2
Study Context
This chapter presents essential context for the remainder of the report, addressing in turn the evolving challenges faced by the health care system, which drive the need for a reformed system and the concomitant transformation of the nursing profession; the three primary concerns targeted by health care reform—quality, access, and value; and the principles the committee determined must guide any reform efforts. The final section summarizes the committee’s conclusions about the implications of this discussion for the role of nurses in transforming the health care system.
EVOLVING HEALTH CARE CHALLENGES
For decades, the major focus of the U.S. health care system has been on treating acute illnesses and injuries, the predominant health challenges of the early 20th century. In the 21st century, the health challenges facing the nation have shifted dramatically:
-
Chronic conditions—While acute injuries and illnesses will never disappear, most health care today relates to chronic conditions, such as diabetes, hypertension, arthritis, cardiovascular disease, and mental health conditions, which in 2005 affected nearly one of every two Americans (CDC, 2010). This shift can be traced in part to the increased capabilities of the health care system to treat these conditions and in part to the
-
health challenges of an aging population, as the prevalence1 of chronic conditions increases with age. Dramatic increases in the prevalence of many of these conditions since 1970 are expected to continue (DeVol et al., 2007). Increasing obesity levels in the United States have compounded the problem, as obesity is related to many chronic conditions.
-
An aging population—According to the most recent census projections, the proportion of the U.S. population aged 65 or older is expected to rise from 12.7 percent in 2008 to 19.3 percent in 2030 (U.S. Census Bureau, 2008), in part as a result of increases in life expectancy and the aging of the Baby Boom generation. As the population continues to age, a dramatic growth in demand for health care services will be seen (IOM, 2008).
-
A more diverse population—Minority groups, which currently make up about a third of the U.S. population, are projected to become the majority by 2042 and 54 percent of the total population by 2050 (U.S. Census Bureau, 2008). Diversity exists not only among but also within various ethnic and racial groups with respect to country of origin, primary language, immigrant status and generation, socioeconomic status, history, and other cultural features.
-
Health disparities—Health disparities are inequities in the burden of disease, injury, or death experienced by socially disadvantaged groups relative to either whites or the general population. Such groups may be categorized by race, ethnicity, gender, sexual orientation, and/or income. Health disparities among these groups are driven in part by deleterious socioenvironmental conditions and behavioral risk factors, and in part by systematic biases that often result in unequal, inferior treatment (IOM, 2003b).
-
Limited English proficiency—The number of people living in the United States with limited English proficiency is increasing (U.S. Census Bureau, 2003). To be effective, care and health information must be accessible and offered in a manner that is understandable, as well as culturally relevant (IOM, 2004a; Joint Commission, 2007). While there are national standards for linguistically and culturally relevant health care services, the rapid growth of diverse populations with limited English proficiency and varying cultural and health practices is emerging as an increasingly complex challenge that few health care providers and organizations are currently prepared to handle (HHS Office of Minority Health, 2007).
PRIMARY CONCERNS IN HEALTH CARE REFORM: QUALITY, ACCESS, AND VALUE
In the search for solutions to improve the health care system, experts target three primary concerns: quality, access, and cost or value (Goldman and McGlynn, 2005). Substantial reforms designed to reshape and realign the major features of the entire health care system are needed to redress deficiencies in these three areas.
Quality
Despite unsustainable growth in health care spending in the United States (discussed below), the care received by individuals can often be too much, too little, too late, or too haphazard. Moreover, substantial geographic variations exist in the intensity of care provided across the nation, with attendant differences in quality, as well as cost (Fisher et al., 2009). The quality improvement movement in health care has grown significantly since the publication of two IOM reports: To Err Is Human: Building a Safer Health System and Crossing the Quality Chasm: A New Health System for the 21st Century (IOM, 2000, 2001). These reports helped shift discussions about quality away from assigning all responsibility and accountability to individual health professionals. They showed that improving quality requires an understanding of how such elements as systems and processes of care, equipment design, and organizational structure can fundamentally enhance or detract from the quality of care. Researchers also have emphasized the importance of building interprofessional teams and establishing collaborative cultures to identify and sustain continuous improvements in the quality of care (Kim et al., 2010; Knaus et al., 1986; Pronovost et al., 2008).
Access
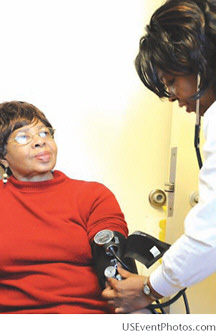
Although the Affordable Care Act (ACA) provides insurance coverage for an additional 32 million Americans, millions of Americans will still lack coverage in 2019 (CBO, 2010). Even for those with insurance, out-of-pocket expenses, such as deductibles and copays, as well as limited coverage for necessary services and medications, create financial burdens that can limit access to care (Doty et al., 2005; Himmelstein et al., 2009). Other significant barriers to access include a lack of providers who are accepting new patients, especially those covered by Medicaid; a lack of providers who offer appointments outside of typical business hours; and for some a lack of transportation to and from appointments. Also hindering access is the above-discussed rapid growth of populations with limited English proficiency (U.S. Census Bureau, 2010), as well as limited health literacy among fluent English speakers.
Value
The term “value” has different meanings in different contexts. For the purposes of this report, the committee uses the following definition: “value in health care is expressed as the physical health and sense of well-being achieved relative to the cost” (IOM Roundtable on Evidence-Based Medicine, 2008). As one of the major components of value—quality—is discussed above, this section focuses on cost.
The United States spends more than any other nation—16.2 percent of gross domestic product in 2008—on health care (CMS, 2010a). Yet this investment is not matched by superlative health care outcomes (OECD, 2010), indicating deficiencies in the value of some aspects of the health care system. Moreover, while the United States spends too much on certain aspects of health care, such as hospital services and diagnostic tests, spending on other aspects is disproportionately low. For example, public health represents less than 3 percent of health care spending (CMS, 2010b).
Health care spending is responsible for large, and ultimately unsustainable, structural deficits in the federal budget (Dodaro, 2008), and many economists believe that rising health care costs are a principal reason why wages have increased so little in recent years (Emanuel and Fuchs, 2008). However, establishing and sustaining legislated cost controls and health care savings has proven elusive. Challenges with regard to costs and spending make achieving value within the health care system difficult.
Throughout its deliberations, the committee found it useful to focus on ensuring that the health care system delivers good value rather than focusing solely on cost. Accordingly, the committee paid particular attention to high-value innovations in nursing care that provide quality, patient-centered care at a lower price. Three specific examples are featured as case studies later in this chapter.
PRINCIPLES FOR CHANGE
The challenges faced by the U.S. health care system have been described and documented in recent years by many government agencies, researchers, policy analysts, and health professionals. From this work, a consensus has begun to emerge regarding some of the fundamental principles that should guide changes to meet these challenges. Broadly, the consensus is that care in the United States must become more patient centered; primary care and prevention must play a greater role relative to specialty care; care must be delivered more often within the community setting and even in people’s homes; and care needs to be coordinated and provided seamlessly across health conditions, settings, and providers. It is also important that all providers practice to the fullest extent allowed by their education, training, and competencies and collaborate so that improvements can be achieved in both their own and each other’s performance. This section pro-
vides an overview of these shifts in thinking and practice that a growing number of health care experts believe should be at the core of any proposed health care solutions.
