4
Transition to Community Care: Models and Opportunities
The focus of this session, moderated by Julie L. Locher, associate professor of medicine, Division of Gerontology, Geriatrics, and Palliative Care at the University of Alabama at Birmingham, was to identify models of transitioning to community care and opportunities for using these models to provide nutrition services. Presenters James A. Hester, Daniel J. Schoeps, Lori Gerhard, and Heather Keller each provided a discussion of specific models of transitional care and providing services in the community setting. The models discussed were the following:
• Centers tor Medicare & Medicaid Services Innovation Center Models
— Patient Care Model
— Seamless Coordinated Care Model
— Community and Population Health Models
• Veterans Directed Home- and Community-Based Services Program
• Canadian Models of Screening and Assessment in the Community
• Evergreen Action Nutrition Program in Canada
INNOVATIONS IN CARE TRANSITIONS: AN OVERVIEW
The Center for Medicare and Medicaid Innovation, known as the Innovation Center, is a new vehicle for improving care transitions said
James Hester, the Acting Director of the Population Health Models Group at the Innovation Center in the Centers for Medicare & Medicaid Services (CMS). The Innovation Center was created under the Patient Protection and Affordable Care Act Section 3021, to “test innovative payment and service delivery models to reduce program expenditures…while preserving or enhancing the quality of care” for those who get Medicare, Medicaid, or Children’s Health Insurance Program benefits (P.L. 111-148 [May 2010]). The Innovation Center’s mission is to be a trustworthy partner to identify, validate, and diffuse new models of care and payment that improve health and health care and reduce the total cost of care.
The Innovation Center: History and Organization
To begin, Hester posed the question, “Why should we innovate?” He suggested that innovation is a tool that can be used to decrease Medicaid and Medicare expenditures through improved care, thereby reducing the country’s budget deficit. Hester also pointed to statistics that show 20 percent of Medicare recipients discharged from the hospital (11.8 million people) are readmitted within 30 days (Jencks et al., 2009). Many of those are readmitted due to preventable hospital-acquired conditions. He noted, however, the ultimate reason for innovation is the medical community’s obligation to provide better health care.
The Innovation Center has $10 billion in funding through 2019 and has been given authority under the Patient Protection and Affordable Care Act that disables some of the constraints on Medicare demonstrations, particularly in regard to budget neutrality (P.L. 111-148, Sec. 2705). Hester explained that the budget neutrality requirement eliminated many promising innovations. If an innovation has been implemented, tested, and found to work effectively, “the Secretary can scale it up nationally” without having to return to Congress for new legislation.
The work of the Innovation Center is organized into three major model groups: (1) the Patient Care Model, (2) the Seamless Coordinated Care Model, and (3) Community and Population Health Models. The Patient Care Model focuses on what happens to a patient in a given episode of care at a given encounter. One initiative under this model is “bundled payments” in which multiple caregivers (e.g., from the surgeon to the postacute care facility) are reimbursed for treatment of a patient as a single episode with a single payment, thereby providing incentive for everyone to work together effectively. A second example of this model is Partnerships for Patients, a public-private partnership for a national patient safety campaign. (See below for further discussion of this initiative.)
The Seamless Coordinated Care Model involves coordinating care across the entire spectrum of the health community to improve health
outcomes for patients. Hester stated that the existing health care system characteristically consists of “silos” within specific care settings resulting in rough transitions between the settings. Initiatives under the Seamless Coordinated Care Models that attempt to address this issue include the Multipayer Advanced Primary Care Practice demonstration project, the Pioneer Accountable Care Organizations (ACO) Model, and the Comprehensive Primary Care initiative.
The Community and Population Health Model explores how to improve the health of targeted populations with specific diseases, such as diabetes, as well as the well-being of communities as a whole. At-risk communities represent opportunities for improving health; and enhancing nutritional status is an aspect of health that can be pursued.
The Innovation Center solicits ideas for new models, selects the most promising, tests and evaluates the models, and finally disseminates the successful models. The measures of success are better health care experiences for patients, better health outcomes for populations, and reduced costs of care through improvement.
The Partnership for Patients Initiative mentioned above has two main goals: (1) a 40 percent reduction in preventable hospital-acquired conditions over 3 years and (2) a 20 percent reduction in 30-day readmissions in 3 years. Success in meeting these two goals could result in saving 60,000 lives and $35 billion in 3 years (CMS, 2011a). According to Hester, bipartisan support has been garnered due to the realization that improved patient outcomes through fewer preventable acquired conditions and fewer readmissions will result in large cost savings.
Care Transitions
Hester focused his discussion on the second goal (decreased readmissions) and noted that transition from one source of care to another is a period of high risk for communication failure, procedural errors, and unimplemented plans. He emphasized that the issue of poor care transitions and readmissions is concentrated in the most vulnerable populations—people with chronic conditions, organ system failure, and frailty. Hester indicated there is strong evidence demonstrating that hospital readmissions caused by flawed transitions can be significantly reduced.
