1
Introduction
In today’s public health world, the term “neglected disease” conjures up obscure tropical illnesses of little relevance to contemporary practice in the United States. Yet, when one considers the actual meaning of the words, the time may be right to add hypertension to this list. Hypertension, or high blood pressure, describes the condition in which systemic arterial blood pressure remains elevated over time. High blood pressure is caused primarily by an increase in the resistance to the flow of blood through arteries and an increase in cardiac output, which is a function of the heart rate and stroke volume. Hypertension is dangerous because it forces the heart to work harder and can contribute to atherosclerosis and hardening of the large arteries causing cardiovascular disease. These factors can also lead to subsequent blockage and weakening of the walls of the smaller cerebral arteries causing them to rupture and result in stroke. The lack of attention to hypertension is difficult to understand. Hypertension is one of the leading causes of preventable death in the United States. A recent study (Danaei et al., 2009) listed it at number two, just behind tobacco. Based on data from the Centers for Disease Control and Prevention (CDC) and the National Heart, Lung, and Blood Institute (NHLBI) from 1995 to 2005, the death rate from high blood pressure increased by 25.2 percent and the actual number of deaths rose by 56.4 percent (Lloyd-Jones et al., 2009). In 2005, high blood pressure was responsible for about one in six deaths of U.S. adults. Further, high blood pressure is the single largest risk factor for cardiovascular mortality accounting for about 45 percent of all cardiovascular deaths. High blood pressure was the leading cause of death among women, accounting for 19 percent of all female deaths, and the
second leading cause of death among men (second to smoking) (Lloyd-Jones et al., 2009). Hypertension is estimated to contribute to 35 percent of myocardial infarctions and strokes and 49 percent of episodes of heart failure (AHRQ, 2007).
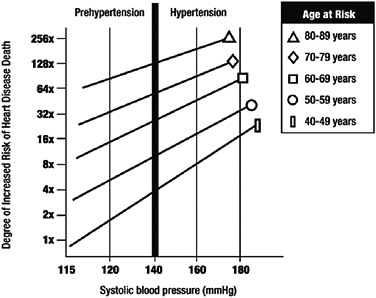
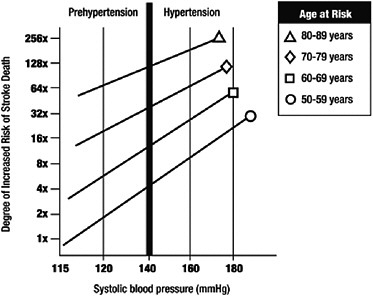
Hypertension is diagnosed by a simple test. Using a sphygmomanometer, blood pressure is typically measured at two points: at peak pressure when the heart is most contracted (this point is referred to as systolic blood pressure) and then when the heart is most relaxed (diastolic pressure). High blood pressure for adults is defined as a systolic pressure of 140 mm Hg or greater or a diastolic pressure of 90 mm Hg or greater or using antihypertensive medication. Using this definition, hypertension is highly prevalent; nearly one in three U.S. adults has hypertension (Fields et al., 2004; Lloyd-Jones et al., 2009). The risk of developing hypertension increases with age. In older age groups it is more common than not; based on data from the Framingham study, the lifetime risk of hypertension is estimated to be 90 percent for people with normal blood pressure at age 55 or 65 who live to be age 80-85, respectively (Cutler et al., 2007; Vasan et al., 2002). Approximately 73 million Americans have high blood pressure, and an additional 59 million have prehypertension, which is defined as blood pressure ranging from 120-139 mm Hg systolic and/or 80-89 mm Hg diastolic. Prehypertension is a new classification introduced by the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (Chobanian et al., 2003)1 because of the increasing amount of data associating cardiovascular complications with what had previously been considered normal blood pressure readings. Figure 1-1 shows the increased risk of heart disease death, and Figure 1-2 shows the increased risk of stroke death, associated with prehypertension and hypertension by decade of life. Starting at a systolic blood pressure of 115 mm Hg, every 20 mm Hg increase in systolic blood pressure is associated with a doubling in the risk of death from both heart disease and from stroke.
