Appendix C
Workshop Report from the Health Literacy Annual Research Conference
Conference Date: October 19–20, 2009
Presented by Michael Paasche-Orlow, M.D., M.A., M.P.H.
Boston University School of Medicine, Department of Medicine, Section of General Internal Medicine, Boston, Massachusetts
The Health Literacy Annual Research Conference (HARC) is an interdisciplinary meeting for investigators dedicated to health literacy research. Our aim is to attract a full range of investigators engaged in health literacy research including those involved in a broad array of public health, health services, epidemiology, translational, and interventional research activities.
The first HARC took place in October 2009 at the National Academy of Sciences Building. This meeting was coordinated with the assistance of Rose Martinez on behalf of the Institute of Medicine Roundtable on Health Literacy and sponsored by a grant from the National Center on Minority Health and Health Disparities (NCMHD), Project Officer - Robert Netty, with additional significant support from the Agency for Healthcare Research and Quality (AHRQ), Project Officer - Cindy Brach. Additional coordination and support was provided by Helen Meissner, of the Office of Behavioral and Social Sciences Research (OBSSR) as well as the National Institute of Biomedical Imaging & Bioengineering (NIBIB), Project Officer - John Haller and the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), Project Officer - Lynne Haverkos. Principal Investigator Michael Paasche-Orlow, MD, MPH, 1 R13 MD003392.
*-*-*-*-*
A second year of funding from the National Center on Minority Health and Health Disparities (NCMHD), Project Officer - Robert Netty, with additional significant support from the Agency for Healthcare Research and Quality (AHRQ), Project Officer - Cindy Brach, has been secured.
HARC II will take place October 18–19, 2010, at the Hyatt Regency, Bethesda, MD. For more information please visit the HARC II website: http://www.bumc.bu.edu/healthliteracyconference/.
It will be an opportunity to advance the field of health literacy, a method to raise the quality of our research, and a venue for professional development.
Table of Contents
I.
Executive Summary
The HARC conference took place over 2 full days in October 2009 and highlighted areas of important research advancement as well as important lacunae in the field. A keynote address by David Baker, MD, MPH examined the role health literacy in patient education and a keynote address by Anne Beal, MD, MPH, focused on the role of health literacy in health disparities. There were four panels of invited speakers dealing with (1) measurement; (2) health literacy and verbal interactions; (3) health information technology interventions; and (4) organizational assessment and change. Current gaps in the research were examined by invited speakers and in breakout sessions relating to Public Health Approaches to Health Literacy, Health Disparities and Health Literacy, and Health Information Technology. An additional 62 posters and 12 oral abstracts were presented, making this clearly the most numerous Health Literacy research presentations in any single meeting to date. The meeting
was attended by an interdisciplinary array of investigators representing the strong majority of health literacy investigators in the United States.
This report describes the rationale for having a Health Literacy Annual Research Conference, the goals for the meeting, and presents the findings of the meeting. In addition, specific discussion is presented regarding two of the recurring themes of the meeting, namely, the Role of Health Literacy Research in Health Disparities and the Role of Information Technology in Health Literacy Research.
Details from the 2009 conference, including panel presentations, accepted abstracts, and evaluation results, can be found on the conference website at http://www.bumc.bu.edu/healthliteracyconference/2009-conference/.
II.