The vision for successful care transitions, as outlined by Hester, is a care system in which each patient with complex needs has a plan that guides all care, moves with the patient across care settings, reflects the priorities of patient and family, and meets the needs of persons living with serious chronic conditions. Accomplishing that vision requires a combination of patient and caregiver engagement, patient-centered care plans, safe medication practices, and communication between the transferring and receiving
providers. Importantly, the sending provider must maintain responsibility for the care of the patient until the receiving caregiver confirms the transfer and assumes responsibility, as opposed to a presumption that the transition went smoothly and the patient is well.
In order to achieve the goal of a 20 percent reduction in hospital readmissions, the Innovation Center estimated that a national network of 2,600 community-based care transition coalitions, partnering hospitals with community resources, would have to be built. Furthermore, a “roadmap” would be needed to help guide partnerships. The Partnership for Patients is building on evidence from research and pilot projects to support existing coalitions and encourage the formation of new ones. The Center provides data, technical support, money, consumer information, and training to support the partnerships and move the coalition forward in transition care.
The Innovation Center’s strategy for the Partnership for Patients1program was to create very broad public-private partnerships; both commercial and philanthropic organizations have been involved. The aim was to have a portfolio of initiatives between communities and hospitals at various levels of development in providing transitional care. The Center established a simple hierarchy of these partnerships based on the level of their development, labeling them “walkers,” “joggers,” and “marathoners.”
“Walkers” are the partnerships that are just beginning. Initiatives in place for “walkers” include the Quality Improvement Organizations (QIOs) and the Health Resources and Services Administration Patient Safety and Clinical Pharmacy Services Collaborative. QIOs are organizations staffed by health care professionals trained to review the medical care of beneficiaries and implement improvements in the quality of care. They provide technical assistance and other support to communities and hospitals in all 50 states, territories, and the District of Columbia. CMS enters into 3-year contracts, labeled as consecutively numbered Statements of Work (SOW), with the QIOs (CMS, 2011b). The QIO “9th SOW focused on improving the quality and safety of health care services to Medicare beneficiaries” (CMS, 2008). Lessons learned from the QIO 9th Scope of Work Care Transitions Theme include the importance of community collaboration, tailoring solutions to fit community priorities, including patients and families in decisions, and public outreach activities.
Hester said the main initiative for the “joggers” is the Community-Based Care Transitions Program (CCTP). CCTP, mandated by Section 3026 of the Patient Protection and Affordable Care Act (P.L. 111-148 [May 2010]), provides the opportunity for community-based organizations (CBOs) to partner with hospitals to improve transitions from hospitals
____________________
1 Information on the Partnership for Patients campaign is available at http://www.healthcare.gov/center/programs/partnership/join/index.html.
to other care settings. The CCTP has $500 million available to support these partnerships and applications are now being accepted. The money is funneled through the CBOs, as opposed to the provider organizations, in order to strengthen the role of the CBO and strengthen the partnerships. The goals of the CCTP are to improve transitions of beneficiaries from the inpatient hospital setting to home or other care settings, reduce readmissions for high-risk beneficiaries, and document measurable savings to the Medicare program.
The final category of partnerships, the “marathoners,” combines the seamless care initiatives of Bundled Payments for Care Improvement and ACOs.
Summary
Hester concluded by suggesting issues to be contemplated when considering care transitions:
• Examine how to build effective hospital-CBO partnerships and create an infrastructure of local CBOs where it does not exist.
• What are the key elements of a care plan? In particular, how can nutrition needs be incorporated into the care plan? Hester noted that needs should be identified; an effective entity for responding to those needs must be created that can recognize and seize the opportunity when the patient will be receptive to delivery of services.
• What payment policy changes are required to sustain better care transitions? Hester encouraged the audience to consider a sustainable payment and business model that can support services in the community over time.
Veterans Directed Home- and Community-Based Services
Lori Gerhard, Director of the Office of Program Innovation and Demonstration for the U.S. Administration on Aging (AoA), opened the presentation by stating that AoA and the Veterans Health Administration (VHA) are interested in continuing to work together with registered dietitians and the nutrition community because nutrition is vital to helping people maintain their independence, health, and well-being and enabling them to be engaged in community life. Gerhard and Daniel J. Schoeps, Director of the Purchased Long-Term Care Group in the Office of Geriatrics and Ex-
tended Care at the Department of Veterans Affairs, presented on the role of the Veterans Directed Home- and Community-Based Services Program (VD-HCBS) in transitioning veterans to home- and community-based settings. The program has been under way for 3 years and lends itself to future models that can enable AoA and VHA to better serve people.
