2
Causes of Death, Health Indicators, and Divergence in Life Expectancy
As discussed in Chapter 1, increases in life expectancy slowed abruptly around 1980 in the United States, Denmark, and the Netherlands. The phenomenon was most noticeable for women in each of these three countries but was also seen to a lesser degree among U.S. men. To better understand these trends, it is useful to examine differences among countries in causes of death, disease prevalence, and biological risk factors.
Because relatively few autopsies are performed and multiple comorbidities are common at older ages, cause-of-death statistics can be somewhat unreliable at older ages. Even though the International Classification of Diseases (ICD) was designed to make it possible to code causes of death uniformly throughout the world, comparative analysis of cause-of-death statistics is complicated by variations in coding practice across countries and changes in the classification scheme over time. Both of these problems can create artificial trends and differentials (see Glei et al., 2010, for a fuller discussion of some of the methodological problems that need to be confronted when using cause-of-death statistics). In any event, information on cause of death is unlikely to tell the whole story. To see whether differences in life expectancy are mirrored in other dimensions of health, it is also useful to examine such factors as disease prevalence; degree of functional disability; and prevalence of risk factors, including high blood pressure, cholesterol, and weight.
THE ROLE OF VARIOUS CAUSES OF DEATH IN DIVERGING LIFE EXPECTANCY TRENDS
Perhaps the most direct approach to understanding diverging trends in life expectancy is to look for differences in trends in the causes of death for
different countries. Meslé and Vallin (2006) compared patterns of cause of death for women in the United States, the Netherlands, France, and Japan to better understand the recent divergent trends in female old-age mortality in those countries. To identify the main causes of death responsible for the differences in female life expectancy at older ages, the authors compared the period 1968-1984 against the period 1984–2000 and decomposed the change in life expectancy at age 65 into age- and cause-specific mortality changes. They found that most of the divergence derived from the fact that the declines in mortality due to heart disease and cerebrovascular disease in the United States and the Netherlands were partially offset by increases in several other causes of death in those countries, while Japan and France managed to achieve lower mortality from a variety of causes at increasingly older ages (Meslé and Vallin, 2006).
In a specially commissioned background paper for this report, Glei, Meslé, and Vallin updated and extended this line of work (see Glei et al., 2010). Instead of considering trends in 4 countries, the authors extended their analysis to 10 countries, paying particular attention to the 3 countries identified earlier as underachieving over this period (the United States, Denmark, and the Netherlands) and to the highest achiever, Japan. The authors also extended their analysis to include both men and women and updated their investigation of age- and cause-specific mortality contributions to changes in life expectancy using data up to 2004.
Trends in Causes of Death for the United States, Denmark, the Netherlands, and Japan
Figures 2-1 and 2-2 display trends in age-standardized mortality among men and women aged 50 and above for the United States, Denmark, the Netherlands, and Japan (Glei et al., 2010). To circumvent coding problems, the authors grouped the causes of death into nine clusters.
In the United States, heart disease is the number one cause of death, responsible for more than 600,000 deaths annually (Xu et al., 2010).1 While the age-standardized mortality rate for both men and women aged 50 and above has declined significantly since 1980 (see Figures 2-1 and 2-2), heart disease remains the number one killer and the major cause of the current
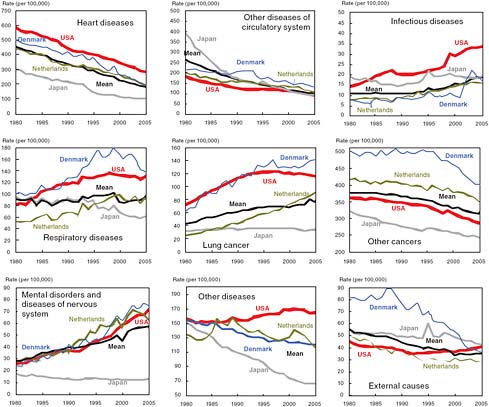
FIGURE 2-1 Age-standardized mortality rates among women aged 50 and older by cause group, United States compared with the Netherlands, Denmark, Japan, and the 10-country average, 1980–2005.
