Page 119
5
High-Cost Case Management
High-cost case management is a set of techniques to promote more cost-effective and appropriate modes of care for patients with expensive illnesses. Even more than prior review, these techniques have gained acceptance in a very short period. As recently as 1983, a survey of employer cost-containment programs conducted for Equitable included no questions about high-cost case management (Equitable Life Assurance Society of the United States, 1983). At that time, formal programs to manage expenditures for very expensive medical cases were uncommon, except for the programs of private firms and state agencies working with recipients of worker's compensation benefits.
The situation is different now. A 1988 survey of benefits managers for large companies found that 83 percent said they used high-cost case management (called "medical case management" in the survey) (Corporate Health Strategies, 1988). Although the surveyed group is not a representative sample, clearly this approach to utilization management has become common. Virtually all major commercial insurers and Blue Cross and Blue Shield plans offer the service either directly or through subsidiaries (Henderson and Wallack, 1987), as do most of the larger utilization management firms and third-party administrators. Some review firms are actually outgrowths of organizations originally established to manage worker's compensation cases. For health care institutions and other organizations trying to cope with the multiple and complex needs of patients with acquired immune deficiency syndrome (AIDS), high-cost case management
Page 120
is one prominent strategy (Health Insurance Association of America, 1988; Taravella, 1987).
Because the case manager is not managing care as a physician does but rather is trying to see that health plan benefits are used wisely, some organizations prefer to call their programs "individual benefits management." Other organizations, reluctant to highlight cost objectives, use the term "medical case management."
Focus of High-Cost Case Management
What distinguishes high-cost case management from other utilization management or managed care programs is its intensive and specialized focus on high-cost medical cases. Preadmission and continued stay review, in contrast, cover a broader array of cases in a much less intense fashion.
The generic label "case management" seems to have arisen in the 1970s with government projects to encourage the integration of services for clients of social welfare programs (Monroe County Long Term Care Program, Inc., 1986). These include the Services Interaction Targets for Opportunities program in the 1970s and the channeling and Social/Health Maintenance Organization demonstration projects for the elderly in the 1980s (Merrill, 1985). High-cost case management shares with other case management approaches an emphasis on assessing individual needs and circumstances and then planning, arranging, and monitoring needed services. However, because it focuses on a relatively small number of expensive cases, high-cost case management can be distinguished from so-called primary-care case management approaches often used in HMOs and Medicaid programs. In these programs, all individuals are assigned to a case manager who ordinarily must authorize or provide most services. And because health care cost containment is a central goal, high-cost case management can be distinguished from social welfare case management that is aimed at helping clients get the services they need from the complex labyrinth of welfare programs and agencies.
In focusing on very expensive patients, high-cost case management responds to an important characteristic of medical care: a small group of individuals with very costly illnesses or injuries account for a large share of the total expenditure. The experience of one company is typical: 2 percent of plan members with yearly expenses of $10,000 or more accounted for 38 percent of plan medical expenses (Rosenbloom and Gertman, 1984). In another company, 6 percent of those making benefit claims (and not all employees submit claims) accounted for more than 55 percent of health plan expenditures (Alexandre, 1988). National data suggest that 1 percent of the U.S. population (all age groups) accounts for 29 percent of total
Page 121
health expenditures (Berk et al., 1988). High-cost case management focuses on these expensive patients.
Two basic types of high-cost patients can be identified (Rosenbloom and Gertman, 1984). The first are those who suffer a sudden, catastrophic event, such as a heart attack, stroke, accident, or complicated birth, that may require a long period of hospitalization. Recovery to normal or near normal functioning is often possible, and even those with a less complete recovery may need little special medical care. The second category of patients is those with serious, often fatal, chronic conditions, such as muscular dystrophy, certain cancers, AIDS, and amyotrophic lateral sclerosis (ALS), who may be hospitalized repeatedly and become more severely ill over time.
Not all high-cost cases are appropriate for case management. Sometimes no less costly modes or sites of care are suitable or the patient's plan of treatment already includes these alternatives.
The opportunities for savings through high-cost case management by third parties arise from the complexity and fragmentation of the medical care system and the limits built into health benefit plans. It is not easy to chart the most cost-effective path of service for patients with catastrophic medical problems. Certainly, most patients and families with high-cost medical problems start out with relatively little knowledge of what lies ahead of them, and they may not always learn from their physician about the subsequent care alternatives that are possible or available. Specialized high-cost case managers can help patients and families to understand what these options are and what they mean in terms of cost, quality, convenience, and comfort.
Although physicians and hospital staff typically are more informed than patients and families, they too may lack detailed knowledge about the range of options that might benefit specific patients, particularly during the recovery or long-term-treatment stages. The care of catastrophically ill patients often involves several specialists, each tending to focus on specific problems, not the whole situation. An individual with severe burns, for example, may receive services from an internist, nephrologist, pulmonary specialist, burn surgeon, infectious disease specialist, orthopedist, neurologist, gastroenterologist, and psychiatrist (Mazoway, 1987). Hospital discharge planners often aid in arranging posthospital services, but identifying the most cost-effective option is generally not their charge.1 A case
1 The prospective per case method of paying hospitals used by Medicare encourages hospitals to discharge Medicare patients as soon as it is medically appropriate. PROs, intermediaries, or carriers are not authorized to undertake case management. The Health Care Financing Administration (HCFA), however, is planning demonstration projects to assess the role it might play, given Medicare's special characteristics. For payers whose method of paying hospitals does not, in itself, stimulate hospital discharge planning, continued-stay review may be used to prompt its
(Footnote continued on next page)
Page 122
manager who is accountable to a purchaser of services, on the other hand, does have that responsibility.
Case managers can also deal with limitations of benefit plans. Some coverage limits, such as restrictions on frequency of home nursing care, may keep down overall expenditures in a benefit plan but nevertheless increase outlays for specific patients. Many employers who shy away from across-the-board expansions in coverage have welcomed high-cost case management because it looks at cost-effectiveness on a patient-specific basis.
