Summary: An overarching theme of this chapter is that interprofessional education provides students with opportunities to learn and practice skills that improve their ability to communicate and collaborate. Through the experience of learning with and from those in other professions, students also develop leadership qualities and respect for each other, which prepares them for work on teams and in settings where collaboration is a key to success. This success is measured by better and safer patient care as well as improved population health outcomes. Although different situations may require different team members, who each bring to the team a unique set of skills, workshop participant Jody Frost emphasized that the patient, the family, other caregivers, and the community are integral members of all teams regardless of the context. These issues and more are described in greater detail below.
WHAT IS INTERPROFESSIONAL EDUCATION?
According to the World Health Organization (WHO), interprofessional education (IPE) is an experience that “occurs when students from two or more professions learn about, from, and with each other” (WHO, 2010). Although having students learn together can improve the health and the safety of patients, workshop planning committee member George Thibault of the Josiah Macy Jr. Foundation, who provided the introductory remarks to the workshop, emphasized that IPE is not a replacement for education specific to each profession. “This is not about totally smudging together
the professions and saying they’re all the same,” he said, adding that each profession is part of the interprofessional collaboration in order to provide something that somebody else cannot provide. “We still need to rigorously defend and improve the education specific to each profession while we accomplish interprofessional education,” he said.
Another important point Thibault raised is that each health profession possesses its own identity and pride in what it does that is special. An interprofessional identity does not replace this, but rather complements the professional identity. Furthermore, Thibault said that IPE is not the only innovation that is needed to improve patient care and health. It is an important innovation which interacts with other educational innovations to improve health professions education, with a goal of improving the health of the public, but it is not a panacea for all health care system problems. There are many other things that require fixing. Sometimes IPE provides a window into what those other problems are (i.e., regulation, reimbursement, workforce), but it alone will not solve those problems.
Thibault also emphasized that experiential learning is a key element of IPE. Experiential learning refers to the practice of students entering a practice environment to better understand how to work collaboratively in “real-life” situations. Thibault also explained that interprofessional learning is different from multidisciplinary learning, in which students from different professions learn or even work in a group. To be truly interprofessional, he said, an interaction requires purposeful integration and collaboration among the disciplines, whether in an educational or practice environment. Workshop speaker Mark Earnest from the University of Colorado echoed Thibault’s remarks, saying, “[W]orking in groups is not the same as learning in teams.” It was noted by a number of participants that educators and care providers often say they educate or work interprofessionally, but when evaluated, the evidence of collaboration is weak or nonexistent.
As was explained by workshop co-chair Lucinda Maine from the American Association of Colleges of Pharmacy, certain key processes—such as communication, cooperation, coordination, and collaboration across as well as within professions—cut across interprofessional education and can be applied to a variety of collaborative work settings. Participant Jody Frost emphasized the need for focusing on a health professional team that includes all of the health professionals that need to be there along with the patient, the family, the caregiver, and the community. “If we’re going to walk the talk,” she said, “we need a new language. I would implore us to start talking about change in education and practice around a health professional team rather than a discipline-specific group.”
Recognizing the importance of coordinated care in hospital settings, Matthew Wynia and colleagues researched the qualities of well-functioning teams (Mitchell et al., 2012). They found that members of
well-functioning teams share an understanding of the team’s goals and that each member understands his or her role within the team. Most important, there is a mutual trust among team members. Ensuring clarity concerning roles and goals is a basic principle of well-functioning teams, regardless of the context within which they are working. Wynia, who was a workshop session moderator, stressed that these qualities correspond to tangible interprofessional skills that should be imparted to students. Such skills include practical techniques to make explicit
• the task and goal of the team,
• who is on the team,
• why certain members are selected to be on the team,
• what the role of each team member is, and
• how the members’ roles fit together to accomplish the desired goal.
A workshop participant stated that students who internalize these principles through experiential learning with well-functioning teams will be better prepared to participate in similar collaborative care situations after graduation. He said that this, in turn, will lead to clearer team goals and more precise measurements of improvements in health outcomes. The following sections provide examples of meaningful, experiential learning using different modalities through which students can be educated about the qualities of a well-functioning team.
