Page 205
Appendix B
Utilization Management and Quality Assurance in Health Maintenance Organizations: an Operational Assessment
In the 1980s, health care payers in the public and private sectors have relied increasingly on utilization management to help control health care costs. As a result, the autonomy of health care providers—hospitals and professionals—has been curtailed as payers have applied predetermined criteria to judge the appropriateness of care. The medical community, in turn, has expressed concerns about the design of the clinical standards or algorithms governing utilization review decisions by health insurers, Blue Cross and Blue Shield plans, third-party administrators, and health maintenance organizations (HMOs). In particular, as payers seek to control costs more aggressively, physician organizations are seeking to review the criteria used for denial of services under second-opinion and prior authorization programs.1
At the same time, federal and state legislators, health policy analysts, and consumer groups are concerned about the impact of physician incentive plans on quality of care and accessibility to services in prepaid delivery systems. This concern was prompted, in part, by concerns about the quality of care delivered to Medicare beneficiaries enrolled in International Medical Centers Inc. (IMC), a for-profit HMO located in south Florida.2 The well-publicized IMC scandals raised a number of public policy issues, including enrollee understanding of benefit restrictions in HMOs,3 ineffective
*The authors are members of the accounting firm Coopers & Lybrand, San Francisco, Calif., and Washington, D.C.
Page 206
quality assurance monitoring in HMOs (both internally by HMO staff and externally by regulatory agencies), and the impact of financial incentives on ordering of services and specialty referrals by HMO physicians.4 The intent of this paper is to describe the range of utilization management and quality assurance strategies that are used by HMOs and then to evaluate their actual implementation. The paper begins with a brief discussion of the methodology used in preparing this paper. The second section describes the organizational structure of existing HMOs, and the third discusses market, structural, and operational factors affecting HMO performance. The fourth section discusses the approaches to utilization management and quality assurance, and the fifth section evaluates the performance of utilization management and quality assurance programs in HMOs. In the sixth section, there is a review of existing research on physician risk incentives in HMOs, while the seventh section addresses some additional policy and research issues. The final section of this paper contains five condensed case histories.
Except for the discussions on the organizational structure of licensed HMOs, the term HMO is generically in this paper to cover all closed systems in which physicians are partly or fully capitated for delivery of care and where enrollees may receive services only from contracting providers.5 All state-licensed prepaid medical plans are included in this definition, regardless of whether they are federally qualified and offer a full range of benefits.
Methodology
This paper reflects the authors' experience as health care consultants for an international accounting firm. During the past 3 years, we have had the opportunity to analyze the health benefits offered by numerous employers in both the public and private sectors and to help design their managed care programs. (By managed care, we refer to any program that channels patients to a specific set of health care providers.) During the same time, we and our associates have conducted operational reviews of over 20 HMOs, ranging from local to regional and multistate plans. In general, the HMO reviews have involved an analysis of financial, actuarial, enrollment, and utilization trends in the context of benefit design, premium pricing, marketing practices, claims processing procedures, contractual arrangements with providers, utilization review, and management reporting procedures.
This managed care and HMO consulting experience provides the background for this paper. To supplement our experience, we reviewed the health services research literature for HMO-related studies. In describing
Page 207
our personal experience, we do not purport to review a statistically representative sample of HMOs. In fact, because many of the plans that we studied are in transition, the paper may magnify some of the problems facing the HMO industry.6 The crucial advantage of an experiential analysis, however, is that it offers an internal view of HMO operations at all organizational levels that is not available through standard survey instruments or through a review of documents filed with regulatory agencies.7
In our HMO discussions, we do not refer to any plans by name, nor do we provide any information on exact plan size, geographic location, plan age, or precise sponsorship in order to preserve client confidentiality. The brief case histories for five plans that appear at the end of this paper do not include any plan identifiers, but do contain actual descriptions of the utilization management programs in place at the time that the operational reviews were conducted. We present these studies to show the range of operational problems that can undermine the structural design of utilization management and quality assurance programs.
Hmo Organizational Structure
According to the current InterStudy classification of HMOs, there are four types: staff, group, network, and individual practice association (IPA) model plans.8 Staff model HMOs deliver health services through physicians who are under salary to the plan. Group model HMOs contract with one independent multispecialty group practice, whereas network model HMOs contract with two or more multispecialty groups. IPAs contract with physicians in private practice, either as individuals, through their group practices, or through separate physician associations.
Under the mandating process established by the HMO Act of 1973, an employer is required to offer only one group or staff model HMO and one IPA in a given service area. (The network classification did not exist under the original HMO Act.) In some geographic areas, HMOs have used a model designation that allows them to take advantage of the mandating process, rather than one that strictly corresponds to their underlying structure. For example, plans that contract almost exclusively with multispecialty groups have sought IPA designations to compete against long-established group or staff model plans. Therefore, any analysis of HMOs requires an assessment of the underlying contractual arrangement with physicians, rather than the plans own self-designation.9
More recently, ICF, Inc. has categorized HMOs as having two-tier or three-tier organizational structures.10 In the two-tier structure (Figure B-1), the HMO contracts directly with individual physicians; in the three-tier structure (Figure B-2), the HMO makes capitation or fee-for-service payments to the IPA or group, which, in turn, contracts with individual
Page 208
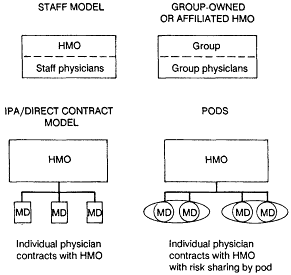
Figure B-1
Organizational structures within HMOs: two-tier structures.
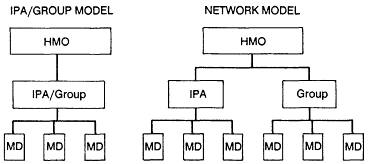
Figure B-2
Organizational structures within HMOs: three-tier structures.
physicians. ICF originally included only staff model plans and direct contract IPAs in the two-tier classification. In Figure B-l, we have added two additional categories: HMOs owned by group practices and HMOs in which physicians contract directly with the HMO but are arbitrarily grouped into risk-sharing pools or ''pods.''
As described in the literature, a two-tier structure may facilitate contracting in areas where physicians are geographically dispersed (that is, suburban or rural areas) or where physicians have not developed their own
Page 209
IPAs. According to the literature, some HMOs elect to use a two-tier structure purposely to forestall physicians from creating IPAs, which, in turn, can function as bargaining units to provide physicians with higher fees.11
Lately, we have come across a new two-tier contractual arrangement involving those HMOs that contract directly with individual physicians and then create arbitrary physician risk pools, or pods. In these arrangements, the financial risk is shared with other providers with whom the physician may or may not have direct contact in daily practice.12 Depending upon the local market, pods may sometimes be organized by group practice or hospital affiliation; in other areas, physicians may be assigned to a pod solely on the basis of practice location.
In this paper, we use the two- and three-tier structure as the basis for much of our analysis. This approach allows us to focus on where responsibility for utilization management decisions actually rests. For example, in two-tier IPA arrangement's, most decision-making resides at the HMO level, whereas in three-tier arrangements those entities that contract with the HMO (for example, IPAs and multispecialty groups) may take over many of these responsibilities. In determining how plans are classified, we ignore the self-designated HMO plan type and instead examine the underlying contractual relationship that exists with participating physicians. In this way, we can describe more precisely utilization management activities in those plans that have contractual arrangements with varying types of provider entities (for example, plans that have group-, staff-, and hospital-based IPA arrangements).
Market, Structural, and Operational Factors Affecting Hmo Performance
We believe that any review of HMO performance that focuses exclusively on structural measures will have serious limitations. The HMO market is in a state of flux. Not only are many plans reporting financial losses, but they are having to contend with employer demands regarding the provision of data and experience rating and with provider concerns about reimbursement rates and design of utilization review programs. In this section, we briefly describe the relationship of the health care marketplace to HMO structure and operations. The intent of the analysis is to show that plan performance, as measured by financial, utilization, and quality indicators, is a function of multiple variables, many of which are beyond the control of HMO management.
Page 210
The Health Care Marketplace
An HMO both reacts to and helps shape the health care market in which it operates. For example, the regulatory environment establishes parameters for benefit design, premium pricing, and marketing practices. The employment market determines eligibility for health benefits, level of employer contributions, and design and pricing of indemnity benefits. Demographic and geographic factors, such as the size of Medicare and Medicaid populations, the location of local industry, and commuting patterns, affect product development and the boundaries of HMO service areas.
The use of a two- or three-tier contracting structure by an HMO is dependent upon existing alternatives to individual physician contracting, such as the presence of multispecialty group practices or hospital-sponsored IPAs, and the prior experience of local providers in working with other HMOs or managed care programs. Negotiation of reimbursement rates, capitation payments, and risk-sharing arrangements are dependent upon (1) hospital and physician supply, (2) the presence of competing HMOs and the design of their payment and risk arrangements, and (3) utilization and cost trends within the local market. In return, as an HMO becomes established, it will have an impact on the design and pricing of health benefits and health services in the local market, as well as on the structure of hospital and physician relationships (including the emergence of new IPAs, group practices, and joint ventures).
Hmo Structure
HMO structure, in part, reflects plan sponsorship, consumer orientation date of entry into the market, and short- and long-term financial goals. The adoption of nonprofit or for-profit status may reflect the history of the sponsoring entity, the availability of capital, and the marketability of the program to investors or joint venture partners. Management's perspective on provider behavior, plus the existence of other HMOs in the local market, help to determine the operating model (staff, group, network, IPA, or hybrid), the approach to contracting (direct contract versus three-tier arrangement), and the extent of any risk-sharing arrangements.
Except in markets with a large oversupply of physicians and hospitals, there generally is some give and take in contract negotiations between an HMO and the provider community. While quality of care is always a concern in these negotiations, actual discussions usually end up focusing on economic considerations. As noted by Gnessin,13 there is an inherent conflict between the goals of any HMO's management and those of its participating physicians. Gnessin defines six goals for HMOs: (1) profit
Page 211
maximization; (2) capital appreciation; (3) enrollment growth; (4) shift of financial risk to third parties; (5) maximum utilization control with minimum malpractice exposure; and (6) control over all components of HMO operations, including the actual health care delivery system. For physicians, Gnessin defines five goals: (1) maximum autonomy in the practice of medicine; (2) minimal loss of existing patient base or patient volume; (3) expansion of patient base and volume; (4) minimal financial risk; and (5) increased income from new revenue sources (other than the direct provision of health services).