Hypertension is highly treatable, and a range of medications—some relatively inexpensive—are available. In the late 1950s and early 1960s, oral diuretics were primarily used to treat hypertension. Since then, additional medications including calcium channel blockers and beta-blockers, angiotensin-converting enzyme (ACE) inhibitors, and angiotensin receptor antagonists can be found among the antihypertensive therapies available
to physicians for managing high blood pressure. Studies comparing the effectiveness of antihypertensive therapies suggest that generally low-dose diuretics, which also tend to be lowest in cost,2 are the most effective first line of treatment for preventing mortality and morbidity from cardiovascular disease (ALLHAT, 2002; Psaty et al., 2002).
More importantly, hypertension is highly preventable through a decrease in obesity, increase in physical activity, and improved diet (particularly through reduced sodium and increases in fruit and vegetable consumption). Moreover, since poor diet, physical inactivity, and obesity appear to be on the increase, reductions in these risk factors takes on even greater importance.
Finally, hypertension is costly to the healthcare system. It is the most common primary diagnosis in America (Chobanian et al., 2003), and it contributes to the costs of cardiovascular disease (coronary heart disease, myocardial infarction) and stroke. The methodologies used to estimate the costs associated with hypertension vary; one estimate reports the total economic burden of coronary heart disease and stroke as $120.6 billion and $48.9 billion, respectively, in 2002 (Cutler et al., 2007). The American Heart Association (AHA) recently reported the direct and indirect costs specifically of high blood pressure as a primary diagnosis as $73.4 billion for 2009 (Lloyd-Jones et al., 2009). With respect to the cost of treating hypertension, an analysis by DeVol and Bedroussian (2007) estimated that the total expenditure for the population reporting hypertension as a condition in the Medical Expenditure Panel Survey (MEPS) was $32.5 billion in 2003. Another study estimated the total incremental annual direct expenditures for treating hypertension (the excess expenditure of treating patients with hypertension compared to patients without hypertension) to be about $55 billion in 2001 (Balu and Thomas, 2006). More specifically, it is estimated that a 10 percent decrease in annual health care visits for hypertension would save $450 million each year in health care costs (NHLBI, 2004b).
CDC EFFORTS TO REDUCE AND CONTROL HYPERTENSION
The CDC is the lead federal agency responsible for promoting health and quality of life by preventing and controlling disease, injury, and disability. The CDC Division for Heart Disease and Stroke Prevention (DHDSP) provides national leadership to reduce the burden of disease, disability,
and death from heart disease and stroke. DHDSP has six programmatic priority areas: (1) control high blood pressure, (2) control high cholesterol, (3) improve emergency response, (4) improve quality of care, (5) increase awareness of the signs and symptoms of heart attack and stroke and of the need to call 911, and (6) eliminate health disparities related to heart disease and stroke. The DHDSP carries out its programmatic responsibilities with a budget of $54 million for fiscal year 2009.
The DHDSP is co-lead, along with the NHLBI, for the Healthy People 2010 Focus Area 12 objectives related to heart disease and stroke including four objectives specific to hypertension (Table 1-1).
Findings from the Healthy People 2010 Midcourse Review (CDC, 2006) indicated that the nation was moving away from making progress in the target objectives as reflected by increases in the prevalence of high blood pressure among adults and among children and adolescents. This moving away from Healthy People 2010 goals provided an increased emphasis for a DHDSP programmatic focus on hypertension.
The DHDSP has developed a strategic plan to reduce and control hypertension that recognizes the urgent need to implement a number of effective practices and to develop new public health practices. The plan identifies a number of action areas and goals for the prevention and control of hypertension from which the most important priorities must be selected. These priorities must also take into consideration state health departments and other critical partners. The CDC requested assistance and guidance from the Institute of Medicine (IOM) to determine a small set of high-priority areas in which public health can focus its efforts to accelerate progress in hypertension reduction and control. Specifically, the CDC requested that
TABLE 1-1 Healthy People 2010 Focus Area 12: Heart and Stroke, Blood Pressure Objectives
|
Number |
Objective |
|
12-9. |
Reduce the proportion of adults with high blood pressure. |
|
12-10. |
Increase the proportion of adults with high blood pressure whose blood pressure is under control. |
|
12-11. |
Increase the proportion of adults with high blood pressure who are taking action (for example, losing weight, increasing physical activity, or reducing sodium intake) to help control their blood pressure. |
|
12-12. |
Increase the proportion of adults who have had their blood pressure measured within the preceding 2 years and can state whether their blood pressure was normal or high. |
|
SOURCE: CDC, 2006. |
|
the IOM convene an expert committee to review available public health strategies for reducing and controlling hypertension in the U.S. population, including both science-based and practice-based knowledge. In conducting its work, the committee was asked to consider the following questions:
What are the highest-priority action areas on which the CDC’s Division for Heart Disease and Stroke Prevention and other partners should focus near-term efforts in hypertension?
