2
Context for LGBT Health Status in the United States
The current health status of lesbian, gay, bisexual, and transgender people of all races, ethnicities, ages, and social backgrounds can be understood only in cultural and historical context. To provide this context, this chapter reviews basic definitions and concepts concerning gender identity, gender expression, and sexual orientation; summarizes key historical events that have shaped contemporary LGBT culture and communities; describes the demography of LGBT people in the United States; and examines barriers to accessing health care for LGBT people. The chapter then presents a discussion of the case of HIV/AIDS as it relates to several important themes of this report. The final section summarizes key findings and research opportunities.
DEFINING GENDER IDENTITY, GENDER EXPRESSION, AND SEXUAL ORIENTATION
To discuss the context surrounding the health of LGBT populations, the committee has adopted working definitions for a number of key terms. Sex is understood here as a biological construct, referring to the genetic, hormonal, anatomical, and physiological characteristics on whose basis one is labeled at birth as either male or female. Gender, on the other hand, denotes the cultural meanings of patterns of behavior, experience, and personality that are labeled masculine or feminine.
Gender Identity and Expression
Gender identity refers to a person’s basic sense of being a man or boy, a woman or girl, or another gender (e.g., transgender, bigender, or gender
queer—a rejection of the traditional binary classification of gender). Gender identity can be congruent or incongruent with one’s sex assigned at birth based on the appearance of the external genitalia. Gender expression denotes the manifestation of characteristics in one’s personality, appearance, and behavior that are culturally defined as masculine or feminine. Gender role conformity refers to the extent to which an individual’s gender expression adheres to the cultural norms prescribed for people of his or her sex.
Gender dysphoria refers to a discomfort with one’s sex assigned at birth (Fisk, 1974). This dysphoria can manifest itself in a persistent unease with one’s primary and secondary sex characteristics, a sense of inappropriateness in one’s gender role, and a strong and persistent identification with and desire to live in the role of the other sex, which has been classified as gender identity disorder in the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV) (American Psychiatric Association, 2000).
The term transgender has come to be widely used to refer to a diverse group of individuals who cross or transcend culturally defined categories of gender (Bockting, 1999); that is, they depart significantly from traditional gender norms. This group includes transsexuals (who desire or have had hormone therapy and/or surgery to feminize or masculinize their body and may live full time in the cross-gender role); cross-dressers or transvestites (who wear clothes and adopt a presentation associated with the other gender for emotional or sexual gratification, and may live part time in the cross-gender role); transgenderists (who live full time in the cross-gender role, may take hormones, but do not desire surgery); bigender persons (who identify as both man and woman, may take hormones, and may live part time in the cross-gender role); drag queens and kings (who dress in clothes associated with the other gender, adopt a hyperfeminine or hypermasculine presentation, and appear part time in the cross-gender role); and other identities, such as gender queer or two-spirit—a term used by some Native Americans for individuals who possess feminine and masculine qualities (who may or may not desire hormones or surgery, and may or may not live part or full time in the cross-gender role). Definitions of these categories vary and continue to evolve over time. The term transgender is increasingly used to encompass this family of gender-variant identities and expressions, but opinions on the term vary by geographic region and by individual. For example, some transsexual women differentiate themselves from those who self-identify as transgender to underscore that they are not gender variant or nonconforming, but instead identify unambiguously with the other gender. As explained in the previous chapter, a person whose gender identity differs from a male sex assignment at birth is often referred to as a male-to-female transgender woman. A person whose gender identity differs from a female sex assignment at birth is often referred to as a female-to-male
transgender man. For research purposes, transsexuals are more often the focus of study than other transgender groups since they are more likely to seek clinical intervention, making data on this subgroup more accessible (Rosser et al., 2007).
Transgender people may be sexually oriented toward men, women, other transgender people, or any combination of these groups. There is no consensus in the research literature as to whether, when describing a transgender person’s sexual orientation, sexual orientation labels should be based on the person’s sex at birth or gender identity. However, transgender people themselves, especially those who live full time in the cross-gender role, more often than not anchor their sexual orientation on gender identity (e.g., a male-to-female transsexual woman who is attracted primarily to women is most likely to refer to herself as lesbian rather than heterosexual or straight) (Amercian Psychological Association, 2009a,b).
Sexual Orientation
The committee’s working definition of sexual orientation incorporates three core ideas. First, sexual orientation is about intimate human relationships—sexual, romantic, or both. These relationships can be actualized through behavior or can remain simply an object of desire. Second, the focus of sexual orientation is the biological sex of a person’s actual or potential relationship partners—that is, people of the same sex as the individual, people of the other sex, or people of either sex. Third, sexual orientation is about enduring patterns of experience and behavior. A single instance of sexual desire or a single sexual act generally is not regarded as defining an individual’s sexual orientation.
Based on these considerations, the committee adopted the following working definition: sexual orientation refers to an enduring pattern of or disposition to experience sexual or romantic desires for, and relationships with, people of one’s same sex, the other sex, or both sexes. As this definition makes clear, sexual orientation is inherently a relational construct. Whether a sexual act or romantic attraction is characterized as homosexual or heterosexual depends on the biological sex of the individuals involved, relative to each other. One’s sexual orientation defines the population of individuals with whom one can potentially create satisfying and fulfilling sexual or romantic relationships. Such relationships help to meet basic human needs for love, attachment, and intimacy and are, for many people, an essential aspect of the self (Herek, 2006; Peplau and Garnets, 2000).
This working definition encompasses attraction, behavior, and identity. As explained in Chapter 3, most researchers studying sexual orientation have defined it operationally in terms of one or more of these three components. Defined in terms of attraction (or desire), sexual orientation is
an enduring pattern of experiencing sexual or romantic feelings for men, women, transgender persons, or some combination of these groups. Defined in terms of behavior, sexual orientation refers to an enduring pattern of sexual or romantic activity with men, women, transgender persons, or some combination of these groups. Sexual orientation identity encompasses both personal identity and social identity. Defined in terms of personal identity, sexual orientation refers to a conception of the self based on one’s enduring pattern of sexual and romantic attractions and behaviors toward men, women, or both sexes. Defined in terms of social (or collective) identity, it refers to a sense of membership in a social group based on a shared sexual orientation and a linkage of one’s self-esteem to that group.
Although sexual attractions and behaviors are generally understood as ranging along a continuum from exclusively heterosexual to exclusively homosexual (Kinsey et al., 1948, 1953), sexual orientation is often discussed according to three main categories, especially when it is defined in terms of identity: (1) heterosexuality (for individuals who identify as, for example, “straight” or whose sexual or romantic attractions and behaviors focus exclusively or mainly on members of the other sex); (2) homosexuality (for individuals who identify as, for example, “gay,” “lesbian,” or “homosexual” or whose attractions and behaviors focus exclusively or mainly on members of the same sex); and (3) bisexuality (for individuals who identify as, for example, “bisexual” or whose sexual or romantic attractions and behaviors are directed at members of both sexes to a significant degree). Which of these categories is used in a particular study or health intervention will depend on the research or treatment goals. Individuals may also have a specific attraction toward transgender persons (Coan et al., 2005; Operario et al., 2008; Weinberg and Williams, 2010).
Some research suggests that within the subgroup of individuals identifying as bisexual, there exists considerable variability in self-identified orientation and identity groups. While some bisexual individuals exhibit approximately equal attraction to males and females, others exhibit varying levels of preference for one sex or another (Herek et al., 2010). Similarly, bisexual individuals may exhibit differing degrees of heterosexual, homosexual, or bisexual identity, identifying with all groups equally or more strongly with one than the others (Weinrich and Klein, 2002; Worthington and Reynolds, 2009).
Individuals vary in the extent to which their behavioral history and patterns of sexual attraction fit neatly within one of the three main sexual orientation categories. As explained in Chapter 3, most adults exhibit consistency across the three categories (e.g., they are exclusively heterosexual or homosexual in their attractions, sexual behavior, and self-labeled identity), but some do not. Moreover, the ways in which people use identity labels—such as gay and bisexual—often vary among cultural, racial, ethnic,
socioeconomic, and age groups. They may also vary from one situation to another and change over time.
In addition, new labels and identities emerge over time in conjunction with societal changes. Since the 1960s, for example, “gay” has become a more widely used identity label than terms such as “homosexual” and “homophile.” More recently, some individuals have adopted the term “queer”—long a derogatory epithet used for gay, lesbian, and bisexual individuals—as a positive self-label. In addition, adolescents and young adults have coined a variety of alternative labels, such as “boi-dyke” and “omnisexual.” Nevertheless, the labels “gay,” “lesbian,” and “bisexual” remain widely used by both adolescents (Russell et al., 2009) and adults (Herek et al., 2010).
Variations in Sexual Orientation
Empirical research shows that men and women overlap considerably in their experiences of sexual desire and behavior. In some aspects of sexuality, however, the experiences of men and women may be more likely to differ, and these areas may have implications for health. Three examples are highlighted here.
First, on average, men tend to show greater interest in sex and express a desire to engage in sex more frequently than women; these patterns appear to occur in both heterosexual and homosexual populations (for a review, see Baumeister et al., 2001). In self-reports, for example, the frequency of solitary masturbation, which is a useful indicator of sexual interest insofar as it is not constrained by the availability of a partner, is generally higher among men than women (Oliver and Hyde, 1993), and this pattern appears among nonheterosexual as well as heterosexual individuals (Laumann et al., 1994a,b).
Second, on average, sexual-minority men and women may differ in their early experiences of their sexuality. Overall, lesbians appear to display greater variability than gay men in the age at which they recall reaching various developmental “milestones,” such as awareness of same-sex attractions, experience of same-sex fantasies, and first pursuit of same-sex sexual contact (for a review, see Diamond, 2008). Data from a 2005 national probability sample reveal that gay men (n = 241) recalled recognizing their homosexual orientation at a significantly earlier average age than lesbians (n = 152) or bisexual women (n = 159), while the average age for bisexual men (n = 110) was between that of women and gay men (Herek et al., 2010).
Third, compared with that of men, women’s sexuality may be more likely to be shaped and altered by cultural, social, and situational influences over time (Baumeister, 2000). As a group, women may exhibit greater
fluidity in their sexuality than men; that is, they may be more likely to experience changes over the life span in their patterns of sexual attraction. As Diamond (2008, p. 3) notes, “This flexibility makes it possible for some women to experience desires for either men or women under certain circumstances, regardless of their overall sexual orientation … women of all orientations may experience variation in their erotic and affectional feelings as they encounter different situations, relationships, and life stages.”
These examples of gender-linked patterns suggest that, on average, men and women may experience some aspects of their sexuality differently. As noted above, however, the sexes overlap considerably on these dimensions.
The extent to which patterns of same-sex sexual behavior differ across racial and ethnic groups is not clear. Using data from the General Social Survey, Turner and colleagues (2005) found that different racial groups did not differ in the extent to which they reported having engaged in same-sex sexual activity since age 18. Using data from the 2002 National Survey of Family Growth, however, Jeffries (2009) found that non-Mexican Latino men were significantly more likely than non-Latino white men to ever have had anal sex with a male partner and were significantly more likely than non-Latino black men to have had oral sex with a male partner. These relationships remained significant after controlling for age, education, and foreign birth. Chae and Ayala (2010) examined data from the National Latino and Asian American study, a national probability household sample of Latino and Asian adults over 18 years of age residing in the United States (n = 2,095 Asian and 2,554 Latino respondents, including 101 Asians and 111 Latinos reporting same-sex behavior during the previous 12 months). They found that 6.2 percent of Asian respondents reported any same-sex behavior during the previous 12 months, compared with 3.9 percent of Latino respondents. Because the authors reported no confidence intervals, however, comparison across the groups is difficult.
As highlighted by the concept of intersectionality, the experience of being a sexual minority is influenced by an individual’s other identities. Thus, the experience of being lesbian, gay, or bisexual appears to vary according to the racial or ethnic group with which one identifies. Chae and Ayala (2010) compared Latino and Asian American respondents who were “LGB-identified” (i.e., self-labeled as homosexual, lesbian, gay, or bisexual) and “non-LGB-identified” (i.e., reporting same-sex behavior during the previous year but not self-labeling as homosexual, lesbian, gay, or bisexual). They found considerable heterogeneity between Asian and Latino respondents, with most participants identified as sexual minorities within the sample not self-identifying as LGB. Furthermore, they found an association between identifying as a sexual minority and psychological distress. There were variations within the two ethnic groups, with participants of
Chinese ancestry more likely than members of other Asian ethnic groups to identify as LGB, and participants of Mexican ancestry less likely than other Latino respondents to identify as LGB. In addition, socioeconomic status was associated with LGB identification: LGB-identified respondents of Asian ancestry were more likely to be employed than their non-LGB-identified counterparts, and non-LGB-identified Latinos had lower levels of education than LGB-identified Latinos (Chae and Ayala, 2010). Another study, conducted in Houston, Texas, with a nonprobability sample of 1,494 black, Latino, Asian, and white men and women, found that concordance rates between sexual behavior and identity varied across racial and ethnic groups (Ross et al., 2003).
Other data indicate that black men who have sex with men are less likely than white men who have sex with men to self-identify as gay (Chu et al., 1992; Doll et al., 1992; Goldbaum et al., 1998; Kramer et al., 1980; McKirnan et al., 1995, 2001; Montgomery et al., 2003; O’Leary et al., 2007; Torian et al., 2002) and are more likely to engage in sexual behavior with both males and females (Flores et al., 2009). Among adults who self-identify as lesbian, gay, or bisexual, self-identified bisexual men appear to be more likely than others to be black or Latino. A 2005 survey with a national probability sample of self-identified lesbian, gay, and bisexual adults found that only 43 percent of the bisexual men were non-Latino white, compared with more than 70 percent of the gay men, lesbians, and bisexual women. Whereas the racial and ethnic characteristics of the lesbian subsample generally corresponded to those of the U.S. adult population, the proportion of non-Latino whites was higher among self-labeled bisexual women than in the national population (Herek et al., 2010).
Consistent with this pattern, black lesbian, gay, and bisexual adults appear to be less likely than those of other races to disclose their sexual orientation in the workplace (Herek et al., 2010). Black men who have sex with men are less likely than other men who have sex with men to join gay-related organizations (Kennamer et al., 2000; Stokes and McKirnan, 1996). Black men who have sex with men also appear less likely than their counterparts of other races to disclose their same-sex behavior or sexual orientation identity to others (CDC, 2003; Kennamer et al., 2000; McKirnan et al., 1995; Stokes and McKirnan, 1996). Another study found that as education increased, white men who have sex with men were more likely to disclose their sexual identity, but black men who have sex with men were substantially less likely to do so (Kennamer et al., 2000). Research with black lesbian and bisexual women suggests that disclosure of sexual orientation varies according to several factors, including whether one’s sexual orientation identity is considered more important than one’s racial identity (Bowleg et al., 2008). In a convenience sample of New York City youths recruited from community organizations and local colleges
(n = 156 youths aged 14–21), black participants reported less disclosure of their identity than white participants (Rosario et al., 1996).
A study examining gender identity affirmation among 571 male-to-female transgender persons focused on gender disclosure in six relationships—with parents, siblings, friends, fellow students, work colleagues, and sexual partners. The authors found that, compared with non-Latino whites, nonwhites had fewer relationships in which they were able to disclose their transgender identity, yet in the relationships available to them, they were more likely to disclose and to receive affirmation of their transgender identity (Nuttbrock et al., 2009).
HISTORICAL PERSPECTIVE
Contemporary health disparities based on sexual orientation and gender identity are rooted in and reflect the historical stigmatization of LGBT people. Most LGBT people encounter stigma from an early age, and this experience shapes how they perceive and interact with all aspects of society, including health-related institutions. Likewise, heterosexual people (including many health care professionals) have been socialized in a society that stigmatizes sexual and gender minorities, and this context inevitably affects their knowledge and perceptions of LGBT people. And institutions and systems that affect the health of LGBT people have evolved within a society that has historically stigmatized those populations, and this has important implications for their ability to address the needs of sexual and gender minorities.
Although an extensive discussion of the history of LGBT populations is beyond the scope of this report, this section highlights some key historical themes relevant to the current health status of LGBT individuals. Specifically, this section describes how LGBT individuals have been marginalized through the law and through psychiatric diagnoses, how they have been affected by the AIDS epidemic, and how their current legal status has evolved. In addition, this section notes some ways in which LGBT individuals’ responses to their differential treatment and stigmatized status have implications for their health. Insofar as contemporary notions of sexual orientation and gender identity have their origins in the beginning of the twentieth century, this historical review focuses mainly on the past 100 years.
Lesbian, Gay, and Bisexual History
Inversion, Homosexuality, and the Origins of Contemporary Notions of Sexual Orientation
Although heterosexual and homosexual behaviors and attractions are ubiquitous across human societies, the idea that individuals can be mean-
ingfully defined or categorized in terms of their patterns of sexual attraction and behavior emerged in science and medicine only in the nineteenth century. When this discourse emerged, its initial focus was on individuals who were perceived as deviating from cultural definitions of gender and sexual “normalcy.”
The category of “the sexual invert” historically preceded that of “the homosexual” as a target for medical and scientific scrutiny. During the 1860s, Ulrichs proposed that male inverts, or “Urnings,” should be understood as “individuals who are born with the sexual drive of women and who have male bodies” (Ulrichs, 1994b, vol. 1, p. 35). Hirschfeld supported this argument and later posited that inverts represented an intermediate sex, reflecting both male and female qualities (Hirschfeld, 2000). Sexual inversion originally described the individual in totality, with sexual conduct being only one of various aspects (Chauncey, 1982–1983). Male inverts were believed to possess “feminine” qualities, including passivity, weakness, and sexual attraction to “masculine” males. Female inverts were believed to manifest “masculine” qualities, including an active interest in sexuality—an abnormal quality in the eyes of a society that believed femininity was inherently passive (Chauncey, 1982–1983).
The modern notion of sexual orientation—defined in terms of whether one’s sexual attractions and interest are directed toward men or women—is usually traced to Sigmund Freud (Freud, 1953). He introduced a distinction between the sexual aim (i.e., preferences for particular types of sexual activity) and the object toward which that aim is directed. Freud’s theory and clinical practice focused on the sexual object, with “homosexuals” and “heterosexuals” being understood entirely in terms of their sexual object (respectively, a person of the same or the other sex). The construct of “the invert,” which focused on the individual’s sexual aim (passive sexuality among male inverts, active sexuality among females), fell into disuse (Chauncey, 1982–1983; Freud, 1953). However, the modern construct of “transgender” has similarities to the notion of sexual inversion insofar as both involve crossing socially defined boundaries of gender.1
Homosexual Conduct as a Crime, Homosexuality as a Diagnosis
Throughout much of the twentieth century, consensual same-sex sexual behavior was illegal, and homosexuality was considered a form of mental illness. This dual stigma historically attached to homosexual behaviors and persons has, as noted earlier, shaped the experiences of many people living today and has influenced many contemporary institutions that affect health.
