Managing and Coordinating Health Care: Creating Collaborative, Proactive Systems
DAVID A. DORR
Oregon Health and Science University
Portland, Oregon
In the last 100 years, huge advances in public health and medical care have resulted in people living longer, healthier lives. These advances have led to a shift from infectious diseases (pneumonia, tuberculosis, and infectious diarrhea) as the top three causes of death to the sequelae of chronic illnesses as the most common causes of death. For instance, heart disease, the most common cause of death in 2000, is hastened by diabetes, hypertension, and high cholesterol (Anderson and Arias, 2003). In addition, as people age, loss of functional ability and increasing disability become primary determinants of increased use of medical services, loss of independence, and death.
It has been shown that increasing disability and multiple conditions near the end of life, rather than single conditions or age alone, are the primary causes of increased hospitalizations and costs (e.g., Shugarman et al., 2009). Nevertheless, the health care system in the United States still focuses on treating individual conditions and meeting acute needs, rather than on ongoing care and overall health. Thus fixing this system will require changing health care delivery to anticipate these needs, teaching and encouraging people and their families to seek help, and providing care that consistently matches medical knowledge.
One possible “fix” is to add care managers—specially trained nurses and social workers who focus on the broad health picture—into primary care clinics. Care managers support a different approach to health care characterized by coordination, prioritization, and protocols for treatment plans assisted by the targeted
use of health information technologies (HIT). With these “fixes,” the health care system would address ongoing changes in a patient’s health as the care manager, supported by HIT, focuses on proactive, collaborative, coordinated care.
COMPLEXITY OF CARE AND THE NEED FOR CARE COORDINATION
In this article, we will consider gaps and potential solutions in the care of a hypothetical elderly patient, Ms. Viera. In this example, we consider two alternate courses in the life of a this hypothetical patient based on differences in care delivery (Figure 1). Ms. Viera is a 75-year-old woman with five common chronic conditions: (1) arthritis in her knees and hips; (2) diabetes, which she has had for the last five years; (3) high blood pressure; (4) moderate kidney problems, which have caused some swelling in her legs; and (5) recent difficulty remembering things day to day. She lives alone and can manage the usual household tasks. Socially, she goes to the senior center once a week, has a part-time professional caregiver, and has a daughter who lives about an hour away by car.
At the start of our hypothetical year, Ms. Viera looks back on last year, during
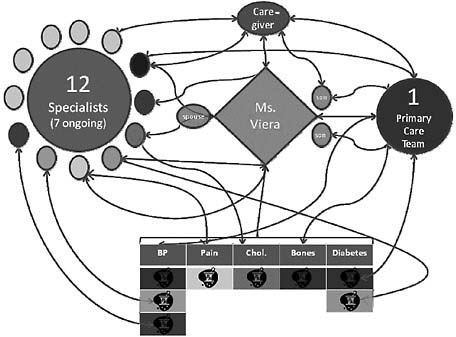
FIGURE 1 An example of average health care and needs for a patient with complex conditions.
which she saw 13 providers, 8 of whom she continues to see regularly. Her regular providers include her primary care provider (PCP), Dr. Smith, a doctor of internal medicine who provides ongoing care with a team of specialists—a rheumatologist for arthritis; a cardiologist; a neurologist, whom she saw in consult for memory loss; a nephrologist for kidney problems and high blood pressure; an orthopedist for her knees; a gynecologist; and an endocrinologist for diabetes. She filled 50 different prescriptions for 8 chronic medications and 4 short-term medications; several of these medications were prescribed by specialists, and some were prescribed by the PCP. She avoided the hospital last year, despite having nearly 90 times the risk of a hospitalization for someone her age with no chronic illnesses (Wolff et al., 2002).
As Figure 1 shows, an enormous number of connections had to be tracked by the patient, the family, and the caregiver—for communication and for changes to medical treatment plans. The coordination of these connections is the primary challenge we address in this paper.
