
The topic of this report was recommended by the Institute of Medicine’s (IOM’s) Standing Committee on Childhood Obesity Prevention. The report grew out of a recognition that early childhood has emerged as a critical period for assessing the beginnings of obesity and instituting preventive measures. Given the evidence linking excessive weight gain in the first years of life to obesity and chronic disease in later years, the Standing Committee believed it was important to bring this issue to the attention of decision makers who influence children’s early years and to recommend policies that can advance obesity prevention for young children. The Standing Committee recognized that prevention strategies focused on this early period, when intervention can affect rapidly developing metabolic and behavioral systems, have the potential to alter the risk for obesity and chronic disease in childhood and throughout the life span. The Standing Committee believed that addressing early childhood obesity offers an important pathway to reversing the childhood obesity epidemic and that, while much research and policy effort had focused on obesity prevention for school-age children and teens, there was a paucity of consistent and authoritative guidance on obesity prevention policy and practice for young children.
Accordingly, the IOM convened the Committee on Obesity Prevention Policies for Young Children. The committee was charged with reviewing the factors related to overweight and obesity in infants, toddlers, and preschool children (from birth to 5 years of age), with a focus on nutrition and physical activity and sedentary behavior, and with making recommendations for early childhood obesity
Box 1-1
Statement of Task
An ad hoc committee will review factors related to overweight and obesity in infants, toddlers, and preschool children (birth to 5 years), with a focus on nutrition, physical activity, and sedentary behavior; identify gaps in knowledge; and make recommendations on early childhood obesity prevention policies, taking into account the differences between children birth to 2 years old and 2 to 5 years old.
In conducting its task, this committee will:
- Draw on primary and secondary sources to assess evidence on the:
- — major factors affecting obesity risk in young children, including the relationship with caregivers, physical activity opportunities and barriers, access to healthy foods, social determinants, and other important factors;
- — major factors in the first 5 years that affect attitudes, preferences, and behaviors important to overweight and obesity; and
- — relationships between elevated weight status and excess weight gain in young children and their health and well-being during childhood and risk for obesity-related comorbidities, across the life course.
- Identify settings, existing programs, and policy opportunities for childhood obesity prevention efforts in the first 5 years;
- Consider the inclusion of illustrative case studies; and
- Make recommendations on early childhood obesity prevention policies across a range of settings and types of programs, taking into account potential distinctions between policy recommendations for the first 2 years (birth to 2 years) and those developed for the next 3 years (2 to 5 years).
The primary audience of the report includes decision makers and stakeholders who have the opportunity to influence the environments in which young children develop and grow.
prevention policies. The focus of the study was on settings, existing programs, and policy opportunities for childhood obesity prevention in the first 5 years of life and on the development of recommendations across a range of settings and types of programs. The primary audience for the report is policy makers and stakeholders who have opportunities to influence the environments in which young children develop and grow.1 The committee’s statement of task is presented in Box 1-1.
_____________
1In this report, the term “young children” refers to ages birth to 5 years.
Obesity takes time to develop and for symptoms to appear. Therefore, children may be at risk for childhood obesity at a very young age but not yet defined clinically as overweight or obese. When children begin to show, for example, excess weight-for-height, this should not be dismissed as something “the child will grow out of with time.” The first years of life are critically important to a child’s health, well-being, and development. Excess weight at a young age can hinder movement and normal levels of activity and ultimately compromise later health and development.
The data reveal that the problem of obesity in infancy and early childhood is pervasive and growing. Approximately 10 percent of children under age 2 years have high weight-for-length (at or above the 95th percentile) (Ogden et al., 2010). The problem persists among children over age 2. Fully 21 percent of children aged 2–5 are overweight or obese, and the proportions of overweight and obese children in this age group have doubled in 30 years (Ogden et al., 2008, 2010). These statistics are of particular concern because rapid weight gain and obesity during the first years of life increase the risk for later obesity (Freedman et al., 2005; Goodell et al., 2009; Ong et al., 2009; Stettler et al., 2003).
The prevalence of overweight and obesity has increased significantly over the past 25 years among all ethnic groups, but is higher in some groups than in others. Variations in the prevalence of overweight among different ethnic groups in the United States are measured regularly in the National Health and Nutrition Examination Survey (NHANES). The Centers for Disease Control and Prevention (CDC) has published the most recent national survey data, showing that Hispanic males and African American females have a higher prevalence of obesity than other groups, particularly in the teenage years (CDC, 2011) (see Figure 1-1).