Historical Context and Development of the VD-HCBS Program
Schoeps provided a brief description of the Department of Veterans Affairs (VA), focusing on the VHA. The VHA has a $60 billion budget and 6 million veterans who use its services for health care in any given year. The VHA has 153 medical centers and 950 community-based outpatient clinics, 135 nursing homes, and 47 residential rehabilitation treatment centers. It is also affiliated with 107 medical schools, 55 dental schools, and 1,200 other schools for training and education purposes. Patient care, education, research, and backup to the Department of Defense in national emergencies are the four main missions of the VHA.
The partnership between VHA and AoA began over 35 years ago; however, the VD-HCBS has significantly changed the dynamic of that partnership. The organizations attempt to merge their expertise without duplicating activities. Veterans enrolled in VD-HCBS are in transition, such as those
• recently discharged from an inpatient hospital or nursing home setting,
• referred to VD-HCBS after an outpatient clinic visit,
• waiting to be admitted to a nursing home,
• recently admitted to a nursing home, or
• receiving traditional home care services but with insufficient quantity of support.
Veterans admitted into this program need to choose to participate because participation involves much work on their part. Potential clients for this program may be identified from the waiting list for a nursing home or as veterans who may be reconsidering their recent admission to a nursing home. Schoeps said that, through VD-HCBS, often clients can be offered more hours of care at home for the same cost of care they would receive through traditional services.
Gerhard continued by explaining the VHA was seeking a participantdirected model to engage the veteran in the design and delivery of his or her own care. At the same time, AoA was preparing to launch a demonstration grant program to reach older adults at risk of nursing home placement and
of spend-down to Medicaid2 to help them stay in the community. AoA was able to leverage that work to begin to develop VD-HCBS.
The research and programs that formed the basis to develop VD-HCBS included the following:
• National Long-Term Care Channeling Demonstration
• Do No ninstitutional Long-Term Care Services Reduce Medicaid? (Kaye et al., 2009)
• Chronic Care Model and Evidence-Based Care Transition Research
• Cash and Counseling Demonstration and Evaluation
• Stanford University Chronic Disease Self-Management Program Research
National Long-Term Care Channeling Demonstration
The Department of Health and Human Services (HHS) funded the National Long-Term Care Channeling Demonstration in 1980 as a model in 10 states to evaluate whether there was a way to change service delivery that would enable the government to serve the magnitude of people expected to need services in the future. The demonstration examined whether older adults who were enrolled in a program providing screening, assessment, care planning, service arrangements, follow-up, and reassessment could remain in the community, thereby avoiding placement in an institutional setting. The results showed no difference in the use of institutional care services, but other outcomes suggested further programming and evaluation were warranted. These outcomes included greater client satisfaction with life and the quality of care being received, as well as increased confidence in services being delivered and a reduction of unmet client needs (HHS ASPE, 1991). Gerhard indicated unmet needs are a risk factor for unnecessary admission to hospitals.
Do Noninstitutional Long-Term Care Services Reduce Medicaid?
The channeling demonstration gave way to the idea of the “woodwork effect.” That is the concept that if access to home- and community-based services is expanded, the increased participation combined with continued nursing home expenditures raises the total cost of providing services to older adults for long-term care. However, more recent research done by Kaye et al. (2009) does not support this concept. Study results showed that, in the states that had robust home- and community-based service programs,
__________________
2 The process of spending down one’s assets to qualify for Medicaid. To qualify for Medicaid Spend-Down, a large part of one’s income must be spent on medical care.
spending initially increased at a rapid pace because access to services was expanding. However, the increase was followed by a drop to a level of expenditure that was less than the original amount being spent, serving more people with fewer dollars. The results of this research began to inform AoA’s and VHA’s ongoing work.
Chronic Care Model and Evidence-Based Care Transition Research
The Chronic Care Model developed by Edward Wagner (see Figure 3-1) not only involves active patient participation, it also engages the larger community in the system. This model encourages coupling the strengths from the health care system and community resources to leverage opportunities to support the citizens in that community to have better health outcomes and quality of life (Wagner, 1998; Wagner et al., 2001). Evidence-based care transition research conducted by various scientists has shown how to form partnerships with people transitioning from hospital to home to facilitate, empower, and activate them to take control of their health and thrive in the community (Boult et al., 2008; Coleman, 2011; Counsell et al., 2006; Naylor et al., 2009).
Cash and Counseling Demonstration and Evaluation
The Cash and Counseling Demonstration and Evaluation, directed by Kevin Mahoney (Doty et al., 2007; Mahoney, 2005), was a concept tested in three states in which older adults received counseling and a flexible budget to personally obtain the care and services they most needed to remain in the community. Evaluation of this demonstration revealed higher satisfaction with care and services by both the individuals receiving care and their caregivers and reduced unmet needs of those requiring personal assistance. Medicaid personal care costs were somewhat higher, mainly because participants received more of the care they were authorized to receive. Gerhard explained that, under traditional delivery service systems, at times caregivers do not arrive to provide home care when scheduled, so the authorized care is not received. Under the Cash and Counseling Demonstration, participants were hiring family, friends, or neighbors and, thus, there was a higher reliability that services were delivered. The increased Medicaid personal care costs were partially offset by savings in institutional and other long-term care costs (NRCPDS, 2011).