It is the tension between these two perspectives that establishes the setting for the negotiation and implementation of financial incentives. According to Gnessin's "fairness doctrine," at any given time either HMO management or HMO providers may be in a superior bargaining position. However, when the dominant party imposes its will unilaterally on the other, this strategy usually proves successful only in the short term; in the long term the imbalance in power will result in acrimony and disintegration of the relationship. In other words, a plan that transfers risk to providers without reimbursing them adequately or providing them with data to manage their practices runs the risk of losing physician participation in the long run. Conversely, a plan that accedes completely to physician demands and pays them market rates without changing practice patterns may price itself out of the marketplace or require the plan sponsors to absorb large operating losses.
Hmo Operations
An HMO cannot transfer risk fairly to providers and deliver quality care in a cost-effective manner without (1) effective management information systems for tracking enrollment, premiums, and utilization and for providing usable and timely reports to management and participating providers; (2) efficient claims processing procedures to ensure prompt payment to providers and the accurate capture of procedural and diagnostic data; (3) accurate actuarial and underwriting procedures for reliable projection of utilization and delivery costs by provider class (hospital, primary care provider, specialist, and other ancillary providers); (4) representation of professional staff and/or a medical director at the HMO's upper management level; and (5) adequate professional staffing to support a utilization management and quality assurance program.
In Figures B-1 and B-2, we described two- and three-tier physician contracting arrangements, as first defined by ICF. There is considerable variation within these two- and three-tier arrangements, however, depending upon how much control any HMO wishes to retain for itself or to
Page 212
delegate to contracting providers. Broadly speaking, there are three issues that influence the HMO's decision-making process: (1) how physician groups and IPAs are organized in the local market in terms of the cost-effectiveness of their delivery networks, the design of their data systems, and their management capabilities; (2) how institutional and professional providers are reimbursed and whether the HMO wishes to retain control over the claims payment process; and (3) whether the HMOs believe that the physicians can discipline themselves effectively through the utilization review and peer review process.
As shown in Table B-1, which describes operational responsibilities, there are two control models for two-tier organizations and three control models for three-tier organizations. Responsibilities for utilization management and financial operations may rest almost entirely with the HMOs (Model 1), may be shared between the HMOs and providers (Model 2), or may be assumed largely by providers (Model 3). In two-tier arrangements, in which the physicians either are not independent contractors (for example, staff model, group-owned, or affiliated HMOs) or are fee-for-service providers contracting directly with the HMO, an arrangement like that in Model 3 is not feasible. Moreover, any sharing of services with providers is more limited in two-tier plans than it is in three-tier plans. Typically, sharing of services involves those utilization management and claims payment activities that revolve around the gatekeeper role of contracting primary care physicians (for example, preadmission authorizations and specialty referrals). In pod-type situations in which primary care physicians are capitated, the physicians may review claims from specialty providers before authorizing them for payment. In rare cases, when providers are individually capitated and have direct control over their own specialty funds, they may actually pay for specialty claims.
In three-tier organizations, HMOs are usually not responsible for physician selection and peer review, as these responsibilities rest with contracting IPAs or groups. In Model 1, the IPA or group may share limited utilization review functions with the HMO. For example, an IPA may receive utilization and financial reports from the HMO's claims system; the IPA, in turn, uses these reports as the basis for remedial action against errant providers. In Model 1, all physician payments and all risk incentives are calculated by the HMO.
In Model 2, the HMO creates a medical (physician) fund, which is then handled by the IPA or groups; this fund may represent a capitated payment or a budget allocation based upon anticipated fee-for-service charges. The IPA or group then processes and pays claims for services rendered by its member physicians, while the HMO continues to pay for hospital services and emergency and out-of-area claims. The IPA or group provides feedback on utilization patterns to contracting providers and provides encounter data
Page 213
| TABLE B-1 Operational Responsibilities in Two- and Three-Tier Organizational Structures by Control Model | ||||||||||
| Two-Tier Organizations (with Pods) | ||||||||||
| MODEL 1 | MODEL 2 | |||||||||
| HMO | MD | HMO | MD | |||||||
| Marketing | X | X | ||||||||
| Enrollment/underwriting | X | X | ||||||||
| Utilization review | X | X | ||||||||
| Claims payment | X | X | X | |||||||
| Encounter data | X | |||||||||
| Data analysis | X | X | ||||||||
| Provider feedback | X | X | ||||||||
| Peer review | X | X | ||||||||
| Quality assurance | X | X | ||||||||
| Three-Tier Organizations | ||||||||||
| MODEL 1 | MODEL 2 | MODEL 3 | ||||||||
| HMO | IPA/Grp | HMO | IPA/Grp | HMO | IPA/Grp | |||||
| Marketing | X | X | X | |||||||
| Enrollment/underwriting | X | X | X | |||||||
| Utilization review | X | X | X | X | X | |||||
| Claims payment | X | X | X | X | X | |||||
| Encounter data | X | X | ||||||||
| Data analysis | X | X | X | X | ||||||
| Provider feedback | X | X | X | X | ||||||
| Peer review | X | X | X | |||||||
| Quality assurance | X | X | X | X | X | X | ||||
| NOTE: MD indicates physician; Grp indicates group practice. | ||||||||||
on medical services to the HMO itself. In Model 2, the HMO may also be responsible for utilization review for services covered by the medical fund (for example, specialty referrals and diagnostic testing). In Model 3, the HMO largely assumes the role of a broker; it markets benefits to employers, enrolls members, and pays claims for noncapitated services. Otherwise, the IPA or group is given complete responsibility for all utilization review and data analysis.
In the case studies, we have provided examples of one two-tier, Model 1 plan (Case 5), three three-tier, Model 1 plans (Case Studies 1, 3 and 4), and one three-tier, Model 3 plan (Case Study 2).
Page 214
Approaches to Utilization Management and Quality Assurance
As previously noted, responsibility for specific aspects of an HMO's operations vary by control model. Understanding where the locus of control rests is particularly important when evaluating those cost-containment approaches that affect patient care decisions. For this analysis, we have divided utilization management into its underwriting benefits, delivery of health services, and quality assurance components.
Underwriting Benefits
Almost always, benefit design and development of underwriting guidelines remain the responsibility of HMO management, not providers. (An exception occurs when providers require the use of copayments for office-based care to control unnecessary demand for services.) These functions can be described as follows.
Enrollment criteria are underwriting guidelines by industry or service class and by group size. Premium pricing and marketing practices also affect enrollment patterns and are included in this subcategory.
There has been a growing body of literature on enrollment patterns in HMOs to study the issue of selection bias. These analyses have been prompted, in part, by employer concerns that HMOs have attracted a disproportionate share of young and presumably healthy employees. In an analysis of 21 studies on self-selection, Wilensky and Rossiter concluded that most of the recent studies have shown HMOs to be enrolling a lower risk population. However, only rarely have any studies examined the impact of enrollee continuity on utilization rates.15
Benefit design relates to (1) the extent of coverage for specific services, drugs, and supplies; (2) any required copayments, coinsurance and/or deductibles; (3) level of services offered (for example, for mental health, the availability of individual or group therapy); (4) number of visits per condition; (5) out-of-pocket maximums; and (6) lifetime dollar benefits. Federally qualified HMOs have historically offered a more comprehensive set of benefits than have nonqualified prepaid plans or exclusive provider arrangements that are indemnity-based. With the recent growth of non-qualified plans and the move away from community rating and defined benefit packages to experience rating and negotiated benefits, there has been increased emphasis on benefit design as a cost-containment mechanism within HMOs.
Page 215
Delivery of Health Services
The delivery component of utilization management involves seven subcategories, as follows.
Utilization review is usually administered under the auspices of a medical director and includes one or more of the following services; (1) preadmission review; (2) concurrent hospital review; (3) second surgical opinions; (4) specialty and/or out-of-network referral authorizations; (5) high-cost case management; (6) retrospective review of services; (7) bill audit; and (8) remedial action for providers suspected of fraud or noncompliance with utilization review or referral procedures.
Clinical protocols or guidelines are used for medical decision-making. Formal protocols exist in writing and define the exact procedures to be followed for specific clinical conditions. There are also informal guidelines that represent a consensus of the participating providers about delivery of care. Protocols and guidelines may define, for example, when it is clinically appropriate for a patient with a specific condition to undergo a surgical or diagnostic procedure; they may also define the types of services to be rendered to a patient with a given medical condition and the appropriate setting where these services should be provided. The development of formularies to control the dispensing of pharmaceuticals also falls into this category.
Patient flow procedures are used to control the scheduling and timing of patient services across the entire HMO physician network. Included in this category are the assignment of patients to "gatekeepers" for primary care services, guidelines for scheduling of visits by patient class (for example, acute-care patients, physical examinations, and follow-up visits), time allocated per appointment, access to specialists and tertiary providers, maintenance of telephone lines, office hours, and facility location. Development of staffing ratios for professional and administrative personnel represents another form of control over patient flow.
Physician selection involves an assessment of a physician's technical capabilities and practice style. In medical groups and staff model HMOs, the selection process begins at the initial time of hire and continues through a probationary period. In IPAs, the process is more limited and often focuses on establishing criteria for physician participation, such as a medical license in good standing, adequate malpractice coverage, local medical staff affiliation, and board certification or eligibility. For some community-based IPA HMOs, participation is on an "every willing provider" basis, with the intent of providing as widespread a geographic distribution of physicians as possible.
Data analysis involves a review of financial and utilization trends by practice site, by primary care or specialty service, by member class (for
Page 216
example, Medicare, Medicaid, commercial group, and individual membership), and by employer group. Data analysis also involves a review of individual provider performance by various utilization and clinical measures; feedback of this information to participating providers allows them to judge their performance relative to the performance of their peers. In two-tier arrangements, the data analysis is typically performed by the HMO. In three-tier, Model 3 IPA or group model HMOs in which providers are capitated for some or all of their services, the data analysis is usually conducted by the IPA or the group. In this situation, many HMOs receive only limited encounter information back from providers; as a result, the HMOs may actually lack the data to evaluate how providers are performing financially under their capitated contracts.