Long before Freud articulated his theory of sexuality, theological doctrine and secular law sought to regulate sexual behaviors and attached punishments to a variety of sex acts that were nonprocreative or occurred outside of marriage. Proscribed sexual behaviors were often referred to collectively as sodomy, a term that was not clearly defined in most religious and legal texts but included homosexual behavior as well as other nonprocreative and extramarital sexual acts (Jordan, 1997). U.S. sodomy laws, which existed in all of the states until 1961, when Illinois eliminated its statute, were the legacy of these prohibitions. Their language varied from state to state, and they outlawed various types of sexual behavior, including some forms of homosexual behavior. The main effect of sodomy laws was not prosecution for homosexual acts—such prosecutions were relatively infrequent. However, the laws were regularly used to justify differential treatment of sexual minorities in a variety of arenas, including employment, child custody, and immigration (Leslie, 2000).
The expansion of discourse about sexuality from the domains of law and theology into medicine, psychiatry, and psychology was considered a sign of progress by many at the time because it offered the hope of treatment and cure (rather than punishment) for phenomena that society generally regarded as problematic. Nevertheless, after Freud, the division of people into “heterosexuals” and “homosexuals” involved stigmatization of the latter. Many early physicians and sexologists regarded homosexuality as a pathology, in contrast to “normal” heterosexuality (e.g., Krafft-Ebing, 1900), although this view was not unanimous (e.g., Ellis, 1901; Ulrichs, 1994a). Freud himself believed that homosexuality represented a less than optimal outcome for psychosexual development, but did not believe it should be classified as an illness (Freud, 1951). In the 1940s, however, American psychoanalysts broke with Freud, and the view that homosexuality was an illness soon became the dominant position in American psychoanalysis and psychiatry (Bayer, 1987).
Thus by the beginning of World War II, sodomy laws continued to criminalize same-sex sexual behavior, even when it occurred in a private setting between consenting adults, while psychiatry and psychology generally regarded homosexuality as an illness. Around this time, the illness model became part of government personnel policies when the U.S. military incorporated psychiatric screening into its induction process and developed formal procedures for rejecting homosexual recruits. Whereas same-sex sexual behavior previously had been classified as a criminal offense under military regulations prohibiting sodomy, the armed services now sought to bar homosexual persons from their ranks (Berube, 1990). However, the screening process was often superficial, especially during the early years of the war when troops were desperately needed. Indeed, many lesbians and gay men served successfully in the military, often with the knowledge
of their heterosexual comrades (e.g., Berube, 1990; Black et al., 2000; Menninger, 1948).
When the need for recruits diminished during the war’s waning years, however, policies prohibiting homosexual personnel were more vigorously enforced, and many gay men and lesbians received undesirable discharges as sexual psychopaths (Berube, 1990). Such discharges had severely negative consequences. Denied benefits under the GI Bill of Rights and socially ostracized in civilian life, gay and lesbian veterans with undesirable discharges often could not secure employment. As Berube (1990, p. 229) notes, “Sometimes their lives became so unbearable as exposed homosexuals that they had to leave home or tried to kill themselves.”
Ironically, the mass courts martial and discharges may have contributed to the development of modern lesbian and gay communities in U.S. urban centers. D’Emilio (1983) observed that, rather than returning to their hometowns after the war, many men and women chose to settle in major port cities and centers of war industry, such as Los Angeles, San Francisco, and New York. Still others later migrated to these cities to join the growing communities. Thus, large gay communities began to emerge in many American cities after World War II ended.
Although gay and lesbian civilians often found some degree of tolerance in the relative anonymity of these large cities, they nevertheless experienced negative consequences related to stigma. Because of the criminalization of homosexual acts and the stigmatization of homosexual identity, local police generally had the freedom to harass and pursue gay men and lesbians at will. Sexual minorities risked arrest when they gathered, even in private homes. Gay bars provided a venue for gay men and lesbians to socialize openly, but they also served as targets for harassment. Police raids were common, with bar patrons routinely being charged with offenses such as disorderly conduct, vagrancy, public lewdness, and solicitation (Boyd, 2003; Johnson, 2004). At the national level, a U.S. Senate committee issued a 1950 report concluding that homosexuals were not qualified for federal employment and that they represented a security risk because they could be blackmailed about their sexuality (Subcommittee on Investigations of the Senate Committee on Expenditures in the Executive Departments, 1950). In response to this report, President Eisenhower issued an executive order dismissing all homosexuals from federal employment, both civilian and military. Reporting on the government’s campaigns against gay, lesbian, and bisexual employees by daily newspapers across the country reinforced the anxiety experienced by sexual minorities (D’Emilio, 1983).
In 1952, the newly created DSM listed homosexuality as a sociopathic personality disturbance, along with substance abuse and sexual disorders (American Psychiatric Association, 1952; Bayer, 1987). This classification of homosexuality was used as the basis for laws and regulations that denied
homosexuals employment or prohibited them from being licensed in many occupations. Thousands lost their jobs (D’Emilio, 1983). Many states also passed sexual psychopath laws that applied to homosexuals as well as rapists, pedophiles, and sadomasochists. In an effort to prevent sex crimes, some psychiatrists encouraged the state to confine sexual nonconformists, including homosexuals, until they were declared “cured” (Chauncey, 1993).
During this time, many psychiatrists and psychologists attempted various “cures” (i.e., attempts to change homosexuals into heterosexuals), including psychotherapy, hormone treatments, aversive conditioning with nausea-inducing drugs, lobotomy, electroshock, and castration (e.g., American Psychological Association, 2009b; Feldman, 1966; Katz, 1976; Max, 1935; Thompson, 1949). These methods proved to be largely unsuccessful (American Psychological Association, 2009b; Friedman and Downey, 1998; Haldeman, 1994).
In summary, lesbians and gay men faced extensive stigma during the World War II era and the years immediately following. Although many of them served in the military during the war, substantial numbers were dishonorably discharged as the war concluded. Public disclosure of one’s sexual orientation could lead not only to personal rejection and ostracism, but also to unemployment and even arrest, fostering a need for considerable secrecy in one’s daily life. Gay men and lesbians were officially classified as mentally ill. Many were pressured to seek psychiatric treatment to become heterosexual, although interventions purporting to change sexual orientation were generally ineffective. At the same time, emerging gay and lesbian communities and enclaves in large urban centers offered their members the opportunity to meet others who shared their sexual orientation. These communities provided a basis for the development of organizational and individual challenges to the stigmatized status of homosexuality.
Creating Community and Change
In the post–World War II era, most gay men and lesbians accepted their stigmatized status as inevitable. However, some organized politically, forming groups that began quietly to endeavor to change societal attitudes and laws while also serving as safe havens for their members. Homophile organizations, such as the Mattachine Society and the Daughters of Bilitis, were, of necessity, highly secret groups whose initial goal was to provide social support and assistance. By the early 1960s, however, some of their members began to advocate for a strategy of publicly confronting anti-homosexual discrimination.
Meanwhile, some scientific research challenged the illness model. In 1948 and 1953, Alfred Kinsey and his colleagues published their ground-
breaking reports on human sexual behavior (Kinsey et al., 1948, 1953), demonstrating that same-sex attraction and behavior were common among American adults. Also around this time, Ford and Beach (1951) published an extensive review of cross-cultural and cross-species studies of sexual behavior, concluding that same-sex sexual behavior occurs in many animal species and that homosexual behavior of some sort was considered normal and socially acceptable in a majority of the societies for which detailed ethnographic data were available (Ford and Beach, 1951).
In a landmark study funded by the National Institute of Mental Health, psychologist Evelyn Hooker directly tested the assumption underlying ho-mosexuality’s inclusion in the DSM, namely, that homosexuality was inherently linked with psychopathology. Based on her data, Hooker (1957) concluded that homosexuality is not inherently associated with psychopathology and is not a clinical entity, a conclusion that received extensive support in subsequent empirical research (e.g., Gonsiorek, 1991) and eventually became the consensus view of mainstream mental health professionals in the United States (see below). The scholarship of Kinsey, Ford and Beach, and Hooker challenged widespread assumptions that homosexuality was a rare and pathological form of sexuality, practiced only by a small number of social misfits.
By the 1960s, homophile activists had begun to challenge publicly the idea that homosexuality was an illness and to seek an end to job discrimination and harassment. The Mattachine Society of Washington, DC, for example, began working to change Civil Service Commission policies regarding the employment of sexual minorities. In 1965, the group organized small demonstrations at locations such as the White House to protest discrimination against homosexuals in government employment (D’Emilio, 1983). And in 1966, the Washington Mattachine Society passed a resolution stating that “in the absence of valid evidence to the contrary, homosexuality is not a sickness, disturbance, or other pathology in any sense, but is merely a preference, orientation, or propensity, on par with, and not different in kind from, heterosexuality” (D’Emilio, 1983, p. 164). Although the homophile movement achieved some small success in its attempts to ensure civil rights for homosexual persons, its membership remained small until the end of the 1960s.
A watershed event occurred on June 27, 1969, in response to a routine police raid on the Stonewall Inn, a New York City gay bar. Such raids were a common occurrence, and police typically encountered little resistance. That night, however, the Stonewall patrons, along with neighborhood residents and passersby, resisted the police in a confrontation that escalated into a riot that continued for several nights. The Stonewall Rebellion, as it is now called, is widely considered to have marked the beginning of the contemporary movement for sexual-minority civil rights. In the wake of
Stonewall, the movement grew rapidly and inspired many sectors of society to reevaluate long-standing assumptions about homosexuality (Adam, 1995). Many lesbians and gay men “came out”—that is, they publicly revealed their sexual orientation—in the professions, academia, churches, and the military.
In the face of rapidly changing cultural views about homosexuality, and recognizing that empirical data to support the illness model were lacking, the American Psychiatric Association’s board of directors voted in December 1973 to remove homosexuality as a diagnosis from the DSM (Bayer, 1987; Minton, 2002).2 Their decision was affirmed by a subsequent vote of the Association’s membership (Bayer, 1987). In 1975, the American Psychological Association strongly endorsed the psychiatrists’ actions and urged its members to work to eradicate the stigma historically associated with a homosexual orientation (Conger, 1975).
The 1970s saw the growth of gay and lesbian communities across the United States. A wide variety of organizations, associations, businesses, and self-help groups formed. More than half of the states repealed their sodomy laws, and some municipalities passed legislation prohibiting discrimination on the basis of sexual orientation. Meanwhile, businesses and social organizations catering to a gay clientele proliferated, and lesbian and gay communities expanded significantly in major cities (Faderman, 1991; Levine, 1979). Nevertheless, gay people remained widely stigmatized. Many gay rights statutes that were passed in the early and mid-1970s were subsequently overturned by voters (Adam, 1987). By the beginning of the 1980s, candidates and organizations that opposed the gay community’s modest gains were increasingly visible in national politics.
The AIDS Epidemic
The first cases of what would come to be known as AIDS were detected in gay men in 1981 (Gottlieb et al., 1981). AIDS has since claimed the lives of a significant portion of the generations of gay and bisexual men who came of age during and after the World War II era, and has dramatically altered the LGBT community in numerous ways. A detailed history of the impact of the AIDS epidemic on sexual and gender minorities is beyond the scope of this report and has been addressed elsewhere (see, e.g., various In-
stitute of Medicine/National Research Council reports on AIDS, including IOM, 1991a,b,c, 2005; NRC, 1989, 1990, 1993, 1995; see also Epstein, 1996; Levine et al., 1997). Nor can the complete history of AIDS yet be written. HIV continues to spread throughout the world and in the United States, where newly diagnosed infections occur disproportionately among black and Latino men who have sex with men.
To better illuminate the historical context for understanding contemporary health disparities among sexual and gender minorities, this section highlights several long-term effects of AIDS. A detailed look at the AIDS epidemic is presented later in the chapter to illustrate a number of themes of particular relevance to the health of LGBT populations that pervade the discussion in the ensuing chapters.
First, AIDS was responsible for the deaths of thousands of gay and bisexual men in the United States. Apart from the individual tragedy represented by the loss of each of these lives, the cumulative loss inevitably affected the entire community. Several AIDS researchers (e.g., Levine, 1998; Martin et al., 1989) likened the epidemic to natural disasters such as floods and hurricanes, albeit without the physical destruction. Writing about AIDS, Levine (1989) noted that disasters can destroy a community’s preexisting sociocultural order and foster both collective and individual trauma among survivors. Collective trauma refers to the loss of communality, that is, the network of relationships and shared meanings that provide intimacy, support, and a sense of self and that tie individuals to the social order. Individual trauma denotes the emotional response to death and devastation, that is, feelings of shock, disorientation, guilt, emotional depletion, and numbness (Levine, 1989; see generally Erikson, 1976).
In addition to individual and collective trauma, the LGBT community faced the challenge of how to respond to AIDS in a society they perceived as already hostile to them. Many sexual- and gender-minority individuals wondered whether they would all be targeted for increased ostracism, discrimination, and stigmatization as a result of AIDS (Bayer, 1989). Mandatory testing of the members of so-called “risk groups” (especially gay and bisexual men) was widely discussed in the larger society, and many LGB individuals feared that such testing could lead to the development of government lists of sexual-minority people for subsequent quarantine and discrimination (Bayer, 1989). Concern was also widespread that state sodomy laws, many of which had been repealed during the 1960s and 1970s, would be reinstated on the pretext of preventing AIDS. This concern received additional impetus when the U.S. Supreme Court upheld the constitutionality of state sodomy laws in 1986 (American Psychological Association and APHA, 1986). One argument made for retaining sodomy laws was that they would contain the spread of AIDS, although an amicus brief filed jointly by the American Public Health Association and the American
Psychological Association rebutted this argument (American Psychological Association and APHA, 1986).
Faced with the challenge of providing care and support to its members, the LGBT community responded by organizing self-help groups and community-based organizations that offered a variety of medical, psychological, and social services to people with AIDS. It also created and maintained community-based prevention programs that disseminated information about sexual risk reduction and promoted norms that encouraged the practice of “safer sex.” Although organizations in major urban centers—including the San Francisco AIDS Foundation, AIDS Project Los Angeles, and the New York Gay Men’s Health Crisis—achieved national prominence, the organizing extended into midsized cities, towns, and rural areas as well. Funded by community donations, private foundations, and government entities, these organizations grew in size and sophistication as the epidemic wore on. They helped create the infrastructure for the provision of health and social services that currently exists in the LGBT community (NRC, 1993).
At the same time, the epidemic fostered widespread activism to speed the testing and approval of new AIDS treatments and to increase government funding for research and prevention. Frustrated by the slow pace of much AIDS-related biomedical research, LGBT activists teamed with health care workers to organize community-based research studies to test promising AIDS drugs. These efforts fostered a new model for health care in which patients and advocates played a highly active role in identifying and implementing treatment strategies (Epstein, 1996). Coalitions also were formed between community activists and public health workers to devise strategies for monitoring HIV transmission that would be sensitive to community concerns about stigma and discrimination.
AIDS probably changed public perceptions of sexual minorities. Although the epidemic was often ignored by the mass media or portrayed in sensationalist ways during its early years (Shilts, 1987), later coverage presented the lives of gay men with AIDS as multilayered. It also showed that many of these men were rejected by their biological relatives and were cared for by same-sex partners and extended gay and lesbian families (Herek, 2009c). In addition, the epidemic provided the impetus for unprecedented numbers of gay, lesbian, and bisexual people to disclose their sexual orientation to family members, friends, neighbors, coworkers, and society at large. Many men who contracted AIDS were involuntarily “outed” by the disease, but many others chose to come out in an attempt to reduce sexual stigma and prejudice. Social psychological research indicated that heterosexuals who reported knowing one or more gay men and lesbians personally were indeed more likely than others to be accepting and supportive of sexual minorities generally (e.g., Herek and Capitanio, 1996; Pettigrew and
Tropp, 2006). Thus as a result of the epidemic, many heterosexuals began to think about gay men and lesbians in ways that went beyond sexuality: as family members and friends, coworkers, contributors to society, and members of a besieged community (Herek, 2009c). These changes in perceptions of sexual minorities may have contributed to decreases in negative attitudes toward homosexuality that were observed in public opinion polls during the 1990s (e.g., Sherrill and Yang, 2000; Herek, 2009d).
Coincident with the first years of the AIDS epidemic was increased public recognition of individuals who identify as bisexual. Although bisexual people began forming social and political groups in the 1970s (Udis-Kessler, 1995; Weinberg et al., 1994), an organized bisexual community did not emerge until the 1980s (Herdt, 2001; Paul, 1983; Rust, 1995; Udis-Kessler, 1995). By the early 1990s, the inclusion of bisexual individuals in the organized gay movement was reflected in the addition of “bisexual” to the names of lesbian and gay organizations and events. It was also in the late 1980s and early 1990s that bisexuals were recognized as a group at heightened risk for HIV infection (Doll et al., 1992).
In summary, although the AIDS epidemic continues to ravage sexual-minority communities today, some of its long-term consequences are already apparent. Many HIV-positive gay and bisexual men are surviving and thriving today thanks to the development of new HIV treatments. Nevertheless, most of them require ongoing medical care and must adhere to drug regimens that are extremely expensive and often have debilitating side effects. Many uninfected gay and bisexual men, especially those who came of age before the era of AIDS, have lost life partners as well as entire networks of male friends and acquaintances. The lives of many lesbians and bisexual women similarly have been altered by extensive experiences with loss. If the epidemic had never occurred, those networks would today be a source of social and emotional support as their members continued through their life course. Yet while the epidemic had considerable impact on individual lives, it also changed the LGBT community, creating an infrastructure of organizations dedicated to meeting the health and social needs of LGBT individuals.
The Last 20 Years: Laws and Policies
During the 1990s and 2000s, the visibility of the LGBT community increased dramatically in most facets of U.S. society. The last 20 years have seen various events that have affected the lives of sexual minorities, including the U.S. Supreme Court decision in Lawrence v. Texas3 that struck down all sodomy laws. This section focuses on some of these events, as
well as trends that are particularly relevant to the health concerns of the contemporary LGBT community, with particular emphasis on the development of laws and policies that continue to shape the experience of sexual minorities today. Although the extent of legal inequalities experienced by LGBT individuals has declined during recent decades, sexual and gender minorities still enjoy overall fewer legal rights, protections, and benefits than the non-gender-variant, heterosexual population. Inequalities in the law can affect fundamental aspects of the lives of LGBT people and can directly impact their ability to access quality health care.
While federal laws and policies govern some areas of import to LGBT populations (e.g., military personnel policy, U.S. Food and Drug Administration [FDA] policy banning men who have sex with men from donating blood), many issues are determined by the laws of the individual states and, at times, those of smaller jurisdictions within the states. Because states vary in their treatment of these issues, the effects of laws and policies on LGBT individuals often depend on where they live or travel.
Criminal victimization and harassment. As noted above, sexual and gender minorities have long been subjected to violence and harassment because of their sexual orientation and gender identity. As early as the 1960s, LGBT communities began to organize to respond collectively to such attacks. By the 1980s, many community-based antiviolence organizations around the United States were conducting community patrols, documenting violent incidents, providing victim services, working with local law enforcement agencies, and organizing violence prevention programs (e.g., Herek, 1992; Wertheimer, 1992). These programs were part of an emerging national movement against hate crimes—criminal actions that are motivated in whole or in part by bias against the victim’s perceived race, religion, ethnicity, sexual orientation, or disability (Department of Justice, 2009; see generally Jenness and Grattet, 2001).
