This chapter provides information to support the committee’s conclusions and recommendations, presented in Chapter 4, for how to establish a baseline of health insurance and health care access for people with HIV in the United States prior to 2014 when key provisions of the Patient Protection and Affordable Care Act (ACA) (P.L. 111-148) are scheduled to be implemented (Statement of Task, subquestions a and b), and for how to continue to obtain data from a large sample of people with HIV to monitor the impact of the ACA on access to health insurance and health care access after 2014 (Statement of Task, subquestion c). In the context of describing how to monitor the impact of the ACA after 2014, the committee discusses an existing surveillance project conducted by the Centers for Disease Control and Prevention (CDC) called the Medical Monitoring Project (MMP) that is designed to obtain nationally representative estimates of the clinical and behavioral characteristics of HIV-diagnosed individuals in care. The committee presents an overview of the project’s design and its strengths and weaknesses for generating nationally representative estimates of HIV care and coverage for people with HIV. The committee also discusses how data from Medicaid, Medicare, and the Ryan White HIV/AIDS Program, which are currently the most common sources of health care coverage for people with HIV, as well as data from private health insurers, might be used to characterize the health care experiences of people with HIV.
The HIV Cost and Services Utilization Study (HCSUS) was the first study designed to produce nationally representative estimates of people with HIV regularly receiving medical care (Shapiro et al., 1999). Active from 1994 to 2000, the HCSUS was a prospective cohort study involving
approximately 3,000 participants. HCSUS participants were interviewed several times over a 3-year period (a baseline interview with follow-up interviews at 6 and 12 months). In addition to the interview, participants’ medical, pharmacy, and financial records were abstracted and a subset of participants had their blood drawn for laboratory testing. Among the study’s main objectives was to guide policy decisions on the allocation of health care resources by providing reliable national estimates of the health care services received by people with HIV and on the costs of those services (RAND, 2011). The HCSUS offers a number of insights and lessons learned concerning the generation of nationally representative estimates of the care experiences of people with HIV, several of which have been incorporated into the MMP protocol. The committee uses HCSUS as a reference throughout its discussion of MMP in this chapter’s section on how to continue to regularly obtain data to monitor health care coverage and utilization after 2014.
The committee reviewed several existing national population-based health surveys as potential sources of data on health care coverage and utilization for a nationally representative sample of people with HIV. These include the National Health Interview Survey (NHIS), which is the principal source of information on the health of the non-institutionalized U.S. population (CDC, 2012a); the Medical Expenditure Panel Survey (MEPS); the National Health and Nutrition Examination Survey (NHANES)1; the Behavioral Risk Factor Surveillance System (BRFSS); and the National Survey on Drug Use and Health (NSDUH). Although these surveys capture data relevant to monitoring care within the context of the ACA (for example, on sources of care coverage, care utilization, and demographic information), the number of people with HIV included in a given sample will be small because the prevalence of HIV in the general U.S. population is less than 1 percent (Shapiro et al., 1999; UNAIDS, 2010). A 2007 study that combined 2002-2004 MEPS data to evaluate the relationship between Ryan White HIV/AIDS Program service utilization and patient characteristics identified 125 people with HIV (Rein, 2007). Even the NHIS, which interviews between 75,000 and 100,000 individuals each year, will not include sufficient numbers of people with HIV to draw meaningful conclusions about their care experiences. Furthermore, while these population-based surveys are designed to be representative of the general U.S. population, they are not designed to be representative of people with any specific disease (CDC, 2010d; Shapiro et al., 1999). Including questions about HIV serostatus and
_________________
1In addition to an interview component, the NHANES includes an examination involving medical, dental, and physiological measurements and the administration of laboratory tests, including HIV antibody tests. Findings from the NHANES are designed to determine the prevalence of and risk factors for diseases (CDC, 2011a).
additional questions on HIV care experiences for HIV-infected individuals in national surveys would not be adequate to generate nationally representative estimates of their health care coverage and utilization. Thus, the committee did not consider national surveys as practical sources of data to establish a nationally representative baseline of health care coverage and utilization for people with HIV prior to 2014, nor to continue to obtain such data after 2014.
HOW TO ESTABLISH A BASELINE OF HEALTH CARE COVERAGE AND UTILIZATION PRIOR TO 2014
There currently is no single source of data to generate a baseline of care coverage and utilization for people with HIV. MMP is an ongoing federal supplemental HIV surveillance project designed to obtain nationally representative estimates of the care experiences of adults with HIV in care that collects data pertinent to monitoring the impact of the ACA on health coverage and utilization. However, as discussed in the following section, MMP currently has limitations to its design and participant response rate that raise concerns about the representativeness of the data. Combining data from multiple data sources is the most viable option for generating a baseline of care coverage and utilization prior to 2014.
In its first report, the committee identifies 14 core indicators to monitor the impact of the ACA and National HIV/AIDS Strategy (NHAS) on improvements in HIV care (see Table 1-4 in Chapter 1). The committee also identifies sources of data to estimate the indicators, including HIV-specific data sources (e.g., the National HIV Surveillance System, the Ryan White HIV/AIDS Program, and ongoing epidemiologic studies of people with HIV) as well as data sources that are not HIV-specific but that collect data relevant to monitoring care for people with HIV (e.g., Medicaid, Medicare, Veterans Health Administration, and private health insurer data). The committee revisited these data sources for this second report and found that many capture data pertinent to monitoring the impact of the ACA on care for people with HIV such as health coverage and service utilization information and receipt of recommended preventive health services. While none of these systems are designed to be nationally representative, together they can provide a reasonably accurate baseline of care coverage and utilization before 2014. As is outlined in the committee’s first report, these data systems also provide a collective platform for estimating indicators of care quality and, thus, can be used to generate estimates of care quality before full implementation of the ACA (IOM, 2012).
HOW TO CONTINUE TO OBTAIN DATA TO MONITOR HEALTH CARE COVERAGE AND UTILIZATION AFTER 2014
Medical Monitoring Project
MMP was initiated by CDC in 2005 in response to the Institute of Medicine (IOM) report Measuring What Matters: Allocation, Planning, and Quality Assessment for the Ryan White CARE Act, which described a need for representative data on the care and preventive service needs of individuals with HIV in the United States (CDC, 2012e; IOM, 2004). MMP utilizes a repeated (annual) cross-sectional design to obtain data from a national probability sample of HIV-diagnosed adults in care to
- describe the clinical and virologic status of these persons;
- describe the prevalence of comorbidities related to HIV disease;
- describe HIV care and supportive services received and the quality of such services; and
- identify met and unmet needs for HIV care and prevention services to inform prevention and care planning groups, health care providers, and other stakeholders (CDC, 2012c).
MMP is the only study since HCSUS (Bozzette et al., 1998; RAND, 2011) that is designed to be nationally representative of HIV-diagnosed adults in care in the United States. Whereas MMP employs a cross-sectional design, however, HCSUS was a prospective study that followed a cohort of individuals in care for HIV over time (RAND, 2011). MMP is conducted through cooperative agreements between CDC’s Division of HIV/AIDS Prevention-Surveillance and Epidemiology and state and local health departments in participating MMP project areas (CDC, 2012c).
Current Sampling Methodology
MMP uses three-stage, probability proportionate to size sampling for the selection of (1) project areas, (2) facilities that provide outpatient HIV medical care in selected project areas, and (3) HIV-infected adults who receive medical care at selected facilities (Figure 3-1). A similar sampling methodology was used in HCSUS to identify a cohort of people with HIV in care. The national population of inference for each MMP data collection cycle is HIV-infected adults age ≥18 years who received care from known providers of HIV medical care in the United States during a predefined population definition period (PDP).2 The PDP has been January 1 through
_________________
2For local estimates in MMP project areas, the population of inference is HIV-infected adults who received care from known providers of HIV care in the project area during the population definition period (CDC, 2012c).
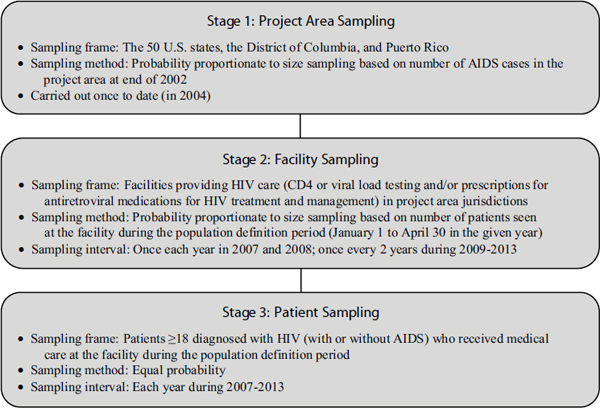

FIGURE 3-1 MMP sampling design.
SOURCE: Adapted from CDC, 2012c; McNaghten et al., 2007.
April 30 for each full year of MMP data collection thus far (CDC, 2012c,e). The first full year of MMP data collection was 2007; 13 project areas were funded to pilot data collection on patients who were in care in 2005,3 and CDC did not collect data on patients in care in 2006 due to delays in the Office of Management and Budget’s (OMB’s) clearance of MMP activities4 (CDC, 2010a).
Project Area Sampling
Project area sampling took place in early 2004. Consistent with the goal of MMP to obtain a national probability sample of adults in care for HIV infection, all 50 U.S. states, the District of Columbia, and Puerto Rico were eligible for selection. Probability proportionate to size sampling was used to select primary geographic sampling units where the measure of size
_________________
3The 13 project areas were Delaware, Florida, Houston (Texas), Illinois, Los Angeles (California), Maryland, Michigan, New Jersey, New York City (New York), Philadelphia (Pennsylvania), South Carolina, Texas, and Washington (CDC, 2012c).
4The Paperwork Reduction Act of 1980 requires Office of Management and Budget approval of federally sponsored data collection activities (HHS, 2012a) such as MMP.
was the total number of people living with AIDS at the end of 2002.5 Based on available funding for MMP, 20 primary geographic sampling units were selected (19 states and 1 territory); 6 municipal jurisdictions located within the selected project areas and separately funded for HIV/AIDS surveillance were also selected, resulting in a total of 26 project areas. All of the project areas agreed to participate in MMP (CDC, 2012c,e).6
Of the 26 project areas initially sampled, 23 have been funded to conduct MMP since 2009. States and territories currently funded for MMP are California (other than Los Angeles and San Francisco), Delaware, Florida, Georgia, Illinois (other than Chicago), Indiana, Michigan, Mississippi, New Jersey, New York (other than New York City), North Carolina, Oregon, Pennsylvania (other than Philadelphia), Puerto Rico, Texas (other than Houston), Virginia, and Washington. Municipal project areas currently funded for MMP are Chicago, Illinois; Houston, Texas; Los Angeles County, California; New York, New York; Philadelphia, Pennsylvania, and San Francisco, California. In addition to the areas noted above, the project areas funded for the 2007 and 2008 data collection cycles included Maryland, Massachusetts, and South Carolina (CDC, 2012c,e). While maintaining a nationally representative system, these states were removed from the project area sample in 2009 to reduce project costs and improve operational efficiency (Personal communication, Jacek Skarbinski, CDC, August 27, 2012).
CDC’s 2012 HIV Surveillance Report includes data from 46 states and 5 dependent areas that have used confidential name-based HIV (in addition to AIDS) reporting since at least January 2007. Although MMP project area sampling was conducted in 2004, data from the report indicate that about 80 percent of the 800,784 people ≥13 reported to be living with a diagnosis of HIV infection in 2009 resided in the 19 states and 1 dependent area that are the current MMP project areas (CDC, 2012b).7
_________________
5The results of MMP are intended to be generalizable to adults with diagnosed HIV infection who are in care, and not limited to those whose infection has progressed to AIDS. However, when project area sampling was carried out in 2004, there was no data system from which to reliably estimate the number of people in the United States with diagnosed HIV infection; several states and dependent areas did not yet use confidential name-based reporting to collect HIV infection data. The estimated number of people diagnosed with AIDS was used as an indirect measure of size to sample project areas because reporting of AIDS diagnoses had been implemented nationally (CDC, 2010b, 2012c,e). All U.S. states, the District of Columbia, and six dependent areas had implemented confidential name-based HIV reporting as of April 2008 (CDC, 2011c).
6Please see CDC, 2012c (Appendix A) for a fuller description of the project area sampling methodology.
72009 is the most recent year for which estimates of the total number of people living with a diagnosis of HIV infection by state and dependent area are available (CDC, 2012b).
Facility Sampling
The second stage of sampling involves the selection of facilities from each project area. Facility samples were drawn each year in 2007 and 2008 and are being drawn every other year during 2009 to 2013. A comprehensive list of eligible facilities providing HIV medical care within a project area jurisdiction serves as the facility sampling frame (CDC, 2012c,e). Compiled by health department staff in the project area (i.e., “project area staff”), the facility sampling frame is composed of facilities that reported patients to the HIV/AIDS Reporting System (HARS) or Enhanced HIV/AIDS Reporting System (eHARS), databases used by health departments to collect, manage, and report state or local HIV/AIDS surveillance data to CDC.8 Project area staff may also consult state or local laboratory reporting databases or prescription drug lists, which contain information on providers who order laboratory tests and prescribe antiretroviral medications, to identify eligible facilities (CDC, 2012c,e).
Outpatient facilities, including hospital-affiliated and freestanding clinics, health care institutions, and private and group physician practices that are providing HIV medical care in the jurisdiction, and that have a centralized medical record system, are eligible for MMP. HIV medical care for purposes of constructing the facility sampling frame is defined as “conducting CD4 or HIV viral load testing and/or providing prescriptions for antiretroviral medications in the context of treating and managing a patient’s HIV disease” (CDC, 2012c, p. 9) (Figure 3-2). Facilities that do not provide medical care (e.g., those that exclusively provide HIV counseling and testing services or that obtain CD4 count and viral load information for referral purposes only) are not eligible. Also ineligible are facilities that only provide inpatient care (e.g., hospices); emergency departments; facilities located outside the project area; correctional and work-release facilities; tribal facilities; and facilities located on military installations.9 Veterans Health Administration (VHA) facilities are eligible to participate in MMP and it is a requirement that they are included on the facility sampling frame (CDC, 2012c).
For each facility included on the facility sampling frame, MMP proj-
_________________
8eHARS is a browser-based system created by CDC and deployed at health departments. CDC developed eHARS as a replacement for the older HARS to help expedite and standardize reporting of HIV/AIDS information (CDC, 2009a).
9According to the 2012 MMP protocol, inpatient facilities and emergency departments are excluded because the medical care provided to people with HIV in these settings may not be HIV-related. Furthermore, some providers in inpatient hospital facilities, such as medical residents, may not be known providers of HIV care and thus not be eligible to carry out MMP patient contact and recruitment activities. Hospices may provide HIV medical care but are excluded from MMP because they are not considered to be known regular providers of such care (CDC, 2012c).
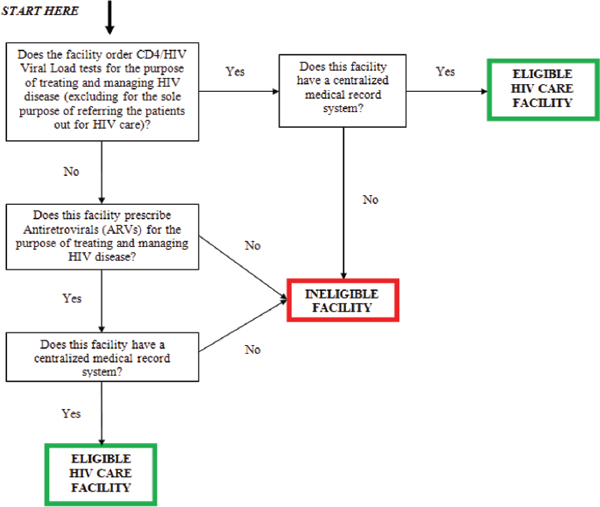
FIGURE 3-2 MMP facility eligibility determination algorithm.
SOURCE: CDC, 2012c.
ect area staff identifies an estimated patient load—a best estimate of the total number of eligible patients who receive care at the facility during the PDP. The estimated patient load is based on data provided directly by facilities, for example, based on patient data runs or another record-based source. Data from HARS, eHARS, state or local laboratory databases, or prescription drug lists may be used to estimate a facility’s patient load in cases where information cannot be obtained from facilities (CDC, 2012c). CDC uses the patient load information reported by facilities to select facilities using probability proportionate to size sampling, where facilities with higher estimated patient loads are more likely to be selected. According to the 2012 MMP protocol, between 25 and 50 facilities were selected in most project areas for the 2011 and 2012 data collection cycles (CDC, 2012c,e).