Patients like Ms. Viera represent approximately 5 percent of people over 65, yet they use about 43 percent of all health care resources (Wolff et al., 2002). When we consider re-engineering the system to improve Ms. Viera’s care, we must first and foremost consider the benefit of those changes to her. A major hypothesis in care-coordination research is that carefully planning and arranging care can result in higher quality, more efficient care. Society, patients, and insurers will all benefit by avoiding waste from errors and “defects” in the care delivered.
A CRUCIAL JUNCTURE
Let us return to the case of Ms. Viera. At the beginning of our year, she is hospitalized briefly for difficulty breathing and dizziness. After about two days, she is diagnosed with out-of-control blood sugars and some excess fluid on her lungs. The hospital team stabilizes her by adjusting several medications, and she is discharged back to her home.
Figure 2 shows one potential course her post-hospital convalescence could take. Based on the hypothetical events listed on the left, in the next year, she goes home, appointments are planned, she attempts to resume her usual activities, sees specialists, has dizziness, chest pain, and some difficulties with control of her chronic conditions. In the usual course of care, “System 1” (on the right), the care-coordination tasks and their method of completion are highlighted. Studies show that upon discharge from the hospital, one-third of patients have care plans that are not followed or communicated (e.g., instructions to make an appointment with a physician). In addition, calls from the hospital staff to the PCP, although helpful, frequently do not lead to follow-up unless there is further communication—from either the hospital or primary-care team—directly with the patient. By the time the provider reviews the faxed discharge summary, Ms. Viera has about a 10 percent chance of being rehospitalized.
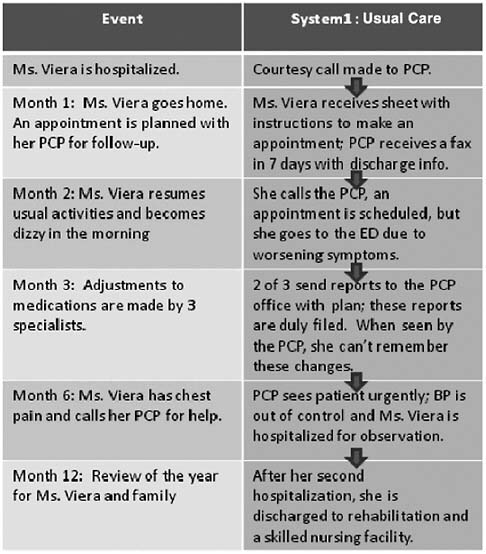
FIGURE 2 A year in the life of Ms. Viera with the usual system of health care.
In the next month, Ms. Viera may increase her activities and develop symptoms from her medications. In the usual system, she may call her PCP and, while waiting for the return call, her symptoms may worsen, and she may go to the emergency department. Upon seeing three of her specialists in follow-up, the lack of information sharing among settings and caregivers leads to new medications being prescribed but not remembered by the patient or family and not reconciled against her old list.
Finally, in month six, Ms. Viera may have a serious new problem—worsening
chest pain. In the usual system, all of her other issues may have distracted the primary-care team from controlling her blood pressure, which leads to a repeat hospitalization for monitoring. Although she does not have a heart attack, the changes in her medications and the unfamiliarity of her surroundings in the hospital may lead to a fall and a further need for rehabilitation.
In each of these common scenarios, gaps in coordination lead to increased use of health care and worse health for Ms. Viera. Our primary purposes in this paper are to elaborate on the reasons for our failure to create reliable health systems and to provide suggestions for improvement.
DEVELOPING A HEALTH CARE SYSTEM OF SYSTEMS
One way to change the current system of coordination “as usual”—which includes many gaps—is to think of health care as a more reliable and effective system of systems. One challenge in creating a reliable system is that gaps are not uniform; they vary over time and from individual to individual based on a wide range of factors, such as social needs, economic conditions, chronic illnesses, personal preferences, and local system infrastructure. Multiple disciplines, such as cognitive engineering, systems science, industrial engineering, and informatics, must be combined to begin to minimize and then close these gaps.