During the 1980s, some states passed laws mandating the collection of data to document the occurrence of hate crimes, including those based on the victim’s sexual orientation. In 1990, Congress passed and President George H. W. Bush signed the Hate Crimes Statistics Act, which mandated the collection of such data on a national scale by the Federal Bureau of Investigation (FBI). Throughout the 1990s and 2000s, antiviolence projects based in sexual- and gender-minority communities continued to collect data and provide related services as more states enacted hate crime laws. In addition to mandating the local collection of data on the extent of hate crimes, many states imposed sentencing enhancement (i.e., a more severe penalty than would otherwise be imposed) for such crimes. The federal Hate Crimes Sentencing Enhancement Act of 1994 directed the U.S. Sentencing Commission to provide a sentencing enhancement for hate crimes, including those
based on the victim’s sexual orientation. This law’s impact was limited because it applied only to existing federal crimes, which, in the case of sexual orientation, included only crimes committed on federal property or during the course of federally protected activities. The Matthew Shepard and James Byrd, Jr. Hate Crimes Prevention Act, enacted in 2009, expanded federal hate crime law to allow federal prosecution of crimes motivated by a victim’s sexual orientation and gender identity. It also mandated the collection of data on crimes motivated by bias against a particular gender or gender identity (FBI, 2010).
Since 1991, the FBI has recorded a substantial number of hate crimes based on sexual orientation annually (FBI, 2010). Through 2009 (the most recent year for which data were available when this report went to press), approximately 17,500 incidents based on sexual orientation had been reported to the FBI. The FBI’s hate crime reports underestimate the actual number of such incidents for several reasons, including that the reports rely on the voluntary cooperation of local law enforcement agencies, that many victims do not report the crime to the police, and that many hate crimes are not accurately classified as such (e.g., Herek and Sims, 2008). Data from the National Crime Victimization Survey, conducted annually by the U.S. Bureau of Justice Statistics with a sample of approximately 42,000 households, suggested an annual average of 210,430 hate crime victimizations in the United States in 190,840 separate incidents between July 2000 and December 2003. Hate crimes were more likely to occur in urban than in suburban or rural settings. More than 37,800 (17.9 percent) of these victimizations were motivated by the victim’s sexual orientation. Approximately 42 percent of those crimes were reported to police authorities (Harlow, 2005).
In addition to hate crimes, other long-standing forms of harassment based on sexual orientation or gender identity or expression were the focus of community organizing and government response during the 1990s and 2000s. Such harassment emerged as a special concern for LGBT youth, who can face harassment and bullying in school because of their actual or perceived sexual orientation or gender identity (see Chapter 4).
An extensive national study released in late 2008 by the Gay, Lesbian, and Straight Education Network found that 86.2 percent of public school LGBT students reported being verbally harassed because of their sexual orientation, 44.1 percent reported being physically harassed, and 22.1 percent reported being physically assaulted. In addition, 32.7 percent of the LGBT students surveyed reported missing a day of school because of feeling unsafe, compared with only 4.5 percent of a national sample of secondary school students (Kosciw et al., 2008). The nonprobability sample of students (n = 6,219, age range = 13–21 in grades 6–12) was recruited through community-based LGBT youth groups and Internet listservs and
websites. The majority of these students did not report the incidents to school officials, believing that little to no action would be taken or that the situation might even be exacerbated if reported.
Currently, federal law does not explicitly prohibit school-based harassment based on sexual orientation or gender identity or expression. A minority of states explicitly prohibit bullying and harassment in public K–12 schools on the basis of sexual orientation or gender identity (Biegel and Kuehl, 2010).
Marriage and relationships. Perhaps one of the most striking developments over the past two decades has been the prominence of debate in the United States and around the world concerning societal recognition of the family relationships of sexual- and gender-minority persons. People in same-sex couples have long sought ways to solemnize and formalize their relationship, including through legal recognition (e.g., Nardi, 1997). In the 1980s, some California municipalities enacted statutes to recognize same-sex relationships (in the form of “domestic partnerships”) and provided the same-sex partners of city employees some of the benefits granted to married heterosexual couples. Throughout the 1990s, other jurisdictions enacted similar legislation, and debate about the issue of marriage equality for same-sex couples began to emerge on a national level (for historical background, see Chauncey, 2004; Lewin, 1998; Nardi, 1997).
A 1996 Hawaii Supreme Court decision4 raised the prospect that marriage rights might eventually be granted to same-sex partners in that state. In response, Congress passed the Defense of Marriage Act (DOMA). DOMA defines marriage as a legal union between one man and one woman for the purposes of federal law, and exempts states from recognizing marriages performed in another state between two people of the same sex (Defense of Marriage Act, 1996). Most states subsequently passed their own versions of DOMA through statute or constitutional amendment (Peterson, 2004; Vestal, 2009).
In 1999, California became the first state to pass a statewide bill recognizing same-sex couples. Although that law bestowed only limited rights, subsequent legislation gave same-sex couples many of the rights of heterosexual married couples. In 2000, Vermont passed the nation’s first civil unions bill, which gave registered same-sex couples all of the same benefits and responsibilities accorded by the state to heterosexual married couples. Other states, including New Jersey, Washington, Oregon, Illinois, and Nevada, subsequently enacted legislation recognizing civil unions or domestic partnerships. Civil unions entitle couples to most of the spousal rights and obligations accorded by the state to different-sex married couples, while
the level of rights conveyed by domestic partnerships varies among states. In addition, some state and local government entities offer limited benefits for the same-sex partners of their employees (e.g., access to group health insurance plans), as do many private employers.
Late in 2003, the Massachusetts Supreme Court ordered that state to begin recognizing marriages between same-sex couples within 6 months.5 Since then, six other states and the District of Columbia have allowed same-sex couples to marry, either through legislation (Maine; New Hampshire; Vermont; Washington, DC) or as a result of a state court ruling (California, Connecticut, Iowa). However, voters passed constitutional amendments that revoked the right to marry in California and prevented the Maine statute from going into effect.
Because same-sex couples are not legally recognized in most states, and because the legal recognitions extended by a handful of states are not recognized by the federal government, same-sex couples are denied a large number of the rights and benefits associated with marriage. At the federal level, DOMA denies same-sex couples access to more than 1,138 federal rights and obligations (GAO, 2004), ranging from spousal immigration rights to the spousal exemption under federal estate tax law.6 In addition, because of DOMA, same-sex couples are ineligible for spousal or survivor benefits from social security, a federal benefit plan (Goldberg, 2009). Even in states where couples with same-sex partners can legally marry, state law cannot require employers to recognize same-sex married couples for the purposes of benefits administered under the Employee Retirement Income Security Act, which governs the health care and retirement benefit plans of many employers (Goldberg, 2009). In states that do not grant same-sex partners the right to marry or do not have civil unions or extend full recognition to domestic partnerships, same-sex couples also are denied a variety of benefits at the state level in such areas as income taxes; inheritance rights; community property; and state-funded benefit programs providing for basic needs, including health care.
The lack of recognition of marriage between two partners of the same sex has other health implications as well. A large body of research has shown that positive health outcomes are associated with marriage (Herdt and Kertzner, 2006; Herek, 2006). These positive effects are derived in part from the increased social support and relative stability associated with a legally recognized commitment (Herek, 2006). One recent study conducted with a nonprobability sample via the Internet (n = 2,677 lesbian, gay, and
bisexual adults) found that same-sex couples in legally recognized relationships experienced fewer depressive symptoms, lower levels of stress, and more meaning in their lives compared with participants in similar long-term relationships that lacked legal recognition (Riggle et al., 2010).
Denial of legal recognition of marriage between same-sex couples also has a direct impact on LGB individuals’ interactions with the health care system. In many cases, employer-sponsored health insurance is not extended to same-sex partners, affecting their access to affordable health care. In addition, LGB individuals often are unable to take medical leave from work to care for an unmarried same-sex partner to the same extent as married couples. In 2010, the U.S. Department of Labor expanded the scope of the Family and Medical Leave Act to ensure that employees would be allowed unpaid leave to care for the children of unmarried same-sex partners; however, the act still does not extend this leave to care for unmarried same-sex partners themselves. Some states have extended medical leave to unmarried same-sex partners, but most have not. LGB people also have experienced the denial of hospital visitation rights for same-sex partners and disregard for advance directives7 with respect to the care of same-sex partners. In 2010, President Obama issued a memorandum directing the U.S. Department of Health and Human Services to adopt regulations requiring all hospitals receiving Medicaid or Medicare dollars to permit visitation by a designated visitor without regard to sexual orientation or gender identity and requiring those hospitals to respect all patients’ advance directives. If a visitor is not designated or an advance directive is not in place before a patient is incapacitated, however, same-sex partners may still be disregarded in terms of visitation or medical decision making.
Transgender people also face some uncertainty concerning access to marriage. No court has issued a published decision regarding the validity of a marriage in which one of the spouses undergoes sex reassignment after the marriage has taken place, although many state agencies, many public and private employers, and several federal agencies have held that such marriages are valid.8 Few courts have ruled on the validity of a marriage in which one of the spouses undergoes sex reassignment before the marriage has taken place, although in practice, the great majority of couples in this situation do not encounter legal problems. One appellate court decision has
recognized the validity of such a marriage,9 and a number of trial courts have done so.10
Parenting and children. Before the emergence of visible gay communities in the United States, many lesbians, gay men, and bisexual people married heterosexually for a variety of reasons, including social and family pressures, a desire to avoid stigma, and a perception that such marriages were the only available route to having children. Sometimes individuals have recognized their homosexuality or bisexuality only after marrying a person of the other sex (e.g., Higgins, 2006). Many lesbian, gay, and bisexual individuals became parents through such marriages. In more recent times, many lesbian, gay, and bisexual adults have conceived and reared children while in a same-sex relationship. Other same-sex couples and sexual-minority individuals have adopted children. In a 2005 Internet survey with a national probability sample of self-identified lesbian, gay, and bisexual adults, approximately 35 percent of lesbians and 8 percent of gay men reported having at least one child, as did 67 percent of bisexual women and 36 percent of bisexual men (Herek et al., 2010). These numbers may be higher among younger sexual-minority individuals. Data from the 2002 National Survey of Family Growth (NSFG) indicate that more than 35 percent of lesbians aged 18–44 had given birth and that 16 percent of gay men in that age group had a biological or adopted child (Gates et al., 2007). Fewer sexual-minority than heterosexual individuals are parents, but there are many lesbian mothers and gay fathers in the United States today (Patterson, 2000, 2009).
Thus, many children are currently being reared by one or more sexual-minority parents. The legal status of those parents and of their children varies from state to state. For example, states differ on whether they consider a parent’s sexual orientation to be relevant to custody or visitation in divorce proceedings (Patterson, 2009). In recent years, some states have enacted laws or policies forbidding gay and lesbian individuals or couples from foster-parenting or adopting children; other states have considered laws banning same-sex couples, or all unmarried couples, from foster-parenting or adopting children (Gates et al., 2007; Joslin and Minter, 2009; Patterson, 2009). A long-standing ban on adoptions by lesbian or gay parents in Florida was overturned in 2010. As discussed in later chapters, this variability in legal status has implications for the health of sexual-minority parents and their children.
Transgender people also can face difficulty in court disputes over custody of their children. Many courts have denied or restricted custody or visitation for transgender parents, or even terminated their parental rights, solely because of their gender identity or expression. Only a few state courts have held that a parent’s transgender status is irrelevant absent evidence of harm to the child. Transgender people who have no biological or adoptive relationship to the children they are raising with a partner face even more difficulties, as they must first convince the court that a person who has raised a child without formal legal or adoptive ties is nonetheless entitled to custody or visitation (Joslin and Minter, 2009).
Transgender History
As noted above, gender and sexuality were closely linked in early conceptualizations of sexual orientation. Over the past century, many transgender people have been a part of the larger gay and lesbian community. Transgender individuals played a key role in the Stonewall Rebellion, and they were instrumental in the organization of a more active gay and lesbian community in the 1970s (Bullough and Bullough, 1993). In many ways, however, the history of the transgender community is distinct from that of the LGB community.
Throughout history, gender variance has at times been both accepted and rejected as a part of many cultures and religions. By the end of the seventeenth century in England, gender crossing (or dressing as the other sex) was considered a crime, which created a foundation for similar laws in the United States (Bullough and Bullough, 1993). Since individuals who cross-dressed were forced to keep their identity a secret, historical data on discrimination and violence toward transgender individuals are scant. However, individual accounts detail many instances of harassment, humiliation, and violence, as well as the fear of being discovered and arrested or killed for their gender variance (Feinberg, 1996).
Hormone Therapy and Genital Reconstructive Surgery
Prior to the twentieth century, the term transsexual was not used to describe individuals with a gender-variant identity. Early sexologists Magnus Hirschfeld and Havelock Ellis defined the term “transvestism,” or “eonism,” as a category distinct from homosexuality that included cross-gender identification as well as cross-dressing (Ellis, 1933; Hirschfeld, 1991). However, the notion of changing one’s sex through surgery or other means existed well before the term transsexual became commonly used. In the early twentieth century, European scientists began to experiment with “sex transformation,” first with animals and then with humans. In Germany, doctors at Magnus
Hirschfield’s Institute for Sexual Science started performing sex-change operations in the 1920s and 1930s (Meyerowitz, 2002).
It is not clear when the first complete “sex-change” operation was performed in the United States, but by the early 1920s, reports emerged of men and women who convinced physicians to perform castrations or hysterectomies as a means of changing their sex (Yawger, 1940). During the 1930s, endocrinologist Harry Benjamin became one of the first physicians in the United States to routinely administer hormone therapy to individuals desiring to change their sex (Benjamin, 1966; Drescher, 2010). During the next 20 years, a few American physicians privately performed sex reassignment surgery on nonintersex patients (Meyerowitz, 2002). However, it was not until the 1950s that the term transsexual became widely used to describe individuals who desired to change their sex.
Although he refused to endorse sex reassignment surgery for nonintersex patients, David Oliver Cauldwell coined the term transsexual in his 1949 essay “Psychopathia Transexualis” to describe individuals whose sex assigned at birth, based on the appearance of their external genitalia, did not match their gender identity (Cauldwell, 1949). Although transsexual individuals who met these criteria later gained access to sex reassignment, many psychiatrists remained critical of sex reassignment surgery as a legitimate form of treatment; they maintained that transsexual individuals were mentally disordered, and they objected to using hormones and surgery to treat these patients irreversibly (Drescher, 2010). Yet over time, understanding and acceptance grew, confirmed by a body of follow-up research (Green and Fleming, 1990; Pfäfflin and Junge, 1992). During this same period, stories of “sex changes” were publicized in sensationalist American magazines and newspapers. However, individuals seeking sex reassignment from physicians were routinely denied and informed that surgery was only for cases of intersexuality (Meyerowitz, 2002).
Much of the popular knowledge about sex reassignment surgery changed in 1952 when Christine Jorgensen, born George Jorgensen, emerged as a public figure in a front-page article of the New York Daily News (White, 1952). Jorgensen underwent sex reassignment surgery in Denmark and lived out the rest of her life as a woman. In the popular press, Jorgensen’s story was unique because she was heralded as the first nonintersex individual to undergo such surgery (Meyerowitz, 2006). Extensive coverage of Jorgensen’s transformation demonstrated to other transsexual people that sex reassignment surgery was feasible. Jorgensen’s story also led to greater awareness of a concept that would later become known as gender identity, a term coined by Robert Stoller (1968) and popularized by John Money (1985, 1994) in his attempt to explain the sexual development of intersex and transsexual individuals (Drescher, 2010). In 1966, The Johns Hopkins University announced its program to perform
and evaluate the efficacy of sex reassignment surgery, thus providing professional legitimacy for sex reassignment as a treatment for transsexualism (Meyerowitz, 2002). This was soon followed by similar programs at the University of Minnesota (Hastings, 1969; Hastings and Markland, 1978) and other university medical centers (Meyerowitz, 2002).
Psychiatric Classification
In 1979, an interdisciplinary group of physicians, therapists, and researchers created the Harry Benjamin International Gender Dysphoria Association, now known as the World Professional Association for Transgender Health (WPATH). Gender dysphoria was defined as serious discomfort with one’s gender identity or gender role, thus acknowledging a spectrum of clinical presentations for which sex reassignment could be therapeutic and broadening the narrowly defined criteria originally used in the early sex reassignment programs (Laub and Fisk, 1974). The Benjamin Association defined standards of care to ensure and legitimize access to quality sex reassignment procedures. It also defined a number of eligibility criteria, including evaluation and recommendation by a mental health professional and, for surgery, a real life experience, referring to a set period of time in which to live full time in the gender role to which one is aspiring (WPATH, 1979).
Around the same time, a formal diagnosis of gender dysphoria was introduced in DSM-III (American Psychiatric Association, 1980), further legitimizing it as a psychiatric condition and providing guidance for treatment. DSM-III included two diagnoses: gender identity disorder of childhood (GIDC) and transsexualism (referring to gender dysphoria in adolescents and adults). In the 1987 revision of DSM-III, a third diagnosis was added: gender identity disorder of adolescence and adulthood, non-transsexual type. In 1994, the fourth edition of the DSM, DSM-IV, omitted this last diagnosis and consolidated GIDC and transsexualism under the diagnosis of gender identity disorder, with different criteria for children, adolescents, and adults (Zucker and Spitzer, 2005). In the last 15 years, however, these diagnoses have become increasingly controversial in the context of a transgender movement advocating for recognition of gender diversity and the depathologizing of gender variance (Bockting and Ehrbar, 2006; Bockting et al., 2009; Knudson et al., 2010).
Emergence of the Transgender Movement
As debate over the psychiatric classification and treatment of transsexualism and gender dysphoria continued for many years in the health field, transsexual and transgender people were frequently targets of stigma and discrimination from both the public at large and the police. The increasing
number of medical centers willing to perform sex reassignment surgery raised the visibility of transsexual persons. By the 1960s, for example, the Tenderloin neighborhood in San Francisco had become a home for many gender- and sexual-variant people. With the changing dynamics of the neighborhood, tension had increased between residents and the police (Meyerowitz, 1998). In August 1966, that tension came to a head at Compton’s Cafeteria, a 24-hour establishment where young male-to-females, cross-dressers, and gay men congregated. When the police attempted to raid the cafeteria and make arrests, the customers fought back, breaking windows and carrying the fighting into the street, including setting a nearby newsstand on fire (Stryker and Van Buskirk, 1996). A watershed event like the 1969 Stonewall Rebellion, the Compton’s Cafeteria riot demonstrated an increasing collective consciousness among transsexual and transgender people. In 1969, a number of transsexual individuals in San Francisco formed the National Transsexual Counseling Unit from a number of smaller organizations (Meyerowitz, 2002).
As transsexual and transgender people fought for recognition and rights during the sexual revolution, they met with resistance from many sides. They were often excluded by gay men and lesbians from the gay liberation movement. However, they continued to advocate for their rights and equal treatment. In 1978, advocates in California successfully pushed for a state law that allowed transsexual individuals to change the name and sex designation on their birth certificate. Around this same time, the publication of Meyer and Reter’s (1979) study claiming that sex reassignment surgery did not “confer [any] objective advantage in terms of social rehabilitation” led to the closing of the Hopkins Gender Identity Clinic, and a number of other, smaller clinics followed (Meyerowitz, 2002), although many critics of Meyer’s study quickly came forward to defend the surgery (Fleming et al., 1980). A handful of university-based gender identity clinics survived, including clinics at Stanford University, the University of Texas, Case Western Reserve University, and the University of Minnesota. Their approach to care gradually changed as research and clinical experience evolved and as a generation of sex-reassigned transsexual individuals and other transgender individuals with various gender-variant identities and expressions continued to gain visibility (e.g., Kimberly, 1997; Stone, 1991; Warren, 1993).
