3
Understanding Pathophysiological Changes
Traumatic brain injury (TBI) is characterized by both the primary damage resulting from physical disruption of neural and vascular structures and the early emergence of secondary pathogenic events, which collectively contribute to neurologic deficits (Andriessen et al., 2010; Dash et al., 2010; Marklund et al., 2006). The identification of nutrients, dietary supplements, or specific diets that may provide resilience or treat TBI requires an understanding of the key pathophysiological events that govern both injury and reparative processes. A detailed description of those events for the various types of TBI can be found in the published literature and will not be repeated in this document. The reader is referred to recent reviews addressing the pathophysiology of focal and diffuse TBI including diffuse axonal injury, a common consequence of TBI (Andriessen et al., 2010; Farkas and Povlishock, 2007); moderate, severe, and penetrating TBI (Dash et al., 2010; Maas et al., 2008); blast TBI (Cernak and Noble-Haeusslein, 2010; Desmoulin and Dionne, 2009; Elder and Cristian, 2009; Hicks et al., 2010; Ling et al., 2009; Taber et al., 2006); and mild or concussion TBI, including recurrent injuries (Dash et al., 2010; Elder and Cristian, 2009; Mazzeo et al., 2009; McKee et al., 2009b; Weber, 2007). As background for the report, this chapter includes a brief review of the literature on the pathophysiological changes that accompany TBI. The sequence of events following TBI has been the subject of different classifications. The committee relies on a recent working definition that describes the onset of secondary pathogenic processes after TBI (Margulies et al., 2009). This chapter will refer to primary or acute effects as those effects that begin within the first minutes after injury, secondary or subacute effects as those that arise over the next 24 hours after injury, and long-term or chronic effects as those that are associated with the insult but occur at a later time. The committee recognizes that, as Margulies and colleagues (2009) observe, these definitions are estimates of the emergence of pathogenic events whose duration is likely to be variable and possibly overlapping. Both the cascade of secondary effects and the long-term effects are consequences of the primary insult and are susceptible to interventions to improve resilience or to treat TBI. The chapter also includes a brief review of the animal models and biomarkers used for TBI. Although the information in this chapter is provided
as background to this report, the committee acknowledges the importance of developing good animal models and identifying biomarkers of the disease progression and outcomes, and therefore recommendations are made for improving these areas of research.
EXPERIMENTAL MODELS OF TBI
Much of our understanding of the pathobiology of TBI has arisen from animal models that mimic features of human TBI. There are a number of detailed reviews of models of TBI (Artinian et al., 2006; Morales et al., 2005; O’Connor et al., 2005). Some examples of in vivo models are presented in Figure 3-1. The general objective of these models is to replicate certain aspects of human brain injury. It is important to note that there is currently no single model that can accurately reflect the heterogeneity of human TBI, and in each of these models, pathologic and neurologic outcomes vary according to the severity and location of the insult and heterogeneity of the vasculature. Also, there are no good animal models for mild or repetitive TBI.
Here the committee briefly reviews several of the most commonly used animal models of TBI (Morales et al., 2005): the weight-drop model, the controlled cortical impact model, the fluid percussion model, and the impact acceleration model (Figure 3-2). Each of these models produces motor/sensory and cognitive impairments. The weight-drop, midline fluid percussion, and controlled cortical impact models produce focal contusions and, depending on injury severity, may be associated with subarachnoid and intraparenchymal hemorrhages,
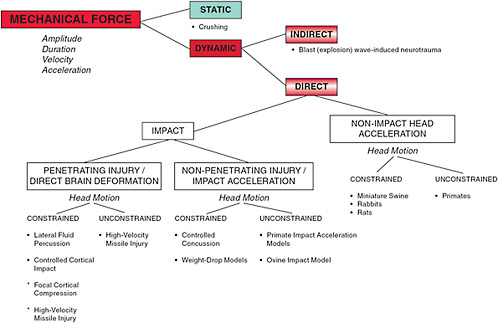
FIGURE 3-1 Classification of in vivo models of TBI.
SOURCE: Cernak, 2005.
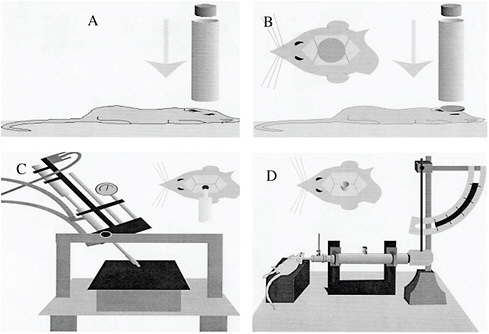
FIGURE 3-2 Rodent models of TBI: (A) weight-drop model, (B) impact acceleration model, (C) controlled cortical impact model, and (D) fluid percussion model.
SOURCE: Morales et al., 2005.
disruption of the blood-brain barrier (BBB), cortical and subcortical cell loss, and diffuse axonal injury. The weight-drop model relies on a free-falling, guided weight that strikes the exposed skull or the dura; the head may be either restrained or unrestrained. The midline fluid percussion injury model entails delivery of a brief pulse of fluid to the intact dura. The skull is exposed and after a craniectomy to expose the dura, an injury is produced by delivery of a fluid bolus, resulting from the release of a pendulum. The controlled cortical impact model utilizes a rigid impactor, controlled by pressurized air, to strike the exposed dura.
The impact acceleration model is characterized by a more diffuse injury that includes hemorrhage (typically intraparenchymal as well as subarachnoid); disruption of the BBB; cortical and subcortical damage; and widespread axonal swelling, damage, or both. This model uses a weight-drop strategy. However, a plate is secured to the skull to distribute the weight and minimize skull fractures. The head is unrestrained and positioned on a cushion with specified properties that allow a defined movement of the head after impact. Finally, it is noteworthy that a modification to the fluid percussion injury, with the insult shifted from midline to a more lateral position, results in both focal and diffuse brain injury.
Models of blast-induced brain injury, developed and characterized in both large and small animals, were reviewed by Cernak and Noble-Haeusslein in 2010. In brief, shock waves are produced by either shock tubes using compressed air or gas, or blast tubes that rely on explosive charges. There is increasing evidence that these models share pathologic and biochemical characteristics seen in the more traditional models of focal and diffuse TBI, including hemorrhage, diffuse axonal injury, cortical and subcortical cell injury, metabolic disturbances/energy failure, inflammation, and oxidative stress. What remains controversial is the extent to which blast-induced brain injuries have unique temporal and spatial profiles of pathogenic events that would distinguish them from other types of TBIs.
MODERATE, SEVERE, AND PENETRATING TBI
As discussed by the National Institutes of Health (NIH) in 2002, while concussion is the most minor and common type of TBI, more severe types of TBI have been described (Chapter 1) as moderate, severe, and penetrating. Moderate, severe, and penetrating TBI will be considered together as one specific type of TBI for the purpose of presenting mechanisms; however, it is important to note that every case will present unique characteristics due to the nature of the insult itself, the location of the injury in the brain, and the individual. Such heterogeneity is a likely determinant of outcome and is considered a major barrier to developing or optimizing therapeutics for the brain-injured patient (Saatman et al., 2008).
This section draws from the 2009 Institute of Medicine (IOM) report Gulf War and Health: Volume 7: Long-Term Consequences of Traumatic Brain Injury, which describes the biology of TBI based on animal models and brain-injured patients and from other reviews (Cederberg and Siesjo, 2010; Margulies et al., 2009; Morganti-Kossmann et al., 2007, 2010; Unterberg et al., 2004; Werner and Engelhard, 2007; Ziebell and Morganti-Kossmann, 2010). A schematic hypothesis of the series of events resulting from injury is shown in Figure 3-3. These events will be presented as primary and secondary, depending on the time of appearance. [This background does not present long-term events because they are not included in the statement of task for this study.] Repair and recovery mechanisms that have also been identified as potential targets for interventions are briefly described as well. Finally, the existence of endogenous neuroprotective factors provides another mechanism to influence the health outcomes of TBI, and it is also included here.
Primary or Acute Effects
Primary (i.e., acute) effects are those that occur during the first minutes after the injury (Table 3-1). The primary effects are the result of mechanical damage that includes stretching and/or rupture of cellular membranes, release of intracellular and vascular contents, and alterations of cerebral blood flow and metabolism. Axons may be severely compromised, as evidenced by perturbations in axonal transport, cytoskeletal damage, swelling, and disconnection (Povlishock and Katz, 2005; Smith et al., 2003). Injury to the head often results in damage to the vascular system that can, depending on the extent of the damage, result in serious complications. For example, hemorrhage and intravascular coagulation can develop, potentially leading to hemorrhagic or ischemic stroke. Studies in animals and humans have revealed that focal or global ischemia frequently occurs both early after the injury and in late stages, and suggest that ischemic stroke and TBI share similar mechanisms. Morphological injury, hypotension, inadequate availability of nitric oxide or cholinergic neurotransmitters, and potentiation of prostaglandin-induced vasoconstriction are all mechanisms that result in ischemia.