Peer review, which can be classified as both a utilization management and quality assurance tool, occurs on both a formal and an informal level. On a formal level, peer review may involve provider feedback, performance evaluations, and disciplinary action. In many plans, the thrust of this activity is on detecting outlier behavior (that is, poor-quality services, excessive ordering of services, referral to nonnetwork providers, etc.). For all two-tier HMOs, the monitoring process is the responsibility of the medical director and/or the peer review committee at the HMO. Here the onus is on plan management to prove that a physician is not performing according to preestablished standards. Typically physicians participating in three-tier IPA or group model HMOs are not subject to formal performance evaluations by HMO management, as this responsibility is handed to the contracting physician entity.
There also is the informal aspect of peer review that occurs during rounds, surgery, case conferences, and consultations. Physicians practicing in group or staff settings are subject to informal peer review on a daily basis. They can observe their fellow physicians both in office and hospital settings, whereas in most IPAs the informal peer review process is limited to the hospital setting.
Physician financial incentives include both the basic method of provider payment (salary, fee-for-service, or capitation) and the use of bonuses, withholds, and sharing of surpluses and deficits with the plan.
The delivery components of utilization management vary markedly by practice setting. In Table B-1, we presented various control models based upon the design of the contractual arrangement between HMOs and physician providers (two- and three-tier arrangements). Here, the emphasis is on the locus of control rather than the underlying organization of the physicians contracting with the HMO. In Table B-2, we look at one type of HMO (three-tier, Model 3), in which the HMO has capitated the physician entity (IPA or group) and has delegated control over the delivery components of utilization management.
Page 217
| TABLE B-2 Provider-Based Utilization Management Activities | |||
| Utilization Management Approach (Three-Tier, Model 3 HMO) | |||
| Activities | Community-Based IPA (FFS/Capitated) | Multispeciality Group (FFS/Capitated) | Multispeciality Group (Capitated) |
| Formal utilization review | |||
| Preadmission reviewa | *** | */** | */*** |
| Concurrent reviewa | **/*** | */** | */*** |
| Second surgical opiniona | */*** | ||
| Referral authorizationa,b | */*** | * | * |
| Case managementa | */*** | */** | */*** |
| Bill audit | */** | * | * |
| Remedial/fraud | *** | ||
| Remedial/penalties | * | ||
| Clinical protocolsc . | In UR | Yes | Yes |
| Formularies | */*** | */*** | |
| Patient flow | |||
| Primary care physician | */** | */** | */*** |
| Staff size | */** | *** | *** |
| Scheduling visits | **/*** | **/*** | |
| Length of appointment | *** | *** | |
| Specialty referrals | **/*** | **/*** | |
| Diagnostic services | **/*** | **/*** | |
| Physician selection | */** | *** | *** |
| Data analysis | */*** | **/*** | *** |
| Provider feedback | */*** | **/*** | **/*** |
| Peer review | |||
| Formal procedures | * | *** | *** |
| Financial incentives | Yes | Yes | Yes |
| NOTE: *, Occasionally used as a utilization management technique; **, Frequently used as a utilization management technique; ***, Regularly used as a utilization management technique. FFS indicates fee-for-service; UR indicates utilization review. | |||
| aIncludes preestablished utilization guidelines by procedure or diagnosis. | |||
| bIncludes diagnostic procedures and out-of-network services. | |||
| cIncludes both protocols and informal clinical guidelines. | |||
In Table B-2, there are three general types of contracting entities: (1) a community-based IPA whose member physicians continue to practice primarily in a fee-for-service setting and who are reimbursed by the IPA on a discounted fee-for-service basis subject to a withhold; (2) a multispecialty group practice with fee-for-service that has both patients and multiple managed care (HMO, exclusive provider, and/or preferred provider) contracts; and (3) a multispecialty group that contracts exclusively with one HMO and that receives almost all of its income from prepaid services. As shown in Table B-2, the IPA relies heavily on formal utilization review procedures to
Page 218
modify continuing fee-for-service incentives. That is, because participating physicians continue to be reimbursed on the basis of the number and level of services provided, the IPA focuses its efforts on controlling unnecessary utilization and on monitoring billing practices by participating physicians. In this environment, the decision-making process for high-cost care is transferred in part from the individual physician to the utilization review team (that is, for decisions involving certain types of diagnostic testing, inpatient admissions, referrals to noncontracting facilities, and rehabilitative services).
Depending upon group size, the other two physician entities in Table B-2 may or may not have formal utilization review programs. The larger the multispecialty group, the more the need for a formal utilization review program to standardize procedures across sites. As described in the literature, the utilization review program used by Kaiser Permanente physicians in southern California includes preadmission and concurrent review; discharge planning; home health; patient education services; and retrospective review of admissions, length of stay, and level of care. 16 Some groups also have case management programs to coordinate care for certain categories of high-cost patients. Some may require authorizations for referrals outside the multispecialty group, and bill audit, when it occurs, is usually for outside services. Unlike IPAs, multispecialty groups are generally not concerned with remedial action for fraud or nonadherence to utilization review protocols, since poorly performing physicians will not be retained in the practice.
In IPAs, clinical protocols are built into the utilization review algorithms, with primary emphasis placed on the control of inpatient and high-cost specialty and diagnostic services. Usually, there is little attempt to influence routine decision-making in the ambulatory setting other than through the referral process and benefit design. In multispecialty group practices, physicians may be encouraged to adopt a specific practice ''style.'' While the group may have developed formal clinical protocols for specific conditions or procedures, typically, the process involves little more than senior physicians serving as mentors for newly hired staff.
In terms of controlling patient flow, IPAs do not generally determine the scheduling practices of their participating physicians, other than requiring plan subscribers to sign up with a primary care gatekeeper. Whereas IPAs rely on formal utilization review programs primarily to control costs, group practices may control utilization through the patient flow process. As shown in Table B-2, multispecialty groups rely on scheduling of appointments, the length of the appointment, and access to specialty providers as utilization management controls.
Typically, IPAs place less emphasis on staff size and physician selection than do multispecialty groups. In fact, many IPA HMOs purposely seek
Page 219
to develop a large physician base to gain market acceptance. As a result, HMO patient volume varies significantly among participating providers. Multispecialty groups, on the other hand, determine staff size for primary care and specialty services on the basis of preestablished patient-physician or enrollee-physician ratios. Recruitment of additional staff generally occurs only when there is sufficient patient or membership volume to provide a patient base for new physicians.
In terms of data analysis, theoretically, all IPAs and groups develop utilization statistics. AS will be discussed subsequently, the accuracy and timeliness of this information and the frequency with which it is supplied to management and to participating physicians differ markedly across individual IPAs and groups. One generalization, however, is that groups operating in the fee-for-service sector tend to have more detailed financial and utilization data, with procedure codes, than do prepaid group practices that do not routinely prepare patient bills.
Finally, while the peer review process exists in all three settings described in Table B-2, the thrust of the activity varies in the IPA versus the group settings. In the former, the emphasis is on detecting outliers, whereas in the latter there is additional emphasis placed on how well a given physician adopts a groups practice style and works cooperatively with his or her peers, as will be discussed subsequently.
Quality Assurance
Quality assessment is an evaluation of quality of care through structure, process, and outcome measures, as originally defined by Donabedian. 17 Quality assurance is quality assessment plus correction of identified deficiencies. Mosser18 has defined quality assurance on three levels. On the first level, and in its broadest sense, quality assurance includes such diverse activities as credentialing of providers, evaluating physician performance, disciplining poor performers, continuing education, tracking malpractice claims, collecting grievance information, conducting member satisfaction surveys, performing facilities review, and establishing laboratory quality control. On the second level, quality assurance is defined as the process of measurement, problem correction, and reevaluation. On the third and narrowest level, it consists of focused problem correction in groups, performance feedback to individuals, and direct surveillance and corrective action.
State HMO licensure requires documentation of a utilization review and quality assurance program, as does eligibility for a Medicare risk contract and participation in prepaid Medicaid programs. The actual implementation of these programs varies widely, with many plans tending to
Page 220
focus on utilization review activities and to pay only very limited attention to quality assurance protocols.
Operational Problems Impairing Utilization Management and Quality Assurance Programs
Utilization Management Programs
Many HMOs have discovered that their utilization management programs in concert with risk incentives have had only limited success in modifying physician practice patterns. The situation is particularly difficult when providers are reimbursed on a fee-for-service basis, either directly by the HMO or through the IPA or group (which itself may be capitated). Additionally, there are specific operational problems that have plagued the HMO industry and that affect implementation of utilization management programs. These problems can be broken down into four broad categories.
1. Inadequate management information systems and claims processing procedures. The first generation of commercially available HMO software typically handled an enrollment size of no more than 40,000-50,000 members and a limited number of HMO benefit packages. Software suitable for IPAs contracting with physicians on a fee-for-service basis (using discounts and/or withholds) often was inappropriate for group and staff model HMOs that used capitated arrangements, and vice versa. Moreover, most of the early software had limited flexibility in terms of report generation, particularly for any analysis of practice patterns on a provider-specific basis.
Since the early 1980s, a number of plans have seen their membership pass the 50,000-member threshold and have experienced significant claims processing delays because of system overload and software design. Some HMOs find that their software cannot accommodate the proliferation of new benefit packages, including high- and low-option plans, the development of vision, mental health, dental and drug riders, and so-called indemnity wraparounds or self-referral options. Existing software also may not handle various hospital and physician risk-sharing arrangements. At one carrier-sponsored HMO, for example, the claims processors had to manually calculate all hospital claims involving per diem payments; another had to send all hospital claims to an affiliated payer to be assigned diagnosis-related groups before calculating any payments. In some cases physician withholds have had to be calculated manually, while other HMOs cannot handle volume discounts.
As a result of inadequate or outmoded management information systems (MIS), many HMOs have suffered such problems as buildup in un-processed claims or encounter forms; inability to implement various forms
Page 221
of reimbursement such as multiple per diems for hospitals and variable risk withholds for physicians; and failure to provide physician-specific utilization data on capitated and noncapitated services, on authorized and nonauthorized admissions and referrals, and on billing practices.
Currently, a number of HMOs across the country are in the process of defining business requirements for new MIS, while others are installing or have just installed new systems. To the extent that these systems can handle a multiplicity of benefit and reimbursement arrangements, some of the problems described in this section will eventually be resolved.