Role of the Purchaser
As is true of other types of utilization management, purchasers can bring high-cost case management into play in at least three different ways. First, the purchaser may actually employ case managers, as, for example, Ciba-Geigy and Zenith have (Henderson and Collard, 1988). Second, and more typical, purchasers may contract with an outside organization—an insurer, a utilization management firm, a PRO, or other entity—for high cost case management services. Third, they may rely on an HMO, insurer, or other entity that bears the financial risk for benefit costs to undertake the function as part of their regular cost-containment activities. For purchasers who offer multiple benefit plans to employees, both the second and third strategies may be in place for different employees, depending on which kind of health plan they select.
For those employers who contract for or agree to case management services, some become closely involved with the function. They look for cases to refer, demand detailed reports, analyze data and estimate savings independently, and insist on controlling all exceptions to coverage limitations. Other employers want only general reports and refuse any role in decisions to waive coverage limitations.2
Employers also vary in their objectives of high-cost case management. Some are concerned almost exclusively with avoiding unnecessary costs. Others have multiple objectives: lower costs, higher quality of care, more humane care, and assistance to patients and families in negotiating the complexities of the health care system during a stressful and difficult period.
(Footnote continued from previous page)
initiation. For uncomplicated cases, discharge planning may be quite modest, involving no need to identify or help in arranging posthospital services.
2 The federal Office of Personal Management (OPM), for example, has been relatively uninvolved with case management. Although OPM has agreed to allow some plans serving federal employees to make coverage exceptions and to provide other case management services, they originally did not allow the program to be mentioned in brochures distributed to employees. In addition, OPM does not ask for reports on costs or savings achieved through high-cost case management (Eileen Thomas, Blue Cross and Blue Shield Federal Employees Program, personal communication, November 22, 1988).
Page 123
The latter group of employers may accept the possibility that high-cost case management might increase the cost of care for some patients. For example, a patient near death from cancer might be allowed, through case management, to receive short-term but expensive support through 24-hour-a-day nursing services so as to be able to die at home—even though palliative care in a hospital might be less expensive.
How High-Cost Case Management Works
Permutations are numerous, but the basic approach of high-cost case management is fairly straightforward: to bring a knowledgeable party who is concerned with cost containment into the process by which patient care decisions are made for patients with expensive medical problems. The most common elements of high-cost case management programs are
• efforts to find less costly alternatives to the care (usually hospital care) that would be provided for specific patients in the absence of case management;
• willingness to approve payment for services not covered by the patient's benefit plan, if doing so will help reduce overall costs; and
• concurrence from all relevant parties—patient, family, and physician—in implementing cost-saving alternatives for meeting the patient's needs.
Although the first two of the above elements appear to be virtually universal in high cost case management programs, the third element is not, even though it is often described as part of a standardized model.
Figure 5-1 charts in more detail the steps that are often involved in high-cost case management. The process starts with case identification, proceeds through assessment of the patient's suitability for high-cost case management and the availability of alternative courses of treatment, and continues with the development of a specific plan that is agreed to by all involved parties and then implemented and monitored. The final step is closure of the case. This may occur when the patient's condition changes or when coverage under a benefit plan is exhausted or otherwise lost. Table 5-1 provides two hypothetical case summaries.
The four categories of utilization management described in Chapter 3 generally apply to high-cost case management. The distinction between those organizations with and without provider contracts is probably less important for high-cost case management because cooperation rather than contractual compliance tends to be stressed in either situation. However, because case identification, as described in the next section, is such an important step in high-cost case management, freestanding programs may face more difficulties than case management undertaken by the insurer
Page 124
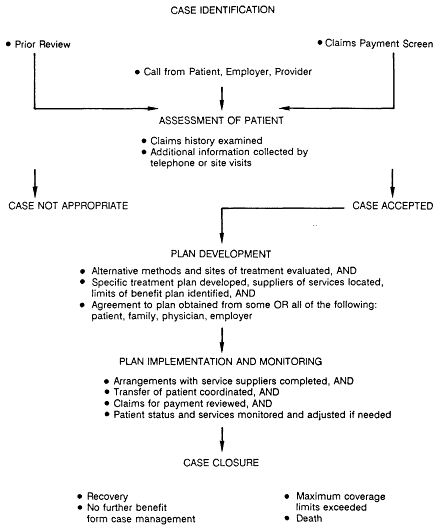
Figure 5-1
Examples of steps and variations in case management.
Page 125
or claims administrator. There is no systematic evidence on this point, however.