Although school-based prevention is critical, it is not where awareness and action on childhood obesity should begin. The childhood obesity epidemic requires a sense of urgency and new avenues for prevention focused on the first 5 years of life. The first years of life are characterized by rapid growth and developmental change. The newborn’s behavioral repertoire is limited to sleeping, feeding, crying, and a few reflexes, but over the next months and years, development proceeds rapidly. In these early years, children will learn to sleep through the night, drink from a cup, walk, and talk; in many cases, they also will learn to drink sugar-sweetened beverages (Fox et al., 2010; Siega-Riz et al., 2010) instead of milk or water, dislike and reject vegetables (except french fries), and watch too much
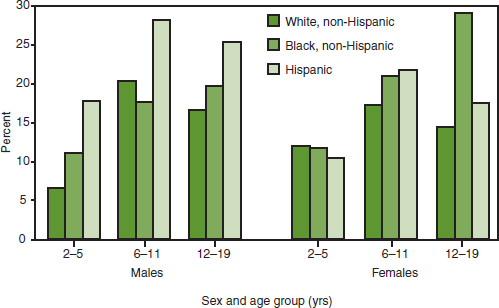
FIGURE 1-1 Prevalence of obesity among children and adolescents, by sex, age group, and race/ethnicity—United States, 2007–2008.
SOURCE: CDC, 2011.
television. By the time they reach ages 6 to 11, 35 percent will have become overweight or obese (Ogden et al., 2010).
Development is more rapid during these early years than at any other time after birth, and young children’s early experiences are “built into their bodies,” affecting neural, metabolic, and behavioral systems in ways that can influence obesity risk, health, and well-being throughout the life span (Birch and Anzman, 2010; Gluckman et al., 2008; NRC and IOM, 2000). Evidence now emerging reveals the potential of this early period for obesity prevention. In contrast to later stages of life, early development is a period when it is not necessary to change established dietary and activity patterns, but to promote the development of healthy patterns. Despite the critical role of early learning and development in shaping obesity risk, infancy and early childhood have not been a focus of obesity prevention efforts. Yet precisely because this early period is one of rapid development, it may afford the best opportunities for altering development in ways that can reduce obesity risk. It is during such periods of rapid change and instability that interventions can alter developmental pathways, and these alterations can
have long-term effects on the risk for obesity and related chronic disease decades later, in adulthood.
Unfortunately, many children learn lifestyles during the first years of life that contribute to excessive weight gain, the risk of obesity, and chronic disease later in life. Early in life, as children are being introduced to the adult diet, it is especially important that they have opportunities to learn to like and eat healthy foods. Recent survey data indicate that even the nation’s youngest children are consuming diets that are too high in energy and added sugar, fat, and salt and that include too few fruits, vegetables, and complex carbohydrates (Reedy and Krebs-Smith, 2010). With respect to activity patterns, many young children are developing lifestyles that include too much screen time, too little sleep, and too little active play (Christakis and Garrison, 2009; Iglowstein et al., 2003; NASPE, 2009; Perrin et al., 2007).
Children learn lifestyles from the adults who care for them. These adults have a powerful impact on children’s developing patterns of eating and activity; they structure their children’s environments through the choices they make, both within the family and through the child care arrangements they select for out-of-home care. These environments can differ in opportunities they provide for activity, for television viewing, and for the consumption of some foods and not others. In addition, adult caregivers serve as models for children’s developing eating and activity patterns. Infants and young children are dependent on their caregivers as well to create safe environments that can promote the development of healthy lifestyles.
Differences in caregivers’ responsiveness also affect children’s development. During the first years of life, both child and caregiver must learn to recognize and respond to the other’s cues. Responsive caregiving has been identified as an effective tool that can foster children’s social, emotional, cognitive, and physical growth, health, and development (Black and Aboud, 2011; Eshel et al., 2006). To be a responsive caregiver requires understanding infants’ and children’s early physical, cognitive, social, and motor development. Responsiveness is characterized by reciprocity between child and caregiver and includes promptly identifying the child’s needs and responding contingently and in ways that are appropriate to the child’s level of development. To be responsive to the child during periods of rapid development in early childhood, caregivers’ responses must change as children are developing new behaviors and abilities. For example, offering a young infant breast milk or formula in response to hunger cues is appropriate, but offering pureed foods before about 6 months of age is not (AAP, 2005). For this reason,
the recommendations and potential implementing actions presented in Chapters 3 through 6 addressing children’s eating, physical activity, media exposure, and sleep, respectively, differ according to the child’s age and developmental level.