Why the Health Literacy Annual Research Conference (HARC) Was Initiated
Introduction
The National Institutes of Health (NIH) has defined health literacy as the “degree to which individuals have the capacity to obtain, process and understand basic health information and services needed to make appropriate health decisions.”1 According to this definition, health literacy relates to an individual’s possession of requisite skills for making health-related decisions. As highlighted in the IOM report, health literacy is dependent on the complexity of the tasks required.2 This means that when we refer to health literacy, we consider not only a patient’s literacy and numeracy skills, but also the literacy burden imposed by health care systems and communities in which care-giving and self-management support take place.3,4
Unfortunately, many of the tasks health consumers need to undertake are very complicated. Over the past 50 years, basic literacy has improved in the United States. However, over 90 million American adults struggle to read and understand basic health materials.5 Thus, given the high literacy demands required to function successfully as a patient, it is no wonder that approximately 36% of US adults have only basic or even below basic health literacy skills.6 This problem is not uniformly distributed in society; the prevalence of limited health literacy is highest among patients who are older and are from ethnic and racial minorities.7
The literature on health literacy also exposes ways in which the health care system exacerbates the impact of underlying educational and income disparities. Indeed, health literacy is emerging as an important causal factor for racial and ethnic health disparities.8-18 The implications of this
research should be understood as a challenge to the basic justice of a health care system organized for the most highly educated and powerful members of our society.19
The relationship between limited literacy and adverse health outcomes has been well documented, and seminal reports about the problem of limited health literacy have been issued by the Institute of Medicine, 20 Agency for Healthcare Research and Quality, 21 American Medical Association,22 and Joint Commission on the Accreditation of Hospital Organizations23 among others. Each of these reports advocates further research to develop an effective response within health care systems to address the problem and research in health literacy has begun to flourish.
An important next step for cultivating this emerging research field is to create a national professional interdisciplinary home for investigators dedicated to health literacy research. Opportunities are available, but only within special interest groups that have either formed in more specialized meetings or that sporadically address health literacy (e.g., National Society of General Internal Medicine Annual Meeting, National American Public Health Association Annual Meeting, Academy Health, and the International Conference on Communication in Health Care). There are, in addition, multiple Health Literacy meetings (e.g., the Annual Institute for Healthcare Advancement Conference) which serve primarily an educational agenda for attendees who are, by and large, not health literacy investigators.
Timeliness
A Pubmed search using the Health Literacy topic specific query under the Pubmed tools tab (see: http://www.nlm.nih.gov/services/health_literacy.html) reveals the tremendous growth of research in this field: in the 5 years between 1986 and 1990 there are 129 references in Pubmed; in the years 1991 to 1995 this search yields 306 references; between 1996 and 2000 there are 307 references; from 2001 to 2005 there are 602 references from this search; and in the current interval, between 2006 and 6/6/2010, there are already 1,576 references returned by this search (see Figure). As striking as this may seem, it is also important to note that this collection of references is dominated by observational research, indeed, fewer than 8% of these citations are tagged as trials as seen in the figure below.
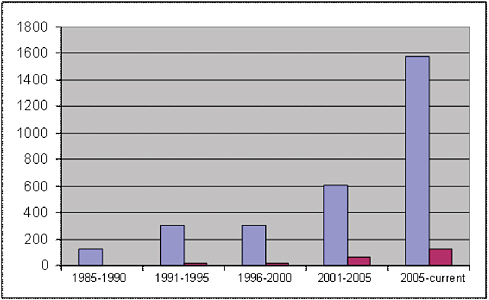
Light bars represent all citations identified by Health Literacy topic specific query. Dark bars represent the subset of these citations identified as trials, clinical trials, or randomized controlled trials.
Despite the rapid growth in the field, driven in large part by the availability of NIH and AHRQ funding, there is currently no national research venue dedicated to the promotion of health literacy as a field of inquiry. Health literacy research is an interdisciplinary endeavor and could greatly benefit at this point from a recurring national research oriented interdisciplinary meeting.
III.
Main Conference Goals
Establishing an interdisciplinary research home for health literacy investigators would be useful for reasons that relate to (1) professional development, (2) advancing the science of health literacy research, and (3) promotion of interdisciplinary research.
1.
Professional Development:
Such a venue could help attract young investigators and new ideas and methods to the field. An annual meeting could be a source and meeting place for mentoring and be an opportunity to establish and advance a career in the field of health literacy. The budget and meeting schedule reflect these priorities by setting aside money to support young investigators and students and by dedicating time at the meeting for one-on-one mentoring sessions and meetings with program officers.
2.
Advancing the Science:
An annual meeting of health literacy researchers could promote the discourse in this field of inquiry. For example, significant controversy exists within the field regarding core definitional issues. This is having a big influence in the arena of measurement. There is broad agreement that current health literacy instruments are insufficient in various ways for many investigators. Investigators have been developing and evaluating new instruments that reflect their understanding of what is or is not part of the concept health literacy. The proposed conferences will allow investigators to more fully debate these issues, more rapidly vet emerging measurement ideas, share early-stage instruments to allow validation activities in various populations, and disseminate newly validated instruments.
