1
Introduction
|
KEY MESSAGES
|
This report focuses on the challenge of obesity prevention, viewed from a population or public health perspective. It is about how to increase the likelihood that the decisions made in the many domains that influence obesity prevention will bring about the desired results. Observations of increases in weight among adults and youth globally within just a few decades have forced a paradigm shift in which overweight and obesity are understood not just as problems of individuals, but also as societal problems, affecting whole populations. Causal explanations and pathways to potential solutions have changed accordingly. The relatively rapid upward trends in average weight levels can in large part be explained by changes in social and environmental
variables that influence energy intake and expenditure—and the evidence of these changes is readily available and consistent.
Changes in the food and physical activity environments have caused sustained positive energy balance, leading to weight gain. For example, energy-dense foods and beverages have become more inexpensive, heavily advertised, and readily available than in the past, and their portion sizes continue to increase. Technological innovation in the home, workplace, and schools has reduced the need for physical effort, leading to sedentary behavior. Many schools have reduced or eliminated recess and physical education programs (IOM, 2005). The field of obesity prevention has made advances in determining the causes of the epidemic, but the complex interrelationships among those many causes have been difficult to address adequately within a given intervention. For this reason, a systems approach to obesity prevention is advocated in this report (see Chapter 4).
Taking a population perspective on obesity does not negate the importance of genetic or biologically mediated influences on the problem. But the increasing prevalence of obesity in diverse populations reveals the limitations of biological controls on energy balance in the face of high caloric availability and diminished caloric expenditure through routine physical activity. Nor does the recognition of environmental influences on obesity negate the importance of individual weight control efforts; however, the level of effort required makes individuals’ attempts to control their weight notoriously ineffective over the long term. Changes in aspects of society that encourage excess caloric consumption and sedentary behavior are therefore necessary to support individual efforts to achieve and maintain energy balance. In fact, measures that have been recommended for populationwide obesity prevention would enhance the potential for obesity treatment to be effective over the long term. Moreover, unless both weight gain trends and average population weight levels decline, progress achieved through treatment for those who are already obese will be offset by the tide of new people needing such treatment.
Calls for multifaceted efforts to prevent obesity have been made repeatedly by governments, scientific and professional societies, advocacy groups, and funding agencies at the local, state, national, and international levels. The case for obesity prevention is especially strong in relation to children and youth. The case was made for U.S. children in a 2005 Institute of Medicine (IOM) report Preventing Childhood Obesity: Health in the Balance—a report that was generated in response to a congressional request for a national action plan addressing the problem. Protecting children from harm and creating social and environmental conditions that support healthy growth and development are fundamental responsibilities of all societies. The physical and psychosocial consequences of obesity begin in childhood and may have a lifelong impact, especially—although not only—if obesity persists into adulthood. Indeed, most obesity and obesity-related diseases develop during adulthood—an important justification for obesity prevention directed at the adult population as well. Another
critical justification is that an obese adult population is an incubator, biologically and environmentally, for childhood obesity.
This chapter describes the charge and scope of the IOM Committee on an Evidence Framework for Obesity Prevention Decision Making, as well as the approach the committee took to fulfill its task. It also sets forth the case for viewing obesity as a problem of whole populations and for conceptualizing prevention strategies from a population perspective. Finally, it provides an orientation to the broad array of decisions of potential interest with respect to obesity prevention.
STUDY CHARGE, APPROACH, AND SCOPE
Several prior IOM committees have faced the need to work around evidence gaps and the fact that evidence hierarchies applied to medical treatment have limitations for assessing population-based preventive interventions. A committee tasked to develop a national action plan for child obesity prevention ultimately developed a set of principles to guide its process for reviewing evidence and making recommendations. These principles underscored the need for evidence to “inform and guide policy and programmatic decisions.” That committee also emphasized that the “absence of experimental evidence does not indicate a lack of causation or the ineffectiveness of an obesity prevention intervention,” that circumstances warrant taking preventive actions “even if there is as-yet-incomplete scientific evidence on the interventions,” but also that “there is an obligation to accumulate appropriate evidence not only to justify a course of action but to assess whether it has made a difference” (IOM, 2005, pp. 111, 114). The committee defined evidence broadly to include several types of quantitative and qualitative research studies or data that it consulted as appropriate to the type of question being answered and used an integrated approach that included multiple types of evidence, drawing on an approach then under development by an international organization. One of the hallmarks of the committee’s report was the use of historical case analyses—a social science method—applied to other complex public health scenarios as an alternative to typical traditional biomedical research studies.