2. Lack of data integrity. Until recently, the focus of claims processing operations was on the turnaround time for paying providers rather than on any statistical review of utilization patterns. In many instances, the data were grouped so arbitrarily as to eliminate the possibility of extracting useful information for actuarial or statistical studies. For example, at one HMO (see Case Study 3), all claims had to be classified into three categories: inpatient, outpatient, and other. Information on service location was missing (for example, emergency room, physician's office, and nursing home). Moreover, when a primary care physician provided services on both a capitated and self-referral basis during the same visit, the services had to be recorded as two separate encounters; a third encounter could result from the same visit if there were any charges for medical supplies. Because the standard reports from the claims system showed such visits as multiple encounters, any analysis of individual physician practice patterns was unreliable. In fact, in Case Study 3, actuarial projections could not be derived from the claims system; rather, they had to come from the data base of an outside consultant. (This consultant provided estimates based upon avarage costs and utilization rates across a series of clients.)
Some of the data integrity issues will be obviated with the purchase of new HMO software; others are a function of data collection and processing procedures that are independent of software design. To the extent that HMOs do not audit the performance of claims processors to ensure accuracy and consistency in data entry, data integrity problems may continue to go unrecognized in a number of plans.
A related issue concerns the noncomparability of data across HMOs for standard utilization measures, such as physician encounters per 1,000 members and hospital admissions or days per 1,000 members.
Some group and staff HMOs do not routinely record certain types of services, such as physician hospital visits, while others do not receive or record encounter information for capitated primary care services. Other plans, as previously noted, may have inflated or deflated visit counts or may arbitrarily collapse service location codes because of the design of their data systems. Also, data on out-of-plan use is often incomplete. 19 Thus,
Page 222
any comparison of utilization trends across plans requires a knowledge of their data classification procedures. 20
3. Lack of an integral role for the medical director at upper level HMO management. Many HMO medical directors are frustrated by their lack of input into HMO operations and their inability to obtain adequate budgets for professional support staff with appropriate statistical, utilization review, and quality assurance experience. In some cases, medical directors cannot reduce or deny payment to providers who are suspected of unusual billing practices or provision of unauthorized services. Depending on the plan, this authority may rest with the chief financial officer, the controller, or the director of provider relations. In HMOs with outmoded MIS, medical directors have expressed concern about their inability to obtain detailed utilization reports because of the priority attached by plan management to producing financial reports. As a result, medical directors may be unable to document poor practice patterns, even though they are aware of their existence; as a result, the entire peer review process suffers.
4. Lack of provider feedback. Provider relations suffer when there is a shortfall between the actual claims experience for an IPA and the projected experience used to calculate the IPA's capitation rate. This problem worsens when the withholding rate proves insufficient to cover the deficit. In control models in which the HMO processes all claims, IPA management cannot anticipate any shortfall and initiate corrective action unless timely utilization data are provided by the HMO. In Case Study 1, local physicians threatened to withdraw from the IPA unless the capitation rate was increased; without appropriate utilization data, the physicians refused to acknowledge that there had been any unnecessary provision of services or unusual billing practices.
The first three problems listed above are not unique to the HMO industry; indemnity carriers and Blue Cross and Blue Shield plans face the same concerns. Increasingly, the fourth problem—lack of provider feedback—is an issue for carriers and Blue Cross and Blue Shield plans, now that traditional fee-for-service coverage is giving way to preferred provider and closed panel arrangements. However, it is the potential for underservice in HMOs that has led to congressional concern about quality assurance in HMOs. However, as discussed in the case studies, many HMOs have failed to thrive precisely because the fee-for-service mentality continues to flourish in the prepaid sector.
Quality Assurance
In our experience, HMO management generally gives the highest priority to day-to-day marketing, underwriting, and financial operations and the lowest priority to programs, such as quality assurance, for which an
Page 223
immediate impact on plan performance is not evident. Additionally, given the understaffing and limited MIS capabilities in many HMOs, implementation of formal quality assurance programs may become problematic. For example, in certain plans, performance feedback to physicians is uneven because of inadequate data systems, poor data entry procedures, claims processing lags, and/or failure to classify claims data in a format useful to participating providers. Conversely, there may be little incentive for capitated IPAs, groups, and individual providers to supply timely or complete encounter data back to the HMOs, since their payment is generally based on the number of covered enrollees, not on the actual services rendered. As a result, the HMOs may be unable to determine actual utilization rates or to detect underservice.
Many HMOs have a two-stage approach to quality assurance. Initially, when signing up physicians (as individuals or through IPAs or groups), they use eligibility criteria to ensure the adequacy of the provider network. Thereafter, quality assurance generally consists of problem identification. The process may be fairly extensive, such as using target medical conditions or types of cases, such as hospital readmissions, as the basis for a periodic review of medical records. HMOs that conduct their own utilization review programs may also obtain feedback on provider performance from their staff. Alternatively, some plans may limit their quality assurance programs to tracking malpractice claims, grievance filings, and disenrollment rates by medical group or by primary care provider if they use individual gatekeepers.
In three-tier model plans, the HMO may require that participating groups or IPAs assume full responsibility for peer review. Network or group model HMOs typically require evidence of a functioning peer review program before they award a contract to a multispecialty practice. HMOs contracting with IPAs may require that a formal peer review system be in place, but since many IPAs lack a track record for judging physician performance, the adequacy of these programs cannot be assured.
Thus, operational reviews frequently disclose that there is a wide gap between quality assurance programs, as they are described in documents supplied to federal and state regulators, and as they actually exist within licensed health plans. Historically, structural measures have been notoriously poor indicators of both HMO performance and quality of care. For example, in California during the mid-1970s, licensing of prepaid health plans, with requisite filing of appropriate quality assurance protocols and provider contracts, did not prevent abuses in the state's prepaid Medicaid program. More recently, in the International Medical Centers, Inc. situation in Florida, structural measures failed to guarantee Medicare beneficiaries adequate access to medical services. The problem with structural measures was highlighted in a recent survey of HMOs in Ohio, as conducted
Page 224
by the Joint Commission on Accreditation of Health Care Organizations (JCAHO). In a review of six HMOs with Medicaid contracts, JCAHO surveyors found that none of the plans had fully implemented its quality assurance program. 21
Because of the limited scope of existing quality assurance programs, federal legislation now mandates review of inpatient and outpatient services provided by HMOs with Medicare risk contracts. External peer review organizations have begun using medical records and target medical conditions as indicators of the appropriateness of treatment, accessibility to services, and timeliness of care provided. The possibility of sanctions resulting from these reviews is now providing the impetus for HMOs to improve their quality assurance programs. For example, of the 15 HMOs in California, Hawaii, and Arizona with Medicare risk contracts, only 3 had fully implemented their quality assurance programs at the time of their initial evaluation by California Medical Review Inc. 22 Some HMOs have also begun to seek voluntary accreditation from external review organizations, such as JCAHO. However, because of the limited disclosure associated with mandatory and voluntary reviews, subscribers signing up with HMOs still have limited information available for evaluating quality of care within a given program.
Design and Use of Physician Incentives
In the preceding section, we looked at the operational problems impairing the administration of utilization management and quality assurance programs. As noted, structural and process measures are often an inadequate measure of plan performance. A similar situation exists for any evaluation of risk incentives. In this section we briefly describe the background on current concerns about risk incentives, the types of risk incentives that have been identified, and the factors that modify their impact on provider performance.
Background
In a report issued in July 1986, the General Accounting Office (GAO) identified three types of physician incentive plans with a potential risk of abuse for Medicare beneficiaries: (1) the Paracelsus or hospital model, in which a monthly bonus was paid to staff physicians on the basis of a favorable ratio of total hospital charges for Medicare patients to Medicare payments for those patients; (2) the Medical Staff-Hospital Joint Venture or the MeSH model, a theoretical model in which an annual bonus was to be paid to those physicians with a positive cost performance using targeted costs per discharge; and (3) the individual practice association model in
Page 225
which incentives, including primary care capitation arrangements, cover inpatient and outpatient services on an annual basis. The GAO report concluded by recommending that any incentive payment programs should average costs versus payments over a fairly large patient base to reduce incentives to undertreat individual patients; the GAO also recommended that the time period for calculating these incentives should be relatively long (1 year).
The Omnibus Budget Reconciliation Act of 1986 specifically prohibited hospitals, as well as HMOs with Medicare risk contracts, from using financial incentives to reduce or limit services provided to Medicare beneficiaries. Because of the widespread use of physician incentive payments by HMOs and CMPs, however, Congress delayed application of this provision to prepaid plans until April 1, 1989, pending further research. Subsequently, the Omnibus Budget Reconciliation Act of 1987 extended the delay to April 1, 1990, and new proposals in Congress make implementation unlikely.
To date, much of the published research on physician incentives has focused on documenting the range of arrangements that exist and the frequency with which they are used by plan model, plan age, plan size, and geographic location. With the exception of recent work by Mathematica Policy Research, Inc. 24 there has been little research on the effectiveness of quality assurance programs or the impact of financial incentives on utilization of services in HMOs.
Current Surveys Concerning Physician Incentives
Since the GAO report, there have been four additional studies on financial risk arrangements in HMOs: (1) the Group Health Association of America (GHAA) Survey mailed to GHAA member organizations in December 1986; 25 (2) a Blue Cross and Blue Shield Association Survey, using the GHAA survey instrument, was mailed in March 1987 to BC/BS plans that sponsored HMOs; 26 (3) a March 1987 survey mailed by Alan Hillman, to all 595 HMOs known to be in operation as of June 1986; 27 and (4) a survey of 215 federally qualified HMOs or CMPs, in combination with a review of documentation in the Office of Prepaid Health Care of the Health Care Financing Administration, was conducted by ICF, Inc. under contract with the U.S. Department of Health and Human Services. 28 The GAO has also conducted an additional study of physician incentives in response to a request by the Ways and Means Committee of the U.S. House of Representatives.
An analysis of the first three surveys revealed that consistent definitions were not used across the studies, leading to variations in findings as to the frequency with which these incentives have been used by various types of HMOs (that is, staff, group, network, IPA, and mixed or hybrid
Page 226
model plans.) In general, financial incentives were broken into four broad categories, as follows: (1) the basic approach to physician payment (that is, salary, capitation, and fee-for-service); (2) sharing of plan surpluses and/or deficits; (3) use of bonuses and/or withholds; and (4) distribution of funds by individual, group or combined individual-group performance.