One way to address these problems is to take a close look at the existing health care delivery system and diagnose the gaps through a structured approach by looking at goals of care, current processes, infrastructure, and participants. We have completed a series of studies of the system of primary care, a subset of the overall health care system that focuses on ongoing, outpatient care by a PCP and a primary-care team (Dorr et al., 2005, 2006a,b, 2007b).
In this system, as shown in Figure 1, coordination of care is crucial to ensure that it is ongoing, comprehensive, and relationship-based. In our studies, we first defined the goals of care coordination and then the crucial processes necessary to attain those goals. These processes are usually nonlinear, are initiated through comprehensive assessments, and require iterative follow-up on care plans and patient needs. Finally, the structure is developed, in terms of the team’s abilities, the clinic-based technology that ensures (or at least supports) reliability, and defined roles, all relevant to the patient’s needs.
IDENTIFYING GAPS
Because patients have complex needs and there are many potential connections, we first identified the major problems by identifying gaps in the provision of care. We and others have used observations and semi-structured interviews of (1) patients with complex conditions, (2) physicians and nurses, and (3) other health care professionals to identify the most common gaps in care coordination in the primary-care clinic (Bodenheimer, 2008; Dorr et al., 2006b; Wilcox et al.,
2007). Principal problems identified in analysis include: (1) a lack of collaboration between patient/family and health-care team; (2) the absence of reliable, complete communication; and (3) failure to prioritize care needs based on both patient input and evidence for effective treatment.
Collaboration requires shared decision-making, a process whereby patients are educated about their condition, are offered options, and are provided with tools to help them make decisions. For patients with multiple chronic conditions, decisions must be made frequently and must be coordinated across conditions. Goal-setting by patients—which has been shown to lead to improved health—is done less than 25 percent of the time, and patients report that they do not feel included in decisions more than 50 percent of the time (Bodenheimer and Handley, 2009).
The reasons for frequent gaps in communication include: (1) the patient’s need for clear communications that focus on goals and outcomes; (2) the need for multiple inputs (e.g., from specialists and the primary-care team, as well as the patient and family) to complete a communication, which requires cyclical or iterative processes; and (3) the mode of communication either requires more attention than is available (e.g., in-person conversations with the provider) or is not timely (e.g., faxes) (Westbrook et al., 2007). With limited time and attention, failures in communication are common, leading to errors and preventable negative outcomes, such as emergency department visits resulting from unreturned calls or unclear instructions.
Finally, as the severity and risk factors of the patient’s condition increase, the prioritization of needs and next steps is crucial. Systems that remind providers and/or patients about every potential treatment or step in a care plan individually lead to provider/patient fatigue and distraction and ultimately fail to improve care. In one study, more than 50 percent of patients did not understand directions given to them by their physicians at the end of a visit (Bodenheimer and Handley, 2009).
COMPONENTS OF A SOLUTION
To understand the components of the solution, we now return to our sample patient, Ms. Viera. Given the same events outlined above over the course of a year, an optimal system, as shown in Figure 3, would address a number of the gaps we identified in the usual system of care.
Reorganizing the Care Team
The first category is team reorganization (Bodenheimer et al., 2002). In other disciplines, such as crew-resource management (e.g., air crews and other teams that work in high-risk, high-attention areas), the crucial requirements for reliable, effective performance include team competencies, thorough training, and
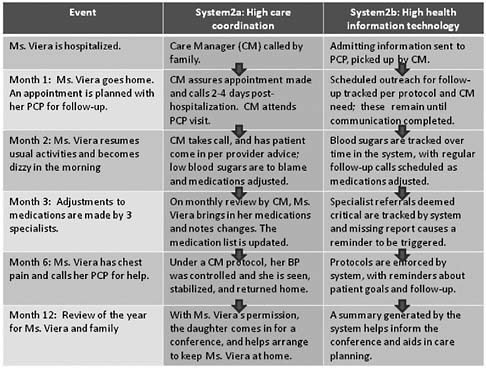
FIGURE 3 A proactive, collaborative system of coordinated health care.
well-defined, well-designed functions (Salas et al., 2006). For care coordination, specific roles—such as the role of a care manager—must be defined to address the need for reliable, effective communication and smooth, efficient workflow (Dorr et al., 2006b).
