HIV Screening and Access to Care: Health Care System Capacity for Increased HIV Testing and Provision of Care
The Institute of Medicine (IOM), in response to a request from the White House Office of National AIDS Policy (ONAP), convened a committee on HIV screening and access to care in 2009 to plan and host a series of three workshops and data gathering activities to evaluate barriers to expanding HIV testing and treatment. The committee’s first report focused on the extent to which federal and state laws and policies, private health insurance policies, and other factors inhibit or promote expanded HIV testing (IOM, 2010). The second report examined how federal and state laws and policies and private health insurance policies and practices affect entry into clinical care and the provision of continuous and sustained care for people with HIV (IOM, 2011b). This third and final report explores the current capacity of the health care system to administer a greater number of HIV tests and to accommodate new HIV diagnoses (see Box 1).
The committee was asked to consider the following questions as part of its charge for this report:
-
Where do HIV-positive patients currently get care?
-
What is the HIV-related training or experience of most HIV care providers (physician, nurse practitioner [NP], physician assistant [PA], registered nurse [RN])?
-
What manpower or training/experience improvements are needed to absorb more newly diagnosed HIV-positive individuals from expanded HIV testing services?
|
BOX 1 Statement of Task
|
-
Is the age profile of providers compatible with sustainability of the HIV care delivery system? That is, are younger clinicians and/or students receiving adequate training and experience to meet future needs?
-
What are the impediments to professionals entering into or continuing to provide HIV/AIDS care?
-
What policies inhibit or enhance the movement of health care professionals into HIV/AIDS specialties?
-
Are there adequate financial or professional incentives to promote HIV/AIDS as a specialty among the health care professions?
The committee hosted its third public workshop September 29-30, 2010, in Washington, DC (see agenda, Appendix C). The committee convened experts from academia, government, and provider groups to offer expert testimony. Also in attendance were more than 30 workshop registrants representing patients, providers of HIV testing and care services, researchers, policy organizations, and others with an interest in this topic (see workshop attendees, Appendix D). Invited experts were asked to present their evidence and perspectives. Following each panel, questions were entertained from the committee and the audience.
REPORT ORGANIZATION
This report begins with a background section outlining the rationale for expanding HIV testing and the potential challenges of providing quality HIV care to a significantly increased number of patients. The report then summarizes information from the expert presentations and discussion from the public workshop as well as information from a literature review that is relevant to the questions posed to the committee in the third part of the statement of task (see number 3 in Box 1).
The report first examines issues surrounding the capacity of the health care system to administer a greater number of HIV tests. The two primary issues raised relate to the personnel and procedures necessary to implement expanded HIV testing successfully in a variety of different venues and to the personnel and procedures needed to provide counseling and linkages to care for individuals who test positive.
The report next provides information about where HIV-positive individuals currently receive care. It then addresses the question of HIV-related training or experience of most HIV care providers, both in terms of their current experience and training and in terms of changes needed to accommodate a greater number individuals diagnosed with HIV. The next section addresses the current capacity of the HIV/AIDS workforce. The following
two sections summarize delivery system strategies and models that might help providers to care for a larger number of HIV-infected patients and strategies to increase the number of providers entering and remaining in the HIV/AIDS workforce. The report then addresses the impact of the Patient Protection and Affordable Care Act (ACA) (P.L. 111-148) on the public health and clinical infrastructure. The report concludes with a summary of the committee’s conclusions.
BACKGROUND
There is a lack of population-based estimates of the numbers of individuals with HIV who are not in care or on treatment, although studies suggest substantial unmet need. There are an estimated 1.1 million people in the United States living with HIV, of which approximately 21 percent are unaware of their infection and so are not receiving HIV/AIDS care (CDC, 2010c). In addition, one analysis of CDC medical record-based data showed that 45 percent of individuals aged 15 to 49 who have been diagnosed with HIV/AIDS and who are eligible for antiretroviral therapy (ART) are not receiving it (Teshale et al., 2005). Moreover, an estimated 56,000 individuals contract HIV each year (CDC, 2010b).
Approximately 55 percent of adults between 18 and 64 years of age and 28 percent of people at higher risk for HIV have never been tested (CDC, 2010c). Identification of undiagnosed HIV-positive individuals is important because early treatment improves the health outcomes of persons infected with HIV1 and decreases the likelihood of transmitting the virus to others. However, enhanced screening efforts and subsequent linkages to care for previously undiagnosed individuals and for previously diagnosed individuals who do not receive regular care will place increased demands on organizations and individual health care providers.
The present capacity of the health care system to administer a greater number of HIV tests and to accommodate a significant increase in the number of HIV-infected individuals in care is strained. Julie Scofield, Executive Director, National Alliance of State and Territorial AIDS Directors (NASTAD), described the situation as a “perfect storm.” The U.S. recession has led to an increased demand for publicly supported services on the part of those with, or at risk for, HIV. Although resources were insufficient to support the demand for HIV prevention, testing, and care before the economic downturn, federal and state budget cuts in response to the financial crisis have made it more difficult to meet the increased demand for services. At the same time, expanded HIV testing initiatives in response to
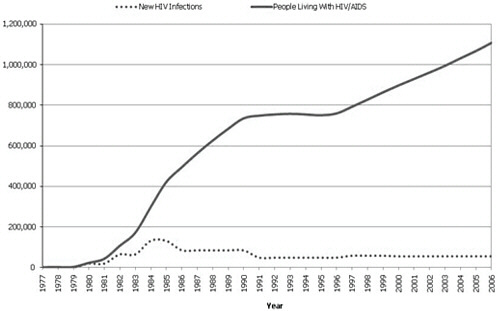
FIGURE 1 HIV incidence and prevalence, United States, 1977–2006.
SOURCE: Hall et al., 2008.
CDC recommendations to promote routine HIV testing (CDC, 2006) have brought more individuals into care.2 In addition, earlier and more effective treatment has greatly improved survival among HIV-positive individuals. It is estimated that by 2015 one half of people living with HIV/AIDS will be over the age of 50 (Effros et al., 2008; Myers, 2009). Although most of these individuals are long-term survivors of HIV, in 2007, people age 50 and over accounted for 16 percent of new HIV diagnoses (CDC, 2007). Figure 1 shows the increase in the number of people living with HIV/AIDS from 1977 to 2006.
In the face of this success, however, serious concerns have arisen regarding the health care system’s ability to meet the growing demand for HIV testing, access to medications, and linkages to sustained care.
Additional factors that affect the ability of the workforce to address the needs of HIV-positive individuals include the complexity of care resulting from improved survival (older individuals with HIV often experience more complex psychosocial and care needs, including increased stigma, dementia, and other comorbidities [GMHC, 2010]), the relatively low numbers of new providers specializing in HIV care, severe provider shortages in rural areas and urban centers with high minority concentrations, and the need
for increased cultural competency among providers to treat an increasingly diverse client population (HRSA, 2010c). At the same time, the initial wave of HIV care providers are approaching retirement age and are either reducing their practices or retiring completely. Taken together the increasing demand for HIV care services and anticipated decrease in the relative number of providers practicing HIV medicine raises concerns about the ongoing ability of the workforce to meet the needs of the HIV/AIDS population in the United States, especially as enhanced screening efforts are expected to increase the number of individuals diagnosed with HIV.
Additionally, changes that are anticipated to result from the ACA potentially could further increase demand on the HIV care workforce. Medicaid is the largest single source of care and coverage for people with HIV with approximately 40 percent of patients receiving services through Medicaid (KFF, 2009b). Medicaid expansion under the ACA expands income eligibility to a national floor of 133 percent of the federal poverty level and is expected to bring millions of low-income individuals, including individuals with HIV, into the Medicaid program. The elimination of categorical eligibility requirements, such as disability, for Medicaid under the ACA is also likely to bring many more individuals with HIV into the program (IOM, 2010).
Grave concern exists about the capacity of the health care workforce to implement expanded testing for HIV throughout the United States and to provide competent HIV/AIDS care to significantly increased numbers of patients. A variety of approaches will be needed to respond to these challenges. The current comprehensive and integrated model of care often exhibited by Ryan White-funded clinics provides a foundation upon which future care systems could be structured.3
EXPANDED HIV TESTING
Since the beginning of the HIV epidemic, HIV testing and counseling traditionally have been administered by providers who are specifically trained in these areas, and providers not trained in HIV testing and counseling would refer patients out to those who were. As a result, providers who have practiced in this environment are less well-equipped to mentor their students and residents in the provision of HIV testing. The practice of referring patients for HIV testing may also have contributed to patients’ belief that their provider does not perform HIV testing. A cultural shift is
needed within the education of students and residents so that over time providers become better equipped to perform HIV testing and counseling and less inclined to refer their patients elsewhere.
Timely diagnosis and treatment can improve survival and quality of life among HIV-positive individuals and reduce the likelihood that they will transmit the disease to others. These reasons provide impetus to increase identification of previously undiagnosed HIV-positive individuals through measures such as the 2006 CDC recommendations for routine screening for HIV for individuals between the ages of 13 and 64 (CDC, 2006). Between 2006 and 2009, the percentage of Americans aged 18 to 64 who reported being tested for HIV at some point in their lives grew only from 40 percent to 45 percent (CDC, 2010c, p. 2). In light of continuing efforts to increase testing for HIV in the United States, the committee was asked to evaluate the current capacity of the health care system to administer a greater number of HIV tests.
In a recent survey of the 65 jurisdictions receiving CDC funding for HIV prevention activities, 75 percent (43 health departments) reported providing financial and programmatic support for the implementation of routine HIV testing for all patients 13 to 64 years of age, in accordance with the 2006 CDC recommendations (NASTAD, 2010, p. 12). Of the 43 health departments that provided support for routine testing, the greatest majority (79 percent) supported routine testing in sexually transmitted disease (STD) clinics. Sixty percent supported routine testing in hospital emergency departments (EDs) and community health clinics, and 51 percent supported routine testing in substance abuse treatment centers, correctional facilities, and family planning clinics (see Table 1).
The first report of the Committee on HIV Screening and Access to Care discussed the various barriers and facilitators to expanding access to HIV testing (IOM, 2010). Recent data from the CDC indicate that in 2009 82.9 million adults between 18 and 64 years of age in the United States reported having been tested at least once for HIV, which represents an increase of 11.4 million since 2006 when the CDC recommendations to expand HIV testing went into effect (CDC, 2010c,e). Despite the progress that has been made, it is estimated that 55 percent of adults (including 28.3 percent of adults with a risk factor for HIV) still have never been tested for HIV (CDC, 2010c,e). Increased testing within the senior population faces unique or greater challenges, such as the stereotype that seniors are not sexually active, greater resistance to discussing sexual activity with health care providers, less knowledge about HIV transmission and prevention, and unique biological risk factors (GMHC, 2010; Myers, 2009).
Kathryn Hafford, Director, Division of Disease Prevention, Virginia Department of Health, described how a survey conducted two years after Virginia changed its law to be consistent with CDC recommendations
TABLE 1 Health Care Settings in Which Health Departments Support Routine HIV Testing
|
Health Care Settings in Which the Health Department Reported Supporting Routine HIV Testing |
% Responding (n=43) |
|
STD clinics |
79% (34) |
|
Hospital emergency departments |
60% (26) |
|
Community health clinics |
60% (26) |
|
Substance abuse treatment centers |
51% (22) |
|
Corrections |
51% (22) |
|
Family planning clinics |
51% (22) |
|
TB clinics |
42% (18) |
|
Prenatal/obstetrical clinics |
35% (15) |
|
Primary care clinics |
28% (12) |
|
Labor and delivery |
28% (12) |
|
Urgent care clinics |
19% (8) |
|
Hospital inpatient settings |
19% (8) |
|
Hospital outpatient settings |
16% (7) |
|
Other (e.g., ASO, CBOs) |
30% (13) |
|
SOURCE: NASTAD, 2010, p. 12 |
|
found that despite educational outreach efforts, providers did not know that written informed consent was no longer needed prior to administering a routine HIV test. Rates of documented routine prenatal HIV testing did not increase following the state’s change in law. Experience with routine prenatal testing varies from state to state, however. In Rhode Island, for example, prenatal testing increased from about 53 percent in 2006 to more than 90 percent following implementation of routine opt-out testing ( Alexander et al., 2009). Hafford indicated that additional provider training is needed so that the legal obligations regarding HIV testing are clear.
Once these and other barriers to the implementation of expanded HIV testing are overcome, the question remains whether various components of the health care system have the capacity to provide such screening. In addition to the need for adequate space to permit privacy when interacting with patients about HIV testing, the primary concern about capacity centers on the question of a sufficient number of adequately trained personnel. A second, somewhat related, general concern is the degree to which testing can be incorporated into the present work flow at facilities. The greater the extent to which it can, the less the need for additional personnel to accommodate the associated tasks.
Hafford explained that the Virginia Department of Health, as in most other states, has received substantial funding to develop and promote routine testing programs around the state. The health department found that the capacity and desire to implement testing programs, as well as the need for support, vary greatly among venues. Some providers say that all they need is funding for test kits and the testing procedure or to hire additional staff; others say that they will not implement a program unless the health department provides the staff.
Incorporation of routine HIV testing into office visits with family practitioners and other primary care providers may present smaller obstacles in terms of logistics and provider capacity. However, some providers do not view such testing as their primary responsibility, and some dismiss the need for such screening among their patients, whom they may view as being at low risk for HIV. This is another area in which provider education may prove beneficial in helping to increase the number of tests performed. In general, however, health department support for HIV testing has resulted in more testing in private settings. Hafford pointed out that many providers are not opposed to testing, but indicated that some providers feel overwhelmed by the prospect of diagnosing and caring for HIV-positive individuals and that they often do not know how to expand HIV testing. Additional training to increase providers’ familiarity and comfort with the processes of HIV testing (e.g., counseling and referral mechanisms for patients diagnosed with HIV, as well as guidance in incorporating routine testing into their practices) may be beneficial here as well.
Based on her experience with health department supported testing programs in Virginia, Hafford reported that testing in non-primary-care settings increases when support is provided but that such increases require a great deal of support. New HIV testing programs in these settings have been successful in identifying previously undiagnosed HIV-infected persons, but staff members have required oversight to ensure that quality standards surrounding testing are being met. In addition, peer navigators had to be hired to ensure that individuals who test positive are linked to care.4
Since EDs are likely to see patients at higher risk for HIV, testing for HIV in EDs may help to identify individuals with undiagnosed HIV infection. However, there are barriers to the implementation of increased HIV testing in EDs. Compared with patients in other medical settings, patients visiting EDs may be more difficult to locate once they leave. Consequently, conventional HIV testing for which results would not be available during the same visit may not be performed because of provider liability con-
cerns. Use of rapid HIV tests, which generate results within minutes, can help to address this concern and reduce the number of people who fail to receive their test results (Branson et al., 2006). The administration of rapid HIV testing in EDs has been found to be acceptable to ED providers and patients (Brown et al., 2007; Freeman et al., 2009; Merchant and Catanzaro, 2009).5
Other barriers to increased HIV testing in EDs remain however. Most notably, because ED providers are concerned with addressing their patients’ immediate health care needs, they may not have the time or other resources to perform routine HIV testing. As discussed in greater detail later, use of hospital-based laboratories for the processing of rapid tests (or expedited processing of conventional tests) would help to address some of these concerns and may help HIV testing fit more seamlessly into the ED workflow and minimize the impact on existing personnel.
