Meeting the Unique Health Needs of Women and Children
Women’s health needs differ from those of men. Likewise, children are not simply miniature adults. A woman’s body differs critically from a man’s in both structure and function, and a child’s body doesn’t fully mimic an adult’s. Each group’s brain functions differently and responds in different ways to even the same stimuli. Each group often processes medications differently. And, of course, men, women, and children interact with the larger world and are affected by events in different ways.
Women and children have been labeled by some observers as the “unequal majority” in health and health care. Historically, the bulk of health studies have used adult men, with researchers and physicians left to infer how the studies apply to women and children. The conditions and needs of women and children, in large measure, have too frequently been set aside.
The Institute of Medicine (IOM) is working to ensure the health of the nation’s women and children by focusing on their respective circumstances, including subject areas drawn from biological, environmental, social, clinical, and legal realms, among others. Studies consider a range of diverse issues that directly affect the health of individuals and their families or affect social programs that, in turn, contribute to the well-being of large groups of people.
Improving women’s health during pregnancy
One question the IOM recently revisited is how much weight a pregnant woman should gain to protect both her health and the health of the developing fetus. Two decades ago, the IOM recommended guidelines, since
widely adopted, for weight gain during pregnancy. But more research has been conducted on this subject, and over the past 20 years, there have been dramatic changes nationally in the diversity and health status of women having babies. Notably, women now tend to be older when they become pregnant, and they tend to be heavier, often entering pregnancy overweight or obese. Such changes may carry added health risks.

The IOM, with support from a number of government agencies and private organizations, has reviewed this changed landscape. The resulting report, Weight Gain During Pregnancy: Reexamining the Guidelines (2009), offers a set of recommendations—and some specific tools—that, if fully implemented, represent an important change in the care provided to women of child-bearing age. The new guidelines consider not only the welfare of the infant, as the original guidelines did, but also the health of the mother.
Among its core findings, the report says that women should have a normal body mass index (a measure of body fat based on weight and
New Recommendations for Total and Rate of Weight Gain During Pregnancy, by Prepregnancy Body Mass Index (BMI)
|
Prepregnancy BMI |
Total Weight Gain |
Rates of Weight Gain* 2nd and 3rd Trimester |
||
|
Range in kg |
Range in lbs |
Mean (range) in kg/week |
Mean (range) in lbs/week |
|
|
Underweight (< 18.5 kg/m2) |
12.5–18 |
28–40 |
0.51 (0.44–0.58) |
1 (1–1.3) |
|
Normal-weight (18.5–24.9 kg/m2) |
11.5–16 |
25–35 |
0.42 (0.35–0.50) |
1 (0.8–1) |
|
Overweight (25.0–29.9 kg/m2) |
7–11.5 |
15–25 |
0.28 (0.23–0.33) |
0.6 (0.5–0.7) |
|
Obese (≥ 30.0 kg/m2) |
5–9 |
11–20 |
0.22 (0.17–0.27) |
0.5 (0.4–0.6) |
|
*Calculations assume a 0.5–2 kg (1.1–4.4 lbs) weight gain in the first trimester. SOURCE: Weight Gain During Pregnancy: Reexamining the Guidelines, p. 254. |
||||
height) when they become pregnant, and that they should gain weight during their pregnancy within a fairly narrow range, based on their age, race or ethnicity, and various other factors that may affect pregnancy outcomes. Meeting these guidelines will require women and their care providers to work together, starting before conception, with counseling efforts, often including planning for preconception weight loss.
Notably, women now tend to be older when they become pregnant, and they tend to be heavier, often entering pregnancy overweight or obese. Such changes may carry added health risks.
The report calls on federal agencies, private voluntary organizations, and medical and public health organizations to adopt the new guidelines and publicize them to their members and to women of childbearing age.
Reviewing federal family planning programs
Family planning is known to help women—as well as men—maintain their reproductive health, and it also enables women to avoid unintended pregnancies and plan for pregnancies. Collectively, such benefits contribute to the well-being of individuals, families, and broader society. Even so, many low-income individuals find it difficult to pay for these services, highlighting the critical role played by the Title X Family Planning Program, the nation’s only federal program, created in 1970, exclusively devoted to providing family planning services.