PURPOSE AND SCOPE OF THE REPORT
Childhood obesity prevention begins with the patterns and behaviors of those who care for infants and young children and in the environments where children grow and develop in their first years of life. A number of key factors influence the weight of an infant or young child, including prenatal influences, eating patterns, environments, physical activity levels, sleep patterns, food and beverage marketing, and screen time. All of these factors come into play in the policy environment that shapes the places where children spend their time and must be addressed in a coordinated manner if progress is to be made against the early onset of childhood obesity.
A wide range of institutions and settings influences young children’s behaviors. The purpose of this report is to provide practical guidance for two primary audiences. The first is those who work with young children in settings where they spend their time outside the home. These comprise child care providers and early childhood educators, as well as others whose direct and indirect messages ultimately shape parents’2 knowledge about health and obesity, including health care providers and those who work in home visiting programs such as the Special Supplemental Nutrition Program for Women, Children and Infants (WIC) and the U.S. Department of Agriculture’s (USDA’s) Cooperative Extension programs. Policies and practices developed by the institutions, programs, and professional organizations with which these individuals are affiliated influence the content and frequency of their communications with parents on a number of issues related to children’s daily routines, including eating patterns, physical activity, and sleep. The second audience for the report is those who make and implement policies that directly affect children from birth to age 5.
Parents play the primary role in shaping children’s development. However, the focus of this report is on policies that are developed and implemented by policy makers and by caregivers who interact with parents and young children. The report does not make recommendations directly to parents, but rather urges these “intermediaries” to ensure that policies are implemented in a way that comple-
_____________
2For purposes of this report, the term “parents” refers to those who have primary responsibility for a child’s welfare in the home.
ments and supports parents’ efforts to maintain healthy weight in their young children. In this model, parents are not “counseled”; rather, they are provided education, knowledge, and awareness. Caregivers and policy makers act as helpful partners in the endeavor to maintain healthy weight in young children.
It is important to remember that the role of intermediary requires what is often called “cultural competency,” or the ability to work in cross-cultural situations. Culturally competent people can act sensitively and effectively in the context of beliefs, actions, and needs of a community different from their own. On its minority health website, the Department of Health and Human Services (HHS) defines culturally competent health care services as those that are “respectful of and responsive to the health beliefs, practices, and cultural and linguistic needs of diverse patients” and suggests that these types of services “can help bring about positive health outcomes” (HHS, 2011). If these beliefs, practices, and needs are not understood, or are ignored, the success of efforts to partner with parents in childhood obesity prevention will be compromised.
Parents also can play an important role beyond the direct role they play at home with their children. Working with other parents, for example, they can influence their children’s child care food environment for the better, support child care staff in making healthy changes in foods and beverages provided in young children’s educational settings, or join with their neighbors to direct local government attention to a neglected or unsafe neighborhood park.
This report briefly addresses the food and physical activity environments of the larger community in which children and families reside. However, its focus is on policy makers and caregivers of young children and their important roles in interacting with children and parents, as well as in helping to create environments and local and national policies specific to young children that can increase their chances of maintaining a healthy weight. A previous IOM publication, Local Government Actions to Prevent Childhood Obesity (IOM and NRC, 2009), addresses issues related to the food and physical activity environments of the broader community for all children and families in much greater detail. That report focuses on improving access to and consumption of healthy, safe, and affordable foods through changes in retail outlets, restaurants, community outlets, public programs, and worksites and encouraging physical activity through improvements in the built environment, initiation of programs for walking and biking, and promotion of increased recreational and routine physical activity.
Access to healthy, safe, and affordable food also is influenced by major food manufacturing decisions, as well as strategic choices made by food retailers and
restaurant industry leaders. In addition, agriculture policy and decisions made by farmers can make a difference in food availability. These decisions, processes, and policies influence the diets of all Americans to a greater or lesser extent. However, this report focuses on obesity prevention policies that are unique to children from birth to age 5 and that can be implemented through the assistance and involvement of caregivers and policy makers.