The specific need for evidence on the effectiveness of interventions undertaken in various sectors and contexts was addressed by the IOM Committee to Assess Progress in Preventing Childhood Obesity (IOM, 2007). The IOM Committee on Food Marketing to Children and Youth (IOM, 2006) also highlighted several evidence issues and gaps that influenced its systematic review of evidence linking food and beverage marketing to childhood obesity or its behavioral determinants. Most recently, the IOM Committee on Local Government Actions to Prevent Childhood Obesity (IOM, 2009) followed the previous IOM recommendation to use the “best available evidence” rather than wait for the “best possible evidence” (IOM, 2005, p. 3) to recommend obesity prevention approaches based on potential effectiveness, impact, and suitability for local settings and authority. In light of the limitations of the current evidence base, that committee chose not to rank the recommended approaches. This deci-
sion was based on a desire to avoid the risk of prematurely devaluing approaches that are promising but still evolving and recognition that many context-specific factors, including the level of community support and the costs involved, determine which approaches are the best fit for a given community.
These evidence issues are not new and have already been the focus of many efforts in the field of public health in relation to other complex health problems. However, the issues are far from resolved and feel very new to the field of obesity because it has heretofore been oriented to treatment rather than public health and prevention. Considering these issues in relation to obesity prevention has the potential to advance the field of public health generally while also meeting the immediate need for clarity on evidence issues related to addressing the obesity epidemic.
Study Charge
Recognizing the importance of the issues outlined above, the IOM formed the Committee on an Evidence Framework for Obesity Prevention Decision Making, with funding from the Centers for Disease Control and Prevention (CDC), Kaiser Permanente, and the Robert Wood Johnson Foundation. The IOM appointed the 16-member committee in November 2008 to address the issues of how to identify, use, and evaluate evidence to inform obesity prevention decisions and how to generate evidence where it is lacking. These issues were identified as being of major concern or relevance to a range of potential users: decision makers in government and the private sector, practitioners in public health and other sectors, and program evaluators and other public health researchers, as well as research funders, journal editors, and the media, which determine, respectively, what research is funded, published, and disseminated. The committee members were selected to include academic researchers, practitioners, and policy makers, representing content expertise in various aspects of child and adult obesity prevention interventions; public health policy practice and research more generally; and research methodology from the perspectives of biomedicine, education, and psychology.
The committee was tasked to:
-
provide an overview of the nature of the evidence base for obesity prevention as it is currently construed;
-
identify the challenges associated with integrating scientific evidence with broader influences on policy and programmatic considerations;
-
provide a practical and action-oriented framework of recommendations for how to select, implement, and evaluate obesity prevention efforts;
-
identify ways in which existing or new tools and methods can be used to build a useful and timely evidence base appropriate to the challenges presented by the obesity epidemic, and describe ongoing attempts to meet these challenges;
-
develop a plan for communicating and disseminating the proposed framework and its recommendations; and
-
specify a plan for evaluating and refining the proposed framework in current decision-making processes.
Study Approach
A variety of sources informed the committee’s work. The committee’s deliberations drew on the findings and conclusions of the above-referenced IOM reports, and on other resources from within and outside the United States related to evidence-based public health and public policy as identified through extensive searches of the literature and a commissioned paper. Two public workshops were convened, in January and March 2009, to obtain additional input on evidence uses and challenges and on systems thinking and methodology (see Appendix F for the workshop agendas).
Obesity prevention differs from obesity treatment in the types of questions being addressed and answers being sought, the contexts in which the questions are asked and the answers are applied, and the types of research and information that may be relevant. The realities of using evidence to inform decisions about obesity treatment and prevention also differ in the availability of relevant research. In addition, because many influences on obesity are outside the health domain, information relevant to obesity prevention may not be readily identified through health research approaches. Given a dearth of information to address an urgent public health problem, the information that is available will be valued differently and efforts to fill evidence gaps given high priority.
Study Scope
This study was designed to go beyond obesity prevention as such, also yielding guidance for more general efforts to address complex, multifactorial public health challenges and examining the application of a systems perspective to the contexts in which policy and programmatic decisions that address such challenges are made. Equally important, the study scope was defined to reflect the need for a framework to guide decision making about obesity prevention in the population at large, rather than only in relation to children and youth. The epidemic of obesity in children and youth continues to be a major driver of preventive initiatives, but obesity prevention is also relevant to adults. As noted earlier, most obesity and obesity-related diseases develop during adulthood, and an obese adult population contributes to the development of obesity in children; indeed, from a population perspective, the environments of children and adults are interdependent and inseparable.
