balcorta has recently worked
with six girls who became pregnant the year they turned 12. There is also a high rate of suicide and other mental health problems, of obesity, and of HIV/AIDS among adolescents.
Despite these problems, border residents have inadequate health coverage. Balcorta explained that Texas, the home of the majority of border residents, has the highest rate of uninsured residents of any U.S. state (25.2 percent compared with 15.4 percent nationally), and that rate is even higher in the border counties (varying from 29 to 35 percent) (Angel et al., 2007). Texas also ranks very low among the states in the percentage of its low-income residents who are covered by Medicaid, and recent policy changes for the State Children’s Health Insurance Program (SCHIP) have made those benefits more difficult to obtain, resulting in a significant decrease in enrollment among border residents, particularly those with the lowest incomes (Angel, Bennett, and El Paso Diabetes Association, 2007; Center for Public Policy Priorities, 2006).
In addition, the border region ranks low among the states in numbers of health professionals per capita and in other health care resources. Adolescents living in this region face an inadequate supply of pediatricians, health care and social assistance facilities, hospital beds, emergency rooms, diagnostic labs, and other resources that are taken for granted in other settings. Indeed, Balcorta observed, the residents of the areas along the U.S.-Mexico border live in third world conditions. The deficits in health care for these adolescents begin with basic services that even very vulnerable groups in other parts of the country may take for granted.
OBSERVATIONS
Morton believes that many programs that serve disadvantaged adolescents fail to capitalize on the strengths that even highly stressed young people have. He argued that programs that serve vulnerable adolescents would do well to adopt the positive youth development approach, in which the focus is not the problems often associated with adolescence, but an intentional and strategic focus on the resilience and positive potential that most young people have. This approach is discussed more extensively in the National Research Council and Institute of Medicine (2002) report Community Programs to Promote Youth Development. Frequently, decisions are made for them and little attempt is made to engage them or encourage them to take responsibility for their own health and well-being.
A related point that Morton made is that health care and other supports look very fragmented from the adolescent’s vantage point. A problem in one area of life—mental, dental, or physical health, housing, or family relationships, for example—can impair any or all other aspects of daily living. However, the programs that offer support typically address
one area only and seldom can encompass the needs of an entire family. Services that are both coordinated and comprehensive could be far more effective in the long run. Moreover, Morton argued, if supports were better coordinated, adolescents could more easily navigate the system for themselves and feel empowered to take charge of their own health and health care.
Other participants echoed these points. Most shared the concern that programs do too little to encourage and support adolescents in taking charge of their own health care, regardless of the populations they serve. Most also made note of the critical importance of coordination among available services.
Morton also identified some concrete needs for mental health services, substance abuse treatment, and oral health care, some of which often are not covered by government-funded health plans. Moreover, adolescents who have little support and guidance from responsible adults tend to lack awareness of the need for and availability of these kinds of services. He summarized the principal holes in health care as follows:
-
Lack of health coverage—many adolescents live in uninsured families. Even young people who are eligible for Medicaid and SCHIP programs may have difficulty because they are transient, cannot follow up with appointments, or cannot obtain and manage complicated forms. They may be unaware of resources available to them and have inadequate documentation, or other paperwork. Young adults ages 18 to approximately 24 may be the most likely to lack coverage and services because they fall between the options available for children and those for adults.
-
Lack of services in rural areas—many vulnerable adolescents live in rural areas, and fewer programs are available to serve them in less populated areas.
-
Poor coordination—adolescents may need support from a variety of sources and are generally ill equipped to inform themselves about resources that are available in their communities. Moreover, coordination of care among providers requires navigation skills that adolescent patients may not have. While the recently passed Tom Osborne Federal Youth Coordination Act (P.L. 109-365, 2006) has drawn attention to the significant problems with coordination of services, particularly for young people in the juvenile justice system, the issue is far from resolved.
-
Lack of cultural sensitivity—a variety of factors may make adolescents at risk uncomfortable and even push them away from services they need. Programs that usually serve families and younger pediatric patients may alienate adolescents from
-
less stable situations, while those that serve adults and adolescents may seem unsafe or uncomfortable. The needs of lesbian, gay, and transgender adolescents are not always recognized or addressed.
-
Lack of parental consent—many states require the consent of a parent or guardian before health care services can be provided, but unaccompanied adolescents may not have anyone to provide that consent.
-
Lack of stability—adolescents who lack a stable home, especially those in foster care, may have difficulty taking medication consistently, receiving follow-up or reminder calls or letters from providers, or making and keeping appointments for preventive or follow-up care.
-
Lack of specialty care—while primary care can be available even to those who lack health insurance, access to specialized services—including mental health and substance abuse treatment, dental care, and other important kinds of care—is even more difficult. For example, while approximately 60 percent of children in out-of-home care have moderate to severe mental health problems, only one-third of them are receiving the care they need (Child Welfare League of America, 2006).
Discussion of these presentations provided some elaboration on several key points. With regard to challenges in mental health care, participants noted that adolescents who lack family supports may be less equipped to recognize a problem, to see it as a priority, or to understand the possibilities that exist for treatment and support. Participants identified the transition from adolescent care to adult care as a great stress for adolescents ages 19 to 21, especially for those who lose coverage under Medicaid. Continuous care for all kinds of services would be affected, for example, mental and dental services. Moreover, the stigma that is often associated with mental health problems can discourage adolescents from acknowledging and addressing a problem. With regard to dental health, participants noted a lack of utilization and lack of adolescent-friendly consistent services. By the same token, young people with disabilities may have difficulty accepting that they have a disability and embracing help that is available.
The young people who spoke all agreed that finding ways to reach and educate vulnerable adolescents, one by one, could make existing services far more effective. Relationships with caring adults who reach out to an individual adolescent may be the most promising way to provide that kind of guidance. Participants reflected on ways to build adolescent-centered interactions into the system, perhaps using training to help
those who work with vulnerable young people recognize, seek, and take advantage of unexpected opportunities to reach, educate, and support them. Adults who have the best opportunity to reach adolescents could have significant impact if they are aware of both the circumstances that are likely to affect adolescent health and available resources that may be outside their area of specialty. As DeFlorimonte noted, every positive interaction with an adolescent is a success story that paves the way for him or her to feel comfortable seeking help when the need arises.
Moreover, if care provided in different contexts could be better coordinated, so that providers had more insight into the histories of their patients or clients, they would be in a better position to recognize and address the full extent of their patients’ pressing needs. However, participants noted that hierarchies within and among the professions can work against coordination among programs and even against collaboration among colleagues. Both nurses and social workers, for example, may have relevant educational credentials and experience, yet informal protocol may inhibit a nurse or social worker from making recommendations to a physician or documenting key points. Because no single discipline has made health care for adolescents a central focus, and because coordinating and collaborating strategies are seldom incorporated into training or institutionalized in other ways, programs tend to struggle on their own with the resulting vacuum.
Shapiro pointed out that his mobile unit is well equipped to address this issue because the staff can deliver care precisely at the sites where adolescents are getting other services, such as food, shelter, or needle exchange. His ideal program would be a mobile team that includes social service, mental health, and medical personnel, all working together every day. Yet the needs are so broad that a mobile team that could truly address them all would be cumbersome. Legal and educational counseling, as well as nutrition counseling for obesity, are part of the picture as well, so interagency cooperation is critical.
At the same time, Balcorta and others stressed that funding is tight for attempting comprehensive service such as this, and that programs and communities cannot afford to be completely dependent on federal funding—they have to find ways to magnify the benefits of federal resources with local support.

