As discussed below, CDC is pilot testing the feasibility of using the National HIV Surveillance System (NHSS) as a patient sampling frame in select MMP project areas during the 2012 and 2013 data collection cycles. If the pilot study is successful and NHSS-based sampling is implemented, facility sampling could be reduced or eliminated (CDC, 2012e).
Patient Sampling
The third stage of sampling involves the selection of patients from each participating facility. To be eligible for MMP, patients must (1) be diagnosed with HIV (with or without AIDS) any time prior to the end of the population definition period or PDP (between January 1 and April 30 of the given year); (2) be at least 18 years of age at the beginning of the PDP; and (3) have received medical care during the PDP. Medical care for purposes of patient sampling is defined as “any visit to the facility for medical care or prescription of medications, including refill authorizations and vaccinations” (CDC, 2012c, p. 14).10 Patients must also be able to provide informed consent and cannot have already participated in MMP during the current data collection cycle to be eligible for participation. Patient sampling is carried out on an annual basis (CDC, 2012c).
Patients are selected for MMP using list-based sampling. Each participating facility provides local project area staff with a list of HIV-infected adults who received medical care at the facility during the PDP. After project area staff have received patient lists from all participating facilities within the jurisdiction, a master file is transmitted to CDC for patient sampling. Sampling is performed so that all patients who were seen during the 4-month sampling period have an equal probability of selection. The identification numbers of selected patients are returned to project areas for patient recruitment (CDC, 2012c,e). CDC determined that 400 is the minimum sample size for a state to obtain population estimates with an acceptable level of precision, including patients sampled in a municipal jurisdiction or statewide project area. Patient sample sizes across all facilities in a project area ranged from 100 to 800 during 2012. Approximately 9,400 participants were sampled in total (Table 3-1; CDC, 2012c).
CDC pilot tested real-time sampling (RTS) in two large facilities in the Philadelphia project area in 2011. RTS can improve coverage, response rates, and data timeliness, including among harder-to-reach populations since study participants are recruited when they come for services (Iachan et al., 2011). In the MMP pilot study, “office period units” were selected using probability proportionate to size sampling where size was the patient flow during a particular time of day in a particular office within the selected facility. Patients believed to be eligible for MMP (as determined by facility staff) with scheduled appointments during the selected office period units comprised the sampling frame. Patients were selected from this sampling frame using systematic random sampling (Iachan et al., 2011). Results from
_________________
10Note that this is different from the definition of medical care used for facility sampling (i.e., “conducting CD4 or HIV viral load testing and/or providing prescriptions for antiretroviral medications in the context of treating and managing a patient’s HIV disease”) (CDC, 2012c, p. 9).
TABLE 3-1 MMP Patient Sample Sizes by Project Area, 2012
|
|
|
| Project Area | Patient Sample Size |
|
|
|
| California (excluding LA, SF) | 500 |
| Los Angeles County | 400 |
| San Francisco | 400 |
| Delaware | 400 |
| Florida | 800 |
| Georgia | 400 |
| Illinois (excluding Chicago) | 100 |
| Chicago | 400 |
| Indiana | 400 |
| Michigan | 400 |
| Mississippi | 400 |
| New Jersey | 500 |
| New York State (excluding NYC) | 200 |
| New York City | 800 |
| North Carolina | 400 |
| Oregon | 400 |
| Pennsylvania (excluding Philadelphia) | 100 |
| Philadelphia | 400 |
| Puerto Rico | 400 |
| Texas (excluding Houston) | 400 |
| Houston | 400 |
| Virginia | 400 |
| Washington | 400 |
| Total | 9,400 |
|
|
|
SOURCE: CDC, 2012c.
the pilot study were promising with regard to sampling completion. HCSUS also used RTS in select sites to good advantage to address several implementation challenges also faced by MMP (Frankel et al., 1999; Shapiro et al., 1999). However, due to additional burden on MMP staff to manage the sampling process and provide statistical assistance, CDC decided not to continue using RTS for the remainder of the 2009-2013 funding cycle (Iachan et al., 2011; Personal communication, James Heffelfinger, CDC, June 11, 2012).
Facility and Patient Recruitment
Facilities sampled for MMP are recruited by project area staff. No substitutions are made for facilities found to be ineligible during recruitment or that decline to participate because doing so could invalidate the project sampling design. Given that the success of MMP is heavily dependent on a high facility response rate, CDC advises that project areas have a plan in place to maximize facility participation based on previous experience with
TABLE 3-2 MMP Facility and Patient (Interview) Response Rates, 2009 and 2010
| Facility Response Rate | Patients Sampled | Interviews Completed | Raw Response Ratea | Adjusted Response Rate | |
| 2009 | 76% | 9,038 | 4,620 | 51% | 56% |
| 2010 | 80% | 9,300 | 4,981 | 54% | 56% |
aBefore adjustment for patients sampled who are later identified as ineligible.
SOURCE: Personal communication, Jacek Skarbinski, CDC, September 12, 2012.
MMP and similar projects, as well as discussions (e.g., on conference calls, at meetings) among staff in the various project areas (CDC, 2012c). The facility response rates for the 2009 and 2010 data collection cycles were 76 percent and 80 percent respectively (Table 3-2) (Personal communication, Jacek Skarbinkski, CDC, September 12, 2012).
Patients may be recruited either by facility or project area staff. The decision of which of the two methods to use is based on local facility preference and state or local project area Institutional Review Board (IRB) requirements. Project area staff is responsible for scheduling interviews (discussed below) for all patients who are eligible and agree to participate in MMP (CDC, 2012c,e). The adjusted response rate for the interview portion of the study in 2010, the most recent year for which data are available, was 56 percent (Table 3-2) (Personal communication, Jacek Skarbinksi, CDC, September 12, 2012). By comparison, the HCSUS interviewed 76 percent of individuals sampled (Shapiro et al., 1999). The interviewer-administered NHIS household survey averages a 90 percent response rate each year, although the response rate for the sample adult core component of the NHIS, which collects information on health conditions and access to and utilization of health care services for one adult per household, was about 61 percent in 2010 (Schiller et al., 2012). The unweighted response rate for the 2009-2010 NHANES interview was 79 percent (CDC, 2011d). The NSDUH, which collects sensitive health information, such as on use of illegal drugs, alcohol, and tobacco by the U.S. civilian, noninstitutionalized population aged 12 or older via face-to-face interviews, achieved a 75 percent response rate in 2010 (SAMHSA, 2011). MMP participants are compensated in either cash or cash equivalent (e.g., personal gifts, gift certificates, bus or subway tokens) for the interview.11 The compensation was valued to be about $25 for the 2012 data collection cycle, with the exact amount varying by project area (CDC, 2012c).
_________________
11Non-cash reimbursements are provided in project areas where local regulations prohibit cash reimbursements (CDC, 2012c).
An MMP Provider Advisory Board and a Community Advisory Board are in place to support facility and patient recruitment. The Provider Advisory Board consists of one provider representative from each project area as well as members of national HIV provider organizations. Members serve as a resource for providers who are approached about participating in MMP and also provide significant input to MMP staff on facility and patient recruitment strategies. The Community Advisory Board is made up of one community representative from each project area and members of national organizations of people living with HIV. It serves as a link between MMP staff and patients invited to enroll in MMP and works with participating health departments to make sure that patients’ rights and privacy are protected. Members of both the Provider Advisory Board and Community Advisory Board consult on barriers to participation in MMP, study methods and data collection instruments, the usefulness of collected data, and best methods for dissemination of study data (CDC, 2009b,c, 2012c).
Other activities to facilitate patient recruitment include bimonthly conference calls with interviewers and annual interviewer trainings hosted by CDC that address recruitment challenges and strategies to ensure that patient participation is maximized. To better enable participation of patients in rural areas, interviewers travel to conduct interviews in patients’ preferred locations. Optional telephone interviewing, which has been implemented in all project areas as of 2012, also makes it more convenient for patients to participate in MMP (Personal communication, James Heffelfinger, CDC, June 11, 2012).
Data Collection
Core MMP data collection activities include interviewing sampled patients and abstracting their medical records. A minimum data set of basic core surveillance information is also obtained for all sampled patients. Data collection activities are carried out by health department staff in each of the project areas (CDC, 2012c).
The 2012 standard MMP questionnaire includes modules in each of the following areas: Demographics; Access to Care (HIV testing and care experiences, sources of care, and met and unmet needs); Stigma and Discrimination; HIV Treatment and Adherence; Sexual Behaviors; Drug and Alcohol Use (cigarette and alcohol use, non-injection drug use, and injection drug use); Prevention Activities; Anxiety and Depression; Gynecological and Reproductive History; and Health Conditions and Preventive Therapy. The questionnaire also includes an optional module on acculturation that project areas may use to assess patients’ native language, languages spoken and read, language used as a child, language spoken at home and with friends, and language used when thinking (CDC, 2012f). The questionnaire
is administered either face-to-face or by telephone by a trained interviewer who is affiliated with the project area health department. Interviewers utilize a handheld-assisted personal interview (HAPI) on a personal digital assistant device or computer-assisted personal interview (CAPI) software on a laptop computer to administer the questionnaire. Paper versions of the questionnaires are also provided to interviewers to use if needed. Face-to-face interviews take place at a location mutually agreed upon by the patient and project area staff where the confidentiality and security of the patient’s information can be guaranteed, such as a medical facility or the participant’s home. A short MMP questionnaire that includes abridged versions of the demographics, access to care, and HIV treatment and adherence modules is available for interview of patients who are too ill to complete the longer standard questionnaire or who do not speak English or Spanish and require an interpreter to complete the interview.12 The standard and short questionnaires take approximately 45 minutes and 20 minutes to complete, respectively (CDC, 2012c).
After patients complete the MMP questionnaire, their medical records are abstracted by trained abstractors using an electronic medical record abstraction (MRA) application. The medical records of patients who do not complete the interview may also be abstracted in certain circumstances, as discussed below. The range of information abstracted is based on the patient’s clinical condition and experiences and may consist of diagnoses of opportunistic illnesses and other HIV-related conditions, provision of preventive care, prescription of antiretroviral and other medications, laboratory results, and health services utilization. Demographic and insurance status data are also collected (CDC, 2012c).13 Beginning in 2012, the MRA focuses on data contained in the medical record at the care facility where
_________________
12There are English and Spanish versions of the questionnaire. With respect to interviews requiring an interpreter (i.e., for non-English, non-Spanish speaking participants), project areas are encouraged to anticipate what languages they are likely to encounter and to make arrangements to have an interpreter available when needed. CDC’s guidelines for MMP interpreters include demonstration that the interpreter is capable of conveying information in both languages and orientation and training in interpretation and interviews, ethical considerations, and confidentiality (CDC, 2012c).
13Medical record information is collected in four linked forms including a Surveillance Period Summary Form (SPSF), Surveillance Period Visit Form (SPVF), Surveillance Period Inpatient Form (SPIF), and Medical History Form (MHF). The SPSF, SPVF, and SPIF are used to abstract clinical data for events that occurred during the “surveillance period” (SP), which is the 12 months prior to the interview for patients who complete an interview and the 12 months prior to the first attempt to contact the patient for interview for patients who do not complete the interview. The MHF is used to abstract clinical data for events that occurred from the date of first medical care for HIV documented in the patient’s medical record through the date prior to the first day of the SP. For patients found to be deceased, the MRA covers the 12 months prior to the date of death (CDC, 2012c).
the patient was sampled. This includes any information from outside facilities (e.g., inpatient records, lab results) that is available in the patient’s medical record at the facility (CDC, 2012c; Personal communication, Jacek Skarbinski, CDC, June 12, 2012). In previous MMP cycles, in addition to information in the medical record at the facility where the patient was sampled, the MRA could include clinical data contained in medical records at other facilities where the patient had received care (CDC, 2010c), but this is no longer part of the protocol.14
The MRA may be conducted for patients who decline to participate in the interview or who cannot be located for interview in project areas with surveillance authority to perform MRA without explicit patient consent. (This is not possible in project areas with more narrow definitions of surveillance that do not include MRA.) A waiver of consent to complete the MRA for patients known to have died may be obtained in project areas where MMP is considered by the local IRB to be research (CDC, 2012c; HIPAA Privacy Rule 45 CFR 164.512[1][1][iii]).
Multiple measures have been implemented to ensure the collection of quality interview and MRA data. Edit checks are built into the software that interviewers use to record patient responses to interview questions. In addition, 5 percent of patient interviews are observed by MMP principal investigators, project coordinators, or other supervisory staff to ensure data completeness and quality. A standardized checklist for structured interviews is provided by CDC for this purpose (see Box 3-1). The MRA modules are reviewed for quality by project area supervisory staff before submission to CDC. Five percent of MRAs completed are re-abstracted by an independent reviewer and compared with the original MRAs for discrepancies and completeness (CDC, 2012c).
To facilitate the completeness of MMP data, project areas may collect data on patients who have moved and are no longer receiving care in the project area and facility from which they were sampled. For example, staff in the jurisdiction from which the patient was sampled may abstract the medical records of patients who have moved to an area that is not conducting MMP to the extent allowed by surveillance authorities, although an interview is not completed for these patients. For patients who have relocated to areas that are conducting MMP, the new project area may conduct an interview if consent requirements and recruitment protocol specifications are agreed upon by MMP principal investigators in both project areas. Staff
_________________
14In the 2011 MMP protocol, for example, CDC recommended that project areas give priority, in decreasing order, to the abstraction of clinical data from (1) the facility where the participant was sampled, (2) the facility reported by the participant as being his or her primary source of medical care for HIV, and (3) facilities where the participant received inpatient care during the surveillance period (CDC, 2010c).
BOX 3-1
Criteria from Checklist for Observation of MMP Interviewsa
Preparation
- Interviewer had all necessary materials.
- Confidential materials were stored in a locked container before and after the interview.
- Interviewer greeted participant in a friendly manner.
Consent Process
- Interviewer followed all aspects of informed consent according to local protocol.
- Interviewer provided the participant with a copy of the consent form to follow along.
- Interviewer gave the participant a personal copy of the consent form.
- Interviewer inquired about and, if applicable, addressed any questions or concerns about the consent form.
Questionnaire Administration
- Interviewer read questions exactly as written.
- Interviewer read questions at an appropriate pace.
- Interviewer avoided leading participant to a particular response.
- Interviewer demonstrated a neutral attitude.
- Interviewer followed instructions (“Read choices” and “Do not read choices”).
- Interviewer read Say Boxes verbatim.
- Interviewer used all response cards when indicated.
- Interviewer used the calendar to aid with time reference changes.
Interviewer Comments
- (If applicable) Interviewer used “Interviewer Comments” function to record additional comments.
Rapport
- Interviewer established a good rapport with the participant at beginning of interview and maintained it throughout interview.
Closing
- Interviewer provided educational materials and referrals when appropriate.
- (If applicable) Interviewer clarified any factual errors expressed by the participant during the interview.
- Interviewer reimbursed the participant according to local protocol.
_________________
aThe individual observing the interview may indicate “Yes,” “Needs improvement,” or “Not done.”
SOURCE: CDC, 2012c.
in the original project area completes the MRA to the extent allowed by surveillance authorities (CDC, 2012c).
All project areas collect a minimum dataset for all patients sampled for MMP regardless of level of participation. This dataset consists of demographic information; transmission category (i.e., how the individual acquired HIV); primary source of reimbursement at the time the individual was diagnosed with HIV and/or AIDS; and clinical information, including CD4 count and HIV viral load test results. These data generally are extracted from project areas’ HARS or eHARS, but may be collected directly from facilities in cases where they cannot be extracted from these systems (CDC, 2012c). Since the information included in the minimum dataset is consistent with that reported to CDC for national HIV/AIDS surveillance, it may be collected without patient consent under project areas’ surveillance authority. MMP obtained a minimum data set for 88 percent of all sampled patients in the 2009 data collection cycle, with a project area completion range of 72 to 100 percent (Personal communication, James Heffelfinger, CDC, June 11, 2012). As is discussed below, CDC recently expanded the linkage of MMP with NHSS by adding additional data elements to the minimum data set to allow prospective monitoring of MMP participants’ HIV disease progression and receipt of care (CDC, 2012c).
Funding
As of the writing of this report, CDC had received OMB approval for MMP operations through May 31, 2015. The cost of the project for 2012-2015 is estimated to be about $44.1 million or $14.7 million per year. The majority of funds are to support cooperative agreements with health departments in project areas which, as indicated previously, carry out the MMP data collection activities (CDC, 2012d).