These developments culminated in a paradigm shift away from changing sex toward facilitating a transgender coming-out process (Bockting, 1997, 2008; Bockting et al., 2009). Instead of viewing gender as binary and helping transgender and transsexual individuals conform, the transgender movement revealed a wide range of gender-variant identities and expressions, consistent with what had been documented in other cultures and throughout history (Coleman et al., 1992; Feinberg, 1996; Nanda, 1990; Roscoe, 1991; Williams, 1986). The focus of clinical management shifted
to ameliorating the negative effects of stigma associated with gender variance and assisting transgender individuals in finding a gender expression that is comfortable and consistent with their gender identity (Bockting and Ehrbar, 2006). Psychotherapy now focuses on facilitating a transgender coming-out process that no longer emphasizes “transitioning” to become a “passing” member of the “opposite” sex, but instead emphasizes affirming a unique transgender identity. Hormone therapy and surgery continue to be options for feminizing or masculinizing the body to alleviate gender dysphoria. Instead of these interventions being viewed as two steps in a linear process toward sex reassignment, however, treatment now may use either hormones or surgery, both, or neither (Bockting, 2008). While research has clearly established the efficacy of sex reassignment that includes hormone therapy and a full-time gender role change followed by genital reconstructive surgery (Murad et al., 2010), virtually no studies have evaluated the contemporary approach to treatment whereby hormone therapy is not necessarily followed by surgery, and gender identity and expression do not conform to binary conceptualizations of sex and gender.
The 1990s saw the creation of many new organizations as transgender activists began to build a community identity, often facilitated by the Internet. In addition, transgender communities established lasting coalitions with gay, lesbian, and bisexual communities to support one another in similar struggles for increased awareness, acceptance, and human rights. In 1992, Minnesota became the first state in the nation to adopt human rights and antidiscrimination legislation that included not only gay men, lesbians, and bisexual men and women but also transgender people (Minnesota Department of Human Rights, 1993). Since then, a number of states and cities have followed suit (Bockting et al., 1999). Also during the 1990s, the National Gay and Lesbian Task Force began to include transgender people in its advocacy, and WPATH revised its standards of care and included transgender community representatives in its deliberations (Levine et al., 1998; Meyerowitz, 2002). Today, the existence of gender identity disorder and its inclusion in the DSM remains controversial and is the subject of intense debate, complicated by the potential implications of further depathologization and removal of the diagnosis for access to transgender-specific health care, particularly treatment of gender dysphoria and the medical interventions of hormone therapy and surgery that continue to be medically necessary for many (Drescher, 2010).
A DEMOGRAPHIC OVERVIEW OF LGBT POPULATIONS IN THE UNITED STATES
Among the first questions typically addressed by researchers who are studying a minority population are its size and its demographic and social
characteristics. Demographic studies of LGBT populations can help make these often hidden groups of individuals visible in public policy discussions and pave the way for economic and public health studies to identify disparities (Gates and Ost, 2004a). However, it has been an ongoing challenge for researchers to collect reliable data from sufficiently large samples to assess the demographic characteristics of LGBT populations. Data from the U.S. census or large, national probability samples are usually required to examine the characteristics of a particular population. As explained in Chapter 3, few such surveys currently include data on sexual orientation and gender identity; some examples of the types of questions asked on these surveys are presented in that chapter. Even when data are derived from probability samples, racial and ethnic minorities and other subgroups of the population may not be represented in sufficient numbers to permit meaningful conclusions to be drawn about their demographic characteristics. With these caveats in mind, this section summarizes what is known from the limited available data about the demographic characteristics of LGBT populations in the United States.
Population Prevalence of Sexual Orientation Categories
Given that sexual orientation encompasses attraction, behavior, and identity and that an individual’s enduring patterns of desires and behaviors can range along a continuum, estimating the number of people in the various sexual orientation categories in the population at any given time is a complex task. Before discussing current population estimates, it is illustrative to consider some examples of earlier attempts and the limitations associated with their findings.
Early Attempts to Estimate Sexual Orientation
Perhaps the most well-known example of an attempt to describe the sexual behavior of the U.S. population is the work of Alfred Kinsey and his colleagues (1948, 1953). In their pioneering descriptive study of the sexual feelings and experiences of thousands of U.S. adults, the Kinsey researchers did not categorize research participants according to sexual orientation categories but instead reported the extent to which their sexual histories included heterosexual and homosexual desires and behavior. For example, Kinsey and colleagues (1948) reported that 37 percent of the males in their sample had had at least some overt homosexual experience to the point of orgasm between adolescence and old age, and another 13 percent had reacted erotically to other males without having overt homosexual contacts after the onset of adolescence. Generalizations from the Kinsey group’s findings to the entire U.S. population are problematic for
several reasons, including the fact that the data were not obtained from a probability sample.11 However, this research demonstrated the feasibility of studying sexuality in the general population. It also showed that human sexual behavior is highly diverse and that a large number of people acknowledged having engaged in sexual behaviors that previously had been considered rare.
Despite Kinsey and colleagues’ eschewal of sexual orientation categories, others extrapolated from their findings to estimate the proportion of the U.S. population in each of the different categories. Based on such an extrapolation (Voeller, 1990), the belief that 90 percent of the U.S. population was heterosexual and 10 percent was gay or lesbian became widely accepted during the early years of the U.S. gay rights movement. Data were lacking, however, with which to gauge the accuracy of this estimate.
Recent Estimates
As noted, while the Kinsey report was important in pioneering the study of sexuality, sampling limitations make the generalizability of its findings uncertain. However, credible estimates of the size of different sexual orientation groups can be derived from the National Health and Social Life Survey (NHSLS), which was conducted by researchers at the National Opinion Research Center (NORC) at the University of Chicago in 1992. The NHSLS is widely regarded as the most authoritative national survey to date of adult sexuality in the United States. It included assessment of the number of people by sexual attraction, behavior, and sexual orientation identity in a large probability sample (n = 3,432) of U.S. adults.12 As detailed in Chapter 3, sexual desire was assessed by asking respondents about who they were “sexually attracted to” (men, mostly men, both women and men, mostly women, only women). A separate question also asked about the appeal of having sex with someone of the same sex. Sexual behavior was assessed with questions about the respondents’ sexual acts with males and with females during three time periods (the past 30 days, the past 12 months, and since adolescence). Identity was assessed by asking respondents whether they thought of themselves as heterosexual, homosexual, bisexual, or something else.
Among the NHSLS respondents, approximately 90 percent of men and 92 percent of women reported exclusively heterosexual attraction, behavior,
TABLE 2-1 Estimated Percentage of People by Sexual Orientation and Behavior from Selected Sample Surveys
and identity. About 2.8 percent of the men and 1.4 percent of the women labeled themselves homosexual or bisexual and reported same-sex desire.13 Others reported having had same-sex partners or some degree of same-sex desire, attraction, or appeal (Laumann et al., 1994a). As shown in Table 2-1, approximately 4 percent of women and 7 percent of men reported having same-sex partners at some point since puberty. More than 7 percent of both men and women reported same-sex desire, attraction, or appeal.
Because the absolute number of both men and women reporting any nonheterosexual attraction, behavior, or identity was quite small (143 men, 150 women), the margin of error associated with these estimates is fairly
large, and any generalizations to the national population must be made with caution (Laumann et al., 1994a).
More recent data from the 2002 NSFG, conducted by the Centers for Disease Control and Prevention’s National Center for Health Statistics, also provide estimates for sexual orientation identification, same-sex sexual behaviors, and same-sex attraction. These estimates are for a more recent and younger cohort (aged 18–44) than those from the NHSLS. In the NSFG, sexual orientation identification was assessed with the question: “Do you think of yourself as heterosexual, homosexual, bisexual, or something else?” Among men aged 18–44, 90.2 percent identified as heterosexual, 2.3 percent as homosexual, 1.8 percent as bisexual, and 3.9 percent as something else; 1.8 percent did not report their orientation. Among women in this age range, 90.3 percent identified as heterosexual, 1.3 percent as homosexual, 2.8 percent as bisexual, and 3.8 percent as something else; again, 1.8 percent did not report their orientation. In terms of behavior, 6.2 percent of men reported same-sex oral or anal sexual behavior, while 11.5 percent of women reported a “sexual experience” with another woman. As Mosher and colleagues (2005) point out, this relatively high number of women may be due to the broad wording used for the question. As for attraction, 7.1 percent of men and 13.4 percent of women acknowledged some degree of same-sex attraction.
Two more recent surveys based on national probability samples provide estimates of LGB identification. Gates (2010) reports that in the 2008 General Social Survey (GSS), a survey with a national probability sample conducted by NORC, 2.2 percent of men identified as gay and 0.7 percent as bisexual, while 2.7 percent of women identified as lesbian and 1.9 percent as bisexual (n = 1,773 for the sexual orientation questions). As in the NHSLS and NSFG, data from the GSS show that rates of same-sex sexual behavior—reported by approximately 10 percent of individuals aged 18–44—are higher than rates of LGB self-identification. Estimates of the number of people who self-identify as LGB also are found in data from the recent 2009 National Survey of Sexual Health and Behavior, collected by Knowledge Networks (Herbenick et al., 2010). As the authors describe, Knowledge Networks generates a national probability sample using random-digit dialing and address-based sampling. Internet access and the necessary hardware are provided to participants who lack them. In this sample, 6.8 percent of men and 4.5 percent of women self-identified as lesbian, gay, or bisexual.
Differences in the rates reported in Table 2-1 are no doubt due in part to the time periods during which the surveys were administered. Differences are also likely to have resulted from age differences across the samples, as younger cohorts are more likely than older adults to report LGB identification and same-sex sexual behavior. Differences across studies may result as
well from variation in the survey instruments used, mode of administration, and methods used to draw the samples. Finally, as discussed above with respect to the NHSLS, there is substantial sampling variation, as the estimates are based on relatively small samples. Consequently, the margin of error associated with each estimate is likely to be fairly large.
Data from these and other national probability samples, as well as U.S. census data, reveal other demographic characteristics of LGBT populations. It should be noted that, because of data limitations, most of the demographic characteristics reported here refer only to gay men and lesbians; demographic information on bisexual and transgender individuals are extremely limited.
Size of the Transgender Population
Data on the proportion of transgender people in the U.S. population are sorely lacking. Rough estimates are available based on parental reports for children and the number of adults seeking hormone therapy or surgery at specialty clinics for the treatment of gender dysphoria. Based on ratings on the Child Behavior Check List (a parental report checklist used to measure behavior problems in children) for non-clinic-referred children (n = 398 boys and 398 girls) 1 percent of boys and 3.5 percent of girls reported “wishes to be of opposite sex” (Zucker et al., 1997). However, it should be noted that boys are referred more often than girls, reflecting, perhaps, greater societal intolerance of gender role nonconformity among boys than among girls (Zucker and Lawrence, 2009). With respect to adults, based on the number of transsexual adults at specialty clinics around the world for treatment of gender dysphoria, the estimated size of the population ranges from 1:2,900 (in Singapore) to 1:100,000 (in the United States) for transsexual women and 1:8,300 (in Singapore) to 1:400,000 (in the United States) for transsexual men. While the estimates for the United States are based on older data (Pauly, 1968), they are included here because they are the only data available from the United States. However, the number of adults seeking treatment appears to be increasing, and the ratio of transgender women to transgender men appears to be decreasing (Zucker and Lawrence, 2009).
Geographic Distribution
Lesbian and gay individuals can be found throughout the United States, being present in 99 percent of all U.S. counties (Gates and Ost, 2004b). U.S. census data on same-sex couples have been the most widely used in studying the geographic distribution of the lesbian and gay populations because the census is the largest and most geographically diverse data source available. As noted in Chapter 3, however, the data are limited in important
respects, including the fact that they exclude LGBT individuals who are not cohabiting with a same-sex partner.
While lesbian and gay populations exist throughout the United States, their distribution is not uniform across all regions. Midwestern states appear to have a disproportionately small concentration of lesbian and gay individuals (Herek et al., 2010). Vermont, California, Washington, Massachusetts, and Oregon are the states with the highest percentage of gay and lesbian inhabitants (Gates and Ost, 2004b). Large metropolitan areas tend to have relatively high concentrations of these populations, among the highest being in San Francisco; Washington, DC; and Atlanta (Black et al., 2000). Moreover, many neighborhoods and communities have proportions of gay and lesbian residents that far exceed the national average. In addition, the gay and lesbian populations themselves differ in their patterns of location. The states with the highest concentration of same-sex male and same-sex female couples differ. Additionally, a larger proportion of gay male than lesbian couples tend to live in urban areas (Gates and Ost, 2004b).
In a study comparing transgender people recruited through online convenience sampling (n = 1,229) with existing U.S. census data, Rosser and colleagues (2007) found that respondents exhibited a wide geographic distribution across the United States. While the proportion of participants from the 15 most populous states generally mirrored the relative population size, some states (Colorado, Minnesota, Missouri, and Oregon) were overrepresented relative to the population size.
Household Composition
Several data sources yield estimates of the proportion of gay men and lesbians in same-sex relationships and the proportions cohabiting. Using data from the NHSLS, Black and colleagues (2000) found that, depending on whether sexual orientation was defined in terms of exclusively same-sex sexual behavior during the previous year or self-labeled identity, between 18.5 percent and 28.6 percent of gay men were partnered at the time they were surveyed; partnership rates among women during the same period were 41.6–43.8 percent. The study also found that 67.9 percent of behaviorally defined gay men and 93.8 percent of behaviorally defined lesbians had lived with a same-sex partner at some point in their lives (Black et al., 2000). However, as with other estimates discussed above, a large margin of error is associated with these estimates because they are based on small numbers of respondents (e.g., just 28 men and 16 women fit the criterion of exclusively same-sex sexual behavior during the previous year). In a more recent survey with a national probability sample, Herek and colleagues (2010) found that approximately 40 percent of self-identified gay men
(n = 241) and 75 percent of lesbians (n = 152) reported they were currently in a same-sex relationship. Approximately one-fourth of the coupled men and four-fifths of the coupled women reported being in a legally recognized relationship (e.g., marriage, civil union) or living with their partner. Recent analysis of data from California by Carpenter and Gates (2008) indicates that 37–46 percent of gay men and 51–62 percent of lesbian women aged 18–59 are in cohabiting partnerships. Finally, the 2000 U.S. census yields an estimate of the absolute number of cohabiting sexual minorities: nearly 1,200,000 individuals indicated that they were cohabiting in same-sex relationships. Recent numbers from the American Community Survey indicate that this number is growing more rapidly than the overall U.S. population (Gates, 2006).
Some data are also available on the numbers of same-sex-couple households with children. In the 2000 census, about 27.5 percent of such households reported having children under the age of 18 (Gates and Ost, 2004b). The proportion of partnered lesbians with children in the home is significantly larger than the proportion of partnered gay males. In households with children under 18, an average of two children are present in both all households nationwide and same-sex-couple households (Gates and Ost, 2004b). Black and Latina women in same-sex couple households were more than twice as likely to be raising a child and black and Latino men in same-sex-couple households were four times more likely to be raising a child than their non-Hispanic white counterparts in same-sex couple households (Gates and Romero, 2009). U.S. census data do not yield a complete picture of gay and lesbian parenting as they do not include data on single gay or lesbian parents, and the data may be more representative of white than of nonwhite respondents, biasing comparisons. An analysis of combined GSS and NHSLS data, which include single gay men and lesbians (either self-identified or reporting that they have sex exclusively with persons of the same sex), indicated that approximately 14 percent of single gay men and 28 percent of single lesbians had children in the household (Black et al., 2000). In the 2005 survey by Herek and colleagues (published in 2010), approximately 8 percent of self-identified gay men and 35 percent of self-identified lesbians reported having one or more children, including adopted and step-children (Herek et al., 2010).
In a study comparing an online convenience sample of the U.S. transgender population (n = 1,229) with the 2000 U.S. census data, Rosser and colleagues (2007) found that transgender participants were more likely to be single, never married, or divorced and less likely to be currently married than the general population.
Income and Education
In many data sources, gay and lesbian individuals report higher average levels of education than their heterosexual counterparts. For example, Black and colleagues (2000) derived such a result from GSS and NHSLS data and for partnered individuals from the 1990 census. The authors caution, however, that this finding could be driven, at least in part, by well-educated people being disproportionately willing to identify as gay or lesbian in the GSS and NHSLS or being disproportionately likely to identify as same-sex partnered in the census.
On average, it appears that gay men have lower incomes than heterosexual men with similar education and occupations (Allegretto and Arthur, 2001; Badgett, 1995; Black et al., 2003; Carpenter, 2007). By contrast, some research has suggested that lesbian women have higher incomes than heterosexual women (e.g., Black et al., 2007), although other studies have not found this difference (e.g., Badgett, 2001; Klawitter and Flatt, 1998). Regardless, it is important to note that, because of differential treatment with respect to taxes and insurance, even lesbian or gay couples whose gross incomes are identical to those of heterosexual men and women may have less disposable income. These factors may contribute to the finding of Black and colleagues (2007) that lesbians and gay men are less likely than heterosexual men and women to own their own homes.
Little research has examined economic outcomes for bisexual individuals specifically. Carpenter (2005) presents evidence from California that bisexual people fare less well than comparable heterosexuals (and comparable gay and lesbian individuals) in the labor market.
Finally, in the study described above, Rosser and colleagues (2007) found that transgender participants were more educated but reported less household income.
Age
As is the case for heterosexual people, all age groups include lesbians and gay men. Similarly, all age groups include transgender individuals (Rosser et al., 2007). Nearly 20 percent of members of cohabiting same-sex couples are at least 55 years of age according to the 2000 census (Gates and Ost, 2004b). Self-identified gay men tend to be older, on average, than self-identified lesbians and bisexual men and women (Herek et al., 2010). Using GSS data collected between 1988 and 2002, Turner and colleagues (2005) found that the number of women who self-reported same-sex behavior was negatively correlated with birth cohort: younger women were significantly more likely to report such behavior. For example, 1.6 percent of women born before 1920 reported ever having had same-sex contact, compared
with 6.9 percent of women born after 1969. The authors note that the increased prevalence of women reporting same-sex contact coincides with an increase in societal tolerance of same-sex sexual activity, although it is not clear whether the two phenomena are linked. A comparable pattern was not evident among men, although men’s self-reports of same-sex behavior increased somewhat during the 1990s.
BARRIERS TO ACCESSING HEALTH CARE
Sexual and gender minorities face a number of barriers to accessing health care, many of which can be traced to stigma and its consequences. Multiple components of stigma influence the health and well-being of sexual and gender minorities. This section defines the components of stigma, reviews barriers to accessing health care for members of LGBT populations, and describes how the cross-cutting theme of stigma is associated with these barriers at both the personal and structural levels.