3.
Promotion of Interdisciplinary Research:
Establishing a collegial network could help promote multisite research. The field has entered into an exciting and creative period of inquiry in which a wide array of interventions is being evaluated. The varied nature of the research that is relevant to the problem of health literacy makes an interdisciplinary conference valuable; bringing such a group of researchers together will provide the milieu for new admixtures, new collaborations, and further creativity. Productive collaboration will also support professional development of the health literacy investigator workforce.
Currently, the majority of health literacy research is conducted in the United States. However, health literacy research is being pursued in other countries. In 2009, Drs. Paasche-Orlow and Wolf served as guest editors for a special issue on health literacy of the journal Patient Education and Counseling. In this capacity, they have been in contact with researchers engaged in health literacy work in England, Germany, Australia, Canada, Netherlands, Israel, France, Korea, and Japan. We are aware of differences in how the field of health literacy is evolving in different parts of the world and plan to have this conference be a meeting place in which international communication and collaboration can be fostered.
Conference Proceedings
The conference took place over 2 full days in October 2009 (see Section VI for the detailed agenda). The sessions included (1) keynote addresses by David Baker, MD, MPH and Anne Beal, MD, MPH, (2) invited panels on measurement, health literacy and verbal interactions, health information technology interventions, and organizational assessment and change, and (3) oral abstract sessions which included presentations of the highest rated abstracts submitted to the conference. In total, 96 abstracts
were submitted for review and 74 were accepted for presentation in either poster (62) or oral (12) form.
The panel and abstract presentations are available on our conference website at http://www.bumc.bu.edu/healthliteracyconference/2009-conference/.
In addition, on the first morning of the conference, Helen Meissner, PhD, Senior Advisor, OBSSR, coordinated a session titled NIH Gaps and Priorities for Future Research. The session was moderated by Ruth Parker, MD. The overall purpose of this session was to identify remaining gaps in our current understanding of the problems that underlie health literacy and approaches to address them. Program officers at the NIH, AHRQ, and CDC, were interested in soliciting investigator input regarding research gaps in the field.
Prior to the conference, registrants were invited to submit ideas regarding broad categories of gaps in our understanding of health literacy. We then invited speakers to address some of the major gaps in a plenary session, after which we broke into smaller groups for further discussion. The major gap topics were
-
Public Health Approaches to Health Literacy
-
Health Disparities and Health Literacy
-
Health Information Technology
See the conference website at http://www.bumc.bu.edu/healthlitera-cyconference/2009-conference/ for a list of speakers and summary of the themes gleaned from these sessions.
Attendance, Evaluation Summary, and Dissemination
The First Annual HARC was very well attended. An online registration site was created, and 206 people registered for the conference, and 198 attended. Participants included the strong majority of all active health literacy researchers in the United States. Two principle dissemination activities were arranged: (1) the Institute of Medicine: Health Literacy Roundtable Workshop on the findings of the HARC meeting, and (2) a special issue on Health Literacy from presentations of the HARC meeting of the Journal of Health Communication. The guest editors of the special issue are Michael Paasche-Orlow, Lauren McCormack, and Elizabeth Wilson. The special issue will be published in September 2010. See the conference website at http://www.bumc.bu.edu/healthliteracyconference/2009-conference/ for complete results of the evaluation.
IV.
Theme 1—Role of Health Literacy Research in Health Disparities Research
In the United States, racial/ethnic and socioeconomic disparities within the educational system have long been reported. As a result, two thirds of African American adults and 74% of Hispanic adults have limited functional literacy skills, compared to 32% of whites.24 The consequences of early failures in education have more recently been linked to problems in healthcare. More than half (58%) of African American adults and 66% of Hispanic adults have limited “health literacy” skills, while less than a third of whites face such problems.25 Research has begun to emerge showing how a health literacy skill set is linked to a range of health outcomes, and evidence has also emerged demonstrating how deficits in these skills possibly explain certain disparities.