Recent Major Developments in the Medical Monitoring Project
In a report to the committee on the use of MMP data to monitor implementation of the ACA, CDC reported that it is carrying out a demonstration project during the 2012 and 2013 data collection cycles to explore the feasibility of using the NHSS as a participant sampling frame which would expand MMP’s population of inference to include individuals with diagnosed HIV who are not in care (CDC, 2012e).15 In the dem-
_________________
15Population-based studies conducted in the United States show that 45 to 55 percent of individuals with diagnosed HIV infection fail to receive care in any given year (Gardner et al., 2011; Ikard et al., 2005; Olatosi et al., 2009; Perkins et al., 2008). In addition, several cohort studies have shown that 25 to 45 percent of people with diagnosed HIV are completely lost
onstration project, a subset of MMP project areas will draw a sample of eligible individuals from local HIV surveillance data, assess eligibility and offer enrollment, and conduct the interview and MRA for participants who consent to participate. The capacity of project areas to obtain current contact information and informed consent from individuals sampled from NHSS and, therefore, to achieve adequate response rates will be evaluated. The project will also assess whether oversampling of individuals who are recently diagnosed with HIV can be used to collect information for improving linkage to HIV care and for enhancing HIV prevention interventions (CDC, 2012e). If the pilot study is successful and NHSS-based sampling is implemented, MMP’s sampling methodology would be simplified as the need for stage two facility sampling would be reduced or eliminated (CDC, 2012e; Personal communication, Amy Lansky, CDC, March 19, 2012).
As noted previously, project areas extract a minimum data set from HARS or eHARS for each individual in the jurisdiction who is sampled for MMP. Beginning with the 2012 data collection cycle, CDC modified the linkage of MMP data with NHSS by adding 56 new data elements to the minimum data set. This modification was implemented to supplement incomplete data due to delays in reporting to complete the interview and MRA as well as to permit longitudinal monitoring of MMP participants’ HIV disease progression and care utilization (CDC, 2012c,e).
Other recent changes relate to data collection. CDC implemented telephone interviews as an alternative to face-to-face interviewing to improve patient response rates and operational efficiency. After a period of pilot testing in select project areas in 2010 and 2011, telephone interviewing is now an option for patients in all project areas. In addition, CDC has made changes to the MRA process to improve the efficiency of data collection while maintaining the ability to collect detailed clinical data. Revisions include simplification of the MRA data collection instruments and possible modification of the existing software application for the collection of MRA data. As noted previously, beginning in 2012 the MRA is limited to information contained in the patient’s medical record at the facility from which he or she was sampled, whereas previously the MRA was expected to include medical records from any facility where the patient received care. CDC also noted that the MRA is being streamlined to collect data relevant to (1) clinical indicators linked to prevention that are included in the NHAS and (2) selected quality-of-care measures that have been proposed
_________________
to care in many settings, although many of them eventually reenter care (Arici et al., 2002; Coleman et al., 2007; Hill et al., 2010; Mocroft et al., 2008).
by various expert panels and cross-federal-agency efforts16 in the areas of viral load suppression, prescription of antiretroviral therapy (ART), retention in care, appropriate health screening, prophylaxis against opportunistic infections, and immunizations (CDC, 2012e).
Strengths and Limitations of the Medical Monitoring Project to Generate Nationally Representative Estimates of Health Care Coverage and Utilization
MMP is the only ongoing study that is designed to provide nationally representative estimates of the clinical and behavioral characteristics of HIV-infected individuals. Comparison of MMP participant data from 2007, the most recent year for which published data are available, with national data from NHSS shows similarities across characteristics of sex, age, and race and ethnicity (Table 3-3) (CDC, 2012b,e). However, MMP may be less representative of the general population of people with HIV for other characteristics. For example, while it is estimated that 17 percent of people living with diagnosed HIV in the United States have private health insurance (HHS, 2012b), 37 percent of MMP participants reported having private health insurance or a health maintenance organization (HMO) as a source of health coverage during the past 12 months (Appendix Table 3-1).
MMP provides an annual “snapshot” of the health care experiences of HIV-diagnosed adults that can be used to monitor trends in health care coverage and utilization over time. As is characteristic of survey research, new questions and variables can be developed, piloted, and added to MMP data collection instruments in response to changing information needs. This is a valuable mechanism for researchers and policy makers as questions about HIV care quality and access are likely to emerge in future stages of ACA implementation. MMP data are currently used to monitor several national initiatives such as the NHAS and Healthy People 2020 HIV-related indicators (CDC, 2012e) and could play a similar role to monitor the impact of the ACA on care coverage and utilization of people with HIV.
There are advantages and disadvantages to a cross-sectional study design, as is primarily used in MMP, and a prospective study design, as was used in HCSUS, to study the care experiences of people with HIV. Cross-sectional surveys are useful for providing information about the characteristics of a population at a specific point in time. Such data can be of great value to policy makers and public health administrators for assessing the
_________________
16Such entities include a National Committee for Quality Assurance-sponsored HIV/AIDS Expert Panel Work Group, the American Medical Association, the Health Resources and Services Administration, the Infectious Disease Society of America, and the HIV Medicine Association (CDC, 2012e).
health status and health care needs of populations, as well as for resource allocation, and is the approach used in population-based health surveys such as the NHIS and NHANES. Cross-sectional studies can be used to generate descriptive statistics (e.g., source of care coverage for various demographic groups) but generally are not useful for making inferences about relationships between exposures and outcomes, although MMP was not designed for this purpose. In contrast, prospective studies follow the same cohort of individuals over a period of time. Because the temporal sequence between exposures and outcomes is more clearly established, prospective studies permit the testing of hypotheses (Hennekens and Buring, 1987).17 A prospective design could be used to monitor changes in care coverage and utilization in a cohort of people with HIV at various stages of ACA implementation, which may allow for more meaningful inferences about the patterns of these changes. A drawback to prospective studies, however, is that they require substantial investment in participant retention to prevent loss to follow-up of study participants (Hennekens and Buring, 1987; Hunt and White, 1998; Shapiro et al, 1999). In addition, although MMP’s cross-sectional design permits the selection of a study population that is reflective of changing trends in the characteristics of people with HIV because a participant sample is drawn each year, a prospective study risks becoming less representative over time unless participant entry and study completion is staggered. In both cross-sectional and prospective studies, differences in the characteristics of participants who respond and who do not respond can bias study results (Hunt and White, 1998; Shapiro et al., 1999). The planned linkage of MMP participant data to NHSS to obtain an expanded minimum data set and to track clinical markers of HIV disease progression and maintenance in medical care will add a prospective element to MMP’s design. Although it is still unclear for how long participants will be followed, data from this linkage could potentially be used to monitor trends in care coverage and utilization for the same individuals over time.
MMP in its current design excludes people with HIV who are not in care but who stand to benefit from the ACA through provisions (e.g., Medicaid expansion) that will improve access to health coverage and care. As noted previously, CDC is undertaking a demonstration project to pilot test the use of NHSS as a participant sampling frame. If NHSS-based sampling is implemented, MMP would provide data on access to health coverage and care for individuals who are not actively seeking care and would help
_________________
17A number of ongoing HIV-related observational cohort studies examine exposures associated with care and treatment among people with HIV. Such studies include various individual U.S. cohorts as well as the North American AIDS Cohort Collaboration on Research and Design (NA-ACCORD), which is a collaboration of a number of HIV-related cohorts in the United States and Canada (McNaghten et al., 2007).
| Characteristic | National HIV Surveillance Report, 2007 (estimated)a | National HIV Surveillance Report, 2009 (estimated)a | Medical Monitoring Project, 2007 | |||
| No. | % | No. | % | No. | % | |
| Sex | ||||||
| Male | 556,477 | 75 | 597,928 | 75 | 2,633 | 72 |
| Female | 183,805 | 25 | 194,656 | 25 | 959 | 26 |
| Transgender Age group (yrs) | NA | NA | 47 | 1 | ||
| <13 | 3,799 | <1 | 2,987 | <1 | NA | |
| 13-14 | 1,497 | <1 | 1,249 | <1 | NA | |
| 15-19 | 6,817 | <1 | 7,155 | <1 | NA | |
| 18-24 | NA | NA | 73 | 2 | ||
| 20-24 | 21,464 | 3 | 26,329 | 3 | NA | |
| 25-29 | 44,022 | 6 | 47,328 | 6 | 143 | 4 |
| 30-34 | 62,951 | 8 | 65,161 | 8 | 219 | 6 |
| 35-39 | 103,850 | 14 | 93,780 | 12 | 481 | 13 |
| 40-44 | 148,610 | 20 | 137,477 | 17 | 720 | 20 |
| 45-49 | 143,314 | 19 | 159,418 | 20 | 807 | 22 |
| 50-54 | 102,937 | 14 | 120,082 | 15 | 589 | 16 |
| 55-59 | 60,784 | 8 | 75,575 | 9 | 340 | 9 |
| 60-64 | 28,720 | 4 | 38,067 | 5 | 161 | 4 |
| ≥65 Race | 22,478 | 3 | 29,164 | 4 | 110 | 3 |
| Black/African American | 313,012 | 42 | 336,144 | 42 | 1,438b | 40 |
| White | 259,665 | 35 | 273,883 | 34 | 1,272b | 35 |
| Asian | 7,129 | <1 | 8,422 | 1 | 19 | <1 |
| Native Hawaiian/Pacific Islander | 497 | <1 | 620 | <1 | 11 | <1 |
| American Indian/Alaska Native | 2,826 | <1 | 3,040 | <1 | 19 | <1 |
| More than one race | 10,941 | 1 | 11,213 | 1 | 119 | 3 |
| Unknown (NHSS)/other (MMP) Ethnicity | 778 | <1 | 770 | <1 | 61 | 2 |
| Hispanic/Latino | 156,396c | 21 | 169,679c | 21 | 699 | 19 |
| Total | 751,244d | 803,770d | 3,643 | |||
aBased on data from 46 states and 5 U.S. dependent areas with confidential name-based reporting since at east June 2007.
bNon-Hispanic.
cHispanic/Latino of any race.
dBecause column totals for estimated numbers were calculated independently of the values for the subpopulations, the values in each column may not sum to the column total.
SOURCES: CDC, 2012b,e.
to elucidate the availability and accessibility of HIV care and supportive services to individuals not currently in care (CDC, 2012e).18 Information about individuals who have a diagnosis of HIV but who are not in care is currently limited (Fagan et al., 2010). A CDC-funded Never in Care (NIC) project used surveillance data to identify individuals with HIV who had never been in care and to describe their demographic characteristics and barriers and facilitators of HIV medical care, among other factors. Individuals identified as never in care were younger and more likely to be African American and Hispanic than those for whom there was evidence of care entry (Fagan et al., 2010). The expansion of MMP to include individuals who are not in care could improve understanding of factors that influence care utilization and the development of interventions to improve access to care for all people with HIV.
MMP also does not currently include adolescents who have unique HIV care and treatment needs. Psychosocial issues, such as coping with a new HIV diagnosis and disclosure to friends and family, and frequently occurring comorbidities of mental illness and substance abuse, can complicate HIV disease management among adolescents. Many adolescents with HIV are recently infected (Catallozzi and Futterman, 2005; CDC, 2011b; Spiegel and Futterman, 2009). For these reasons it is important to monitor adolescents’ linkage to and engagement in care. The exclusion of adolescents from MMP leaves a gap in information concerning health care coverage and utilization for people with HIV in this age group. While MMP does include individuals with a history of homelessness or housing instability, it is unclear that there is adequate representation of immigrants, people with mental and substance abuse disorders, and people who flow in and out of the corrections system. These populations are more likely to experience gaps in coverage and care (Altice et al., 2010; Baillargeon et al., 2010; Chen et al., 2011; Dang et al., 2012; Mellins et al., 2009; Springer et al., 2011).
Another limitation of the current MMP design is that the sampling frame is limited to HIV-diagnosed adults who receive care during the PDP of January 1 to April 30 of the given year (CDC, 2012d). If there are systematic differences in the characteristics of patients seen for care during this 4-month period and patients seen for care at other times during the calendar year, the study population may not be fully representative of HIV-diagnosed adults in care. In addition, as was noted about the 2-month PDP used in HCSUS, the 4-month PDP will result in the exclusion of some patients who are infrequent users of care (Shapiro et al., 1999).
_________________
18For example, MMP’s standard questionnaire asks if participants had unmet needs for services (e.g., medicines through the ADAP, dental health care, mental health services, etc.) in the past 12 months and, if so, the reason the participant was not able to get the service (e.g., waiting list too long, transportation problems, lack of insurance) (CDC, 2012f).
The MMP questionnaire may be administered either face-to-face or via telephone by a trained interviewer. Research on mode of questionnaire administration has shown that face-to-face interviews are often less burdensome for respondents because they usually only require that respondents speak the language in which the questions are being asked and have basic verbal and listening skills (Bowling, 2005). Reading skills are not required to the extent required for self-administered questionnaires. In addition, trained interviewers can help to maintain motivation with longer questionnaires, such as the MMP questionnaire, and utilize techniques to aid participant recall of past events and behavior. Although costly in terms of staffing and training requirements, face-to-face interviews often achieve higher response rates than other methods of survey administration (Bowling, 2005; Kelley et al., 2003). Telephone interviews can be more burdensome (e.g., because visual aids cannot be used) and make greater auditory demands on respondents than face-to-face interviews (Bowling, 2005). Nevertheless they are a useful alternative to the face-to-face interview to increase response rates of MMP participants who are unable to complete the interview in person. Self-administered questionnaires are most burdensome because they require that respondents are literate in reading the language of the survey, do not have visual impairments, and have the dexterity to respond to questions (e.g., tick a box on a paper questionnaire, key in responses on a computer-based questionnaire). Respondents may also need the ability to follow routing and skipping instructions on paper questionnaires (Bowling, 2005).
As with all epidemiologic studies based on self-reported data, patients’ inability to accurately recall information during the MMP interview has the potential to result in measurement error that can lead to inaccurate inferences from the interview data (Coughlin, 1990). In MMP, clinical information such as laboratory values, history of vaccinations, and other medical information may be particularly difficult for patients to recall (Blair et al., 2011). Inaccurate recall is a threat to the validity of findings based on clinical information captured solely via patient interview. However, an important advantage of the MMP protocol is that the MRA allows for checking of self-reported data against data in the medical record for agreement. Another potential limitation of self-reported data is the possibility for social desirability response bias, where socially undesirable behaviors (such as drug use or certain sexual behaviors) are underreported and socially desirable behaviors (such as condom use) are overreported (Blair et al., 2011; Bowling, 2005; Coughlin, 1990). Interviewer-administered surveys have several advantages over self-administered questionnaires, as noted above. Yet, some research on the reporting of sensitive and stigmatized behavior has shown that surveys that require social interaction with an interviewer, either face-to-face or by telephone, are more susceptible to social desirability bias than self-administered surveys (Bowling, 2005; Butler et al.,
2009; Drapeau et al., 2011; Tourangeau and Smith, 1996; Tourangeau et al., 1997). Currently, MMP study participants do not have the option to self-administer any parts of the interview. In its first report, the committee noted that allowing patients who participate in MMP to directly enter their responses to sensitive questions into a computer or on the questionnaire may be one way to counteract the potential for social desirability bias (IOM, 2012).
MMP collects a minimum set of data consistent with information collected for national HIV/AIDS surveillance on all patients enrolled in MMP regardless of level of participation. In addition to providing a core set of data for the majority of patients sampled, the minimum data set can be used to support quality control (e.g., ensure patients were not sampled for participation more than once). Because the minimum data include information on patient demographics and other characteristics, they also may be used to evaluate potential nonresponse bias for data collected through the interview and MRA (CDC, 2012c).
A significant concern with MMP is its low response rate (IOM, 2012). The facility and patient response rates in 2010 were 80 percent and 56 percent, respectively (Table 3-2). Without an adequate response rate, MMP becomes a convenience sample study of those willing to be interviewed (Groves et al., 2006; Shapiro et al., 1999). In a response to an inquiry from the committee on the most common reasons for nonparticipation in MMP, CDC indicated that direct facility refusals are low. When facilities do refuse to participate, it is most often due to a lack of time or bureaucratic barriers such as the need for IRB review and Veterans Administration regulatory restrictions for VHA facilities. Furthermore, a number of facilities that do agree to participate are subsequently unable to do so because they cannot provide access to sampled patients (e.g., due to IRB approval delays). With respect to patients, CDC stated that many who do not participate cannot be located or do not respond to attempts at contact made by facility or project area staff. Some project areas and facilities prefer, or have IRB mandates that require, facility staff to recruit and enroll patients. Patients may not be recruited when facilities are not persistent enough in their recruiting efforts, such as calling patients at different times and searching for updated contact information (Personal communication, James Heffelfinger, CDC, June 11, 2012). Measures have been implemented to improve patient participation starting with the 2009 data collection cycle. One change was that the time between patient sampling and recruitment was narrowed to expedite location of patients for interview after receipt of care at participating facilities
(Blair et al., 2011).19 Also, as noted earlier, MMP implemented telephone interviewing as an alternative to the in-person interview in all project areas in 2012.