While the three studies reported varying use of payment mechanisms and risk incentives by plan type, the single most important difference between the three related to the prevalence of financial incentives based on individual performance factors. The GHAA study found that 140 of 164 responding plans (85.4 percent) had some form of financial incentive for primary care physicians. Sixty percent of the plans reporting on the design of these incentives used some type of individual incentive; 11.2 percent reported exclusive use of individual incentives. The Hillman survey reported that two-thirds of all contractual arrangements (232 of 353) withheld a portion of payments to primary care physicians, but only 18 percent (38 of 211) of the HMOs held physicians at risk on an individual basis for deficits beyond the withhold. Although the ICF study did not separate reporting of withholds from other financial incentives, this study reported that 0.5 percent of responding HMOs relied solely on individual performance for the distribution of deficits and surplus funds. In a recent reconciliation of their findings, ICF and GHAA have concluded that in their common sample of 54 plans, individual physician incentives (including individual cost- or utilization-based withholds) were used in 20 percent of plans. 29
Administering Physician Incentives
Often, there is a discrepancy between risk incentives as defined in physician contracts and as administered by either the HMO, the IPA, or the group. The failure to implement risk incentives, according to contract terms, may reflect a conscious policy decision by management and/or operational difficulties. For example, one large network model HMO has reported that each month it withholds 10 percent from "an actuarially generous" capitation payment to participating multispecialty groups. The groups, however, record this withhold amount on their accounts receivable and anticipate the return of the funds. In the event of a deficit in any of the group's accounts because of unanticipated referral or ancillary service costs, the HMO would still return the withhold to maintain a good working relationship with the group.
The converse of this situation occurs when physicians automatically assume that the withhold will not be returned. The ICF study reported on one IPA HMO in which the withhold amount was seldom returned; the medical director stated that the withhold was not perceived as a financial incentive by the physicians but as a discount or as a business cost comparable
Page 227
to denied or suspended claims in the fee-for-service environment. We also found in several of our reviews that physicians respond to loss of the withholds by changing their billing patterns. For example, physicians may attempt to compensate for the withhold loss by inflating the CPT codes for consultations and office and hospital visits and by unbundling routine services, such as charging for component parts of blood chemistry panels.
In our experience, certain HMOs cannot readily detect inappropriate billing practices by individual physicians because of inadequate claims processing systems. In other cases, HMOs may control upcoding and un-bundling by specifying acceptable CPT codes for specific types of visits and/or procedures. Alternatively, HMO management may choose to ignore these billing practices, particularly when taking action may antagonize providers and lead to loss of their participation.
Sometimes risk incentives are short-circuited when an HMO cannot fulfill the terms of its contracts because of operational difficulties. For example, if an HMO has a claims processing backlog and cannot provide requested utilization reports according to a predefined schedule, the HMO may have to return all or part of the withholds, despite the existence of deficits in the physician accounts. For example, one carrier-sponsored HMO, described in Case Study 3, recently made a conscious decision to distribute 75 percent of all physician withholds despite deficits in existing risk pools and despite the knowledge that some primary care providers were self-referring excessively for specialty services not included in their own capitation rates. This management decision was based, in part, upon the fact that the HMO was unable to produce its utilization reports according to schedule and, in part, to placate participating physicians.
Finally, there are cases in which physicians may actually be unaware of any financial incentives related to effective utilization management. For example, in the situation described in Case Study 2, the salaried physicians were not informed during recruitment of a possible bonus based on plan performance. In this plan, utilization management was more a function of scheduling rather than of any financial incentives.
Thus, the issues to be addressed when reviewing the financial incentives within HMOs include the degree to which they have been fully implemented and the degree to which participating providers are fully aware of them. The Hillman, GHAA, and ICF survey instruments have focused on the design of contractual arrangements, but further research is needed to assess the ability of HMOs and CMPs to support these arrangements.
Policy and Research Issues
There is a whole body of literature involving analysis of utilization rates in HMO and fee-for-service settings. Another set of studies looks at
Page 228
utilization rates in different HMO settings (for example, comparisons of the performance of totally versus partly prepaid group practices and of IPAs versus totally or partly prepaid group practices). 30 There also has been a growing interest in utilization rates and outcomes for specific medical conditions in the two settings. 31
To date, health services researchers have assumed that differing financial incentives are responsible for the lower utilization rates in prepaid versus fee-for-service settings and have focused little attention on how HMOs achieve these reductions. 32 The literature on the delivery component of utilization management in HMOs consists largely of anecdotal reports detailing controls in place at specific plans and case studies involving one or more components of a utilization management program at a single HMO, IPA, or multispecialty group practice. For example, a recent report in the New England Journal of Medicine described one physician's negative experience working in a for-profit, staff model HMO. 33 Other studies have reported on the use of referrals or the impact of provider feedback on ordering of diagnostic tests in specific plans. 34
Our operational reviews suggest that the structure of utilization management and quality assurance programs and their actual implementation vary widely across plans. On-site evaluations of these programs are currently being conducted by mandatory and voluntary review organizations. Until the findings of these review organizations are made public, it will be difficult to generalize about which types of HMOs and which control models have implemented utilization management/quality assurance programs the most successfully. Moreover, if the findings from the reviews do not address where the responsibility for utilization management rests, it may be difficult to develop a policy response that can be used to ensure quality of care in HMOs.
It also should be stressed that a large number of HMOs are not subject to federally mandated review, as they do not participate in the Medicare risk program. As already noted, state licensing has tended to focus on structural measures, with on-site reviews across plans occurring infrequently or restricted to problem plans. Additionally, none of the voluntary or mandatory reviews is specifically designed to evaluate the impact of various types of risk incentives on provider performance.
The Hillman, GHAA, and ICF surveys described above looked at risk incentives from a structural perspective. Each of the three studies used the HMO as the unit of observation. The survey information on physician practices that is currently available from the American Medical Association, from state medical societies, and from the Medical Economics Company Inc. (Oradell, New Jersey) does not have sufficient detail to evaluate the financial impact of risk incentives by HMO plan type or control model. Thus, to better understand how financial incentives affect practice patterns,
Page 229
there may be a need to modify existing survey instruments or to undertake a separate study that focuses on primary care physicians with and without HMO affiliations. For HMO physicians, the future studies should evaluate (1) HMO model type, control model, geographic location, and enrollment; (2) the gross income of the primary care physician and overall patient volume, as compared with HMO patient income and volume; (3) the structure of HMO risk incentives and their financial impact on the responding physicians; and (4) the design and implementation of utilization management and quality assurance programs, as perceived by the responding physician.
The results of this survey can then be correlated with findings from outcome studies, consumer satisfaction surveys, and on-site reviews, as conducted by various regulatory agencies, peer review organizations, consumer or employer coalitions, and university-based research teams. Only then will it be possible to ascertain definitively which types of HMO financial incentives are the most problematic in terms of their impact upon quality of care. Until then, it is probably premature to develop legislation that eliminates the use of any particular form of financial incentives in the HMO setting.
Case Studies Introduction
The following case studies are not based on a representative sample of HMOs. We present them solely with the intent of showing the range of problems that may be encountered by HMOs when implementing utilization management programs. The background material at the beginning of each case study has been altered to maintain client confidentiality. All plans are defined as staff, group, or IPA, according to their operational characteristics, rather than their federal or InterStudy designation. The network category has intentionally been eliminated, as have any descriptors indicating location of the plan, plan age, nonprofit, or for-profit status. Size is defined by three categories: under 25,000, 25,000-49,999, and 50,000 and over. Also, any descriptors that might allow for identification of the plan, such as university affiliation, hospital ownership, Medicare risk status, or unique organizational characteristics, have been removed. However, the descriptions of the control type, the financial incentives, the design of the MIS, the role of the medical director, and the structure of the utilization management program are reported precisely as they were found in each of the plans.
Page 230
Case Study 1: Hospital-Sponsored Ipa
Background
In the mid-1980s, management of a hospital with 350+ beds decided to establish an IPA model HMO in order to contract with one of the major employers in the state; simultaneously, physician leadership at the hospital helped to set up an IPA, which was open to any active member of the hospital's medical staff. After the HMO became operational, membership climbed rapidly to the range of 25,000-49,999, with the growth exceeding original forecasts. However, the plan posted larger financial losses than anticipated because its operating and administrative procedures, along with its MIS, could not keep pace with the enrollment growth. The sponsoring hospital was forced to subsidize the health plan, both directly and indirectly, by underwriting the operating losses and by charging the plan a composite per diem that was actually below its own operating costs.
Eventually, the sponsoring hospital sought financial relief and asked the hospital system with which it was affiliated to take over the HMO. When the hospital system took over management of the HMO, it attempted to cut the financial losses through new reimbursement procedures and risk-sharing arrangements; as a result, there was a serious breakdown in provider relations.
Control Type
Three-tier, with the HMO controlling most services (Model 1).
Financial Incentives
Under the original risk model, physicians contracted with an IPA that was fully at risk for all inpatient and outpatient physician services, including outpatient mental health, ancillary, and in-area emergency services; durable medical equipment; prosthetic devices; and prescription drugs. The HMO allocated a flat monthly capitation rate per adult and per child member to the IPA; physicians submitted their claims directly to the HMO, with payment based on a predetermined fee schedule subject to a 20 percent percent withhold. The 20 percent withhold was used to fund an IPA reserve account, as well as to fund any deficits in a separate hospital fund.
The HMO also allocated a flat per-member, per-month amount to the hospital fund, which covered inpatient hospital and mental health services, same-day surgery, skilled nursing and home health care, and out-of-area emergency services. Providers rendering services covered by the hospital
Page 231
fund, including the sponsoring hospital, billed the HMO directly for their services according to prenegotiated rates. (There was no withhold for any services covered by the hospital fund.) Any deficits beyond the 20 percent physician withhold in either the IPA or hospital funds were the responsibility of the HMO, while any surplus in the hospital fund was to be allocated between the IPA reserve fund and the HMO on an 80-20 basis. The targeted utilization rate for all inpatient services was set at 350 days per 1,000 members; in 1985 and 1986, the actual hospital utilization, after adjusting for coordination of benefits, was approximately 300 days per 1,000 members.