As one of the primary public health goals in the U.S. and other industrialized countries is to better understand and respond to health disparities, a health literacy perspective provides an important new direction for seeking perhaps more potentially modifiable strategies for reducing inequities in the short-term, with a multitude of targets. Health literacy researchers are now recognizing the need for comprehensive strategies that go beyond considering only a patient’s functional literacy abilities. Rather, health literacy interventions should examine the complexity of the tasks required of patients and families within healthcare settings, the accessibility of providers for the target populations, the preparedness of health and public health professionals to engage productively with patients, and the features of the health care system, working environments, and communities in which caregiving and self-management support take place.
Health literacy research calls attention to the ways in which unnecessarily complex healthcare exacerbates the impact of underlying educational and income disparities. The implications of this extensive body of literature should be understood as a direct challenge to health systems that have been organized for the most highly educated and affluent members of a society. While seminal reports about the problem of limited health literacy have been issued by the Institute of Medicine,20 Agency for Healthcare Research and Quality,21 American Medical Association,22 and Joint Commission on the Accreditation of Hospital Organizations23 among others, none have focused on how health literacy research may help eliminate disparities.
Opportunities to integrate these fields of inquiry are likely to be mutually beneficial. Yet, currently health literacy and health disparities research typically occur in their own silos. Several key aspects of how research in health literacy can help eliminate health disparities are discussed.
A.
Integrate Health Literacy Assessment in Disparities Research
The first step in measurement. Without measurement, it is not possible to know when and how health literacy may be relevant to various forms of disparities, and it would be very easy to design interventions that fail to attend to relevant factors. For example, in an adjusted analysis that excluded literacy, African Americans were 2.40 times more likely to be non-adherent to their HIV-medication regimen than whites (95% confidence interval [CI]=1.14−5.08). When literacy was included in the final model adjusting for relevant covariates, the effect estimates of race diminished to non-significance and health literacy remained a significant independent predictor of non-adherence (adjusted odds ratio [AOR]=2.12, 95% CI=1.93−2.32).26 In another study, patients were asked their preferences regarding end-of-life care after hearing a verbal description of advanced dementia and then they were asked to relay their preferences again after viewing a 2 minute video of a patient with advanced dementia. The African American subjects were found to prefer more aggressive care than the white subjects. When health literacy was included in the final model, health literacy—but not race—was significant and independent predictor of preferences for care (low literacy OR 7.1, 95% CI 2.1−24.2; marginal literacy 5.1, 95% CI 1.6−16.3).27 Health literacy clearly mediated the influence of race on end-of-life preferences. In both of these investigations, completely different conclusions would have been made without concurrent evaluation of race and health literacy.
B.
Improve Patient Education
Patients at every education level will benefit from a reduction of paperwork, plain and simple communication, and standardized processes. Satisfaction, comprehension, and retention of information are enhanced for all patients when they are presented with plain language materials.28 While a fair amount of research has already focused on methods of patient education, there is still a tremendous unfulfilled agenda. There remain many open questions about approaches to optimizing the types of simplification called for by the health literacy literature and the types of cultural tailoring called for by the cultural competence literature.
C.
Simplification of the health care system: Access and Utilization
Unneeded complexity in healthcare exacerbates the impact of underlying educational disparities. The healthcare system is not the cause of the educational disparities that exist in the US; however, without simplification in all arenas (access, patient-clinician interactions, support of self-care) the health care system transforms educational disparities into health
disparities. Benefit systems need to be designed to succeed. Complex application forms, terms, and documentation requirements are significant barriers that disproportionately burden vulnerable populations.29-30 A health literacy lens should be taken to all public programs: How will a person with limited literacy get and use this program?
D.