At the request of the Office of Family Planning, the agency within the U.S. Department of Health and Human Services (HHS) that administers the Title X Family Planning Program, the IOM conducted a comprehensive review of the program. The resulting report, A Review of the HHS Family Planning Program: Mission, Management, and Measurement of Results (2009), finds that the Title X program, in large measure, has successfully delivered critical services to those who have the most difficulty obtaining them. However, if the program is going to truly meet the needs of its targeted groups—low-income individuals and adolescents—several structural components need to be improved.
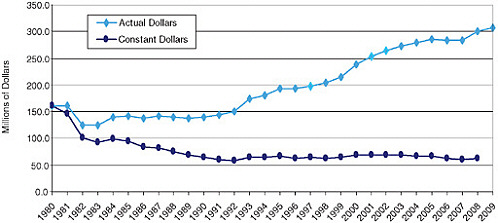
Estimated funding for Title X when adjusted for inflation, FY 1980–2009.
SOURCE: A Review of the HHS Family Planning Program: Mission, Management, and Measurement of Results, p. 111.
In particular, the Office of Family Planning lacks a clear process for establishing or revising program priorities and guidelines, and developing such a process is an important priority. The strategic plan must reflect the original mission of the Title X program and an understanding of its target population; incorporate lessons gained from the field of family planning and reproductive health; provide a vision for coordination, leadership, and evaluation; address the family planning needs of individuals over the full reproductive lifespan; and be firmly grounded in high-quality evidence.
Reducing depression’s grip on parents and children
Depression affects millions of U.S. adults over their lifetime, many of whom are parents with children. The burden of depression and the barriers to quality of care for depressed adults are increasingly well understood, but the ways in which depression affects parenting—and, in turn, children’s health and psychological functioning—are often ignored.
To illuminate this problem and identify solutions, the IOM and National Research Council convened a committee to consider the identification, prevention, and treatment of parental depression, along with its interaction with parenting practices, and its effects on children and fami-
lies. The resulting report, Depression in Parents, Parenting, and Children: Opportunities to Improve Identification, Treatment, and Prevention (2009), finds that parental depression is prevalent, but a comprehensive strategy to treat the depressed adults and to prevent problems in their children is absent.
The report concludes that national leadership, interagency collaboration, federal–state cooperation, and government collaboration with the private sector are needed to support the development and evaluation of a framework that integrates health, mental health, public health, and parenting in a life-course framework, from pregnancy through adolescence. Federal and state governments also should provide additional support for public and professional education, training, infrastructure development, and implementation efforts to improve the quality of services for affected families and vulnerable children. Likewise, more funding is needed for research, data collection, and evaluation efforts that might lead to improved prevention and treatment services for this population.
Improving adolescent health services
Nearly 42 million adolescents aged 10 to 19 live in the United States, and most of them are healthy. But all too frequently, young people engage in risky behavior, develop unhealthful habits, or have chronic conditions that can jeopardize both their immediate and long-term health and safety. The three leading causes of death in adolescents—motor vehicle crashes, homicide, and suicide—all are tied to risky and unhealthful behaviors. As well, adolescence is a critical period for developing positive habits and skills that create a strong foundation for healthful lifestyles and behavior over the full lifespan. Growing up without having developed these habits can be detrimental to an adult’s health and well-being.
The system should foster coordination between primary and specialty care, and it should enable primary care providers to more easily reach and follow adolescents through “safety net” settings such as hospitals and community health centers.
The U.S. health care system has a potentially key role in promoting adolescent health. But an IOM study, conducted with the National Research Council and funded by The Atlantic Philanthropies, finds that the system is failing in that role. The study report, Adolescent Health Services: Missing Opportunities (2009), says that services often
are fragmented and poorly coordinated across various settings, resulting in gaps in care in reaching all of the nation’s adolescents during this critical period. Many health services also are poorly equipped to meet the disease prevention, health promotion, and behavioral needs of adolescents, and many care providers lack the necessary skills to interact appropriately and effectively with this age group. Moreover, large numbers of adolescents are uninsured or have inadequate health insurance, and so are unable to access care, even where available.