A Social Responsibility for Collaboration
The authors of WHO’s 2010 publication Framework for Action on Interprofessional Education and Collaborative Practice defined a professional within “interprofessional education” as any individual “with the knowledge and/or skills to contribute to the physical, mental and social well-being of a community.” In addressing the social well-being of a community, Sandeep Kishore—who represented one of the student perspectives presented a the workshops—referred to this definition when emphasizing the social responsibility of health professionals to work together to provide optimal services to communities. He went on to say that part of the social responsibility of health professionals is to work together in addressing the “causes of the causes” of ill health that must then be taught to students in an interprofessional manner (see Box 2-1).
Knowing the “causes of the causes” sheds light on the inequalities in living conditions that often shape the quality of people’s health and health care. Such “glaring gaps and inequities,” according to the commissioners of the Lancet report on health professional education (Frenk et al., 2010), “persist both within and between countries.” Thibault said that no country
BOX 2-1
Sandeep Kishore, Ph.D.
Cornell Medical College

Workshop speaker Sandeep Kishore is a student at Cornell Medical College. His mentors exposed him to data from the U.S. Department of Health and Human Services showing that only 5 of the 30-plus years gained in U.S. life expectancy over the past century were directly due to medical care. The other roughly 25 years gained were the result of improved social conditions, structural development, and behavioral determinants. This realization had a dramatic impact on Kishore’s thinking. He began referring to these determinants as the “causes of the causes.” It is not just the high cholesterol, Kishore said, but the tobacco addictions, the food addictions, and the policies and structures that influence them. Kishore further commented, “If I’m a health practitioner, a professional who already has an M.D., I’m saying 5 years? That’s all we got? This to me has been my pivot to think about systems and change the whole culture of how we work. We can’t operate as health professionals alone. We have to reach out to other professions. I would say it’s beyond health professions. It’s the urban planners, it’s the architects, it’s the folks that think about inequality. Within health care 5 years is horrific for spending 17 percent of our GDP [gross domestic product] in this country.”
is immune from this, including resource-rich nations. In particular, Paul Worley from Flinders University in Australia focused on this point in his presentation, which is summarized in Box 2-2.
Presenters at the workshop offered three examples of interprofessional education grounded in coursework and experiences that teach social responsibility. Jan De Maeseneer from Ghent University described how students at his university learn about social determinants and health inequities by traveling to impoverished communities in Ghent, Belgium, to learn with students from other disciplines. Stefanus Snyman and Marietjie de Villiers from Stellenbosch University in South Africa described how they use the unifying structure of the WHO International Classification of Functioning, Disability and Health Framework1 (ICF) in clinical care settings to bring different student and faculty professions together around a holistic assessment of the patient. And Elizabeth Speakman described the Health Mentors Program at Thomas Jefferson University, which involves students from different professions learning about the social, cultural, and environmental conditions in which their clinic patients live. Details of each of these presentations are given below.
Jan De Maeseneer, M.D., Ph.D.
Ghent University, Belgium
In the third year of their health professional education at Ghent University, students are exposed to impoverished communities in Ghent, Belgium, to learn with groups of students from medicine, social pedagogy, sociology, and health promotion. Each team explores its assigned neighborhood to observe the characteristics of that neighborhood and the composition of its population. According to De Maeseneer, who is the chair of the Ghent University Educational Committee for the undergraduate medical curriculum, the teams then collect medical data as well as nonmedical indicators such as criminology data, which tell a lot about the quality of life in certain neighborhoods.
Students later come together in a group to discuss the information they collected and observed. This is where culture clashes can arise between medical and social science students, De Maeseneer said, because medical students often want to solve problems immediately, whereas social science students are more apt to analyze the problem, consider the determinants,
_________________
1 The WHO International Classification of Functioning, Disability and Health is one of several WHO classifications on health that has been endorsed by the international community to provide meaningful comparisons between and among populations and countries. This tool separates health into four areas: body functions, body structures, activities and participation, and environmental factors. When the four areas are combined, they create an ideal framework for assessing the bio-psycho-social-spiritual health and well-being of a patient.
BOX 2-2
Paul Worley, M.B.B.S., Ph.D.
School of Medicine at Flinders University, Australia

The stark divide between the number of health care workers serving urban Australia versus the number serving rural Australia is striking in every provider category except nursing, whose shortage is seen continent-wide. However, this divide is not just a rural/urban phenomenon; it can also be seen across socioeconomic strata in Australia and around the world, where health outcomes vary greatly by wealth (Marmot, 2012) (see Table 2-1).