Simplification of the health care system: Education and Training of Health Professionals
Health professionals contribute to the unneeded complexity of the healthcare system with poor communication and limited dedication to patient education. Clinicians frequently use jargon,31 rarely confirm if their patients understand what is being discussed,32 and patients frequently misunderstand a broad array of critical information.33 Health literacy curricula need to be integrated into professional education and such efforts need to be evaluated. To date, there is a dearth of research on the impact of educational initiatives to promote the knowledge and skills of health professionals regarding health literacy. Curricular initiatives to address health disparities are further advanced. There is a National Consortium for Multicultural Education for Health Professionals including educators from 18 US medical schools, which collect lessons learned from curriculum implementation to guide similar educational endeavors across the consortium.34 Indeed, several states have laws and or regulations that mandate training health professions in cultural competence (https://www.thinkculturalhealth.org/cc_legislation.asp). Inclusion of health literacy in such policy initiatives can help promulgate health literacy curricula, but research will be needed to identify programs that work, can be replicated, and help eliminate health disparities.
E.
Simplification of the health care system: Self-Care
High-quality medical care integrates evidence-based clinical care with a patient-centered orientation. A patient-centered orientation for health care is one that (1) includes pre-activation to prepare patients and tailor appropriate messages; (2) prioritizes collaborative goal-setting and relationship-centered care during the visit; (3) delivers post visit reinforcements and follow-up services for both cognitive and behavioral outcomes; (4) offers proactive surveillance during the inter-visit period to identify unanticipated changes in health trajectory or access difficulties; and (5) broadens the array of available self-management support strategies. The systematic delivery of these steps requires more than a motivated clinician; it requires a redesigned medical home as described by the Care Model. A growing body of literature suggests that tailored
implementation of elements of the Care Model can disproportionately benefit those with limited literacy;35,36 however, only a very small proportion of patients with limited literacy have access to such programs.28
V.
Theme 2—The Role of Information Technology in Health Literacy Research
There has been an explosion of creativity and investment in health information technologies. However, there is a significant risk that this current rapid expansion will worsen health disparities as many of the electronic systems will disproportionately benefit those with higher education and income.37 The chief challenges are to ensure that people with limited literacy have access to technologies and that they are designed for ease of use by people with limited literacy. How will people get the technology? Will people be able to use technology?
A.
Access to Technologies
While the internet has emerged as a major source of health information, access to and use of the internet to learn health information has been shown to be very strongly linked to health literacy.25,38 However, this is a moving target and will need to be monitored as social norms regarding the internet evolve rapidly.39 There is great potential for web-based projects and various authors have begun to explore how to deliver health information in a web-based fashion that is sensitive to literacy, culture, and linguistic needs.40 We are on the cusp of a wide range of patient-facing technological advances in personal health records, smart phone-based health applications, and biometric monitoring systems, and yet a large percentage of community physicians work without even a rudimentary electronic health record. As such, the issue of access needs to be viewed from both the perspective of patient-facing technologies as well as basic electronic health record infrastructure.
B.
User Interface
Sarkar and colleagues (in press, Journal of Health Communication) have shown that use of a patient portal system is linked to health literacy even when controlling for access. Attention is needed to simplify all aspects of the user interface with whatever form of technology that is being considered. Such simplification is clearly the goal of work led by Bickmore and colleagues who have explored the use of “embodied conversational agents”—animated computer characters—to interact with people (the character talks and the user responds with a touch-screen) in
a variety of settings to promote health. Bickmore and colleagues (in press, Journal of Health Communication) have shown that people with limited health literacy and no computer literacy are able to and do use them, at least in a variety of study settings.
C.
Behavioral Informatics
The chief focus of technology presentations at the HARC were oriented to behavioral informatics, i.e., information technologies (e.g., automated telephone calls, integrated electronic health record systems with patient portals, and computerized agents) that are designed to engage people in health activities. The value is clear; as health systems become automated, these tools allow for greater outreach, accountability, and standardization in the way health and healthcare is communicated to patients and families. Sarkar and colleagues compared the effectiveness of a diabetes self-management intervention using automated telephone calls with a nurse follow-up versus group medical visits and usual care.41 Those receiving the automated calls reported better perceived diabetes care, communication, and both intervention arms documented improved self-care behaviors, fewer bed days, and less interference with daily activities. In a small pilot of an animated, computerized agent to standardize communication for an informed consent process, Bickmore et al. found patients to be more accepting of the technology even compared to human interactions, although no differences in knowledge acquisition were noted.42 Both of these studies highlight the potential value of health technologies for engaging patients, particularly those with limited health literacy, yet more research is needed to better document the link between these interventions and health outcomes.