The Need for Patient-Centered Care
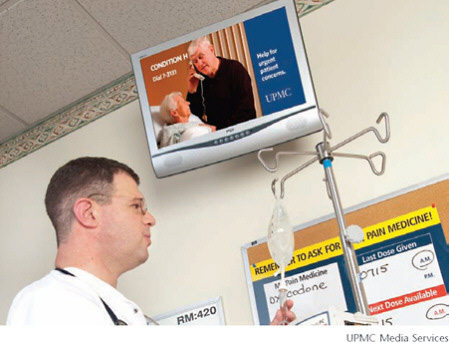
Health care research is demonstrating the benefits of reorganizing the delivery of health care services around what makes the most sense for patients (Delbanco et al., 2001; Hibbard, 2004; Sepucha et al., 2004). As outlined in Crossing the Quality Chasm, patient-centered care is built on the principle that individuals should be the final arbiters in deciding what type of treatment and care they receive (IOM, 2001). Yet practice still is usually organized around what is most convenient for the provider, the payer, or the health care organization and not for the patient. Patients are repeatedly asked, for example, to change their expectations and schedules to fit the needs of the system. They are required to provide the same information to multiple caregivers or in sequential visits to the same provider. Primary care appointments typically are not available outside of work hours. The counseling, education, and coaching needed to help patients make informed decisions have historically been given insufficient attention (Hibbard, 2004). Additionally, patients’ insurance policies often limit their choice of provider, especially if the provider is not a physician (Craven and Ober, 2009). Box 2-1 presents an example of how one health system, the University of Pittsburgh Medical Center, has implemented a truly patient-centered program.
How Patient-Centered Care Improves Quality, Access, and Value
A number of studies have linked patient-centered and quality care (Sepucha et al., 2004). For example, studies that compared surgery with watchful waiting for patients with benign prostatic hyperplasia showed how strong a role patient preference played in determining quality of life (Barry et al., 1988; Fowler et al., 1988; Wennberg et al., 1988). Likewise, involving patients more directly in the management of their own condition was found to result in significant improvements in health outcomes for individuals with insulin-dependent diabetes mellitus (Diabetes Control and Complications Trial Research Group, 1993). By 2001, so many different studies had found similar results that Crossing the Quality Chasm identified patient-centered care as one of six pillars on which a 21st-century health care system should be built (the others being safety, effectiveness, timeliness, efficiency, and equity) (IOM, 2001).
One of the hallmarks of patient-centered care is improving access to care, a key component of which is access to information. For example, a growing number of patients have greater access to their own laboratory results and diagnostic writeups about their procedures through such electronic forums as personal health records and patient portals. Many people participate in online communities to
|
BOX 2-1 Case Study: When Patients and Families Call a Code The University of Pittsburgh Medical Center Is Transforming Care at the Bedside In 2001, 18-month-old Josie King was hospitalized at Johns Hopkins Children’s Center with burns she had sustained in a bathtub accident. Josie responded well to treatment at first, but her condition quickly deteriorated. When her mother, Sorrel King, expressed concern, the staff nurses and physicians repeatedly dismissed them, and 2 days before her scheduled discharge Josie died. The cause was dehydration and a wrongly administered opioid—the result of a series of errors the hospital acknowledged. Ms. King has since devoted herself to the elimination of medical errors, founding the Josie King Foundation (www.josieking.org) and addressing clinicians, policy makers, and consumers on the importance of creating a “culture of safety.” And the need is pressing. According to a 2000 Institute of Medicine report, up to 98,000 people die from medical errors each year (IOM, 2000); nearly 10 years after that report’s publication, despite improved patient-safety systems, a 2009 report gave a grade of C+ to efforts to empower patients to prevent errors (Wachter, 2009). Tami Minnier, MSN, RN, FACHE, heard Ms. King speak in 2005, and the message was clear: if the staff had listened to her mother’s concerns, Josie would have lived. “When I came back to work the following Monday,” said Ms. Minnier, at the time chief nursing officer at the University of Pittsburgh Medical Center (UPMC) at Shadyside, “I told my chief medical officer, ‘We’re going to let patients and families call a rapid-response team’—a group of staff who are designated by the hospital to respond immediately to other staff’s requests for help with critical or emergency patient situations. He thought I was insane.”
Shadyside had been one of the first three hospitals to participate in Transforming Care at the Bedside (TCAB), an initiative of the Institute for Healthcare Improvement (IHI) and the Robert Wood Johnson Foundation, enabling front-line nurses to test their ideas for improving the safety and quality of care. Ms. Minnier called on Sorrel King to work with the nurses in Shadyside’s TCAB unit in creating what they called Condition H (or Condition Help). They interviewed patients and families about when and why they might call for a rapid-response team, consisting of a nurse administrator, a physician, a staff nurse, and a patient advocate who would convene immediately in response to a patient’s or visitor’s call. They held drills with staff, and within |
learn more about or even how to manage their own conditions. Improving access also requires delivering care in a culturally relevant and appropriate manner so that patients can contribute positively to their own care.
Fewer studies have examined the economic value of patient-centered care. One such study found that offering a nurse advice phone number and a pediatric after-hours clinic resulted in a 17 percent decrease in emergency department visits (Wilson, 2005). Yet there is no reason to believe that enhancing patient-centered care will or even should always lead to lower costs. For example, truly patient-centered approaches to care may require new programs or additional services that go beyond current standards of practice.
Nurses and Patient-Centered Care
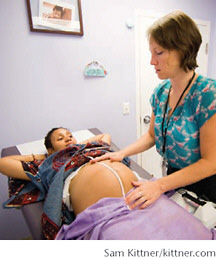
Nurses have long emphasized patient-centered care. The case study in Box 2-2 provides but one example—the patient-centered approach of midwifery care at the Family Health and Birth Center (FHBC) in Washington, DC. Through the FHBC, mothers-to-be who often have little control over their own lives develop a sense of control over one very important part of their lives. From such modest beginnings, many more hopeful futures have been launched.
The Need for Stronger Primary Care Services
Consensus is also strong on the need to make primary (rather than specialty) care a greater part of the health care system. Despite steps taken by the ACA to support the provision of primary care, however, the shortage of primary care providers is projected to worsen in the United States in the coming years (Bodenheimer and Pham, 2010; Doherty, 2010).
Primary care has been described in many ways. The IOM has defined it as “the provision of integrated, accessible health care services by clinicians who are accountable for addressing a large majority of personal health care needs, developing a sustained partnership with patients, and practicing in the context of family and community” (IOM, 1996). Starfield and colleagues identify the functions of primary care as “first-contact access for each new need; long-term person- (not disease) focused care; comprehensive care for most health needs; and coordinated care when it must be sought elsewhere” (Starfield et al., 2005). Similarly, the Government Accountability Office (GAO) has cited the following hallmarks of primary care: preventive care, care coordination for chronic illnesses, and continuity of care (Steinwald, 2008). Thus primary care is closely tied to two of the principles for change discussed below—the need to deliver more care in the community and the need for seamless, coordinated care.
How Primary Care Improves Quality, Access, and Value
Countries that build their health care systems on the cornerstone of primary care have better health outcomes and more equitable access to care than those that do not (Starfield et al., 2005). However, primary care plays a less central role in the U.S. health care system than many health policy experts believe it should (Bodenheimer, 2006; Cronenwett and Dzau, 2010; IOM, 1996; Starfield et al., 2005; Steinwald, 2008). Geographic variations nationwide illustrate the importance of primary care. Regions of the United States with a higher ratio of generalists to specialists provide more effective care at lower cost (Baicker and Chandra, 2004), and studies have shown that those states with a greater ratio of primary care providers to the general population experience lower mortality rates for all causes of death (Shi, 1992, 1994). The positive effect is more pronounced among African Americans who have access to primary care than among whites, thus indicating that this is a promising approach to decreasing health disparities (Starfield et al., 2005). Yet primary care services have been so difficult to access in parts of the United States that one in five adults has sought nonurgent care at an emergency department (IOM, 2009).
Nurses and Primary Care
Nurses with varying levels of education and preparation play important roles in primary care. Health promotion, education, and assessment are essential components of primary care that are also traditional strengths of the nursing profession; these services may be provided by either registered nurses (RNs) or advanced practice registered nurses (APRNs). RNs provide primary care services across the spectrum of health care settings—from acute care to home care to public health and community care. As visiting or home health nurses, RNs are positioned to identify new health problems or needs, such as medication education, prevention services, or nutrition counseling. In public health clinics, they may provide community assessments, developmental screenings, or disease surveillance. RNs in acute care settings may identify new health care problems and needs as they care for patients and their families. The range of possibilities for RNs providing primary care is significant, and their capacity for filling these roles is not always recognized.