The committee defined “framework” to mean a process for identifying, evaluating, and compiling evidence relevant to various obesity prevention decision-making scenarios based on clearly specified concepts, assumptions, or rules. The process of developing the framework involved:
-
clarifying what is meant by population-based obesity prevention, that is, the types of initiatives that are undertaken to improve environments for eating and physical activity in ways that will reduce the likelihood of excess weight gain among people in general, as well as among particularly high-risk populations;
-
envisioning potential users and uses of such a framework, including the types of decisions to be made and ways in which evidence might enter into these decisions;
-
assessing the strengths and limitations of current approaches to evaluating and generating evidence about obesity prevention; and
-
identifying research approaches and forms of evidence that could be used to expand the options available to inform decision making on obesity prevention.
The assessment of the strengths and limitations of current approaches included a review of several ongoing efforts to improve research and practice in the field of obesity prevention or public health. These efforts focus on improving methods for characterizing the strength of evidence for prevention approaches, incorporating issues of generalizability of the research or relevance to practice into effectiveness studies, identifying appropriate outcome measures for obesity prevention, or enhancing the reporting of the results of prevention studies. Appendix B describes these efforts.
This report has two primary audiences: (1) decision makers and the intermediaries who assist them in making decisions and (2) because much of the evidence that is needed does not now exist, those who conduct research relevant to obesity prevention or who evaluate existing programs, as well as research-trained academics or other professionals with direct access to and knowledge of methods of evidence review and synthesis. Other important audiences include research funders and publishers of research findings.
OBESITY AS A SOCIETYWIDE PROBLEM
Overweight and obesity—reflecting a gain of excess body fat—result from the cumulative and initially imperceptible effects of hour-to-hour and day-to-day eating and physical activity behaviors that create a surplus of calories consumed relative to calories expended. Excess weight gain is usually unintentional and gradual, and it is difficult to reverse on a permanent basis.
Obesity prevention includes the need both to help those who are already overweight or obese avoid further weight gain and to help people who are not overweight or obese to avoid gaining excess weight. As suggested above, even if all those who are currently obese were to be treated effectively today, growth in the numbers of people becoming obese would continue without preventive efforts. Trend data from the National Health Examination and the National Health and Nutrition Examination Surveys between 1960 and 2002 indicate that the average body weight of U.S. men and women increased by 24.7 pounds (11.2 kg) and 24.1 pounds (11.0 kg), respec-
tively, while there was a relatively small increase in average height. The associated shift in average body mass index (BMI)—the typical weight-for-height measure used to assess obesity—was 3 kg/m2 in adults, in both men and women, from approximately 25 to 28 (Ogden et al., 2004). Figure 1-1 shows the shift in the distribution of BMI among U.S. adults between 1976-1980 and 2005-2006, with the gain being most pronounced among the heaviest people (Ogden et al., 2007).
Data from the 2007-2008 National Health and Nutrition Examination Surveys (NHANES)2 show that among adults aged 20 or older, nearly 34 percent have weight levels in the obese range (BMI ≥ 30) and another 34 percent are classified as overweight (BMI between 25 and 30), thus the combined prevalence of overweight and obesity is nearly 68 percent (Flegal et al., 2010). Among children and adolescents aged 2 through 19, nearly 17 percent are classified as obese (BMI for age and sex ≥ 95th percentile), and 15 percent are classified as overweight (BMI for age and sex ≥ 85th but < 95th percentile), thus close to 32 percent are either overweight or obese (Ogden et al., 2010). There is no evidence that underlying biological susceptibility to weight gain has changed, although there is ample evidence of increases in such factors as the amount of food available and where it is available, creating eating environments that are highly conducive to the consumption, often unintentional, of excess calories (Kral and Rolls, 2004; Ledikwe et al., 2005; Story et al., 2008; Wansink, 2004). There is also no evidence that the prevalence of individual weight control attempts has decreased as average population weights have increased. For example, the proportion of U.S. adult men and women who reported attempting to lose weight was, respectively, 29 and 44 percent in 1996 and 33 and 46 percent in 2000 (Bish et al., 2005; Serdula et al., 1999). Accordingly, the increasing prevalence of obesity in diverse populations reveals the limitations of biological and behavioral controls on caloric balance in the face of high caloric availability and the relatively low levels of physical activity that are common in urban and westernized societies (Booth et al., 2001; French et al., 2001; IOM, 2005; Kumanyika et al., 2002; Popkin and Gordon-Larsen, 2004). The need for multifaceted actions to prevent obesity should no longer be a subject of serious debate.