TBI patients might experience hypoperfusion or hyperfusion; each represents a mismatch between cerebral blood flow and metabolism, and both are pathological conditions with detrimental outcomes. For example, cerebral blood flow that exceeds the metabolic requirement would result in increased cerebral blood volume and intracranial pressure. Intracranial pressure also occurs as a result of swelling of tissues and fluid accumulation. Depending on the injury, metabolic failure also occurs, leading to mitochondrial dysfunction (i.e., reduced respiratory rates and production of adenosine 5′-triphosphate [ATP] and calcium overload) (see also Sullivan in Appendix C). The ischemia pattern and impaired regulation of aerobic metabolism result in greater reliance upon anaerobic metabolism of glucose that in turn results in an accumulation of lactic acid from the accelerated anaerobic
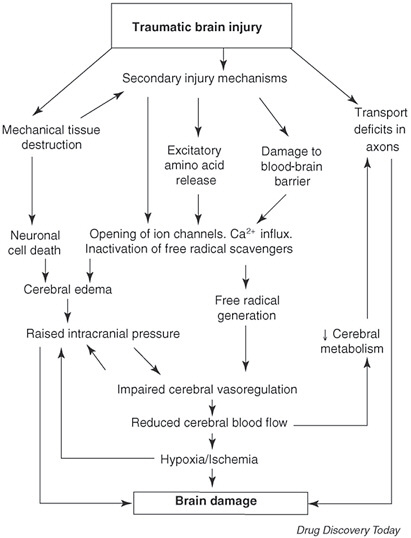
FIGURE 3-3 Cascade of pathophysiological events after traumatic brain injury.
SOURCE: Jain, 2008.
glycolysis. Hypermetabolism and anaerobic glycolysis from glucose occur in an attempt to meet energy needs.
One major event that happens early after insult is the massive ionic influx referred to as traumatic depolarization. Anaerobic glycolysis is inadequate to maintain energy states of the transient transmembrane ionic fluxes and neuroexcitation, and the consequent depletion of ATP results in alterations of ion pumps (i.e., efflux of potassium and influx of sodium and calcium) and the release of neurotransmitters. The release of neurotransmitters, specifically glutamate, into the extracellular compartment results in an overstimulation of glutamate receptors linked to ion channels and creates prolonged membrane depolarization, depletion of ATP stores, and an increase in intracellular calcium derived from both extracellular and intracellular stores, indicating disturbances in mitochondrial function. (For a discussion of the timing of the cascade typically seen in experimental brain injury models and the consequences of the early, high glycolytic rate resulting in ionic pump disturbance, the reader
TABLE 3-1 Initiation of Acute Secondary Events Post-TBI
|
Within Minutes |
Minutes–24 Hours |
24–72 Hours |
|
Cell/axon stretching, compaction of neurofilaments, impaired axonal transport, axonal swelling, axonal disconnection |
Oxidative damage: increased reactive oxygen and nitrogen species (lipid peroxidation, protein oxidation, peroxynitrite), reduction in endogenous antioxidants (e.g., glutathione) |
Nonischemic metabolic failure |
|
Disruption of the blood-brain barrier |
Ischemia |
|
|
Excessive neuronal activity: glutamate release |
Edema: cytotoxic vasogenic |
|
|
Widespread changes in neurotransmitters: catecholamines, serotonin, histamine, GABA, acetylcholine |
Enzymatic activation: kallikrein-kinins, calpains, caspases, endonucleases, metalloproteinases |
|
|
Hemorrhage (heme, iron-mediated, toxicity) |
Decreased ATP: changes in brain metabolism (altered glucose utilization and switch to alternative fuels), elevated lactate |
|
|
Physiologic disturbances: decreased cerebral blood flow, hypotension, hypoxemia, increased cranial pressure, decreased cerebral perfusion pressure |
Cytoskeletal changes in cell somas and axons |
|
|
Increased free radical production |
Widespread changes in gene expression: cell cycle, metabolism, inflammation, receptors, channels and transporters, signal transduction, cytoskeleton, membrane proteins involved in transcription/translation |
|
|
Disruption of calcium homeostasis |
Inflammation: Cytokines, chemokines, cell adhesion molecules, influx of leukocytes, activation of resident macrophages |
|
|
Mitochondrial disturbances |
|
|
|
SOURCE: Margulies and Hicks, 2009. |
||
is referred to Hovda et al., 1995.) A series of proteases becomes activated by the increase in calcium, resulting in cytoskeletal damage and further BBB breakdown, cell injury, and generation of free radicals. In this sense, a decrease in glutamate transporters in glial cells is also thought to be responsible for the significant increase in glutamate levels early after TBI.
Although there may be direct damage to axons from shear and tensile forces, it is now the prevalent opinion that damage to axons occurs mostly via deformation and changes in permeability that permit the influx of calcium and the opening of calcium channels. This increase in intracellular calcium induces proteolysis by calcium-dependent proteases; calcium may also enter and damage the mitochondria and disrupt ionic homeostasis, leading to more proteolysis and swelling, impaired axonal transport, and disconnection.
After head injury, electroencephalogram recordings show early signs of dysfunction. There is a significant risk of developing recurrent seizures that can start as early as within a week of injury, or as late as years afterward. The hippocampus is particularly vulnerable to TBI, as evidenced in part by immediate mechanically induced damage to interneurons in the dentate granule cell layer of the hippocampus that are remote from the site of insult (Gallyas and Zoltay, 1992; Toth et al., 1997). These morphologic findings correlate with an
early selective depolarization of the resting membrane potentiation, attributed to a decrease in the activity of the electrogenic Na+/K+-ATPase, that results in an enhancement of the efficacy of excitatory inputs to these interneurons (Ross and Soltesz, 2000).
Secondary or Subacute Effects
Secondary (i.e., subacute) effects are defined as those experienced up to 24 hours after injury (Table 3-1). There are multiple sources of reactive oxygen and nitrogen species, as mentioned in the process described in the preceding paragraphs. The formation of free radicals is augmented by their own reactivity as lipid, protein, and DNA (deoxyribonucleic acid) oxidation continues. The brain is especially vulnerable to oxidative damage, in part because of its high rate of oxidative activity and relatively low antioxidant capacity. In the setting of TBI, the oxidative cascade overwhelms endogenous antioxidants (e.g., superoxide dismutase and catalase) and low-molecular antioxidants (e.g., glutathione and melatonin, tocopherol, and ascorbic acid), resulting in cell injury and death.
Ischemia may occur at this stage of the injury, leading to further accumulation of lactic acid, depletion of ATP, alteration of membrane function, and release of neurotransmitters. The depolarization of membranes in smooth muscle, release of endothelin and reduced nitric oxide, vasoconstriction, and formation of free radicals may lead to cerebral vasospasm, a condition that determines the outcome of the patient.
The immune response to TBI may promote both pathogenesis and recovery processes; the precise mechanisms underlying the duality of inflammation are not yet clearly defined. The BBB is compromised early after TBI, resulting in the emergence of vasogenic edema and an influx of circulating leukocytes including neutrophils, monocytes, and lymphocytes (Ziebell and Morganti-Kossmann, 2010). These leukocytes release inflammatory mediators such as prostaglandins, free radicals, complement factors, and cytokines, which in turn further support the travel of leukocytes into the brain and mobilize glia to the injury site (Morganti-Kossmann et al., 2007). Cytokines generated in response to TBI likely have multiple roles that may support tissue damage as well as repair mechanisms. For example, interleukin-1, which triggers cell activation by binding to specific membrane receptors, plays a key role in initiating an inflammatory cascade, but interleukin-10, produced by microglia and astrocytes and lymphopoietic cells, appears to play a neuroprotective role by producing anti-inflammatory cytokines. Opposing roles may even be seen in the same cytokine. For example, whether the cytokine tumor necrosis factor, which is released early after injury, will function as a neuroprotectant or neurotoxin seems to be related to concentration and the timing of release. Vasoactive inflammatory molecules promote vascular dilation and trigger vasogenic edema, resulting in decreased oxygen and failure of metabolism. Further damage from inflammation comes directly from the triggering of death receptors leading to apoptotic death, and direct cell death by nitrogen oxide. From a prophylactic point of view, the increased permeability of the BBB during injury presents an opportunity for beneficial nutrients to reach the injury site. Reviews that identify inflammation as a target for interventions conclude that novel treatments should aim at minimizing the secondary injury by modifying the inflammatory response, rather than completely eliminating it.