The study timeline submitted to OMB for approval of MMP through April 2015 notes that project areas have 4 to 5 months to recruit participants and to complete the MRA (CDC, 2012d). Expansion of the window for recruitment and data collection could help to increase both facility and patient participation because facilities would have more time to secure local IRB approval and to work out a site-specific protocol for contacting sampled participants.
A potential protocol change that CDC has considered but not implemented to improve patient response rates is real-time sampling (RTS), a variety of time-space sampling where a random sample of patients with appointments scheduled during the busiest times of day is recruited for participation in MMP. CDC’s pilot study demonstrated that the use of RTS in two large facilities had a positive impact on patient response rates, showed potential to reach participants who are hard to reach using traditional recruitment methods, and was less burdensome to the participating facilities, which may in turn increase facility participation. CDC expressed concern that using RTS would place additional burden on MMP staff to manage RTS and provide statistical assistance (Personal communication, James Heffelfinger, CDC, June 11, 2012). However, the methodological gains resulting from a more complete and thus more representative sample may warrant further consideration of using RTS sampling in select facilities. Similar sampling approaches have been used in a number of studies to identify hard-to-reach populations such as individuals who use drugs and young MSM (Choi et al., 2005; Forney et al., 2012; Grov et al., 2009; Lo et al., 2012; Parsons et al., 2008). In describing lessons learned from HCSUS, the study investigators noted that list-based sampling saved on up-front costs because a staff person did not need to be located on site to perform RTS, but that broader use of RTS (which was used in select HCSUS sites) ultimately would have reduced the expense of participant location and recruitment (Shapiro et al., 1999).
CDC reported that MMP activities require substantial staff and financial resources to produce nationally representative estimates but that possible changes to the sampling design as well as recent changes to the data collection, described previously, could help to reduce current resource needs (CDC, 2012d). The HCSUS investigators also reported a large investment to achieve nationally representative estimates from a sample of HIV-
_________________
19Contacting patients more quickly after receipt of care might increase the likelihood of having up-to-date contact information and, therefore, the location of individuals for recruitment and participation (Blair et al., 2011).
diagnosed individuals in care, but felt that this investment was justified if the data obtained are unbiased and of high quality (Shapiro et al., 1999).
As discussed in Chapter 2, many of the key changes resulting from the ACA—such as expansion of the Medicaid program, phasing out the Medicare Part D prescription drug coverage gap, increased access to private health insurance (e.g., through elimination of preexisting condition exclusions) and consumer protections, and expansion of coverage for preventive health services—are expected to increase the number of people with HIV who have health care coverage and access to benefits and services. Among MMP’s strengths to monitor the health experiences of people with HIV in the context of the ACA is that it already collects data on dimensions of HIV care that correspond to key areas of health care reform (CDC, 2012e). For example, MMP data can be used to evaluate the following:
- sources of health care coverage and the distribution of different sources of coverage (e.g., private health insurance, Medicaid, Ryan White HIV/AIDS Program, Tricare or CHAMPUS, VHA coverage) among study participants;
- primary method of payment for prescription medications for HIV and related illnesses;
- access to HIV care and met and unmet need for supportive services (e.g., HIV case management, AIDS Drug Assistance Program [ADAP] services, dental care, mental health services, housing assistance), including for persons with different types of care coverage;
- the quality and comprehensiveness of HIV care, such as receipt of recommended clinical (e.g., use of ART) and preventive (e.g., immunizations, screening examinations) interventions; and
- the organizational context and structure of HIV care, including where care is provided (e.g., community health centers, hospital-affiliated outpatient clinics), who is providing that care (e.g., infectious disease physicians, nurse practitioners), and whether care is occurring in the context of new organizational models intended to improve service coordination (e.g., patient-centered medical homes, accountable care organizations).
MMP also collects detailed demographic information (age, race and ethnicity, country of birth, sex at birth, gender, sexual orientation, education, and income) that can be used to monitor health care coverage and utilization for subpopulations of people with HIV and to identify and address disparities. MMP project area sample sizes allow national estimates at an acceptable level of precision for subpopulations as small as 5 percent of the total population of interest (CDC, 2012c).
Increased access to health insurance and health care under the ACA
will not ensure linkage to, retention in, and the provision of quality care for people with HIV. For some individuals, movement among sources of care coverage may disrupt the continuity of care and the package of benefits available to them at any given time. For this reason, it is important to monitor care quality and outcomes in addition to care coverage and utilization in the context of ACA implementation. In its first report, the committee identifies 14 core indicators to monitor the impact of the NHAS and ACA that are also measures of HIV care quality (see Table 1-4 in Chapter 1); these include 9 indicators for clinical HIV care and 5 indicators for mental health, substance abuse, and supportive services (housing, food, and transportation assistance), which are important mediators of access to care for people with HIV (Anema et al., 2009; Buchanan et al., 2009; IOM, 2012; Kalichman et al., 2011; Sarnquist et al., 2011).20 MMP captures many of the data elements needed to estimate these indicators. Appendix Table 3-2 maps the committee’s core indicators with questions from the MMP questionnaire and MRA forms that might provide the data needed to estimate the indicators. Once laboratory reporting of CD4 and viral load results is implemented in all states, the NHSS may be the most robust source of information to estimate indicators for individuals who are recently diagnosed with HIV, such as the proportion of people who are newly diagnosed who have clinical diagnosis of AIDS.21 Since MMP’s current sampling methodology involves sampling participants from care facilities, it is less likely to select individuals who are recently diagnosed with HIV who do not yet have an HIV care provider. However, MMP’s capacity to generate nationally representative estimates for these indicators should be improved if CDC implements NHSS-based sampling. MMP does not currently provide all of the data needed to estimate the committee’s recommended indicators for mental health and substance abuse, but it is one of only a few sources of data, along with the Ryan White HIV/AIDS Program, that captures information to estimate indicators of need for housing, food, and transportation assistance (IOM, 2012).
Although designed to be nationally representative, MMP does not collect data on individuals with HIV in all U.S. states and territories. Data from Medicaid and the Ryan White HIV/AIDS Program, because they are captured for all states and territories, can serve as useful sources of state-
_________________
20The committee also identified additional (noncore) indicators that could be used for more comprehensive assessment of HIV care quality (IOM, 2012).
21Currently, there is some variation among states in the specific values of CD4 and HIV viral load that are required to be reported.
level information on care coverage and utilization to supplement findings from MMP. Medicaid and the Ryan White HIV/AIDS Program, along with Medicare, are also currently the most common sources of care coverage for people with HIV (HHS, 2011, 2012b). Although not generalizable to all HIV-infected individuals in the United States, analysis of data from these specific programs, in addition to data from MMP, is essential to highlight how ACA provisions that affect program eligibility and coverage of services impact the care experiences of people with HIV. Provisions of the ACA will not be implemented by states uniformly, resulting in variation among states in eligibility for health coverage and, consequently, access to health care (IOM, 2012). State-by-state monitoring of the care experiences of people with HIV will be important for this reason.
Medicaid Program Data
The Medicaid program is currently the largest single source of care coverage for people with HIV in the United States. Forty-seven percent of people with HIV in regular care in FY 2007 were enrolled in Medicaid (Kates, 2011). The ACA expands the Medicaid program to include non-Medicare eligible individuals under age 65 with incomes up to 133 percent of the federal poverty level (FPL) (a standard 5 percent income disregard effectively increases the income limit to 138 percent of the FPL). The ACA also calls for the removal of categorical eligibility requirements, such as being disabled.22 This means that people with HIV will no longer be required to have a diagnosis of AIDS or other disability to qualify for Medicaid. Disability is currently the most common pathway to Medicaid for those with HIV, with about three in four such individuals qualifying on the basis of being disabled (Kates, 2011). Medicaid expansion is expected to considerably reduce the number of people who are uninsured in the United States. However, in June 2012 the U.S. Supreme Court ruled that the federal government cannot penalize states that choose to opt out of Medicaid expansion by withholding state Medicaid funding (National Federation of Independent Business v. Sebelius, 567 U.S.____ [2012]). Because many states are not likely to comply with Medicaid expansion in the wake of the Supreme Court’s ruling, the impact of this provision may not be as significant as earlier anticipated (Daily Briefing, 2012).
Analysis of data from the Medicaid program is essential to monitoring access to health coverage and utilization for people with HIV because of the large proportion of people with HIV who are currently enrolled in
_________________
22Prior to the passage of the ACA, in addition to meeting income eligibility requirements, individuals were required to be “categorically eligible” for Medicaid. Categorical eligibility groups include the disabled; parents, children, and pregnant women; the elderly; and other groups.
the program and the anticipated increase in program enrollment starting in 2014. The nature of Medicaid as a source of care coverage for low-income individuals makes it a useful source of data for tracking the care experiences of people with HIV who are economically disadvantaged and who are more likely to have multiple care and supportive service needs. In addition, Medicaid data will encompass the care experiences of a greater number of HIV-infected individuals from racial and ethnic minority groups since racial and ethnic minorities disproportionately rely on the program as a source of health coverage. States administer the Medicaid program under broad federal guidelines and have some independence in determining income and other eligibility requirements. Program data are reported by states to the Centers for Medicare & Medicaid Services (CMS) and can be used for both state specific and inter-state analyses of Medicaid enrollment and care utilization.
As discussed in the committee’s first report, the Medicaid Statistical Information System (MSIS) is the primary source of Medicaid data. MSIS is a claims processing system that captures utilization and management information on medical care and services provided to Medicaid beneficiaries. MSIS is populated with data reported by states on a quarterly basis, including eligibility and demographic characteristics of each person enrolled in Medicaid, and claims adjudicated for drugs, long-term care services, inpatient stays, and other services during the quarter (CMS, 2012b,c). MSIS data are also available through the Chronic Condition Data Warehouse (CCW), created by CMS, to approved researchers and certain government agencies through the Research Data Assistance Center (ResDAC, a CMS contractor). These files are called “Medicaid Analytic eXtract” (MAX) files and are formatted in a way to facilitate research and public policy needs. MAX files include a person summary file with enrollment information, as well as inpatient hospital, long-term care, prescription drug, and other services files (ResDAC, 2012). Both MSIS and MAX files provide data that could be used to monitor the impact of the ACA on health care coverage and utilization for people with HIV. Comparison of Medicaid enrollment data pre- and post-2014, and beyond 2014, could be used to track how many additional people with HIV gain access to this source of health coverage over time. Analysis of Medicaid data also could be used to track beneficiary receipt of preventive and care services, including benefits outlined in a package of essential health benefits that states will be required to provide most newly eligible Medicaid beneficiaries starting in 2014 (KFF, 2010).23
_________________
23These benefits include ambulatory patient services; emergency services; hospitalization; maternity and newborn care; mental health and substance use disorder services, including behavioral health treatment; prescription drugs; rehabilitative and habilitative services and devices; laboratory services; preventive and wellness services and chronic disease manage-
In addition to the strengths of Medicaid data for monitoring the care experiences of people with HIV noted above, MSIS data should have lower occurrence of reporting inaccuracies than patient-reported information since data come from claims submitted by providers (although providers may inaccurately report data due to coding and other errors). MSIS uses unique identifiers to link information across time for individuals, permitting longitudinal evaluation of their care experiences. Data are collected quarterly (moving to monthly within 2 years), which allows for regular updating of the data (IOM, 2012).
There are a few limitations to MSIS data. Many people with HIV who are enrolled in Medicaid should be identifiable by diagnostic code for HIV/AIDS. However, the diagnostic code may not be recorded for some individuals (e.g., because they were diagnosed with HIV before they enrolled in Medicaid and the new provider failed to enter the diagnosis). Use of a combination of codes for diagnoses, procedures (e.g., CD4 counts, viral load tests), and prescription drugs (e.g., antiretrovirals used to treat HIV) may be the best way to identify Medicaid beneficiaries with HIV with the greatest positive predictive value (Crystal et al., 2007; IOM, 2012; Koroukian et al., 2003). Another challenge is fluctuating eligibility requirements for Medicaid, which cause people to shift in and out of coverage so that any medical care they receive during the period they are not enrolled in Medicaid will not be recorded in MSIS. In addition, some services that Medicaid beneficiaries receive may not be recorded in the claim record (for example, if the service was carved out to another provider) and, therefore, not available in MSIS.
As noted previously, the data contained in MSIS are reported by states to CMS. It can take states a year or more to complete their reporting resulting in an approximately 2-year lag time for MSIS files to be created. The lag time is longer (2.5-3 years) for MAX data files because the raw MSIS data must be extracted and consolidated. A built-in lag time of at least 13 to 14 months is required to ensure that claims for most services delivered in a given calendar year are captured, and another 9 to 10 months is needed to validate the data (ResDAC, 2006). This delay should not preclude the use of Medicaid data for monitoring access to health insurance and health care for people with HIV. Data that are currently available could be used to establish a baseline of the number of Medicaid beneficiaries with HIV and their receipt of preventive and other services of interest (Kates, 2011); data available after 2014 (starting in 2016, given the approximately 2-year lag time) could be used for longitudinal monitoring.
Care for most Medicaid beneficiaries is provided through managed
_________________
ment; and pediatric services, including oral and vision care (Affordable Care Act of 2010, Sec. 1302[b]).
care arrangements where states contract with managed care organizations to provide Medicaid services. Under this model, providers are paid a capitated (i.e., fixed) rate per enrolled Medicaid beneficiary. Similar to Medicaid claims for services provided on a fee-for-service basis, encounter data serve as the primary record of services provided to program beneficiaries enrolled in capitated managed care (HHS, 2009). Although many states with Medicaid managed care have collected, used, and reported encounter data for a number of years, CMS has not enforced the reporting of encounter data as it has for fee-for-service claims data (Byrd and Verdier, 2011). Studies have shown that encounter data are not always reported as required or that reporting may be delayed, limiting the usefulness of MSIS (and MAX) data for research and policy analysis (HHS, 2009; Klein, 2002). Missing Medicaid encounter information may further limit the usefulness of MSIS data going forward to the extent that states rely on managed care for Medicaid expansion.
With respect to indicators to measure care quality, MSIS might provide data to estimate the indicators recommended in the committee’s first report for continuity of care (two or more visits for routine HIV medical care in the preceding 12 months at least 3 months apart) and regular CD4 and viral load testing (two or more tests in the preceding 12 months). These data would be available from claims for office visits submitted by providers with HIV listed as one of the diagnostic codes and claims submitted for CD4 and viral load tests. All claims capture dates of service to determine when beneficiaries received a service. Medicaid claims do not record the results of CD4 and viral load tests and thus cannot be used to calculate indicators of clinical HIV care that require such measures, such as the proportion of people with HIV with a CD4+ cell count <500 cell/mm3 who are not on ART (IOM, 2012). MSIS captures date of death and could provide data to calculate the mortality rate of individuals with HIV enrolled in Medicaid. MSIS includes data on screening and visits for mental health and substance abuse services covered by Medicaid, but it does not specifically capture the dates of diagnosis or referral and first visit for services to assess the mental health and substance abuse indicators. MSIS also does not collect data on the housing, food, and transportation needs of beneficiaries to estimate indicators of these supportive services. The demographic data collected would permit estimation of indicators for racial and ethnic subpopulations and by sex, age, and location of residence (IOM, 2012).
Medicare Program Data
Medicare is a public health insurance program for individuals age 65 or older, people under age 65 with certain disabilities, and people of all
ages with end-stage renal disease.24 Approximately one in five individuals with HIV is a beneficiary of the program. The majority of people with HIV who are enrolled in Medicare are under age 65 and qualify on the basis of disability. A small share qualify as seniors. The number of people with HIV who are enrolled in Medicare has grown over time. This growth is likely to continue as a result of advances in treatment that allow people with HIV to live longer lives (KFF, 2009).
The ACA eliminated Medicare Part B (Medical Insurance) coinsurance and deductibles for recommended preventive services beginning in January 2011 (HHS, 2012d). Covered preventive services include screenings for conditions that frequently co-occur with HIV, such as diabetes, sexually transmitted infections, and depression, as well as immunizations for seasonal influenza, hepatitis B, and pneumonia.25 Medicare also now pays for an annual wellness visit that focuses on helping enrollees establish and maintain a personalized prevention plan (CMS, 2012d). Also relevant to people with HIV who are enrolled in Medicare is the closure of the Medicare Part D prescription drug coverage gap (IOM, 2012). Continuous access to prescription medications is a vital component of HIV care. For example, people with HIV who are on and adherent to ART are more likely to achieve and maintain viral suppression and thus have improved health outcomes. They are also less likely to transmit the virus to others (Cohen et al., 2011; Granich et al., 2009). Prior to the passage of the ACA, individuals enrolled in Medicare Part D were required to pay out-of-pocket for the full cost of prescription drugs while in a coverage gap spanning the time between when enrollees and their drug plans had spent a certain amount for covered medications and the initiation of catastrophic coverage.26 The ACA has begun phasing down this coverage gap so that, by 2020, beneficiaries will be responsible for 25 percent of the costs for brand name and generic drugs while in the coverage gap (CMS, 2012a). This change makes drugs more affordable for people with HIV who have Medicare Part D prescription drug coverage. Prior to the ACA, many individuals with HIV had expenditures within the coverage gap unless they were receiving low-income subsidies (KFF, 2006). As of January 2011, ADAP benefits are considered contributions to out-of-pocket spending for Medicare beneficiaries. This will help low-income Medicare beneficiaries with HIV move through the
_________________
24HIV disease and some HIV treatments are associated with renal complications. Some individuals with HIV may qualify for Medicare because they have end stage renal disease (KFF, 2009).