Many multifaceted interventions for obesity prevention influence the calorie balance by focusing on either energy intake or energy expenditure. According to Swinburn and colleagues (2009), it is important to know whether one of these two factors is the primary driver of the obesity epidemic in order to prioritize potential interventions. The relative contributions of increased energy intake and decreased energy expenditure to the obesity epidemic have been debated, with some suggesting that increased energy intake is sufficient to explain the weight gain of the American population since the 1970s (Bleich et al., 2008; Swinburn et al., 2009). Both factors are clearly important for energy balance and other health outcomes, and this report does not aim to tell decision makers whether to focus on energy intake, energy expen-
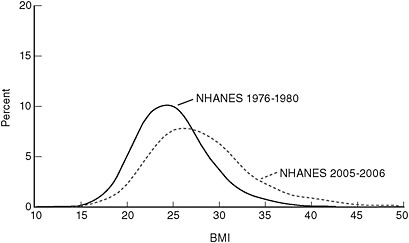
FIGURE 1-1 Changes in the distribution of body mass index (BMI) between 1976-1980 and 2005-2006 among U.S. adults aged 20-74.
NOTE: NHANES = National Health and Nutrition Examination Survey, a continuous program of studies designed to assess the health and nutritional status of a nationally representative sample of children and adults in the United States.
SOURCE: Ogden et al., 2007.
diture, or both. Indeed, the relative importance of each may vary across populations and settings.
Figures 1-2 and 1-3 show recent levels of obesity in three racial/ethnic groups in the United States and projections of future prevalence under the assumption that recently observed rates of increase will continue (Wang et al., 2008). The approximately one-third of men in all three groups who were obese in 1999-2004 could increase to nearly one-half within two decades. The same could be true for non-Hispanic white women, with even higher levels for non-Hispanic black and Mexican American women, for whom the prevalence of obesity was already greater than 50 percent and 40 percent, respectively.
Prevention efforts should not only aim to improve weight levels in the population at large but also target subpopulations with higher-than-average risk. Figures 1-2 and 1-3 identify key high-risk population subgroups—Mexican Americans and African Americans (Hedley et al., 2004; Ogden et al., 2007). Other U.S. ethnic groups with above-average obesity prevalence include American Indians, Pacific Islanders, and Native Hawaiians (Anderson and Whitaker, 2009; Broussard et al., 1991; Davis et al., 2004; Kumanyika, 1993). Low-income children and youth are also at high risk for obesity.
In many cases, above-average obesity prevalence is also observed in low-income populations, or high income is associated with lower obesity prevalence. In adults, the inverse gradient in obesity levels is seen most clearly in white females (Ogden, 2009). Figure 1-4 shows data for children with both sexes combined (Freedman et al., 2007).
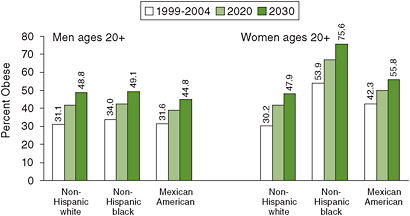
FIGURE 1-2 Projected increases in adult obesity (defined as BMI ≥ 30 kg/m2) if current trends continue, for males and females in three U.S. ethnic groups.
SOURCE: Adapted from Wang et al., 2008.
Obesity prevalence decreases with increasing income in non-Hispanic white children and is lowest in the high-income group among Mexican American children. No clear income gradient is observed in African American children, although higher risk with increasing income is suggested. However, the proportion of African American children who are obese is higher than that of white children at all income levels. The overall burden of obesity associated with living below the poverty line applies to 43 percent of African American and 40 percent of Mexican American children and to 16 percent of white children.
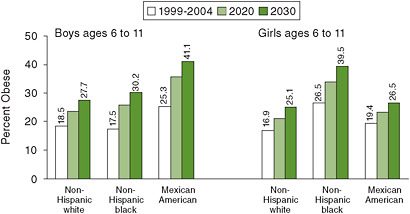
FIGURE 1-3 Projected increases in childhood obesity (defined as BMI ≥ 95th percentile based on CDC growth charts) if current trends continue, for males and females in three U.S. ethnic groups.
SOURCE: Adapted from Wang et al., 2008.
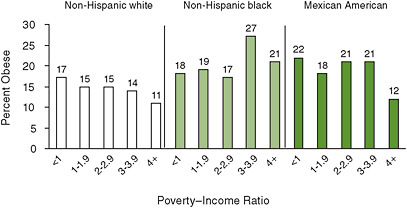
FIGURE 1-4 Percent of children and youth aged 2-19.9 who are obese (defined as BMI ≥ 95th percentile based on CDC growth charts), by family poverty−income ratio.
NOTES: The poverty−income ratio is the ratio of the income of the family to family income at the poverty level. Families with an income ratio of < 1 are below the poverty threshold.
SOURCE: Freedman et al., 2007.