While the IPA had historically operated at a loss because of overutilization in the outpatient setting, in 1985 and 1986, the plan was able to return the physician withhold because of the surplus in the hospital fund. Problems emerged, however, when the plan was taken over in 1987 and new management wanted to lower the targeted hospital utilization rate, to share surplus and deficits in the hospital withhold pool on a 50-50 basis, and to increase the per diem paid to the sponsoring hospital. The physicians recognized that they would no longer be able to anticipate a return of their withhold and asked the health plan to modify their capitation to reflect their actual utilization experience. The net result was a standoff between the doctors and the health plan.
Design of Mis System
The claims processing system was using ''first-generation'' software and was incapable of handling the volume of claims that were being received. As a result, there was an emphasis on rapid claims payment, without appropriate controls on data entry or claims review procedures.
There was no automatic linkage of the authorization files to the claims history files. Therefore, before any inpatient, emergency, durable medical equipment, or out-of-area claims were paid, they were sent to a nurse coordinator for approval. All other claims were entered directly into the claims system, and unless they were suspended for lack of a provider number or a duplicate payment, they were paid as billed according to the existing fee schedule. In other words, outpatient claims were paid without any automatic review of frequency of service, procedure coding, or consideration of whether the service was appropriate, given the diagnosis, age, or sex of the patient.
Utilization Management
Primary care physicians theoretically were to act as gatekeepers and to approve all specialty referrals and hospital admissions. In reality, patients
Page 232
continued to self-refer themselves to specialists. The primary care providers (PCPs) were not required to adhere to any protocols for authorizing the use of specialty or ancillary services, nor had any procedures been established for the management of high-cost patients.
PCPs were required to notify the HMO's medical director of pending hospital admissions for his approval. This procedure was generally well observed, because of the widespread recognition by IPA members of the financial impact of controlled hospital utilization on the IPA reserve fund. The surplus in the hospital fund, in effect, had allowed the IPA physicians to continue practicing on an "as usual" basis in the ambulatory setting.
With the HMO takeover, the physician leadership of the IPA was vehemently opposed to any changes in allocation of the hospital fund surplus and to the repricing of the hospital per diem. The IPA leadership believed firmly that participating physicians were delivering efficient care and did not want to use the withhold to cover IPA deficits. Meanwhile, HMO management believed that there was excessive utilization in the ambulatory setting. Neither side, however, had any documentation to support its argument, as the IPA did not collect claims data and the HMO had never produced any physician-specific data or developed any normative standards for evaluating physician performance in the outpatient setting.
Medical Director and Utilization Management Support Staff
The medical director reported that he had not been an integral member of top plan management but had been hired only part-time to oversee the nurse coordinators and to review pending hospital admissions. The utilization review staff did not have well-defined policies or procedures to guide them, particularly when adjudicating claims. As a result, claims payment was not consistent across reviewers (for example, the same services might be paid in some cases and denied in others).
Although the HMO had a written quality assurance plan, the nurses had little time to undertake chart audits or to review treatment plans for target conditions; instead, as much as 50 percent of their time was spent on clerical work associated with claims processing. While the nurse reviewers recognized that some IPA physicians regularly did not adhere to utilization review requirements, they did not have the authority to apply any penalties. Therefore, of approximately 100 physician infractions identified in 1987 involving the provision of medically unnecessary services or referrals to nonparticipating physicians, only two resulted in warning letters from the plan.
Page 233
Case Study 2: Group-Model Hmo
Background
In 1985, a multispecialty group practice, which contracts primarily with one group-model HMO, expanded its operations into two metropolitan areas where, historically, fee-for-service providers had been highly resistant to participation in any form of managed care (i.e., HMOs or preferred provider organizations [PPOs]). The move into the other communities was made at the request of several large public and private employers anxious to have an alternative to fee-for-service medicine. Membership at the new sites grew rapidly. At the end of 2 years, membership size far exceeded HMO projections, and the medical group found that they had outgrown their facilities at the two sites. Also, recruitment of additional professional and administrative staff was not feasible until the practice sites could be expanded (membership size cannot be specified, per client request).
To ensure appropriate levels of care at the expansion sites, group physicians began referring patients out on a fee-for-service basis into the community for primary, specialty, and ancillary services that ordinarily would have been provided in-house. Lacking contracts with most of the local specialists, the group was forced to pay for these referrals from its capitation fund on the basis of billed charges. Because of the lack of cost controls over these outside referrals, the group sustained operating losses at the expansion sites in 1986 and 1987.
Control Type
Three-tier, with delivery of services controlled by the medical group (Model 3).
Financial Incentives
With the exception of the medical director in each of the two sites and one practicing physician per site, the rest of the physicians at the expansion sites had no prior experience working for the group. The newly hired physicians had a 3-year probationary period before they became eligible for partnership benefits; in the interim they were paid a fiat salary with no productivity incentives. Salary levels were based on specialty training, board certification, and prior practice experience. There also was a profit-sharing program in which partners were eligible to participate; theoretically, the new hires were eligible for a year-end bonus, but only if the group had a profitable year. However, knowing the operating losses sustained by the
Page 234
group, the medical directors generally did not include any mention of a bonus in salary discussions with new recruits.
Design of Mis System
The MIS in place at the original practice sites had been designed to support the group's own internal data needs. This system had not been built to track or adjudicate fee-for-service claims from outside providers, under the assumption that the amount of care provided in the fee-for-service sector would be very limited. (At its main site, outside physician bills were reviewed manually, with payment made according to prenegotiated rates and authorized services.) When the expansion sites were opened, the group purchased software to allow for tracking of referral and hospital authorizations and for collection of information on fee-for-service claims, using standard CPT codes. However, fee caps or fee schedules were not installed in the system, and clinical edits, which determine whether procedures had been appropriately billed given the patient's age, sex, or diagnosis, were not activated. Thus, as long as a preauthorization for a referral existed in the new MIS, claims from community-based physicians were paid, without questioning the need for billed services or the use of specific CPT codes.
Utilization Management
The primary factor controlling outpatient utilization at each of the practice sites was the scheduling process. Each salaried physician was scheduled for a set number of morning and afternoon patient sessions per week, with a predetermined number of time slots allotted for acute-care patients, continuing patients, and physical examinations. As membership soared, the primary care physicians were unable to schedule specialty care within the group or handle conditions requiring intensive, short-term follow-up care on a timely basis, given the overbooking that was already taking place. As a result, they began to refer out into the community cases that ordinarily could have been handled in-house.
When outside referrals were authorized, there was no dollar limitation placed on the services to be provided, nor was the level of care specified (that is, type of consultation or office visit, by CPT code). The only requirement was that certain laboratory and x-ray tests be performed at the groups facilities; additionally, any surgical procedures or hospital admissions required another preauthorization. Aggregate reports summarizing referral rates and costs, by group physician, were received monthly by the medical directors, as were summaries on the number of patients seen and billed charges from each outside provider. However, none of this information
Page 235
was provided to the group physicians or their support staffs. Thus, there was no consensus among the group physicians and the referral clerks as to which local providers were the most cost-efficient, in terms of future referrals.
Medical Director and Utilization Management Support Staff
Both of the medical directors devoted approximately 50 percent of their time to their clinical practices and appeared to have taken on the management role with some reluctance. Neither had worked with their medical staffs to develop referral protocols or had undertaken any educational efforts to make them aware of referral costs by specialty. Moreover, both medical directors were extremely fearful about undertaking any program that would antagonize local physicians; thus, they did not encourage any claims review that would result in fee cutbacks by eliminating billing abuses or by using a fee schedule. Rather, the intent of the medical directors was twofold: to initiate preferred provider contracting with the specialists identified as being the most cost efficient and to internalize the high-volume specialties as quickly as possible to control the dollar outflow. However, the plan's ability to recruit specialty staff was dependent, in part, on its ability to expand its existing facilities and/or develop new clinical sites.
Case Study 3: Carrier-Sponsored Hmo
Background
In the mid-1980s, a carrier took over an existing IPA model HMO operation that had a number of start-up sites. The computer system that was in place was inadequate to handle the variations in benefit packages across sites, as well as the different payment mechanisms used to reimburse hospitals and physicians. Because of the losses sustained at most of the HMO sites and the costs associated with upgrading the HMO software and developing new products (that is, triple option or a point-of-service HMO), the carrier decided to evaluate the future of each HMO site. The following description relates to one of the sites with fewer than 25,000 enrollees.
Control Type
Three-tier, with control resting with the HMO (Model 1).
Page 236
Financial Incentives
Participating primary care providers received a monthly age- and sex-adjusted capitation payment for a CPT-coded list of services; this payment was subject to a 20 percent withhold (that could be increased to 30 percent, under specific conditions). Primary care physicians retained the right to self-refer for services not covered under the capitation agreement. The individual PCPs were then grouped into pods or arbitrary physician incentive pools with a minimum of at least 1,000 members; the withholds of all PCPs in each pod were then combined. For each pod, there was a separate referral services budget to cover the costs for specialty, hospital, and ancillary services; this payment was based upon the number of members in the pod, adjusted for their age and sex mix.
Specialists were paid out of the referral services budget, according to the 70th percentile of usual and customary rates, subject to a withhold. Hospitals were paid according to diagnosis-related groups (DRGs) or discounted charges, but not per diems. During the calendar year, if there were deficits in the referral services fund, the overrun was to be made up first through withholds in the specialist pool and then through withholds in the primary care pool, and finally, any remaining deficits were the responsibility of the carrier. Individual stop-loss coverage from the carrier protected the PCP from responsibility for charges in excess of $7,000 per calendar year.
Despite the ability of the HMO to penalize physicians for poor performance, there was a strong fear by plan management of antagonizing primary care doctors and losing their participation in the plan. Thus, for calendar years 1986 and 1987, a corporate decision was made to return 75 percent of the physician withholds at each of the HMO sites, regardless of the extent of deficits in the referral services funds.
Design of Mis System
The hardware and software were inadequate to support membership size, leading to a backlog of claims in excess of 20 days for the HMO site as of December 31, 1987. Moreover, at any given time, the number of unentered claims and their dollar value were unknown. Once a claim was entered into the system, there were minimal edits to allow processors to detect inappropriate or unnecessary services or unusual billing practices by referral physicians.