Operational Variations
The committee learned during its site visits that high-cost case management programs are highly variable in ways that are not always easy to describe. The narrowest programs are, in essence, hospital discharge planning programs that operate by means of telephone and confine themselves
| TABLE 5-1 Typical Case Management Summary and Analysis | |||
| CONFIDENTIAL CASE REPORT 1 | |||
| Patient: YYYY | Client: XXXX | ||
| Referred by: VVVV | |||
| Prepared by: WWWW | |||
| Diagnosis: Lymphoma | Date Opened: 2/14/88 | Date closed: 3/9/88 | |
| INITIAL CASE SUMMARY | |||
| Patient is a 56-year-old woman with terminal breast cancer. Chemotherapy has been ineffective, and death is expected within a month of this referral. Patient requires pain management and skilled nursing and personal care. Family can provide some care but not 24 hours a day. Physician will continue hospitalization unless adequate home support can be arranged. | |||
| OUTCOME | |||
| Patient was transferred home with support from registered nurse and home health aide. Death occurred 14 days later. | |||
| COST ANALYSIS ASSUMPTIONS | |||
| Patient would have required continued hospital care. | |||
| Case management permitted discharge and maintenance at home. | |||
| Hospital days averted: 14 days | |||
| Dollars per hospital day averted: $600 (average billed this admission to date) | |||
| Actual home health expenses: | (within contract) $2,000 | ||
| (outside contract) $1,200 | |||
| Case management fee: $700 | |||
| SAVINGS | |||
| Hospital costs averted (14 days × $600) | $8,400 | ||
| Home health expenses | ($3,200) | ||
| Case management fee | ($700) | ||
| Net savings | $4,500 | ||
(Table continued on next page)
Page 126
| TABLE 5-1 (continued) | |||
| CONFIDENTIAL CASE REPORT 2 | |||
| Patient:RRRR | Client: XXXX | ||
| Referred by: SSSS | |||
| Prepared by: WWWW | Date Opened: 4/15/88 | Date dosed: 10/88 | |
| INITIAL CASE SUMMARY | |||
| Patient is a 15-year-old boy with head injury suffered in football game. After surgery, patient was comatose and was in intensive care unit (ICU) for 1 week before mother's employer contacted case manager. Attending physician estimates hospital care will be needed for at least an additional 3 months followed by transfer to a rehabilitation facility for several weeks. | |||
| OUTCOME | |||
| Patient spent 3 more weeks in ICU and was then transferred to a rehabilitation unit for an additional 4 weeks. Home care was provided for 3 months. Family has taken over therapy and the state is providing a tutor to prepare the boy to return to classes. | |||
| COST ANALYSIS ASSUMPTIONS | |||
| Patient would have been hospitalized for 3.5 months and would have spent another 3 months in a rehabilitation facility. | |||
| Case management permitted earlier transfer to rehabilitation facility and then substitution of home care. | |||
| Hospital days averted: 75 at $1,200/day | |||
| Rehabilitation hospital days averted: 21 at $900/day | |||
| Actual home care expenses: $8,000 | |||
| Case management fee: $6,200 | |||
| SAVINGS | |||
| Hospital costs averted: | $80,000 | ||
| Rehabilitation costs averted: | $18,900 | ||
| Home health expenses: | ($8,000) | ||
| Fee: | ($6,200) | ||
| Net savings | $64,700 | ||
to arranging out-of-hospital services that will allow earlier discharge of patients. In broader programs, case managers may be involved with patients and their families for many months and may visit them in the hospital, home, or elsewhere. The activities of these case managers are not confined to facilitating discharge from the hospital but extend to identifying and coordinating a broad range of services.
High-cost case management programs also vary in how they identify cases, who acts as case manager, who the case manager works with, and how directly case managers are involved with patients and providers. The differences among case management programs undoubtedly have important implications for the impact and effectiveness of high-cost case management.
Page 127
However, these differences have received virtually no empirical study, and studies of one particular program are often generalized and assumed to apply to quite different strategies.
How Cases Are Identified and Screened
The case management process may be activated in several different ways. In many instances, the case manager is notified of a potential case by an employer, family member, or provider who is aware of the program and knows a patient who may benefit from it. In such situations, the case manager is likely to become involved early when the opportunities are greater for influencing the course of treatment to avoid needless expense. For these reasons, case management organizations may work with the purchaser to increase employees' awareness of the program and encourage early contact. Organizations with a significant presence in a local area may also work with community hospitals and physicians to bring them into the case identification process. In addition, an employer's disability insurance plan may refer cases for high-cost case management
If the organization providing high-cost case management also provides other utilization management services, it may use its preadmission, admission, and continued-stay review programs to identify patients that are candidates for preadmission review. Generally, this involves specifying a set of target diagnoses such as stroke, ALS, or muscular dystrophy that are flagged by reviewers or their computer software. The lists of target diagnoses overlap but are not identical across different companies. Repeated admissions or multiple extensions of length of stay may also serve as flags. Overall, preadmission review and admission review may be of limited use, because many patients with catastrophic illnesses or injuries are admitted on an emergency basis and the prognosis may be highly uncertain for several days. Also, high-cost case management is generally handled by a separate staff that may not routinely communicate with the prior review nurses.
Potential high-cost cases may also be identified through the claims administration process. Claims may be screened for target diagnoses; for cumulative payments beyond a certain threshold, for example, $25,000; or for certain patterns of care, such as repeat admissions. However, by the time a high-cost case is identified from claims for payment, several months of care may already have been provided and chances to initiate less costly care missed. Nevertheless, retrospective analysis of claims caught and missed by a case management program may be useful in improving the program by suggesting where opportunities are being overlooked.
To avoid inefficient use of expensive case management resources, the first step is a review of basic demographic, clinical, and claims information.
Page 128
Cases with a reasonable potential for case management may then be subject to a more intensive review, including direct communication with the patient and family.
Although all case managers make judgments about what cases to accept, they vary in how they make their decisions. These variations relate either to client objectives and concerns or to vendor capacities and strategies. Some organizations, based on their own and their client's objectives, reject cases with no or little potential for short-term savings. Other organizations reject cases with complications they feel they are unable to handle (for example, psychosis). Some clients want intensive case management efforts for AIDS and psychiatric cases but are less concerned about other problems. If high-cost case management operates in tandem with per-case payment to hospitals, third-party case managers may get involved only when hospital staff face an unusual case, perhaps one that requires exceptions to benefit plan limitations to make more cost-effective care feasible.3 These sorts of decision rules may or may not be codified in internal procedure manuals and contracts with clients.
Who Serves as Case Manager?
One of the largest national companies offering high-cost case management services uses physicians as case managers. In all other programs known to the committee, nurses are used. The nurse managers always have access to physicians for consultation but manage most assessment, planning, coordinating, and monitoring activities themselves. Organizations differ in whether their nurses handle a wide array of cases or specialize. The most frequent area of specialization is in psychiatric case management. Some organizations use psychologists, social workers, and other professionals to assist case managers or handle certain types of patients or specific problems. They often speak of a ''team approach'' to case management in which several types of professionals contribute to patient assessment and recommendations.