-
Identify the particular role of the CDC’s DHDSP in addressing the highest-priority areas.
-
Identify the role of state health departments in advancing progress in the priority action areas.
-
Identify the role of other public health partners.
-
What visible impacts can be expected if the DHDSP focuses its efforts in these priority areas?
-
What indicators should be monitored to assess the progress of the DHDSP, state health departments, and partners in implementing the committee’s recommendations?
-
What are the potential positive and negative impacts on health disparities that could result if the committee’s recommendations are implemented?
-
What indicators should be monitored related to health disparities to ensure the intended impact of the DHDSP priority action areas identified?
The committee was not expected to conduct a new, detailed review of peer-reviewed literature on hypertension because such literature reviews, meta-analyses, and syntheses already exist and have been used to inform existing guidelines and recommendations.
The report is organized into six chapters, including this introduction, which discusses the study process and the committee’s approach to questions it was asked to address. Chapter 2 provides a discussion of the public health importance of hypertension and an overview of hypertension trends in the United States. Chapter 3 provides an overview of the CDC’s Division for Heart Disease and Stroke Prevention and background information on its budget and activities. Chapters 4 and 5 provide the committee’s response to the task of identifying a small set of priority areas for the DHDSP in which public health can focus its efforts to accelerate progress in hypertension reduction and control. Specifically, Chapter 4 addresses priority areas for interventions that are directed at population-based risk factors that are known to increase the risk of hypertension in the general population. Chapter 5 addresses priority areas for interventions directed at individuals with hypertension. The recommendations in Chapters 4 and 5 are specifically
directed to the DHDSP. The committee recognizes that the DHDSP cannot work in isolation to implement the population-based policy and system change approach to prevent and control hypertension; thus, it notes when partnerships with other partners are appropriate (for example the business community, health care quality community, and the Centers for Medicare & Medicaid Services). The committee, however, views state and local health jurisdictions to be critical DHDSP partners. In Chapter 6, the committee specifically recommends the action steps state and local health jurisdictions can take to implement the priority actions (response to question 2). Chapter 6 also provides the potential short-term and intermediate outcomes and potential indicators to be monitored to assess the progress made in implementing the committee’s recommendations (questions 4 and 5). Because the committee’s recommendations are population-based policy and system changes, it is expected that they could improve hypertension prevention, treatment, and control across all population and subgroups. However, the committee also argues that hypertension is a sentinel indicator for how well the public health system is reducing health disparities (racial and ethnic, age, geographic). Chapter 6 briefly comments on the potential positive and negative impacts on health disparities (questions 6 and 7).
Much is known about the health consequences and costs associated with hypertension. Robust clinical and public health research efforts have developed safe and cost-effective nonpharmacological and pharmacological interventions (Chapters 4 and 5) to prevent, treat, and control hypertension. Nonetheless, millions of Americans continue to develop, live with, and die from hypertension because we are failing to translate our public health and clinical knowledge into effective prevention, treatment, and control programs. In the committee’s view this current state is one of neglect, defined by Merriam-Webster as “giving insufficient attention to something that merits attention.” The recommendations offered in this report outline a population-based policy and systems change approach to addressing hypertension that can be applied at the federal, state, and local levels. It is time to give full attention and take concerted actions to prevent and control hypertension.
STUDY PROCESS
In response to the study request, the IOM established the Committee on Public Health Priorities to Reduce and Control Hypertension in the U.S. Population. The committee comprised experts from the areas of public health, prevention, epidemiology, health care, hypertension, cardiovascular disease, health disparities, and community-based interventions. (See Appendix A for biographies of the committee members.)