Evidence based on studies of care managers or care coordinators have increasingly shown that they can be crucial to minimizing the exacerbation of disease (Dorr et al., 2005), reducing the number of hospitalizations (Dorr et al., 2008), and improving patient satisfaction with their care (Wilcox et al., 2007). The essential competencies of care managers include the ability to educate patients and motivate them to set and follow goals and care plans, as well as to communicate effectively with members of the team, the patient, and the patient’s family.
Processes tested and implemented for the care of patients with specific conditions have been codified in primary-care team protocols that include identification of common conditions (e.g., elevated blood pressure), a treatment plan, and a flow chart. With the protocol, tasks are disseminated to appropriate team members beyond the beleaguered physician by pre-defining, in sequence, the steps that must be ordered manually under the current system. For protocols to be reliable, however, they must include collaboration, prioritization, and the complexity of the patient’s needs. Comprehensive assessments of preferences and goals that include
multiple conditions and patients’ needs have been shown to improve the health of older adults and to facilitate patient decision-making (Boult et al., 1999).
In our sample case, the care manager would facilitate coordination by receiving the call from the hospital, making the post-hospitalization follow-up call to the patient and family, and following protocols and proactively identifying the patient’s needs. Care managers can help close the communication loop because they remain focused on the key communication tasks for at-risk patients, follow up on critical referrals to specialists, and arrange conferences to consolidate communication. In the usual flow of things, the clinical staff must attend to many urgent needs as they arise and therefore have limited time to perform these less urgent, but no less important, tasks. Research has shown that trained care managers can accomplish these tasks and hence greatly improve the effectiveness and efficiency of health care delivery.
Health Information Technology
The number of patients that can be followed by a care manager is limited. Studies have shown that 2 to 5 percent of patients in a usual primary care clinic meet the criteria of Ms. Viera’s case: an at-risk patient diagnosed with multiple comorbid illnesses in need of ongoing care coordination. In a clinic of seven physicians, more than a thousand patients may meet these criteria, which could easily overwhelm care managers.
The primary goal of care coordination is to monitor, over time, the active care and treatment plan for patients and to take necessary steps to ensure that the plan is completed successfully. For example, health information technology (HIT) can greatly increase the likelihood of success. Key process points can be defined and programmed to remind care managers about crucial tasks. Whereas electronic health record systems usually focus on individual clinic visits and work flow and relegate hundreds of items to unstructured to-do lists, in our example, HIT functions can be adapted to help prioritize tasks by (1) identifying crucial elements that should be shared by members of the primary-care team, (2) ensuring that relevant information is delivered to the correct team members in the appropriate format, and (3) reminding clinicians about uncompleted tasks. To start the process, HIT, using filtering and prioritized data flow, must identify all patients under care management and the state of their current treatment plans and goals.
In our studies, by using HIT, care managers were able to follow an average of 350 patients at a time, approximately 1,000 per year (Dorr et al., 2007a). Patients under care management received prioritized messages about their hospital stay, were given automatic follow-up after sentinel events that persisted beyond an individual call or visit, and were moved to the top of the queue for attention when necessary.
The HIT system can embed protocols, although they must be flexible enough to accommodate the needs of care managers; for example, care managers only
need the next step defined and a reminder sent to address a patient’s rapidly changing status. Even for individual patients, care managers must identify the highest priority tasks and should be reminded about these first (Dorr et al., 2006a). For Ms. Viera, who sees 12 specialists a year, the care manager would designate which of these referrals are critical and directly affect the care plan; HIT would then remind the caregiver about these elements only.