NOTE: Deaths from ill-defined causes have been redistributed proportionately to all other categories.
SOURCE: Glei et al. (2010, Figure 2-6). Reprinted with permission.
gap in female life expectancy at age 50 between the United States and the countries with the highest life expectancies, accounting for 44 percent of the gap with Japan and 50 percent of the gap with France. At the same time, Figures 2-1 and 2-2 demonstrate that the difference in the age-standardized mortality rate due to heart disease has not changed significantly among these four countries over the past 25 years. Consequently, even though the United States has the highest level of mortality due to heart disease of any of the four countries shown, heart disease does not explain the divergent trends in life expectancy. All four countries appear to have experienced similar success in combating heart disease (Glei et al., 2010).
Success in lowering mortality from other diseases of the circulatory system, predominantly cerebrovascular disease, has contributed to life ex-
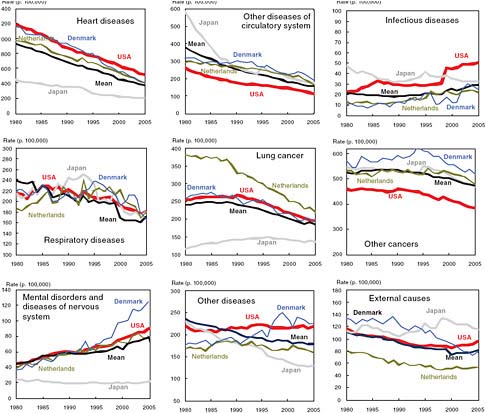
FIGURE 2-2 Age-standardized mortality rates among men aged 50 and older by cause group, United States compared with the Netherlands, Denmark, Japan, and the 10-country average, 1980–2005.
NOTE: Deaths from ill-defined causes have been redistributed proportionately to all other categories.
SOURCE: Glei et al. (2010, Figure 2-7). Reprinted with permission.
pectancy gains in the United States over the past 25 years. But Japan (and other countries such as France, Italy, and Australia) have achieved far greater success, so that differences in mortality related to cerebrovascular disease and other diseases of the circulatory system are an important source of divergence in the trajectories of life expectancy among countries (Glei et al., 2010).
Since 1964, when the first U.S. Surgeon General’s report documenting the harmful effects of smoking was published, smoking has been identified as the single greatest cause of preventable morbidity and mortality in the United States. Besides lung cancer, smoking increases the risk of a large number of other cancers, chronic pulmonary obstructive disease (COPD), heart disease, and stroke (Centers for Disease Control and Prevention, 2004).
To examine the extent to which differences in progress in life expectancy can be attributed to smoking-related causes of death, Glei and colleagues (2010) looked at trends in two groups of causes of death strongly associated with smoking: lung cancer and respiratory diseases. For women, they found important differences in both levels and trends in lung cancer among Japan, Denmark, the Netherlands, and the United States. Japan has much lower rates of lung cancer than the three laggards, particularly the United States and Denmark. Age-standardized mortality rates for lung cancer for women over age 50 have risen in the past 25 years in the United States, the Netherlands, and Denmark but have remained flat in Japan. Similarly, women in the United States, Denmark, and to a lesser extent the Netherlands have higher rates of respiratory disease than women in Japan, and these rates have diverged significantly since 1980. The story is slightly different for men (Figure 2-2). The mortality rate for lung cancer among men is lower in Japan than in the other three countries, but these rates appear to be converging rather than diverging over time. In addition, there are virtually no differences in mortality due to respiratory disease among older men in these four countries.