In addition, it should be noted that, although this report does not focus on pregnancy and prepregnancy, the committee decided to devote a significant portion of Chapter 2 to prenatal influences because what happens in utero may predispose young children to metabolic imbalances that lead them to gain excess weight as they grow and develop. In that chapter, the committee reaffirms prior IOM recommendations regarding healthy weight prepregnancy and healthy weight gain during pregnancy as important factors in the prevention of early childhood obesity. That chapter also comments on the need for further research in the area of prepregnancy and other influences on early childhood weight.
Finally, there is growing interest in the potential role of exogenous agents—including chemical pollutants, drugs, and microorganisms—that may disturb metabolism in a manner that promotes obesity in young children. These agents generally are thought to be potentially influential through prenatal exposure, but could also be associated with exposures in early childhood. These emerging issues in early childhood obesity prevention are covered briefly in Appendix B.
The committee’s approach to this study encompassed gathering and assessing the evidence, formulating recommendations, and exploring child care standards.
Gathering and Assessing the Evidence
The formulation of policy recommendations calls for careful consideration of the evidence associated with one course of action or another. The committee carefully considered both direct and indirect evidence regarding the likely impact of a given policy on reducing childhood obesity, as well as evidence pertaining to the potential for unintended adverse effects. The committee did not carry out a comprehensive, systematic evidence review on each important policy-related question. However, its expertise and consideration of the most pertinent studies led to recommendations that are consistent with the evidence base. Evidence on obesity prevention for young children is limited, especially for those under 2 years of age. There are multiple reasons for this lack of data. First, it is difficult and expensive
to design studies that satisfy Institutional Review Board criteria for conducting research with young children and infants. Second, both federal and private funding for research has targeted primarily school-age children. Third, most policy and environmental interventions are expensive and time-consuming, while impact is often difficult to observe in a short time period, which is the norm for many research studies. Fourth, younger children are more difficult to reach and include in primary data studies than older children. Finally, childhood obesity prevention is a relatively new area for research funding, particularly research focused on policy.
Despite the scarcity of data, the urgency of the issue of obesity in young children demands that action be taken now with the best available evidence. As noted in a previous IOM report, obesity prevention actions “should be based on the best available evidence—as opposed to waiting for the best possible evidence” (IOM, 2005, p. 3). Therefore, in addition to reviewing the published literature, the committee examined reports from organizations that work with young children; invited presentations from experts on a range of scientific, programmatic, and policy issues related to children from birth to age 5; and explored a variety of materials that have been developed for programs and practitioners.
Experimental studies testing the impact of childhood obesity prevention policies are rare. The committee gave strong observational studies serious consideration and was also receptive to evidence that a policy would be likely to affect a determinant of childhood obesity even if not studied for its direct influence on obesity. Thus, for example, policy changes that are expected to increase physical activity or promote more healthy eating in children are recommended because such intermediate outcomes are themselves associated with prevention of childhood obesity.
In reviewing the available literature, the committee drew on the extensive experience and expertise of its members. The committee’s 15 members brought to bear a broad array of knowledge and experience related to young children in the areas of
- child development,
- obesity prevention,
- child health,
- nutrition,
- infant development,
- physical activity,
- pediatrics,
- child psychology and behavior,
- child care regulations and policy,
- food marketing and media,
- health disparities,
- family health,
- federal and state child programs, and
- community health.
In areas in which the committee identified a need for additional information, outside experts were called upon at a public workshop held on June 2, 2010, in Washington, DC, titled “Emerging Issues, Programs, and Policy Needs in Early Childhood Obesity Prevention.” These experts specialized in the areas of
- injury prevention,
- motor development,
- electronic media,
- sleep,
- introduction of solids and complementary feeding,
- WIC and Head Start, and
- child care practices and policy.
Appendix A provides greater detail on the study methods, while Appendix E contains the workshop agenda.
Formulating Recommendations
For young children, actions that promote healthy development often also support obesity prevention. In formulating its recommendations, therefore, the committee considered policies that would promote young children’s health, with a focus on the key factors linked to obesity in early childhood, such as eating patterns, physical activity levels, television viewing, marketing, and sleep. The committee formulated policy recommendations and also identified potential actions that could be taken to implement those recommendations. These actions lie within the jurisdiction of relevant decision makers, were determined to be actionable based on a combination of precedent and committee members’ judgment, and have the potential to make a positive contribution to the implementation of the recommendations.
