Summary
The human immunodeficiency virus (HIV) attacks the immune system, resulting in a progressive immunodeficiency that predisposes the infected person to opportunistic infections and cancers. This immunodeficiency is eventually fatal in nearly all cases in the absence of potent antiretroviral treatment. The advanced stage of HIV-induced immunodeficiency is termed acquired immunodeficiency syndrome or AIDS.
Before the availability of potent therapy in 1996, AIDS resulted in death in less than 2 years in most cases, usually as a direct result of one or more opportunistic infections or cancers. Advances in HIV research have led to the widespread availability of potent combination antiretroviral therapy, which has dramatically changed the course of HIV infection, making it a chronic, manageable disease in many people. These advances have important implications for treatment and outcomes as well as policies addressing the disease.
The U.S. Social Security Administration (SSA) responded early to the HIV/AIDS epidemic by providing disability benefits beginning in 1983 to people diagnosed with AIDS. In 1993 it adopted disability criteria for HIV (i.e., the HIV Infection Listings) as an administrative tool to more rapidly adjudicate claims. These criteria were loosely based on the Centers for Disease Control and Prevention’s (CDC’s) definition of AIDS. Despite the remarkable advances in HIV/AIDS management resulting from the availability of potent antiretroviral therapy in 1996, the HIV Infection Listings have not been substantially revised. In 2009, SSA asked the Institute of Medicine to establish the Committee on Social Security HIV Disability
Criteria to recommend improvements to the HIV Infection Listings (see Box S-1 for the statement of work).
Throughout its discussions, the committee acknowledged that listings cannot be viewed in a vacuum. The committee recognized that HIV/AIDS outcomes are improved by adhering to potent antiretroviral regimens. Adherence requires timely diagnosis of HIV infection, linkage and retention in HIV care, as well as continuous access and adherence to these drugs and to expert medical care. Recognition of this connection is critical because Social Security benefits have a great impact on access to care and treatment for people living with HIV/AIDS. Qualifying for Social Security disability benefits in many states is seen as an entrée to other public programs, such as Medicare and Medicaid and housing programs. The 2010 Patient Protection and Affordable Care Act will undoubtedly affect these social programs and others, but it is too early to determine how the Social Security disability program will be affected. While the issues of adherence and access to care are critical in the discussion of Social Security disability benefits, in-depth discussion about the means by which people receive treatment and medications are outside the committee’s scope.
SOCIAL SECURITY DISABILITY EVALUATION PROCESS
SSA pays disability benefits through two programs: Social Security Disability Insurance (SSDI) and Supplemental Security Income (SSI). To qualify, individuals must meet SSA’s definition of disability, which differs for adults and children,1 defined as follows:
-
Adults: “an inability to engage in any substantial gainful activity2 by reason of any medically determinable physical or mental
|
BOX S-1 Statement of Work An ad hoc committee of medical experts will conduct a study to assist the Social Security Administration (SSA) on HIV disability issues. The committee will review the current medical criteria for disability resulting from HIV infection in SSA’s Listing of Impairments (“the Listings”) and identify areas in which the HIV Infection Listings should be revised and updated based on current medical knowledge and practice. Specifically, the committee will (1) conduct a comprehensive review of the relevant research literature and current professional practice guidelines; (2) assess the current HIV Infection Listings in light of current research knowledge and evidence-based medical practice; and (3) produce a short report with specific recommendations for revision of the HIV Infection Listings based on evidence (to the extent possible) and professional judgment (where evidence is lacking). |
-
impairment(s)3 which can be expected to result in death or which has lasted or can be expected to last for a continuous period of not less than 12 months.”
-
Children: a child is “considered disabled if he has a medically determinable physical or mental impairment which results in marked and severe functional limitations, and which can be expected to result in death or which has lasted or can be expected to last for a continuous period of not less than 12 months.”
For adults applying for SSDI or SSI, SSA uses a five-step sequential evaluation process to determine whether a claimant is disabled (see Figure S-1). The process is modified for children applying for SSI benefits.