Rural Workforce
This is the situation that Worley found when he worked as a doctor in rural Australia. The lack of health providers drove him to the university sector to train and influence future health professionals. His efforts began with just eight students receiving education in rural health clinics. Today, roughly 25 percent of all medical students in Australia are trained in small rural communities rather than in large tertiary hospitals. This is part of a health care transformation meant to graduate roughly 2,000 additional doctors who are prepared to serve rural communities.
Part of the transformational change involved government investment in university departments of rural health with the goal of increasing the rural intellectual capital. Academics would now be based in small rural communities rather than solely in cities talking about small rural communities. Importantly, this investment was described as being not in “rural medicine” but in “rural health,” which explicitly demands interprofessional training.
Interprofessional Education
The only way to improve the health of individuals in rural communities is to work interprofessionally. There can be no siloed care. Before the transformation, Flinders University was divided along disciplinary lines. All the doctors were in
TABLE 2-1 Regional Health Disparities for Selected Health Indicators
| Region | Mortality rate for children under 5 years/ 1,000 live births (2001) |
Infant mortality rate/1,000 live births (2000) |
Maternal mortality rate/100,000 live births (2001) |
Prevalence of tuberculosis/ 100,000 population (2001) |
| Developed regions | 9 | 8 | 20 | 23 |
| Developing regions | 90 | 63 | 440 | 144 |
| Northern Africa | 43 | 39 | 130 | 27 |
| Sub-Saharan Africa | 172 | 106 | 920 | 197 |
| Latin America and | 36 | 29 | 190 | 41 |
| the Caribbean | ||||
| Eastern Asia | 36 | 31 | 55 | 184 |
| South-Central Asia | 95 | 70 | 520 | 218 |
| South-Eastern Asia | 51 | 39 | 210 | 108 |
| Western Asia | 62 | 51 | 190 | 40 |
| Oceania | 76 | 66 | 240 | 215 |
SOURCE: Ostlin et al., 2004.
one area, the allied health professionals in another, and the public health clinicians in yet a third. Following the transformation, the structure better reflected the interprofessional research, teaching, and care that the university desired. Six interprofessional clusters were formed. One was the clinical effectiveness cluster, which includes physiotherapists, occupational therapists, orthopedic surgeons, rheumatologists, aged-care physicians, rehabilitation practitioners, and researchers studying the disability sector. These are disciplines that work together in the real world but that are typically trained separately on university campuses. This restructuring challenges the standard hierarchical structure of the university, as the professor of surgery may be supervised in the university sector by a dietitian. It also changes the dynamics and provides an opportunity for understanding how other health providers think.
Benefits of a Community-Based Interprofessional Education
Community Benefits
• University engagement in rural communities: Asking community members to set the program outcomes establishes a direct link between community values and program results. Rural residents appear to value using universities as vehicles to invest in their communities.
• Indigenous participation in medical programs: Rural communities are involved in the selection of the medical students who represent the population being served.
• More rural doctors: Graduates from the rural programs are seven times more likely to choose regional, rural, or remote practices than graduates from a tertiary hospital.
• More primary care physicians: Graduates trained in a primary care setting are twice as likely to choose a primary care practice.
Student Benefits
• A more realistic education: Students learn from the people who make up the population rather than learn about rare diseases of individual patients admitted to a tertiary or quaternary hospital every year.
• Better student scores on examinations: With patients as their teachers, students who learned in small rural communities saw their work as more meaningful. This resulted in these students getting better test scores than students who learned in tertiary institutions despite the exams being set by the tertiary clinicians.
Educator Benefits
• Students serve for the whole year in an interprofessional environment: Students receive orientation for the first three weeks, and then they become productive team members and offer a benefit to those educating them.
• Supervisors have the opportunity to give back to the educational system that trained them and to help form the next generation of health care delivery teams.
Success Factors
The success of the rural interprofessional health education organized by Worley and his colleagues was due to four main factors. The first was the passionate leadership of the clinicians and the second was an acceptance of the work as a “health” alliance rather than a “medical” alliance. A third reason for success resulted from empowering students to be agents of change. Students co-design the curriculum with faculty, which ensures that the curriculum will have greater relevance to them and that they will have greater commitment to the work. The fourth and most important factor was the political campaign from the community
and question whether the problem is something that can be addressed by their group. He added that these discussions expose students to different ways of thinking about health predicaments and the thought processes of other disciplines.