Stigma
As used in this report, the term stigma refers to the inferior status, negative regard, and relative powerlessness that society collectively assigns to individuals and groups that are associated with various conditions, statuses, and attributes (Goffman, 1963; Herek, 2009a; Link and Phelan, 2001). Social scientists have long recognized that stigma is not inherent in a particular trait or in membership in a particular group. Rather, society collectively identifies and assigns negative meaning and value to certain characteristics and groups, thereby “constructing” stigma. Thus, in perhaps the best known theoretical analysis of the concept, Erving Goffman (1963, p. 5) characterized stigma as “an undesired differentness.” Sexual stigma refers specifically to the stigma attached to any nonheterosexual behavior, identity, relationship, or community (e.g., Herek, 2009a). Transgender stigma is used here to refer to the stigma attached to individuals who self-identify as transgender or transsexual or whose gender expression or comportment varies from societal gender norms.
Access and Barriers to Care
The Institute of Medicine (IOM) defines access to health care as the “timely use of personal health services to achieve the best possible outcomes” (IOM, 1993, p. 4). Drawing on the social ecology model, the committee categorized barriers to accessing high-quality care as both personal and structural. LGBT individuals face both types of barriers. Although many of these barriers can be traced to sexual and transgender
stigma, many LGBT individuals also experience barriers to care related to their membership in other marginalized groups in society (e.g., racial/ ethnic minorities, low-income groups, and those from certain geographic locations).
It is worth noting that while most of the literature on access to care focuses on adults, there are some issues specific to adolescents as well. In its report Adolescent Health Services, the IOM (2009) highlights the importance of providing all adolescents with health services that attract and engage them and give them opportunities to discuss sensitive health issues. Moreover, states the report, health services that are confidential are perceived as more accessible and are more likely to be utilized by adolescents, particularly for issues related to sexual behavior. For adolescents who are sexual or gender minorities, these factors may be more complex. LGBT adolescents may have access to providers, but if they are not given an opportunity to discuss such topics as sexual or gender orientation, they may not seek care or discuss confidential information. Similarly, if care is not confidential, LGBT adolescents may be less likely to access it.
Personal-Level Barriers
Personal-level barriers are created by the attitudes, beliefs, and behaviors of individuals within the health care system—both providers and patients. Individual expressions of sexual and transgender stigma create significant personal barriers for LGBT people attempting to access high-quality care. Three such expressions are discussed here: enacted stigma, felt stigma, and internalized stigma (Herek, 2009d).
Enacted stigma. Enacted stigma refers to explicit behaviors that express stigma. These behaviors can take the form of verbal epithets, shunning, overt discrimination, and even violence. Individuals are often targeted for enactments of sexual stigma because of their perceived gender nonconformity, and transgender individuals are often targeted because they are assumed to be homosexual. Thus, many stigma enactments against sexual and gender minorities alike are rooted in both sexual and transgender stigma.
Some LGBT individuals face discrimination in the health care system that can lead to an outright denial of care or to the delivery of inadequate care. There are many examples of manifestations of enacted stigma against LGBT individuals by health care providers. LGBT individuals have reported experiencing refusal of treatment by health care staff, verbal abuse, and disrespectful behavior, as well as many other forms of failure to provide adequate care (Eliason and Schope, 2001; Kenagy, 2005; Scherzer, 2000; Sears, 2009).
Felt stigma. Because any individual may be perceived to be gay, lesbian, or bisexual, virtually anyone—regardless of sexual orientation—can be the target of an enactment of sexual stigma. Most people, heterosexuals and nonheterosexuals alike, recognize this possibility, and that recognition often leads them to modify their own behavior to avoid such an experience. Heterosexuals and nonheterosexuals alike may modify or adapt their behavior in a variety of ways to avoid stigma; sexual-minority individuals may hide their sexual orientation from others, including health care providers. This awareness of the possibility that stigma will be enacted in particular situations is referred to as felt stigma. Felt stigma can be adaptive to the extent that it protects the individual from enacted stigma. At the same time, this adaptation has costs. Fear of stigmatization or previous negative experiences with the health care system may lead LGBT individuals to delay seeking care. Confidentiality also can be an issue, given that most health insurance is provided through an individual’s place of employment. If he or she is not “out” as a sexual or gender minority in the workplace, and because there is no legal protection in many jurisdictions for sexual or gender minorities in the workplace, patients may fear loss of employment due to their sexual- or gender-minority status. Ponce and colleagues (2010) suggested this explanation after demonstrating significant disparities in health care access for gay men and lesbians compared with heterosexuals. In addition, many LGBT individuals do not disclose their sexual orientation because of fear of provider bias, although it should be noted that many patients, regardless of sexual orientation, are unwilling to disclose information about their sexual behaviors to a health care provider (Jillson, 2002). For example, in-depth qualitative interviews with LGBT individuals in a rural setting revealed that many would strategically remain silent to health care providers about their sexuality or gender status (Willging et al., 2006). Others may fail to complete advance directives and powers of attorney for partners as a way of concealing their sexual orientation.
Internalized stigma. A third way in which individuals manifest stigma is by accepting the legitimacy of society’s negative regard for the stigmatized group. In non-gender-variant heterosexuals, this internalized stigma is expressed as prejudice against sexual minorities (commonly labeled sexual prejudice or homophobia) and transgender people (sometimes labeled transphobia and referred to here as transgender prejudice).
Sexual prejudice on the part of health care providers often underlies enactments of stigma. Although there has been little recent research investigating provider attitudes toward LGBT patients, earlier studies have shown that provider attitudes toward sexual-minority patients can be barriers to care (IOM, 1993; Jillson, 2002). From the available literature, it appears that many providers are uncomfortable with providing services to LGBT
patients. In one study published during the 1980s, 40 percent of physicians surveyed reported being sometimes or often uncomfortable providing care to lesbian or gay patients (Mathews et al., 1986). In a survey conducted with a nonprobability sample of members of the Gay and Lesbian Medical Association (GLMA), 67 percent of respondents believed they had seen gay or lesbian patients receive substandard care because of their sexual orientation (Schatz and O’Hanlan, 1994). On the other hand, in a recent follow-up to the earlier Matthews and colleagues (1986) study, Smith and Mathews (2007) found that levels of sexual prejudice among health care providers had declined substantially.
Among sexual- and gender-minority individuals, internalized stigma leads to denigration of the self, termed self-stigma (this phenomenon has been labeled internalized homophobia in sexual-minority individuals). Self-stigma may cause sexual and gender minorities to feel that they do not deserve respect from their health care provider or the same access to health care as heterosexuals. As a result, they may not disclose key information to their provider, may avoid seeking treatment, or may refrain from challenging discrimination and other forms of enacted stigma.
Other personal barriers. As noted, in addition to stigma related to their sexual-minority status, LGBT individuals may face barriers to care due to other characteristics, such as their racial/ethnic minority status, education level, income level, geographic location, language, immigration status, knowledge, and cultural beliefs. The intersection of these dimensions with the stigma associated with sexual- and gender-minority status results in unique barriers and challenges to accessing high-quality care for many LGBT individuals.
Structural Barriers
Structural barriers relate to the health care system at the institutional level. These barriers operate regardless of the attitudes of individuals. Examples of such barriers include an employer-based health care system that limits LGBT individuals’ access to marital benefits, including eligibility for health insurance; lack of training in LGBT health received by providers; and insurance practices that limit the types of care covered for LGBT individuals.
Structural stigma. Structural stigma (or institutional stigma) is the manifestation of stigma within the institutions of society (Corrigan et al., 2005). Structural stigma often perpetuates stigma-based differentials in status and power (Link and Phelan, 2001) and may operate even in the absence of prejudice on the part of individual members of an institution. For example,
if a health maintenance organization provides care for members’ different-sex spouses but not their same-sex partners, its sexual-minority members have a lower status than their heterosexual counterparts, regardless of whether individual staff members are personally prejudiced against sexual minorities. Just as institutional racism works “to the disadvantage of racial minority groups even in the absence of individual prejudice or discrimination” (Link and Phelan, 2001), structural sexual stigma disadvantages and restricts the opportunities of sexual and gender minorities by perpetuating their lower status and power relative to non-gender-variant heterosexuals (Herek, 2009b).
As discussed earlier, structural stigma occurs in the health care system as well in society at large (e.g., with respect to employment benefits for same-sex couples and government rules and regulations regarding marriage between same-sex couples). For example, a major structural barrier is the lack of legal recognition of partners, which has prevented many hospitals and health care providers from according partners and family members of LGBT individuals the same rights to visit and access information that are provided to heterosexual spouses. There have been cases of legal refusal to recognize the partner of a sexual-minority patient as a health care proxy even when so designated by the patient (IOM, 1999).
Provider knowledge and training. With respect to the health care provided to LGBT people, a number of structural barriers result from providers’ lack of training in the health needs of LGBT patients. Cultural competency, referring to a set of skills that allows providers to give culturally appropriate high-quality care to individuals of cultures different from their own, is an important aspect of care (IOM, 1999). Patient–provider communication is important. In fact, studies suggest that poor patient–provider communication is strongly associated with adverse health behaviors such as decreased levels of adherence to physician advice; it is also associated with decreased rates of satisfaction (Cortes et al., 2009; Inui and Carter, 1989; Stewart, 1995). Yet many providers are not trained to provide care for LGBT individuals, and providers themselves report a lack of knowledge about the issues facing their sexual- and gender-minority patients. Particularly for transgender patients, access to providers who are knowledgeable about transgender health issues is critical. In fact, few physicians are knowledgeable about or sensitive to LGBT health risks or health needs (IOM, 1999, p. 43). Medical schools teach very little about sexuality in general and little or nothing about the unique aspects of lesbian, gay, and bisexual health (Makadon, 2006; Tesar and Rovi, 1998; Wallick et al., 1993), and it is rare for medical students to receive any training in transgender health (AAMC GSA and AAMC OSR, 2007).
While the Association of American Medical Colleges issued recommen-
dations for institutional programs and educational activities to address the needs of LGBT patients in 2007, including training in communication skills regarding sexual orientation and gender identity, it is not evident that all medical schools have embraced these recommendations. The Lesbian, Gay, Bisexual, and Transgender Medical Education Research Group, a group of medical students at Stanford University, surveyed deans of medical education at 116 universities in the United States and Canada. They found variability in the content and quality of the LGBT-specific instruction medical students received, with HIV, sexual orientation, and gender identity being the most common LGBT topics included in the curricula. Fully 70 percent of the deans rated their school’s curriculum in this area as “fair” or worse (Obedin-Maliver et al., 2010).
While many providers report high levels of discomfort with taking the sexual history of any patient, this lack of training exacerbates this discomfort when providers are dealing with LGBT patients. A qualitative study involving 13 HIV providers found that discomfort with asking questions was one of their greatest issues with respect to the treatment and care of transgender patients (Lurie, 2005). Likewise, a survey of 60 pediatricians in Washington, DC, that examined their approach to the health of LGB youth found that discussions of sex and sexual orientation were difficult even for those who were well intentioned (East and El Rayess, 1998).
Health insurance. Lack of health insurance is a major structural barrier to care, and LGBT people and their children are more likely to lack health insurance than heterosexual people and their children (Badgett, 1994; Cochran, 2001; Diamant et al., 2000; Ponce et al., 2010). This is due at least partially to the fact that LGBT families often lack access to employer-sponsored health insurance (Ash and Badgett, 2006; Heck et al., 2006). As was noted in the earlier discussion of laws and policies, unmarried same-sex partners of employees often are ineligible for employer-sponsored health insurance. While 57 percent of Fortune 500 companies now extend domestic partner benefits to their LGB employees (HRC, 2010), this practice is much less common for smaller companies. Ponce and colleagues (2010) examined disparities in health insurance coverage faced by same-sex couples and found significant disparities in access to care. Using population-based data from California, the authors found that partnered gay men were less than half as likely (42 percent) as married heterosexual men to receive employer-sponsored dependent coverage, and partnered lesbians were 28 percent less likely to receive such coverage than married heterosexual women. As a result, gay men and partnered lesbians are more than twice as likely to be uninsured as married heterosexuals (Ponce et al., 2010).
Even when LGBT people have access to health insurance, they often are still at a disadvantage in relation to their heterosexual peers. Unlike most
heterosexual married couples, employees are required to pay federal taxes on employer-provided health insurance for a same-sex partner (Badgett, 2007). Moreover, health plans often fail to cover many services that impact LGBT individuals, including infertility treatment for lesbians. In some instances, access to reproductive and fertility services is denied on the basis of marital status or sexual orientation (Ethics Committee of the American Society for Reproductive Medicine, 2009).
High levels of joblessness and poverty among transgender populations, particularly those of color, make lack of health insurance a problem for these individuals (Xavier et al., 2005). In addition, both private and public health care plans severely limit transgender people’s access to sex reassignment surgery or other treatments related to transgender status. Most private insurance plans, as well as Medicare, contain explicit exclusions for such treatments.
THE CASE OF HIV/AIDS
In the chapters that follow, this report addresses a variety of issues related to the health of LGBT populations. Several themes pervade this discussion, including stigma, the resilience of LGBT communities and individuals, the importance of research funding, and persistent health inequities among racial and ethnic minority LGBT individuals. This section returns to the HIV/AIDS epidemic, whose history and impact were briefly described above, to set the stage for the following chapters by illustrating how these themes continue to influence LGBT health today. The IOM has a long history of studying AIDS, having published more than 20 reports on the subject since 1986.
The HIV/AIDS epidemic remains one of the most critical health issues faced by some subgroups within the LGBT population in the United States, namely gay and bisexual men and transgender women. As discussed below, the epidemic is another example of how the intersection of multiple identities (e.g., racial, ethnic, socioeconomic, sexual, and gender) increases risks for some individuals.
Stigma
As noted earlier, the first cases of what would eventually be labeled AIDS were diagnosed in the United States in 1981 in several white gay men (Gottlieb, 2001). The public continued to regard AIDS mainly as a “gay disease” long after health professionals had abandoned this idea (Herek and Capitanio, 1999). The association of AIDS with homosexuality and its attendant stigma shaped and intensified societal responses to AIDS while hindering research and prevention efforts.
As a new, transmissible disease that was not understood by medical science and was perceived as inevitably fatal, AIDS probably would have evoked stigma regardless of whom it affected. But the fact that the public associated it with gay men—an already marginalized group, as explained earlier in this chapter—compounded the stigma experienced by those who were diagnosed with the disease (Herek, 1990). Public opinion surveys conducted in the United States during the epidemic’s early years revealed widespread fear of AIDS, inaccurate beliefs about how it could be transmitted, and a willingness to restrict the civil liberties of people perceived to be at risk for contracting it (Blake and Arkin, 1988; Clendinen, 1983; Herek, 1990). Such beliefs and opinions tended to be strongest among respondents with negative attitudes toward gay men and lesbians. In numerous studies, respondents who expressed negative attitudes toward gay people were more likely than others to be poorly informed about AIDS, to overestimate the risks of HIV transmission through casual social contact, to endorse punitive and restrictive AIDS-related policies (e.g., mass quarantine), and to stigmatize people with the disease (D’Augelli, 1989; Goodwin and Roscoe, 1988; Herek and Glunt, 1991; Pleck et al., 1988; Price and Hsu, 1992; Pryor et al., 1989; Stipp and Kerr, 1989).
Negative attitudes toward AIDS and its perceived association with gay men found expression in a variety of ways. Men with AIDS faced ostracism and discrimination both because of their illness and because they were assumed to be gay. Many were fired from their jobs, evicted from their homes, and shunned by their relatives and friends (NRC, 1993). When public awareness about AIDS increased during the mid-1980s, groups that monitored antigay violence reported an increase in incidents, with many assailants making verbal references to AIDS during the attacks (Berrill, 1990). More than 7,200 incidents of antigay harassment and victimization were reported to the National Gay and Lesbian Task Force in 1988. Of these, 17 percent were AIDS-related. The percentages were similar in 1986 and 1987 (Berrill, 1992).
In its early stages, AIDS was perceived not as a national health problem but as a problem for homosexuals and intravenous drug users. Because of the marginal status of these groups, societal response to the epidemic was slow. It was not until there was widespread awareness that AIDS was affecting the “mainstream” population that the disease garnered significant attention. Indeed, it was Ryan White, an Indiana adolescent who contracted AIDS through treatment for hemophilia, who became the sympathetic face of AIDS to the nation (White and Cunningham, 1991).
The response of the federal government to the epidemic also was slow. Inadequate efforts were undertaken to intervene in the spread of HIV, especially compared with the response to other new diseases. Throughout most of the 1980s, the disease was seldom acknowledged by the federal
government. President Ronald Reagan mentioned AIDS publicly for the first time only in 1987.
Furthermore, HIV/AIDS research and prevention efforts were hampered by the stigma associated with homosexual behavior. Researchers and public health officials were hindered from the outset of the epidemic by the relative lack of reliable scientific data on gay and bisexual men and the LGBT community. Early in the epidemic, researchers and public health officials attempting to respond to the epidemic had to base many of their predictions and much of their planning on population estimates derived from the Kinsey studies of the 1940s and 1950s. As noted above, the generalizability of these data was questionable. However, the funding and resources needed to collect data on homosexuality and bisexuality from high-quality probability samples had not been made available during the intervening years. In addition, scientists conducting research on sexual behavior among gay and bisexual men, men who have sex with other men but do not identify as gay or bisexual, and transgender people often came under political scrutiny.
Facing stigma related to both HIV/AIDS and homosexuality, many gay and bisexual men, as well as other men who have sex with men, have been reluctant to undergo HIV testing, to seek treatment for HIV, and to participate in scientific research (Chesney and Smith, 1999; Herek, 1999; Stall et al., 1996).
The marginalized status of transgender people similarly delayed government’s responses to HIV/AIDS in the transgender community. As noted by Herbst and colleagues (2008), there was virtually no attention to infection rates in the transgender community until the mid-1990s, largely because transgender individuals were not included in federal surveillance efforts.
Although the cultural climate regarding HIV-positive individuals has become more inclusive since the early days of the AIDS epidemic, stigmatization continues to affect all LGBT people.
Resilience
As discussed earlier, AIDS was a devastating disease for LGBT people, yet they responded to this unprecedented challenge with resilience. Community-based organizations were created and provided a variety of medical, psychological, and social services to people with AIDS and disseminated information about sexual risk reduction and “safer sex.” These organizations were visible in major urban centers, but these kinds of activities extended into smaller cities and towns as well.
It can be argued that the AIDS epidemic created a greater sense of community among LGBT people than had previously existed, with far-reaching effects. In the absence of an early political or cultural response to
AIDS, gay-based organizations were the first to respond, caring for those who were infected, advocating for increased attention, and raising funds to promote scientific research. The disease forged new and stronger bonds among LGBT people. For example, although political divides along gender lines were often evident in the LGB community during the 1970s, lesbians and bisexual women, who themselves were considerably less likely to be infected with HIV than gay and bisexual men, played prominent roles in the community’s response to the epidemic.
Gerald (1989, p. 450) notes that “far from destroying the gay community, the concern over AIDS has strengthened it.” A sense of community emerged that was able to confront the challenges posed by the disease. With the creation of this organized community, new models of care and support for members of the community were developed. In addition, LGBT organizations learned how to work with foundations and corporations in new ways to access funding to address the epidemic. The community built partnerships and coalitions with research and health institutions and with federal, state, and local policy makers. The mobilization of the LGBT community was a major positive response to the epidemic, and the structures created in response to the disease continue to exist today.
Importance of Research Funding
One of the major successes that emerged from the AIDS epidemic was the confirmation that funding for research can drive progress. “Beginning in 1981 with the allocation of several hundred thousand dollars for research, U.S. government spending on HIV/AIDS nearly doubled every year between FY1982 and FY1989. Since then, annual increases in Federal spending have been more gradual” (Funders Concerned About AIDS, 2003, p. 45).