APRNs, especially nurse practitioners (NPs), also provide primary care services across all levels of the health care system. In many situations, NPs provide care that is comparable in scope to that provided by primary care physicians. As discussed in Chapter 3, in many situations, APRNs are qualified to diagnose potential and actual health problems, develop treatment plans, in some case
|
BOX 2-2 Case Study: Nurse Midwives and Birth Centers The Midwifery Model of Maternity Care Gives Mothers Control and Improves Outcomes When Wendy Pugh delivered her first child at age 30 in a Washington, DC, hospital in 1999, her labor was induced—not out of medical necessity, she said, but because “there was a scheduling issue with the doctor.” She didn’t question the obstetrician’s decision at the time, but when she got pregnant again, she polled her friends and discovered that many had had cesarean sections. When she asked why, few gave medical reasons. She decided she wanted “a more organic process.”
Seven months into her second pregnancy, Ms. Pugh arrived at the Family Health and Birth Center (FHBC) in northeast Washington, DC (www.yourfhbc.org), where certified nurse midwives provide pre- and postnatal care and assist with labor and delivery with little technological intervention. Delivery takes place at a homelike freestanding birth center or at a nearby hospital, depending on the woman’s choice, her health, and such factors as whether she is homeless. The FHBC accepts Medicaid and private insurance and offers a sliding-scale fee for those ineligible for Medicaid. No one is turned away. Ruth Watson Lubic, EdD, CNM, opened the FHBC in 2000 in response to the disproportionately high rates of infant and maternal death, cesarean section, and premature birth among poor and minority women in Washington, DC. In 2009 the infant mortality rate in the city was 12.22 per 1,000 live births, far exceeding that of any state in the nation (Heron et al., 2007). Nationwide, nearly four times as many black as white infants die as a result of premature birth or low birth weight (HRSA, 2006). Dr. Lubic had already founded the first freestanding birth center in the country (in 1975 in New York City) and |
prescribe medication, and create teams of providers to help manage the needs and care of patients and their families. APRNs are educated to refer patients to physicians or other providers when necessary.
Box 2-3 illustrates how one NP provides primary care both in a school, where she is required by the school district regulations to do less than she is trained to do, and in a low-cost clinic, where she may practice to the full extent of her training and licensure. Chapter 3 examines in detail why NPs, and more broadly APRNs, are often limited by regulations in the extent of the health services they may provide.
The Need to Deliver More Care in the Community
Care in the community—defined as those places where individuals live, work, play, and study—encompasses care that is provided in such settings as community and public health centers, long-term care and assisted-living facilities, retail clinics, homes, schools, and community centers. While acute care medical facilities will always be needed, the delivery of primary care and other health services in the community must grow significantly if the U.S. health care system is to be both widely accessible and sustainable (Dodaro, 2008; Steinwald, 2008).
Along with an emphasis on primary care, a key component of providing care in the community is a strong public health infrastructure to ensure the availability of a range of services that includes prevention, education, communication, and surveillance. The public health infrastructure and workforce are vulnerable and perpetually face fiscal and political barriers. As a 2002 IOM report notes, “public health infrastructure has suffered from political neglect and from the pressure of political agendas and public opinion that frequently override empirical evidence” (IOM, 2002). The public health workforce, including public health nurses, is aging rapidly. Between 20 and 50 percent of public health workers at the local, state, and national levels are eligible to retire in the next few years (ASPH, 2008; ASTHO, 2004; Perlino, 2006). Between 2008 and 2009, health departments at the local level lost 23,000 jobs—or approximately 15 percent of their total workforce—to recession-related layoffs and attrition in 2008 and 2009 (NACCHO, 2010). The number of nurses employed in public and community health settings underwent a marked decline from 18.3 percent of the RN workforce in 2000 to 15.2 percent in 2004 to 14.2 percent in 2008 (HRSA, 2010). The case study in Box 2-4 illustrates the value of nurses working in the public health sector, where many more nurses are needed.
Providing effective care in the community will require improvements in community infrastructures, resources, and the workforce. Health care providers, including nurses, will need to form new partnerships with community leaders and have strong community care–oriented competencies, such as the ability to develop, implement, and assess culturally relevant interventions.
|
Healthy People 2010 recommendation of one nurse for every 750 healthy children. She is responsible for 2,000 children and works part time at each of the two schools.
Indeed, California is 42nd on NASN’s list of states ranked by student-to-registered nurse (RN) ratios, with 2,187 students for every school nurse (Vermont is first and Michigan is last, with 311 and 4,836 students per RN, respectively) (NASN, 2010). To fill the gap, some school districts hire non-nurse technicians, a move Ms. Sandoval said does not benefit students. She pointed out that nurses’ skills in assessment and critical thinking come into play constantly in handling the conditions that affect students’ ability to learn: obesity and chronic illness, vision deficits, behavioral problems, allergies, and asthma, to name the most common. Having moved to Southern California at age 15 from Mexico, where, she said, a school nurse would have been an unthinkable luxury, Ms. Sandoval has a particular appreciation of the school nurse’s role as child advocate. She now acts as a spokesperson for NASN’s Voices of Meningitis Campaign (www.voicesofmeningitis.org), sponsored by Sanofi Pasteur, a vaccine manufacturer. Preteens and teens are at the greatest risk for meningococcal meningitis, a preventable infection that can rapidly be fatal and is spread through utensil sharing or kissing. Through radio, television, and other venues, Ms. Sandoval teaches parents and children, in Spanish, about prevention, symptoms, and treatment. School district regulations do not permit Ms. Sandoval to use all of her skills as a nurse practitioner. She cannot diagnose or prescribe in the school, for example, even when children have symptoms of conjunctivitis or otitis media; she must refer them to other providers outside of the school. And because many of the children she sees come from uninsured families that may not have access to affordable care, she often refers families to a low-cost clinic where she works one evening a week as a nurse practitioner and can practice to the full extent of her training and licensure. Ms. Sandoval tells the story of another routine intervention, involving a seventh-grader who was falling behind in his classes. She met with the boy and checked his vision; it was quite poor, and she gave his parents a certificate for a discounted eye exam and glasses. “We cannot change the whole world,” she said. “But maybe we can change one student. And someday that student is going to go to college, and he’ll remember the school nurse who took the time to look at his eyes.” |
How Care in the Community Improves Quality, Access, and Value
In the 1990s, the state of New York pioneered quality assessment and improvement in the management of HIV/AIDS in community health clinics, drug treatment centers, and hospitals (New York State Department of Health AIDS Institute, 2003). The program proved so successful that it soon became the model for a national effort at assessing and improving treatment and care for people with HIV (IOM, 2004b). Similarly, studies have found that improving nurse-to-student ratios in public schools results in higher immunization rates, increased vision screenings and more effective follow-up, and significant gains in identifying asthma and life-threatening conditions. As more care moves from the acute to the community setting, quality measurement must expand to ensure that quality care is maintained throughout the transition.
Investments in community care can improve access and value as well. In the 1990s, the Department of Veterans Affairs (VA) began shifting its programs from the acute care to the community setting, dramatically increasing the number of veterans who were able to access care (CBO, 2009; VA, 2003) while improving health outcomes and lowering costs per patient (Asch et al., 2004; CBO, 2009; Jha et al., 2003; Kerr et al., 2004). Likewise, community health centers and nurse-managed health centers have provided quality, high-value care in many socially disadvantaged neighborhoods.
Nurses and Care in the Community
Providing care for underserved populations in community settings has long been a major goal of the nursing profession. Box 2-4 illustrates how one public health nurse provides infant care, primary care, environmental health services, and care to individuals with infectious diseases in the community. In another example, Lilian Wald founded the Visiting Nurse Service of New York (VNSNY) in 1893 to help improve the health and social outcomes of those with lesser means. Today, VNSNY is the largest nonprofit home health care agency in the United States (IOM, 2010).
A growing number of nurses are embracing technology to expand care in the community. A study conducted in Florida showed that telehealth services brought directly to patients’ communities and provided by nurses may increase access to care for children with special health care needs in rural, medically underserved parts of the state at no additional cost (Hooshmand, 2010). The alternative for these patients was to travel many miles, usually to an academic health center, to the site of a doctor’s office.