Finally, summaries of the complex care and needs of patients are crucial to addressing emerging issues quickly and integrating the patient’s history with anticipated care needs in one place. Figure 4 shows this summary mechanism, the
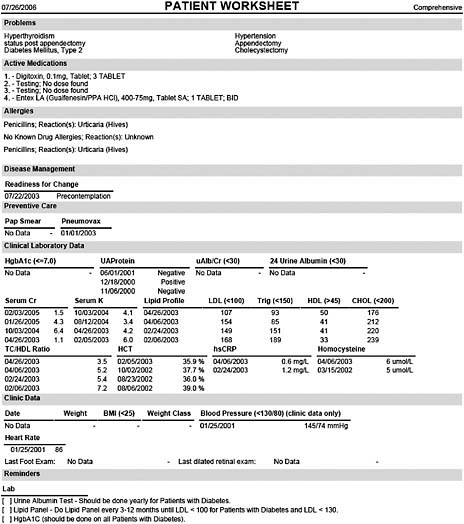
FIGURE 4 Comprehensive summary sheet.
patient’s worksheet (which, by itself, has been shown to improve adherence with evidence-based treatments for chronic and preventive illness by 17 to 30 percent) (Wilcox et al., 2005).
BUILDING A SUSTAINABLE MODEL
Once a patient’s needs and potential solutions have been identified, we work to implement them into a model of care. In seven intervention clinics at Intermountain Healthcare, a large, integrated health-delivery system, we installed care managers, trained them, and adapted HIT over a period of two years to develop the protocols and system described above. Over the next four years, patients seen by care managers lived longer, had 24 to 40 percent fewer hospitalizations, and had significantly better control of their conditions than similar patients at clinics without care managers (Dorr et al., 2005, 2008). The clinics with care managers also achieved higher efficiency levels, as measured by clinical output (patients seen and complexity of conditions treated). Lower costs that resulted from greater efficiency covered the costs of the care managers and the costs of expanding the program (Dorr et al., 2007b).
Unanticipated effects included variations in referral patterns and care-management patterns that led to some variations in outcomes. For instance, patients with predominantly social or financial problems did not have significantly fewer hospitalizations or emergency department visits, despite the care managers’ efforts. A positive unanticipated effect was a result of integrating a set of providers and patients. A number of patients described the care manager as “a life-saver,” and a number of providers said they “could not imagine practicing without the care manager.”
MAINTENANCE AND SUSTAINABILITY OF THE CARE-MANAGER MODEL
The next step is to determine the maintenance and sustainability of the caremanager model. In our qualitative studies, we defined core aspects of successful care management and embedded these in a training- and HIT-enhancement program. The core components of the model were defined as: (1) a trained care manager; (2) a supportive, trained team; and (3) specialized HIT. We then created a training and HIT support program (for details, see caremanagementplus.org). To date, more than 75 clinical teams have participated in the training and have been working on improving their HIT systems. In all, 73 percent of the teams were able to implement the core components of the model.
Further work is being done on sustainability, which can be a problem because many care-management tasks are not specifically reimbursed, despite their value. Changes in the reimbursement system (e.g., payments for the “medical home,” a
comprehensive model of primary care) or direct payments for care coordination may enable many more primary care teams to adopt these models.
CONCLUSIONS
Successful models of coordinated care that meet identified needs and improve patient health can be created by identifying gaps in current care systems, developing solutions that meet a particular patient’s needs, and developing changemanagement processes. We have shown that one successful model is to use care managers to augment primary-care teams and HIT to remind care managers and clinicians about prioritized tasks. The next steps will be to explore ways to ensure sustainability and to reinforce changes in the current health care system.
ACKNOWLEDGMENTS
Funding for this research comes from The John A. Hartford Foundation, Agency for Healthcare Research and Quality, and National Library of Medicine. This paper does not reflect the official positions of any of these institutions. Thank you also to the Care Management Plus team and collaborators.