Stanford University’s Chronic Disease Self-Management Program
The last piece of research used was Stanford University’s Chronic Disease Self-Management Program (CDSMP). This community-based program
was designed to teach self-management skills to individuals with chronic disease conditions to improve health behaviors and outcomes (Lorig et al., 1999, 2001). HHS has contributed funding to this program since 2003, most recently under the American Recovery and Reinvestment Act, establishing CDSMPs for people with multiple chronic conditions in 45 states, the District of Columbia, and Puerto Rico.
Gerhard closed by noting that VD-HCBS is a partnership between administrative infrastructures. The goal for AoA is to assist the VA with rebalancing Long Term Services and Supports, which is currently spending about 80 percent of its budget on institutional care.
VD-HCBS Key Components
VD-HCBS provides veterans of all ages participant-directed HCBS options and empowers them to direct their own care. The goals of VD-HCBS are to increase the range of choices beyond traditional services and to provide the opportunity and ability for veterans to participate in design of services and planning of allocations for services. Veterans receive a participant-directed assessment performed in collaboration with an options counselor to develop a care plan. Together they manage a flexible service budget and decide what mix of goods and services will best meet their specific needs to live independently in the community. Each individual has his or her own unique situation and circumstances, so the veteran may hire and supervise their own service providers, including family or friends, and purchase items or other services to fill the gaps in care in a way that is most beneficial for the individual.
Another key component of VD-HCBS is the establishment of financial management services (FMS) entities throughout the country to assist the veterans with the management of their flexible service budget. The veteran is essentially an employer who must hire caregivers, negotiate rates for services and schedules, and provide a paycheck, which involves withholding taxes. The FMS entity assists with these tasks and issues fiscal reports on a monthly basis to the aging network engaged in the delivery of care to be able to ensure the fiscal accountability of the program.
Operations and Discovery
Schoeps reported that there are currently 33 operational VA Medical Center programs collaborating with 81 Area Agencies on Aging and Aging and Disability Resource Centers. Figure 4-1 indicates these locations as well as planned program sites.
Schoeps also highlighted discoveries made in the course of operating this program, saying it has been enlightening to see the types of services
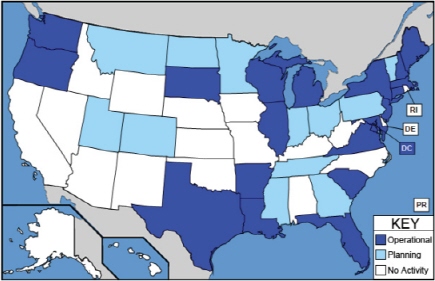
FIGURE 4-1 VD-HCBS operational and planned sites.
SOURCE: Schoeps and Gerhard, 2011.
the veterans are selecting and what they consider valuable. The majority choose to use their funds for personal care services, but other services have also been purchased. Schoeps gave an example of a young traumatic brain-injured veteran who needed to run. The vet identified someone to run with him and used his allotted money to pay for the service. The program will review invoices to learn what other new purchased services emerge. The VHA will also examine the relative cost of the VD-HCBS program as compared to the cost of traditional home care. Schoeps concluded by saying that the veterans-directed program has been well received by veterans and their families.
IMPROVING COMMUNITY NUTRITION CARE FOR OLDER ADULTS IN CANADA
Transition care in Canada is somewhat fractured according to Heather Keller, a professor in the Department of Family Relations and Applied Nutrition at the University of Guelph in Ontario and a research scientist with the RBJ Schlegel-University of Waterloo Research Institute of Aging.
Although the Canadian Healthcare Act ensures that nationally all Canadian citizens receive universal health care, community health programs are very individualized and regionalized. Of the 34 million people in Canada, 14 percent of Canadians are over the age of 65 (Statistics Canada, 2011).
Keller discussed the role of nutrition screening in the context of a prevention model. In the community setting, screening is conducted on people who are asymptomatic in order to classify them as either likely or unlikely to have a specific disease (Morrison, 1992) or to identify nutritional risk (Posthauer et al., 1994). In an acute care setting, patients are already symptomatic and have significant risk factors.
Keller developed a process (see Figure 4-2) that examines the sectors of care around three levels of prevention. The process begins with primary prevention under the purview of public health units, which are funded by the ministries of health in each province, and primary care physicians. For example, dietitians may provide global messages about eating well that reach the entire population.