Providers also may be concerned about how to approach individuals about HIV testing. Several issues arise, including a lack of comfort among many providers in addressing matters pertaining to individuals’ sexual history and practices. Providers additionally are concerned about the amount of time potentially needed to counsel patients who test positive and link them into care. Hafford described how providers who have worked with HIV/STD or high-risk clients are more comfortable with providing HIV testing. However, providers without such experience often feel unprepared to handle a positive test result. In fact, she mentioned that some providers in her state ask the health department to handle all positive test results. She indicated that education and guidance in this area are needed and that health professional schools are not spending enough time training students in taking a sexual history and providing counseling.
Hafford indicated that, as frequently is the case in hospital EDs, some community health centers (CHCs) already are so overwhelmed by patient case loads that they resist the addition of routine screening to the services they provide. Often the CHCs that are most interested in establishing routine HIV testing are in rural areas with a lower percentage of HIV positive individuals. These centers have the time and the personnel to introduce
|
5 |
Conventional testing refers to the use of ELISA (or enzyme immunoassay [EIA]) tests to detect the presence of HIV antibodies in blood, oral fluid (mucus, not saliva), or urine. The test takes 3.5 to 4 hours to run, but samples generally are processed in batches and frequently are sent to outside labs, resulting in a wait of a day or two to 1 to 2 weeks for the result (http://www.cdc.gov/hiv/topics/testing/resources/qa/index.htm [accessed March 3, 2011]; San Francisco AIDS Foundation, 2009). Rapid testing refers to the use of a test strip to detect the presence of HIV antibodies by visually comparing the test window to a control window. Similar to a home pregnancy test, rapid HIV tests provide results in as little as 20 minutes (http://www.cdc.gov/hiv/topics/testing/resources/qa/index.htm [accessed March 3, 2011]; San Francisco AIDS Foundation, 2009). |
routine testing, but they do not see many HIV-positive patients, raising the issue of how to prioritize the distribution of health department support for routine HIV testing programs.
Finally, Hafford noted the difficulty the Virginia health department has experienced in getting buy-in to routine screening from correctional facilities. For example, testing within correctional facilities (and some other high-risk settings) often depends on the willingness of the health department to provide counseling and other services associated with the identification of a positive case. Committee member Beth Scalco mentioned that this dependence on the health department support is also present in Louisiana.
Andrew Young, Associate Professor, Emory University School of Medicine, also provided the committee with information on the capacity implications of expanded HIV testing, addressing both the ED and clinical laboratory settings. HIV testing in EDs can occur by either rapid testing or expedited conventional testing6 in the hospital laboratory or by rapid testing directly at the point of care. Young discussed the advantages and disadvantages of each approach.
The advantage of conventional testing when next-day turnaround times are acceptable (e.g., for hospital inpatients) is the laboratory’s ability to accommodate a greater increase in testing, due to automation, without additional equipment, testing personnel, or training, according to Young. However, the implementation of routine testing programs with immediate processing of samples so that results become available during the patient encounter creates challenges for laboratories and testing personnel. Although such immediate testing is favored by many organizations because of better patient acceptance, follow-up, and linkages to care (Freeman et al., 2009; Haukoos et al., 2008; Jain et al., 2008), laboratories may not be able to provide expedited conventional testing for a large number of specimens because conventional HIV tests often are performed on batch analyzers. Different equipment, such as random-access analyzers,7 likely would be necessary to provide continuous expedited testing, but not all laboratories have such equipment. Therefore, in order for in-house laboratories to support extensive HIV testing through expedited conventional testing, new funds, space, and personnel likely would be needed. In addition to these laboratory-specific resources, new hospital staff, resources, and training may be needed to process test orders, obtain and transport specimens,
|
6 |
Expedited conventional testing would involve the hospital laboratory running a conventional HIV test either individually or in small batches so that the results could be delivered while the patient is still in the ED. In addition to other drawbacks, such an approach still would require a number of hours to perform, making it less timely than the use of rapid testing. |
|
7 |
For more information, see http://www.hivandhepatitis.com/recent/2008/060608_e.html (accessed March 3, 2011). |
report and receive positive results, and counsel a greater number of patients diagnosed with HIV.
Different challenges arise with point-of-care HIV testing. Although administration of rapid tests at the point-of-care allows clinicians to receive and transmit results more quickly during a patient encounter (i.e., results are available within minutes, compared with hours for expedited conventional testing), it can raise issues related to capacity and quality assurance. Young described how for clinic- or office-based testing, RNs or other personnel undertake a manual process that can take 20 to 40 minutes. According to Young, in low-volume, low-acuity settings, where there is limited access to clinical laboratories, rapid HIV testing is useful and feasible. In busy EDs, however, more pressing patient concerns, such as life-threatening trauma or medical emergencies, may distract personnel from the testing process. Since the accuracy of the test results depend on reading the test within the timeframe specified by the manufacturer, the possibility of the tester being occupied by other duties may lead to a greater number of false negatives or positives or wasted time and materials, when clearly invalid tests must be discarded. Young noted that to avoid specimen errors, only one patient (or very few) should be tested at one time.8
Young also expressed concern about ensuring compliance with Clinical Laboratory Improvement Amendments (CLIA) standards in non-laboratory-based testing, even when CLIA-waived rapid tests are being used. The Clinical Laboratory Improvement Amendments9 regulate all laboratory testing performed on humans in the United States and list legal standards for waived testing. The Food and Drug Administration (FDA) defines tests as “waived” or “not waived” from CLIA based on their level of complexity (Table 2). Waived tests are those that generally are easy enough to administer at home, that carry minimal risk of harm, and that therefore have less stringent requirements. Non-waived tests have more stringent requirements (e.g., personnel qualifications, quality management).
Young cited Centers for Medicare and Medicaid (CMS) surveys revealing high rates (e.g., 20 percent) of noncompliance with CLIA standards (Howerton et al., 2005). These issues arise in testing at the point of care, even when simple CLIA-waived tests are used. The Joint Commission on Accreditation of Healthcare Organizations also lists standards for waived testing in accredited health care organizations, with similar high rates of noncompliance (JCAHO, 2010). If clinical personnel were to add high-
|
8 |
November 2010, the Food and Drug Administration approved a new rapid test for HIV-1 that provides results in as little as 60 seconds (Klein and Struble, 2010). The test requires a fingerstick or venipuncture to obtain blood, unlike some other rapid tests that can be run on oral fluids. However, the very rapid result time may facilitate usage and streamline routine HIV testing in busy hospital-based settings and help to extend routine HIV-testing to novel venues. |
|
9 |
See http://www.cms.gov/CLIA/ (accessed March 3, 2011). |
TABLE 2 Approaches to Routine HIV Screening
|
Location of Testing |
Common Testing Platform |
CLIA Category |
|
Large commercial and hospital laboratories |
Automated assays (standard tests) |
Non-waived |
|
Small hospital, clinic or physician office laboratories |
Non-automated assays (standard tests); rapid tests |
Non-waived; waived |
|
Point of care (e.g., emergency departments, clinics) |
Rapid tests |
Waived |
|
SOURCE: Young, 2010. |
||
volume, manual HIV screening to their existing duties, the risks of noncompliance would probably increase significantly. Thus, point-of-care screening may require the addition of dedicated staff. The concern about CLIA compliance would be reduced if expedited laboratory testing were available.
Much of the literature on point-of-care rapid HIV screening comes from large hospital EDs, with externally funded programs and dedicated staff trained in point-of-care testing (Arbelaez et al., 2009; Brown et al., 2007; Haukoos et al., 2010; White et al., 2009). Documentation of testing and test results, as well as meeting administrative reporting requirements, is time-consuming. In addition, the costs per test and risks of regulatory noncompliance are greater. Young indicated that these point-of-care testing programs may not be sustainable over the long term, or be able to expand to test a larger percentage of emergency room traffic without additional external resources.
Young discussed the point-of-care rapid testing program being conducted at a Grady Health System ED as part of a CDC demonstration project (THRIVE Project). Through August 2010, there was high test acceptance (85 percent) and more than 10,000 patients were tested. The program has identified 172 patients with new preliminary HIV diagnoses (1.7 percent of those tested). Young characterized the program as successful, but he indicated that it has reached capacity in terms of the number of HIV tests that can be performed in the ED with available staff and resources, despite having hired dedicated staff (a full-time program coordinator/HIV counselor; two additional, full-time HIV counselors; and a half-time database manager) to manage the testing and linkages to care. There are approximately 150,000 visits to the Grady ED each year, so routine HIV testing has been extended to only a fraction of patients seen there. In addition, since CDC funding of the program has helped to cover the cost of the dedicated staff to administer the tests, provide counseling,
and link those who test HIV positive to follow-up care, the sustainability of the program following the demonstration stage is questionable.
Instead of extensive use of point-of-care HIV testing in high-volume EDs, Young advocated movement toward an expedited laboratory-based HIV testing program. If sites can develop good systems for rapid ordering of tests and transport of specimens, in-house laboratories could immediately process HIV tests, just as they process emergent tests such as those for cardiac markers in heart attack patients. Such programs would require laboratory staff and equipment capable of processing HIV tests on an expedited basis around the clock, as well as a plan and hospital staff person to explain the results and arrange linkage to care for those individuals who test positive. But because of the need for other expedited testing in laboratories, the long-term sustainability of such a program is more assured.
Another possibility would be the use of hospital laboratories to process rapid HIV tests rather than conducting them in the EDs. According to Young, this approach would help to ensure around-the-clock availability of trained personnel, lessen the risk of regulatory noncompliance, and potentially avoid the need to purchase new laboratory equipment. However, Young noted, the need to transport rapid tests to the central lab would eliminate much of the advantage of the quick turnaround time for rapid tests; the cost of performing rapid HIV tests is much greater than with automated analyzers; and regardless of where they are performed, rapid tests pose a significant challenge for high-volume testing because of the total lack of automation.
In response to a question from committee member Scott Burris, Young discussed the difficulties of providing counseling in the context of a busy ED and the need for dedicated staff to ensure that prevention messages are communicated, both to patients who do and do not test positive for HIV, and that patients who test HIV positive are linked to appropriate follow-up care. Hafford mentioned that EDs in Virginia often rely on the health department to handle the counseling needed for those who test positive. In higher risk settings, such as STD clinics, the HIV counseling is handled by clinic staff. Committee member Beth Scalco described how, in Louisiana, EDs rely on hospital-based infection control nurses to provide counseling and linkages to care. Registered nurses, along with testing counselors, can be effectively utilized in the provision of testing, prevention counseling, and care linkage for individuals who test positive.
Young also raised concerns about a rise in the rate of false positive tests as routine HIV screening programs are implemented in lower prevalence areas. This problem will be minimized by the relatively high accuracy of HIV testing, although high false positive rates have been reported (Walensky et al., 2008). The problem could be further addressed by use of rapid tests (in the clinical laboratory or at the point of care) for confirma-
tory diagnostic purposes, as well as screening. In this model, patients would not be informed of positive results until they are verified by a second rapid test. Currently, the FDA has only approved Western blotting and RNA hybridization for confirmation in the United States, but it is considering approval of rapid tests for this use.
Young mentioned the advent of “fourth generation” assays for HIV antibody and antigen and discussed how they might improve screening. These fourth generation assays can detect acute HIV infection, when antibodies have not yet developed but viral antigen and RNA are present. Patients with acute infection who are unaware of their status are more likely to engage in high-risk behavior. They are also at high risk for transmission due to their high viral load. To date, the FDA has approved one fourth generation assay for use as an aid in the diagnosis of HIV infection, including acute or primary HIV infection (FDA, 2011), with others under review (Abbott, 2010).
In terms of administrative issues, Young mentioned the uncertainty over the provision of reimbursement for HIV screening tests, given insurers’ policies to limit payment for preventive services to those rated highly by the U.S. Preventive Services Task Force (USPSTF).10,11
Young identified the need to educate hospital leaders, through organizations such as the American College of Healthcare Executives, about the importance of HIV screening and opportunities for funding. High-level administrative involvement is critical in large health care systems to ensure institutional endorsement of screening and to provide the necessary leadership and resources to clinical departments and laboratories, so that their roles are coordinated and HIV screening programs are affordable, sustainable, and compliant with regulations. He also discussed the merits of support for demonstration programs that would allow clinical laboratories to explore methods to expedite testing to meet the needs of EDs and other settings where routine HIV testing is taking place.
The SAMHSA National Survey of Substance Abuse Treatment Services, an annual census of substance abuse treatment centers throughout the United States, helps to assess the availability of HIV testing and ancillary
services for HIV (including early intervention services and education and counseling) in substance abuse and treatment centers (SAMHSA, 2010). The survey can help to identify locations where there may be gaps in HIV testing and ancillary services.
Conclusions
Currently, many programs are receiving significant funding to support the development and implementation of HIV screening in various venues. However, the long-term sustainability of such programs is uncertain, especially if outside funding ceases. It is clear that sustainable programs need to fit as seamlessly as possible into the care flow of the venues in which they are instituted. Accomplishing this may necessitate the use of different testing procedures in different venues. For example, there is value to rapid, point-of-care testing, but it is more difficult to incorporate such testing into the flow of a high-volume ED than into a private family practice setting. Development of a streamlined approach to expedited laboratory-based HIV testing may be more feasible for busy EDs that already have procedures in place for other expedited laboratory testing.
Aside from the testing itself, a major issue is how to handle the positive results. Patients who test positive for HIV require at least minimal point-of-care counseling and linkage into follow-up care. Current experience indicates that provision of these services requires about 30 minutes per patient. Likely the best way to address this need is to use a dedicated staff person (e.g., a designated RN or testing counselor) who would have the time, training, and comfort level needed to address the individual’s needs. In addition, increased emphasis on sexual history taking and HIV training in professional schools may decrease provider discomfort in addressing all aspects of testing, including positive results, with their patients.
Another long-term consideration is the need for access to ongoing care by those receiving new diagnoses. The second report of the Committee on HIV Screening and Access to Care addresses policies that may inhibit entry into clinical care by newly diagnosed HIV-positive individuals and the provision of continuous, sustained clinical care for HIV-positive individuals.
WHERE PERSONS WITH HIV CURRENTLY RECEIVE CARE
Laura Cheever, Deputy Associate Administrator and Chief Medical Officer, HIV/AIDS Bureau, Health Resources and Services Administration (HRSA), provided the committee with an overview of the limited data available on patterns of care for HIV/AIDS patients. Unfortunately, the most comprehensive study of sites of HIV/AIDS care is from the HIV Cost and Services Utilization Study (HCSUS) (Bozzette et al., 1998), which was
TABLE 3 Usual Source of Care for Individuals with HIV/AIDS in Care, United States 1996
|
Provider Type |
Percent |
|
Private MD office |
35 |
|
Hospital-based clinic |
30 |
|
Community/neighborhood clinic |
25 |
|
Health Maintenance Organization (HMO) |
4 |
|
Other medical clinic |
6 |
|
SOURCE: Cheever, 2010 (provisional analysis of 1996 HCSUS data by John Fleishman, Agency for Healthcare Research and Quality, September, 2010). |
|
conducted from 1994 to 2000 and the data from which are now outdated. More recent data are available from Ryan White providers, but the sample is limited to those receiving Ryan White funding. A current effort to compile nationally representative data on people living with HIV/AIDS who are receiving care in the United States is the Medical Monitoring Project,12 although data pertinent to this report are not presently available.