While obesity is a priority from an epidemiologic and health status perspective, it gains further precedence because of the way it influences other aspects of American society. Obesity carries substantial direct and indirect costs for the nation’s economy, such as discrimination, economic disenfranchisement, lost productivity, and disability. As a result, states and communities end up diverting resources to prevention and treatment, and the nation’s health care system is burdened with the comorbidities of obesity, such as type 2 diabetes, hypertension, cardiovascular disease, osteoarthritis, and cancer (IOM, 2005). According to a recent analysis (Finkelstein et al., 2009), the annual medical burden of obesity is nearly 10 percent of all medical spending and may have risen to $147 billion per year by 2008. Further, obesity places at risk the long-term welfare and readiness of the U.S. military services by reducing the pool of individuals eligible for recruitment and decreasing the retention of new recruits (IOM, 2005). In addition to these societal costs, obesity imposes a broad range of costs on individuals. Tables 1-1 and 1-2, respectively, highlight the myriad effects of adult and child obesity on physical and mental health and quality of life.
DECISION MAKING, OBESITY PREVENTION, AND EVIDENCE NEEDS
In an ideal world, perhaps, policy decisions would be made primarily as a result of review and analysis of a carefully selected body of evidence that provided certainty and specificity as to the best approach or approaches, the outcomes that would result, and the cost of achieving those outcomes. However, real-life experience demonstrates that policy or programmatic decision making is not always such a linear process and that initiatives grounded in an idea generated by a research study may be the exception. Formal evidence may be used in highly variable ways, at different stages of a
TABLE 1-1 Relative Risk of Health Problems Associated with Obesity in Adultsa
|
Greatly Increased (relative risk > 3) |
Moderately Increased (relative risk 2-3) |
Slightly Increased (relative risk 1-2) |
|
• Type 2 diabetes |
• Coronary heart disease |
• Cancerb |
|
• Gallbladder disease |
• Hypertension |
• Reproductive hormone abnormalities |
|
• Dyslipidemia |
• Osteoarthritis |
• Polycystic ovary syndrome |
|
• Insulin resistance |
• Hyperuricemia and gout |
• Lower back pain |
|
• Breathlessness |
|
• Anesthesia complications |
|
• Sleep apnea |
|
• Fetal defects |
|
a All relative risk values are approximate. b Breast cancer in postmenopausal women, endometrial cancer, colon cancer. SOURCE: Reprinted with permission from World Health Organization, 2000. Copyright (2000) by the World Health Organization. |
||
process of instituting policies or programs, and for different reasons. Decision makers (i.e., those who make a decision to implement an intervention) may consider research-based evidence useful for supporting or opposing certain actions, but may also rely on a range of other information related to feasibility, political acceptability, and public support. Community programs may view research-based evidence as interesting but not entirely relevant to initiatives they may undertake in the real world. Program evaluators may share this view, emphasizing research that begins with projects of proven practicability that are shown to have promise or impact based on how things transpire. Members of the public may be frustrated with new evidence that appears daily and is often discordant with evidence from the day before. Additionally, making decisions about prevention is inherently complex, especially for problems, such as obesity, with multiple types and layers of causation. Moreover, prevention (keeping something
TABLE 1-2 Physical, Social, and Emotional Health Consequences of Obesity in Adults, Children, and Youth
|
Physical Health |
Social Health |
Emotional Health |
|
• Cardiovascular disease |
• Stigma |
• Low self-esteem |
|
• Cancer |
• Negative stereotyping |
• Negative body image |
|
• Glucose intolerance and insulin resistance |
• Discrimination |
• Depression |
|
• Type 2 diabetes |
• Teasing and bullying |
|
|
• Hypertension |
• Social marginalization |
|
|
• Dyslipidemia |
|
|
|
• Hepatic steatosis |
|
|
|
• Cholelithiasis |
|
|
|
• Sleep apnea |
|
|
|
• Menstrual abnormalities |
|
|
|
• Impaired balance |
|
|
|
• Orthopedic problems |
|
|
|
SOURCES: IOM, 2005; WHO, 2000. |
||
from happening) may be a much less dramatic or salient outcome than treatment (removing a problem), whose effects are not only obvious but also potentially more rewarding—personally and politically. Thus, although the case for prevention is compelling, making the decision to give it priority and determining which strategies will lead to more “nonevents” are highly challenging.
The widely held conviction that such decisions should be “evidence-based” only increases the challenge. How does one best determine which aspects of the environment to change, what changes to make, and how to effect these changes? Which interventions can potentially be effective on a large scale and sustainable over time? Where are the synergies among interventions? Could there be undesirable effects not readily apparent at the outset? Ideally, there would be a firm and comprehensive evidence base to inform the myriad decision makers whose actions—intentionally or unintentionally—influence the social and environmental determinants of unwanted weight gain and obesity. In reality, the approaches to evidence that apply to decision making about the treatment of obesity or other clinical problems are inadequate and sometimes inappropriate for application to decisions about public health initiatives such as obesity prevention. This situation poses a dilemma, one that is clearly compounded by the urgency of deciding which interventions can best address the problem. Evidence is needed to support such decisions for many reasons:
-
to justify interventions generally, particularly when there is competition for resources or opposition;
-
to inform priority setting and justify actions targeting high-risk populations, differentiate actions that are likely to be effective from those that are not, and quantify likely impacts;
-
to estimate costs and cost-effectiveness and anticipate unintended consequences, including harms to individuals or businesses; and
-
to help understand implementation factors, that is, what to do and how to do it.