As a blueprint for action, the report highlights critical health needs of adolescents, details promising models of health services, and identifies components of care that could strengthen and improve health services for adolescents and contribute to healthy adolescent development. Among specific steps, federal and state agencies, private foundations, and insurers should work together to develop a care system that improves services for all ado-
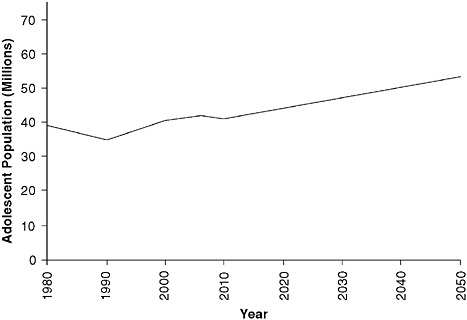
Growth in the adolescent population, aged 10 to 19, 1980–2006 and 2006–2050 (projected).
SOURCE: Adolescent Health Services: Missing Opportunities, p. 32.
lescents. The system should foster coordination between primary and specialty care, and it should enable primary care providers to more easily reach and follow adolescents through “safety net” settings such as hospitals and community health centers.
Training health professionals will be critical as well. At all levels of professional education, providers should receive comprehensive education about adolescents’ health problems and effective ways to treat their diseases and promote healthful behaviors. Furthermore, confidentiality should be protected for adolescents receiving care. They should give their own consent before receiving care and before their health information is shared with others, even their parents. Finally, the more than 5 million medically uninsured adolescents indicate a clear need for federal and state policy makers to develop strategies to ensure that all adolescents have comprehensive, continuous health insurance coverage.
Improving mental, emotional, and behavioral health among young people
Among the most dangerous risks to the health and well-being of young people are depression, conduct disorder, substance abuse, and similar disorders. They are as commonplace today as are fractured limbs—not inevitable, but not at all unusual—and they often carry over into adulthood. Almost one in five young people has such a disorder, or even multiple disorders, at any given time. Among adults, half of all mental, emotional, and behavioral disorders were first diagnosed by age 14 and three-fourths by age 24. In addition to their health toll, the disorders exact high economic and psychosocial costs, not only for the young people, but also for their families, schools, and communities. The price tag for treatment services and lost productivity runs an estimated $247 billion annually.
Among adults, half of all mental, emotional, and behavioral disorders were first diagnosed by age 14 and three-fourths by age 24.
The good news is that much is known about how to prevent these disorders before they occur. Risk factors are well established, preventive interventions are available, and the first symptoms typically precede a disorder by 2 to 4 years. Yet the nation’s health system approach largely has been to wait to act until a disorder is well established and has already done considerable harm. All too often, opportunities are missed to use evidence-based
approaches to prevent the occurrence of mental, emotional, or behavioral disorders; establish building blocks for healthy development in all young people; and limit the environmental exposures that increase risk—approaches likely to be far more cost effective in addressing such disorders in the long run.

To help in building a better health system, the National Research Council and the IOM recently reviewed the research on the prevention of mental disorders and substance abuse among young people. Preventing Mental, Emotional, and Behavioral Disorders Among Young People: Progress and Possibilities (2009) recommends a variety of strategies to improve the psychological and emotional well-being of this target population. The report updates a key 1994 IOM report, Reducing Risks for Mental Disorders, focusing special attention on the research and program experiences that have emerged since that time.
The report describes the value of a number of prevention strategies, including:
-
Strengthening families by targeting problems such as substance use or aggressive behavior; teaching effective parenting skills; improving communication; and helping families deal with disruptions (such as divorce) or adversities (such as parental mental illness or poverty).
-
Strengthening individuals by building resilience and skills and improving cognitive processes and behaviors.
-
Preventing specific disorders, such as anxiety or depression, by screening individuals at risk and offering cognitive training or other preventive interventions.
-
Promoting mental health in schools by offering support to children encountering serious stresses; modifying the school environment to promote healthful social behavior; developing students’ skills at decision making, self-awareness, and conducting relationships; and targeting violence, aggressive behavior, and substance use.
-
Promoting mental health in communities by supporting programs designed to foster healthful social behavior; teach coping skills; and target modifiable lifestyle factors, such as sleep, diet, activity and
-
physical fitness, exposure to sunshine and light, and television viewing, that can affect behavior and emotional health.