REFERENCES
Anderson, R.N., and E. Arias. 2003. The effect of revised populations on mortality statistics for the United States, 2000. National Vital Statistics Reports: From the Centers for Disease Control and Prevention, National Center for Health Statistics, National Vital Statistics System 51(9): 1–24.
Bodenheimer, T. 2008. The future of primary care: transforming practice. New England Journal of Medicine 359(20): 2086, 2089.
Bodenheimer, T., and M.A. Handley. 2009. Goal-setting for behavior change in primary care: an exploration and status report. Patient Education and Counseling 76(2): 174–180.
Bodenheimer, T., E.H. Wagner, and K. Grumbach. 2002. Improving primary care for patients with chronic illness. Journal of the American Medical Association 288(14): 1775–1779.
Boult, C., R.L. Kane, J.T. Pacala, and E.H. Wagner. 1999. Innovative healthcare for chronically ill older persons: results of a national survey. American Journal of Managed Care 5(9): 1162–1172.
Dorr, D.A., A. Wilcox, S.M. Donnelly, L. Burns, and P.D. Clayton. 2005. Impact of generalist care managers on patients with diabetes. Health Services Research 40(5 Pt 1): 1400–1421.
Dorr, D.A., H. Tran, P. Gorman, and A.B. Wilcox. 2006a. Information needs of nurse care managers. Pp. 913 in AMIA Annual Symposium Proceedings. Bethesda, Md.: American Medical Informatics Association.
Dorr, D.A., A. Wilcox, L. Burns, C.P. Brunker, S.P. Narus, and P.D. Clayton. 2006b. Implementing a multidisease chronic care model in primary care using people and technology. Disease Management: DM 9(1): 1–15.
Dorr, D.A., A. Wilcox, S. Jones, L. Burns, S.M. Donnelly, and C.P. Brunker. 2007a. Care management dosage. Journal of General Internal Medicine 22(6): 736–741.
Dorr, D.A., A. Wilcox, K.J. McConnell, L. Burns, and C.P. Brunker. 2007b. Productivity enhancement for primary care providers using multicondition care management. American Journal of Managed Care 13(1): 22–28.
Dorr, D.A., A.B. Wilcox, C.P. Brunker, R.E. Burdon, and S.M. Donnelly. 2008. The effect of technology-supported, multidisease care management on the mortality and hospitalization of seniors. Journal of the American Geriatrics Society 56(12): 2195–2202.
Salas, E., K.A. Wilson, C.S. Burke, and D.C. Wightman. 2006. Does crew resource management training work? An update, an extension, and some critical needs. Human Factors 48(2): 392–412.
Shugarman, L.R., S.L. Decker, and A. Bercovitz. 2009. Demographic and social characteristics and spending at the end of life. Journal of Pain and Symptom Management 38(1): 15–26.
Westbrook, J.I., J. Braithwaite, A. Georgiou, A. Ampt, N. Creswick, E. Coiera, and R. Iedema. 2007. Multimethod evaluation of information and communication technologies in health in the context of wicked problems and sociotechnical theory. Journal of the American Medical Informatics Association 14(6): 746–755.
Wilcox, A.B., S.S. Jones, D.A. Dorr, W. Cannon, L. Burns, K. Radican, K. Christensen, C. Brunker, A. Larsen, S.P. Narus, S.N. Thornton, and P.D. Clayton. 2005. Use and impact of a computergenerated patient summary worksheet for primary care. Pp. 824–828 in AMIA Annual Symposium Proceedings. Bethesda, Md.: American Medical Informatics Association.
Wilcox, A.B., D.A. Dorr, L. Burns, S. Jones, J. Poll, and C. Bunker. 2007. Physician perspectives of nurse care management located in primary care clinics. Care Management Journals: Journal of Case Management; The Journal of Long Term Home Health Care 8(2): 58–63.
Wolff, J.L., B. Starfield, and G. Anderson. 2002. Prevalence, expenditures, and complications of multiple chronic conditions in the elderly. Archives of Internal Medicine 162(20): 2269–2276.