The Need for Seamless, Coordinated Care
One of the major challenges facing the U.S. health care system is its high degree of fragmentation. Nowhere is this fragmentation more evident than in the transitions patients must undergo among multiple providers or different services for a single health problem. When care is seamless, these multiple aspects of care are coordinated to enhance the quality of care and the patient’s experience of care. The ACA contains provisions that address coordination of care, but these initiatives are just the beginning of what is needed.
How Seamless, Coordinated Care Improves Quality, Access, and Value
In 2003, the IOM singled out coordination of care as indispensible to improving the quality of health care in the United States (IOM, 2003a). Likewise, the ACA highlights coordination of services as one of the required measures for reporting on the quality of care. The Medicare Payment Advisory Commission (MedPAC) also concluded that better coordination clearly improved the quality of beneficiaries’ care. Proof that care coordination saves money was less apparent in part because measuring cost savings is so difficult. Investments in care coordination for a group of people with diabetes, for example, may take a long time to demonstrate cost savings because it can take years for poor glucose control to manifest itself as stroke, myocardial infarction, and other severe complications. However, the value of preventing these outcomes, from both a quality-of-life and financial perspective, is clear.
One particularly compelling example of the multiple benefits of seamless care is the On Lok program—an initiative that began in California in the 1970s (On Lok PACEpartners, 2006). Its successes inspired a new model of care—the Program of All-Inclusive Care for the Elderly (PACE), which now serves 19,000 frail older individuals in 31 states.2 On Lok and the PACE programs that it inspired demonstrate that innovative programs that integrate care across the continuum can lead to synergistic improvements in quality, access, and value. The creativity and willingness to look beyond traditional solutions that animate these programs need to be adapted to other health care settings.
Nurses and Seamless, Coordinated Care
Coordinating care is one of the traditional strengths of the nursing profession, whether in the community or the acute care setting. For example, an interprofessional research team funded by the Robert Wood Johnson Foundation, called the Interdisciplinary Nursing Quality Research Initiative (INQRI), developed a Staff
Nurse Care Coordination model that features six nurse care coordination activities regularly performed by staff nurses in hospital settings as part of their daily activities—mobilizing, exchanging, checking, organizing, assisting, and backfilling (Lamb et al., 2008). Box 2-5 describes a program in the community setting called Living Independently for Life (LIFE), a PACE program in Pennsylvania that is led by nurse practitioners and provides interprofessional health services to low-income, frail, chronically ill older adults who are eligible for nursing home care (LIFE, 2010).
In acute care settings, care coordination is showing particular promise in efforts to reduce rehospitalizations. All 15 demonstration program sites under the Medicare Coordinated Care Demonstration program, for example, adopted interventions that relied on nurses as care coordinators (Peikes et al., 2009). Box 2-6 provides an in-depth look at the Transitional Care Model, developed by nursing researcher Mary Naylor. This model was designed to facilitate patients’ transitions within and across settings and to break the cycle of acute flare-ups of chronic illness. The protocol goes beyond usual case management and home care by employing an APRN who is proficient in comprehensive in-hospital assessment, evaluation of medications, coordination of complex care, and in-home follow-up. By collaborating with the patient, family caregivers, specialists, primary care providers, and others, this nurse works to improve the management of multiple complex chronic conditions and thus reduce readmissions.
The Need for Reconceptualized Roles for Health Professionals
Many of the roles health professionals are being called upon to fill in the evolving U.S. health care system are not technically new. Nurses, physicians, and pharmacists, for example, have educated patients, helped coordinate care, and collaborated with other clinicians for decades. What is new is the extent and the centrality of these roles. Previous IOM studies have found that systemwide changes are necessary to meet higher standards for quality care, the growing requirements of an aging population, and the need to deliver more care in the community setting. Crossing the Quality Chasm introduced the idea of the advisability of expanding the scope of practice for many health workers (IOM, 2001). Retooling for an Aging America advised that meeting the needs of the growing geriatric population would require expanding the roles of health professionals “beyond the traditional scope of practice” (IOM, 2008).
In light of these considerations, the committee concludes that nurses, in concert with other health professionals, need to adopt reconceptualized roles as care coordinators, health coaches, and system innovators. This chapter has already provided examples of nurses working as care coordinators; the following subsections elaborate on what the committee means by health coaches and system innovators. Filling these roles, whether in entry-level nursing or advanced practice, will require that nurses receive greater education and preparation in
leadership, care management, quality improvement processes, and systems thinking—a subject discussed in Chapter 4.
Nurses as Health Coaches
The committee envisions a health care system in which all individuals have a health coach who helps stay them healthy. The coach ensures that they understand why their primary care provider—whether a physician, physician assistant, or NP—has recommended a particular course of treatment. He/she coordinates patients’ care with multiple providers so that, for example, an elderly grandfather with diabetes, arthritis, and heart disease can continue to live at home and avoid costly hospitalizations. The role of health coach has much in common with case management services, but it goes even further. The coach educates family, friends, and other informal caregivers about how they can help, addressing not just physical needs but also social, environmental, mental, and emotional factors that may promote or interfere with the maintenance of health. The coach helps overcome features in the health care system that may lead to inequities in care delivery. He/she also stays involved with patients if they enter the hospital and coordinates transitional services with APRNs and other care providers after discharge. Given all these job requirements, the health coach most often will be an RN. Box 2-7 presents a case study in which baccalaureate-trained RNs serve as health coaches for women who are first-time mothers and may be at risk of abusing or neglecting their children.
Nurses as System Innovators3
One of the fundamental insights of the quality improvement movement is that all health professionals should both perform their current work well and continuously look for ways to make their performance and that of the larger system better. Or as one nurse told a physician 20 years ago in a course on health care improvement, “I see. You’re saying that I have two jobs: doing my job and making my job better” (Berwick, 2010).
The nursing profession is well positioned to produce system innovators. A few years ago, the Institute for Healthcare Improvement (IHI) launched a national project to reduce patient injuries, called the 100,000 Lives Campaign. The project translated the aims of safety and effectiveness into operational form as “bundles” of care procedures (Berwick et al., 2006; McCannon et al., 2006), such as the Central Line Bundle to prevent catheter-associated bloodstream infections. Hundreds of hospitals reported success in terms of improved patient outcomes.
|
3 |
This section draws on a paper commissioned by the committee on “Preparing Nurses for Participation in and Leadership of Continual Improvement,” by Donald M. Berwick, Institute for Healthcare Improvement (see Appendix I on CD-ROM). |
|
BOX 2-5 Case Study: Living Independently for Elders (LIFE) Nurses Supporting Older Adults to Stay in the Community In 2002, when Lillie Mashore was in her late 50s, she was diagnosed with multiple sclerosis. Just a year later her diabetes was so severe she had to be placed in intensive care. Too ill in December 2003 to return to the West Philadelphia home she shared with her husband, who had cancer, she entered a nursing home. She was greeted there with the words, “You’re going to leave here in a body bag.” But Ms. Mashore defied that prediction. In April 2005 she went home and spent the last year of her husband’s life with him. With the support of the Living Independently for Elders (LIFE) program, she is still at home, receiving help twice a day from visiting nurses and aides and attending LIFE’s adult day care center 3 days a week. “I’m limited to certain things,” Ms. Mashore, now age 66, said of her recovered independence. “But I can wash dishes. I didn’t think I could do that. I was so proud when I washed those dishes.” Ms. Mashore is one of the nearly 700 elderly Philadelphians eligible for nursing home admission who have stayed in their homes with the help of LIFE—a program that provides all primary and specialty care services to low-income, frail, chronically ill older adults (age 55 or older). About 95 percent of members are African American. Nurse practitioner–led teams include nurses, physicians, social workers, physical and occupational therapists, dieticians, nurses’ aides, and drivers. Although home care is available for LIFE members like Ms. Mashore who need help managing household tasks or medications, it is not the primary focus. Many services are provided at the LIFE adult day care center, and groups take outings, such as to Phillies baseball games or a nearby Dave and Buster’s restaurant. (Roughly 20 bed-bound members receive all LIFE services at home.) Also available are respite care for family caregivers, transportation to the center, and a “circle of care” for people with dementia. About 185 members are at the center each day.