How best to capitalize on such strategies? Many providers and agencies are responsible for the care, protection, or support of young people: the child welfare, education, and juvenile justice systems, as well as medical and mental health care providers and community organizations. Yet resources within these agencies are scattered, not coordinated, and often do not effectively support prevention programs or policies. To stitch together such patchwork national leadership is necessary to make systematic prevention efforts a high priority in the health care system as well as an integral component of local, state, and federal programs that serve young people and families.
Prevalence Estimates of Mental, Emotional, and Behavioral Disorders in Young People
Among specific steps, the committee recommends that the White House develop an interdepartmental strategy that identifies specific prevention goals, directs multiple federal agency resources toward these goals, and provides guidance to state and local partners. In turn, governments at all levels should increase their investments in prevention and promotion, including setting aside resources for evidence-based prevention in mental health service programs and funding proven prevention approaches by school systems. Adequately funded state and local systems should craft partnerships among families, schools, courts, health care providers, and local programs to create coordinated approaches that support healthy development.
Public and private organizations also should increase efforts to beef up the professional workforce by fostering development of training programs and prevention standards across disciplines, including health, education, and social work. On a broader stage, a range of public and private organizations should join in promoting public education, making use of mass media and the Internet to share information about risk factors and available interventions, as well as to reduce the stigma often associated with mental, emotional, and behavioral disorders.
Assessing early childhood enrichment programs
In the nation’s increasing drive to improve young children’s education and development, a host of public and private organizations have developed programs to enhance the school readiness of all children, especially those from economically disadvantaged homes and communities, those with special needs, and those who learn English as a second language. These early childhood education and child care programs, such as Head Start, run by the HHS, are designed to enhance social, language, and academic skills, as well as to identify children with developmental problems so they can be given appropriate interventions.
At the same time, early childhood education and intervention programs are increasingly being asked to prove their worth. At the request of Congress, the National Research Council, with the assistance of the IOM and funding from HHS, considered how to identify important developmental outcomes of preschool children—from birth to age 5—and how best to assess them in preschools, child care settings, and other early childhood programs. The resulting report, Early Childhood Assessment: Why, What,
and How (2008), concludes that well-planned assessments can inform teaching and efforts to improve programs and can contribute to better outcomes for children. Poor assessments or misuse of the results, however, can harm both children and programs.
The report emphasizes the need to view assessment as part of a broader system of early childhood interventions. It offers a set of principles to guide the design, implementation, and use of assessments in early childhood settings. As an overarching rule, good assessments must be designed for specific purposes, and their aims should not be mixed. For example, the assessment of a program’s performance should not be used to judge the performance of an individual child. The purpose of any assessment should be made explicit and public in advance, and it should be conducted within a coherent system of health, educational, and family support services that promote optimal development for all children. System officials should provide clearly articulated standards for what children should learn and what constitutes a quality program.

The report also pays attention to the limits of assessments and their possible adverse effects. On the practical side, some types of assessments may make children feel anxious, incompetent, or bored, while other types may constitute a burden on adults. Assessments also cost money, and they may deflect time and resources from instruction. Therefore it is important to ensure that the value of the information gathered through assessments outweighs any negative effects on adults or children and that it merits the investment of resources. Assessments done improperly also can lead to bad high-stakes decisions, all of which should be considered seriously.
The report calls for future research to improve the quality and suitability of developmental assessment across a wide array of purposes. For example, some assessment measures have been tested only with populations that do not represent the diversity of children enrolled in today’s early childhood programs. Thus, care should be used in assessing the status or progress of young children with special needs and those for whom English is a second language, as many existing assessment tools have not demonstrated their validity for these groups.
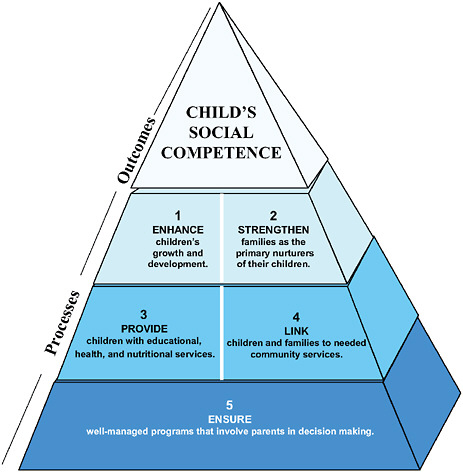
Head Start Program performance measures conceptual framework.