To implement the committee’s recommendations, health and child care providers often will need education and training, implementation tools they obtain from others or create, and limited or extensive technical assistance. Identifying specific tools was beyond the scope of this study, but each chapter does contain training recommendations for different audiences that are relevant to the topic at hand. Training can take a number of forms: in-service training and continuing education provided on the job, training that is part of college and associate degree programs, clinical training in health care providers’ degree programs, and certification programs (which also require continuing education) offered by national professional organizations.
All young children share the need for healthy food, optimum physical activity, sufficient sleep, health care providers who monitor their growth for healthy patterns and who advise and assist their parents in following through, and protection from the negative influences of too much sedentary behavior and the marketing of unhealthy foods and beverages to children. Nonetheless, in developing obesity prevention recommendations and implementation strategies that will be effective for young children and their families, the committee recognized the importance of negative social and economic factors in some communities that can act as barriers to a recommendation’s success.
It is widely recognized that many low-income neighborhoods have limited access to healthy foods because of a lack of nearby supermarkets (Morland et al., 2006; Powell et al., 2007; Zenk and Powell, 2008) and that places to be physically active in these communities are in short supply (Lovasi et al., 2009). At the same time, access to less healthy foods and advertising for these foods has been shown to be higher in lower-income neighborhoods (Baker et al., 2006; Black and Macinko, 2008; Kumanyika and Grier, 2006; Yancey et al., 2009). For example, fast-food restaurants and the relatively inexpensive calorie-dense foods they sell are more available in such neighborhoods (Baker et al., 2006; Larson et al., 2009). In these same neighborhoods, many stores where food is sold are small, with limited equipment and shelf space, and lack fruits and vegetables, whole grains, and low- and nonfat dairy products (IOM and NRC, 2009; Morland et al., 2002). Families with limited resources and time who must make their food purchases in these environments face difficult choices related to cost, availability, and quality.
Moreover, affordable child care providers in low-income neighborhoods may not have the resources to offer optimal opportunities for physical activity because of a lack of space or equipment (Copeland et al., 2011; Trost et al., 2010). Likewise, low-income parents and caregivers may have limited budgets
for providing nutritious meals to young children (Ding et al., in press; Kelly and Patterson, 2006; Omar et al., 2001; Slusser et al., 2011). Parents with several jobs or unusual working hours who are picking up their young children at child care centers or bringing their children to health care centers also may have very limited time to interact with their children’s providers and learn what they have to offer. Mothers who of necessity return to work soon after giving birth may have workplaces that are not friendly to breastfeeding (Guendelman et al., 2009; Kimbro, 2006; Rojjanasrirat and Sousa, 2010).
In this context, the committee attempted to formulate recommendations to caregivers and policy makers that would be universal with respect to the optimal health of young children but also feasible in the short term through creative adaptation in many different settings with families at all socioeconomic levels.
As noted earlier, the committee’s recommendations are aimed at policy makers at all levels, as well as professionals in a variety of settings where young children receive care. Given that childhood obesity is a multidimensional problem requiring a multidimensional solution, the committee believes it will be helpful for both of these groups to examine the full report as a broad base for specific actions. Obesity prevention efforts in early childhood require consistent and common policy, practices, and information across multiple settings; innovative thinking about implementation; effective communication among caregivers; and shared concerns for healthy development and obesity prevention in young children.
Exploring Child Care Standards
Throughout this report, the committee makes recommendations for the development of standards by state child care regulatory agencies. These standards have to do with physical activity, healthy eating, screen time, and sleep. They are based on a combination of the best evidence available on actions that can support obesity prevention in young children, best practices for child care settings founded on widely recommended practices, and the judgment of the committee.
Several overall strategies could be employed to foster adoption of these standards by child care providers. They include focused outreach campaigns to child care providers and parents of young children; criteria for program accreditation; the Quality Rating and Improvement System (QRIS); and state voluntary regulations and mandatory regulations developed by state regulatory agencies, often in response to specific state legislation. Focused outreach campaigns could be conducted by both private and public entities. Several national organizations offer accreditation programs for child care providers seeking to improve the quality of
care and compete better in the child care market. QRIS is not in effect in all states, but it is usually separate from state licensing standards. Typically, as with accreditation, meeting QRIS standards can make child care providers more attractive in the market, depending on their ratings, and in some cases the level of subsidies they may receive from the state to provide child care to individual children can be based on their QRIS rating. State voluntary standards often are tied to an incentive that benefits the child care program; if a program complies, for example, its licensing fee is reduced.