25Some preventive services are available to beneficiaries who meet age, risk factor, or other eligibility requirements, while others are available to all Medicare enrollees; see CMS, 2012e.
26In FY 2012, the Part D prescription drug coverage gap began at $2,930 and catastrophic coverage began after an individual paid $4,700 in out-of-pocket expenses for prescription medications (CMS, 2012a).
Part D coverage gap and into catastrophic coverage more quickly (HHS, 2011; KFF, 2012a).
Medicare data are available in a format to support research through the CCW. CCW contains enrollment and fee-for-service claims data for all Medicare beneficiaries. Fee-for-service claims include data on outpatient care, preventive services, and a variety of other services that could be used to assess the care experiences of beneficiaries with HIV. As of June 2008, CCW makes Part D prescription drug enrollment and utilization data available to researchers for approved studies (Schneider et al., 2010). Prescription drug events are available for all filled prescriptions that are covered by the Part D benefit. Researchers may choose to have event characteristics, such as drug name (brand or generic), appended to the prescription drug event file (Schneider et al., 2010). These data may be useful for monitoring dispensing of ART or other prescription drugs to people with HIV enrolled in Part D as the prescription drug coverage gap is phased down. Basic demographic data captured should allow for analysis of program data by age, sex, race and ethnicity, and Medicare status (i.e., whether an individual qualified for Medicare based on age or disability).
Weaknesses of Medicare data are similar to those of Medicaid. For example, it may be difficult to extract data for all enrollees with HIV. One recent study evaluated the effectiveness of algorithms to identify data from the CCW for individuals who were diagnosed with chronic conditions prior to enrolling in Medicare. The CCW algorithm identified about 70 percent of individuals with preexisting diabetes, but just 17 percent of individuals with preexisting arthritis. The study authors speculated that conditions needing less frequent health care utilization (e.g., because they are not identified by the Medicare provider) may be underestimated (Gorina and Kramarow, 2011). As a condition that requires continuous treatment and regular visits with providers, HIV may be less susceptible to problems of data extraction than other conditions. As with Medicaid data, there is a delay of a couple of years for Medicare data to be made available through the CCW. Medicare is funded in part by payroll taxes paid by most employees. To qualify for Medicare on the basis of age, individuals or their spouses must have 10 or more years of Medicare-covered employment. Thus, program data will not include information for people with HIV age 65 or older who do not meet this eligibility requirement, unless they qualify based on disability.
Medicare is similar to Medicaid in terms of data collected to estimate indicators of care quality. Since Medicare claims capture dates of services, program data can inform indicators related to continuity of care and regular CD4 and viral load testing. Medicare does not collect data to estimate clinical HIV care indicators requiring specific CD4 or viral load values. Program data can be used to measure the mortality rate of people with HIV who are Medicare beneficiaries. Medicare does not have data on
screening for mental health disorders or substance use, but it does capture service utilization information on diagnosis of and covered treatment for these conditions. The data generally do not allow for calculation of the time between referral and receipt of mental health and substance abuse services, although an approximation might be made if the first visit is covered by Medicare. As with Medicaid, Medicare does not collect data on housing, food, or transportation to estimate indicators for these supportive services (IOM, 2012).
Ryan White HIV/AIDS Program Data
The Ryan White HIV/AIDS Program is the largest federal program designed specifically to serve the health care needs of people with HIV. Administered by the Health Resources and Services Administration (HRSA), the Ryan White HIV/AIDS Program provides medical and supportive services to more than 550,000 people each year.27 The program often serves as a wrap around program to pay for medications and supportive services (e.g., case management, housing services, psychosocial support services) that are not paid for through other sources of health care coverage. The program has been reauthorized every 3 to 5 years since it was established in 1990 (Ryan White Care Act, P.L. 101-381), with the next reauthorization scheduled for 2013. Ryan White HIV/AIDS Program funding is provided to cities, states and territories, providers, and other organizations. Given variations in the nature of the HIV epidemic and service needs across geographic areas and providers, program grantees are given discretion to determine client eligibility and service priorities (HRSA, 2012a; KFF, 2011b).
As noted in the committee’s first report, the Ryan White HIV/AIDS Program model of care helps to overcome barriers to care posed by the fragmented health care system in the United States, because clinical and supportive services are coordinated within a single “medical home” (IOM, 2012). The expansion of the Medicaid program, changes in access to private health insurance, and other ACA provisions are expected to reduce
_________________
27In order to most effectively execute the services necessary, the Ryan White HIV/AIDS Program developed five “Parts,” each of which is designed to help accommodate the needs of people living with HIV in the United States: Part A provides emergency assistance to Eligible Metropolitan Areas and Transitional Grant Areas that are most severely affected by the HIV epidemic; Part B provides grants to all 50 states, the District of Columbia, Puerto Rico, Guam, the U.S. Virgin Islands, and 5 U.S. Pacific Territories or Associated Jurisdictions; Part C provides comprehensive primary health care in an outpatient setting for people living with HIV; Part D provides family-centered care involving outpatient or ambulatory care for women, infants, children, and youth with HIV; Part F provides funding for a variety of programs, including the Special Projects of National Significance Program, the AIDS Education and Training Centers Program, the Dental Programs, and the Minority AIDS Initiative (HRSA, 2012a).
the number of people with HIV who are uninsured and, therefore, who require medical services through the Ryan White HIV/AIDS Program (HHS, 2012c). Although the long-term impact of health care reform on the Ryan White HIV/AIDS Program remains to be seen, the program will likely continue to play an important role in filling gaps in care. Many individuals, such as legal and undocumented immigrants, will remain uninsured even after the ACA is fully implemented (Buettgens and Hall, 2011). In addition, for people with HIV who are currently enrolled in or who transition to other sources of care coverage, the Ryan White HIV/AIDS Program may serve as a source of medical and supportive services not covered by public and private insurance (HHS, 2012c). The program may also have new roles in assisting clients with health insurance premiums, deductibles, copays, and other out-of-pocket costs (Cross, 2011; Martin and Schackman, 2012).
Ryan White HIV/AIDS Program data may be useful for evaluating the ACA. For example, program data may provide insights into shifts in enrollment into other sources of health care coverage. Data can also be used to assess changes in utilization patterns for specific services in order to measure care quality in the context of the ACA. Program data can provide information on an important at-risk and underserved population, as most of clients have incomes at or below the FPL. In addition, the majority of Ryan White HIV/AIDS Program clients are racial and ethnic minorities (HRSA, 2010).
One source of Ryan White HIV/AIDS Program data is the Ryan White HIV/AIDS Program Services Report (RSR). This report is submitted to HRSA by program grantees and service providers on an annual basis to report information on their programs and the clients they serve (HRSA, 2012d). The RSR collects a number of data elements relevant to monitoring the impact of the ACA on the Ryan White HIV/AIDS Program as well as care for people with HIV who are enrolled in the program. Such information includes provider organization information; types of services delivered by the agency during the reporting period (e.g., core medical and supportive services,28 HIV counseling and testing); and client-level data,
_________________
28Core medical services include outpatient/ambulatory medical care; local AIDS pharmaceutical assistance (not ADAP); oral health care; early intervention services; health insurance premium and cost sharing assistance; home health care; home and community-based health services; hospice services; mental health services; medical nutrition therapy; medical case management, including treatment adherence; and substance abuse services (outpatient). Support services include non-medical case management; child care; pediatric development assessment/early intervention services; emergency financial assistance; food bank/home-delivered meals; health education/risk reduction; housing services; legal services; linguistic services; medical transportation; outreach services; permanency planning; psychosocial support services; referrals; rehabilitation services; respite care; substance abuse services (residential); and treatment adherence counseling.
including demographic information, number of visits for core medical services for each quarter in the reporting period, and supportive services received for each quarter in the reporting period. Client-level demographic information includes sources of health insurance allowing for analysis of types of Ryan White HIV/AIDS Program services that continue to be utilized by individuals with other types of health coverage (HRSA, 2012d). Outpatient and ambulatory care providers report clinical information, such as laboratory test results, prescription of ART, and receipt of preventive screenings and immunizations. These data can be used to assess care quality for program clients. For example, clinical data captured in the RSR permit the calculation of indicators recommended by the committee for continuity of HIV care, regular CD4 and viral load testing, and ART initiation. The RSR collects client housing status as well as receipt of housing, food, and transportation assistance, making it one of the few sources of data available, along with MMP, to estimate need for these supportive services. The demographic data collected permit analyses of data by race and ethnicity, sex, age, gender identity, sexual orientation, and location of residence (HRSA, 2012d; IOM, 2012).
The ADAP is a component of the Ryan White HIV/AIDS Program that provides HIV-related prescription drugs to low-income people with HIV who have limited or no prescription drug coverage. ADAPs are a major source of prescription drug coverage for people with HIV; they provided services to about one-third of people with HIV in care in 2010 (KFF, 2012a). With the passage of the ACA, ADAPs are legislatively required to report drug assistance provided to clients with Medicare Part D prescription drug coverage. Consequently, ADAP data can be used to monitor the extent to which ADAP funds are used to fund out-of-pocket expenses for ADAP clients receiving Medicare Part D benefits who fall into the drug coverage gap. Other data reported by ADAPs that may be useful for monitoring prescription drug access under the ACA are enrollment information, demographic characteristics of clients served, and limits applied to the program (e.g., enrollment caps, waiting lists) (HRSA, 2012b). Data are currently reported in aggregate on a quarterly basis. Beginning in 2013, ADAPs will report client-level information on a semiannual basis. Information collected will be expanded to include additional information relevant to evaluate the role of ADAPs under ACA such as client sources of health insurance, reasons for disenrollment from ADAP, and more detailed payment information. The new report will also collect CD4 and viral load test dates and results which can be used to assess indicators of care quality for ADAP enrollees (HRSA, 2012c; IOM, 2012).
In June 2012, the HHS Office of the Assistant Secretary for Planning and Evaluation submitted a request for OMB approval of a Ryan White HIV/AIDS Program Modeling Study to understand changes in Ryan White
HIV/AIDS Program services utilization and funding needs under the ACA. To supplement the analysis of quantitative data from the Ryan White HIV/AIDS Program, Medicaid, and NHSS, the study would involve the collection of interview data from program grant managers, administrators, and providers. The interviews would assess HIV service needs and use; Ryan White HIV/AIDS Program funding prioritization and allocation processes; factors that influence regional variation in HIV care costs and Ryan White HIV/AIDS Program funding needs; third-party payment policies and reimbursement for HIV services; and methods of ensuring quality care under the ACA (HHS, 2012c). Findings from the study might be an additional source of information to evaluate the continuing role of the Ryan White HIV/AIDS Program.
Private Health Insurer Data
Approximately 17 percent of individuals with HIV have private health insurance (HHS, 2012b). It is likely that many more individuals with HIV will gain access to private insurance under the ACA. In 2014, a guaranteed availability of insurance provision ensures the issuance and renewability of health insurance regardless of health status and without increased premiums for individuals with preexisting conditions, such as HIV. Currently, temporary preexisting insurance plans with subsidized premiums are available to adults with preexisting conditions who have been uninsured for at least 6 months. In addition, low- to middle-income individuals with HIV will have improved access to private insurance through health insurance exchanges, slated to be in place in states by 2014,29 that will serve as points of access to commercial health insurance for individuals and employers.30 Health plans offered under the exchanges will be required to cover services in the essential benefits package for newly eligible individuals.
Monitoring the enrollment of individuals with HIV in private health
_________________
29The ACA sets broad parameters for the exchanges. However, states are given flexibility on a number of aspects of the exchanges, such as governance structure and administration; key functions and responsibilities; whether to establish their own exchange or rely on the federal government to do so; and how the exchange will interact with the state’s Medicaid program (Carey, 2010). Fifteen states and the District of Columbia had established health insurance exchanges as of August 1, 2012. A few states have chosen to allow the federal government to set up their exchanges. Other states have slowed or halted their exchange preparations due to legal challenges to the ACA and uncertainty about the fate of the exchanges. This means that fewer states may meet the timeline for implementation and will default to a federal or federal–state partnership exchange (KFF, 2012b).
30The Kaiser Family Foundation projects that the 2019 exchange population would be somewhat older, less educated, lower income, and more racially diverse than current privately insured populations. In addition, most individuals in this population will have transitioned from being previously uninsured (KFF, 2011a).
insurance plans and their receipt of relevant health care services would provide a fuller picture of the impact of the ACA on health care coverage and utilization for this population. MMP, which tracks private health insurance as a source of health care coverage for study participants, is one source of these data. Although they are proprietary, private health insurer enrollment and claims data could be used for larger-scale analyses. One source of such data is the Ingenix Normative Health Information Database® (NHID). NHID contains de-identified Health Insurance Portability and Accountability Act-compliant claims data from commercial health insurers, self-funded employer group plans, and Medicare Advantage plans. The commercial health insurer data consist of transaction-level claims data for more than 14 million covered lives annually from all 50 states and the District of Columbia. Of all individuals in the database at any time during 1994-2010, 67,929 had a diagnosis of HIV/AIDS. NHID includes claims-level information in the following categories that may be relevant to monitoring care for people with HIV under the ACA: care provided in physician offices or other outpatient ambulatory care settings such as urgent care or Minute-Clinics inpatient hospital stays; care provided at ambulatory centers, hospital clinics, and emergency rooms; self-administered prescription drugs; laboratory, imaging and diagnostic services; and goods or services related to specific episodes of care, such as reimbursed transportation (Dore, 2011).
CHALLENGES OF COMBINING DATA FROM DIFFERENT SOURCES
As discussed in detail in the committee’s first report, combining data from multiple data systems presents a range of analytic and logistical challenges. One challenge is the lack of interoperability among health information technology (IT) systems. Interoperability—the ability of different IT systems and software applications to communicate, exchange, and use information—is not fully possible in the United States at this time due to a lack of infrastructure to support it. For the most part, the various sources of health coverage and care for people with HIV have their own health IT systems with disparate architectures and vocabularies, posing a challenge to the exchange of data across systems (IOM, 2012).
A second challenge is the multiplicity of federal and state privacy laws designed to protect patient health information. The privacy and security of health information is particularly important to people with HIV and their providers. HIV continues to be a stigmatized disease (Sengupta et al., 2011). Besides HIV status, other patient information contained in health IT systems (e.g., information on drug use, sexually transmitted diseases, etc.) may be considered sensitive information and, if released, could potentially be used to discriminate against an individual. The current lack of an
infrastructure to support the secure exchange of health information across health IT systems (e.g., electronic health records) and organizations heightens privacy and security concerns because the accessibility of information may increase the potential for access and misuse by authorized and unauthorized users. Concern for patient privacy has led to numerous federal laws and state statutes and regulations on the proper use and disclosure of patient information with which care providers and data collection systems must contend. Although important to patient privacy, the often inconsistent nature of these protections, which leave the decision of whether or not to disclose requested patient information open to various interpretations, may result in discrepancies in data sharing and reporting across states and providers. Such discrepancies may influence the availability and quality of data needed to monitor trends in health care coverage and utilization.
A third challenge to combining data from multiple data systems relates to differences in the way that the systems operationalize data elements or define concepts to allow them to be measured. In addition, linkage between sources at the individual subject level may be uncertain or impossible, and even when linkages with high levels of certainty are possible, all of the relevant information may not be available on all subjects. Furthermore the level of precision of information may not be equal across studies and optimal estimation may have to take this into account as well (IOM, 2012).
Despite significant challenges such as these, advances are being made in the linkage and analysis of data from multiple disparate data systems. A number of large data linkage initiatives are under way, including linkages between the MSIS and the Current Population Survey; MSIS and NHIS; MSIS and the MEPS; survey data from the National Center for Health Statistics (NCHS) and death certificate records from the National Death Index; and survey data from NCHS and claims data from CMS (O’Grady and Mahmud, 2011).