Cause-of-Death Contributions to Country-Level Changes in Life Expectancy at Age 50
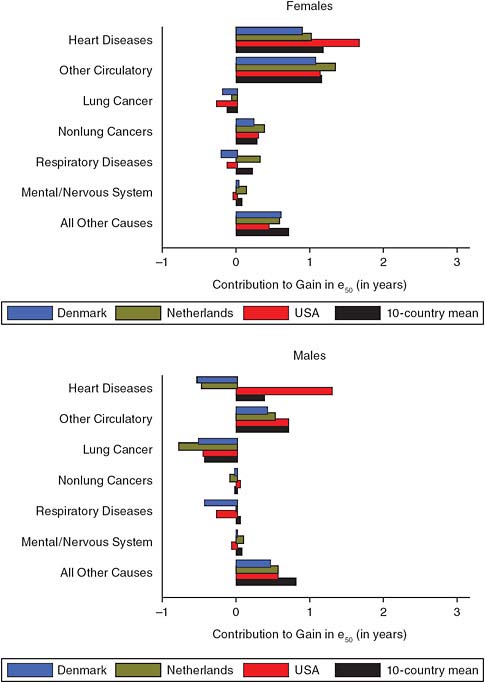
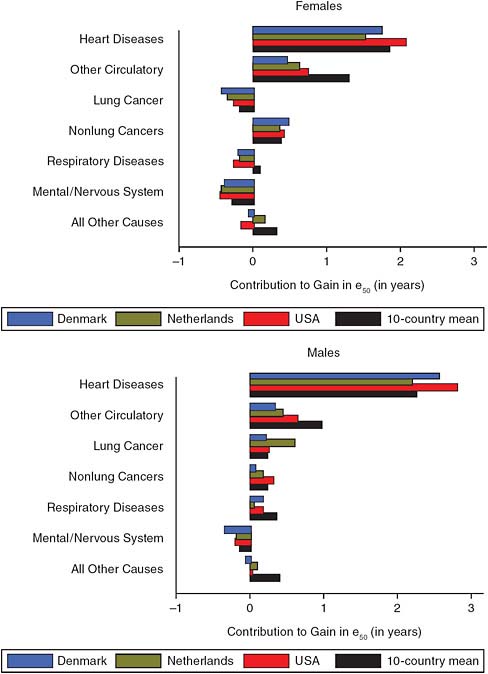
Glei and colleagues (2010) used a decomposition technique to separate out the contribution of various causes of death to gains in life expectancy at age 50. Figure 2-3 displays the contributions of the various causes of death to increases in life expectancy at age 50 during 1955–1980 for women (top panel) and men (bottom panel) in the United States, Denmark, and the Netherlands, as well as the mean of the 10 countries the authors analyzed. Figure 2-4 provides the same information for the period 1980–2004. These calculations confirm that the slowdown in life expectancy at age 50 among women in the United States, Denmark, and the Netherlands was not due to heart disease; as noted above, reductions in the rate of mortality from heart disease played an important role in increasing life expectancy in all countries after 1980. On the other hand, other circulatory diseases (which include stroke) did contribute to divergence, as the decreases in mortality from this group of diseases were much smaller for the United States, Denmark, and the Netherlands than they were in other countries for both men and women.
The other important contributors to the slowdown in gains in life expectancy at age 50 among women in the United States, Denmark, and the Netherlands were lung cancer, respiratory diseases, mental and nervous system diseases,2 and “other diseases.” Rising numbers of lung cancer
deaths reduced female life expectancy in the United States, Denmark, and the Netherlands during 1955–1980 and even more so during 1980–2004. It is worth noting that, although lung cancer had a negative effect on gains in life expectancy at age 50 for women in the underperforming countries, the same was not true for other types of cancer. Progress against nonlung cancers in the United States, Denmark, and the Netherlands was comparable to that in other countries during both periods. By contrast, although mortality due to lung cancer had a negative effect on gains in life expectancy at age 50 among men during 1955–1980, its effect was positive for men in the United States and most other countries during 1980–2004.
The importance of smoking as an explanation for the observed divergence in trends in life expectancy is also suggested by the fact that respiratory diseases appear to have played a role in the divergence during 1980–2004. Mortality from respiratory diseases most commonly implies death from COPD, the leading cause of which is smoking. Since 1980, mortality from respiratory diseases has fallen for men in all countries shown in Figure 2-4 but has risen for women in the United States, Denmark, and the Netherlands.