Secondary prevention includes early identification of asymptomatic people who are likely to experience health problems in attempts to prevent or delay progression of such problems. At this step in the process, screening is crucial and should be undertaken in the community. Secondary prevention efforts are carried out at social services agencies and wellness programs in the community, in addition to public health units and primary care offices. Primary care varies across Canadian provinces. For example, Ontario uses family health teams—dietitians, social workers, and kinesiologists located in doctors’ offices conducting secondary prevention and treatment programs. Community services available to older adults in Canada at this level include meal programs, senior centers, transportation, and grocery delivery.
Tertiary prevention seeks to keep individuals who have already developed a chronic condition from declining in health, which Keller said is the goal of home care programs in Canada and nutrition programs for older adults in the United States. Tertiary prevention involves social service agencies, outpatient clinics, home care, and hospitals and includes typical medical model services, such as referrals to registered dietitians. The goal at the tertiary level is to keep older adults out of more expensive systems, such as nursing homes, which can actually contribute to further declines in their health.
Screening and Assessment
Keller posed the question, “How can screening promote secondary prevention?” Screening can identify the nutritional needs of older adults, thereby enabling services to be provided and appropriate referrals to be
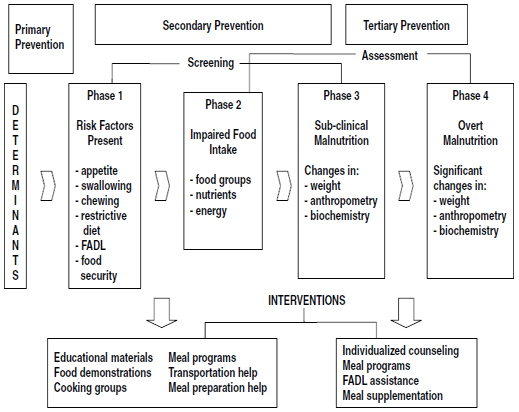
FIGURE 4-2 Screening and assessment across the continuum of care for older Canadians.
NOTE: FADL, food-related activities of daily living.
SOURCE: Adapted from H. H. Keller. 2007. Promoting food intake in older adults living in the community: A review. Applied Psychology, Nutrition and Metabolism 32(6):991–1000 © 2008 Canadian Science Publishing or its licensors. Reproduced with permission.
made to other community programs. It can also raise awareness of nutrition and health risks for the older adults and their families, prompting behavior change.
Screening and assessment can be thought of as overlapping activities that occur across four phases which make up a continuum of malnutrition (Figure 4-2). Initially, the health care professional reviews risk factors that may contribute to impaired food intake, such as poor appetite. The next phase involves progression of risk factors so that food intake is impaired, while the third phase is the presence of subclinical malnutrition identified by either screening or assessment as identified by changes in anthropometric and biochemical measurements. Significant anthropometric, biochemical, and functional changes as seen in phase 4 indicate overt malnutrition, which is the end state assessed only with a comprehensive assessment.
Interventions that may be implemented as a result of screening in phases 1 and 2 would center on food-related activities of daily living, such as grocery shopping, cooking, meal delivery, meal preparation, and transportation. Assessment during the later phases would require additional higher-end interventions, including individualized counseling, meal programs, and meal supplementation.
Keller described SCREEN, a paper-and-pencil nutrition risk tool used to evaluate older adults in the community. SCREEN stands for Seniors in the Community: Risk Evaluation for Eating and Nutrition and can be self-administered or completed by an interviewer. SCREEN was validated against the criterion of a dietitian’s assessment of nutritional risk and demonstrated test-retest reliability and an intermodal and inter-rater reliability. SCREEN is not only a tool, but a screening program that includes a referral process to services and educational needs based on identified risk items (Keller, 2007; Keller et al., 2006a).
Keller described an ethical screening process involving identification of an individual at risk through initial screening, followed by a referral to a physician or dietitian for nutritional assessment and treatment if necessary. The individual may also be referred to other professionals and services, such as a social worker or family counselor. Subsequently, since a new program of care was implemented, the client restarts the cycle of rescreening to be monitored continuously.
She then reviewed a screening demonstration project conducted with 1,200 older adults in five diverse communities in Canada. A referral system was developed to link the adults with services in their communities. For example, if they were identified as high risk at a Meals On Wheels Program, they could be referred to receive more meals, a congregate dining program, or a dietitian. Sixty percent of those identified as “at risk” refused referrals because they either felt their current services were sufficient or did not feel nutrition was a priority for them at that point. Of those referred, 62 per-
cent were referred to a dietitian but faced barriers related to long waiting times, cost, access, and doctors unwilling to make the necessary referral. Twenty-three percent of referrals were to the Meals On Wheels program, but reported barriers to participation included cost and dislike of the food (Keller et al., 2007).