SOURCE: Early Childhood Assessment: Why, What, and How, p. 51.
Critiquing a national child health study research plan
As important as it is to evaluate children’s developmental programs, it is similarly important to monitor the impact of a child’s environment on his or her health. A variety of environmental influences are said to threaten children’s health. Some are well known and widely studied. For example, a child who was exposed as a fetus to certain compounds, including lead and alcohol, often experiences a range of serious health problems. But there is considerable uncertainty about the relationship of other environmental factors to what often appear to be growing health problems among
children, including asthma, autism, developmental disorders, obesity, and childhood cancers.
In response to both congressional and presidential initiatives, the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), in cooperation with several other federal agencies, is undertaking the National Children’s Study (NCS). The NCS will be the largest long-term study of environmental effects on children’s health ever conducted in the United States. It proposes to examine the effects of environmental influences on the health and development of approximately 100,000 children nationwide, following them from before birth until age 21. Data will be gathered on an array of measures of biological, chemical, physical, genetic, social, cultural, geographical, and other factors in a child’s environment that can affect health and development. The NCS proposes to examine many different exposures and establish—or rule out—relationships between them with many different outcomes. In archiving the data, the NCS is intended to provide a valuable resource for analyses conducted many years into the future.

But how should the study be done? At the request of NICHD, the National Research Council and the IOM studied the proposed research plan to assess its scientific rigor and the extent to which the NCS is being carried out with methods, measures, and collection of data and specimens to maximize scientific yields. The National Children’s Study Research Plan: A Review (2008) finds that overall, the NCS looks promising. As proposed, the resulting database should be valuable for investigating the various hypotheses about exposures and health effects described in the plan, as well as additional hypotheses that are likely to evolve as the study proceeds.
Among the plan’s strengths, it would provide enough statistical power to examine many hypothesized relations that cannot be investigated with smaller samples. The data, gathered prospectively over the entire course of pregnancy, childhood, adolescence, and early adulthood, will enable exploration of many new relations between exposures and outcomes. For example, data will be collected in women from before they conceive and during the early stages of gestation, a period when certain environmental
|
A New Definition of Children’s Health The report of the Committee on Evaluation of Children’s Health, Children’s Health, The Nation’s Wealth (National Research Council and Institute of Medicine, 2004), defines children’s health as follows: Children’s health is the extent to which individual children or groups of children are able or enabled to (a) develop and realize their potential, (b) satisfy their needs, and (c) develop the capacities that allow them to interact successfully with their biological, physical, and social environments. This definition draws upon an explanation from the World Health Organization that health is a state of complete physical, mental, and social well-being, not merely the absence of disease or infirmity; a collaborative effort of the European Union Health Monitoring Programme to develop the Child Health Indicators of Life and Development model; the positive health principles embraced by the Ottawa Charter for Health Promotion (1986); and the research literature cited in the report. Key features of the new definition of children’s health include three distinct but related domains:
|
exposures may prove to be critically important. Additionally, the array of measures to be documented will permit investigation of relationships that have not previously been studied.
But the NCS also has some important weaknesses and shortcomings that may diminish the study’s value. First, the study is being implemented without sufficient pilot testing. The study design is extremely complex in
The report describes these domains in detail and also describes ways to measure not only aspects of each domain, but also the influences on children’s health, which are defined to include:
SOURCE: The National Children’s Study Research Plan: A Review, p. 45. |
terms of identifying subjects, enlisting their enrollment and continued participation, administering the large number of survey and clinical instruments, and managing huge databases generated by disparate organizations. In addition, there are various technical questions concerning the kinds of measurement instruments to be used and the timing of their application. Such concerns could be addressed during an expanded pilot phase to great benefit.
Another potential trouble spot is the plan’s failure to prepare adequately for disclosure of risk to participants. As soon as data collection begins, the NCS will face questions about the circumstances under which information about a child’s health and development, as well as his or her exposure to toxic agents, should be conveyed to participants and their parents. The study calls for providing information on conditions that are “clinically relevant and actionable,” but this category needs to be better defined and made operational. Similarly, there is insufficient detail in the plan about how decisions will be made about what to disclose. Some of the decisions—for example, regarding transmitting information about fetal defects encountered through ultrasounds—urgently need to be made.
