Mental and nervous system diseases had a negative effect on gains in life expectancy at age 50 for nearly all 10 countries and for both men and women for the period 1980–2004, but this effect was largest among women in the United States, the Netherlands, Denmark, Canada, and Spain. It is difficult to say what these trends might mean, however. Some of the numerically important diseases in this category are Alzheimer’s, Parkinson’s, and Huntington’s diseases. There are questions about how systematically this category of diseases is coded in different countries and over time. For instance, as Alzheimer’s disease became a recognized and diagnosed disease, the propensity to code it as a cause of death may have varied across countries. It is impossible to distinguish this possibility from real differences in mortality due to these diseases across countries. Finally, while the category of “other diseases” contributed to increases in life expectancy at age 50 in most countries and for both men and women, it had a negative effect on life expectancy among women in the United States and Denmark. The most important single disease in this category is diabetes.
Discussion
One of the most striking features of the divergence in life expectancy trends since 1980 is that it has been seen mainly in women. Cause-of-death data point to the particular areas in which progress has slowed for women. The most notable gender differences in the United States, Denmark, and the Netherlands are in the contributions to changes in life expectancy at age 50 made by lung cancer and respiratory diseases. Both diseases had a positive effect on the change in life expectancy at age 50 among men but
a negative effect among women; that is, mortality from these causes was decreasing among men while it was increasing among women. Moreover, women from the United States, Denmark, and the Netherlands exhibited larger increases in mortality related to lung cancer and respiratory diseases during the period 1980–2004 compared with 1955–1980 and compared with women from the remaining countries during 1980–2004 (Glei et al., 2010). In short, the increase in mortality from these diseases during this period and in these countries was an anomaly regardless of what it is measured against: mortality in the earlier period, male mortality, or female mortality in other countries.
Although this analysis does not identify the factors underlying the differences in the cause-of-death trends, it does point clearly in a particular direction: “Based on the evidence presented here, the most obvious explanation for the slowing of mortality decline among women in the United States, Denmark, and the Netherlands is smoking, which is strongly correlated with lung cancer and respiratory diseases such as chronic obstructive pulmonary disease” (Glei et al., 2010, p. 44). The existence of gender differences in the contributions of lung cancer and respiratory diseases to life expectancy would appear to point to gender differences in smoking behavior within the United States, Denmark, and the Netherlands, and such differences have indeed been observed: increases in smoking occurred later among women, while declines in smoking took place earlier among men (Forey et al., 2009).
While the evidence presented in the Glei et al. analysis is consistent with the hypothesis that smoking was an important factor in the slowing of mortality decline among women in these three countries, smoking is unlikely to be the entire story. The data suggest that mental and nervous system diseases, including Alzheimer’s disease, may also play a role. Of interest, in the Netherlands, where women again began seeing a steady increase in life expectancy at age 50 after 2002, the gains in mortality resulted from improvement in the mortality risk for mental disorders as well as other causes of death, such as diabetes (Glei et al., 2010).
The cause-of-death data reviewed here provide some important insights into the reasons for diverging levels and trends in life expectancy. For a more complete picture, however, it is necessary to examine how these countries differ in a variety of health indicators.
THE ROLE OF DIFFERENCES IN HEALTH INDICATORS IN DIVERGING LIFE EXPECTANCY TRENDS
The panel considered the questions of whether increasing life expectancy has been a result of improvements in health and whether the countries with the greatest increases in life expectancy also have seen greater improvements in health. Such questions cannot be answered fully, as the
data are both incomplete and not totally comparable from country to country. Nonetheless, enough data exist to address the issue of whether countries lagging behind in life expectancy currently have worse health than countries experiencing more rapid improvement.