As for outcomes, LIFE keeps nearly 90 percent of its members out of nursing homes, according to unpublished data. LIFE also reports reduced rates of falls, pressure |
 Among many services LIFE provides, routine preventive services such as measuring blood pressure enables older Philadelphia residents to stay healthy and remain in their own homes. ulcers, preventable hospitalizations, and emergency room visits among members (LIFE, 2010). LIFE is one of 72 programs in 31 states that are part of the Program for All-Inclusive Care for Elders (PACE)—a model of care begun in San Francisco in the 1970s that is now a national network offering services to elderly Medicare and Medicaid beneficiaries—and it is the only PACE program to be affiliated with a school of nursing, the University of Pennsylvania’s. (See the websites of LIFE [www.lifeupenn.org] and PACE [www.npaonline.org] for more information.) And because PACE programs receive capitated payments—per member, rather than per service provided—from government and private insurers, LIFE is both provider and payer for specific services, said Mary Austin, MSN, RN, NHA, LIFE’s chief nursing officer and chief operating officer. “If members go to the hospital or a nursing home, we pay for all of that care as well,” she said. The team makes all care decisions, including some that might seem unconventional, such as buying an air conditioner for a member with asthma. Despite potential financial barriers—some might deem the $2 million required to start a PACE program prohibitive, and some private insurers do not cover PACE services—LIFE is fiscally sound. “We operate on a shoestring, to a degree. But we operate responsibly, and we get the money we need to run the program,” said Eileen M. Sullivan-Marx, PhD, RN, FAAN, associate dean for practice and community affairs at the University of Pennsylvania School of Nursing. She also said that the state saves 15 cents on every dollar spent on LIFE members who would otherwise be in nursing homes. The program makes up about 41 percent of the nursing school’s operating budget (Sullivan-Marx et al., 2009). Ms. Mashore is quite clear that the program has strengthened her ability to care for herself. When a nurse suggested that she not use her electric wheelchair because using a manual one would strengthen her arms, Ms. Mashore was angry at first. “But I see what she’s saying,” Ms. Mashore said. “My arms are very strong. I pull my own self up in the bed. I can do things that I couldn’t do when I was in the nursing home.” |
|
BOX 2-6 Case Study: The Transitional Care Model Easing Transitions, Fostering Freedom: The Transitional Care Model “Speaks to What Nurses Really Do” Mary Manley was accustomed to her independence. Having lived for many years on her own in North Philadelphia, worked until age 74, and cared for her infant great-granddaughter in her early 80s, she was undaunted by a diagnosis of diabetes in late 2007. “I didn’t have to go to doctors too much,” she said. “I was perfectly healthy, doing anything I wanted to do—“until 2009, that is, when ‘the sickness’ came.” “The sickness” was, in fact, many chronic conditions (among them hypertension, mild cognitive impairment, coronary artery disease, and chronic obstructive pulmonary disease) and two life-threatening acute conditions. The latter conditions—pneumonia and pancolitis, an intestinal inflammation caused by Clostridium difficile, a “superbug” that is often resistant to treatment—required hospitalization. Ms. Manley received vancomycin intravenously for the C. difficile for two weeks as an inpatient. She was discharged on a Thursday afternoon with a prescription for oral vancomycin that her niece dropped off at a neighborhood pharmacy. But on Friday the pharmacy claimed not to have received the order and refused to dispense the drug. While hospitalized, Ms. Manley had met a transitional care nurse, Ellen McPartland, MSN, APRN, BC, who made a home visit on Friday. When she heard about the potentially grave delay in antibiotic therapy, she called the pharmacy immediately, demanding to speak with a supervisor. The pharmacy dispensed enough medication to get Ms. Manley through the weekend at home until the full amount could be obtained on Monday—an outcome that prevented immediate rehospitalization and may have saved Ms. Manley’s life.
According to a recent study, 20 percent of hospitalized Medicare beneficiaries are readmitted within 30 days of discharge and 34 percent within 90 days, at an estimated cost in 2004 of “$17.4 billion of the $102.6 billion in hospital payments from Medicare” (Jencks et al., 2009). Among innovations aimed at reducing rehospitalization rates, the Transitional Care Model (TCM) relies on an advanced practice registered nurse (APRN), like Ms. McPartland, who meets with the patient and family caregivers during a hospitalization to devise a plan for managing chronic illnesses (see www.transitionalcare.info). |
|
But the model involves more than discharge planning and home care, said TCM developer Mary D. Naylor, PhD, RN, FAAN, a professor of gerontology and director of the NewCourtland Center for Transitions and Health at the University of Pennsylvania. The first step is for the APRN to help the patient and family set goals during hospitalization. The nurse identifies the reasons for the patient’s instability, designs a plan of care that addresses them, and coordinates various care providers and services. The APRN then visits the home within 48 hours of discharge and provides telephone and in-person support as often as needed for up to 3 months. Assessing and counseling patients and accompanying them to medical appointments are aimed at helping patients and caregivers to learn the early signs of an acute problem that might require immediate help and to better manage patients’ health care. Also essential is ensuring the presence of a primary care provider. “Patients might have six or seven specialists, but nobody who’s taking care of the big picture,” Dr. Naylor said. In three randomized controlled trials of Medicare beneficiaries with multiple chronic illnesses, use of the TCM lengthened the period between hospital discharge and readmission or death and resulted in a reduction in the number of rehospitalizations (Naylor et al., 1994, 1999, 2004). The average annual savings was $5,000 per patient. Until now, transitional care has not been covered by Medicare and private insurers. But the Affordable Care Act sets aside $500 million to fund pilot projects on transitional care services for “high-risk” Medicare beneficiaries (such as those with multiple chronic conditions and hospital readmissions) at certain hospitals and community organizations over a 5-year period. The secretary of the Department of Health and Human Services is authorized to remove the pilot status of this program if it demonstrates cost savings.  Mary Manley relied heavily on her nurse, Ellen McPartland, during her transition from the hospital back to home. Now age 85, Ms. Manley takes eight medications regularly, and with the help of Ms. McPartland and a new primary care team is spending more time with family and attending church again. Said Ms. McPartland, “Of all the roles I have had in nursing, this brings it all together. To see them going from so sick to back home and stable—the Transitional Care Model speaks to what nurses really do.” |
Recurrent patterns of success included actively engaged nurses supported in standardizing their own processes of care according to the IHI bundles and empowered and supported in monitoring and enforcing those standards across disciplines, including with their physician colleagues (Berwick et al., 2006). Encouraged to innovate locally to adapt changes to local contexts, nurses proved the ideal leaders for changing care systems and raising the bar on results.
One new role for nurses that taps their potential as innovators is the clinical nurse leader (CNL), an advanced generalist clinician role designed to improve clinical and cost outcomes for specific groups of patients. Responsible for coordinating care and in some cases actively providing direct care in complex situations, the CNL has the responsibility for translating and applying research findings to design, implement, and evaluate care plans for patients (AACN, 2007). This new role has been adopted by the VA system.
The Need for Interprofessional Collaboration
The need for greater interprofessional collaboration has been emphasized since the 1970s. Studies have documented, for example, the extent to which poor communication and lack of respect between physicians and nurses lead to harmful outcomes for patients (Rosenstein and O’Daniel, 2005; Zwarenstein et al., 2009). Conversely, a growing body of evidence links effective teams to better patient outcomes and more efficient use of resources (Bosch et al., 2009; Lemieux-Charles and McGuire, 2006; Zwarenstein et al., 2009), while good working relationships between physicians and nurses have been cited as a factor in improving the retention of nurses in hospitals (Kovner et al., 2007). As the delivery of care becomes more complex across a wide range of settings, and the need to coordinate care among multiple providers becomes ever more important, developing well-functioning teams becomes a crucial objective throughout the health care system.
