7
Data and Communications
Drew Dawson, director of the Office of Emergency Medical Services at the National Highway Traffic Safety Administration (NHTSA), served as the session chair for the panel on data and communications. He noted that the central recommendation from the 2006 Institute of Medicine (IOM) report on the Future of Emergency Care was to establish a “coordinated, regionalized, accountable system.” Specifically, the report stated that “the emergency care system of the future should be one in which all participants—from 9-1-1 to ambulances to EDs [emergency departments]—fully coordinate their activities and integrate communications to ensure seamless emergency and trauma services for the patient.”
“We have talked about the need to have regionalized systems in their response to a variety of specialty care areas,” Dawson observed. “The item that remains constant in all of these is the emergency medical services system. The prehospital Emergency Medical Services (EMS) system is needed to respond to almost everything, including the specialty areas that have been discussed.”
He pointed out that there are not different EMS systems for each patient condition. “We don’t have a ‘stroke EMS system.’ We don’t have a ‘cardiac EMS system.’ [W]hat we really [need] is a system that is well-structured, well-resourced, [and] adaptable to responding to a variety of needs and emergency conditions.”
Dawson noted that NHTSA’s initial involvement in emergency medical services was centered on preventing people from dying after automobile crashes. But their response was to develop an emergency medical services system—not just a prehospital trauma care system—that is capable of responding to all emergencies, regardless of etiology.
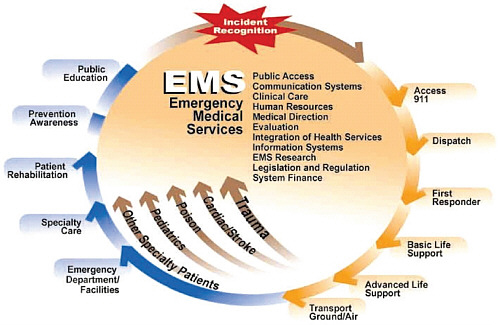
There are some core elements that run through every emergency medical services system, Dawson said, regardless of specialty. For example, each EMS system has core needs relating to infrastructure. Dawson presented a slide that shows “what an emergency medical services system is all about” (see Figure 7-1). He said it starts with notification through 9-1-1, and continues on through response, specialization, responding to specialty care patients, rehab, and public education. Dawson noted that this panel’s charge was to focus on a couple of the infrastructure elements listed on the slide, in particular communications. Communications are central to achieving the IOM recommendation of a coordinated system. In addition, the panel will focus on data and data collection, which are essential to measuring and improving the system.
EMS COMMUNICATIONS CHALLENGES
Kevin McGinnis, former emergency medical services director for the state of Maine and consultant to the National Association of State EMS Officials, said that he has been involved with building EMS systems since 1974. A lot has changed about EMS in the last 35 years, he said, but one constant has been its communication system, with its almost total reliance on voice communications with some telemetry and other data thrown in. The result is an aging and challenged infrastructure.
McGinnis said there is an immediate call for action in this area. A Federal Communications Commission (FCC) mandate for narrowbanding—which means making the small pipes smaller—has a drop-dead date of January 1, 2013, at which point many of the systems in use today will become illegal. McGinnis said this is one of the biggest EMS communications challenges in 35 years. In some places, it will mean wholesale replacement of radios—a costly proposition in a cash-strapped field. In other places, radios will need to be reprogrammed. Exquisite choreography among hospitals and ambulance services will be required to make this transition simultaneously.
The second area of challenge (and opportunity), he said, is technology. Done properly, this can substantially contribute to the regionalization effort. As a number of associations have begun planning around the communications capabilities that will be needed in the next 10 years, it has become clear that EMS will need to transition from about 90 percent voice to some mix of voice and data, perhaps 60/40 or 50/50. Otherwise, voice communications will become a bottleneck in communications between the field and the hospital, not a facilitator.