Health Versus Life Expectancy
It makes sense intuitively that better health should be directly correlated with greater life expectancy—that a “healthier” population should be one in which people live longer—but this relationship is not always simple. In the past, when infectious diseases played a major role in mortality, healthier groups of people were likely to have lower death rates (Crimmins et al., 2010). Today, however, death is more likely to be caused by long-term chronic conditions that have been treated but not cured. Modern medicine enables people to live for many years with conditions that have been ameliorated and controlled, so modern populations include large numbers of people living with various diseases and disorders, some of them for decades. This means that a longer-lived group may not necessarily be “healthier” than a group with a shorter life expectancy; the group may instead consist of many ill people whom modern medicine has kept alive but not cured.
One important type of data denotes the percentage of people in a country who are experiencing a particular health problem at a particular point in time, termed the prevalence of the problem (Crimmins et al., 2010). A population can be “healthier” in terms of the prevalence of a particular disease in two ways: (1) the incidence of the disease can be lower—that is, fewer people develop it to begin with—or (2) the people who develop the disease do not survive as long. Conversely, prevalence will be higher if either the incidence of the disease is higher—more people develop it—or people live longer after developing it. A further difficulty in international comparisons arises from varying levels of screening and identification of some health problems and some risk factors. A country, such as the United States, with aggressive screening will appear to have both greater incidence and greater prevalence of health problems than a country with poorer screening, all other things being equal. So the existence of national differences in health problems—incidence or prevalence—is not free of some difficulty in interpretation.
Several different dimensions of health—risk factors, diseases, disability—may be related to life expectancy in varying ways (Crimmins et al., 2010). A number of conditions, such as arthritis, cause disability but are not major causes of mortality. Conversely, diseases such as cancer affect mortality but are not a major cause of disability. And some diseases, such as heart disease, lead to both disability and mortality. In the remainder of this section, data from a variety of self-reports in nationally representative surveys and medical records are presented for the 10 countries that are the focus of this
study. The data, taken mainly from Crimmins et al. (2010), include various indicators of functioning and disability, estimates of disease prevalence, and estimates of the prevalence of three major risk factors—high body mass index, cholesterol levels, and levels of hypertension.
Differences in Disease Prevalence
Heart Disease, Stroke, and Diabetes
Cardiovascular disease accounts for about half of the female gap in life expectancy at age 50 between the United States and the nine other countries studied here and for most of the male gap. Self-reports of having been diagnosed with heart disease among those aged 65 and over are more numerous in the United States than in the other countries: only England has a rate close to that of the United States, while people in Japan and Denmark report heart disease at a rate less than half that in the United States (see Table 2-1). The highest prevalence of self-reported stroke is found among Danish men, with men from the United States, Japan, and England fairly close behind. By contrast, the highest rates among women are reported in the United States, followed by women from the Netherlands and Denmark. Glei and colleagues (2010) report a convergence in death rates from cerebrovascular disease between the United States and other countries; this is the category that includes stroke deaths. This convergence has occurred because other countries have improved more than the United States, which used to have relatively favorable stroke death rates.
TABLE 2-1 Percentage of Population Self-Reporting Diseases by Gender and Country: Ages 65+
|
Country |
Men |
Women |
||||
|
Heart Disease |
Stroke |
Diabetes |
Heart Disease |
Stroke |
Diabetes |
|
|
United States |
36.4 |
9.4 |
21.4 |
28.0 |
8.6 |
17.6 |
|
Denmark |
15.9 |
9.9 |
11.1 |
13.0 |
7.3 |
8.7 |
|
France |
28.8 |
5.5 |
13.0 |
16.3 |
5.8 |
10.8 |
|
Italy |
18.7 |
5.8 |
17.6 |
14.3 |
4.0 |
15.7 |
|
Netherlands |
21.7 |
7.1 |
10.6 |
12.9 |
7.8 |
12.2 |
|
Spain |
15.1 |
2.9 |
20.4 |
15.5 |
2.8 |
17.1 |
|
England |
32.2 |
8.2 |
11.2 |
26.4 |
6.4 |
8.0 |
|
Japan |
14.4 |
9.3 |
10.1 |
12.2 |
6.0 |
7.5 |
|
Canada |
21.8 |
5.2 |
15.6 |
18.1 |
3.9 |
11.9 |
|
Australia |
|
|
16.2 |
|
|
11.5 |
|
SOURCE: Adapted from Crimmins et al. (2010, Table 3-2). Reprinted with permission. |
||||||
Glei and colleagues found that deaths from diabetes contributed about 0.1 year to the difference in life expectancy at age 50 between the United States and the other nine countries (Glei et al., 2010). When Crimmins and colleagues (2010) examined the self-reported prevalence of diabetes in the different countries, they found it to be highest in the United States, with Spain and Italy close behind. The prevalences in Denmark, England, and Japan were only about half those in the United States (see Table 2-1).