At Step 1, SSA determines whether the claimant is engaging in substantial gainful activity. If not, the claim progresses to Step 2 to determine whether the claimant has a severe impairment that significantly limits the claimant’s ability to perform basic work activities (e.g., standing and sitting). If the claimant is found to have a severe impairment then SSA determines whether it satisfies the medical condition found in the Listing of Impairments, also referred to as the Listings. Adult claims not allowed
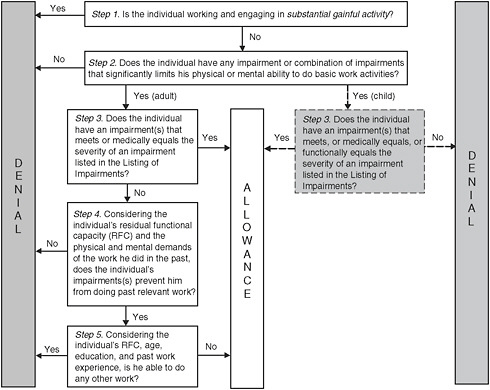
FIGURE S-1 Social Security Administration five-step sequential evaluation process.
at the Listings level proceed to Step 4 and, if necessary, Step 5, which considers a claimant’s ability to perform past work and to do other work in the national economy, respectively. This is assessed through a time- and resource-intensive process based on all relevant medical and other evidence in the case record.
For children under age 18 applying for SSI benefits, Steps 1 and 2 are the same. At Step 3, the considerations are whether a child’s impairment meets or medically equals a listing; if the claim does not meet or medically equal a listing, it may be found to functionally equal a listing. To make this determination, SSA assesses the interactive and cumulative effects of all of the child’s impairments in terms of six domains of functioning: (1) acquiring and using information; (2) attending and completing tasks; (3) interacting and relating with others; (4) moving about and manipulating objects; (5) caring for yourself; and (6) health and physical well-being.
The Listing of Impairments
To save time and resources, and to ease the administrative burden of determining the functional capacity of each claimant, SSA adopted a list of
serious medical conditions (the Listings), which are applied at Step 3 of the sequential evaluation process. The Listings consist of Part A (primarily for adults) and Part B (applies to children in cases where specific considerations are needed) and are organized into 14 body systems for adults and 15 for children (e.g., musculoskeletal, respiratory, neurological). The listing for each body system begins with a narrative introductory text that defines key concepts and terms used in that body system. Each body system and listing is identified by a number. For example, the immune system disorders body system for Part A is Listing 14.00, and HIV infection is Listing 14.08. The Part A HIV Infection Listing consists of 11 sublistings, from 14.08A to 14.08K, and the Part B HIV Infection Listing consists of 12 sublistings, from 114.08A to 114.08L.
In determining whether an individual is disabled, SSA decides whether the claimant’s impairment meets or medically equals a listing, as explained below:
-
Meets: If the evidence in a case establishes the presence of all the criteria required by one of the listings, then the claimant’s impairment meets that specific listing; and
-
Equals: If an individual is not found to meet the exact requirements of a specific listing, he can still be found disabled if the impairment is at least equal in severity and duration to the criteria of any listed impairment, as established by the relevant evidence in the claimant’s case record.
REVISING THE HIV INFECTION LISTING
SSA’s Listing of Impairments needs to be highly valid and reliable to efficiently and effectively recognize disabled claimants. The committee developed the following principles on which a new Listing ought to be based:
-
Reflect current medical practice;
-
Determine severity fairly;
-
Use objective evidence, to the extent possible;
-
Incorporate work-related functioning, to the extent possible;
-
Be simple and easy to implement; and
-
Use flexible language to account for changes in the disease and its treatment over time.