The cascade of events described (activation of proteases, generation of free radicals, and inflammation) after TBI results in cytoskeletal damage, death of glia and neurons, and white matter degeneration. The two types of cell death that have been most studied are necrosis (due to mechanical or hypoxic tissue damage) and apoptosis (programmed cell death). Necrosis appears within hours to days after injury and is characterized by neurons that initially appear swollen, and over time assume a shrunken eosinophilic phenotype with
pyknotic nuclei (Raghupathi, 2004). In contrast to necrosis, cells that die via apoptosis show membrane disintegration, chromatin condensation, and DNA fragmentation. Recent discoveries suggest a less obvious distinction between necrosis and apoptosis, with dying cells showing structural changes that are common to both necrosis and apoptosis (Raghupathi, 2004). Such findings have led to the definition of cell death evolving to reflect a continuum between necrosis and apoptosis. Experimentally, the time course may show a biphasic pattern with peak periods of death occurring at 24 hours and one week after injury (Conti et al., 1998). Activation and deactivation of caspases are important mediators of programmed cell death. It is also believed that the delayed occurrence of cell death may offer opportunity for interventions.
Other important effects of this secondary phase are both vasogenic and cytotoxic brain edema (Unterberg et al., 2004). Vasogenic edema arises from disruption of the BBB and the concurrent ion and plasma protein transfer to the extracellular matrix, and results in accumulation of extracellular water. Cytotoxic edema reflects the intracellular accumulation of water. Cytotoxic edema is partly associated with the early release of glutamate and accumulation of ions and osmotically active solutes, and with failure of the active ion pumps in the neurons and glia. The ion pump system of the membrane cannot compensate for the increase in sodium uptake. This failure of the ion pump to maintain homeostasis and the associated cytotoxic edema is aggravated by mitochondrial structural and functional impairment. Importantly in the setting of TBI, a marked increase in net water content of the brain leads to an increase in tissue volume. With limited ability to expand due to the confines of the intracranial compartment, there is an increase in intracranial pressure and a reduction in perfusion and oxygenation, giving rise to additional ischemic damage.
BIOMARKERS OF INJURY AND OUTCOMES
Excellent reviews on biomarkers for TBI appeared in 2009 and 2010 (Dash et al., 2010; Svetlov et al., 2009). These included consideration of TBI biomarkers, inflammatory biomarkers, small-molecule biomarkers, lipid metabolite biomarkers, and biomarkers for mild and penetrating TBIs, secondary pathologies, predicting outcome, and polytrauma (Dash et al., 2010). Dash et al. (2010) provides a complete listing of these biomarkers, including their diagnostic value. Table 3-2 summarizes those biomarkers of greatest interest in the scientific community (Svetlov et al., 2009): S-100B, neuron-specific enolase, glial fibrillary acidic protein, and myelin basic protein. Cellular localization as well as strengths and limitations for each of these candidate markers are summarized in Table 3-2.
There is also an emerging interest in brain-type fatty acid–binding proteins, phosphorylated neurofilament H and ubiquitin C-terminal hydrolase, and proteolytic breakdown products of cell proteins such as alpha-II spectrin and the microtubule-binding protein tau (Dash et al., 2010). These candidates show general promise in terms of specificity and, in some cases, sensitivity. There is additional ongoing research to address pro- and anti-inflammatory biomarkers and lipid metabolites such as F2-isoprostane and 4-hydroxynonenol (Dash et al., 2010). Although the newest imaging may suggest brain damage after mild traumatic brain injury (mTBI) (Mayer et al., 2010), the committee concluded that there is not enough data yet to demonstrate that the results of imaging can be used as accurate markers of outcome.
Researchers are also interested in blast injury biomarkers in an animal model. Recent studies modeling blast injury show that glial fibrillary acidic protein (GFAP) and neuron-specific enolase (NSE) are increased in blood within the first 48 hours after blast injury. Ubiquitin C-terminal hydrolase-L1 (UCH-L1) shows a similar early increase in blood, and is also detected in cerebrospinal fluid (CSF) throughout 14 days after injury (Svetlov et al.,
TABLE 3-2 Examples of Biomarkers for TBI
|
Biomarker |
Description |
Localization |
Strengths |
Limitations |
|
S-100B |
Calcium binding protein. Serum half-life is < 60 minutes. |
Astrocytes, Schwann cells, adipocytes, chondrocytes, melanocytes |
Readily detected early after injury. Correlated to injury magnitude and outcome. |
May be insensitive to mild TBI. Poor correlation between serum and brain levels suggesting that barrier integrity is a determinant of serum levels. Increases after extracranial trauma. |
|
Neuron-specific enolase |
Isozyme of enolase. Serum half-life is 24 hours; can be detected within 6 hrs after TBI |
Neuronal cytoplasm, platelets, erythrocytes |
Serum levels thought to be sensitive indicator of mortality and outcomes. |
Possible cross-contamination with blood. May not correlate with injury severity. Limited sensitivity. Systemic increase can occur with trauma in the absence of TBI. |
|
Glial fibrillary acidic protein |
Intermediate filament protein |
Astrocytes |
Specific for brain. Not affected by extra-cranial trauma. Serum levels predictive of mortality, increased intracraneal pressure, and poor Glacow outcome scores. |
Not studied in mild or moderate TBI. |
|
Myelin basic protein |
Major constituent of myelin |
Myelin |
Marker of axonal damage—released into serum and CSF after white-matter injury. Specificity in both CSF and serum. May be predictive of outcome. |
Limited sensitivity. |
2010). Other strategies are being developed to define biomarkers for blast-induced brain injury. Among them is blastomics, an approach involving delineation of a functional interaction map of proteins that are affected by a blast-wave exposure (Svetlov et al., 2009).
While the list of putative biomarkers continues to expand, it is becoming increasingly clear that there may be no single biomarker that can adequately meet the requirements of specificity and sensitivity, and that multiple biomarkers, in conjunction with clinical data, may offer better predictability (Dash et al., 2010). There are new approaches being applied, such as trajectory analysis that takes into account temporal changes in multiple biomarkers (Berger et al., 2010).
ENDOGENOUS NEUROPROTECTIVE TARGETS
The brain produces endogenous substances that protect against insults or neurodegenerative diseases (Leker and Shohami, 2002). Enhancing their activity or increasing their levels is another target for interventions that is already under investigation. Compounds that serve as antioxidants, such as enzymes (e.g., Cu/Zn-superoxide dismutase [SOD], extracellular SOD, Mn-SOD, glutathione peroxidase, catalase) and low-molecular-weight antioxidants (e.g., uric acid and ascorbate), are induced early after ischemia and trauma. Heat shock proteins (i.e., HSP-70, HSP-90, GRP-78, HSP-27) are also induced after ischemia; they mainly prevent protein denaturation. Many growth factors (e.g., bFGF, NGF, BDNF,
TABLE 3-3 Biological Role of Neurotrophins in Axonal Guidance and Nerve Regeneration
|
Neurotrophins |
Action |
|
Nerve Growth Factor (NGF) |
Stimulates nerve regeneration Axonal guidance molecule |
|
Neurotrophin-3 (NT-3) |
Stimulates neurite outgrowth Stimulates nerve regeneration Axonal guidance molecule Growth cone collapse |
|
Neurotrophin-4/5 (NT-4/5) |
Stimulates nerve regeneration |
|
Brain-derived Neurotrophic Factor (BDNF) |
Essential condition for nerve regeneration Stimulates nerve generation |
|
SOURCE: Lykissas et al., 2007. |
|
NT-4, TGF-B, GDNF; Table 3-3) and their receptors have been implicated in the repair and recovery phase of injury. However, many questions remain about their control and modulation of repair, and it appears that their effects depend on many determinants, including timing, levels, specific binding to receptors, and interaction with other factors. As mentioned above, inflammatory processes also contribute to resolution of inflammation, and cytokines have been identified that could be targeted as interventions to enhance the reparative processes. One cytokine that has received much attention is erythropoietin, which regulates hematopoiesis as a growth factor and inhibits apoptotic cell death. It is induced in cultured neurons and astrocytes under hypoxic and ischemic conditions, and it has been shown to have neuroprotective properties in various animal models of brain injury. Sex hormones (i.e., estrogen and progesterone) protect the brain from ischemia via both vascular and neuronal mechanisms. In the setting of TBI, progesterone has received more attention. Progesterone functions as a pleiotropic drug; it reduces edema, excitotoxicity, lipid peroxidation, and ischemia, and increases prosurvival growth factors and improves mitochondrial function (Cekic and Stein, 2010). It is currently being investigated in a phase III, multi-center, double-blind, randomized clinical trial for TBI (Cekic and Stein, 2010). Hypoxia-inducible factor 1 is a key regulator in hypoxia and is thought to be an important player in neurological outcomes following ischemic stroke. It regulates the functions of downstream genes that are involved in promoting glucose metabolism, angiogenesis, erythropoiesis, and cell survival. Its effects on neuronal tissue injuries, based on evidence from in vitro and preclinical studies, are still debatable. Understanding the fundamental mode of action and modulation of these potential endogenous neuroprotectants will provide a more complete picture of the pathophysiology of TBI, together with more opportunities for effective therapies, including nutritional therapies.