From a statistical perspective, the information that came off the claims system was suspect. For example, if a PCP submitted a bill that included both capitated services and specialty care (for a self-referral), two encounter numbers had to be generated; if supplies, reimbursable on a cost basis, were also included in the billing, a third encounter form was generated. Thus,
Page 237
the reports on cost per PCP encounter were unreliable. Another example related to classification of claims by location of service. All claims had to be grouped into one of three categories: inpatient, outpatient, or other. As a result, nursing home expenses could not be easily separated out from hospital expenses, while home health care expenses, for example, could not easily be separated from those for physical and occupational therapy. As reported by the executive director at the local site, the system was designed strictly to allocate costs to the pods and to calculate withholds.
Utilization Management
There were no data by pod on patient demographics and no analysis of utilization patterns within pods to determine where or why deficits were occurring. In effect, there was no way to evaluate the performance of individual PCPs, except in terms of expenditures for self-referrals and outside referrals. Yet, the physicians in the pod were supposed to be self-disciplining. Their contract, however, did not specify the mechanics of any review process, nor did it define how a poorly performing physician could be removed from a pod.
Medical Director and Utilization Management Support Staff
At the local level there was a part-time medical director who largely handled physician and hospital contracting. Utilization review was handled by three nurses who functioned as patient care coordinators. They received all incoming calls for the authorization of hospital admissions, and depending upon the case and available time, they were responsible for conducting on-site concurrent review. The three nurses were also supposed to authorize referrals for some 20 high-cost diagnostic tests and procedures, such as use of magnetic resonance imagers and lithotripters. However, a number of PCPs regularly ignored this requirement, knowing that the plan had no intent of closely monitoring their behavior. In fact, other than the initial credentialing process, there was no quality assurance program in place.
Case Study 4: Carrier-Sponsored Hmo
Background
A carrier established an IPA model HMO which then contracted with a series of open panel IPAs. Each IPA was responsible for delivering care in one or two counties of the state. The HMO provided all marketing, administrative, enrollment, accounting, financial, claims processing, and
Page 238
MIS services for the IPAs. Under its contract, it was also responsible for supplying the IPAs with necessary data and reports to enable the IPAs to perform peer review, to operate a quality assurance program, and to determine the status of withhold accounts.
Problems arose when one of the IPAs discovered that it was operating at a deficit and requested an increase in its monthly capitation rate. The physicians in this IPA were convinced that the deficits were attributable to three problems: (1) the HMO's use of outmoded actuarial information, leading to an underestimation of outpatient costs and a miscalculation of the capitation payment to the IPA; (2) the miscoding or misclassification of claims data, preventing a meaningful comparison between capitated payments and actual claims costs; and (3) the failure of the HMO to provide the IPA with detailed financial and utilization reports on a timely basis. This case study examines the experience of this one IPA.
Control Type
Three-tier, with control resting with the HMO (Model 1).
Financial Incentives
The HMO allocated to the IPA capitation on a per-member, per-month basis (not adjusted by age or sex), with the HMO processing all hospital and professional claims. Claims from participating IPA physicians were to be paid by the HMO according to the lesser of billed charges or a maximum fee schedule. This schedule was approximately 10 percent higher than the sponsoring carrier's schedule for its standard business. Twenty percent of all physician's fees were to be withheld and placed in a risk account.
The IPA required enrolled members to sign up with a primary care physician, but did not actively support a gatekeeper system. Patients could self-refer to participating specialists. Authorizations for hospital admissions could be requested by primary care physicians or treating specialists. Moreover, there were no built-in financial incentives for performing the gatekeeper function. For example, the IPA did not allocate any percentage of funds in the withhold to primary care physicians, but distributed the funds on a pro-rata basis across the entire IPA membership.
Design of Mis System
Only management reports, not claims processing procedures, were reviewed. By April 30 of each year, an annual financial accounting was due, showing all capitation payments to the IPA for covered services and all billed and paid services adjusted for incurred but not reported claims;
Page 239
from this accounting, the HMO would determine whether any or all of the physician withhold would be available to the IPA for distribution to participating physicians.
The reports received from the HMO in April 1986 indicated that the IPA did not have an operational deficit, and, therefore, the 1985 withhold was returned and the amount of the withhold was decreased from 20 to 10 percent. IPA leadership continued to believe that the IPA was operating profitably until the end of the year, when the HMO reported a substantial deficit in the IPA account, requiring an increase in the withhold.
Apparently, during the year the HMO had experienced a buildup in unpaid claims, resulting in a miscalculation of the incurred but not reported claim and a restatement of the IPA's financial position. At the same time, the IPA was not receiving adequate information from the HMO to develop any estimates of its own performance. For example, while the HMO provided monthly totals on admissions per 1,000 members and the average length of stay per discharge, there was no financial information on average cost per patient-day or per discharge, by type of service, or by diagnosis. Detailed information on cost per patient visit and average cost per procedure was not provided to the IPA prior to the announcement of the IPA's operational deficit.
The capitation shortfall was attributed in part to the fact that the HMO was predicating utilization rates on statistics presented by outside actuarial consultants; however, the data classification system in place at the HMO did not correspond to that used by the outside consultants. For example, laboratory and x-ray costs were allocated differently in the two systems, resulting in an underestimation of the cost of outpatient services in the capitation payment.
Utilization Management and Support Staff
For all hospital admissions, the admitting physician was to call the utilization review department at the HMO for preauthorization. The appropriateness of the admission and the site (inpatient versus outpatient) was not questioned initially by the staff, but rather was reviewed retrospectively. Nurses at the HMO were responsible for conducting concurrent utilization review by phone and/or handling on-site reviews. An additional team of one physician and two nurses handled all psychiatric admissions.
For outpatient services, the claims were screened by processors at the HMO by using a series of routine edits to detect duplicate billings, noncovered services, medically outmoded services, and services covered by total charges. Otherwise, there were no screens to review the frequency of services or upgrading of procedure codes. Individual claims were not subject to special review unless physicians contested not getting paid for all
Page 240
services rendered. There were no reports issued on a regular basis (that is, monthly or quarterly) listing physicians who routinely billed for more services per visit or had higher costs per visit than the IPA average—or the average across all participating IPAs. There was no separate tracking of ancillary services with respect to volume and dollar amounts, by referring or treating physician.
Approximately every 6 months, on an "as-needed basis," there was a joint meeting of IPA leadership and the HMO medical director and review staff to resolve outstanding problems. Actions of that committee typically included a determination of which physicians were utilizing nonparticipating providers and/or failing to notify the HMO of inpatient admissions. The IPA was then authorized to levy a $100 fine against noncomplying physicians; over a 2-year period, approximately 12 fines were issued. Otherwise, the combined HMO-IPA review team, which theoretically was responsible for quality assurance activities, did not undertake any analysis of member grievances, incident reports, admissions by diagnosis, or mortality rates.
Medical Director and Utilization Management Support Staff
There was a nominal flow of information down to the IPA from the medical director and his support staff at the HMO. As a result, physicians participating in the IPA continued to practice under fee-for-service incentives. The medical director of the IPA, along with the leadership of the IPA, had never supported an active utilization management program. For example, using annual information produced by the HMO on the distribution of office visits by specialty, the medical director had never sought to review the practice patterns of individual physicians identified as being in the top 25 percent by cost per visit. He had not worked with IPA leadership to develop protocols to curb unnecessary ordering of ancillary services and diagnostic testing or to foster the use of outpatient surgery. Rather, the focus of the IPA's management—and the medical director—had been directed to renegotiation of the capitation payment to eliminate the IPAs operational deficit.
Case Study 5: Physician-Sponsored Ipa
Background
A physician-owned IPA model HMO with under 25,000 members and a panel of more than 1,000 physicians had consistently reported operating losses since its founding in the mid-1980s. In 1987, it was reported to be out of compliance with the capital reserve requirements of the state's insurance department. Accordingly, the IPA sought to determine how best to obtain
Page 241
an immediate infusion of funds. Two primary sources had previously been identified: additional contributions from participating physicians or a loan from one or more local hospitals. However, the analysis revealed that the physicians were quickly becoming disenchanted with the plan and were unlikely to contribute additional monies, while the hospitals were not anxious to loan money unless the operational expenses of the plan could be brought under control.
Control Type
Two-tier, with control resting with the HMO (Model 1).
Financial Incentives
The physician shareholders in the plan each originally contributed between $600 and $1,750 to finance the plan's start-up. The HMO has operated on a discounted fee-for-service basis, with reimbursement predicated upon the 85th percentile of the customary and reasonable rates used by carriers operating in the local market. After the first full year's experience, these rates were reviewed and adjusted downward to control operating costs. In addition, the plan retained 20 percent of paid charges as a withhold; this withhold was not returned after the initial year of operation, but was returned after the second year as a good faith effort on the part of the IPA leadership.
There were no other incentives in this plan other than the discounted fees and the withhold. Participating physicians who were interviewed felt that the withhold had no impact on utilization patterns in terms of frequency of office visits, ordering of ancillary services, or use of referrals. In fact, with the discounted fee arrangement, some primary care physicians noted that it was more cost-efficient to refer difficult or time-consuming patients to a specialist in order to maintain the patient flow within their own offices.
Because of the failure of the withhold to control utilization, plan management is now considering a preestablished budget by practice type or specialty; under this approach, a percentage of the premium will be designated to cover specific services (for example, family practice, obstetrical care, surgery, and allergy), with a reserve fund created from the premium allocation. Payback of this withhold would be based upon the combined experience of the specialties covered under each withhold.
Design of Mis System
The claims processing section was originally under the jurisdiction of the chief financial officer, who had no previous experience with a claims
Page 242
operation. As a result, the operation was poorly managed find understaffed, resulting in low morale, high employee turnover, and periodic claims lags. As for the claims system, the existing hardware was adequate to support the membership size, but the software lacked the necessary edits to detect unusual physician billing practices as well as a flexible report writer to produce reports according to management specifications.
Utilization Management
The primary care physician functioned as a gatekeeper and in that capacity was responsible for completing referral forms for all specialty, ancillary, and hospital services. Once an authorization was entered into the system, all claims were automatically paid without review, except for emergency room visits, mental health services, physical therapy, speech and occupational therapy, out-of-area claims, and out-of-plan referrals.
Because the IPA was originally established by the leaders of several local medical societies and/or hospital boards and because these individuals collectively represented the medical establishment in their communities, there was a reluctance on the part of the nurse reviewers to challenge participating physicians regarding their practice patterns. This problem was further compounded by the fact that there were few or no data with which to document consistent patterns of overutilization of services or unnecessary admissions.