McGinnis predicted that as the physicians in emergency departments who provide online medical direction get busier, and as medics adopt diagnostic and other technology that provides much more information about the patient, changes will be needed. We’ll need to be able to take a lot of
that data and push it someplace and park it, so that when the physician is ready to consume the information, he or she can pull it in, consume it, and react to it. “That’s something we simply don’t do today. It’s a foreign concept.”
Technology will create the need for better communications in a number of areas, including multi-vital signs transmission capabilities, EKG (electro-cardiogram), and capnography, he said. There will be more use of video, for example in aiding decision making in long rural transports. There will also be technology that will be able to transmit patient medical records to and from the scene in real time.
The use of CT (computed tomography) and FAST (focused assessment with sonography for trauma) scans to get the patients going in the right direction to the right centers are all technologies that will increase the need for different kinds of communications. The current system of communications is narrowband and too slow to support that. So we are going to need broadband access all over, especially in rural areas. Unfortunately, these are the hardest places to get broadband, McGinnis said.
STANDARDIZING EMS DATA COLLECTION
N. Clay Mann, professor in the Department of Pediatrics at the University of Utah School of Medicine and principal investigator for the National Emergency Medical Services Information System (NEMSIS) Technical Assistance Center said, “Systems can’t really exist without communication. [T]he same can be said for data. Data is paramount to the existence of a system, regardless of what system of care we are talking about regionalizing.”
However, system of care data “is really a slippery fish,” Mann said. There are only rare instances where this type of data exists. For example, probably 80-85 percent of the evidence evaluating the effectiveness of trauma systems uses survival during hospitalization as the outcome measure. So, Mann pointed out, even in these instances where we are attempting to evaluate systems, we miss deaths that occur in the field (such as before EMS arrives or while EMS is there) and deaths that occur shortly after hospitalization. With that larger picture of injury-related mortality in mind, he said, “[valid] efforts to evaluate systems are very, very hard to find.”
Mann went on to describe the NEMSIS project and provide an update on its data collection activities, and also share some of the benefits and pitfalls of trying to develop data systems that can evaluate systems of care.
NEMSIS was born out of the events of September 11, 2001 (8 years ago to the day), Mann said. It has had two primary goals. First, standardize the data collection efforts of all EMS agencies in the country, including language and definitions. Second, and importantly for regionalization of care, provide a standard to ensure that all data exported from EMS agencies is uniform.
Mann said that he is working with states to help standardize their EMS data collections. Twenty-three states are now participating and sending data to the NEMSIS Technical Assistance Center. Eight more are expected to join this year. “It has been a bumpy ride,” he said, “but we [now] have approximately 7 million records in the national data set.” The portion of EMS agencies that are participating within a state varies from about 30 to 100 percent. Timeliness in receiving the data also varies. Some states are sending in their data daily, others quarterly.
Mann said that the data that comes in needs to provide not only denominator data, but also patient-level care data. He said that NEMSIS has attempted to do that, and the data results are available for viewing on the system’s Website (www.nemsis.org).
One barrier that NEMSIS has encountered in collecting data, Mann noted, is that EMS systems are not oriented to the importance of providing quality care. NEMSIS has also had a hard time collecting data that is nonclinical. He said, “We need to reeducate our EMS folks on the importance of collecting data that would support evaluation and improvement of systems.”
Mann said EMS officials would like the NEMSIS data system to be able to link to associated data sets, such as automated crash-notification data, 9-1-1 call center data, and police data. He said, “These need to be able to talk together.” However, there are barriers to providing seamless interoperability. NEMSIS has been working with HL7 to become a national standard for EMS data collection, but the many other public safety data-collection systems have not standardized their data processing, data definitions, and data export procedures. Mann noted that one big success has been linking with the American College of Surgeons Committee on Trauma (ACS-COT) National Trauma Data Bank (NTDB). He said “ACS-COT accepted and integrated the back [end] of NEMSIS into the NTDB, so those two are well connected. As a result, trauma care data can be collected in real time and moved between these two data sets in real time.”