REPAIR AND RECOVERY MECHANISMS
This section draws from a 2007 review of the topic by Lykissas and colleagues. As a result of the processes described above, repair and recovery mechanisms are initiated concomitantly with the resolution of inflammation and edema. Although much of the information in this section comes from research in the areas of stroke and spinal cord injury, the processes described are also relevant for head injury. Processes that belong to the category of repair and recovery are revascularization of the surviving area (angiogenesis), cell genesis (glio-
and neurogenesis), axonal plasticity, and changes in the neuronal network (synaptogenesis). From a temporal perspective, these mechanisms fall into three consecutive phases: recovery of function and cell repair, axonal growth, and consolidation of new neural networks. Like the events leading to death and damage, repair and recovery processes are amenable to interventions that facilitate them and that might improve functional outcomes beyond what the normal repair mechanisms could achieve. Angiogenesis is prominent after brain injury, and it has a crucial role in supporting wound healing. Among several angiogenesis factors, vascular endothelial growth factor (VEGF) has been the most thoroughly studied. In recent reviews (Greenberg and Jin, 2005; Rosenstein et al., 2010), the authors highlight the neuroprotective role of VEGF and the detrimental effects (e.g., in motor function) of reduced levels of VEGF in animal models. VEGF has been shown to be neuroprotective after experimental TBI models (Thau-Zuchman et al., 2010). Altogether, it appears that VEGF might have two roles in neuroprotection: as a direct neurotrophic agent and as an angiogenic factor stimulating endothelial cells to provide adequate perfusion and neurotrophic factors (Rosenstein et al., 2010).
Neurogenesis, arising within the subventricular zone (SVZ) and the subgranular zone of the dentate gyrus, has led to the speculation that neurons recruited from these regions may contribute to some functional recovery after brain injury. For example, cerebral ischemia and seizures stimulate neurogenesis and the migration of neurons toward the affected zone. TBI induces hippocampal cell proliferation, with many of these cells differentiating into neurons that sometimes extend axonal projections and glia. As in cerebral ischemia, cortical injuries also result in the migration of new cells, generated in the SVZ, to areas of tissue damage. Of particular interest are treatments to enhance neurogenesis to promote cognitive recovery after TBI (Kernie and Parent, 2010).
Neurotrophic factors also may modulate recovery processes. Neutrophins constitute a family of neurotrophic factors (other families include neuropoietic cytokines, including interleukin-6; fibroblast growth factors; transforming growth factors; and insulin-like growth factors) that regulate neuronal survival, growth, and synaptic plasticity and neuro-transmission both in the central and peripheral nervous system. They may act in other target organs, in nearby cells, or in the same cell. A discussion of the identification, functions, and interactions of the neurotrophins is beyond the scope of this study, and the reader is referred to existing reviews (Hagg, 2009; Lykissas et al., 2007). Table 3-3 lists examples of neurotrophins with roles in axonal guidance and nerve regeneration. Neurotrophins perform their functions by binding to two different types of receptors, tyrosine kinase receptors and neurotrophic receptor 75. Nerve growth factor (NGF), brain-derived neurotrophic factor (BDNF), and neurotrophin 3 (NT-3) are perhaps the most studied neurotrophic factors in the context of axonal growth. Of these, the role of BDNF has generated interest among nutritionists because it has been suggested that some food components (e.g., docosahexaenoic acid and curcumin) may act as neuroprotectants by affecting the levels of this neurotrophin in the brain (Wu et al., 2004; see also Gomez-Pinilla in Appendix C).
Although in vitro studies of the injured peripheral nerve suggest a role in neuronal regeneration, neurotrophins—BDNF and N/T-4/5 in particular—have the ability to bind both growth-promoting and growth-inhibiting receptors. In vitro experiments also suggest that the timing of the signaling, the level, and the type of neurotrophin are key variables in nerve regeneration. Importantly, in vitro assays may not accurately predict the behavior of these growth factors in the central nervous system, particularly in the complex environment of the injured brain.
MILD TRAUMATIC BRAIN INJURY
The term mild traumatic brain injury (mTBI) is interchangeable with concussion. Mild TBI as defined by the Veterans Affairs/Department of Defense Clinical Practice Guidelines, is classified as structural or physiological disruption of brain function resulting from an external traumatic force. Presentation includes loss of consciousness for < 30 minutes, alteration of mental state for < 24 hours, posttraumatic amnesia for < 1 day, and a Glasgow Coma Score of 13–15 (Maruta et al., 2010). Postconcussion syndrome, which may follow mTBI, is characterized by experiencing numerous cognitive, affective, or somatic symptoms (Table 3-4) for longer than three months, and can lead to chronic disability. Recent data from the military suggest that about five percent of all the mild TBI cases suffer from postconcussion syndrome, which still represents a high number of cases (Ling, 2010).
Mild TBI is difficult to model because the insults, whether produced by fluid percussion, cortical impact, or focal brain contusions, often generate focal damage, diffuse axonal damage, cell loss, and varying degrees of hemorrhage. Nevertheless, there has been a growing effort to refine these models to better approximate the mTBI seen in a clinical setting. Several examples, listed in Table 3-5, demonstrate that although only relatively modest changes are seen in the histopathology, brain-injured animals show cognitive deficits. Of interest, despite negative findings by magnetic resonance imaging (MRI), patterns of neuronal cell loss are apparent by subsequent histological analysis (Henninger et al., 2005). Finally, it is noteworthy that following mTBI, the cortex presents with very early alterations in mitochondrial bioenergetics (Gilmer et al., 2009). Early initiation of strategies to support mitochondrial function may therefore limit the subsequent progression of secondary pathogenesis.
A common feature of TBI is diffuse axonal injury (DAI) (Maruta et al., 2010), which is characterized by a focal alteration of the axolemma, leading to an impairment in axonal transport and the appearance of a local swelling that then detaches from its distal segment (Povlishock and Katz, 2005). The latter culminates in disconnection from its downstream segment. DAI may be an accompanying feature of mTBI (Maruta et al, 2010). Because structural features of DAI are difficult to detect by traditional computed tomography (CT) or magnetic resonance imaging (MRI) scans (Maruta et al, 2010), mTBI is not easily diagnosed in the acute stage, and in fact may go unnoticed until the emergence of postconcussion symptoms (Maruta et al, 2010). Nevertheless, recent advances in neuroimaging using high resolution MRI and diffusion tensor imaging have made it possible to identify axonal damage in the brain after an mTBI (Barkhoudarian et al., 2011). Such advances offer the opportunity to better understand the vulnerability of the brain to a mild insult, and to determine the extent to which indices of damage correlate with measures of functional outcomes.