On a smaller scale, the Louisiana Public Health Information Exchange (LaPHIE), described in the committee’s first report (IOM, 2012, Chapter 5), overcame technical and privacy barriers to implement electronic exchange of electronic medial record data and surveillance data between the Louisiana State University Health Care Services Division and the Louisiana Office of Public Health in order to identify people with HIV who have not been linked to or have fallen out of care (Herwehe et al., 2012). On a more general level, the Indiana Network for Patient Care has established the feasibility of linking records across different systems by successfully linking data from hospitals, public health departments, and state Medicaid programs (McDonald et al., 2005).
Ongoing research to develop “new” methodologies to address the statistical challenges of combining data sets, as well as financial and policy support, will be needed to ensure the sustainability of current linkage initia-
tives and to facilitate the development of new ones. Cross-agency efforts by the federal statistical agencies to examine potential linkage opportunities might accelerate developments in this area.
An alternative to combining data sets quantitatively for statistical analysis is the qualitative synthesis of data found in “public health triangulation,” “an iterative process in which key questions and hypotheses that potentially explain them are formulated, examined and reexamined as additional data become available” (Rutherford et al., 2010, p. 4). Such a process may permit the synthesis and interpretation of HIV-related data from disparate sources (e.g., surveillance, programs, research studies) for use in public health decision making, especially in the absence of or as a supplement to traditional intervention research and metaanalysis (Rutherford et al., 2010).
Altice, F. L., A. Kamarulzaman, V. V. Soriano, M. Schechter, and G. H. Friedland. 2010. Treatment of medical, psychiatric, and substance-use comorbidities in people infected with HIV who use drugs. Lancet 37:6367-6387.
Anema, A., N. Vogenthaler, E. A. Frongillo, S. Kadiyala, and S. D. Weiser. 2009. Food insecurity and HIV/AIDS: Current knowledge, gaps, and research priorities. Current HIV/AIDS Report 6(4):224-231.
Arici, C., D. Ripamonti, F. Maggiolo, M. Rizzi, M. G. Finazzi, P. Pezzotti, and F. Sutter. 2002. Factors associated with the failure of HIV-positive persons to return for scheduled medical visits. HIV Clinical Trials 3(1):52-57.
Baillargeon, J. G., T. P. Giordano, A. J. Harzke, G. Baillargeon, J. D. Rich, and D. P. Paar. 2010. Enrollment in outpatient care among newly released prison inmates with HIV infection. Public Health Reports 125(Suppl 1):64-71.
Blair, J. M., A. D. McNaghten, E. L. Frazier, J. Skarbinski, P. Huang, and J. D. Heffelfinger. 2011. Clinical and behavioral characteristics of adults receiving medical care for HIV infection—Medical Monitoring Project, United States, 2007. MMWR Surveillance Summaries 60(11):1-20.
Bowling, A. 2005. Mode of questionnaire administration can have serious effects on data quality. Journal of Public Health 27(3):281-291.
Bozzette, S. A., S. H. Berry, N. Duan, M. R. Grankel, A. A. Leibowitz, D. Lefkowitz, C. A. Emmons, J. W. Senterfitt, M. L. Berk, S. C. Morton, and M. F. Shapiro. 1998. The care of HIV-infected adults in the United States: HIV Cost and Services Utilization Study Consortium. New England Journal of Medicine 339(26):1897-1904.
Buchanan, D., R. Kee, L.S. Sadowski, and D. Garcia. 2009. The health impact of supportive housing for HIV-positive homeless patients: A randomized controlled trial. American Journal of Public Health 99(Suppl 3):S675-S680.
Buettgens, M., and M. Hall. 2011. Who Will be Insured After Health Insurance Reform? http://www.rwjf.org/files/research/71998.pdf (accessed August 6, 2012).
Butler, S. F., A. Villapiano, and A. Malinow. 2009. The effect of computer-mediated administration on self-disclosure of problems on the addiction severity index. Journal of Addiction Medicine 3(4):194-203.
Byrd, V. L. H., and J. Verdier. 2011. Collecting, Using, and Reporting Medicaid Encounter Data: A Primer for States. http://www.cms.gov/Research-Statistics-Data-and-Systems/Computer-Data-and-Systems/MedicaidDataSourcesGenInfo/Downloads/MAX_PDQ_Task_X_EncounterDataPrimerforStates.pdf (accessed August 20, 2012).
Carey, R. 2010. Health Insurance Exchanges: Key Issues for State Implementation. http://www.rwjf.org/files/research/70388.pdf (accessed July 12, 2012).
Catallozzi, M, and D. C. Futterman, 2005. HIV in adolescents. Current Infectious Disease Reports 7:401-405.
CDC (Centers for Disease Control and Prevention). 2009a. DHAP News. http://www.cdc.gov/hiv/resources/newsletter/dhap_news/102009/index.htm#link11 (accessed September 11, 2012).
CDC. 2009b. Q and A for Consumers. http://www.cdc.gov/hiv/topics/treatment/mmp/resources/patient.htm (accessed September 11, 2012).
CDC. 2009c. Q and A for Professional Partners. http://www.cdc.gov/hiv/topics/treatment/mmp/resources/provider.htm#pab (accessed September 11, 2012).
CDC. 2010a. Clinical and Behavioral Characteristics of Adults Receiving Medical Care for HIV Infection: Medical Monitoring Project, 2005 Pilot Data Collection Cycle. HIV Special Surveillance Report 6. http://www.cdc.gov/hiv/topics/surveillance/resources/reports/pdf/MMP_2005_Report_6.pdf (accessed September 11, 2012).
CDC. 2010b. Medical Monitoring Project. http://www.cdc.gov/hiv/topics/treatment/mmp/index.htm (accessed September 11, 2012).
CDC. 2010c. Medical Monitoring Project 2011 protocol.
CDC. 2010d. National Health Interview Survey. The Principal Source of Information on the Health of the U.S. Population. http://www.cdc.gov/nchs/data/nhis/brochure2010January.pdf (accessed August 30, 2012).
CDC. 2011a. About the National Health and Nutrition Examination Survey. http://www.cdc.gov/nchs/nhanes/about_nhanes.htm (accessed August 30, 2012).
CDC. 2011b. HIV among Youth. http://www.cdc.gov/hiv/youth/pdf/youth.pdf (accessed August 31, 2012).
CDC. 2011c. HIV Infection Reporting. http://www.cdc.gov/hiv/topics/surveillance/reporting.htm (accessed September 11, 2012).
CDC. 2011d. NHANES Response Rates and CPS Totals. http://www.cdc.gov/nchs/nhanes/response_rates_cps.htm (accessed August 26, 2012).
CDC. 2012a. About the National Health Interview Survey. http://www.cdc.gov/nchs/nhis/about_nhis.htm/ (accessed August 26, 2012).
CDC. 2012b. HIV Surveillance Report. Diagnoses of HIV Infection and AIDS in the United States and Dependent Areas, 2010. Volume 22.
CDC. 2012c. Medical Monitoring Project 2012 protocol.
CDC. 2012d. Medical Monitoring Project. Supporting Statement Part A. http://www.reginfo.gov/public/do/PRAViewDocument?ref_nbr=201203-0920-011 (accessed September 18, 2012).
CDC. 2012e. Report on the Use of Centers for Disease Control and Prevention’s Medical Monitoring Project to Monitor the Implementation of the Affordable Care Act. Submission to committee. January.
CDC. 2012f. Standard Questionnaire for Medical Monitoring Project, 2012.
Chen, N. E., J. P. Meyer, A. K. Avery, J. Draine, T. P. Flannigan, T. Lincoln, A. C. Spaulding, S. A. Springer, and F. L. Altice. 2011. Adherence to HIV treatment and care among previously homeless jail detainees. AIDS and Behavior (November 8). DOI 10.1007/s10461-011-0080-2.
Choi, K. H., W. McFarland, T. B. Neilands, S. Nguyen, G. Secura, S. Behel, D. Mackellar, and L. Valleroy. 2005. High level of hepatitis B infection and ongoing risk among Asian/Pacific Islander men who have sex with men, San Francisco, 2000-2001. Sexually Transmitted Diseases 32(1):44-48.
CMS (Centers for Medicare & Medicaid Services). 2012a. Closing the Coverage Gap. http://www.medicare.gov/publications/pubs/pdf/11493.pdf (accessed September 11, 2012).
CMS. 2012b. Medicaid Statistical Information System. http://www.cms.gov/ResearchStatistics-Data-and-Systems/Computer-Data-and-Systems/MSIS/index.html (accessed September 11, 2012).
CMS. 2012c. Medicaid Statistical Information System (MSIS) State Summary Datamart. http://www.cms.gov/Research-Statistics-Data-and-Systems/Computer-Data-and-Systems/MedicaidDataSourcesGenInfo/MSIS-Mart-Home.html (accessed September 11, 2012).
CMS. 2012d. Prevention—General Information. http://www.cms.gov/Medicare/Prevention/PrevntionGenInfo/index.html?redirect=/PrevntionGenInfo/ (accessed September 11, 2012).
CMS. 2012e. Quick reference information: Preventive services. https://www.cms.gov/Medicare/Prevention/PrevntionGenInfo/Downloads/MPS_QuickReferenceChart_1.pdf (accessed September 11, 2012).
Cohen, M. S., Y. Q. Chen, M. McCauley, T. Gamble, M. C. Hosseinipour, N. Kumarasamy, J. G., Hakim, J. Kumwenda, B. Grinsztein, J. H. S. Pilotto, S. V. Godbole, S. Mehendale, S. Charjvalertsak, B. R. Santos, K. H. Mayer, I. F. Hoffman, S. H. Eshelman, E. PiwowarManning, L. Wang, J. Makhema, L. A. Mills, G. de Bruyn, I. Sanne, J. Eron, J. Gallant, D. Havlir, S. Swindells, H. Ribaudo, V. Elharrar, D. Burns, T. E. Taha, K. Nielsen-Saines, D.Celentano, M. Essex, and T. R. Fleming. 2011. Prevention of HIV-1 infection with early antiretroviral therapy. New England Journal of Medicine 365:493-505.
Coleman, S., U. Boehmer, F. Kanaya, C. Grasso, J. Tan, and J. Bradford. 2007. Retention challenges for a community-based HIV primary care clinical and implications for intervention. AIDS Patient Care STDs 21(9):691-701.
Coughlin, S. S. 1990. Recall bias in epidemiologic studies. Journal of Clinical Epidemiology 43(1):87-91.
Cross, J. 2011. Pre-existing Condition Insurance Plans (PCIPs). July 13. http://prod.nastad.dotnet-web1.advansiv.com/Docs/094424_presentation_NASTAD_PCIP_July2011.pdf (accessed August 30, 2012).
Crystal, S., A. Akincigil, S. Bilder, and J. T. Walkup. 2007. Studying prescription drug use and outcomes with Medicaid claims data: Strengths, limitations, and strategies. Medical Care 45(10 Suppl 2):S58-S65.
Daily Briefing. 2012. Where Each State Stands on ACA’s Medicaid Expansion: A Roundup of What Each State’s Leadership Has Said About Their Medicaid Plans. http://www.advisory.com/Daily-Briefing/2012/07/05/Where-each-state-stands-of-the-Medicaidexpansion (accessed September 11, 2012).
Dang, B. N., T. P. Giordano, and J. H. Kim. 2012. Sociocultural and structural barriers to care among undocumented Latino immigrants with HIV infection. Journal of Immigrant and Minority Health 14(1):124-131.
Dore, D. 2011. Commercial Health Insurance Claims Data for Studying HIV/AIDS Care. 2011. Presentation to committee. April 28.
Drapeau, A., R. Boyer, and F. B. Diallo. 2011. Discrepancies between survey and administrative data on the use of mental health services in the general population: Findings from a study conducted in Quebec. BMC Public Health 11:837.
Fagan, J. L., J. Bertolli, and A. D. McNaghten. 2010. Understanding people who have never received HIV medical care: A population-based approach. Public Health Reports 125(4):520-527.
Forney, J. C., R. L. Miller, and City Project Study Team. 2012. Risk and protective factors related to HIV-risk behavior: A comparison between HIV-positive and HIV-negative young men who have sex with men. AIDS Care 24(5):544-552.
Frankel, M. R., M. F. Shapiro, N. Duan, S. C. Morton, S. H. Berry, J. A. Brown, M. A. Burnam, S. E. Cohn, D. P. Goldman, D. F. McCaffrey, S. M. Smith, P. A. St. Clair, J. F. Tebow, and S. A. Bozzette. 1999. National probability samples in studies of low-prevalence diseases. Part II: Designing and implementing the HIV cost and services utilization study sample. Health Services Research 345(5, Part 1):969-992.
Gardner, E. M., M. P. McLees, J. F. Steiner, C. del Rio, and W. J. Burman. 2011. The spectrum of engagement in HIV care and its relevance to test-and-treat strategies for prevention of HIV infection. Clinical Infectious Diseases 52(6):793-800.
Gorina, Y., and E. A. Kramarow. 2011. Identifying chronic conditions in Medicare claims data: Evaluating the Chronic Condition Data Warehouse algorithm. Health Services Research 45(5):1610-1627.
Granich, R. M., C. F. Gilks, C. Dye, K. M. De Cock, and B. G. Williams. 2009. Universal voluntary HIV testing with immediate antiretroviral therapy as a strategy for elimination of HIV transmission: A mathematical model. Lancet 373(9657):48-57.
Grov, C., B. C. Kelly, and J. T. Parsons. 2009. Polydrug use among club-going young adults recruited through time-space sampling. Substance Use and Misuse 44(6):848-864.
Groves, R. M., M. P. Couper, S. Presser, E. Singer, R. Tourangeau, G. P. Acosta, and L. Nelson. 2006. Experiments in producing non-response bias. Public Opinion Quarterly 70(5): 720-736.
Hennekens, C. H., and J. E. Buring. 1987. Epidemiology in Medicine. Boston, MA: Little Brown and Company.
Herwehe, J., W. Wilbright, A. Abrams, S. Bergson, J. Foxhood, M. Kaiser, L. Smith, K. Xiao, A. Zapata, and M. Magnus. 2012. Implementation of an innovative, integrated electronic medical record (EMR) and public health information exchange for HIV/AIDS. Journal of the American Medical Informatics Association 19(3):448-452.
HHS (U.S. Department of Health and Human Services). 2009. Office of the Inspector General. 2009. Medicaid Managed Care Encounter Data: Collection and Use. http://oig.hhs.gov/oei/reports/oei-07-06-00540.pdf (accessed August 20, 2012).
HHS. 2011. How the Affordable Care Act Helps People Living with HIV/AIDS: 2011 and Beyond. http://www.healthcare.gov/news/factsheets/2011/11/hiv-aids11092011a.html (accessed September 11, 2012).
HHS. 2012a. Frequently Asked Questions About PRA/Information Collection. http://www.hhs.gov/ocio/policy/collection/infocollectfaq.html#4 (accessed September 11, 2012).
HHS. 2012b. Health Care Reform and HIV/AIDS. http://aids.gov/federal-resources/policies/health-care-reform/ (accessed September 11, 2012).
HHS. 2012c. Ryan White HIV/AIDS Program Modeling Study. Paperwork Reduction Act Supporting Statement Part A. http://www.reginfo.gov/public/do/PRAViewDocument?ref_nbr=201206-0990-003 (accessed August 6, 2012).
HHS. 2012d. The Affordable Care Act: Strengthening Medicare in 2011. http://www.cms.gov/apps/files/MedicareReport2011.pdf (accessed September 11, 2012).
Hill, T., L. Bansi, C. Sabin, A. Phillips, D. Dunn, J. Anderson, P. Easterbrook, M. Fisher, B. Gazzard, R. Gilson, M. Johnson, C. Leen, C. Orkin, A. Schwenk, J. Walsh, A. Winston, A. Babiker, and V. Delpech. 2010. Data linkage reduces loss to follow-up in an observational HIV cohort study. Journal of Clinical Epidemiology 63(10):1101-1109.
HRSA (Health Resources and Services Administration). 2010. Going the Distance: The Ryan White HIV/AIDS Program. http://www.impactmc.net/downloads/samples/writing/Goingthe-Distance-20-years-of-the-Ryan-White-HIV-AIDS-Program.pdf (accessed September 11, 2012).
HRSA. 2012a. About the Ryan White HIV/AIDS Program: Legislation. http://hab.hrsa.gov/abouthab/aboutprogram.html (accessed September 11, 2012).
HRSA, 2012b. AIDS Drug Assistance Program. Quarterly Data Report. http://hab.hrsa.gov/manageyourgrant/adap/adapformfeb08.pdf (accessed August 6, 2012).
HRSA. 2012c. Crosswalk of Changes between the Proposed ADAP Data Report (ADR) Client Report and the ADAP Quarterly Report (AQR). http://hab.hrsa.gov/manageyourgrant/files/adraqrcrosswalk.pdf (accessed August 7, 2012).