How Case Managers Relate to Patients and Providers
Most high-cost case management programs report that they seek to work with all interested parties—the patient and family, the doctor, the
3 Blue Cross and Blue Shield plans that pay hospitals on a diagnosis-related group (DRG) or other per-case basis report some difficulties in serving national employers who want a uniform program at all company locations—even if it is not cost-effective at some sites (Michael Cologero, Blue Cross and Blue Shield Association, November 21, 1988).
Page 129
discharge planners at the hospital, home care agencies, and others. Their initial contact may be with any of these parties. However, some organizations work primarily with the patient and family, whereas at least one major national company works only with the patient's physician.
The emphasis placed on patient and family concurrence with high-cost case management recommendations varies. HMOs appear to be more directive, perhaps insisting on a choice between termination of coverage for services outside the treatment plan or agreement to follow the plan. However, not a lot is documented about HMO management of high-cost cases. Much of that management may be invisible to the patient because it occurs when the physician calls for approval for hospitalization or use of out-of-plan facilities or services. High-cost case management appears to be integrated into HMO administration (group, staff, and independent practice associations [IPAs]) more than in fee-for-service administration.
To date, most utilization management organizations and insurers working with fee-for-service health plans appear to use a voluntary approach. There are no statistics on patients who refuse case management, but some patients are reported to regard coordination with the case managers as a hassle rather than a help. The committee heard suggestions that some purchasers could become more insistent on high-cost case management when the likely cost of a patient's rejecting case management is significant. Some case management organizations do follow-up surveys of patients and families who have been involved in the process; others do not.
Case managers generally seek the cooperation of attending physicians. The attending physicians have essential information about the patient and the course of treatment, can influence patients' and families' acceptance of case management recommendations, and can assist in implementing recommendations by approving hospital discharges, ordering or providing necessary medical services, or supervising the care provided by others.
Face-to-face work with patients and physicians is most characteristic of HMOs and utilization management programs that operate in a relatively confined geographic area. However, at least one national company the committee visited attempts to do on-site case management through a national network of offices and employees. Blue Cross and Blue Shield plans in different states sometimes contract with each other to provide on-site case management services for patients located outside of their service area. Over 25 Blue Cross and Blue Shield plans are involved in a program for national employers that includes a utilization management component and involves a certification process using written application forms, site reviews, and ongoing guidance groups. Since on-site work is more expensive, particularly if it involves travel or subcontracting, most organizations target its use carefully.
Page 130
Some case management firms establish contractual relations with home health care agencies, nursing homes, rehabilitation centers, durable medical equipment suppliers, and other institutions. These contracts may specify that clients of the firm have priority when the health care organization is operating near capacity. Contracts may also provide for discounts or negotiations on charges. However, even without such contracts, case managers may negotiate with provider organizations on charges for particular patients. Centralized firms without a local presence may be at some disadvantage in developing these kinds of relationships with providers.
How Much Case Management Costs
Another variable factor with high-cost case management programs is their cost, whether cost is defined as the price the purchaser of the service pays or the resources the utilization management organization requires to operate (Henderson and Wallack, 1987; Cologero, personal communication, 1988). Some insurers have not explicitly charged for case management services but have incorporated the cost as part of their premium or administrative services charge. Other insurers and some independent firms set a flat charge per covered employee, particularly if high-cost case management is part of a larger package of utilization management services. Most commonly, programs bill on a flat-fee or hourly basis for assessment, coordination, and other services. Hourly charges of $25 to $100 or more have been reported, with charges tending to fall toward the higher end of this range. For a case involving 40 hours of management services, the difference in administrative fee could be $3,000 for companies at the low versus the high end of the range.
Impact of High-Cost Case Management
There seems to be general acceptance that high-cost case management can save money and improve the quality of care and the quality of life for patients and families. Results probably vary depending on a large number of factors—the nature of the patient's problem, the family circumstances, physician and hospital cooperation, community health resources, employer objectives, and sophistication of the case management program. However, very little systematic evidence is available to support any specific conclusions about the effects of high-cost case management. Illustrative reports on case management program results suggest the kind of information and analysis typically available.
In Oregon, for example, the Bargaining Unit Benefits Board for the Service Employees International Union (SEIU) decided in 1985 to replace concurrent review with high-cost case management. The case management
Page 131
services were provided by the Oregon PRO that also administers preadmission review and second surgical opinion programs for SEIU. Program savings from case management were calculated by projecting charges that were averted by the use of case management (such as additional days of hospital care) and subtracting the cost of alternative services and the PRO administrative fee. In the first year, the union reported that more than $13 was saved for each program dollar spent, but the savings-to-cost ratio subsequently dropped to 4:1 (Service Employees International Union, 1988; Jo Anne Browne, Service Employees International Union, personal communication, January 19, 1989).
The Bank of America adopted a case management program for patients with catastrophic illnesses as one outgrowth of its efforts to deal with its growing number of employees with AIDS. In the program's first year, the bank reported savings of $1.2 million compared with costs of $155,000, a savings-to-cost ratio of more than 7.5:1 (Ricklefs, 1988).
Independence Blue Cross of Philadelphia (formerly Blue Cross of Greater Philadelphia) began individual case management in 1987. For the 30 cases actively managed in that year, it reported savings of nearly $2 million, over $65,000 per case on average (Independence Blue Cross and Pennsylvania Blue Shield, 1988).
Intracorp, a firm with a history in case management in the workers compensation arena, has reported savings as high as $75 for every dollar spent on case management. It reports a savings ratio of 17:1 for a recent review of 14 typical cases (Tonsfelt, 1986).