LINKING WITH AUTOMATIC CRASH NOTIFICATION
Richard Hunt, director of the Division of Injury Response at the National Center for Injury Prevention and Control at the Centers for Disease Control and Prevention (CDC) said, “I think all of us in this room would probably agree that an approach to regionalization really needs to begin with some data.” One of the approaches that we have taken at the Injury Center, in collaboration with many of you in the audience, and many national organizations and federal partners, he said, is to capitalize on the data that came out of Dr. MacKenzie’s trauma outcomes study, demonstrating a 25 percent decrease in mortality if you are severely injured and land in a Level I trauma center.
Hunt continued, “Indeed, it really matters where the EMT [emergency medical technician] or the paramedic turns the wheel of the ambulance. It really matters. So, we wondered, how are we going to get them to turn the wheel and get them to the right place?” Hunt said the CDC and NHTSA collaborated with the American College of Surgeons’ Committee on Trauma, which had laid much of the foundation regarding triage of injured patients. Our organizations, he said, came out with a report called Guidelines for Field Triage of Injured Patients: Recommendations from the National Expert Panel.
These experts agreed that vehicle telematics is a promising approach and included recommendations on the use of advanced automatic collision notification for triage of the injured patient. This includes General Motors’ OnStar system, but also versions produced by Ford, BMW, and emerging technologies from Honda, Toyota, the European Union, and China.
The expert panel’s findings showed that these technologies show promise in improving outcomes in severely injured crash patients by predicting the likelihood of serious injury following a crash with greater precision, decreasing response times, aiding field triage decisions regarding destination and transportation mode (ground versus air EMS), decreasing time to definitive trauma care, and hopefully reducing deaths and disabilities.
Hunt said that OnStar generates a terabyte of data—a lot of data—regarding the exact time, location, and mechanics of the injury, and they can provide some predictability about likely injury severity. So, he said, “we have the data. We have the technology.” One of the expert panel’s recommendations is to make sure that the Division of Injury Response at CDC merges with NEMSIS and with the NTDB and other systems, because “without that data, we are flying blind with mechanism of injury.” He said, “I think we have a real opportunity to do it.”
This will be a challenge, though, because the automotive industry is in disarray due to the recession, governments are rapidly changing policies, and medicine is changing by the second. But, he said, “We are working hard to try to make it so that indeed these [ACN (automatic crash notification) technologies] can form an integrated system.”
THE BIRMINGHAM ALABAMA REGIONAL SYSTEM
Joseph Acker, executive director of the Birmingham Regional Emergency Medical Services System (BREMSS) and former Tennessee emergency medical services director, said “when you have [seen] one regionalized system … you have [seen] one regionalized system. What works for us in Birmingham may not work elsewhere.” But Acker said he wanted to present an overview of the Birmingham regional system, a model of a low-cost, high-impact approach to managing regional data.
BREMSS, part of the University of Alabama at Birmingham Health System, provides system coordination and education. The region encompasses 7 counties in central Alabama and stretches from Jefferson County (with 42 municipalities, including Birmingham), to Winston County (mostly rural) and includes 19 hospitals.
BREMSS has developed, instituted, and operates acute-event coordination systems. These events include trauma (which they have been doing since 1996 and are now expanding statewide), stroke (since 2000), and STEMI (just starting). The system manages about 4,000 transports per year.
The way the system works, Acker explained, is that when a paramedic responds to an incident, if he or she finds a patient who meets the entry criteria for one of these three conditions, the medic calls the Trauma Communication Center (TCC), which is staffed 24/7/365 by EMT-Ps [emergency medical technician-paramedics].
Every hospital in the region that is enrolled as a trauma, stroke, or STEMI hospital reports their status to the system through an intranet computer system. BREMSS-TCC always knows each hospital’s capability and capacity of service lines needed to treat these acute-event patients real-time, minute to minute.
The TCC takes the information from the paramedic and performs a secondary triage. TCC makes the decision of hospital destination based on hospital availability, transport time (ground or air), and patient condition. “We match the patient to the right hospital,” Acker said.