TABLE 3-4 Symptoms of Postconcussion Syndrome
|
Cognitive |
Somatic |
Affective |
|
Memory difficulties Decreased concentration Decreased processing speed |
Headache Dizziness Nausea Fatigue Sleep disturbances Blurred vision Tinnitus Hypersensitivity to light/noise |
Irritability Depression Anxiety |
|
SOURCE: Maruta et al., 2010. |
||
TABLE 3-5 Animal Models of Mild TBI
|
Model |
Pathologic Findings |
Behavioral Findings |
Molecular/Biochemical Findings |
Reference |
|
Cortical impact (rat) |
Neuronal vulnerability in the hippocampus |
Deficits in performance on Morris water maze |
Involvement of sulfonylurea receptor 1 in hippocampal cell injury |
Patel et al., 2010 |
|
Fluid percussion injury (rat) |
|
Deficits in performance on Morris water maze |
Protein oxidation (elevated protein carbonyls and reduced levels of SOD and Sir2) Reduced levels of BDNF, synapsin I, CREB, CaMKII |
Wu et al., 2010 |
|
Cortical contusion (rat) |
|
|
Alterations in mitochondrial respiration |
Gilmer et al., 2009 |
|
Weight-drop (rat) |
Serial MRI: no abnormalities in the cerebrum. Histology: loss of neurons in the frontal cortex and hippocampus, but preserved cytoskeletal architecture |
Brief loss of consciousness, extended loss of the corneal and righting reflexes; deficits in performance on Morris water maze |
|
Henninger et al., 2005 |
RECURRENT MILD HEAD INJURIES/CONCUSSIONS
There is a substantial body of literature to support recognition of second impact syndrome, which results when a mild head injury is followed shortly thereafter by a second one. Such a situation has marked clinical ramifications, including possible death. This has been documented most recently in the sphere of competitive contact sports, where determining the resting time needed before an injured athlete (e.g., a football player) can return to play has been the focus of much debate. Like competitive athletes, military personnel are also subject to recurrent concussions. If these are mild concussions (see definitions in Chapter 1), they may go unrecognized. As part of an effort to manage episodes of recurrent mild TBI, the U.S. military (the Department of Defense [DoD] and Department of Veterans Affairs [VA]) convened an expert committee in 2008 to develop evidence-based guidelines for the management of concussion/mild TBI; the product was the first system-wide codified approach to mTBI (Ling, 2010). DoD’s Policy Guidance for Management of Concussion/ Mild Traumatic Brain Injury in the Deployed Setting was updated in June 2010, and the 2008 Zurich Consensus Statement on Concussion in Sports (McCrory et al., 2009) has been adapted to determine when a soldier can return to duty, based on a functional assessment of the individual. Among military personnel, there is no epidemiological data available on the incidence of recurrent head injury (Ling, 2010).
Second impact syndrome is a rare complication associated mostly with contact sports but also with active duty military service. There is often no loss of consciousness, but suffering a second concussion before complete recovery from the first can cause cerebral edema and death. It has been suggested that the effect of recurrent mild concussions is synergistic instead of additive. Based on a handful of case reports that involved a second injury within days of the primary event, it is hypothesized that second impact syndrome results from a loss of autoregulation of cerebral blood flow and a resultant vascular engorgement. These authors (Mori et al., 2006) have also postulated that acceleration forces, substantial enough
to produce a small acute subdural hematoma in many cases, are the cause of second impact syndrome and hyperemic swelling.
Repetitive mild TBIs have been studied in vitro and in vivo using weight-drop and controlled cortical impact injuries to either the rodent skull or to the dural surface (see Table 3-6 for examples). In vitro studies, such as those that produce a stretch-induced model of injury to murine hippocampal cells, demonstrate that repeated insults produce more pronounced damage to both neurons and glia than single insults (Slemmer and Weber, 2005; Slemmer et al., 2002). Although in vivo findings vary depending on the experimental design, there are also some common characteristics. In general, a single mild injury may show either no or only a modest behavioral phenotype in terms of cognitive or motor sensory impairments, whereas repeated injuries produce a more robust adverse behavioral phenotype. An exception to this is one report that mild repetitive injuries may have a conditioning effect on the brain, with a subsequent severe injury producing no or modest effects on motor control loss when compared to severe injury alone (Allen et al., 2000). Histologic evidence of cell injury or loss and BBB dysfunction after repeated mild injuries is variable, and may reflect differences in the experimental design. There is some evidence for a temporal window of
TABLE 3-6 Examples of Experimental Models of Repetitive TBI
|
Experimental Model |
Experimental Design |
Species/Strain/Age/Sex |
General Findings |
|
Concussion weight-drop (closed head injury) (DeFord et al., 2002) |
1 or 4 mild injuries each separated by 24 hours. Various weight-drop distances (40 and 60 cm) and masses (50, 100, and 150 g) were studied. |
Mice/B6C3/9 weeks old/male |
No overt cell death or evidence of disruption of the barrier in any groups. Some groups (100 and 150 g masses) showed greater spatial learning deficits than other groups. |
|
Concussion weight-drop (closed head injury) (Laurer et al., 2001) |
1 or 2 mild injuries separated by 24 hours. |
Mice/C57BL6/10 weeks old/male |
More pronounced disruption of the BBB and somatodendritic cytoskeletal damage and motor sensory impairment after a second hit. No cognitive dysfunction or overt cell loss between groups. |
|
Weight-drop injury (exposed dural surface) (Allen et al., 2000) |
3 groups: mild, repetitive mild (3 mild injuries separated by 3 days), repetitive mild + severe as above followed by a severe injury between 3 and 5 days after last mild injury, and severe TBI. |
Rats/Sprague-Dawley/adult/male |
Repetitive mild injuries had little or no effect on motor function, whereas severe injuries showed motor dysfunction. Severe injury preceded by mild injuries showed little or no motor deficits. Cell injury and loss were minimal in mild and repetitive mild, whereas severe and repetitive mild + severe produced a similar-sized necrotic cavity. |
|
Controlled cortical impact (closed head injury) (Longhi et al., 2005) |
1 or 2 mild injuries separated by 3, 5, or 7 days. |
Mice/C57BL6/6–8 weeks old/male |
When injuries were separated by 3 days there were significantly more learning impairment, greater axonal injury and somatodendritic cytoskeletal damage, and prolonged cognitive deficits. No differences in water content or neuronal injury (Fluoro-Jade staining). |
|
Controlled cortical impact (closed head injury) (Manville et al., 2007) |
1 versus 2 mild injuries, separated by 1 day. |
Mice/C57BL6/adult/male |
Single injury did not affect ATP, glucose, or lactate, whereas repetitive injury caused severe depression in cerebral metabolism. |
vulnerability, with repeated mild injuries in close temporal proximity producing greater damage than injuries separated by longer periods of time (in the case of rodents, a separation of seven days) (Longhi et al., 2005).
Postmortem studies of athletes have suggested that repetitive head injury is associated with chronic traumatic encephalopathy (CTE) (McKee et al., 2009b). CTE presents memory disturbances, behavioral and personality changes, parkinsonism, and speech and gait abnormalities that may arise long after the last concussion blow. De Beaumont and colleagues (2009) have demonstrated neurophysiological changes in Canadian football players decades after their last game. The neuropathology consists of atrophy of the cerebral hemispheres, medial temporal lobe, thalamus, mammillary body, and brainstem, with ventricular dilation and fenestrated cavum septum pellucidum. At the microscopic level, the pathology of CTE is characterized by a tauopathy where neurofibrillary tangles are found throughout the brain in the relative absence of b-amyloid deposits. A 2010 investigation (McKee et al., 2010) indicated the presence of the DNA-binding protein TDP-43 in the frontal and temporal cortices, medial temporal lobe, basal ganglia, diencephalon, and brainstem among athletes with CTE. An association between the presence of TDP-43 in the spinal cord and CTE cases with a progressive motor neuron disease, amyotrophic lateral sclerosis (ALS), is evidence that repetitive head trauma might be linked to impairments in the motor system. TDP-43 was also found in the cerebral cortex of boxers with CTE, and in cases with a variety of neurodegenerative disorders including frontotemporal lobar degeneration as well as Alzheimer’s disease and ALS. It has been hypothesized that ALS develops as an interaction between genetic and environmental factors. Several epidemiological investigations document the incidence of ALS in athletes who had been exposed to repetitive head trauma (Chiò et al., 2005; Chen et al, 2007). Notably, the time between the injury-related events and diagnosis of ALS seems to be less than previously thought (Chiò et al., 2005). Among those who had experienced repetitive head injuries within the previous 10 years, the diagnosis of ALS was calculated to be three times higher than in those with no history of head injury (Chen et al., 2007). A few epidemiological investigations with military personnel reveal similar findings. For example, the risk of ALS among veterans of the 1991 Gulf War was about double the risk among civilians during the 10 years after the war (Horner et al., 2003).
There are many mechanisms by which recurrent head concussions may trigger neuronal degeneration (see above in moderate and severe TBI). As with moderate and severe TBI, in the case of mild concussions, there is an opportunity to investigate interventions that will impede the progress of the pathology. There are also, as with moderate and severe TBI, genetic factors contributing to this pathology that have not been identified. Neural degeneration might be associated with a widespread TDP-43 proteinopathy that contributes to the clinical manifestations of recurrent TBI, such as cognitive and memory loss, behavioral changes, and motor dysfunction. Mechanisms for the involvement of TDP-43 in neuronal degeneration have been hypothesized. For example, loss of TDP-43 activity due to sequestration in inclusions could affect its regulatory function during transcription of neurofilaments, leading to aggregates. Alternatively, abnormal phosphorylation of TDP-43 may disrupt important signaling pathways, leading to neuronal dysfunction (Forman et al., 2007).