In a study of an unnamed insurer (and an unnamed separate utilization management firm), Brandeis University researchers tried to project what would have happened without high-cost case management. They asked consultant physicians to examine a sample of the study and project how much hospital care would likely have occurred without the intervention of the case manager. Among the small numbers of cases examined initially, savings to cost ratios ranged from 1.18:1 to 0.42:1. The researchers identified spinal injury cases as likely to have higher rather than lower costs under case management because of improved identification and use of rehabilitation options and institutions. In general, the consultants were considerably more conservative in their projections of savings than the case managers (Henderson et al., 1987; Mary Henderson, Brandeis University, personal communication, November 21, 1988). One purchaser of case management services, Caterpillar, Inc., attempts to compensate for exaggerated estimates of cost savings by making its own projections of what use and costs would be in the absence of intervention and then cutting those estimates by one-quarter. Caterpillar uses a PRO to provide the case management services (Richard Wright, personal communication, November 22, 1988).
Page 132
Effects of High-Cost Case Management on Specific Parties
For the most part, high-cost case management appears to have been favorably received by patients, families, and health care providers. The committee heard few complaints but numerous anecdotes of positive responses. The following discussion is based on the committee members' experience, testimony at the committee's June 1988 hearings, the 12 site visits, the roundtable discussion among corporate benefits managers in January 1989, and the six meetings of the committee.
Effects on Enrollees
In discussions with those offering and purchasing high-cost case management services, most recounted—with some feeling—stories of individuals who have been assisted by case management in confronting devastating medical problems. Even in the less dramatic cases, the picture conveyed is of people who are grateful for additional information, guidance, and support in dealing with stressful and complex situations. The major concern expressed to the committee involved questions of confidentiality for patients with AIDS, cancer, or other conditions that might provoke negative reactions at their place of work.
Three characteristics of case management, as currently practiced, appear to be responsible for its generally positive reception. First, case management tends to be quite individualized and cognizant of the special problems created for the patient and family by the particular nature of the patient's medical problem, the quality of the home environment, and the limitations of the community's health care resources. To some degree, then, high-cost case management escapes the impersonality and rule-bound image that tends to accompany programs dealing less intensively generally with more patients. Second, most organizations emphasize cooperative work with patients, families, and physicians and consensus on the design and implementation of the treatment plan. They do not put patients in the position of going along or losing benefits. Third, high-cost case management is often a vehicle for providing a patient and family with more services and options than would normally be available under the patient's benefit plan. The patient and family ordinarily are quite aware of these extra benefits.
To the extent that the administration of high-cost case management departs from these patterns, this largely positive assessment may not hold. For instance, if the case manager offers the patient and family a choice between loss of coverage and implementation of an alternative treatment plan, then the program may be perceived negatively. Likewise, if the
Page 133
family must take on substantial extra burdens of care but the assistance of special home services is denied, then high-cost case management may add rather than relieve stress. And poor administration of a program—by virtue of poorly selected and trained staff, inadequate documentation of conditions and decisions, and weak assessment and monitoring of alternative providers—an easily undermine the potential positive features of high-cost case management. The committee notes these possibilities but does not have evidence that they now constitute real problems.
Effects on Health Care Providers
Although the pattern of effects on health care providers may be somewhat more mixed than they are for patients and families, the committee believes that high-cost case management has probably had a preponderance of positive effects. For the attending physician and hospital discharge planner, the case manager can often bring to bear a more specialized knowledge of certain alternative treatments and providers and a more intensive assessment of patient circumstances and options. For example, the case manager may know more about innovative rehabilitation services or specialized home care options and have established relationships with these providers so that it is easier to tailor services for particular patients. The committee has no information about the administrative costs that high-cost case management creates for physicians and hospitals, but the interactions described by those involved suggest that it imposes few additional costs and may, in some cases, substitute its resources for those of the physician or hospital.
Physicians and hospital discharge planners faced with high-cost case management for the first time may feel somewhat threatened, but familiarity seems to mitigate initial sensitivities. Most firms say that they try very hard to select and train case managers to work constructively with physicians and hospital staffs. One potential source of conflict with providers is the contractual or other preferential arrangements with particular health care institutions that some case management organizations have established. Selective arrangements, per se, may create hard feelings, but the charge that high-cost case management companies may have a conflict of interest and may be channeling patients to lower-quality institutions is a more serious charge. The committee was unable to find specific evidence on this point and heard only a few references to this possibility during its deliberations.
Effects on Purchasers
Although the benefits of case management can be identified in the abstract, it seems that purchasers have sometimes been surprised at how
Page 134
positive the reactions from employees have been. The personalized nature of most high-cost case management may make the benefits more tangible to both employers and employees. And it promises more support for access and quality care than it poses threats. However, the lack of concrete, reliable information on whether high-cost case management is saving money is an irritant to purchasers. There is some suspicion that savings are overestimated and that more time is being charged than is strictly necessary. The committee heard few complaints about the lack of empirical data on health outcomes, patient satisfaction, or the impact of alternative program designs. On balance, high-cost case management seems to be regarded by purchasers as more of a "win/win" program than other utilization management and cost-containment programs are.
Questions About Available Evidence
As the study committee discovered for other utilization management programs, much of the evidence cited in support of high-cost case management is of questionable value—for many of the same methodological and organizational reasons. (Table 5-2 summarizes measures of impact commonly reported for high-cost case management programs and notes some of their limitations.) On the other hand, certain characteristics of case management programs can make their evaluation easier.
One characteristic of high-cost case management that facilitates evaluation of utilization and savings is the explicit focus on the cost-effectiveness of proposed alternative care. For each case, an estimate is made of the cost of alternative care versus that of care that is likely to be provided without case management. These cost estimates are sounder when they rely on information about the specific hospitals, home health agencies, and other providers that are involved or likely to be involved with the patient. Some programs track billing data during the period of active case management to determine the actual cost of care. Since alternative treatment plans may be changed, complications may arise, and other divergences from the projected course of care may occur, this sort of follow-up is important in assessing cost and other impacts.4 Such tracking and follow-up may be easier when the high-cost case management and claims administration functions are managed by the same organization.