Information is then entered into a database, which automatically transmits via the intranet to the hospital’s work station. The patient is routed appropriately to the hospital, which is waiting in readiness for the patient. The hospital gives BREMSS control over destination decisions and “we guarantee [every participating] hospital that we will not send them a patient they don’t have the resource availability to treat.”
The system also facilitates interfacility transfers. Emergency physicians who are not able to locate a specialist or subspecialist can call TCC and immediately identify a facility that is able to care for their patient. “We have taken care of our EMTALA issues on that,” Acker said. “One call does it all.”
The system is voluntary. Until 2 years ago, there was no enabling legislation from the state. The system was funded with local dollars. The software system that ties everything together was built with local dollars. The hospitals supported and paid for the system. “That’s what happens when you give value to what the EMS system can do for acute-event patients and hospitals,” Acker said. “We make or save the hospitals money, because we match the right patient to the right hospital, and we guarantee that we are going to be responsive to the patient, hospitals, and emergency medicine’s needs.”
AUDIENCE DISCUSSION
Dawson asked, as we move forward with a regionalized, accountable emergency medical services system, and we examine demonstration projects in this area, what do the panelists feel would be the most important item—with respect to either data or communication—to include in a demonstration program?
McGinnis replied, “Acquiring wireless and connections to fiber for broadband communications.” Mann suggested, “Funding for the standardization of the different types of data that need to go into the national electronic health record, and then harmonizing those data sets.” Hunt said integrating NEMSIS and NTDB data, both for real-time and retrospective use. Finally, Acker said, “if funds are going to be there to support data, communications, system development, [and] system operation … those funds need to go to teaching hospitals. … That’s where the minds are. That’s where the systems can be developed. That’s where the accountability is.”
David Boyd noted that in the EMS Act of 1973, about 40 percent of his budget went to support communication systems. He said, if we go the route of demonstration projects “you are going to see at least a 40 percent communication need, right off the bat.”
Telemedicine’s Potential
Bill Hanson, an intensivist who runs a telemedical intensive care unit (ICU) program from the University of Pennsylvania, said his organization has also addressed issues about whether to keep patients in place and when to move them. They have discussed colocating a stroke center and a home telehealth center in the same physical core, and he believes there is an opportunity there.
Hanson said that some of the infrastructure costs that may seem prohibitive aren’t necessarily in play when it involves an existing core location with experts or nurses or doctors in position. You can put very inexpensive hardware in place in a variety of emergency rooms, move it around from bed to bed to bed, capture some of the data using video, and just receive information through the monitors or from streaming data through low-bandwidth connections. This might be a good demonstration project in an existing location.
McGinnis said, “I absolutely agree. I think the tele-trauma, tele-ICU capabilities of that sort are going to increase our ability to keep patients in their communities, which is the other side of regionalization, and are going to be critical.” He added that there are likely to be EMS/telemedicine applications that can do the same kinds of things.
Acker also agreed, saying “we have pitched this to potential client hospitals as a win-win opportunity. It allows them to keep patients in their
hospital that can be appropriately cared for and we will assist in transferring those patients the hospital does not have the current resources to care for. It allows them to identify patients that should be moved and move them very quickly.”
Hunt said that in the early 1990s, East Carolina University initiated a telemedicine program for trauma patients. He said, “I saw real changes. I saw us not transport a patient by helicopter because of telemedicine. I saw it change what happened to patients.” But, he said, “That concept hasn’t seemed to take off in the way I think may have been envisioned at the beginning.”
Hunt observed that last year, there seemed to be “a very new sense that this was much readier for primetime than it may have been previously.” Nevertheless, he said, “I don’t know where the initiatives are,” and “it [still] hasn’t taken off the way I thought it would have.” But he added that he has seen it make some difference, particularly in neurosurgery patients, where you can make some decisions about transfer very, very quickly, without spending a lot of resources.