The committee considered incorporating measures of work-related functioning to complement declines in organ or physical functioning because many patients with HIV/AIDS show a decline in functional abilities after diagnosis and as their diseases progress. Additionally, comorbid condi-
tions often lead to a more disabling condition than would be predicted from the sum of their individual effects. The committee concludes that measures of functional capacity are critical in assessing whether patients living with HIV/AIDS can participate meaningfully in social and employment activities. However, upon reviewing the literature, the committee found no single test to measure the overall functional capacity or functional limitation of an individual with HIV. Functional limitations in adults are primarily assessed in three domains (i.e., physical, mental, neurocognitive), but are difficult to define or measure in a cost-effective and reproducible manner.
Without strong, valid, and easy-to-conduct functional measures, the committee sought to identify current equivalents to the earlier CDC definition of AIDS in the context of disability. Upon evaluating the medical literature, the committee identified four categories under which claimants should be considered disabled: those with CD4 ≤ 50 cells/mm3; those with imminently fatal or severely disabling HIV-associated conditions; those with HIV-associated conditions without listings elsewhere in the Listing of Impairments; and those with HIV-associated conditions with listings elsewhere in the Listing of Impairments.
Low CD4 Count
The committee tried to identify a laboratory marker that could be used to make decisions about functional impairment and disability, but no direct associations were found. In the absence of such associations, the committee considered measures predictive of disease progression, morbidity, and mortality as surrogate markers of disability.
The CD4+ T-cell (also known as CD4 cells or T-cells) count is a common standard laboratory marker of disease stage for HIV/AIDS patients. The 1993 CDC AIDS definition was expanded to include a CD4 count below 200 cells/mm3 as indicative of an AIDS diagnosis. Varying CD4 levels indicate different levels of disease severity. A CD4 ≤ 50 cells/mm3 has been associated with poorer response to antiretroviral therapy, increased short-term all-cause mortality, and increased incidence of HIV-associated illnesses. Additionally, the majority of early mortalities from those with opportunistic infections occur at CD4 ≤ 50 cells/mm3. Although CD4 count is a continuous variable, CD4 ≤ 50 cells/mm3, as compared to other values, is most indicative of severe advanced immunodeficiency. It is comparable to the previous CDC AIDS definition based on opportunistic infections and cancers in its ability to indicate impairment. Although other clinical markers exist, such as HIV plasma viral load, none predict disease stage as well as CD4 count. The HIV viral load is clinically useful in monitoring the response to antiretroviral therapy and is a good predictor of the rate of CD4 decline, but it is not a direct measure of disease stage.
Although widely accepted measures of HIV functional impairments are limited, a strong relationship exists between advanced immune impairment and clinical outcomes, including mortality. The committee concludes that a threshold can be drawn at CD4 ≤ 50 cells/mm3 as an indicator of disability. Because CD4 count can change in response to antiretroviral therapy, claimants allowed disability under such a listing should be periodically reevaluated. The committee believes 3 years would allow for a sustained response and is the maximum practical period for SSA reassessment.
RECOMMENDATION 1. SSA should use CD4 count as an indicator of disability. Specifically, CD4 ≤ 50 cells/mm3is an indicator that a claimant’s HIV infection is disabling. This allowance should be reevaluated periodically by SSA.
Imminently Fatal or Severely Disabling HIV-Associated Conditions
A number of imminently fatal or severely disabling HIV-associated conditions exist, even in the era of potent antiretroviral therapy. These rare but very aggressive diseases will likely lead to death or severe disability within a year and patients are unlikely to improve. Although much less common than early in the epidemic, these generally untreatable conditions resemble the AIDS-defining infections or cancers that were considered appropriate for disability allowance in the current listing. The committee therefore concludes that claimants with these conditions need to be considered separately from other HIV infection claimants and that these conditions should be specifically included in the HIV Infection Listings as permanent disabilities.