While the initial response of the federal government was slow, a strong funding commitment since the late 1980s can be linked to impressive advances. After the discovery of HIV as a viral agent, the development of a blood test to diagnose HIV-infected patients and screen the blood supply followed rapidly. In 1987, the licensing of Zidovudine (AZT), the first clinically effective drug against HIV, appeared to offer great promise. As HIV quickly became resistant to AZT, however, the initial optimism dissipated (Fauci, 2008; Sepkowitz, 2001).
By 1990, 9 years after the epidemic emerged, researchers had achieved great progress in understanding the epidemiology, natural history, and pathogenesis of the disease (IOM, 1991a). In 1991, the discovery of two other pharmaceutical agents that could be used in combination with AZT to target the virus led to the development of highly active antiretroviral therapy. By the mid-1990s, protease inhibitors had reached the market and were used successfully in combination with existing therapies to improve the prognosis
of many HIV-infected individuals. Within 2 years, the AIDS death rate in the United States dropped by more than two-thirds (Fauci, 2008).
Given that the most effective strategy against AIDS was to prevent infection in the first place and that HIV transmission occurs between people in social settings and involves individual behavior, the social and behavioral sciences clearly had an important role to play in the fight against AIDS (IOM, 1995). Much of the dramatic decline in AIDS cases observed among gay and bisexual men during the 1980s was attributable to large-scale behavior changes within the community, in which social and behavioral research played a key role (IOM, 2001).
AIDS prevention activities began in gay communities in the early 1980s in San Francisco and New York City (Shilts, 1987). Later efforts led by the Centers for Disease Control and Prevention expanded prevention activities to other populations. These early interventions focused mainly on increasing knowledge about HIV transmission, but over time, interventions were developed at the individual, small-group, and community levels that were aimed at changing behavior associated with HIV transmission (CDC, 2006).
Behavior change strategies for men who have sex with men utilized a variety of interventions, including problem solving, self-management, skills building, delivery of information, and fostering of heightened self-efficacy and intentions to reduce risk (NIH, 1997). Studies using a variety of evaluation designs (descriptive studies, nonrandomized and randomized studies) showed that risk reduction strategies for men who have sex with men had positive behavioral effects (NIH, 1997).
Figure 2-1 shows discretionary funding (including funding for research, prevention, and treatment) by the Department of Health and Human Services for HIV/AIDS from fiscal year 1981 to fiscal year 2008. It should be noted that much of the research that has been undertaken on LGBT health generally has been made possible through HIV funding.
Today, the budget for the National Institutes of Health’s (NIH) AIDS research program totals more than $3 billion, representing approximately 10 percent of the total NIH budget. Funding priorities encompass not only etiology and pathogenesis, epidemiology, preventive measures, and treatment, but also the investigation of innovative means of prevention (NIH, 2010).
Health Inequities
The progress mentioned in the previous section has not translated into benefits for all members of the LGBT community. An estimated 28,720 new HIV cases occurred among men who have sex with men in 2006. Although black people made up only 12.8 percent of the U.S. population in 2006 (U.S. Census Bureau, 2006), 35 percent (10,130) of the estimated new HIV
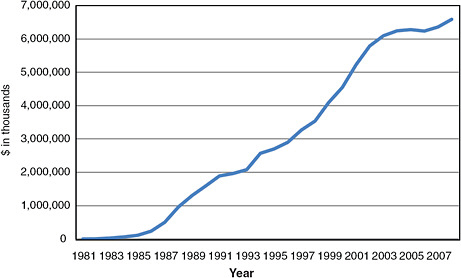
FIGURE 2-1 Discretionary funding for HIV/AIDS by the Department of Health and Human Services in thousands of dollars.
SOURCE: Adapted from a table prepared by the Congressional Research Services based on analysis from HHS Budget Office, March 20, 2008 (Johnson, 2008).
cases were among black men who have sex with men, while 46 percent (13,230) were among white men who have sex with men. Similarly, Latino people accounted for 14.8 percent of the U.S. population in 2006 (U.S. Census Bureau, 2006), but Latino men who have sex with men accounted for 18.6 percent (5,360) of new HIV cases (CDC, 2010). While HIV/AIDS diagnoses among American Indians and Alaska Natives represented less than 1 percent of all HIV/AIDS diagnoses in 2005, this group is ranked third among the U.S. population in rates of diagnosis (behind blacks and Latinos). Of the 1,447 American Indian/Alaska Native men with HIV/AIDS at the end of 2005, 74 percent had been infected through male-to-male sexual contact or male-to-male sexual contact combined with intravenous drug use (CDC, 2008).
The disproportionate impact of HIV/AIDS on nonwhite men who have sex with men may not be linked exclusively to individual risk behaviors. Social determinants, such as low education level, can be associated with a number of factors that have been understood to play a significant role in the spread of HIV/AIDS, although their effects have been largely understudied. These factors include a higher likelihood of unemployment or low-wage employment, less likelihood of having health care coverage, inferior quality of care, limited accessibility of treatment medications and interventions, community destabilization, and sexual networks composed of high-risk (more likely to have HIV infection) members (Peterson and Jones, 2009).
Black transgender individuals have a significantly higher infection rate than other racial or ethnic groups, with male-to-females being at a particularly high risk of infection. In their systematic review, Herbst and colleagues (2008) found that some of the risk factors that may contribute to the high infection rates among male-to-females include multiple sex partners who are male, casual sex, and sex while under the influence of drugs or alcohol. The authors also note that the studies considered in their meta-analysis included a high percentage of male-to-females who engage in sex work. Figure 2-2 presents a breakdown of new HIV infections in 2006, the most recent year for which data are available, by race/ethnicity among men who have sex with men. Note that the figure presents absolute numbers.
Members of racial and ethnic minority groups have typically been underrepresented in the mainstream LGBT movement. HIV in racial and ethnic minority communities, particularly the black community, is complicated by a range of issues, including, among others, a lower likelihood of getting tested, greater discomfort with the health care system and with medical institutions, lower levels of acceptance of same-sex and bisexual sexual behavior, and racism (Peterson and Jones, 2009).
Furthermore, a systematic review of HIV interventions notes the lack of interventions targeting black, Latino, or other racial and ethnic minority men who have sex with men (Lyles et al., 2007). Similarly, no evidence-based HIV prevention interventions have been identified as effective for members of the black transgender community (Herbst et al., 2008).
The health inequities illustrated by the HIV/AIDS example persist in
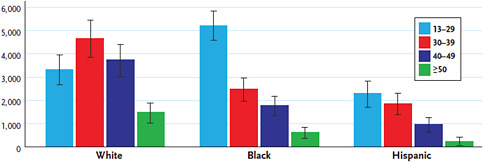
FIGURE 2-2 Estimated number of new HIV infections by race/ethnicity among men who have sex with men.
NOTES: Incidence estimates are adjusted for reporting delays and reclassification of cases reported without a known risk factor for HIV, but not for underreporting; non-Hispanic whites and non-Hispanic blacks are referred to as white and black, respectively. Persons of Hispanic ethnicity might be of any race; the “I” bars denote the data range for each confidence interval.
SOURCE: CDC, 2010.
many areas of LGBT health today. The challenges associated with understanding racial, ethnic, geographic, socioeconomic, and other LGBT sub-populations are discussed throughout the remainder of the report.
SUMMARY OF KEY FINDINGS AND RESEARCH OPPORTUNITIES
Findings
Operationally defining LGBT populations requires considerable care and attention to the focus of the research question. Basic demographic data, which are critical to understanding and meeting the needs of populations, are lacking for LGBT populations. From the data that are available, much more is known about lesbians and gay men than about bisexual and transgender people. Further complicating the situation is the fact that not only are lesbians, gay men, bisexual women, bisexual men, transgender women, and transgender men all discrete populations, but each group is further shaped by racial, ethnic, and other cultural influences. The available demographic data fail to adequately describe the variations within each LGBT population; however, existing research provides some pertinent findings:
-
Self-identification as lesbian, gay, or bisexual and disclosure of this identity may vary by race, ethnicity, income level, or geographic location.
-
If one examines the historical trajectory of LGBT populations in the United States, it is clear that stigma has exerted an enormous and continuing influence on the life and consequently the health status of LGBT individuals.
-
LGBT individuals live in most geographic areas throughout the United States, but studies have shown higher proportions in urban areas on the East and West Coasts.
-
On average, gay men appear to have lower incomes than heterosexual men with similar education and occupations. While some research has suggested that lesbian women have higher incomes than heterosexual women, other studies have not found this difference. In comparison with non-gender-variant heterosexual adults, bisexual and transgender people also appear to have lower incomes.
-
As a result of differential treatment in such areas as taxes and insurance, even lesbian or gay individuals whose gross incomes are identical to those of heterosexual men and women can be expected to have less disposable income.
-
While lesbians and gay men are less likely to be parents than their heterosexual peers, substantial numbers of lesbians and gay men have children.
-
Lesbians, gay men, and bisexual and transgender people exist across all age groups.
-
LGBT individuals face financial barriers, limitations on access to health insurance, insufficient provider knowledge, and negative provider attitudes that can be expected to have an effect on their access to health care.
-
A lack of training for health care providers may lead to less than optimal care for LGBT adolescents and adults.
-
LGBT individuals face barriers to care related to sexual and transgender stigma, and some are further marginalized by additional barriers such as racial/ethnic minority status, low income, immigrant status, and limited English proficiency.
Research Opportunities
Research on the influence of contextual factors (e.g., income, geographic location, race, ethnicity, stigma) on LGBT health status is lacking. Although limited data are available with which to assess how many individuals identify as lesbian, gay, bisexual, or transgender, as well as how many report same-sex sexual behavior, demographic data on LGBT populations from large-scale surveys are largely absent from the literature. There are many opportunities for future research:
-
large-scale surveys examining the demographic and social characteristics of sexual and gender minorities;
-
patterns of household composition within LGBT populations, specifically rates of partnership and children with gay, lesbian, bisexual, or transgender parents;
-
income and education differences among both single and partnered sexual- and gender-minority individuals;
-
impacts of barriers to care—particularly provider knowledge about and attitudes toward LGBT patients, limited access to health insurance, and discrimination within the health care system—on the health of LGBT individuals; and
-
the extent to which LGBT individuals experience enactments of stigma and the impact of sexual and transgender stigma, at both the personal and structural levels, on LGBT health.
REFERENCES
AAMC GSA and AAMC OSR (Association of American Medical Colleges Group on Student Affairs and Association of American Medical Colleges Organization of Student Representatives). 2007. Institutional programs and educational activities to address the needs of GLBT students and patients. Washington, DC: AAMC GSA and AAMC OSR.
Adam, B. D. 1987. The rise of a gay and lesbian movement. New York: Twayne Publishers.
Adam, B. D. 1995. The rise of a gay and lesbian movement (revised edition). New York: Twayne Publishers.
Allegretto, S. A., and M. M. Arthur. 2001. An empirical analysis of homosexual/heterosexual male earnings differentials: Unmarried and unequal? Industrial and Labor Relations Review 54:631–646.
American Psychiatric Association. 1952. Mental disorders: Diagnostic and statistical manual. Washington, DC: American Psychiatric Association.
American Psychiatric Association. 1980. Diagnostic and statistical manual of mental disorders. 3rd ed. Washington, DC: American Psychiatric Association.
American Psychiatric Association. 1987. Diagnostic and statistical manual of mental disorders. 4th ed. Washington, DC: American Psychiatric Association.
American Psychiatric Association. 2000. Diagnostic and statistical manual of mental disorders (DSM-IV-TR). 4th ed. Washington, DC: American Psychiatric Association.
American Psychological Association. 2009a. Report of the APA task force on gender identity and gender variance. Washington, DC: American Psychological Association.
American Psychological Association. 2009b. Report of the task force on appropriate therapeutic responses to sexual orientation. Washington, DC: American Psychological Association.
American Psychological Association and APHA (American Public Health Association). 1986. Bowers v. Hardwick: Brief for amicus curiae, Supreme Court of the United States. Washington, DC: American Psychological Association and APHA.
Ash, M. A., and M. V. L. Badgett. 2006. Separate and unequal: The effect of unequal access to employment-based health insurance on same-sex and unmarried different-sex couples. Contemporary Economic Policy 24(4):582–599.
Badgett, M. V. L. 1994. Civil rights, civilized research: Constructing a sexual orientation anti-discrimination policy based on the evidence. Paper presented at APPAM Research Conference, San Francisco, CA.
Badgett, M. V. L. 1995. The wage effects of sexual orientation discrimination. Industrial and Labor Relations Review 48(4):726–739.
Badgett, M. V. L. 2001. Money, myths, and change: The economic lives of lesbians and gay men. Chicago, IL: University of Chicago Press.
Badgett, M. V. L. 2007. Unequal taxes on equal benefits: The taxation of domestic partner benefits. Echelon Magazine 22–22.
Baumeister, R. F. 2000. Gender differences in erotic plasticity: The female sex drive as socially flexible and responsive. Psychological Bulletin 126(3):347–374; discussion 385–389.
Baumeister, R. F., K. R. Catanese, and K. D. Vohs. 2001. Is there a gender difference in strength of sex drive? Theoretical views, conceptual distinctions, and a review of relevant evidence. Personality and Social Psychology Review 5(3):242–273.
Bayer, R. 1987. Homosexuality and American psychiatry: The politics of diagnosis (revised edition). Princeton, NJ: Princeton University Press.
Bayer, R. 1989. Private acts, social consequences: AIDS and the politics of public health. New York: The Free Press.
Benjamin, H. 1966. The transsexual phenomenon. New York: Julian Press.
Berrill, K. T. 1990. Anti-gay violence and victimization in the United States. Journal of Interpersonal Violence 5(3):274-294.
Berrill, K. T. 1992. Anti-gay violence and victimization in the United States: An overview. In Hate crimes: Confronting violence against lesbians and gay men, edited by G. M. Herek and K. T. Berrill. Newbury Park, CA: SAGE Publications. Pp. 19–45.
Berube, A. 1990. Coming out under fire: The history of gay men and women in World War Two. New York: The Free Press.
Biegel, S., and S. J. Kuehl. 2010. Safe at school: Addressing the school environment and LGBT safety through policy and legislation. Los Angeles, CA: The Williams Institute, The Great Lakes Center for Education Research and Practice, and the National Education Policy Center.
Black, D., G. Gates, S. Sanders, and L. Taylor. 2000. Demographics of the gay and lesbian population in the United States: Evidence from available systematic data sources. Demography 37(2):139–154.
Black, D. A., H. R. Makar, S. G. Sanders, and L. J. Taylor. 2003. The earnings effects of sexual orientation. Industrial and Labor Relations Review 56:449–469.
Black, D. A., S. G. Sanders, and L. J. Taylor. 2007. The economics of lesbian and gay families. The Journal of Economic Perspectives 21:53–70.
Blake, S. M., and E. B. Arkin. 1988. AIDS information monitor: A summary of national public opinion surveys on AIDS: 1983 through 1986. Washington, DC: American Red Cross.
Bockting, W. O. 1997. Transgender coming out: Implications for the clinical management of gender dysphoria. In Gender blending, edited by B. Bullough, V. L. Bullough, and J. Elias. Amherst, NY: Prometheus Books. Pp. 48–52.
Bockting, W. O. 1999. From construction to context: Gender through the eyes of the transgendered. SIECUS Report 28(1):3–7.
Bockting, W. O. 2008. Psychotherapy and the real-life experience: From gender dichotomy to gender diversity. Sexologies 17(4):211–224.
Bockting, W. O., and R. Ehrbar. 2006. Commentary: Gender variance, dissonance, or identity disorder. Journal of Psychology and Human Sexuality 17(3/4):125–134.
Bockting, W. O., B. R. Rosser, and K. Scheltema. 1999. Transgender HIV prevention: Implementation and evaluation of a workshop. Health Education Research 14(2):177–183.
Bockting, W., A. Benner, and E. Coleman. 2009. Gay and bisexual identity development among female-to-male transsexuals in North America: Emergence of a transgender sexuality. Archives of Sexual Behavior 38(5):688–701.
Bowleg, L., G. Burkholder, M. Teti, and M. L. Craig. 2008. The complexities of outness: Psychosocial predictors of coming out to others among black lesbian and bisexual women. Journal of LGBT Health Research 4(4):153–166.
Boyd, N. A. 2003. Wide-open town: A history of queer San Francisco to 1965. Berkeley: University of California Press.
Bullough, V. L., and B. Bullough. 1993. Crossdressing, sex, and gender. Philadelphia, PA: University of Pennsylvania Press.
Carpenter, C. S. 2005. Self-reported sexual orientation and earnings: Evidence from California. Industrial and Labor Relations Review 58(2):258–273.
Carpenter, C. S. 2007. Revisiting the income penalty for behaviorally gay men: Evidence from NHANES III. Labour Economics 14(1):25–34.
Carpenter, C. S., and G. J. Gates. 2008. Gay and lesbian partnership: Evidence from California. Demography 45(3):573-590.
Cauldwell, D. O. 1949. Psychopathia transexualis. Sexology 16:139–152.
CDC (Centers for Disease Control and Prevention). 2003. HIV/STD risks in young men who have sex with men who do not disclose their sexual orientation—six U.S. cities, 1994–2000. Atlanta, GA: CDC.
CDC. 2006. Evolution of HIV/AIDS prevention programs—United States, 1981-2006. Morbidity and Mortality Weekly Report 55(21):597–603.
CDC. 2008. HIV/AIDS among American Indians and Alaska natives. Atlanta, GA: CDC.
CDC. 2010. HIV and AIDS among gay and bisexual men. Atlanta, GA: CDC.
Chae, D. H., and G. Ayala. 2010. Sexual orientation and sexual behavior among Latino and Asian Americans: Implications for unfair treatment and psychological distress. Journal of Sex Research 47(5):451–459.
Chauncey, G., Jr. 1982–1983. From sexual inversion to homosexuality: Medicine and the changing conceptualization of female deviance. Salmagundi 58–59:114–146.
Chauncey, G., Jr. 1993. The postwar sex crime panic. In True stories from the American past, edited by W. Graebner. New York: McGraw-Hill. Pp. 160–178.
Chauncey, G, Jr. 2004. Why marriage? The history shaping today’s debate over gay equality. New York: Basic Books.
Chesney, M. A., and A. W. Smith. 1999. Critical delays in HIV testing and care. American Behavioral Scientist 42(7):1162–1174.
Chu, S. Y., T. A. Peterman, L. S. Doll, J. W. Buehler, and J. W. Curran. 1992. AIDS in bisexual men in the United States: Epidemiology and transmission to women. American Journal of Public Health 82(2):220–224.
Clendinen, D. 1983. AIDS spreads pain and fear among ill and healthy alike. New York Times, A1, B4.
Coan, D. L., W. Schrager, and T. Packer. 2005. The role of male sexual partners in HIV infection among male-to-female transgendered individuals. In Transgender health and HIV prevention: Needs assessment studies from transgender communities across the United States, edited by W. Bockting and E. Avery. New York: The Haworth Medical Press. Pp. 21–30.
Cochran, S. D. 2001. Emerging issues in research on lesbians’ and gay men’s mental health: Does sexual orientation really matter? American Psychologist 56(11):931–947.