In order to ameliorate or treat the effects of concussion, there are many research questions to answer, such as the physiological and biochemical pathways that lead to proteinopathies and tauopathies in recurrent head injuries, and the contribution of genetic or other factors (e.g., age) to outcome. As will be apparent below, an understanding of the effects of exposure to repetitive blasts and the proximity of each exposure is even more incomplete. Although human epidemiological studies are being conducted to address the effect of repetitive blasts (e.g., with Marines) and a longitudinal study is being carried out with combat
veterans and retired athletes (see Stern et al., Appendix C), there is also a need for animal models that replicate repetitive TBI in humans.
BLAST INJURIES
Relatively few studies have been conducted to elucidate the mechanisms of blast TBI and even fewer have examined the consequences of exposure to repetitive blast episodes. One 2010 study examined whether exposure to repeated explosions or firing is associated with detection of neurochemical markers of brain damage (Blennow et al., 2011). Biomarkers measured in cerebrospinal fluid were tau and neurofilament protein (for neuron damage), GFAP and S-100b (for glial cell injury), and hemoglobin and bilirubin (for hemorrhage). Serum levels of GFAP and S-100b also were measured. All levels were normal, suggesting that repeated exposure to blasts does not result in neurochemical effects. This study presents some potential limitations, however, such as the timing of sampling and the sensitivity and specificity of the biomarkers. Another study with 12 Iraq war veterans diagnosed with mTBI who reported one or more blast injuries showed decreased cerebral metabolic rate for glucose in the cerebellum, vermis, pons, and medial temporal lobe. Clinical examination revealed impairments in verbal and cognitive abilities (Peskind et al., 2011). At the time of this writing, a two-week controlled study was being conducted with Marines who, during their training to be breachers, are exposed to 50 to 70 blasts of weapons-grade explosives. The outcomes will be measured using magnetic resonance imaging (MRI), functional magnetic resonance imaging (fMRI), electroencephalogram, and neurobehavioral and biochemical testing (Ling, 2010). Although repeated blast exposures below a certain threshold result in no cumulative damage, the long-term impacts of multiple blasts above that threshold are not known (Ling, 2010).
There have been ongoing efforts to correlate some of the emerging clinical data from service members and veterans with blast as a mechanism of injury. Severe TBI from blast has been associated with a greater incidence of traumatic vasospasm (Armonda et al., 2006) than severe nonblast TBI. Evaluation of the performance of severity-matched populations with blast and nonblast injuries using neuropsychological testing did not find any significant difference between these two populations (Belanger et al., 2009). Evaluations of vestibular assessment with blast patients have shown a pattern different from that seen in nonblast injuries (Hoffer et al., 2010). There are some data utilizing neuroimaging techniques such as diffusion tensor imaging, which, in patients whose injuries were matched for severity, has shown a more diffuse pattern of brain injury in patients with blast as part of their contributing mechanism than in those without blast (Moore, 2009). To better understand and determine the role of blast as a mechanism of injury, 75 experts from the Department of Defense, the Department of Transportation, the Department of Veterans Affairs, academia, and industry were gathered from five countries in May 2009 to evaluate evidence from past and ongoing blast research at the International State-of-the-Science Meeting on Non-Impact, Blast-Induced Mild Traumatic Brain Injury. Based on the data reviewed, which included published and unpublished data from human and animal research, the participants determined there was evidence that mild trauma to the brain can occur because of blast and that this injury is different from nonblast injury. From the proceedings, this conclusion was based on evidence that demonstrated:
-
Statistically significant differences in diffusion tensor imaging-based fractional anisotropy between service members with documented mTBI associated with blast, and service members with impact-only mTBI.
-
Statistically significant differences in event-related potentials between blast and nonblast exposures in human studies.
-
Preliminary evidence of disturbed phase synchrony following blast exposure.
-
Differences in fMRI between breacher instructors and students (statistically significant fMRI results, statistically nonsignificant neurocognitive results).
-
Alterations in inflammatory markers in animal studies.
-
Physiological, histological, and/or behavioral differences between blast and nonblast exposures in shock tubes models with rodents.
-
Low-level axonal, neuronal, and/or glial damage/reactivity in blast studies (including free field and other) in porcine models.
The existence of comorbidities with psychological stress for those who sustained a TBI involving blast as a mechanism has been another challenge in attempting to compare blast TBI with nonblast (impact) TBI. One attempt to better understand and clinically correlate some of the disparate findings described above is comparison of the total number of domains or symptoms produced by those who have had TBI with a comorbidity of posttraumatic stress disorder (PTSD), those with TBI without a PTSD comorbidity, and those with PTSD but with no history of TBI or concussion. For example, it has been demonstrated (Brenner et al., 2010) that patients who had TBI with a PTSD comorbidity reported more symptoms than patients who had TBI without PTSD or patients who had PTSD without a history of TBI or concussion.
Furthermore, there is an acknowledged lack of data about long-term complications from blast injury (IOM 2009) and about how blast also may have similar effects to emerging data on CTE from recurrent injuries from sports concussions (McKee et al., 2009a).
CONCLUSIONS AND RECOMMENDATIONS
In general, TBI is characterized by its heterogeneity, reflecting the nature, severity and location of the insult. Despite this heterogeneity, there are shared mechanisms of secondary pathogenesis that are potentially amenable to therapeutic intervention. This chapter is written as background and serves as the basis for subsequent chapters in which the committee considers nutrients, dietary supplements, or specific diets whose functions and mechanisms of action suggest they might promote resilience, be efficacious when provided after TBI, or both.
Appropriate animal study designs and biomarkers of injury and recovery are considerable components of the exploration of hypotheses about the benefits of nutritional interventions. Therefore, although not related to nutrition specifically, the committee thought it important to urge the advancing of these experimental tools. There are still significant inadequacies in the current TBI animal models and biomarkers of injury, and greater advances will be realized in TBI management when these are improved. The committee made two general recommendations: first, to continue to develop better animal models, and second, to identify biomarkers of injury and improved brain function.
RECOMMENDATION 3-1. The committee recommends that DoD, in cooperation with others, refine existing animal models to investigate the potential benefits of nutrition throughout the spectrum of TBI injuries, that is, concussion/mild, moderate, severe, and penetrating, as well as repetitive and blast injuries. Development of animal models is particularly urgent for concussion/mild TBI and brain injuries because of blast as well as
for repetitive injuries. These models will also aid in understanding the pathobiology of TBI, which is particularly needed for concussion/mild TBI, blast, and repetitive injuries.
RECOMMENDATION 3-2. The committee recommends that DoD, in cooperation with others, continue to develop better clinical biomarkers of TBI (i.e., concussion/mild, moderate, severe, penetrating, repetitive, and blast injuries) for the purposes of diagnosis, treatment, and outcome assessment. In addition, the committee recommends the identification of biomarkers specifically related to proposed mechanisms of action for individual nutritional interventions.
REFERENCES
Allen, G. V., D. Gerami, and M. J. Esser. 2000. Conditioning effects of repetitive mild neurotrauma on motor function in an animal model of focal brain injury. Neuroscience 99(1):93–105.
Andriessen, T. M., B. Jacobs, and P. E. Vos. 2010. Clinical characteristics and pathophysiological mechanisms of focal and diffuse traumatic brain injury. Journal of Cellular and Molecular Medicine 14(10):2381–2392.
Armonda, R. A., R. S. Bell, A. H. Vo, G. Ling, T. J. DeGraba, B. Crandall, J. Ecklund, and W. W. Campbell. 2006. Wartime traumatic cerebral vasospasm: Recent review of combat casualties. Neurosurgery 59(6):1215–1225.
Artinian, V., H. Krayem, and B. DiGiovine. 2006. Effects of early enteral feeding on the outcome of critically ill mechanically ventilated medical patients. Chest 129(4):960–967.
Barkhoudarian, G., D. A. Hovda, and C. C. Giza. 2011. The molecular pathophysiology of concussion brain injury. Clinics in Sports Medicine 30(1):33–48.
Belanger, H. G., T. Kretzmer, R. Yoash-Gantz, T. Pickett, and L. A. Tupler. 2009. Cognitive sequelae of blast-related versus other mechanisms of brain trauma. Journal of the International Neuropsychological Society 15(1):1–8.
Berger, R. P., M. C. Bazaco, A. K. Wagner, P. M. Kochanek, and A. Fabio. 2010. Trajectory analysis of serum biomarker concentrations facilitates outcome prediction after pediatric traumatic and hypoxemic brain injury. Developmental Neuroscience 32(5–6):396–405.