HCSUS collected information on a nationally representative sample of people in care for HIV infection. The data are now more than 10 years old, and the epidemic has shifted in demographic and clinical terms. However, HCSUS found that in 1996, HIV/AIDS patients in care were seen predominantly in private physicians’ office practices, hospital-based outpatient clinics, and community/neighborhood clinics (Table 3). It is unknown the extent to which source of care patterns are similar today or whether they have changed with the shifts in the HIV epidemic.
Along with Medicaid, an essential source of care for the estimated 529,000 uninsured and under-insured persons infected with HIV in the United States is the Ryan White program administered by HRSA. The Ryan White program is the single largest federal program designed specifically for people with HIV/AIDS, including the nondisabled poor and undocumented immigrants. The program is considered a lifeline in terms of its payments for health and dental care, medications, and other services (e.g., case management and transportation) that are not covered by other funding sources and complete a comprehensive program of care for people with HIV/AIDS.13 There is, however, considerable variation in the availability of Ryan White services across the country, since federal Ryan White funding
|
12 |
See http://www.cdc.gov/hiv/topics/treatment/MMP/index.htm (accessed February 25, 2011). |
|
13 |
Besides a confirmed HIV diagnosis, to be eligible for care and support services through the Ryan White program, persons must have an income too low to pay for care and have no insurance or not enough insurance to pay for care (HRSA, 2011). |
TABLE 4 Medical Clients Served within the Ryan White Program (All Parts), 2009, by Provider Type
|
Type of Provider |
Percent of Providers |
Number of Medical Clientsa |
Percent of Clients |
|
Hospital-based clinics |
34 |
186,463 |
48 |
|
Publicly funded Community Health Centers (CHC) |
23 |
63,481 |
16 |
|
Other community-based organizations |
22 |
62,958 |
16 |
|
Health departments |
16 |
57,406 |
15 |
|
Private practices |
2 |
5,859 |
2 |
|
Substance abuse treatment centers |
1 |
604 |
<1 |
|
Publicly funded community mental health centers |
<1 |
307 |
<1 |
|
Agencies representing multiple fee-for-service providers |
<1 |
2,663 |
1 |
|
Other |
2 |
9,869 |
3 |
|
Total |
100 |
389,610 |
100 |
|
aSome of these clients use private insurance or Medicare/Medicaid to pay for their care, but their medical provider does receive Ryan White funds to care for uninsured or underinsured clients. SOURCE: Cheever, 2010, citing unpublished HRSA/HAB program data for 2009. |
|||
is provided to state and local jurisdictions, which tend to tailor services based on the needs of local communities (Rawlings and Hopson, 2009).14
Cheever presented 2009 Ryan White program data showing that there were nearly 390,000 medical clients served by 876 Ryan White-funded care sites (Table 4).15 Hospital-based clinics provide medical care to almost half (48 percent) of these clients. Publicly-funded CHCs, other community-based organizations (CBOs), and health departments provide medical care to another 47 percent of the clients at Ryan White-funded sites. Additional providers of medical care services include private doctors’ offices, day treatment programs, home care programs, skilled nursing facilities, and correctional facilities (New York State Department of Health, 2006).
The AIDS Drug Assistance Program (ADAP) is a component of the Ryan White program that provides HIV-related prescription drugs to low-income people with HIV who have limited or no prescription drug coverage. Approximately 183,000 HIV-infected people received medications
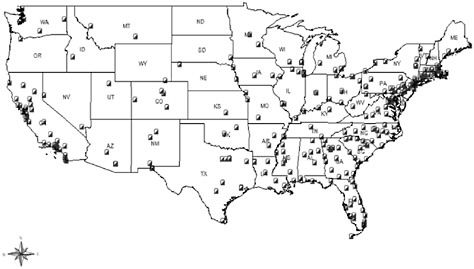
FIGURE 2 Ryan White Part C outpatient care centers of expert HIV care in the United States, 2010.
SOURCE: Kitahata, 2010 (HRSA Geospatial Data Warehouse—2010).
through the ADAP in 2009. Approximately one-third of people with HIV receiving care are estimated to be enrolled in the program (KFF, 2009a).
Sixty-two percent of Ryan White medical provider organizations are not-for-profit, and 35 percent are publicly owned. Just under half (45 percent) are minority organizations (i.e., more than half of board members or professional staff represent racial/ethnic minorities), and 41 percent historically have served racial/ethnic minority clients (Cheever, 2010, citing unpublished HRSA/HAB program data for 2009).
The high volume of HIV/AIDS care provided in the Ryan White-funded clinics has led to their becoming centers of expert HIV care in the United States. Part C of the Ryan White program funds planning grants, capacity development grants, and grants to service providers to support early intervention outpatient services and ambulatory care. Figure 2 shows a map of the Part C-funded outpatient clinics in the United States with more clinics in regions where HIV is more heavily concentrated.
Despite the success of Ryan White-funded clinics as models for the provision of expert HIV care in the United States, a 2008 survey of Ryan White Part C-funded programs16 conducted by the HIV Medicine Association (HIVMA) and the Forum for Collaborative HIV Research showed that a majority of the programs reported that it was difficult or very difficult to
TABLE 5 Services Provided by Ryan White Care Sites (All Parts), 2009
recruit physicians (69 percent), NPs (56 percent), and PAs (57 percent) to serve their clients (Weddle and Hauschild, 2010; personal communication with Andrea Weddle, January 21, 2011).
Steven Johnson, Medical Director of the Mountain-Plains AIDS Education Training Center and Professor of Medicine, Division of Infectious Diseases, University of Colorado School of Medicine, pointed out that in areas of high HIV/AIDS prevalence, newly diagnosed patients are likely able to access expert HIV programs. In lower prevalence areas, however, where there are no such programs, patients may have to see providers with less HIV training and experience. This is the case in his experience as the Medical Director of the Mountain-Plains AETC that serves an eight-state region17 where there may be just a few HIV expert programs per state. In the Mountain-Plains region, there are many areas of low prevalence, and low population density, in a large geographic area. It may be especially difficult for uninsured and/or undocumented residents of rural or frontier areas to find care.
In addition to medical care, Ryan White providers offer comprehensive ancillary services. Examining the array of services available to clients helps to understand staffing needs at these care sites. Table 5 shows the extent to which case management, treatment adherence, mental health, substance abuse, oral health, and other services are provided by Ryan White funded sites. The table shows a heavy reliance on nonmedical support personnel
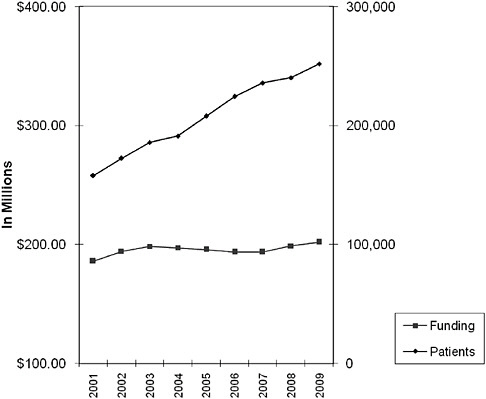
FIGURE 3 Ryan White Part C clients and funding, 2001–2009.
SOURCES: KFF, 2009c; Andrea Weddle, personal communication with HRSA HIV/AIDS Bureau, 2009.
(e.g., social workers and outreach workers). The provision of support services improves retention in care (Sherer et al., 2002).
There has been a dramatic increase in the number of clients served in Ryan White clinics in the past decade. Figure 3 shows a 59 percent increase in the number of clients served in Ryan White Part C clinics from 2001 to 2009, with a concurrent increase in funding of only 8.6 percent, representing a decline in dollars per client served of about one-third.
Conclusions
Including both diagnosed and undiagnosed cases, a substantial number of people living with HIV in the United States have not received medical
care or are not currently in care for HIV.18 The potential to increase demand for care with more active outreach and testing is therefore considerable.
The most recent nationally representative data on the characteristics of HIV/AIDS care and providers date from 1994 to 2000. At that time the most frequent sources of HIV care were physicians’ offices and hospital- or community-based clinics. Provider data available for Ryan White funded programs in 2009 indicate that hospitals, CHCs, other CBOs, and health departments are now the most frequent sources of HIV medical care. These data, however, do not reflect full range of HIV provider usage in the United States. There is, therefore, a great need to compile current nationally representative data on the care that HIV-infected individuals receive and where the care is delivered to help inform policy decisions in this area. The Medical Monitoring Project is a current effort in this regard.
HIV-infected individuals living in rural or sparsely populated areas may experience difficulty in accessing HIV care (Kempf et al., 2010; Ohl et al., 2010; Sarnquist et al., 2011). Having an HIV expert or experienced provider visit a local medical practice or clinic periodically and linking experts to rural providers via telemedicine technology could increase access to expert care for individuals in these areas.
HIV-RELATED TRAINING AND EXPERIENCE OF HIV CARE PROVIDERS
The committee was asked to explore the HIV-related training or experience of HIV care providers (i.e., physicians, PAs, advanced practice registered nurses [APRNs]/NPs, and RNs) as well as improvements in training or experience that are needed to help absorb an increased number of newly diagnosed individuals as a result of expanded HIV testing services. The discussion of “HIV care providers” is complicated by the numerous specific subgroups that provide medical care for individuals with HIV/AIDS. Within each of the health professions listed (physicians, PAs, APRNs/NPs, and RNs), practitioners may have specialized training or experience in the provision of HIV/AIDS care or have minimal training or experience in HIV/AIDS care yet be called upon to provide care to patients with HIV. For example, there are (1) non-HIV/primary care providers (e.g., physicians, APRNs, and PAs who have no specialized training in or significant experience with HIV/AIDS care), (2) HIV/primary care providers (e.g., physicians, APRNs, and PAs who have specialized training in and/or significant expe-
rience with HIV/AIDS care), (3) non-primary care/HIV/infectious disease specialists (e.g, physicians who are HIV/infectious disease specialists, but provide no routine primary care for their patients), and (4) primary care/HIV/infectious disease specialists (e.g, physicians who are HIV/infectious disease specialists, but provide routine primary care for their patients). For patients receiving HIV and primary care from more than one provider, the definition of and critical interactions between “primary care” and “HIV” interventions may become blurred. For example, does the management of hyperlipdemia, a frequent complication of HIV medications, fall within the realm of the “non-primary care HIV” provider or the “primary care” provider?
To the extent possible, this report applies the following designations:
-
HIV care providers: any health care providers who routinely care for one or more individuals with HIV/AIDS;
-
Primary care providers: physicians, APRNs/NPs, and PAs who are trained to provide primary care to patients (they may or may not also be certified, credentialed, or experienced in HIV/AIDS care);
-
Infectious disease specialists: physicians sub-boarded in infectious diseases (they may or may not also serve as the principal source of primary care for their patients and may or may not be experienced in HIV care); and
-
Generalists: health care providers who have neither specialized nor are certified, credentialed, or experienced in HIV/AIDS care.
Primary care providers (physicians, APRNs/NPs, PAs) provide much of the medical care for individuals living with HIV/AIDS. Since the early years of the epidemic, substantial and similar proportions of persons with HIV have received their HIV-related care from primary care providers and from infectious disease specialists. In some analyses, primary care physicians have comprised more than half (56–58 percent in two studies) of physicians who care for persons with HIV (HRSA, 2010c).
In a 1997 to 1999 survey of physicians19 designated by patients as their HIV provider found that 60 percent were generalists and 40 percent had infectious disease training (RWJF, 2008). About one-third of the generalists did not consider themselves to be HIV experts, whereas only 4 percent of those specializing in infectious disease reported that they were not experts in HIV (RWJF, 2008). Andrea Weddle, Executive Director, HIV Medicine Association, provided the committee with data on the medical specialty distribution of the membership of HIVMA, an organization of medical professionals, including physicians, NPs, PAs, and other professionals,
who practice HIV medicine. Among the 3,155 members who responded to a HIVMA survey, 71 percent are adult infectious disease specialists and 7 percent are internal medicine providers (personal communication with Andrea Weddle, December 2010).20
Defining HIV Expertise
Studies have suggested that provider experience caring for people with HIV improves the care and outcomes of individuals with HIV/AIDS (Landon et al., 2003, 2005; Wilson et al., 2005b). There are challenges, however, in designating an HIV/AIDS provider as “expert.” Mari Kitahata, Director, Clinical Epidemiology and Health Services Research, Center for AIDS Research, University of Washington, discussed how providers ideally would be deemed “experts” on the basis of their patients’ outcomes, for example, whether patients’ survival was lengthened or quality of life improved. However, measuring providers’ influence on outcomes is difficult. There are some limited measures of processes of care that are indicators of quality of care. Most of these indicators assess routine tasks, for example, the administration of vaccinations, prophylaxis for pneumocystis carinii pneumonia, and screening for AIDS-related infections (Gross et al., 2000; Kitahata et al., 2003; Wilson et al., 2005b). There are a few indicators in use of more complex tasks, such as appropriate highly active antiretroviral therapy (HAART) therapy and monitoring of viral load.
Although there is no uniform definition of or standard for recognizing HIV expertise among providers, there is some agreement that a combination of provider experience with HIV patients and continuing education in HIV patient care are important elements. Three professional bodies that have specified standards for HIV expertise are HIVMA, created in 2000 by the Infectious Diseases Society of America; the Association of Nurses in AIDS Care (ANAC), and its sister body the HIV/AIDS Nursing Certification Board (HANCB); and AAHIVM.
HIVMA does not certify or credential physicians as experts in HIV medicine (e.g., through use of a standardized exam), but it does recommend that determination of the expertise of “HIV-qualified physicians be based on a combination of patient experience and the demonstration of ongoing education and training in HIV care, especially in the area of antiretroviral
therapy” (HIVMA, 2010). In particular, HIV-qualified physicians should, “in the immediately preceding 36 months,”
-
have “provided continuous and direct medical care, or direct supervision of medical care, to a minimum of 25 patients with HIV”;
-
have “successfully completed a minimum of 40 hours of Category 1 continuing medical education [CME] addressing diagnosis of HIV infection, treatment for HIV disease and comorbidities, and/or the epidemiology of HIV disease”21; and
-
continue to earn “a minimum of 10 hours per year” (HIVMA, 2010).
In addition, HIV-qualified physicians should “[b]e board certified or equivalent in one or more medical specialties or subspecialties recognized by the American Board of Medical Specialties or the American Osteopathic Association” (HIVMA, 2010).
HIVMA further states:
Recently trained infectious diseases (ID) fellows or those recently certified or recertified in infectious diseases should be considered qualified providers of patients with HIV/AIDS for 12 months after certification or recertification as outlined above. However, given the rapid pace of change in HIV medicine, board certification in infectious diseases and pediatric infectious diseases does not guarantee sufficient knowledge to assure that an ID specialist will remain an expert in HIV disease over time. Therefore, all physicians (including ID and pediatric ID physicians) should meet the [ongoing] experience and education based criteria outlined above to retain their HIV-qualified status. (HIVMA, 2010)
Although HIVMA recognizes the critical role of nurse practitioners and physician assistants in the provision of HIV care, the preceding qualifications were developed specifically for physicians (HIVMA, 2010).