Although Ghent University has been offering this community-based experience for 10 years, it has not gotten any easier. Indeed, De Maeseneer
to instigate change. Universities advocating for money for rural health did not have an impact, but rural communities advocating for the government to give money to the universities to do something about the health iniquities was a powerful motivator for change.
Reflections
For a small medical school serving a rural community in Australia, the triple aim may not be the best measure of health from the perspective of the patients in this rural, low-income environment. Much can be hidden within this outcome measure. Improved patient health and even disability-free years are not necessarily correlated with what people report wanting in their lives. People want peace. They want hope. They want love. They want happiness. There is a wealth of research that says health contributes to those feelings, but actually it is quite poorly correlated in many studies (Seligman, 2011). If asked, members of a community such as this may not identify improved health as their ultimate goal. Similarly, improved population health also has faults as an outcome measure of health in rural communities. In Australia overall population health has improved, but the life expectancy of the aboriginal population is 15 to 30 years less than that of the Australian white population. This situation is completely hidden if overall population health statistics are the only outcome measure. Another issue is the strong emphasis on decreasing health care costs when many rural communities may require increased investments, particularly in areas with fewer resources than some high-income areas.
Rural Australia has long suffered from the requirement that it live up to the standard of evidence-based medicine created in—and best suited for—tertiary hospitals. For example, when a patient comes into the emergency department with a headache, the gold standard of care is a CT scan, but this is not the standard in a rural environment, and if a rural clinic fails to meet the higher standard designed for tertiary hospitals, it may be labeled as not providing high-quality care. Similarly, IPE will need to redefine the evidence base used for practice and for quality improvement strategies in various settings. Such strategies are very different in a large hierarchical organization than in a flat, small, primary care system that might have an interprofessional focus.
Finally, no one should underestimate the opportunities for students in IPE to make a difference to health care and to outcomes while they are students, not just in the future. The key is to give learners enough space to be the amazing creative individuals that they are and to develop the relationships with the inspiring people with whom they have to work.
said, the logistics are even more daunting now than they were at the beginning. The experience involves 84 homes that have to be ready to receive the students, 252 caregivers, and 10 community stakeholders as well as tutors, coordinators, assessors, and panel members. “The logistics are really challenging,” he said, but clearly not impossible.
Stefanus Snyman, M.B.Ch.B., and Marietjie de Villiers, Ph.D.,
M.B.Ch.B., M.Fam.Med.
Stellenbosch University, South Africa
As at Ghent University, the IPE strategy at Stellenbosch University in Capetown, South Africa, is to educate students through a socially accountable IPE program. Stefanus Snyman, the coordinator of interprofessional learning and teaching at Stellenbosch’s Centre for Health Professions Education, said that he sees IPE as a tool for equipping students to become change agents in order to improve patient outcomes and strengthen health systems in Africa. He believes that IPE can be a vehicle for transformative learning and that it is an instrument to foster educational interdependence between the health and the educational systems.
The university’s IPE strategy (see Figure 2-1) is based on three pillars and is described fully in Appendix C of this report. The first pillar is the integration of graduate attributes or core competencies into the curriculums and the interprofessional assessment of the competencies. The second
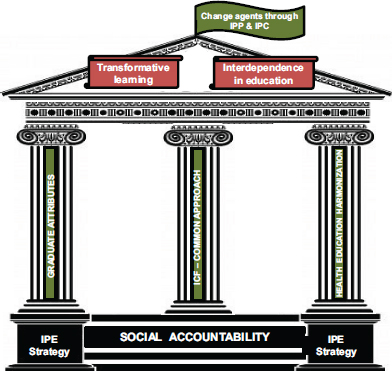
FIGURE 2-1 Stellenbosch University interprofessional education (IPE) strategy.
SOURCE: Snyman, 2012.