Blennow, K., M. Jonsson, N. Andreasen, L. Rosengren, A. Wallin, P. A. Hellstrom, and H. Zetterberg. 2011. No neurochemical evidence of brain injury after blast overpressure by repeated explosions or firing heavy weapons. Acta Neurologica Scandinavica 123(4):245–251.
Brenner, L. A., B. J. Ivins, K. Schwab, D. Warden, L. A. Nelson, M. Jaffee, and H. Terrio. 2010. Traumatic brain injury, posttraumatic stress disorder, and postconcussion symptom reporting among troops returning from Iraq. Journal of Head Trauma Rehabilitation 25(5):307–312.
Cederberg, D., and P. Siesjo. 2010. What has inflammation to do with traumatic brain injury? Childs Nervous System 26(2):221–226.
Cekic, M., and D. G. Stein. 2010. Traumatic brain injury and aging: Is a combination of progesterone and vitamin D hormone a simple solution to a complex problem? Neurotherapeutics 7(1):81–90.
Cernak, I. 2005. Animal models of head trauma. NeuroRx 2(3):410–422.
Cernak, I., and L. J. Noble-Haeusslein. 2010. Traumatic brain injury: An overview of pathobiology with emphasis on military populations. Journal of Cerebral Blood Flow and Metabolism 30(2):255–266.
Chen, H., M. Richard, D. P. Sandler, D. M. Umbach, and F. Kamel. 2007. Head injury and amyotrophic lateral sclerosis. American Journal of Epidemiology 166(7):810–816.
Chiò, A., G. Benzi, M. Dossena, R. Mutani, and G. Mora. 2005. Severely increased risk of amyotrophic lateral sclerosis among Italian professional football players. Brain 128(3):472–476.
Conti, A. C., R. Raghupathi, J. Q. Trojanowski, and T. K. McIntosh. 1998. Experimental brain injury induces regionally distinct apoptosis during the acute and delayed post-traumatic period. Journal of Neuroscience 18(15):5663–5672.
Dash, P. K., J. Zhao, G. Hergenroeder, and A. N. Moore. 2010. Biomarkers for the diagnosis, prognosis, and evaluation of treatment efficacy for traumatic brain injury. Neurotherapeutics 7(1):100–114.
De Beaumont, L., H. Theoret, D. Mongeon, J. Messier, S. Leclerc, S. Tremblay, D. Ellemberg, and M. Lassonde. 2009. Brain function decline in healthy retired athletes who sustained their last sports concussion in early adulthood. Brain 132(Pt 3):695–708.
DeFord, S. M., M. S. Wilson, A. C. Rice, T. Clausen, L. K. Rice, A. Barabnova, R. Bullock, and R. J. Hamm. 2002. Repeated mild brain injuries result in cognitive impairment in B6C3F1 mice. Journal of Neurotrauma 19(4):427–438.
Desmoulin, G. T., and J. P. Dionne. 2009. Blast-induced neurotrauma: Surrogate use, loading mechanisms, and cellular responses. Journal of Trauma 67(5):1113–1122.
Elder, G. A., and A. Cristian. 2009. Blast-related mild traumatic brain injury: Mechanisms of injury and impact on clinical care. The Mount Sinai Journal of Medicine, New York 76(2):111–118.
Farkas, O., and J. T. Povlishock. 2007. Cellular and subcellular change evoked by diffuse traumatic brain injury: A complex web of change extending far beyond focal damage. Progress in Brain Research 161:43–59.
Forman, M. S., J. Q. Trojanowski, and V. M. Y. Lee. 2007. TDP-43: A novel neurodegenerative proteinopathy. Current Opinion in Neurobiology 17(5):548–555.
Gallyas, F., and G. Zoltay. 1992. An immediate light microscopic response of neuronal somata, dendrites and axons to non-contusing concussion head injury in the rat. Acta Neuropathologica 83(4):386–393.
Gilmer, L. K., K. N. Roberts, K. Joy, P. G. Sullivan, and S. W. Scheff. 2009. Early mitochondrial dysfunction after cortical contusion injury. Journal of Neurotrauma 26(8):1271–1280.
Greenberg, D. A., and K. Jin. 2005. From angiogenesis to neuropathology. Nature 438(7070):954–959.
Hagg, T. 2009. From neurotransmitters to neurotrophic factors to neurogenesis. Neuroscientist 15(1):20–27.
Henninger, N., S. Dutzmann, K. M. Sicard, R. Kollmar, J. Bardutzky, and S. Schwab. 2005. Impaired spatial learning in a novel rat model of mild cerebral concussion injury. Experimental Neurology 195(2):447–457.
Hicks, R. R., S. J. Fertig, R. E. Desrocher, W. J. Koroshetz, and J. J. Pancrazio. 2010. Neurological effects of blast injury. Journal of Trauma-Injury Infection and Critical Care 68(5):1257–1263.
Hoffer, M. E., C. Balaban, K. Gottshall, B. J. Balough, M. R. Maddox, and J. R. Penta. 2010. Blast exposure: Vestibular consequences and associated characteristics. Otology & Neurotology 31(2):232–236.
Horner, R. D., K. G. Kamins, J. R. Feussner, S. C. Grambow, J. Hoff-Lindquist, Y. Harati, H. Mitsumoto, R. Pascuzzi, P. S. Spencer, R. Tim, D. Howard, T. C. Smith, M. A. Ryan, C. J. Coffman, and E. J. Kasarskis. 2003. Occurrence of amyotrophic lateral sclerosis among Gulf War veterans. Neurology 61(6):742–749.
Hovda, D. A., S. M. Lee, M. L. Smith, S. Von Stuck, M. Bergsneider, D. Kelly, E. Shalmon, N. Martin, M. Caron, J. Mazziotta, et al. 1995. The neurochemical and metabolic cascade following brain injury: Moving from animal models to man. Journal of Neurotrauma 12(5):903–906.
IOM (Institute of Medicine). 2009. Gulf War and health: Long-term consequences of traumatic brain injury. Vol. 7. Washington, DC: The National Academies Press.
Jain, K. K. 2008. Neuroprotection in traumatic brain injury. Drug Discovery Today 13(23–24):1082–1089.
Kernie, S. G., and J. M. Parent. 2010. Forebrain neurogenesis after focal ischemic and traumatic brain injury. Neurobiology of Disease 37(2):267–274.
Laurer, H. L., F. M. Bareyre, V. Lee, J. Q. Trojanowski, L. Longhi, R. Hoover, K. E. Saatman, R. Raghupathi, S. Hoshino, M. S. Grady, and T. K. McIntosh. 2001. Mild head injury increasing the brain’s vulnerability to a second concussion impact. Journal of Neurosurgery 95(5):859–870.
Leker, R. R., and E. Shohami. 2002. Cerebral ischemia and trauma-different etiologies yet similar mechanisms: Neuroprotective opportunities. Brain Research. Brain Research Reviews 39(1):55–73.
Ling, G. 2010. Explosive blast traumatic brain injury. Presented at the IOM Nutrition and Neuroprotection in Military Personnel Workshop, Washington, D.C.
Ling, G. S. F., F. Bandak, R. Armonda, G. Grant, and J. M. Ecklund. 2009. Explosive blast neurotrauma. Journal of Neurotrauma 26(6):815–825.
Longhi, L., K. E. Saatman, S. Fujimoto, R. Raghupathi, D. F. Meaney, J. Davis, A. McMillan, V. Conte, H. L. Laurer, S. Stein, N. Stocchetti, and T. K. McIntosh. 2005. Temporal window of vulnerability to repetitive experimental concussion brain injury. Neurosurgery 56(2):364–373.
Lykissas, M. G., A. K. Batistatou, K. A. Charalabopoulos, and A. E. Beris. 2007. The role of neurotrophins in axonal growth, guidance, and regeneration. Current Neurovascular Research 4(2):143–151.
Maas, A. I., N. Stocchetti, and R. Bullock. 2008. Moderate and severe traumatic brain injury in adults. Lancet Neurology 7(8):728–741.
Manville, J., H. L. Laurer, W. I. Steudel, and A. E. M. Mautes. 2007. Changes in cortical and subcortical energy metabolism after repetitive and single controlled cortical impact injury in the mouse. Journal of Molecular Neuroscience 31(2):95–100.
Margulies, S., R. Hicks, and B. Combination Therapies Traumatic. 2009. Combination therapies for traumatic brain injury: Prospective considerations. Journal of Neurotrauma 26(6):925–939.
Marklund, N., A. Bakshi, D. J. Castelbuono, V. Conte, and T. K. McIntosh. 2006. Evaluation of pharmacological treatment strategies in traumatic brain injury. Current Pharmaceutical Design 12(13):1645–1680.