HANCB offers two levels of HIV/AIDS nursing certification to formally recognize that certified nurses have met a national standard of requisite HIV/AIDS knowledge. Eligible candidates who pass the certification exam receive certification for a period of 4 years. Certification may be renewed by retaking and passing the current exam or submission of continuing education credits as specified by HANCB. Registered nurses are eligible for certification as an AIDS Certified Registered Nurse (ACRN). In addition,
HANCB recommends that candidates have a minimum of 2 years of experience in “clinical practice, education, management, or research related to HIV/AIDS nursing.”22 Registered nurses are eligible for certification as an Advanced AIDS Care Registered Nurse (AACRN) if they hold an advanced degree (master’s degree or higher) in nursing, ideally with a focus in HIV/AIDS nursing, and have a minimum of 3 years experience as a RN and a minimum of 2,000 hours of HIV/AIDS nursing within the 5 years preceding application.23
AAHIVM has a credentialing program for several types of providers. Eligible physicians (M.D., O.D.), NPs, and PAs can receive a 2-year certification as a HIV Specialist or HIV Expert upon successful completion of a knowledge-based exam in HIV medical care. Clinicians who provide ongoing care for a specified number of HIV patients (e.g., at least 20 HIV patients) are eligible for credentialing as an HIV Specialist (AAHIVS). Providers who care for fewer than 20 patients may receive HIV-Specialist certification under AAHIVM’s clinical consultant program. The experience requirement is effectively waived for nonpracticing clinicians; those providers are eligible for certification as HIV Experts (AAHIVE). HIV-specialized pharmacists are eligible to receive HIV Pharmacist (AAHIVP) certification. All providers who are eligible for certification must have at least 30 hours of HIV-related continuing education credits (or equivalent) in the 24 months preceding their application. AAHIVM-credentialed providers must retake the exam every 2 years in order to recertify.24
Current HIV-Related Training of Physicians, Nursing Professionals, and Physician Assistants
Physicians
Stephen Boswell, President and CEO of Fenway Health, Boston, Massachusetts, presented an overview of potential HIV/AIDS physician providers in the United States. There are approximately 350,000 primary care physicians25 (e.g., internal medicine, family practice, pediatrics) (Sataline and Wang, 2010) and about 4,500 infectious disease specialists engaged in patient care in the United States (AAMC, 2008). Research has shown that sufficient provider experience with HIV patients is more important than area of specialization in the quality of care provided to HIV-positive
|
22 |
See http://www.hancb.org/certification.htm (accessed March 3, 2011). |
|
23 |
See http://www.ptcny.com/clients/HANCB/ (accessed March 3, 2011). |
|
24 |
The information about AAHIVM credentialing is drawn from AAHIVM (2011a), as well as a prior version of the website that was last accessed on February 22, 2011. |
|
25 |
In 2008, the AAMC suggested that there were approximately 228,000 physicians practicing patient care AAMC (2008). |
individuals (Kitahata et al., 2003; Landon et al., 2003, 2005; Wilson et al., 2005b). Different studies cite different numbers of HIV patient encounters in their characterization of more experienced physicians (Brosgart et al., 1999; Kitahata et al., 2003; Landon et al., 2002; Stone et al., 2001). HIVMA cites provision of care or supervision of care for a minimum of 25 patients with HIV as a qualification of physicians who manage the treatment of persons with HIV (HIVMA, 2010), and AAHIVM requires provision of care for at least 20 HIV patients over the past 24 months for certification as an HIV specialist (see footnote 23).
Training primary care providers in the care of people with HIV has been proposed as a way to better meet the health care needs of this population (Adams et al., 2010). There is a lack of data on the current HIV-related training of primary care physicians as well as for physicians in other specialties. Although the mode of care for HIV has shifted to one that is based primarily on outpatient rather than inpatient care, there is evidence that the limited training in HIV that internal medicine residents receive is largely inpatient-based. In a recent multicenter study of internal medicine residents (n = 223) in Baltimore, Boston, Detroit, and New York City, for instance, 50 percent of respondents had more than 30 HIV inpatient encounters in the past year, but the majority of respondents had limited outpatient exposure to HIV care, providing care for only 1 to 5 HIV outpatients. Thirty-nine percent of the residents stated that they did not feel competent to provide HIV outpatient care (Phillips et al., 2010). In another study, a review of U.S. internal medicine residency programs found that only 45.6 percent of programs offer a dedicated rotation in outpatient HIV care, and only 50.5 percent of programs had HIV care curricula in place (Adams et al., 2010).
Steven Johnson described the general lack of HIV experience and training of health care providers in the eight-state Mountain-Plains region served by the AETC. At the University of Colorado, where he cares for HIV/AIDS patients and provides training, he noted the following shortcomings of resident training:
-
Most HIV care experiences are limited to inpatient settings.
-
HIV training is not a mandatory part of any of the residency programs apart from the infectious disease fellowship.
-
Less than 10 percent of internal medicine residents rotate through the outpatient HIV program.
-
Trainees in the Family Practice program receive virtually no HIV experience.
Compared with other medical specialty areas, there are few opportunities for physicians interested in HIV/AIDS to pursue advanced training.
Andrea Weddle mentioned that a recent HIVMA review of fellowship programs determined that four programs that were known to be available had been eliminated due to a lack of financial support and not a lack of interest on the part of medical graduates (personal communication with Andrea Weddle, January 20, 2011).
CME is another potential source of HIV training. Johnson described the difficulties of providing sufficient training in a CME environment to enable generalists to become HIV experts. At the Mountain-Plains AETC, the training offered to non-HIV providers tends to emphasize HIV testing, post-exposure prophylaxis, and the recognition of HIV/AIDS complications, rather than the ongoing treatment and care of HIV-positive individuals. In addition, there is difficulty in attracting providers to educational programs that involve little or no portion of their practice. Despite the challenges of reaching community-based providers, Johnson noted the role of AETCs as an important source of HIV-related education and training for physicians, nursing professionals, and other providers. In addition, there is potential to expand this existing training and education resource to a broader audience, such as by linking with universities to offer training for undergraduate and graduate students.
Nursing Professionals
Nursing constitutes the largest health care occupation, with more than 2.6 million registered nursing jobs in 2008 (BLS, 2010b). More than 250,000 nurses are APRNs (HRSA, 2010b), including more than 157,000 NPs,26 who hold advanced degrees and have passed national certification exams. As noted in the 2011 IOM report “The Future of Nursing: Leading Change, Advancing Health,” the nursing profession has the potential to affect wide reaching changes within the health care system because of its numbers and capacity (IOM, 2011a). Furthermore, nurses’ proximity to patients and understanding of care processes across the continuum of care poise them to act as partners with other health professionals and help coordinate comprehensive care for their patients (IOM, 2011a). Driven in part by technologic advances in patient care that enable people to live longer with chronic disease, increasing emphasis on preventive care, and the aging of the Baby Boomer generation, employment of RNs is expected to grow by 22 percent from 2008 to 2018 (BLS, 2010b).
In the areas of HIV prevention, testing, care, and treatment, nurses may assume multiple roles and responsibilities, depending upon their level of education and training and the state regulations under which they prac-
|
26 |
See http://www.statehealthfacts.org/comparetable.jsp?ind=773&cat=8&sort=1771 (accessed March 3, 2011). |
tice. The roles of nursing professionals in HIV care include, but are not limited to, prevention counseling, referrals for testing, pre- and post-test counseling, symptom recognition and management, referrals and linkages into care, patient navigation, and supporting medication adherence. APRNs are qualified primary care providers who may diagnose patients, prescribe medication, and oversee treatment. As such, APRNs play an important role providing medical care to HIV patients. As noted in the IOM report, however, state nursing board regulations may limit the ability of APRNs to maximally utilize their education and training by, for example, prohibiting them from prescribing certain medications or not permitting them to practice without physician oversight (IOM, 2011a).
In addition, many nursing professionals are not exposed to adequate HIV training and thus may not be prepared to assume essential roles and responsibilities in the care of HIV patients. Adele Webb, Executive Director/CEO, Association of Nurses in AIDS Care, described how, for example, nursing students may have little or no exposure to HIV content in nursing school curricula.27 If HIV is covered, it may be covered briefly in the context of other infectious diseases. Furthermore, clinical rotations during nursing school often do not expose nursing students to HIV patients. Webb stated that there are few, if any, designated inpatient HIV/AIDS units or rotations outside of hospitals. In the area of psychosocial training, nursing school curricula do not adequately address HIV-stigma-related issues or the myths and fears that persist about HIV. The national examination required for graduating nurses includes very little on HIV, giving instructors little incentive to cover HIV issues extensively in their teaching, according to Webb.
HIV/AIDS nursing exists as a specialty for nurses who focus their work on provision of care for patients diagnosed with HIV/AIDS. As previously described, RNs and APRNs can become certified/credentialed in HIV care (e.g., ACRN, AACRN, AAHIVM credentialing), but the number of nursing professionals earning certification/credentials in HIV care has declined, according to Webb. Today, nurses in a variety of specialties and settings are providing care to individuals with HIV in part due to the evolution of HIV into a more chronic condition (Bradley-Springer et al., 2010).
A 2009 ANAC assessment (focus groups and online surveys) of education and knowledge gaps underscored the lack of HIV training, education, and knowledge among nurse generalists (non-HIV specialists). Participants (n = 1,600) were nurses of all ages and education and experience levels who worked in hospitals, hospital-based clinics, primary care clinics, and home care agencies. Respondents self-identified as representing the fields of primary care, maternal/child health, emergency medicine, critical care,
and home care. Regardless of experience, level of education, or age, a large majority (88 percent) of the participants stated that they had very little or no HIV education during school and very little or no HIV training during employment. Thirty-seven percent stated that they do not refer patients for HIV testing, and 35 percent did not know where to refer a patient for HIV care. Respondents cited prevention, testing guidelines, testing methods, risk assessment, symptom recognition, access to care and referral issues, and post-exposure prophylaxis when asked what they felt they needed to know about HIV (personal communication with Adele Webb, November 2010).
Federally Qualified Health Centers (FQHCs) and Nurse Managed Health Centers28 are increasingly asked to take on the role of providing care to individuals with HIV. The general shortage of nurses in the context of expansion of these health centers has created an acute shortage of nurses at these facilities, which are an important source of care for many individuals with HIV, according to Webb.
Physician Assistants
PAs have played a critical role in caring for persons with HIV since the beginning of the epidemic, both as members of care teams and as primary HIV care providers (Wilson et al., 2005a). PAs work under the supervision of a physician (either on- or offsite), performing a broad array of services traditionally carried out by physicians such as examinations and procedures, ordering treatments, prescribing medication, and referring patients to specialists. PAs may function as the primary care provider in medical offices in rural or inner-city areas where there are physician shortages and where a physician may be present only 1 or 2 days per week (BLS, 2010a). PAs held about 74,900 jobs in 2008, and employment for PAs is expected to grow by 39 percent from 2008 to 2018, reflecting the expansion of health care and an emphasis on cost containment (BLS, 2010a). The quality of HIV care provided by PAs who are experienced in the care of individuals with HIV has been found to be comparable to that of physicians on measures such as use of HAART and control of patient viral load (Wilson et al., 2005a).
I. Jean Davis, Associate Professor, Charles Drew University of Medicine and Science, described the current HIV-related training and experience of PAs as inadequate. PAs receive little HIV-related education while in training and, other than the training provided through AETCs, there are no HIV-related post-graduate training opportunities for PAs. As is the case for physicians and nursing professionals, PAs may have few opportunities during training to care for HIV patients in outpatient settings where most
HIV-infected individuals receive their care. Davis noted that PAs, along with NPs and physicians, can be credentialed as HIV specialists or experts by the AAHIVM (as described previously).
Improvements in Training and Experience Needed to Absorb a Greater Number of Newly Diagnosed Individuals Resulting from Expanded HIV Testing
Physicians
Training of primary care physicians to diagnose and provide quality treatment and care for HIV-infected individuals is crucial not only to treat a greater number of newly diagnosed individuals, but also to ensure the best care possible for those currently in care. Greater exposure of medical students and residents to HIV patients in outpatient settings will help them develop an increased level of comfort and cultural competence in interacting with HIV-positive individuals, as well as a greater appreciation for the complexity of care such patients may require. In addition, such exposure may help to challenge any stigmas and stereotypes they might hold about the population of individuals infected with HIV. Cultural competency increases when trainees care for racial/ethnic minority group members, individuals who exhibit high-risk behaviors (e.g., men who have sex with men, intravenous drug users), and people living in poverty.
For medical students and residents, exposure to HIV care could be augmented, especially in outpatient settings, and the importance of taking a comprehensive sexual history and providing routine HIV testing emphasized. Cultural competence could be improved through experiential learning, especially regarding differences in knowledge, attitudes, and practices regarding sex, alcohol and drug dependency, and poverty and its effects on health behaviors. A potentially under-recognized area of cultural (in)competence is the senior population, which, as already noted, poses additional challenges in terms of sexual history taking, education about HIV transmission and prevention, and provision of HIV testing, as well as the care needs of those living with HIV/AIDS.
For medical residents there is a need to expand outpatient training opportunities in HIV medicine, for example, by offering an HIV clinic as an option for residents’ primary care clinic experience. Residency programs in FQHCs and other primary care settings could be established or expanded. To facilitate this, grant mechanisms could be developed to encourage health centers to be accredited as Teaching Health Centers.29
Ties between community-based providers and medical schools, academic hospitals, and/or academic health centers can enhance the quality of care and potential for workforce development.30
The committee heard that there is also a general need for support of HIV-related clinical training opportunities for primary care providers. Support is needed for AETC provision of HIV/AIDS-related CME to practicing physicians and other health care providers. Opportunities for CME might be increased through satellite learning and consultation through HIV/AIDS-related teleconferences and web-based programs; mini-sabbatical trainings (3 to 5 days in duration); independent, multi-company sponsored CME programs; and HIV certification after residency (e.g., credentialing through the AAHIVM and HIV fellowships, such as those available through the Doris Duke Charitable Foundation’s Clinical Research Fellowship program). Brian Hujdich, HealthHIV, stated that requests for information from HealthHIV, which functions as the AETC National Center for HIV Care in Minority Communities, by providers have included how to improve patient access to substance abuse treatment, reproductive services, and oral health care. Primary care provider organizations also have expressed interest in education on HIV-related topics, including HIV comorbidity and pre-exposure prophylaxis.