During the course of the study, the committee gathered information
to address its charge through a variety of means. It conducted a review of pertinent literature and held three in-person information-gathering meetings with sessions that were open to the public. The first meeting included presentations from the sponsor and hypertension experts. The committee also received input on hypertension prevention and control strategies from representatives of a number of state, local, and nongovernmental agencies. The second meeting focused on learning more about the CDC Division for Heart Disease and Stroke Prevention’s activities and reviewing data on blood pressure trends. At that meeting the committee also received information on the lessons learned from the National High Blood Pressure Education Program, the Hypertension Detection and Follow-up Program, and the Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT) sponsored by the National Institutes of Health. The third meeting included presentations on health disparities in hypertension; past large-scale community-based interventions; and the effectiveness, cost, and coverage of hypertension interventions. Appendix B contains the agendas for public meetings. The committee also met in executive session for deliberative discussions following the information-gathering meetings.
Two additional meetings with open public sessions were held via tele-conference calls. These sessions included presentations to the committee on blood pressure trends in birth cohorts, dietary interventions to reduce hypertension, the experiences of one State Heart Disease and Stroke Prevention Program, and specific aspects of the CDC’s Heart Disease and Stroke Prevention Program. In addition to these meetings, the committee held conference calls to further discuss findings and to formulate recommendations.
STUDY APPROACH
The overall public health impact of high blood pressure is a function of the distribution of blood pressure in the population as well as the outcomes or health consequences of high blood pressure. Because of the continuous and graded relationship between blood pressure and adverse health outcomes, the committee supports the notion that public health efforts to prevent the health consequences of high blood pressure must consider not only reducing blood pressure among those with high levels but also shifting the distribution of blood pressure in the population as a whole (Ahern et al., 2008; Rose, 2001; Whelton et al., 2002). The committee also decided that a framework would be useful in the process of identifying potential priority public health strategies to reduce and control hypertension. The following section provides the framework used by the committee and the selection criteria considered in identifying potential priority strategies.
The population distribution of blood pressure and the health consequences of high blood pressure are the end results of a complex set of
processes involving the action of factors at multiple levels ranging from macro-level and societal factors (e.g., policies related to the production and distribution of foods), to intermediate factors related to the characteristics of the living and working environments (e.g., access to healthy foods, physical activity resources), and to personal characteristics (e.g., genetic predisposition, behavioral choices). Health system factors also affect blood pressure levels through access to and quality of care. Additional examples of relevant factors at different levels are shown in Figure 1-3. This figure served as a heuristic to help the committee to think about the multiple factors that influence the population blood pressure distribution, the incidence and prevalence of hypertension, and blood pressure control; it was not intended to be a full representation of the many factors affecting blood pressure or to concretely specify the inter-relationships among the factors.
Within each of the levels shown in Figure 1-3, some factors may affect primarily the population distribution of blood pressure, whereas others may affect primarily the health consequences of hypertension (which in turn depend on early detection, treatment, and control of high blood pressure). In general the more “macro” factors (sometimes termed population-level factors) will affect primarily the distribution of blood pressure; in contrast the adequate control of high blood pressure will likely require the consid-
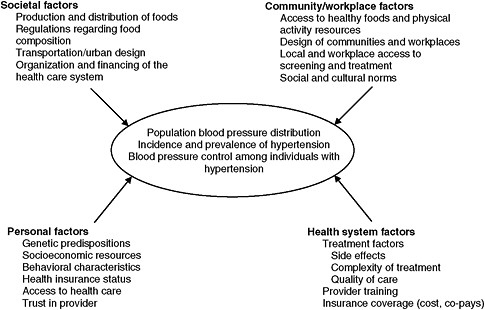
FIGURE 1-3 Schematic framework of factors affecting blood pressure.
eration of personal factors. However, these distinctions are not clear-cut. For example, societal factors related to the sodium content of processed foods may primarily affect the population distribution of blood pressure, but may also have important effects on blood pressure control among individuals diagnosed with hypertension. In addition, blood pressure control, including adherence to medication, among hypertensive individuals will be affected by personal factors such as health insurance status, access to providers, socioeconomic resources and other behavioral factors, but may also be impacted by societal health system organization as well as access to follow-up and monitoring in communities and workplaces.