The focus of the committee’s recommended strategy for child care settings is mandatory regulation. This decision was made for several reasons. All states already have child care regulations of some type; thus the impact of state regulations reaches all preschool children in licensed care in a state, regardless of their geographic location or socioeconomic status. These regulations have the force of law and the potential to reach young children in an efficient and timely manner (National Association for Regulatory Administration, 2011). The reach of voluntary standards, guidelines, and criteria, by their nature, will not be as broad or thorough.
There is currently a national thrust, including among national health and child care organizations and at HHS, toward encouraging state child care regulations that will contribute to obesity prevention in young children (AAP et al., 2010; National Resource Center for Health Safety in Child Care and Early Education, 2011). For example, in Healthy People 2020 (HHS, 2010), the physical activity objectives include “increase the number of states with licensing regulations for physical activity provided in child care,” and under that objective are the sub-objectives of requiring children to engage in vigorous or moderate physical activity and requiring a certain number of minutes of physical activity per day or length of time in care. In addition, the recently passed Healthy, Hunger-Free Kids Act of 2010 (Public Law 111-296 [December 13, 2010]), through which Congress reauthorized funding for federal school meal and child nutrition programs for the next 5 years and provided new funding for these programs over 10 years, includes a requirement for interagency coordination to promote health and wellness in child care licensing. The act requires the Secretary of Agriculture to “coordinate with the Secretary of Health and Human Services to encourage state licensing agencies to include nutrition and wellness standards within licensing standards that ensure, to the maximum extent practicable, that licensed child care centers and family or group day care homes provide to all children under their supervision daily opportunities for age-appropriate physical activity,” “limit the use of electronic media
and the time spent in sedentary activity to an appropriate level,” “serve meals and snacks that are consistent with the requirements of the Child and Adult Care Food Program,” and “promote such other nutrition and wellness goals as the Secretaries determine to be necessary.”
Over the past 2 years, a number of states, including Arizona, Delaware, Massachusetts, North Carolina, Tennessee, and Texas, as well as Washington, DC, have adopted mandatory regulations related to obesity prevention in child care settings related to breastfeeding, nutrition, physical activity and inactivity, and screen time. (These and other state standards can be found on the website of the National Resource Center for Health and Safety in Child Care and Early Education at http://www.nrckids.org.) The committee recognizes that a regulatory requirement may take time to implement in some states. In the interim, this report’s recommendations could be used in developing and encouraging voluntary standards in those states.
Chapter 2 addresses the importance of beginning growth monitoring at birth in order to gauge and respond to a child’s risk of developing obesity, as well as the usefulness of understanding the major prenatal influences on early childhood weight. Chapters 3 through 6 are organized around the key factors that play a role in early childhood obesity development and prevention: physical activity (Chapter 3), eating patterns (Chapter 4), food and beverage marketing and screen time (Chapter 5), and sleep (Chapter 6). Each of these chapters begins with one or more goals that underlie the recommendations on that topic, which are then presented along with their rationale and potential actions for implementation.
AAP (American Academy of Pediatrics). 2005. Breastfeeding and the use of human milk. Pediatrics 115(2):496-506.
AAP, APHA (American Public Health Association), and National Resource Center for Health Safety in Child Care and Early Education. 2010. Preventing Childhood Obesity in Early Care and Education Programs: Selected Standards from Caring for Our Children: National Health and Safety Performance Standards. Aurora, CO: NRC.
Baker, E. A., M. Schootman, E. Barnidge, and C. Kelly. 2006. The role of race and poverty in access to foods that enable individuals to adhere to dietary guidelines. Preventing Chronic Disease [electronic resource] 3(3).
Birch, L. L., and S. L. Anzman. 2010. Learning to eat in an obesogenic environment: A developmental systems perspective on childhood obesity. Child Development Perspectives 4(2):138-143.
Black, J. L., and J. Macinko. 2008. Neighborhoods and obesity. Nutrition Reviews 66(1):2-20.
Black, M. M., and F. E. Aboud. 2011. Responsive feeding is embedded in a theoretical framework of responsive parenting. Journal of Nutrition 141(3):490-494.