Cochran, W. G., F. Mosteller, and J. W. Tukey. 1953. Statistical problems of the Kinsey Report. Journal of the American Statistical Association 48(264):673–716.
Coleman, E., P. Colgan, and L. Gooren. 1992. Male cross-gender behavior in Myanmar (Burma): A description of the acault. Archives of Sexual Behavior 21(3):313–321.
Conger, J. J. 1975. Proceedings of the American Psychological Association, Incorporated, for the year 1974: Minutes of the annual meeting of the Council of Representatives. American Psychologist 30:620–651.
Corrigan, P. W., A. C. Watson, M. L. Heyrman, A. Warpinski, G. Gracia, N. Slopen, and L. L. Hall. 2005. Structural stigma in state legislation. Psychiatric Services 56(5):557–563.
Cortes, D. E., N. Mulvaney-Day, L. Fortuna, S. Reinfeld, and M. Alegría. 2009. Patient-provider communication. Health Education & Behavior 36(1):138–154.
D’Augelli, A. R. 1989. Lesbians’ and gay men’s experiences of discrimination and harassment in a university community. American Journal of Community Psychology 17(3):317–321.
D’Emilio, J. 1983. Sexual politics, sexual communities. Chicago, IL: The University of Chicago Press.
Department of Justice. 2009. 2008 hate crime statistics: Incidents, offenses, victims, and known offenders by bias motivation. http://www2.fbi.gov/ucr/hc2008/data/table_01.html (accessed November 4, 2010).
Diamant, A. L., C. Wold, K. Spritzer, and L. Gelberg. 2000. Health behaviors, health status, and access to and use of health care: A population-based study of lesbian, bisexual, and heterosexual women. Archives of Family Medicine 9(10):1043–1051.
Diamond, L. M. 2008. Sexual fluidity: Understanding women’s love and desire. Cambridge, MA: Harvard University Press.
Doll, L. S., L. R. Petersen, C. R. White, E. S. Johnson, J. W. Ward, and The Blood Donor Study Group. 1992. Homosexually and nonhomosexually identified men who have sex with men: A behavioral comparison. Journal of Sex Research 29(1):1–14.
Drescher, J. 2010. Queer diagnoses: Parallels and contrasts in the history of homosexuality, gender variance, and the diagnostic and statistical manual. Archives of Sexual Behavior 39(2):427–460.
East, J. A., and F. El Rayess. 1998. Pediatricians’ approach to the health care of lesbian, gay, and bisexual youth. Journal of Adolescent Health 23(4):191–193.
Eliason, M. J., and R. D. Schope. 2001. Does “don’t ask don’t tell” apply to health care? Lesbian, gay, and bisexual people’s disclosure to health care providers. Journal of the Gay and Lesbian Medical Association 5(4):125–134.
Ellis, H. 1901. Studies in the psychology of sex: Volume 2: Sexual inversion. Philadelphia, PA: F.A. Davis.
Ellis, H. 1933. Psychology of sex. London: William Heinemann.
Epstein, S. 1996. Impure science: AIDS, activism, and the politics of knowledge. Berkeley, CA: University of California Press.
Erikson, K. T. 1976. Everything in its path: Destruction of community in the Buffalo Creek flood. New York: Simon and Schuster.
Ethics Committee of the American Society for Reproductive Medicine. 2009. Access to fertility treatment by gays, lesbians, and unmarried persons. Fertility & Sterility 92(4): 1190–1193.
Faderman, L. 1991. Odd girls and twilight lovers: A history of lesbian life in twentieth-century America. New York: Columbia University Press.
Fauci, A. S. 2008. 25 years of HIV. Nature 453(7193):289–290.
FBI (Federal Bureau of Investigation). 2010. About hate crime statistics. http://www2.fbi.gov/ucr/hc2009/abouthcs.html (accessed December 7, 2010).
Feinberg, L. 1996. Transgender warriors. Boston, MA: Beacon Press.
Feldman, M. P. 1966. Aversion therapy for sexual deviations: A critical review. Psychological Bulletin 65(2):65–79.
Fisk, N. M. 1974. Editorial: Gender dysphoria syndrome—the conceptualization that liberalizes indications for total gender reorientation and implies a broadly based multi-dimensional rehabilitative regimen. Western Journal of Medicine 120(5):386–391.
Fleming, M., C. Steinman, and G. Bocknek. 1980. Methodological problems in assessing sex-reassignment surgery: A reply to Meyer and Reter. Archives of Sexual Behavior 9(5):451–456.
Flores, S. A., R. Bakeman, G. A. Millett, and J. L. Peterson. 2009. HIV risk among bisexually and homosexually active racially diverse young men. Sexually Transmitted Diseases 36(5):325–329.
Ford, C. S., and F. Beach. 1951. Patterns of sexual behavior. New York: Harper and Row.
Freud, S. 1951. Letter from Freud. American Journal of Psychiatry 107(10):786-787.
Freud, S. 1953. Three essays on the theory of sexuality. In The standard edition of the complete psychological works of Sigmund Freud, Vol. 7, edited by J. Strachey. London: Hogarth Press. Original edition, original work published in 1905. Pp. 123–243.
Friedman, R. C., and J. I. Downey. 1998. Psychoanalysis and the model of homosexuality as psychopathology: A historical overview. American Journal of Psychoanalysis 58(3):249–270.
Funders Concerned About AIDS. 2003. HIV/AIDS philanthropy: History and current parameters, 1981–2000. New York: Funders Concerned About AIDS.
GAO (General Accounting Office). 2004. Defense of marriage act: Update to prior report. Washington, DC: GAO.
Gates, G. 2006. Same-sex couples and the gay, lesbian, bisexual population: New estimates from the American Community Survey. Los Angeles, CA: The Williams Institute on Sexual Orientation.
Gates, G. J. 2010. Sexual minorities in the 2008 General Social Survey: Coming out and demographic characteristics. Los Angeles, CA: The Williams Institute.
Gates, G., and J. Ost. 2004a. Estimating the size of the gay and lesbian population. In The gay and lesbian atlas, edited by G. Gates and J. Ost. Washington, DC: The Urban Institute Press. Pp. 17–21.
Gates, G., and J. Ost. 2004b. The gay and lesbian atlas. Washington, DC: The Urban Institute Press.
Gates, G., and A. P. Romero. 2009. Parenting by gay men and lesbians: Beyond the current research. In Marriage and family: Perspectives and complexities, edited by E. Peters and C. M. Kamp Dush. New York: Columbia University Press. Pp. 227–243.
Gates, G., M. V. L. Badgett, J. E. Macomber, and K. Chambers. 2007. Adoption and foster care by gay and lesbian parents in the United States. Los Angeles, CA: The Williams Institute.
Gerald, G. 1989. What can we learn from the gay community’s response to the AIDS crisis? Journal of the National Medical Association 81(4):449–452.
Goffman, E. 1963. Stigma: Notes on the management of spoiled identity. New York: Simon and Schuster.
Goldbaum, G., T. Perdue, R. Wolitski, C. Rietmeijer, A. Hedrich, R. Wood, M. Fishbein, D. Cohn, N. Corby, A. Freeman, C. Guenther-Grey, J. Sheridan, and S. Tross. 1998. Differences in risk behavior and sources of AIDS information among gay, bisexual, and straight-identified men who have sex with men. AIDS and Behavior 2(1):13–21.
Goldberg, N. G. 2009. The impact of inequality for same-sex partners in employer-sponsored retirement plans. Los Angeles, CA: The Williams Institute.
Gonsiorek, J. C. 1991. The empirical basis for the demise of the illness model of homosexuality. In Homosexuality: Research implications for public policy, edited by J. C. Gonsiorek and J. D. Weinrich. Newbury Park, CA: SAGE Publications. Pp. 115–136.
Goodwin, M. P., and B. Roscoe. 1988. AIDS: Students’ knowledge and attitudes at a Midwestern university. Journal of American College Health 36(4):214–222.
Gottlieb, M. S. 2001. AIDS—past and future. New England Journal of Medicine 344(23): 1788–1791.
Gottlieb, M. S., H. M. Schanker, P. T. Fan, A. Saxon, J. D. Weisman, and I. Pozalski. 1981. Pneumocystis pneumonia—Los Angeles. Morbidity and Mortality Weekly Report 30:250–252, http://www.cdc.gov/mmwr/preview/mmwrhtml/june_5.htm (accessed December 22, 2010).
Green, R., and D. T. Fleming. 1990. Transsexual surgery follow-up: Status in the 1990s. Annual Review of Sex Research 1:163–174.
Haldeman, D. C. 1994. The practice and ethics of sexual orientation conversion therapy. Journal of Consulting & Clinical Psychology 62(2):221–227.
Harlow, C. W. 2005. Hate crime reported by victims and police. Washington, DC: Department of Justice.
Hastings, D., and C. Markland. 1978. Post-surgical adjustment of twenty-five transsexuals (male-to-female) in the University of Minnesota Study. Archives of Sexual Behavior 7(4):327–336.
Hastings, D. W. 1969. Inauguration of a research project on transsexualism in a university medical center. In Transsexualism and sex reassignment, edited by R. Green and J. Money. Baltimore, MD: Johns Hopkins Press. Pp. 243–251.
Heck, J. E., R. L. Sell, and S. S. Gorin. 2006. Health care access among individuals involved in same-sex relationships. American Journal of Public Health 96(6):1111–1118.
Herbenick, D., M. Reece, V. Schick, S. A. Sanders, B. Dodge, and J. D. Fortenberry. 2010. Sexual behavior in the United States: Results from a national probability sample of men and women ages 14–94. The Journal of Sexual Medicine 7:255–265.
Herbst, J. H., E. D. Jacobs, T. J. Finlayson, V. S. McKleroy, M. S. Neumann, N. Crepaz, and HIV/AIDS Prevention Research Synthesis Team. 2008. Estimating HIV prevalence and risk behaviors of transgender persons in the United States: A systematic review. AIDS & Behavior 12(1):1–17.
Herdt, G. 2001. Social change, sexual diversity, and tolerance for bisexuality in the United States. In Lesbian, gay, and bisexual identities and youth: Psychological perspectives, edited by A. R. D’Augelli and C. J. Patterson. New York: Oxford University Press. Pp. 267–283.
Herdt, G., and R. Kertzner. 2006. I do, but I can’t: The impact of marriage denial on the mental health and sexual citizenship of lesbians and gay men in the United States. Sexuality Research and Social Policy 3(1):33–49.
Herek, G. M. 1990. Illness, stigma, and AIDS. In Psychological aspects of serious illness: Chronic conditions, fatal diseases, and clinical care, edited by P. T. Costa, Jr., and G. R. VandenBos. Washington, DC: American Psychological Association. Pp. 103–150.
Herek, G. M. 1992. The community response to violence in San Francisco: An interview with Wenny Kusuma, Lester Olmstead-Rose, and Jill Tregor. In Hate crimes: Confronting violence against lesbians and gay men, edited by G. M. Herek and K. T. Berrill. Thousand Oaks, CA: SAGE Publications. Pp. 241–258.
Herek, G. M. 1999. AIDS and stigma. American Behavioral Scientist 42(7):1106–1116.
Herek, G. M. 2006. Legal recognition of same-sex relationships in the United States—a social science perspective. American Psychologist 61(6):607–621.
Herek, G. M. 2009a. Hate crimes and stigma-related experiences among sexual minority adults in the United States: Prevalence estimates from a national probability sample. Journal of Interpersonal Violence 24(1):54–74.
Herek, G. M. 2009b. Sexual prejudice. In Handbook of prejudice, stereotyping, and discrimination, edited by T. D. Nelson. New York: Psychology Press. Pp. 441–467.
Herek, G. M. 2009c. Sexual stigma and sexual prejudice in the United States: A conceptual framework. Nebraska Symposium on Motivation 54:65–111.
Herek, G. M. 2009d. Sexual stigma and sexual prejudice in the United States: A conceptual framework. In Contemporary perspectives on lesbian, gay, and bisexual identities, edited by D. A. Hope. New York: Springer Science + Business Media. Pp. 65–111.
Herek, G. M., and J. P. Capitanio. 1996. “Some of my best friends”: Intergroup contact, concealable stigma, and heterosexuals’ attitudes toward gay men and lesbians. Personality & Social Psychology Bulletin 22:412–424.
Herek, G. M., and J. P. Capitanio. 1999. Sex differences in how heterosexuals think about lesbians and gay men: Evidence from survey context effects. Journal of Sex Research 36(4):348–360.
Herek, G. M., and E. K. Glunt. 1991. AIDS-related attitudes in the United States: A preliminary conceptualization. Journal of Sex Research 28(1):99–123.
Herek, G. M., and C. Sims. 2008. Sexual orientation and violent victimization: Hate crimes and intimate partner violence among gay and bisexual males in the United States. In Unequal opportunity: Health disparities among gay and bisexual men in the United States, edited by R. J. Wolitski, R. Stall, and R. O. Valdiserri. New York: Oxford University Press. Pp. 35–71.
Herek, G. M., A. Norton, T. Allen, and C. Sims. 2010. Demographic, psychological, and social characteristics of self-identified lesbian, gay, and bisexual adults in a US probability sample. Sexuality Research and Social Policy 7(3):176–200.
Higgins, D. J. 2006. Same-sex attraction in heterosexually partnered men: Reasons, rationales and reflections. Sexual and Relationship Therapy 21(2):217–228.
Hirschfeld, M. 1991. The transvestites: The erotic drive to cross-dress. Translated by M. A. Lombardi-Nash. Buffalo, NY: Prometheus Books. Original edition, 1910.
Hirschfeld, M. 2000. The homosexuality of men and women (2nd edition). Translated by M. A. Lombardi-Nash. Buffalo, NY: Prometheus Books.
Hooker, E. 1957. The adjustment of the male overt homosexual. Journal of Projective Techniques 21(1):18–31.
HRC (Human Rights Campaign). 2010. LGBT equality at the fortune 500. http://www.hrc.org/issues/workplace/fortune500.htm (accessed February 9, 2011).
Inui, T. S., and W. B. Carter. 1989. Design issues in research on doctor-patient communication. In Communicating with medical patients, edited by M. Stewart and D. Roter. London: SAGE Publications.
IOM (Institute of Medicine). 1991a. The AIDS Research Program of the National Institutes of Health. Washington, DC: National Academy Press.
IOM. 1991b. Expanding access to investigational therapies for HIV infection and AIDS. Washington, DC: National Academy Press.
IOM. 1991c. HIV screening of pregnant women and newborns. Washington, DC: National Academy Press.
IOM. 1993. Access to health care in America. Washington, DC: National Academy Press.
IOM. 1995. HIV and the blood supply: An analysis of crisis decision making. Washington, DC: National Academy Press.
IOM. 1999. Lesbian health: Current assessment and directions for the future. Washington, DC: National Academy Press.
IOM. 2001. No time to lose: Getting more from HIV prevention. Washington, DC: National Academy Press.
IOM. 2005. Public financing and delivery of HIV/AIDS care: Securing the legacy of Ryan White. Washington, DC: The National Academies Press.
IOM. 2009. Adolescent health services: Missing opportunities. Washington, DC: The National Academies Press.
Jeffries, W. L. T. 2009. A comparative analysis of homosexual behaviors, sex role preferences, and anal sex proclivities in Latino and non-Latino men. Archives of Sexual Behavior 38(5):765–778.
Jenness, V., and R. Grattet. 2001. Making hate a crime: From social movement to law enforcement. New York: Russell Sage.
Jillson, I. A. 2002. Opening closed doors: Improving access to quality health services for LGBT populations. Clinical Research and Regulatory Affairs 19(2–3):153–190.
Johnson, D. K. 2004. The lavender scare: The Cold War persecution of gays and lesbians in the federal government. Chicago: University of Chicago Press.
Johnson, J. A. 2008. AIDS funding for federal government programs: FY1981–FY2009. Washington, DC: Congressional Research Service.
Jordan, M. D. 1997. The invention of sodomy in Christian theology. Chicago, IL: University of Chicago Press.
Joslin, C. G., and S. P. Minter. 2009. Lesbian, gay, bisexual and transgender family law. Eagan, MN: Thomson West.
Katz, J. N. 1976. Gay American history: Lesbians and gay men in the U.S.A. New York: Thomas Y. Crowell Company.
Kenagy, G. P. 2005. Transgender health: Findings from two needs assessment studies in Philadelphia. Health & Social Work 30(1):19–26.
Kennamer, J. D., J. Honnold, J. Bradford, and M. Hendricks. 2000. Differences in disclosure of sexuality among African American and white gay/bisexual men: Implications for HIV/ AIDS prevention. AIDS Education & Prevention 12(6):519–531.
Kimberly, J. A. 1997. I am transsexual—hear me roar. Minnesota Law and Politics 21–49.
Kinsey, A. C., W. B. Pomeroy, and C. E. Martin. 1948. Sexual behaviour in the human male. Philadelphia, PA: W.B. Saunders.
Kinsey, A. C., W. B. Pomeroy, C. E. Martin, and P. H. Gebhard. 1953. Sexual behavior in the human female. Philadelphia, PA: W.B. Saunders.
Klawitter, M. M., and V. Flatt. 1998. The effects of state and local antidiscrimination policies on earnings for gays and lesbians. Journal of Policy Analysis and Management 17(4):658–686.
Knudson, G., G. DeCuypere, and W. Bockting. 2010. Recommendations for revision of the DSM diagnoses of gender identity disorders: Consensus Statement of the World Professional Association for Transgender Health. International Journal of Transgenderism 12(2):115–118.
Kosciw, J. G., A. Diaz, and E. A. Greytak. 2008. 2007 National School Climate Survey: The experiences of lesbian, gay, bisexual and transgender youth in our nation’s schools. New York: The Gay, Lesbian and Straight Education Network.
Krafft-Ebing, R. V. 1900. Psychopathia sexualis with especial reference to antipathetic sexual instinct: A medico-forensic study. Chicago, IL: W.T. Keener.
Kramer, M. A., S. O. Aral, and J. W. Curran. 1980. Self-reported behavior patterns of patients attending a sexually transmitted disease clinic. American Journal of Public Health 70(9):997–1000.
Laub, D. R., and N. Fisk. 1974. A rehabilitation program for gender dysphoria syndrome by surgical sex change. Plastic and Reconstructive Surgery 53(4):388–403.
Laumann, E. O., J. H. Gagnon, R. T. Michael, and S. Michaels. 1994a. Homosexuality. In The social organization of sexuality: Sexual practices in the United States, edited by E. O. Laumann, J. H. Gagnon, R. T. Michael, and S. Michaels. Chicago, IL: The University of Chicago Press. Pp. 283.
Laumann, E. O., R. T. Michael, and J. H. Gagnon. 1994b. A political history of the national sex survey of adults. Family Planning Perspectives 26(1):34–38.
Leslie, C. 2000. Creating criminals: The injuries inflicted by “unenforced” sodomy laws. Harvard Civil Rights-Civil Liberties Law Review 35(1):103–181.
Levine, M. P. 1979. Gay ghetto. Journal of Homosexuality 4(4):363–377.
Levine, M. P. 1989. The impact of AIDS on the homosexual clone community in New York City. Paper presented at V International Conference on AIDS, Montreal.
Levine, M. P. 1998. Gay macho: The life and death of the homosexual clone. New York: New York University Press.