NOTE: ICF = International Classification of Functioning, Disability, and Health; IPC = interprofessional care; IPP = interprofessional practice.
pillar is the use of the ICF framework as a common language among all professionals at the school in the management of patient care. According to Snyman and de Villiers, using the ICF Framework in the clinical care setting gives students and faculty a unified structure with which to conduct a holistic assessment of the patient. Under each of the four topic areas (body functions and structures, activities, participation, and environmental factors) are five to nine subdivisions that cover a wide range of health-related issues, including mental function, the cardiovascular system, mobility, self-care, support and relationships, and attitudes. As Snyman said, given the expansive list of assessment items in the framework, no one profession could ever manage the full range of needs identified in a managed care plan. And he added that, in using the framework, students and faculty realize they cannot manage the care of a patient alone and begin the process of working together.
The third pillar is health education and harmonization, which requires leadership from the top as well as learners to make the necessary changes. According to de Villiers, this pillar is designed to equip faculty and community preceptors with interprofessional skills and to develop strategies that bring them together to work collaboratively.
Elizabeth Speakman, Ed.D., R.N.
Thomas Jefferson University
According to Elizabeth Speakman, co-director at the Jefferson InterProfessional Education Center, the Health Mentors Program at Thomas Jefferson University in Philadelphia has been available to students as long as the university’s InterProfessional Education Center has been in existence. This program involves roughly 250 health mentors and roughly 1,300 students from the Jefferson Medical College and the schools of nursing, pharmacy, and health professions, the last of which includes occupational therapy, physical therapy, and couples and family therapy. Each team is made up of students from these different health disciplines, and over the course of 2 years, the students in the teams learn directly from their health mentors—who are patients in the community—about these individuals’ health status and living conditions. Speakman said that the work of the students on a team culminates in the fourth and final semester with a visit to their mentor’s home in order to experience the conditions and limitations under which their mentor lives.
Following this experience, students are required to write reflective papers. In those papers, Speakman said, students often cite a better understanding of the other health disciplines for their in-depth understanding of the community and the environment in which their patient lives; occupational therapy is often singled out for particular respect because they un-
derstand the physical and environmental challenges patients are confronted with outside of the health care facility. Speakman added that students also write about the value of the group leaders who provide guidance on how to communicate effectively with patients and other team members.
Learning IPE Through Patient Safety Activities
Pamela H. Mitchell wrote in the chapter “Defining Patient Safety and Quality Care” that “safety is the foundation upon which all other aspects of quality care are built” (Mitchell, 2008). Linking this notion of patient safety to interprofessional practice, workshop session moderator, Hugh Barr of the U.K. Centre for the Advancement of Interprofessional Education, commented on the recent work of Sexton and colleagues. Those researchers found that improvements in teamwork and culture in intensive care units improved the overall safety climate (Sexton et al., 2011). Using safety as a way to educate students on how to collaborate interprofessionally resonated with a number of presenters at the workshop. Two examples of this approach, from Curtin University and from the University of Missouri, are described below.
At Curtin University, Brewer and Jones developed a framework for IPE curriculum development, which is shown in Figure 2-2. Workshop presenter Dawn Forman from Curtin discussed this framework, which underlies the curriculum and also extends into interprofessional practice. The IPE curriculum starts in the first year, she said, with 23 health professional schools following a model for ensuring client safety and quality. The foundation laid in this first year is built upon in the second, third, and fourth years for each of the programs by having one unit for each profession, which is integrated into each of the subsequent years through workshops, simulation activities, and most importantly, placement activities.
Like Forman, workshop speaker Carla Dyer of the University of Missouri School of Medicine uses IPE patient safety as a way to teach collaboration to her students. She and her colleagues address patient safety and quality improvement using “fall prevention” as the interprofessional teaching modality.
According to Dyer, students first learn about fall prevention through an independent, online study that quickly shifts to a simulation and bedside encounter where students are grouped in dyads consisting of a medical student and a nursing student. The interprofessional simulation first focuses on fall risks in the inpatient setting and then transitions to the home environment. For the bedside encounter, Dyer said, students begin by completing a chart review to gather information about the patient’s risk for falls. They
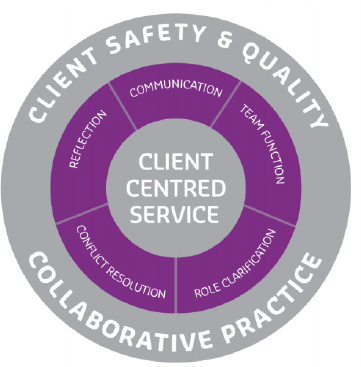
FIGURE 2-2 Framework for IPE curriculum development.