CDC (Centers for Disease Control and Prevention). 2011. CDC grand rounds: Childhood obesity in the United States. Morbidity and Mortality Weekly Report 60(2):42-46.
Christakis, D. A., and M. M. Garrison. 2009. Preschool-aged children’s television viewing in child care settings. Pediatrics 124(6):1627-1632.
Copeland, K. A., S. N. Sherman, J. C. Khoury, K. E. Foster, B. E. Saelens, and H. J. Kalkwarf. 2011. Wide variability in physical activity environments and weather-related outdoor play policies in child care centers within a single County of Ohio. Archives of Pediatrics and Adolescent Medicine 165(5):435-442.
Ding, D., J. F. Sallis, G. J. Norman, B. E. Saelens, S. K. Harris, J. Kerr, D. Rosenberg, N. Durant, and K. Glanz. In press. Community food environment, home food environment, and fruit and vegetable intake of children and adolescents. Journal of Nutrition Education and Behavior.
Eshel, N., B. Daelmans, M. C. D. Mello, and J. Martines. 2006. Responsive parenting: Interventions and outcomes. Bulletin of the World Health Organization 84:991-998.
Fox, M. K., E. Condon, R. R. Briefel, K. C. Reidy, and D. M. Deming. 2010. Food consumption patterns of young preschoolers: Are they starting off on the right path? Journal of the American Dietetic Association 110(12):S52-S59.
Freedman, D. S., L. K. Khan, M. K. Serdula, W. H. Dietz, S. R. Srinivasan, and G. S. Berenson. 2005. The relation of childhood BMI to adult adiposity: The Bogalusa Heart Study. Pediatrics 115(1):22-27.
Gluckman, P. D., M. A. Hanson, C. Cooper, and K. L. Thornburg. 2008. Effect of in utero and early-life conditions on adult health and disease. New England Journal of Medicine 359(1):61-73.
Goodell, L. S., D. B. Wakefield, and A. M. Ferris. 2009. Rapid weight gain during the first year of life predicts obesity in 2-3 year olds from a low-income, minority population. Journal of Community Health 34(5):370-375.
Guendelman, S., J. L. Kosa, M. Pearl, S. Graham, J. Goodman, and M. Kharrazi. 2009. Juggling work and breastfeeding: Effects of maternity leave and occupational characteristics. Pediatrics 123(1):e38-e46.
HHS (U.S. Department of Health and Human Services). 2010. Healthy People 2020. http://www.healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicId=33 (accessed June 11, 2011).
HHS. 2011. What Is Cultural Competency? http://www.minorityhealth.hhs.gov/templates/browse.aspx?lvl=2&lvlID=11 (accessed March 22, 2011).
Iglowstein, I., O. G. Jenni, L. Molinari, and R. H. Largo. 2003. Sleep duration from infancy to adolescence: Reference values and generational trends. Pediatrics 111(2):302-307.
IOM (Institute of Medicine). 2005. Preventing Childhood Obesity: Health in the Balance. Washington, DC: The National Academies Press.
IOM and NRC (National Research Council). 2009. Local Government Actions to Prevent Childhood Obesity. Washington, DC: The National Academies Press.
Kelly, L. E., and B. J. Patterson. 2006. Childhood nutrition: Perceptions of caretakers in a low-income urban setting. The Journal of School Nursing: The Official Publication of the National Association of School Nurses 22(6):345-351.
Kimbro, R. T. 2006. On-the-job moms: Work and breastfeeding initiation and duration for a sample of low-income women. Maternal and Child Health Journal 10(1):19-26.
Kumanyika, S., and S. Grier. 2006. Targeting interventions for ethnic minority and low-income populations. Future of Children 16(1):187-207.
Larson, N. I., M. T. Story, and M. C. Nelson. 2009. Neighborhood environments. Disparities in access to healthy foods in the U.S. American Journal of Preventive Medicine 36(1).
Lovasi, G. S., M. A. Hutson, M. Guerra, and K. M. Neckerman. 2009. Built environments and obesity in disadvantaged populations. Epidemiologic Reviews 31(1):7-20.
Morland, K., S. Wing, A. Diez Roux, and C. Poole. 2002. Neighborhood characteristics associated with the location of food stores and food service places. American Journal of Preventive Medicine 22(1):23-29.