Acker said that “one of the most basic needs that we have in any system is the ability to transmit digital studies.” There are significant potential cost savings there, both in not having to repeat the studies and in not having to move patients from a non-metropolitan hospital to a metropolitan hospital. There are systems out there that make this possible and don’t cost much money. He argued that “that makes more difference and will save more dollars and more times when a patient shouldn’t be transported than probably almost anything we can do.”
For example, Acker said, “We have a terrible, terrible problem with spontaneous head-bleed patients, which are not stroke patients, which are not trauma patients. It eats up our neurosurgical resources, [although] those patients really don’t need to be transferred from that rural hospital. They just need somebody to look at the film, or at the study, and comfort that physician at the other end and say, ‘This patient just needs to be watched. Call me back if certain things occur.’”
Boyd, who currently works for the Indian Health Service, said that the IHS is not quite sure whether to buy into the tele-trauma video business because there is no data to support it and they believe it could just be a fad. They are concerned that any equipment they buy will simply “lie around.” But, he said, “Transmission of CT [images] we are locked into.” He added, “we think that’s the greatest thing and that it’s going to improve the trauma care for our rural-placed hospitals.” If the Indian Health Service puts a CT in each one of its 40 hospitals, he said, and those are linked into their regional trauma centers, they could get an immediate read, which would definitely help determine the proper management plan for minor head injuries and other issues.
Boyd said that by having the images read in its hospitals and making provisions for the patients to be kept at home, Indian Health Service (IHS) could save over $35 million in unnecessary transport. “This is big-time dough. So we are really looking at that hard.”
Sanddal argued that there is also an increasing body of evidence that documents the efficacy of telemedicine/telehealth. He said that Dr. Jeffrey Saffle at Intermountain Burn Center in Utah has generated a comprehensive bibliography that supports its use in trauma and burns. He said that at a recent meeting, Saffle provided a case example of the need for telemedicine: a patient was shipped to Salt Lake City for burn care, but once the soot was removed from the patient’s face, all he needed was a 79-cent tube of Bacitracin. But it had cost $15,000 to transport him, plus he was hospitalized for 2 days while his family drove from Montana to get him.
Reimbursement and Regulation of Telemedicine
Dave Thompson from Syracuse said that when he worked with Dr. Hunt at East Carolina in earlier days, telemedicine “obviously had bandwidth issues and equipment issues.” The telemedicine unit used to take up a quarter of the attending office. Now, he said, “you can do it from a laptop, and clearly the bandwidth is there.”
“One issue that hasn’t changed very much has been reimbursement,” Thompson pointed out. Reimbursement for telemedicine has been “very variable.” Also, one of the things we need to address is who is going to pay for all this equipment? Telemedicine is getting cheaper and easier, “but you still have to pay for the equipment, maintain it, and [pay] all the people that are going to be on the other end sitting there waiting.” He asked Acker how they pay for having physicians, or whoever is in the unit, taking those calls.
Acker said that they staff with paramedics. With respect to the telemedicine component, they have five hospitals that contribute so that they can be part of the system. But, he added, “I think you are exactly right on with the issue of telemedicine. We will never build statewide stroke systems—wall-to-wall stroke systems—if we don’t do it with telemedicine. Somebody has to wake up in the federal government, in the reimbursement process, and recognize that there has to be better support for telemedicine, especially for stroke, which is the number-three killer and the number-one cause of adult disability.” He added, “It won’t happen without telemedicine, and telemedicine won’t happen if we don’t get reimbursement.”
Thompson added that “the other piece that inhibits telemedicine is licensure issues.” He said you can send images all over the world, “but I can’t talk to somebody in Pennsylvania and look at their images without running afoul of the law.” Acker said the American Stroke Association is really pushing on that issue now.
Hunt added that we need to take a stand in which we are really connecting with the regulators and the payers. We need to let them know that “telemedicine is integral to making the emergency care system more functional, more cost-effective, [with improved] quality.” He said, “I don’t think we have made a very deliberate approach [with regard] to telemedicine.”