SOURCE: Brewer and Jones, in press.
then review the home environment and the patient care setting. With this information, the students jointly develop a customized fall prevention plan that is discussed with the patient and his or her family member.
Both the medical students’ and the nursing students’ skills in assessing patient falls are measured before and after their simulation experiences. The results of this assessment showed statistically significant improvements in responses in all of the measured categories, Dyer said. Students were also asked to reflect on the value of the interprofessional experience through an online module; their answers indicated that they valued this experiential leaning opportunity. Program evaluators also wanted to know whether the intervention was valuable to the patients. Dyer and colleagues reported that roughly 250 patients were involved in the simulation activity over the past 3 years and that 93 percent of patients interviewed since the start of the simulation reported that the experience and their interactions with the students were valuable.
Learning IPE Through Community Service
Workshop speaker Gillian Barclay of the Aetna Foundation encouraged the audience to consider interprofessional opportunities that are community-based and that go beyond health. To explain her point, Barclay drew upon the work that Jack Geiger did in the 1960s in rural Mississippi to describe how agriculture specialists engaged with urban planners and health professionals to place farmers’ markets near community health centers. She also said the Aetna Foundation is funding evaluation measures within this unique interprofessional space to see how the agriculture experts, the urban planners, the physicians, the managers, and the chief executive officers of these community health centers develop sustainable farmers’ markets. This is the sort of culture shift to which students should be exposed, Barclay said, and it was the sort of interprofessional education offered to students in North Carolina under the direction of J. Lloyd Michener and his colleagues at Duke University (see Box 2-3 for a summary of Michener’s presentation at the workshop).
Key Messages Raised by Individual Speakers
• Learning in groups is not the same as learning interprofessionally. (Earnest and Thibault)
• An important part of IPE learning is experiential. (De Maeseneer, de Villiers, Snyman, Speakman, and Thibault)
• Interprofessional opportunities that go beyond health can help students understand and address the “causes of the causes.” (Barclay and Kishore)
• It is the “causes of causes” of health that need to be addressed and taught to students in an interprofessional manner. (Kishore)
BOX 2-3
Durham and Duke:
A Story of One Community’s Journey Toward Health
J. Lloyd Michener, M.D.
Duke University School of Medicine
Department of Community and Family Medicine

North Carolina is a southern state. It ranks 32nd on the U.S. health rankings and 30th for obesity. One in 10 North Carolinians has diabetes and more than one-quarter of the population is now obese. Trying to deal with these social factors and social issues raises significant challenges, particularly for practitioners at Duke University who provide services to more than 200 sites across the central region of North Carolina. More than half those sites provide primary care.
Community-Based Caring
Michener has been working for more than 20 years in this region of the state. It is a state where the medical home movement has some of its roots and where Michener worked tirelessly with colleagues to improve health care so that the system would be more effective and work better for the communities. Duke now manages networks of Medicaid providers in six counties involving 60,000 people in every primary care site, every health department, and numerous other community groups. To provide the sort of comprehensive care needed in complex societies with complex medical needs, their group required not only committed doctors but also health departments, care managers, dentists, dietitians, health educators, information technicians, physician assistants, nurse practitioners, pharmacists, physical therapists, psychologists, public health workers, and social workers. They also needed the community and its members.
After listening to community needs, neighborhood clinics were built which led to a reduction in the number of emergency room visits, which was a significant savings to the hospital. This led to an expansion of the use of “micro-clinics” in
community “hot spots” with the support of a Federally Qualified Health Center (FQHC) and the hospital because of the significant cost savings.
Practitioners from Duke University are now engaged in a process of slowly weaving health into various aspects of the communities they serve, largely through affiliations with health departments. For example, practitioners work with community groups and health departments to identify safe places to exercise as a way to deal with the obesity epidemic in the neighborhoods. They also staff school clinics, support healthy food programs, and assist with school gardens. In addition, Duke supports access to health information in places of worship and for community groups, and it has provided the funds for community health workers to partner with community members and church groups to spread health information more widely within neighborhoods.
Michener and his colleagues think of their support as weaving health care into the community so that health is actually achieved. The needs of the community dictate who will be assigned to work in an area—with particular attention paid to matching the skill sets of individuals with the needs of an area. The final determination of who provides care is not dictated by who is available; it is determined by what works for that community. In this sense, the Duke program is outcome driven.