Nursing Professionals
Webb discussed interventions recommended by ANAC to increase the number of HIV-trained nursing professionals. Webb highlighted the need to conduct a national assessment of the readiness of nonspecialist RNs and APRNs to provide testing, care, and treatment for an increased number of people with HIV/AIDS. The assessment would help to identify knowledge, competence, performance, and skills gaps to guide development of training tools. Appropriately trained RNs can fill important roles in the implementation of routine HIV testing, prevention counseling, and care for HIV-infected individuals, including patient education and care coordination. Registered nurses, licensed practical nurses, nursing assistants, and other providers in long-term care facilities increasingly will be called upon to care
|
in subsequent years to encourage “teaching health centers” (THCs) to expand or establish new primary care residency programs. The law defines a THC as an entity that (1) is a community-based, ambulatory patient care center, and (2) operates a primary care residency program (AAMC.org [accessed October 5, 2010]). |
for HIV-positive individuals experiencing dementia and other debilitating comorbidities. Training to develop the cultural and clinical competence to care for this subpopulation of persons living with HIV/AIDS will be an important factor in meeting their needs. Nurse practitioners experienced in HIV/AIDS care are an important resource in the provision of medical care to greater numbers of HIV-infected individuals. Their role as primary care providers may be especially important in addressing the need for medical care in areas experiencing a shortage of physicians. Data from the national needs assessment could be used to ensure that health workforce shortages and education and training needs are included and strengthened through implementation of the National HIV/AIDS Strategy (ONAP, 2010), the ACA, and the Ryan White Care Act. To improve HIV nursing education further, Webb recommended
-
integration of more substantial HIV prevention, care, and treatment education into nursing school curricula (e.g., ANAC’s Core Curriculum for HIV/AIDS Nursing);
-
increased opportunities for nursing students to learn about the field of HIV through exposure to HIV care environments during clinical rotations (e.g., Ryan White clinics, public health departments, community health centers);
-
development and availability of clinical fellowships in HIV care for RNs and NPs at all levels of experience;
-
increased emphasis on HIV/AIDS at nursing schools and the establishment of programs throughout the United States that encourage nursing students to enter the HIV/AIDS workforce;
-
support for the National HIV/AIDS Strategy recommendation that HRSA issue guidance to encourage HIV-specific training in curricula (specifically including RN and NP programs); and
-
utilization of ANAC, AETC, and other HIV care provider networks to conduct nationwide training on HIV care.
Physician Assistants
There is a need for increased HIV-related education and training opportunities for PAs, including exposure to the treatment of individuals with HIV in outpatient settings. As noted previously, in addition to working within care teams PAs may function, under the supervision of a physician, as principal care providers and are particularly important in areas where there are physician shortages (e.g., rural areas, inner cities). Employment for PAs is expected to grow substantially over the next several years (BLS, 2010a). Ensuring adequate HIV education and training for this segment
of the health care workforce is an important opportunity to accommodate increases in HIV testing and care.
Conclusions
A critical shortcoming of the training of physicians, nursing professionals, and physician assistants is the limited exposure to patients infected with HIV in outpatient settings, the site of most HIV/AIDS care. With advances in antiretroviral drug therapy and medical management, most HIV-infected individuals receive care outside of hospitals. When the clinical experiences of providers in training are limited to inpatient settings, trainees are not exposed to the full range of care and treatment needs of individuals living with HIV. They also do not benefit from learning directly of the successes of HIV/AIDS care. In addition they may miss opportunities to increase their exposure to a patient population more representative of patients with HIV. At the same time, there is a need for greater attention to and preparation to meet the needs of the aging population of persons living with HIV/AIDS, who are increasingly likely to require long-term care for dementia and other debilitating conditions.
Although medical students generally learn about HIV/AIDS during their infectious disease courses, there is little emphasis on the practical aspects of caring for individuals with HIV/AIDS. Primary care physicians also have very few post-graduate HIV-related training opportunities. Such experiences in HIV care are essential, both to increase interest among physicians in becoming experts with a substantial focus on HIV care, and to familiarize all physicians with the disease and its complications so they are better prepared to assume responsibility for the patients in settings where HIV experts are not consistently available. A number of the HIV fellowship programs that were available within the last five years have been closed due to a lack of financial support.
The absence of basic curriculum content pertaining to HIV/AIDS in nursing training programs poses serious challenges to meeting future HIV/AIDS staffing needs. Registered nurses and APRNs assume central roles in testing and treatment programs, yet there is virtually no HIV-related content for nurses in training and few outpatient placements.
AETCs are in place to provide ongoing training opportunities for physicians, nursing professionals, and other health care professionals, but there are difficulties in reaching community-based providers who may not have many HIV/AIDS patients in their practices. Providers need to be aware of the changing landscape of HIV/AIDS care and also of the legal/regulatory environment in which HIV testing occurs. They may not be familiar with CDC’s revised recommendations for routine HIV testing in health care settings, which recommend that separate written informed consent and
prevention counseling not be required for HIV screening in these settings (Branson et al., 2006; Burke et al., 2007; Jain et al., 2009).31 Providers also are often unprepared to provide education and counseling following the receipt of a patient’s positive HIV test result. As many community-based providers are in the position to implement CDC’s recommendations for routine HIV testing, these areas could be considered important areas of focus for AETCs.
HIV-infected patients of providers with substantial HIV/AIDS experience/expertise have better outcomes, but there are few widely used measures of such expertise. The qualification requirements issued by HIVMA, HANCB, and AAHIVM are helpful in this regard.
Increased trainee exposure to outpatient primary care environments, such as in FQHCs, could improve provider competence in HIV care and facilitate future practice in such settings. Experience in community-based HIV care environments also could improve trainee cultural competence. Expansion of post-graduate education and training opportunities, particularly fellowship programs, for physicians, APRNs, PAs, and other care providers is needed. Finally, although AETCs are viewed as important sites for CME, wider application of innovative models for CME, including web-based programs, could expand training opportunities for practicing clinicians.
THE CAPACITY OF THE HIV/AIDS CARE DELIVERY SYSTEM
The capacity of the HIV care workforce to accommodate an increased demand for care by persons with HIV depends upon both the availability of sufficient positions and the availability of providers to fill those positions. In terms of the latter, projections indicate that the supply of HIV providers is not keeping up with demand for HIV care (HRSA, 2010c). In addition, funding cuts and reductions in available positions that support HIV programs that have occurred, such as in health departments (NACCHO, 2010), may decrease the health care system’s capacity to provide care for more persons with HIV.
Capacity Implications of the Aging HIV/AIDS Workforce
The committee was asked to address whether the age profile of providers is compatible with sustainability of the HIV care delivery system.
Specifically, “are younger clinicians and/or students receiving adequate training/experience to meet future needs?”
With regard to the health care workforce in general, an estimated 33 percent of physicians and 24 percent of pharmacists are expected to reach retirement age by 2020 (AAMC, 2010; HRSA, 2010c) and are either reducing their practices or retiring altogether. The AAMC Center for Workforce Studies projects a shortage of 45,000 primary care physicians by 2020 (AAMC, 2010). The nursing workforce currently includes substantial numbers of nurses who are reaching retirement as well as a high proportion of nurses at the beginning of their careers. A 2006 report prepared by the Center for Health Workforce Studies, School of Public Health, University at Albany, projected that 45 percent of RNs in 2006 would reach retirement age by 2020 (CHWS, 2006). The report further estimated that total replacement needs for APRNs due to retirement would exceed 61,000, with at least 40,000 replacement openings for NPs (CHWS, 2006). Midcareer nurses, the group most needed to fill the roles of those leaving the workforce and with the knowledge, experience, and mentoring that senior nurses can provide, are the lowest in number (Bleich et al., 2009; IOM, 2011a). Almost 65 percent of professionally active dentists in 2006 were age 45 or older (ADEA, 2008), and 44 to 46 percent are expected to retire by 2020 (CHWS, 2006; HRSA, 2010c). Other providers are closing their practices due to underfunding (HRSA, 2010c). At the same time, the United States population is expected to increase by 29 percent between 2000 and 2030 (HRSA, 2010c), and the average age of the overall population is increasing as well, resulting in more people seeking care. The numbers of new providers entering the workforce are projected to be inadequate to meet the growing demand.
There are no current nationally representative estimates of the size and demographic composition of the HIV workforce. To help the committee better understand the implications of the aging HIV/AIDS workforce, Andrea Weddle presented information on the age distribution of the 3,155 U.S.-based members of HIVMA, the majority of whom are physicians. Forty-five percent of the workforce is more than 50 years of age and the proportion by decade of age is highest for those 51 to 60 (Table 6).
These findings are consistent with a 2008 survey of 400 providers and student members of the American Academy of HIV Medicine (AAHIVM).32 Almost one-third of the respondents reported that they were in the last quarter of their careers, with plans to retire within 10 years (Carmichael et al., 2009). A majority of respondents were concerned about impending shortages of HIV providers as more than 90 percent of them reported that they had seen an increase in patient load in the last 2 years.
TABLE 6 Age Distribution of U.S. HIVMA Members, 2010
|
Age Group |
Percent |
|
30 and younger |
2 |
|
31 to 40 |
22 |
|
41 to 50 |
23 |
|
51 to 60 |
28 |
|
61 and older |
17 |
|
No response |
8 |
|
NOTE: n = 3,155. SOURCE: Weddle and Hauschild, 2010. |
|
Adele Webb provided information on the aging of the nursing workforce. The average age of registered nurses in the United States is projected to be 44.5 years by 2012, meaning that nurses close to retirement age are expected to be the largest segment of the RN workforce in the next five years (AACN, 2010). The number of nurses over age 50 more than quadrupled between 1983 and 2009, and the number of middle-aged nurses (age 35-49) doubled. Together these two age groups comprise almost 75 percent of the nursing workforce (IOM, 2011a). In terms of nurses specializing in HIV/AIDS care, Webb reported that nearly 60 percent of ANAC members are between 40 and 50 years of age (Association of Nurses in AIDS Care database, compiled by Kimberly Carbaugh, September 2010), while only 7 percent of ANAC members are 20 to 29 years old, evidence that recent nursing school graduates are not entering the HIV/AIDS field at a pace necessary to keep up with future needs.
Just as the physician and nursing workforces are aging, so too is the public health workforce, which serves an essential role in the delivery of HIV prevention and care services and programs. This is occurring at the same time as demands for services in the areas of surveillance, education, administration, and care have increased. Kathryn Hafford provided the committee with data pertaining to the public health workforce. The Association of Schools of Public Health has estimated that 250,000 more public health workers will be needed by 2020 (ASPH, 2007). However, this workforce is diminishing, forcing public health workers to do more with fewer resources.
In addition to shortfalls in training, the public health workforce is aging. According to a 2007 workforce trends profile, the average age of a state public health worker was 47 and within three years, 20 percent of State Health Agency’s workforce would be eligible to retire. The public
health occupation most frequently cited as experiencing a severe worker shortage was public health nursing (ASTHO, 2007).
Capacity Implications of Fiscal Constraints for the HIV/AIDS Workforce
Even as the data projections indicate a growing shortage of health care professionals, especially in the area of HIV/AIDS care, fiscal constraints are reducing the number of available state health department staff positions, compounding the problem of the shortage of providers.
Individual health care providers are on the front lines of HIV/AIDS clinical care. Supplementing this workforce are individuals staffing health departments across the country and their programs. Anna Buchanan, Senior Director, Immunization and Infectious Disease Association of State and Territorial Health Officials, and Julie Scofield, representing NASTAD, described the essential role of state health departments and their staffs in meeting the needs of individuals with HIV/AIDS. Scofield pointed out that state health departments are responsible for programs that administer more than half of the CDC’s domestic HIV prevention budget and Ryan White program funding. In addition to these federal sources of support, she discussed how state health departments provide additional support to implement the National HIV/AIDS Strategy. State support, however, has declined sharply as states grapple with severe budget constraints following the nationwide recession. For example, states contributed 28 percent of funding available for ADAP in 1998, but only about 14 percent of funding in 2009 ($215 million of $1.59 billion), according to Scofield.
In 2009, NASTAD conducted three surveys of state HIV and viral hepatitis programs to assess the impact of state revenue reductions for fiscal year 2009 and anticipated reductions for 2010.33 In 2010, NASTAD and the National Coalition of STD Directors are conducting a survey of FY 2010 budget cuts.34
According to the 2009 survey, 29 of 45 states reported a total loss of more than $170 million in HIV-related state funding. Specific findings included
-
Twenty-five states reported cuts to HIV prevention programs.
-
Twenty-two states reported cuts to care and treatment programs.
-
Seventeen ADAPs reported cuts from state contributions.
-
Eight states reported cuts to viral hepatitis programs.
-
Six states reported cuts to surveillance programs.
The 2010 survey found 38 states making additional cuts of approximately $70 million. Six states reported the restoration of $44.8 million in state funding, mostly for ADAPs. By September 2010, however, almost $1 million in state funding had already been cut from FY 2011 HIV and viral hepatitis budgets.
State budget cuts have resulted in staff reductions and hiring freezes. Over the past 2 years, 41 states reported more than 200 open or unfilled positions in HIV/AIDS and viral hepatitis programs, representing roughly 20 percent of the total workforce in responding state health department HIV/AIDS, STD, and viral hepatitis programs. Positions that are 100 percent federally funded have not been exempt in most jurisdictions. In 2010, 20 states (up from 13 in 2009) reported mandatory staff furloughs ranging from 1 to 36 days a year. States also have reported pay cuts of up to 2.5 percent, pay freezes, freezes on promotions, early retirements, realignments, and combining field staff duties, along with the resulting negative impact on local health department capacity.
Scofield described how states have reduced grant awards to CBOs to provide HIV care, scaled back training and quality improvement activities, and increased barriers for clients to access care. The budget cuts also have resulted in expanded waiting lists for ADAP. As of mid-March 2011 there were 6,972 individuals on ADAP waiting lists in 11 states, more than double the number of individuals that were on ADAP waiting lists in mid-September 2010.35 Cost containment strategies instituted in 17 states (with an additional 9 states considering them) include reduction of drug formularies, more restrictive income eligibility requirements, and required client cost sharing.
Scofield described how many of the budget cuts and cost containing measures have been implemented on already “trimmed” budgets making it increasingly difficult for the public health workforce to continue “doing more with less.”
Conclusions
Each year, the number of persons with HIV infection who require care in the United States grows. That trend will continue, given the ongoing incident infections, the improved ability to manage complications of the disease, and the policy developments favoring earlier treatment. The HIV/AIDS workforce is decreasing relative to the number of individuals expected to require care. Many physicians, nursing professionals (APRNs and RNs), dentists, PAs, and public health workers engaged in HIV/AIDS-related
|
35 |
See http://www.statehealthfacts.org/comparetable.jsp?ind=552&cat=11 (accessed March 21, 2011). |
prevention and care are aging and nearing retirement. At the same time, younger cohorts of practitioners appear to include fewer members focused on HIV care, and insufficient numbers of new graduates are available to assume responsibility for the population of HIV patients that need care.
The capacity of the HIV/AIDS workforce to accommodate increased numbers of HIV-positive individuals also is strained by fiscal constraints leading to staff reductions in state and local health departments, limiting the public health response to HIV/AIDS at the state and local levels.
Addressing the shortage of providers through strategies to maximize the capacity of the current workforce (discussed in the following section) is only part of the answer. The number of people working in the area of HIV/AIDS care also must increase to meet the patient care demand. In addition to adequate funding to support and maintain necessary staff positions, consideration of various strategies to increase the number of new providers entering the field of HIV/AIDS care is needed.
DELIVERY SYSTEM STRATEGIES TO MAXIMIZE CAPACITY OF CURRENT WORKFORCE
The committee was asked to examine the increases in workforce that would be needed to provide care for the greater number of newly diagnosed HIV-positive individuals expected to result from expanded HIV testing services. This issue is all the more pressing in light of the anticipated provider shortages outlined in the previous section and the anticipated increase in the number of individuals previously diagnosed with HIV accessing health care in the wake of the ACA and more effective efforts to bring people into care. In general terms, there are two approaches to increasing provider capacity. The first, addressed in this section, utilizes delivery system strategies to maximize the capacity of the current health care workforce to care for HIV-positive individuals. The capacity of current providers can only be expanded so much, however. At some point more personnel are needed to accommodate further increases in demand. The second approach employs “pathway” strategies, discussed later in the report, to increase the number of HIV care providers (HRSA, 2010c).