D.
Electronic Health Records
A common and important focus of health information technology is electronic health records. Electronic health records, however, was not a significant focus of the HARC meeting. This is almost certainly due to the fact that this is completely assumed to be an uncontroversial necessity.
VI.
Conference Agenda
Schedule of Events—Health Literacy Annual Research Conference 2009 National Academy of Sciences, Washington, DC
Time Day 1: Monday October 19, 2009
|
8:00am–9:00am |
Breakfast/Registration |
|
9:00am–11:00am |
NIH Gaps and Priorities Session, Moderator Ruth Parker |
|
11:00am–12:00pm |
Gaps/Priorities Small Group Breakout Sessions/Box Lunch |
|
12:00pm–12:45pm |
Keynote Address: David C. Baker, MD, MPH Michael A. Gertz Professor in Medicine, Chief, Division of General Internal Medicine, Feinberg School of Medicine, Northwestern University |
|
1:00pm–2:15pm |
Abstract I—Oral Presentations, Moderator: Joanne Schwartzberg
|
|
2:30pm–3:45pm |
Invited Panel A—Measurement, Moderator: Terry Davis Speakers: Elizabeth Hahn, Lauren McCormack, Russell Rothman |
|
4:00pm–5:15pm |
Invited Panel B—Health Literacy and Verbal Interactions, Moderator: Scott Ratzan Speakers: Kathy Mazur, Don Rubin, Debra Roter |
|
5:30pm–7:00pm |
Reception/Poster Session For Directions to hotel, see map in your blue registration folder |
Time Day 2: Tuesday October 20, 2009
|
8:00am–8:30am |
Breakfast |
|
8:30am–9:45am |
Abstract II—Oral Presentations, Moderator: Irene Dankwa-Mullan
|
|
10:00am–10:45am |
Keynote Address—Anne Beal, MD, MPH, President, Aetna Foundation |
|
10:45am: |
Presentation of Sabra Woolley Memorial Award for highest rated abstract—Linda Harris |
|
11:00am–12:15pm |
Invited Panel C—Health Information Technology Interventions, Moderator: Michael Paasche-Orlow Speakers: Timothy Bickmore, Dean Schillinger, Mike Wolf |
|
11:00am–12:15pm |
Invited Panel D—Organizational Assessment and Change, Moderator: Rima Rudd Speakers: Julie Gazmararian, Matthew Wynia, Beverly Weidmer |
|
12:30pm–2:00pm |
1-on-1 Meetings with NIH Project Officers and/or Research Mentors and Box Lunch |
|
12:30pm–2:00pm |
Poster Session |
|
2:00pm–3:15pm |
Abstract III—Oral Presentations, Moderator: Cindy Brach
|
|
|
|
|
3:30pm–4:00pm |
Final Session/Evaluations If you are unable to complete your evaluation at the conference, be sure to visit our website and complete it online: http://www.bumc.bu.edu/healthliteracyconference/ |
Reference List
1. National Institutes of Health Program Announcement: Understanding and Promoting Health Literacy. http://grants.nih.gov/grants/guide/pa-files/PAR-07-020.html. 2007.
2. Nielsen-Bohlman LT, Panzer AM, Hamlin B, Kindig DA. Institute of Medicine. Health Literacy: A Prescription to End Confusion. Committee on Health Literacy, Board on Neuroscience and Behavioral Health. 2004. Washington DC, National Academies Press.
3. Paasche-Orlow MK, Schillinger D, Greene SM, Wagner EH. How health care systems can begin to address the challenge of limited literacy. J Gen Intern Med 2006; 21(8):884-887.
4. Paasche-Orlow MK, Wolf MS. The causal pathways linking health literacy to health outcomes. Am J Health Behav 2007; 31 Suppl 1:S19-S26.
5. National Assessment of Adult Literacy (NAAL) http://nces.ed.gov/naal/kf_ demographics.asp
6. Kutner, M., Greenberg, E., Jin,Y., and Paulsen, C. (2006). The Health Literacy of America’s Adults: Results From the 2003 National Assessment of Adult Literacy (NCES 2006– 483). U.S.Department of Education. Washington, DC: National Center for Education Statistics.