Differing professional perspectives—with attendant differences in training and philosophy—can be beneficial. Nurses are taught to treat the patient not only from a disease management perspective but also from psychosocial, spiritual, and family and community perspectives. Physicians are experts in physiology, disease pathways, and treatment. Social workers are trained in family dynamics. Occupational and physical therapists focus on improving the patient’s functional capacity. Licensed practical nurses provide a deeply ground-level perspective, given their routine of measuring vital signs and assisting patients in feeding, bathing, and movement. All these perspectives can enhance patients’ well-being—provided the various professionals keep the patient and family at the center of their attention.
Finding the right balance of skills and professional expertise is important under the best of circumstances; in a time of increasing financial constraints, personnel shortages, and the growing need to provide care across multiple settings, it is crucial. Care teams need to make the best use of each member’s education,
|
BOX 2-7 Case Study: The Nurse–Family Partnership Nurses Visit the Homes of First-Time At-Risk Mothers, and the Results Are Wide-Ranging In 2007 Crystalon Rodrigue, a recent high school graduate living in St. James, Louisiana, had an adverse reaction to an injectable contraceptive. She discontinued it and soon got pregnant. She was 19 years old and unemployed and living with her mother, and her relationship with her boyfriend was faltering. She turned to the state department of health; was referred to the Nurse–Family Partnership (NFP); and met “Miss Tina,” a nurse who visited her at home. “In the beginning of my pregnancy, and maybe all throughout, I was a little stressed out,” the 21-year-old Ms. Rodrigue said recently. “I was depressed because I was having relationship problems with my child’s father. Miss Tina helped me….” Ms. Rodrigue was interrupted by the chatter of her 19-month-old daughter, Nalayia, who was learning to read, her mother said with pride. Then she continued, “Miss Tina helped me to think about myself.” It was a quiet, almost offhand remark, but it represents the kind of shift in attitude that the NFP has helped foster among young women for more than 30 years. Now active in 375 counties in 29 states, the NFP sends registered nurses (RNs), usually with baccalaureate degrees, into the homes of at-risk, low-income, firsttime mothers for 64 planned visits over the course of a pregnancy and the child’s first 2 years.
Improving the lives of children is the chief aim of the NFP, yet the interventions target mothers. The |
|
nurse discusses options for the mother’s continued education and economic self-sufficiency; supports her in reducing or quitting smoking or drinking; teaches her about child development, nonviolent discipline, and breastfeeding; and helps her make decisions about family planning. The nurse does this by engaging the mother in a relationship that provides a model for interactions with others. The child’s father and other family members are encouraged to participate. “We don’t look for the great big change,” said Luwana Marts, BSN,  Tina Becnel, a nurse who provides home visits, helped Crystalon Rodrigue during her pregnancy and continued through her daughter Nalayia’s second birthday. |
|
RN, regional nurse consultant for the NFP in Louisiana. “A part of the model is that only a small change is necessary. So if a client never quits smoking but she doesn’t smoke in the presence of her child, that’s a plus.” In case-controlled, longitudinal trials conducted among racially and ethnically diverse populations—beginning in 1977 in Elmira, New York, and continuing in Memphis, Tennessee, and Denver, Colorado—the NFP has shown reductions in unintended second pregnancies and increases in mothers’ employment. Children of mothers visited by nurses are less likely to be abused and by age 15 to be arrested. (For links to these and other studies of the NFP, visit www.nursefamilypartnership.org/provenresults/published-research.) The per-child cost is $9,118; for the highest-risk children, a return of $5.70 per dollar spent is realized (Karoly et al., 2005). Several models of home visitation are in use, but the NFP relies on trained RNs for its interventions. A 2002 study compared home visits by untrained “paraprofessionals” and nurses. On almost all measures, the nurses produced far stronger outcomes (Olds et al., 2002). “People trust nurses,” said Ruth A. O’Brien, PhD, RN, FAAN, professor of nursing at the University of Colorado in Denver and an author of the study. “Low-income, minority people who have not had a lot of trust in the health care system might be willing to let a nurse in the door.” Barriers to implementation include the fact that states use various sources to fund the NFP, and in some the funding is limited. The Affordable Care Act mandates that $1.5 billion be spent over 5 years on home visitation programs for at-risk mothers and infants*—substantially less than the $8.5 billion over 10 years that President Obama requested in his 2010 budget (OMB, 2010). While the act establishes a federal agency to oversee such home visitation programs, it does not specify that nurses provide the care. Also, some municipalities increase the nurse’s caseload beyond the recommended 25, diminishing the intensity and effectiveness of the interventions. For her part, Ms. Rodrigue is looking ahead. She had completed a certified nursing assistant program while pregnant and will soon start nursing school, in which she had enrolled but quit shortly after high school. “I wasn’t ready for it,” she said. “But now I have a child and I know what to expect. I feel like I’m ready. I want to better myself.” |
skill, and expertise, and all health professionals need to practice to the full extent of their license and education. Where the competency and skills of doctors and nurses safely overlap, it makes sense to rely on nurses to provide many of those services. Similarly, where the competency and skills of RNs and licensed practical or vocational nurses safely overlap, it makes sense to rely on the latter—or as the case may be, nurses’ aides—to provide many of those services. In this way, more specialized skills and competencies are appropriately reserved for the most complex needs. This type of skill balancing should not, however, be used as a means of cutting costs by indiscriminately replacing more skilled with less skilled clinicians.
CONCLUSION
Nurses are well positioned to help meet the evolving needs of the health care system. They have vital roles to play in achieving patient-centered care; strengthening primary care services; delivering more care in the community; and providing seamless, coordinated care. They also can take on reconceptualized roles as health care coaches and system innovators. In all of these ways, nurses can contribute to a reformed health care system that provides safe, patient-centered, accessible, affordable care. Their ability to make these contributions, however, will depend on a transformation of nursing practice, education, and leadership, as discussed in Chapters 3, 4, and 5, respectively. Nurses must remodel the way they practice and make clinical decisions. They must rethink the ways in which they teach nurses how to care for people. They must rise to the challenge of providing leadership in rapidly changing care settings and in an evolving health care system. In short, nurses must expand their vision of what it means to be a nursing professional. At the same time, society must amend outdated regulations, attitudes, policies, and habits that unnecessarily restrict the innovative contributions the nursing profession can bring to health care.
REFERENCES
AACN (American Association of Colleges of Nursing). 2007. White paper on the education and role of the clinical nurse leader. Washington, DC: AACN.
Asch, S. M., E. A. McGlynn, M. M. Hogan, R. A. Hayward, P. Shekelle, L. Rubenstein, J. Keesey, J. Adams, and E. A. Kerr. 2004. Comparison of quality of care for patients in the Veterans Health Administration and patients in a national sample. Annals of Internal Medicine 141(12):938-945.
ASPH (Association of Schools of Public Health). 2008. Confronting the public health workforce crisis. Washington, DC: ASPH.
ASTHO (Association of State and Territorial Health Officials). 2004. State public health employee worker shortage report: A civil service recruitment and retention crisis. Washington, DC: ASTHO.
Baicker, K., and A. Chandra. 2004. Medicare spending, the physician workforce, and beneficiaries’ quality of care. Health Affairs Suppl Web Exclusives:W184-197.
Barry, M. J., A. G. Mulley, Jr., F. J. Fowler, and J. W. Wennberg. 1988. Watchful waiting vs. immediate transurethral resection for symptomatic prostatism. The importance of patients’ preferences. JAMA 259(20):3010-3017.
Berwick, D. M. 2010. Preparing nurses for participation in and leadership of continual improvement. Paper commissioned by the Committee on the RWJF Initiative on the Future of Nursing, at the IOM (see Appendix I on CD-ROM).
Berwick, D. M., D. R. Calkins, C. J. McCannon, and A. D. Hackbarth. 2006. The 100,000 lives campaign: Setting a goal and a deadline for improving health care quality. JAMA 295(3):324-327.
Bodenheimer, T. 2006. Primary care—will it survive? New England Journal of Medicine 355(9): 861-864.
Bodenheimer, T., and H. H. Pham. 2010. Primary care: Current problems and proposed solutions. Health Affairs 29(5):799-805.
Bosch, M., M. J. Faber, J. Cruijsberg, G. E. Voerman, S. Leatherman, R. P. Grol, M. Hulscher, and M. Wensing. 2009. Review article: Effectiveness of patient care teams and the role of clinical expertise and coordination: A literature review. Medical Care Research and Review 66(6 Suppl):5S-35S.