Certainly, the case-by-case projections of use and costs incurred and avoided by high-cost case management may be flawed in various respects.
4 predetermination programs, in contrast, rarely if ever attempt any case-by-case assessment of whether outpatient surgery will likely be less expensive than inpatient care in a specific case. That is, the probable expenditure for inpatient care at a particular hospital is not compared with the probable outlay for a particular alternative site of care. The assumption has been that, on average, the alternative care will be cheaper—an assumption that is no longer taken for granted.
Page 135
The program may take credit for treatment strategies that would have been adopted anyway. For example, home care is often arranged for terminally ill patients through family, physician, and hospital initiatives without the involvement of a third-party case manager. In these situations, net savings may still occur from case management if the program produces earlier and
| TABLE 5-2 Measures of High-Cost Case Management Impact | |
| ACTIVITY DATA | |
| Number of cases referred for assessment | |
| Number of cases initiated | |
| Number of cases closed | |
| Number of cases ongoing | |
| Average length of case management | |
| Source | |
| Review organization | |
| Comments | |
| • Are not impact measures. | |
| • Cannot be used to evaluate efficiency absent additional information on characteristics of cases, client preferences, cases missed or identified late, etc. | |
| UTILIZATION | |
| Inpatient days of care projected without case management | |
| Alternative services (projected or actual) | |
| Home health | |
| Skilled nursing facility | |
| Durable medical equipment | |
| Other | |
| Source | |
| Claims data | |
| Review organization | |
| Comments | |
| • Projected utilization of hospital care is easy to overstate, particularly during periods of changing practice patterns. | |
| • Projected use of alternative services is less satisfactory than are reports based on actual claims data. | |
| • Generally focused on short-term costs and savings. | |
| BENEFIT COSTS | |
| Projected costs of care without case management | |
| Projected or actual cost of substituted services | |
| Cost of services for which contract limitations are waived | |
| Source | |
| Claims data | |
| Bills submitted for special services | |
| Review organization | |
| Comments | |
| • See comments on utilization projections. | |
| • Cost estimates may not differentiate between more expensive early days of stay and less expensive (typically) later days and, thereby, may overestimate savings from reduced length of stay. | |
Page 136
(Table continued from previous page)
| TABLE 5-2 (continued) | |
| ADMINISTRATIVE COSTS | |
| Billed services during specified period | |
| Per contract charge for all contracts | |
| Source | |
| Review organization | |
| Comments | |
| • Charges to client may not reflect the real administrative cost of the program, particularly in a multiservice organization that has not done cost studies for the service. | |
| • Do not reflect any costs to patient or providers. | |
| • May not always be billed separately from other utilization or benefits management services. | |
| SAVINGS | |
| Projected cost of care without intervention minus high-cost case management benefit and administrative costs | |
| Ratio of benefit savings to benefit and administrative costs | |
| Source | |
| Claims data | |
| Review organization | |
| Comments | |
| • See comments on use and cost measures. | |
| • Needed to assess net impact of high-cost case management on purchaser costs. | |
| • Do not include any costs or savings for patient or provider. | |
more successful transfers (consistent with physician and patient preferences) and if administrative fees do not exceed savings.
Some projections of averted costs are more plausible than others. To cite one case, during the process of planning a case management program, staff for one insurer examined computer printouts to locate patients who had generated very high costs in recent years. In the process, they discovered a child with muscular dystrophy who was ventilator dependent and had been hospitalized continuously for 8 years. The parents' benefit plan had covered the care and would have covered continued hospitalization. With the family's and physician's cooperation, the insurer arranged appropriate home care and waived contract provisions restricting payment for some of these services. The insurer's intervention clearly precipitated the move to home care for this child and reduced expenditures for the insurance plan (Thomas, personal communication, 1988).
Nevertheless, trying to assess more generally the savings produced through case management is difficult without some assessment of comparable groups not subject to the program. Clearly, practice patterns are changing for many reasons—new technologies, more sophisticated resources for out-of-hospital care, expanded health plan coverage of such
Page 137
care, and new methods for paying institutions and physicians. In the absence of comparative data, it is hard to know what savings attributed to high-cost case management may really be due to other factors.
The committee was unable to discover any studies that included comparison of a group subject to case management with one having no such program. Researchers at Brandeis University attempted such comparisons in their work with one insurer, but limitations in the claims data precluded it (Henderson, personal communication, 1988).
The relatively small number of cases subject to case management compared with the large numbers processed through predetermination programs and the relatively intense nature of the case management process do ease some burdens of projecting and comparing use and costs. However, the time horizon for assessment still tends to be constrained, partly for practical reasons, such as lack of historical data and a short program life span, and occasionally for policy reasons, in particular, a preference for being conservative in projecting savings.
One example of this conservatism can be found in the Brandeis University research just mentioned. The researchers concentrated in their initial reports on short-term savings that "would be realized within six months of implementation of the case management plan" and that ''were clearly documented and supported by medical record data and physician input" (Henderson, 1987, p. 44). Longer-term savings were not studied in the initial assessment because they were both harder to track and more speculative.5
Although the relatively small number of patients in most high-cost case management programs has some advantages for evaluation purposes, it also means that the mix of cases—and program effects—can fluctuate for reasons unrelated to the program or to other systematic influences. Case mix and program results can also be affected by program design.
For instance, how cases are targeted and screened for acceptance into case management programs can systematically affect the composition of a group subject to case management. A program that does not accept a case unless there is potential for short-term savings could be expected to show higher per-case savings than one that accepted cases with potential for long-term savings only. Programs that accept cases with little potential for cost savings but considerable potential for improving patient and family quality of life would also show lower per-case savings. Ignoring such program
5 The potential for longer-term savings seems reasonable in some cases, such as chronically ill patients who, with careful management, can avoid repeated hospitalizations. The possibility that long-term effects could include higher costs because of inappropriate short-term treatment under the case management plan does not seem to be expected. This may be because the intensive nature of the management process and the communication with the attending physician and the voluntary aspect of high-cost case management is thought to make this prospect unlikely.