HRSA. 2012d. The Ryan White HIV/AIDS Program Services Report. http://hab.hrsa.gov/manageyourgrant/clientleveldata.html (accessed August 6, 2012).
Hunt, J. R., and E. White. 1998. Retaining and tracking cohort study members. Epidemiologic Reviews 20(1):57-70.
Iachan, R., T. Kyle, and D. Farrell. 2011. Real time sampling in patient surveys. Joint Statistical Meetings—Section on Government Statistics.
Ikard, K., J. Janney, L. C. Hsu, D. J. Isenberg, M. B. Scalco, S. Schwarcz, L. Beer, D. A. Wendell, P. E. Franks, and J. G. Kahn. 2005. Estimation of unmet need for HIV primary medical care: A framework and three case studies. AIDS Education and Prevention 17(6 Suppl B):26-38.
IOM (Institute of Medicine). 2004. Measuring What Matters: Allocation, Planning, and Quality Assessment for the Ryan White CARE Act. Washington, DC: The National Academies Press.
IOM. 2012. Monitoring HIV Care in the United States: Indicators and Data Systems. Washington, DC: The National Academies Press.
Kalichman, S.C., J. Pellowski, M.O. Kalichman, C. Cherry, M. Detorio, A. M. Caliendo, and R. F. Schinazi. 2011. Food insufficiency and medication adherence among people living with HIV/AIDS in urban and peri-urban settings. Prevention Science 12(3):324-332.
Kates, J. 2011. Medicaid and HIV: A National Analysis. Washington, DC: Henry J. Kaiser Family Foundation. http://www.kff.org/hivaids/upload/8218.pdf (accessed September 11, 2012).
Kelley, K., B. Clark, V. Brown, and J. Sitzia. 2003. Good practice in the conduct and reporting of survey research. International Journal for Quality in Health Care 15(3):261-266.
KFF (Kaiser Family Foundation). 2006. The Role of Part D for People with HIV/AIDS: Coverage and Costs of Antiretrovirals Under Medicare Drug Plans. http://www.kff.org/hivaids/upload/7548.pdf (accessed September 11, 2012).
KFF. 2009. Medicare and HIV/AIDS. HIV/AIDS Policy Fact Sheet. February. http://www.kff.org/hivaids/upload/7171_04.pdf (accessed September 11, 2012).
KFF. 2010. Explaining Health Care Reform: Questions About Health Insurance Exchanges. http://www.kff.org/healthreform/7908.cfm (accessed September 11, 2012).
KFF. 2011a. A Profile of Health Insurance Exchange Enrollees. http://www.kff.org/healthreform/upload/8147.pdf (accessed September 11, 2012).
KFF. 2011b. The Ryan White Program. HIV/AIDS Policy Fact Sheet. November. http://www.kff.org/hivaids/upload/7582-06.pdf (accessed August 6, 2012).
KFF. 2012a. AIDS Drug Assistant Programs (ADAPs). HIV/AIDS Policy Fact Sheet. May. http://www.kff.org/hivaids/upload/1584-11.pdf (accessed September 11, 2012).
KFF. 2012b. State Health Facts. State Action Toward Creating Health Insurance Exchanges, August 1, 2012. http://statehealthfacts.kff.org/comparemaptable.jsp?ind=962&cat=17 (accessed September 11, 2012).
Klein, J. 2002. Report on the Use of Medi-Cal Managed Care Encounter Data for Research Purposes. http://www.dhcs.ca.gov/dataandstats/statistics/Documents/Report%20on%20the%20Use%20of%20Medi-Cal%20Managed%20Care%20Encounter%20Data%20for%20Research%20Purposes.pdf (accessed November 5, 2012).
Koroukian, S. M., G. S. Cooper, and A. A. Rimm. 2003. Ability of Medicaid claims data to identify incident cases of breast cancer in the Ohio Medicaid population. Health Services Research 38(3):947-960.
Lo, Y. C., G. Turabelidze, M. Lin, and Y. Friedberg. 2012. Prevalence and determinants of recent HIV testing among sexually active men who have sex with men in the St. Louis metropolitan area, Missouri, 2008. Sexually Transmitted Diseases 39(4):306-311.
Martin, E.G., and B. R. Schackman. 2012. What does U.S. health reform mean for HIV clinical care? Journal of Acquired Immune Deficiency Syndrome. 2012 May 1;60(1):72-6.
McDonald, C. J., J. M. Overhage, M. Barnes, G. Schadow, L. Blevins, P. R. Dexter, B. Mamlin, and the INPC Management Committee. 2005. The Indiana Network for Patient Care: A working local health information infrastructure. Health Affairs 24(5):1214-1220.
McNaghten, A. D., M. I. Wolfe, I. Onorato, A. K. Nakashima, R. O. Valdiserri, E. Mokotoff, R. A. Romaguera, A. Kroliczak, R. S. Janssen, and P. S. Sullivan. 2007. Improving the representativeness of behavioral and clinical surveillance for persons with HIV in the United States: The rationale for developing a population-based approach. PLoS One 2(6):e550. doi:10.1371/journal.pone.0000550.
Mellins, C. A., J. F. Havens, C. McDonnell, C. Lichtenstein, K. Uldall, M. Chesney, E. K. Santamaria, and J. Bell. 2009. Adherence to antiretroviral medications and medical care in HIV-infected adults diagnosed with mental and substance abuse disorders. AIDS Care 21(2):168-177.
Mocroft, A., O. Kirk, P. Aldins, A. Chies, A. Blaxhult, N. Chentsova, N. Vetter, F. Dabis, J. Gatell, and J. D. Lundgren. 2008. Loss to follow-up in an international, multicentre observational study. HIV Medicine 9(5):261-269.
O’Grady, M. J., and A. Mahmud. 2011. The Next Generation of Data Linkage Projects: Priority Areas for SNACC under the ACA. http://www.shadac.org/files/SNACCDataLinkageBrief_1of3.pdf (accessed September 12, 2012).
Olatosi, B. A., J. C. Probst, C. H. Stoskoph, A. B. Martin, and W. A. Duffus. 2009. Patterns of engagement in care by HIV-infected adults: South Carolina, 2004-2006. AIDS 23(6):725-730.
Parsons, J. T., C. Gov, and B. C. Kelly. 2008. Comparing the effectiveness of two forms of time-space sampling to identify club drug-using young adults. Journal of Drug Issues 38(4):1061-1081
Perkins, D., B. E. Meyerson, D. Klinkenberg, and B. T. Laffoon. 2008. Assessing HIV care and unmet need: Eight databases and a bit of perseverance. AIDS Care 20(3):318-326.
RAND. 2011. HIV Cost and Services Utilization Study (HCSUS). http://www.rand.org/health/projects/hcsus.html (accessed July 17, 2012).
Rein, D. B. 2007. Should Patient Characteristics be Included in a Severity of Need Index for Ryan White Program, Part A Services? An Evaluation Based on the Medical Expenditure Panel Survey http://hab.hrsa.gov/manageyourgrant/severityofneed/supppatient.pdf (accessed August 30, 2012).
ResDAC. 2006. Medicaid Analytic eXtract (MAX) data FAQ. www.resdac.org/medicaid/FAQs-draft-08172006.doc (accessed June 20, 2012).
ResDAC. 2012. Medicaid data available. http://www.resdac.org/Medicaid/data_available.asp (accessed June 20, 2012).
Rutherford, G. W., W. McFarland, H. Spindler, K. White, S. V. Patel, J. Aberle-Grasse, K. Sabin, N. Smith, S. Taché, J. M. Calleja-Garcia, and R. L. Stoneburner. 2010. Public health triangulation: Approach and application to synthesizing data to understand national and local HIV epidemics. BMC Public Health 10:477.
SAMHSA (Substance Abuse and Mental Health Services Administration). 2011. Results from the 2010 National Survey on Drug Use and Health: Summary of National Findings. http://www.samhsa.gov/data/nsduh/2k10nsduh/2k10results.htm#TabB-5 (accessed November 5, 2012).
Sarnquist, C. C., S. Soni, H. Hwang, B. B. Topol, S. Mutima, and Y. A. Maldonado. 2011. Rural HIV-infected women’s access to medical care: Ongoing needs in California. AIDS Care 23(7):793-796.
Schiller, J. S., J. W. Lucas, B. W. Ward, and J. A. Peregoy. 2012. Summary health statistics for U.S. adults: National Health Interview Survey, 2010. National Center for Health Statistics. Vital Health Statistics 10(252).
Schneider, K., B. O’Donnell, J. O’Donnell, and C. Powers. 2010. Technical Guidance for Researchers Summarizing and Describing Prescription Drug Utilization. http://www.ccwdata.org/cs/groups/public/documents/document/ccw_part_d_tech_guidance.pdf (accessed July 12, 2012).
Sengupta, S., B. Banks, D. Jonas, M. S. Miles, and G. C. Smith. 2011. HIV interventions to reduce HIV/AIDS stigma: A systematic review. AIDS and Behavior 15(6):1075-1087.
Shapiro, M., M. L. Berk, S. H. Berry, C. Emmons, L. A. Athey, D. C. Hsia, A. A. Leibowitz, C. A. Maida, M. Marcus, J. F. Perlman, C. L. Schur, M. A. Schuster, J. W. Senterfitt, and S. A. Bozzette. 1999. National probability samples in studies of low prevalence diseases. Part I: Perspectives and lessons learned from the HIV Costs and Services Utilization Study. Health Services Research 34(5, Part 1):951-968.
Spiegel, H. M. L., and D. C. Futterman. 2009. Adolescents and HIV: Prevention and clinical care. Current HIV/AIDS Reports 6(2):100-107.
Springer, S. A., A. C. Spaulding, J. P. Meyer, and F. L. Altice. 2011. Public health implications for adequate transitional care for HIV-infected prisoners: Five essential components. Clinical Infectious Diseases 53(5):469-479.
Tourangeau, R., and T. W. Smith. 1996. Asking sensitive questions: The impact of data collection mode, question format, and question context. Public Opinion Quarterly 60:275-304.
Tourangeau, R., K. Raskinski, J.B. Jobe, T. W. Smith, and W. F. Pratt. 1997. Sources of error in a survey of sexual behavior. Journal of Official Statistics 13:341-365.
UNAIDS. 2010. UNAIDS Report on the Global AIDS Epidemic 2010. http://www.unaids.org/GlobalReport/Global_report.htm (accessed August 30, 2012).
|
|
||
| Characteristic | No.a | %b |
|
|
||
| Genderc | ||
| Male | 2,633 | 72 |
| Female | 959 | 26 |
| Transgender | 47 | 1 |
| Self-reported sexual orientation | ||
| Heterosexual or straight | 1,791 | 49 |
| Homosexual, gay, or lesbian | 1,514 | 42 |
| Bisexual | 278 | 8 |
| Race/Ethnicityd | ||
| Black, non-Hispanic | 1,438 | 40 |
| White, non-Hispanic | 1,272 | 35 |
| Hispanic or Latino | 699 | 19 |
| American Indian/Alaska Native | 19 | <1 |
| Asian | 19 | <1 |
| Native Hawaiian/Pacific Islander | 11 | <1 |
| Multiracial | 119 | 3 |
| Other | 61 | 2 |
| Age at time of interview (yrs) | ||
| 18-24 | 73 | 2 |
| 25-29 | 143 | 4 |
| 30-34 | 219 | 6 |
| 35-39 | 481 | 13 |
| 40-44 | 720 | 20 |
| 45-49 | 807 | 22 |
| 50-54 | 589 | 16 |
| 55-59 | 340 | 9 |
| 60-64 | 161 | 4 |
| ≥65 | 110 | 3 |
| Education | ||
| <High school | 790 | 22 |
| High school diploma or GED credential | 987 | 27 |
| >High school | 1,865 | 51 |
| Country/territory of birth | ||
| United States | 2,984 | 82 |
| Puerto Rico | 281 | 8 |
| Mexico | 103 | 3 |
| Other | 273 | 8 |
| Time since HIV diagnosis | ||
| ≥5 yrs | 2,836 | 78 |
| <5 yrs | 785 | 22 |
| Homeless at any time during past 12 monthse | ||
| Yes | 280 | 8 |
| No | 3,363 | 92 |
|
|
||
| Characteristic | No.a | %b |
|
|
||
| Health insurance or coverage during past 12 months | ||
| Yes | 3,040 | 84 |
| No | 599 | 16 |
| Type of health insurance or coverage during past 12 monthsf | ||
| Medicaid | 1,366 | 45 |
| Private health insurance or HMO | 1,136 | 37 |
| Medicare | 896 | 30 |
| Otherg | 475 | 16 |
| Primary method of paying for prescription medications for HIV and related illnesses during past 12 monthsh | ||
| Medicaid/Medicare | 1,509 | 41 |
| Private health care coverage | 896 | 25 |
| AIDS Drug Assistance Program | 915 | 25 |
| Not taking any prescription medications for HIV or related illnesses | 187 | 5 |
| Paid for medications themselves (i.e., out of pocket) | 194 | 5 |
| Received medications from a public clinic | 88 | 2 |
| Received medications from an AIDS service organization | 50 | 1 |
| Participated in a clinical trial or research study that provided medications | 12 | <1 |
| Applied for public assistance during past 12 months | ||
| Yes | 708 | 19 |
| No Received any form of public assistance including SSI or SSDI during past 12 months | 2,932 | 81 |
| Yes | 1,798 | 49 |
| No | 1,843 | 51 |
| Primary source of money or financial support during past 12 months | ||
| SSI or SSDI | 1,463 | 40 |
| Salary or wages | 1,403 | 39 |
| Spouse, partner, or family | 244 | 7 |
| Public assistance | 211 | 6 |
| Pension or retirement fund | 81 | 2 |
| No income or financial support | 43 | 1 |
| Friends | 35 | 1 |
| Savings/investments | 28 | <1 |
| Total | 3,643 | 100 |
|
|
||
NOTE: GED = general equivalency degree; HMO = health maintenance organization; SSDI = Social Security Disability Insurance; SSI = Social Security Supplemental Income.
aNumbers might not add to total because of missing data. Analyses limited to persons with diagnosis of HIV infection for at least 12 months before the interview. Values exclude categories with fewer than five responses, responses of “don’t know,” and skipped (missing) responses.
bPercentages may not add to 100% because of rounding.
cParticipants were classified as transgender if sex at birth and gender reported by the participant were different or if the participant chose transgender in response to the question about self-identified gender.
dHispanics or Latinos might be of any race.
eMcKinney-Vento definition of homelessness: living on the street, in a shelter, in a single-room occupancy hotel, temporarily staying with friends or family, or living in a car. A person is categorized as homeless if that person lacks a fixed, regular, adequate nighttime residence or has a steady nighttime residence that is (1) a supervised publicly or privately operated shelter designed to provide temporary living accommodation, (2) an institution that provides a temporary residence for persons intended to be institutionalized, or (3) a public or private place not designed for or ordinarily used as a regular sleeping accommodation for human beings (e.g., in an automobile or under a bridge) (Stewart B. McKinney Homeless Assistance Act, 42 U.S.C. § 11301, et seq.; 1987).
fAmong 3,040 participants who reported having health insurance or coverage during the past 12 months. Participants could select more than one response.
gIncludes Tricare/CHAMPUS, Veterans Administration coverage, and insurance classified as “other” health insurance.
hParticipants could select more than one response.