Increased and more effective use of several strategies would help to maximize the ability of the current HIV care workforce to absorb an influx of newly diagnosed individuals, and/or a reduction in the number of available providers. These strategies include task shifting, comanagement, and care coordination models, including medical homes and integrated delivery systems.36
Task Shifting
Task shifting refers to the redirection of tasks from more to less highly trained workers, thereby permitting a more efficient use of human resources. Since the mid-1960s, NPs and PAs have assumed many of the tasks traditionally performed by physicians, freeing physicians either to see more patients or to increase the number or length of visits with existing patients. Similarly RNs may assume expanded procedure-based and clinical judgment skills and designate more routine tasks to others, such as licensed practical nurses, nursing assistants, and community health workers (IOM, 2011a). Task shifting occurs both within health care teams and outside of them, when, for example, NPs practice independently of physicians. In addition to making the greatest use of available providers, task shifting may reduce health care costs and increase provider satisfaction, potentially decreasing attrition from the professions.
Although the concept of task shifting is not new, multiple barriers remain that prevent maximal use of the strategy, including scope-of-practice limitations, payor reimbursement policies, professional resistance, and fragmentation of the health care system.37 Scope-of-practice limitations often prevent qualified providers from practicing to the full extent of their education and training. For example, as discussed in detail in the IOM report The Future of Nursing, APRNs face regulatory scope-of-practice limitations that vary widely from state to state (IOM, 2011a). In some states NPs may practice independently of any physician oversight, while other states place restrictions on the authority of APRNs to prescribe medications, admit patients to hospitals, assess patient conditions, and order and evaluate tests (IOM, 2011a).
Payor reimbursement policies represent another barrier to maximal implementation of task shifting. Scope-of-practice regulations affect credentialing and payor reimbursement eligibility and/or level, for example, by influencing which practitioners are considered “primary care providers” for reimbursement purposes. In addition, NPs and PAs may be reimbursed at lower levels than primary care physicians despite having performed the same tasks (IOM, 2011a).
Full realization of the potential for task shifting to maximize the ability of the current HIV care workforce to absorb a significant increase in patients will depend upon efforts to address such regulatory and policy barriers.
Comanagement
Comanagement refers to the practice of having an HIV expert available to oversee and consult with less experienced generalist practitioners on the provision of HIV care. The generalist practitioner serves as the primary care provider, with the HIV expert available in person and/or by phone, e-mail, or teleconference to advise on the care of patients regularly or as needed. The comanagement strategy may be particularly useful in addressing an increased need for quality HIV care in rural and other settings where HIV care and services are limited. Issues such as billing for consultations and liability concerns may need to be addressed.
Care Coordination Models
Care coordination models take a multidisciplinary approach to addressing the complex care needs of patients who often require the services of a variety of specialists or care providers. Coordination among the various providers should improve the quality of patient care and maximize the efficiency of the system through shared information, expertise, and labor. One coordinated care model is the patient-centered medical home (PCPCC, 2007). A medical home coordinates the provision of comprehensive HIV care within one practice setting. In addition to providing medical care, patients’ primary care providers coordinate and help to arrange for their dental, pharmacy, counseling, educational, and other support service needs. The flexible nature of some Ryan White funding has permitted some medical providers to hire the support staff needed to facilitate access to these other important nonmedical services.
Integrated delivery systems, another type of coordinated care model, build upon the medical home strategy by providing a comprehensive array of services within one system, a sort of “one-stop shopping” for individuals with HIV (HRSA, 2010c). Physicians, PAs, APRNs, RNs, dentists, pharmacists, counselors, and other providers attend to patients in a central location and work together to ensure that care is coordinated and comprehensive. One provider may alert others to missed appointments or medication lapses, permitting someone to reach out to the patients and ensure they return to care. Integrated delivery systems may pay particular attention to factors outside of care that may affect patients’ adherence to visit and drug treatment schedules. They might work with patients who are transitioning from inpatient to outpatient care or from a correctional facility back to society to ensure that the patient does not lapse and services are not dropped during the transition.
Hujdich discussed the role of HealthHIV,38 and potentially other AETCs, in offering capacity building assistance to organizations in the areas of care coordination, clinical services, infrastructure planning, financial support, and information technology. This assistance helps programs with strategic planning to foster linkages to CBOs and to assist with implementation of HIV screening. Financial assistance through the AETC has allowed organizations to hire needed personnel to support HIV-related activities. Such support could help organizations to become medical homes for their patients and even, perhaps, to work toward an integrated delivery system model.
Conclusions
Increased use of strategies such as task shifting, comanagement, and care coordination can help to maximize the ability of the current health care workforce to accommodate an increased number of HIV-positive individuals. In addition, these strategies may result in improved patient care and increased provider satisfaction, which, in turn, may increase the retention of HIV/AIDS care providers in the field. Promotion of such strategies will require changes in some current scope-of-practice regulations and reimbursement, billing, consultation, and liability systems/policies and sufficient flexibility to permit coordination of care among a variety of health and nonmedical care providers.
STRATEGIES TO INCREASE THE NUMBER OF PROVIDERS ENTERING AND REMAINING IN THE HIV/AIDS WORKFORCE
The committee was asked to address the impediments to professionals entering into, or continuing to provide, HIV/AIDS care, as well as policies that inhibit or enhance the movement of health care professionals into HIV/AIDS specialties.
Two physicians, each of whom has delivered care to HIV/AIDS patients for more than two decades, Michael Saag, President of the HIV Medical Association, and Joel Gallant, Professor of Medicine, Division of Infectious Diseases, Johns Hopkins University School of Medicine, described the changing face of the practice of HIV care. They contrasted the care environment that existed in the early days of the epidemic to the care environment today (Table 7). Indeed, most of the presenters invited to speak on the topic described the changing face of the epidemic as one important impediment to the ongoing provision of HIV care and to the movement of health care professionals into HIV/AIDS care.
TABLE 7 HIV/AIDS Care: Then and Now
|
Aspect of Care |
Then |
Now |
|
Hospital care |
Almost all HIV-infected patients were hospitalized at some point |
Few patients are hospitalized |
|
Inpatient profile |
Patients represented a cross section of the epidemic and clinical issues were intellectually stimulating |
Patients are often hospitalized for non-HIV conditions (e.g., psychiatric illness) |
|
Outpatient care |
Little chance of success; feelings of depression and hopelessness |
Trainees are not exposed to the successes of treatment visible in the outpatient setting |
|
Reimbursement |
High rates due to hospitalization and home care |
Low rates |
|
Funding for research from government and institutions |
Available; opportunities for young investigators to advance their careers |
In decline; fewer clinical trials conducted, with greater opportunities in other clinical areas (hepatitis C) |
|
Environment/climate |
HIV medicine viewed as new and exciting and considered a cause and a passion |
HIV medicine viewed as one of many low-paying career choices |
|
|
Epidemic concentrated in the gay community, which was politically organized and active |
Epidemic diffuse, with a concentration among poor, disenfranchised populations |
|
SOURCES: Gallant, 2010; Saag, 2010. |
||
In the following sections, the impediments to new providers entering the HIV/AIDS workforce are described for different professional groups. Following that is a discussion of the challenges of retaining professionals in the field of HIV/AIDS care.
Barriers to Expanding the HIV/AIDS Workforce
Physicians
A number of factors affect HIV/AIDS physician shortages, but key issues identified by Saag, Gallant, and Johnson include financial disincen-
tives, inadequate education/training opportunities, unattractive characteristics of the practice environment, and “reverse brain drain” (see later discussion), in which physicians interested in HIV medicine may pursue what they perceive to be the more interesting challenges of international HIV/AIDS care. Other contributing factors include a reluctance to work with HIV patients, geographic considerations, and more general issues such as too few openings in medical schools.
Financial disincentives Saag pointed to the general unattractiveness of contemporary primary care practice in general as a significant inhibition for entry into HIV/AIDS care. Recently trained graduates of medical schools are typically heavily indebted. The average educational debt of medical school graduates in 2009 was $156,456. Eighty-seven percent of graduating medical students carry outstanding loans (AMA, 2009). When examining their options, graduates know that physicians in primary care settings earn much less than their specialty counterparts and often work longer, less predictable hours. Because of the complexity of HIV/AIDS care, the need to address multiple medical and psychosocial issues when providing care, and the relatively poor patient population served, providers may be unable to cover the expenses of their practices.
Saag shared financial data from his clinic in Birmingham, Alabama, showing very poor physician reimbursement, even for fully insured patients. He suggested that if the Ryan White program were not in place, practices specializing in HIV/AIDS care would not be sustainable. Loida Bonney, Assistant Professor of Medicine, Division of General Medicine, Emory University, stated that the median salary for an assistant professor in infectious disease is approximately $130,000 per year, compared to $148,000 for an assistant professor in general internal medicine (AAMC, 2009).
Inadequate education/training opportunities Since many graduates leave medical school without adequate exposure to HIV/AIDS care, they may never have considered focusing their postgraduate training on this area of medicine. Gallant described how medical students have few opportunities to train with HIV experts and to see them as mentors or role models because of the paucity of medical education taking place in the outpatient and community-based settings where HIV/AIDS care is now provided. According to Webb, this lack of familiarity with HIV/AIDS care is common among nursing graduates as well. Trainees who have had an opportunity to work in public clinics serving poor patients are more likely to work in such settings following graduation.
Gallant described a 2004 HIVMA survey of first-year internal medicine residents conducted in the 10 states with the highest HIV prevalence. Of 729 residents surveyed, 40 percent indicated an interest in working in HIV
medicine or research. Of those, 79 percent reported that they would prefer to prepare for a career in the HIV field through a 1-year focused HIV training program instead of a 2- to 3-year fellowship. Fifty-one percent of respondents said that their medical residency had not prepared them to practice HIV medicine.
Gallant went on to describe another study, a 2008 survey of internal medicine program directors that concluded that internal medicine residents were unprepared for HIV care management (Adams et al., 2010). Although 42 percent of program directors felt that it was important to train residents to be primary care providers for HIV-infected patients, only 19 percent of directors felt that their graduates had the necessary skills. The responding program directors reported the belief that patients prefer to be seen, and receive better care, in infectious disease or HIV clinics than in general medicine clinics, despite the evidence that many HIV/AIDS patients receive care from primary care providers without specialty training in HIV/AIDS. (The response rate to this survey was 62 percent [230 of 372 program directors responded].)
Gallant also discussed the results of a survey conducted to gauge knowledge about antiretroviral drug therapy among physicians caring for hospitalized HIV-infected patients in two community teaching hospitals. In response to a series of 10 clinical scenarios based on antiretroviral prescribing errors, infectious disease or HIV specialist physicians were relatively well informed (the mean percentage of correct answers was 93 percent for infectious disease or HIV specialist physicians), while resident physicians and attending nonspecialist physicians did not perform as well (the mean percentage of correct responses was 33 percent and 37 percent, respectively) (Arshad et al., 2009). High scores were associated with the number of HIV outpatients seen per month and the reported comfort level in managing HIV-infected patients. Errors included those related to dose, frequency, renal dosing, drug interactions, and missing agents.
Gallant discussed how the acknowledgment of evidence showing that “expert” HIV/AIDS care improves health outcomes for HIV/AIDS patients may have discouraged primary care providers from even considering this as an area of special interest, despite the fact that studies indicate that providers’ amount of experience in caring for HIV/AIDS patients (i.e., number of patients served) is a better indicator than specialty training of the quality of care they provide.
Unattractive practice environment Most HIV/AIDS care is provided in outpatient settings, with much of the care provided in publicly supported clinics. Stephen Boswell contrasted the practice environment typical of general outpatient care settings to that of CHCs where HIV/AIDS patients are often seen. Considering all of the health providers available, the ratio
TABLE 8 Staffing Patterns and Benchmark Ratios for Workforce Projections
|
|
Benchmark Ratios |
|
|
Health Center Median (Patients/Staff) |
National Comparison (Patients/Staff) |
|
|
Physicians |
1,709 |
1,500 |
|
NPs/PAs/CNMs |
3,025 |
4,155 |
|
Nurses |
1,479 |
1,298 |
|
All Health Providersa |
1,092 |
958 |
|
aAll health providers include NPs, PAs, certified nurse midwives (CNMs), and physicians. SOURCE: Boswell, 2010 (2006 Uniform Data System, Bureau of Primary Health Care, HRSA, HHS). |
||
of patient to staff is somewhat lower in general outpatient care settings than that typically seen in community health centers (958 vs. 1,092) (Table 8). As Table 8 illustrates, there is a greater burden of care placed on physicians in CHCs as well as a greater reliance on nursing support. Boswell pointed out that not only are patient-to-staff ratios higher in CHCs, the patients cared for in these settings are often poor and disenfranchised with a complex array of medical and social problems that must be addressed. To meet these needs physicians, PAs, NPs, and RNs in CHCs rely on the services provided by medical assistants, medical social workers, and outreach workers.
Bonney described how HIV/AIDS providers working in very busy out-patient settings, frequently without adequate workforce support, are often stressed. Stress and the inability to manage work stress (i.e.,“burnout”) are regular consequences of HIV care (Benevides-Pereira and Das Neves Alves, 2007; Brown and Lescano, 2000; Gerbert et al., 2004; Saag, 2006). These issues affect primary care in general. Medical graduates understand these issues in the context of the substantial income disparities affecting HIV/AIDS and other primary care fields, and opt to enter other medical specialty fields at the expense of primary care. Boswell provided data on changes in residency positions from 1998 to 2006, showing a shift away from primary care and toward specialty practice. The percentage of graduates choosing family practice residencies declined by 51 percent, while those choosing anesthesiology increased by 150 percent (Figure 4). Boswell indicated that in his experience, issues related to the quality of life of a primary care provider are as important as compensation in deterring graduates from pursuing primary care as a career. He highlighted the administrative burdens of primary care practice, for example, spending an hour on paperwork and administrative tasks for every hour of clinic time.
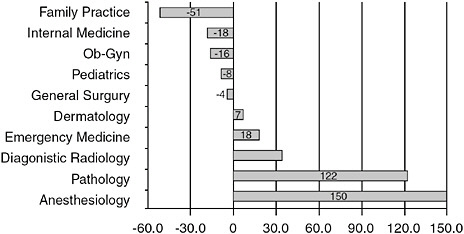
FIGURE 4 Percent change in percentage of U.S. medical school graduates filling select residency positions, 1998–2006.
SOURCE: Woo, 2006.
“Reverse brain drain” Finally, another barrier to providers entering the domestic HIV/AIDS workforce is a kind of “reverse brain drain.” Gallant mentioned the sense that providers in training may perceive HIV/AIDS as a problem of the past and/or as no longer a “cause.” Kitahata observed the need to refocus HIV domestically, noting that the President’s Emergency Plan for AIDS Relief (PEPFAR) has raised the visibility of HIV care in international settings. For those with some interest in HIV/AIDS, attention has shifted to the interesting challenges of international work. The tendency for providers thinking about careers in HIV medicine to consider working abroad was mentioned by Kitahata, Cheever, and committee chair Paul Cleary.39
Nursing Professionals
A key factor affecting the shortage of APRNs and RNs to accommodate increases in HIV testing and care is the lack of training programs resulting, in part, from a shortage of nursing school faculty (IOM, 2011a). Thousands of qualified nursing school applicants were not admitted to nursing programs in 2009 because of a lack of faculty, according to Webb.
|
39 |
Similar observations were made by several speakers at the 2008 National Summit on HIV Diagnosis, Prevention and Access to Care (http://hivforum.blogspot.com/search?q=brain+drain [accessed March 1, 2010]). |
With respect to the capacity of the HIV workforce, the problem of this shortage is compounded by the specialty choices made by graduates of nursing programs. Few young nurses are selecting HIV as a specialty. Non-specialist nurses may lack the specific knowledge, competence, and confidence to provide adequate HIV testing and care. Webb anticipates that the HIV care workforce, under an expanded testing framework and in the context of changes resulting from the ACA, cannot practically accommodate an increased demand without consideration of the training needs of all levels of nursing professionals.