Page 138
features could lead to incomplete judgments about the effectiveness of particular programs. However, these details may not be identified explicitly in the program description or assessment.
In addition, the potential impact of other cost-containment initiatives may be not be considered. For example, if a purchaser or insurer moved to a per-case payment method with limited provision for outlier payments at the same time that it implemented high-cost case management, it might find case management of little or no marginal value. The results under these circumstances should not be generalized to programs associated with more traditional provider payment methods. (Note that Medicare does not have a high-cost case management feature, although demonstration projects are being planned.)
Learning Curve in High-Cost Case Management
One reason that relatively little objective evidence is available on the impact of high-cost case management is that the programs are relatively new. Most are still evolving. Savings may grow, administrative costs may drop, and documentation of results may become more specific and realistic. Such improvements seem likely because of several types of changes in case management programs. These include
• better targeting and earlier identification of cases,
• elimination of overlapping cost-containment efforts,
• increases in administrative efficiency and computer support,
• development of standardized clinical protocols to guide the management of more cases, and
• establishment of more economical and effective arrangements with health care providers.
As organizations gain familiarity with high-cost case management, they generally look for ways to improve case identification and screening. In some cases, this means adding new conditions to their lists of target diagnoses or problems, for example, AIDS cases, spinal cord injuries, and psychiatric cases. Or certain target diagnoses may be eliminated, and some diagnoses may be subject to more up-front screening for associated diagnoses, past hospitalizations, or other indicators of high-cost potential.
Yet another targeting strategy is to examine whether certain services can be more effectively managed as part of the basic benefit plan rather than through an exceptions process. A manager for Caterpillar tractor said that adding a regular home care benefit in April 1988 ''almost put their case management program out of business'' (William Beale, Caterpillar, Inc., personal communication, November 30, 1985). Patients recuperating from relatively straightforward acute problems are now rarely seen by
Page 139
case managers whose smaller caseload consists mostly of chronically and terminally ill individuals.
Another way organizations try to improve their results is through earlier identification of potential cases when more options for lower-cost care may be considered.6 Links to precertification and continued-stay review, informational mailings and seminars for health care providers, and involvement of employer personnel offices are common strategies. These steps involve closer integration of high-cost case management, claims administration, provider relations, and human resources functions, which can be difficult even when the first three functions are handled by a single organization.
As links to other aspects of utilization management are developed, it is sometimes possible to gain administrative efficiencies. For example, continued-stay review is unnecessary for cases already accepted for case management. Other administrative efficiencies are possible through refinement of information collection procedures and routinization of some communications with health care providers. Better computer support can increase efficiency at all stages in the case management process, from case identification and screening through outcome documentation and reporting.
Standardized protocols for managing certain kinds of cases (for example, substance abuse or AIDS) may minimize the need for intensive involvement of a case manager in the clinical assessment of the patient and the development of a treatment plan (Henderson and Wallack, 1987). If methods for identifying when monitoring or intervention is no longer cost-effective can be improved, cases may be closed more promptly, resulting in lower administrative and benefit costs.
Experience can also help case managers develop greater sensitivity and efficiency in handling certain kinds of difficult cases, for example, AIDS patients with dementia or nonaccepting families. In addition, as relationships with providers are established and reinforced over time, the identification of good alternative sources of care requires less effort. The prospects for negotiating reduced prices for care or other special arrangements increase.
6 For example, AIDS cases are thought to be good targets for case management to reduce costs and improve patient quality of life (DiBlase, 1987; Health Insurance Association of America, 1988; Taravella, 1987). However, the immediate cause of hospitalization is generally a problem such as pneumonia, and there are understandable reasons an explicit AIDS diagnosis may not be mentioned in information provided to an insurer, employer, or utilization management firm. A diagnosis-based method for identifying probable high-cost cases will not, absent other information, pick up such cases. Therefore, some case management programs are trying to develop better early identification strategies such as having predetermination software screen each pneumonia case for age and sex of patient and any previous admissions. Sensitivity to confidentiality is a particular concern for this kind of approach, but confidentiality issues are significant for many high-cost care management cases.
Page 140
Potential Legal Issues
There is virtually no case law, legislation, or regulation that specifically delineates the responsibilities and liabilities of organizations involved in high-cost case management. However, three areas of potential concern can be identified.
First, there are several questions about liability for harm to a patient. Because high-cost case management can shape the course of treatment for a patient, the possibility exists that a patient or family who has suffered a bad outcome will claim that case management contributed, and a jury may agree. The case of Wickline v. the State of California, discussed in the paper by William A. Helvestine in Appendix A of this report, makes it clear that organizations engaged in utilization management may be held liable for their failure to exercise clue care in designing and administering a program. Although not mentioned in the Wickline case, a number of cases involving claims payment administration suggest that an organization would also have to act in "good faith" in administering a case management program. Some employers, citing sensitivity about perceived conflicts of interest, are reluctant to have their own physicians or other employees involved in high-cost case management and prefer to hire outside firms instead.
Actions that might put an organization at risk are the use of poorly selected and trained personnel, negligent referrals to particular providers, and poor protocols for collecting information about patients' conditions. A capricious refusal to make an exception to a benefit contract might also give rise to a legal challenge. Good documentation of decisions and rationales, as well as reliance on written protocols for developing treatment plans and referrals, help demonstrate the exercise of clue care and good faith (Saue, 1988). The degree to which the attending physician and the patient are involved in developing and consenting to the treatment plan may also be relevant in assessing liability.