Telemedicine Through Poison Control Centers
Lewis Goldfrank said that 35 years ago he and Dr. Boyd set up a telemedicine system for poison control. It was based originally on the telephone but has since become a very sophisticated electronic system. Goldfrank said it allows people to call and receive advice for free. Moreover, it has allowed large numbers of people to stay at home rather than use the EMS system or go to the emergency department. Estimates suggest that 20,000-40,000 fewer people go to emergency department (ED) per year because of poison centers. Because of the phone interventions, most hospital intensive-care units don’t ever see a child with a poisoning, or they see less than a handful a year, he said. This represents multiple millions of dollars in reduced health care costs, much of which would be borne by hospitals in the case of patients without insurance.
Goldfrank argued the call centers could become “a very consequential model.” He said, “We have a model that works, [largely] because no one was interested in it, so no one got in the way of its development. It’s quite remarkable. I think it could be used as something that is very helpful for the rest of us.” He posed the question, “Why couldn’t you use a call center for many other disorders?”
Medical Records and Hospital Diversion in an Air Traffic Control Model
Stephen Epstein of Beth Israel Deaconess Medical Center in Boston said to Acker, “It sounds like you operate with primarily one major tertiary center, a lot of feeders into that.” He said he was curious whether it would be possible to expand that system into a much larger venue where there are multiple organizations competing within a single region or metropolitan area. Referring to Magid’s presentation (see Chapter 3), he said “if you have sort of an air-traffic-control system, which you do, one of the things that must happen so that the patient doesn’t go to Elsewhere General Hospital, [which won’t have] their records, is to have some portability of patient records.”
Epstein said that it’s relatively easy to make sure that that information is going to flow if you are within one system in a metropolitan area. But how do we get that patient’s records to flow when it turns out that the closest,
best hospital, not on diversion, that has the service line available, is not in the system network where my patient’s records are? “As we all know, there are legal, technical, cultural challenges to getting those records to where they need to go.”
Mann replied that NEMSIS is attempting to do that by serving as a national standard for EMS data collection. Probably the long-term solution is that there will be a national electronic health care record, and all those who participate in the care of a patient, in whatever phase, will have to stick to the standardized data set that flows into one central repository. Acker said that they had tried to establish a regional system of patient medical records, but it had failed because it relied on patients and physicians to take steps to provide the information.
Epstein asked a second question regarding diversion in that type of system: “There are hospital systems which purposely, I believe, try to keep their emergency departments on diversion in order to allow inpatient bed availability for more lucrative patients, such as elective surgery [and] cardiac catheterization. They purposely keep their EDs dysfunctional.” He said, “There is no shaming that has changed that. The fiscal notes are the fiscal notes.” He asked whether Acker could address that particular type of gaming of the system.
Acker replied that, in their system, “Every hospital sees the performance of every other hospital. That does work, [through] peer pressure.” He explained, “It goes in front of all of the hospital administrators in the region, who sit by themselves in a room after I leave, and they discuss things. The peer pressure from one hospital group to another hospital group solves dramatic problems, let me tell you.”
Boyd said, “I believe that. Anytime you get the hospitals on a basis where they are all looking at each other, they are more honest.”
Hunt said that he had a similar experience in his previous position, with administrators looking at diversion data. But, he said, the pivot point only comes when you have all the CEOs in the room. Until it got to that level, nothing happened. Acker said he agreed “1,000 percent.”
Details on the Birmingham System
Workshop chair Arthur Kellermann asked Acker how much his system costs and how small rural hospitals have fared under it. He replied that the cost of operating the trauma communication system each year is about $450,000-$500,000. Two communicators are there 24 hours a day, 7 days a week, and they have added a third communicator, because they now dispatch five aircraft. He said the hospitals pay all the overhead costs and they pay for one full-time communicator and part of another communicator. The state also pays for one communicator.
“Our hospitals think enough of this that they are willing to put dollars on the line,” Acker said. Furthermore, they have not lost a single hospital out of the system.