In considering possible strategies for the prevention of high blood pressure and its adverse health consequences, the committee was guided by two basic features of the general framework illustrated in Figure 1-3: (1) the need to consider strategies aimed at shifting the population distribution of blood pressure (and thus preventing high blood pressure) as well as those targeted at persons considered to have hypertension based on current guidelines (to prevent the adverse consequences of high blood pressure); and (2) the need to consider factors at multiple levels, from societal to personal. Multiple categorizations of the possible interventions are possible. For simplicity, in this report, interventions are categorized in two broad domains: (1) population-wide strategies aimed at preventing high blood pressure by shifting the population distribution (referred to as population-based strategies) and (2) targeted strategies directed toward persons with, or at high risk, of high blood pressure aimed at reducing the adverse health consequences of hypertension through the early detection, treatment, and control hypertension (referred to as individual-based strategies).
Criteria for Identifying and Prioritizing Interventions
The committee developed a series of criteria to identify and prioritize recommended strategies and interventions. It was recognized that the information available to assess each of these criteria is highly variable and sometimes limited. Nevertheless it was agreed that public health decisions and recommendations need to be based on the best available evidence to date, with the recognition that the evidence may not be perfect and may evolve over time. No attempt was made to give specific weights to each of these criteria; rather they were used by the committee as general qualitative guidelines to help identify the most promising strategies for the CDC to pursue at this juncture. The criteria represent various domains relevant to prioritizing the CDC’s strategy. Two criteria (potential impact on population prevalence and evidence of effectiveness) assess the expected impact of the intervention on hypertension at the population level. A third criterion (relative cost or feasibility) incorporates the practical issues of cost
TABLE 1-2 Criteria Considered for Selecting Priority Areas for the Prevention and Control of Hypertension
|
Criteria |
Defining Questions |
Considerations |
|
Impact |
To what extent will the strategy or intervention reduce the incidence of hypertension or complications associated with hypertension? |
Effect size Proportion of people potentially affected |
|
Effectiveness |
What is the evidence of the strategy or intervention’s impact in real-world settings? |
Degree of generalizability to uncontrolled environments |
|
Relative cost or feasibility |
Is the strategy or intervention cost-effective? Qualitatively, how expensive is it to implement? |
Cost-effectiveness analysis |
|
Uniqueness |
Is there a special role for the CDC and its partners in implementing the strategy or intervention? |
Organizational authorities and mandates and roles |
|
Synergy with other CDC programs |
Will the strategy or intervention leverage or duplicate activities in other CDC units or activities conducted by other partners? |
Division for Heart Disease and Stroke Prevention core efforts and resources |
|
Reduction in disparities |
Will the strategy or intervention reduce disparities in risk factors or health care? |
Opportunity to narrow gaps in risk, disease burden, and care |
and feasibility. Two additional criteria (unique contribution of the CDC and synergy among other CDC programs) consider specific issues related to the role of the CDC. Finally, the last criterion considers whether the interventions are likely to benefit the most vulnerable groups and reduce disparities. A brief description of each of the criteria is provided below and in Table 1-2.
Potential Impacts of Interventions on Population Prevalence of Hypertension (or distribution of blood pressure) and on Adverse Health Consequences
This first criterion assesses the potential impact of the intervention on the prevalence of hypertension (or its complications). Impact is a function
of (1) the effect size of the intervention (as assessed by the relative risk or the risk difference) and (2) the proportion of people with the risk factor or condition at which the intervention is directed. Population impact is assessed through the calculation of the population attributable risk defined as the expected percentage reduction in the prevalence or incidence of the outcome in the population if the intervention were implemented in an ideal setting (i.e., the risk factor was entirely eliminated). The committee commissioned a review of the best available evidence on population attributable risk of a number of interventions intended to prevent hypertension. Although the ideal evidence would incorporate information on changes in blood pressure distributions rather than changes in arbitrarily defined dichotomous outcomes, very little information on the former exists. However, it is reasonable to make the assumption that the prevalence or incidence of hypertension is at least partly a function of the underlying blood pressure distribution.
The potential benefits of interventions focused on the early detection, treatment, and control of hypertension are also considered. In this case the potential benefit is not the prevention of hypertension but the reduction of its adverse health consequences through early detection, treatment, and control of individuals with hypertension (sometimes referred to as secondary prevention).