RECOMMENDATION 2. SSA should make disability determination allowances permanent for imminently fatal and/or severely disabling HIV-associated conditions. These conditions may be appropriate as compassionate allowances. These include the following:
-
HIV-associated dementia;
-
Multicentric Castleman’s disease;
-
Kaposi’s sarcoma involving the pulmonary parenchyma;
-
Primary central nervous system lymphomas;
-
Primary effusion lymphoma; and
-
Progressive multifocal leukoencephalopathy.
Other Severe HIV-Associated Conditions
A new set of nonimminently fatal medical conditions associated with HIV infection has emerged in recent years. Among these are conditions also seen in the general population, including cardiovascular disease and
osteoporosis. In the United States, these and other HIV-associated conditions have become leading causes of morbidity and mortality for persons living with HIV infection. They can be the result of the disease itself, adverse effects of HIV treatments, comorbid diseases, or from the treatment of those conditions. Additionally, longer recognized conditions such as distal sensory polyneuropathy also continue to be disabling.
The committee believes that the presence of an opportunistic infection or a manifestation of HIV alone is no longer sufficient to declare a person unable to work. However, the combination of clinical severity and limited functional capacity would allow for an appropriate determination of disability to be made. The severity of such conditions can be assessed by coupling objective tests of medical impairment with an evaluation of functioning. Although few measures of functioning exist for people living with HIV/AIDS, three measures of functioning are currently used in other areas of the Listing of Impairments, including 14.08K of the HIV Infection Listing: ability to perform activities of daily living; maintenance of social functioning; and completion of tasks in a timely manner due to deficiencies in concentration, persistence, or pace. This sublisting is the second most frequently used sublisting, leading the committee to conclude that disability examiners are comfortable with using these measures. In the absence of a single, widely used measure of functioning for people living with HIV/ AIDS, the committee believes these three measures should be retained in revisions to improve the effectiveness of the Listing.
RECOMMENDATION 3. SSA should continue to include measures of functional capacity in the HIV Infection Listings and update these measures with research advances.
Although opportunistic infections now occur at a lower rate, they can still be associated with early mortality. The committee believes the majority of HIV-infected people with severe opportunistic infections would be captured by a CD4 ≤ 50 cells/mm3 listing; disability assessment could also be triggered by poor functional status.
Some HIV-associated conditions are not addressed in other sections of the Listing of Impairments, while others are. The committee considered the two groups separately because if a current listing does not exist for conditions that can be truly disabling, a path to receive disability benefits will need to be identified. Having a condition with a current listing elsewhere also provides a path to being deemed disabled in Step 3.
HIV-Associated Conditions Without Listings Elsewhere
The committee suggests that a Listing be developed that identifies potentially severe HIV-associated conditions currently without listings elsewhere
in the Listing of Impairments (i.e., outside of Listings 14.08 and 114.08). An assessment of functioning should be completed in disability claims that present with (1) HIV-associated conditions, (2) adverse effects of treatment for HIV or comorbid conditions, or (3) other significant, documented symptoms (e.g., fatigue, malaise, pain). To account for the unpredictable nature of HIV and its treatment, allowances made under these parameters should be considered a disability for 3 years following the last documentation of the manifestation, adverse effects, or symptoms. This time period reflects the fact that HIV is now generally a manageable chronic disease and that the immunologic and functional status of many HIV claimants is likely to improve once they are engaged in care and receiving therapy. It should be noted that the benefits of therapy may decrease as comorbidities continue to develop, therefore requiring regular reevaluation.
RECOMMENDATION 4. Comorbidities induced by HIV infection or adverse effects of treatment should be considered disabling if they markedly limit functioning in one or more of the following areas: ability to perform activities of daily living; maintenance of social functioning; or completion of tasks in a timely manner due to deficiencies in concentration, persistence, or pace. This includes, but is not limited to, the following conditions:
-
Diarrhea;
-
Distal sensory polyneuropathy;
-
HIV-associated neurocognitive disorders;
-
HIV-associated wasting syndrome;
-
Kaposi’s sarcoma;
-
Lipoatrophy or lipohypertrophy; and
-
Osteoporosis.