7. Paasche-Orlow MK, Parker RM, Gazmararian JA, Nielsen-Bohlman LT, Rudd RR. The prevalence of limited health literacy. J Gen Intern Med 2005; 20(2):175-184.
8. Volandes AE, Paasche-Orlow M, Gillick MR, Cook EF, Shaykevich S, Abbo ED, et al. Health Literacy not Race Predicts End-of-Life Care Preferences. J Palliat Med 2008; 11(5):754-762.
9. Osborn CY, Paasche-Orlow MK, Davis TC, Wolf MS. Health literacy: an overlooked factor in understanding HIV health disparities. Am J Prev Med. 2007 Nov;33(5):374-8.
10. Kalichman SC, Ramachandran B, Catz S. Adherence to combination antiretroviral therapies in HIV patients of low health literacy. J Gen Intern Med 1999; 14(5):267-273.
11. Wilson FL, Racine E, Tekieli V, Williams B. Literacy, readability and cultural barriers: critical factors to consider when educating older African Americans about anticoagulation therapy. J Clin Nurs 2003; 12(2):275-282.
12. Kalichman SC, Rompa D. Functional health literacy is associated with health status and health-related knowledge in people living with HIV-AIDS. J Acquir Immune Defic Syndr 2000; 25(4):337-344.
13. Sudore RL, Mehta KM, Simonsick EM, Harris TB, Newman AB, Satterfield S et al. Limited literacy in older people and disparities in health and healthcare access. J Am Geriatr Soc 2006; 54(5):770-776.
14. Sentell TL, Halpin HA. Importance of adult literacy in understanding health disparities. J Gen Intern Med 2006; 21(8):862-866.
15. Saha S. Improving literacy as a means to reducing health disparities. J Gen Intern Med 2006; 21(8):893-895.
16. Rothman RL, DeWalt DA, Malone R, Bryant B, Shintani A, Crigler B et al. Influence of patient literacy on the effectiveness of a primary care-based diabetes disease management program. JAMA 2004; 292(14):1711-1716.
17. Howard DH, Sentell T, Gazmararian JA. Impact of health literacy on socioeconomic and racial differences in health in an elderly population. J Gen Intern Med 2006; 21(8):857-861.
18. Lindau ST, Basu A, Leitsch SA. Health literacy as a predictor of follow-up after an abnormal Pap smear: a prospective study. J Gen Intern Med 2006; 21(8):829-834.
19. Volandes AE, Paasche-Orlow MK. Health literacy, health inequality and a just healthcare system. Am J Bioeth 2007; 7(11):5-10.
20. National Institutes of Health Program Announcement: Understanding and Promoting Health Literacy. http://grants.nih.gov/grants/guide/pa-files/PAR-07-020.html. 2007.
21. Berkman ND, Dewalt DA, Pignone MP, Sheridan SL, Lohr KN, Lux L, Sutton SF, Swinson T, Bonito AJ. Literacy and health outcomes. Evid Rep Technol Assess (Summ). 2004 Jan;(87):1-8. Review.
22. Ad Hoc Committee on Health Literacy, American Medical Association Council on Scientific Affairs. Health literacy: report of the Council on Scientific Affairs. JAMA. 1999;281:552–7.
23. Joint Commission for the Accreditation of Hospital Organization (JCAHO). What Did the Doctor Say? Improving Health Literacy to Protect Patient Safety. Health Care at the Crossroads Report. Oakbrook, IL, 2007. February.
24. Kutner, M., Greenberg, E., Jin,Y., Boyle, B., Hsu, Y., and Dunleavy, E. (2007). Literacy in Everyday Life: Results From the 2003 National Assessment of Adult Literacy (NCES 2007–480).U.S. Department of Education. Washington, DC National Center for Education Statistics.
25. Kutner, M., Greenberg, E., Jin,Y., and Paulsen, C (2006). The Health Literacy of America’s Adults: Results From the 2003 National Assessment of Adult Literacy (NCES 2006–483). Washington, DC, U.S. Department of Education: National Center for Education Statistics.