When all three of the diseases—heart disease, stroke, and diabetes—are considered, a pattern emerges: Americans report a high prevalence of each of these diseases relative to the other nine countries. It is not always the highest prevalence, but it is generally in the top two or three. Other countries may rank high on one disease, but it is usually just one. The high prevalence of these diseases in the United States is not surprising given the comparative mortality levels for heart disease and some other diseases shown in Figures 2-1 and 2-2; however, it is also true that national levels of self-reported rates of these three diseases do not correlate well with life expectancy. When the prevalence of self-reported heart disease, stroke, and diabetes is compared with life expectancy from country to country, little correlation is found (see Crimmins et al., 2010).3
Cancer
It may be particularly difficult to know which countries have a high incidence of cancer because variations in intensity of screening can produce differences in reported incidence that are unrelated to actual incidence. Rates of screening for prostate, breast, and colorectal cancers differ across these countries (Crimmins et al., 2010; Garcia, 2010; Preston and Ho, 2010). With respect to reported incidence, the United States has the highest rates for lung, prostate, and breast cancers (Crimmins et al., 2010; Preston and Ho, 2010), while Japanese men have the highest rates for colorectal cancer.
Preston and Ho (2010) discuss the link between high levels of screening and the relatively low mortality from both prostate and breast cancers in the United States. The Japanese have particularly low rates of both incidence and mortality for these cancers. Relative to Europe, mortality rates from colorectal cancers in the United States are quite low (Garcia, 2010). The high levels of mortality from lung cancer among American women were discussed above; because lung cancer is not screened for, its incidence is likely to reflect clinically diagnosed cases. The fact that several cancer incidence rates are so high in the United States while cancer mortality rates—except for lung cancer among women—are not particularly high is likely to stem
from differences in screening. It appears probable that higher levels of cancer screening in the United States have led to the greater reported incidence of a number of cancers and to a reduction in mortality (Crimmins et al., 2010; Preston and Ho, 2010). Denmark and the Netherlands have higher mortality from prostate, breast, and colorectal cancers than the United States; as indicated above, they also have relatively high levels of lung cancer. Screening appears to be markedly less prevalent in Denmark (Garcia, 2010).
Differences in Risk Factors
A high cholesterol level, high blood pressure, diabetes, smoking, and obesity are well known to be risk factors for morbidity and mortality from cardiovascular disease and other causes of death. The panel considered whether differences in these risk factors might play a role in the diverging trends in life expectancy between the United States and other high-income countries. Recent research indicates that certain biological risk factors, such as high levels of glycated hemoglobin, cholesterol, C-reactive protein, systolic blood pressure, or fibrinogen, are more common among Americans than among the English and Japanese (Banks et al., 2006; Crimmins et al., 2008).