Keller mentioned a small pilot study illustrating that behavior and knowledge can be changed through provision of an education pamphlet and administration of a screening tool alone (Southgate et al., 2010), suggesting that self-management of screening might be a consideration.
Over the past year, Keller has been collaborating with dietitians in Canada to develop an Internet version of SCREEN (www.eatrightontario.ca/escreen/) for older adults. It is a self-management tool, allowing older adults to assess their own nutritional risk. The screening tool guides the individual to credible educational resources and activities that can assist in changing his or her behavior.
Other Research
A study being conducted by the Canadian Malnutrition Task Force is examining the prevalence of malnutrition upon admission to and discharge from the hospital; the nutrition process during the hospital stay; and outcomes at 30 days, including readmission and mortality. To date, 10 hospitals are collecting data and expect to have studied 500 patients by the end of the year; the goal is 1,000 patients. Using Subjective Global Assessment and albumin status, preliminary data from 160 patients indicate that 45 percent of people admitted were malnourished. At discharge, although the percentage is reduced, 35 percent are still in a malnourished state. Keller surmised that these data are indicative of the malnutrition that occurs in the community and demonstrate that Canada and the United States experience the same problems with transitional care.
In another study, conducted by Keller and McKenzie (2003), vulnerable older adults across Canada who participated in home care and Meals On Wheels were surveyed to determine their nutrition-related risk factors. Results are shown in Table 4-1.
Community Services in Canada
Keller noted that Canada does not have an elder nutrition program comparable to that of the AoA. She explained this may be in part because the base-level annual income for persons over the age of 65 in Canada is $15,000 and perhaps this supports free medical care, medications, and access to home care if eligibility criteria are met. However, Keller explained that home care is not part of the act in which national health care is pro-
TABLE 4-1 Percent of Older Canadians Reporting Nutrition-Related Risk Factors
| Nutrition-Related Risk Factor | Percent of Participants Reporting Risk Factor |
| Difficulty shopping | 69 |
| Low fruit and vegetable intake | 48 |
| Restricts food intake | 45 |
| Difficulty cooking | 42 |
| Difficulty chewing | 34.6 |
| Weight change | 33 |
| Poor appetite | 28 |
| Difficulty swallowing | 22.9 |
| Weight loss | 22 |
SOURCE: Keller and McKenzie, 2003.
vided to every citizen in Canada. It is considered an extended service, and services can vary among provinces or even communities within a province.
The Inter-RAI Home Care Assessment System3 is used in several provinces to screen for advanced nutrition problems, such as unintended weight loss of 5 percent in 30 days, cachexia, or enteral nutrition. Keller indicated that relatively few people (e.g., < 20 percent) in home care trigger the need for a dietitian service using this assessment, although Keller believes that in reality many of participants are malnourished. In Keller’s opinion, the use of this tool does not adequately identify those people with unmet nutritional needs whose health may be improved with nutrition services that can prevent further decline.
In general throughout Canada, meal programs are arranged through referral to social service agencies, long-term care hospitals, Red Cross programs, or similar organizations. Government funding for meal programs is nonexistent, apart from a small amount of subsidies for which organizations must apply. Meal services are primarily financially supported by philanthropic programs or fee-for-service payments (fees vary by location) and are delivered by volunteers. Home aides also prepare meals and assist with basic activities, but the services provided vary by province.
The Evergreen Action Nutrition Program is an example of a successful community education and secondary prevention program in Canada. It was developed to provide some of the services and information that seniors want—food workshops, cooking classes for older men, and information
____________________
3 A person-centered assessment system, focusing on the person’s functioning and quality of life by assessing needs, strengths, and preferences, that informs and guides comprehensive care and service planning in community-based settings (http://www.interrai.org/section/view/?fnode=15).
to support behavioral changes to improve dietary intake. The program was funded for 3 years at $70,000 through a research grant. Through this program fruit and vegetable intake improved, men learned new cooking skills, 94 percent of participants reported increased nutrition knowledge, and 50 percent of participants reported increased pleasure from eating (Keller et al., 2004, 2005, 2006b). In the diabetes support groups, 50 percent of participants changed their diet, 56 percent lost excess weight, and 50 percent had lower blood sugars (Keller, unpublished data).
Summary
Keller summarized the highlights of her presentation, noting that the nutrition problems in Canada are consistent with those in the United States. She stated that older adults want to improve their nutrition, are motivated to do so, and can implement secondary prevention interventions. Although screening programs can lead to secondary prevention and be models for producing linkages to services in the community, there is inadequate funding for secondary prevention in Canada. Finally, there is a place for selfmanagement of nutrition needs which requires support in Canada.
Keller suggested that research priorities include the following:
• Demonstrating the effectiveness of nutrition screening programs in the community
• Identifying best practices for transition to the community from the hospital and answering questions such as “What forms of communication are needed between sectors?”