Levine, M. P., P. M. Nardi, P. M., and G. H. Gagnon. 1997. In changing times: Gay men and lesbians encounter HIV/AIDS. Chicago, IL: University of Chicago Press.
Levine, S. B., G. Brown, E. Coleman, P. Cohen-Kettenis, J. J. Hage, J. Van Maasdam, M. Petersen, F. Pfafflin, and L. C. Schaefer. 1998. The standards of care for gender identity disorders. International Journal of Transgenderism 2(2).
Lewin, E. 1998. Recognizing ourselves. New York: Columbia University Press.
Link, B. G., and J. C. Phelan. 2001. Conceptualizing stigma. Annual Review of Sociology 27(1):363.
Lurie, S. 2005. Identifying training needs of health-care providers related to treatment and care of transgendered patients: A qualitative needs assessment conducted in New England. In Transgender health and HIV prevention: Needs assessment studies from transgender communities across the United States, edited by W. Bockting and E. Avery. New York: The Haworth Medical Press. Pp. 93–112.
Lyles, C. M., L. S. Kay, N. Crepaz, J. H. Herbst, W. F. Passin, A. S. Kim, S. M. Rama, S. Thadiparthi, J. B. DeLuca, M. M. Mullins, and HIV/AIDS Prevention Research Synthesis Team. 2007. Best-evidence interventions: Findings from a systematic review of HIV behavioral interventions for US populations at high risk, 2000–2004. American Journal of Public Health 97(1):133–143.
Makadon, H. J. 2006. Improving health care for the lesbian and gay communities. New England Journal of Medicine 354(9):895–897.
Martin, J. L., L. Dean, M. Garcia, and W. Hall. 1989. The impact of AIDS on a gay community: Changes in sexual behavior, substance use, and mental health. American Journal of Community Psychology 17:269–293.
Mathews, W. C., M. W. Booth, J. D. Turner, and L. Kessler. 1986. Physicians’ attitudes toward homosexuality—survey of a California county medical society. Western Journal of Medicine 144(1):106–110.
Max, L. W. 1935. Breaking up a homosexual fixation by the conditioned reaction technique: A case study. Psychological Bulletin 32:734.
McKirnan, D. J., J. P. Stokes, L. Doll, and R. G. Burzette. 1995. Bisexually active men: Social characteristics and sexual behavior. Journal of Sex Research 32(1):65–76.
McKirnan, D. J., P. A. Vanable, D. G. Ostrow, and B. Hope. 2001. Expectancies of sexual “escape” and sexual risk among drug and alcohol-involved gay and bisexual men. Journal of Substance Abuse 13(1–2):137–154.
Menninger, W. C. 1948. Psychiatry in a troubled world. New York: Macmillan.
Meyer, J. K., and D. J. Reter. 1979. Sex reassignment: Follow-up. Archives of General Psychiatry 36(9):1010–1015.
Meyerowitz, J. 1998. Sex change and the popular press: Historical notes on transsexuality in the United States, 1930-1955. GLQ: A Journal of Lesbian and Gay Studies 4(2):159–187.
Meyerowitz, J. 2002. How sex changed: A history of transsexuality in the United States. Cambridge, MA: Harvard University Press.
Meyerowitz, J. 2006. Transforming sex: Christine Jorgensen in the postwar U.S. (cover story). OAH Magazine of History 20(2):16–20.
Michaels, S. 1996. The prevalence of homosexuality in the United States. In Textbook of homosexuality and mental health, edited by R. P. Cabaj and T. S. Stein. Washington, DC: American Psychiatric Press. Pp. 43–63.
Miller, P. V. 1995. They said it couldn’t be done: The National Health and Social Life Survey. Public Opinion Quarterly 59(3):404–419.
Minnesota Department of Human Rights. 1993. How Minnesota protects gender identity. http://www.humanrights.state.mn.us/education/articles/rs06_4gender_protections.html (accessed December 31, 2010).
Minton, H. L. 2002. Departing from deviance: A history of homosexual rights and emancipatory science in America. Chicago, IL: University of Chicago Press.
Money, J. 1985. The destroying angel: Sex, fitness & food in the legacy of degeneracy theory, graham crackers, Kellogg’s corn flakes & American health history. Buffalo, NY: Prometheus Books.
Money, J. 1994. The concept of gender identity disorder in childhood and adolescence after 39 years. Journal of Sex & Marital Therapy 20(3):163–177.
Montgomery, J. P., E. D. Mokotoff, A. C. Gentry, and J. M. Blair. 2003. The extent of bisexual behaviour in HIV-infected men and implications for transmission to their female sex partners. AIDS Care 15(6):829–837.
Mosher, W. D., A. Chandra, and J. Jones. 2005. Sexual behavior and selected health measures: Men and women 15-44 years of age, United States, 2002. Advanced Data (362):1–55.
Murad, M. H., M. B. Elamin, M. Z. Garcia, R. J. Mullan, A. Murad, P. J. Erwin, and V. M. Montori. 2010. Hormonal therapy and sex reassignment: A systematic review and meta-analysis of quality of life and psychosocial outcomes. Clinical Endocrinology 72(2):214–231.
Nanda, S. 1990. Neither man nor woman: The Hijras of India. Belmont, CA: Wadsworth Publishing Company.
Nardi, P. M. 1997. Friends, lovers, and families: The impact of AIDS on gay and lesbian relationships. In In changing times: Gay men and lesbians encounter HIV/AIDS, edited by M. P. Levine, P. M. Nardi, and J. H. Gagnon. Chicago, IL: University of Chicago Press. Pp. 55–82.
NIH (National Institutes of Health). 1997. Interventions to prevent HIV risk behaviors. Bethesda, MD: NIH.
NIH. 2010. FY 2011 trans-NIH AIDS research by-pass budget estimate. Bethesda, MD: NIH.
NRC (National Research Council). 1989. AIDS: Sexual behavior and intravenous drug use. Washington, DC: National Academy Press.
NRC. 1990. AIDS: The second decade. Washington, DC: National Academy Press.
NRC. 1993. The social impact of AIDS in the United States. Washington, DC: National Academy Press.
NRC. 1995. Assessing the social and behavioral science base for HIV/AIDS prevention and intervention: Workshop summary. Washington, DC: National Academy Press.
Nuttbrock, L., W. Bockting, S. Hwahng, A. Rosenblum, M. Mason, M. Marci, and J. Becker. 2009. Gender identity affirmation among male-to-female transgender persons: A life course analysis across types of relationships and cultural/lifestyle factors. Sexual and Relationship Therapy 24(2):108–125.
O’Leary, A., H. H. Fisher, D. W. Purcell, P. S. Spikes, and C. A. Gomez. 2007. Correlates of risk patterns and race/ethnicity among HIV-positive men who have sex with men. AIDS & Behavior 11(5):706-715.
Obedin-Maliver, J., M. R. Lunn, E. Goldsmith, L. Stewart, E. Tran, W. White, M. Wells, S. Brenman, and G. Garcia. 2010, November 5-10. Lesbian, gay, bisexual, and transgender-related content in medical curricula. Paper presented at 2010 Annual Meeting of the Association of American Medical Colleges, Washington, DC.
Oliver, M. B., and J. S. Hyde. 1993. Gender differences in sexuality: A meta-analysis. Psychological Bulletin 114(1):29.
Operario, D., J. Burton, K. Underhill, and J. Sevelius. 2008. Men who have sex with transgender women: Challenges to category-based HIV prevention. AIDS & Behavior 12(1):18–26.
Patterson, C. J. 2000. Family relationships of lesbians and gay men. Journal of Marriage & the Family 62(4):1052–1069.
Patterson, C. J. 2009. Children of lesbian and gay parents: Psychology, law, and policy. American Psychologist 64(8):727–736.
Paul, J. P. 1983. The bisexual identity: An idea without social recognition. Journal of Homosexuality 9(2/3):45–63.
Pauly, I. B. 1968. The current status of the change of sex operation. The Journal of Nervous and Mental Disease 147(5):460–471.
Peplau, L. A., and L. D. Garnets. 2000. A new paradigm for understanding women’s sexuality and sexual orientation. Journal of Social Issues 56(2):329–350.
Peterson, K. 2004. 50-state rundown on gay marriage laws. http://www.stateline.org/live/ViewPage.action?siteNodeId=136&languageId=1&contentId=15576 (accessed December 13, 2010).
Peterson, J. L., and K. T. Jones. 2009. HIV prevention for black men who have sex with men in the United States. American Journal of Public Health 99(6):976–980.
Pettigrew, T. F., and L. R. Tropp. 2006. A meta-analytic test of intergroup contact theory. Journal of Personality and Social Psychology 90:751–783.
Pfäfflin, F., and A. Junge. 1992. Sex reassignment. Thirty years of international follow-up studies after sex reassignment surgery: A comprehensive review, 1961–1991. http://web.archive.org/web/20070503090247/http://www.symposion.com/ijt/pfaefflin/1000.htm (accessed November 17, 2010).
Pleck, J. H., L. O’Donnell, C. O’Donnell, and J. Snarey. 1988. AIDS-phobia, contact with AIDS, and AIDS-related job stress in hospital workers. Journal of Homosexuality 15(3–4):41–54.
Ponce, N. A., S. D. Cochran, J. C. Pizer, and V. M. Mays. 2010. The effects of unequal access to health insurance for same-sex couples in California. Health Affairs hlthaff.2009.0583.
Price, V., and M. L. Hsu. 1992. Public opinion about AIDS policies. The role of misinformation and attitudes toward homosexuals. Public Opinion Quarterly 56(1):29–52.
Pryor, J. B., G. D. Reeder, R. Vinacco, and T. L. Kott. 1989. The instrumental and symbolic functions of attitudes toward persons with AIDS. Journal of Applied Social Psychology 19(5):377–404.
Riggle, E. D., S. S. Rostosky, and S. G. Horne. 2010. Psychological distress, well-being, and legal recognition in same-sex couple relationships. Journal of Family Psychology 24(1):82–86.
Rosario, M., H. F. L. Meyer-Bahlburg, J. Hunter, T. M. Exner, M. Gwadz, and A. M. Keller. 1996. The psychosexual development of urban lesbian, gay, and bisexual youths. Journal of Sex Research 33(2):113–126.
Roscoe, W. 1991. The Zuni man-woman. Albuquerque, NM: The University of New Mexico Press.
Ross, M. W., E. J. Essien, M. L. Williams, and M. E. Fernandez-Esquer. 2003. Concordance between sexual behavior and sexual identity in street outreach samples of four racial/ ethnic groups. Sexually Transmitted Diseases 30(2):110–113.
Rosser, B. R. S., J. M. Oakes, W. Bockting, and M. Miner. 2007. Capturing the social demographics of hidden sexual minorities: An Internet study of the transgender population in the United States. Sexuality Research and Social Policy 4(2):50–64.
Russell, S. T., T. J. Clarke, and J. Clary. 2009. Are teens “post-gay”? Contemporary adolescents’ sexual identity labels. Journal of Youth and Adolescence 38(7):884–890.
Rust, P. C. 1995. Bisexuality and the challenge to lesbian politics: Sex, loyalty, and revolution. New York: New York University Press.
Schatz, B., and K. O’Hanlan. 1994. Anti-gay discrimination in medicine: Results of a national survey of lesbian, gay, and bisexual physicians. San Francisco, CA: American Association of Physicians for Human Rights/Gay Lesbian Medical Association.
Scherzer, T. 2000. Negotiating health care: The experiences of young lesbian and bisexual women. Culture, Health & Sexuality 2(1):87–102.
Sears, B. 2009. Delaware—sexual orientation and gender identity law and documentation of discrimination. Los Angeles, CA: The Williams Institute.
Sepkowitz, K. A. 2001. AIDS—the first 20 years. New England Journal of Medicine 344(23):1764–1772.
Sherrill, K., and A. Yang. 2000. From outlaws to in-laws: Anti-gay attitudes thaw. The Public Perspective 11(1):20–23.
Shilts, R. 1987. And the band played on: Politics, people, and the AIDS epidemic. New York: St. Martin’s Press.
Smith, D. M., and W. C. Mathews. 2007. Physicians’ attitudes toward homosexuality and HIV: Survey of a California medical society-revisited (PATHH-II). Journal of Homosexuality 52(3-4):1–9.
Stall, R., C. Hoff, T. J. Coates, J. Paul, K. A. Phillips, M. Ekstrand, S. Kegeles, J. Catania, D. Daigle, and R. Diaz. 1996. Decisions to get HIV tested and to accept antiretroviral therapies among gay/bisexual men: Implications for secondary prevention efforts. Journal of Acquired Immune Deficiency Syndromes and Human Retrovirology 11(2):151–160.
Steinberger, M. D. 2009. Federal estate tax disadvantages for same-sex couples. Los Angeles, CA: The Williams Institute.
Stewart, M. A. 1995. Effective physician-patient communication and health outcomes: A review. Canadian Medical Association Journal 152(9):1423–1433.
Stipp, H., and D. Kerr. 1989. Determinants of public opinion about AIDS. The Public Opinion Quarterly 53(1):98–106.
Stokes, J. P., and D. J. McKirnan. 1996. Female partners of bisexual men. Psychology of Women Quarterly 20(2):267.
Stoller, R. 1968. Sex and gender: On the development of masculinity and femininity. New York: Science House.
Stone, S. 1991. The empire strikes back: A posttranssexual manifesto. In Body guards: The cultural politics of gender ambiguity, edited by J. Epstein and K. Straub. New York: Routledge. Pp. 280–304.
Stryker, S., and J. Van Buskirk, eds. 1996. Gay by the bay: A history of queer culture in the San Francisco Bay area. San Francisco, CA: Chronicle Books.
Subcommittee on Investigations of the Senate Committee on Expenditures in the Executive Departments. 1950. Interim report: Employment of homosexuals and other sex perverts in government. Washington, DC: U.S. Senate, 81st Congress, 2nd Session.
Terman, L. M. 1948. Kinsey’s sexual behavior in the human male; some comments and criticisms. Psychological Bulletin 45(5):443–459.
Tesar, C. M., and S. L. Rovi. 1998. Survey of curriculum on homosexuality/bisexuality in departments of family medicine. Family Medicine 30(4):283–287.
Thompson, G. N. 1949. Electroshock and other therapeutic considerations in sexual psychopathy. Journal of Nervous and Mental Disease 109(6):531–539.
Torian, L. V., H. A. Makki, I. B. Menzies, C. S. Murrill, and I. B. Weisfuse. 2002. HIV infection in men who have sex with men, New York City Department of Health sexually transmitted disease clinics, 1990-1999: A decade of serosurveillance finds that racial disparities and associations between HIV and gonorrhea persist. Sexually Transmitted Diseases 29(2):73–78.
Turner, C. F., M. A. Villarroel, J. R. Chromy, E. Eggleston, and S. M. Rogers. 2005. Same-gender sex among U.S. adults. Public Opinion Quarterly 69(3):439–462.
U.S. Census Bureau. 2006. General demographic characteristics, 2006 population estimates, United States. http://factfinder.census.gov/servlet/QTTable?-ds_name=PEP_2006_EST&-qr_name=PEP_2006_EST_DP1&-geo_id=01000US (accessed January 14, 2011).
Udis-Kessler, A. 1995. Identity/politics: A history of the bisexual movement. In Bisexual politics: Theories, queries, and visions, edited by N. Tucker. New York: Haworth Press.
Ulrichs, K. H. 1994a. The riddle of “man-manly” love: The pioneering work on male homosexuality, Vol. 2. Translated by M. A. Lombardi-Nash. Buffalo, NY: Prometheus Books.
Ulrichs, K. H. 1994b. The riddle of man-manly love: The pioneering work on male homosexuality, Vol. 1. Translated by M. A. Lombardi-Nash. Buffalo, NY: Prometheus Books.
Vestal, C. 2009. Gay marriage legal in six states. http://www.stateline.org/live/details/story?contentId=347390 (accessed December 13, 2010).
Voeller, B. 1990. Some uses and abuses of the Kinsey scale. In Homosexuality/heterosexuality: Concepts of sexual orientation, edited by D. P. McWhirter, S. A. Sanders, and J. M. Reinisch. New York: Oxford University Press. Pp. 32–38.
Wallick, M. M., K. M. Cambre, and M. H. Townsend. 1993. Freshman students’ attitudes toward homosexuality. Academic Medicine 68(5):357–358.
Wallis, W. A. 1949. Statistics of the Kinsey Report. Journal of the American Statistical Association 44(248):463–484.
Warren, B. 1993. Transexuality, identity, and empowerment: A view from the front lines. SIECUS Report 14–16.
Weinberg, M. S., and C. J. Williams. 2010. Men sexually interested in transwomen (MSTW): Gendered embodiment and the construction of sexual desire. Journal of Sex Research 47(4):374–383.
Weinberg, M. S., C. J. Williams, and D. W. Pryor. 1994. Dual attraction: Understanding bisexuality. New York: Oxford University Press.
Weinrich, J. D., and F. Klein. 2002. Bi-gay, bi-straight, and bi-bi: Three bisexual subgroups identified using cluster analysis of the Klein sexual orientation grid. Journal of Bisexuality 2(4):109–139.
Wertheimer, D. M. 1992. Treatment and service interventions for lesbian and gay male crime victims. In Hate crimes: Confronting violence against lesbians and gay men, edited by G. M. Herek and K. T. Berrill. Newbury Park, CA: SAGE Publications. Pp. 227–240.
White, B. 1952. Ex-GI becomes blonde beauty: Operations transform Bronx youth. New York Daily News, December 1, 1952.
White, R., and A. M. Cunningham. 1991. Ryan White, my own story. New York: Dial Books.
Willging, C. E., M. Salvador, and M. Kano. 2006. Pragmatic help seeking: How sexual and gender minority groups access mental health care in a rural state. Psychiatric Services 57(6):871–874.
Williams, W. 1986. The spirit and the flesh: Sexual diversity in American Indian culture. Boston, MA: Beacon Press.
Worthington, R. L., and A. L. Reynolds. 2009. Within-group differences in sexual orientation and identity. Journal of Counseling Psychology 56(1):44–55.
WPATH (World Professional Association for Transgender Health). 1979. Standards of care for gender identity disorders. http://www.wpath.org/publications_standards.cfm (accessed February 23, 2011).
Xavier, J. M., M. Bobbin, B. Singer, and E. Budd. 2005. A needs assessment of transgendered people of color living in Washington, DC. International Journal of Transgenderism 8(2/3):31–47.
Yawger, N. S. 1940. Transvestism and other cross-sex manifestations. The Journal of Nervous and Mental Disease 92(1):41–48.
Zucker, K. J., and A. A. Lawrence. 2009. Epidemiology of gender identity disorder: Recommendations for the standards of care of the world professional association for transgender health. International Journal of Transgenderism 11(1):8–18.
Zucker, K. J., and R. L. Spitzer. 2005. Was the gender identity disorder of childhood diagnosis introduced into DSM-III as a backdoor maneuver to replace homosexuality? A historical note. Journal of Sex & Marital Therapy 31(1):31–42.
Zucker, K. J., S. J. Bradley, and M. Sanikhani. 1997. Sex differences in referral rates of children with gender identity disorder: Some hypotheses. Journal of Abnormal Child Psychology 25(3):217.
































