The plan had two medical directors; one was largely responsible for utilization review and the other was responsible for physician relations and for recruiting primary care physicians for outlying areas. To date, the approach to utilization management has been through gentle persuasion, rather than tightly written protocols. However, the failure of the plan to bring utilization rates down (for example, to lower hospital utilization under 375 days per 1,000 members for the under age 65 population) has resulted in a decision to implement a more stringent review process.
Ipa Management
The same chief executive officer has remained in place since the plan was founded. However, within the first year of its operations, the plan lost its original chief financial officer, its director of management information systems, its director of claims, its nursing supervisor (who was responsible for quality assurance), and several other key administrative staff. There continues to be a high degree of tension between the physician leadership of the IPA and its lay management. One area of major conflict has been over underwriting practices. Plan management had established a policy of not accepting groups with fewer than 25 employees because of potential high
Page 243
utilization. However, the IPA board of directors overruled management and decreed that participating physician offices and families were eligible for HMO membership. The offering was also extended to members of the local medical societies. Despite evidence to show that the physician offices had been high utilizers, the IPA physicians continued to overrule plan management.
Notes and References
1. Page, Leigh, ''New Era in Utilization Review,'' American Medical News, Vol. 1, December 9, 1988, pp. 48-49. (See also Scheier, Ronni, "Medicine by the Book," American Medical News, January 6, 1989, pp. 1, 20).
2. U.S. General Accounting Office, Medicare Issues Raised by Florida Health Maintenance Organization Demonstrations, Report to Congress, GAO/HRD-86-97, Washington, DC, July 1986.
3. U.S. Congress, House, Maintaining Medicare's HMOs: Problems, Protections, and Prospects, Hearing before the Select Committee on Aging, 100th Congress, First Session, Washington, DC, June 11, 1987.
4. U.S. General Accounting Office, Medicare: Physician Incentive Payments by Hospitals Could Lead to Abuse, Report to the Chairman, Subcommittee on Health, Committee on Ways and Means, U.S. House of Representatives, GAO/HRD-86-103, Washington, DC, July 1986.
5. Trauner, Joan B., "The HMO Identity Crisis." Best's Review 87, April 1987, pp. 60-70.
6. The Group Health Association of America's 1988 analysis of HMO industry performance, using 1986 survey data, showed that 39.2 percent of 181 plans submitting financial data had a profit or surplus. Of the HMOs that we reviewed, 25 percent were profitable in 1986. See Group Health Association of America, Inc., HMO Industry Profile: Financial Performance, Vol. 3, Washington, DC, September 1988.
7. In a study of physician incentives in HMOs, ICF researchers noted that they were unable to check the consistency or accuracy of information supplied by the plans. They also noted that information on file at the federal Office of Prepaid Health Care (OPHC) was not always reliable; in some cases, financial incentive arrangements contained in applications for federal qualification had never become operational, and in other cases, design of incentives had changed without being reported to OPHC. ICF, Inc., Final Report: Study of Incentive Arrangements Offered by HMOs and CMPs to Physicians, Submitted to the Office of the Assistant Secretary for Planning and Evaluation, Department of Health and Human Services, Washington, DC, May 18, 1988, p. II21.
8. InterStudy, The InterStudy Edge, Excelsior, MN, Spring 1988, p. 54.
9. For a different approach, when traditional community- or foundation-based IPAs are contrasted with newer group-based IPAs, see Welch, W. P., "The New Structure of Individual Practice Associations, Journal of Health Politics Policy and Law, Vol. 12, Winter 1987, pp. 723-739.
10. ICF, Inc., Final Report, p. IV-6 (see note 7 above).
11. Gnessin, Alan M., "Physician Incentive Payment Systems and Risk Sharing Alternatives," in Group Health Association of America, Inc., Physician Incentive Programs: Defining the Risk, Washington, DC, October 28-30, 1987.
12. For a description of an HMO in which individual physician incentives are used within pods, see the statement by Jerome Beloff, Corporate Medical Director, Av-Med Health
Page 244
Plan of Florida before the Physician Payment Review Commission, Washington, DC, July 15, 1988.
13. Gnessin, Alan M., "Physician Incentive Payment Systems and Risk Sharing Alternatives," 1987 (see note 11 above).
14. Wilensky, Gall R., and Rossiter, Louis E, "Patient Self-Selection in HMOs," Health Affairs, Vol. 5, Spring 1986, pp. 66-80. For a more recent study showing the impact of dependents' claims on health plan selection see Lairson, David R., and Herd, J. Alan, "The Role of Health Practices, Health Status, and Prior Health Care Claims in HMO Selection Bias," Inquiry, Vol. 24, Fall 1987, pp. 276-284.
15. Neipp, Joachim, and Zeckhauser, Richard, "Persistence in the Choice of Health Plans," Advances in Health Economics and Health Services Research, Vol. 6, 1985, pp. 47-72.
16. Borok, Gerald M., "Appropriate Utilization of Resources Program," Quality Assurance and Utilization Review, Vol. 2, May 1987, pp. 57-61.
17. Donabedian, Avedis, "Explorations in Quality Assessment and Monitoring," The Definition of Quality and Approaches to Its Assessment, Vol. I, Ann Arbor, MI: Health Administration Press, 1980.
18. Mosser, Gordon, "Quality Assurance in HMOs," Presentation to Management and Physician Orientation Program, Group Health Association of America, Inc., New Orleans, December 9-11, 1987.
19. For a discussion of 15 ways in which out-of-plan use may occur, see Mott, Peter D., "Hospital Utilization by Health Maintenance Organizations: Separating Apples from Oranges," Medical Care, Vol. 24, May 1986, pp. 398-406.
20. For a discussion of the process used by the Rand Corporation to impute mental health visits and expenditures at one large HMO (Group Health Cooperative of Puget Sound), see Wells, Kenneth, Manning, Willard Jr., and Benjamin, Bernadette, "Comparison of Use of Outpatient Mental Health Services in an HMO and Fee-for-Service Plans: Sensitivity to Definition of a Visit," Medical Care, Vol. 25, September 1987, pp. 894-903.
21. Joint Commission on Accreditation of Health Care Organizations, Report of the Findings of the Joint Commission's Quality Assurance Evaluation and Medical Records Audits of Health Maintenance Organizations in Ohio under the Medical Assistance Program, Submitted to the Bureau of Alternative Delivery Systems, Ohio Department of Human Services, December 1987.
22. Conversation with Jo Ellen Ross, Chief Executive Office, California Medical Review Inc., San Francisco, January 17, 1989.
23. U.S. General Accounting Office, Medicare: Physician Incentive Payments, Washington, DC, July 1986.
24. Mathematica Policy Research, Inc., National Medicare Competition Evaluation, Final Analysis Report: The Structure of Quality Assurance Programs in HMOs and CMPs Enrolling Medicare Beneficiaries, Washington, DC, February 1987.
25. Gold, Marsha and Reeves, Ingrid, "Preliminary Results of the GHAA-BC/BS Survey of Physician Incentives in Health Maintenance Organizations (HMOs)," Group Health Association of America, Inc., Research Briefs, Vol. 1, November 1987, pp. 1-15.
26. Findings from the BC/BS survey have been used to augment the GHAA survey, with duplications removed. For the BC/BS results, see Blue Cross and Blue Shield Association, "A Survey of Physician Financial Payment Arrangements in Blue Cross and Blue Shield Plan HMOs," Chicago, January 1987.
27. Hillman, Alan, "Sounding Board: Toward Full Disclosure of Referral Restrictions and Financial Incentives by Prepaid Health Plans," New England Journal of Medicine, Vol. 317, December 31, 1987, pp. 1743-1748.
Page 245
28. ICF, Inc., Final Report (see note 7 above).
29. Memorandum from Lewin/ICF, Inc. and Group Health Association of America to Chris Bladen, Division of Health Financing Policy, U.S. Department of Health and Human Services, Washington, DC, June 24, 1988.
30. For a review of early research studies on utilization rates in HMO and fee-for-service settings and across HMOs, see Luft, Harold S., Health Maintenance Organizations: Dimensions of HMO Performance, New York: Wiley, 1981.
31. See, for example, Yelin, Edward H., Henke, Curtis J., Kramer, Jane S., Nevitt, Michael C., Shearn, Martin, and Epstein, Wallace V., "A Comparison of the Treatment of Rheumatoid Arthritis in Health Maintenance Organizations and Fee-for-Service Practices," New England Journal of Medicine, Vol. 312, April 11, 1985, pp. 962-967. Also see Quick, Jonathan D., Greenlick, Merwyn R., and Roghmann, Klaus J., "Prenatal Care and Pregnancy Outcome in an HMO and General Population: A Multivariate Cohort Analysis," American Journal of Public Health, Vol. 71, April 1981, pp. 381-390.
32. For a study that assumed that the differential use of diagnostic testing was due to its increased profitability to fee-for-service providers, see Epstein, Arnold M., Begg, Colin B., and McNeil, Barbara J., "The Use of Ambulatory Testing in Prepaid and Fee-for-Service Group Practices: Relation to Perceived Profitability," New England Journal of Medicine, Vol. 314, April 24, 1986, pp. 1089-1094.
33. Scovern, Henry, "Hired Help: A Physician's Experiences in a For-Profit Staff-Model HMO," New England Journal of Medicine, Vol. 319, September 22, 1988, pp. 787-790.
34. For an example of a discussion on referral patterns, see Piland, Neil E, White, Robert E., and Smith, Howard L., "Physician Referral Patterns: Implications for Group Practice," GHAA Journal, Vol. 7, Winter 1986, pp. 4-12. For an example of a discussion on provider feedback, see Berwick, Donald M., and Coltin, Kathryn L., "Feedback Reduces Test Use in a Health Maintenance Organization," Journal of the American Medical Association, Vol. 255, March 21, 1986, pp. 1450-1454. See also Braham, Robert L, and Ruchlin, Hirsch S., "Physician Practice Profiles: A Case Study of the Use of Audit and Feedback in an Ambulatory Care Group Practice,'' Health Care Management Review, Vol. 12, 1987, pp. 11-16.









