CBO (Congressional Budget Office). 2009. Quality initiatives undertaken by the Veterans Health Administration. Washington, DC: CBO.
CBO. 2010. Cost estimates for the 111th Congress: H.R. 4872, Reconciliation Act of 2010 (final health care legislation). http://www.cbo.gov/costestimates/CEBrowse.cfm (accessed June 28, 2010).
CDC (Centers for Disease Control and Prevention). 2010. Chronic diseases and health promotion. http://www.cdc.gov/chronicdisease/overview/index.htm (accessed July 23, 2010).
CMS (Centers for Medicare and Medicaid Services). 2010a. National health expenditure data: Historical. http://www.cms.gov/NationalHealthExpendData/02_NationalHealthAccountsHistorical.asp#TopOfPage (accessed May 17, 2010).
CMS. 2010b. Table 2. National health expenditures aggregate amounts and average annual percent change, by type of expenditure: Selected calendar years 1960-2008. Available from National Health Expenditure Data: Historical. https://www.cms.gov/NationalHealthExpendData/02_NationalHealthAccountsHistorical.asp#TopOfPage (accessed August 29, 2010).
Craven, G., and S. Ober. 2009. Massachusetts nurse practitioners step up as one solution to the primary care access problem: A political success story. Policy, Politics, & Nursing Practice 10(2):94-100.
Cronenwett, L., and V. J. Dzau. 2010. Who will provide primary care and how will they be trained?, Proceedings of a conference sponsored by the Josiah Macy, Jr. Foundation. Edited by B. Culliton and S. Russell. Durham, NC: Josiah Macy, Jr. Foundation.
Delbanco, T., D. M. Berwick, J. I. Boufford, S. Edgman-Levitan, G. Ollenschlager, D. Plamping, and R. G. Rockefeller. 2001. Healthcare in a land called peoplepower: Nothing about me without me. Health Expectations 4(3):144-150.
DeVol, R., A. Bedroussian, A. Charuworn, A. Chatterjee, I. Kim, S. Kim, and K. Klowden. 2007. An unhealthy America: The economic burden of chronic disease. Santa Monica, CA: The Milken Institute.
Diabetes Control and Complications Trial Research Group. 1993. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus New England Journal of Medicine 329(14):977-986.
Dodaro, G. L. 2008. Long-term fiscal outlook: Long-term federal fiscal challenge driven primarily by health care. Washington, DC: GAO.
Doherty, R. B. 2010. The certitudes and uncertainties of health care reform. Annals of Internal Medicine 152(10):679-682.
Doty, M. M., J. N. Edwards, and A. L. Holmgren. 2005. Seeing red: Americans driven into debt by medical bills: Results from a national survey. New York: The Commonwealth Fund.
Emanuel, E. J., and V. R. Fuchs. 2008. Who really pays for health care? The myth of “Shared responsibility.” JAMA 299(9):1057-1059.
Fisher, E., D. Goodman, J. Skinner, and K. Bronner. 2009. Health care spending, quality, and outcomes: More isn’t always better. A Dartmouth Atlas project topic brief. Hanover, NH: The Dartmouth Atlas.
Fowler, F. J., Jr., J. E. Wennberg, R. P. Timothy, M. J. Barry, A. G. Mulley, Jr., and D. Hanley. 1988. Symptom status and quality of life following prostatectomy. JAMA 259(20):3018-3022.
Goldman, D. P., and E. A. McGlynn. 2005. U.S. Health care: Facts about cost, access, and quality. Santa Monica, CA: RAND.
Hassmiller, S. B., and L.B. Bolton (eds.). 2009. Transforming care at the bedside: Paving the way for change. American Journal of Nursing 109(11):3-80.
Hatem, M., J. Sandall, D. Devane, H. Soltani, and S. Gates. 2008. Midwife-led versus other models of care for childbearing women. Cochrane Database of Systematic Reviews (4):CD004667.
Heron, M., P. Sutton, J. Xu, S. Ventura, D. Strobino, and B. Guyer. 2007. Annual summary of vital statistics. Pediatrics 125(1):4-15.
HHS (Health and Human Services) Office of Minority Health. 2007. National standards on culturally and linguistically appropriate services. http://minorityhealth.hhs.gov/templates/browse.aspx?lvl=2&lvlID=15 (accessed June 30, 2010).
Hibbard, J. H. 2004. Moving toward a more patient-centered health care delivery system. Health Affairs Suppl Web Exclusives:VAR133-135.
Himmelstein, D. U., D. Thorne, E. Warren, and S. Woolhandler. 2009. Medical bankruptcy in the United States, 2007: Results of a national study. American Journal of Medicine 122(8):741-746.
Hodnett, E. D., S. Gates, G. Hofmeyr, and C. Sakala. 2007. Continuous support for women during childbirth. Cochrane Database Systematic Reviews 7(3).
Hooshmand, M. 2010. Comparison of telemedicine to traditional face-to-face care for children with special health care needs: Analysis of cost, caring, and family-centered care. School of Nursing and Health Studies, University of Miami, Coral Gables, FL.
HRSA (Health Resource and Services Administration). 2006. Evidence of trends, risk factors, and intervention strategies: A report from the Healthy Start national evaluation 2006. Rockville, MD: HRSA.
HRSA. 2010. The registered nurse population: Findings from the 2008 National Sample Survey of Registered Nurses. Rockville, MD: HRSA.
IOM (Institute of Medicine). 1996. Primary care: America’s health in a new era. Washington, DC: National Academy Press.
IOM. 2000. To err is human: Building a safer health system. Washington, DC: National Academy Press.
IOM. 2001. Crossing the quality chasm: A new health system for the 21st century. Washington, DC: National Academy Press.
IOM. 2002. The future of the public’s health in the 21st century. Washington, DC: The National Academies Press.
IOM. 2003a. Priority areas for national action: Transforming health care quality. Washington, DC: The National Academies Press.
IOM. 2003b. Unequal treatment: Confronting racial and ethnic disparities in health care. Washington, DC: The National Academies Press.
IOM. 2004a. Health literacy: A prescription to end confusion. Washington, DC: The National Academies Press.
IOM. 2004b. Measuring what matters: Allocation, planning, and quality assessment for the Ryan White CARE Act. Washington, DC: The National Academies Press.
IOM. 2008. Retooling for an aging America: Building the health care workforce. Washington, DC: The National Academies Press.
IOM. 2009. The healthcare imperative: Lowering costs and improving outcomes: Brief summary of a workshop Washington, DC: The National Academies Press.
IOM. 2010. A summary of the December 2009 Forum on the Future of Nursing: Care in the community. Washington, DC: The National Academies Press.
IOM Roundtable on Evidence-Based Medicine. 2008. Learning healthcare system concepts, v. 2008. Washington, DC: The National Academies Press.
Jacobson, J. 2009. School nurses nationwide respond to influenza A (H1N1) outbreaks. American Journal of Nursing 109(6):19.
Jencks, S. F., M. V. Williams, and E. A. Coleman. 2009. Rehospitalizations among patients in the Medicare fee-for-service program. New England Journal of Medicine 360(14):1418-1428.
Jha, A. K., J. B. Perlin, K. W. Kizer, and R. A. Dudley. 2003. Effect of the transformation of the Veterans Affairs health care system on the quality of care. New England Journal of Medicine 348(22):2218-2227.
Joint Commission. 2007. What did the doctor say?: Improving health literacy to protect patient safety. Oak Brook, IL: Joint Commission.
Karoly, L. A., M. R. Killburn, and J. S. Cannon. 2005. Early childhood interventions: Proven results, future promise. Arlington, VA: RAND Corporation.
Kerr, E. A., R. B. Gerzoff, S. L. Krein, J. V. Selby, J. D. Piette, J. D. Curb, W. H. Herman, D. G. Marrero, K. M. Narayan, M. M. Safford, T. Thompson, and C. M. Mangione. 2004. Diabetes care quality in the Veterans Affairs health care system and commercial managed care: The triad study. Annals of Internal Medicine 141(4):272-281.