Randy Pilgrim, emergency physician and chief medical officer of a practice management firm, the Schumacher Group, said that he is involved in advocacy at the state and federal levels regarding health care reimbursement changes that support improved quality and outcomes. Pilgrim said, “Questions come up very frequently around how you drive accountability with the reimbursement structure.”
With regard to the Birmingham system, he said, “I get that your system [is] regionalized, [and] that it’s coordinated, [and] your slide said [it’s] also accountable.” Pilgrim said that if the hospitals fund this, then you are accountable to them directly. “You are also very transparent hospital to hospital, so there are a lot of eyes watching.”
But Pilgrim asked to hear more about the fiscal accountability. He said he understands that, long term, if you do a bad job and the hospitals are funding you, they will pull the plug. “But,” he asked, “is there an episode-by-episode accountability where they would know if you were doing the wrong thing episode-by-episode?” If for some reason, you stopped doing a good job, would you see an immediate financial penalty?
Acker said that his organization produces an invoice on a month-to-month basis, and if a hospital is unhappy, they don’t pay for that month. Also, he noted that the Veterans Administration participates in the system in trauma, stroke, and ST-evaluation myocardial infarction (STEMI) and “they pay the same kind of money that the rest of the hospitals in the system pay.”
The other thing that creates accountability, he said, especially in the routing of patients, is that “third-party payers call us out if we misroute a patient.” But he said just the opposite is occurring. The third-party payers are calling us to find out if hospital X was on divert that day.
Acker said that to date they “have not had a single third-party payer refuse to pay the bill for a patient we routed, even if that was not the traditional hospital that that patient would have gone to. The third-party payers like us, because we make sure we get the patient to the right hospital in the right time frame, when that resource availability is there, and we don’t stick a patient in a hospital that doesn’t have the resources, where it prolongs their length of stay and [increases] the complications that occur.”
Linda Cole, of Children’s Healthcare of Atlanta, asked Acker whether diversion rates, mortality, and hospital length-of-stay outcomes have shown changes during their tenure and whether these results have been published.
Acker replied that “we are part of the UAB [University of Alabama at Birmingham] health system, so that gives us the resource capability for a lot
of study issues.” He said that one study reported in the American Surgeon found a 12 percent decrease in overall trauma deaths within the BREMSS region after implementation of the system. Also, length of stay for those with Injury Severity Score (ISS) of 15 or greater dropped from 16 days to 11 days. Today, patients with an ISS of 15 or greater have dropped to 9 days.
He cited another study by a colleague at UAB who looked at trauma patients who were in the trauma system and who were transported directly to a Level I center. They looked at the same class of patients, those with ISS of 15 or greater, who went to a community hospital first and then were transferred to the Level 1 (UAB). They found that patients who went to the community hospital first had 50 percent greater mortality. Moreover, their cost of care within UAB was twice what the cost of care was for comparable patients taken directly to UAB.
Acker added that the area hospitals have actually reduced their divert processes. The number of hours of divert for emergency departments have decreased about 15 percent over the last four and a half years. He said they have not been able to solve their divert problem for psychiatric cases, which, he called, “a terrible problem.”
But, in general, we have the divert status in front of all of the hospitals all the time, Acker said, and “they literally will do everything they can do stay off of divert.” However, his own view is that patient care suffers when the hospitals exceed a certain capacity—whether it’s for a trauma, stroke, STEMI, or general medical patient. He said “I think to turn your head and say there’s no need for divert in a system is foolish, and the patient ultimately pays the price for that.”
REFERENCE
Dawson, D. 2009. PowerPoint slide presented at the Regionalizing Emergency Care Workshop, Washington, DC.
Sasser, S. M., R. C. Hunt, E. E. Sullivent, M. M. Wald, J. Mitchko, G. J. Jurkovich, M. C. Henry, J. P. Salomone, S. C. Wang, R. L. Galli, A. Cooper, L. H. Brown, and R. W. Sattin. 2009. Guidelines for field triage of injured patients: Recommendations of the National Expert Panel on Field Triage. Morbidity and Mortality Weekly Report: Recommendations and Reports 58(RR01):1-35.