SOURCE: Submission to committee, January 2012.
| Indicator | Does MMP Adhere to Indicators? | Question ID | Questions Collecting Data Related to Indicator |
| Proportion of people newly diagnosed with HIV with a CD4+ cell count >200 cells/mm3 and without a clinical diagnosis of AIDS | Yes | From questionnaire: | |
| A1 |
• What month and year did you first test positive for HIV? Tell me when you got your result, not when you got your first test. (MM/YYYY; Refused to answer; Don’t know) |
||
| C2a |
• What was the result of your most recent CD4 count? (0-49; 50-99; 100-199; 200-349; 350-499; 500 or more; Refused to answer; Don’t know) |
||
| C8 |
• Have you ever been told by a doctor, nurse, or other health care worker that you had PCP [Pneumocystis jirovecii pneumonia]? (No; Yes; Refused to answer; Don’t know) |
||
| From medical record abstraction forms: | |||
|
• Is there documentation that any AIDS defining opportunistic illnesses (AIDS OI) were diagnosed prior to the SP start date? (If yes, abstractor checks which AIDS OI was diagnosed and enters the date of first diagnosis) (MHF) |
|||
|
• Is there documentation of CD4 cell count test results prior to the SP start date? (If yes, abstractor enters lowest CD4 count and date of lowest CD4 count) (MHF) |
|||
|
• Is there documentation of any new or existing diagnoses of AIDS defining opportunistic illnesses (AIDS OI) during this visit? (If yes, abstractor checks which AIDS OI was diagnosed) (SPVF) |
|||
|
• Is there documentation of CD4 cell count done at this visit? (If yes, abstractor enters value) (SPVF) |
|||
|
• Is there documentation of any new or existing diagnoses of AIDS defining opportunistic illnesses (AIDS OI) during this inpatient stay? (If yes, abstractor checks which AIDS OI was diagnosed) (SPIF) |
|||
|
• Is there documentation of CD4 cell count test results during this inpatient stay? (If yes, abstractor enters value) (SPIF) |
|||
| Proportion of people newly diagnosed with HIV who are linked to clinical care for HIV within 3 months of diagnosis | Yes | A1 | From questionnaire: |
|
• What month and year did you first test positive for HIV? Tell me when you got your result, not when you got your first test. (MM/YYYY; Refused to answer; Don’t know) |
|||
| A5 |
• Since testing positive for HIV, what month and year did you first visit a doctor, nurse, or other health care worker for HIV medical care? (MM/YYYY; Refused to answer; Don’t know) |
||
| From medical record abstraction forms: | |||
|
• (Newly diagnosed) Is there documentation of the first positive HIV test result, or laboratory test results for CD4 cell count, or HIV viral load, prior to the SP start date? (If yes, abstractor enters date of first positive test result). (MHF) |
|||
| Proportion of people with diagnosed HIV infection who are in continuous care (two or more visits for routine HIV medical care in the preceding 12 months at least 3 months apart) | Yes | From questionnaire: | |
| A8 |
• During the past 12 months, was there one usual place, like a doctor’s office or clinic, where you went for most of your HIV medical care? (No; Yes; Refused to answer; Don’t know) |
||
| A10 |
• What is the name of this place where you went for most of your HIV medical care during the past 12 months? |
||
| A10a |
• Did you get any sort of care at [USE FACILITY NAME] between [INSERT START DATE] and [INSERT END DATE]? (No; Yes; Refused to answer; Don’t answer) |
||
| A10b |
• Between [INSERT START DATE] and [INSERT END DATE], how many times had you been to [USE FACILITY NAME] for any sort of care? (__ __ __; Refused to Answer; Don’t know) |
| Indicator | Does MMP Adhere to Indicators? | Question ID | Questions Collecting Data Related to Indicator |
| From medical record abstraction forms: Dates of visits for medical care and dates of laboratory test results, etc. | |||
| Proportion of people with diagnosed HIV infection who received two or more CD4 tests in the preceding 12 months | Yes | C3 | From questionnaire: |
|
• During the past 12 months, how many CD4 counts have you had? (__ __; Refused to answer; Don’t know) |
|||
| From medical record abstraction forms: • Is there documentation of CD4 cell count done at this visit? (If yes, abstractor enters value) (SPVF) | |||
|
• Is there documentation of CD4 cell count test results during this inpatient stay? (If yes, abstractor enters value) (SPIF) |
|||
| Proportion of people with diagnosed HIV infection who received two or more viral load tests in the preceding 12 months | Yes | C6 | From questionnaire: |
|
• During the past 12 months, how many viral load tests have you had? (__ __; Refused to answer; Don’t know) |
|||
| From medical record abstraction forms: | |||
|
• Is there documentation of HIV viral load test done at this visit? (If yes, abstractor enters value) (SPVF) |
|||
|
• Is there documentation of HIV viral load test results during this inpatient stay? (If yes, abstractor enters value) (SPIF) |
|||
| Proportion of people with diagnosed HIV infection in continuous care for 12 or more months and with a CD4+ cell count ≥350 cells/mm3 | Yes | From questionnaire: | |
| C2a |
• What was the result of your most recent CD4 count? (0-49; 50-99; 100-199; 200-349; 350-499; 500 or more; Refused to answer; Don’t know) |
||
| A8 |
• During the past 12 months, was there one usual place, like a doctor’s office or clinic, where you went for most of your HIV medical care? (No; Yes; Refused to answer; Don’t know) |
||
| A10 |
• What is the name of this place where you went for most of your HIV medical care during the past 12 months? |
||
| A10a |
• Did you get any sort of care at [USE FACILITY NAME] between [INSERT START DATE] and [INSERT END DATE]? (No; Yes; Refused to answer; Don’t know) |
||
| A10b |
• Between [INSERT START DATE] and [INSERT END DATE], how many times had you been to [USE FACILITY NAME] for any sort of care? (__ __ __; Refused to Answer; Don’t know) |
||
| From medical record abstraction forms: | |||
|
• Dates of visits for medical care and dates of laboratory test results, etc. |
|||
|
• Is there documentation of CD4 cell count test results prior to the SP start date? (If yes, abstractor enters lowest CD4 cell count and date of lowest CD4 count) (MHF) |
|||
|
• Is there documentation of CD4 cell count done at this visit? (If yes, abstractor enters value) (SPVF) |
|||
|
• Is there documentation of CD4 cell count test results during this inpatient stay? (If yes for CD4 count, abstractor enters value) (SPIF) |
|||
| Indicator | Does MMP Adhere to Indicators? | Question ID | Questions Collecting Data Related to Indicator |
| Proportion of people with diagnosed HIV infection with a measured CD4+ cell count <500 cells/mm3 who are not on ART | Yes | From questionnaire: | |
| C2a |
• What was the result of the most recent CD4 count? (0-49; 50-99; 100-199; 200-349; 350-499; 500 or more; Refused to answer; Don’t know) |
||
| T4 |
• Are you currently taking any antiretroviral medicines for your HIV? (No; Yes; Refused to answer; Don’t know) |
||
| From medical record abstraction forms: | |||
|
• Is there documentation of CD4 cell count test results prior to the SP start date? (If yes, abstractor enters lowest CD4 cell count and date of lowest CD4 count) (MHF) |
|||
|
• Is there documentation of CD4 cell count done at this visit? (If yes, abstractor enters value) (SPVF) |
|||
|
• Is there documentation of CD4 cell count results during this inpatient stay? (If yes, abstractor enters value) (SPIF) |
|||
|
• Is there documentation of prescription of antiretroviral therapy (ART) prior to the SP start date? (If yes, abstractor enters date of first prescribed ART) (MHF) |
|||
|
• Is there documentation of prescription or continuation of antiretroviral therapy (ART) during this visit? (If yes, abstractor enters the type of ART prescribed) (SPVF) |
|||
|
• Is there documentation of prescription of antiretroviral therapy (ART) during this inpatient stay? (If yes, abstractor enters the type of ART prescribed) (SPIF) |
|||
| Proportion of people with diagnosed HIV infection who have been on ART for 12 or more months and have a viral load below the level of detection | Yes | From questionnaire: | |
| C5b |
• What was the month and year of your most recent viral load? (MM/YYYY; Refused to answer; Don’t know) |
||
| C5c |
• What was the result of your most recent viral load test? (Below the level of detection, undetectable; detectable, but less than 5,000 viral copies/ml; 5,000 to 100,000 viral copies/ml; Greater than 100,000 viral copies/ml; Refused to answer; Don’t know) |
||
| T3 |
• When was the first time you ever took any antiretroviral medicines for your HIV? (MM/YYYY; Refused to answer; Don’t know) |
||
| T4 |
• Are you currently taking any antiretroviral medicines for your HIV? (No; Yes; Refused to answer; Don’t know) |
||
| T14 |
• During the past 12 months, have you taken any antiretroviral medicines? (No; Yes; Refused to answer; Don’t know) |
||
| T16 |
• During the past 12 months, have you ever purposefully taken a “drug holiday” from your antiretroviral medicines that wasn’t recommended by your doctor? That is, did you plan to not take any doses of one or more of your antiretroviral medicines for at least two whole days in a row? (No; Yes; Refused to answer; Don’t know) |
| Indicator | Does MMP Adhere to Indicators? | Question ID | Questions Collecting Data Related to Indicator |
|
From medical record abstraction forms:
• Is there documentation of prescription of antiretroviral therapy (ART) prior to the SP start date? (If yes, abstractor enters date of first prescribed ART) (MHF) • Is there documentation of the first positive HIV test result, or laboratory test results for CD4 cell count, or HIV viral load, prior to the SP start date? (If yes for viral load, abstractor enters date of most recent undetectable result) (MHF) • Is there documentation of prescription or continuation of antiretroviral therapy (ART) during this visit? (Yes; No) (SPVF) • Is there documentation of any of HIV viral load test done at this visit? (If yes, abstractor enters value) (SPVF) • Is there documentation of prescription of antiretroviral therapy (ART) during this inpatient stay? (Yes; No) (SPIF) • Is there documentation of any HIV viral load test during this inpatient stay? (If yes, abstractor enters value) (SPIF) |
|||
| All-cause mortality rate among people diagnosed with HIV infection | Yes | Section XI |
From medical record abstraction forms:
• Is there documentation that the patient died during the SP? (Yes/No) If yes: o Date of death during the Surveillance Period (MM/DD/YYYY) o Cause of death (accident, homicide, suicide, natural, other (specify), cause not documented) (SPSF) |
| Proportion of people with diagnosed HIV infection and mental health disorder who are referred for mental health services and receive these services within 60 days | No | From questionnaire: | |
| A18 |
• During the past 12 months, were you enrolled in an inpatient mental health facility? (No; Yes; Refused to answer; Don’t know) |
||
| A26a |
• During the past 12 months, did you get mental health services? (No; Yes; Refused to answer; Don’t know) |
||
| A26b |
• During the past 12 months, have you needed mental health services? (No; Yes; Refused to answer; Don’t know) |
||
| From medical record abstraction forms: | |||
|
• Is there documentation of any of the following mental illnesses prior to the SP start date? (Anxiety disorder [generalized anxiety disorder, GAD], Bipolar disorder, Depression [major depression, depressive disorder], Psychosis) (MHF) |
|||
|
• Is there documentation of any of the following referrals during the SP? (Responses include referrals for mental health services) (SPSF) |
|||
|
• Is there documentation of any new or existing diagnoses of conditions other than AIDS OI during this visit? (If yes, abstractor enters the type of diagnosis which may include anxiety disorder, depression diagnosed by physician, and psychosis including schizophrenia) (SPVF) |
|||
|
• Is there documentation of any new or existing diagnoses of conditions other than AIDS OI during this inpatient stay? (If yes, abstractor enters the type of diagnosis which may include anxiety disorder, depression diagnosed by physician, and psychosis including schizophrenia) (SPIF) |
| Indicator | Does MMP Adhere to Indicators? | Question ID | Questions Collecting Data Related to Indicator |
| Proportion of people with diagnosed HIV infection and substance use disorder who are referred to substance abuse services and receive these services within 60 days | No | From questionnaire: | |
| A19 |
• During the past 12 months, were you enrolled in an inpatient drug or alcohol treatment facility? (No; Yes; Refused to answer; Don’t know) |
||
| A27a |
• During the past 12 months, did you get drug or alcohol counseling or treatment? (No; Yes; Refused to answer; Don’t know) |
||
| A27b |
• During the past 12 months, have you needed drug or alcohol counseling or treatment? (No; Yes; Refused to answer; Don’t know) From medical record abstraction forms: • Is there documentation of reported or suspected alcohol abuse or other non-prescribed use of substances, including counseling or treatment for alcohol and/or substance use/abuse prior to the SP? If yes: o Is there documentation of alcohol abuse prior to the SP? o Is there evidence of any injection substance use (e.g., track marks) documented prior to the SP? (If yes, abstractor enters the type of substance and type of use [e.g., injection, non-injection]) (MHF) • Is there documentation of any referrals for substance abuse prevention services during the SP? (Yes; No) (SPSF) |
||
|
• Is there documentation of reported or suspected alcohol abuse or other non-prescribed use of substances, including counseling or treatment for alcohol and/or substance use/abuse, during the SP? If yes: o Is there documentation of alcohol abuse during the SP? o Is there evidence of any injection substance use (e.g., track marks) documented during the SP? (If yes, abstractor enters the type of substance and type of use [e.g., injection, non-injection]) (SPSF) |
|||
|
• Is there documentation of any new or existing diagnoses of conditions other thanAIDS OI during this visit? (If yes, abstractor enters the type of diagnosis which may include alcoholism) (SPVF) |
|||
|
• Is there documentation of any new or existing diagnoses of conditions other than AIDS OI during this inpatient stay? (If yes, abstractor enters the type of diagnosis which may include alcoholism) (SPIF) |
| Indicator | Does MMP Adhere to Indicators? | Question ID | Questions Collecting Data Related to Indicator |
| Proportion of people with diagnosed HIV infection who were homeless or temporarily or unstably housed at least once in the preceding 12 months | Yes | From questionnaire: | |
| D10 |
• During the past 12 months, have you |
||
|
o lived on the street? (No; Yes; Refused to answer; Don’t know) |
|||
|
o lived in a shelter? (No; Yes; Refused to answer; Don’t know) |
|||
|
o lived in a Single Room Occupancy (SRO) hotel (No; Yes; Refused to answer; Don’t know) |
|||
| A30a |
o lived in a car? (No; Yes; Refused to answer; Don’t know) • During the past 12 months, did you get shelter or housing services? (No; Yes; Refused to answer; Don’t know) |
||
| A30b |
• During the past 12 months, have you needed shelter or housing services? (No; Yes; Refused to answer; Don’t know) |
||
| A6 |
Housing Status data also captured in the following questions:
• What was the main reason you did not go to a doctor, nurse, or other health care worker for HIV medical care within 3 months of testing positive for HIV? (“Experienced homelessness” is a response option) |
||
| A7a |
• What was the main reason you didn’t visit a doctor, nurse, or other health care worker for HIV medical care during the past 6 months? (“Experienced homelessness” is one of the response options) |
||
| T2 |
• What is the main reason you have never taken any antiretroviral medicines? (“Homeless” is a response option) |
||
| T4a |
• What is the main reason you aren’t currently taking any antiretroviral medicines? (“Homeless” is a response option) |
||
| T10 |
• The last time you missed taking your antiretroviral medicines, what were the reasons? (“Homeless” is a response options) |
||
| From medical record abstraction forms: | |||
|
• Is there documentation of any of the following referrals during the SP? (If yes, abstractor enters the type of referral which may include food and housing support services) (SPSF) |
|||
| Proportion of people with diagnosed HIV infection who experienced food or nutrition insecurity at least once in the preceding 12 months | Yes | From questionnaire: | |
| A31a |
• During the past 12 months, did you get meal or food services? (No; Yes; Refused to answer; Don’t know) |
||
| A31b |
• During the past 12 months, have you needed meal or food services? (No; Yes; Refused to answer; Don’t know) |
||
| A36a |
• During the past 12 months, did you get nutritional services? (No; Yes; Refused to answer; Don’t know) |
||
| A36b |
• During the past 12 months, have you needed nutritional services? (No; Yes; Refused to answer; Don’t know) |
||
| From medical record abstraction forms: | |||
|
• Is there documentation of any of the following referrals during the SP? (If yes, abstractor enters the type of referral which may include food and housing support services) (SPSF) |
| Indicator | Does MMP Adhere to Indicators? | Question ID | Questions Collecting Data Related to Indicator |
| Proportion of people with diagnosed HIV infection who had an unmet need for transportation services to facilitate access to medical care and related services at least once in the preceding 12 months | Yes | From questionnaire: | |
| A33a |
• During the past 12 months, did you get transportation assistance? (No; Yes; Refused to answer; Don’t know) |
||
| A33b |
• During the past 12 months, have you needed transportation assistance? (No; Yes; Refused to answer; Don’t know) Transportation data also captured in the following questions: |
||
| A6 |
• What was the main reason you did not go to a doctor, nurse, or other health care worker for HIV medical care within 3 months of testing positive for HIV? (“Unable to get transportation” is a response option) |
||
| A7a |
• What was the main reason you didn’t visit a doctor, nurse, or other health care worker for HIV medical care during the past 6 months? (“Unable to get transportation” is a response option) |
||
NOTE: Although the indicators for clinical HIV care and mental health and substance abuse recommended in the committee’s first report are targeted toward adults, they apply to adolescents (≥13 years) as well (IOM, 2012). The Medical Monitoring Project does not include children or adolescents; the population of inference is individuals with HIV ≥18 who are in care. Therefore, as currently designed the MMP does not provide data to estimate indicators for individuals under the age of 18. MHF = Medical History Form; SP = Surveillance Period; SPIF = Surveillance Period Inpatient Form; SPSF = Surveillance Period Summary Form; VL = Viral Load.






























