Evidence of Effectiveness in Real-World Settings
In addition to the potential impact of interventions (as quantified by the population attributable risk) based on effect sizes under ideal conditions (i.e., efficacy) and population prevalence, the committee also considered evidence of the impact or outcomes of interventions in practice or real-life settings. This real-life impact is sometimes referred to as effectiveness (Zaza et al., 2005). More generally, this criterion refers to the extent to which estimates of effect sizes of the intervention obtained from a given study (often conducted under ideal circumstances with excellent participation, fidelity of the intervention, and compliance) can be generalized to the slightly different circumstances that may arise in less controlled settings—for example, when the same intervention is implemented in the real world. Although efficacy and effectiveness are theoretically clearly distinguished in the extreme case, the extent to which a given study assesses efficacy or effectiveness is sometimes debatable. Therefore, the committee viewed this criterion in a qualitative way by considering the kinds of studies conducted and the extent to which their estimates are derived under conditions more akin to a laboratory or real-life setting.
Relative Cost or Feasibility
Despite the magnitude of hypertension-associated morbidity and mortality, current public health resources available for hypertension prevention and control are surprisingly limited, thus, hypertension interventions must be prioritized not only by effectiveness but also by cost, including both cost-effectiveness and absolute cost. Where possible, the committee reviewed available data on the cost of potential interventions and current DHDSP resources.
Unique Contribution of the CDC and Partner Agencies
In general, the CDC and state and local public health agencies are more experienced and skilled in population-based interventions than in interventions that provide health care directly to individuals. Government public health agencies are the only organizations with the mandate to provide population-wide services. Through leadership and convening strategies, government public health agencies can galvanize political commitment, develop policy, prioritize funding, and coordinate programs (Baker and Porter, 2005). In general, direct interventions providing health care to individuals (treatment) are much more distant from the unique skills and value-added of the CDC and state and local health partners.
Synergy with Other CDC Programs and Gap Analysis
Risk factors for and consequences of hypertension are common, overlap with other health conditions, and play a very large role in our overall population health. Thus, there already is substantial activity and prevention programming in place at the CDC and in state and local health departments. CDC priorities for hypertension prevention and control should not be duplicative of, but rather synergistic with, existing prevention programs in place within the CDC and in state and local health departments and in the community or individual health care settings. A similar dynamic of cross-cutting activities should, in theory, be present for health care interventions for communities or individuals.
Intervention Would Benefit the Most Vulnerable Groups and Reduce Disparities in Hypertension
Hypertension is so common that broad-based interventions are essential. That said, it is also a disease for which there are major inequities across racial and economic groups—along the entire spectrum from risk factors to the delivery of medical care. Interventions directed toward gen-
eral population groups historically do not correct these inequities and can even worsen them. Care was taken to identify a portfolio of interventions that might minimize existing inequities in the prevention, detection, and control of hypertension.
Hypertension is also a disease of aging, becoming increasingly prevalent as one grows older. From the perspective of the proportion affected, attention must be directed toward groups with the highest prevalence. However, from the perspective of the individual, hypertension in younger age groups has a greater potential for causing premature morbidity and mortality, so special attention needs to be paid to this at-risk population.
In the next chapters the committee reviews trends in hypertension and then applies the framework and criteria, to the extent possible, to the selection of priority strategies for the CDC and its partners.
REFERENCES
Ahern, J., M. R. Jones, E. Bakshis, and S. Galea. 2008. Revisiting Rose: Comparing the benefits and costs of population-wide and targeted interventions. Milbank Quarterly 86(4):581-600.
AHRQ (Agency for Healthcare Research and Quality). 2007. Screening for high blood pressure. Rockville, MD: U.S. Preventive Services Task Force.
ALLHAT (Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial). 2002. Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). Journal of the American Medical Association 288(23):2981-2997.
Baker, E. L., and J. Porter. 2005. Practicing management and leadership: Creating the information network for public health officials. Journal of Public Health Management and Practice 11(5):469-473.
Balu, S., and J. Thomas, 3rd. 2006. Incremental expenditure of treating hypertension in the United States. American Journal of Hypertension 19(8):810-816.