High Cholesterol Levels
Self-reports of ever having been diagnosed with high cholesterol are two to three times more frequent in the United States than in other countries (Crimmins et al., 2010). According to available data from the World Health Organization (WHO), however, people in the United States do not have higher measured cholesterol levels than people in other high-income countries (see Table 2-2). Among the countries under study with comparable data, measured cholesterol levels are broadly similar, with the exception of higher levels among the English. This national difference in the ranking
TABLE 2-2 Percentage of Population Having Measured Prevalence of High Cholesterol (≥240 mg/dl), Ages 50–64
|
Country |
Men |
Women |
|
United States (2001–2006) |
19.7 |
26.7 |
|
Netherlands (2001) |
23.8 |
28.3 |
|
Spain (1992) |
24.3 |
32.8 |
|
England (2004) |
38.7 |
51.2 |
|
Japan (2004) |
14.4 |
28.6 |
|
Canada (1990) |
27.8 |
28.6 |
|
SOURCE: Adapted from Crimmins et al. (2010, Table 3-3). Reprinted with permission. |
||
of ever having been diagnosed with high cholesterol and currently being measured as having high cholesterol is related to the increasing tendency to take drugs that lower cholesterol levels. Although the use of cholesterol-lowering drugs is increasing rapidly in most high-income countries, it is particularly high in the United States (see Table 2-3). In short, more people in the United States have been diagnosed with high cholesterol levels and prescribed drugs to lower those levels, and because the drugs are effective, the percentage of people in the United States with measured high cholesterol is lower than that in some other countries (see Table 2-2).
High Blood Pressure
The picture for high blood pressure is in many ways parallel to that for high cholesterol levels. People in the United States are more likely to report that they have been told they have hypertension at some time in the past (Crimmins et al., 2010). Yet men in the United States generally have relatively low measured blood pressure levels compared with men in other countries; this is less true for women (see Table 2-4). Notably, Japan appears
TABLE 2-3 Percentage of Population Taking Lipid-Lowering Drugs
|
|
Ages 50+ |
|
|
Country |
Men |
Women |
|
United States (2001–2006) |
26.8 |
24.1 |
|
Denmark (2004) |
12.9 |
9.4 |
|
France (2004) |
23.3 |
21.6 |
|
Italy (2004) |
12.2 |
12.9 |
|
Netherlands (2004) |
15.0 |
12.3 |
|
Spain (2004) |
15.4 |
16.1 |
|
Japan (2004, 2006) |
8.3 |
15.1 |
|
Canada (2003) |
24.5 |
20.3 |
|
Australia (1999–2001) |
16.3 |
16.5 |
|
SOURCE: Adapted from Crimmins et al. (2010, Table 3-4). Reprinted with permission. |
||
TABLE 2-4 Percentage of Population Having Measured High Blood Pressure (≥140/90 mm Hg), Ages 50–64
|
Country |
Men |
Women |
|
United States (2001–2006) |
28.1 |
36.6 |
|
France (1996) |
60.6 |
65.2 |
|
England (2004) |
33.4 |
27.9 |
|
Japan (2000) |
52.5 |
41.2 |
|
Australia (1999–2000) |
39.0 |
33.4 |
|
SOURCE: Adapted from Crimmins et al. (2010, Table 3-5). Reprinted with permission. |
||
TABLE 2-5 Percentage of Population Using Antihypertensive Drugs by Gender and Country: Ages 50+
|
Country |
Men |
Women |
|
United States |
47.2 |
50.4 |
|
Denmark |
28.3 |
25.8 |
|
France |
29.4 |
34.6 |
|
Italy |
34.1 |
38.8 |
|
Netherlands |
22.4 |
27.7 |
|
Spain |
24.6 |
36.9 |
|
England |
27.7 |
29.8 |
|
Japan |
28.0 |
31.0 |
|
Canada |
27.0 |
30.7 |
|
Australia |
28.0 |
36.2 |
|
SOURCE: Adapted from Crimmins et al. (2010, Table 3-6). Reprinted with permission. |
||
to have more measured high blood pressure than the United States. The fact that Americans have the highest use of antihypertensive medications (see Table 2-5) is probably part of the explanation: it appears that hypertension has been screened for and treated much more aggressively in the United States than in most other countries (Wang et al., 2007).