Symptoms such as fatigue, malaise, and pain should also be considered if found to limit functioning. Periodically, SSA should reevaluate claims made using these comorbidities, consistent with the reevaluation of other disability allowances.
HIV-Associated Conditions With Listings Elsewhere
The committee identified a number of HIV-associated conditions with high morbidity and mortality currently represented in other sections of the Listing of Impairments. The prevalence of these diseases is growing among HIV-infected populations and will likely increase as these populations live longer. HIV infection typically results in an increased risk of developing comorbid conditions and an accelerated rate of progression to a severe or fatal outcome. However, the literature suggests the disability caused by co-morbid conditions is not usually clinically distinct and therefore is captured by other disability listings.
Upon assessment of the criteria currently in the Listing of Impairments for these other conditions, the committee determined that these were appropriate for assessing disability for people also infected with HIV. Because the condition is not unique, the committee concluded that current, existing listings are adequate for determining disability resulting from these conditions in HIV-infected people. Comorbid conditions should be cross-referenced to other listings and follow the disability criteria of those listings.
RECOMMENDATION 5. SSA should cross-reference the following HIV-associated conditions to existing listings:
-
Cardiovascular disease (Listings 4.00 and 104.00);
-
Chronic kidney disease, including HIV-associated nephropathy (Listings 6.00 and 106.00);
-
Diabetes (Listings 9.08 and 109.08);
-
Hepatitis (Listings 5.05 and 105.05); and
-
Malignancies (Listings 13.00 and 113.00), not otherwise specified in the report.
Recommendation 5 differs from Recommendation 4 in two ways. First, the duration of these allowances should follow the durations identified by the other sublistings. However, if it is found in the literature that HIV coinfection causes changes to the disease not effectively captured in other disability listings, SSA may want to consider adding the disease to the HIV Infection Listings. Second, the conditions discussed in this recommendation are not linked to functional criteria to allow for the conditions to be easily cross-referenced.
Concepts Specific to Children
When children receiving disability benefits reach age 18, they need to reapply to sustain their benefits. This can result in HIV-infected children switching from Part B (114.08) to Part A (14.08) to qualify as disabled. To allow for a smooth transition, the committee recommends that the listing specific to children follow as closely as possible to the Listing in Part A of the SSA Listing of Impairments.
RECOMMENDATION 6. SSA should ensure that the HIV Infection Listings in Parts A and B of the SSA Listing of Impairments are constructed similarly. However, conditions specific to children not found in adults should also be listed in Part B, including age-appropriate CD4 and developmental criteria, neurological manifestations of HIV infection, and HIV-related growth disturbance.
Because of the differences in CD4 count and percentage and prognosis between children and adults, Recommendation 1 needs to be modified for children, but still easily abstracted from the medical record. Count, percentage, or both may be available in medical records, but recent studies indicate that CD4 percentage adds little to the prognostic value of CD4 count. Based on approximate equivalency for the various age groups for HIV disease progression and death, the committee suggests the age-specific CD4 count and percentage criteria for children shown in Table S-1.
The conditions listed in Recommendation 2 are also rare in children but have been reported. Accordingly, a similar listing should be included in the pediatric HIV Infection Listing. Modifications should include the replacement of HIV-associated dementia with the current listing for neurological manifestations of HIV infection (currently 114.08G). Even in the era of combination antiretroviral therapy, neurological manifestations still present serious challenges for children. Therefore, neurological manifestations in children and adolescents should be maintained under Part B. In addition, growth development is an important indicator of their health and is seen as one of the most sensitive indicators of disease progression. Growth disturbance or failure to grow has been associated with rapid progression from asymptomatic HIV infection to AIDS in children thus leading to shorter survival. As a result, the committee concluded that the current listing for growth disturbance (currently 114.08H) should be retained in Part B.
In Part B, the measures of functioning used in Recommendation 4 should reflect measures relevant to children—developmental and emotional disorders of newborn and younger infants (currently paragraphs A–E of 112.12) and organic mental disorders (currently paragraphs B1–B2 of 112.02).