The purpose of this report is to present a framework that will make it possible to meet these evidence needs.
Figure 1-5, which illustrates the levels and sectors of influence on obesity in populations, is helpful for understanding why decisions about obesity prevention are so complex (IOM, 2007). The figure shows the variety of levels at which interventions may be aimed and demonstrates how, taken together, a set of actions across levels might interrelate. Actions within many of these levels are focal points for discussion on how to combat the obesity epidemic within the United States and globally. Pathways or logic models can be drawn to link these levels to weight-related behaviors of population groups and individuals, such as food purchases; intakes of sugar-sweetened beverages, fruits and vegetables, whole grains, and total calories; television watching and other screen time; automobile use; breastfeeding; and routine and recreational physical activity. Relevant initiatives might focus on international trade
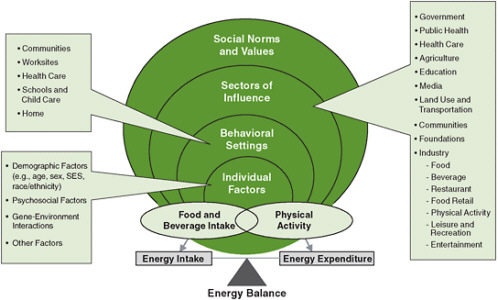
FIGURE 1-5 Comprehensive approach for preventing and addressing childhood obesity.
NOTE: SES = socioeconomic status.
SOURCE: IOM, 2007.
agreements that affect the food supply, food advertising, retail and restaurant food locations and marketing practices (including labeling and portion sizes), food prices, agricultural policies and food production systems, community design aspects that influence outdoor activity, building design aspects that influence indoor activity, public transportation, insurance coverage for wellness services, poverty levels, funding levels for and regulations guiding federal nutrition assistance programs, and school and worksite environments related to food and physical activity (IOM, 2009; James et al., 2006; WHO, 2004; World Cancer Research Fund and American Institute for Cancer Research, 2009).
Obesity prevention initiatives related to the settings and pathways shown on Figure 1-5 are ongoing, and more are undertaken or proposed every day. Many are quite far-reaching in their potential implications for such variables as food prices; food availability; community infrastructure; entertainment; and the nature and flow of information about food, activity, and weight. When the needed evidence exists to inform these decisions, the challenge is how to ensure that it appears in the right place at the right moment in the decision-making process and is taken to heart. If the evidence that exists is faulty or biased, the challenge is how to prevent this evidence from being used to support decisions that will ultimately prove to be poor ones. If the evidence is inadequate, one challenge is to prevent the lack of evidence from preclud-
ing timely and needed best guesses about potentially helpful solutions; another is to create the evidence to fill the gap. In the dynamic context of such issues as the obesity epidemic, the uneasy but necessary balance among making use of the best available evidence, avoiding the pitfalls of poor evidence, taking reasonable actions in the face of absent or grossly insufficient evidence, and waiting for the long process of formulating and generating relevant new evidence is a key challenge facing decision makers. Guidance is needed to keep a fruitful balance in view as progress toward solutions is made.
Box 1-1 presents some decision scenarios related to obesity prevention policies and programs. Those shown in italics are decisions likely to be made based on priorities unrelated to obesity but with potential effects on eating or physical activity. The decision scenarios in Box 1-1 all relate in some way to decisions about interventions; these types of questions are central to obesity prevention. However, decisions about the selection, implementation, and evaluation of interventions are closely tied to questions about why the intervention is needed and how a specific intervention can be expected to work in a given context. Some of these scenarios illustrate the potential for making arguments on obesity issues to justify changes in well-established policies and practices that affect marketing, services, or infrastructure related to patterns of eating and physical activity so as to ultimately influence consumer behavior. Consideration of these types of scenarios was core to the committee’s deliberations, undertaken to ensure that the resulting framework would be practical and broadly relevant.
ORGANIZATION OF THE REPORT
The remainder of this report is organized as follows:
-
Section I provides background on obesity prevention concepts and approaches (Chapter 2) and on evidence issues, including the results of the committee’s review of the limitations of current approaches to evaluating obesity prevention research (Chapter 3). Chapter 3 also introduces the committee’s proposed framework for using evidence to inform decision making on obesity prevention.