With respect to financial incentives, practicing and experienced nurses often opt out of HIV nursing because of more attractive compensation in other specialty fields.
As discussed previously, RNs and APRNs can earn advanced certification or credentials in HIV care (e.g., ACRN, AACRN, AAHIVM credentials). However, they do not necessarily reap financial or professional gains if credentialed, as they would in other specialties, Webb indicated. Additionally, the reimbursement to experienced HIV APRNs may be inadequate for the complex care that they provide to their patients.
Webb pointed out that all nursing professionals and other health professionals working in Ryan White-funded clinics depend on the program’s continued reauthorization as well as adequate appropriations for continued employment at their clinics. Health professionals working in Ryan White clinics depend largely on grant funding. This instability of funding sources can lead to a sense of job insecurity, making these settings less attractive than other, better supported, sites of care.
Webb described how FQHCs and Nurse Managed Health Centers40 are increasingly asked to take on the role of providing HIV/AIDS care in lieu of AIDS service organizations. The overall shortage of APRNs and RNs specializing in HIV/AIDS care and the rapid expansion of these Health Centers have created acute shortages of nursing professionals at these facilities. Educational opportunities and financial incentives will be necessary to ensure that there is a sufficient supply of qualified APRNs and RNs to handle the influx of HIV/AIDS cases following more widespread HIV testing and the expansion of CHC program capacity after implementation of the ACA. Webb discussed the importance of special outreach to ensure that RNs and APRNs at these facilities have the training and education needed to provide quality HIV treatment and care. Webb concluded her remarks by observing that an adequate supply of appropriately trained nursing
professionals and other health care providers underpins the success of any expanded framework of care for HIV patients.
Physician Assistants
Jean Davis spoke about the importance of PAs in the provision of HIV/AIDS care. She noted the importance of focusing on health care capacity in HIV/AIDS, not only from a clinical perspective, but also from that of cultural competency and fluency. Cultural competency encompasses not just race and ethnicity, but gender, age, biological sex, and so on.
Davis noted that there are no programs that specifically train PAs for HIV/AIDS care, although PAs can participate in the AAHIVM credentialing program. She emphasized the importance of including training in taking a sexual history from patients. HIV/AIDS as a topic should be discussed when learning about the reproductive health system, dermatology, and infectious disease.
PAs should also be exposed to HIV patients as they do their rotation in internal medicine. However, since most HIV/AIDS patients receive routine care in outpatient settings, there may not be adequate exposure to HIV care in hospital-based rotations. Davis recommends that there be a specific HIV rotation for PA students, where they do a rotation in facilities where HIV/AIDS patients are being seen.
Davis concluded her presentation by noting that fellowships allowing specialization in HIV/AIDS care and loan repayment programs would be incentives for PAs to specialize in HIV/AIDS care. She also noted the importance of ensuring that there are enough providers of all types that are people of color in order to provide care for patients living in communities of color.
Implementation of steps to address a number of these issues, such as improved training in taking sexual histories, increased exposure to HIV medicine in outpatient settings, and perhaps even programs to enable more underrepresented minorities to enter primary care (e.g., loan subsidies and repayment options) may be relatively inexpensive strategies to help meet capacity needs.
Adequacy of Incentives to Attract and Retain Health Care Professionals in HIV/AIDS Care
The committee was asked to address the adequacy of financial or professional incentives to promote HIV/AIDS as a specialty among the health care professions. A number of workshop presenters described the inadequacy of current incentives to promote HIV/AIDS as a specialty and proposed various strategies to encourage medical (and other health care
professional) trainees to pursue careers in HIV/AIDS medicine, engage physicians in the care of HIV/AIDS patients, and ensure the availability of community-based and academic-centered care for HIV/AIDS patients. Given that ethnic and racial minorities represented 70 percent of new AIDS cases in 2006 (HRSA, 2010c), it is important to promote racial and ethnic diversity and cultural competency among HIV care providers. Stigma and discrimination are major barriers to accessing HIV/AIDS care for immigrants and other groups; culturally competent providers can help to facilitate enrollment and retention of such individuals in care (HRSA, 2010a). The following suggestions, many of them presented as recommendations previously made by HIVMA, AAHIVM, and ANAC, were discussed as being key to enlarging the presently overtaxed HIV/AIDS care system.
Physicians
Financial incentives More incentives could be implemented to help alleviate the financial burden on physicians practicing or entering primary care fields in general and HIV/AIDS care in particular, thereby promoting entry into and retention in HIV care. To better meet the needs of an increasingly diverse patient population, some incentive programs might focus specifically on attracting practitioners from underrepresented groups, as well as promoting practice in traditionally underserved areas or populations.
Recruitment Among the incentives that may help to attract more providers, including those from underrepresented groups, into the practice of HIV medicine are loan forgiveness/scholarships to medical residents choosing HIV/AIDS-related specialties; full-funding of the Health Professions Title VII program,41 which supports expansion of the geographic, racial, and ethnic distribution of the workforce; and designation of Ryan White-funded clinics as National Health Service Corps-eligible sites.42
Retention Incentives that might encourage HIV/AIDS providers to continue practicing in the field include the development and application of innovative
payment structures to adequately support the delivery of comprehensive, coordinated HIV/AIDS care, such as
-
application of Medicare reimbursement rates to Medicaid,43
-
increased Medicare and Medicaid reimbursement rates for HIV infectious disease specialists who provide primary care, enhancement of primary care rates for experienced/expert HIV primary care providers under Medicare and Medicaid,
-
risk-adjusted provider reimbursement,44 and
-
reimbursement for alternative models of expert/primary care collaboration and consultation (e.g., distance consultation via telemedicine, phone/e-mail).
Education and training opportunities Reforming medical curricula to increase student and postgraduate experience in HIV/AIDS medicine is important for addressing several of the barriers to physicians entering the field. First, increased exposure to the (outpatient) practice of HIV/AIDS medicine will permit trainees to become more knowledgeable about and familiar and comfortable with the specialty. This, in conjunction with the opportunity to find a mentor in the field, may stimulate greater interest in pursuing a career in HIV medicine. Second, the more familiar students and residents become with the realities of caring for HIV-positive individuals, the more likely that any previous stigma or preconceived notions they associated with HIV practice will be dispelled. Third, engaged faculty mentors may stimulate sufficient interest in the practice of HIV medicine both to draw more graduates into the field and to counteract the tendency toward “reverse brain drain.” Fourth, clinics partnering with hospital-based residency programs not only provide improved educational opportunities for trainees, but also increase the interest level among clinic practitioners, leading to improved retention. Similarly, some of the collaborative delivery system strategies (coordinated care models) stimulate greater interest among practitioners by promoting collegiality and providing opportunities to collaborate with others. Specific considerations include increased reimbursement to FQHCs that provide residency training and maintaining
|
43 |
Medicaid reform under the ACA includes an increase in Medicaid reimbursement rates, to the level that is provided for Medicare. However, the increase may only last 2 years (see http://www.kaiserhealthnews.org/Stories/2010/April/06/Medicaid-Expansion-And-Payment-Increase-Causes-Mixed-Feelings-For-MDs.aspx [accessed March 3, 2011]). |
|
44 |
In risk-adjusted reimbursement, provider payment is based on patient risk and need to properly compensate for estimated work load. It is designed to remove volume from the payment equation and reward providers who achieve desired outcomes in quality, cost, and patient experience with a risk-adjusted bonus (see http://www.medscape.com/viewarticle/730872_6 [accessed March 3, 2011]). |
levels of Ryan White, or other flexible funding source, funding to support models of coordinated care.
Nursing Professionals
Webb discussed a number of recommendations of the ANAC to address the shortage of APRNs and RNs in HIV/AIDS care.
Financial incentives
-
Offer loan repayment and forgiveness programs to RNs and APRNs who work in HIV/AIDS care.
-
Develop and encourage widespread adoption of financial and professional incentives to promote HIV/AIDS as a specialty (e.g., increased compensation upon earning ACRN/AACRN certification or AAHIVM credentials).
-
Ensure adequate Medicaid reimbursement to allow clinics to hire or continue to hire sufficient numbers of APRNs and RNs to provide needed medical and nursing services.
Work environment
-
As HIV testing is expanded and more patients enter into care, ensure that adequate resources for staffing are considered and allocated.
Public policy development
-
Include HIV nurse leaders in national-level stakeholder meetings and policy forums to ensure that a nursing perspective is included, especially as the National HIV/AIDS Strategy is implemented.
Funding of Title VIII programs that support training of APRNs, increase the number of minority and disadvantaged students entering nursing programs, and improve nurse retention may also help to facilitate entry of nursing professionals into HIV care. There has been a reduction in Title VIII funding in recent years (APHA, 2009). Regulatory and other barriers that limit the ability of APRNs to practice to the full extent of their education and training could also be addressed.
Conclusions
Declining interest in primary care among medical trainees is partially responsible for current and anticipated HIV/AIDS workforce shortages. This disinterest can be traced to financial pressures facing trainees (e.g., mounting education debt and considerations of future income) among other factors. Difficult working environments leading to stress and burnout are also evident among all HIV professionals. Primary care physicians often work long, unpredictable hours and are burdened by administrative responsibilities (e.g., communicating with insurance companies, documenting care). Deficiencies in training, specifically the lack of outpatient setting experiences and opportunities to be mentored by HIV/AIDS experts, mean that medical trainees gain little insight into the potential for a satisfying career in HIV/AIDS. The growing interest of those trained in infectious diseases in the alleviation of HIV/AIDS suffering overseas comes at the expense of domestic care.
The lack of exposure of entry- and graduate-level nursing students to HIV/AIDS related curricula and clinical experiences has contributed to the shortage of RNs and APRNs in HIV/AIDS care. The reliance on grants and unstable sources of financial support on the part of many of the community-based clinics that serve HIV-infected individuals also deters nurses from entering the field of HIV/AIDS care. In addition, state licensing regulations that restrict the scope-of-practice for APRNs and payor reimbursement policies may deter some APRNs from entering the field. Some APRNs and RNs do receive HIV/AIDS specialty certification or credentials; however, there are no financial rewards associated with developing HIV/AIDS expertise.
There also are shortages of physician assistants entering HIV/AIDS care. As in other health professions, this may stem in part from a lack of specific focus on HIV/AIDS care during their initial professional training, as well as the absence of financial incentives to enter the field.
In summary, there are inadequate financial and professional incentives to promote HIV/AIDS as a specialty among the health care professions. Options to consider to encourage HIV/AIDS specialization among physicians, APRNs, RNs, and PAs include loan repayment/forgiveness and scholarships for trainees, the use of reimbursement mechanisms to compensate HIV/AIDS specialists fairly, and the provision of adequate and stable financial support to clinics serving HIV/AIDS patients. Financial incentives (e.g., loan forgiveness) may also be used to attract practitioners of diverse races and ethnicities, as well as to encourage providers to practice in and among traditionally underserved areas and populations.
Steps to reform medical, nursing, and other health professional curricula to increase opportunities to learn about outpatient care for HIV/AIDS
patients are important to promote interest in the field among trainees and to encourage collaboration, collegiality, and retention among more experienced providers. Another strategy to improve retention is to promote interactions between HIV specialists and primary care generalists, particularly in the community health care setting. CHCs serve as the medical home for many HIV/AIDS patients, and also play a critical role in care coordination for those patients. Collaboration among colleagues may alleviate some of the burdens of the workplace, as well as the sense of isolation that some practitioners may experience, especially in rural or other underserved areas. The development of patient-centered models of care and the use of interdisciplinary care teams in the provision of HIV/AIDS care not only may improve patient care, but also may improve job satisfaction among the providers.
IMPACT OF THE AFFORDABLE CARE ACT ON THE PUBLIC HEALTH AND CLINICAL INFRASTRUCTURE
Jeffrey Levi, Executive Director, Trust for America’s Health, provided the committee with an overview of the issues related to the testing and treatment of HIV-infected individuals and the potential impact of the ACA. Levi cited literature supporting the need for insurance reform for HIV-infected individuals. According to a recent CDC study of 21 U.S. cities, 57 percent of HIV-infected men who have sex with men are uninsured. Furthermore, 81 percent of those who were unaware of their HIV infection had not visited a health care provider in the past year (CDC, 2010d).45 This study provides further evidence that expanding insurance coverage and improving provider capacity could greatly increase opportunities to bring many at-risk individuals into care.
Levi outlined some of the shortcomings of the health insurance system that have limited access to care for HIV-infected individuals. First, Medicaid traditionally has been restricted to those who are very poor and who also meet certain criteria, for example, those who are disabled, pregnant, or children. Second, Medicare eligibility for people under age 65 has been restricted to those who have long-term disabilities (i.e., 29 months, with two waiting periods) and there have been limits to prescription drug coverage (i.e., the “donut hole”) whereby, after a certain amount of charges for prescription drugs has been incurred, beneficiaries are temporarily responsible for paying 100 percent of their prescription drug costs (RWJF, 2010). Third, private insurers often deem HIV-infected individuals uninsurable or
require high premiums and/or lifetime limits on coverage for those they have insured.
Levi reviewed provisions of the ACA that will improve health insurance coverage for individuals with, or at risk for, HIV/AIDS. By 2014, the ACA will greatly expand Medicaid to cover individuals with incomes up to 133 percent of the federal poverty level (FPL). In addition, income level will be the sole eligibility criterion with no need to meet additional categorical requirements (e.g., disability). Until 2014, states may elect the option to extend Medicaid to individuals with incomes up to 133 percent of the FPL. In addition, for Medicare beneficiaries there will be a gradual closing of the prescription drug coverage gap beginning in 2011 (RWJF, 2010). In the private insurance market, there will be guaranteed issue46 of health insurance by 2014 (and a mandate to have health insurance coverage). Private insurers will have to limit their underwriting to age, geography, and smoking history (e.g., no HIV history restrictions). Subsidies will be available for those with incomes between 133 and 400 percent of the FPL and who are unable to afford private health insurance (covering both premiums and cost sharing). By 2014, routine costs associated with participation in clinical trials also will be covered by private plans.
Coverage of preventive services under the ACA will expand as well but will vary by insurance provider:
-
New plans offered by private insurers will be required to cover, without cost sharing, preventive services rated A or B by the USPSTF, immunizations recommended by the Advisory Committee on Immunization Practices (ACIP), and certain preventive care services recommended by HRSA for infants, children, adolescents, and women.
-
Under Medicaid, the federal government will offer a 1 percent increase in the federal match to states that offer Medicaid coverage of, and remove cost sharing for, A and B USPSTF recommended services and ACIP recommended immunizations (effective January 1, 2013).
-
Medicare will eliminate cost sharing for Medicare-covered preventive services that are USPSTF recommended A or B services.