Although the conditions contained in Recommendation 5 are not common in children, they do occur and may become more evident as perinatally infected children continue to age. Additionally, there are current pediatric listings for these conditions that would be applicable. Therefore, the com-
mittee concludes that Recommendation 5 should also be applied to the Part B HIV Infection Listings.
MAXIMIZING THE UTILITY OF THE LISTINGS
The success of the HIV Infection Listings relies in part on how it is used, including general guidance for how to implement the Listings, how to reflect future changes in clinical practice, and how to more effectively obtain medical evidence.
Guidance for how to interpret and implement the Listings is in the introductory text, which precedes each section of the Listing of Impairments. The intended audience is broad and includes claimants and their families, the general public, disability examiners, medical consultants, and adjudicators. According to some disability examiners and medical consultants, the introductory text helps guide interpretation of the Listings, but at the same time it is confusing, disjointed, and difficult to read. In an effort to improve the usability of the introductory text, the committee believes that it should be reorganized and simplified.
RECOMMENDATION 7. SSA should rewrite the introductory text for Parts A and B of the SSA Listing of Impairments by:
-
Simplifying and reorganizing the text to address the appropriate audiences; and
-
Consolidating all HIV references into one section.
It will be important to reflect changes in the management and care of HIV infection in future revisions. Areas of particular concern for future assessments include long-term adverse events of treatment; newly emerging clinical manifestations of HIV infection; and consequences of nonadherence and resistance to HIV therapies. SSA should monitor these issues and others and consider adding them to the HIV Infection Listings as appropriate.
Data can be very informative in making the listings as effective as possible. SSA collects detailed data on each claim submitted and to an extent uses the data to inform its processes. Evaluations of these data can be important in identifying trends and patterns to help revise and inform the relevancy of the Listings. In addition, these data currently are not available for public use. However, making deidentified data publicly accessible for relevant analysis could result in improving the timeliness and applicability of the HIV Infection Listings.
RECOMMENDATION 8. SSA should use its database to maximize the utility of the HIV Infection Listings by:
-
Collecting and analyzing data to evaluate their effectiveness; and
-
Making data more widely accessible for outside analysis to better inform their currency and efficiency.
The initial information SSA uses to adjudicate a claim is generally acquired through the medical record, SSA disability application forms, and supplemental documents submitted by other health professionals. The committee expects that these forms will be updated to reflect Listing revisions and include measures of impairment, disability, and functioning. The forms should also be responsive to the decision-making needs of disability examiners and medical consultants.
Finally, the information that SSA uses to make its decisions often comes from an “acceptable medical source.”4 While “other sources”5 may have more meaningful and informative interactions with a claimant, their opinions may not receive equal weight to an “acceptable medical source.” The current hierarchy of health professionals delineated in the determination process may not be appropriate, especially when discussing functional ability. The committee concludes that SSA ought to consider including a wide array of licensed health professionals as acceptable medical sources (e.g., nurses, dentists, allied health professionals) for determining the functional effects of impairments.
CONCLUSION
An opportunity exists to improve the effectiveness of the HIV Infection Listings. The current Listings represent a time prior to the availability of effective antiretroviral therapy when HIV/AIDS was defined largely by having an opportunistic infection or malignancy resulting in a fatal outcome in a short period of time. Widespread availability of combination antiretroviral therapies has dramatically changed the course of HIV/AIDS. For many individuals it is now a chronic, manageable disease that is no longer characterized solely by opportunistic infections and malignancies. More importantly, HIV infection no longer equates with being permanently disabled. Instead, disability in HIV-infected claimants can now be more precisely identified by clinical markers and specific sets of medical conditions. By revising the HIV Infection Listings to better reflect current clinical practice, SSA will be able to more accurately identify those who need Social Security disability benefits.