Morland, K., A. V. Diez Roux, and S. Wing. 2006. Supermarkets, other food stores, and obesity: The Atherosclerosis Risk in Communities Study. American Journal of Preventive Medicine 30(4):333-339.
NASPE (National Association for Sport and Physical Education). 2009. Active Start: A Statement of Physical Activity Guidelines for Children Birth to Five Years. Reston, VA: NASPE Publications.
National Association for Regulatory Administration. 2011. Strong Licensing: The Foundation for a Quality Early Care and Education System. http://naralicensing.org/ Strong_Licensing (accessed June 10, 2011).
National Resource Center for Health and Safety in Child Care and Early Education. 2011. Achieving a State of Healthy Weight: A National Assessment of Obesity Prevention Terminology in Child Care Regulations 2010. Aurora, CO: National Resource Center for Health and Safety in Child Care and Early Education.
NRC (National Resource Council) and IOM. 2000. From Neurons to Neighborhoods: The Science of Early Childhood Development. Washington, DC: National Academy Press.
Ogden, C. L., M. D. Carroll, and K. M. Flegal. 2008. High body mass index for age among U.S. children and adolescents, 2003-2006. Journal of the American Medical Association 299(20):2401-2405.
Ogden, C. L., M. D. Carroll, L. R. Curtin, M. M. Lamb, and K. M. Flegal. 2010. Prevalence of high body mass index in U.S. children and adolescents, 2007-2008. Journal of the American Medical Association 303(3):242-249.
Omar, M. A., G. Coleman, and S. Hoerr. 2001. Healthy eating for rural low-income toddlers: Caregivers’ perceptions. Journal of Community Health Nursing 18(2):93-106.
Ong, K. K., P. Emmett, K. Northstone, J. Golding, I. Rogers, A. R. Ness, J. C. Wells, and D. B. Dunger. 2009. Infancy weight gain predicts childhood body fat and age at menarche in girls. Journal of Clinical Endocrinology and Metabolism 94(5):1527-1532.
Perrin, J. M., S. R. Bloom, and S. L. Gortmaker. 2007. The increase of childhood chronic conditions in the United States. Journal of the American Medical Association 297(24):2755-2759.
Powell, L. M., M. C. Auld, F. J. Chaloupka, P. M. O’Malley, and L. D. Johnston. 2007. Associations between access to food stores and adolescent body mass index. American Journal of Preventive Medicine 33(Suppl. 4):S301-S307.
Reedy, J., and S. M. Krebs-Smith. 2010. Dietary sources of energy, solid fats, and added sugars among children and adolescents in the United States. Journal of the American Dietetic Association 110(10):1477-1484.
Rojjanasrirat, W., and V. D. Sousa. 2010. Perceptions of breastfeeding and planned return to work or school among low-income pregnant women in the USA. Journal of Clinical Nursing 19(13-14):2014-2022.
Siega-Riz, A. M., D. M. Deming, K. C. Reidy, M. K. Fox, E. Condon, and R. R. Briefel. 2010. Food consumption patterns of infants and toddlers: Where are we now? Journal of the American Dietetic Association 110(12):S38-S51.
Slusser, W., M. Prelip, J. Kinsler, J. T. Erausquin, C. Thai, and C. Neumann. 2011. Challenges to parent nutrition education: A qualitative study of parents of urban children attending low-income schools. Public Health Nutrition 1-9.
Stettler, N., S. K. Kumanyika, S. H. Katz, B. S. Zemel, and V. A. Stallings. 2003. Rapid weight gain during infancy and obesity in young adulthood in a cohort of African Americans. American Journal of Clinical Nutrition 77(6):1374-1378.
Trost, S. G., D. S. Ward, and M. Senso. 2010. Effects of child care policy and environment on physical activity. Medicine and Science in Sports and Exercise 42(3):520-525.
Yancey, A. K., B. L. Cole, R. Brown, J. D. Williams, A. Hillier, R. S. Kline, M. Ashe, S. A. Grier, D. Backman, and W. J. McCarthy. 2009. A cross-sectional prevalence study of ethnically targeted and general audience outdoor obesity-related advertising. The Milbank Quarterly 87(1).
Zenk, S. N., and L. M. Powell. 2008. US secondary schools and food outlets. Health and Place 14(2):336-346.


