• Exploring the use of a social care model versus a medical need model for home care services
DISCUSSION
The discussion focused on nutrition in transitional care and patientdirected care of the frail.
Nutrition in Transitional Care
Gordon Jensen asked about concrete plans for transitional care—specifically related to nutrition concerns—from acute care, subacute care, or chronic care back home to independent living for people at high risk of readmission. Locher proposed that a significant barrier to providing nutri-
tion services during transitional care is reimbursement for registered dietitians (RDs) to provide such services in the community setting. Although hospitals and home health care agencies are required to have RDs on staff, in the community setting the mechanism for an RD to independently request reimbursement is cumbersome and the amount so minimal it is not to the dietitian’s benefit to seek reimbursement. Hester pointed to the Section 3026 Community-Based Care Transition Program as an ideal vehicle for a local community organization in partnership with the hospital to design a nutrition intervention. Flexibility is given to the community to determine priorities in needed services. A proposal, which includes nutrition services requiring the support of an RD, could be developed and then the payment model would be included. Therefore, he suggested the goal should be to raise the awareness of the communities that nutrition needs to be a key part of transition care when developing specific proposals. He continued by saying to the extent that the focus is on a patient-centered model, noting the importance of listening to the patients and patient-driven goals as Eric Coleman discussed, the task is to determine how to increase patients’ awareness of their nutritional needs in order to make nutrition services a priority among their requests.
Gerhard suggested that, as the consumer gets more involved, RDs should consider ways to package their services in a way that consumers with funds could purchase them.
Nancy Wellman asked whether a list of available services is provided through CMS or the VD-HCBS and, if so, is nutrition one of the services listed? Schoeps replied that the VD-HCBS does have a list of services that includes nutrition. Hester stated that Section 3026 does not offer a list of potential services, as it is left to the community to determine the appropriate mix of services to provide based on a root-cause analysis of the patients in their community and then develop a proposal. It is not a prescriptive program, but provides flexibility to meet individual community needs.
Patient-Directed Care of the Frail
A participant suggested that patient-directed care is not realistic for the frail older adult, since the responsibilities would be more than such a person is able to manage and caregivers are already overwhelmed. Gerhard reported that people with disabilities have expressed the belief that they know best how to train caregivers to provide care to them. Schoeps said the majority of veterans enrolled in VD-HCBS are older persons, many of whom choose to have a representative make the day-to-day decisions (e.g., a spouse). Additionally, the financial management services entities complete much of the paperwork involved in employing a caregiver.
Connie Bales suggested that nutrition services are about changing be-
haviors, which is different than assisting with physical needs. She questioned, “How do we let the patient decide what’s good for them when they don’t know [what that is]?” Keller responded that screening can be a very effective tool in raising self-awareness of health-related issues. She proposed the self-directed model can come with screening, because sometimes people do not know what their needs are until confronted with a screening tool that identifies an issue that indicates a health risk. For example, it may be that if the person has a poor appetite, he or she may realize that is not normal, but until they have a conversation with a health care provider about this risk and learn that there are services available (e.g., congregate dining) that may help, they are not typically going to see the need for the service.
REFERENCES
Boult, C., L. Karm, and C. Groves. 2008. Improving chronic care: The “guided care” model. The Permanente Journal 12(1):50–54.
CMS (Centers for Medicare & Medicaid Services). 2008. CMS Awards Contracts for Quality Improvement Organizations’ 9th Statement of Work. https://www.cms.gov/qualityimprovementorgs/downloads/9thsowannouncement080508.pdf (accessed November 3, 2011).
CMS. 2011a. Partnership for Patients. http://innovations.cms.gov/areas-of-focus/patient-care-models/partnerships-for-patients/ (accessed November 3, 2011).
CMS. 2011b. Quality Improvement Organizations. https://www.cms.gov/qualityimprovementorgs/ (accessed November 3, 2011).
Coleman, E. A. 2011. The Care Transitions Program®. http://www.caretransitions.org/ (accessed December 12, 2011).
Counsell, S. R., C. M. Callahan, A. B. Buttar, D. O. Clark, and K. I. Frank. 2006. Geriatric Resources for Assessment and Care of Elders (GRACE): A new model of primary care for low-income seniors. Journal of the American Geriatrics Society 54(7):1136–1141.
Doty, P., K. J. Mahoney, and L. Simon-Rusinowitz. 2007. Designing the Cash and Counseling Demonstration and Evaluation. Health Services Research 42(1 Pt II):378–396.
HHS ASPE (U.S. Department of Health and Human Services Office for the Assistant Secretary for Planning and Evaluation). 1991. National Long-Term Care Channeling Demonstration: Summary of Demonstration and Reports. Washington, DC: HHS ASPE. http://aspe.hhs.gov/daltcp/reports/chansum.pdf (accessed December 22, 2011).