A somewhat different risk may arise if a case manager becomes aware of improper treatment by a patient's physician. One commentator believes that the case manager may be responsible for discussing such problems with attending physicians and, if that does not work, notifying the quality assurance committee of the hospital or medical society (Blum, 1989).7
A second legal concern about high-cost case management is whether exceptions that are made to limits in benefit contracts will set a precedent
7 One question not raised in the site visits or hearings is whether a nurse case manager might be practicing beyond the scope of his or her nursing license. Blum (1989) raises this question but suggests that problems are unlikely so long as a nurse manager does not attempt to control treatment decisions. Blum does, however, raise doubts about whether the use of licensed practical nurses rather than registered nurses as case managers is appropriate.
Page 141
that undermines the contract. For instance, if a patient for whom exceptions have been made, say, to cover special home care services, reaches the maximum dollar coverage of the benefit plan, that patient might argue that since some limits had already been waived, the limit on maximum benefits should not be enforced.8 Such situations do not appear to be very common, but case management organizations do report a few sensitive cases. Written agreements among parties descrying the nature and limits of any benefit exceptions are a recommended protection (Saue, 1988). Another way organizations can minimize problems when coverage maximums are being approached is to work with patients and their families, state Medicaid agencies, and charitable organizations to arrange a smooth transition to other sources of financing and avoid disruption in the plan of treatment.
A third concern is that an individual whose request for an exception to contract restrictions was denied could try to argue unfair treatment because exceptions had been made for others covered under the same plan. A related worry is that a claim of discriminatory treatment might be prompted under Section 89 of the Internal Revenue Service Code, which forbids discrimination between more and less highly paid employees. In order to protect against a successful charge of discrimination, some organizations involved in high-cost case management are improving their case documentation, clarifying contract provisions, securing written agreements to contract exceptions, and tracking the characteristics of employees assisted by case management (Cologero, personal communication, 1988).
In general, reasonable administrative procedures should be in place to guide any prospective or retrospective case-by-case decisions about benefits. And these procedures should be implemented responsibly and documented systematically for both routine and exceptional cases. Evidence of careless, biased, and uninformed decision making is hazardous whether a complaint involves a routine payment denial, a bad health outcome, or a charge of discriminatory treatment.
Conclusion
Case management has become a popular utilization management strategy in a very short period of time. Although it has been the subject of even less systematic research than prior review techniques, claims of positive impact for case management appear to be generally accepted. The committee believes that several characteristics of high-cost case management
8. Some plans set no limit on the maximum total amount that may be paid under the contract. Where limits exist, they vary from less than $250,000 in some groups to more than $1,000,000 in others. Many plans set lower limits—often $50,000—on psychiatric benefits.
Page 142
account for this acceptance: the relatively personalized and intensive assessment of patient situations; the explicit attention to the cost-effectiveness of alternative care; the potential for patients to receive extra benefits; and the emphasis on consensus in arranging alternative treatment. During the committee's deliberations, few concerns were raised about high-cost case management specifically. In the concluding chapter, the committee's concerns focus less on case management and more on issues involving the less individualized methods of prior review.
References
Alexandre, Leslie M., "Who Are the High Cost Cases in a Health Benefits Plan?," Medical Benefits, September 15, 1988, p. 7.
Berk, Marc L, Monheit, Alan C., and Hagen, Michael H., "How the U.S. Spent its Health Care Dollar, 1929-80," Health Affairs, Fall 1988, pp. 46-60.
Blum, John D., "An Analysis of Legal Liability in Healthcare: Utilization Review and Case Management," Houston Law Review, January 1989, pp. 191-228.
Corporate Health Strategies, The Health Poll, Fall 1988, p. 1.
DiBlase, Donna, "AIDS Claims Hard to Track for Insurers," Business Insurance, September 7, 1987, p. 22.
Equitable Life Assurance Society of the United States, The Equitable Health Care Survey: Options for Controlling Costs, conducted by Lou Harris and Associates, Inc., New York, August 1983.
Health Insurance Association of America, AIDS Case Management: What Health Insurance Companies Are Doing, Washington, DC, 1988.
Henderson, Mary, and Collard, Anne, "Measuring Quality in Medical Case Management Programs," Quality Review Bulletin, February 1988, pp. 33-39.
Henderson, Mary, and Wallack, Stanley, "Evaluating Case Management for Catastrophic Illness," Business and Health, January 1987, pp. 7-11.
Henderson, Mary G., Souder, Barbara A., and Bergman, Andrew, "Measuring Efficiencies of Managed Care," Business and Health, October 1987, pp. 43-46.
Independence Blue Cross and Pennsylvania Blue Shield, Independence and Leadership in Health Care: Community Health Care Report 1988, Philadelphia, June 1988.
Mazoway, Jackie M., "Early Intervention in High Cost Care," Business and Health, January 1987, pp. 12-16.
Merrill, Jeffrey C., "Defining Case Management," Business and Health, July/August 1985, pp. 5-9.
Monroe County Long Term Care Program, Inc., "Direct Assessment vs. Brokerage: A Comparison of Case Management Models," Final Report for Robert Wood Johnson Foundation, East Rochester, NY, October 1986.
Ricklefs, Roger, "Firms Turn to 'Case Management' To Bring Down Health-Care Costs," Wall Street Journal, February 7, 1988, p. D1.
Rosenbloom, David, and Gertman, Paul M., "An Intervention Strategy for Controlling Costly Care," Business and Health, July/Angust 1984, pp. 17-21.
Saue, Jacqueline M., "Legal Issues Related to Case Management," Quality Review Bulletin, August 1988, pp. 239-244.
Service Employees International Union, "Utilization Review and Case Management in Employee Benefit Plans," Washington, DC, July 1988.
Taravella, Steve, "Coping with AIDS," Business Insurance, September 7, 1987, pp. 1, 20-22.
Tonsfeldt, Lynne, "Using Medical Case Management to Reduce Catastrophic Injury and Chronic Illness Coverage Costs," FORUM, 1986.
