-
Section II presents an elaboration of each component of the proposed framework (Chapters 4 through 8). The importance of taking a systems perspective and how such a perspective can be useful in the process of using evidence to inform obesity prevention decisions is discussed in Chapter 4. Chapter 5 presents a typology of decisions and evidence that can guide the task of identifying useful evidence, a classification and discussion of various forms of evidence, and guidance on the process of searching for evidence. Chapter 6 explains the committee’s recommended approach to evidence evaluation as embodied in the framework; the discussion includes references to resources that can be useful in assessing the credibility of different forms of evidence. Chapter 7 addresses the
-
processes of assembling and reporting results, translating evidence to and from practice, deciding on the implications of the information for decision making, and integrating the overall knowledge gained from the evidence review process. Chapter 8 addresses the need for researchers to use the framework to motivate their work and think systematically about how to make progress in the inevitable, ongoing context of inadequate and imperfect evidence, and highlights other approaches to evidence generation for increased use in research on obesity prevention.
-
Finally, Section III turns to next steps. Chapter 9 provides guidance for future efforts of communicating, disseminating, refining, and updating the framework as new evidence and new methods emerge. Chapter 10 summarizes the committee’s conclusions and presents recommendations for supporting the identification, use, and evaluation of evidence to inform obesity prevention decisions and generate evidence when it is lacking.
For reference throughout the report, a list of acronyms and glossary of terms is provided in Appendix A; a table listing current efforts to improve research and practice in the field of obesity prevention or public health is given in Appendix B; Appendix C contains a table listing current reviews of obesity prevention interventions and strategies; Appendix D provides a list of selected information sources for locating evidence; Appendix E presents an in-depth discussion of some study design alternatives to randomized controlled trials and how theory, professional experience, and local wisdom can be used when evidence is lacking; Appendix F contains the agenda of two public workshops held by the committee; and Appendix G presents biographical sketches of the committee members.
REFERENCES
Anderson, S. E., and R. C. Whitaker. 2009. Prevalence of obesity among US preschool children in different racial and ethnic groups. Archives of Pediatrics and Adolescent Medicine 163(4):344-348.
Bish, C. L., H. M. Blanck, M. K. Serdula, M. Marcus, H. W. Kohl III, and L. K. Khan. 2005. Diet and physical activity behaviors among Americans trying to lose weight: 2000 behavioral risk factor surveillance system. Obesity Research 13(3):596-607.
Bleich, S., D. Cutler, C. Murray, and A. Adams. 2008. Why is the developed world obese? Annual Review of Public Health 29:273-295.
Booth, S. L., J. F. Sallis, C. Ritenbaugh, J. O. Hill, L. L. Birch, L. D. Frank, K. Glanz, D. A. Himmelgreen, M. Mudd, B. M. Popkin, K. A. Rickard, S. St. Jeor, and N. P. Hays. 2001. Environmental and societal factors affect food choice and physical activity: Rationale, influences, and leverage points. Nutrition Reviews 59(3, Supplement 2):S21-S39.
Broussard, B. A., A. Johnson, J. H. Himes, M. Story, R. Fichtner, F. Hauck, K. Bachman-Carter, J. Hayes, K. Frohlich, N. Gray, S. Valway, and D. Gohdes. 1991. Prevalence of obesity
in American Indians and Alaska natives. American Journal of Clinical Nutrition 53(6, Supplement).
Davis, J., J. Busch, Z. Hammatt, R. Novotny, R. Harrigan, A. Grandinetti, and D. Easa. 2004. The relationship between ethnicity and obesity in Asian and Pacific Islander populations: A literature review. Ethnicity and Disease 14(1):111-118.
Finkelstein, E. A., J. G. Trogdon, J. W. Cohen, and W. Dietz. 2009. Annual medical spending attributable to obesity: Payer and service-specific estimates. Health Affairs 28(5): w822-w831.
Flegal, K. M., M. D. Carroll, C. L. Ogden, and L. R. Curtin. 2010. Prevalence and trends in obesity among U.S. adults, 1999-2008. Journal of the American Medical Association 303(3):235-241.
Freedman, D. S., C. L. Ogden, K. M. Flegal, L. K. Khan, M. K. Serdula, and W. H. Dietz. 2007. Childhood overweight and family income. Medscape General Medicine 9(2).
French, S. A., M. Story, and R. W. Jeffery. 2001. Environmental influences on eating and physical activity. Annual Review of Public Health 22:309-335.
Hedley, A. A., C. L. Ogden, C. L. Johnson, M. D. Carroll, L. R. Curtin, and K. M. Flegal. 2004. Prevalence of overweight and obesity among U.S. children, adolescents, and adults, 1999-2002. Journal of the American Medical Association 291(23):2847-2850.