Jencks, S. F., M. V. Williams, and E. A. Coleman. 2009. Rehospitalizations among patients in the Medicare Fee-for-Service Program. New England Journal of Medicine 360(14):1418–1428.
Kaye, H. S., M. P. LaPlante, and C. Harrington. 2009. Do noninstitutional long-term care services reduce Medicaid spending? Health Affairs 28(1):262–272.
Keller, H. H. 2007. Promoting food intake in older adults living in the community: A review. Applied Physiology, Nutrition and Metabolism 32(6):991–1000.
Keller, H. H., and J. D. McKenzie. 2003. Nutritional risk: In vulnerable community-living seniors. Canadian Journal of Dietetic Practice and Research 64(4):195–201.
Keller, H. H., A. Gibbs, S. Wong, P. D. Vanderkooy, and M. Hedley. 2004. Men can cook! Development, implementation, and evaluation of a senior men’s cooking group. Journal of Nutrition for the Elderly 24(1):71–87.
Keller, H. H., M. R. Hedley, T. Hadley, S. Wong, and P. D. Vanderkooy. 2005. Food workshops, nutrition education, and older adults: A process evaluation. Journal of Nutrition for the Elderly 24(3):5–23.
Keller, H. H., B. Brockest, and H. Haresign. 2006a. Building capacity for nutrition risk screening. Nutrition Today 41(4):164–170.
Keller, H. H., M. R. Hedley, S. S. L. Wong, P. Vanderkooy, J. Tindale, and J. Norris. 2006b. Community organized food and nutrition education: Participation, attitudes and nutritional risk in seniors. Journal of Nutrition, Health and Aging 10(1):15–20.
Keller, H. H., H. Haresign, and B. Brockest. 2007. Process evaluation of Bringing Nutrition Screening to Seniors in Canada (BNSS). Canadian Journal of Dietetic Practice and Research 68(2):86–91.
Lorig, K. R., D. S. Sobel, A. L. Stewart, B. W. Brown Jr., A. Bandura, P. Ritter, V. M. Gonzalez, D. D. Laurent, and H. R. Holman. 1999. Evidence suggesting that a chronic disease self-management program can improve health status while reducing hospitalization a randomized trial. Medical Care 37(1):5–14.
Lorig, K. R., P. Ritter, A. L. Stewart, D. S. Sobel, B. W. Brown Jr., A. Bandura, V. M. Gonzalez, D. D. Laurent, and H. R. Holman. 2001. Chronic disease self-management program: 2-year health status and health care utilization outcomes. Medical Care 39(11):1217–1223.
Mahoney, K. J. 2005. Cash & Counseling: Congressional Briefing. http://www.allhealth.org/briefingmaterials/Mahoney-194.pdf (accessed November 30, 2011).
Morrison, A. S. 1992. Screening in chronic disease. In Monographs in Epidemiology and Biostatistics, 2nd ed. New York: Oxford University Press.
Naylor, M. D., P. H. Feldman, S. Keating, M. J. Koren, E. T. Kurtzman, M. C. MacCoy, and R. Krakauer. 2009. Translating research into practice: Transitional care for older adults. Journal of Evaluation in Clinical Practice 15(6):1164–1170.
NRCPDS (National Resource Center for Participant-Driven Services). 2011. Cash & Counseling. http://www.bc.edu/schools/gssw/nrcpds/cash_and_counseling.html (accessed November 30, 2011).
Posthauer, M. E., B. Dorse, R. A. Foiles, S. Escott-Stump, L. Lysen, and L. Balogun. 1994. Identifying patients at risk: ADA’s definitions for nutrition screening and nutrition assessment. Journal of the American Dietetic Association 94(8):838–839.
Schoeps, D. J., and L. Gerhard. 2011. The Veterans Directed Home & Community Based Services (VD-HCBS) Program. Presented at the Institute of Medicine Workshop on Nutrition and Healthy Aging in the Community. Washington, DC, October 5–6.
Southgate, K. M., H. H. Keller, and H. D. Reimer. 2010. Determining knowledge and behaviour change: After nutrition screening among older adults. Canadian Journal of Dietetic Practice and Research 71(3):128–133.
Statistics Canada. 2011. Canada’s Population Estimates: Age and Sex. http://www.statcan.gc.ca/daily-quotidien/110928/dq110928a-eng.htm (accessed November 28, 2011).
Wagner, E. H. 1998. Chronic disease management: What will it take to improve care for chronic illness? Effective Clinical Practice 1(1):2–4.
Wagner, E. H., B. T. Austin, C. Davis, M. Hindmarsh, J. Schaefer, and A. Bonomi. 2001. Improving chronic illness care: Translating evidence into action. Health Affairs 20(6):64–78.




