As mentioned earlier, routine HIV screening (i.e., testing of those not at increased risk) is rated C by the USPSTF and therefore is not included in the aforementioned extensions of coverage (IOM, 2010).
Boswell described how reimbursement for HIV care provided in health
centers will be affected by the ACA. The ACA requires insurance exchanges to include all 340B eligible providers,47 such as FQHCs and state ADAP programs, in their networks. Also under the ACA, insurance exchanges will pay FQHCs no less than the rate provided under their Medicaid prospective payment system (PPS) (a method of reimbursement where payment is based on a predetermined, fixed amount). Payment to FQHCs for patients covered by Medicare will be based on a modified PPS that includes all preventive benefits and elimination of current caps and screens. A phased transition of financing HIV/AIDS care is needed as future methods of reimbursement under the ACA are untested and will require years to develop (e.g., accountable care organizations [ACOs], Alternative Quality Contract).
Although many ACA provisions will not be phased in until 2014, some are effective immediately:
-
Individuals denied insurance coverage due to a pre-existing condition have immediate access to federally subsidized high-risk pools.
-
Private insurers cannot rescind an insurance policy, for example, canceling insurance after a claim is made.
-
Pre-existing condition exclusions for children have been eliminated.
-
Lifetime caps on coverage have been eliminated and annual caps have been subject to regulation.
-
Coverage of children under a family plan has been extended to age 26.
Levi described some of the efforts to expand health care capacity under the ACA:
-
To expand the safety net, $11 billion has been allocated over the next 5 years to CHCs.
-
In FY 2010, $30 million was made available to the CDC, of which $21.6 million is to be used for HIV testing.
-
As of 2013, temporary improved reimbursement rates will be offered to Medicaid providers (these Medicare reimbursement rates will expire after 2014).
-
Community Transformation Grants will begin to be available in 2011 to facilitate policy, structural, and environmental change favoring prevention.
-
A program to support community health workers will be supported as of 2011.
In conjunction with previous investments made through the American Recovery and Reinvestment Act, provisions of the ACA are designed to support the training, development, and placement of more than 16,000 new primary care providers over the next 5 years. Among other efforts, an allocation of $250 million from the Prevention and Public Health Fund48 in 2010 is providing new resources for the training of 500 new primary care physicians by 2015, more than 600 new PAs, and 600 additional NPs. The allocation also helps to establish new NP-lead clinics in medically underserved areas and provide support for states to develop and implement strategies for expanding their primary care workforces over the next 10 years.49 Although not specifically addressing the need for more HIV/AIDS providers, these steps should help to increase the primary care workforce in general.
The ACA has several provisions to support quality improvement efforts. HIV issues are included on the agenda for comparative effectiveness research. Major investments in health information technology also will improve capacity for HIV surveillance and for measuring the quality of HIV care.
Levi pointed out that although expansions in coverage and focus on prevention are welcome, they do not necessarily guarantee adequate access to preventive services and care. Many challenges to the implementation of the ACA remain. For example, yet to be determined is the “essential health benefits package” that insurers will be required to cover. States will be determining the full range of benefits for the expanded Medicaid population so there likely will be significant variation across the country. States can choose between the relatively comprehensive standard Medicaid package and a “benchmark” program that would be more like a private plan. In addition, the makeup of health care provider networks is not well defined. Whether Ryan White providers or “expert” HIV providers will be included in networks is to be determined. Finally, how reimbursement for HIV testing will be administered is unclear. For example, alternative testing
|
48 |
Established as part of the ACA, the Prevention and Public Health Fund is a 10-year $15 billion commitment designed to help create the necessary infrastructure to prevent disease, detect it early, and manage conditions before they become severe. Among other things, this new initiative will increase the national investment in prevention and public health by, for example, supporting preventive health services such as smoking cessation, exercise programs, and other efforts to reduce the burden of chronic diseases. |
|
49 |
See http://www.healthcare.gov/news/factsheets/primarycareworkforce.html (accessed March 15, 2011). |
sites that currently receive grant support for HIV tests may be required to submit insurance claims for individuals with insurance coverage.
The fate of the Ryan White program after implementation of the ACA is also uncertain. Ryan White was initially meant to be a temporary measure until more fundamental changes in health care insurance and provision could be developed. Over time the Ryan White program has evolved to accommodate new and emerging needs. Originally designed in part to provide emergency assistance to areas disproportionately affected by the HIV epidemic, it now serves to fill gaps in medical care and to provide support services that are not covered by other funding sources. Many workshop participants raised concerns over the many services that are needed by persons living with HIV that are not generally covered by health insurance. These wraparound services, such as case management and substance abuse and mental health services, may be vulnerable under the ACA. Prescription drug coverage under ADAP is an essential Ryan White program whose future is uncertain now that the ACA has been passed. The Ryan White program also has been able to provide services to individuals who are excluded from health care coverage under the ACA.
In his remarks, Boswell suggested that to better understand how best to allocate scarce personnel and resources, studies are needed to document models and best practices for HIV care. The CMS Innovation Center, for example, could evaluate the impact of the Ryan White model for patient-centered, medical-home care on patient outcomes and costs of care.
Levi concluded his remarks by pointing out that until 2014, there are opportunities to gain coverage of vulnerable populations through high-risk insurance pools and to make investments in preventive services. By 2014, there are opportunities to redesign health care programs to meet the needs of those who are in need of HIV/AIDS services.
Committee member Ron Bayer asked Levi to describe how the Ryan White program might be reshaped after implementation of the ACA. He pointed out that the Ryan White program covers some essential services that health insurance was never designed to address (e.g., outreach and patient navigation). The demand for some services, now covered by Ryan White, will decline as uninsured individuals gain coverage. Levi and Cheever raised the concern that the reauthorization of the Ryan White program will take place in 2013 before full implementation of the ACA. There are risks associated with changing the program before the implications of the ACA are known.
Arleen Leibowitz from the committee asked Levi about reimbursement mechanisms that might be used by ACOs and whether risk adjustment has been considered to take into account the complex care requirements of HIV/AIDS patients and others with chronic conditions. Levi replied that
these types of adjustments are needed, but that decisions about such reimbursement mechanisms have not yet been made.
Committee member Eric Bing asked Levi about options that undocumented individuals will have in terms of gaining insurance. Levi replied that undocumented individuals with HIV may have access to care through CHCs, which do not have the same restrictions as other programs with respect to the individuals to whom they may provide services. Access to care for undocumented individuals would depend on the adequacy of support going to CHCs.
Committee member Scott Burris asked about marginalized populations’ access to care following implementation of the ACA, for example, individuals who are in and out of prison and/or who use intravenous drugs. Levi mentioned that many such individuals would be eligible for Medicaid and that ease of enrollment will be important to ensure access to care. Another issue for this population is whether culturally competent providers will be available in provider networks and whether a usual provider of care, for example, a community-based clinic dependent on discretionary support, will remain as a viable provider following implementation of the ACA.
Committee member Martin Shapiro asked whether certain portions of the ACA are more vulnerable to legislative change than others and whether, in the wake of the ACA, the Ryan White Care Act may be vulnerable. Levi replied that support for the Ryan White program has, in general, been constant and bipartisan. In terms of the ACA, Levi pointed out that retaining popular aspects of reform (e.g., elimination of underwriting) while repealing other less popular provisions would have significant fiscal ramifications that would be identified by the Congressional Budget Office. Consequently, in his opinion, changing the ACA may prove difficult.
Committee member Susan Cu-Uvin called attention to the centrality of CHCs in the ACA and asked Levi to anticipate how HIV/AIDS patients would be served following the implementation of the ACA. Would patients, for example, receive primary care from a CHC and then get referred to a Ryan White program for HIV/AIDS specialty care? She observed that many HIV/AIDS patients receive all of their care, primary and specialty care, within Ryan White programs. Saag added that the shifting focus to CHCs for HIV care is a potential threat to Academic Health Centers that want to remain engaged in HIV care. Levi indicated that the main factor that will determine the site of patient care is the makeup of provider networks. It is unclear in the early days of the ACA how the networks will be defined and whether Ryan White providers will routinely be included in them. Levi speculated that there will be a redistribution of money in the system that will potentially also affect the distribution of patients across care sites.
Levi suggested that HRSA may need to resolve some issues around
its “payor of last resort” provisions. Ryan White providers are obligated to obtain reimbursement for services rendered from all available insurers before using Ryan White dollars. With an expanded population of individuals with third party insurance, Ryan White programs will be in a position to seek third party reimbursement more often. If health care services are being supported through insurance payments, Ryan White funds might be redirected to other services.
When asked by committee chairman Paul Cleary to outline his main conclusions, Levi indicated that there are three main areas to consider as the ACA is implemented:
-
How health care benefits are defined by insurers and which clinicians (including, e.g., APRNs and PAs) should be included in provider networks are the main “threshold” issues for HIV/AIDS care providers and patients under the ACA.
-
Ensure that HIV/AIDS is a fundamental part of new prevention initiatives such as the Community Transition Grants and the community health workers program.
-
Maintain discretionary program funding streams that provide wraparound services needed by HIV/AIDS patients at least until full implementation of the ACA and evaluations are completed to assess the adequacy of HIV/AIDS services under new delivery and reimbursement structures.
Conclusions
Full implementation of the ACA would address shortcomings of the current health insurance system. It would ease restrictions and expand access to Medicare (prescription drug coverage) and Medicaid and private insurance programs. To bolster the nation’s health care safety net, the ACA increases support to CHCs, temporarily improves reimbursement to Medicaid providers, and makes investments in public health programs. The fate of the Ryan White program under the ACA is uncertain. The program is to be reauthorized in 2013, before full implementation of the ACA in 2014. Because certain essential HIV/AIDS services and providers are only available through the Ryan White program, workshop participants felt strongly that key components of the program are vital. With increased support of CHCs, there are some concerns that academic-based HIV/AIDS programs which have served as centers of excellence of HIV/AIDS care may be in jeopardy. It is unclear how sites of HIV/AIDS care might shift following implementation of the ACA. The need to maintain centers of excellence of HIV/AIDS care provides another rationale for maintaining key elements
of the Ryan White program as these have been essential to the support of academic programs.
SUMMARY
In the wake of the 2006 CDC recommendations to implement routine HIV testing in health care settings for individuals 13 to 64 years of age, state health departments and other organizations are receiving financial support for the development and implementation of HIV screening. However, it is not clear whether the support has been sufficient, and the long-term sustainability of the programs is in question, especially once outside funding ceases. It is clear that sustainable programs need to fit as seamlessly as possible into the care flow of the venues in which they are instituted, which will necessitate the use of different testing procedures in different venues. A willingness and flexibility to develop and implement procedures that best match the needs of the setting are important to the success of expanded HIV testing efforts. A big challenge to the implementation of routine HIV testing, especially in busy, high-volume settings where patient follow-up is more challenging, is the question of who will inform and address the needs of individuals who are found to be HIV-positive. Providers in these and other HIV testing venues may have neither the comfort level nor perceive themselves to have the expertise to respond to these patients. In addition to training for providers on the provision of HIV counseling and education, the availability of resources (e.g., computer/Internet tools) to help providers link patients with care and treatment, as well as psychosocial support, could help in this regard.50
In assessing the current capacity of the health care system to incorporate an increased number of HIV-positive individuals into care, the committee encountered a paucity of data on patterns of care for HIV/AIDS patients. The most comprehensive, nationally representative study of sites of HIV/AIDS care is the now dated HIV Cost and Services Utilization Study. Although more recent data are available from Ryan White providers, that sample is limited to those receiving Ryan White funding. Similarly, there is a lack of data on the HIV-related training of providers.
Nevertheless, it is clear that primary care physicians, infectious disease specialists, APRNs, and PAs provide the vast majority of medical care for HIV-positive individuals. Registered nurses, dentists, pharmacists, and social workers are among the providers necessary to provide quality HIV/AIDS care in a variety of settings. In terms of training, one of the challenges
|
50 |
One example is the CDC National Prevention Information Network, which contains a list of HIV/AIDS counseling, testing, and referral resources (see http://www.cdcnpin.org/scripts/hiv/ctr.asp [accessed March 3, 2011]). |
is the emergence of HIV as a chronic medical condition, increasing the complexity of treating HIV-positive individuals. Infectious disease specialists and primary care providers who are HIV experts due to substantial patient care experiences, formal training, or both, are generally better-prepared to manage HIV disease than are primary care generalists, who lack such experience or expertise. However, most HIV-positive patients can benefit greatly from the broader skills of primary care providers in addressing their other health care needs.
Another clear message is the lack of adequate provider training and experience in HIV care, especially in outpatient clinics, where most routine HIV care now occurs. Increased exposure of trainees to outpatient HIV care throughout school and post-graduate (residency) training, as well as new and ongoing provider training through continuing education programs, is crucial to developing and maintaining a sufficient supply of appropriately trained providers to accommodate increased numbers of HIV-positive individuals.
Moreover, there are more clinicians retiring from or leaving HIV care than there are new clinicians entering the field. At the same time, the number of HIV-positive patients in care is growing, due to increased longevity as well as increased numbers of newly diagnosed individuals. Efforts to bring into care individuals with HIV who currently do not receive regular care will further increase that number. For example, the changes to Medicaid eligibility criteria under the ACA are likely to increase the number of individuals with HIV accessing care. It is important to have not only adequate numbers of HIV care providers, but also adequate racial/ethnic diversity and cultural competency among providers given the large percentage of HIV patients from racial/ethnic minority populations (HRSA, 2010a).
A number of strategies could help to maximize the capacity of the health care workforce to accommodate the increased demand for HIV care. Delivery system strategies, such as task shifting, comanagement, and care coordination models, including integrated delivery systems, are designed to maximize the capacity of the current workforce to provide quality care to HIV-positive individuals. “Pathway” strategies are designed to increase the supply of HIV-trained care providers through, for example, greater exposure of trainees to HIV care and financial and other incentives to encourage more providers to enter HIV care.
The current and projected capacity of the health care workforce to implement routine testing for HIV throughout the nation and to provide competent HIV/AIDS care to significantly increased numbers of patients is of grave concern. Clearly, a variety of approaches will be needed to meet the needs for diagnosis and treatment of HIV-positive individuals in the United States. In addition, barriers to the ability of providers such as APRNs to practice to the full extent of their education and training will need to be
addressed. The current Ryan White model of care, which provides a wide range of medical and nonmedical services, allows for task shifting across provider levels to the extent permitted by state regulations, and supports the provision of comprehensive services, offers an example of the type of integrated delivery system that serves HIV/AIDS clients well and upon which future care systems could be modeled.
Regardless of the approach taken, the committee was impressed by the urgency of addressing these HIV/AIDS care capacity issues. With each additional HIV infection detected, the care system inherits a responsibility to counsel, refer, treat, and monitor an additional patient, at an average per-infection cost of $19,912 per year (Gebo et al., 2010). Interruptions in care, such as have occurred with the freeze on some ADAP programs, and the provision of inadequate care due to long waiting periods and provider shortages are costly not only in human suffering and lost productivity, but also in increased transmission, with each new infection adding a very costly liability for the future ($355,000 for HIV treatment alone [CDC, 2010a]).
































