26. Osborn CY, P.-O. M., Davis TC, Wolf MS. (2007). “Health literacy: an overlooked factor in understanding HIV health disparities.” Am J Prev Med 33(5): 374-8.
27. Volandes AE, P.-O. M., Gillick MR, Cook EF, Shaykevich S, Abbo ED, Lehmann L. (2008). “Health literacy not race predicts end-of-life care preferences.” J Palliat Med 11(5): 754-62.
28. Paasche-Orlow, M. K., Schillinger, Dean, Greene, Sarah M, and Wagner, Edward H (2006). “How Health Care Systems Can Begin to Address the Challenge of Limited Literacy” J Gen Intern Med 21(8): 884-887.
29. Davidoff AJ, S. B., Shaffer T, Shoemaker JS, Kim M, Zacker C (2010). “Lessons Learned: Who Didn’t Enroll In Medicare Drug Coverage In 2006, And Why?” Health Aff (Millwood).
30. Ettner SL, S. N., Duru OK, Turk N, Quiter E, Schmittdiel J, Mangione CM (2010). “Entering and exiting the medicare part d coverage gap: role of comorbidities and demographics.” J Gen Intern Med 25(6): 568-74.
31. Castro CM, W. C., Wang F, Schillinger D (2007). “Babel babble: physicians’ use of unclarified medical jargon with patients.” Am J Health Behav 31(Suppl 1): S85-95.
32. Schillinger D, P. J., Grumbach K, Wang F, Wilson C, Daher C, Leong-Grotz K, Castro C, Bindman AB (2003). “Closing the loop: physician communication with diabetic patients who have low health literacy.” Arch Intern Med 163(1): 83-90.
33. Fang MC, P. P., Machtinger EL, Schillinger D. (2009). “Language, literacy, and characterization of stroke among patients taking warfarin for stroke prevention: Implications for health communication.” Patient Educ Couns 75(3): 403-10.
34. Carter-Pokras O, B. S., Lie D, Braddock CH 3rd; National Consortium for Multicultural Education for Health Professionals (2010). “Surmounting the unique challenges in health disparities education: a multi-institution qualitative study.” J Gen Intern Med 25(Suppl 2): S108-14.
35. Rothman R, Malone R, Bryant B, Horlen C, DeWalt D, Pignone M. The relationship between literacy and glycemic control in a diabetes disease-management program. Diabetes Educ. 2004 Mar-Apr;30(2):263-73.
36. DeWalt DA, Pignone M, Malone R, Rawls C, Kosnar MC, George G,BryantB,Rothman RL, Angel B. Development and pilot testing of a disease management program for low literacy patients with heart failure. Patient Educ Couns. 2004 Oct;55(1):78-86.
37. Viswanath K., Kreuter, MW. Health Disparities, Communication Inequalities and E-health: A Commentary. American Journal of Preventive Medicine. 2007; 32 (5 Suppl): S131-3.
38. Czaja SJ, S. J., Nair SN (2008). “Usability of the Medicare health web site.” JAMA 300(7): 790-2.
39. Samal L, Yeh HC, Gary-Webb TL, Jackson CL, Brancati FL. Computer and internet use of urban african americans with type 2 diabetes in relation to glycemic control, emergency department use, diabetes-related knowledge, and health literacy. Diabetes Care. 2010 Jan;33(1):e9.
40. Neuhauser L, Kreps GL. Online cancer communication: meeting the literacy, cultural and linguistic needs of diverse audiences. Patient Educ Couns. 2008 Jun;71(3):365-77.
41. Sarkar U, H. M., Gupta R, Tang A, Murphy E, Seligman HK, Shojania KG, Schillinger D (2008). “Use of an interactive, telephone-based self-management support program to identify adverse events among ambulatory diabetes patients.” J Gen Intern Med 23(4): 459-65.
42. Bickmore TW, P. L., Paasche-Orlow MK (2009). “Using computer agents to explain medical documents to patients with low health literacy.” Patient Educ Couns 75(3): 315-20.


