Maruta, J., S. W. Lee, E. F. Jacobs, and J. Ghajar. 2010. A unified science of concussion. Annals of the New York Academy of Sciences 1208:58–66.
Mayer, A. R., J. Ling, M. V. Mannell, C. Gasparovic, J. P. Phillips, D. Doezema, R. Reichard, and R. A. Yeo. 2010. A prospective diffusion tensor imaging study in mild traumatic brain injury. Neurology 74(8):643–650.
Mazzeo, A. T., A. Beat, A. Singh, and M. R. Bullock. 2009. The role of mitochondrial transition pore, and its modulation, in traumatic brain injury and delayed neurodegeneration after TBI. Experimental Neurology 218(2):363–370.
McCrory, P., W. Meeuwisse, K. Johnston, J. Dvorak, M. Aubry, M. Molloy, and R. Cantu. 2009. Consensus statement on concussion in sport—The 3rd International Conference on concussion in sport, held in Zurich, November 2008. Clinical Journal of Sport Medicine 19(3):185–200.
McKee, A. C., R. C. Cantu, C. J. Nowinski, E. T. Hedley-Whyte, B. E. Gavett, A. E. Budson, V. E. Santini, H. S. Lee, C. A. Kubilus, and R. A. Stern. 2009a. Chronic traumatic encephalopathy in athletes: Progressive tauopathy after repetitive head injury. Journal of Neuropathology and Experimental Neurology 68(7):709–735.
McKee, A. C. M., R. C. M. Cantu, C. J. A. Nowinski, E. T. M. Hedley-Whyte, B. E. P. Gavett, A. E. M. Budson, V. E. M. Santini, H.-S. M. Lee, C. A. Kubilus, and R. A. P. Stern. 2009b. Chronic traumatic encephalopathy in athletes: Progressive tauopathy after repetitive head injury. Journal of Neuropathology and Experimental Neurology 68(7):709–735.
McKee, A. C., B. E. Gavett, R. A. Stern, C. J. Nowinski, R. C. Cantu, N. W. Kowall, D. P. Perl, E. T. Hedley-Whyte, B. Price, C. Sullivan, P. Morin, H. S. Lee, C. A. Kubilus, D. H. Daneshvar, M. Wulff, and A. E. Budson. 2010. TDP-43 proteinopathy and motor neuron disease in chronic traumatic encephalopathy. Journal of Neuropathology and Experimental Neurology 69(9):918–929.
Moore, D. F. 2009. Diffusion Tensor Imaging and mTBIóA Case-Control Study of Blast (+) in Returning Service Members Following OIF and OEF. Seattle, WA: 61st Annual Meeting of the American Academy of Neurology Platform Presentation.
Moore, D. F., et al. 2010. Diffusion Tensor Imaging and mTBI—A Case-Control Study of Blast (+) in Returning Service Members Following OIF and OEF. Under review Journal of Neurotrauma. Platform presentation at American Academy of Neurology, 2009.
Morales, D. M., N. Marklund, D. Lebold, H. J. Thompson, A. Pitkanen, W. L. Maxwell, L. Longhi, H. Laurer, M. Maegele, E. Neugebauer, D. I. Graham, N. Stocchetti, and T. K. McIntosh. 2005. Experimental models of traumatic brain injury: Do we really need to build a better mousetrap? Neuroscience 136(4):971–989.
Morganti-Kossmann, M. C., L. Satgunaseelan, N. Bye, and T. Kossmann. 2007. Modulation of immune response by head injury. Injury 38(12):1392–1400.
Morganti-Kossmann, M. C., E. Yan, and N. Bye. 2010. Animal models of traumatic brain injury: Is there an optimal model to reproduce human brain injury in the laboratory? Injury 41(Suppl. 1):S10–S13.
Mori, T., Y. Katayama, and T. Kawamata. 2006. Acute hemispheric swelling associated with thin subdural hematomas: Pathophysiology of repetitive head injury in sports. Acta Neurochirurgica. Supplement 96:40–43.
O’Connor, C. A., I. Cernak, and R. Vink. 2005. Both estrogen and progesterone attenuate edema formation following diffuse traumatic brain injury in rats. Brain Research 1062(1–2):171–174.
Patel, A. D., V. Gerzanich, Z. H. Geng, and J. M. Simard. 2010. Glibenclamide reduces hippocampal injury and preserves rapid spatial learning in a model of traumatic brain injury. Journal of Neuropathology and Experimental Neurology 69(12):1177–1190.
Peskind, E. R., E. C. Petrie, D. J. Cross, K. Pagulayan, K. McCraw, D. Hoff, K. Hart, C. E. Yu, M. A. Raskind, D. G. Cook, and S. Minoshima. 2011. Cerebrocerebellar hypometabolism associated with repetitive blast exposure mild traumatic brain injury in 12 Iraq war veterans with persistent post-concussion symptoms. Neuroimage 54(Suppl. 1):S76–S82.
Povlishock, J. T., and D. I. Katz. 2005. Update of neuropathology and neurological recovery after traumatic brain injury. Journal of Head Trauma Rehabilitation 20(1):76–94.
Raghupathi, R. 2004. Cell death mechanisms following traumatic brain injury. Brain Pathology 14(2):215–222.
Ross, S. T., and I. Soltesz. 2000. Selective depolarization of interneurons in the early posttraumatic dentate gyrus: Involvement of the Na(+)/K(+)-ATPase. Journal of Neurophysiology 83(5):2916–2930.
Rosenstein, J. M., J. M. Krum, and C. Ruhrberg. 2010. VEGF in the nervous system. Organogenesis 6(2):107–114.
Saatman, K. E., A. C. Duhaime, R. Bullock, A. I. R. Maas, A. Valadka, G. T. Manley, and P. Workshop Sci Team Advisory. 2008. Classification of traumatic brain injury for targeted therapies. Journal of Neurotrauma 25(7):719–738.
Slemmer, J. E., E. J. T. Matser, C. I. De Zeeuw, and J. T. Weber. 2002. Repeated mild injury causes cumulative damage to hippocampal cells. Brain 125(Pt 12):2699–2709.
Slemmer, J. E., and J. T. Weber. 2005. The extent of damage following repeated injury to cultured hippocampal cells is dependent on the severity of insult and inter-injury interval. Neurobiology of Disease 18(3):421–431.
Smith, D. H., D. F. Meaney, and W. H. Shull. 2003. Diffuse axonal injury in head trauma. Journal of Head Trauma Rehabilitation 18(4):307–316.
Svetlov, S. I., S. F. Larner, D. R. Kirk, J. Atkinson, R. L. Hayes, and K. K. W. Wang. 2009. Biomarkers of blast-induced neurotrauma: Profiling molecular and cellular mechanisms of blast brain injury. Journal of Neurotrauma 26(6):913–921.
Taber, K. H., D. L. Warden, and R. A. Hurley. 2006. Blast-related traumatic brain injury: What is known? The Journal of Neuropsychiatry and Clinical Neurosciences 18(2):141–145.
Thau-Zuchman, O., E. Shohami, A. G. Alexandrovich, and R. R. Leker. 2010. Vascular endothelial growth factor increases neurogenesis after traumatic brain injury. Journal of Cerebral Blood Flow and Metabolism 30(5):1008–1016.
Toth, Z., G. S. Hollrigel, T. Gorcs, and I. Soltesz. 1997. Instantaneous perturbation of dentate interneuronal networks by a pressure wave-transient delivered to the neocortex. Journal of Neuroscience 17(21):8106–8117.
Unterberg, A. W., J. Stover, B. Kress, and K. L. Kiening. 2004. Edema and brain trauma. Neuroscience 129(4): 1021–1029.
Weber, J. T. 2007. Experimental models of repetitive brain injuries. Progress in Brain Research 161:253–261.
Werner, C., and K. Engelhard. 2007. Pathophysiology of traumatic brain injury. British Journal of Anaesthesia 99(1):4–9.
Wu, A., Z. Ying, and F. Gomez-Pinilla. 2004. Dietary omega-3 fatty acids normalize BDNF levels, reduce oxidative damage, and counteract learning disability after traumatic brain injury in rats. Journal of Neurotrauma 21(10):1457–1467.
Wu, A. G., Z. Ying, and F. Gomez-Pinilla. 2010. Vitamin E protects against oxidative damage and learning disability after mild traumatic brain injury in rats. Neurorehabilitation and Neural Repair 24(3):290–298.
Ziebell, J. M., and M. C. Morganti-Kossmann. 2010. Involvement of pro- and anti-inflammatory cytokines and chemokines in the pathophysiology of traumatic brain injury. Neurotherapeutics 7(1):22–30.






