Kim, M. M., A. E. Barnato, D. C. Angus, L. A. Fleisher, and J. M. Kahn. 2010. The effect of multidisciplinary care teams on intensive care unit mortality. Archives of Internal Medicine 170(4):369-376.
Knaus, W. A., E. A. Draper, D. P. Wagner, and J. E. Zimmerman. 1986. An evaluation of outcome from intensive care in major medical centers. Annals of Internal Medicine 104(3):410-418.
Kovner, C. T., C. S. Brewer, S. Fairchild, S. Poornima, H. Kim, and M. Djukic. 2007. Newly licensed RNs’ characteristics, work attitudes, and intentions to work. American Journal of Nursing 107(9):58-70; quiz 70-51.
Lamb, G., M. Schmitt, P. Edwards, F. Sainfort, I. Duva, and M. Higgins. 2008 October 2-4. Measuring staff nurse care coordination in the hospital. Paper presented at National State of the Science Congress on Nursing Research, Washington, DC.
Lemieux-Charles, L., and W. L. McGuire. 2006. What do we know about health care team effectiveness? A review of the literature. Medical Care Research and Review 63(3):263-300.
LIFE (Living Independently for Elders). 2010. LIFE receives innovative care model award. http://www.lifeupenn.org/innovative%20care%20models%20award.pdf (accessed March 28, 2010.
Matthews, S. 2009. Channeling grief into action: Creating a culture of safety conference call, February 25, 2009, Hosted by Institute for Healthcare Improvement.
McCannon, C. J., M. W. Schall, D. R. Calkins, and A. G. Nazem. 2006. Saving 100,000 lives in US hospitals. BMJ 332(7553):1328-1330.
NACCHO (National Association of County and City Health Officials). 2010. LHD budget cuts and job losses. http://www.naccho.org//topics/infrastructure/lhdbudget/index.cfm (accessed July 2, 2010).
NASN (National Association of School Nurses). 2010. Healthy children learn better! School nurses make a difference. Silver Spring, MD: NASN. Available from http://www.nasn.org/Portals/0/about/2009_press_room_faq.pdf.
Naylor, M. D., D. Brooten, R. Jones, R. Lavizzo-Mourey, M. Mezey, and M. Pauly. 1994. Comprehensive discharge planning for the hospitalized elderly. A randomized clinical trial. Annals of Internal Medicine 120(12):999-1006.
Naylor, M. D., D. Brooten, R. Campbell, B. S. Jacobsen, M. D. Mezey, M. V. Pauly, and J. S. Schwartz. 1999. Comprehensive discharge planning and home follow-up of hospitalized elders: A randomized clinical trial. JAMA 281(7):613-620.
Naylor, M. D., D. A. Brooten, R. L. Campbell, G. Maislin, K. M. McCauley, and J. S. Schwartz. 2004. Transitional care of older adults hospitalized with heart failure: A randomized, controlled trial. Journal of the American Geriatrics Society 52(5):675-684.
New York State Department of Health AIDS Institute. 2003. Clinical management of HIV infection: Quality of care performance in New York State 1999-2001. Albany, NY: New York State Department of Health.
OECD (Organisation for Economic Co-operation and Development). 2010. OECD health data 2010—frequently requested data. http://www.oecd.org/document/16/0,3343,en_2649_34631_2085200_1_1_1_1,00.html (accessed July 21, 2010).
Olds, D. L., J. Robinson, R. O’Brien, D. W. Luckey, L. M. Pettitt, C. R. Henderson, Jr., R. K. Ng, K. L. Sheff, J. Korfmacher, S. Hiatt, and A. Talmi. 2002. Home visiting by paraprofessionals and by nurses: A randomized, controlled trial. Pediatrics 110(3):486-496.
OMB (Office of Management and Budget). 2010. President Obama’s fiscal 2010 budget. http://www.whitehouse.gov/omb/fy2010_key_education (accessed March 27, 2010).
On Lok PACEpartners. 2006. History. http://www.pacepartners.net/history.php (accessed August 20, 2010).
Peikes, D., A. Chen, J. Schore, and R. Brown. 2009. Effects of care coordination on hospitalization, quality of care, and health care expenditures among Medicare beneficiaries: 15 randomized trials. JAMA 301(6):603-618.
Perlino, C. M. 2006. The public health workforce shortage: Left unchecked, will it be protected? Washington, DC: APHA.
Pronovost, P. J., S. M. Berenholtz, C. Goeschel, I. Thom, S. R. Watson, C. G. Holzmueller, J. S. Lyon, L. H. Lubomski, D. A. Thompson, D. Needham, R. Hyzy, R. Welsh, G. Roth, J. Bander, L. Morlock, and J. B. Sexton. 2008. Improving patient safety in intensive care units in Michigan. Journal of Critical Care 23(2):207-221.
Rosenstein, A. H., and M. O’Daniel. 2005. Disruptive behavior and clinical outcomes: Perceptions of nurses and physicians. American Journal of Nursing 105(1):54-64; quiz 64-55.
Sepucha, K. R., F. J. Fowler, Jr., and A. G. Mulley, Jr. 2004. Policy support for patient-centered care: The need for measurable improvements in decision quality. Health Affairs Suppl Web Exclusives:VAR54-62.
Shi, L. 1992. The relationship between primary care and life chances. Journal of Health Care for the Poor and Underserved 3(2):321-335.
Shi, L. 1994. Primary care, specialty care, and life chances. International Journal of Health Services 24(3):431-458.
Starfield, B., L. Shi, and J. Macinko. 2005. Contribution of primary care to health systems and health. The Milbank Quarterly 83(3):457-502.
Steinwald, A. B. 2008. Primary care professionals: Recent supply trends, projections, and valuation of services. Washington, DC: GAO.
Sullivan-Marx, E., C. Bradway, and J. Barnsteiner. 2009. Innovative collaborations: A case study for academic owned nursing practice. Journal of Nursing Scholarship 42(1):50-57.
U.S. Census Bureau. 2003. Language use and English-speaking ability: 2000. Washington, DC: U.S. Census Bureau.
U.S. Census Bureau. 2008. An older and more diverse nation by midcentury. http://www.census.gov/newsroom/releases/archives/population/cb08-123.html (accessed July 9, 2010).
U.S. Census Bureau. 2010. New Census Bureau report analyzes nation’s linguistic diversity: Population speaking a language other than English at home increases by 140 percent in past three decades. http://www.census.gov/newsroom/releases/archives/american_community_survey_acs/cb10cn58.html (accessed June 30, 2010).
VA (Department of Veterans Affairs). 2003. VHA vision 2020. Washington, DC: VA.
Wachter, R. M. 2009. Patient safety at ten: Unmistakable progress, troubling gaps. Health Affairs 29(1):165-173.
Wennberg, J. E., A. G. Mulley, Jr., D. Hanley, R. P. Timothy, F. J. Fowler, Jr., N. P. Roos, M. J. Barry, K. McPherson, E. R. Greenberg, D. Soule, T. Bubolz, E. Fisher, and D. Malenka. 1988. An assessment of prostatectomy for benign urinary tract obstruction. Geographic variations and the evaluation of medical care outcomes. JAMA 259(20):3027-3030.
Wilson, C. F. 2005. Community care of North Carolina: Saving state money and improving patient care. North Carolina Medical Journal 66(3):229-233.
Xu, X., J. R. Lori, K. A. Siefert, P. D. Jacobson, and S. B. Ransom. 2008a. Malpractice liability burden in midwifery: A survey of Michigan certified nurse-midwives. Journal of Midwifery & Women’s Health 53(1):19-27.
Xu, X., K. A. Siefert, P. D. Jacobson, J. R. Lori, and S. B. Ransom. 2008b. The effects of medical liability on obstetric care supply in Michigan. American Journal of Obstetrics and Gynecology 198(2):205, e201-e209.
Zwarenstein, M., J. Goldman, and S. Reeves. 2009. Interprofessional collaboration: Effects of practice-based interventions on professional practice and healthcare outcomes. Cochrane Database of Systematic Reviews (3):CD000072.