IOM (Institute of Medicine). 2005. Preventing childhood obesity: Health in the balance. Edited by J. Koplan, C. T. Liverman, and V. I. Kraak. Washington, DC: The National Academies Press.
IOM. 2006. Food marketing to children and youth: Threat or opportunity? Edited by J. M. McGinnis, J. Gootman, and V. I. Kraak. Washington, DC: The National Academies Press.
IOM. 2007. Progress in preventing childhood obesity: How do we measure up? Edited by J. Koplan, C. T. Liverman, V. I. Kraak, and S. L. Wisham. Washington, DC: The National Academies Press.
IOM. 2009. Local government actions to prevent childhood obesity. Edited by L. Parker, A. C. Burns, and E. Sanchez. Washington, DC: The National Academies Press.
James, W. P. T., N. J. Rigby, R. J. Leach, S. Kumanyika, T. Lobstein, and B. Swinburn. 2006. Global strategies to prevent childhood obesity: Forging a societal plan that works. Paper presented at Global Prevention Alliance McGill Integrative Health Challenge, October 2627, 2006.
Kral, T. V. E., and B. J. Rolls. 2004. Energy density and portion size: Their independent and combined effects on energy intake. Physiology and Behavior 82(1):131-138.
Kumanyika, S. K. 1993. Special issues regarding obesity in minority populations. Annals of Internal Medicine 119(7, Part 2):650-654.
Kumanyika, S., R. W. Jeffery, A. Morabia, C. Ritenbaugh, and V. J. Antipatis. 2002. Obesity prevention: The case for action. International Journal of Obesity 26(3):425-436.
Ledikwe, J. H., J. A. Ello-Martin, and B. J. Rolls. 2005. Portion sizes and the obesity epidemic. Journal of Nutrition 135(4):905-909.
Ogden, C. L. 2009. Disparities in obesity prevalence in the United States: Black women at risk. American Journal of Clinical Nutrition 89(4):1001-1002.
Ogden, C. L., C. D. Fryar, M. D. Carroll, and K. M. Flegal. 2004. Mean body weight, height, and body mass index, United States 1960-2002. Advance data from Vital and Health Statistics, No. 347. Hyattsville, MD: National Center for Health Statistics.
Ogden, C. L., M. D. Carroll, M. A. McDowell, and K. M. Flegal. 2007. Obesity among adults in the United States—No statistically significant change since 2003-2004. NCHS Data Brief No. 1. Hyattsville, MD: National Center for Health Statistics.
Ogden, C. L., M. D. Carroll, L. R. Curtin, M. M. Lamb, and K. M. Flegal. 2010. Prevalence of high body mass index in U.S. children and adolescents, 2007-2008. Journal of the American Medical Association 303(3):242-249.
Popkin, B. M., and P. Gordon-Larsen. 2004. The nutrition transition: Worldwide obesity dynamics and their determinants. International Journal of Obesity 28(Supplement 3):S2-S9.
Serdula, M. K., A. H. Mokdad, D. F. Williamson, D. A. Galuska, J. M. Mendlein, and G. W. Heath. 1999. Prevalence of attempting weight loss and strategies for controlling weight. Journal of the American Medical Association 282(14):1353-1358.
Story, M., K. M. Kaphingst, R. Robinson-O’Brien, and K. Glanz. 2008. Creating healthy food and eating environments: Policy and environmental approaches. Annual Review of Public Health 29:253-272.
Swinburn, B., G. Sacks, and E. Ravussin. 2009. Increased food energy supply is more than sufficient to explain the U.S. epidemic of obesity. American Journal of Clinical Nutrition 90(6):1453-1456.
Wang, Y., M. A. Beydoun, L. Liang, B. Caballero, and S. K. Kumanyika. 2008. Will all Americans become overweight or obese? Estimating the progression and cost of the U.S. obesity epidemic. Obesity 16(10):2323-2330.
Wansink, B. 2004. Environmental factors that increase the food intake and consumption volume of unknowing consumers. Annual Review of Nutrition 24:455-479.
WHO (World Health Organization). 2000. Obesity: Preventing and managing the global epidemic. Report of a WHO consultation. WHO Technical Report Series 864. Geneva: World Health Organization. Available online: http://www.who.int/nutrition/publications/obesity/en/index.html.
WHO. 2004. Global strategy on diet, physical activity, and health. Geneva: World Health Organization.
World Cancer Research Fund and American Institute for Cancer Research. 2009. Policy and action for cancer prevention. Food, nutrition, and physical activity: A global perspective. Washington, DC: American Institute for Cancer Research.


