Interprofessional Education
Having developed a clear understanding of how to engage with communities and how to provide optimal care that saves money, the Duke University School of Medicine’s Department of Community and Family Medicine is now redesigning its educational programs to align student educational experiences with the lessons learned from the department’s community engagement. The new curricula emphasize teamwork and collaboration at all levels.
The department offers pipeline programs that expose students in the health professions to community clinics, where they are taught how to work effectively in different cultures. Teamwork is an integral part of this training. There is also a primary care leadership program in the school of medicine that emphasizes teamwork, training, leadership, and improving health outcomes. In this program students do a year of community-engaged research as part of a team.
The Department of Community and Family Medicine is composed of the following seven interdependent groups:
1. Community health
2. Diet and fitness center
3. Family medicine
4. Occupational and environmental medicine
5. Physician assistant
6. Doctor of physical therapy
7. Prevention research
All of the Duke Family Medicine offerings are extremely competitive, and the restructured family medicine residency is no exception, having received 540 excellent applicants for 4 total slots.
Faculty Development
Somewhat unexpectedly, the learners in the department’s programs accelerated past the faculty in terms of their understanding of IPE and community-based care. This made it necessary to retrain the faculty. There is now a mandate that all faculty within the family medicine, physician assistant, and physical therapy groups become competent in population health. Currently, faculty are partnering with learners and the community to define the competencies that will then become incorporated into the retraining of faculty members.
Final Thoughts
The work at Duke emphasizes service to the community over professional boundaries. It is the community service that binds the different professions together along with the unified goal of achieving health for all those living in the communities. An important lesson from Michener’s experience is that communities vary and that respectful attention needs to be paid to each community’s unique history and culture. Communities must be served according to their preference and not that of the professionals working for and with those in the community. This means that what has worked in Durham may not be successful elsewhere. But through active community engagement, other health care systems can be redesigned to improve health and save money along the way. The time to act is now!
REFERENCES
Brewer, M., and S. Jones. In press. An interprofessional practice capability framework focusing on safe, high quality client centred health service. Journal of Allied Health.
Frenk, J., L. Chen, Z. A. Bhutta, J. Cohen, N. Crisp, T. Evans, H. Fineberg, P. Garcia, Y. Ke, P. Kelley, B. Kistnasamy, A. Meleis, D. Naylor, A. Pablos-Mendez, S. Reddy, S. Scrimshaw, J. Sepulveda, D. Serwadda, and H. Zurayk. 2010. Health professionals for a new century: Transforming education to strengthen health systems in an interdependent world. Lancet 376(9756):1923–1958.
Marmot, M. 2012. Health equity: The challenge. Australian and New Zealand Journal of Public Health 36(6):513–514.
Mitchell, P. 2008. Defining patient safety and quality care. In R. G. Hughes, ed., Patient safety and quality: An evidence-based handbook for nurses. Rockville, MD: Agency for Healthcare Research and Quality.
Mitchell, P., M. Wynia, R. Golden, B. McNellis, S. Okun, C. E. Webb, V. Rohrbach, and I. von Kohorn. 2012. Core principles and values of effective team-based care. Discussion Paper, Institute of Medicine, Washington, DC. http://iom.edu/Global/Perspectives/2012/TeamBasedCare.aspx (accessed March 12, 2013).
Piroska Östlin, P., G. Sen, and A. George. 2004. Paying attention to gender and poverty in health research: Content and process issues. Bulletin of the World Health Organization 82(10):740–745.
Seligman, M. 2011. Flourish: A Visionary New Understanding of Happiness and Well-Being. New York: Free Press.
Sexton, J. B., S. M. Berenholtz, C. A. Goeschel, S. R. Watson, C. G. Holzmueller, D. A. Thompson, R. C. Hyzy, J. A. Marsteller, K. Schumacher, and P. J. Pronovost. 2011. Assessing and improving safety climate in a large cohort of intensive care units. Critical Care Medicine 39(5):934–939.
Snyman, S. 2012. Stellenbosch IPE strategy. Presented at the IOM Workshop: Educating for Practice. Washington, DC, November 30.
WHO (World Health Organization). 2010. Framework for action on interprofessional education and collaborative practice. http://www.who.int/hrh/resources/framework_action/en/index.html (accessed March 4, 2013).


