Obesity
One of the most notable health issues in the developed world over the past several decades is the rise of obesity. Obesity is linked to higher risk of cardiovascular disease, cancer, hypertension, type-2 diabetes, and a host of other cardiovascular and metabolic disorders (Hu, 2008). People have been getting heavier in every developed country, but nowhere is that pattern as pronounced as in the United States. Americans have been gaining more weight and gaining it at earlier ages than people in other countries (Andreyeva et al., 2007; Bleich et al., 2008; Rabin et al., 2007), and the percentage of those who are obese is higher in the United States than in any other developed country (Michaud et al., 2007). For ages 50 and above, the only groups with current levels of obesity even close to those in the United States are English men and Spanish women; for ages 65 and over, the levels of obesity are actually higher among English men and women and Spanish women. On the other hand, the obesity rate is very low in Japan. The link between obesity and mortality in the 10 countries studied here is addressed in detail in Chapter 3.
Differences in Levels of Disability
In studying disability, Crimmins and colleagues (2010) used two measures, indicating less severe and more severe disability. The first was diffi-
culty in performing at least one of 10 tasks known as Nagi functions, which include such things as lifting one’s arms above the head, carrying an object that weighs as much as 10 pounds, walking two to three blocks, and grasping small objects. The second measure was having difficulty performing at least one of the six so-called activities of daily living (ADLs), which include walking, eating, dressing, and using the toilet. Difficulty in performing an ADL typically indicates a higher level of disability than difficulty performing a Nagi function.
Americans aged 50 and older report greater levels of functional disability than people in the seven other countries for which data are available (see Table 2-6); the Danish and the Dutch report the lowest levels. The situation is similar for ADLs, except that among those aged 50 and over, English men and women report the highest levels of ADL disability, with U.S. men and women in second place. For those over age 65, somewhat smaller differences exist among the countries: Japan and the Netherlands are the only two whose prevalence of ADL disability is lower than that of the other countries.
Although there do appear to be higher levels of functional disability in the United States than in most of the other countries in the study, higher disability does not appear to be significantly correlated with lower life expectancy (see Crimmins et al., 2010).
Discussion
The United States appears to have worse health than the comparison countries by many indicators. Death rates from two leading causes of death—heart disease and diabetes—are both relatively high in the United States. The fact that heart disease accounts for most of the differences in life expectancy between the United States and the other countries must be related to higher levels of heart disease per se in the United States, although
TABLE 2-6 Percentage of Population Self-Reporting Functioning Problems: Ages 50+
|
Country |
Men |
Women |
|
United States |
61.5 |
74.0 |
|
Denmark |
34.2 |
50.3 |
|
France |
38.3 |
59.0 |
|
Italy |
43.8 |
60.2 |
|
Netherlands |
31.7 |
51.5 |
|
Spain |
43.1 |
64.9 |
|
England |
49.2 |
64.0 |
|
SOURCE: Adapted from Crimmins et al. (2010, Table 3-1). Reprinted with permission. |
||
it may also be related to the much higher levels of diagnosed heart disease in the United States. Through high levels of diagnosis and treatment, however, the levels of measured risk from high blood pressure and cholesterol—two major cardiovascular risk factors—have been reduced below those in most of the comparison countries. National levels of obesity, which are related to national levels of diabetes, may explain the high levels of the latter condition and its relative contribution to loss of life expectancy in the United States.
In many ways, Japan is the antithesis of the United States. Its population has relatively little heart disease and diabetes; functioning is good, and disability is low. In addition, a number of cancers are quite low in terms of both incidence and mortality in Japan. On the other hand, Japan has managed to be the world leader in life expectancy despite relatively high levels of high blood pressure and stroke. While the United States and Japan line up well at the extremes of longevity and disease prevalence, the association is less clear for other countries. In particular, while they share poor life expectancy trends with the United States, the Netherlands and Denmark differ from the United States in a number of aspects of health. They report relatively low levels of heart disease and diabetes and have relatively little disability. On the other hand, women in these three countries report more stroke than those in other countries. While morbidity and disability supply some pieces to the longevity puzzle, then, their signals are somewhat ambiguous.