CDC (Centers for Disease Control and Prevention). 2006. Healthy People 2010 Midcourse Review: Section 12: Heart disease and stroke. http://www.healthypeople.gov/data/mid course/pdf/fa12.pdf (accessed February 4, 2010).
Chobanian, A. V., G. L. Bakris, H. R. Black, W. C. Cushman, L. A. Green, J. L. Izzo, Jr., D. W. Jones, B. J. Materson, S. Oparil, J. T. Wright, Jr., and E. J. Roccella. 2003. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: The JNC 7 Report. Journal of the American Medical Association 289(19):2560-2572.
Cutler, D. M., G. Long, E. R. Berndt, J. Royer, A. A. Fournier, A. Sasser, and P. Cremieux. 2007. The value of antihypertensive drugs: A perspective on medical innovation. Health Affairs 26(1):97-110.
Danaei, G., E. L. Ding, D. Mozaffarian, B. Taylor, J. Rehm, C. J. Murray, and M. Ezzati. 2009. The preventable causes of death in the United States: Comparative risk assessment of dietary, lifestyle, and metabolic risk factors. PLoS Medicine 6(4):e1000058.
DeVol, R., and A. Bedroussian. 2007. An unhealthy America: The economic burden of chronic disease. Santa Monica, CA: Milken Institute.
Fields, L. E., V. L. Burt, J. A. Cutler, J. Hughes, E. J. Roccella, and P. Sorlie. 2004. The burden of adult hypertension in the United States 1999 to 2000: A rising tide. Hypertension 44(4):398-404.
Lloyd-Jones, D., R. Adams, M. Carnethon, G. De Simone, T. B. Ferguson, K. Flegal, E. Ford, K. Furie, A. Go, K. Greenlund, N. Haase, S. Hailpern, M. Ho, V. Howard, B. Kissela, S. Kittner, D. Lackland, L. Lisabeth, A. Marelli, M. McDermott, J. Meigs, D. Mozaffarian, G. Nichol, C. O’Donnell, V. Roger, W. Rosamond, R. Sacco, P. Sorlie, R. Stafford, J. Steinberger, T. Thom, S. Wasserthiel-Smoller, N. Wong, J. Wylie-Rosett, and Y. Hong. 2009. Heart disease and stroke statistics—2009 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 119(3):480-486.
Miller, G. E., and M. Zodet. 2006. Trends in the pharmaceutical treatment of hypertension, 1997 to 2003. Research findings no. 25. http://meps.ahrq.gov/mepsweb/data_files/publications/rf25/rf25.pdf (accessed January 20, 1010).
NHLBI (National Heart, Lung, and Blood Institute). 2004a. JNC7 media kit. http://www. nhlbi.nih.gov/guidelines/hypertension/media_kit.htm (accessed January 27, 2010).
———. 2004b. Prevent and control America’s high blood pressure: Mission possible. Bethesda, MD: National Institutes of Health.
Psaty, B. M., T. A. Manolio, N. L. Smith, S. R. Heckbert, J. S. Gottdiener, G. L. Burke, J. Weissfeld, P. Enright, T. Lumley, N. Powe, and C. D. Furberg. 2002. Time trends in high blood pressure control and the use of antihypertensive medications in older adults: The Cardiovascular Health Study. Archives of Internal Medicine 162(20):2325-2332.
Rose, G. 2001. Sick individuals and sick populations. International Journal of Epidemiology 30(3):427-432.
Vasan, R. S., A. Beiser, S. Seshadri, M. G. Larson, W. B. Kannel, R. B. D’Agostino, and D. Levy. 2002. Residual lifetime risk for developing hypertension in middle-aged women and men: The Framingham Heart Study. Journal of the American Medical Association 287(8):1003-1010.
Whelton, P. K., J. He, L. J. Appel, J. A. Cutler, S. Havas, T. A. Kotchen, E. J. Roccella, R. Stout, C. Vallbona, M. C. Winston, and J. Karimbakas. 2002. Primary prevention of hypertension: Clinical and public health advisory from the National High Blood Pressure Education Program. Journal of the American Medical Association 288(15):1882-1888.
Zaza, S., P. A. Briss, and K. Harris (editors). 2005. The guide to community preventive services: What works to promote health? Task Force on Community Preventive Services. London, UK: Oxford University Press.